cb71effcd37415479c87b773bb040ea6.ppt
- Количество слайдов: 34
 Interpretation of Neuropsychological Information Overview • What is a deficit? – Estimating Pre-injury function – Deficits on a Single Test – Patterns of Deficits on Multiple Tests • Integrating Test Data with other clinical information
Interpretation of Neuropsychological Information Overview • What is a deficit? – Estimating Pre-injury function – Deficits on a Single Test – Patterns of Deficits on Multiple Tests • Integrating Test Data with other clinical information
 Is there a deficit? Normative Standard • Readily defined as binary • Low-level functions Arousal Orientation Speech Finger Movement Deficit Coma Confused Mute Paralyzed Normal Awake Oriented Speaks Moving
Is there a deficit? Normative Standard • Readily defined as binary • Low-level functions Arousal Orientation Speech Finger Movement Deficit Coma Confused Mute Paralyzed Normal Awake Oriented Speaks Moving
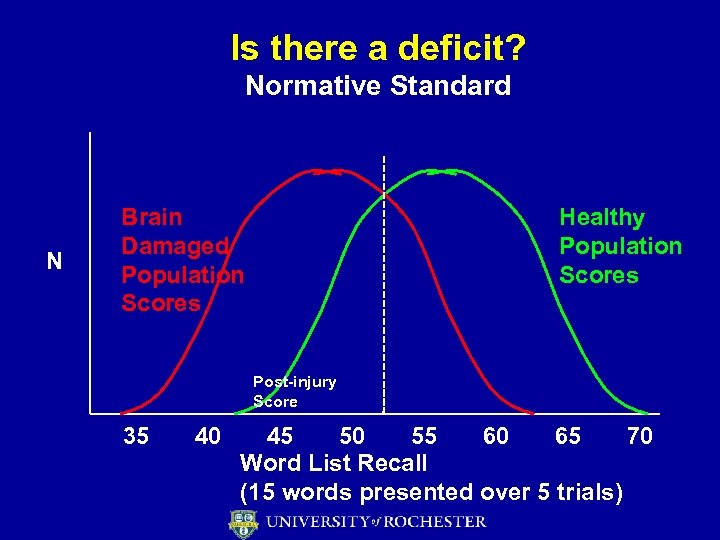 Is there a deficit? Normative Standard N Brain Damaged Population Scores Healthy Population Scores Post-injury Score 35 40 45 50 55 60 65 70 Word List Recall (15 words presented over 5 trials)
Is there a deficit? Normative Standard N Brain Damaged Population Scores Healthy Population Scores Post-injury Score 35 40 45 50 55 60 65 70 Word List Recall (15 words presented over 5 trials)
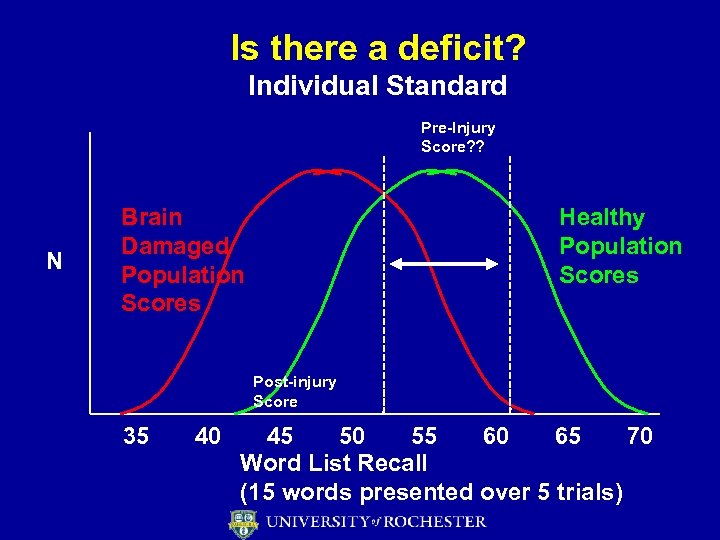 Is there a deficit? Individual Standard Pre-Injury Score? ? N Brain Damaged Population Scores Healthy Population Scores Post-injury Score 35 40 45 50 55 60 65 70 Word List Recall (15 words presented over 5 trials)
Is there a deficit? Individual Standard Pre-Injury Score? ? N Brain Damaged Population Scores Healthy Population Scores Post-injury Score 35 40 45 50 55 60 65 70 Word List Recall (15 words presented over 5 trials)
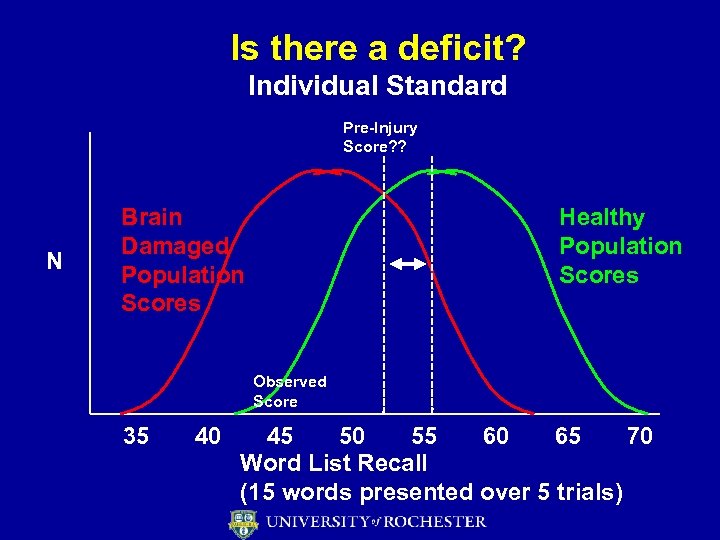 Is there a deficit? Individual Standard Pre-Injury Score? ? N Brain Damaged Population Scores Healthy Population Scores Observed Score 35 40 45 50 55 60 65 70 Word List Recall (15 words presented over 5 trials)
Is there a deficit? Individual Standard Pre-Injury Score? ? N Brain Damaged Population Scores Healthy Population Scores Observed Score 35 40 45 50 55 60 65 70 Word List Recall (15 words presented over 5 trials)
 Estimating Pre-Injury Abilities • Pre-injury data – Standardized educational tests (Iowa, SAT, GRE) – Academic record • Post-injury data – – – Demographics Fund of vocabulary Best performance method Reading irregular words Combined reading and demographics
Estimating Pre-Injury Abilities • Pre-injury data – Standardized educational tests (Iowa, SAT, GRE) – Academic record • Post-injury data – – – Demographics Fund of vocabulary Best performance method Reading irregular words Combined reading and demographics
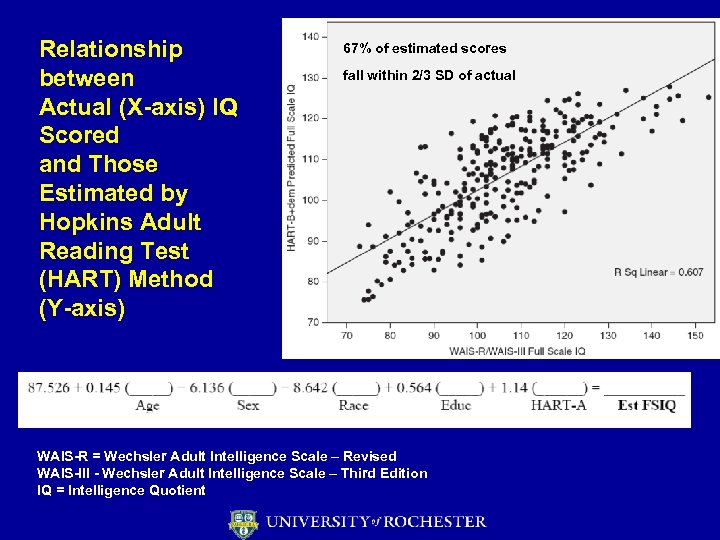 Relationship between Actual (X-axis) IQ Scored and Those Estimated by Hopkins Adult Reading Test (HART) Method (Y-axis) 67% of estimated scores fall within 2/3 SD of actual WAIS-R = Wechsler Adult Intelligence Scale – Revised WAIS-III - Wechsler Adult Intelligence Scale – Third Edition IQ = Intelligence Quotient
Relationship between Actual (X-axis) IQ Scored and Those Estimated by Hopkins Adult Reading Test (HART) Method (Y-axis) 67% of estimated scores fall within 2/3 SD of actual WAIS-R = Wechsler Adult Intelligence Scale – Revised WAIS-III - Wechsler Adult Intelligence Scale – Third Edition IQ = Intelligence Quotient
 Is there a deficit? What is a difference that makes a difference? • Sources of test score differences – True difference, reflecting brain damage – Less-than-perfect reliability of the test (error variance) – Patient factors – Effort – Alertness – Random variability » Number of items » Standardization of test administration » Environmental distraction
Is there a deficit? What is a difference that makes a difference? • Sources of test score differences – True difference, reflecting brain damage – Less-than-perfect reliability of the test (error variance) – Patient factors – Effort – Alertness – Random variability » Number of items » Standardization of test administration » Environmental distraction
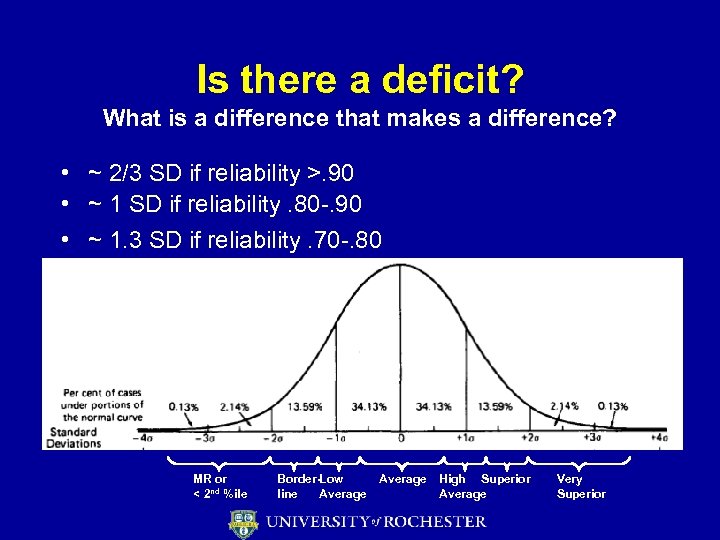 Is there a deficit? What is a difference that makes a difference? • ~ 2/3 SD if reliability >. 90 • ~ 1 SD if reliability. 80 -. 90 • ~ 1. 3 SD if reliability. 70 -. 80 MR or < 2 nd %ile Border-Low line Average High Superior Average Very Superior
Is there a deficit? What is a difference that makes a difference? • ~ 2/3 SD if reliability >. 90 • ~ 1 SD if reliability. 80 -. 90 • ~ 1. 3 SD if reliability. 70 -. 80 MR or < 2 nd %ile Border-Low line Average High Superior Average Very Superior
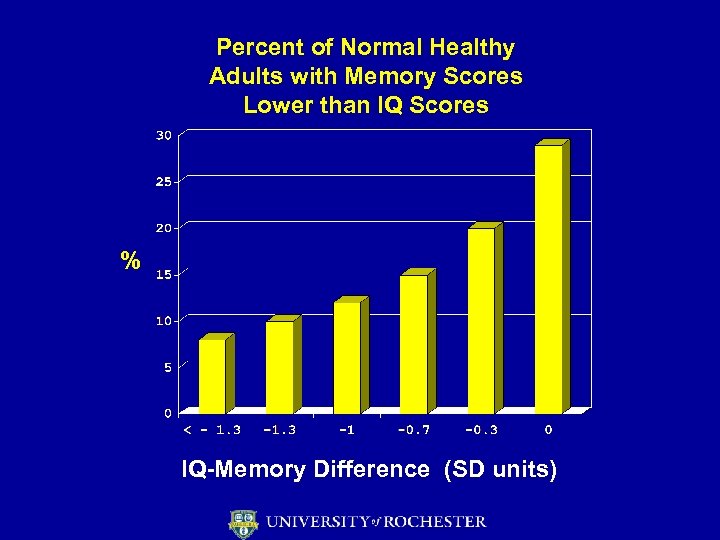 Percent of Normal Healthy Adults with Memory Scores Lower than IQ Scores % IQ-Memory Difference (SD units)
Percent of Normal Healthy Adults with Memory Scores Lower than IQ Scores % IQ-Memory Difference (SD units)
 Is there a deficit? How many differences make a difference? 4 6 10 2 8 8 4 12 4 6 4 10 6 5 4 5 25 0
Is there a deficit? How many differences make a difference? 4 6 10 2 8 8 4 12 4 6 4 10 6 5 4 5 25 0
 Is there a deficit? Which differences make a difference? Language 4 Visual 12 Motor 6 Visual 10 Language Proc. Speed 4 Proc. Speed 5 Attention Visual 2 8 Memory Attention 6 4 10 Mental Flexibility Organization Visual 4 5 25 Memory 8 Inhibition 4 Language 0
Is there a deficit? Which differences make a difference? Language 4 Visual 12 Motor 6 Visual 10 Language Proc. Speed 4 Proc. Speed 5 Attention Visual 2 8 Memory Attention 6 4 10 Mental Flexibility Organization Visual 4 5 25 Memory 8 Inhibition 4 Language 0
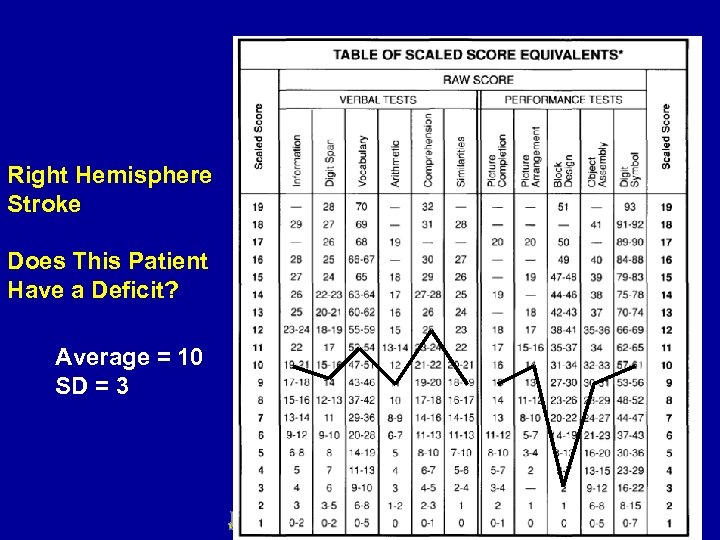 Right Hemisphere Stroke Does This Patient Have a Deficit? Average = 10 SD = 3
Right Hemisphere Stroke Does This Patient Have a Deficit? Average = 10 SD = 3
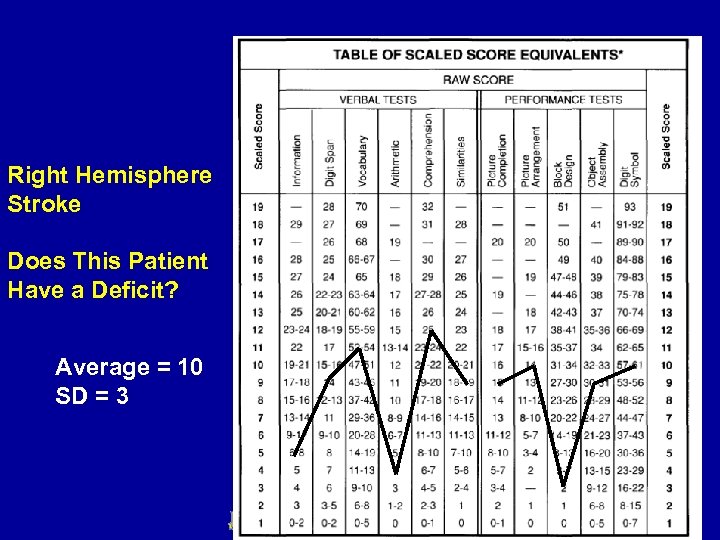 Right Hemisphere Stroke Does This Patient Have a Deficit? Average = 10 SD = 3
Right Hemisphere Stroke Does This Patient Have a Deficit? Average = 10 SD = 3
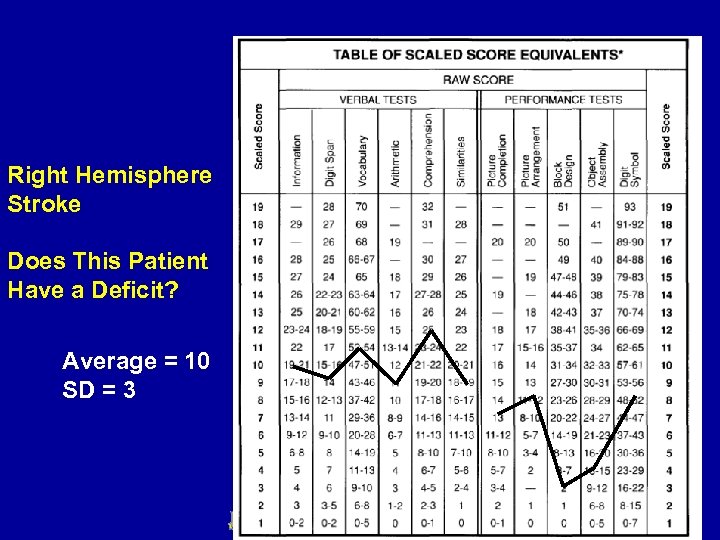 Right Hemisphere Stroke Does This Patient Have a Deficit? Average = 10 SD = 3
Right Hemisphere Stroke Does This Patient Have a Deficit? Average = 10 SD = 3
 Effects of Age, Gender, Race/Ethnicity & Education on Tests • Age – changes reflect age-related change in brain structure– varies by domain – Preserved/Gains – ‘crystallized’ abilities (verbal & academic skills, acquired knowledge), except verbal retrieval – Losses – ‘fluid’ abilities (novel reasoning, problem solving), memory, motor • Education – effects across tasks, more for ‘academic’ skills • Sex – language less strongly lateralized in females – Performance differences small and inconsistent – verbal memory advantage for females, visuospatial/math for males • Newer tests provide norms by race/ethnicity • Cultural bias in some tests
Effects of Age, Gender, Race/Ethnicity & Education on Tests • Age – changes reflect age-related change in brain structure– varies by domain – Preserved/Gains – ‘crystallized’ abilities (verbal & academic skills, acquired knowledge), except verbal retrieval – Losses – ‘fluid’ abilities (novel reasoning, problem solving), memory, motor • Education – effects across tasks, more for ‘academic’ skills • Sex – language less strongly lateralized in females – Performance differences small and inconsistent – verbal memory advantage for females, visuospatial/math for males • Newer tests provide norms by race/ethnicity • Cultural bias in some tests
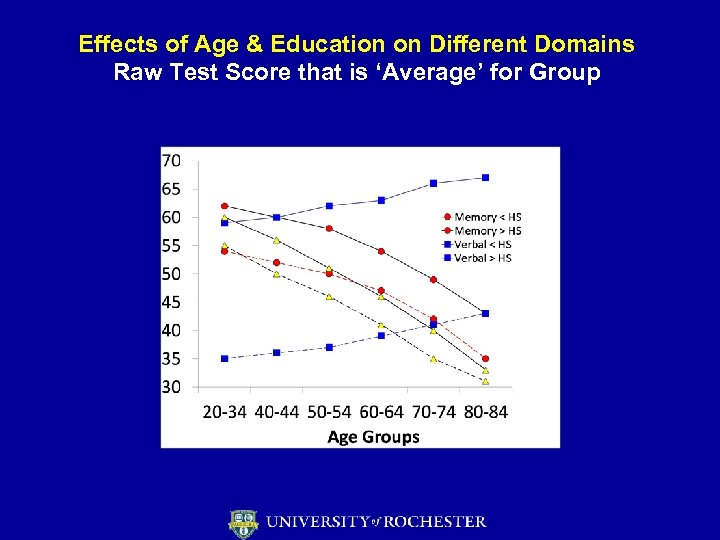 Effects of Age & Education on Different Domains Raw Test Score that is ‘Average’ for Group
Effects of Age & Education on Different Domains Raw Test Score that is ‘Average’ for Group
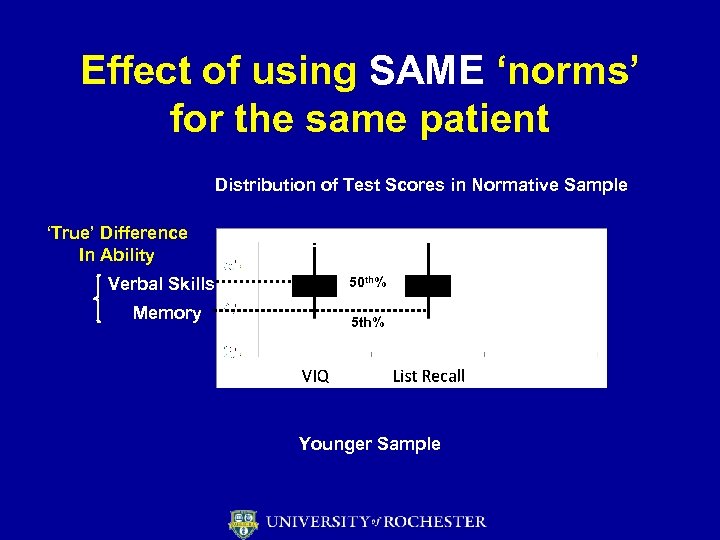 Effect of using SAME ‘norms’ for the same patient Distribution of Test Scores in Normative Sample ‘True’ Difference In Ability Verbal Skills Memory 50 th% 5 th% Younger Sample
Effect of using SAME ‘norms’ for the same patient Distribution of Test Scores in Normative Sample ‘True’ Difference In Ability Verbal Skills Memory 50 th% 5 th% Younger Sample
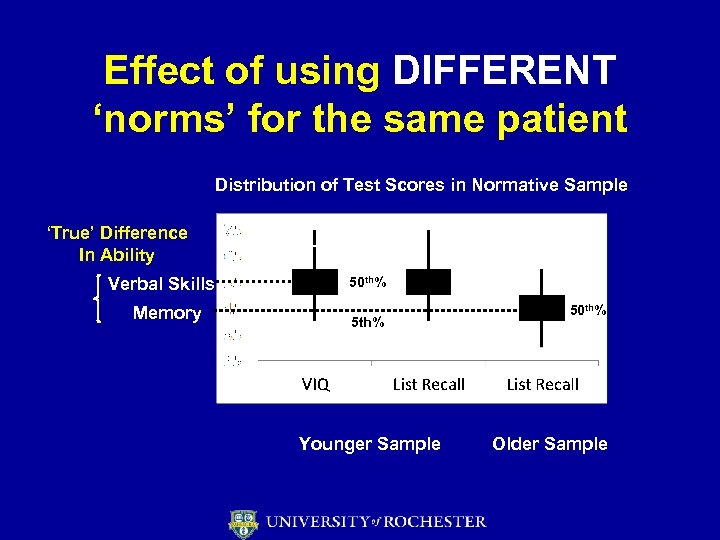 Effect of using DIFFERENT ‘norms’ for the same patient Distribution of Test Scores in Normative Sample ‘True’ Difference In Ability Verbal Skills Memory 50 th% 5 th% Younger Sample 50 th% Older Sample
Effect of using DIFFERENT ‘norms’ for the same patient Distribution of Test Scores in Normative Sample ‘True’ Difference In Ability Verbal Skills Memory 50 th% 5 th% Younger Sample 50 th% Older Sample
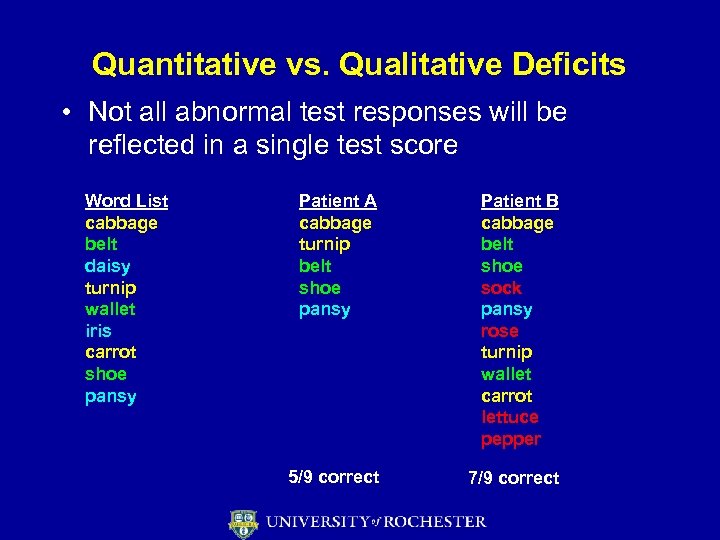 Quantitative vs. Qualitative Deficits • Not all abnormal test responses will be reflected in a single test score Word List cabbage belt daisy turnip wallet iris carrot shoe pansy Patient A cabbage turnip belt shoe pansy Patient B cabbage belt shoe sock pansy rose turnip wallet carrot lettuce pepper 5/9 correct 7/9 correct
Quantitative vs. Qualitative Deficits • Not all abnormal test responses will be reflected in a single test score Word List cabbage belt daisy turnip wallet iris carrot shoe pansy Patient A cabbage turnip belt shoe pansy Patient B cabbage belt shoe sock pansy rose turnip wallet carrot lettuce pepper 5/9 correct 7/9 correct
 Naming Failures (all score 0) ‘water bird in ‘thing you lie Florida’ in in summer’ ‘rough skin, from Africa’ ‘helmet’ ‘fishing net’ ‘pig’ ‘duck’ ‘bed’ ‘elephant’ ‘pemlican’ ‘hannock’ ‘rhisocerus’ ‘palifrene’ ‘habiteller’ ‘cantifron’
Naming Failures (all score 0) ‘water bird in ‘thing you lie Florida’ in in summer’ ‘rough skin, from Africa’ ‘helmet’ ‘fishing net’ ‘pig’ ‘duck’ ‘bed’ ‘elephant’ ‘pemlican’ ‘hannock’ ‘rhisocerus’ ‘palifrene’ ‘habiteller’ ‘cantifron’
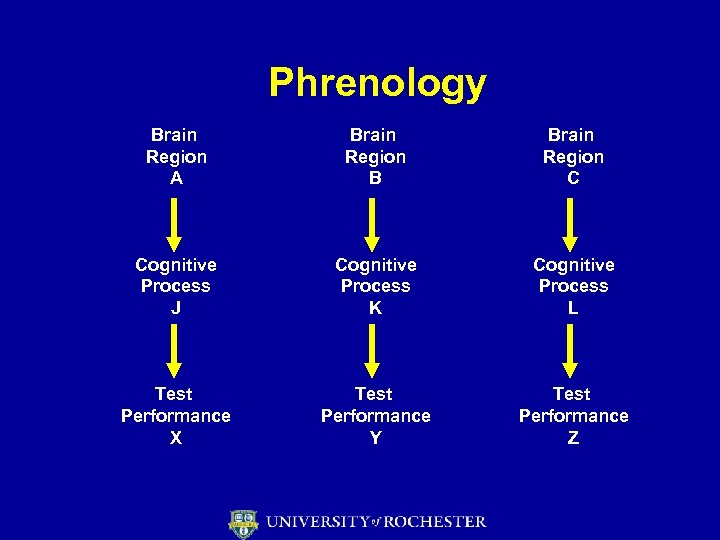 Phrenology Brain Region A Brain Region B Brain Region C Cognitive Process J Cognitive Process K Cognitive Process L Test Performance X Test Performance Y Test Performance Z
Phrenology Brain Region A Brain Region B Brain Region C Cognitive Process J Cognitive Process K Cognitive Process L Test Performance X Test Performance Y Test Performance Z
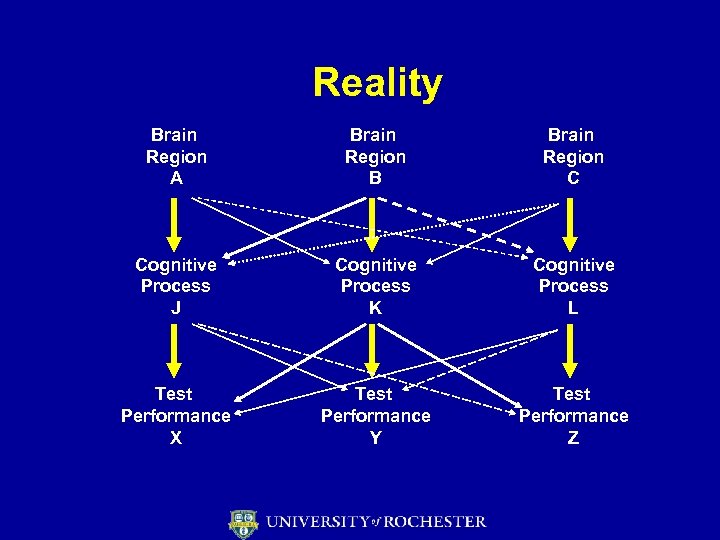 Reality Brain Region A Brain Region B Brain Region C Cognitive Process J Cognitive Process K Cognitive Process L Test Performance X Test Performance Y Test Performance Z
Reality Brain Region A Brain Region B Brain Region C Cognitive Process J Cognitive Process K Cognitive Process L Test Performance X Test Performance Y Test Performance Z
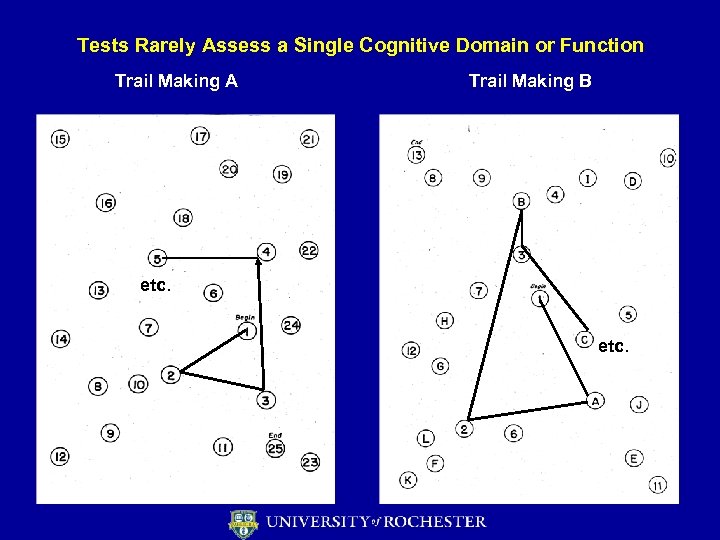 Tests Rarely Assess a Single Cognitive Domain or Function Trail Making A Trail Making B etc.
Tests Rarely Assess a Single Cognitive Domain or Function Trail Making A Trail Making B etc.
 Tests and the Processes they Assess COGNITIVE PROCESS Cognitive Flexibility TEST Trail Making A Trail Making B Arithmetic Symbol Search Vocabulary Verbal Fluency Working Memory Visual Scanning Verbal Retrieval Processing Speed + + + + - + + + +
Tests and the Processes they Assess COGNITIVE PROCESS Cognitive Flexibility TEST Trail Making A Trail Making B Arithmetic Symbol Search Vocabulary Verbal Fluency Working Memory Visual Scanning Verbal Retrieval Processing Speed + + + + - + + + +
 Focal vs. Diffuse Test Patterns • Focal – 1 -2 domains significantly affected – Other domains typically WNL – Seen in focal neurologic process involving area critical to affected domains • Diffuse – milder deficits in attention, concentration, memory, processing speed, executive function – Seen in diffuse neurologic process affecting information processing speed and integration
Focal vs. Diffuse Test Patterns • Focal – 1 -2 domains significantly affected – Other domains typically WNL – Seen in focal neurologic process involving area critical to affected domains • Diffuse – milder deficits in attention, concentration, memory, processing speed, executive function – Seen in diffuse neurologic process affecting information processing speed and integration
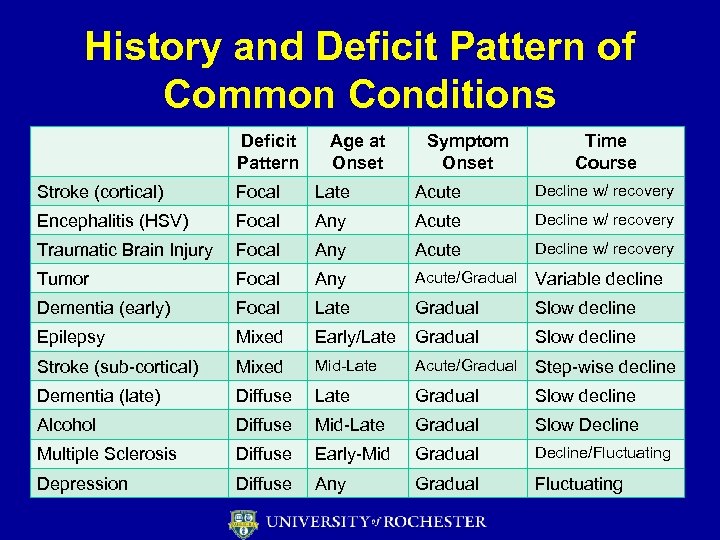 History and Deficit Pattern of Common Conditions Deficit Pattern Age at Onset Symptom Onset Time Course Stroke (cortical) Focal Late Acute Decline w/ recovery Encephalitis (HSV) Focal Any Acute Decline w/ recovery Traumatic Brain Injury Focal Any Acute Decline w/ recovery Tumor Focal Any Acute/Gradual Variable decline Dementia (early) Focal Late Gradual Slow decline Epilepsy Mixed Early/Late Gradual Slow decline Stroke (sub-cortical) Mixed Mid-Late Acute/Gradual Step-wise decline Dementia (late) Diffuse Late Gradual Slow decline Alcohol Diffuse Mid-Late Gradual Slow Decline Multiple Sclerosis Diffuse Early-Mid Gradual Decline/Fluctuating Depression Diffuse Any Gradual Fluctuating
History and Deficit Pattern of Common Conditions Deficit Pattern Age at Onset Symptom Onset Time Course Stroke (cortical) Focal Late Acute Decline w/ recovery Encephalitis (HSV) Focal Any Acute Decline w/ recovery Traumatic Brain Injury Focal Any Acute Decline w/ recovery Tumor Focal Any Acute/Gradual Variable decline Dementia (early) Focal Late Gradual Slow decline Epilepsy Mixed Early/Late Gradual Slow decline Stroke (sub-cortical) Mixed Mid-Late Acute/Gradual Step-wise decline Dementia (late) Diffuse Late Gradual Slow decline Alcohol Diffuse Mid-Late Gradual Slow Decline Multiple Sclerosis Diffuse Early-Mid Gradual Decline/Fluctuating Depression Diffuse Any Gradual Fluctuating
 Integrating Test Data with other Clinical Information • Three Important Principles – Avoid the Fallacy of Affirming the Consequent • because B often follows A, occurrence of B proves that A has occurred – Be Open Minded • generate as many reasonable explanations for what you see – Apply Occam’s Razor • “the most likely explanation for a pattern is the one that requires the least number of unlikely events to account for it “
Integrating Test Data with other Clinical Information • Three Important Principles – Avoid the Fallacy of Affirming the Consequent • because B often follows A, occurrence of B proves that A has occurred – Be Open Minded • generate as many reasonable explanations for what you see – Apply Occam’s Razor • “the most likely explanation for a pattern is the one that requires the least number of unlikely events to account for it “
 Errors in Formulation Affirming the Consequent • Complains of memory change after MVA • Testing - diffuse pattern (moderate-severe deficits in attention, executive function, processing speed c/w traumatic brain injury) • MRI – subtle, diffuse changes in deep white matter
Errors in Formulation Affirming the Consequent • Complains of memory change after MVA • Testing - diffuse pattern (moderate-severe deficits in attention, executive function, processing speed c/w traumatic brain injury) • MRI – subtle, diffuse changes in deep white matter
 Additional History • No loss of consciousness in MVA • History of functional declines, sensory and motor changes in year prior to MVA • Testing 1 year later shows further declines • Neurologic examination shows abnormal nerve conduction consistent with multiple sclerosis
Additional History • No loss of consciousness in MVA • History of functional declines, sensory and motor changes in year prior to MVA • Testing 1 year later shows further declines • Neurologic examination shows abnormal nerve conduction consistent with multiple sclerosis
 Errors in Formulation Keeping an Open Mind • • Acute onset word-finding deficits – no recent events History of worsening depression Neurologic exam normal Neuropsychological testing is normal except for severe impairment in confrontation naming with paraphasias • Imaging shows multiple lesions, one in right temporal lobe with fresh blood
Errors in Formulation Keeping an Open Mind • • Acute onset word-finding deficits – no recent events History of worsening depression Neurologic exam normal Neuropsychological testing is normal except for severe impairment in confrontation naming with paraphasias • Imaging shows multiple lesions, one in right temporal lobe with fresh blood
 Additional History • Left-handed • Strong family history of – left-handedness – early strokes • Consistent with hemorrhage of genetically-based, cavernous angioma (small tumor of vessel wall) in right, language dominant hemisphere • Depression is irrelevant in this context
Additional History • Left-handed • Strong family history of – left-handedness – early strokes • Consistent with hemorrhage of genetically-based, cavernous angioma (small tumor of vessel wall) in right, language dominant hemisphere • Depression is irrelevant in this context
 Errors in Formulation ‘Occam’s Razor’ • • 54 yo. M with recent memory complaints Neurologic exam normal Normal neuroimaging Family is concerned about ‘early Alzheimer’s’
Errors in Formulation ‘Occam’s Razor’ • • 54 yo. M with recent memory complaints Neurologic exam normal Normal neuroimaging Family is concerned about ‘early Alzheimer’s’
 Additional History • Long-standing history of major depressive disorder • No family history of dementia • Trouble caring for home and finances after partner died 4 years ago • Recently ‘got lost’ standing in front of his house, recovered quickly • Continues to perform at high level at cognitively demanding job
Additional History • Long-standing history of major depressive disorder • No family history of dementia • Trouble caring for home and finances after partner died 4 years ago • Recently ‘got lost’ standing in front of his house, recovered quickly • Continues to perform at high level at cognitively demanding job


