0e05cba8756fac00e1455876122f5ad5.ppt
- Количество слайдов: 14

International Healthcare Systems Bernardo Ramirez MD, MBA HSA 6112 University of Central Florida College of Health and Public Affairs Health Management & Informatics Department
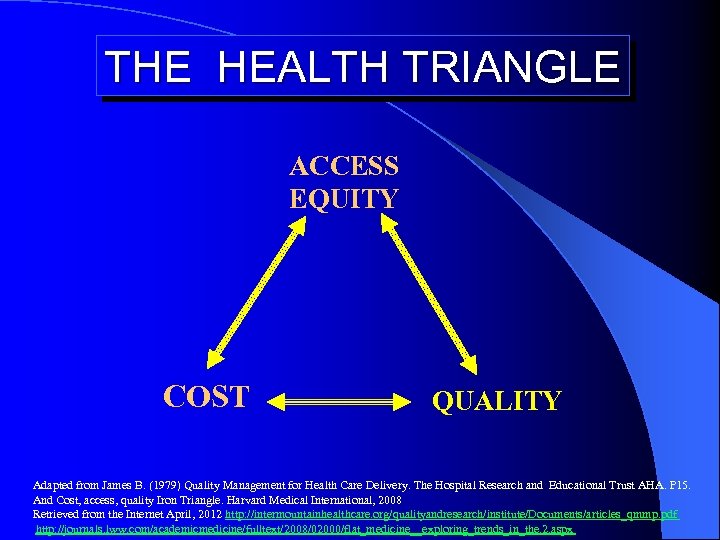
THE HEALTH TRIANGLE ACCESS EQUITY COST QUALITY Adapted from James B. (1979) Quality Management for Health Care Delivery. The Hospital Research and Educational Trust AHA. P 15. And Cost, access, quality Iron Triangle. Harvard Medical International, 2008 Retrieved from the Internet April, 2012 http: //intermountainhealthcare. org/qualityandresearch/institute/Documents/articles_qmmp. pdf http: //journals. lww. com/academicmedicine/fulltext/2008/02000/flat_medicine__exploring_trends_in_the. 2. aspx
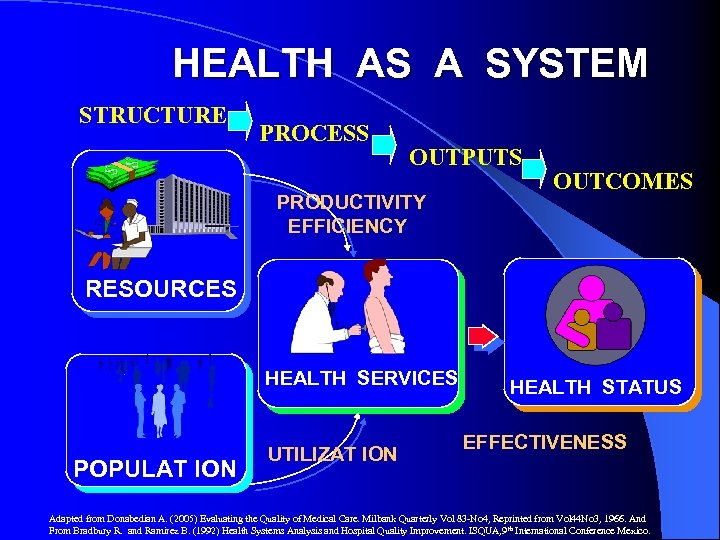
HEALTH AS A SYSTEM STRUCTURE PROCESS OUTPUTS PRODUCTIVITY EFFICIENCY OUTCOMES RESOURCES HEALTH SERVICES POPULAT ION UTILIZAT ION HEALTH STATUS EFFECTIVENESS Adapted from Donabedian A. (2005) Evaluating the Quality of Medical Care. Milbank Quarterly Vol 83 -No 4, Reprinted from Vol 44 No 3, 1966. And From Bradbury R. and Ramirez B. (1992) Health Systems Analysis and Hospital Quality Improvement. ISQUA, 9 th International Conference Mexico.

Health Services Elements l Population – Access/utilization (Education, Health Promotion, Options for Care, Legal Aspects, Geographical and Cultural Barriers) – Epidemiology (Transition, Mortality, Morbidity, Population, Life Expectancy) – Life Styles and behaviors (Prevention and chronic health, Patient & Family Centered)

Health Services Elements l Resources – Physical Resources, (hospitals, clinics, private- public, Ambulatory services) – Equipment/Technology, Medicines – Human resources (Education, health manpower, Incentives, training, continuing education, Physicians, nurses, technicians and emerging professions) – Financial Resources (Resource allocation, budgets, financial schemes, reimbursement, insurance mechanisms)

Health Services Elements l Health Services – Primary/Secondary health care. Systems. – Management Information Systems – Clinical Standards and Protocols. Safety Issues. – Quality Assurance and Quality Improvement – Legal aspects (malpractice) – Incentives, Performance management. – Cost or services – Efficiency, clinical & Management efficiency – Effectiveness, Health Impact and outcomes
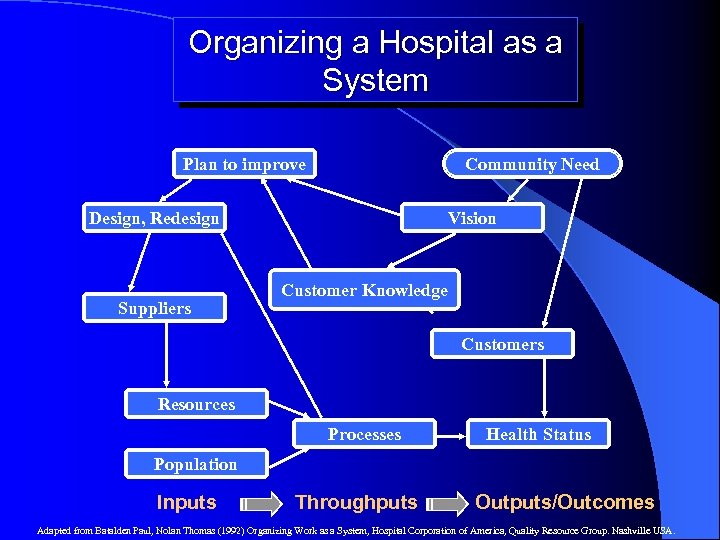
Organizing a Hospital as a System Community Need Plan to improve Design, Redesign Suppliers Vision Customer Knowledge Customers Resources Processes Health Status Population Inputs Throughputs Outputs/Outcomes Adapted from Batalden Paul, Nolan Thomas (1992) Organizing Work as a System, Hospital Corporation of America, Quality Resource Group. Nashville USA.
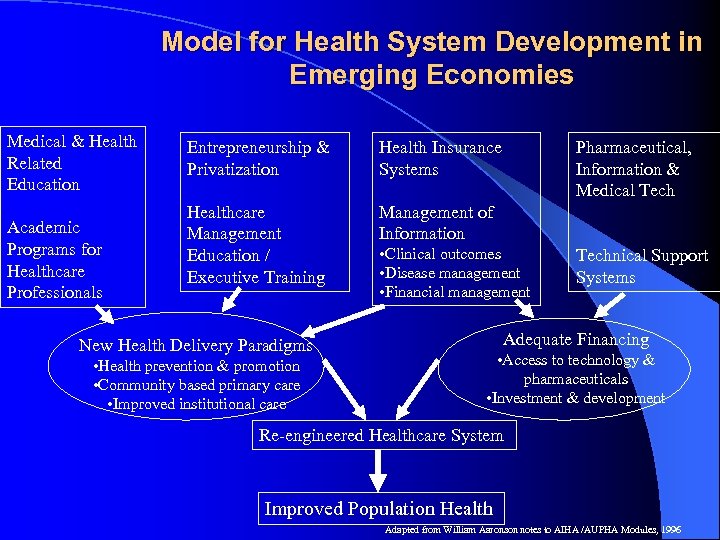
Model for Health System Development in Emerging Economies Medical & Health Related Education Academic Programs for Healthcare Professionals Entrepreneurship & Privatization Health Insurance Systems Healthcare Management Education / Executive Training Management of Information New Health Delivery Paradigms • Health prevention & promotion • Community based primary care • Improved institutional care Pharmaceutical, Information & Medical Tech • Clinical outcomes • Disease management • Financial management Technical Support Systems Adequate Financing • Access to technology & pharmaceuticals • Investment & development Re-engineered Healthcare System Improved Population Health Adapted from William Aaronson notes to AIHA /AUPHA Modules, 1996

Public Health Care l Public Health Agencies are Local, state and federal and serve as primary organizations to serve community wide efforts for health promotion, disease prevention, health assessment and provision of medical care to vulnerable population groups

Strong Evidence for Vulnerability § § § § Minority populations Lower socioeconomic status Substandard Housing Chronic illness-mental/physical/addicts Immigrants and Prisoners Un- or underinsured Extremes of Age Socially Isolated Presented by Margaret Wheeler MD, Disparities in Care of Vulnerable Patients, San Francisco General Hospital_University of California San Francisco. AUPHA Leaders meeting Orlando, FL, 2000

Government Programs l Medicare (elderly and disabled) l Medicaid (poor, vulnerable) l Federal Employees Health Benefit Program l Military Programs (Tricare, Uniform services & US Family Health Plan) l Veterans Administration l US Public Health Service l Indian Health Service
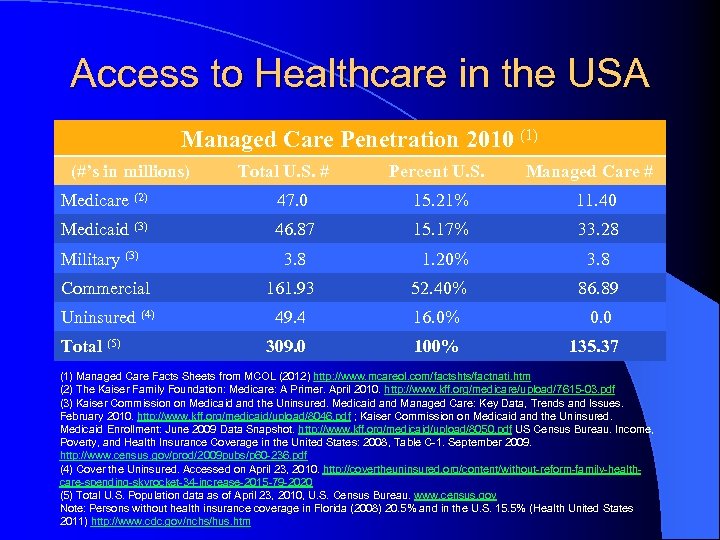
Access to Healthcare in the USA Managed Care Penetration 2010 (1) (#’s in millions) Total U. S. # Percent U. S. Managed Care # Medicare (2) 47. 0 15. 21% 11. 40 Medicaid (3) 46. 87 15. 17% 33. 28 Military (3) 3. 8 1. 20% 3. 8 Commercial 161. 93 52. 40% 86. 89 Uninsured (4) 49. 4 16. 0% 0. 0 309. 0 100% Total (5) 135. 37 (1) Managed Care Facts Sheets from MCOL (2012) http: //www. mcareol. com/factshts/factnati. htm (2) The Kaiser Family Foundation: Medicare: A Primer. April 2010. http: //www. kff. org/medicare/upload/7615 -03. pdf (3) Kaiser Commission on Medicaid and the Uninsured. Medicaid and Managed Care: Key Data, Trends and Issues. February 2010. http: //www. kff. org/medicaid/upload/8046. pdf ; Kaiser Commission on Medicaid and the Uninsured. Medicaid Enrollment: June 2009 Data Snapshot. http: //www. kff. org/medicaid/upload/8050. pdf US Census Bureau. Income, Poverty, and Health Insurance Coverage in the United States: 2008, Table C-1. September 2009. http: //www. census. gov/prod/2009 pubs/p 60 -236. pdf (4) Cover the Uninsured. Accessed on April 23, 2010. http: //covertheuninsured. org/content/without-reform-family-healthcare-spending-skyrocket-34 -increase-2015 -79 -2020 (5) Total U. S. Population data as of April 23, 2010, U. S. Census Bureau. www. census. gov Note: Persons without health insurance coverage in Florida (2008) 20. 5% and in the U. S. 15. 5% (Health United States 2011) http: //www. cdc. gov/nchs/hus. htm
Causes of Disparities l Physician variables – Biases, uncertainty l Patient variables – Attitudes, expectations, preferences, biases l System variables – Administrative, financing, accessibility Presented by Margaret Wheeler MD, Disparities in Care of Vulnerable Patients, San Francisco General Hospital_University of California San Francisco. AUPHA Leaders meeting Orlando, FL, 2000

Causes for lack of access l Geographical l Socioeconomic l Cultural l Environment l Vulnerability-Risk (extremes of life) l Discrimination (Minorities-less care even when insured, ethnic, disability)
0e05cba8756fac00e1455876122f5ad5.ppt