df4f7a4c0003d827726a5f545f3b76a8.ppt
- Количество слайдов: 23

Intensified TB case-finding: still wide open to questions and answers Dr Liz Corbett Bloomsbury Wellcome Trust Centre & Clinical Research Unit, London School Hygiene Tropical Medicine Biomedical Research & Training Institute, Harare

Pre-DOTS era l ICF widely used in all continents – Mass mini-radiographs and household enquiries – Diagnosis and treatment +/- sanatoria – Still used in some settings today l Use associated with declining TB incidence rates in many settings l Not formally evaluated as an isolated intervention

Kolin l 1961 – 1972 Kolin study – – l 5 rounds of MMR Point prevalence of s+ TB fell from 233 to 56 per 100 k Incidence of s+ TB fell from 142 to 52 per 100 k per year Effective TB treatment introduced + BCG 72% of all cases detected between MMR rounds through passive CFT l More effective to focus on effective treatment of cases presenting passively

India l Tumkur District prevalence survey 1960 s (TST and CXR) – No TB treatment programme l Follow-up investigation for symptoms (? delay) – 70% of smear-positive patients aware of symptoms – 50% had already sought care l Bangalore – CXR versus CXR plus symptom screen • Symptoms added little to CXR • Symptoms alone identified 70% culture-positive TB patients Banerji D, Anderson S. A sociological study of awareness of symptoms among persons with pulmonary tuberculosis. Bull Wld Hlth Org 1963; 29: 665 -683. Gothi GD, et al. Estimation of prevalence of bacillary tuberculosis on basis of chest x-ray and-or symptomatic screening. Indian J Med Res 1976; 64(8): 1150 -1159.

Kenya l Case-finding studies in 1970 s and 1980 s – House-to-house surveys most effective • 80% of cases had been to clinic with symptoms • Distance to clinic – Interview of village elders ineffective – Mothers asked to refer anyone with symptoms in their household • High yield in those who attended • Low population impact (4% all cases)

Korea l Routine use of “school leavers” for door-to-door enquiry – Each employee covered 10, 000 pop – Over 50% of cases picked up this way during 1970 s
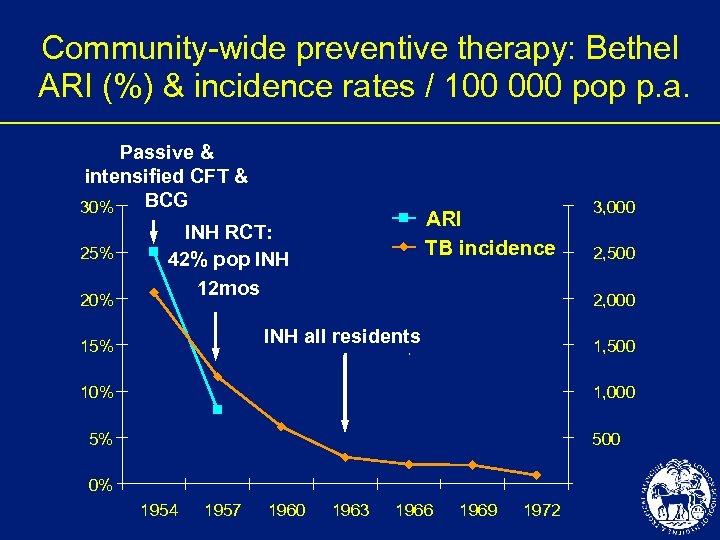
Community-wide preventive therapy: Bethel ARI (%) & incidence rates / 100 000 pop p. a. Passive & intensified CFT & BCG 30% 25% 20% ARI TB incidence INH RCT: 42% pop INH 12 mos 2, 500 2, 000 INH all residents 15% 3, 000 1, 500 10% 1, 000 5% 500 0% 1954 1957 1960 1963 1966 1969 1972

Other studies l Toman (1976) – 75% of cases self-presenting in countries covered by MMR programmes – Netherlands – annual CXR (2. 5 million adults) • 15% of s+ and 25% of c+ TB detected through MMR – Expensive, not cost-effective – Assumes equal public health impact of ACF & PCF pick-up Toman K. Mass radiography in tuberculosis-control. Who Chronicle 1976; 30(2): 51 -57

Fate of pulmonary TB treated under routine conditions l High rates of treatment failure and recurrence l Increasing recognition of the importance of adequate treatment l First priorities: – Effective diagnosis in patients presenting passively – Effective treatment of those presenting passively – Don’t waste money and risk overwhelming health systems with ICF until these basics are in place DOTS

ICF in the DOTS era l Low case-detection a major factor limiting TB control – Patients with symptoms cannot access investigations – Marginalised populations – Not all TB is highly symptomatic l HIV-associated TB – Driving up global incidence rates – High prevalence of active TB in HIV care settings – High mortality rates l Modeling the impact of better case-finding l Time ripe to reconsider ICF

ICF goals l Reduce morbidity and mortality – More intensive case-finding leads to fewer TB deaths and less severe post-TB complications – Focus on those most at risk of severe morbidity l Reduce TB transmission – General community – Institutional settings – Marginalised populations l Increase case-finding – Target high risk groups – Community-wide approach

ICF challenges l Poor treatment outcomes – Patients detected through ICF unwilling to be treated – ICF in settings of high primary MDR-TB l Diagnostic approach – Active versus inactive TB – Relatively low % smear-positive cases • Choice of screening and diagnostic tests – Illnesses other than TB • OIs & HIV itself l Overwhelm the health system
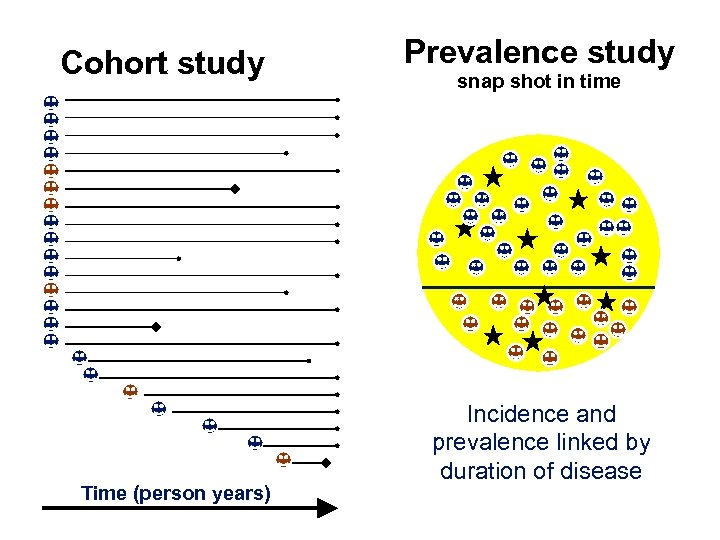
Cohort study Time (person years) Prevalence study snap shot in time Incidence and prevalence linked by duration of disease

Prevalent TB disease l High ratio of prevalent: incident disease among HIV-ves – See next slide l Risk groups for prevalent TB disease – Household contacts – Homeless – IDU – VCT attenders – Home based care – Congregate settings: prisons and miners – Old age and male sex

Prevalence: incidence
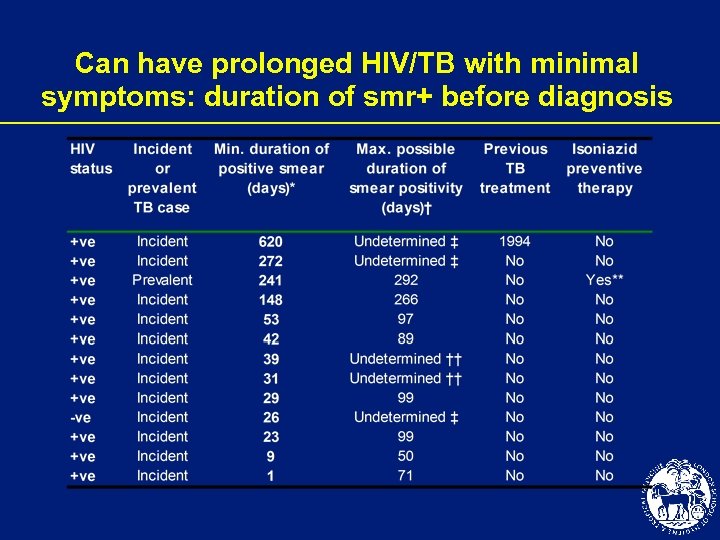
Can have prolonged HIV/TB with minimal symptoms: duration of smr+ before diagnosis

What do we need to know? l ICF in high HIV prevalence populations – Screening algorithms • Expect these to vary by HIV status • Expect these to vary by effectiveness of DOTS – Can ICF substantially improve TB control? l ICF and treatment outcomes – High and low MDR-TB settings – IDU l Better understanding of prevalent TB disease – Impact of HIV – Why is prevalent TB so common in HIV-ve pops? – Does IPT increase risk of prolonged TB excretion

What do we need to know? l Targeted ICF: how to do it better – Strategies to reach high risk populations (Tables 1 & 2) • High risk of TB morbidity • High risk of prevalent active TB – Strategies accessible by the general population • ZAMSTAR • TB screening clinics akin to VCT clinics • TB screening clinics accessible only on referral – Involving the community • TB clubs / shop keepers / home based care – Linked to better management of smear-negative TB

Institutional TB l How much TB is institutionally acquired? – TST conversion in student nurses • 18% p. a. strict US criteria after negative 2 -step in Harare – Will have parallel ELISPOT data • ? 10+% annual risk of TB disease if HIV+ve – HIV care patients • Recurrent TB disease in patients on ARVs • Gold miners: – recurrent TB increased from ~8% p. a to ~25% p. a. in HIV+ – Coincided with introduction of HIV care clinic l Can ICF control institutional TB transmission? – Long term preventive therapy? – Role of culture-based ICF

Ongoing research l Shop keepers: Malawi l ZAMSTAR l DETECTB l Cambodia l Kenya l Others? l Institutional TB: ARTI in student nurses – Others?

Recommended priority groups for targeted ICF l VCT clients l HIV care clinics l Patients starting ARVs (IRIS) l Household contacts l IVDU l Institutions – Prisons – hospitals

General population screening l Insufficient evidence on which to base recommendations – Potential HUGE: true TB prevention – Impact of a single round or brief period of highly effective population -based ICF? • DOTS can be the sustainable element (Bethel 0 • One passive = one ICF patient? • Respective roles of reactivation and recent TB infection l Effective screening tool: digital MMR? ? l Effective diagnostic test l Effective case-management – Note that in high HIV prevalence settings the ratio of prevalent to incident cases may not be all that high – Would expect a rapid impact on new TB cases if prevalent TB disease control is improved

Conclusions l ICF is natural extension of DOTS – Operational research priorities & interim recommendations – p 7 – Targeted linked to IPT and ARVS • • VCT clients Institutional TB control Household contact screening IDUs – General populations: model / demonstration programmes? • • • l TB screening clinics Shop-keepers ZAMSTAR approach Household screening MMRs TB case-finding is HIV case finding – Chronic cough patients in Harare • HIV prevalence 83% overall: 88% in TB patients
df4f7a4c0003d827726a5f545f3b76a8.ppt