73e1c462a7f3bbb4298b5cc82c981d11.ppt
- Количество слайдов: 66
 Integration of Mental Health and Primary Health Care for the Older Patient Stephen J. Bartels, M. D. , M. S. Professor of Psychiatry and Community and Family Medicine Co-Director Dartmouth Center on Aging
Integration of Mental Health and Primary Health Care for the Older Patient Stephen J. Bartels, M. D. , M. S. Professor of Psychiatry and Community and Family Medicine Co-Director Dartmouth Center on Aging
 Overview • Background: Mental Health, Primary Care, and the Older Patient • Outcomes: Integration of Mental Health Services in Primary Care and the Older Patient • Policy Implications for The President’s Commission on Mental Health
Overview • Background: Mental Health, Primary Care, and the Older Patient • Outcomes: Integration of Mental Health Services in Primary Care and the Older Patient • Policy Implications for The President’s Commission on Mental Health
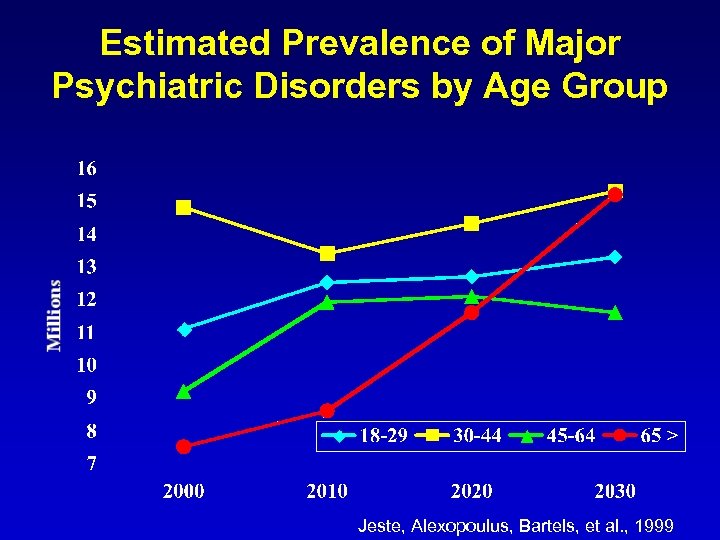 Estimated Prevalence of Major Psychiatric Disorders by Age Group Jeste, Alexopoulus, Bartels, et al. , 1999
Estimated Prevalence of Major Psychiatric Disorders by Age Group Jeste, Alexopoulus, Bartels, et al. , 1999
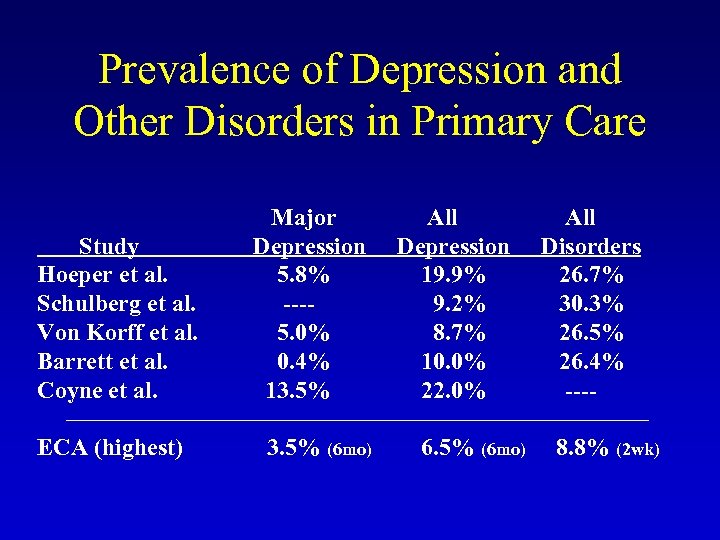 Prevalence of Depression and Other Disorders in Primary Care Study Hoeper et al. Schulberg et al. Von Korff et al. Barrett et al. Coyne et al. ECA (highest) Major Depression 5. 8% ---5. 0% 0. 4% 13. 5% (6 mo) All Depression 19. 9% 9. 2% 8. 7% 10. 0% 22. 0% 6. 5% (6 mo) All Disorders 26. 7% 30. 3% 26. 5% 26. 4% ---8. 8% (2 wk)
Prevalence of Depression and Other Disorders in Primary Care Study Hoeper et al. Schulberg et al. Von Korff et al. Barrett et al. Coyne et al. ECA (highest) Major Depression 5. 8% ---5. 0% 0. 4% 13. 5% (6 mo) All Depression 19. 9% 9. 2% 8. 7% 10. 0% 22. 0% 6. 5% (6 mo) All Disorders 26. 7% 30. 3% 26. 5% 26. 4% ---8. 8% (2 wk)
 Depression Associated with Worse Health Outcomes • Worse outcomes – Hip fractures – Myocardial infarction – Cancer (Mossey 1990; Penninx et al. 2001; Evans 1999) • Increased mortality rates – Myocardial Infarction (Frasure-Smith 1993, 1995) – Long term Care Residents (Katz 1989, Rovner 1991, Parmelee 1992; Ashby 1991; Shah 1993, Samuels 1997)
Depression Associated with Worse Health Outcomes • Worse outcomes – Hip fractures – Myocardial infarction – Cancer (Mossey 1990; Penninx et al. 2001; Evans 1999) • Increased mortality rates – Myocardial Infarction (Frasure-Smith 1993, 1995) – Long term Care Residents (Katz 1989, Rovner 1991, Parmelee 1992; Ashby 1991; Shah 1993, Samuels 1997)
 Suicide and the Older Patient • Older adults: Highest risk of suicide of any age group • 70% of elderly completing suicide have seen their primary care physician in the prior month, 40% prior week, 20% same day (Conwell et al. , 1994) • Screening all primary care patients impractical…. But identification of higher risk patients important
Suicide and the Older Patient • Older adults: Highest risk of suicide of any age group • 70% of elderly completing suicide have seen their primary care physician in the prior month, 40% prior week, 20% same day (Conwell et al. , 1994) • Screening all primary care patients impractical…. But identification of higher risk patients important
 Primary Care Elderly with Depression, Anxiety, or At-risk Alcohol Use • 27. 5% Report Death Ideation • 10. 5% Report Active Suicidal Ideation • Greatest Suicidal Ideation: Depression with Anxiety (18%), Poor Social Support • Suicidal Ideation NOT associated with increased visits to the PCP Bartels et al. , Am J. Geriatric Psychiatry 2002, 10: 417 -427
Primary Care Elderly with Depression, Anxiety, or At-risk Alcohol Use • 27. 5% Report Death Ideation • 10. 5% Report Active Suicidal Ideation • Greatest Suicidal Ideation: Depression with Anxiety (18%), Poor Social Support • Suicidal Ideation NOT associated with increased visits to the PCP Bartels et al. , Am J. Geriatric Psychiatry 2002, 10: 417 -427
 Quality of Mental Health, Care and the Older Patient • Fragmentation of the Mental Health service delivery system for older persons • Primary Care as the “de facto” mental health system of care for the older person
Quality of Mental Health, Care and the Older Patient • Fragmentation of the Mental Health service delivery system for older persons • Primary Care as the “de facto” mental health system of care for the older person
 Quality of Mental Health Care for Older Primary Care Patients The older primary care patient with depression compared to younger: • More likely to receive benzodiazepines • Less likely to receive SSRIs • Less likely to receive psychotherapy Bartels et al. , International J. Psychiatry in Medicine 27 (3): 215 -231, 1997.
Quality of Mental Health Care for Older Primary Care Patients The older primary care patient with depression compared to younger: • More likely to receive benzodiazepines • Less likely to receive SSRIs • Less likely to receive psychotherapy Bartels et al. , International J. Psychiatry in Medicine 27 (3): 215 -231, 1997.
 Health Service Use and Costs Associated with Depression for Older Primary Care Patients
Health Service Use and Costs Associated with Depression for Older Primary Care Patients
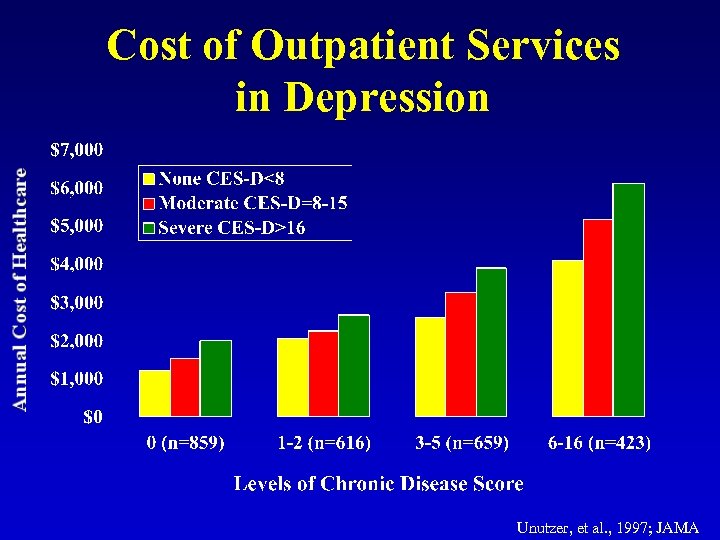 Cost of Outpatient Services in Depression Unutzer, et al. , 1997; JAMA
Cost of Outpatient Services in Depression Unutzer, et al. , 1997; JAMA
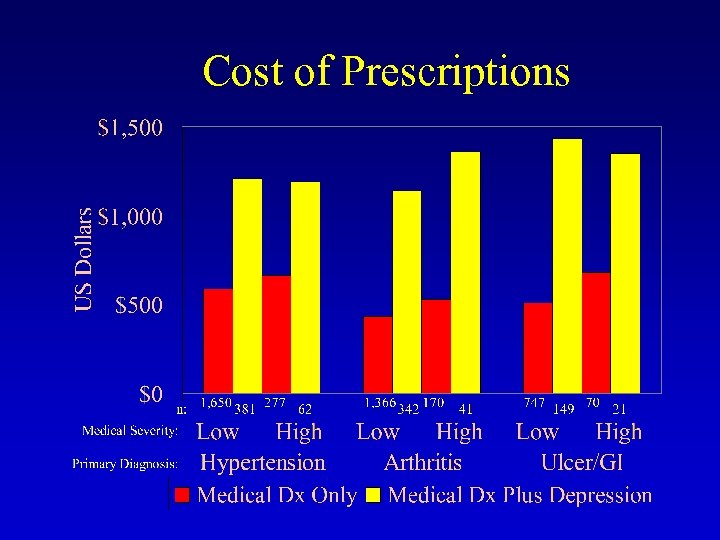 Cost of Prescriptions
Cost of Prescriptions
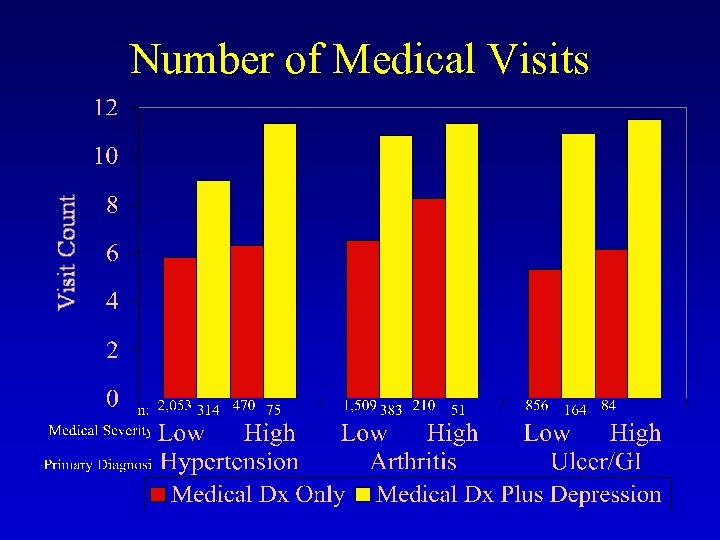 Number of Medical Visits
Number of Medical Visits
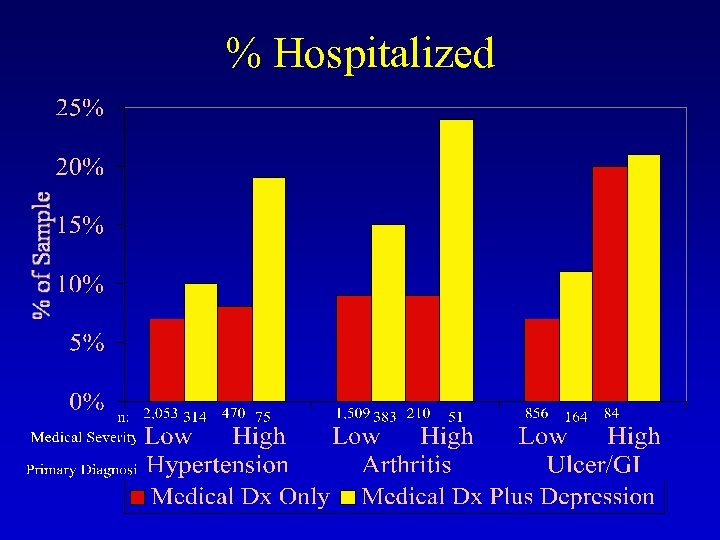 % Hospitalized
% Hospitalized
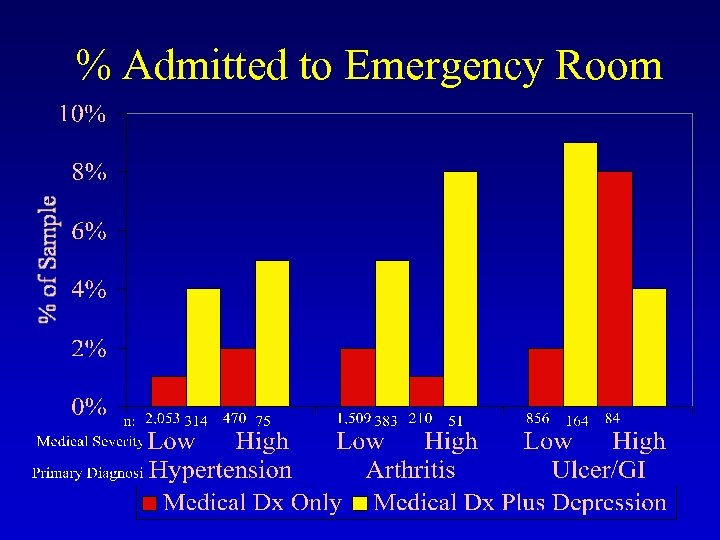 % Admitted to Emergency Room
% Admitted to Emergency Room
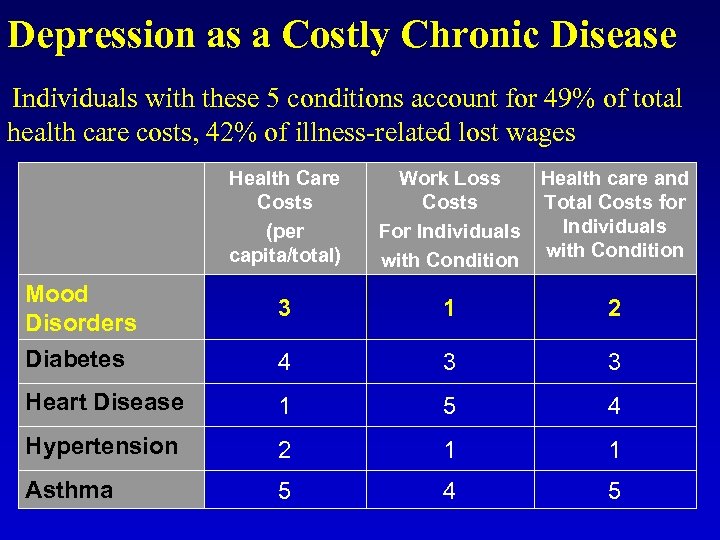 Depression as a Costly Chronic Disease Individuals with these 5 conditions account for 49% of total health care costs, 42% of illness-related lost wages Health Care Costs (per capita/total) Work Loss Health care and Costs Total Costs for Individuals For Individuals with Condition Mood Disorders 3 1 2 Diabetes 4 3 3 Heart Disease 1 5 4 Hypertension 2 1 1 Asthma 5 4 5
Depression as a Costly Chronic Disease Individuals with these 5 conditions account for 49% of total health care costs, 42% of illness-related lost wages Health Care Costs (per capita/total) Work Loss Health care and Costs Total Costs for Individuals For Individuals with Condition Mood Disorders 3 1 2 Diabetes 4 3 3 Heart Disease 1 5 4 Hypertension 2 1 1 Asthma 5 4 5
 Summary of Findings • Comorbid Depression in Medical Disorders Commonly Affecting Older Patients • Greater Use and Costs of Medications • Greater Use of Health Services (medical outpatient visits, emergency visits, and hospitalizations)
Summary of Findings • Comorbid Depression in Medical Disorders Commonly Affecting Older Patients • Greater Use and Costs of Medications • Greater Use of Health Services (medical outpatient visits, emergency visits, and hospitalizations)
 The Research Question: What is the Most Effective Way to Organize and Deliver Mental Health Services to Older Persons in Primary Care Settings?
The Research Question: What is the Most Effective Way to Organize and Deliver Mental Health Services to Older Persons in Primary Care Settings?
 Primary Care Research in Substance Abuse and Mental Health for the Elderly
Primary Care Research in Substance Abuse and Mental Health for the Elderly
 A Comparison of Two Service Models • Integrated/Collaborative Care – Co-Located – Concurrent – Collaborative • Enhanced Referral to Specialty Mental Health and Substance Abuse Clinics – Preferred Providers and Facilitated appointments, transportation, payment
A Comparison of Two Service Models • Integrated/Collaborative Care – Co-Located – Concurrent – Collaborative • Enhanced Referral to Specialty Mental Health and Substance Abuse Clinics – Preferred Providers and Facilitated appointments, transportation, payment
 Primary Hypotheses • Engagement Hypothesis • Participation Hypothesis • Outcomes Hypothesis • Cost Hypothesis
Primary Hypotheses • Engagement Hypothesis • Participation Hypothesis • Outcomes Hypothesis • Cost Hypothesis
 Is the Integrated Model More Likely to Result in Engagement in Mental Health Care by Older Persons?
Is the Integrated Model More Likely to Result in Engagement in Mental Health Care by Older Persons?
 STUDY TARGET CONDITIONS • • Major Depression Dysthymic Disorder Minor Depression Depressive Disorder NOS • Generalized Anxiety Disorder (GAD) • Panic Disorder • Anxiety Disorder NOS • At-risk Alcohol Use
STUDY TARGET CONDITIONS • • Major Depression Dysthymic Disorder Minor Depression Depressive Disorder NOS • Generalized Anxiety Disorder (GAD) • Panic Disorder • Anxiety Disorder NOS • At-risk Alcohol Use
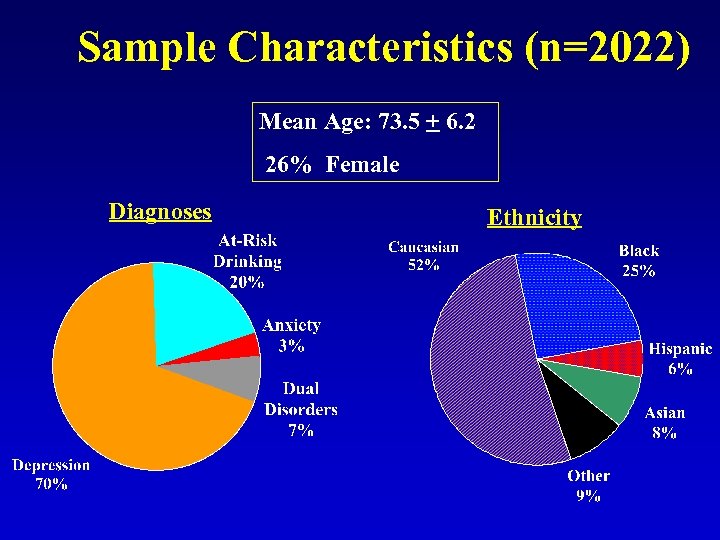 Sample Characteristics (n=2022) Mean Age: 73. 5 + 6. 2 26% Female Diagnoses Ethnicity
Sample Characteristics (n=2022) Mean Age: 73. 5 + 6. 2 26% Female Diagnoses Ethnicity
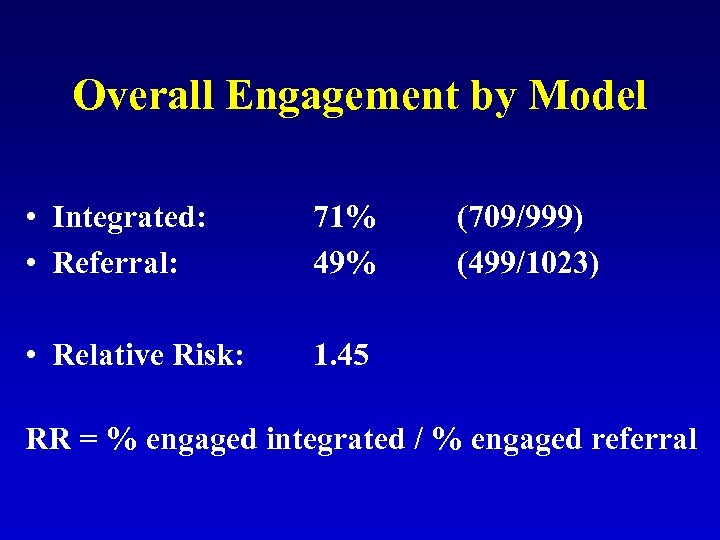 Overall Engagement by Model • Integrated: • Referral: 71% 49% • Relative Risk: 1. 45 (709/999) (499/1023) RR = % engaged integrated / % engaged referral
Overall Engagement by Model • Integrated: • Referral: 71% 49% • Relative Risk: 1. 45 (709/999) (499/1023) RR = % engaged integrated / % engaged referral
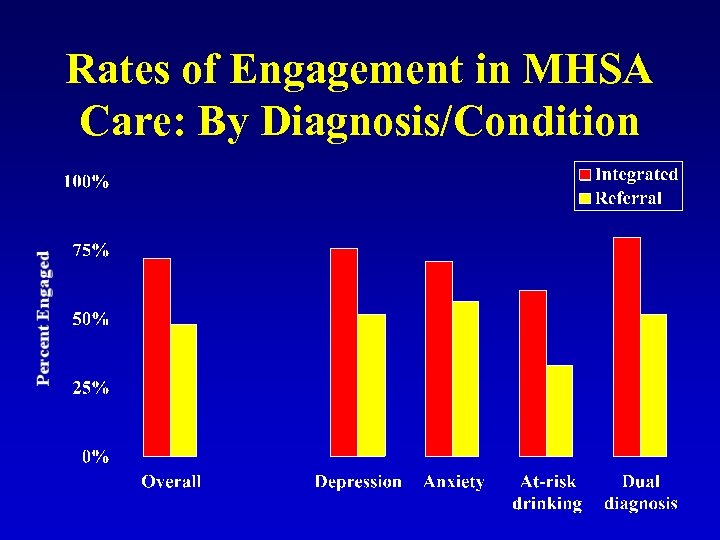 Rates of Engagement in MHSA Care: By Diagnosis/Condition
Rates of Engagement in MHSA Care: By Diagnosis/Condition
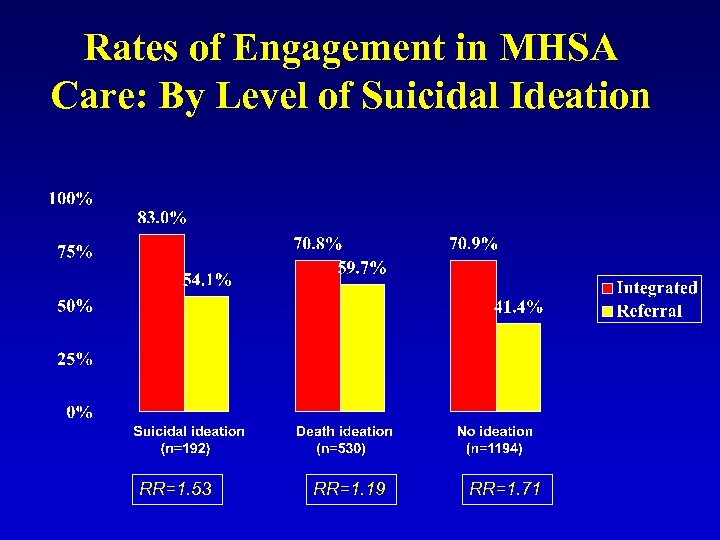 Rates of Engagement in MHSA Care: By Level of Suicidal Ideation RR=1. 53 RR=1. 19 RR=1. 71
Rates of Engagement in MHSA Care: By Level of Suicidal Ideation RR=1. 53 RR=1. 19 RR=1. 71
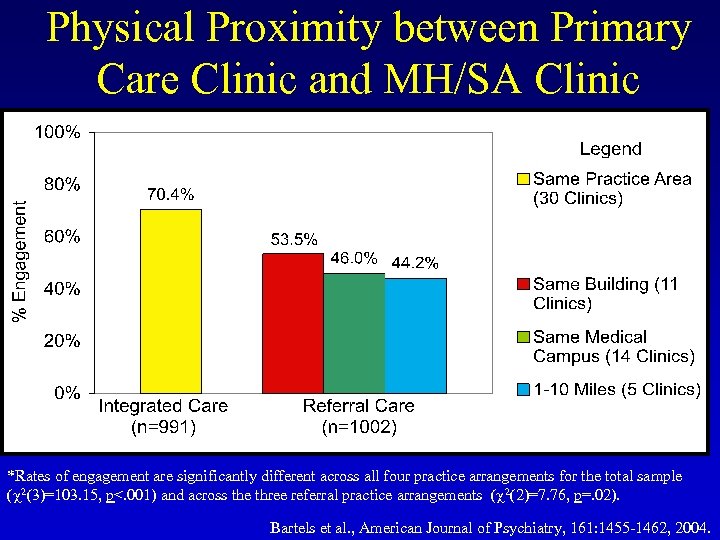 Physical Proximity between Primary Care Clinic and MH/SA Clinic *Rates of engagement are significantly different across all four practice arrangements for the total sample ( 2(3)=103. 15, p<. 001) and across the three referral practice arrangements ( 2(2)=7. 76, p=. 02). Bartels et al. , American Journal of Psychiatry, 161: 1455 -1462, 2004.
Physical Proximity between Primary Care Clinic and MH/SA Clinic *Rates of engagement are significantly different across all four practice arrangements for the total sample ( 2(3)=103. 15, p<. 001) and across the three referral practice arrangements ( 2(2)=7. 76, p=. 02). Bartels et al. , American Journal of Psychiatry, 161: 1455 -1462, 2004.
 Outcomes • Integrated Care (compared to specialty referral) Associated with Greater Engagement in Treatment ……. Similar Outcomes (slightly better for major depression in specialty referral) • Are Integrated Services with Depression Care Management (including use of specified treatment protocols) Better than Usual Care? – IMPACT (Hartford Foundation) – PROSPECT (NIMH)
Outcomes • Integrated Care (compared to specialty referral) Associated with Greater Engagement in Treatment ……. Similar Outcomes (slightly better for major depression in specialty referral) • Are Integrated Services with Depression Care Management (including use of specified treatment protocols) Better than Usual Care? – IMPACT (Hartford Foundation) – PROSPECT (NIMH)
 The IMPACT Treatment Model • Collaborative care model includes: – Care manager: Depression Clinical Specialist • Patient education • Symptom and Side effect tracking • Brief, structured psychotherapy: PST-PC – Consultation / weekly supervision meetings with • Primary care physician • Team psychiatrist • Stepped protocol in primary care using antidepressant medications and / or 6 -8 sessions of psychotherapy (PST-PC)
The IMPACT Treatment Model • Collaborative care model includes: – Care manager: Depression Clinical Specialist • Patient education • Symptom and Side effect tracking • Brief, structured psychotherapy: PST-PC – Consultation / weekly supervision meetings with • Primary care physician • Team psychiatrist • Stepped protocol in primary care using antidepressant medications and / or 6 -8 sessions of psychotherapy (PST-PC)
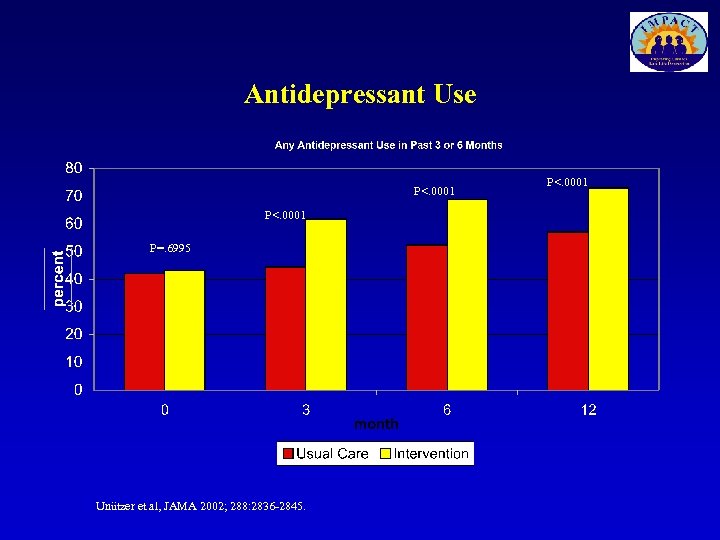 Antidepressant Use P<. 0001 P=. 6995 Unützer et al, JAMA 2002; 288: 2836 -2845. P<. 0001
Antidepressant Use P<. 0001 P=. 6995 Unützer et al, JAMA 2002; 288: 2836 -2845. P<. 0001
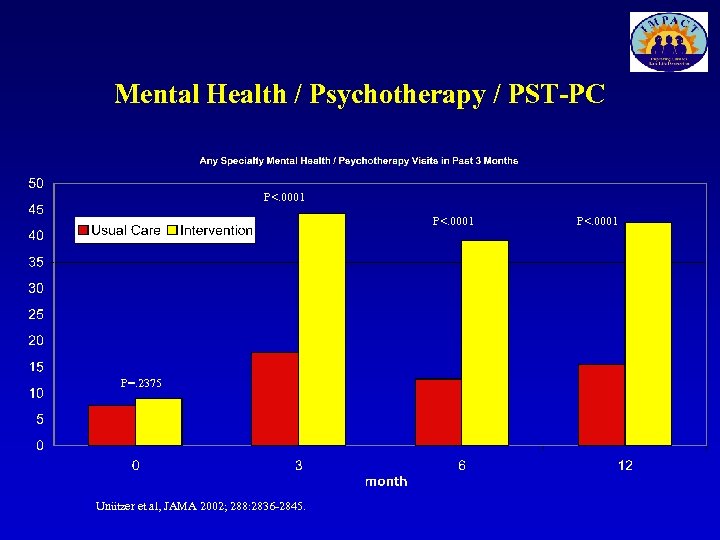 Mental Health / Psychotherapy / PST-PC P<. 0001 P=. 2375 Unützer et al, JAMA 2002; 288: 2836 -2845. Unutzer et al, JAMA 2002. P<. 0001
Mental Health / Psychotherapy / PST-PC P<. 0001 P=. 2375 Unützer et al, JAMA 2002; 288: 2836 -2845. Unutzer et al, JAMA 2002. P<. 0001
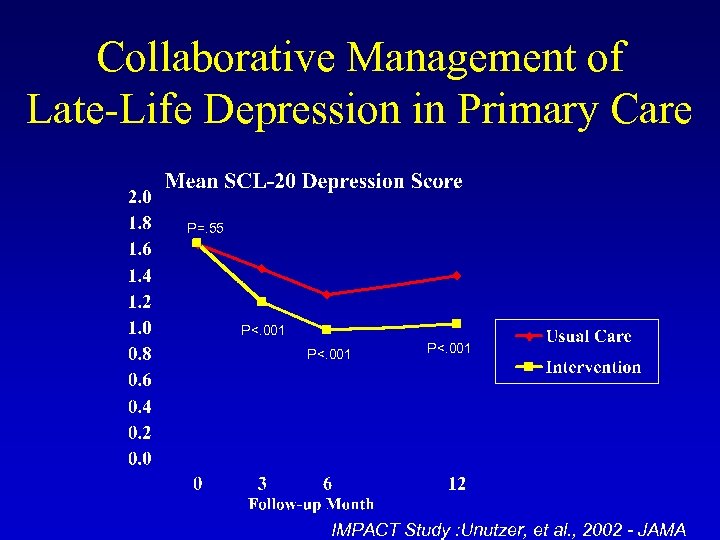 Collaborative Management of Late-Life Depression in Primary Care P=. 55 P<. 001 IMPACT Study : Unutzer, et al. , 2002 - JAMA
Collaborative Management of Late-Life Depression in Primary Care P=. 55 P<. 001 IMPACT Study : Unutzer, et al. , 2002 - JAMA
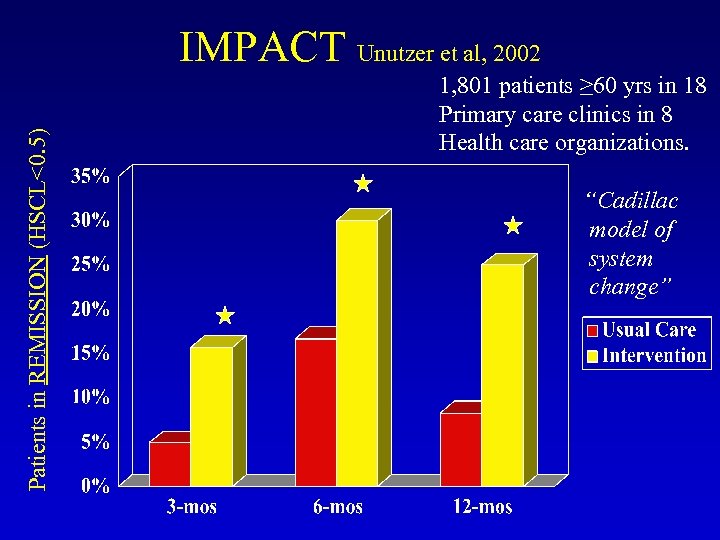 Patients in REMISSION (HSCL<0. 5) IMPACT Unutzer et al, 2002 1, 801 patients ≥ 60 yrs in 18 Primary care clinics in 8 Health care organizations. “Cadillac model of system change”
Patients in REMISSION (HSCL<0. 5) IMPACT Unutzer et al, 2002 1, 801 patients ≥ 60 yrs in 18 Primary care clinics in 8 Health care organizations. “Cadillac model of system change”
 PROSPECT • USUAL CARE vs. INTERVENTION: • Clinical Algorithm for Geriatric Depression Consisting of Citalopram or IPT (based on patient preference) • Depression Care Manager: Social Workers, Nurses, Psychologists in Primary Care: Depression recognition, guideline based treatment, monitoring of response to treatment, follow-up
PROSPECT • USUAL CARE vs. INTERVENTION: • Clinical Algorithm for Geriatric Depression Consisting of Citalopram or IPT (based on patient preference) • Depression Care Manager: Social Workers, Nurses, Psychologists in Primary Care: Depression recognition, guideline based treatment, monitoring of response to treatment, follow-up
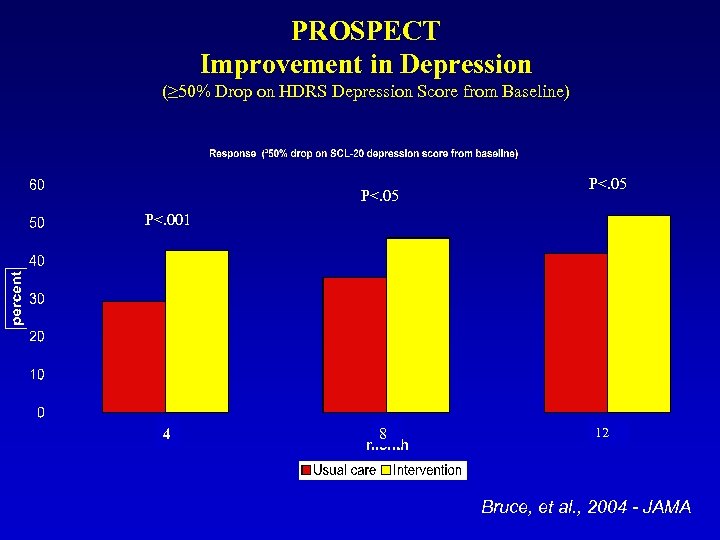 PROSPECT Improvement in Depression (≥ 50% Drop on HDRS Depression Score from Baseline) P<. 05 P<. 001 4 8 12 Bruce, et al. , 2004 - JAMA
PROSPECT Improvement in Depression (≥ 50% Drop on HDRS Depression Score from Baseline) P<. 05 P<. 001 4 8 12 Bruce, et al. , 2004 - JAMA
 PROSPECT Depression Specialist with Treatment Algorithm • Practices with Depression Specialist Using Treatment Algorithm for Depression had Greater Reduction in Depression Compared to Usual Care Practices • However, Better Outcomes Only For Major Depression, Not for Minor Depression Bruce, et al. , 2004 - JAMA
PROSPECT Depression Specialist with Treatment Algorithm • Practices with Depression Specialist Using Treatment Algorithm for Depression had Greater Reduction in Depression Compared to Usual Care Practices • However, Better Outcomes Only For Major Depression, Not for Minor Depression Bruce, et al. , 2004 - JAMA
 Conclusions: Integrated Mental Health Services in Primary Care • Better engagement …. similar outcomes compared to referral care (perhaps slightly less effective for major depression) • Better engagement and outcomes compared to usual care…. . especially with care management, standardized screening and outcome tracking, and treatment protocols
Conclusions: Integrated Mental Health Services in Primary Care • Better engagement …. similar outcomes compared to referral care (perhaps slightly less effective for major depression) • Better engagement and outcomes compared to usual care…. . especially with care management, standardized screening and outcome tracking, and treatment protocols
 st & 2 nd Generation Summary of 1 Studies • Multiple component interventions • Lectures &/or distributing guidelines do not change behavior nor outcomes • Adding patient tracking with a care manager significantly improves outcomes • Including a mental health specialist in an integrated treating or consulting role improves outcomes the most
st & 2 nd Generation Summary of 1 Studies • Multiple component interventions • Lectures &/or distributing guidelines do not change behavior nor outcomes • Adding patient tracking with a care manager significantly improves outcomes • Including a mental health specialist in an integrated treating or consulting role improves outcomes the most
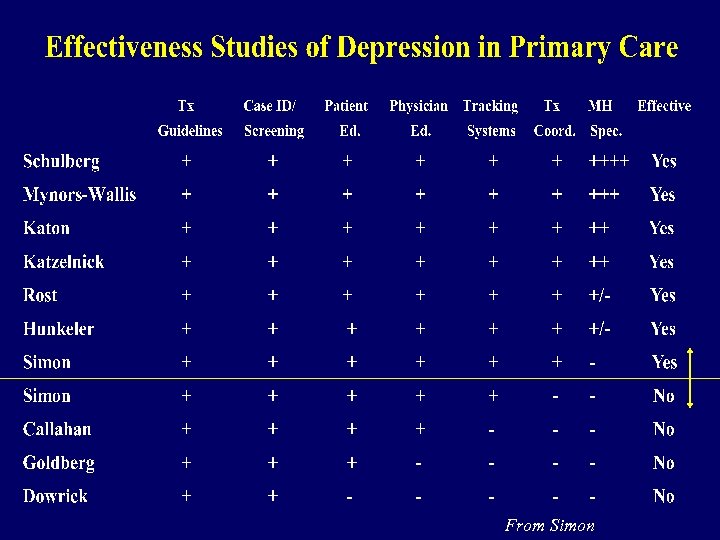 From Simon
From Simon
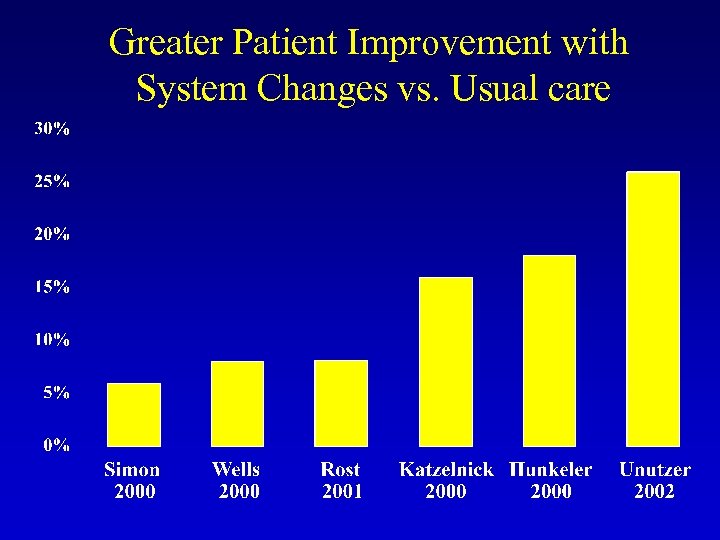 Greater Patient Improvement with System Changes vs. Usual care
Greater Patient Improvement with System Changes vs. Usual care
 st & 2 nd Generation Summary of 1 Studies • Multiple component interventions • Lectures &/or distributing guidelines do not change behavior nor outcomes • Adding patient tracking with a care manager significantly improves outcomes • Including a mental health specialist in an integrated treating or consulting role improves outcomes the most
st & 2 nd Generation Summary of 1 Studies • Multiple component interventions • Lectures &/or distributing guidelines do not change behavior nor outcomes • Adding patient tracking with a care manager significantly improves outcomes • Including a mental health specialist in an integrated treating or consulting role improves outcomes the most
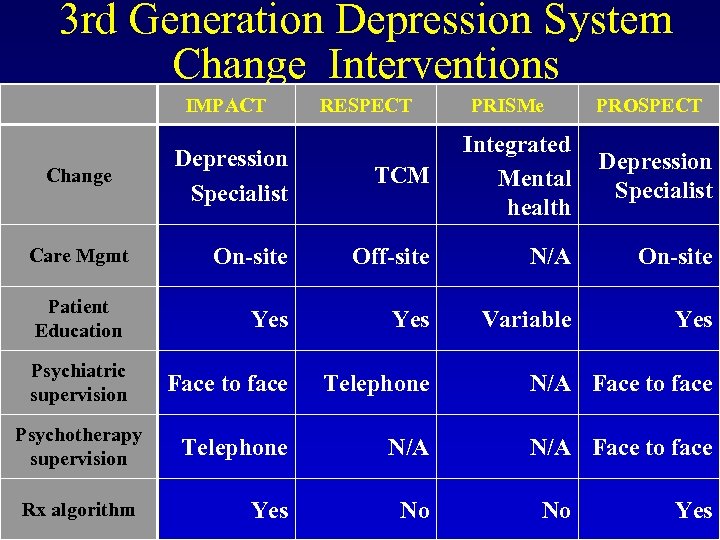 3 rd Generation Depression System Change Interventions IMPACT RESPECT PRISMe PROSPECT Depression Specialist TCM Integrated Mental health Care Mgmt On-site Off-site N/A On-site Patient Education Yes Variable Yes Psychiatric supervision Face to face Telephone N/A N/A Face to face Yes No Change Psychotherapy supervision Rx algorithm No Depression Specialist Yes
3 rd Generation Depression System Change Interventions IMPACT RESPECT PRISMe PROSPECT Depression Specialist TCM Integrated Mental health Care Mgmt On-site Off-site N/A On-site Patient Education Yes Variable Yes Psychiatric supervision Face to face Telephone N/A N/A Face to face Yes No Change Psychotherapy supervision Rx algorithm No Depression Specialist Yes
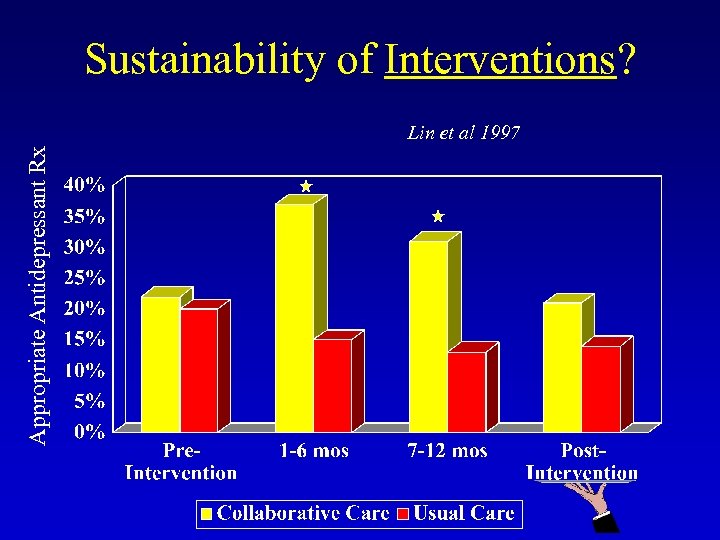 Sustainability of Interventions? Appropriate Antidepressant Rx Lin et al 1997
Sustainability of Interventions? Appropriate Antidepressant Rx Lin et al 1997
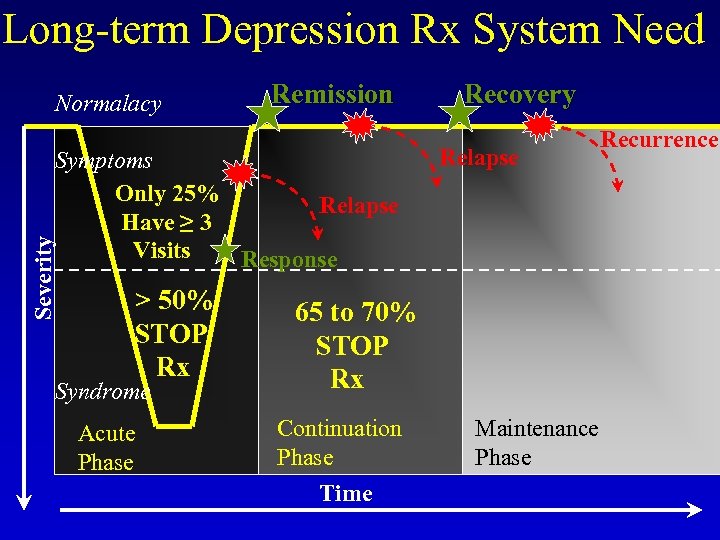 Long-term Depression Rx System Need Normalacy Remission Severity Symptoms Only 25% Relapse Have ≥ 3 Visits Response > 50% STOP Rx Syndrome Acute Phase Recovery Relapse 65 to 70% STOP Rx Continuation Phase Time Maintenance Phase Recurrence
Long-term Depression Rx System Need Normalacy Remission Severity Symptoms Only 25% Relapse Have ≥ 3 Visits Response > 50% STOP Rx Syndrome Acute Phase Recovery Relapse 65 to 70% STOP Rx Continuation Phase Time Maintenance Phase Recurrence
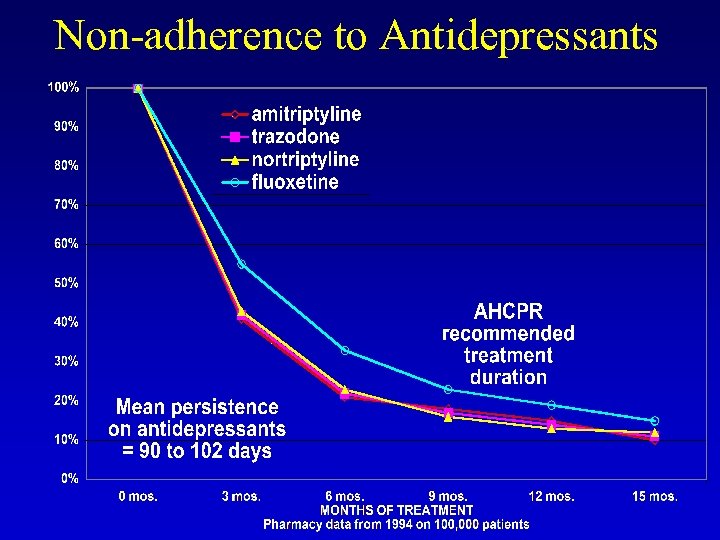 Non-adherence to Antidepressants
Non-adherence to Antidepressants
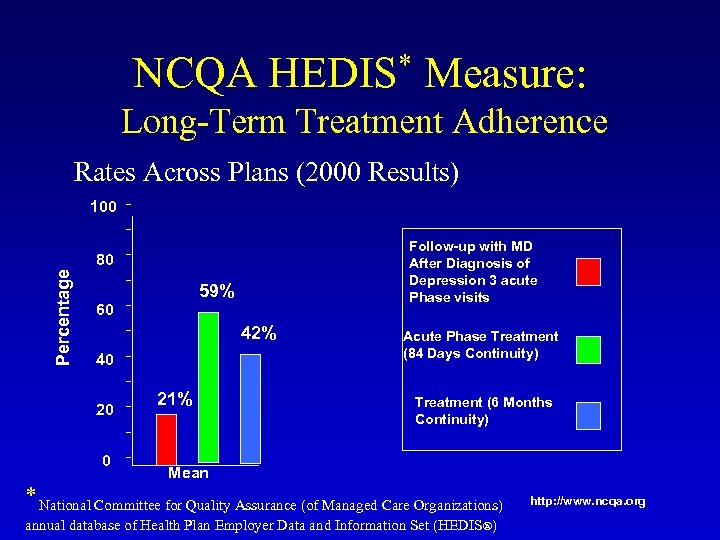 NCQA HEDIS* Measure: Long-Term Treatment Adherence Rates Across Plans (2000 Results) 100 Follow-up with MD After Diagnosis of Depression 3 acute Phase visits Percentage 80 59% 60 42% 40 20 0 21% Acute Phase Treatment (84 Days Continuity) Treatment (6 Months Continuity) Mean * National Committee for Quality Assurance (of Managed Care Organizations) annual database of Health Plan Employer Data and Information Set (HEDIS®) http: //www. ncqa. org
NCQA HEDIS* Measure: Long-Term Treatment Adherence Rates Across Plans (2000 Results) 100 Follow-up with MD After Diagnosis of Depression 3 acute Phase visits Percentage 80 59% 60 42% 40 20 0 21% Acute Phase Treatment (84 Days Continuity) Treatment (6 Months Continuity) Mean * National Committee for Quality Assurance (of Managed Care Organizations) annual database of Health Plan Employer Data and Information Set (HEDIS®) http: //www. ncqa. org
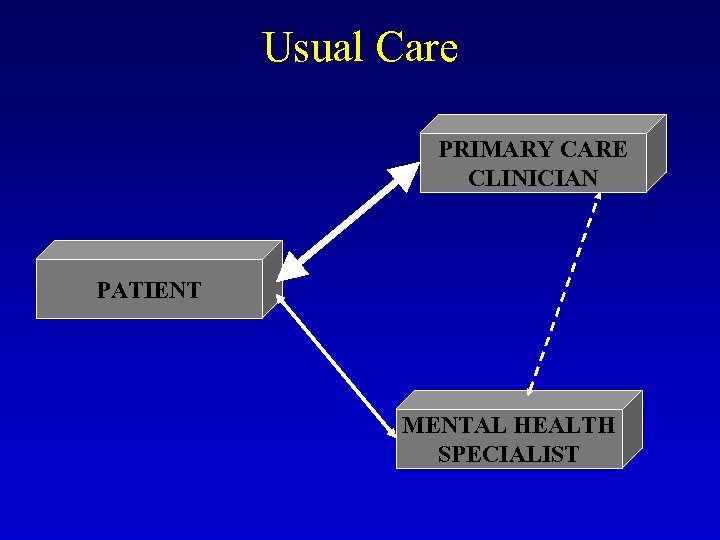 Usual Care PRIMARY CARE CLINICIAN PATIENT MENTAL HEALTH SPECIALIST
Usual Care PRIMARY CARE CLINICIAN PATIENT MENTAL HEALTH SPECIALIST
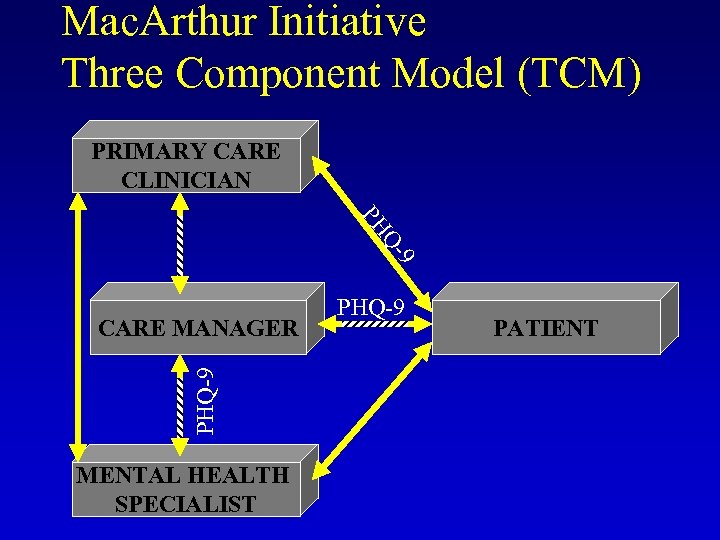 Mac. Arthur Initiative Three Component Model (TCM) PRIMARY CARE CLINICIAN PH 9 Q- PHQ-9 CARE MANAGER MENTAL HEALTH SPECIALIST PHQ-9 PATIENT
Mac. Arthur Initiative Three Component Model (TCM) PRIMARY CARE CLINICIAN PH 9 Q- PHQ-9 CARE MANAGER MENTAL HEALTH SPECIALIST PHQ-9 PATIENT
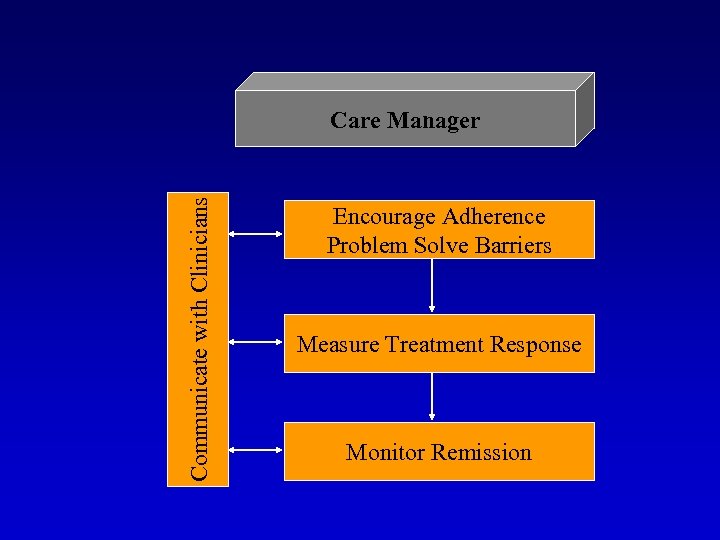 Communicate with Clinicians Care Manager Encourage Adherence Problem Solve Barriers Measure Treatment Response Monitor Remission
Communicate with Clinicians Care Manager Encourage Adherence Problem Solve Barriers Measure Treatment Response Monitor Remission
 Two Question Screen U. S. Preventive Services Task Force Ann Intern Med 2002; 136: 760 -4 Over the past 2 weeks, have you: • Felt little interest or pleasure in doing things? • Felt down, depressed, or hopeless?
Two Question Screen U. S. Preventive Services Task Force Ann Intern Med 2002; 136: 760 -4 Over the past 2 weeks, have you: • Felt little interest or pleasure in doing things? • Felt down, depressed, or hopeless?
 PHQ-9 Spitzer R, et al. Validation and utility of a self-report version of PRIMEMD: the PHQ Primary Care Study. JAMA 1999; 282: 1737 -1744 Kroenke K, et al. The PHQ-9: validity of a brief depression severity measure. Journal of General Internal Medicine 2001; 16: 606 -613 Sensitivity = 73% Specificity = 94% Correlation between PHQ self-report and psychiatrist interview =. 84
PHQ-9 Spitzer R, et al. Validation and utility of a self-report version of PRIMEMD: the PHQ Primary Care Study. JAMA 1999; 282: 1737 -1744 Kroenke K, et al. The PHQ-9: validity of a brief depression severity measure. Journal of General Internal Medicine 2001; 16: 606 -613 Sensitivity = 73% Specificity = 94% Correlation between PHQ self-report and psychiatrist interview =. 84
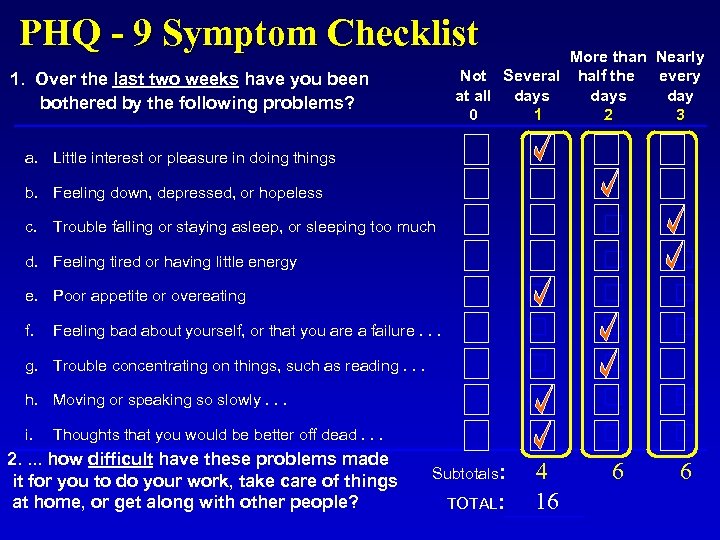 PHQ - 9 Symptom Checklist More than Nearly Not Several half the every at all days day 0 1 2 3 1. Over the last two weeks have you been bothered by the following problems? a. Little interest or pleasure in doing things b. Feeling down, depressed, or hopeless c. Trouble falling or staying asleep, or sleeping too much d. Feeling tired or having little energy e. Poor appetite or overeating f. Feeling bad about yourself, or that you are a failure. . . g. Trouble concentrating on things, such as reading. . . h. Moving or speaking so slowly. . . i. Thoughts that you would be better off dead. . . 2. . how difficult have these problems made it for you to do your work, take care of things at home, or get along with other people? Subtotals: 4 TOTAL: 16 6 6
PHQ - 9 Symptom Checklist More than Nearly Not Several half the every at all days day 0 1 2 3 1. Over the last two weeks have you been bothered by the following problems? a. Little interest or pleasure in doing things b. Feeling down, depressed, or hopeless c. Trouble falling or staying asleep, or sleeping too much d. Feeling tired or having little energy e. Poor appetite or overeating f. Feeling bad about yourself, or that you are a failure. . . g. Trouble concentrating on things, such as reading. . . h. Moving or speaking so slowly. . . i. Thoughts that you would be better off dead. . . 2. . how difficult have these problems made it for you to do your work, take care of things at home, or get along with other people? Subtotals: 4 TOTAL: 16 6 6
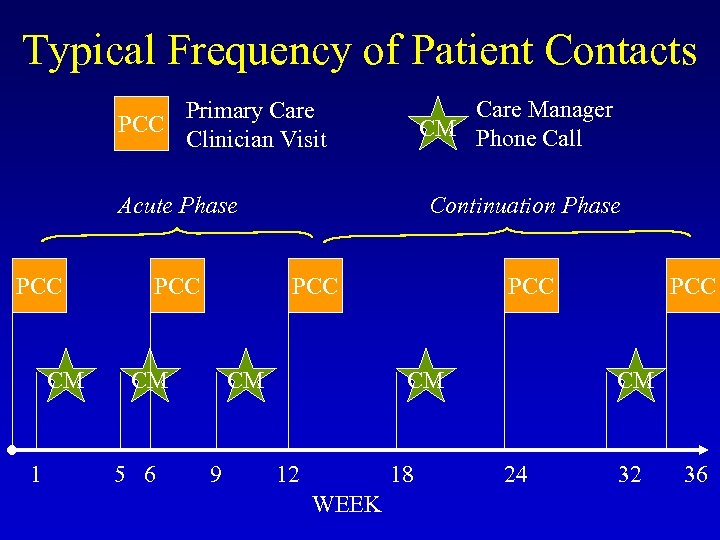 Typical Frequency of Patient Contacts PCC Primary Care Clinician Visit Acute Phase PCC CM Care Manager CM Phone Call Continuation Phase PCC CM 1 5 6 9 12 18 24 32 36 WEEK
Typical Frequency of Patient Contacts PCC Primary Care Clinician Visit Acute Phase PCC CM Care Manager CM Phone Call Continuation Phase PCC CM 1 5 6 9 12 18 24 32 36 WEEK
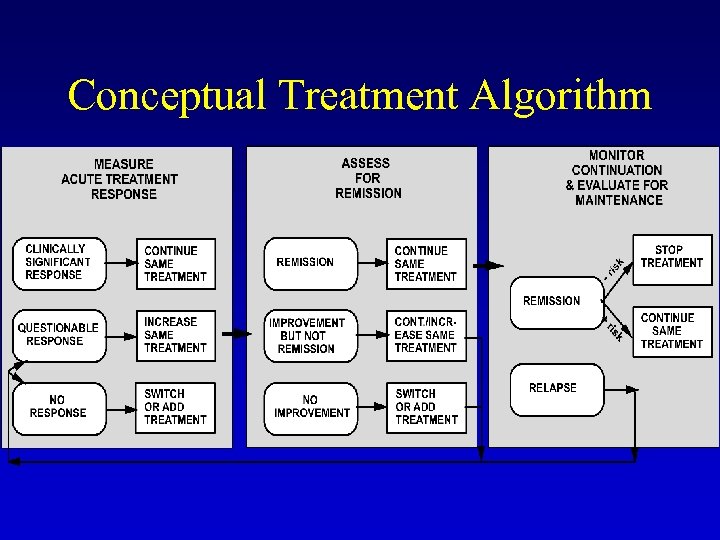 Conceptual Treatment Algorithm
Conceptual Treatment Algorithm
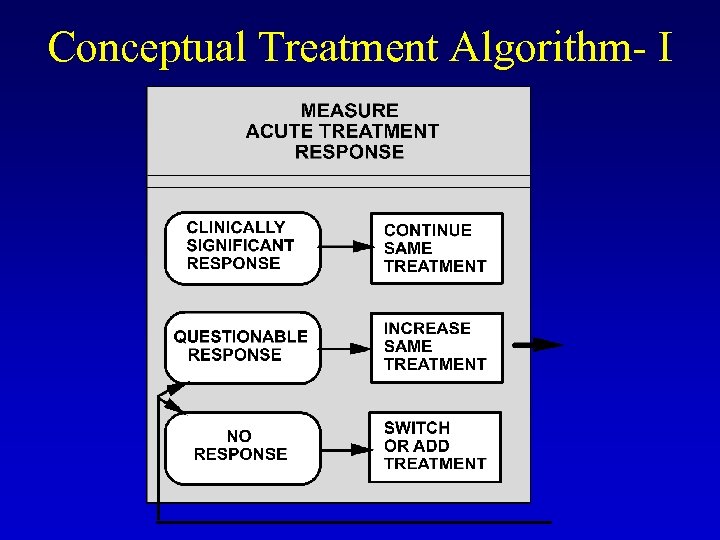 Conceptual Treatment Algorithm- I
Conceptual Treatment Algorithm- I
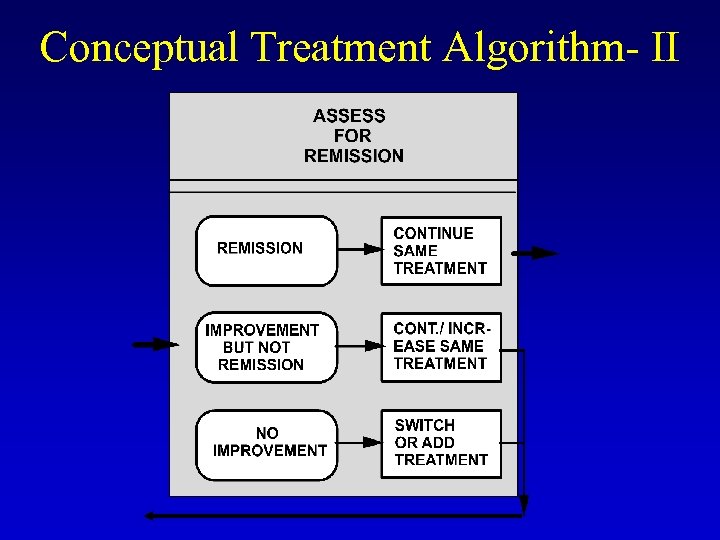 Conceptual Treatment Algorithm- II
Conceptual Treatment Algorithm- II
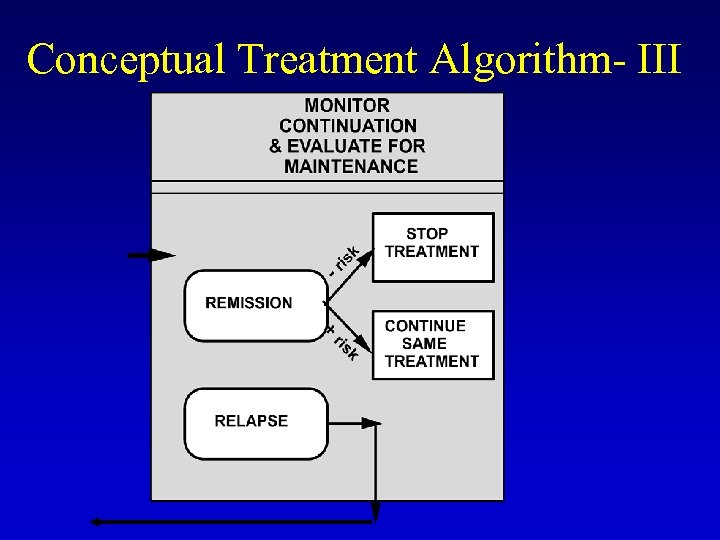 Conceptual Treatment Algorithm- III
Conceptual Treatment Algorithm- III
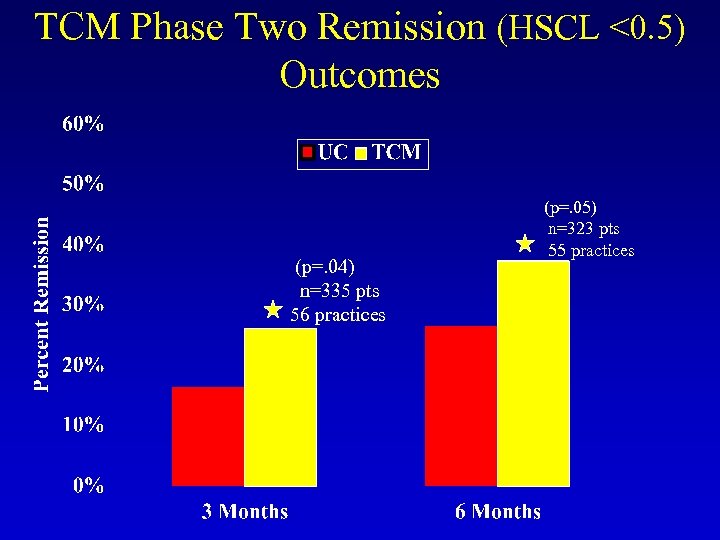 TCM Phase Two Remission (HSCL <0. 5) Outcomes (p=. 04) n=335 pts 56 practices (p=. 05) n=323 pts 55 practices
TCM Phase Two Remission (HSCL <0. 5) Outcomes (p=. 04) n=335 pts 56 practices (p=. 05) n=323 pts 55 practices
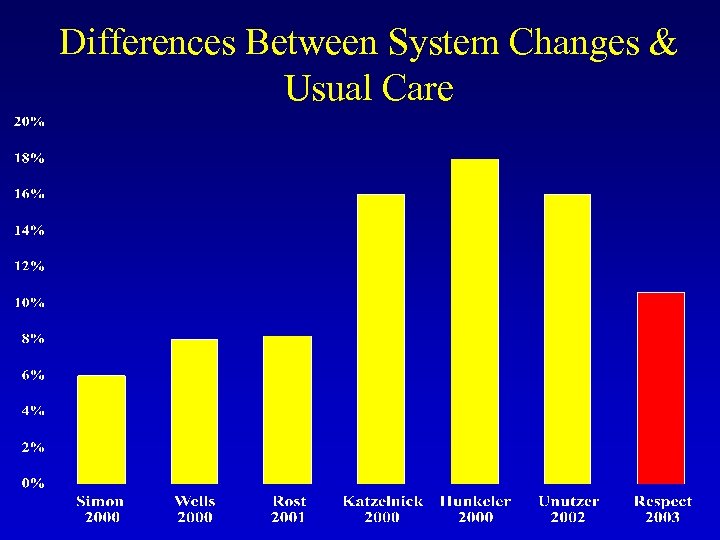 Differences Between System Changes & Usual Care
Differences Between System Changes & Usual Care
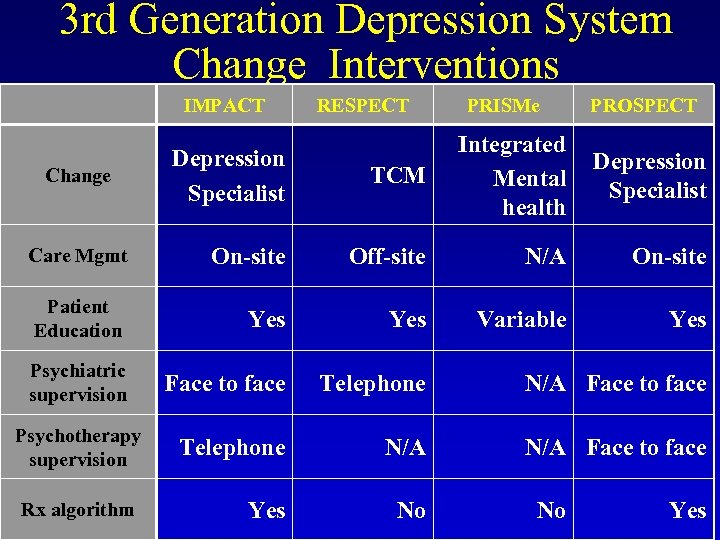 3 rd Generation Depression System Change Interventions IMPACT RESPECT PRISMe PROSPECT Depression Specialist TCM Integrated Mental health Care Mgmt On-site Off-site N/A On-site Patient Education Yes Variable Yes Psychiatric supervision Face to face Telephone N/A N/A Face to face Yes No Change Psychotherapy supervision Rx algorithm No Depression Specialist Yes
3 rd Generation Depression System Change Interventions IMPACT RESPECT PRISMe PROSPECT Depression Specialist TCM Integrated Mental health Care Mgmt On-site Off-site N/A On-site Patient Education Yes Variable Yes Psychiatric supervision Face to face Telephone N/A N/A Face to face Yes No Change Psychotherapy supervision Rx algorithm No Depression Specialist Yes
 Implications for Applied Policy and Practice
Implications for Applied Policy and Practice
 Leon Eisenberg SOUNDING BOARD TREATING DEPRESSION AND ANXIETY IN PRIMARY CARE. Closing the gap between knowledge and practice N Engl J Med 1992; 326: 1080 -1084, Apr 16, 1992 7 th Annual Rosalyn Carter Symposium on Mental Health Policy, Atlanta, Nov 21, 1991 • Depression is common in primary care, with substantial morbidity • Under recognized - not because of curriculum, but values of patients and physicians, inappropriate DSM nosology • Target physicians in practice, involve patient, more follow-up consider special nurses, improve payment - reward time, assess quality
Leon Eisenberg SOUNDING BOARD TREATING DEPRESSION AND ANXIETY IN PRIMARY CARE. Closing the gap between knowledge and practice N Engl J Med 1992; 326: 1080 -1084, Apr 16, 1992 7 th Annual Rosalyn Carter Symposium on Mental Health Policy, Atlanta, Nov 21, 1991 • Depression is common in primary care, with substantial morbidity • Under recognized - not because of curriculum, but values of patients and physicians, inappropriate DSM nosology • Target physicians in practice, involve patient, more follow-up consider special nurses, improve payment - reward time, assess quality
 • Subcommittee on Mental Health and Aging: Recommendations on Policy • Subcommittee on the Mental Health Interface with General Medicine • Integrating Mental Health and General Health Care • Implementing Evidence-based Medicine
• Subcommittee on Mental Health and Aging: Recommendations on Policy • Subcommittee on the Mental Health Interface with General Medicine • Integrating Mental Health and General Health Care • Implementing Evidence-based Medicine
 • “The Federal Government should add evidence-based collaborative care services for psychiatric disorders to the list of covered services through the Medicare National Coverage Process”
• “The Federal Government should add evidence-based collaborative care services for psychiatric disorders to the list of covered services through the Medicare National Coverage Process”
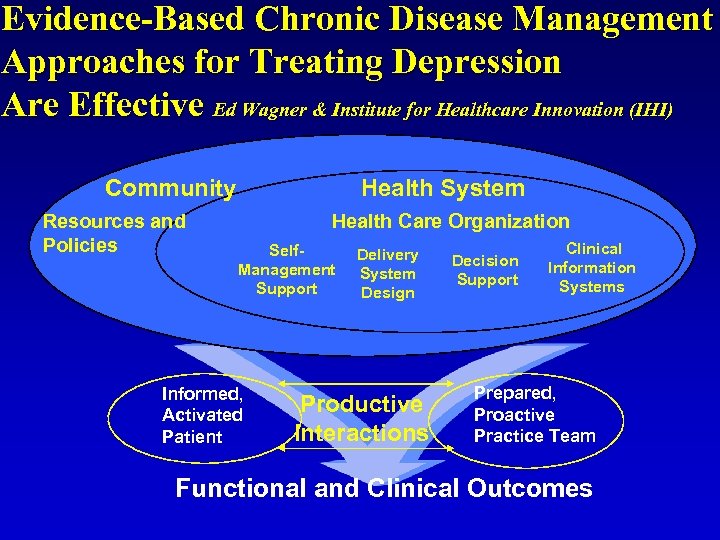 Evidence-Based Chronic Disease Management Approaches for Treating Depression Are Effective Ed Wagner & Institute for Healthcare Innovation (IHI) Community Resources and Policies Health System Health Care Organization Self. Management Support Informed, Activated Patient Delivery System Design Productive Interactions Decision Support Clinical Information Systems Prepared, Proactive Practice Team Functional and Clinical Outcomes
Evidence-Based Chronic Disease Management Approaches for Treating Depression Are Effective Ed Wagner & Institute for Healthcare Innovation (IHI) Community Resources and Policies Health System Health Care Organization Self. Management Support Informed, Activated Patient Delivery System Design Productive Interactions Decision Support Clinical Information Systems Prepared, Proactive Practice Team Functional and Clinical Outcomes


