850414a86185ba826753153b74cb347e.ppt
- Количество слайдов: 68
 Innovation in Occupational Therapy Practice Evidence of OT Effectiveness in Working with Family Caregivers of Individuals with Dementia Results from the NIH REACH Initiative Laura N. Gitlin, Ph. D. Professor, Department of Occupational Therapy Director, Community and Homecare Research Division, Thomas Jefferson University Funded by NIA # U 01 AG 013265
Innovation in Occupational Therapy Practice Evidence of OT Effectiveness in Working with Family Caregivers of Individuals with Dementia Results from the NIH REACH Initiative Laura N. Gitlin, Ph. D. Professor, Department of Occupational Therapy Director, Community and Homecare Research Division, Thomas Jefferson University Funded by NIA # U 01 AG 013265
 Research Team Members Co-investigators • Mary Corcoran, Ph. D. , OTR/L • Susan Klein, MSW Project Managers • Laraine Winter, Ph. D. • Sandy Schinfeld, MPH Data management/analysis • Marie Dennis, Ph. D. • Mary Barnett • Walter Hauck, Ph. D. Interviewers • Annemarie Gregory • Julie Liebman, MA Interventionists • Geri Shaw, OTR/L • Tracey Vause Earland, MS, OTR/L • Susan Eckhardt, OTR/L • Linda Levy, MS, OTR/L • Roz Lipsett, MS, OTR/L • Pam Kearney, MS, OTR/L
Research Team Members Co-investigators • Mary Corcoran, Ph. D. , OTR/L • Susan Klein, MSW Project Managers • Laraine Winter, Ph. D. • Sandy Schinfeld, MPH Data management/analysis • Marie Dennis, Ph. D. • Mary Barnett • Walter Hauck, Ph. D. Interviewers • Annemarie Gregory • Julie Liebman, MA Interventionists • Geri Shaw, OTR/L • Tracey Vause Earland, MS, OTR/L • Susan Eckhardt, OTR/L • Linda Levy, MS, OTR/L • Roz Lipsett, MS, OTR/L • Pam Kearney, MS, OTR/L
 Overview of Presentation • Quick facts about family caregivers • Environment as treatment modality • NIH REACH initiative • Environmental Skill-building program • Study outcomes • Clinical guidelines • Conclusions
Overview of Presentation • Quick facts about family caregivers • Environment as treatment modality • NIH REACH initiative • Environmental Skill-building program • Study outcomes • Clinical guidelines • Conclusions

 Case Scenario • 72 year old wife caring for 75 year old husband with moderate stage dementia: – – – – Husband verbally abusive Wakes up several times at night Difficulty with dressing and bathing but resists care Tries to leave home Suspicious of visitors Has had several falls Constant supervision required • Caregiver has osteoporosis and high blood pressure • Caregiver providing care for 8 years
Case Scenario • 72 year old wife caring for 75 year old husband with moderate stage dementia: – – – – Husband verbally abusive Wakes up several times at night Difficulty with dressing and bathing but resists care Tries to leave home Suspicious of visitors Has had several falls Constant supervision required • Caregiver has osteoporosis and high blood pressure • Caregiver providing care for 8 years
 Key Facts About Dementia and Caregiving • 4 million+ diagnosed with Alzheimer’s disease or related disorder • 50% + persons >85 years of age have mild cognitive impairment or dementia • >50% of persons with dementia cared for at home • Average course of disease is 8 years – Range from 4 to 20 years
Key Facts About Dementia and Caregiving • 4 million+ diagnosed with Alzheimer’s disease or related disorder • 50% + persons >85 years of age have mild cognitive impairment or dementia • >50% of persons with dementia cared for at home • Average course of disease is 8 years – Range from 4 to 20 years
 Who Provides Care to Persons with Dementia? • Most caregivers are: – Women (spouses and daughters) – Spouses – Aging • Caregiving occurs across all racial, ethnic and socioeconomic groups • Caregiving does not stop with nursing home placement
Who Provides Care to Persons with Dementia? • Most caregivers are: – Women (spouses and daughters) – Spouses – Aging • Caregiving occurs across all racial, ethnic and socioeconomic groups • Caregiving does not stop with nursing home placement
 Family Caregivers: The Hidden Patient AT RISK FOR: – Depression (>50% caregivers are depressed) – Morbidity – Financial loss – Social isolation – Extreme fatigue, stress – Anxiety, upset, feeling overwhelmed – Mortality Schulz, et al, 1995. The Gerontologist, 35, 771 -791; Ory et al. , 1999, The Gerontologist, 37, 804 -815 Schulz & Beach, 1999, JAMA, 282, 22152219
Family Caregivers: The Hidden Patient AT RISK FOR: – Depression (>50% caregivers are depressed) – Morbidity – Financial loss – Social isolation – Extreme fatigue, stress – Anxiety, upset, feeling overwhelmed – Mortality Schulz, et al, 1995. The Gerontologist, 35, 771 -791; Ory et al. , 1999, The Gerontologist, 37, 804 -815 Schulz & Beach, 1999, JAMA, 282, 22152219
 Clinical Trial Research with Family Caregivers • 10+ years of research substantiates negative consequences of caregiving • Clinical trials show: – Underutilization of services – Minimal to modest treatment benefits – Interventions not well-described/difficult to replicate – Need for new models and in-home supportive services
Clinical Trial Research with Family Caregivers • 10+ years of research substantiates negative consequences of caregiving • Clinical trials show: – Underutilization of services – Minimal to modest treatment benefits – Interventions not well-described/difficult to replicate – Need for new models and in-home supportive services
 Stress Health Process Model Stressors • Care Recipient Behavior • Social Environment • Physical Environment Appraisals of Demands and Adaptive Capacities Perceived Stress PRIMARY TARGET: Environmental Strategies Targeting Care Recipient, and/or Social and Physical Environment SECONDARY TARGET: Environmental Strategies Targeting Caregiver Cognitive Skills and Knowledge Negative Physiological, Affective, Behavioral Response Increased Risk for Mental/Physical Health Problems Schulz R (Ed) Handbook on Dementia Caregiving, (pp. 33 -56), NY: Springer.
Stress Health Process Model Stressors • Care Recipient Behavior • Social Environment • Physical Environment Appraisals of Demands and Adaptive Capacities Perceived Stress PRIMARY TARGET: Environmental Strategies Targeting Care Recipient, and/or Social and Physical Environment SECONDARY TARGET: Environmental Strategies Targeting Caregiver Cognitive Skills and Knowledge Negative Physiological, Affective, Behavioral Response Increased Risk for Mental/Physical Health Problems Schulz R (Ed) Handbook on Dementia Caregiving, (pp. 33 -56), NY: Springer.
 Environment as Treatment Modality • Based in competence-environmental press model • Involves modification to physical, task and social dimensions of environments (Barris et al) • Purpose: – Achieve balance between environmental demands (press) and person capabilities (competencies) – Reduce environmental press to match person capabilities – Decrease excess disability
Environment as Treatment Modality • Based in competence-environmental press model • Involves modification to physical, task and social dimensions of environments (Barris et al) • Purpose: – Achieve balance between environmental demands (press) and person capabilities (competencies) – Reduce environmental press to match person capabilities – Decrease excess disability
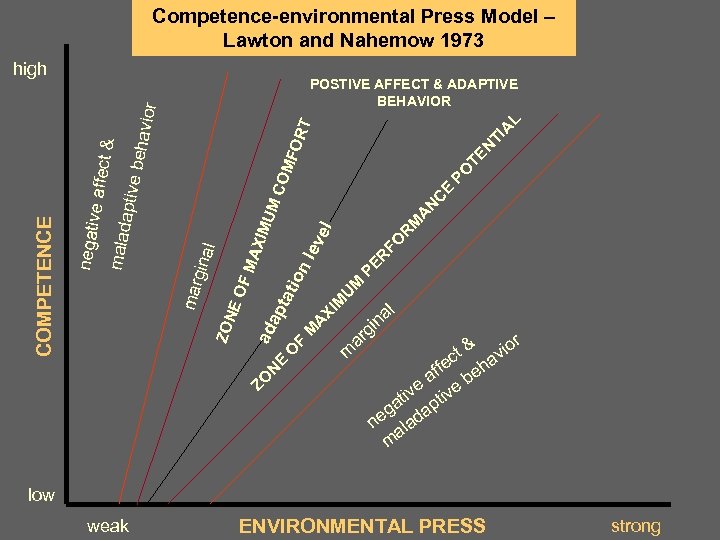 Competence-environmental Press Model – Lawton and Nahemow 1973 ZO N E O F L M R FO U M M A XI ap ta t M ion PE R l ev AX I ad ZON EO FM l gina ma r el MU A N C E MC PO OM TE N TI FOR A T behav ior POSTIVE AFFECT & ADAPTIVE BEHAVIOR aptive ma l a d negat iv COMPETENCE e af f ec t& high m ar g a in l & io ct hav fe af be e e t iv pt iv a eg ada n l a m r low weak ENVIRONMENTAL PRESS strong
Competence-environmental Press Model – Lawton and Nahemow 1973 ZO N E O F L M R FO U M M A XI ap ta t M ion PE R l ev AX I ad ZON EO FM l gina ma r el MU A N C E MC PO OM TE N TI FOR A T behav ior POSTIVE AFFECT & ADAPTIVE BEHAVIOR aptive ma l a d negat iv COMPETENCE e af f ec t& high m ar g a in l & io ct hav fe af be e e t iv pt iv a eg ada n l a m r low weak ENVIRONMENTAL PRESS strong
 For Persons with Dementia Use Environmental Modifications To: • • • Decrease disorientation Increase way finding Support functionality Increase activity engagement Increase safety Minimize behavioral disturbances
For Persons with Dementia Use Environmental Modifications To: • • • Decrease disorientation Increase way finding Support functionality Increase activity engagement Increase safety Minimize behavioral disturbances
 For Family Caregivers Use Environmental Modifications To: • • • Increase personal safety Enhance ability to manage day to day Enhance mastery Decrease stress Decrease need for assistance Decrease amount of time in hands-on supervision
For Family Caregivers Use Environmental Modifications To: • • • Increase personal safety Enhance ability to manage day to day Enhance mastery Decrease stress Decrease need for assistance Decrease amount of time in hands-on supervision
 Evidence of Effectiveness of Environment Approach • Institutional-based research: – Special Dementia Units – Reduction of disruptive behaviors – Enhancement of orientation, engagement • In-home descriptive studies: – Family CGs modify homes for safety – Families lack information about equipment and environmental strategies Calkins, (1989). Design for dementia; Pynoos & Ohta (1991). Occupational Therapy and Physical Therapy in Geriatrics, 9, 83 -92; Gitlin & Corcoran, (1996). Technology and Disability, 2, 112 -21.
Evidence of Effectiveness of Environment Approach • Institutional-based research: – Special Dementia Units – Reduction of disruptive behaviors – Enhancement of orientation, engagement • In-home descriptive studies: – Family CGs modify homes for safety – Families lack information about equipment and environmental strategies Calkins, (1989). Design for dementia; Pynoos & Ohta (1991). Occupational Therapy and Physical Therapy in Geriatrics, 9, 83 -92; Gitlin & Corcoran, (1996). Technology and Disability, 2, 112 -21.
 Evidence of Effectiveness of Environment Approach 3 month in-home OT environmental intervention (NIA) with 202 caregivers: • Slows decline in CR’s IADL and ADL dependence • Enhances CG self-efficacy • Decreases upset with ADL dependence and behavior disturbances • Women benefit more than men caregivers Gitlin, et al. , (2001). The Gerontologist, 41, 4 -14. Gitlin, et al. , (1999). Family Relations, 48, 363 -372.
Evidence of Effectiveness of Environment Approach 3 month in-home OT environmental intervention (NIA) with 202 caregivers: • Slows decline in CR’s IADL and ADL dependence • Enhances CG self-efficacy • Decreases upset with ADL dependence and behavior disturbances • Women benefit more than men caregivers Gitlin, et al. , (2001). The Gerontologist, 41, 4 -14. Gitlin, et al. , (1999). Family Relations, 48, 363 -372.
 HOME ENVIRONMENTAL SKILLBUILDING PROTGRAM (ESP) • NIH REACH Multi-site 6 year initiative • 6 sites each testing a different intervention • Phila site – ESP – Built on previous dementia study – Greater intensity, more systematic, installation of equipment – Examined broader range of outcomes and validation of previous findings
HOME ENVIRONMENTAL SKILLBUILDING PROTGRAM (ESP) • NIH REACH Multi-site 6 year initiative • 6 sites each testing a different intervention • Phila site – ESP – Built on previous dementia study – Greater intensity, more systematic, installation of equipment – Examined broader range of outcomes and validation of previous findings
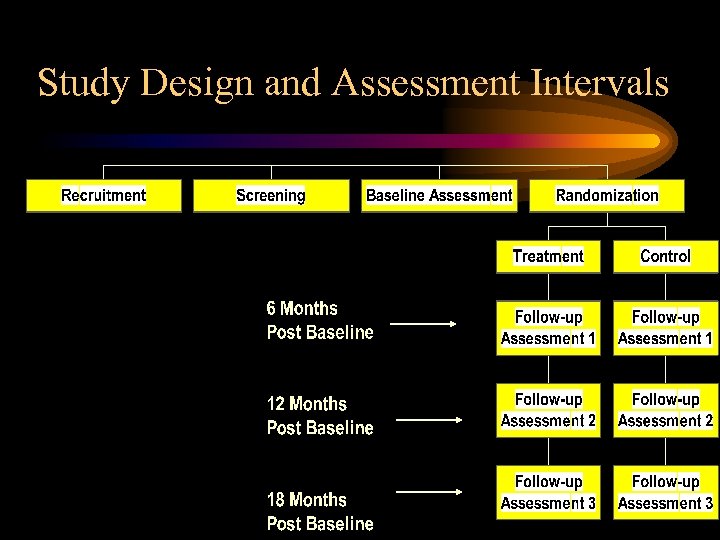 Study Design and Assessment Intervals
Study Design and Assessment Intervals
 Baseline Characteristics of Sample (N = 255) • Gender – 74. 5% female • Race – 48. 2% White – 47. 8% African American – 4% Other • Relationship – 38. 8% Spouses – 61. 2% Non spouses
Baseline Characteristics of Sample (N = 255) • Gender – 74. 5% female • Race – 48. 2% White – 47. 8% African American – 4% Other • Relationship – 38. 8% Spouses – 61. 2% Non spouses
 Sample • 255 Caregivers enrolled • 190 had 6 -month data available – 89 experimental, 101 controls • 26% rate of attrition
Sample • 255 Caregivers enrolled • 190 had 6 -month data available – 89 experimental, 101 controls • 26% rate of attrition
 Characteristics (cont. ) Characteristics – CG Age – CG Education – Years Caregiving – CR MMSE – CG depression MEAN (SD) 61. 01 (14. 30) 12. 23 (2. 62) 4. 24 (3. 77) 12. 30 (7. 05) 14. 90 (11. 6)
Characteristics (cont. ) Characteristics – CG Age – CG Education – Years Caregiving – CR MMSE – CG depression MEAN (SD) 61. 01 (14. 30) 12. 23 (2. 62) 4. 24 (3. 77) 12. 30 (7. 05) 14. 90 (11. 6)
 Environmental Skill-building Program (ESP)
Environmental Skill-building Program (ESP)
 Environmental Skill-building Program (ESP) ACTIVE PHASE (6 Months - 5 home visits & 1 tele-contact) • Education about role of environment and dementia • Skills in problem-solving, simplifying the environment to address 11 potential problem areas • Technical support (e. g. , adaptive devices and training in use)
Environmental Skill-building Program (ESP) ACTIVE PHASE (6 Months - 5 home visits & 1 tele-contact) • Education about role of environment and dementia • Skills in problem-solving, simplifying the environment to address 11 potential problem areas • Technical support (e. g. , adaptive devices and training in use)
 Intervention Protocol • 1 st home visit – assessment; education about dementia, identification of problem areas • 2 nd home visit – problem solving about target problem (antecedents, behavior, consequences) • 3 -5 th home and telephone contact – introduce, practice, modify, refine strategies for each target problem; installation of equipment, adaptive devices • 6 th home visit – review strategies, generalize process
Intervention Protocol • 1 st home visit – assessment; education about dementia, identification of problem areas • 2 nd home visit – problem solving about target problem (antecedents, behavior, consequences) • 3 -5 th home and telephone contact – introduce, practice, modify, refine strategies for each target problem; installation of equipment, adaptive devices • 6 th home visit – review strategies, generalize process
 Eleven Target Problems Care Recipient: • Bathing • Toileting • Dressing • Eating • Communication • Mobility • • Catastrophic Reactions Wandering Safety Leisure/IADL • Caregiver-centered concerns
Eleven Target Problems Care Recipient: • Bathing • Toileting • Dressing • Eating • Communication • Mobility • • Catastrophic Reactions Wandering Safety Leisure/IADL • Caregiver-centered concerns
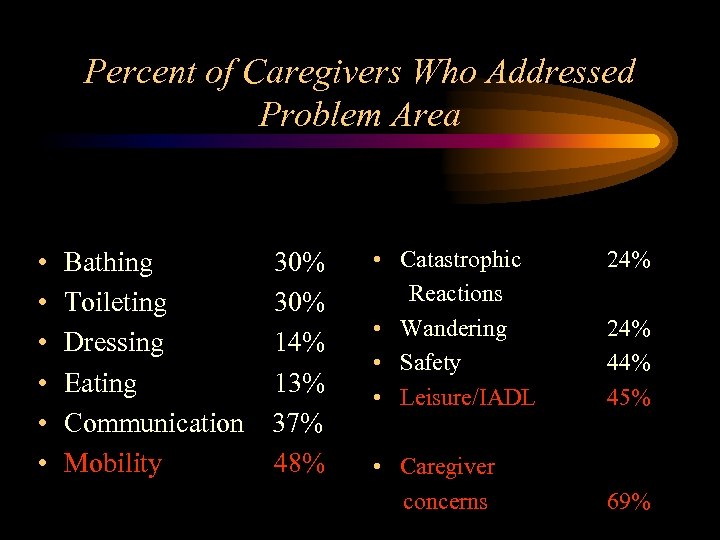 Percent of Caregivers Who Addressed Problem Area • • • Bathing Toileting Dressing Eating Communication Mobility 30% 14% 13% 37% 48% • Catastrophic Reactions • Wandering • Safety • Leisure/IADL • Caregiver concerns 24% 44% 45% 69%
Percent of Caregivers Who Addressed Problem Area • • • Bathing Toileting Dressing Eating Communication Mobility 30% 14% 13% 37% 48% • Catastrophic Reactions • Wandering • Safety • Leisure/IADL • Caregiver concerns 24% 44% 45% 69%
 Physical Modifications to the Home – Install equipment and assistive devices – Remove objects – Rearrange objects – Label objects – Color contrast objects – Place objects in sequence of use – Declutter Corcoran, M. , & Gitlin, L. N. (1991, Fall/Winter). Environmental influences on behavior of the elderly with dementia: Principles for intervention in the home. Occupational and Physical Therapy in Geriatrics, 9(3&4), 5 -21.
Physical Modifications to the Home – Install equipment and assistive devices – Remove objects – Rearrange objects – Label objects – Color contrast objects – Place objects in sequence of use – Declutter Corcoran, M. , & Gitlin, L. N. (1991, Fall/Winter). Environmental influences on behavior of the elderly with dementia: Principles for intervention in the home. Occupational and Physical Therapy in Geriatrics, 9(3&4), 5 -21.
 Physical Environment Bathroom Equipment • Tub bench • Toilet rail • Grab bars • Hand held shower • Long handled sponge • Pictures
Physical Environment Bathroom Equipment • Tub bench • Toilet rail • Grab bars • Hand held shower • Long handled sponge • Pictures
 Physical Environment Bed rail
Physical Environment Bed rail
 Physical Environment Clutter • Disorientation • Agitation • Decreased function
Physical Environment Clutter • Disorientation • Agitation • Decreased function
 Physical Environment Decluttering • Low demand • Appropriate level of stimulation • Comfortable and calming
Physical Environment Decluttering • Low demand • Appropriate level of stimulation • Comfortable and calming
 Physical Environment Caregiver Concerns • CR confused • Inappropriate dress • Decreased function
Physical Environment Caregiver Concerns • CR confused • Inappropriate dress • Decreased function
 Physical Environment Strategies: • Color contrast • Object Placement • Previous habits Outcome: • Increased independence
Physical Environment Strategies: • Color contrast • Object Placement • Previous habits Outcome: • Increased independence
 Physical Environment White commode on white wall Disorienting cue Red duct tape for color contrast
Physical Environment White commode on white wall Disorienting cue Red duct tape for color contrast
 Physical Environment Visual Cue to prevent egress
Physical Environment Visual Cue to prevent egress
 Physical Environment Case Scenario • Distractible • Poor eating • Fear of malnutrition First Set of Strategies • Red placemat • White plate • One food item • Cereal • Spoon
Physical Environment Case Scenario • Distractible • Poor eating • Fear of malnutrition First Set of Strategies • Red placemat • White plate • One food item • Cereal • Spoon
 Use of turban • Culturally appropriate • Preservation of role • Reduce distraction
Use of turban • Culturally appropriate • Preservation of role • Reduce distraction
 Modifications to Task Dimension - Give short verbal/written instructions - Provide verbal/tactile cueing Keep needed items in easy reach Simplify activities Plan a routine Instruct CR through demonstration Gitlin, et al. , 2002, Strategies Used by Families to Simplify Tasks for Individuals with Alzheimer's Disease and Related Disorders: Psychometric Analysis of the Task Management Strategy Index (TMSI). The Gerontologist
Modifications to Task Dimension - Give short verbal/written instructions - Provide verbal/tactile cueing Keep needed items in easy reach Simplify activities Plan a routine Instruct CR through demonstration Gitlin, et al. , 2002, Strategies Used by Families to Simplify Tasks for Individuals with Alzheimer's Disease and Related Disorders: Psychometric Analysis of the Task Management Strategy Index (TMSI). The Gerontologist
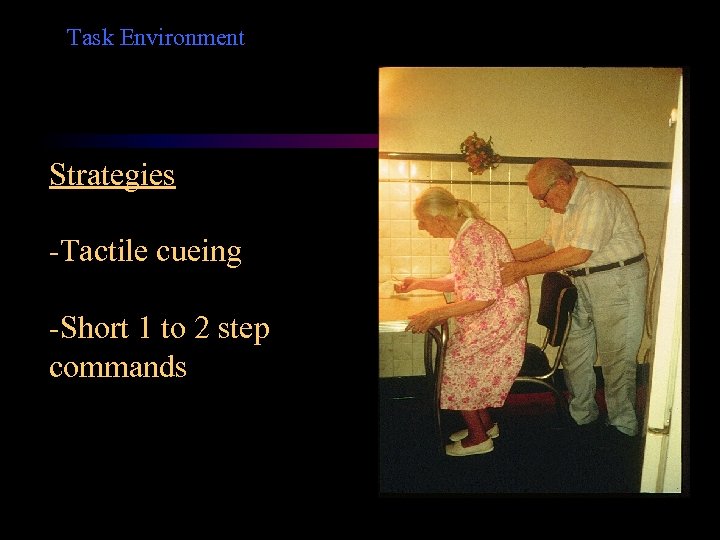 Task Environment Strategies -Tactile cueing -Short 1 to 2 step commands
Task Environment Strategies -Tactile cueing -Short 1 to 2 step commands
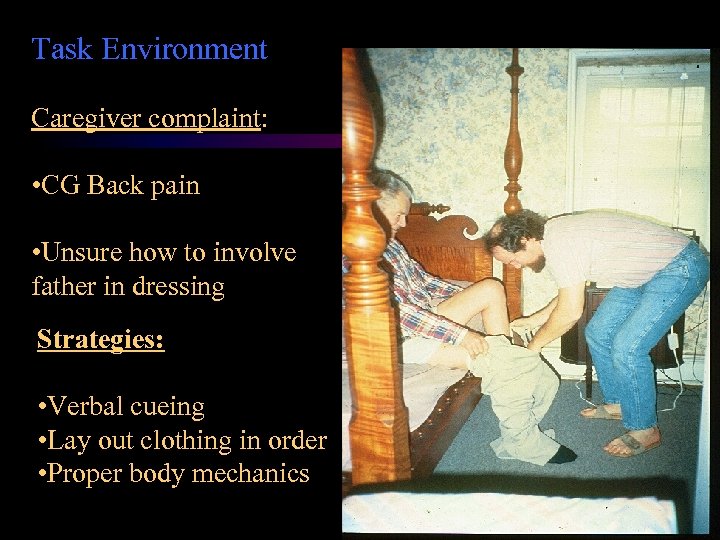 Task Environment Caregiver complaint: • CG Back pain • Unsure how to involve father in dressing Strategies: • Verbal cueing • Lay out clothing in order • Proper body mechanics
Task Environment Caregiver complaint: • CG Back pain • Unsure how to involve father in dressing Strategies: • Verbal cueing • Lay out clothing in order • Proper body mechanics
 Task Environment Case Scenario • CG no time for self • CR bored, agitated Strategies • Repetitive motion • Simplified task • Set up objects • Preserved role
Task Environment Case Scenario • CG no time for self • CR bored, agitated Strategies • Repetitive motion • Simplified task • Set up objects • Preserved role

 Task Environment • Control center • Engagement of CR • Rail for balance
Task Environment • Control center • Engagement of CR • Rail for balance
 Modification to Social Dimension - Help coordinate care among social network - Instruct in assertiveness and communication skills - Help CG develop consistency in interactions with CR - Help CG involve others in daily care provision
Modification to Social Dimension - Help coordinate care among social network - Instruct in assertiveness and communication skills - Help CG develop consistency in interactions with CR - Help CG involve others in daily care provision
 Social Dimension • Educate children • Help with interaction
Social Dimension • Educate children • Help with interaction
 Is ESP Effective? Who Benefits from ESP? - Men vs. women - Spouses vs. non-spouses - African American vs. White
Is ESP Effective? Who Benefits from ESP? - Men vs. women - Spouses vs. non-spouses - African American vs. White
 Objective Caregiver Burden Does ESP reduce amount of help needed for ADL care? “How many days in a week have other family members or friends (not being paid) provided help? ”
Objective Caregiver Burden Does ESP reduce amount of help needed for ADL care? “How many days in a week have other family members or friends (not being paid) provided help? ”
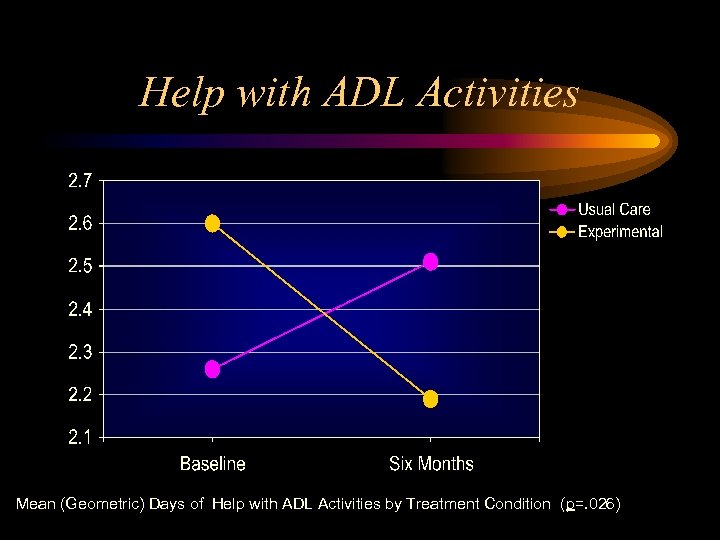 Help with ADL Activities Mean (Geometric) Days of Help with ADL Activities by Treatment Condition (p=. 026)
Help with ADL Activities Mean (Geometric) Days of Help with ADL Activities by Treatment Condition (p=. 026)
 Objective Caregiver Burden Does ESP reduce amount of time providing care? “About how many hours a day do you estimate that you are actually doing things for CR? ”
Objective Caregiver Burden Does ESP reduce amount of time providing care? “About how many hours a day do you estimate that you are actually doing things for CR? ”
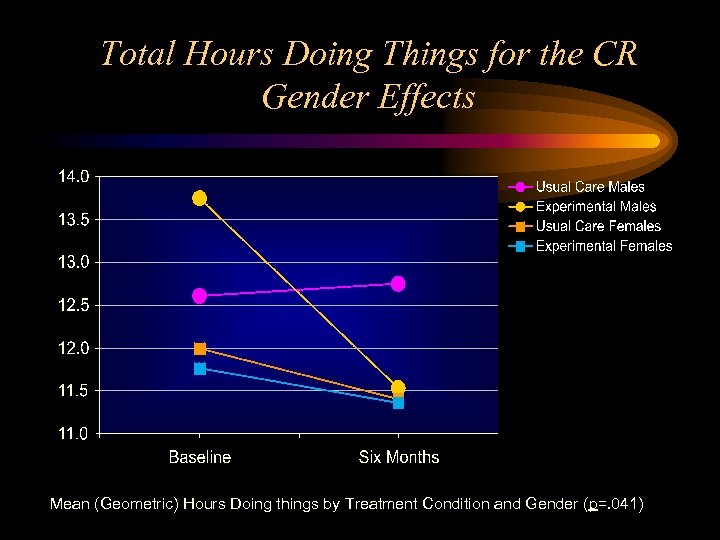 Total Hours Doing Things for the CR Gender Effects Mean (Geometric) Hours Doing things by Treatment Condition and Gender (p=. 041)
Total Hours Doing Things for the CR Gender Effects Mean (Geometric) Hours Doing things by Treatment Condition and Gender (p=. 041)
 Subjective Caregiver Burden Does ESP reduce caregiver upset with: – Memory-related behaviors? – Disruptive behaviors - 0 (Not at all) to 4 (Extremely) - Low score indicate less upset
Subjective Caregiver Burden Does ESP reduce caregiver upset with: – Memory-related behaviors? – Disruptive behaviors - 0 (Not at all) to 4 (Extremely) - Low score indicate less upset
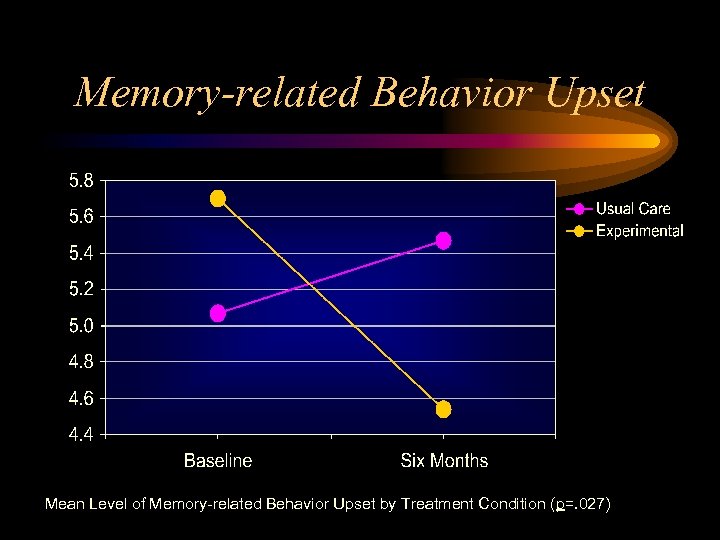 Memory-related Behavior Upset Mean Level of Memory-related Behavior Upset by Treatment Condition (p=. 027)
Memory-related Behavior Upset Mean Level of Memory-related Behavior Upset by Treatment Condition (p=. 027)
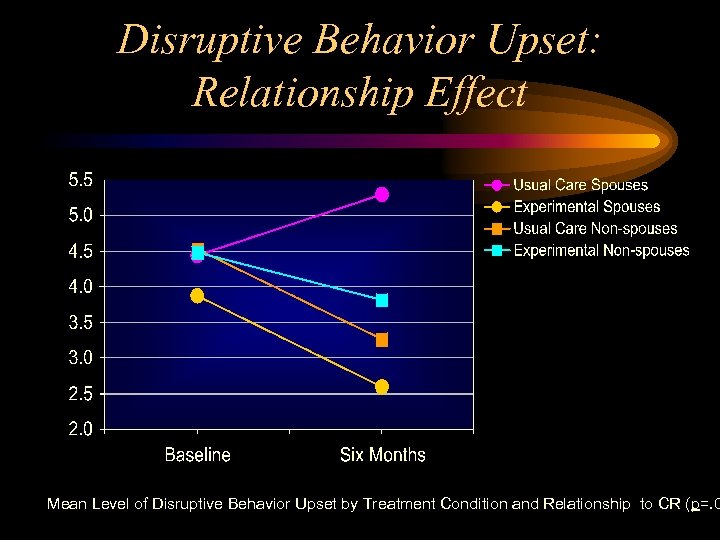 Disruptive Behavior Upset: Relationship Effect Mean Level of Disruptive Behavior Upset by Treatment Condition and Relationship to CR (p=. 0
Disruptive Behavior Upset: Relationship Effect Mean Level of Disruptive Behavior Upset by Treatment Condition and Relationship to CR (p=. 0
 Enhancement of Well-being Does ESP enhance caregiver affect? “In the past month have your feelings of being (angry) gotten much worse, somewhat worse, stayed the same, improve somewhat, improved a lot? ” Gitlin, et al (submitted) Caregiver appraisals of well being: The Perceived Change Index
Enhancement of Well-being Does ESP enhance caregiver affect? “In the past month have your feelings of being (angry) gotten much worse, somewhat worse, stayed the same, improve somewhat, improved a lot? ” Gitlin, et al (submitted) Caregiver appraisals of well being: The Perceived Change Index
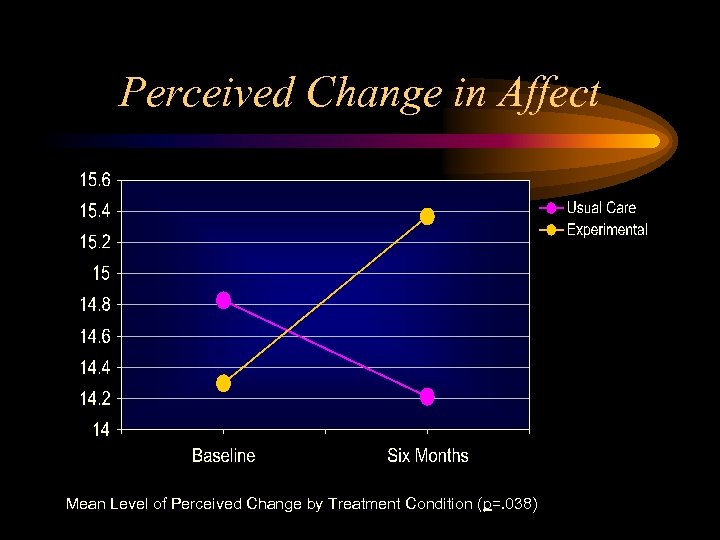 Perceived Change in Affect Mean Level of Perceived Change by Treatment Condition (p=. 038)
Perceived Change in Affect Mean Level of Perceived Change by Treatment Condition (p=. 038)
 Enhancement of Skills Does ESP enhance caregiver skills? “In the past month have your ability to manage day to day caregiving gotten much worse, somewhat worse, stayed the same, improve somewhat, improved a lot? ”
Enhancement of Skills Does ESP enhance caregiver skills? “In the past month have your ability to manage day to day caregiving gotten much worse, somewhat worse, stayed the same, improve somewhat, improved a lot? ”
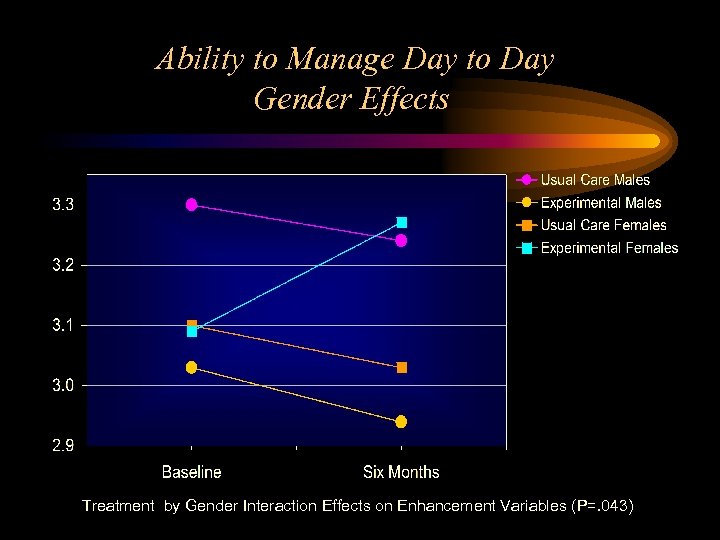 Ability to Manage Day to Day Gender Effects Treatment by Gender Interaction Effects on Enhancement Variables (P=. 043)
Ability to Manage Day to Day Gender Effects Treatment by Gender Interaction Effects on Enhancement Variables (P=. 043)
 Enhanced Mastery Does ESP enhance caregiver’s sense of personal mastery? e. g. , “How often do you feel you should be doing more for CR? ” Lawton, Kleban, Moss, Rovine, & Glicksman (1989) Measuring caregiver appraisal. Journal of Gerontology, 3, P 61 -P 71
Enhanced Mastery Does ESP enhance caregiver’s sense of personal mastery? e. g. , “How often do you feel you should be doing more for CR? ” Lawton, Kleban, Moss, Rovine, & Glicksman (1989) Measuring caregiver appraisal. Journal of Gerontology, 3, P 61 -P 71
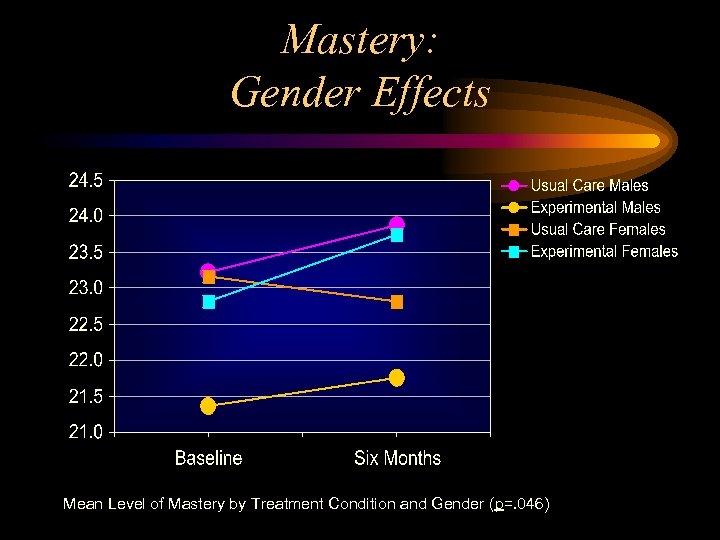 Mastery: Gender Effects Mean Level of Mastery by Treatment Condition and Gender (p=. 046)
Mastery: Gender Effects Mean Level of Mastery by Treatment Condition and Gender (p=. 046)
 Summary of Main Treatment Effects Compared to controls ESP: • Reduces upset with memory-related behaviors (subjective burden) • Decreases help received from family/friends (objective burden) • Improves affect (enhancement)
Summary of Main Treatment Effects Compared to controls ESP: • Reduces upset with memory-related behaviors (subjective burden) • Decreases help received from family/friends (objective burden) • Improves affect (enhancement)
 Summary of Treatment Interaction Effects • Decrease in time spent in vigilance for men who receive ESP • Reduced upset with disruptive behaviors for spouses who receive ESP • Improved affect, management ability and mastery for women who receive ESP
Summary of Treatment Interaction Effects • Decrease in time spent in vigilance for men who receive ESP • Reduced upset with disruptive behaviors for spouses who receive ESP • Improved affect, management ability and mastery for women who receive ESP
 No Treatment or Interaction Effects for: • CR behavioral occurrences • CR level of ADL/IADL functioning • White versus African American caregivers
No Treatment or Interaction Effects for: • CR behavioral occurrences • CR level of ADL/IADL functioning • White versus African American caregivers
 So What? • • Implications for Caregiver Research: Complex picture Subscale analyses offer nuanced understanding Subgroup analyses very important We can describe what happens but not sure why
So What? • • Implications for Caregiver Research: Complex picture Subscale analyses offer nuanced understanding Subgroup analyses very important We can describe what happens but not sure why
 So What? • • • Clinical Implications ESP has positive effects in select domains of caregiver well-being Environmental modification important role in supporting CG efforts Early intervention may enhance CR daily functioning Women and spouses benefit most Environmental approach should be integrated into clinical practice with CG-CR dyads
So What? • • • Clinical Implications ESP has positive effects in select domains of caregiver well-being Environmental modification important role in supporting CG efforts Early intervention may enhance CR daily functioning Women and spouses benefit most Environmental approach should be integrated into clinical practice with CG-CR dyads
 Health Policy Supports OT Home Environmental Interventions • Medicare coverage now authorized for treatment of Alzheimer’s Disease • Occupational therapy and physical therapy allowable • Modification to home environments allowable New York Times, Vol. CLI, 2002
Health Policy Supports OT Home Environmental Interventions • Medicare coverage now authorized for treatment of Alzheimer’s Disease • Occupational therapy and physical therapy allowable • Modification to home environments allowable New York Times, Vol. CLI, 2002
 Clinical Guidelines for Implementing ESP · Observe each room of home; · Evaluate individual capabilities, family concerns and home environmental features; · Involve family members and if possible the person with dementia in the evaluative and decision-making process; · Introduce small, incremental changes to the home environment; · Use validation, reevaluate with caregiver what works/what doesn’t/make adjustments accordingly
Clinical Guidelines for Implementing ESP · Observe each room of home; · Evaluate individual capabilities, family concerns and home environmental features; · Involve family members and if possible the person with dementia in the evaluative and decision-making process; · Introduce small, incremental changes to the home environment; · Use validation, reevaluate with caregiver what works/what doesn’t/make adjustments accordingly
 Guidelines (continued) · Use role play/demonstration to instruct in use of new strategy · Readjust environmental strategies based on family feedback as to what works best · Provide family with information about the disease and how to obtain other environmental strategies in the future Gitlin, L. N. , (2001). Effectiveness of Home Environmental Interventions for Individuals with Dementia and Family Caregivers, Home Health Care Consultant
Guidelines (continued) · Use role play/demonstration to instruct in use of new strategy · Readjust environmental strategies based on family feedback as to what works best · Provide family with information about the disease and how to obtain other environmental strategies in the future Gitlin, L. N. , (2001). Effectiveness of Home Environmental Interventions for Individuals with Dementia and Family Caregivers, Home Health Care Consultant



