Meningococcal infection.ppt
- Количество слайдов: 81
 Infections of CNS
Infections of CNS
 Clinical forms of CNS infections • • Acute bacterial meningitis Acute viral meningitis Encephalitis Local infections: • • Brain abscess Cerebellitis Subdural empyema Infectious thrombophlebitis of brain vessels
Clinical forms of CNS infections • • Acute bacterial meningitis Acute viral meningitis Encephalitis Local infections: • • Brain abscess Cerebellitis Subdural empyema Infectious thrombophlebitis of brain vessels
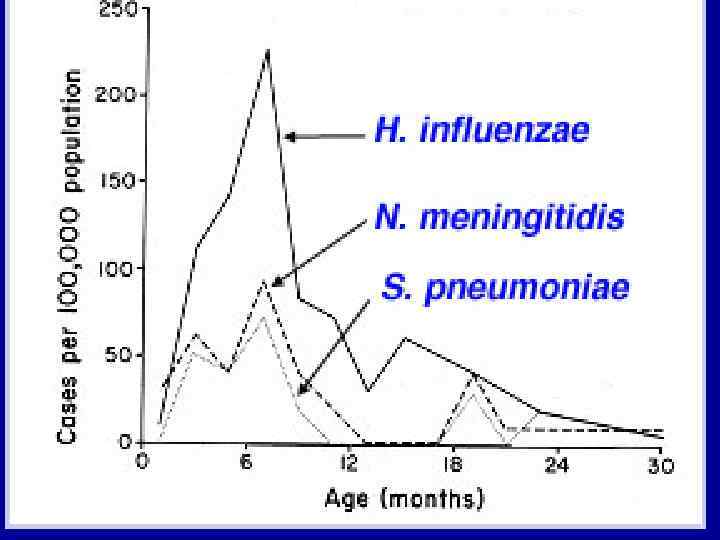
 Etiology of meningitis in different age groups Age Causative agent 0 – 3 months Listeria monocytogenes, 3 – 36 months Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Listeria monocytogenes, Group B streptococci, E. Coli and other Gram- bacteria Enterobacteriaceae, HSV-1, 2 Group B streptococci Older than 3 years Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Enteroviruses
Etiology of meningitis in different age groups Age Causative agent 0 – 3 months Listeria monocytogenes, 3 – 36 months Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Listeria monocytogenes, Group B streptococci, E. Coli and other Gram- bacteria Enterobacteriaceae, HSV-1, 2 Group B streptococci Older than 3 years Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Enteroviruses
 Etiotropic therapy of meningitis depending on age Under 1 month Listeria monocytogenes, Group B streptococci, 1 – 3 months E. Coli Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Ampicillin + cefotaxim (or gentamycin) Ampicillin + cefotaxim Enterobacteriaceae, HSV, Group B streptococci Older 3 months Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Enteroviruses Ceftriaxon (or cefotaxim)
Etiotropic therapy of meningitis depending on age Under 1 month Listeria monocytogenes, Group B streptococci, 1 – 3 months E. Coli Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Ampicillin + cefotaxim (or gentamycin) Ampicillin + cefotaxim Enterobacteriaceae, HSV, Group B streptococci Older 3 months Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae, Enteroviruses Ceftriaxon (or cefotaxim)
 Bacterial causes of meningitis and encephalitis Aerobic bacteria Neisseria meningitidis* Salmonella spp. , S. typhi, Haemophilus S. enteritidis influenzae* Klebsiella pneumoniae Streptococcus Serratia marcescens pneumoniae* Proteus spp. Streptococcus gr. "B" Pseudomonas Streptococcus viridans aeruginosa Staphylococcus aureus Citrobacter diversus Enterococcus Listeria monocytogenes Escherichia coli
Bacterial causes of meningitis and encephalitis Aerobic bacteria Neisseria meningitidis* Salmonella spp. , S. typhi, Haemophilus S. enteritidis influenzae* Klebsiella pneumoniae Streptococcus Serratia marcescens pneumoniae* Proteus spp. Streptococcus gr. "B" Pseudomonas Streptococcus viridans aeruginosa Staphylococcus aureus Citrobacter diversus Enterococcus Listeria monocytogenes Escherichia coli
 Bacterial causes of meningitis and encephalitis Anaerobic bacteria Bacteroides fragilis Bacteroides spp. Peptostreptococcus Fusobacterium meningosepticum, etc.
Bacterial causes of meningitis and encephalitis Anaerobic bacteria Bacteroides fragilis Bacteroides spp. Peptostreptococcus Fusobacterium meningosepticum, etc.
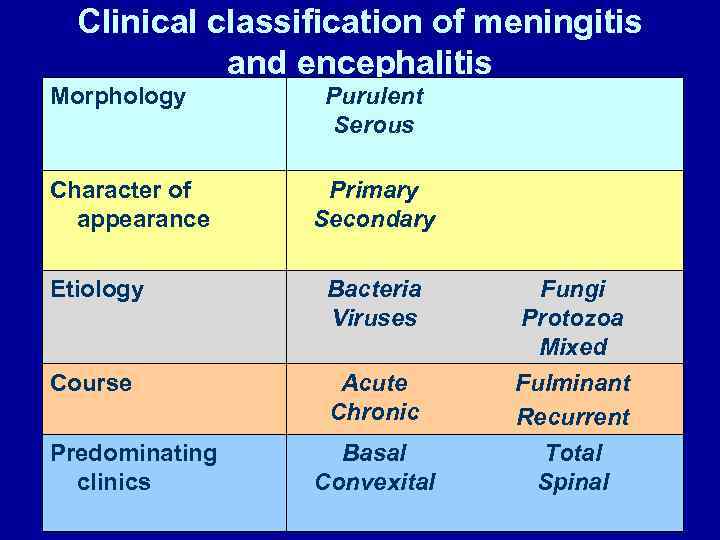 Clinical classification of meningitis and encephalitis Morphology Character of appearance Purulent Serous Primary Secondary Etiology Bacteria Viruses Course Acute Chronic Predominating clinics Basal Convexital Fungi Protozoa Mixed Fulminant Recurrent Total Spinal
Clinical classification of meningitis and encephalitis Morphology Character of appearance Purulent Serous Primary Secondary Etiology Bacteria Viruses Course Acute Chronic Predominating clinics Basal Convexital Fungi Protozoa Mixed Fulminant Recurrent Total Spinal
 Primary purulent meningitis • Meningococcus • Pneumococcus (Strep. Pneumonia) • Haemophylus Influenza type B
Primary purulent meningitis • Meningococcus • Pneumococcus (Strep. Pneumonia) • Haemophylus Influenza type B
 Primary serous meningitis • • Acute lymphocytic choriomeningitis Enteroviral Poliomyelitis Parotitis
Primary serous meningitis • • Acute lymphocytic choriomeningitis Enteroviral Poliomyelitis Parotitis
 Secondary purulent meningitis Bacterial • Staphylococcus • Streptococcus • E. coli • Salmonella • Proteus • Klebsiella • Pseudomonas • Anthrax • Listeria • Pasterilia • Micoplasma • Acinetobacter Fungi • Candida • Aspergillus Protozoa • Ameba • Toxoplasma
Secondary purulent meningitis Bacterial • Staphylococcus • Streptococcus • E. coli • Salmonella • Proteus • Klebsiella • Pseudomonas • Anthrax • Listeria • Pasterilia • Micoplasma • Acinetobacter Fungi • Candida • Aspergillus Protozoa • Ameba • Toxoplasma
 Bacterial serous meningitis • • • Tuberculosis Syphilis Leptospirosis Ornithosis Brucellosis
Bacterial serous meningitis • • • Tuberculosis Syphilis Leptospirosis Ornithosis Brucellosis
 Ways of infection penetration into CNS Hematogenous (systemic septicemia) Axonal (HSV-1, 2) Contact (mastoiditis, epitympanitis, sinusitis) Along perineural spaces of craniocerebral nerves (otits, mastoiditis)
Ways of infection penetration into CNS Hematogenous (systemic septicemia) Axonal (HSV-1, 2) Contact (mastoiditis, epitympanitis, sinusitis) Along perineural spaces of craniocerebral nerves (otits, mastoiditis)
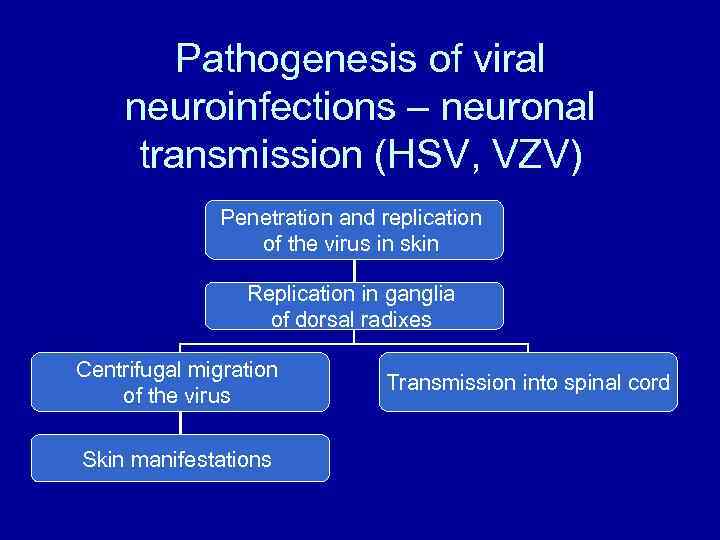 Pathogenesis of viral neuroinfections – neuronal transmission (HSV, VZV) Penetration and replication of the virus in skin Replication in ganglia of dorsal radixes Centrifugal migration of the virus Skin manifestations Transmission into spinal cord
Pathogenesis of viral neuroinfections – neuronal transmission (HSV, VZV) Penetration and replication of the virus in skin Replication in ganglia of dorsal radixes Centrifugal migration of the virus Skin manifestations Transmission into spinal cord
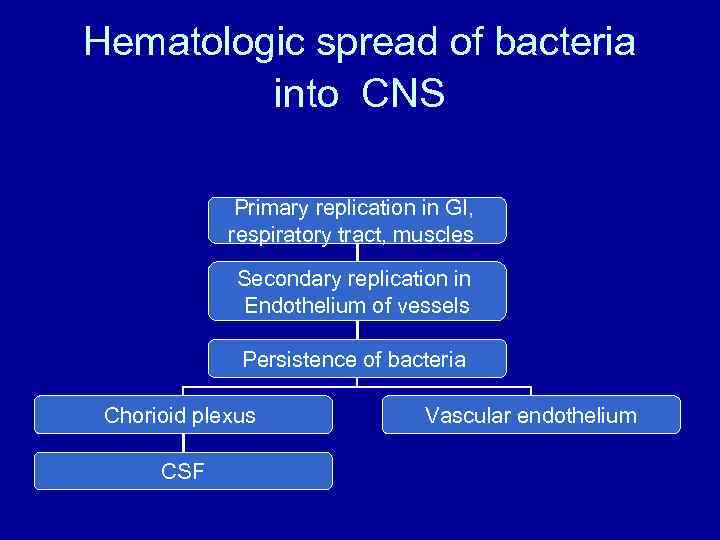 Hematologic spread of bacteria into CNS Primary replication in GI, respiratory tract, muscles Secondary replication in Endothelium of vessels Persistence of bacteria Chorioid plexus CSF Vascular endothelium
Hematologic spread of bacteria into CNS Primary replication in GI, respiratory tract, muscles Secondary replication in Endothelium of vessels Persistence of bacteria Chorioid plexus CSF Vascular endothelium
 Aseptic meningitis Viral meningitis Fungi meningitis Bacterial meningitis (caused by bacteria which can not be seen on Gram staining) Toxic meningitis (drugs, toxins) Meningitis at systemic diseases Meningitis at neoplastic diseases Parameningeal processes
Aseptic meningitis Viral meningitis Fungi meningitis Bacterial meningitis (caused by bacteria which can not be seen on Gram staining) Toxic meningitis (drugs, toxins) Meningitis at systemic diseases Meningitis at neoplastic diseases Parameningeal processes
 Meningococcal Infection
Meningococcal Infection
 History First described by Vieusseaux in 1805 as epidemic cerebrospinal fever
History First described by Vieusseaux in 1805 as epidemic cerebrospinal fever
 Epidemiology Spread All over the world Dominating serotypes А, W-135, Y В, С Source of the infection China, Nepal, India, Mongolia, Africa, Saudi Arabia USA, Canada, Europe, Australia Symptomatic patients and carriers (up to 2000 carriers per 1 symptomatic) Way of transmission Respiratory Morbidity 41, 19 per 100 000 (Ukraine 1998 y. ) Epidemic cycle 8 -30 years
Epidemiology Spread All over the world Dominating serotypes А, W-135, Y В, С Source of the infection China, Nepal, India, Mongolia, Africa, Saudi Arabia USA, Canada, Europe, Australia Symptomatic patients and carriers (up to 2000 carriers per 1 symptomatic) Way of transmission Respiratory Morbidity 41, 19 per 100 000 (Ukraine 1998 y. ) Epidemic cycle 8 -30 years
 Epidemiology • Serogroups A, B, C, W 135, X, Y, and Z – by capsular polysaccharide antigen. • Most strains causing meningococcal disease have the of groups A, B, or C.
Epidemiology • Serogroups A, B, C, W 135, X, Y, and Z – by capsular polysaccharide antigen. • Most strains causing meningococcal disease have the of groups A, B, or C.
 Epidemiology Contagiousness 10 -15% in non-vaccinated Seasonal morbidity January-March <2 years – 50% Age distribution 15 -19 years – 15% >30 years– 25% In total infectious pathology - 9, 1% Mortality (Ukraine 1998 y. ) From meningococcemia - 20, 1% From meningococcal meningitis 5, 2%
Epidemiology Contagiousness 10 -15% in non-vaccinated Seasonal morbidity January-March <2 years – 50% Age distribution 15 -19 years – 15% >30 years– 25% In total infectious pathology - 9, 1% Mortality (Ukraine 1998 y. ) From meningococcemia - 20, 1% From meningococcal meningitis 5, 2%
 Epidemiology Carriage rate 5 -10% Carriage rate during epidemics in 100% closed populations
Epidemiology Carriage rate 5 -10% Carriage rate during epidemics in 100% closed populations
 Higher risk of meningococcal infection • Freshmen college students, especially living in dormitories • Viral infections (facilitate invasion) • Smoking and smoke exposure • Crowded living conditions • Underlying chronic diseases • Low socioeconomic status
Higher risk of meningococcal infection • Freshmen college students, especially living in dormitories • Viral infections (facilitate invasion) • Smoking and smoke exposure • Crowded living conditions • Underlying chronic diseases • Low socioeconomic status
 Importance üEvery year about 250 000 children die from meningococcal infection in the world ü 70% of all cases are generalized ones ü 45% of all home-acquired sepsis cases are caused by N. meningitidis ü 30 -40% cases of primary meningitis in children are due to N. meningitidis üAbout 86% children with invasive forms of meningococcal infection require immediate emergency care ü 25% of patients are misdiagnosed primary and 70% receive inadequate emergency care
Importance üEvery year about 250 000 children die from meningococcal infection in the world ü 70% of all cases are generalized ones ü 45% of all home-acquired sepsis cases are caused by N. meningitidis ü 30 -40% cases of primary meningitis in children are due to N. meningitidis üAbout 86% children with invasive forms of meningococcal infection require immediate emergency care ü 25% of patients are misdiagnosed primary and 70% receive inadequate emergency care
 Microbiology 1. Polysaccharide capsule → resist phagocytosis 2. Lipo-oligosaccharide endotoxin → fever, shock 3. Immunoglobulin A 1 protease → cleavage of lysosomal membrane glycoprotein-1 → intracellular surviving 4. Fimbria → adhesion to epithelium N. meningitidis – Gram negative incapsulated dyplococcus
Microbiology 1. Polysaccharide capsule → resist phagocytosis 2. Lipo-oligosaccharide endotoxin → fever, shock 3. Immunoglobulin A 1 protease → cleavage of lysosomal membrane glycoprotein-1 → intracellular surviving 4. Fimbria → adhesion to epithelium N. meningitidis – Gram negative incapsulated dyplococcus
 N. meningitidis • • Gram-negative Intra- and extracellular bacteria not stable to outer influence Serogroups А and В typically give generalized infections • Serogroup A is responsible for epidemics • Can autolyse – endotoxin is released
N. meningitidis • • Gram-negative Intra- and extracellular bacteria not stable to outer influence Serogroups А and В typically give generalized infections • Serogroup A is responsible for epidemics • Can autolyse – endotoxin is released
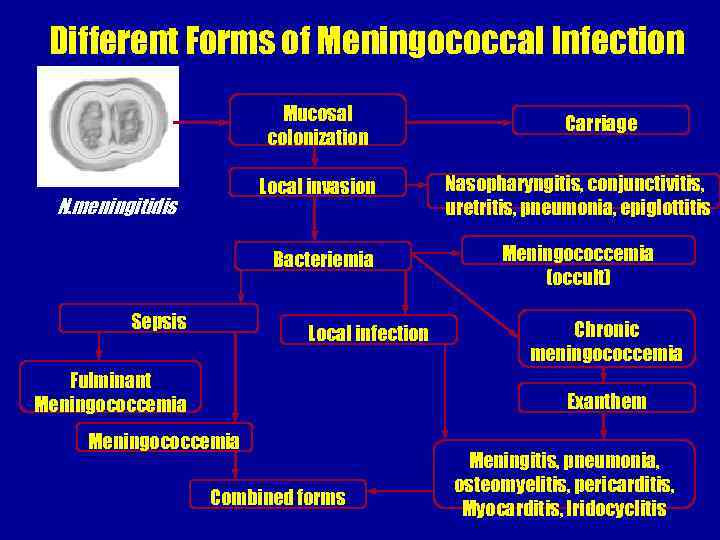 Different Forms of Meningococcal Infection Mucosal colonization Carriage Local invasion Bacteriemia N. meningitidis Sepsis Nasopharyngitis, conjunctivitis, uretritis, pneumonia, epiglottitis Meningococcemia (occult) Local infection Fulminant Meningococcemia Chronic meningococcemia Exanthem Meningococcemia Combined forms Meningitis, pneumonia, osteomyelitis, pericarditis, Myocarditis, Iridocyclitis
Different Forms of Meningococcal Infection Mucosal colonization Carriage Local invasion Bacteriemia N. meningitidis Sepsis Nasopharyngitis, conjunctivitis, uretritis, pneumonia, epiglottitis Meningococcemia (occult) Local infection Fulminant Meningococcemia Chronic meningococcemia Exanthem Meningococcemia Combined forms Meningitis, pneumonia, osteomyelitis, pericarditis, Myocarditis, Iridocyclitis
 Development of meningococcemia Absence of antimeningococcal antibody ↓ Bacteriemia ↓ Interaction with phagocytes + adhesion to endothelial cells ↓ Complement system activation + attachment of white blood cells to endothelium ↓ Production of multiple proinflammatory cytokines (TNFa, IL-1ß, IL-6, and IL-8) + activation of both the extrinsic and intrinsic pathways of coagulation ↓
Development of meningococcemia Absence of antimeningococcal antibody ↓ Bacteriemia ↓ Interaction with phagocytes + adhesion to endothelial cells ↓ Complement system activation + attachment of white blood cells to endothelium ↓ Production of multiple proinflammatory cytokines (TNFa, IL-1ß, IL-6, and IL-8) + activation of both the extrinsic and intrinsic pathways of coagulation ↓
 Development of meningococcemia Capillary leak and disseminated intravascular coagulopathy (DIC) ↓ Leukocyte-rich fibrin clots in small vessels ↓ Focal hemorrhage and necrosis in any organ system ↓ Heart, CNS, skin, mucous and serous membranes, and adrenals are affected in most fatal cases ↓ Multiple organ system failure, septic shock, and sometimes death
Development of meningococcemia Capillary leak and disseminated intravascular coagulopathy (DIC) ↓ Leukocyte-rich fibrin clots in small vessels ↓ Focal hemorrhage and necrosis in any organ system ↓ Heart, CNS, skin, mucous and serous membranes, and adrenals are affected in most fatal cases ↓ Multiple organ system failure, septic shock, and sometimes death
 Development of meningococcemia Fatal cases typically have higher concentrations of TNFa and ILs levels decrease rapidly once antibiotics are given ________________ Fatality risk is higher in children capable of strong immune response
Development of meningococcemia Fatal cases typically have higher concentrations of TNFa and ILs levels decrease rapidly once antibiotics are given ________________ Fatality risk is higher in children capable of strong immune response
 Development of meningococcemia Meningococcal survival is enhanced by: • Polysaccharide capsule, which helps resist phagocytic killing • Iron scavenging system that can use host transferrin and lactoferrin
Development of meningococcemia Meningococcal survival is enhanced by: • Polysaccharide capsule, which helps resist phagocytic killing • Iron scavenging system that can use host transferrin and lactoferrin
 Predisposition • Complement component deficiencies → increased susceptibility to and recurrent cases of meningococcal infections • Immunoglobulin G 2 subclass deficiency → recurrent meningococcemia • Hereditary properdin deficiency → predisposition to meningococcal disease
Predisposition • Complement component deficiencies → increased susceptibility to and recurrent cases of meningococcal infections • Immunoglobulin G 2 subclass deficiency → recurrent meningococcemia • Hereditary properdin deficiency → predisposition to meningococcal disease
 Natural immunity against N. meningitidis • After repeated colonization with different serogroups or serotypes • From gastrointestinal colonization with enteric bacteria that express cross-reactive antigens • Infants also have high carriage rates of the unencapsulated, nonpathogenic neisserial strain, N. lactamica → immunity against meningococci • Protective effects of maternal Ig. G during only the first 3 months of life
Natural immunity against N. meningitidis • After repeated colonization with different serogroups or serotypes • From gastrointestinal colonization with enteric bacteria that express cross-reactive antigens • Infants also have high carriage rates of the unencapsulated, nonpathogenic neisserial strain, N. lactamica → immunity against meningococci • Protective effects of maternal Ig. G during only the first 3 months of life
 Classification of meningococcal infection Form Course Severity Localized Generalized Rare forms Acute Subacute Fulminant Recurrent Mild Moderate Severe
Classification of meningococcal infection Form Course Severity Localized Generalized Rare forms Acute Subacute Fulminant Recurrent Mild Moderate Severe
 Forms of meningococcal infection Localized forms: Rare forms: Carriage Nasopharyngitis Endocarditis Arthritis Iridocyclitis Pneumonia Urethritis Otitis Conjunctivitis Generalized forms: Meningococcemia Meningitis Meningoencephalitis Meningococcemia with meningitis
Forms of meningococcal infection Localized forms: Rare forms: Carriage Nasopharyngitis Endocarditis Arthritis Iridocyclitis Pneumonia Urethritis Otitis Conjunctivitis Generalized forms: Meningococcemia Meningitis Meningoencephalitis Meningococcemia with meningitis
 Meningococcemia (meningococcal sepsis) üAccounts for 15 -20% of all invasive cases of meningococcal infection. üMortality is 20 - 40%. üSuperacute meningococcal sepsis develops in 10 -20% of cases. üMortality from Superacute meningococcal sepsis is over 90%.
Meningococcemia (meningococcal sepsis) üAccounts for 15 -20% of all invasive cases of meningococcal infection. üMortality is 20 - 40%. üSuperacute meningococcal sepsis develops in 10 -20% of cases. üMortality from Superacute meningococcal sepsis is over 90%.
 Clinical Presentations Main : üHemorrhagic rash üFever, chills Additional: üPale, mottled or cyanotic skin (capillary refill >2 sec. ) üIrritation and crying or lethargy (till coma) üSeizures üVomiting, nausea, diarrhea üFeeding refusal üMyalgias and Arthralgias üDecreased urination
Clinical Presentations Main : üHemorrhagic rash üFever, chills Additional: üPale, mottled or cyanotic skin (capillary refill >2 sec. ) üIrritation and crying or lethargy (till coma) üSeizures üVomiting, nausea, diarrhea üFeeding refusal üMyalgias and Arthralgias üDecreased urination
 Meningococcal rash Hemorrhagic rash with uneven borders and central necrosis, first appear on lower extremities and buttocks
Meningococcal rash Hemorrhagic rash with uneven borders and central necrosis, first appear on lower extremities and buttocks
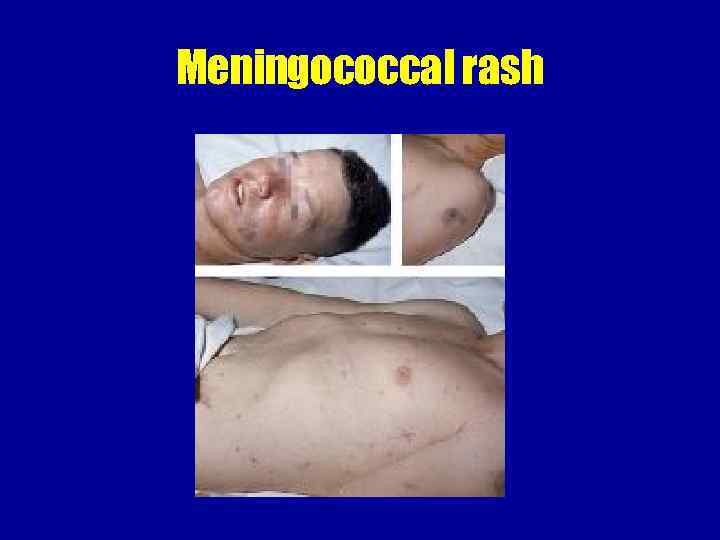 Meningococcal rash
Meningococcal rash
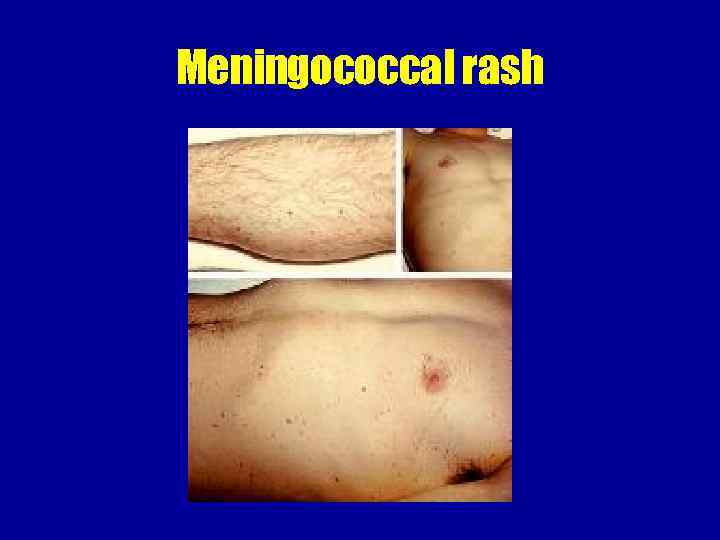 Meningococcal rash
Meningococcal rash
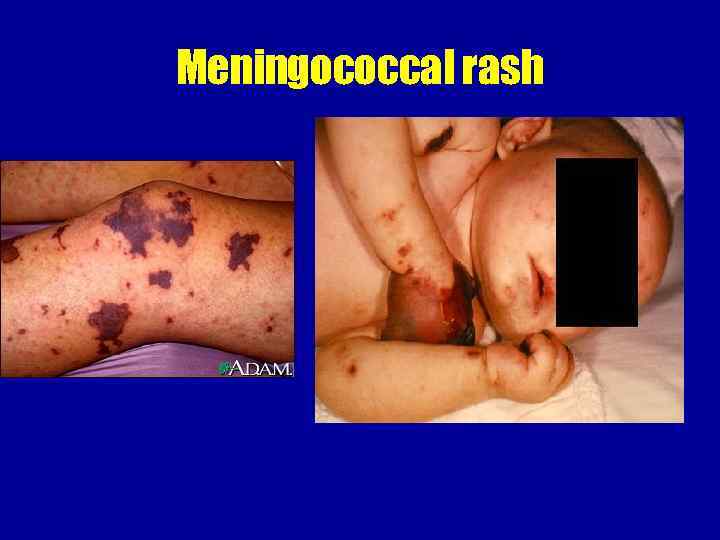 Meningococcal rash
Meningococcal rash
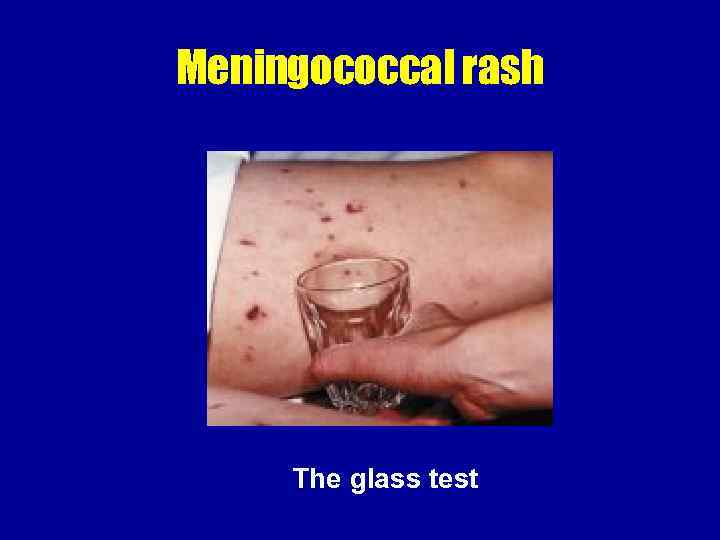 Meningococcal rash The glass test
Meningococcal rash The glass test
 Waterhouse-Friderichsen syndrome • In fulminant cases, the disease progresses rapidly over hours to septic shock characterized by hypotension, DIC, acidosis, adrenal hemorrhage, renal failure, myocardial failure, and coma.
Waterhouse-Friderichsen syndrome • In fulminant cases, the disease progresses rapidly over hours to septic shock characterized by hypotension, DIC, acidosis, adrenal hemorrhage, renal failure, myocardial failure, and coma.
 Criteria of severity Damroshe Scale (1966) 1. 2. 3. 4. 5. Appearance of hemorrhagic rash within 12 hours from the beginning of the diseases Presence of shock (systolic pressure <70 mm. Hg. ) Absence of meningitis (CSF cytosis <20 cells/mm 3) WBC count in peripheral blood <10 х109/l ESR normal or low (<10 mm/h) Every index has 1 point. 3 points: case fatality rate is 85, 7%, ≥ 4 points: 100%
Criteria of severity Damroshe Scale (1966) 1. 2. 3. 4. 5. Appearance of hemorrhagic rash within 12 hours from the beginning of the diseases Presence of shock (systolic pressure <70 mm. Hg. ) Absence of meningitis (CSF cytosis <20 cells/mm 3) WBC count in peripheral blood <10 х109/l ESR normal or low (<10 mm/h) Every index has 1 point. 3 points: case fatality rate is 85, 7%, ≥ 4 points: 100%
 Criteria of severity Niklasson Scale (1971) 1. 2. 3. 4. 5. 6. Absence of meningitis (CSF cytosis <100 cells/mm 3) Hypotension (systolic pressure <70 mm. Hg. ) Appearance of hemorrhagic rash within 12 hours from the beginning of the diseases WBC count in peripheral blood <15 х109/l Fever > 40°С Thrombocytopenia (<100 000 /mm 3) Every index has 1 point. ≥ 4 points: case fatality rate is 100%
Criteria of severity Niklasson Scale (1971) 1. 2. 3. 4. 5. 6. Absence of meningitis (CSF cytosis <100 cells/mm 3) Hypotension (systolic pressure <70 mm. Hg. ) Appearance of hemorrhagic rash within 12 hours from the beginning of the diseases WBC count in peripheral blood <15 х109/l Fever > 40°С Thrombocytopenia (<100 000 /mm 3) Every index has 1 point. ≥ 4 points: case fatality rate is 100%
 Criteria of severity Glasgow Meningococcal Septicemia Scale (1991) Systolic pressure < 75 mm. Hg. (under 4 years), < 85 mm. Hg. (older 4 years) 3 points Gradient of skin-rectal temperature >3°С 3 points Glasgow Coma Scale < 8 points 3 points . “Every hour” previous worsening of condition 2 points Absence of Meningeal signs 2 points Spread hemorrhagic rash with large elements 1 point Base deficit (p. H>8, 0) 1 point 8 points– fatality rate 73%, 10 points – 87, 5%, 12 and more – 100%
Criteria of severity Glasgow Meningococcal Septicemia Scale (1991) Systolic pressure < 75 mm. Hg. (under 4 years), < 85 mm. Hg. (older 4 years) 3 points Gradient of skin-rectal temperature >3°С 3 points Glasgow Coma Scale < 8 points 3 points . “Every hour” previous worsening of condition 2 points Absence of Meningeal signs 2 points Spread hemorrhagic rash with large elements 1 point Base deficit (p. H>8, 0) 1 point 8 points– fatality rate 73%, 10 points – 87, 5%, 12 and more – 100%
 Differential diagnosis Scarlet fever Measles Rubella Exanthema subitum Dengue Fever Gonococcal infection Influenza Mycoplasma infections Rocky Mountain Spotted Fever Streptococcal Group A & B infections Thrombocytopenic Purpura Ebola Virus Enterovirus Infective Endocarditis Malaria Drug reactions Poisonings
Differential diagnosis Scarlet fever Measles Rubella Exanthema subitum Dengue Fever Gonococcal infection Influenza Mycoplasma infections Rocky Mountain Spotted Fever Streptococcal Group A & B infections Thrombocytopenic Purpura Ebola Virus Enterovirus Infective Endocarditis Malaria Drug reactions Poisonings
 Diseases with hemorrhagic rash • • Neisseria meningitidis Haemophilus influenzae Streptococcus pneumoniae Neisseria gonorrhoeae
Diseases with hemorrhagic rash • • Neisseria meningitidis Haemophilus influenzae Streptococcus pneumoniae Neisseria gonorrhoeae
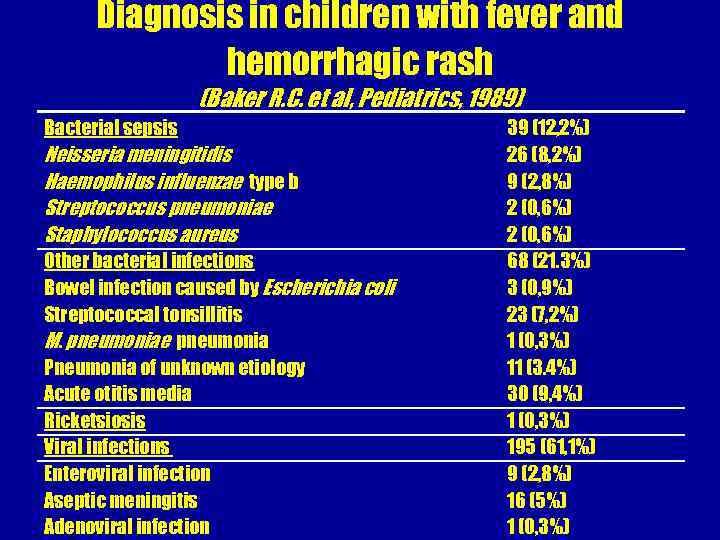 Diagnosis in children with fever and hemorrhagic rash (Baker R. C. et al, Pediatrics, 1989) Bacterial sepsis Neisseria meningitidis Haemophilus influenzae type b Streptococcus pneumoniae Staphylococcus aureus Other bacterial infections Bowel infection caused by Escherichia coli Streptococcal tonsillitis M. pneumoniae pneumonia Pneumonia of unknown etiology Acute otitis media Ricketsiosis Viral infections Enteroviral infection Aseptic meningitis Adenoviral infection 39 (12, 2%) 26 (8, 2%) 9 (2, 8%) 2 (0, 6%) 68 (21. 3%) 3 (0, 9%) 23 (7, 2%) 1 (0, 3%) 11 (3. 4%) 30 (9, 4%) 1 (0, 3%) 195 (61, 1%) 9 (2, 8%) 16 (5%) 1 (0, 3%)
Diagnosis in children with fever and hemorrhagic rash (Baker R. C. et al, Pediatrics, 1989) Bacterial sepsis Neisseria meningitidis Haemophilus influenzae type b Streptococcus pneumoniae Staphylococcus aureus Other bacterial infections Bowel infection caused by Escherichia coli Streptococcal tonsillitis M. pneumoniae pneumonia Pneumonia of unknown etiology Acute otitis media Ricketsiosis Viral infections Enteroviral infection Aseptic meningitis Adenoviral infection 39 (12, 2%) 26 (8, 2%) 9 (2, 8%) 2 (0, 6%) 68 (21. 3%) 3 (0, 9%) 23 (7, 2%) 1 (0, 3%) 11 (3. 4%) 30 (9, 4%) 1 (0, 3%) 195 (61, 1%) 9 (2, 8%) 16 (5%) 1 (0, 3%)
 Diagnosis in children with fever and hemorrhagic rash –cont. 12 (3, 8%) RS-infection Human methapneumovirus Rotavirus 11 (3, 4%) 1 (0, 3%) HHV-6 (exanthema subitum) Probable viral infection Other causes Hemorrhagic vasculitis Kawasaki disease Thrombocytopenic purpura Vaccination reaction Acute leukemia Febrile seizures Partially treated meningitis Partially treated septicemia Exudative tonsillitis Reaction to ampicillin Unknown 1 (0, 3%) 144 (45, 1%) 25 (7, 9%) 2 (0, 6%) 1 (0, 3%) 3 (0. 9%) 2 (0, 6%) 5 (1, 6%) 2 (0, 6%) 1 (0, 3%) 4 (1, 3%)
Diagnosis in children with fever and hemorrhagic rash –cont. 12 (3, 8%) RS-infection Human methapneumovirus Rotavirus 11 (3, 4%) 1 (0, 3%) HHV-6 (exanthema subitum) Probable viral infection Other causes Hemorrhagic vasculitis Kawasaki disease Thrombocytopenic purpura Vaccination reaction Acute leukemia Febrile seizures Partially treated meningitis Partially treated septicemia Exudative tonsillitis Reaction to ampicillin Unknown 1 (0, 3%) 144 (45, 1%) 25 (7, 9%) 2 (0, 6%) 1 (0, 3%) 3 (0. 9%) 2 (0, 6%) 5 (1, 6%) 2 (0, 6%) 1 (0, 3%) 4 (1, 3%)
 Occult meningococcemia • Fever with or without associated symptoms that suggest minor viral infections • Resolution may occur without antibiotics, but some cases will develop meningitis
Occult meningococcemia • Fever with or without associated symptoms that suggest minor viral infections • Resolution may occur without antibiotics, but some cases will develop meningitis
 Chronic meningococcemia Rare form : Intermittent Bacteriemia illness that lasts from at least one week to as long as several months – Intermittent fever, with afebrile periods ranging from 2 -10 days, during which the patient seems entirely healthy → febrile periods occur more frequently, fever may become continuous; – Headache, arthritis can develop; – Eventually, skin hemorrhages or signs of meningitis appears during a febrile episode; – Blood cultures may initially be sterile.
Chronic meningococcemia Rare form : Intermittent Bacteriemia illness that lasts from at least one week to as long as several months – Intermittent fever, with afebrile periods ranging from 2 -10 days, during which the patient seems entirely healthy → febrile periods occur more frequently, fever may become continuous; – Headache, arthritis can develop; – Eventually, skin hemorrhages or signs of meningitis appears during a febrile episode; – Blood cultures may initially be sterile.
 Meningitis Inflammation of soft meningeals of viral, bacterial or fungi etiology or as a complication or presentation of systemic septicemia
Meningitis Inflammation of soft meningeals of viral, bacterial or fungi etiology or as a complication or presentation of systemic septicemia
 Current epidemiology of meningitis • • • Streptococcus pneumoniae – 50 % Neisseria meningitidis - 25 % Group B streptococci – 15 % Listeria monocytogenes - 10 % Haemophilus influenzae < 10 % (vaccination !)
Current epidemiology of meningitis • • • Streptococcus pneumoniae – 50 % Neisseria meningitidis - 25 % Group B streptococci – 15 % Listeria monocytogenes - 10 % Haemophilus influenzae < 10 % (vaccination !)
 Meningococcal meningitis • Meningococcal meningitis - 50 -60% of all invasive cases of meningococcal infection • Case fatality rate is 3 - 10% • About 30% of cases are combined with meningococcemia
Meningococcal meningitis • Meningococcal meningitis - 50 -60% of all invasive cases of meningococcal infection • Case fatality rate is 3 - 10% • About 30% of cases are combined with meningococcemia
 Clinical Signs - main ü Fever ü Headache ü Positive Meningeal signs : - Neck stiffness - Brudzinski sign - Kernig sign - Lessage’s sign - Fontanel bulging - Position of the “kicking dog” - Lobzin’s sign - Guillain’s sign - Flatau’s sign
Clinical Signs - main ü Fever ü Headache ü Positive Meningeal signs : - Neck stiffness - Brudzinski sign - Kernig sign - Lessage’s sign - Fontanel bulging - Position of the “kicking dog” - Lobzin’s sign - Guillain’s sign - Flatau’s sign
 Clinical Signs – additional ü Irritability ü Somnolence ü Vomiting (repeated regurgitations) ü Groaning crying ü High-pitch cry at irritation ü Light fear ü Decreased feeding ü Decreased consciousness ü Delirium ü Convulsions ü Craniocerebral nerves involvement ü Pain in joints and muscles
Clinical Signs – additional ü Irritability ü Somnolence ü Vomiting (repeated regurgitations) ü Groaning crying ü High-pitch cry at irritation ü Light fear ü Decreased feeding ü Decreased consciousness ü Delirium ü Convulsions ü Craniocerebral nerves involvement ü Pain in joints and muscles
 Meningeal signs – cont. Neck stiffness Inability to touch sternum with chin Kernig Flexed in hip and knee joints leg can not be straightened in knee joint Brudzinski (upper) At head bending the legs are flexed in hip and knee joints Brudzinski (lower) At Straightening of the flexed in hip and knee joints leg, the second leg is flexed Lessage’s At lifting up, the infant flexes legs and remains in this position
Meningeal signs – cont. Neck stiffness Inability to touch sternum with chin Kernig Flexed in hip and knee joints leg can not be straightened in knee joint Brudzinski (upper) At head bending the legs are flexed in hip and knee joints Brudzinski (lower) At Straightening of the flexed in hip and knee joints leg, the second leg is flexed Lessage’s At lifting up, the infant flexes legs and remains in this position
 Meningeal signs Position of the The patient is lying on the back with thrown “kicking dog” back head and legs flexed to the bowel Guillain’s Compression of leg’s quadriceps causes other leg’s flexion hip and knee joints Lobzin’s Pain increase at pressure on the eyeballs Flatau’s Pupils’ widening at head flexion Amoss’ Leaning on hands behind when sitting, inability to touch knee with lips Herman’s Passive head flexion to the sternum causes extension of toes Levinson’s Mouth opening at head flexion to the sternum
Meningeal signs Position of the The patient is lying on the back with thrown “kicking dog” back head and legs flexed to the bowel Guillain’s Compression of leg’s quadriceps causes other leg’s flexion hip and knee joints Lobzin’s Pain increase at pressure on the eyeballs Flatau’s Pupils’ widening at head flexion Amoss’ Leaning on hands behind when sitting, inability to touch knee with lips Herman’s Passive head flexion to the sternum causes extension of toes Levinson’s Mouth opening at head flexion to the sternum
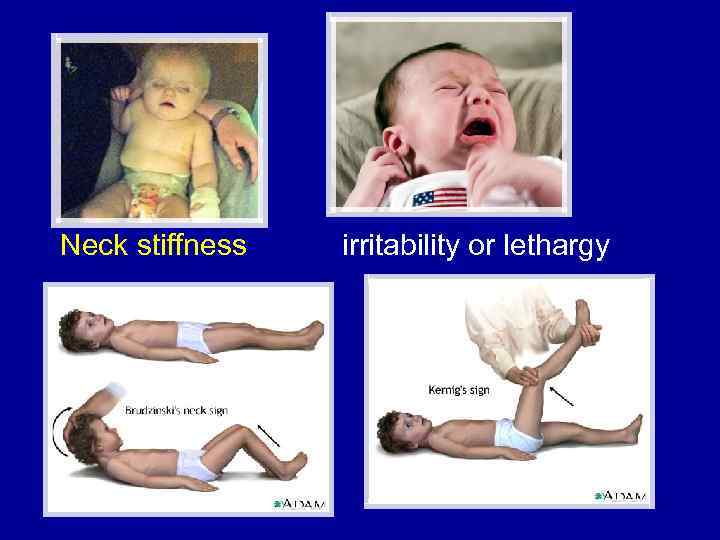 Neck stiffness irritability or lethargy
Neck stiffness irritability or lethargy
 Particularities of meningitis clinics in infants • • Irritability / somnolence Mild fever “Brain cry” – headache equivalent Large fontanelle bulging Lessage’s sign Head retroflexion Tonic and clonic seizures Transient diarrhea
Particularities of meningitis clinics in infants • • Irritability / somnolence Mild fever “Brain cry” – headache equivalent Large fontanelle bulging Lessage’s sign Head retroflexion Tonic and clonic seizures Transient diarrhea
 Meningitis diagnosis • The only way to exclude/diagnose neuroinfection is to investigate CSF • Pleocytosis proves a CNS infection
Meningitis diagnosis • The only way to exclude/diagnose neuroinfection is to investigate CSF • Pleocytosis proves a CNS infection
 Differential diagnosis ü Encephalitis and meningitis caused by other viruses or bacteria ü Acute bowel infections ü Pneumonia ü Septic shock ü Rhinosinusitis ü Acute poisoning ü Encephalopathies
Differential diagnosis ü Encephalitis and meningitis caused by other viruses or bacteria ü Acute bowel infections ü Pneumonia ü Septic shock ü Rhinosinusitis ü Acute poisoning ü Encephalopathies
 Differential diagnosis – cont. ü Acute myositis ü Infectious delirium ü Retropharyngeal abscesses ü Shaken baby syndrome ü Subdural haematoma ü CSF hypertension syndrome ü Brain blood circulation damage ü Hypertensive crisis
Differential diagnosis – cont. ü Acute myositis ü Infectious delirium ü Retropharyngeal abscesses ü Shaken baby syndrome ü Subdural haematoma ü CSF hypertension syndrome ü Brain blood circulation damage ü Hypertensive crisis
 Required tests at meningitis • CSF • CBC • Signs of brain edema: – Eye fundus examination (edema) – CT, MRI • Blood electrolytes • Glucose of blood and SCF • CRP
Required tests at meningitis • CSF • CBC • Signs of brain edema: – Eye fundus examination (edema) – CT, MRI • Blood electrolytes • Glucose of blood and SCF • CRP
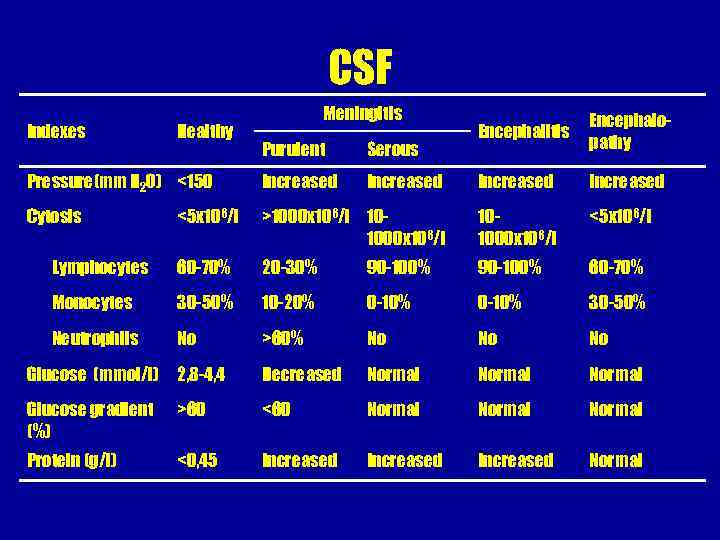 CSF Indexes Healthy Meningitis Encephalopathy Purulent Serous Pressure(mm Н 2 О) <150 Increased Cytosis <5 x 106/l >1000 x 106/l 101000 x 106/l <5 x 106/l Lymphocytes 60 -70% 20 -30% 90 -100% 60 -70% Monocytes 30 -50% 10 -20% 0 -10% 30 -50% Neutrophils No >60% No No No Glucose (mmol/l) 2, 8 -4, 4 Decreased Normal Glucose gradient (%) >60 <60 Normal Protein (g/l) <0, 45 Increased Normal
CSF Indexes Healthy Meningitis Encephalopathy Purulent Serous Pressure(mm Н 2 О) <150 Increased Cytosis <5 x 106/l >1000 x 106/l 101000 x 106/l <5 x 106/l Lymphocytes 60 -70% 20 -30% 90 -100% 60 -70% Monocytes 30 -50% 10 -20% 0 -10% 30 -50% Neutrophils No >60% No No No Glucose (mmol/l) 2, 8 -4, 4 Decreased Normal Glucose gradient (%) >60 <60 Normal Protein (g/l) <0, 45 Increased Normal
 Etiologic diagnosis Test Gram’s stain Culture Material Comments CSF, aspirate from skin rash or üRapid test sinovial fluid or üCSF Sensitivity – 65% other sterile üSkin rash sensitivity - 30 -70% material ü“Golden” standard for CSF, blood, aspirate diagnosis from skin rash or üResult in 1 -2 days sinovial fluid or any üCSF Sensitivity – 95% (without other sterile antibiotics) material üBlood culture Sensitivity – 50% (without antibiotics) Nasopharyngeal üConfirms carriage secretion
Etiologic diagnosis Test Gram’s stain Culture Material Comments CSF, aspirate from skin rash or üRapid test sinovial fluid or üCSF Sensitivity – 65% other sterile üSkin rash sensitivity - 30 -70% material ü“Golden” standard for CSF, blood, aspirate diagnosis from skin rash or üResult in 1 -2 days sinovial fluid or any üCSF Sensitivity – 95% (without other sterile antibiotics) material üBlood culture Sensitivity – 50% (without antibiotics) Nasopharyngeal üConfirms carriage secretion
 Etiologic diagnosis – cont. Test PCR Material Comments CSF, blood üCSF: Sensitivity Specificity– 100% üBlood: Sensitivity Specificity -97% - 89%, – 81%, Serology Blood üSpecific Ig. M or Ab titer increase 4 times and more (low informativity and sensitivity) Antigen test üLow sensitivity, additional test to Gram’s staining CSF
Etiologic diagnosis – cont. Test PCR Material Comments CSF, blood üCSF: Sensitivity Specificity– 100% üBlood: Sensitivity Specificity -97% - 89%, – 81%, Serology Blood üSpecific Ig. M or Ab titer increase 4 times and more (low informativity and sensitivity) Antigen test üLow sensitivity, additional test to Gram’s staining CSF
 Complications • • Disseminated intravascular coagulation Vasomotor collapse and shock Seizures or deafness in the acute stages of meningitis Ependimatitis Postmeningitic epilepsy (rare) Coma Thrombocytopenia Septic arthritis
Complications • • Disseminated intravascular coagulation Vasomotor collapse and shock Seizures or deafness in the acute stages of meningitis Ependimatitis Postmeningitic epilepsy (rare) Coma Thrombocytopenia Septic arthritis
 Complications – cont. • • • Herpes labialis (5 -20% of patients) Immune complex arthritis of multiple joints Pericarditis Bacterial endocarditis Myocarditis Gangrene Urethritis and endometritis Osteomyelitis Purulent conjunctivitis and sinusitis
Complications – cont. • • • Herpes labialis (5 -20% of patients) Immune complex arthritis of multiple joints Pericarditis Bacterial endocarditis Myocarditis Gangrene Urethritis and endometritis Osteomyelitis Purulent conjunctivitis and sinusitis
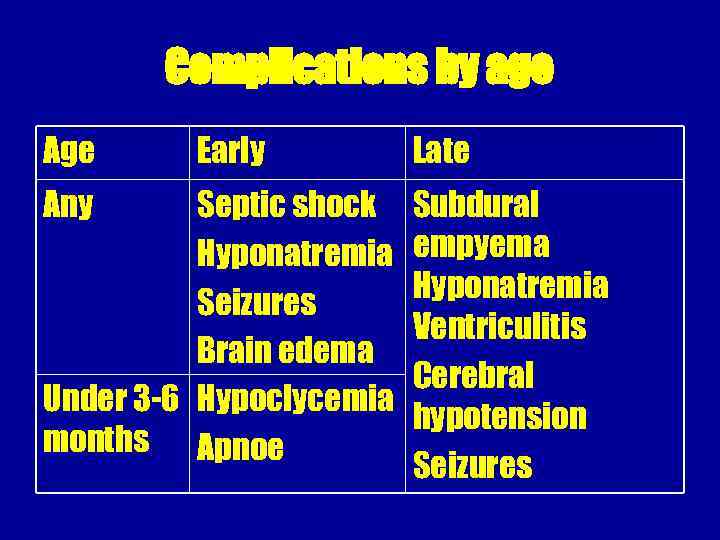 Complications by age Any Early Septic shock Hyponatremia Seizures Brain edema Under 3 -6 Hypoclycemia months Apnoe Late Subdural empyema Hyponatremia Ventriculitis Cerebral hypotension Seizures
Complications by age Any Early Septic shock Hyponatremia Seizures Brain edema Under 3 -6 Hypoclycemia months Apnoe Late Subdural empyema Hyponatremia Ventriculitis Cerebral hypotension Seizures
 Uncommon manifestations of meningococcal disease • • • Endocarditis Purulent pericarditis Pneumonia (in 15% + pleural effusion or empyema) Endophthalmitis Mesenteric lymphadenitis Osteomyelitis Sinusitis Otitis media Periorbital cellulitis Primary purulent conjunctivitis Urethritis, cervicitis, vulvovaginitis, proctitis
Uncommon manifestations of meningococcal disease • • • Endocarditis Purulent pericarditis Pneumonia (in 15% + pleural effusion or empyema) Endophthalmitis Mesenteric lymphadenitis Osteomyelitis Sinusitis Otitis media Periorbital cellulitis Primary purulent conjunctivitis Urethritis, cervicitis, vulvovaginitis, proctitis
 Antibiotic therapy before hospitalization for meningococcal, pneumococcal and hemophylus infections (Writing Group for Therapeutic Guidelines: Antibiotic 11 -th edition: Therapeutic Guidelines LTd. 2000. Melbourne) Drug Ceftriaxon Age Dosage Under 10 years Once, IV or IM 100 mg/kg (not exceed 2 g) Older 10 years and adults Once, IV or IM, 1000 mg
Antibiotic therapy before hospitalization for meningococcal, pneumococcal and hemophylus infections (Writing Group for Therapeutic Guidelines: Antibiotic 11 -th edition: Therapeutic Guidelines LTd. 2000. Melbourne) Drug Ceftriaxon Age Dosage Under 10 years Once, IV or IM 100 mg/kg (not exceed 2 g) Older 10 years and adults Once, IV or IM, 1000 mg
 Treatment before hospitalization at the presence of meningitis and gemorrhagic rash 1. 2. 3. 4. Dexamethazone – 4 mg IM once Ceftriaxon – 100 mg/kg IM once – 15’ later Analgin 0. 1 ml/year at fever > 38 C IV normal saline (10 -20 ml/kg/hour)
Treatment before hospitalization at the presence of meningitis and gemorrhagic rash 1. 2. 3. 4. Dexamethazone – 4 mg IM once Ceftriaxon – 100 mg/kg IM once – 15’ later Analgin 0. 1 ml/year at fever > 38 C IV normal saline (10 -20 ml/kg/hour)
 Etiologic treatment • Start antibiotic – ceftriaxon (100 mg/kg/d) or cefotaxim (200 mg/kg/d) • Reserve antibiotic – meropenem (120 mg/kg/d) Length of therapy – 10 -14 days, till clinics disappearance and normal cytosis of CSF (50 cells are admissible if lymphocytes)
Etiologic treatment • Start antibiotic – ceftriaxon (100 mg/kg/d) or cefotaxim (200 mg/kg/d) • Reserve antibiotic – meropenem (120 mg/kg/d) Length of therapy – 10 -14 days, till clinics disappearance and normal cytosis of CSF (50 cells are admissible if lymphocytes)
 Etiologic treatment Proved meningococcal infection: Penicillin G – starting dose • Meningococcemia – 300 000 U/kg/d • Meningitis - 500 000 U/kg/d Maximal allowed dose - 1 000 U/kg/d
Etiologic treatment Proved meningococcal infection: Penicillin G – starting dose • Meningococcemia – 300 000 U/kg/d • Meningitis - 500 000 U/kg/d Maximal allowed dose - 1 000 U/kg/d
 Pathogenic therapy for meningitis Septic shock • Bolus 0. 9% Na. Cl, start with 20 ml/kg, then – 10 ml/kg every hour before hematocrit → 33 %; • Cardiotonic drugs (dopamin) Brain edema • Osmotic dehydratation: mannitol, manit • Hyperventilation Seizures • • • Deafness prophylaxis Barbiturates, benzodiazepins Hyponatremic seizures: 3 % Na. Cl – 10 -12 ml/kg/h Hypoglycemic seizures (under 3 mo): 5 -10 % glucose • Dexametazone 0, 15 mg/kg every 6 h – 2 days, first dose - 15 minutes before antibiotics
Pathogenic therapy for meningitis Septic shock • Bolus 0. 9% Na. Cl, start with 20 ml/kg, then – 10 ml/kg every hour before hematocrit → 33 %; • Cardiotonic drugs (dopamin) Brain edema • Osmotic dehydratation: mannitol, manit • Hyperventilation Seizures • • • Deafness prophylaxis Barbiturates, benzodiazepins Hyponatremic seizures: 3 % Na. Cl – 10 -12 ml/kg/h Hypoglycemic seizures (under 3 mo): 5 -10 % glucose • Dexametazone 0, 15 mg/kg every 6 h – 2 days, first dose - 15 minutes before antibiotics
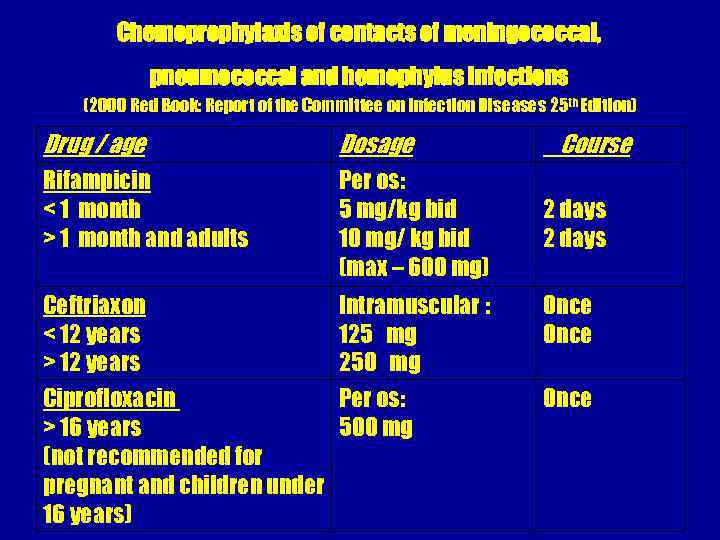 Chemoprophylaxis of contacts of meningococcal, pneumococcal and hemophylus infections (2000 Red Book: Report of the Committee on Infection Diseases 25 th Edition) Drug / age Dosage Rifampicin < 1 month > 1 month and adults Per os: 5 mg/kg bid 10 mg/ kg bid (max – 600 mg) Ceftriaxon < 12 years > 12 years Intramuscular : 125 mg 250 mg Ciprofloxacin Per os: > 16 years 500 mg (not recommended for pregnant and children under 16 years) Course 2 days Once
Chemoprophylaxis of contacts of meningococcal, pneumococcal and hemophylus infections (2000 Red Book: Report of the Committee on Infection Diseases 25 th Edition) Drug / age Dosage Rifampicin < 1 month > 1 month and adults Per os: 5 mg/kg bid 10 mg/ kg bid (max – 600 mg) Ceftriaxon < 12 years > 12 years Intramuscular : 125 mg 250 mg Ciprofloxacin Per os: > 16 years 500 mg (not recommended for pregnant and children under 16 years) Course 2 days Once
 Specific prophylaxis Total vaccination against meningococcal infection is not performed routinely in Ukraine. Vaccination is indicated to patients older 18 months with: Functional or anatomical asplenia Complement components insufficiency Properdin insufficiency Factor B insufficiency People from endemic areas
Specific prophylaxis Total vaccination against meningococcal infection is not performed routinely in Ukraine. Vaccination is indicated to patients older 18 months with: Functional or anatomical asplenia Complement components insufficiency Properdin insufficiency Factor B insufficiency People from endemic areas
 Specific prophylaxis Vaccination is indicated to patients older 18 months with (cont. ): • • • Hemoglobinopathies Nephrotic syndrome CSF shunting Cellular and humoral immunodeficiencies HIV infection Chronic diseases of cardiovascular, respiratory systems and liver
Specific prophylaxis Vaccination is indicated to patients older 18 months with (cont. ): • • • Hemoglobinopathies Nephrotic syndrome CSF shunting Cellular and humoral immunodeficiencies HIV infection Chronic diseases of cardiovascular, respiratory systems and liver
 Specific prophylaxis Characteristics of vaccine (Meningitis Vaccine Project, 2007) Characteristics Tetravalent polysaccharide (MPSV 4) Tetravalent conjugated (MCV 4) Composition Pure polysaccharides A, C, Y, W-135, conjugated to Diphhteria toxoid Immunogenic in children Low High Bactericidal activity of Аb Low in children Immunologic memory No induction Nasopharyngeal carriage Transitory and incomplete High Yes Documented decrease
Specific prophylaxis Characteristics of vaccine (Meningitis Vaccine Project, 2007) Characteristics Tetravalent polysaccharide (MPSV 4) Tetravalent conjugated (MCV 4) Composition Pure polysaccharides A, C, Y, W-135, conjugated to Diphhteria toxoid Immunogenic in children Low High Bactericidal activity of Аb Low in children Immunologic memory No induction Nasopharyngeal carriage Transitory and incomplete High Yes Documented decrease


