c7086b2f609f28590ed7c3024e3f1bb0.ppt
- Количество слайдов: 40
 Increasing Participation in the NHS Delivering the NHS Mandate Giles Wilmore Luke O’Shea NHS England 2 nd December 2013
Increasing Participation in the NHS Delivering the NHS Mandate Giles Wilmore Luke O’Shea NHS England 2 nd December 2013
 Structure of presentation 1. Patient Participation – The Mandate & legislation 2. Three great challenges for the NHS. Safety, changing burden of disease and finance 3. Establishing a way forward – building the House of Care 4. How do you empower patients? – the evidence base 5. What might it look like for your area? 6. What are the barriers to change? Practice, culture change, professional leadership 2
Structure of presentation 1. Patient Participation – The Mandate & legislation 2. Three great challenges for the NHS. Safety, changing burden of disease and finance 3. Establishing a way forward – building the House of Care 4. How do you empower patients? – the evidence base 5. What might it look like for your area? 6. What are the barriers to change? Practice, culture change, professional leadership 2
 Patient Participation – The Mandate & legislation ‘Personalising services from the front door’ 3
Patient Participation – The Mandate & legislation ‘Personalising services from the front door’ 3
 The NHS Mandate – objective on patient participation in care The NHS Mandate Objective: • “To ensure the NHS becomes dramatically better at involving patients… empowering them to manage and make decisions about their own care and treatment. ” • “by 2015… more people managing own health… everyone with LTCs including MH, offered a personalised care plan… patients who could benefit have the option to hold a personal health budget… information to make fully informed decisions. ” • Shared decision making, self-management, PHBs, information and personalised care planning all linked 4
The NHS Mandate – objective on patient participation in care The NHS Mandate Objective: • “To ensure the NHS becomes dramatically better at involving patients… empowering them to manage and make decisions about their own care and treatment. ” • “by 2015… more people managing own health… everyone with LTCs including MH, offered a personalised care plan… patients who could benefit have the option to hold a personal health budget… information to make fully informed decisions. ” • Shared decision making, self-management, PHBs, information and personalised care planning all linked 4
 Legal duties on commissioners and providers around participation 2012 Health and Social Care Act. Legal duty to promote individual participation in their own treatment and care: 1. Personalised care planning – including Personal Health Budgets, good information and support 2. Self-management support 3. Shared decision making NHS Constitution: • A patient right to participate fully in healthcare decisions • Commitment to transparency in service planning 5
Legal duties on commissioners and providers around participation 2012 Health and Social Care Act. Legal duty to promote individual participation in their own treatment and care: 1. Personalised care planning – including Personal Health Budgets, good information and support 2. Self-management support 3. Shared decision making NHS Constitution: • A patient right to participate fully in healthcare decisions • Commitment to transparency in service planning 5
 What is shared Decision Making? Two experts in the room. Clinician Patient • Diagnosis • Disease aetiology • Prognosis • Treatment options • Outcome probabilities • Experience of illness • Social circumstances • Attitude to risk • Values • Preferences • Goals Reference: adapted from Angela Coulter
What is shared Decision Making? Two experts in the room. Clinician Patient • Diagnosis • Disease aetiology • Prognosis • Treatment options • Outcome probabilities • Experience of illness • Social circumstances • Attitude to risk • Values • Preferences • Goals Reference: adapted from Angela Coulter
 Three great challenges for the NHS: 1. Safety 2. The changing burden of disease 3. Finance 7
Three great challenges for the NHS: 1. Safety 2. The changing burden of disease 3. Finance 7
 1) Safety - Patient participation key line of defence. Francis & Berwick “The patient was presented with medication & discharged. No one had told her of her diagnosis. ” Francis Report “Patient involvement is crucial to the delivery of appropriate, meaningful and safe healthcare…The goal is to achieve a pervasive culture that welcomes authentic patient partnership – in their own care” 8 Berwick Report
1) Safety - Patient participation key line of defence. Francis & Berwick “The patient was presented with medication & discharged. No one had told her of her diagnosis. ” Francis Report “Patient involvement is crucial to the delivery of appropriate, meaningful and safe healthcare…The goal is to achieve a pervasive culture that welcomes authentic patient partnership – in their own care” 8 Berwick Report
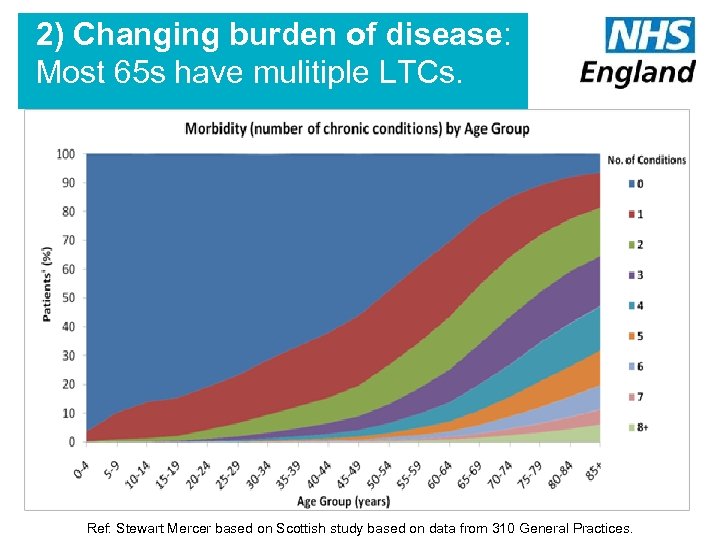 2) Changing burden of disease: Most 65 s have mulitiple LTCs. 9 Ref: Stewart Mercer based on Scottish study based on data from 310 General Practices.
2) Changing burden of disease: Most 65 s have mulitiple LTCs. 9 Ref: Stewart Mercer based on Scottish study based on data from 310 General Practices.
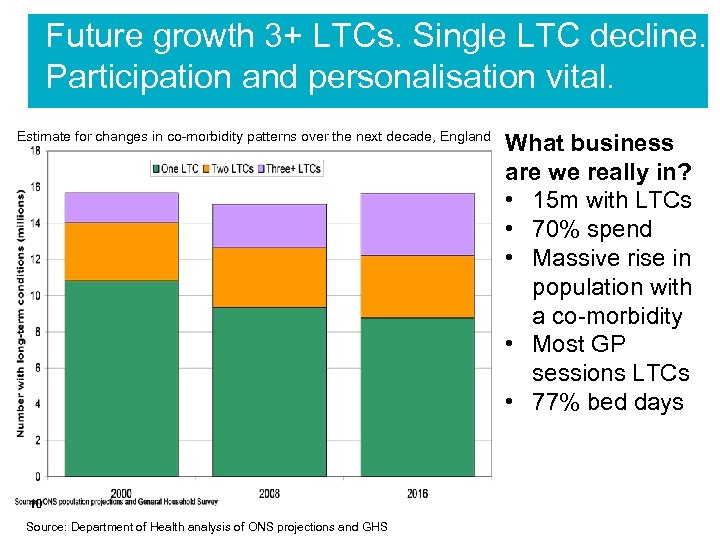 Future growth 3+ LTCs. Single LTC decline. Participation and personalisation vital. Estimate for changes in co-morbidity patterns over the next decade, England 10 Source: Department of Health analysis of ONS projections and GHS What business are we really in? • 15 m with LTCs • 70% spend • Massive rise in population with a co-morbidity • Most GP sessions LTCs • 77% bed days
Future growth 3+ LTCs. Single LTC decline. Participation and personalisation vital. Estimate for changes in co-morbidity patterns over the next decade, England 10 Source: Department of Health analysis of ONS projections and GHS What business are we really in? • 15 m with LTCs • 70% spend • Massive rise in population with a co-morbidity • Most GP sessions LTCs • 77% bed days
 Investing in the capacity of patients to create value in health • Current model medical staff, tech and drugs create value. QIPP 1 model was pay and provider efficiency. • More of the same model will mean unsustainable demands on staff. • QIPP 2 – New model must build capacity of patients to add value into the health system. • Increasing contribution of 53 m patients. All other industries look do this (e. g. banks, supermarkets). • Contribution of 3 m volunteers in health and care • Self management is key – increasing effectiveness of patients 5800 waking hours vs few hours with NHS. 11 NHS | Presentation to [XXXX Company] | [Type Date]
Investing in the capacity of patients to create value in health • Current model medical staff, tech and drugs create value. QIPP 1 model was pay and provider efficiency. • More of the same model will mean unsustainable demands on staff. • QIPP 2 – New model must build capacity of patients to add value into the health system. • Increasing contribution of 53 m patients. All other industries look do this (e. g. banks, supermarkets). • Contribution of 3 m volunteers in health and care • Self management is key – increasing effectiveness of patients 5800 waking hours vs few hours with NHS. 11 NHS | Presentation to [XXXX Company] | [Type Date]
 Commissioners signposted to programmes, tools and training Information Services: • Patient Decision Aids, Information Prescriptions, Accessible Information Standards, Access to electronic records. Enabling self-management & care planning: • Personalised Care Plans for all with LTC. Personal Health Budgets. Tools and apps (e. g. Vitrucare, Health Fabric) • Health literacy programmes, Expert Patient, community health champions, volunteer health trainers, Personal/tele coaching • Peer support networks (face to face & online) Training and leadership • Training for health professionals in shared decision making and personalisation; Patient leadership programmes; Info Standard. Local support through CCGs, CSUs and VCS. 12
Commissioners signposted to programmes, tools and training Information Services: • Patient Decision Aids, Information Prescriptions, Accessible Information Standards, Access to electronic records. Enabling self-management & care planning: • Personalised Care Plans for all with LTC. Personal Health Budgets. Tools and apps (e. g. Vitrucare, Health Fabric) • Health literacy programmes, Expert Patient, community health champions, volunteer health trainers, Personal/tele coaching • Peer support networks (face to face & online) Training and leadership • Training for health professionals in shared decision making and personalisation; Patient leadership programmes; Info Standard. Local support through CCGs, CSUs and VCS. 12
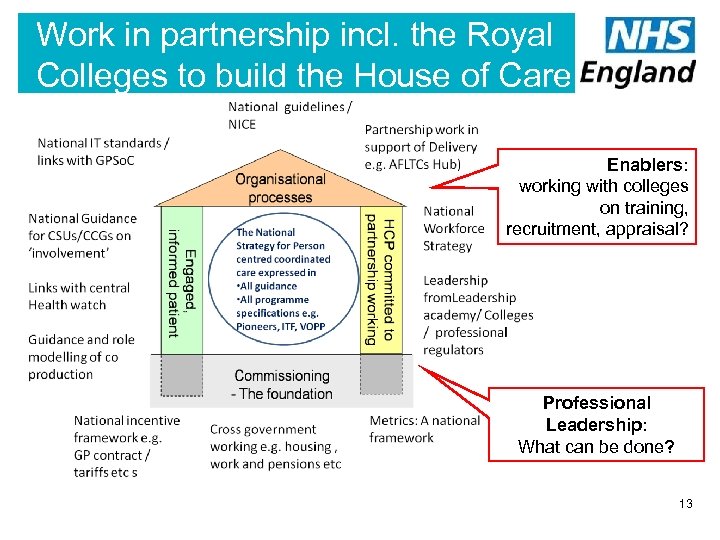 Work in partnership incl. the Royal Colleges to build the House of Care Enablers: working with colleges on training, recruitment, appraisal? Professional Leadership: What can be done? 13
Work in partnership incl. the Royal Colleges to build the House of Care Enablers: working with colleges on training, recruitment, appraisal? Professional Leadership: What can be done? 13
 Patient activation can be improved - interventions & clinician training Self-Management Support, such as Expert Patient • Impact of behaviours, Quality of life, symptoms and better use of resources. • Not just technical information, but behaviour change Personal Health Budgets & personalised care planning • RCT: cost effective, improved Quality of Life, best for high needs. Other studies show impact on carer well-being Shared Decision Making, including Patient Decision Aids • Better experience of care, some reduction in use of services, less surgery. 14 NHS | Presentation to [XXXX Company] | [Type Date]
Patient activation can be improved - interventions & clinician training Self-Management Support, such as Expert Patient • Impact of behaviours, Quality of life, symptoms and better use of resources. • Not just technical information, but behaviour change Personal Health Budgets & personalised care planning • RCT: cost effective, improved Quality of Life, best for high needs. Other studies show impact on carer well-being Shared Decision Making, including Patient Decision Aids • Better experience of care, some reduction in use of services, less surgery. 14 NHS | Presentation to [XXXX Company] | [Type Date]
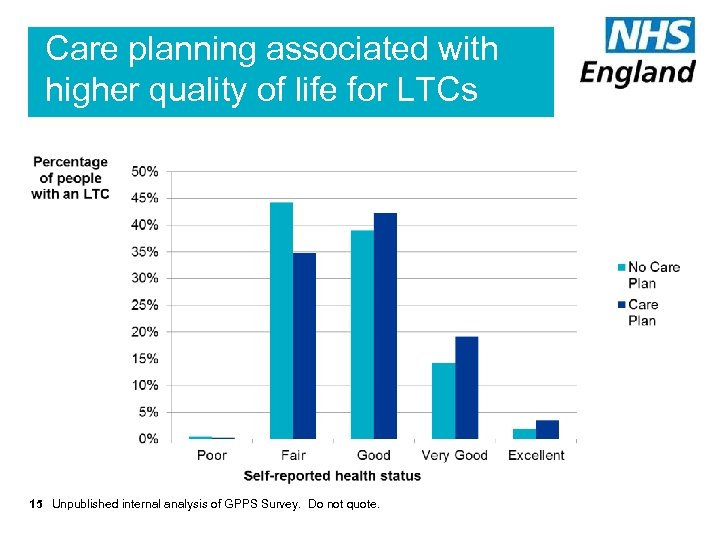 Care planning associated with higher quality of life for LTCs 15 Unpublished internal analysis of GPPS Survey. Do not quote.
Care planning associated with higher quality of life for LTCs 15 Unpublished internal analysis of GPPS Survey. Do not quote.
 What are the barriers to change? Changing practice, systems, culture change, professional leadership 16
What are the barriers to change? Changing practice, systems, culture change, professional leadership 16
 This means changing practice. How does your area look? Passive model of NHS care Participative model Acute – Poorly informed patients and paternalistic treatment Acute – Informed patients & shared decision making Primary care - Single disease treated reactively. 10 minute consultation. Primary Care - Personalised proactive care planned for multiple LTCs. Greater self management. Mental Health – treat and manage symptoms of disease. Dependency Mental Health – holistic support focused on wider personal goals. Greater self and peer support. Information one size fits all. Not a commissioned service Information and support services built into commissioning The consultation – single patient meets professional face to face Consultation in groups, peer support, expert patients, Skype Disjointed services for people with multiple Integrated services and 17 morbidity. No care planning. personalised care planning
This means changing practice. How does your area look? Passive model of NHS care Participative model Acute – Poorly informed patients and paternalistic treatment Acute – Informed patients & shared decision making Primary care - Single disease treated reactively. 10 minute consultation. Primary Care - Personalised proactive care planned for multiple LTCs. Greater self management. Mental Health – treat and manage symptoms of disease. Dependency Mental Health – holistic support focused on wider personal goals. Greater self and peer support. Information one size fits all. Not a commissioned service Information and support services built into commissioning The consultation – single patient meets professional face to face Consultation in groups, peer support, expert patients, Skype Disjointed services for people with multiple Integrated services and 17 morbidity. No care planning. personalised care planning
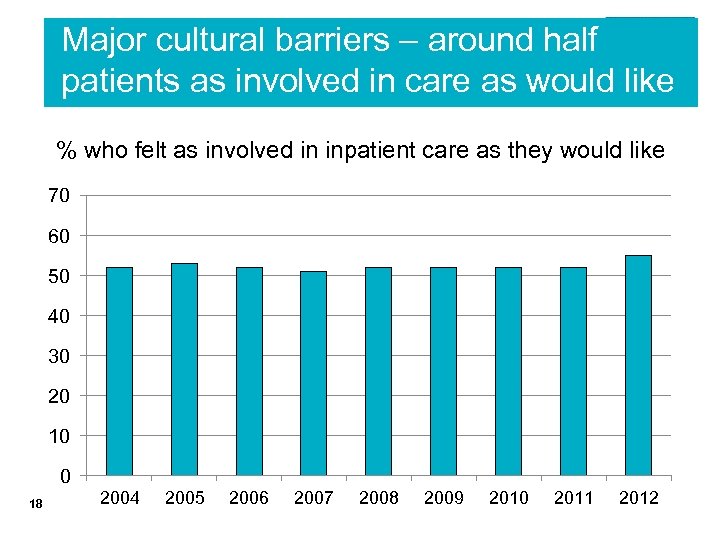 Major cultural barriers – around half patients as involved in care as would like % who felt as involved in inpatient care as they would like 70 60 50 40 30 20 10 0 18 2004 2005 2006 2007 2008 2009 2010 2011 2012
Major cultural barriers – around half patients as involved in care as would like % who felt as involved in inpatient care as they would like 70 60 50 40 30 20 10 0 18 2004 2005 2006 2007 2008 2009 2010 2011 2012
 Complex cultural change and alignment of incentives needed • Participation has been hard to shift over last 10 years • Biggest challenge is cultural change, workforce development and patient demand • Developing a Coalition committed to personalised care • Need to shift incentives from activity based payment • Need to support commissioning capacity and capability • How important is this? • What can the Royal Colleges do? • Would your members want to be involved in research and debate? 19
Complex cultural change and alignment of incentives needed • Participation has been hard to shift over last 10 years • Biggest challenge is cultural change, workforce development and patient demand • Developing a Coalition committed to personalised care • Need to shift incentives from activity based payment • Need to support commissioning capacity and capability • How important is this? • What can the Royal Colleges do? • Would your members want to be involved in research and debate? 19
 PHB Update
PHB Update
 What’s happening nationally and in Yorkshire and Humber? Nationally: • PHB Delivery team, website and resources and workstreams eg for continuing health care, children’s, peer network, financial sustainability, mental health, on line self assessment tools, • Accelerated development programme Yorkshire and Humber • Personal Health Budget Network for commissioners • Development programme of events and seminars • Awareness raising eg CCGs, networks, CVS 21
What’s happening nationally and in Yorkshire and Humber? Nationally: • PHB Delivery team, website and resources and workstreams eg for continuing health care, children’s, peer network, financial sustainability, mental health, on line self assessment tools, • Accelerated development programme Yorkshire and Humber • Personal Health Budget Network for commissioners • Development programme of events and seminars • Awareness raising eg CCGs, networks, CVS 21
 Accelerated Development Programme Leeds: • Day 1 - 17 th July 2014 Day 2 - 4 th September 2014 Day 3 - 8 th October 2014 Day 4 – 11 th November 2014 Day 5 – 11 th December 2014
Accelerated Development Programme Leeds: • Day 1 - 17 th July 2014 Day 2 - 4 th September 2014 Day 3 - 8 th October 2014 Day 4 – 11 th November 2014 Day 5 – 11 th December 2014
 Making personal health budgets work for children • As well as for NHS Continuing Healthcare - the 'right to ask' for a personal health budget also applies to children receiving continuing care. The national PHB team have just published a new page on the website about making personal budgets work for children, as part of the roll out of SEND reforms and the new EHC (Education, Health & Care) plans from September 2014.
Making personal health budgets work for children • As well as for NHS Continuing Healthcare - the 'right to ask' for a personal health budget also applies to children receiving continuing care. The national PHB team have just published a new page on the website about making personal budgets work for children, as part of the roll out of SEND reforms and the new EHC (Education, Health & Care) plans from September 2014.
 Demand for PHBs • New member of the national PHB delivery team is Alix Crawford • Alix will be working with community voluntary sector and peer networks to raise awareness of PHBs
Demand for PHBs • New member of the national PHB delivery team is Alix Crawford • Alix will be working with community voluntary sector and peer networks to raise awareness of PHBs
 Peer Leadership • A national peer leadership programme to encourage people with PHB/experience to learn leadership skills • Yorkshire and Humber PHB network will be working with Rita Brewis and Colin Royle later in the year to encourage peers to join the network and contribute to PHB development
Peer Leadership • A national peer leadership programme to encourage people with PHB/experience to learn leadership skills • Yorkshire and Humber PHB network will be working with Rita Brewis and Colin Royle later in the year to encourage peers to join the network and contribute to PHB development
 Mental Health • Webinars • Demonstrator sites: Devon Partnership NHS Trust and Positive Opportunities for Wellbeing CIC , Dorset CCG , South London and Maudsley NHS Foundation Trust Addictions Clinical Academic Group , Stockport CCG and Stockport Local Authority , Southwark CCG and Southwark Local Authority , South Coast Kent CCG , South West London and St George's Mental Health NHS Trust and Kingston CCG and Royal Borough of Kingston. • A further six network sites are also joining the programme: Notttingham City CCG, Brighton & Sussex Care, Islington CCG, Central & North West London, Warrington CCG, Castlepoint & Rochford CCG
Mental Health • Webinars • Demonstrator sites: Devon Partnership NHS Trust and Positive Opportunities for Wellbeing CIC , Dorset CCG , South London and Maudsley NHS Foundation Trust Addictions Clinical Academic Group , Stockport CCG and Stockport Local Authority , Southwark CCG and Southwark Local Authority , South Coast Kent CCG , South West London and St George's Mental Health NHS Trust and Kingston CCG and Royal Borough of Kingston. • A further six network sites are also joining the programme: Notttingham City CCG, Brighton & Sussex Care, Islington CCG, Central & North West London, Warrington CCG, Castlepoint & Rochford CCG
 Plus. . . • • Financial sustainability Markers of progress POET Integration pioneers
Plus. . . • • Financial sustainability Markers of progress POET Integration pioneers
 Building capacity Having the right conversation In Yorkshire and Humber for Year of Care training we now have; One fully trained trainer Six trainers completing their training Programmes in May/June July (Leeds) November (Leeds) One tbc 7/19 national trainers in Yorkshire and Humber
Building capacity Having the right conversation In Yorkshire and Humber for Year of Care training we now have; One fully trained trainer Six trainers completing their training Programmes in May/June July (Leeds) November (Leeds) One tbc 7/19 national trainers in Yorkshire and Humber
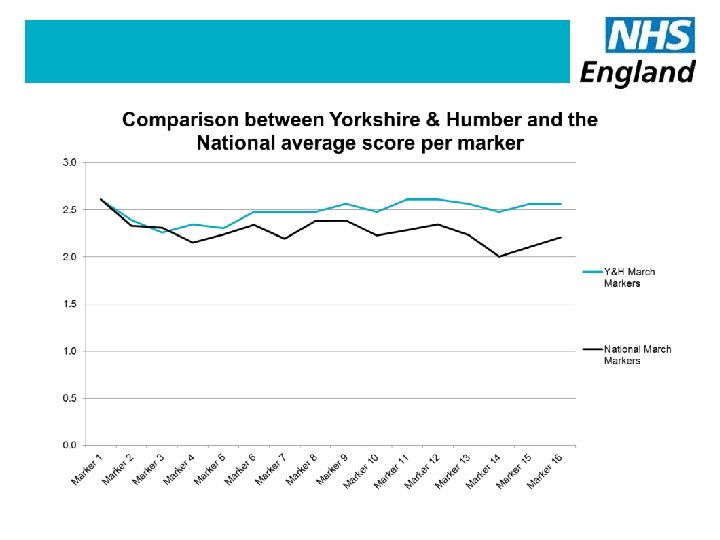
 Markers of Progress
Markers of Progress
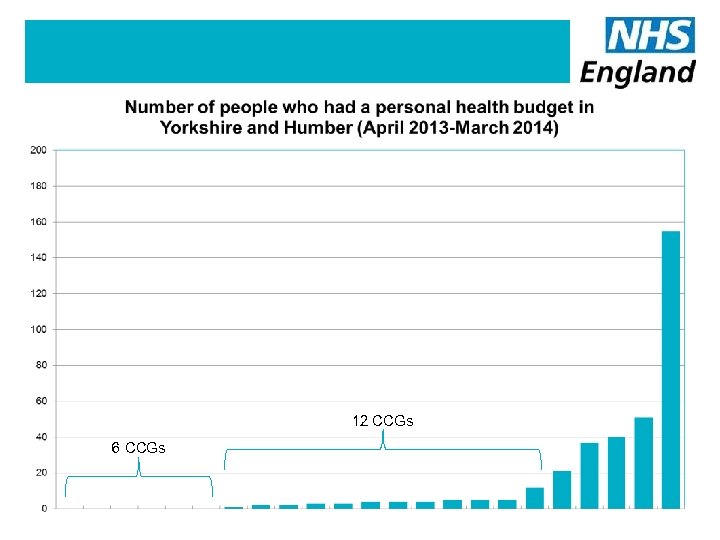 12 CCGs 6 CCGs
12 CCGs 6 CCGs
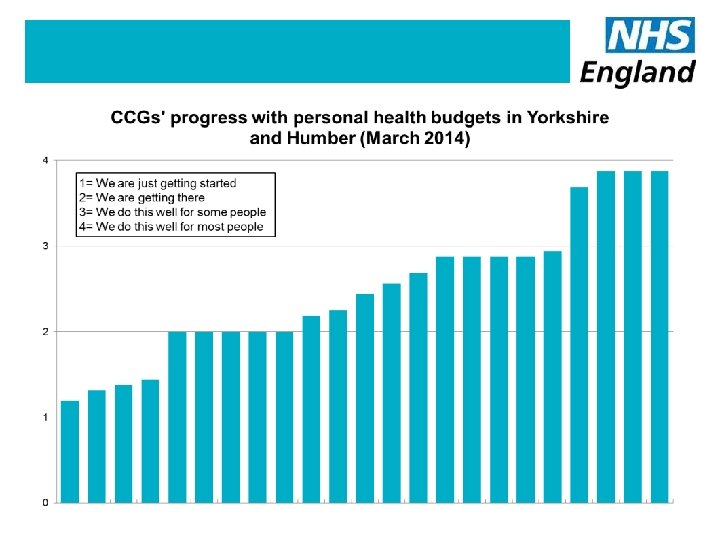
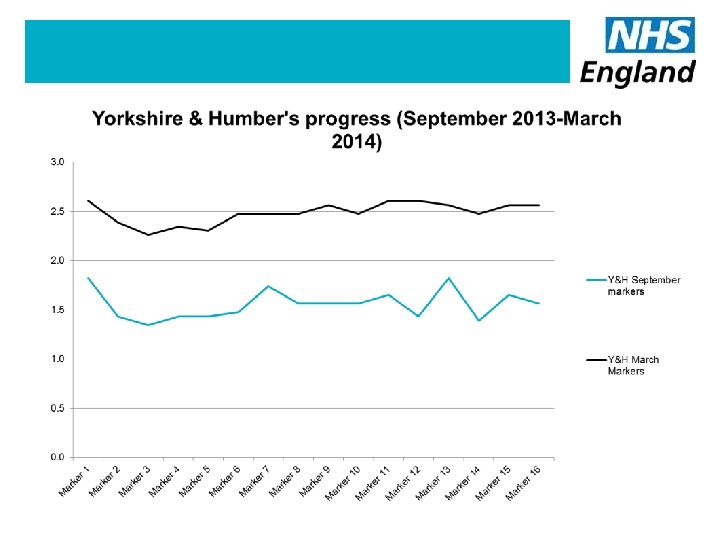
 How many personal health budgets ? Nationally in March 2014 • 206 of the 211 CCGs reported that over 2, 200 people had a PHB • 63% of those were a direct payment • 134 CCGs were delivering PHBs • 77 had yet to offer a PHB Yorkshire and Humber • 335 people had a PHB (15% of the national total) and an increase from 103 budgets in January 2014 • 17 of the 23 CCGs are offering PHBs 34
How many personal health budgets ? Nationally in March 2014 • 206 of the 211 CCGs reported that over 2, 200 people had a PHB • 63% of those were a direct payment • 134 CCGs were delivering PHBs • 77 had yet to offer a PHB Yorkshire and Humber • 335 people had a PHB (15% of the national total) and an increase from 103 budgets in January 2014 • 17 of the 23 CCGs are offering PHBs 34
 Resources Introduction to the personal health budgets toolkit Quick guide. . . www. personalhealthbudgets. england. nhs. uk 35
Resources Introduction to the personal health budgets toolkit Quick guide. . . www. personalhealthbudgets. england. nhs. uk 35
 Steph Carson Personal Health Budget Network Lead s. carson@darleyconsulting. co. uk Mob : 07894387556 www. personalhealthbudgets. england. nhs. uk Yorkshire and Humber : A personal approach to healthcare
Steph Carson Personal Health Budget Network Lead s. carson@darleyconsulting. co. uk Mob : 07894387556 www. personalhealthbudgets. england. nhs. uk Yorkshire and Humber : A personal approach to healthcare
 Table top discusssions. . What are the key issues around personalising health and social care? - Nationally? - Locally ? 37
Table top discusssions. . What are the key issues around personalising health and social care? - Nationally? - Locally ? 37
 Challenges. . What are the main challenges to personalising health and social care? 38
Challenges. . What are the main challenges to personalising health and social care? 38
 Risks and Opportunities. . . What are the risks and opportunities to personalising health and social care? 39
Risks and Opportunities. . . What are the risks and opportunities to personalising health and social care? 39
 Resources. . What do you have in place locally already? eg senior leadership sign up, levels of coproduction and engagement, equal access to budgets, communicating local deals, informed care planning, a whole life approach, risk enablement, a developed market, review. . and what else? 40
Resources. . What do you have in place locally already? eg senior leadership sign up, levels of coproduction and engagement, equal access to budgets, communicating local deals, informed care planning, a whole life approach, risk enablement, a developed market, review. . and what else? 40


