e4da3705e78c8fe86b9920fc487ac8fc.ppt
- Количество слайдов: 172

In the Name of God Obstetrics Study Guide 3 Mitra Ahmad Soltani 2008

References • • Iranian Council for graduate Medical Education. Board and pre-board Exam questions for OBS and Gyn. 2001 -2006 Panda S. IUGR. Department of Obstetrics & Gynecology Medical College of India 2002 Pritchard JA, Mac. Donald PC, Gant NF. Williams Obstetrics. 22 nd ed. New York, NY: Mc. Graw-Hill; 2005. Tan T and Yeo G. IUGR. Current Opinion in Obstetrics and Gynecology 2005, 17: 135142 emedicine e-journal: • • • Butler J. postterm delivery. emedicine. June 19. 2006 Gaufberg S. Abruptio placenta. emedicine. Aug 29. 2006 Gibson P. HTN in Pregnancy. emedicine. DEC 13 2007 Hernandez E. GTN. emedicine. Jan 26, 2007 Marinnan G. Placenta Previa. emedicine. Aug 26. 2005 Ross M. preterm. emedicine. 31 may 2007 • Zach T. multiple pregnancy. emedicine. Oct 2. 2007 Pictures and material of multiple pregnancy are adapted with permission from:

HTN in Pregnancy

classification • Hypertension is the most common medical problem encountered during pregnancy, complicating 2 -3% of pregnancies. • HTN is classified into 4 categories 1) chronic hypertension, 2) preeclampsia-eclampsia, 3) preeclampsia superimposed on chronic hypertension 4) gestational hypertension (transient hypertension of pregnancy or chronic hypertension identified in the latter half of pregnancy).

Chronic HTN • blood pressure exceeding 140/90 mm Hg before pregnancy or before 20 weeks' gestation. It persists after 12 wks postpartum.

Gestational Age – New-onset or worsening hypertension after 20 weeks' gestation should lead to a careful evaluation for manifestations of preeclampsia. – The diagnosis of severe hypertension or preeclampsia in the first or early second trimester necessitates exclusion of GTD and/or molar pregnancy.

Maternal Risk factors • First pregnancy • New partner/paternity • Age younger than 18 or older than 35 years • History of preeclampsia • Family history of preeclampsia in a firstdegree relative • Black race • Obesity (BMI >35) • Interpregnancy interval less than 2 years or more than 10 years • Chronic hypertension • Preexisting diabetes (type 1 or type 2) • Renal disease • SLE • Obesity • Thrombophilia

Placental Risk factor – Multiple gestations – Hydrops fetalis – Gestational trophoblastic disease – Triploidy

BP measurement Blood pressure should be measured in the sitting position, with the cuff at the level of the heart. Women should be allowed to sit quietly for 5 -10 minutes before each blood pressure measurement. Korotkoff sounds I (the first sound) and V (the disappearance of sound) should be used to denote the systolic blood pressure (SBP) and DBP, respectively.
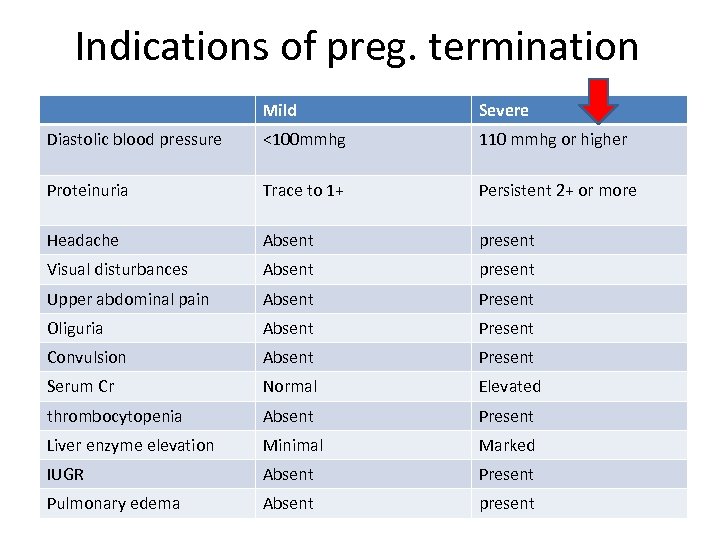
Indications of preg. termination Mild Severe Diastolic blood pressure <100 mmhg 110 mmhg or higher Proteinuria Trace to 1+ Persistent 2+ or more Headache Absent present Visual disturbances Absent present Upper abdominal pain Absent Present Oliguria Absent Present Convulsion Absent Present Serum Cr Normal Elevated thrombocytopenia Absent Present Liver enzyme elevation Minimal Marked IUGR Absent Present Pulmonary edema Absent present

CBC • Platelet counts less than 100, 000/µL suggest preeclampsia or ITP. • Hemoglobin levels greater than 13 g/d. L suggest hemoconcentration. • Low Hbg levels may be due to microangiopathic hemolysis or iron deficiency.

Proteinurea – Trace levels to +1 proteinuria are acceptable, but levels of +2 or greater are abnormal and should be quantified with a 24 -hour urine collection or spot urine protein: creatinine ratio. – In a 24 -hour urine collection, the reference range for protein excretion in pregnancy is up to 300 mg/d.

Protein: Cr ratio • Creatinine clearance increases approximately 50% during pregnancy, and levels less than 100 m. L/min suggest renal dysfunction that is either chronic or due to preeclampsia. • protein: Cr ratios appear to be more accurate than urinalysis, although an abnormal result should still be confirmed with a 24 -hour urine collection.

Coagulation tests • • • LDH, bilirubin, haptoglobin, fibrinogen, D-dimers If: PT/INR/a. PTT results are abnormal, thrombocytopenia is present, the hemoglobin level is dropping

Fetal Monitoring –Alternate a biophysical profile with a fetal NST twice each week. – Ask for Serial fetal ultrasound starting at 18 weeks.

Methyldopa (Aldomet) Centrally acting antihypertensive agent widely considered the first-line agent for treatment of hypertension during pregnancy. 250 mg PO bid/tid; increase q 2 d prn; not to exceed 3 g/d

Hydralazine (Apresoline) Intravenous form is useful when treating severe hypertension due to preeclampsia/eclampsia. 10 -20 mg/dose IV q 4 -6 h prn initial; increase to 40 mg per dose prn BP >170/110 mm Hg: 0. 1 -0. 2 mg/kg/dose IV q 4 -6 h prn; not to exceed 20 mg or 1. 7 -3. 5 mg/kg/d IV divided q 4 -6 h

Life-threatening complications in preeclampsia • • Seizures Cerebral hemorrhage Pulmonary edema Acute renal failure DIC HELLP syndrome Hepatic infarction/rupture and subcapsular hematoma

IMP: mild preeclampsia • General: condition/position/diet =low salt, high prot • Lab: CBC , BG, Rh, U/A, 24 hr urine (prot, cr, vol), BUN/Cr, PT, PTT, Fib, ALT, AST, Al P, Bil (T, D) • reserve of 2 units of PC • IV : Ringer at heparin lock • OTHER: Control of vital sign q 4 hrs, control of FHR, FAD chart , NST, sono OB, daily weight inform if BP>160/110, blurred vision, head ache, epigastric pain, seizure
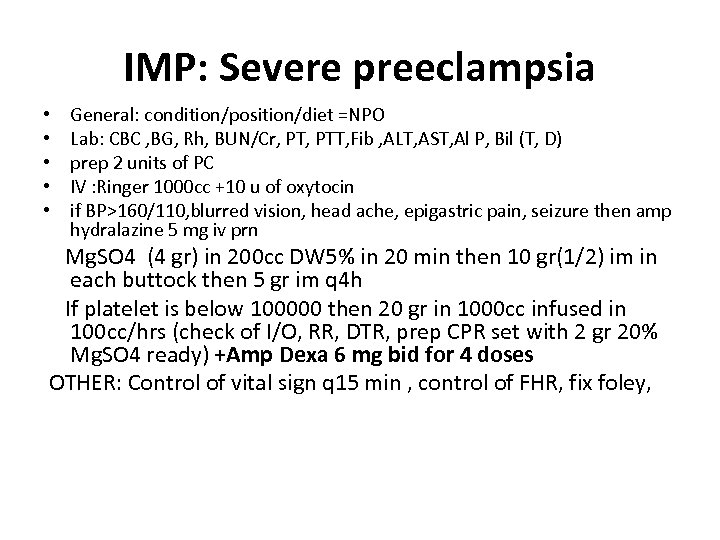
IMP: Severe preeclampsia • • • General: condition/position/diet =NPO Lab: CBC , BG, Rh, BUN/Cr, PTT, Fib , ALT, AST, Al P, Bil (T, D) prep 2 units of PC IV : Ringer 1000 cc +10 u of oxytocin if BP>160/110, blurred vision, head ache, epigastric pain, seizure then amp hydralazine 5 mg iv prn Mg. SO 4 (4 gr) in 200 cc DW 5% in 20 min then 10 gr(1/2) im in each buttock then 5 gr im q 4 h If platelet is below 100000 then 20 gr in 1000 cc infused in 100 cc/hrs (check of I/O, RR, DTR, prep CPR set with 2 gr 20% Mg. SO 4 ready) +Amp Dexa 6 mg bid for 4 doses OTHER: Control of vital sign q 15 min , control of FHR, fix foley,

Preterm Pregnancy

Definition • Preterm labor is defined as the presence of uterine contractions of sufficient frequency and intensity to effect progressive effacement and dilation of the cervix prior to term gestation (between 20 and 37 wk). • It is the leading cause of neonatal mortality.

Causes of preterm Labor • decidual hemorrhage, (eg, abruption, mechanical factors such as uterine overdistension from multiple gestation or polyhydramnios), • cervical incompetence (eg, trauma, cone biopsy), • uterine distortion (eg, müllerian duct abnormalities, fibroid uterus), • cervical inflammation (bacterial vaginosis [BV], trichomonas), • maternal inflammation/fever (eg, urinary tract infection), • hormonal changes (eg, mediated by maternal or fetal stress), • Uteroplacental insufficiency (eg, hypertension, insulindependent diabetes, drug abuse, smoking, alcohol).

Risk factors of preterm birth • Demographic factors for preterm labor include nonwhite race, extremes of maternal age (<17 y or >35 y), low socioeconomic status, and low prepregnancy weight. • Preterm labor and birth can be associated with stressful life situations (eg, domestic violence; close family death; insecurity over food, home, or partner; work and home environment) • Previous preterm delivery

Methods for predicting preterm birth • home uterine activity monitoring (HUAM) • salivary estriol : DHEA increases before the onset of labor. This results in an increase of maternal estriol. • FFN is a basement membrane protein that helps bind placental membranes to the decidua. FFN has a predictive value in identifying patients who will or will not deliver within the subsequent 1 -2 weeks. • A short cervical length in the early or late second trimester has been associated with a markedly increased risk of preterm labor and delivery.

Contraindication to tocolysis 1 -Fetal growth restriction 2 -Oligohydramnios 3 -Nonreactive NST, Positive CST 4 -Absent or reversed diastolic flow upon Doppler examination of umbilical blood flow 5 -Repetitive severe variable decelerations 6 -Significant vaginal bleeding consistent with abruption.

Definition of IAI (Intra Amniotic Infection) A temperature greater than 38. 0°C (100. 0°F) and 2 of the 5 following signs: 1 -WBC > 15, 000 cells/mm 3 2 -Maternal HR> 100 (bpm) 3 - Fetal HR> 160 bpm 4 -Tender uterus 5 -Foul-smelling discharge

Chorioamnionitis Order • General: condition/position/diet=NPO • Lab: CBC diff, MP, WW, B/C X 2, U/A , U/C, CXR, BUN/Cr • IV : 1000 cc Ringer +10 units of oxytocin start at 2 drops /min, add 2 drops every 15 min if FHR and contractions are normal Amp ampicillin 2 gr iv qid +gentamicin im 80 mg stat then 60 mg TDS AMP clindamycin 900 mg iv TDS for allergic women to penicillin(continue antibiotics after delivery until the mother is a febrile OTHER: Control of vital sign hourly
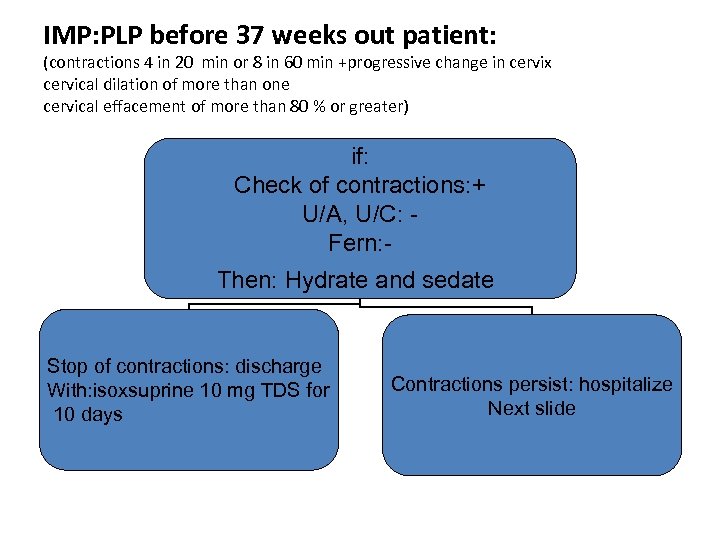
IMP: PLP before 37 weeks out patient: (contractions 4 in 20 min or 8 in 60 min +progressive change in cervix cervical dilation of more than one cervical effacement of more than 80 % or greater) if: Check of contractions: + U/A, U/C: Fern: Then: Hydrate and sedate Stop of contractions: discharge With: isoxsuprine 10 mg TDS for 10 days Contractions persist: hospitalize Next slide

IMP: PLP before 37 weeks, hospitalized • General: condition/position/diet • Lab: CBC, BG, Rh, U/A, U/C, fern, reserve of 2 units of PC • IV : 1 -1000 cc Ringer free 2 -Mg. SO 4 (4 gr) in 200 cc DW 5% in 20 min then 20 gr in 1000 cc infused in 100 cc/hrs (check of I/O, RR, DTR, prep CPR set- I/O with measure) 3 -Amp pethidine 25 mg iv 25 mg im 4 -Amp ampicillin 2 gr IV qid 5 -Amp erythromicin 400 mg QID 6 - Amp betamethasone 12 mg im, repeat after 24 hrs for GA below 34 wks • OTHER: Control of vital sign q 4 hrs, Inform if LP, leakage, VB, ab VS or FHR

Contraindication for beta mimetics Maternal • cardiac disease • Diabetes • Thyrotoxicosis • HTN

Contraindication for Mg. SO 4 • Hypocalcemia • Myasthenia gravis • Renal failure

Dosage of Ritodrine or Terbutaline for tocolysis • 50 -100 mcg/min increase by 50 mcg/min every 10 min • max dose: 350 mcg/min If labor is arrested continue the infusion for at least 12 hrs • SC: 250 mcg q 3 -4 hrs

Length of GA with multiple fetuses • Twin=36 wks • Triplets=33. 5 wks • Quadruplets=31 wks

Postterm

Definition of postterm • Postterm pregnancies define pregnancies extending up to or after 42 weeks. • The reported frequency is 3 -12%.

Cause of postterm P. • The most frequent cause of postterm pregnancy is inaccurate dating criteria • primiparity, • prior postterm pregnancy, • male gender of the fetus, • genetic factors

Risks of postterm P • Macrosomia complications like shoulder dystocia, CPD and Maternal risks like an increase in labor dystocia, perineal injuries, and cesarean deliveries. • dysmaturity syndrome: affects 20% of postterm fetuses and is thought to be caused by chronic uteroplacental insufficiency resulting in oligohydramnios, meconium aspiration, and reversible neonatal complications.

surveillance • NST and AFI 2 times per week for pregnancies continuing past 41 weeks.

Intra Uterine Growth Retardation

Definition • Intrauterine growth restriction (IUGR) occurs when the unborn baby is at or below the 10 th weight percentile for his or her age (in weeks). The fetus is affected by a pathologic restriction in its ability to grow. • Low birth weight (LBW) means a baby with a birth weight of less than 2500 Gms, which could be due to IUGR or Prematurity
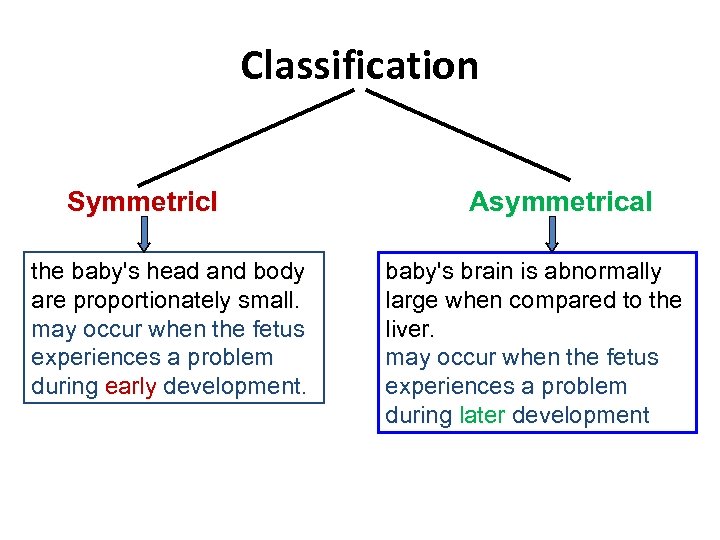
Classification Symmetricl the baby's head and body are proportionately small. may occur when the fetus experiences a problem during early development. Asymmetrical baby's brain is abnormally large when compared to the liver. may occur when the fetus experiences a problem during later development

Etiology of IUGR Idiopathic- In a majority of cases (40%)

• • Maternal Risk Factors Has had a previous baby with IUGR Extremes of age Small mothers (Ht & Wt) poor weight gain and malnutrition during preg. socially deprived Substance abuse (like tobacco, narcotics, alcohol) low total blood volume during early pregnancy

• • Maternal Risk Factors Multiple pregnancy Living in High altitude locations Drugs like anticoagulants, anticonvulsants Cardio-vascular disease: preeclampsia, HTN, cyanotic heart disease, cardiac disease Gr III & IV, diabetic vascular lesions Chronic kidney disease Chronic infection- UTI, Malaria, TB, genital infections Antibody abnormality like antiphospholipid antibody syndrome, SLE

Fetal Risk Factors • Intrauterine infection: German measles (rubella), cytomegalovirus, herpes simplex, tuberculosis, syphilis, or toxoplasmosis, TB, Malaria, Parvo virus B 19. • Birth defect (cardiovascular, renal, anencephally, limb defect, etc). • Chromosome defect(trisomy-18 (Edwards’ syndrome), 21(Down’s syndrome), 16, 13, xo (turner’s syndrome. ) • Primary disorder of bone or cartilage. • Chronic lack of oxygen during development (hypoxia). • Developed outside of the uterus. • Placenta or umbilical cord defects.

Placental Factors • Uteroplacental insufficiency: – Improper / inadequate trophoblastic invasion and placentation in the first trimester. • Lateral insertion of placenta. • Reduced maternal blood flow to the placental bed. • Fetoplacetal insufficiency due to: • Vascular anomalies of placenta and cord • Decreased placental functioning mass: • Small placenta, abruptio placenta, placenta previa, post term pregnancy.

Screening: • US fetal biometry: HC- BPD- AC • Uterine Doppler studies (Doppler Velocimetry): bilateral notches and a mean resistance index of at least 0. 55 Or • Unilateral notches and a mean resistance index of at least 0. 65 at 20 weeks. • Biochemistry: CRH level at 33 weeks

Neonatal Diagnosis Low ponderal index (Wt. /Fl). Decreased subcutaneous fat. Presence / appearance of – Hypoglycemia, Hyperbilirubinemia, Necrotizing enterocolitis, Hyper viscosity syndrome

Prevention Strong evidence of benefit only for the following interventions: • balanced protein/energy supplementation, • strategies to reduce maternal smoking, • antibiotic administration to prevent urinary tract infections • antimalarial prophylaxis.

Surveillance • • Non-Stress Test, Amniotic Fluid Index, Doppler of the Umbilical Artery Biophysical Profile

Surveillance n Amniotic Fluid Index (AFI) The current recommendations are that if the AFI decreases below 5 after 35 weeks, then delivery should occur.

Treatment • Bed rest • Aspirin before 20 wk GA • Nutritional supplementation: zinc , fish oil, hormones • Oxygen therapy.

For cases termination is indicated: • Corticosteroids with a delay in delivery for 2. 4 days • Mode of delivery depends on the bishop score and IUGR severity • For dichorionic twins : injection of KCl into the heart of the weaker fetus ( in most cases management is expectant) • For monochorionic twins photocoagulation of anastomoses or diathermy in cases of TTTS and AAA

Short Term Risks of IUGR for the neonate • • • Meconium Aspiration Syndrome, infection, hypoglycemia, hypothermia, Sudden Infant Death Syndrome,

Long term Prognosis • Fetal Death • low blood sugar • low body temperature • abnormal development of the nervous system Adulthood aftermath : • CAD • HTN • Diabetes II • Dyslipidemia • Stroke • Depression • Suicide attempts

abruptio

Definition • Abruptio placentae (ie, placental abruption) refers to separation of the normally located placenta after the 20 th week of gestation. • Abruptio placentae occurs in about 1% of all pregnancies.

Symptoms and signs – Vaginal bleeding - 80% – Abdominal or back pain and uterine tenderness - 70% – Fetal distress - 60% – Abnormal uterine contractions (eg, hypertonic, high frequency) - 35% – Idiopathic premature labor - 25% – Fetal death - 15%

Classification of abruptio • extent of separation (ie, partial vs complete) • location of separation (ie, marginal vs central) • Clinical
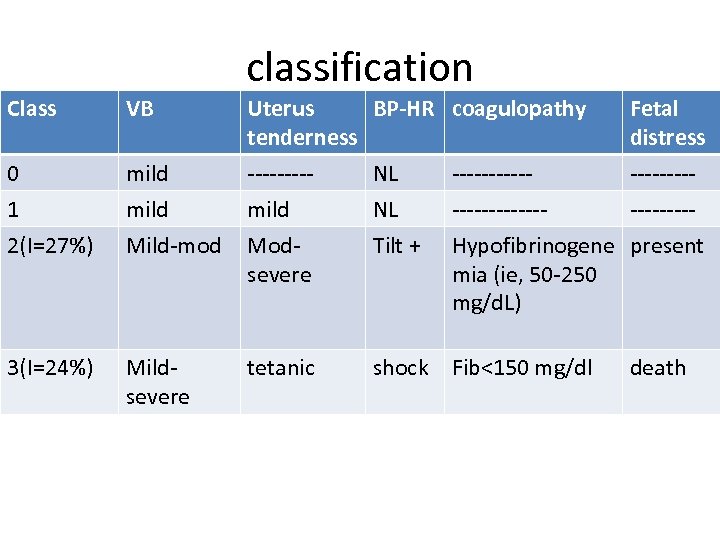
classification Class VB Uterus BP-HR coagulopathy tenderness ----NL -----mild NL ------- 0 1 mild 2(I=27%) Mild-mod Modsevere Tilt + 3(I=24%) Mildsevere tetanic shock Fib<150 mg/dl Fetal distress --------- Hypofibrinogene present mia (ie, 50 -250 mg/d. L) death

Causes 1 • • • Maternal HTN(44% of all cases) Maternal trauma Cigarette smoking Alcohol consumption Cocaine use Advanced maternal age

causes 2 • Short umbilical cord • Sudden decompression of the uterus (eg, PROM, delivery of first twin) • Retroplacental fibromyoma • postamniocentesis • Idiopathic (probable abnormalities of uterine blood vessels and decidua)

Imaging Studies • Ultrasonography is not very useful in diagnosing placental abruption. – Retroplacental hematoma may be recognized in 225% of all abruptions. – Recognition of retroplacental hematoma depends on the degree of hematoma and on the operator's skill level.

IMP: R/O abruption Condition/position/diet: NPO Lab: CBD-BG-Rh-U/A-U/C-PT-PTT-Fib-FDP-D-Dimer. Prep 4 units of crossmatched packed red blood cells Prep 5 units of platelets, prep 10 units of FFP Continuous high-flow supplemental oxygen One or 2 large-bore IV lines with normal saline (NS) or lactated Ringer (LR) solution+10 units of oxytocin in 1 lit of ringer start at 2 drops/min add 2 drops every 15 min if fetal heart rate and uterine contractions are favorable. • perform amniotomy • Closely observe the patient. Monitor vital signs and urine output, fetal heart rate and uterine height measurement. • Prepare OR for emergent C/S • • •

Placenta Previa

subtypes • (1) complete or total: the placenta covers 360° of the internal cervical os; • (2) incomplete or partial: 0°-360° of the internal cervical os is covered by placental tissue; • (3) marginal: the placental tissue does not cover the internal cervical os; • (4) low lying: the edge of the placenta lies abnormally close to but does not abut the internal cervical os.

Risk factors prior placenta previa, prior cesarean delivery, increased maternal age, large placentae (eg, multiple gestations or erythroblastosis), • maternal history of smoking. • •

Frequency • 1 in 200 deliveries

Vaginal Bleeding • painless vaginal bleeding during the second half of pregnancy (70%). • It can occur without an inciting cause, although pelvic examination, intercourse, or labor may provoke it. • The average gestational age at presentation is 32 weeks. • Hemorrhage recurs, and, in nearly all cases, it is more severe the second time.

management • • • Patients are treated expectantly, with: volume replacement, transfusions, tocolytics, emergent cesarean delivery Without endangering the life of the mother, all attempts are made to delay delivery until the fetal lungs mature.

Preferred Examination • Physical examination should be performed only with a fetus that has achieved pulmonary maturity and only in a fully staffed operating room.

Preferred examination • TA sonography is the test of choice to confirm placenta previa. • When the internal cervical os cannot be visualized or when the results are inconclusive, transperineal or transvaginal sonography is recommended as an adjunct. • No increased risk of hemorrhage has been associated with transvaginal or transperineal sonography in this clinical setting.

Blood loss classifications
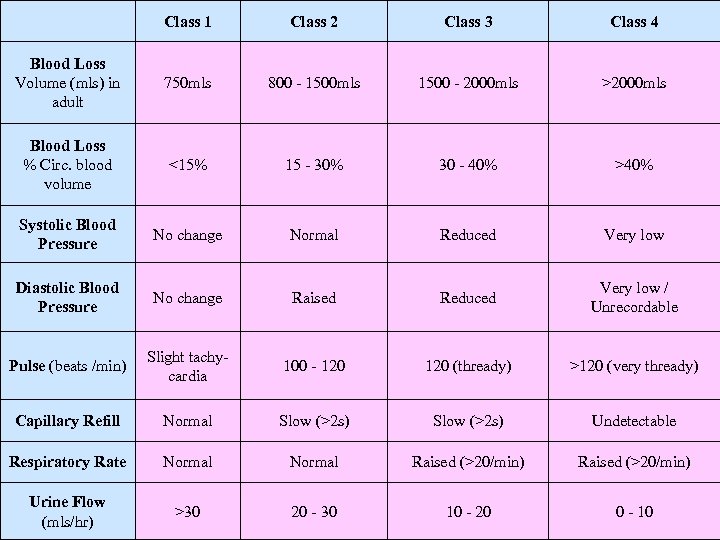
Class 1 Class 2 Class 3 Class 4 Blood Loss Volume (mls) in adult 750 mls 800 - 1500 mls 1500 - 2000 mls >2000 mls Blood Loss % Circ. blood volume <15% 15 - 30% 30 - 40% >40% Systolic Blood Pressure No change Normal Reduced Very low Diastolic Blood Pressure No change Raised Reduced Very low / Unrecordable Pulse (beats /min) Slight tachycardia 100 - 120 (thready) >120 (very thready) Capillary Refill Normal Slow (>2 s) Undetectable Respiratory Rate Normal Raised (>20/min) Urine Flow (mls/hr) >30 10 - 20 0 - 10 20 med-ed-online 2007 - 30
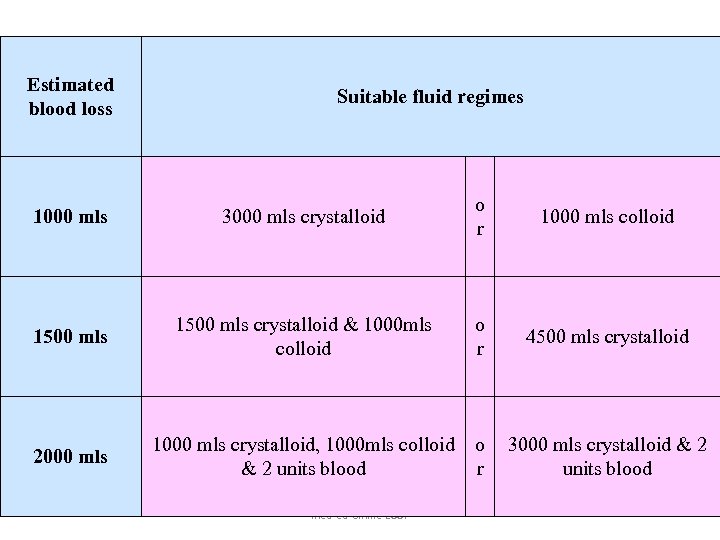
Estimated blood loss Suitable fluid regimes 1000 mls 3000 mls crystalloid o r 1000 mls colloid 1500 mls crystalloid & 1000 mls colloid o r 4500 mls crystalloid 2000 mls 1000 mls crystalloid, 1000 mls colloid & 2 units blood o r 3000 mls crystalloid & 2 units blood med-ed-online 2007

Multiple pregnancy Pictures and material of multiple pregnancy are adapted from: Zach T. multiple pregnancy. emedicine. Oct 2. 2007 with permission

pathophysiology 1 • Dizygotic twins(fraternal) are produced when 2 sperm fertilize 2 ova. Separate amnions, chorions, and placentas are formed in dizygotic twins. The placentas in dizygotic twins may fuse if the implantation sites are proximate. The fused placentas can be easily separated after birth. • Monozygotic twins (Identical)develop when a single fertilized ovum splits during the first 2 weeks after conception. An early splitting (ie, within the first 2 d after fertilization-30%) of monozygotic twins produces separate chorions and amnions. These dichorionic twins have different placentas that can be separate or fused.
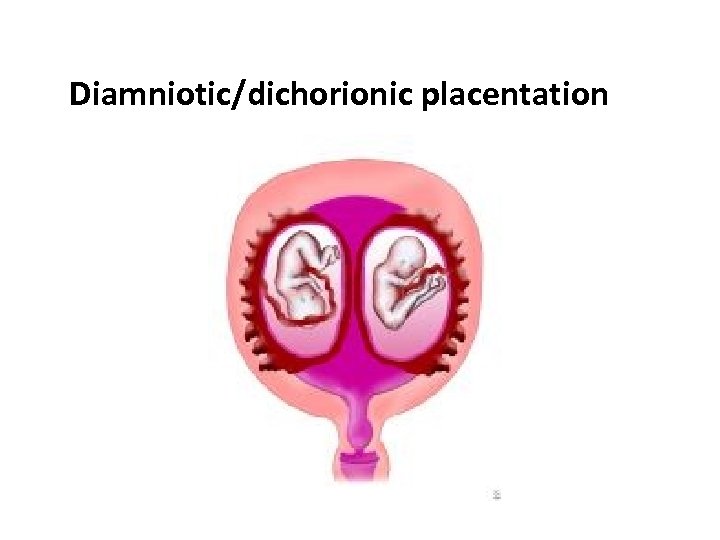
Diamniotic/dichorionic placentation

pathophysiology 2 • Later splitting (ie, 3 -8 d after fertilization) results in monochorionic/diamniotic placentation. • Approximately 70% of monozygotic twins are monochorionic/diamniotic.
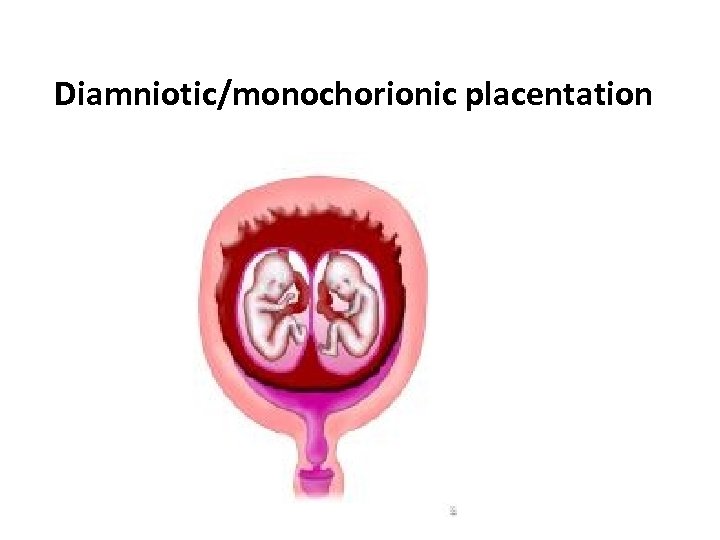
Diamniotic/monochorionic placentation

pathophysiology 3 • If splitting occurs even later (ie, during 9 -12 d after fertilization), monochorionic/monoamniotic placentation occurs. • Monochorionic/monoamniotic twins are rare; only 1% of monozygotic twins have this form of placentation.
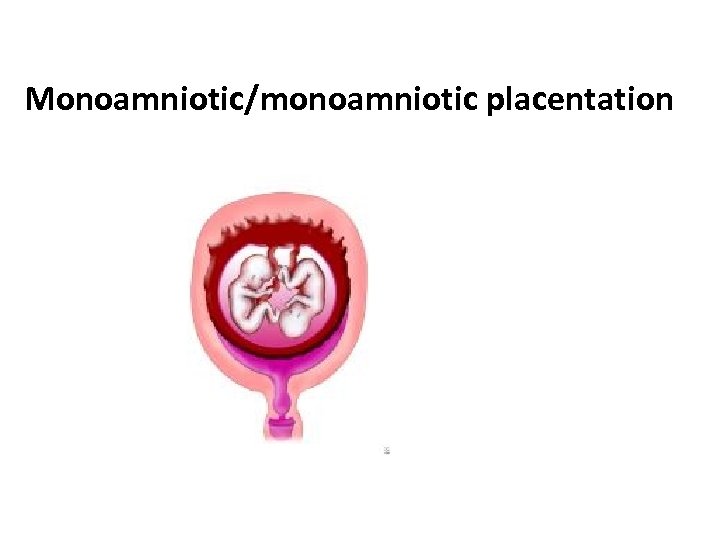
Monoamniotic/monoamniotic placentation

pathophysiology 4 • Monochorionic/monoamniotic twins have a common placenta with vascular communications between the 2 circulations.

pathophysiology 5 • Trizygotic triplets occur when 3 sperm fertilize 3 ova. • Dizygotic triplets develop from one set of monozygotic cotriplets and a third cotriplet derived from a different zygote. • Finally, 2 consecutive zygotic splittings with one split results in a vanished fetus and monozygotic triplets.

Frequency • The birth rate of monozygotic twins is constant worldwide (approximately 4 per 1000 births). • Birth rates of dizygotic twins vary by race. (Highest in Africans and lowerest in Asians)

mortality • low birth weight infants( due to prematurity and (IUGR) • congenital anomalies, • placenta previa, abruptio placenta, • preeclampsia, • cord accidents, • malpresentations, • asphyxia/perinatal depression, • group B streptococcal (GBS) infections, • hyaline membrane disease (HMD), • TTTS.

History • • • excessive weight gain, hyperemesis gravidarum, sensation of more than one moving fetus use of ovulation-inducing drugs family history of dizygotic twins

Neonatal Lab Studies • CBC count: In TTTS, the donor twin is frequently anemic at birth. The recipient twin is polycythemic at birth. • Calcium level: Hypocalcemia is common in premature infants, especially the donor twin in TTTS. • Glucose level: Hypoglycemia is common in premature infants, especially if TTTS is present. • Bilirubin level: Hyperbilirubinemia due to TTTS may develop in polycythemic infants.

TRAP • Twin reversed arterial perfusion (TRAP) sequence occurs when an acardiac twin receives all of the blood supply from the normal "pump" twin. This only occurs in monochorionic twins.

TTTS • Occurs in monochorionic/monoamniotic or monochorionic/diamniotic twins. Vascular anastomoses in the monochorionic placenta result in transfusion of blood from one twin (ie, donor) to the other twin (ie, recipient). Polyhydramnios develops in the sac of the recipient twin and oligohydramnios develops in the sac of the donor twin.

Conjoined twins – Incomplete late division of monozygotic twins produces conjoined twins. – Classification: • • • Thoracopagus - Joined at chest (40%) Xiphopagus/omphalopagus - Joined at abdomen (34%) Pygopagus - Joined at buttocks (18%) Ischiopagus - Joined at ischium (6%) Craniopagus - Joined at head (2%)

Discordant . Birth weight discrepancies of more than 20 -25% are considered discordant. Discordant birth weights occur in 10% of twins.

Gestational Trophoblastic Neoplasia

classification • hydatidiform mole : is the most common form of gestational trophoblastic neoplasia it can behave in a malignant or benign fashion, • invasive mole (chorioadenoma destruens), • choriocarcinoma, • and placental site trophoblastic tumor (PSTT).

Clinical course • In 80% of patients with a benign hydatidiform mole, serum HCG titers steadily drop to normal within 8 -12 weeks after evacuation of the molar pregnancy. • In the other 20% of patients with a malignant hydatidiform mole, serum HCG titers either rise or plateau.

staging • • Stage I – Confined to the uterus Stage II – Limited to the genital structures Stage III – Lung metastases Stage IV – Other metastases

WHO prognostic criteria 1 Age 40 years or older = 1 point Antecedent pregnancy terminated in abortion = 1 point Antecedent full-term pregnancy = 2 points Interval of 4 months to less than 7 months between antecedent pregnancy and start of chemotherapy = 1 point • Interval of 7 -12 months between antecedent pregnancy and start of chemotherapy = 2 points • Interval of more than 12 months between antecedent pregnancy and start of chemotherapy = 4 points • •

WHO prognostic criteria 2 • Beta-HCG level in serum is 1000 m. IU/m. L but less than 10, 000 m. IU/m. L = 1 point • Beta-HCG level in serum is 10, 000 m. IU/m. L but less than 100, 000 m. IU/m. L = 2 points • Beta-HCG level in serum is 100, 000 m. IU/m. L or greater = 4 points • Largest tumor is 3 cm but less than 5 cm = 1 point • Largest tumor is 5 cm or greater = 2 points • Site of metastases is spleen or kidney = 1 point

WHO prognostic criteria 3 • • Site of metastases is gastrointestinal tract = 2 points Site of metastases is brain or liver = 4 points Number of metastases is 1 -4 = 1 point Number of metastases is 5 -8 = 2 points Number of metastases is more than 8 = 4 points Prior chemotherapy with single drug = 2 points Prior chemotherapy with multiple drugs = 4 points

Sign and Symptoms • Patients with a hydatidiform mole present with signs and symptoms of pregnancy. – The most frequent symptom of gestational trophoblastic neoplasia (GTN) is abnormal uterine bleeding. – Patients have a history of amenorrhea. Occasionally, the typical hydatid vesicles (edematous villi) are passed through the vagina.

Sign and Symptoms • • Prolonged hyperemesis gravidarum preeclampsia Hyperthyroidism signs and symptoms associated with the metastatic disease, such as hematuria, hemoptysis, abdominal pain, and neurologic symptoms

Physical Exam • a positive pregnancy test result occurs in the absence of a fetus. • vesicles in the vagina is diagnostic • Enlarged ovaries secondary to theca lutein cysts are found in up to 20% of cases. – The cysts regress after evacuation of the hydatidiform mole for 12 weeks.

Cause • A hydatidiform mole occurs when a haploid sperm fertilizes an egg that has no maternal chromosomes and then duplicates its chromosomal complement. – Most complete hydatidiform moles are 46, XX, and all the chromosomes come from the male. – Of hydatidiform moles, 10 -15% are 46, XY. This occurs when 2 sperm, 1 carrying an X and the other carrying a Y, fertilize an "empty" egg. • Partial moles are 69, XXY, and 2 sets of chromosomes are of paternal origin.

Medical care 1 • • Emergency department care involves : starting intravenous (IV) fluids (crystalloids) sending blood for type and antibody screen Rh-negative patients should receive anti–Rh. D immune globulin, such as Rho. GAM, if not already immunized

Medical Care 2 • Patients with benign do not require medical therapy. • observing patients with weekly serum HCG titers. • Only patients with rising or plateauing titers should be treated with chemotherapy.

Medical care 3 • Patients with malignant nonmetastatic or metastatic lowrisk GTN are treated with single-agent chemotherapy like MTX or actinomycin D in patients with poor liver function • During treatment, the serum HCG titers are monitored every week. • One additional course of chemotherapy is administered after a normal serum HCG titer. • After 3 -4 normal serum HCG titers, the titers are followed once per month for 1 year. • A switch from MTX to actinomycin D is made if the patient receiving MTX for nonmetastatic or metastatic low-risk GTN develops rising or plateauing serum HCG titers.

Medical care 4 • Patients with high-risk metastatic are subdivided into 2 groups: – In patients with a WHO score of less than 8, a combination of MTX, actinomycin D, and cyclophosphamide can be used. This is known as the MAC regimen. This chemotherapeutic regimen is administered every 19 -21 days (from day 1 of the previous chemotherapy cycle) until the serum HCG titers normalize.

Medical Care 5 – Patients with WHO scores of 8 or higher are treated with a combination of etoposide, MTX, and actinomycin D administered in the first week of a 2 -week cycle and cyclophosphamide and vincristine (Oncovin) administered in the second week. This is known as the EMA-CO regimen. Two additional courses of EMA-CO or EMA-CE are administered after a normal serum HCG titer in very high-risk patients.
Medical care 6 – Patients with metastasis to the brain receive whole brain irradiation (3000 c. Gy) in combination with chemotherapy. Corticosteroids (Decadron) with systemic effect are administered to reduce brain edema. – Patients with liver metastasis are considered for liver irradiation (2000 c. Gy).

Surgical care • The treatment of a hydatidiform mole is evacuation of the uterus by suction and sharp curettage. – To avoid excessive bleeding, oxytocin is administered intravenously at the initiation of the suctioning of the uterine contents. – The largest possible suction curet is used, usually a 10 F or 12 F.

Further Care • Obtain follow-up serum HCG titers : • once per week until 3 -4 normal values are obtained. • Then, obtain them once per month for 6 months. • Have patients use reliable contraception, such as oral contraceptives or depot progesterone injections, during the period of follow-up care.

Prognosis 1 • Nonmetastatic GTN has a cure rate with chemotherapy of close to 100%. • Metastatic low-risk gestational trophoblastic neoplasia has a cure rate with chemotherapy of close to 100%. • Metastatic high-risk gestational trophoblastic neoplasia has a cure rate with chemotherapy of approximately 75%. • After 12 months of normal HCG titers, less than 1% of patients with malignant gestational trophoblastic neoplasia have recurrences.

Prognosis 2 • The rate of occurrence of a repeat molar pregnancy is approximately 1 -2%. • The rate of occurrence of a repeat molar pregnancy in a patient with a history of 2 previous hydatidiform moles is approximately 10 -20%. • The pregnancy rate after chemotherapy with MTX and cyclophosphamide is 80%. Of women treated with EMA-CO, 46% have had at least 1 live birth after chemotherapy. • Patients who become pregnant after treatment for GTN should have a pelvic ultrasound early during the pregnancy to confirm that the pregnancy is normal.

PREGNANT DIABETICS

ADAPTATION TO PREGNANCY • In early pregnancy Estrogen and Progesterone stimulate beta cell hyperplasia and increased insulin secretion • Glycogenolyis and peripheral utilization increase • The net result is relative hypoglycemia

GLUCOSE LEVELS IN NORMAL PREGNANCY • Fasting levels decline by 10 – 11 mg/dl • Postprandial levels rarely exceed 120 -140 mg/dl • Glucose excursions with meals 30 – 35 mg/dl • Marked increase in insulin levels with feeding

CHO METABOLISM 20 - 24 WEEKS • Increased human placental lactogen – diabetogenic • Increased prolactin – insulin resistance • Increased cortisol – decreased glycogen storage

OTHER METABOLIC CHANGES • Stable amounts of FFA • Increased cholesterol and TG • Reduced amino acid levels

MATERNAL COMPLICATIONS • • Retinopathy Nephropathy Chronic hypertension Preeclampsia

RETINOPATHY • Remains the leading cause of blindness in women ages 24 -64 • Every patient with pre-gestational diabetes should have a retinal examination in early pregnancy • Laser therapy is safe and effective during pregnancy • Has a variable course during pregnancy

NEPHROPATHY • Accounts for 1/3 of the deaths in diabetics < 31 • Renal findings are present as early as 1 -2 years after diagnosis • Creatinine clearance may improve in pregnancy due to increased renal blood flow • Proteinuria may increase substantially

CHRONIC RENAL FAILURE • Pregnancy is possible even in patients requiring hemodialysis • Reliable contraception is advised • Fertility and successful pregnancy outcomes are reduced with serum Cr > 2. 0

CHRONIC HYPERTENSION • Should be aggressively controlled • ACE inhibitors are contraindicated • Calcium channel blockers are probably a reasonable alternative and are safe during pregnancy • Increases the incidence of fetal growth restriction and superimposed preeclampsia

PREECLAMPSIA • BP > 140/90 • Proteinuria > 300 mg/24 hours or increase in baseline • May be difficult to diagnose in the presence of renal disease and chronic HTN • 25% incidence of superimposed disease with CHTN

SEVERE PREECLAMPSIA • • • BP > 180/110 Proteinuria > 5 g/24 hours Lab: elevated LFT’s. thrombocytopenia Sxs: headache, epigastric pain, blurred vision Oliguria, pulmonary edema, fetal growth restriction

PREGNANCY COMPLICATIONS • • • Hydramnios Spontaneous abortions Congenital malformations Macrosomia Diabetic ketoacidosis Neonatal metabolic complications

HYDRAMNIOS • 1 -2 % in normals and 18% of diabetics • Fetal osmotic diuresis is etiologic • May also be due to fetal cardiac CNS malformations • May be associated with preterm labor • ? Associated with level of glycemic control

SPONTANEOUS ABORTIONS • In well controlled patients the rate is similar to the non-diabetic • Glycosylated hemoglobin levels are higher in women who have a SAB • Higher rates of spontaneous abortion in diabetics with vascular disease

CONGENITAL MALFORMATIONS • Associated with periconceptual glucose control • In general the rate is 2 -3 x that of the nondiabetic gravida • No increase when the father is diabetic • “Fuel mediated teratogenesis”

TYPES OF CONGENITAL MALFORMATIONS • • Fetal cardiac anomalies may be complex CNS – Spina Bifida, Anencephaly Caudal regression syndrome Must consider family history of other malformations that are unrelated to DM

GLYCOSYLATED HGB AND MALFORMATIONS • HBA 1 C <8. 5% , 3. 4% malformations • HBA 1 C > 8. 5% , 22. 4 % malformations • Reflects glucose control over the preceeding 60 – 90 days

MACROSOMIA • Seen more frequently with GDM and IDDM without vascular complications • Related to level of 3 rd trimester glucose control • May occur in up to 25% of diabetics

DIABETIC KETOACIDOSIS • Seen in type I DM • Infection, fever, beta – agonists are frequent predisposing factors • Suspected with +serum ketones and blood glucose levels above 300 • Fetal distress is common

NEONATAL METABOLIC COMPLICATIONS • • • Hypoglycemia Hypocalcemia Hypothermia Hypomagnesemia Hyyperbilirubinemia

PRECONCEPTION COUNSELING • • “Tight” periconceptual control is essential The diabetes should be stable Multidisciplinary team maybe helpful Diabetic education Dietary counseling Assessment of renal function Retinal exam

PRECONCEPTION GLUCOSE CONTROL • • • Fasting blood glucose < 100 mg/dl Pre-meal levels <110 mg/dl Post-meal levels <140 – 150 mg/dl Avoid wide swings in control Normalize hemoglobin A 1 C

PREVENTION OF MALFORMATIONS • Normal glucose levels • Folic acid supplementation • Dose: 4 mg/day from 1 month pre-pregnancy to 12 weeks

FOLIC ACID • All women of reproductive age should consume at least 0. 4 mg of folic acid • High risk women should consume 4 mg/day • This reduces the risk of neural tube defects • Newer evidence suggests a lower risk of facial clefting and congenital heart disease as well

INDICATIONS FOR HOSPITALIZATION • • • Persistent nausea and vomiting Significant maternal infection DKA Poor control/compliance Preterm labor

ASSESSMENT OF FETAL WELL-BEING • Daily fetal movement counting • Twice weekly NST by 32 weeks • At least weekly assessment of AFV OR • Weekly biophysical profiles • With more advanced disease, earlier testing is recommended

FIRST PRENATAL VISIT • Routine prenatal lab • Baseline 24 hour UA for protein and Cr Clearance • Baseline retinal exam • EKG • Thyroid function tests in Type 1 Diabetics • Hemoglobin A 1 C • Schedule 10 -12 week USN

EARLY PREGNANCY CARE Diabetic education and dietary instruction Multi-disciplinary care is helpful Calibrate reflectance meters Adjust caloric needs for pregnancy and lactation • Review benefits of physical activity • •

TIMING OF DELIVERY • Well controlled IDDM: at term • Poorly controlled: after documentation of fetal lung maturity • If fetal surveillance reassuring, delivery before 39 weeks should be unusual

INTRAPARTUM GLUCOSE CONTROL • No breakfast the morning of induction • Establish IV with D 5/. 45% Na. Cl at 125 cc/hour • Capillary blood glucose levels every 1 – 2 hours • Begin continuous infusion of insulin with levels above 120 mg/dl • Avoid fluid boluses with D 5
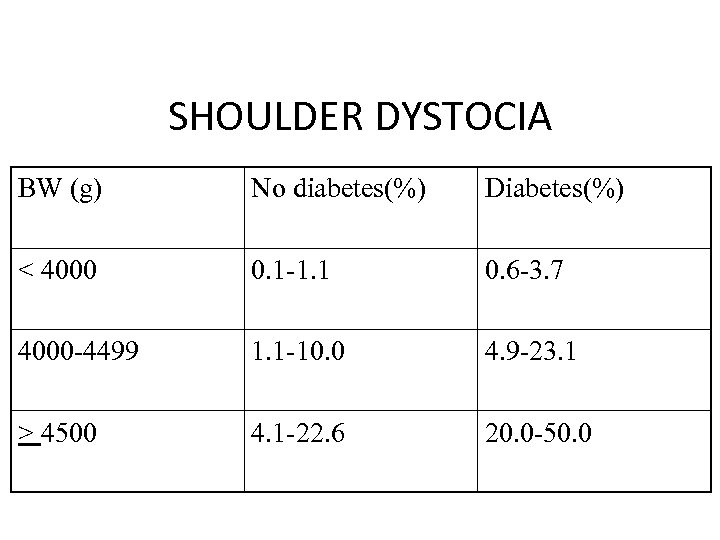
SHOULDER DYSTOCIA BW (g) No diabetes(%) Diabetes(%) < 4000 0. 1 -1. 1 0. 6 -3. 7 4000 -4499 1. 1 -10. 0 4. 9 -23. 1 > 4500 4. 1 -22. 6 20. 0 -50. 0

NERVE INJURY • Rate varies from 4 -40% following shoulder dystocia • Most (90%) resolve without sequelae • Can occur with EFW < 4000 g • Can occur in utero and therefore not preventable by cesarean

POSTPARTUM GLUCOSE CONTROL • Insulin requirements may fall 50% in the 1 st 24 hours • Little need for treatment if under 200 mg/dl

CONTRACEPTION • Reliable contraception should be offered • Low-dose combination OCP’s do not significantly impair carbohydrate metabolism • Progestin only oral contraceptives appear to accelerate the development of Type 2 DM in women with gestational diabetes • Barrier methods and even IUD may be acceptable

ACOG Low Risk • Age < 25 • Not a member of an at risk ethnic group (Hispanic, African, Native American, South or East Asian, Pacific Islanders) • BMI < 25 (non-obese) • No history of abnormal glucose tolerance or FH • No adverse outcomes

Screening • If FBS is 110 -126: • Then 1 hr 50 gr or 3 hrs 100 gr • remember 105– 195— 165 ---145

Summary • Every practice should adopt a screening strategy, either by historical or laboratory means • Screening best between 24 -28 weeks • Remember to screen post delivery

Some diabetic cases

Bita Hazrati A PLP case complicated by HTN and GD • 24 yrs old • G 2 P 1 L 0 D 1/ first fetal loss due to preterm c/s delivery • ( because of placenta previa) • GA on admission 32 -33 w • CC: LP ( contractions mild/20 seconds D/ 2 in a • 10 - minute interval) • WB: Intact • ROM: - ( detected by Fern test) • Reduced fetal movement: -

• Ph E: PR= 86/min RR: 16/min T: 36 BP= 140/90 mm. Hg • BS: FBS=112 /10 am=134 /4 pm=145 /8 pm=163

20 -30 units total : 2/3 intermediate 1/3 regular Morning: 10 units of NPH- 4 units of regular Afternoon: 4 units of NPH – 4 units of regular

FBS is used to adjust evening NPH 2 -hr PP (10 am) is used to adjust morning Regular Afternon preprandial (4 pm) is used to adjust morning NPH 2 hr PP is used to adjust evening Regular

What is your management of this combined case of : 1 - preeclampsia 2 - GD 3 - PLP

Answer: Mg so 4 Ampicillin+ Erythro Isoxsuprine Sedation FBS-BS NST-FAD-OB US (AFI and GA) Insulin

Which is true about gestational diabetes? A-This happens during pregnancy with FBS less than 105 mg/dl. Its treatment is insulin. B-It is a kind of type 2 diabetes. C- All cases will develop overt diabetes within 20 years. D- It happens because of reduced pancreas b cell function. Ans: B

Which is an independent cause of IUFD in diabetes? A-hydramnios B-abruptio C-oligohydramnios D-oxygen and metabolites transportation Ans: D

Which is not a good method of contraception in a diabetic woman? A-LD OCP B-medroxy progesterone acetate C- HD OCP D-norplant Ans: C

What is the test for a 30 year old 10 wk pregnant woman whose FBS is 85/ 2 hr PP is 125? A- 3 hr GTT B-Repeat of FBS and 2 hr PP next week. C-Repeat of FBS and 2 hr PP in 24 -28 wk. D-Repeat of FBS and 2 hr PP in 34 wk. Ans: C

Which is not a cause of PIH for a diabetic pregnant woman? A-poor blood glucose control B-albuminurea C-high creatinine D-chronic HTN Ans: A

What is the most common cause of perinatal mortality in diabetic pregnancies? A- malformations B- RDS C-metabolic errors D- IUFD Ans: A

What is one stage screening test for diabetes in pregnancy? A-100 grs oral glucose in 24 -28 wk. B-50 grs oral glucose in 20 -22 wk. C-75 grs oral glucose in 18 -20 wk. D-25 grs oral glucose in 30 -32 wk. Ans: A

What is your plan for a 35 wk diabetic pregnant woman whose BP is 140/90 mm. Hg/ is on 60 units of insulin /FBS=120 mg/dl? A-increasing the insulin dose B- no treatment C-hospitalization and adjusting insulin dose D-termination of pregnancy Ans: C

What is your management of a 30 yr old 35 wk pregnant woman class R diabetic with severe retinopathy? A-termination of pregnancy B-Laser photocoagulation C- high dose steroids D-No action is needed now. Ans: B

Which is not among the complications of type A 2 diabetes in pregnancy? A- macrosomia B-increased C/S C- still birth D-malformations Ans: D

A woman with a history of gestation diabetes is asking for follow-up management after her delivery. Her FBS is 108 mg/dl and 2 hr PP 135 mg/dl. What do you suggest? A-repeat of FBS and 2 hr PP a year after delivery. B- repeat of FBS and 2 hr PP 3 yrs after delivery. C-GTT with 100 grs glucose. D-Hb. A 1 C 6 months after delivery. Ans: B

In a woman with overt diabetes , BS is reported to be 130 mg/dl. What do you suggest for her IV infusion? A- RL and DW 5% B-RL and DW 5% +insulin 1 unit/hr C-NS +insulin 1. 5 units/hr D- NS+insulin 2 units/hr Ans: B

Points to remember about diabetic labor: • • • BS below 100 mg/dl : no insulin is needed 100 -140 mg/dl: 1 unit insulin 140 -180 mg/dl: 1. 5 units insulin 180 -220 mg/dl: 2 units insulin More than 220 mg/dl: 2. 5 units insulin • BS more than 140 mg/dl needs NS as IV infusion
e4da3705e78c8fe86b9920fc487ac8fc.ppt