aca397f31a9ff33e34739a266c8b558b.ppt
- Количество слайдов: 62
 Improving the Quality of Clinical Preceptors Practical Applications for Bench Teaching Donald D. Simpson, Ph. D. , M. P. H. , CT(ASCP)CM University of Arkansas for Medical Sciences Little Rock, AR 24 February 2011
Improving the Quality of Clinical Preceptors Practical Applications for Bench Teaching Donald D. Simpson, Ph. D. , M. P. H. , CT(ASCP)CM University of Arkansas for Medical Sciences Little Rock, AR 24 February 2011
 Don Simpson simpsondonald@uams. edu (501) 686 -5776
Don Simpson simpsondonald@uams. edu (501) 686 -5776
 “My method (is) to lead my students by hand to the practice of medicine, taking them every day to see patients in the public hospital, that they may hear the patients' symptoms and see their physical findings. Then I question the students as to what they have noted in the patients and about their thoughts and perceptions regarding the cause of the illness and the principles of treatment” Dr. Franciscus de la Boe Sylvius, 17 th century professor of medicine at the University of Leyden, Netherlands
“My method (is) to lead my students by hand to the practice of medicine, taking them every day to see patients in the public hospital, that they may hear the patients' symptoms and see their physical findings. Then I question the students as to what they have noted in the patients and about their thoughts and perceptions regarding the cause of the illness and the principles of treatment” Dr. Franciscus de la Boe Sylvius, 17 th century professor of medicine at the University of Leyden, Netherlands
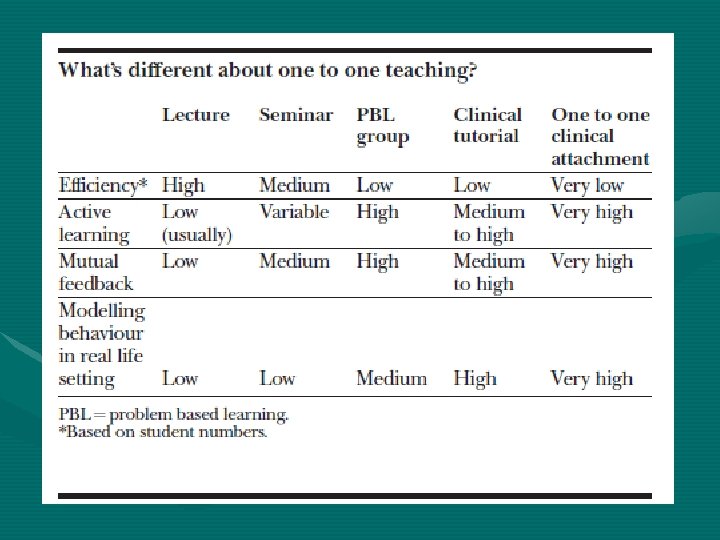
 What “Makes” An Effective Teacher
What “Makes” An Effective Teacher
 Effective Teachers. . . • Demonstrates respect for the learner • Challenges the learner to think • Encourages learners to focus on things they can use immediately, practice and take responsibility • Know the difference between “Gremlins” and “Gnomes”
Effective Teachers. . . • Demonstrates respect for the learner • Challenges the learner to think • Encourages learners to focus on things they can use immediately, practice and take responsibility • Know the difference between “Gremlins” and “Gnomes”
 G. N. O. M. E. • • • G – goals (often silent) N – needs (learner’s deficit in relation to goals) O – objectives (‘E’ in GNOME informs about ‘O’) M – methods (must be compatible with objectives) E – evaluation (feedback and judgment)
G. N. O. M. E. • • • G – goals (often silent) N – needs (learner’s deficit in relation to goals) O – objectives (‘E’ in GNOME informs about ‘O’) M – methods (must be compatible with objectives) E – evaluation (feedback and judgment)
 Rationale
Rationale
 What is your teaching mission statement? Example: “I intend to teach the learner the differential diagnoses (in my content area) from clinical cases, such that they can demonstrate this reasoning strategy when seeing patients in the clinic” Relatively short; easily communicated; memorable; and frequently revisited “The unexamined life is not worth living” - Socrates
What is your teaching mission statement? Example: “I intend to teach the learner the differential diagnoses (in my content area) from clinical cases, such that they can demonstrate this reasoning strategy when seeing patients in the clinic” Relatively short; easily communicated; memorable; and frequently revisited “The unexamined life is not worth living” - Socrates
 Habits are Habit-Forming
Habits are Habit-Forming
 Training MY Replacement Eager
Training MY Replacement Eager
 Workforce Shortage § 43% of laboratories report difficulties hiring personnel § Median age = 48 years § Shortage will exacerbate as baby boomers retire and more people utilize the health care system § ~25% of workforce (73, 000 ) will retire in next 10 years § Only 2 laboratorians enter the field for every 7 that retire
Workforce Shortage § 43% of laboratories report difficulties hiring personnel § Median age = 48 years § Shortage will exacerbate as baby boomers retire and more people utilize the health care system § ~25% of workforce (73, 000 ) will retire in next 10 years § Only 2 laboratorians enter the field for every 7 that retire
 National Outlook • BLS projects 13, 700 new Medical Laboratory professionals will be needed per year • CLS/CLT employment is expected to grow by 14% by 2016, which is faster than the average for all occupations – The number of openings is expected to continue to exceed the number of job seekers – Most jobs will continue to be in hospitals, but employment will grow faster in other settings (medical and diagnostic laboratories, offices of physicians, and all other ambulatory health care services) * data from the Bureau of Labor Statistics
National Outlook • BLS projects 13, 700 new Medical Laboratory professionals will be needed per year • CLS/CLT employment is expected to grow by 14% by 2016, which is faster than the average for all occupations – The number of openings is expected to continue to exceed the number of job seekers – Most jobs will continue to be in hospitals, but employment will grow faster in other settings (medical and diagnostic laboratories, offices of physicians, and all other ambulatory health care services) * data from the Bureau of Labor Statistics
 Graduate Shortfall In 2005 National Accrediting Agency for Clinical Laboratory Science (NAACLS) summarized: # graduates needed/yr = 13, 700* # graduating/yr = 4, 445 yearly shortfall = 9, 200 * data from the Bureau of Labor Statistics
Graduate Shortfall In 2005 National Accrediting Agency for Clinical Laboratory Science (NAACLS) summarized: # graduates needed/yr = 13, 700* # graduating/yr = 4, 445 yearly shortfall = 9, 200 * data from the Bureau of Labor Statistics
 Cost to Train a CLS Student • Student rotations are 19 – 26 weeks • On average there is a 50% productivity impact for the trainer in a hospital setting. • Assuming a CLS salary for trainer = $50, 000 • Other miscellaneous costs may be minimal
Cost to Train a CLS Student • Student rotations are 19 – 26 weeks • On average there is a 50% productivity impact for the trainer in a hospital setting. • Assuming a CLS salary for trainer = $50, 000 • Other miscellaneous costs may be minimal
 Clinical Rotation Cost to Educate a CLS Student • Hospital Setting Cost Analysis: – Train for 26 weeks or 1/2 year = 0. 5 FTE – 0. 5 FTE @ 50% productivity loss = 0. 25 FTE in dedicated training time – 0. 25 FTE x $50, 000 = $12, 500 to train CLS student
Clinical Rotation Cost to Educate a CLS Student • Hospital Setting Cost Analysis: – Train for 26 weeks or 1/2 year = 0. 5 FTE – 0. 5 FTE @ 50% productivity loss = 0. 25 FTE in dedicated training time – 0. 25 FTE x $50, 000 = $12, 500 to train CLS student
 Cost to Recruit New Employee • Most HR departments factor 1 to 1. 5 times the employee’s annual salary • This includes direct and indirect costs for: – – – Processing the termination, payout of benefits Review and authorization to replace vacated position Job posting and advertising Interviews Processing the hired applicant (Health Service and screening) – Orientation and Training • Assuming an annual salary of $50, 000, replacement cost will range from $50, 000 – 75, 000 SHRM Metrics Staffing Report http: //www. shrm. org/metrics/library/
Cost to Recruit New Employee • Most HR departments factor 1 to 1. 5 times the employee’s annual salary • This includes direct and indirect costs for: – – – Processing the termination, payout of benefits Review and authorization to replace vacated position Job posting and advertising Interviews Processing the hired applicant (Health Service and screening) – Orientation and Training • Assuming an annual salary of $50, 000, replacement cost will range from $50, 000 – 75, 000 SHRM Metrics Staffing Report http: //www. shrm. org/metrics/library/
 Math Matters • Assumptions: – Training CLS student for complete internship – Using internship of about 19 - 26 weeks – Using conservative estimate of 1 year salary to replace • Break-even point is to hire 1 student for every 4 trained ! ! !
Math Matters • Assumptions: – Training CLS student for complete internship – Using internship of about 19 - 26 weeks – Using conservative estimate of 1 year salary to replace • Break-even point is to hire 1 student for every 4 trained ! ! !
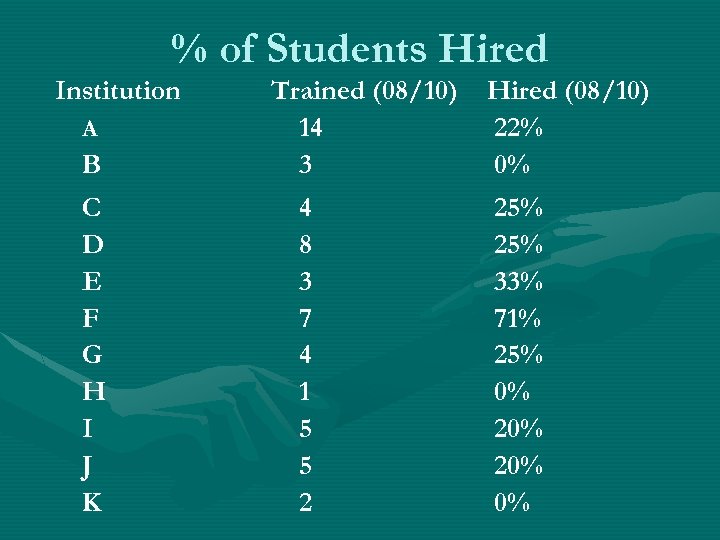 % of Students Hired Institution A B C D E F G H I J K Trained (08/10) 14 3 4 8 3 7 4 1 5 5 2 Hired (08/10) 22% 0% 25% 33% 71% 25% 0% 20% 0%
% of Students Hired Institution A B C D E F G H I J K Trained (08/10) 14 3 4 8 3 7 4 1 5 5 2 Hired (08/10) 22% 0% 25% 33% 71% 25% 0% 20% 0%
 Cost to Train Non-traditional path Employee to be Eligible for Certification • Minimum 4 months of training for one clinical area • Total of 1 year training for a CLS Generalist equivalent • Productivity loss is much higher due to lack of educational background (75%) • 1 FTE x $50, 000 x. 75 = $37, 500 to train 1 new employee – Plus salary cost of that individual - $35, 000 – Total = $72, 500
Cost to Train Non-traditional path Employee to be Eligible for Certification • Minimum 4 months of training for one clinical area • Total of 1 year training for a CLS Generalist equivalent • Productivity loss is much higher due to lack of educational background (75%) • 1 FTE x $50, 000 x. 75 = $37, 500 to train 1 new employee – Plus salary cost of that individual - $35, 000 – Total = $72, 500
 Value to Employer • Having students helps keep procedures up to date and easy to follow • Patient safety • Keeps existing employees “sharp” on their skills, knowledge, and behaviors – – – Follow and explain procedures Utilize best practice or standard work practices Model proper behaviors for customer service, etc. • Ability to “pre-screen” before hiring (i. e. , 4 – 5 month interview period
Value to Employer • Having students helps keep procedures up to date and easy to follow • Patient safety • Keeps existing employees “sharp” on their skills, knowledge, and behaviors – – – Follow and explain procedures Utilize best practice or standard work practices Model proper behaviors for customer service, etc. • Ability to “pre-screen” before hiring (i. e. , 4 – 5 month interview period
 Value to Employer • “Many of our students stay on and become valuable employees” • “They may one day become employees in our facility and by training the students we are retraining ourselves and learning along with them” • “We were all students at one point in our careers and we want the students to become good practitioners who will care for us some day”
Value to Employer • “Many of our students stay on and become valuable employees” • “They may one day become employees in our facility and by training the students we are retraining ourselves and learning along with them” • “We were all students at one point in our careers and we want the students to become good practitioners who will care for us some day”
 The Challenge Consider the value to your organization to provide additional clinical laboratory rotation opportunities
The Challenge Consider the value to your organization to provide additional clinical laboratory rotation opportunities
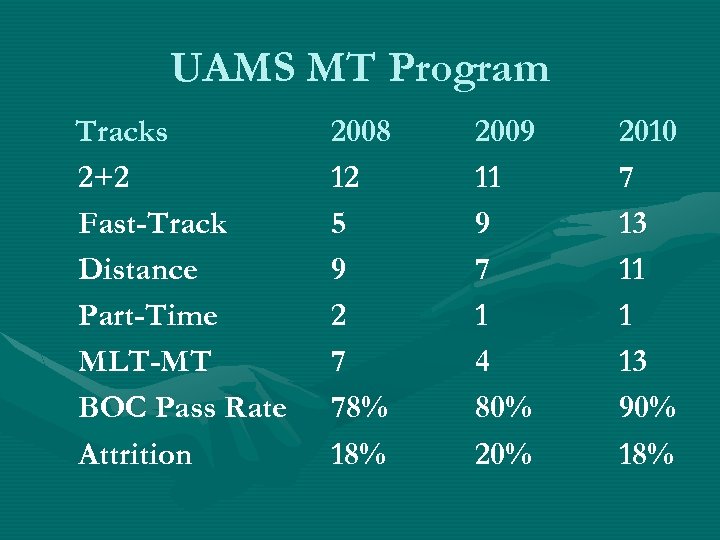 UAMS MT Program Tracks 2+2 Fast-Track Distance Part-Time MLT-MT BOC Pass Rate Attrition 2008 12 5 9 2 7 78% 18% 2009 11 9 7 1 4 80% 2010 7 13 11 1 13 90% 18%
UAMS MT Program Tracks 2+2 Fast-Track Distance Part-Time MLT-MT BOC Pass Rate Attrition 2008 12 5 9 2 7 78% 18% 2009 11 9 7 1 4 80% 2010 7 13 11 1 13 90% 18%
 Methodology
Methodology
 The Five P’s of Effective Teaching • Preparation • Perceptions • Professionalism • Presentation • Participation
The Five P’s of Effective Teaching • Preparation • Perceptions • Professionalism • Presentation • Participation
 Preparation • Determine the need of students • Integrate previous learning into present lesson • Determine the educational level of the students • Assemble teaching accessories
Preparation • Determine the need of students • Integrate previous learning into present lesson • Determine the educational level of the students • Assemble teaching accessories
 Perceptions • • Student and preceptor Integration of one’s ideas during teaching Positively reinforce the practice of medicine Attitudes are easily conveyed
Perceptions • • Student and preceptor Integration of one’s ideas during teaching Positively reinforce the practice of medicine Attitudes are easily conveyed
 Professionalism • Appearance (clean lab coat) • Demeanor – Polite without being overly friendly • Preceptor is addressed as Dr. , Ms. , etc. • Know students name
Professionalism • Appearance (clean lab coat) • Demeanor – Polite without being overly friendly • Preceptor is addressed as Dr. , Ms. , etc. • Know students name
 Presentation • • Competing student interest and material Focus on student attention Positive learning environment Three points (presented at first meeting): – What you are going to do – How you are going to do it – What the students are expected to do
Presentation • • Competing student interest and material Focus on student attention Positive learning environment Three points (presented at first meeting): – What you are going to do – How you are going to do it – What the students are expected to do
 Participation • • • Bilateral participation Eye contact Questions=feedback Questions=fact finding mission Orient learners to lesson Review past material Reflect on learning OK to say “I don’t know” Give feedback to learners often Praise is important to the group and individual
Participation • • • Bilateral participation Eye contact Questions=feedback Questions=fact finding mission Orient learners to lesson Review past material Reflect on learning OK to say “I don’t know” Give feedback to learners often Praise is important to the group and individual
 Conclusion • Reflect on the five P’s and make adjustments for the next teaching experience – Prepare early – Discuss your perceptions – Be professional – Design your presentation – Allow bilateral participation
Conclusion • Reflect on the five P’s and make adjustments for the next teaching experience – Prepare early – Discuss your perceptions – Be professional – Design your presentation – Allow bilateral participation
 Teaching in the Clinical Setting In-depth Lectures Seminars Formal Educational Sessions Extensive Discussion
Teaching in the Clinical Setting In-depth Lectures Seminars Formal Educational Sessions Extensive Discussion
 Efficient and effective bench teaching requires that both the student and preceptor accept the limitations of the setting Example: in an outpatient ambulatory care setting extensive discussions of differential diagnoses, pathophysiology and psychosocial problems are not possible nor necessarily desirable
Efficient and effective bench teaching requires that both the student and preceptor accept the limitations of the setting Example: in an outpatient ambulatory care setting extensive discussions of differential diagnoses, pathophysiology and psychosocial problems are not possible nor necessarily desirable
 • • • Demonstrate enthusiasm Give meaningful (“authentic”) responsibility Possess credible clinical skills
• • • Demonstrate enthusiasm Give meaningful (“authentic”) responsibility Possess credible clinical skills
 Pitfalls in clinical case-based teaching • “Taking over” the case • Inappropriate lectures • Insufficient “wait-time” - 3 – 5 second wait to answer your questions • Pre-programmed answers - What do you think is going on? Could it be an ulcer?
Pitfalls in clinical case-based teaching • “Taking over” the case • Inappropriate lectures • Insufficient “wait-time” - 3 – 5 second wait to answer your questions • Pre-programmed answers - What do you think is going on? Could it be an ulcer?
 Pitfalls continued… • Rapid reward - Effectively ends the student’s thinking process • Pushing past ability - Persisting in carrying the students beyond their understanding of what is being asked
Pitfalls continued… • Rapid reward - Effectively ends the student’s thinking process • Pushing past ability - Persisting in carrying the students beyond their understanding of what is being asked
 The “One-Minute Preceptor” 1. Get a commitment 2. Probe for supporting evidence 3. Tell them what they did right 4. Teach general rules - Take each encounter to a learning point 5. Provide feedback (correct errors) A. Positive B. Corrective
The “One-Minute Preceptor” 1. Get a commitment 2. Probe for supporting evidence 3. Tell them what they did right 4. Teach general rules - Take each encounter to a learning point 5. Provide feedback (correct errors) A. Positive B. Corrective
 “One-Minute Preceptor” Microskills • Get commitment (Assess ) • • – “What do you think is going on? ” Probe for rationale (Assess ) – “What led you to that conclusion? ” Reinforce what was correct (Feedback ) – “You did an excellent job of…” Teach general rules (Instruct ) – “When this happens, do this…” Correct mistakes (Feedback ) – “Next time this happens, try this…”
“One-Minute Preceptor” Microskills • Get commitment (Assess ) • • – “What do you think is going on? ” Probe for rationale (Assess ) – “What led you to that conclusion? ” Reinforce what was correct (Feedback ) – “You did an excellent job of…” Teach general rules (Instruct ) – “When this happens, do this…” Correct mistakes (Feedback ) – “Next time this happens, try this…”
 “One-Minute Preceptor” Quiz 1. Get a ____________ 2. Probe for __________ 3. Tell them __________ 4. ______ general rules 5. _______ errors
“One-Minute Preceptor” Quiz 1. Get a ____________ 2. Probe for __________ 3. Tell them __________ 4. ______ general rules 5. _______ errors
 “Trainees do not perform required skills incorrectly on purpose…errors in performance are typically the result of insufficient feedback” “They (errors) are seldom the result of insufficient interest or caring” Microskills of the One-Minute Preceptor (W. Fred Miser, M. D. )
“Trainees do not perform required skills incorrectly on purpose…errors in performance are typically the result of insufficient feedback” “They (errors) are seldom the result of insufficient interest or caring” Microskills of the One-Minute Preceptor (W. Fred Miser, M. D. )
 Q: Information you provide to learners about their clinical performance that is intended to guide their future clinical performance A: What is feedback
Q: Information you provide to learners about their clinical performance that is intended to guide their future clinical performance A: What is feedback
 The Feedback Sandwich What was done “right” What needs improvement What to do next time
The Feedback Sandwich What was done “right” What needs improvement What to do next time
 Feedback Checklist Make sure learner is ready Give it soon and often Link to goals Be specific & non-judgmental Give positive and constructive comments Suggest correct performance Don’t give too much Make sure feedback is understood Follow up your feedback Expect learners to develop skills in self-evaluation
Feedback Checklist Make sure learner is ready Give it soon and often Link to goals Be specific & non-judgmental Give positive and constructive comments Suggest correct performance Don’t give too much Make sure feedback is understood Follow up your feedback Expect learners to develop skills in self-evaluation
 Case Study UAMS Example
Case Study UAMS Example
 Advantages to Serving as Clinical Internship Site • • Source of potential employees Keeps staff current on theory Reputation of facility Increase job satisfaction and self esteem of staff • Professional responsibility
Advantages to Serving as Clinical Internship Site • • Source of potential employees Keeps staff current on theory Reputation of facility Increase job satisfaction and self esteem of staff • Professional responsibility
 Disadvantages • Use more supplies • Increase in daily duties – Already overworked professionals • Staff resistance – not all are teachers
Disadvantages • Use more supplies • Increase in daily duties – Already overworked professionals • Staff resistance – not all are teachers
 Making Internships Successful • • • Make students feel welcome Reassure students as they progress Keep the roles of instructor and student well defined • Selector instructors who have patience, positive attitude, and want to teach • An Orientation on the first day – – – Cover safety regulations Lab/hospital regulations Dress code Expectations Exam dates Introduction to staff
Making Internships Successful • • • Make students feel welcome Reassure students as they progress Keep the roles of instructor and student well defined • Selector instructors who have patience, positive attitude, and want to teach • An Orientation on the first day – – – Cover safety regulations Lab/hospital regulations Dress code Expectations Exam dates Introduction to staff
 CLS/MT Program will Provide • Support to clinical rotation site • Student internship manual – Evaluation forms – Learning Objective – Complete with study questions for each discipline and answer keys – List of Required tests • Exams
CLS/MT Program will Provide • Support to clinical rotation site • Student internship manual – Evaluation forms – Learning Objective – Complete with study questions for each discipline and answer keys – List of Required tests • Exams
 Schedules & Expectations • Provide each site with a schedule template to help schedule weekly activities for student • Date of departmental practical exam – This should be established by teaching tech • Dates for internship exams
Schedules & Expectations • Provide each site with a schedule template to help schedule weekly activities for student • Date of departmental practical exam – This should be established by teaching tech • Dates for internship exams
 Grades for Each Course • Needed from clinical rotation – Practical exam – be consistent for each student • Practical exam – Use controls, patient samples – Save/freeze serum with interesting results – Can use photos, CD images, etc… • UAMS faculty – May need to support preceptors in the design of practical exams
Grades for Each Course • Needed from clinical rotation – Practical exam – be consistent for each student • Practical exam – Use controls, patient samples – Save/freeze serum with interesting results – Can use photos, CD images, etc… • UAMS faculty – May need to support preceptors in the design of practical exams
 Practical Exam • • Objectively assess a technical performance Use worksheets Students should interpret and assess Can grade on oral responses or observations
Practical Exam • • Objectively assess a technical performance Use worksheets Students should interpret and assess Can grade on oral responses or observations
 Practical Exam. . . continued • Example of Course Grade – Exam for the department – Laboratory practicals – Performance evaluation = 30% = 45% = 25% • Be sure to review evaluation with each student and have them sign all forms (feedback and DOCUMENTATION)
Practical Exam. . . continued • Example of Course Grade – Exam for the department – Laboratory practicals – Performance evaluation = 30% = 45% = 25% • Be sure to review evaluation with each student and have them sign all forms (feedback and DOCUMENTATION)
 Students Like • • • Helpful, enthusiastic and pleasant techs When their questions are well received When they are treated with respect They receive praise when they do well When they need help, receive patient and kind guidance
Students Like • • • Helpful, enthusiastic and pleasant techs When their questions are well received When they are treated with respect They receive praise when they do well When they need help, receive patient and kind guidance
 What Students DO NOT Like • • • Being called “the Student” Having nothing to do Reading procedure manuals for extended periods Being left alone in an area Not knowing expectations Inconsistency with procedures
What Students DO NOT Like • • • Being called “the Student” Having nothing to do Reading procedure manuals for extended periods Being left alone in an area Not knowing expectations Inconsistency with procedures
 Bench Teaching • Teach concepts, problems solving and principles along with specific procedures • Encourage student to carry a small notebook to jot things down • Demo a test and then let a student perform the test using a manual and you watch • Principle of test is very important and necessary for trouble shooting • Students learn basic procedures on campus, but we cannot simulate a real lab environment • Be consistent
Bench Teaching • Teach concepts, problems solving and principles along with specific procedures • Encourage student to carry a small notebook to jot things down • Demo a test and then let a student perform the test using a manual and you watch • Principle of test is very important and necessary for trouble shooting • Students learn basic procedures on campus, but we cannot simulate a real lab environment • Be consistent
 Bench Teaching • Keep students informed of progress • Teaching a new procedure – Demo, go slowly repeat and emphasize key points – Read procedure including principle – Watch student perform the new test – Check results • Students performs work independently
Bench Teaching • Keep students informed of progress • Teaching a new procedure – Demo, go slowly repeat and emphasize key points – Read procedure including principle – Watch student perform the new test – Check results • Students performs work independently
 Students NEED to Perform Test • We Remember – 20% of what we hear – 30% of what we see – 50% of what we see and hear – 70% of what we participate in or say – 90% of what we say and do – Learning has not occurred unless learners change their behavior as a result of what we do
Students NEED to Perform Test • We Remember – 20% of what we hear – 30% of what we see – 50% of what we see and hear – 70% of what we participate in or say – 90% of what we say and do – Learning has not occurred unless learners change their behavior as a result of what we do
 Students Doing Patient Work? • • When (completed rotation and passed) If (there is time; after teaching) You must be comfortable with decision Does not need to be the same for each student • Verify results
Students Doing Patient Work? • • When (completed rotation and passed) If (there is time; after teaching) You must be comfortable with decision Does not need to be the same for each student • Verify results
 If Problems Arise • • • Questions we can’t answer Work with supervisor for minor problems Unresolved problems contact the Department of Laboratory Sciences
If Problems Arise • • • Questions we can’t answer Work with supervisor for minor problems Unresolved problems contact the Department of Laboratory Sciences
 References: • Bennett, A. , Thompson, N. , Holladay, B. , Bugbee, A. , & Steward. ASCP wage and vacancy survey of U. S. medical laboratories. 2009 • Passiment, K. Update on the laboratory workforce-shortage crisis. Washington Report. March: 2006; www. mlo-online. com • Irby, D. How attending physicians make instructional decisions when conducting teaching rounds. Academic Medicine , 1992; 67(10): 630 -638 • Gordon, J. ABC of learning and teaching in medicine: One-to-one teaching and feedback. British Medical Journal, 2003; 326: 543 -545 Acknowledgements: • Mark Quirk, Ed. D. • Tatum Langford Korin, Ed. D. • W. Fred Miser, M. D.
References: • Bennett, A. , Thompson, N. , Holladay, B. , Bugbee, A. , & Steward. ASCP wage and vacancy survey of U. S. medical laboratories. 2009 • Passiment, K. Update on the laboratory workforce-shortage crisis. Washington Report. March: 2006; www. mlo-online. com • Irby, D. How attending physicians make instructional decisions when conducting teaching rounds. Academic Medicine , 1992; 67(10): 630 -638 • Gordon, J. ABC of learning and teaching in medicine: One-to-one teaching and feedback. British Medical Journal, 2003; 326: 543 -545 Acknowledgements: • Mark Quirk, Ed. D. • Tatum Langford Korin, Ed. D. • W. Fred Miser, M. D.


