e25a5e21680ed67699737ef04b09a333.ppt
- Количество слайдов: 71

Improving Outcomes for Diabetes in African Americans: Lessons Learned for REACH Charleston and Georgetown Diabetes Coalition Carolyn Jenkins, Dr. PH, APRN-BC, RD, FAAN Ann Darlington Edwards Chair and Professor Medical University of South Carolina phone: 843 -792 -4625 e-mail: jenkinsc@musc. edu

Goals for Today • Review diabetes statistics. • Share some processes and outcomes from community-based participatory research and service learning. • Review an expanded chronic care model for improving outcomes in African American communities. • Explore needed community changes.

Diabetes is the Fifth Deadliest Disease in the U. S. and Its Prevalence is Increasing 1999 1990 U. S. Prevalence (% of population) 4. 9% 6. 9% Males Lifetime Risk if Born in 2000 Whites: African Americans: Hispanics: 39% 27% 31% 40% 50% 45% 7 to 9. 6% Females 33% 2005 53% Sources: American Diabetes Association: Economic Costs of Diabetes in the U. S. in 2002. Diabetes Care. 2003; 26: 917 -932. Venkat Narayan KM, Boyle JP, Thompson TJ, Sorensen SW, Williamson DF. Lifetime risk of diabetes mellitus in the United States. JAMA. 2003; 290: 1884 -1890. American Diabetes Association: Diabetes Statistics for African Americans. Available at: www. diabetes. org/diabetes-statistics/african-americans. jsp. Accessed March 14, 2005. American Diabetes Association: Diabetes Statistics for Latinos. Available at: www. diabetes. org/diabetes-statistics/latinos. jsp. Accessed March 14, 2005.

How Serious Is Diabetes? It predictably affects both lifespan and quality of life Males Females Age at diagnosis: 40 40 Lost # of life years: 11 - 13 12 - 17 Lost # of quality-adjusted life years: 18 - 20 21 - 24 Source: Venkat Narayan KM, Boyle JP, Thompson TJ, Sorensen SW, Williamson DF. Lifetime risk of diabetes mellitus in the United States. JAMA. 2003; 290: 1884 -1890.

The Burden of Diabetes Is Greater for Minority Populations in the United States Diabetes affects: 10. 8% of African 10. 6% of Americans Hispanics Diabetes in African Americans • 2. 7 million (11. 4%) over age 20 – 60% higher than in whites • Higher complication rates – 2 X as likely to suffer lower-limb amputations – 2 X as likely to suffer from diabetes-related blindness 6. 2% of Whites Sources: American Diabetes Association: Diabetes Statistics for African Americans. Available at: www. diabetes. org/diabetesstatistics/african-americans. jsp. Accessed March 14, 2005. American Diabetes Association: Diabetes Statistics for Latinos. Available at: www. diabetes. org/diabetesstatistics/latinos. jsp. Accessed March 14, 2005. Mokdad AH, Ford ES, Bowman BA, et al. Diabetes trends in the U. S. : 1990 -1998. Diabetes Care. 2000; 23: 1278 -1283.
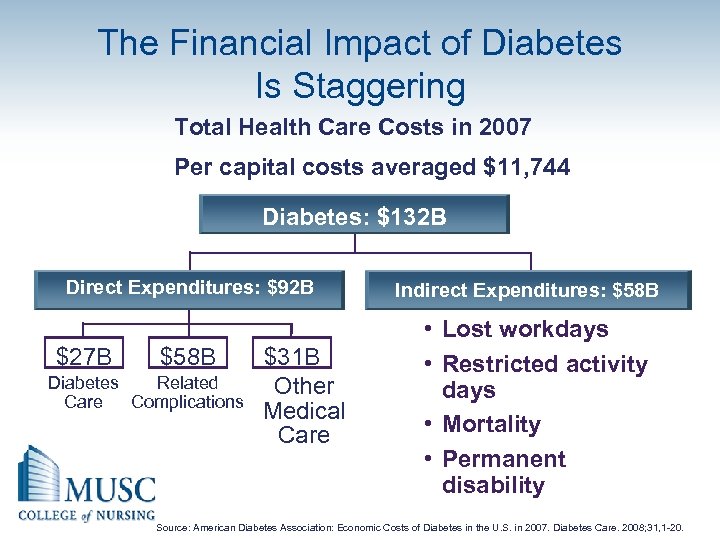
The Financial Impact of Diabetes Is Staggering Total Health Care Costs in 2007 Per capital costs averaged $11, 744 Diabetes: $132 B Direct Expenditures: $92 B $27 B $58 B Diabetes Related Care Complications $31 B Other Medical Care Indirect Expenditures: $58 B • Lost workdays • Restricted activity days • Mortality • Permanent disability Source: American Diabetes Association: Economic Costs of Diabetes in the U. S. in 2007. Diabetes Care. 2008; 31, 1 -20.

Diabetes Costs • Annual health care costs for people with diabetes: $11, 744. • One of every 5 health care $ spent caring for person with diabetes. • One of every 10 health care $ is attributed to diabetes. – Costs for people with diabetes 2. 3 X higher than those without diabetes. Diabetes Care 2008

South Carolina Statistics • In 2005 BRFSS: – 10. 3% reported they had diabetes • African Americans (15. 4%) • Non-Hispanic Whites (8. 4%) – Insulin treated (29. 5%) – “Pills” (72. 9%) – A 1 C test in past year (77%) – Never had A 1 c (23%) – Diabetic eye disease (21. 7%) – No insurance and/or no doctor (~18%) • African Americans (26. 6%) • Non-Hispanic whites (15. 1%)
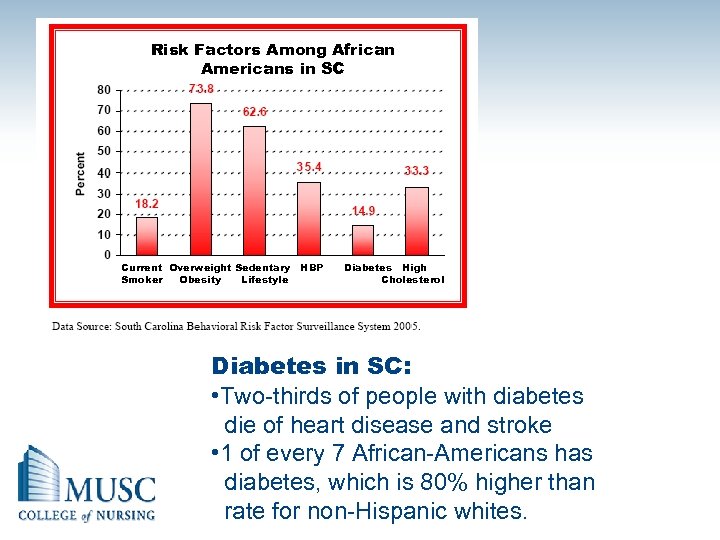
Risk Factors Among African Americans in SC Current Overweight Sedentary HBP Smoker Obesity Lifestyle Diabetes High Cholesterol Diabetes in SC: • Two-thirds of people with diabetes die of heart disease and stroke • 1 of every 7 African-Americans has diabetes, which is 80% higher than rate for non-Hispanic whites.

Diabetes in African Americans in South Carolina • In Charleston and Georgetown Counties, 21% of African Americans reported having diabetes (2005 RRFS) • Rural African Americans with diabetes: – 60. 6 % have inadequate control versus 42. 5% of urban whites (SC BRFSS)

Disease risk, diagnosis, progression of disease, response to treatment, caregiving, and overall quality of life are all affected by a number of variables including race, ethnicity, gender, socioeconomic status, age, education, occupation, country of origin, and perhaps other lifetime and lifestyle differences.
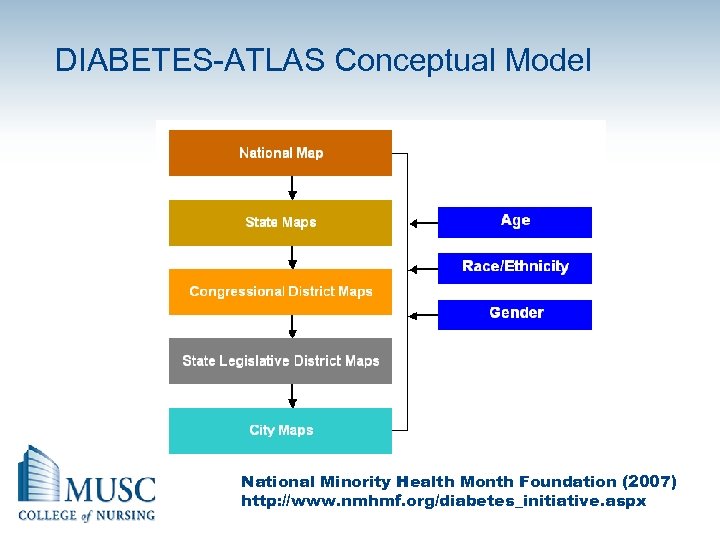
DIABETES-ATLAS Conceptual Model National Minority Health Month Foundation (2007) http: //www. nmhmf. org/diabetes_initiative. aspx
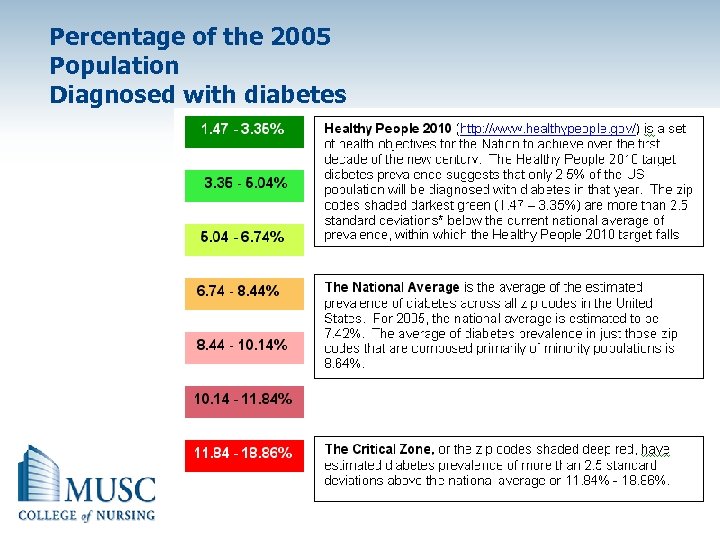
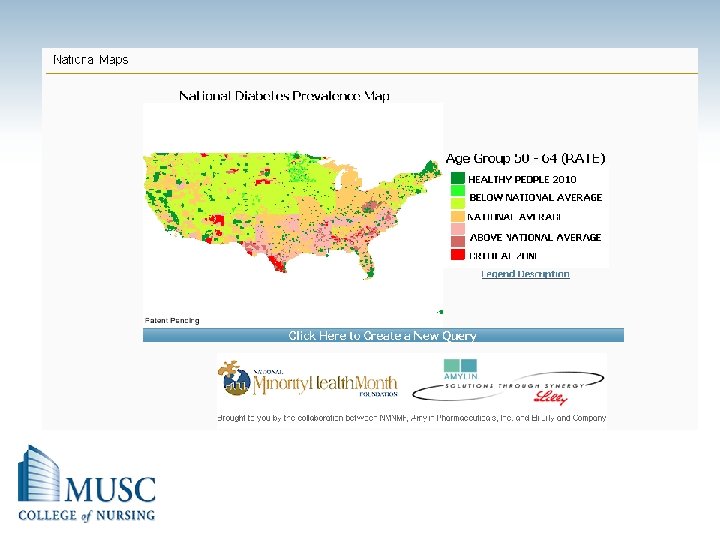
Percentage of the 2005 Population Diagnosed with diabetes

CBPAR Activities and Diabetes Management 1994 -present

From Meredith Minkler, Dr. PH University of California, Berkeley

Enterprise Neighborhood Health Program (1994 – 1998) • HUD Grant with Charleston’s Enterprise Community to a) recruit and train community leaders to become Community Health Advocates; b) conduct needs assessment. – Needs assessment identified diabetes and HTN as priority issues. – 61 community health advisors trained. – Video documenting needs and assets using community voices – AKA Summer Enrichment Program for children

Diabetes Initiative of South Carolina • 1994—Report to SC Legislature on “Scope and Problems of Diabetes in SC” • Funding by State Legislature to create Center to address diabetes in SC – Center of Excellence at MUSC • Professional Council • Outreach Council • Surveillance Council • Annual Report on activities and outcomes to South Carolina Legislature and Governor

Enterprise Health Center 1995 - 2001 Donation of Lot Building Completed Opened November 2001 Now a FQHC site (FCFFHC)

Service-Learning • An educational methodology based on a community-campus partnership which combines student community service with explicit learning objectives. Students participating in service-learning are not only expected to provided direct community service but also to learn about the context in which the service is provided, and to understand the connection between the service and their academic coursework. Seifer 1998

Service Learning with Students >700 students (MUSC, Clemson, Howard, USC, Rhode Island, UNC) 7 Doctoral Candidates/Graduates 6 Certified Diabetes Educators 7 doctoral dissertations 3 masters thesis 20 regional or national presentations 10 peer-reviewed publications

Healthy South Carolina Hypertension and Diabetes Management and Education Program (HAD-ME) • Health care team conducted weekly screening, management, and education clinics (with linkages to primary care) in inner-city neighborhoods (1997 -2001) – > 900 community residents with diabetes and/or hypertension participated. – > 1, 100 referrals to primary care – Significant decreases in BP, blood glucose, and weight

REACH 2010: Charleston And Georgetown Diabetes Coalition’s Efforts to Decrease Disparities for Diabetes Arlene Case-The Lesson

A heath disparity population is “a population where there is significant disparity in the overall rate of disease incidence, prevalence, morbidity, mortality, or survival rates in the population as compared to the health 1 status of the general population”. Minority Health and Health Disparities Research and Education Act of 2000
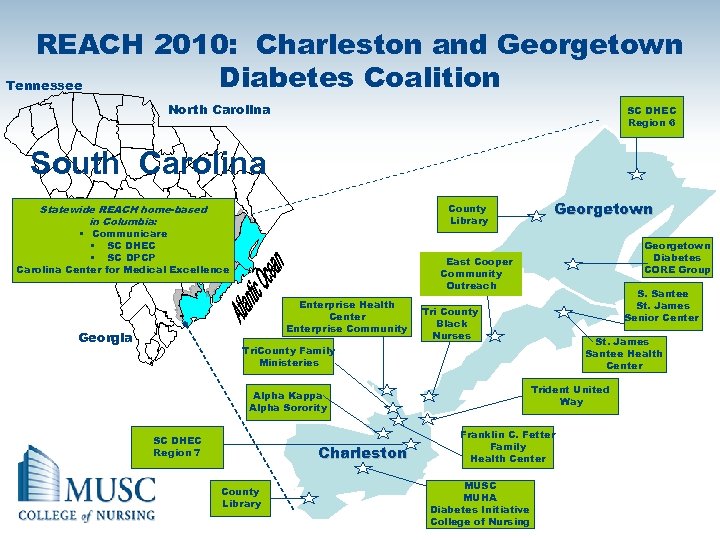
REACH 2010: Charleston and Georgetown Diabetes Coalition Tennessee North Carolina SC DHEC Region 6 South Carolina County Library Statewide REACH home-based in Columbia: § Communicare § SC DHEC § SC DPCP Georgetown Diabetes CORE Group East Cooper Community Outreach Carolina Center for Medical Excellence Enterprise Health Center Enterprise Community Georgia Georgetown S. Santee St. James Senior Center Tri County Black Nurses St. James Santee Health Center Tri. County Family Ministeries Trident United Way Alpha Kappa Alpha Sorority SC DHEC Region 7 Charleston County Library Franklin C. Fetter Family Health Center MUSC MUHA Diabetes Initiative College of Nursing

Methods and Interventions • Community skill-building and neighborhood clinics – 175 lay educators trained – Diabetes self management education – Foot care training – Wise Woman for AA women 40 -70 years old • Community health professional training – 145 RNs with advanced foot/wound education – 27 physicians with foot care education • Outreach by professional and lay educators – 30 minute TV program aired 34 times on cable – Library program/Internet use – Weekly diabetes management classes in 8 sites • Health systems change – Registry and reminder system – CQI teams • Coalition building and policy change

Community and Media Activities reached >40, 000 African Americans Neighborhood Walk and Talk Groups Skill-Building for CHAs and Volunteers Community Screening and Education Individual and Group Education Sessions
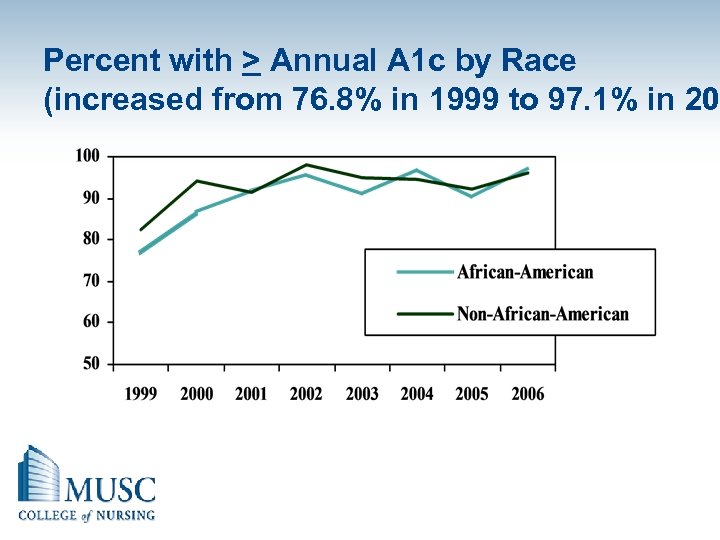
Percent with > Annual A 1 c by Race (increased from 76. 8% in 1999 to 97. 1% in 20
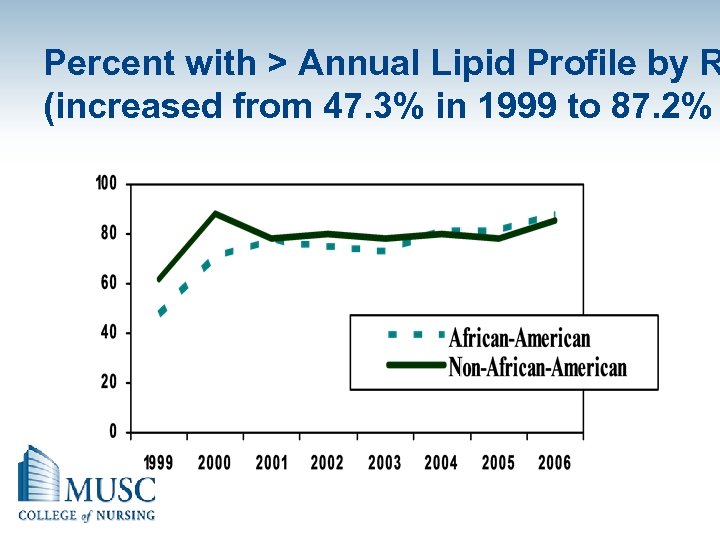
Percent with > Annual Lipid Profile by R (increased from 47. 3% in 1999 to 87. 2%
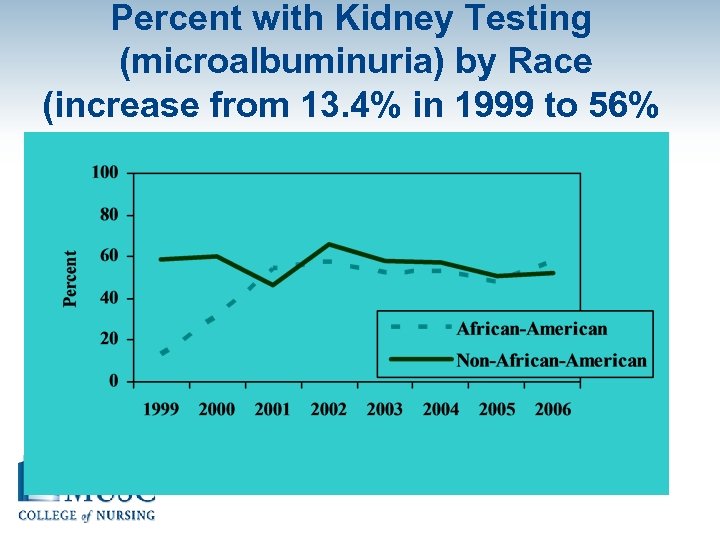
Percent with Kidney Testing (microalbuminuria) by Race (increase from 13. 4% in 1999 to 56% in 2006)
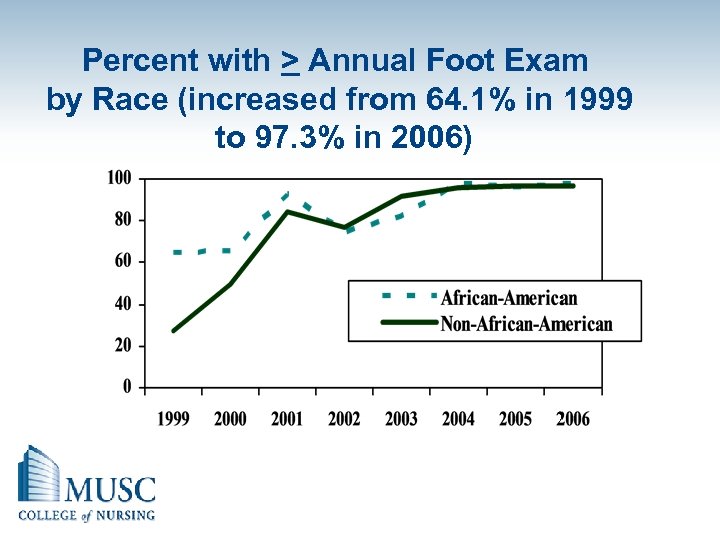
Percent with > Annual Foot Exam by Race (increased from 64. 1% in 1999 to 97. 3% in 2006)
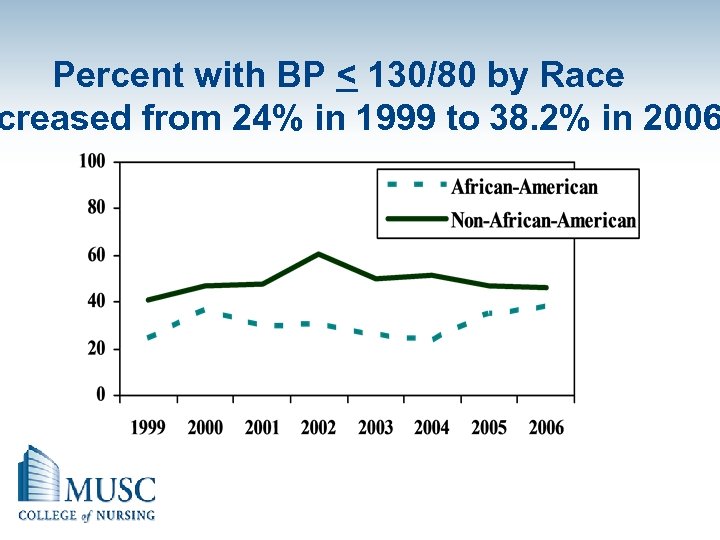
Percent with BP < 130/80 by Race creased from 24% in 1999 to 38. 2% in 2006
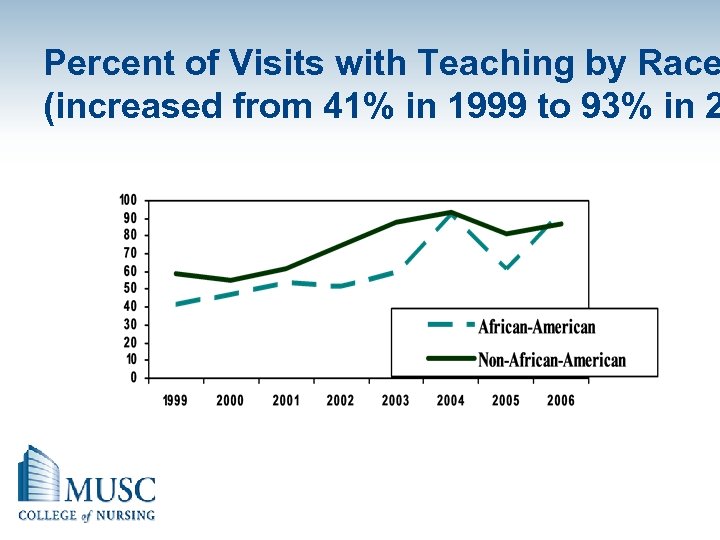
Percent of Visits with Teaching by Race (increased from 41% in 1999 to 93% in 2
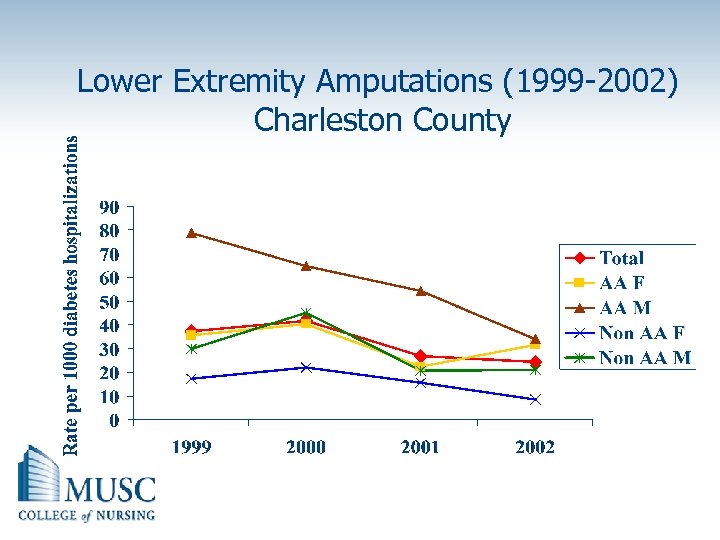
Lower Extremity Amputations (1999 -2002) Charleston County


www. musc. edu/reach

Although studies documenting disparities are not in short supply, findings about what works to reduce disparities are. A 3 -year, $6 -million program called Finding Answers: Disparities Research for Change, sponsored by the Robert Wood Johnson Foundation, seeks to identify effective interventions to eliminate disparities. Under the direction of Marshall Chin, MD, MPH, an associate professor of medicine at the University of Chicago Pritzker School of Medicine, the program reviewed more than 200 journal articles on disparity reduction interventions in cardiovascular disease, depression, diabetes, and breast cancer. The results appeared in October 2007 in a supplement to Medical Care Research and Review. One of the few studies in the review that showed a reduction in racial disparities was part of the Racial and Ethnic Approaches to Community Health (REACH 2010) program, sponsored by the US Centers for Disease Control and Prevention in Atlanta, Ga. The demonstration program, which took place in Charleston and Georgetown counties in South Carolina, brought together 28 community partners, from health professionals to college sororities and local media, that set goals to improve diabetes care for blacks as well as eliminate health care disparities between black and white patients with diabetes. The partners documented disparities in care for 12, 000 black patients with diabetes in the 2 county community. The intervention included such community activities as health fairs, support groups, grocery store tours, community clinics, and church-based educational programs. After 24 months, the partners audited medical charts for 158 black patients and 112 patients who were white or of other racial or ethnic groups. They found that differences between black and white patients in rates of hemoglobin A 1 c testing, lipid and kidney testing, eye examinations, and blood pressure control that had ranged from 11% to 28% at baseline had been eliminated (Jenkins C et al. Public Health Rep. 2004; 119[3]: 322 -330). Chin is optimistic that other communities will develop their own, similar programs in the future. "There a lot of promising models, " he says. "But you may have to revise as you go along, just like in patient care. " Quote from R. Voelker in JAMA 2008; 299(12): 1411 -1413.

REACH US: South. Eastern African American Center of Excellence for Eliminating Disparities for Diabetes REACH US SEA-CEED

REACH US Center of Excellence • A coordinated multi-system, multimedia, intergenerational approach to prevention and control of diabetes and its cardiovascular complications to eliminate health disparities in African Americans at risk and with diabetes.
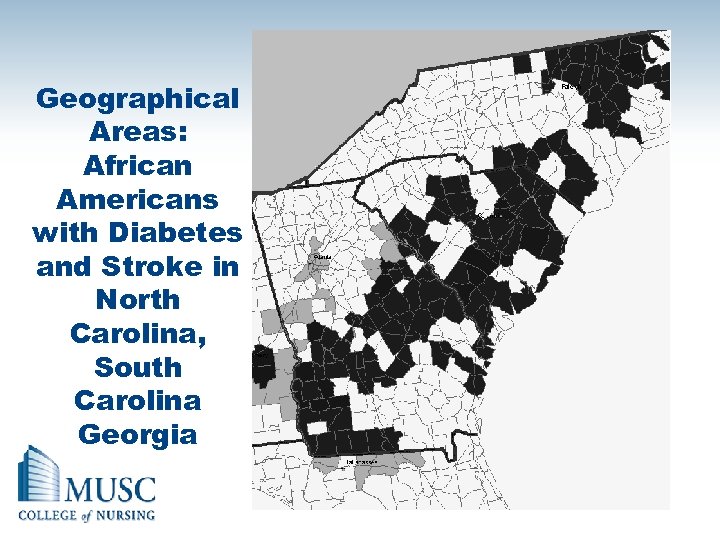
Geographical Areas: African Americans with Diabetes and Stroke in North Carolina, South Carolina Georgia
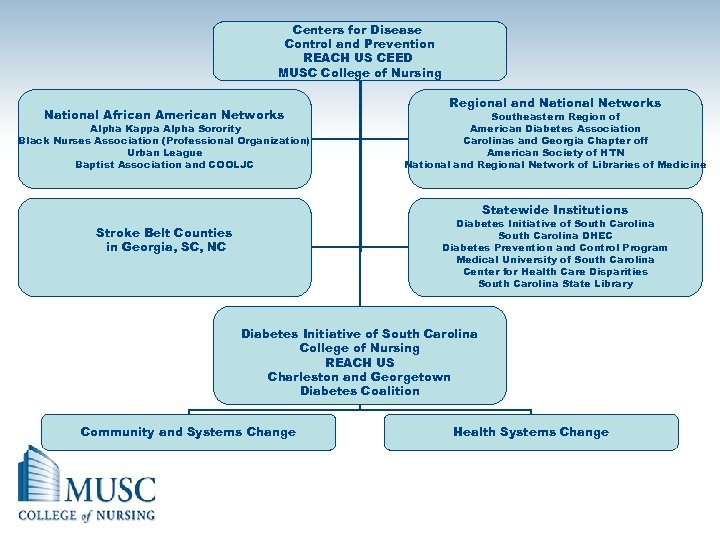
Centers for Disease Control and Prevention REACH US CEED MUSC College of Nursing National African American Networks Alpha Kappa Alpha Sorority Black Nurses Association (Professional Organization) Urban League Baptist Association and COOLJC Regional and National Networks Southeastern Region of American Diabetes Association Carolinas and Georgia Chapter off American Society of HTN National and Regional Network of Libraries of Medicine Statewide Institutions Diabetes Initiative of South Carolina DHEC Diabetes Prevention and Control Program Medical University of South Carolina Center for Health Care Disparities South Carolina State Library Stroke Belt Counties in Georgia, SC, NC Diabetes Initiative of South Carolina College of Nursing REACH US Charleston and Georgetown Diabetes Coalition Community and Systems Change Health Systems Change

What is needed to improve diabetes care and outcomes in African Americans in South Carolina?

IOM’s 8 Competency Areas • • Informatics Genomics Cultural competence Communications Community based participatory research Ethics Policy and law Global health Gebbie et al. (2001)

Evidence-Based Practice • Practice supported by research findings and/or demonstrated as being effective through a critical examination and review of current and past practices. EBP integrates patient preferences with research evidence, to determine best course of action to improve health.

Listen to the Stories While the stories are being told, don’t offer solutions too early!! Work together to identify the issues and develop the solutions. 45

Go to the people. Live among the people. Learn from the people. Work with the people. Start with what the people know. Build on what the people have. Teach by showing, learn by doing. Not a showcase but a pattern. Not odds and ends, but a system. Not piece meal, but an integrated approach. 46

Li fe C ou rs e Determinants of Health from National Academy of Sciences, Epidemiology Review 2004; 26: 124125 Social & Economic Policies Institutions Neighborhoods/Communities Living Conditions Social Relationships Individual Risk Factors Genetic/Constitutional Factors Pathophysiologic Pathways Individual and Population Health E i nv r nm o t en

Chronic Care Model Community Health System Health Care Organization Resources and Policies Self. Management Support Informed, Activated Patient Delivery System Design Productive Interactions Decision Support Clinical Information Systems Prepared, Proactive Practice Team Improved Outcomes Wagner, E. H. (1998). Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice(1), 2 -4.
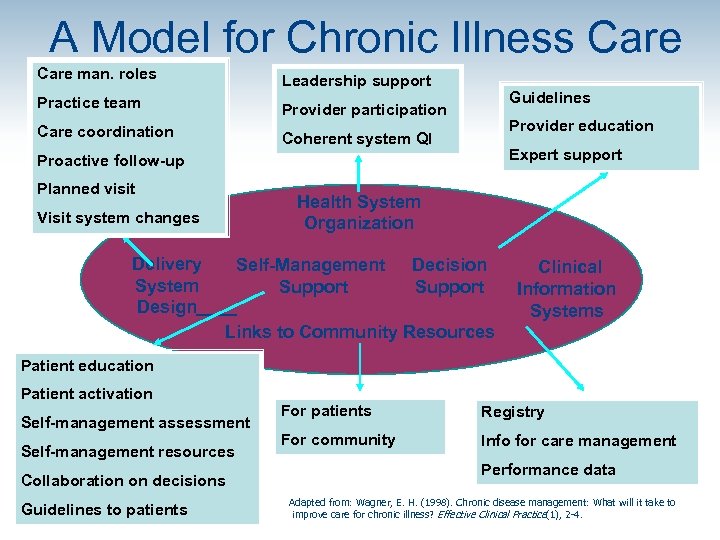
A Model for Chronic Illness Care man. roles Leadership support Practice team Provider participation Care coordination Coherent system QI Guidelines Provider education Expert support Proactive follow-up Planned visit Visit system changes Health System Organization Delivery Self-Management Decision System Support Design Links to Community Resources Clinical Information Systems Patient education Patient activation Self-management assessment Self-management resources Collaboration on decisions Guidelines to patients For patients Registry For community Info for care management Performance data Adapted from: Wagner, E. H. (1998). Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice(1), 2 -4.
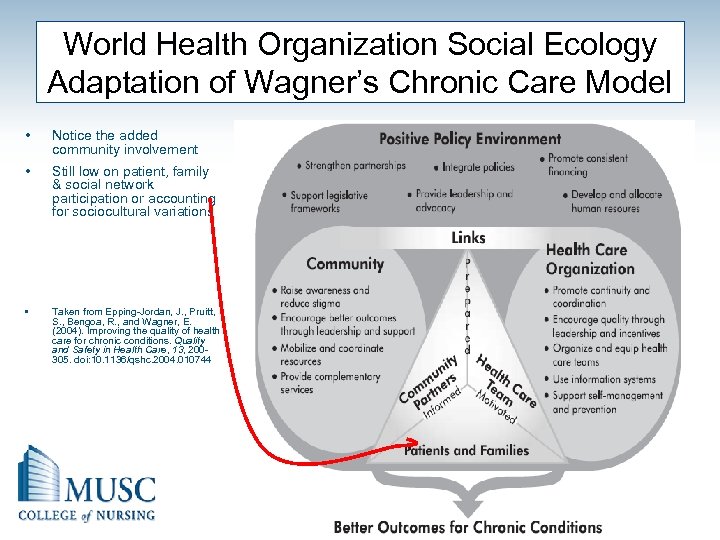
World Health Organization Social Ecology Adaptation of Wagner’s Chronic Care Model • Notice the added community involvement • Still low on patient, family & social network participation or accounting for sociocultural variations • Taken from Epping-Jordan, J. , Pruitt, S. , Bengoa, R. , and Wagner, E. (2004). Improving the quality of health care for chronic conditions. Quality and Safety in Health Care, 13, 200305. doi: 10. 1136/qshc. 2004. 010744
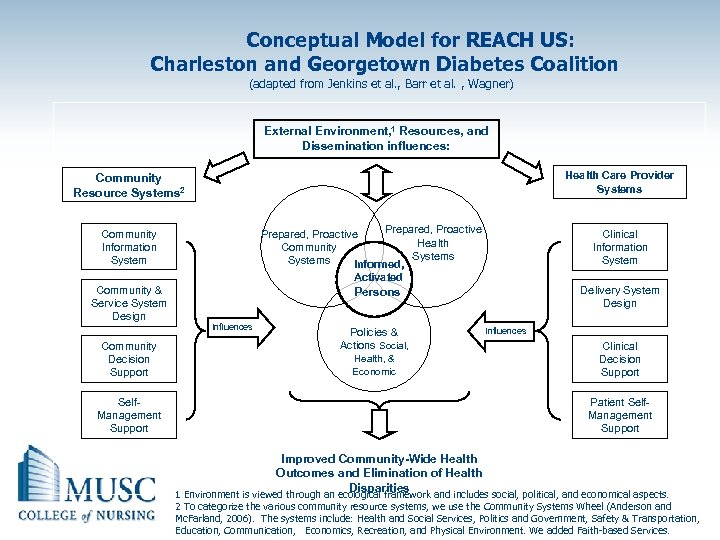
Conceptual Model for REACH US: Charleston and Georgetown Diabetes Coalition (adapted from Jenkins et al. , Barr et al. , Wagner) External Environment, 1 Resources, and Dissemination influences: Health Care Provider Systems Community Resource Systems 2 Prepared, Proactive Health Community Systems Informed, Community Information System Clinical Information System Activated Community & Service System Design Community Decision Support Delivery System Design Persons Influences Policies & Actions Social, Health, & Economic Influences Clinical Decision Support Patient Self. Management Support Improved Community-Wide Health Outcomes and Elimination of Health Disparities 1 Environment is viewed through an ecological framework and includes social, political, and economical aspects. 2 To categorize the various community resource systems, we use the Community Systems Wheel (Anderson and Mc. Farland, 2006). The systems include: Health and Social Services, Politics and Government, Safety & Transportation, Education, Communication, Economics, Recreation, and Physical Environment. We added Faith-based Services.

Community-Based Participatory Action Research • A collaborative approach to research that equitably involves all partners in the research process and recognizes the unique strengths that each brings. CBPR begins with a research topic of importance to the community, has the aim of combining knowledge with action and achieving social change. WK Kellogg Foundation Community Health Scholars Program

Fundamental Characteristics of CBPAR • It is: – participatory. – cooperative, engaging community members and researcher(s) in a joint process with both contributing equally. – a co-learning process. – an empowerment process through which participants can increase control over their lives.

Fundamental Characteristics of CBPAR • It involves systems development and local community capacity building. • It achieves a balance between research and action. (Israel et al. 1998) • It involves sharing of funding among partners (usually equally). 54

Identified Challenges for Communities and Academic Institutions • Understanding cultures – Community culture – Academic and institutional culture • Differing philosophies. • Sharing of budgets in an equitable way. • Clearly defining and continuously implementing our principles for the partnership in a fair and equitable way.

Instructions for Community for Partnering with Academic Institutions--Look For People that: • Begin their discussions with you by asking questions, rather than offering solutions. • Recognize the gap between measuring differences and making differences. • Demonstrate a willingness to help you measure the differences you make. • Share control over financial resources and decisions with community representatives. • Express commitment to a working relationship built on trust and equity. Prev Chronic Dis. 2004 January; 1(1): A 12.

Common Characteristics of Successful Community. Institutional Partnerships • • • Trusting relationships Equitable processes and procedures Diverse membership Tangible benefits to all partners Balance between partnership process, activities, and outcomes • Significant community involvement in scientifically sound research (Continued on next slide) Seifer, 2006

Common Characteristics of Successful Community-Institutional Partnerships • Supportive organizational policies/reward structure • Leadership at multiple levels • Culturally competent and appropriately skilled staff and researchers • Collaborative dissemination • Ongoing partnership assessment, improvement and celebration • Sustainable impact Seifer, 2006

Recommendations for Emerging and Established Partnerships • Pay close attention to membership issues • Build on prior history of positive working relationships • Obtain support and involvement of both top leadership and “front line” staff of partner organizations • Embrace diversity in the partnership • Decide who the “community” is and who “represents” the community. Seifer, 2006

Recommendations for Emerging and Established Partnerships (continued) • Develop rationale, criteria and procedures for adding new partners • Develop structures and processes that facilitate the development of trust and sharing of influence and control among partners • Jointly develop partnership principles and operating procedures • Jointly create mission, vision, and priorities for the partnership Seifer, 2006

Recommendations for Emerging and Established Partnerships (continued) • Strive to achieve an equitable distribution of costs, benefits, and resources among the partners • Conduct ongoing evaluation of partnership process • Build the capacity of all partners • Plan ahead for sustainability • Pay close attention to the balance of activities within the partnership • Be strategic about dissemination Seifer, 2006

Build Capacity of All Partners • Facilitate partner training, technical assistance and continuing education • Invest partnership resources in local community • Establish and maintain partnership infrastructure Seifer, 2006

Cultural Humility: “A life long commitment to self evaluation and self critique” to redress power imbalances and “develop and maintain respectful and dynamic partnerships with communities” Tervalon & Garcia, 1998 63
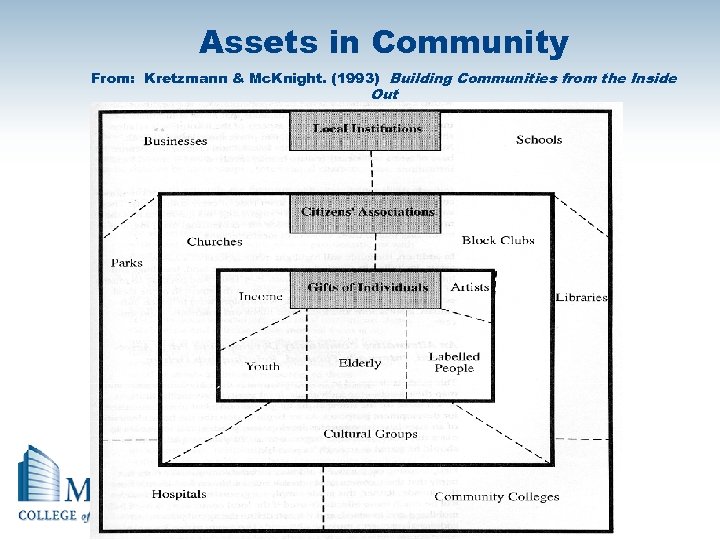
Assets in Community From: Kretzmann & Mc. Knight. (1993) Building Communities from the Inside Out 64

Identifying Natural Community Leaders § When you have a problem, who do you go to for advice? § Who do others go to? § When people in the neighborhood have come together around a problem in the past, did a particular individual or group play a key role? § What things do people tell you’re good at? Eng et al, 1990; Israel, 1985; Sharpe, 2000 65

Insider-Outsider Tensions • Power dynamics; the “power of authority” of the outsider’s often multiple sources of unspoken privilege (Wallerstein, 1999) • Conflicting time tables & demands • Differential reward structures (Minkler, 2006)

Perceived clash between community desires and “good science”

“We want to know how much you care, before we know how much you know. ” Alma Joseph Flores Enterprise Community 68

Partnership • A strategic combining of resources that create power far beyond the capabilities of individual players working alone.

Thanks to Our Team (and to you)! • REACH Community Partners and Staff • REACH Partners Coaltion • • • Charleston Diabetes Coalition Georgetown Diabetes CORE Group Diabetes Initiative of South Carolina • • SC Diabetes Prevention and Control Program Centers for Disease Control and Prevention National Institutes of Health-NIDDK American Diabetes Association – Gayenell Magwood, Barbara Carlson, Jane Zapka, Martina Mueller, Leonard Egede, Marilyn Laken, Montrese Edwards, Virginia Thomas, Joyce Linnen, Lee Moultrie, Sonja Smalls, Syndia Moultrie, Karen Hill, George Bush – – – Dr. John Colwell Dr. Kathie Hermayer Dr. Dan Lackland Dr. Brent Egan Pamela Arnold
e25a5e21680ed67699737ef04b09a333.ppt