c9805a844881a89ce2b99aa8fe84712b.ppt
- Количество слайдов: 53
 Improving Healthcare for Hoosier Children Jay L. Grosfeld, MD Lafayette F. Page Professor of Pediatric Surgery Indiana University School of Medicine
Improving Healthcare for Hoosier Children Jay L. Grosfeld, MD Lafayette F. Page Professor of Pediatric Surgery Indiana University School of Medicine
 Provision of Health Care in Indiana • State population: 6, 120, 000 in 2002 • 20% are children (1, 574, 396 in 2001) • 83, 000 annual births • 70 % of children are covered by private healthcare insurance • Others: Medicaid (475, 464) Hoosier Health Care CHIPS - Programs A, C Uninsured (11%)
Provision of Health Care in Indiana • State population: 6, 120, 000 in 2002 • 20% are children (1, 574, 396 in 2001) • 83, 000 annual births • 70 % of children are covered by private healthcare insurance • Others: Medicaid (475, 464) Hoosier Health Care CHIPS - Programs A, C Uninsured (11%)
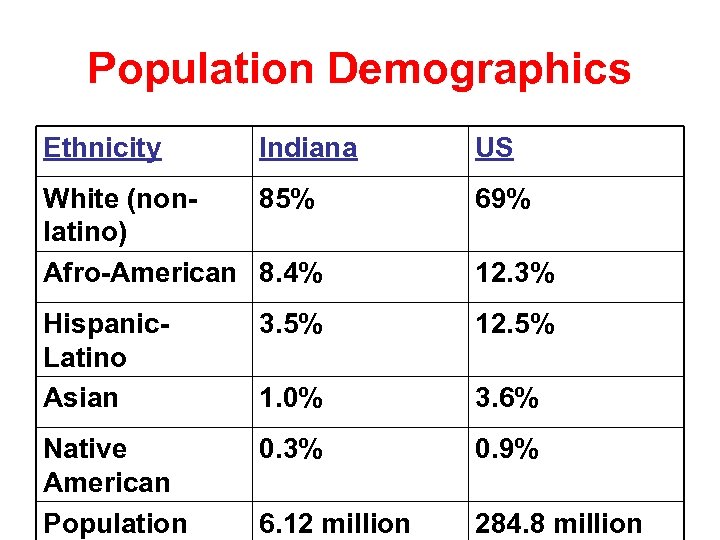 Population Demographics Ethnicity Indiana US White (non 85% latino) Afro-American 8. 4% 69% Hispanic. Latino Asian 3. 5% 12. 5% 1. 0% 3. 6% Native American Population 0. 3% 0. 9% 6. 12 million 284. 8 million 12. 3%
Population Demographics Ethnicity Indiana US White (non 85% latino) Afro-American 8. 4% 69% Hispanic. Latino Asian 3. 5% 12. 5% 1. 0% 3. 6% Native American Population 0. 3% 0. 9% 6. 12 million 284. 8 million 12. 3%
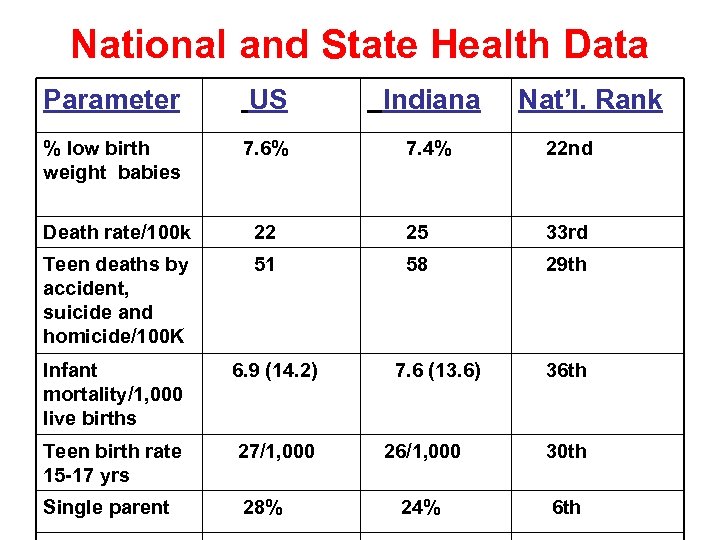 National and State Health Data Parameter US Indiana % low birth weight babies 7. 6% 7. 4% 22 nd Death rate/100 k 22 25 33 rd Teen deaths by accident, suicide and homicide/100 K 51 58 29 th Infant mortality/1, 000 live births 6. 9 (14. 2) Teen birth rate 15 -17 yrs 27/1, 000 Single parent 28% 7. 6 (13. 6) Nat’l. Rank 36 th 26/1, 000 30 th 24% 6 th
National and State Health Data Parameter US Indiana % low birth weight babies 7. 6% 7. 4% 22 nd Death rate/100 k 22 25 33 rd Teen deaths by accident, suicide and homicide/100 K 51 58 29 th Infant mortality/1, 000 live births 6. 9 (14. 2) Teen birth rate 15 -17 yrs 27/1, 000 Single parent 28% 7. 6 (13. 6) Nat’l. Rank 36 th 26/1, 000 30 th 24% 6 th
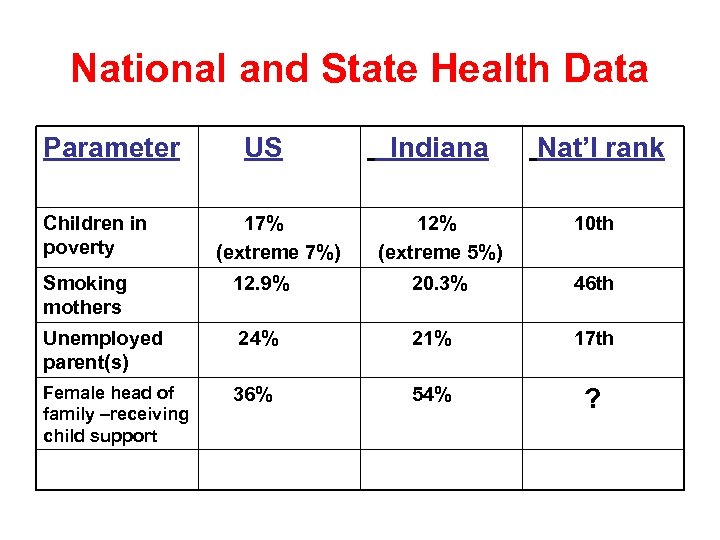 National and State Health Data Parameter Children in poverty US 17% (extreme 7%) Indiana Nat’l rank 12% (extreme 5%) 10 th Smoking mothers 12. 9% 20. 3% 46 th Unemployed parent(s) 24% 21% 17 th 36% 54% ? Female head of family –receiving child support
National and State Health Data Parameter Children in poverty US 17% (extreme 7%) Indiana Nat’l rank 12% (extreme 5%) 10 th Smoking mothers 12. 9% 20. 3% 46 th Unemployed parent(s) 24% 21% 17 th 36% 54% ? Female head of family –receiving child support
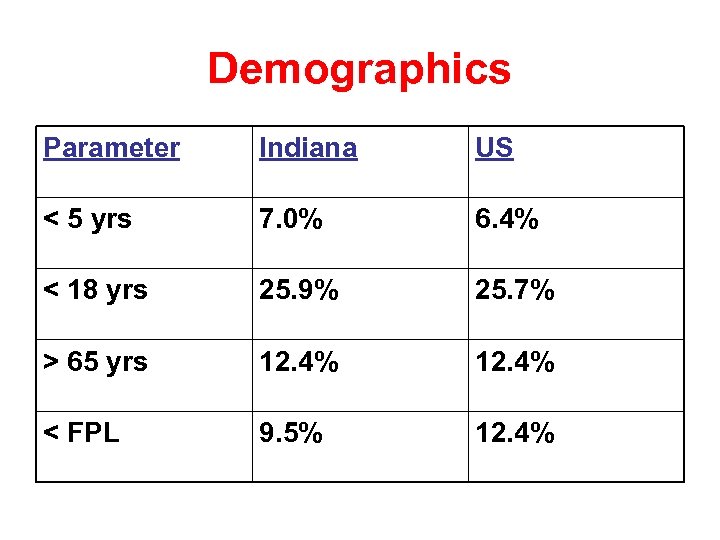 Demographics Parameter Indiana US < 5 yrs 7. 0% 6. 4% < 18 yrs 25. 9% 25. 7% > 65 yrs 12. 4% < FPL 9. 5% 12. 4%
Demographics Parameter Indiana US < 5 yrs 7. 0% 6. 4% < 18 yrs 25. 9% 25. 7% > 65 yrs 12. 4% < FPL 9. 5% 12. 4%
 Medicaid • Office of Medicaid Planning and Policy • • • (OMPP) designated state agency for Medicaid. 475, 464 covered by MK Hoosier Healthwise Program managed by the managed care division of the OMPP Children’s Health Insurance Program (CHIPS) Joint Federal-State funded program with State receiving federal matching dollars. Indiana matching rate = 74. 43%
Medicaid • Office of Medicaid Planning and Policy • • • (OMPP) designated state agency for Medicaid. 475, 464 covered by MK Hoosier Healthwise Program managed by the managed care division of the OMPP Children’s Health Insurance Program (CHIPS) Joint Federal-State funded program with State receiving federal matching dollars. Indiana matching rate = 74. 43%
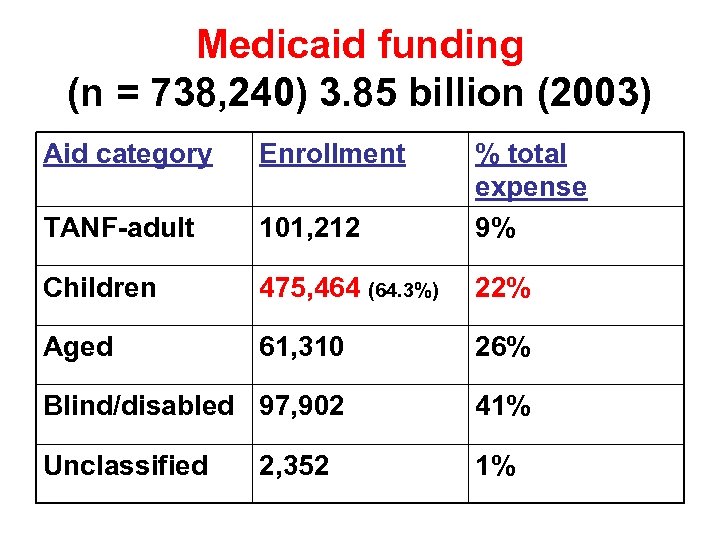 Medicaid funding (n = 738, 240) 3. 85 billion (2003) Aid category Enrollment TANF-adult 101, 212 % total expense 9% Children 475, 464 (64. 3%) 22% Aged 61, 310 26% Blind/disabled 97, 902 41% Unclassified 1% 2, 352
Medicaid funding (n = 738, 240) 3. 85 billion (2003) Aid category Enrollment TANF-adult 101, 212 % total expense 9% Children 475, 464 (64. 3%) 22% Aged 61, 310 26% Blind/disabled 97, 902 41% Unclassified 1% 2, 352
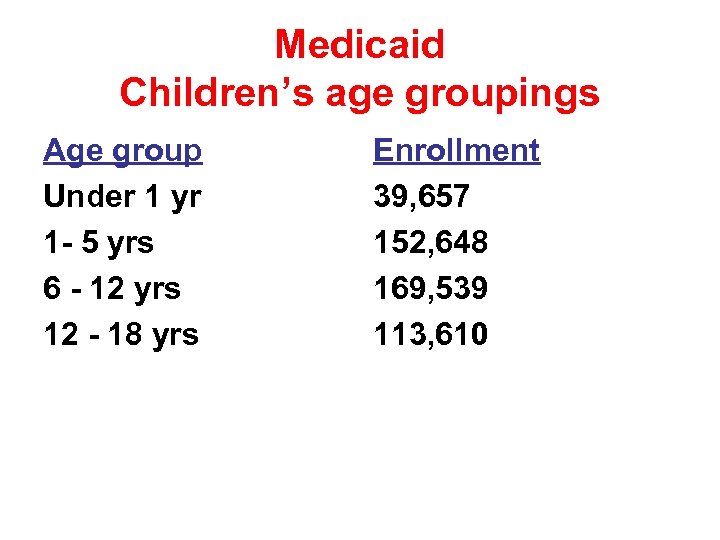 Medicaid Children’s age groupings Age group Under 1 yr 1 - 5 yrs 6 - 12 yrs 12 - 18 yrs Enrollment 39, 657 152, 648 169, 539 113, 610
Medicaid Children’s age groupings Age group Under 1 yr 1 - 5 yrs 6 - 12 yrs 12 - 18 yrs Enrollment 39, 657 152, 648 169, 539 113, 610
 Medicaid/CHIPS • CHIPS – two phases • Phase I (Medicaid expansion) provides • • medicaid to children birth to < 19 yrs old with family incomes no more than 150% FPL($27, 150 for family of 4) n = 54, 050 Phase II (non-Medicaid expansion) State defined - not an entitlement. Monthly premium share program provides care from birth -18 yrs with family incomes 200% FPL ($36, 200 for family of 4) n = 12, 900 Total 66, 950 children Phase I and II
Medicaid/CHIPS • CHIPS – two phases • Phase I (Medicaid expansion) provides • • medicaid to children birth to < 19 yrs old with family incomes no more than 150% FPL($27, 150 for family of 4) n = 54, 050 Phase II (non-Medicaid expansion) State defined - not an entitlement. Monthly premium share program provides care from birth -18 yrs with family incomes 200% FPL ($36, 200 for family of 4) n = 12, 900 Total 66, 950 children Phase I and II
 Hoosier Healthcare for Children Medicaid delivery system Based on monthly income, family size Family size $/mo “A” $/mo “C” 1 2 3 4 5 6 7 8 1, 044. 00 1, 407. 00 1, 769. 00 2, 132. 00 2, 494. 00 2, 857. 00 3, 219. 00 3, 582. 00 no insurance no co-pay FPL= $ 18, 100 for a family of 4 1, 392. 00 1, 875. 00 2, 359. 00 2, 842. 00 3, 325. 00 3, 809. 00 4, 292. 00 4, 775. 00 monthly premium 1 child $11 -16. 50 2 or more $16. 50 -24. 75 Up to 250% of FPL
Hoosier Healthcare for Children Medicaid delivery system Based on monthly income, family size Family size $/mo “A” $/mo “C” 1 2 3 4 5 6 7 8 1, 044. 00 1, 407. 00 1, 769. 00 2, 132. 00 2, 494. 00 2, 857. 00 3, 219. 00 3, 582. 00 no insurance no co-pay FPL= $ 18, 100 for a family of 4 1, 392. 00 1, 875. 00 2, 359. 00 2, 842. 00 3, 325. 00 3, 809. 00 4, 292. 00 4, 775. 00 monthly premium 1 child $11 -16. 50 2 or more $16. 50 -24. 75 Up to 250% of FPL
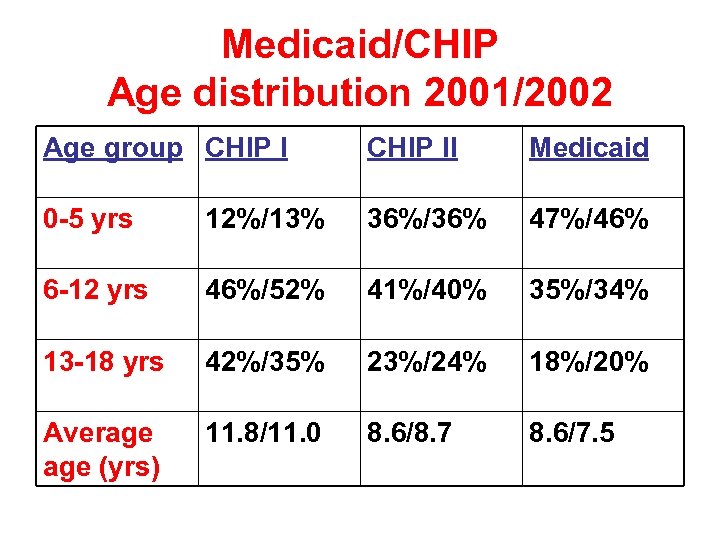 Medicaid/CHIP Age distribution 2001/2002 Age group CHIP II Medicaid 0 -5 yrs 12%/13% 36%/36% 47%/46% 6 -12 yrs 46%/52% 41%/40% 35%/34% 13 -18 yrs 42%/35% 23%/24% 18%/20% Average (yrs) 11. 8/11. 0 8. 6/8. 7 8. 6/7. 5
Medicaid/CHIP Age distribution 2001/2002 Age group CHIP II Medicaid 0 -5 yrs 12%/13% 36%/36% 47%/46% 6 -12 yrs 46%/52% 41%/40% 35%/34% 13 -18 yrs 42%/35% 23%/24% 18%/20% Average (yrs) 11. 8/11. 0 8. 6/8. 7 8. 6/7. 5
 Utilization • CHIP expenses are less than MK for primary • • • care MD services, non-primary care MD services, in-patient and outpatient hospital services CHIP uses more dental services , and Pharmacy costs were similar to MK CHIP II has a higher MD use and Dental use than CHIP I 37% CHIP II and 39% CHIP I patients are in risk based managed care (RBMC). 9/10 CHIP I children have a single coordinator of primary care case management.
Utilization • CHIP expenses are less than MK for primary • • • care MD services, non-primary care MD services, in-patient and outpatient hospital services CHIP uses more dental services , and Pharmacy costs were similar to MK CHIP II has a higher MD use and Dental use than CHIP I 37% CHIP II and 39% CHIP I patients are in risk based managed care (RBMC). 9/10 CHIP I children have a single coordinator of primary care case management.
 Medicaid/CHIPS • State supported recipients: Medicaid 85%; CHIPS 15% • 86% Medicaid recipients and 81% CHIPS children live in urban communities • Hoosier Health Care Program is mandatory in Marion, Lake, Allen, Elkhart and St. Joseph counties • Indiana children have a higher rate of IP & OP hospital utilization, pharmacy and dental services when compared to national averages and the highest utilization rates in the region for IP, physician and dental services.
Medicaid/CHIPS • State supported recipients: Medicaid 85%; CHIPS 15% • 86% Medicaid recipients and 81% CHIPS children live in urban communities • Hoosier Health Care Program is mandatory in Marion, Lake, Allen, Elkhart and St. Joseph counties • Indiana children have a higher rate of IP & OP hospital utilization, pharmacy and dental services when compared to national averages and the highest utilization rates in the region for IP, physician and dental services.
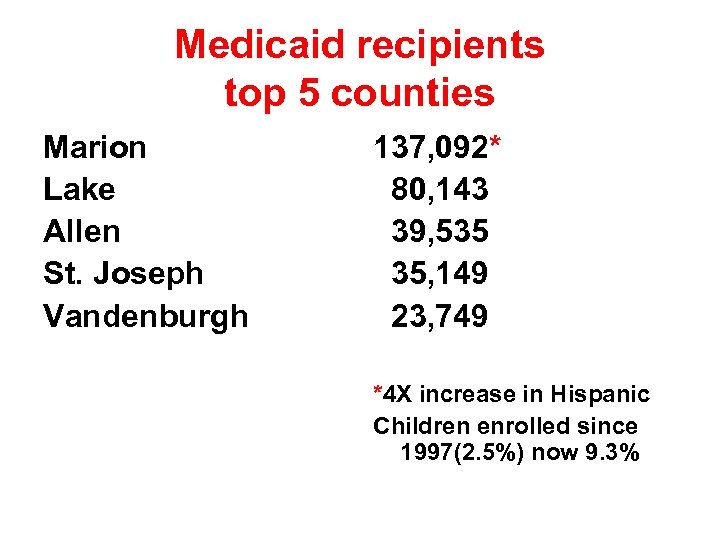 Medicaid recipients top 5 counties Marion Lake Allen St. Joseph Vandenburgh 137, 092* 80, 143 39, 535 35, 149 23, 749 *4 X increase in Hispanic Children enrolled since 1997(2. 5%) now 9. 3%
Medicaid recipients top 5 counties Marion Lake Allen St. Joseph Vandenburgh 137, 092* 80, 143 39, 535 35, 149 23, 749 *4 X increase in Hispanic Children enrolled since 1997(2. 5%) now 9. 3%
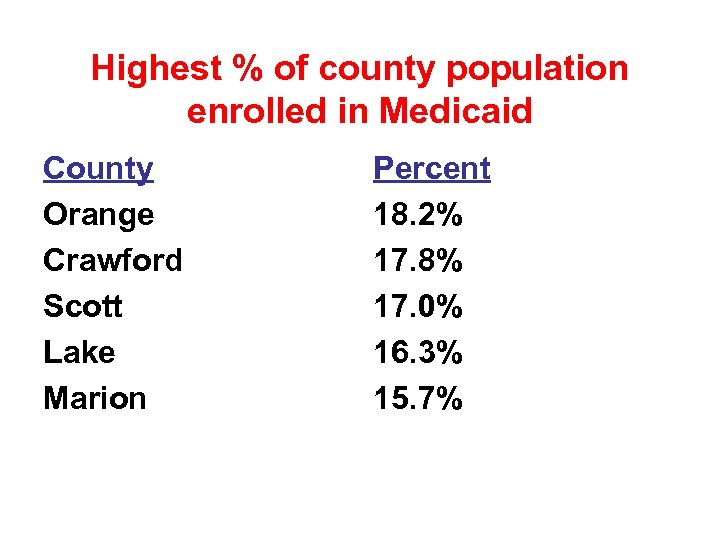 Highest % of county population enrolled in Medicaid County Orange Crawford Scott Lake Marion Percent 18. 2% 17. 8% 17. 0% 16. 3% 15. 7%
Highest % of county population enrolled in Medicaid County Orange Crawford Scott Lake Marion Percent 18. 2% 17. 8% 17. 0% 16. 3% 15. 7%
 Children’s Special Healthcare Services (CSHCS*) Program • Primary Care benefit • Dental care benefit • Specialty care (qualified serious chronic medical • • diagnosis - CP, CF**, M/M, Asthma, CHD, Cancer etc. “eligible medical conditions” only) Slightly more than 8, 300 patients statewide Used as a supplemental program (birth - 21 yr**) – eligibility 250% of FPL – Private insurance – Hoosier Healthwise for Children/Medicaid using CSHCS providers and obtaining prior authorization *formerly Crippled Children’s Program **CF on program for life
Children’s Special Healthcare Services (CSHCS*) Program • Primary Care benefit • Dental care benefit • Specialty care (qualified serious chronic medical • • diagnosis - CP, CF**, M/M, Asthma, CHD, Cancer etc. “eligible medical conditions” only) Slightly more than 8, 300 patients statewide Used as a supplemental program (birth - 21 yr**) – eligibility 250% of FPL – Private insurance – Hoosier Healthwise for Children/Medicaid using CSHCS providers and obtaining prior authorization *formerly Crippled Children’s Program **CF on program for life
 CSHCS - exclusions • Over the counter drugs and supplies • Mental health and substance abuse services • Prenatal or other pregnancy related care • ER visits or hospitalization un-associated • • with specific eligible diagnosis (fracture, appendicitis, hernia etc. ) Organ transplantation Eyeglasses, earplugs, diapers,
CSHCS - exclusions • Over the counter drugs and supplies • Mental health and substance abuse services • Prenatal or other pregnancy related care • ER visits or hospitalization un-associated • • with specific eligible diagnosis (fracture, appendicitis, hernia etc. ) Organ transplantation Eyeglasses, earplugs, diapers,
![Childhood deaths ages 1 -14 yrs • • All causes 1] Accidents 2] Cancer Childhood deaths ages 1 -14 yrs • • All causes 1] Accidents 2] Cancer](https://present5.com/presentation/c9805a844881a89ce2b99aa8fe84712b/image-19.jpg) Childhood deaths ages 1 -14 yrs • • All causes 1] Accidents 2] Cancer 3] Cong. Anomalies 4] Homicide 5] Cardiac disease 6] Resp. disease 7] Suicide Nat’l Center for Health Statistics 2002 12, 392 (22/100, 000) 4, 805 (8. 5/100, 000) 1, 434 (2. 5/100, 000) 894 (1. 6/100, 000) 727 (1. 3/100, 000) 452 (0. 8/100, 000) 380 (0. 6/100, 000) 307 (0. 3/100, 000)
Childhood deaths ages 1 -14 yrs • • All causes 1] Accidents 2] Cancer 3] Cong. Anomalies 4] Homicide 5] Cardiac disease 6] Resp. disease 7] Suicide Nat’l Center for Health Statistics 2002 12, 392 (22/100, 000) 4, 805 (8. 5/100, 000) 1, 434 (2. 5/100, 000) 894 (1. 6/100, 000) 727 (1. 3/100, 000) 452 (0. 8/100, 000) 380 (0. 6/100, 000) 307 (0. 3/100, 000)
 Obstetrical/Perinatal Problems • Appropriate Prenatal Care • Pre-eclampsia • Pitocin related Uterine rupture • Minority disparity infant mortality (2. 5 X) • Prematurity • Sepsis • Progeny of Diabetic mothers – IUGR, SGA • Birth Depression - neuromorbidity
Obstetrical/Perinatal Problems • Appropriate Prenatal Care • Pre-eclampsia • Pitocin related Uterine rupture • Minority disparity infant mortality (2. 5 X) • Prematurity • Sepsis • Progeny of Diabetic mothers – IUGR, SGA • Birth Depression - neuromorbidity
 Advances in neonatal care • High frequency ventilators – oscillators, more patient friendly (less barotrauma) • ECMO • Nitric oxide – pulmonary hypertension • Surfactant • Immunomodulation – enhance immune response (Monoclonal antibodies) • Stem cell alteration of immature tissues – replacement of damaged tissues • Gene therapy • Neuromorbidity – response to inflammatory cascade in premature infants
Advances in neonatal care • High frequency ventilators – oscillators, more patient friendly (less barotrauma) • ECMO • Nitric oxide – pulmonary hypertension • Surfactant • Immunomodulation – enhance immune response (Monoclonal antibodies) • Stem cell alteration of immature tissues – replacement of damaged tissues • Gene therapy • Neuromorbidity – response to inflammatory cascade in premature infants
 Very low birth rate survival Birth weight 1, 000 -1, 500 gms Survival >95% 750 -999 gms 80% 550 -600 gms 50%
Very low birth rate survival Birth weight 1, 000 -1, 500 gms Survival >95% 750 -999 gms 80% 550 -600 gms 50%
 Neonatal Surgery Ongoing problems • Necrotizing enterocolitis • Congenital diaphragmantic hernia • Giant omphalocele • Gastroschisis with loss of intestine • Short bowel syndrome – Extensive aganglionosis – Malrotation with midgut volvulus – Multiple atresias – Pseudo-obstruction – Microviullus disease – Trauma – Crohn’s disase
Neonatal Surgery Ongoing problems • Necrotizing enterocolitis • Congenital diaphragmantic hernia • Giant omphalocele • Gastroschisis with loss of intestine • Short bowel syndrome – Extensive aganglionosis – Malrotation with midgut volvulus – Multiple atresias – Pseudo-obstruction – Microviullus disease – Trauma – Crohn’s disase
 Obstacles to improved care • Managed Care • De-regionalization of Care • Unnecessary duplication of services in same community – competition for $$$ • Physician and hospital resistance • Identification of high risk pregnancies, prenatal diagnosis and referral of selected mothers to high risk centers with appropriate personnel, resources and programs in place (access)
Obstacles to improved care • Managed Care • De-regionalization of Care • Unnecessary duplication of services in same community – competition for $$$ • Physician and hospital resistance • Identification of high risk pregnancies, prenatal diagnosis and referral of selected mothers to high risk centers with appropriate personnel, resources and programs in place (access)
 Future Programs • Improved access to prenatal care • Reduce minority disparity in child mortality • Identify high risk pregnancies-selective referral of mothers prior to delivery • Categorize facilities regarding level of care – focus • • patients in facilities that provide the appropriate level of care according to severity Continued research to solve ongoing problems with premature labor and delivery and high mortality conditions (prematurity, NEC, CDH, Neuro-morbidity, sepsis Indiana Perinatal Network
Future Programs • Improved access to prenatal care • Reduce minority disparity in child mortality • Identify high risk pregnancies-selective referral of mothers prior to delivery • Categorize facilities regarding level of care – focus • • patients in facilities that provide the appropriate level of care according to severity Continued research to solve ongoing problems with premature labor and delivery and high mortality conditions (prematurity, NEC, CDH, Neuro-morbidity, sepsis Indiana Perinatal Network
 Childhood Trauma • Leading cause of death in children • No statewide trauma System in Indiana • No uniform pre-hospital standards • Patients taken to nearest facility – that may not be appropriate for trauma care • Local hospital may transfer patient to a parent hospital that is a non-trauma center facility
Childhood Trauma • Leading cause of death in children • No statewide trauma System in Indiana • No uniform pre-hospital standards • Patients taken to nearest facility – that may not be appropriate for trauma care • Local hospital may transfer patient to a parent hospital that is a non-trauma center facility
 Vehicular Accidents in Children • In 2001 there were(4 -14 yrs). 4% fatalities inoccupant 42, 116 traffic the US. 5% were children of vehicle • • • fatalities were children. Children represented 9% of all those injured (267, 000). Six children are killed and 732 injured daily in MVA. 23% that die are in alcohol related crashes. The number of childhood pedestrian fatalities have decreased in the past decade from 789 in 1991 to 444 in 2001. 85% of non-occupant fatalities. 69% occur in urban areas. 65% were boys. 50% on weekends, 45% between 3 -7: 00 PM. 47% alcohol related. 728 pedalcyclists were killed by MVA in 2001. 19% (n=137) were children < 15 yrs. 13% of non-occupant fatalities. Others 2% (Roller-skates, skate boards).
Vehicular Accidents in Children • In 2001 there were(4 -14 yrs). 4% fatalities inoccupant 42, 116 traffic the US. 5% were children of vehicle • • • fatalities were children. Children represented 9% of all those injured (267, 000). Six children are killed and 732 injured daily in MVA. 23% that die are in alcohol related crashes. The number of childhood pedestrian fatalities have decreased in the past decade from 789 in 1991 to 444 in 2001. 85% of non-occupant fatalities. 69% occur in urban areas. 65% were boys. 50% on weekends, 45% between 3 -7: 00 PM. 47% alcohol related. 728 pedalcyclists were killed by MVA in 2001. 19% (n=137) were children < 15 yrs. 13% of non-occupant fatalities. Others 2% (Roller-skates, skate boards).
 Childhood traffic accidents • Child Safety seats reduced the risk of (1 - 4 yr) by in fatal injury infants < 1 yr by 71% and for toddlers • • • 54%. Half of the children that died were unrestrained. Fewer children are restrained in rural settings than in urban areas and on weekends compared to weekday travel. Mortality is higher in rural areas because of ↓access to care School bus transportation is relatively safe: 26 deaths annually , only 6 were occupants of the bus and 19 were pedestrians (5 -7 yr old group)
Childhood traffic accidents • Child Safety seats reduced the risk of (1 - 4 yr) by in fatal injury infants < 1 yr by 71% and for toddlers • • • 54%. Half of the children that died were unrestrained. Fewer children are restrained in rural settings than in urban areas and on weekends compared to weekday travel. Mortality is higher in rural areas because of ↓access to care School bus transportation is relatively safe: 26 deaths annually , only 6 were occupants of the bus and 19 were pedestrians (5 -7 yr old group)
 Young drivers 15 -20 yrs Risky group • 190. 6 million licensed drivers in US. 6. 8% (12. 9 million) are between 15 -20 yrs old. • 8, 137 of 57, 480 fatal crashes involved drivers • 15 -20 years old (14%). 3, 608 drivers were killed. 1% decrease for boys but 15% increase for girls. This age group also girls involved in 17% of the car crashes (1. 8 million of 11. 1 million crashes). 33% invalid license, 31% drinking alcohol
Young drivers 15 -20 yrs Risky group • 190. 6 million licensed drivers in US. 6. 8% (12. 9 million) are between 15 -20 yrs old. • 8, 137 of 57, 480 fatal crashes involved drivers • 15 -20 years old (14%). 3, 608 drivers were killed. 1% decrease for boys but 15% increase for girls. This age group also girls involved in 17% of the car crashes (1. 8 million of 11. 1 million crashes). 33% invalid license, 31% drinking alcohol
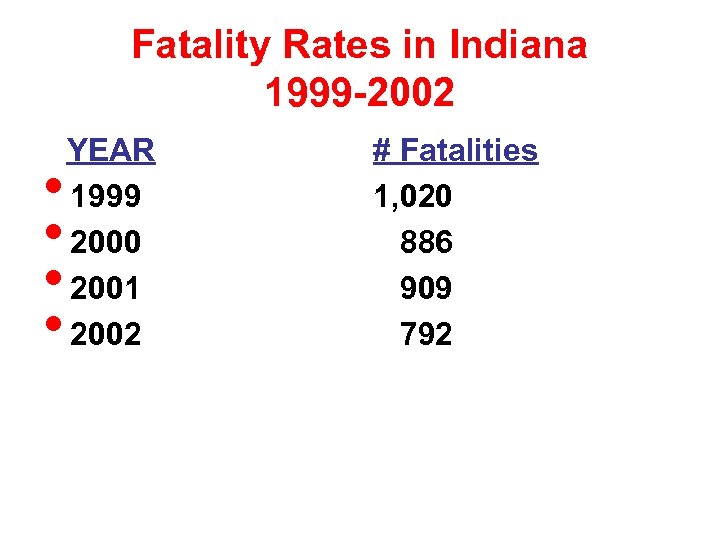 Fatality Rates in Indiana 1999 -2002 • • YEAR 1999 2000 2001 2002 # Fatalities 1, 020 886 909 792
Fatality Rates in Indiana 1999 -2002 • • YEAR 1999 2000 2001 2002 # Fatalities 1, 020 886 909 792
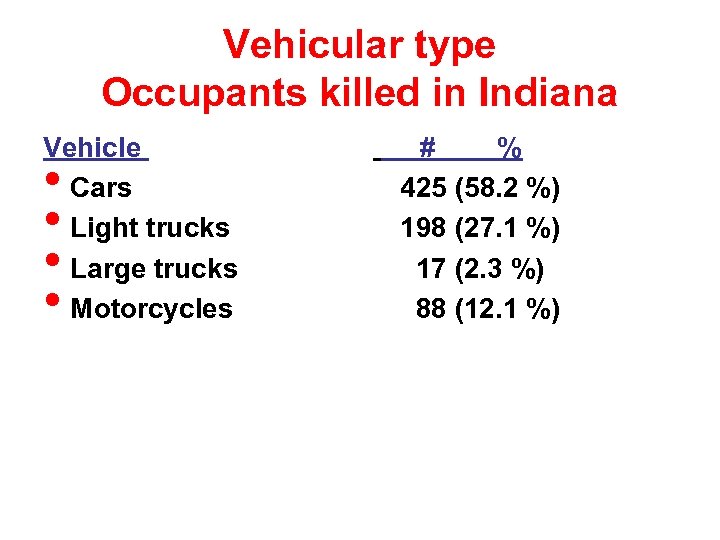 Vehicular type Occupants killed in Indiana Vehicle Cars Light trucks Large trucks Motorcycles • • # % 425 (58. 2 %) 198 (27. 1 %) 17 (2. 3 %) 88 (12. 1 %)
Vehicular type Occupants killed in Indiana Vehicle Cars Light trucks Large trucks Motorcycles • • # % 425 (58. 2 %) 198 (27. 1 %) 17 (2. 3 %) 88 (12. 1 %)
 Alcohol related crashes (Indiana) • 171 of 546 (31%) driver fatalities were related to alcohol • 269 of 792 total persons killed (34%) were related to alcohol Only 12% of drivers survived alcohol related crashes that involved fatalities •
Alcohol related crashes (Indiana) • 171 of 546 (31%) driver fatalities were related to alcohol • 269 of 792 total persons killed (34%) were related to alcohol Only 12% of drivers survived alcohol related crashes that involved fatalities •
 Childhood Trauma System • Develop pre-hospital standards of care • Develop EMS Hospital triage system – for • • patients defined as having a significant injury going to dedicated level 1 or 2 trauma center Develop hospital standards and performance guidelines Cost-effective Decreases mortality Improves outcomes
Childhood Trauma System • Develop pre-hospital standards of care • Develop EMS Hospital triage system – for • • patients defined as having a significant injury going to dedicated level 1 or 2 trauma center Develop hospital standards and performance guidelines Cost-effective Decreases mortality Improves outcomes
 Indiana Trauma Centers • Verified by the Committee on Trauma. American College of Surgeons • Level 1 (n=3) Methodist Hospital, • • Wishard Memorial Hospital, Riley Children’s Hospital (all in Indianapolis) Level 2 (n = 1) Fort Wayne None verified in South, East or West sectors of the state (South Bend, Evansville trying for Level 2)
Indiana Trauma Centers • Verified by the Committee on Trauma. American College of Surgeons • Level 1 (n=3) Methodist Hospital, • • Wishard Memorial Hospital, Riley Children’s Hospital (all in Indianapolis) Level 2 (n = 1) Fort Wayne None verified in South, East or West sectors of the state (South Bend, Evansville trying for Level 2)
 Trauma System • Permits triage to appropriate care facility based on severity of injury. • Permits injury pattern surveillance • Documents where injuries are occurring – urban vs. rural • Allows development of childhood (specific) injury prevention programs • Trauma education: ATLS, ACLS, BCLS, EMSC-program, ER/ICU Nurses program • Indiana State Committee on Trauma (ACS)
Trauma System • Permits triage to appropriate care facility based on severity of injury. • Permits injury pattern surveillance • Documents where injuries are occurring – urban vs. rural • Allows development of childhood (specific) injury prevention programs • Trauma education: ATLS, ACLS, BCLS, EMSC-program, ER/ICU Nurses program • Indiana State Committee on Trauma (ACS)
 Statewide “Safe-Kids” Program • Coordinated program-main base in Indianapolis • Lots of local chapters – • South Bend, Fort Wayne, Evansville, Porter County, Car seats, Fire-prevention, MVA, Pedestrian, water-safety, Falls, bicycle safety (helmets), fire-arms
Statewide “Safe-Kids” Program • Coordinated program-main base in Indianapolis • Lots of local chapters – • South Bend, Fort Wayne, Evansville, Porter County, Car seats, Fire-prevention, MVA, Pedestrian, water-safety, Falls, bicycle safety (helmets), fire-arms
 Child Abuse • A growing problem (1 million/yr abused) • 5, 000 deaths/yr in the US (27@day) • Riley Hospital: 200 cases/yr (most < 2 yrs) • • • 10 deaths/yr (5%) Lower socio-economic groups and younger parents more prone to commit abuse (financial and social stress) Some die at home (risk: ↑ 6 -12 mo old group) Increased societal exposure to violence ?
Child Abuse • A growing problem (1 million/yr abused) • 5, 000 deaths/yr in the US (27@day) • Riley Hospital: 200 cases/yr (most < 2 yrs) • • • 10 deaths/yr (5%) Lower socio-economic groups and younger parents more prone to commit abuse (financial and social stress) Some die at home (risk: ↑ 6 -12 mo old group) Increased societal exposure to violence ?
 Child Abuse: Patterns of injury Order of Frequency • Repetitive soft tissue injuries • Contusions, abrasions, lacerations, burns • Evidence of repetitive fractures (long bones, ribs, skull) • Solitary head injury, subdural hematoma, retinal hemorrhage • Visceral injuries – spleen, liver, duodenal • hematoma, pancreatic injury, renal, bowel perforation (often (50% ) fatal) < 3 yrs = abuse until proven otherwise
Child Abuse: Patterns of injury Order of Frequency • Repetitive soft tissue injuries • Contusions, abrasions, lacerations, burns • Evidence of repetitive fractures (long bones, ribs, skull) • Solitary head injury, subdural hematoma, retinal hemorrhage • Visceral injuries – spleen, liver, duodenal • hematoma, pancreatic injury, renal, bowel perforation (often (50% ) fatal) < 3 yrs = abuse until proven otherwise
 Child abuse • Physical abuse– battered child syndrome, shaken baby syndrome • Boys >> girls: mother, boyfriend, battering sibling, babysitter etc. • Sexual abuse – girls > 10 yrs: rape, incest • Psychological and emotional abuse • Child neglect: failure to thrive, nutritional deficiency/starvation, lack of supervision and hygienic neglect
Child abuse • Physical abuse– battered child syndrome, shaken baby syndrome • Boys >> girls: mother, boyfriend, battering sibling, babysitter etc. • Sexual abuse – girls > 10 yrs: rape, incest • Psychological and emotional abuse • Child neglect: failure to thrive, nutritional deficiency/starvation, lack of supervision and hygienic neglect
 Special types of child abuse • Growing International problem • Childhood slavery • Childhood soldiers (Africa, Middle East, Indonesia) • Adolescent prostitution (Asia, India, Africa) • Munchausen syndrome
Special types of child abuse • Growing International problem • Childhood slavery • Childhood soldiers (Africa, Middle East, Indonesia) • Adolescent prostitution (Asia, India, Africa) • Munchausen syndrome
 Child abuse Intervention • Verification of diagnosis – physician protected in reporting process • Breaking the cycle – immediate intervention, prevent subsequent injury • Treat child and the family • “family” rehabilitation, social services , long-term psychiatric care • 10% taken from the home permanently
Child abuse Intervention • Verification of diagnosis – physician protected in reporting process • Breaking the cycle – immediate intervention, prevent subsequent injury • Treat child and the family • “family” rehabilitation, social services , long-term psychiatric care • 10% taken from the home permanently
 Obesity in children • Prevalence is rising - has become an • • important public health issue referred to as the “obesity epidemic” Defined as a BMI (body mass index kg/m 2) of >95 percentile for age and sex. Overweight = BMI >85 percentile Indiana ranks 6 th in the nation. Obesity is observed in 14% of children nationally while 19 -20% of the children in Indiana are obese.
Obesity in children • Prevalence is rising - has become an • • important public health issue referred to as the “obesity epidemic” Defined as a BMI (body mass index kg/m 2) of >95 percentile for age and sex. Overweight = BMI >85 percentile Indiana ranks 6 th in the nation. Obesity is observed in 14% of children nationally while 19 -20% of the children in Indiana are obese.
 Childhood obesity • Strong genetic predisposition that facilitates storage of fat • Easy access to calorically dense foods • Low levels of physical activity that characterizes • • modern societies (couch potato, TV, “gameboy”mentality) Psychosocial stigma and medical consequences Hypertension, cardiovascular disease, metabolic, diabetes, sleep-apnea, orthopedic problems (osteoporosis, joint degeneration), neurologic, and increased risk of cancer in later life.
Childhood obesity • Strong genetic predisposition that facilitates storage of fat • Easy access to calorically dense foods • Low levels of physical activity that characterizes • • modern societies (couch potato, TV, “gameboy”mentality) Psychosocial stigma and medical consequences Hypertension, cardiovascular disease, metabolic, diabetes, sleep-apnea, orthopedic problems (osteoporosis, joint degeneration), neurologic, and increased risk of cancer in later life.
 Childhood obesity • There is a definite association between birth • • • weight and attained BMI. Higher birth weight has a tendency toward obesity. Parental adiposity is directly associated with offspring’s birth weight; Mom>>Dad Maternal diabetes and fetal hyperinsulinism? Effect on fat cell size and number? Reduced size at birth associated with central (truncal) obesity and increased cardiovascular risk, hypertension, dyslipidemia, diabetes and insulin resistance (“metabolic syndrome”)
Childhood obesity • There is a definite association between birth • • • weight and attained BMI. Higher birth weight has a tendency toward obesity. Parental adiposity is directly associated with offspring’s birth weight; Mom>>Dad Maternal diabetes and fetal hyperinsulinism? Effect on fat cell size and number? Reduced size at birth associated with central (truncal) obesity and increased cardiovascular risk, hypertension, dyslipidemia, diabetes and insulin resistance (“metabolic syndrome”)
 Prevention of obesity • An immediate Public Health challenge • No specific nationwide or Statewide policy or programs in place • Prevention starting in childhood is critical • Can have a life-long and perhaps multigenerational impact • Interventions directed toward improving diet, physical activity and sedentary activities is essential.
Prevention of obesity • An immediate Public Health challenge • No specific nationwide or Statewide policy or programs in place • Prevention starting in childhood is critical • Can have a life-long and perhaps multigenerational impact • Interventions directed toward improving diet, physical activity and sedentary activities is essential.
 Childhood obesity Interventional strategies • Psychological and family therapy • Lifestyle and behavior modification • Nutritional education and dietary modification • Regular physical exercise • Drugs not recommended in children • Surgical intervention for extremely obese patients (adolescents) the treatment of last resort (BMI >45 -50 kg/m 2)
Childhood obesity Interventional strategies • Psychological and family therapy • Lifestyle and behavior modification • Nutritional education and dietary modification • Regular physical exercise • Drugs not recommended in children • Surgical intervention for extremely obese patients (adolescents) the treatment of last resort (BMI >45 -50 kg/m 2)
 Childhood obesity Surgical management • Bariatric surgery is effective in managing severely • • • obese adolescent patients that fail conservative treatment programs. Gastric by-pass procedure effective Laparoscopic minimally invasive approach is safe, reduces morbidity, fewer wound infections, avoids scars, ventral hernias, reduces postoperative pain requirements, shortens hospital stay, more rapid recovery Treatment should be carried out in centers with comprehensive, multidisciplinary childhood obesity prevention/management programs.
Childhood obesity Surgical management • Bariatric surgery is effective in managing severely • • • obese adolescent patients that fail conservative treatment programs. Gastric by-pass procedure effective Laparoscopic minimally invasive approach is safe, reduces morbidity, fewer wound infections, avoids scars, ventral hernias, reduces postoperative pain requirements, shortens hospital stay, more rapid recovery Treatment should be carried out in centers with comprehensive, multidisciplinary childhood obesity prevention/management programs.
 Future Goals • Improve health care quality, utilization and outcomes • Statewide Trauma System – optimal • • • trauma care and injury prevention programs Perinatal Statewide Network Health Maintenance Programs Electronic records and tracking system for outreach and outcomes studies. Telemedicine and informatics.
Future Goals • Improve health care quality, utilization and outcomes • Statewide Trauma System – optimal • • • trauma care and injury prevention programs Perinatal Statewide Network Health Maintenance Programs Electronic records and tracking system for outreach and outcomes studies. Telemedicine and informatics.
 Programs • Chronic disease management programs –Children with Special Health Care Needs –Coalition for Childhood Obesity –Childhood Type 2 Diabetes Studies –Statewide Asthma Coalition –Childhood Cancer • Need more adequate funding specifically for children to integrate new information, technology, treatment and education into the health care package for children
Programs • Chronic disease management programs –Children with Special Health Care Needs –Coalition for Childhood Obesity –Childhood Type 2 Diabetes Studies –Statewide Asthma Coalition –Childhood Cancer • Need more adequate funding specifically for children to integrate new information, technology, treatment and education into the health care package for children
 Medicaid Funding • Three top expenditures: nursing homes(25%), pharmacy and hospital care • Indiana has a significant overcapacity of • nursing home beds. With a cost based reimbursement scheme – paying for empty beds instead of needed services. Medicaid covers 2 out of 3 nursing home beds in the state. Children represent 64. 3 % of the recipients but only receive 22% of the Medicaid funding
Medicaid Funding • Three top expenditures: nursing homes(25%), pharmacy and hospital care • Indiana has a significant overcapacity of • nursing home beds. With a cost based reimbursement scheme – paying for empty beds instead of needed services. Medicaid covers 2 out of 3 nursing home beds in the state. Children represent 64. 3 % of the recipients but only receive 22% of the Medicaid funding
 Medicaid funding • Estimated projected expenses $4. 3 billion in • • • 2004 and $4. 75 billion in 2005. But MK frozen at the 2003 rate despite adding more recipients (mainly adults). Disproportionate share also reduced by $19 million in 2003. As the population ages their expenditures will threaten other areas of the program i. e. the children. The system needs to change – our children represent our future. We need to improve their care.
Medicaid funding • Estimated projected expenses $4. 3 billion in • • • 2004 and $4. 75 billion in 2005. But MK frozen at the 2003 rate despite adding more recipients (mainly adults). Disproportionate share also reduced by $19 million in 2003. As the population ages their expenditures will threaten other areas of the program i. e. the children. The system needs to change – our children represent our future. We need to improve their care.
 About change • Adversity often opens new windows of opportunity to improve upon the past. • Failure to adapt appropriately to change may lead to extinction. • We must embrace change with open arms but never change our values.
About change • Adversity often opens new windows of opportunity to improve upon the past. • Failure to adapt appropriately to change may lead to extinction. • We must embrace change with open arms but never change our values.
 Response to change “ Change is the law of life, and those who look only to the past or the present are certain to miss the future” John F. Kennedy
Response to change “ Change is the law of life, and those who look only to the past or the present are certain to miss the future” John F. Kennedy


