057431cbcefa68446ede9133a455ee80.ppt
- Количество слайдов: 27
 Impact of the 80 Hour Workweek on Surgical Case Exposure Within a General Surgery Residency Daniel R. Watson, MD Timothy D. Flesher Oscar Ruiz, MD Josh Chung, MD Riverside Methodist Hospital, Columbus, Ohio
Impact of the 80 Hour Workweek on Surgical Case Exposure Within a General Surgery Residency Daniel R. Watson, MD Timothy D. Flesher Oscar Ruiz, MD Josh Chung, MD Riverside Methodist Hospital, Columbus, Ohio
 Impact of the 80 Hour Workweek The role and training of the general surgical resident has perpetually evolved since its inception in the mid 19 th century. Most recently, the Accreditation Council for Graduate Medical Education’s (ACGME) resident workweek regulations, instituted on July 1, 2003, have been a major influence on the present structure of residency training.
Impact of the 80 Hour Workweek The role and training of the general surgical resident has perpetually evolved since its inception in the mid 19 th century. Most recently, the Accreditation Council for Graduate Medical Education’s (ACGME) resident workweek regulations, instituted on July 1, 2003, have been a major influence on the present structure of residency training.
 Impact of the 80 Hour Workweek The 80 -hour work week was created in response to medical educators and the public’s concern for patient safety. In the field of surgical training, the impact of the new work week regulations on operative experience has become a grave concern, relative to the conventional paradigm. Although resident quality of life has been reported as improved, there is still much debate as to the effect that the new restrictions will have on general surgery resident education and surgical training.
Impact of the 80 Hour Workweek The 80 -hour work week was created in response to medical educators and the public’s concern for patient safety. In the field of surgical training, the impact of the new work week regulations on operative experience has become a grave concern, relative to the conventional paradigm. Although resident quality of life has been reported as improved, there is still much debate as to the effect that the new restrictions will have on general surgery resident education and surgical training.
 Skilled Surgeons-the Legacy Harvey W. Cushing, M. D. Theodore Billroth, M. D. Oscar Ruiz, M. D. Emil Theodor Kocher, M. D. Michael E. De. Bakey, M. D.
Skilled Surgeons-the Legacy Harvey W. Cushing, M. D. Theodore Billroth, M. D. Oscar Ruiz, M. D. Emil Theodor Kocher, M. D. Michael E. De. Bakey, M. D.
 80 Hour Workweek “ 10, 000 hour rule” -- Malcolm Gladwell Key to success in any field is, to a large extent, a matter of practicing a specific task for a total of atleast 10, 000 hours. Surgery is similar to activities such as practicing piano or playing hockey Need for repetition and consistency Practice makes perfect. Less practice, …?
80 Hour Workweek “ 10, 000 hour rule” -- Malcolm Gladwell Key to success in any field is, to a large extent, a matter of practicing a specific task for a total of atleast 10, 000 hours. Surgery is similar to activities such as practicing piano or playing hockey Need for repetition and consistency Practice makes perfect. Less practice, …?
 Impact of the 80 Hour Workweek Numerous studies have been conducted to evaluate the effects of the work week regulation on surgical training. Conflicting evidence continues to emerge regarding the potential risks and benefits associated with resident duty-hour restrictions.
Impact of the 80 Hour Workweek Numerous studies have been conducted to evaluate the effects of the work week regulation on surgical training. Conflicting evidence continues to emerge regarding the potential risks and benefits associated with resident duty-hour restrictions.
 80 Hour Workweek When the Residency Review Committee considered General Surgery Resident case logs across the country between 1997 and 2004, they found no decrease in the average number of cases performed per resident in the 2003 -2004 year. The Committee concluded that resident surgical volume was not affected by the new work-hour restrictions
80 Hour Workweek When the Residency Review Committee considered General Surgery Resident case logs across the country between 1997 and 2004, they found no decrease in the average number of cases performed per resident in the 2003 -2004 year. The Committee concluded that resident surgical volume was not affected by the new work-hour restrictions
 Study Objective Now that a 5 -year cycle is complete, we sought to test the hypothesis that restrictions on the 80 hour workweek for General Surgery Residents at Riverside Methodist Hospital implemented after July 2003 significantly decreased the volume of operative cases performed by surgical residents, compared to surgical residents at Riverside training prior to July 2003.
Study Objective Now that a 5 -year cycle is complete, we sought to test the hypothesis that restrictions on the 80 hour workweek for General Surgery Residents at Riverside Methodist Hospital implemented after July 2003 significantly decreased the volume of operative cases performed by surgical residents, compared to surgical residents at Riverside training prior to July 2003.
 Methods Data were collected from the Accreditation Council for Graduate Medical Education (ACGME) national database and from Riverside Hospital’s General Surgery Residency files for a sampling of academic years before and after the duty-hour changes in surgical education (July 1, 2003). CPT surgical procedure codes logged by PGY-5 General Surgery residents 15 years before and 5 years after implementation of the 80 -hour workweek were compared. Total General Surgery Department volume per year was also compared to this data.
Methods Data were collected from the Accreditation Council for Graduate Medical Education (ACGME) national database and from Riverside Hospital’s General Surgery Residency files for a sampling of academic years before and after the duty-hour changes in surgical education (July 1, 2003). CPT surgical procedure codes logged by PGY-5 General Surgery residents 15 years before and 5 years after implementation of the 80 -hour workweek were compared. Total General Surgery Department volume per year was also compared to this data.
 The Riverside Methodist Hospital General Surgery Residency program accepts two categorical surgical residents each year into a 5 -year program, covering a 1000 bed medical center.
The Riverside Methodist Hospital General Surgery Residency program accepts two categorical surgical residents each year into a 5 -year program, covering a 1000 bed medical center.
 Methods The outcome variables “PGY-5 Cases” and “Major Cases” (the aggregate number of cases done during their resident tenure) were compared between two study groups defined by the time intervals exclusively before July 2003 (“pre”) and inclusively after July 2003 (“post”). Statistical analyses included one-sided and two-sided t-tests, non-parametric tests, and t-tests on a 3 -parameter logarithmic transformation of the raw data to satisfy normality and equal variance assumptions necessary for ttesting.
Methods The outcome variables “PGY-5 Cases” and “Major Cases” (the aggregate number of cases done during their resident tenure) were compared between two study groups defined by the time intervals exclusively before July 2003 (“pre”) and inclusively after July 2003 (“post”). Statistical analyses included one-sided and two-sided t-tests, non-parametric tests, and t-tests on a 3 -parameter logarithmic transformation of the raw data to satisfy normality and equal variance assumptions necessary for ttesting.
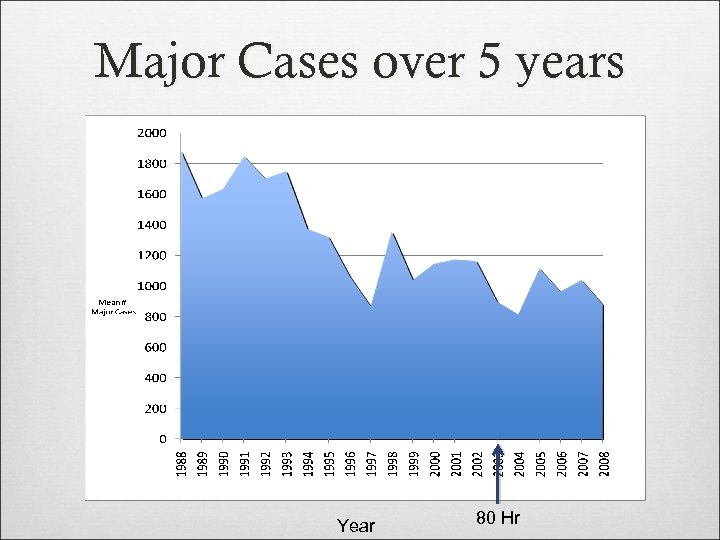 Major Cases over 5 years Year 80 Hr
Major Cases over 5 years Year 80 Hr
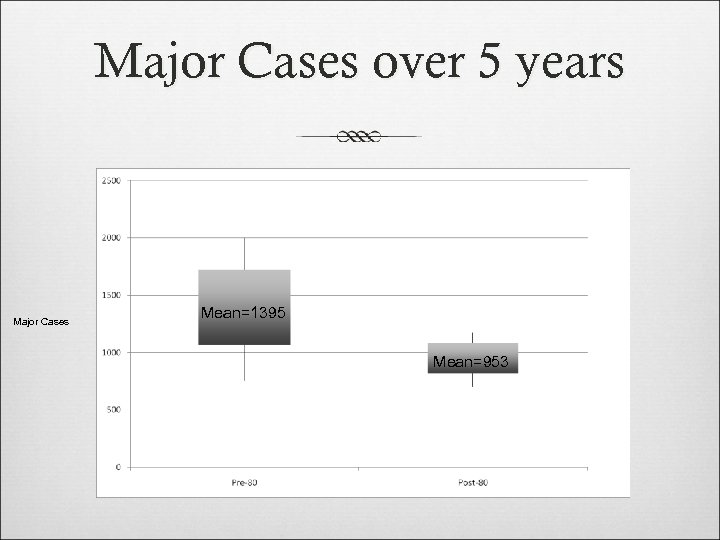 Major Cases over 5 years Major Cases Mean=1395 Mean=953
Major Cases over 5 years Major Cases Mean=1395 Mean=953
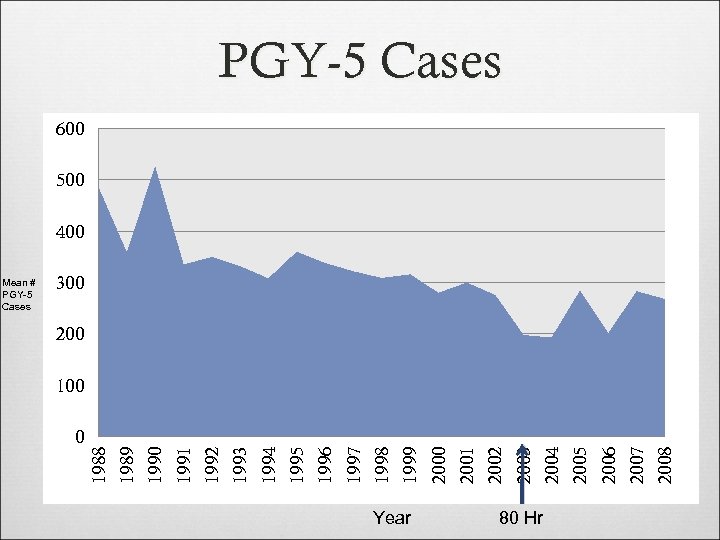 0 Year 80 Hr 2008 2007 2006 2005 2004 2003 2002 2001 2000 1999 1998 1997 1996 1995 1994 1993 1992 1991 1990 1989 Mean # PGY-5 Cases 1988 PGY-5 Cases 600 500 400 300 200 100
0 Year 80 Hr 2008 2007 2006 2005 2004 2003 2002 2001 2000 1999 1998 1997 1996 1995 1994 1993 1992 1991 1990 1989 Mean # PGY-5 Cases 1988 PGY-5 Cases 600 500 400 300 200 100
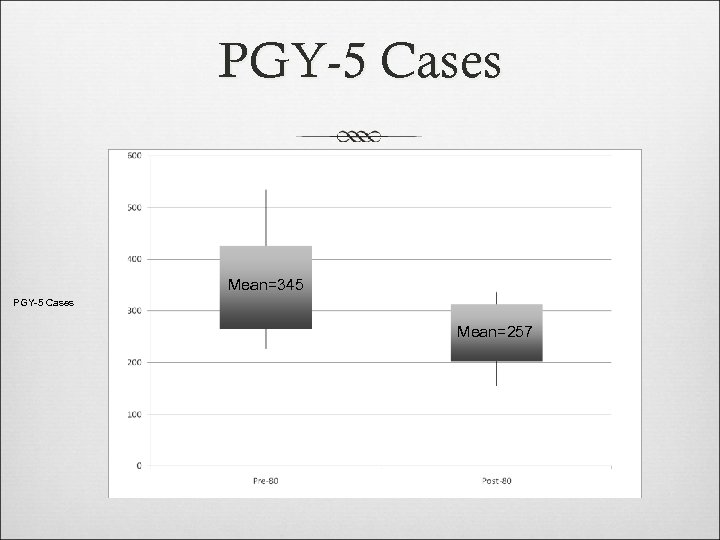 PGY-5 Cases Mean=345 PGY-5 Cases Mean=257
PGY-5 Cases Mean=345 PGY-5 Cases Mean=257
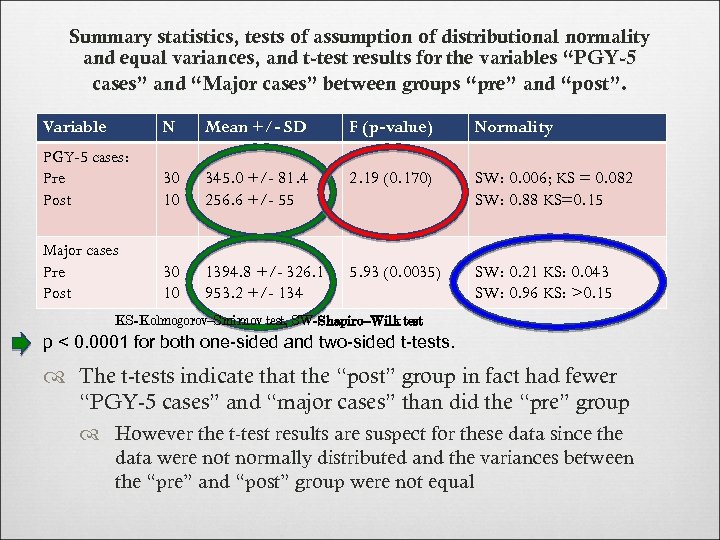 Summary statistics, tests of assumption of distributional normality and equal variances, and t-test results for the variables “PGY-5 cases” and “Major cases” between groups “pre” and “post”. Variable N Mean +/- SD F (p-value) Normality PGY-5 cases: Pre Post 30 10 345. 0 +/- 81. 4 256. 6 +/- 55 2. 19 (0. 170) SW: 0. 006; KS = 0. 082 SW: 0. 88 KS=0. 15 Major cases Pre Post 30 10 1394. 8 +/- 326. 1 953. 2 +/- 134 5. 93 (0. 0035) SW: 0. 21 KS: 0. 043 SW: 0. 96 KS: >0. 15 KS=Kolmogorov–Smirnov test, SW=Shapiro–Wilk test p < 0. 0001 for both one-sided and two-sided t-tests. The t-tests indicate that the “post” group in fact had fewer “PGY-5 cases” and “major cases” than did the “pre” group However the t-test results are suspect for these data since the data were not normally distributed and the variances between the “pre” and “post” group were not equal
Summary statistics, tests of assumption of distributional normality and equal variances, and t-test results for the variables “PGY-5 cases” and “Major cases” between groups “pre” and “post”. Variable N Mean +/- SD F (p-value) Normality PGY-5 cases: Pre Post 30 10 345. 0 +/- 81. 4 256. 6 +/- 55 2. 19 (0. 170) SW: 0. 006; KS = 0. 082 SW: 0. 88 KS=0. 15 Major cases Pre Post 30 10 1394. 8 +/- 326. 1 953. 2 +/- 134 5. 93 (0. 0035) SW: 0. 21 KS: 0. 043 SW: 0. 96 KS: >0. 15 KS=Kolmogorov–Smirnov test, SW=Shapiro–Wilk test p < 0. 0001 for both one-sided and two-sided t-tests. The t-tests indicate that the “post” group in fact had fewer “PGY-5 cases” and “major cases” than did the “pre” group However the t-test results are suspect for these data since the data were not normally distributed and the variances between the “pre” and “post” group were not equal
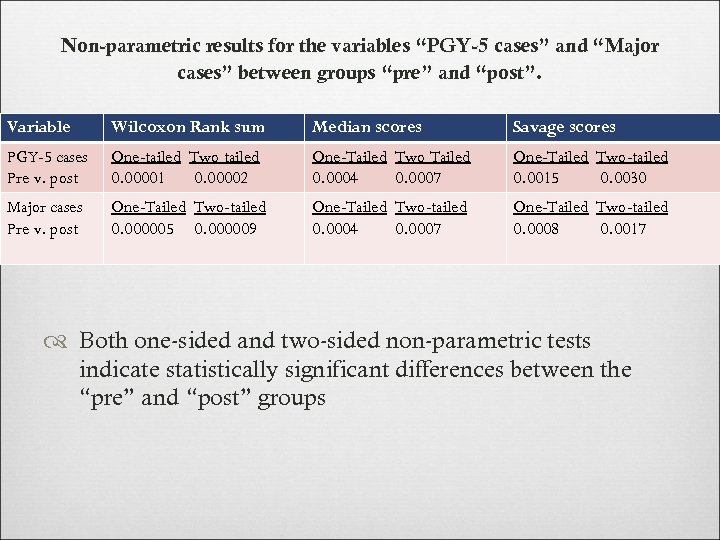 Non-parametric results for the variables “PGY-5 cases” and “Major cases” between groups “pre” and “post”. Variable Wilcoxon Rank sum Median scores Savage scores PGY-5 cases Pre v. post One-tailed Two tailed 0. 00001 0. 00002 One-Tailed Two Tailed 0. 0004 0. 0007 One-Tailed Two-tailed 0. 0015 0. 0030 Major cases Pre v. post One-Tailed Two-tailed 0. 000005 0. 000009 One-Tailed Two-tailed 0. 0004 0. 0007 One-Tailed Two-tailed 0. 0008 0. 0017 Both one-sided and two-sided non-parametric tests indicate statistically significant differences between the “pre” and “post” groups
Non-parametric results for the variables “PGY-5 cases” and “Major cases” between groups “pre” and “post”. Variable Wilcoxon Rank sum Median scores Savage scores PGY-5 cases Pre v. post One-tailed Two tailed 0. 00001 0. 00002 One-Tailed Two Tailed 0. 0004 0. 0007 One-Tailed Two-tailed 0. 0015 0. 0030 Major cases Pre v. post One-Tailed Two-tailed 0. 000005 0. 000009 One-Tailed Two-tailed 0. 0004 0. 0007 One-Tailed Two-tailed 0. 0008 0. 0017 Both one-sided and two-sided non-parametric tests indicate statistically significant differences between the “pre” and “post” groups
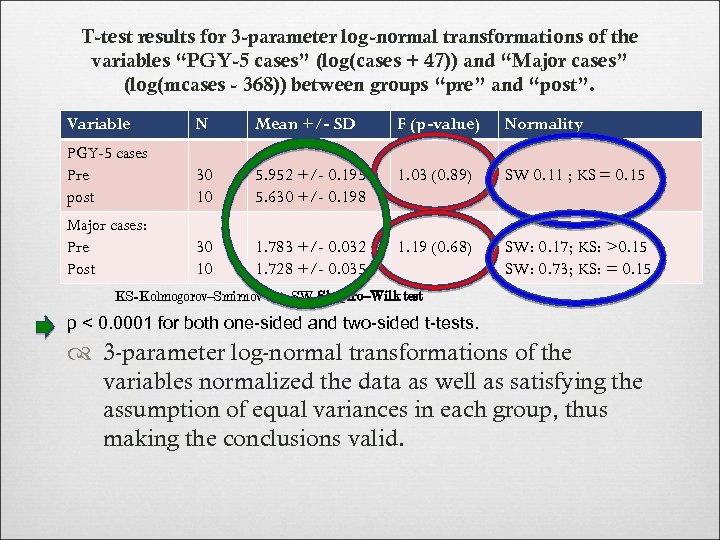 T-test results for 3 -parameter log-normal transformations of the variables “PGY-5 cases” (log(cases + 47)) and “Major cases” (log(mcases - 368)) between groups “pre” and “post”. Variable N Mean +/- SD F (p-value) Normality PGY-5 cases Pre post 30 10 5. 952 +/- 0. 195 5. 630 +/- 0. 198 1. 03 (0. 89) SW 0. 11 ; KS = 0. 15 Major cases: Pre Post 30 10 1. 783 +/- 0. 032 1. 728 +/- 0. 035 1. 19 (0. 68) SW: 0. 17; KS: >0. 15 SW: 0. 73; KS: = 0. 15 KS=Kolmogorov–Smirnov test, SW=Shapiro–Wilk test p < 0. 0001 for both one-sided and two-sided t-tests. 3 -parameter log-normal transformations of the variables normalized the data as well as satisfying the assumption of equal variances in each group, thus making the conclusions valid.
T-test results for 3 -parameter log-normal transformations of the variables “PGY-5 cases” (log(cases + 47)) and “Major cases” (log(mcases - 368)) between groups “pre” and “post”. Variable N Mean +/- SD F (p-value) Normality PGY-5 cases Pre post 30 10 5. 952 +/- 0. 195 5. 630 +/- 0. 198 1. 03 (0. 89) SW 0. 11 ; KS = 0. 15 Major cases: Pre Post 30 10 1. 783 +/- 0. 032 1. 728 +/- 0. 035 1. 19 (0. 68) SW: 0. 17; KS: >0. 15 SW: 0. 73; KS: = 0. 15 KS=Kolmogorov–Smirnov test, SW=Shapiro–Wilk test p < 0. 0001 for both one-sided and two-sided t-tests. 3 -parameter log-normal transformations of the variables normalized the data as well as satisfying the assumption of equal variances in each group, thus making the conclusions valid.
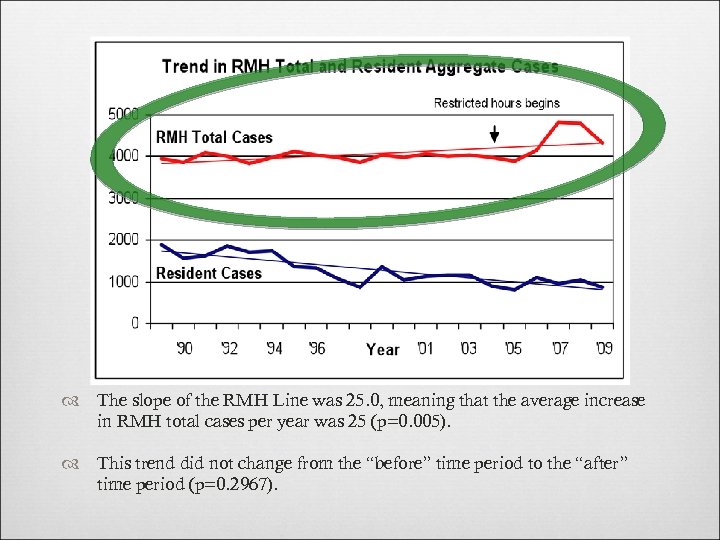 The slope of the RMH Line was 25. 0, meaning that the average increase in RMH total cases per year was 25 (p=0. 005). This trend did not change from the “before” time period to the “after” time period (p=0. 2967).
The slope of the RMH Line was 25. 0, meaning that the average increase in RMH total cases per year was 25 (p=0. 005). This trend did not change from the “before” time period to the “after” time period (p=0. 2967).
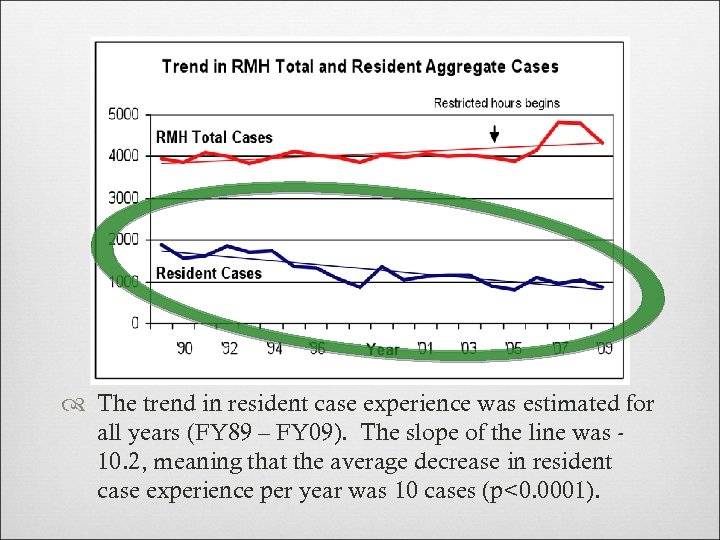 The trend in resident case experience was estimated for all years (FY 89 – FY 09). The slope of the line was 10. 2, meaning that the average decrease in resident case experience per year was 10 cases (p<0. 0001).
The trend in resident case experience was estimated for all years (FY 89 – FY 09). The slope of the line was 10. 2, meaning that the average decrease in resident case experience per year was 10 cases (p<0. 0001).
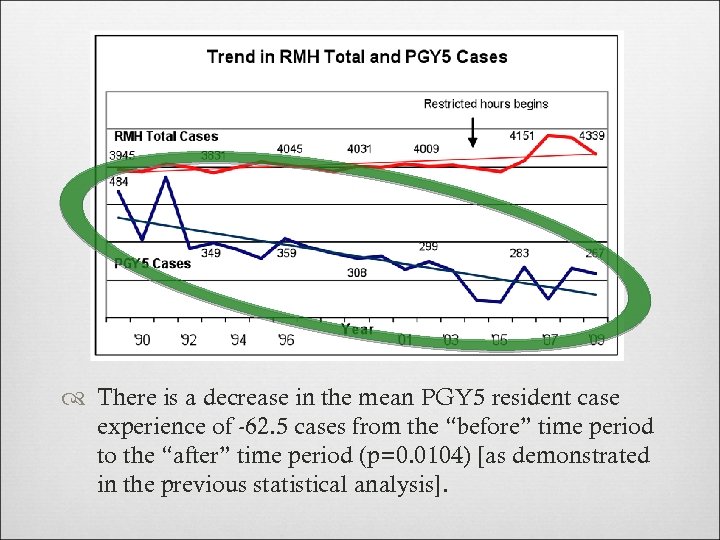 There is a decrease in the mean PGY 5 resident case experience of -62. 5 cases from the “before” time period to the “after” time period (p=0. 0104) [as demonstrated in the previous statistical analysis].
There is a decrease in the mean PGY 5 resident case experience of -62. 5 cases from the “before” time period to the “after” time period (p=0. 0104) [as demonstrated in the previous statistical analysis].
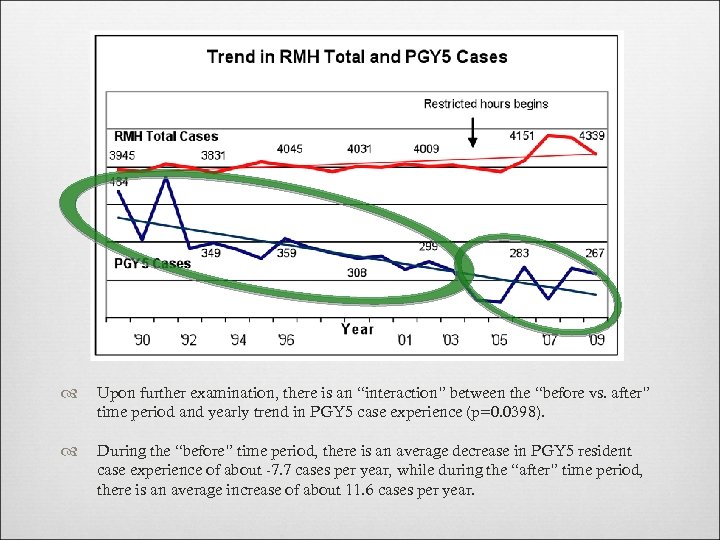 Upon further examination, there is an “interaction” between the “before vs. after” time period and yearly trend in PGY 5 case experience (p=0. 0398). During the “before” time period, there is an average decrease in PGY 5 resident case experience of about -7. 7 cases per year, while during the “after” time period, there is an average increase of about 11. 6 cases per year.
Upon further examination, there is an “interaction” between the “before vs. after” time period and yearly trend in PGY 5 case experience (p=0. 0398). During the “before” time period, there is an average decrease in PGY 5 resident case experience of about -7. 7 cases per year, while during the “after” time period, there is an average increase of about 11. 6 cases per year.
 Conclusions Restrictions dictated by the 80 hour work week for surgical residents at Riverside Methodist Hospital implemented after July 2003 decreased the volume of operative cases performed by surgical residents during both their junior and PGY-5 years, as compared to surgical residents prior to July 2003, determined by non-parametric tests and t-tests on transformed data. This decrease was not influenced by overall surgical volume
Conclusions Restrictions dictated by the 80 hour work week for surgical residents at Riverside Methodist Hospital implemented after July 2003 decreased the volume of operative cases performed by surgical residents during both their junior and PGY-5 years, as compared to surgical residents prior to July 2003, determined by non-parametric tests and t-tests on transformed data. This decrease was not influenced by overall surgical volume
 Conclusions/RMH Action Recognition of the change in culture within the program Increase Physician Extenders Attending coverage of Senior Call Elimination of Senior “Night-Float” Attending Mentors- Optimize Quality-time
Conclusions/RMH Action Recognition of the change in culture within the program Increase Physician Extenders Attending coverage of Senior Call Elimination of Senior “Night-Float” Attending Mentors- Optimize Quality-time
 Implications The ACGME-mandated 80 -hour work week restrictions have challenged surgical educators to creatively reduce work hours while trying to maintain the same high standard of surgical resident education. There is no easy answer as to how to accomplish this, nor is it yet clear whether the future U. S. -trained general surgeon will have the same level of clinical competence as in the past. It is incumbent on each individual surgery program to devise strategies to maintain the legacy of excellence in surgical education.
Implications The ACGME-mandated 80 -hour work week restrictions have challenged surgical educators to creatively reduce work hours while trying to maintain the same high standard of surgical resident education. There is no easy answer as to how to accomplish this, nor is it yet clear whether the future U. S. -trained general surgeon will have the same level of clinical competence as in the past. It is incumbent on each individual surgery program to devise strategies to maintain the legacy of excellence in surgical education.
 Impact of the 80 Hour Workweek on Surgical Case Exposure Within a General Surgery Residency Daniel R. Watson, MD Timothy D. Fletcher Oscar Ruiz, MD
Impact of the 80 Hour Workweek on Surgical Case Exposure Within a General Surgery Residency Daniel R. Watson, MD Timothy D. Fletcher Oscar Ruiz, MD
 ABSITE Influence?
ABSITE Influence?


