52441f814f1d49e5286153a315cf3027.ppt
- Количество слайдов: 46
 I solemnly pledge myself to consecrate my life to the service of humanity; I will give to my teachers the respect and gratitude which is their due; I will practice my profession with conscience and dignity; I will respect the secrets, which are confided in me, even after the patient has died; I will maintain by all the means in my power, the honour of the noble traditions of the medical profession; My colleagues will be my brothers; I will not permit considerations of religion, nationality, race, party politics or social standing to intervene between my duty and my patients; I will maintain the utmost respect for human life from its beginning even under threat, and I will not use my medical knowledge contrary to the laws of humanity; I will make these promises solemnly, freely and upon honour.
I solemnly pledge myself to consecrate my life to the service of humanity; I will give to my teachers the respect and gratitude which is their due; I will practice my profession with conscience and dignity; I will respect the secrets, which are confided in me, even after the patient has died; I will maintain by all the means in my power, the honour of the noble traditions of the medical profession; My colleagues will be my brothers; I will not permit considerations of religion, nationality, race, party politics or social standing to intervene between my duty and my patients; I will maintain the utmost respect for human life from its beginning even under threat, and I will not use my medical knowledge contrary to the laws of humanity; I will make these promises solemnly, freely and upon honour.

 Functions of the Medical Council Ø………. ØExercise and maintain discipline in the practice of medicine with the assistance of its Medical Disciplinary Tribunal ØEstablish a code of practice for the medical profession on standards of professional conduct and medical ethics and monitor compliance with such a code
Functions of the Medical Council Ø………. ØExercise and maintain discipline in the practice of medicine with the assistance of its Medical Disciplinary Tribunal ØEstablish a code of practice for the medical profession on standards of professional conduct and medical ethics and monitor compliance with such a code
 13. 1 -PRELIMINARY INVESTGATION BY COUNCIL “Subject to section 18, the Council may investigate any complaint of -professional misconduct, -Malpractice, -Dishonesty or -Negligence or -A breach of the code of practice against a registered person including a public officer in respect of whom it holds a delegated power.
13. 1 -PRELIMINARY INVESTGATION BY COUNCIL “Subject to section 18, the Council may investigate any complaint of -professional misconduct, -Malpractice, -Dishonesty or -Negligence or -A breach of the code of practice against a registered person including a public officer in respect of whom it holds a delegated power.
 COMPLAINT RECEIVED AT COUNCIL Possible fault on the part of M. P • Medical practitioner not concerned • No obvious fault of doctor Preliminary Investigation (I. C)(Section 13) Council informed Notify Doctor of the nature of the complaint Summon and hear doctor +/-complainant Summon and hear witness Call for documents Judge in chambers(if refusal by a person to give evidence or communicate document on ground of confidentiality Set aside Complainant informed
COMPLAINT RECEIVED AT COUNCIL Possible fault on the part of M. P • Medical practitioner not concerned • No obvious fault of doctor Preliminary Investigation (I. C)(Section 13) Council informed Notify Doctor of the nature of the complaint Summon and hear doctor +/-complainant Summon and hear witness Call for documents Judge in chambers(if refusal by a person to give evidence or communicate document on ground of confidentiality Set aside Complainant informed
 Evidence of fault of doctor Section 14(1) No prima facie evidence of fault of doctor Section 14(2) Charges drafted Set aside • Breach of code of • Prima facie evidence of practice negligence, incompetence or Inform MDT grave misconduct • Act of fraud, dishonesty, • Public interest requires that Report to Council not >14 negligence the registered person should days after completion of • Act of professional instantly cease to practice proceedings medicine misconduct or malpractice • Any other act likely to bring the medical profession into disrepute doctor & complainant Suspend for not > 6 mths Private Disciplinary Proceedings • Show cause • Warning/severe warning Inform doctor & complainant Cont/d Public officer (+delegation of power) Report to PSC for decision on suspension D Proceedings cont/d
Evidence of fault of doctor Section 14(1) No prima facie evidence of fault of doctor Section 14(2) Charges drafted Set aside • Breach of code of • Prima facie evidence of practice negligence, incompetence or Inform MDT grave misconduct • Act of fraud, dishonesty, • Public interest requires that Report to Council not >14 negligence the registered person should days after completion of • Act of professional instantly cease to practice proceedings medicine misconduct or malpractice • Any other act likely to bring the medical profession into disrepute doctor & complainant Suspend for not > 6 mths Private Disciplinary Proceedings • Show cause • Warning/severe warning Inform doctor & complainant Cont/d Public officer (+delegation of power) Report to PSC for decision on suspension D Proceedings cont/d
 17(3) Charges not proven • Charges proven • Aggravating/alleviating circumstance 17(4)a Public Officer (+delegated power) 17(4) b Every Other Case • Warning/severe warning • Reprimand/severe reprimand Report to PSC • Suspension from medical practice for not>12 months • Removal of name from register Set Aside Inform doctor & complainant
17(3) Charges not proven • Charges proven • Aggravating/alleviating circumstance 17(4)a Public Officer (+delegated power) 17(4) b Every Other Case • Warning/severe warning • Reprimand/severe reprimand Report to PSC • Suspension from medical practice for not>12 months • Removal of name from register Set Aside Inform doctor & complainant
 17(5) Punishment (Dismissal or Retirement) by PSC COUNCIL Removal of name from the Register • Decision under 17(4) or (5): inform doctor within 14 days
17(5) Punishment (Dismissal or Retirement) by PSC COUNCIL Removal of name from the Register • Decision under 17(4) or (5): inform doctor within 14 days
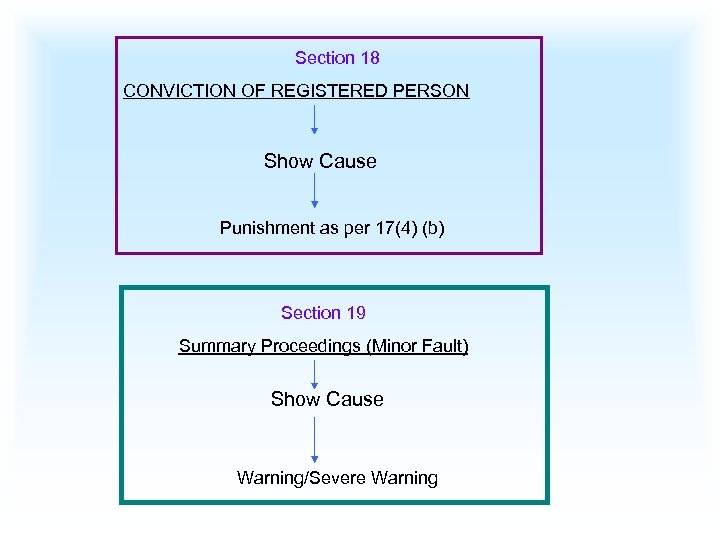 Section 18 CONVICTION OF REGISTERED PERSON Show Cause Punishment as per 17(4) (b) Section 19 Summary Proceedings (Minor Fault) Show Cause Warning/Severe Warning
Section 18 CONVICTION OF REGISTERED PERSON Show Cause Punishment as per 17(4) (b) Section 19 Summary Proceedings (Minor Fault) Show Cause Warning/Severe Warning
 ØPreliminary Investigation – Evidence based -Accepted practice - Literature - Expert opinion - Written explanations/interview of defendant doctor - Interview of complainant party - Documents: patient file, Investigations ØDeliberations at Council - Views of full board - Composition of Council -Doctors : public/private : General practitioner/specialist -Nominated members (non-medical) -1 Rep. each from PMO, MOH, SLO -vote ± casting vote of Chairman ØSanction- Show cause ØJudicial review – aggrieved parties.
ØPreliminary Investigation – Evidence based -Accepted practice - Literature - Expert opinion - Written explanations/interview of defendant doctor - Interview of complainant party - Documents: patient file, Investigations ØDeliberations at Council - Views of full board - Composition of Council -Doctors : public/private : General practitioner/specialist -Nominated members (non-medical) -1 Rep. each from PMO, MOH, SLO -vote ± casting vote of Chairman ØSanction- Show cause ØJudicial review – aggrieved parties.
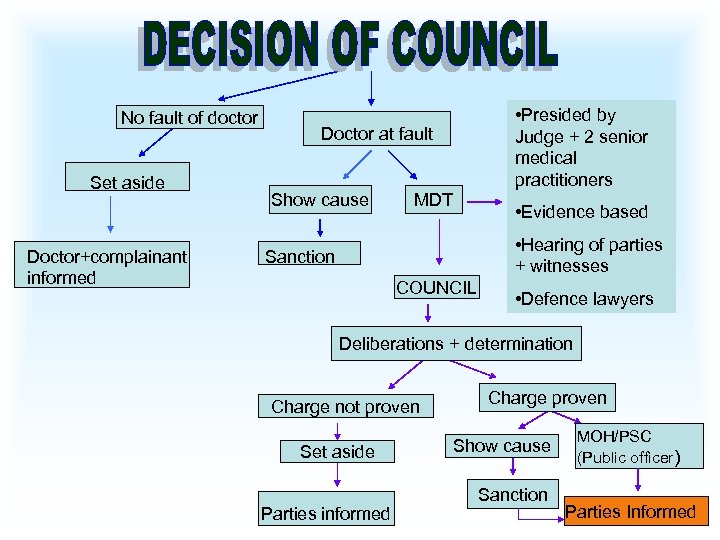 No fault of doctor Set aside Doctor+complainant informed • Presided by Judge + 2 senior medical practitioners Doctor at fault Show cause MDT • Evidence based • Hearing of parties + witnesses Sanction COUNCIL • Defence lawyers Deliberations + determination Charge not proven Set aside Parties informed Charge proven Show cause Sanction MOH/PSC (Public officer) Parties Informed
No fault of doctor Set aside Doctor+complainant informed • Presided by Judge + 2 senior medical practitioners Doctor at fault Show cause MDT • Evidence based • Hearing of parties + witnesses Sanction COUNCIL • Defence lawyers Deliberations + determination Charge not proven Set aside Parties informed Charge proven Show cause Sanction MOH/PSC (Public officer) Parties Informed
 • Malpractice Medical Council Act: “includes a failure to exercise due professional skill or care, which results in injury to or loss of life of a person”.
• Malpractice Medical Council Act: “includes a failure to exercise due professional skill or care, which results in injury to or loss of life of a person”.
 • Medical Negligence ØMedical Council Act: “includes failure on the part of a registered person to exercise the proper and timely care expected from a registered person”. ØAct of Omission ØAct of Commission
• Medical Negligence ØMedical Council Act: “includes failure on the part of a registered person to exercise the proper and timely care expected from a registered person”. ØAct of Omission ØAct of Commission
 To succeed in a claim for negligence, a plaintiff patient must prove, on a balance of probabilities, The following: ØThe defendant doctor owed him a duty of care ØThe defendant doctor breached that duty by failing to exercise the necessary level of care ØHarm and injury was caused by that breach and ØHe suffered damages which was not too remote ( i. e. it was foreseeable by the doctor) “But for” test for proving causation.
To succeed in a claim for negligence, a plaintiff patient must prove, on a balance of probabilities, The following: ØThe defendant doctor owed him a duty of care ØThe defendant doctor breached that duty by failing to exercise the necessary level of care ØHarm and injury was caused by that breach and ØHe suffered damages which was not too remote ( i. e. it was foreseeable by the doctor) “But for” test for proving causation.
 “ A doctor is not negligent if he has conformed with responsible professional practices”. ØA G. P must meet the standards of a competent G. P ØA Consultant Gynaecologist must meet the standard of a competent consultant in that speciality
“ A doctor is not negligent if he has conformed with responsible professional practices”. ØA G. P must meet the standards of a competent G. P ØA Consultant Gynaecologist must meet the standard of a competent consultant in that speciality
 Ø A common practice might be declared not to be rightly accepted: (common professional practices might be wrong) Ø The judiciary find it acceptable to challenge medical opinion, but only when the latter has no rational basis. Ø There may be circumstances where the provision of information will be “ so obviously necessary to an informed choice that no prudent medical men would fail to make it”.
Ø A common practice might be declared not to be rightly accepted: (common professional practices might be wrong) Ø The judiciary find it acceptable to challenge medical opinion, but only when the latter has no rational basis. Ø There may be circumstances where the provision of information will be “ so obviously necessary to an informed choice that no prudent medical men would fail to make it”.
 Ø“the facts speak for themselves” can help a patient in situations where he cannot specify what exactly caused the injury. Ø the doctor has to establish his innocence, rather than the patient having to prove the doctor’s guilt. Ø
Ø“the facts speak for themselves” can help a patient in situations where he cannot specify what exactly caused the injury. Ø the doctor has to establish his innocence, rather than the patient having to prove the doctor’s guilt. Ø
 n “take your victim as you find him” the doctor is liable for all damages even if the damages are more serious because of the patient’s pre-existing illness or condition.
n “take your victim as you find him” the doctor is liable for all damages even if the damages are more serious because of the patient’s pre-existing illness or condition.
 Ø Ø Failure in regard to the contractual obligations by a doctor when he agreed to treat a person. Burden of proving negligence and damage on a balance of probabilities lies with the patient plaintiff. A medical accident can be compensated but not the natural development of an illness. Claims for compensation may be based on: - the tort of negligence - tresspass to the person and battery; or - breach of contract
Ø Ø Failure in regard to the contractual obligations by a doctor when he agreed to treat a person. Burden of proving negligence and damage on a balance of probabilities lies with the patient plaintiff. A medical accident can be compensated but not the natural development of an illness. Claims for compensation may be based on: - the tort of negligence - tresspass to the person and battery; or - breach of contract
 Ø Arises in case of death or serious injury to a patient. Ø The degree of negligence must be so grave as to go beyond a matter of compensation. Ø The doctor may be prosecuted by police or charged in a criminal court for culpable homicide.
Ø Arises in case of death or serious injury to a patient. Ø The degree of negligence must be so grave as to go beyond a matter of compensation. Ø The doctor may be prosecuted by police or charged in a criminal court for culpable homicide.
 Ø Concurrent negligence by the patient and the doctor, resulting in delayed recovery or harm to the patient. Ø Defence for the doctor in civil cases. Ø Burden of proof on doctor.
Ø Concurrent negligence by the patient and the doctor, resulting in delayed recovery or harm to the patient. Ø Defence for the doctor in civil cases. Ø Burden of proof on doctor.
 Ø Liability of the master (employer) inspite of absence of blame worthy conduct on his part. Ø Negligence Ø Employer responsible for negligent acts of his servants. Ø Within the scope of his employment/range of services. Ø Tort of occupier’s liability (e. g. visitor injured on hospital grounds).
Ø Liability of the master (employer) inspite of absence of blame worthy conduct on his part. Ø Negligence Ø Employer responsible for negligent acts of his servants. Ø Within the scope of his employment/range of services. Ø Tort of occupier’s liability (e. g. visitor injured on hospital grounds).
 Ø Ø The assailant is responsible for all the consequences of his assault – the immediate and remote – which link the injury to death. ! Breach in continuity of events by entirely new and unexpected happening (not reasonably foreseeable).
Ø Ø The assailant is responsible for all the consequences of his assault – the immediate and remote – which link the injury to death. ! Breach in continuity of events by entirely new and unexpected happening (not reasonably foreseeable).
 Doctor Patient Non- medical staff Institution (Employer)
Doctor Patient Non- medical staff Institution (Employer)
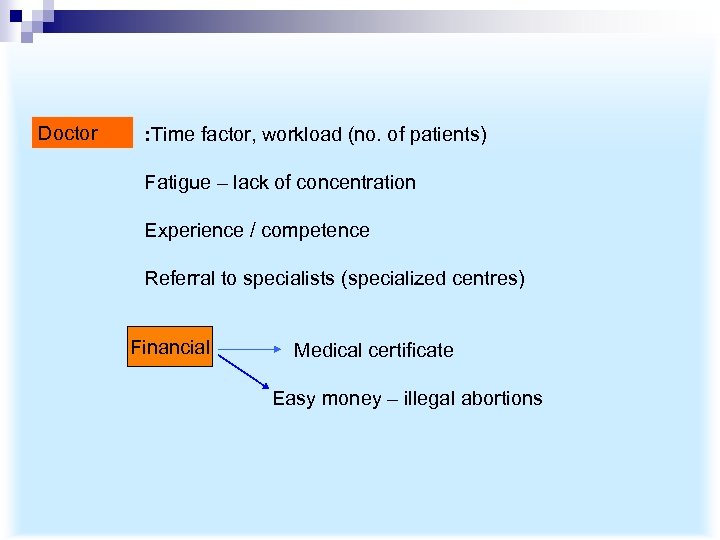 Doctor : : Time factor, workload (no. of patients) Fatigue – lack of concentration Experience / competence Referral to specialists (specialized centres) Financial Medical certificate Easy money – illegal abortions
Doctor : : Time factor, workload (no. of patients) Fatigue – lack of concentration Experience / competence Referral to specialists (specialized centres) Financial Medical certificate Easy money – illegal abortions
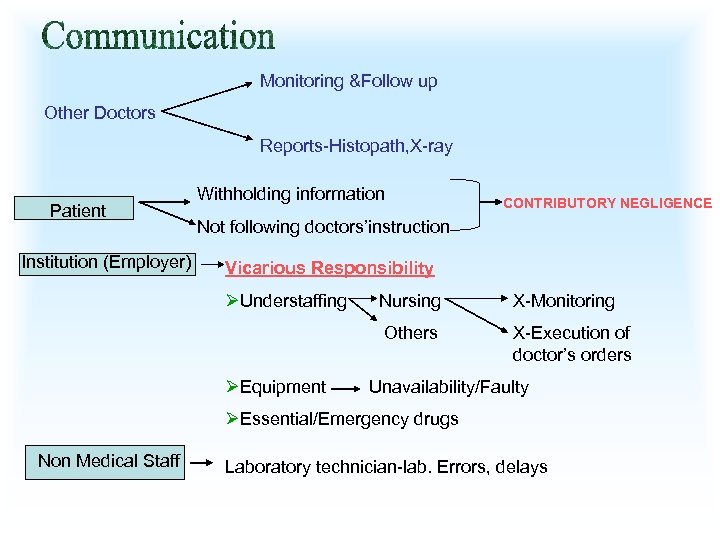 Monitoring &Follow up Other Doctors Reports-Histopath, X-ray Patient Institution (Employer) Withholding information CONTRIBUTORY NEGLIGENCE Not following doctors’instruction Vicarious Responsibility ØUnderstaffing X-Monitoring Others ØEquipment Nursing X-Execution of doctor’s orders Unavailability/Faulty ØEssential/Emergency drugs Non Medical Staff Laboratory technician-lab. Errors, delays
Monitoring &Follow up Other Doctors Reports-Histopath, X-ray Patient Institution (Employer) Withholding information CONTRIBUTORY NEGLIGENCE Not following doctors’instruction Vicarious Responsibility ØUnderstaffing X-Monitoring Others ØEquipment Nursing X-Execution of doctor’s orders Unavailability/Faulty ØEssential/Emergency drugs Non Medical Staff Laboratory technician-lab. Errors, delays
 ØProfessional relationship between colleagues ØMaking disparaging comments about colleagues( in front of other colleagues, staff, patient party). ØTaking over a patient under care of another colleague without prior information to the latter. ØProper referral of patients to other colleagues. ØSharing of medical knowledge/new technologies + assistance to colleagues. Ø“Overcharging” of patients.
ØProfessional relationship between colleagues ØMaking disparaging comments about colleagues( in front of other colleagues, staff, patient party). ØTaking over a patient under care of another colleague without prior information to the latter. ØProper referral of patients to other colleagues. ØSharing of medical knowledge/new technologies + assistance to colleagues. Ø“Overcharging” of patients.
 ØDuring surgery/anesthesia, e. g. monitoring ØEsp. after surgery/intervention ØInstructions/orders not executed properly ØAvailability of treating doctor Postoperative complications Anaphylactic shock ØHanding over to other colleagues in case of unavailability ØDeficiencies in nursing care-monitoring of head injured patient -delay in executing instructions ØPatient smelling alcohol: injured patient May mask certain signs in head- ØWrongly tagging as alcoholic without excluding other diagnosis ØFollow up, monitoring + management of critically ill-patient especially in ICU ØToo many patients in casualty
ØDuring surgery/anesthesia, e. g. monitoring ØEsp. after surgery/intervention ØInstructions/orders not executed properly ØAvailability of treating doctor Postoperative complications Anaphylactic shock ØHanding over to other colleagues in case of unavailability ØDeficiencies in nursing care-monitoring of head injured patient -delay in executing instructions ØPatient smelling alcohol: injured patient May mask certain signs in head- ØWrongly tagging as alcoholic without excluding other diagnosis ØFollow up, monitoring + management of critically ill-patient especially in ICU ØToo many patients in casualty
 ØRationale for request ØNot seeing results of URGENT INVESTIGATIONS ØUnnecessary delay in requesting special investigations, e. g. CT scan
ØRationale for request ØNot seeing results of URGENT INVESTIGATIONS ØUnnecessary delay in requesting special investigations, e. g. CT scan
 ØUse of decorative letter head ØOver description of doctor’s qualities /competence (publicity) ØHandwriting – wrong dispensing ØExplaining to patient ØPerception of indiscriminate prescription / over prescription of certain drugs (e. g. steroids) in chikungunya Gastric perforation (in patient of chikungunya)
ØUse of decorative letter head ØOver description of doctor’s qualities /competence (publicity) ØHandwriting – wrong dispensing ØExplaining to patient ØPerception of indiscriminate prescription / over prescription of certain drugs (e. g. steroids) in chikungunya Gastric perforation (in patient of chikungunya)

 Death certificate issue ØWithout examining corpse ØCause of death (true? ) ØUse of abbreviations ØTime of death
Death certificate issue ØWithout examining corpse ØCause of death (true? ) ØUse of abbreviations ØTime of death
 Requirements of Medical Council Act ØDate of examination ØFull name and address of the patient ØRegistered name and address of the RMP ØSignature of the RMP Cases: Backdating and postdating diagnosis (? confidentiality) Not confirming identity of patient (patient in police custody)
Requirements of Medical Council Act ØDate of examination ØFull name and address of the patient ØRegistered name and address of the RMP ØSignature of the RMP Cases: Backdating and postdating diagnosis (? confidentiality) Not confirming identity of patient (patient in police custody)
 e. g. . Blood transfusion form –Identity of patient - Degree of urgency/when needed - X-match/type & screening - type of products and quantity
e. g. . Blood transfusion form –Identity of patient - Degree of urgency/when needed - X-match/type & screening - type of products and quantity
 Doctor-Doctor Patient Non Medical Staff
Doctor-Doctor Patient Non Medical Staff
 Scanty/ no clinical notes Name of doctor Date and time of examination, diagnosis/D. D ØPre operative status ØTreatment/Operation notes ØProgress ØInvestigations/Monitoring ØHandwriting-wrong dispensing ØUse of Abbreviations (CST, ISQ, ADS)
Scanty/ no clinical notes Name of doctor Date and time of examination, diagnosis/D. D ØPre operative status ØTreatment/Operation notes ØProgress ØInvestigations/Monitoring ØHandwriting-wrong dispensing ØUse of Abbreviations (CST, ISQ, ADS)
 “If it isn’t written, it wasn’t done” Four most frequent themes in case of a bad outcome: 1. Believe your monitors! 2. Record keeping 3. Surgical team agreeing as to what occured 4. (Avoid rushing to condemn) 5. 4. Communicate with patient before and after
“If it isn’t written, it wasn’t done” Four most frequent themes in case of a bad outcome: 1. Believe your monitors! 2. Record keeping 3. Surgical team agreeing as to what occured 4. (Avoid rushing to condemn) 5. 4. Communicate with patient before and after
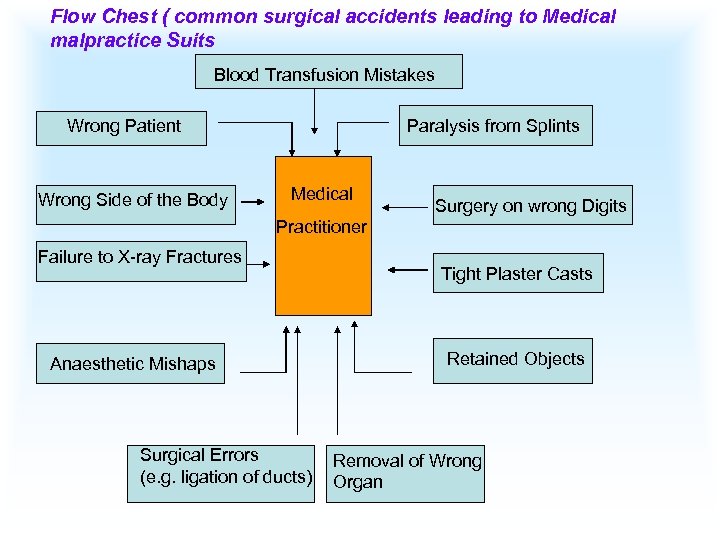 Flow Chest ( common surgical accidents leading to Medical malpractice Suits Blood Transfusion Mistakes Wrong Patient Wrong Side of the Body Paralysis from Splints Medical Surgery on wrong Digits Practitioner Failure to X-ray Fractures Anaesthetic Mishaps Surgical Errors (e. g. ligation of ducts) Tight Plaster Casts Retained Objects Removal of Wrong Organ
Flow Chest ( common surgical accidents leading to Medical malpractice Suits Blood Transfusion Mistakes Wrong Patient Wrong Side of the Body Paralysis from Splints Medical Surgery on wrong Digits Practitioner Failure to X-ray Fractures Anaesthetic Mishaps Surgical Errors (e. g. ligation of ducts) Tight Plaster Casts Retained Objects Removal of Wrong Organ
 Good-Proper-Adequate……? Questioning-Listening-Responding-Explaining Precautions to comply with: ØDisclose information only to the proper person or authority ØPreserve confidences as far as possible (avoid idle conversation about patients, use “aliases”) ØDo not disclose beyond what is required by the law and the situation ØDocument in patient’s record the reasons for and circumstances of the disclosure.
Good-Proper-Adequate……? Questioning-Listening-Responding-Explaining Precautions to comply with: ØDisclose information only to the proper person or authority ØPreserve confidences as far as possible (avoid idle conversation about patients, use “aliases”) ØDo not disclose beyond what is required by the law and the situation ØDocument in patient’s record the reasons for and circumstances of the disclosure.
 Situations where it is ethically and legally required to reveal information: ØWhen the patient consents ØTo medical colleagues ØAs a statutory duty (Re: Infectious diseases) ØAs information to relatives ØIn the interest of research projects ØIn disclosure to court ØIn the discovery of documents in court proceedings ØIn the public’s interest
Situations where it is ethically and legally required to reveal information: ØWhen the patient consents ØTo medical colleagues ØAs a statutory duty (Re: Infectious diseases) ØAs information to relatives ØIn the interest of research projects ØIn disclosure to court ØIn the discovery of documents in court proceedings ØIn the public’s interest
 INFORMED CONSENT 1 (BRAND) ØBenefits of treatment ØRisks of treatment ØAlternatives (other treatment options) ØNo treatment (risks of) ØDocumentation + signature(patient, doctor, independent witness) Ø Material Risk Ø The “Prudent Patient” Test Ø Therapeutic Priviledge ØBattery/Tresspass
INFORMED CONSENT 1 (BRAND) ØBenefits of treatment ØRisks of treatment ØAlternatives (other treatment options) ØNo treatment (risks of) ØDocumentation + signature(patient, doctor, independent witness) Ø Material Risk Ø The “Prudent Patient” Test Ø Therapeutic Priviledge ØBattery/Tresspass
 INFORMED CONSENT 2 based on information about: ØThe name of the operation ØThe nature of the proposed treatment ØWhat the operation involves ØThe potential complications ØThe special precautions required postoperatively ØThe limitations of treatment ØThe success rate of the operation ØHow the patient will feel after treatment ØWhat happens on admission
INFORMED CONSENT 2 based on information about: ØThe name of the operation ØThe nature of the proposed treatment ØWhat the operation involves ØThe potential complications ØThe special precautions required postoperatively ØThe limitations of treatment ØThe success rate of the operation ØHow the patient will feel after treatment ØWhat happens on admission
 Ø Respect for patient’s autonomy (self determination) Ø Non-maleficence (the duty to do no harm) Ø Beneficence (contribute to patient’s welfare). Ø Justice (equitable distribution of benefits and burden). Ø Fidelity (truthfulness and medical confidentiality). Ø Veracity (honesty).
Ø Respect for patient’s autonomy (self determination) Ø Non-maleficence (the duty to do no harm) Ø Beneficence (contribute to patient’s welfare). Ø Justice (equitable distribution of benefits and burden). Ø Fidelity (truthfulness and medical confidentiality). Ø Veracity (honesty).
 Concerned with the conventional laws and customs of courtesy which are generally followed between members of the same profession. A doctor should behave with his colleagues as he would like to have them behave with him.
Concerned with the conventional laws and customs of courtesy which are generally followed between members of the same profession. A doctor should behave with his colleagues as he would like to have them behave with him.
 ØConcerned with moral principles for members of the medical profession in their dealings with each other, their patients, and the state. AIM: to honour and maintain the noble traditions of the medical profession
ØConcerned with moral principles for members of the medical profession in their dealings with each other, their patients, and the state. AIM: to honour and maintain the noble traditions of the medical profession



