9695d4695dba55169009eef07856b58d.ppt
- Количество слайдов: 48
 Hypothermia Post Cardiac Arrest Mazen Kherallah, MD, FCCP Infectious Disease and Critical Care Medicine
Hypothermia Post Cardiac Arrest Mazen Kherallah, MD, FCCP Infectious Disease and Critical Care Medicine
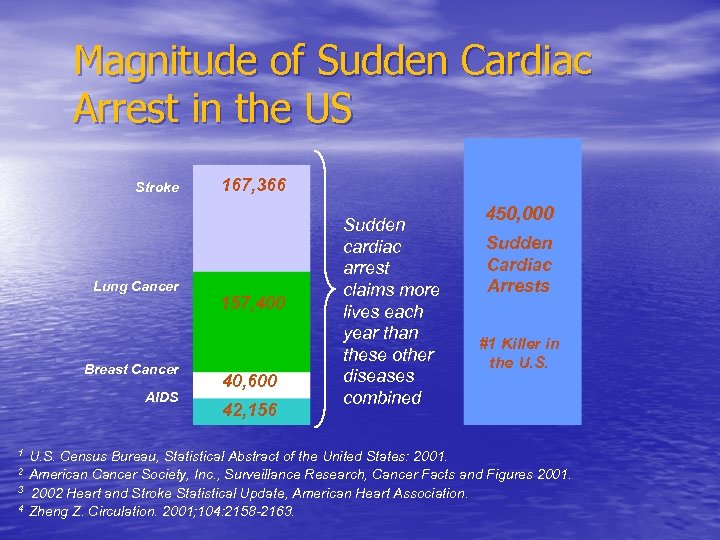 Magnitude of Sudden Cardiac Arrest in the US Stroke Lung Cancer Breast Cancer AIDS 167, 366 157, 400 40, 600 42, 156 Sudden cardiac arrest claims more lives each year than these other diseases combined 450, 000 Sudden Cardiac Arrests #1 Killer in the U. S. 1 U. S. Census Bureau, Statistical Abstract of the United States: 2001. 2 American Cancer Society, Inc. , Surveillance Research, Cancer Facts and Figures 2001. 3 2002 Heart and Stroke Statistical Update, American Heart Association. 4 Zheng Z. Circulation. 2001; 104: 2158 -2163.
Magnitude of Sudden Cardiac Arrest in the US Stroke Lung Cancer Breast Cancer AIDS 167, 366 157, 400 40, 600 42, 156 Sudden cardiac arrest claims more lives each year than these other diseases combined 450, 000 Sudden Cardiac Arrests #1 Killer in the U. S. 1 U. S. Census Bureau, Statistical Abstract of the United States: 2001. 2 American Cancer Society, Inc. , Surveillance Research, Cancer Facts and Figures 2001. 3 2002 Heart and Stroke Statistical Update, American Heart Association. 4 Zheng Z. Circulation. 2001; 104: 2158 -2163.
 EMS systems have improved outcome of cardiac arrests
EMS systems have improved outcome of cardiac arrests
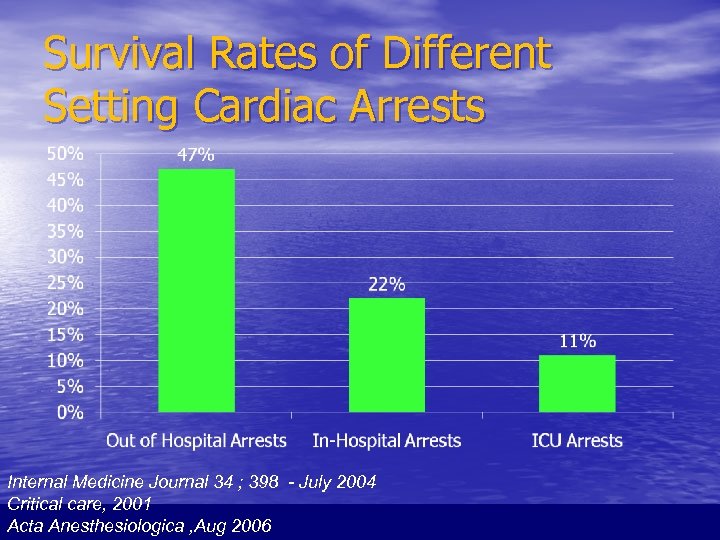 Survival Rates of Different Setting Cardiac Arrests Internal Medicine Journal 34 ; 398 - July 2004 Critical care, 2001 Acta Anesthesiologica , Aug 2006
Survival Rates of Different Setting Cardiac Arrests Internal Medicine Journal 34 ; 398 - July 2004 Critical care, 2001 Acta Anesthesiologica , Aug 2006
 Survival According to Initial Rhythm Critical care medicine 1999
Survival According to Initial Rhythm Critical care medicine 1999
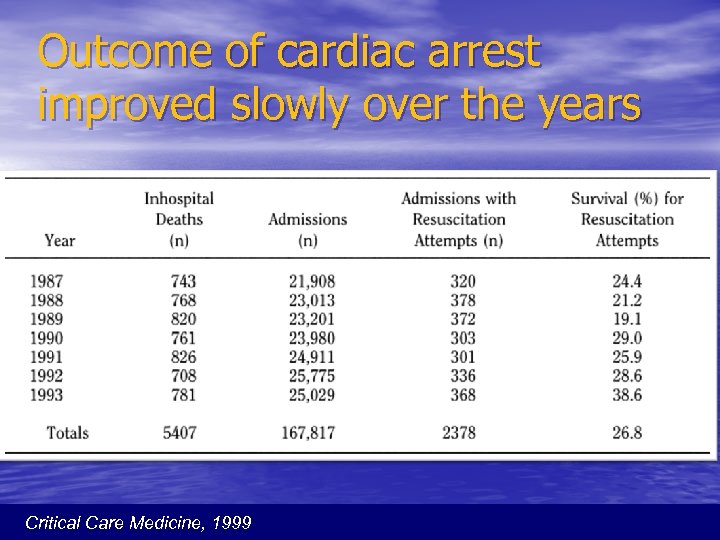 Outcome of cardiac arrest improved slowly over the years Critical Care Medicine, 1999
Outcome of cardiac arrest improved slowly over the years Critical Care Medicine, 1999
 Cerebral Energy Requirements • CMRO 2: 3. 5 cc O 2/min/100 g • CMR glucose: 5. 5 mg/min/100 g – Activation Metabolism • 55 -60% – Residual Metabolism • 40 -45% 60% 40% Barash, Cullen, Stoelting. Clinical Anethesia, 5 th Ed. Lippincott Williams & Wilkins, 2006; p 751.
Cerebral Energy Requirements • CMRO 2: 3. 5 cc O 2/min/100 g • CMR glucose: 5. 5 mg/min/100 g – Activation Metabolism • 55 -60% – Residual Metabolism • 40 -45% 60% 40% Barash, Cullen, Stoelting. Clinical Anethesia, 5 th Ed. Lippincott Williams & Wilkins, 2006; p 751.
 Global Ischemia
Global Ischemia
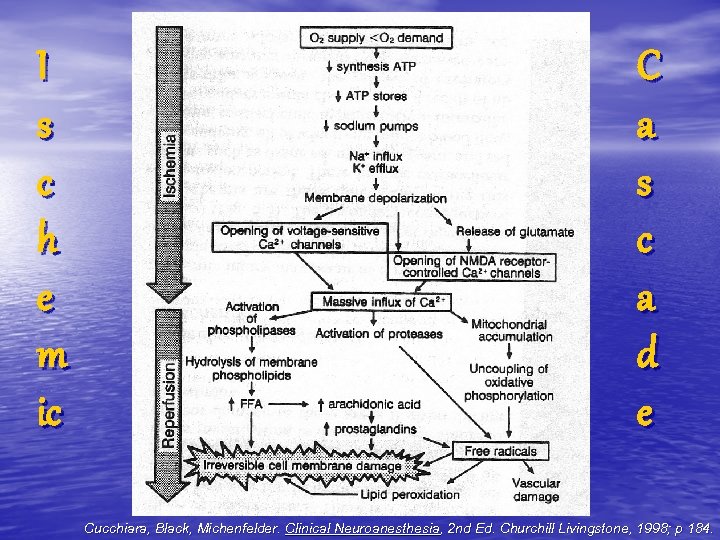 I s c h e m ic C a s c a d e Cucchiara, Black, Michenfelder. Clinical Neuroanesthesia, 2 nd Ed. Churchill Livingstone, 1998; p 184.
I s c h e m ic C a s c a d e Cucchiara, Black, Michenfelder. Clinical Neuroanesthesia, 2 nd Ed. Churchill Livingstone, 1998; p 184.
 Neuro-Protection? • Maintain blood flow • Maintain ATP levels by reducing CMR • Blocking Na and Ca influx • Scavenge free radicals • Block release/receptors for excitatory amino • • • acids Delay membrane failure & apoptotic processes Inhibiting proteins that activate or contribute to damage (proteases, phospholipases, certain kinases) Activating proteins that induce repair or rescue Barash, Cullen, Stoelting. Clinical Anethesia, 5 th Ed. Lippincott Williams & Wilkins, 2006; p 751.
Neuro-Protection? • Maintain blood flow • Maintain ATP levels by reducing CMR • Blocking Na and Ca influx • Scavenge free radicals • Block release/receptors for excitatory amino • • • acids Delay membrane failure & apoptotic processes Inhibiting proteins that activate or contribute to damage (proteases, phospholipases, certain kinases) Activating proteins that induce repair or rescue Barash, Cullen, Stoelting. Clinical Anethesia, 5 th Ed. Lippincott Williams & Wilkins, 2006; p 751.
 Hypothermia
Hypothermia
 Beneficial Effects of Hypothermia • Decrease in cerebral metabolism • Maintains integrity of membranes • Preserves ion homeostasis • Decreases excitatory AA release • Decrease Ca influx • Decrease lipid peroxidation • Decrease free radical formation • Decrease nitric oxide synthase activity
Beneficial Effects of Hypothermia • Decrease in cerebral metabolism • Maintains integrity of membranes • Preserves ion homeostasis • Decreases excitatory AA release • Decrease Ca influx • Decrease lipid peroxidation • Decrease free radical formation • Decrease nitric oxide synthase activity
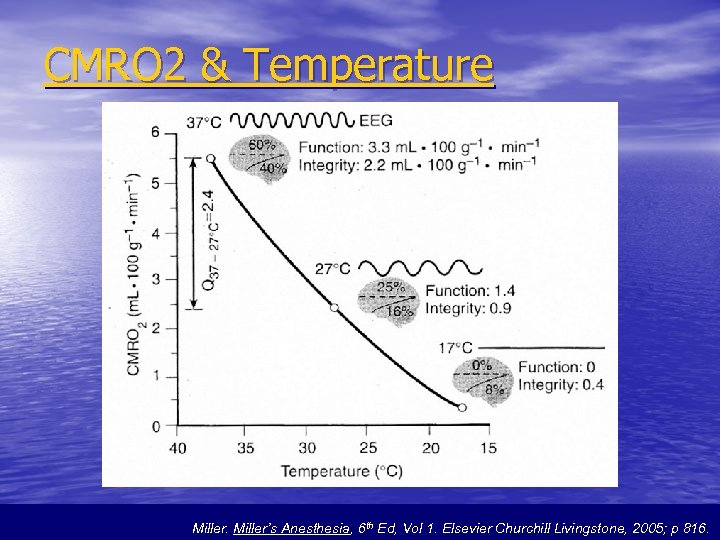 CMRO 2 & Temperature Miller’s Anesthesia, 6 th Ed, Vol 1. Elsevier Churchill Livingstone, 2005; p 816.
CMRO 2 & Temperature Miller’s Anesthesia, 6 th Ed, Vol 1. Elsevier Churchill Livingstone, 2005; p 816.
 Therapeutic Hypothermia Post Resuscitation
Therapeutic Hypothermia Post Resuscitation
 Therapeutic Hypothermia • 1 st reported use of therapeutic hypothermia in TBI in 1943. • 1 st reported use as a protective adjunct to neurosurgery in 1955.
Therapeutic Hypothermia • 1 st reported use of therapeutic hypothermia in TBI in 1943. • 1 st reported use as a protective adjunct to neurosurgery in 1955.
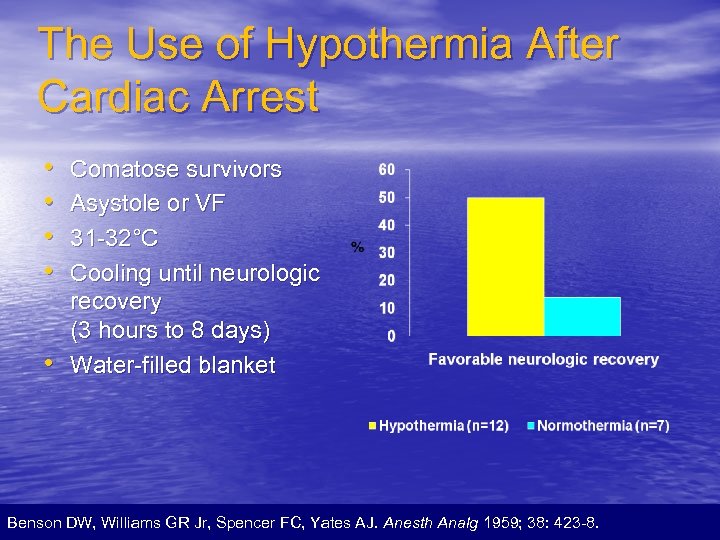 The Use of Hypothermia After Cardiac Arrest • • • Comatose survivors Asystole or VF 31 -32°C Cooling until neurologic recovery (3 hours to 8 days) Water-filled blanket Benson DW, Williams GR Jr, Spencer FC, Yates AJ. Anesth Analg 1959; 38: 423 -8.
The Use of Hypothermia After Cardiac Arrest • • • Comatose survivors Asystole or VF 31 -32°C Cooling until neurologic recovery (3 hours to 8 days) Water-filled blanket Benson DW, Williams GR Jr, Spencer FC, Yates AJ. Anesth Analg 1959; 38: 423 -8.

 Michael Holzer N Engl J Med 2002; 346: 549 -56 Vienna, Austria
Michael Holzer N Engl J Med 2002; 346: 549 -56 Vienna, Austria
 Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest (HACA) Inclusions: Exclusion: q Tympanic-membrane temperature q Witnessed cardiac arrest, below 30°C q Ventricular fibrillation or q Comatose state before the cardiac nonperfusing ventricular tachycardia arrest q Presumed cardiac origin of the q pregnancy arrest q Response to verbal commands after q Age of 18 to 75 years q Estimated interval of 5 to 15 minutes ROSC q Evidence of hypotension; MAP< 60 from the patient’s collapse to the first mm Hg for more than 30 minutes after attempt at resuscitation q Interval of no more than 60 minutes ROSC q Evidence of hypoxemia: O 2 Sat from collapse to restoration of <85% for more than 15 minutes after spontaneous circulation. ROSC q Terminal illness that preceded the arrest q Preexisting coagulopathy. The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest (HACA) Inclusions: Exclusion: q Tympanic-membrane temperature q Witnessed cardiac arrest, below 30°C q Ventricular fibrillation or q Comatose state before the cardiac nonperfusing ventricular tachycardia arrest q Presumed cardiac origin of the q pregnancy arrest q Response to verbal commands after q Age of 18 to 75 years q Estimated interval of 5 to 15 minutes ROSC q Evidence of hypotension; MAP< 60 from the patient’s collapse to the first mm Hg for more than 30 minutes after attempt at resuscitation q Interval of no more than 60 minutes ROSC q Evidence of hypoxemia: O 2 Sat from collapse to restoration of <85% for more than 15 minutes after spontaneous circulation. ROSC q Terminal illness that preceded the arrest q Preexisting coagulopathy. The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
 Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest (HACA) 275/3, 551 (8%) Pts s/p Witnessed V-fib Arrest Multicenter RCT, Blinded assessment outcome. Hypothermia (32 -34 o. C) x 24 hrs 137 Patients normothermia (37 -38 o. C) 138 Patients Primary endpoint: favorable neuro outcome* w/in 6 mo Secondary: 6 mo mortality & 7 day complication rate. * Pittsburgh cerebral-performance category, 1 [good recovery] or 2 [moderate disability] The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest (HACA) 275/3, 551 (8%) Pts s/p Witnessed V-fib Arrest Multicenter RCT, Blinded assessment outcome. Hypothermia (32 -34 o. C) x 24 hrs 137 Patients normothermia (37 -38 o. C) 138 Patients Primary endpoint: favorable neuro outcome* w/in 6 mo Secondary: 6 mo mortality & 7 day complication rate. * Pittsburgh cerebral-performance category, 1 [good recovery] or 2 [moderate disability] The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
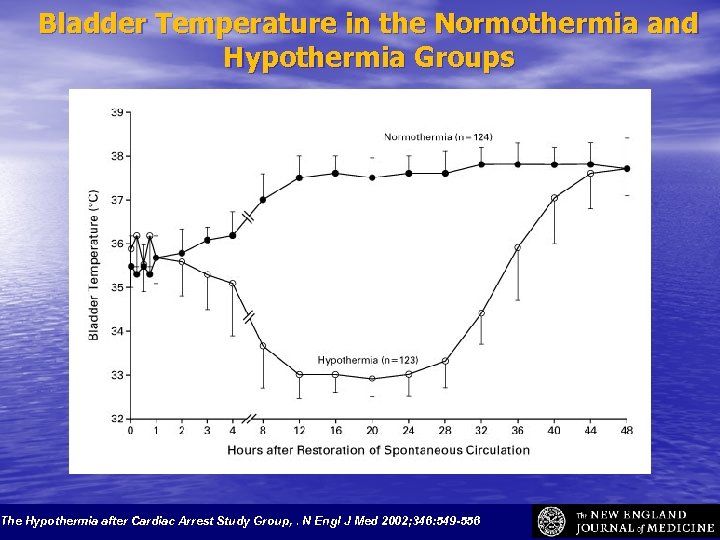 Bladder Temperature in the Normothermia and Hypothermia Groups The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
Bladder Temperature in the Normothermia and Hypothermia Groups The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
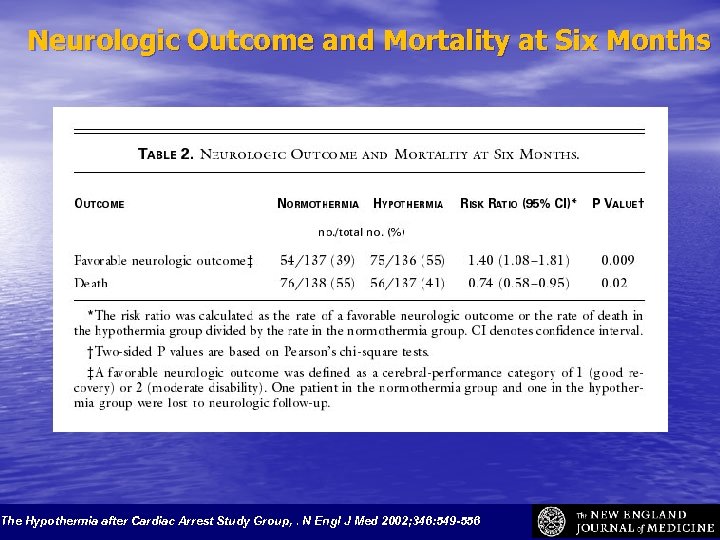 Neurologic Outcome and Mortality at Six Months The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
Neurologic Outcome and Mortality at Six Months The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
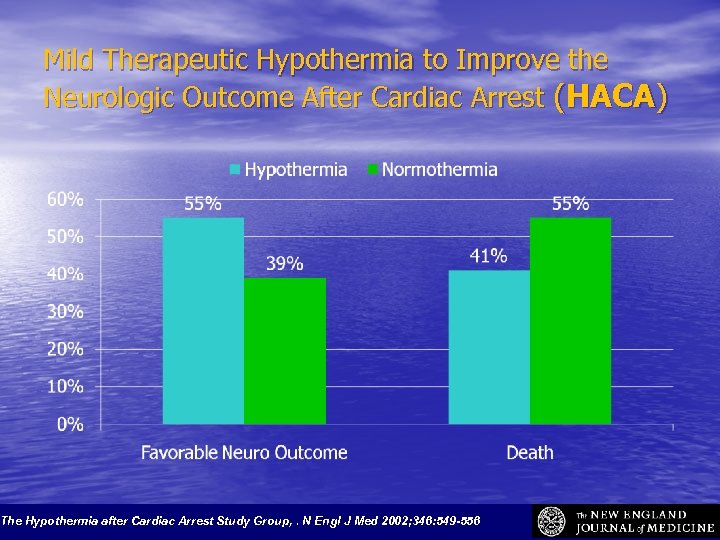 Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest (HACA) The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest (HACA) The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
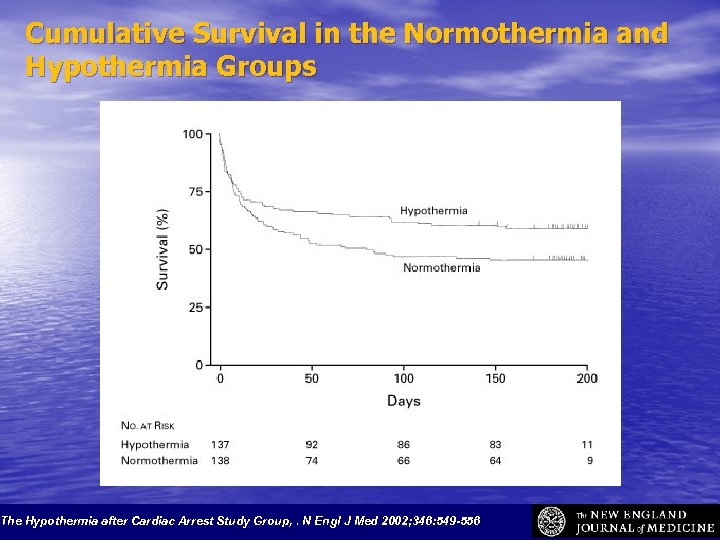 Cumulative Survival in the Normothermia and Hypothermia Groups The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
Cumulative Survival in the Normothermia and Hypothermia Groups The Hypothermia after Cardiac Arrest Study Group, . N Engl J Med 2002; 346: 549 -556
 Bernard et al. N Engl J Med 2002; 346: 557 -563 Melbourne, Australia
Bernard et al. N Engl J Med 2002; 346: 557 -563 Melbourne, Australia
 Treatment of Comatose Survivors of OOH Cardiac Arrest with Induced Hypothermia • Multicenter r. CT 77 Pts who remained unconscious s/p out of hospital cardiac arrest (V-fib @ scene). • Randomized (by day) to hypothermia group (33 o. C 2 hrs after return of spont circulation maintained for 12 hours) or normothermia. Bernard, S. et al. N Engl J Med 2002; 346: 557 -563
Treatment of Comatose Survivors of OOH Cardiac Arrest with Induced Hypothermia • Multicenter r. CT 77 Pts who remained unconscious s/p out of hospital cardiac arrest (V-fib @ scene). • Randomized (by day) to hypothermia group (33 o. C 2 hrs after return of spont circulation maintained for 12 hours) or normothermia. Bernard, S. et al. N Engl J Med 2002; 346: 557 -563
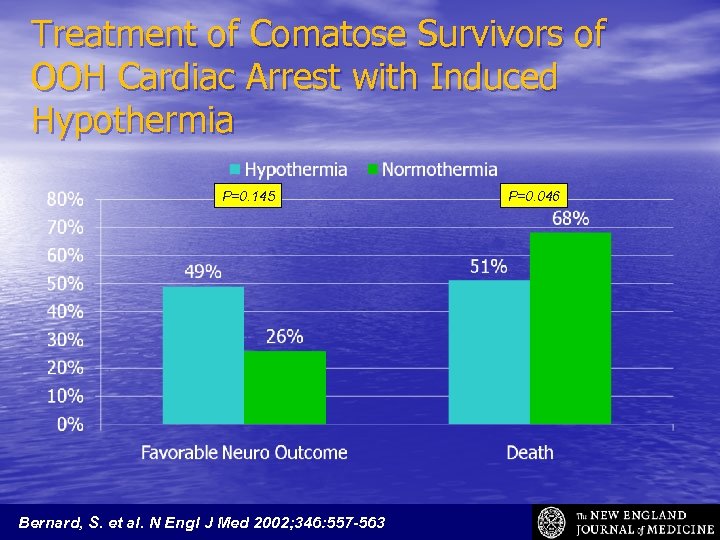 Treatment of Comatose Survivors of OOH Cardiac Arrest with Induced Hypothermia P=0. 145 Bernard, S. et al. N Engl J Med 2002; 346: 557 -563 P=0. 046
Treatment of Comatose Survivors of OOH Cardiac Arrest with Induced Hypothermia P=0. 145 Bernard, S. et al. N Engl J Med 2002; 346: 557 -563 P=0. 046
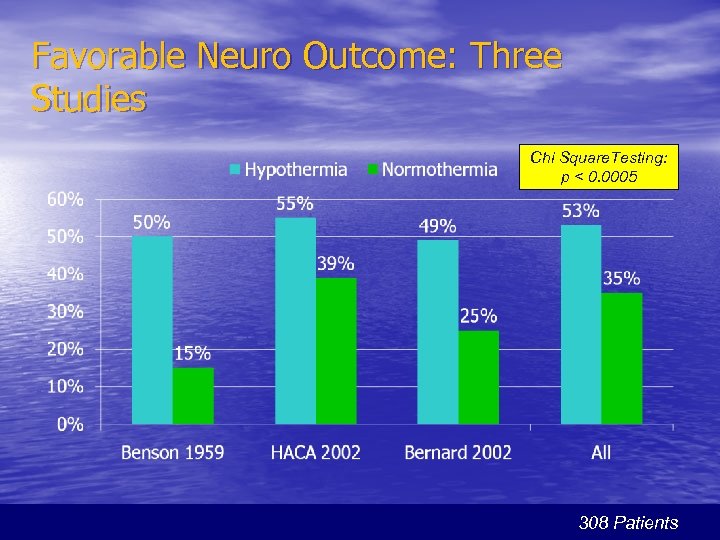 Favorable Neuro Outcome: Three Studies Chi Square. Testing: p < 0. 0005 308 Patients
Favorable Neuro Outcome: Three Studies Chi Square. Testing: p < 0. 0005 308 Patients
 Conclusion… • In patients who have been successfully resuscitated after cardiac arrest due to ventricular fibrillation, therapeutic mild hypothermia increased the rate of a favorable neurologic outcome and reduced mortality.
Conclusion… • In patients who have been successfully resuscitated after cardiac arrest due to ventricular fibrillation, therapeutic mild hypothermia increased the rate of a favorable neurologic outcome and reduced mortality.
 ILCOR Advisory Statement q. Unconscious adult patients with ROSC after out-of-hospital VF cardiac arrest should be cooled to 32°C - 34°C for 12 - 24 hours q. Possible benefit for other rhythms or inhospital cardiac arrest
ILCOR Advisory Statement q. Unconscious adult patients with ROSC after out-of-hospital VF cardiac arrest should be cooled to 32°C - 34°C for 12 - 24 hours q. Possible benefit for other rhythms or inhospital cardiac arrest
 2005 AHA guidelines for ACLS and post CPR care • In a select subset of patients who were initially comatose but hemodynamicaly stable after a witnessed VF arrest of presumed cardiac etiology, active induction of hypothermia was beneficial. Thus, unconscious adult patients with ROSC after out-of-hospital cardiac arrest should be cooled to 32°C to 34°C for 12 to 24 hours when the initial rhythm was VF (Class IIa). Similar therapy may be beneficial for patients with non-VF arrest out of hospital or for in-hospital arrest (Class IIb). 2005 AHA guidelines, Circulation, 2005
2005 AHA guidelines for ACLS and post CPR care • In a select subset of patients who were initially comatose but hemodynamicaly stable after a witnessed VF arrest of presumed cardiac etiology, active induction of hypothermia was beneficial. Thus, unconscious adult patients with ROSC after out-of-hospital cardiac arrest should be cooled to 32°C to 34°C for 12 to 24 hours when the initial rhythm was VF (Class IIa). Similar therapy may be beneficial for patients with non-VF arrest out of hospital or for in-hospital arrest (Class IIb). 2005 AHA guidelines, Circulation, 2005
 How to apply hypothermia It is not that complicated!!
How to apply hypothermia It is not that complicated!!
 Hypothermia Protocol • Indications: – Only comatose adults after ROSC who are “hemodynamically stable” • Initiation: – ASAP, but at least within 6 hours of event • Degree of Hypothermia – 32 -35 o. C core temperature • Duration: – At least 12 hours; 24 hours probably better
Hypothermia Protocol • Indications: – Only comatose adults after ROSC who are “hemodynamically stable” • Initiation: – ASAP, but at least within 6 hours of event • Degree of Hypothermia – 32 -35 o. C core temperature • Duration: – At least 12 hours; 24 hours probably better
 How to Cool: Four Modes of Heat Transfer • Conduction – Cold water immersion • Radiation – Cold room • Convection – Fans (do not use for infection control purposes) • Evaporation – Sweating
How to Cool: Four Modes of Heat Transfer • Conduction – Cold water immersion • Radiation – Cold room • Convection – Fans (do not use for infection control purposes) • Evaporation – Sweating
 How to Cool: Hypothermia Protocol • Blanket cooling not effective in adults; • Intravascular cooling with bolus of iced RL or NS is effective • Surface SURFACE COOLING – Sub. Zero, Aquamatic (conventional watercirculating) – Polar Air (forced air convection cooling) – Arctic Sun (“adhesive hyrogel, water circulating) – MTRE (tight wrap water circulating)
How to Cool: Hypothermia Protocol • Blanket cooling not effective in adults; • Intravascular cooling with bolus of iced RL or NS is effective • Surface SURFACE COOLING – Sub. Zero, Aquamatic (conventional watercirculating) – Polar Air (forced air convection cooling) – Arctic Sun (“adhesive hyrogel, water circulating) – MTRE (tight wrap water circulating)
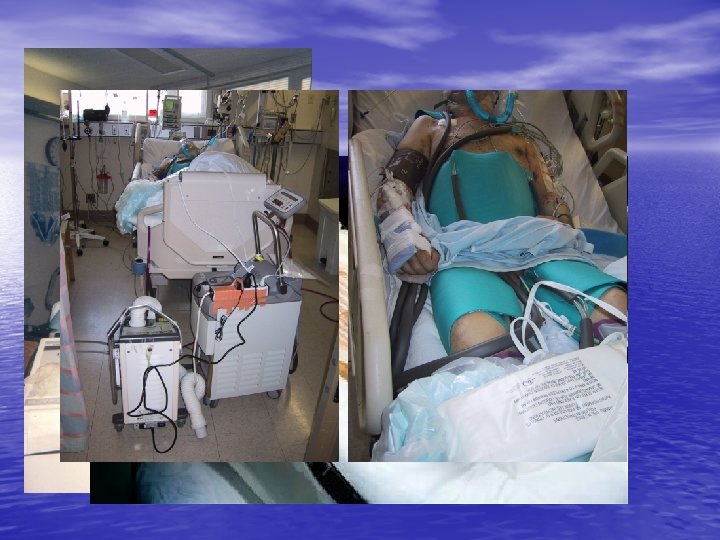
 HOW TO COOL: Hypothermia Protocol • ENDOVASCULAR CATHETER COOLING – Radiant – Alsius – Innercool (metallic)
HOW TO COOL: Hypothermia Protocol • ENDOVASCULAR CATHETER COOLING – Radiant – Alsius – Innercool (metallic)
 Monitoring: Mild/Moderate Hypothermia Protocol (33° C) • Endotracheal intubation • Sedation: fentanyl & midazolam • Paralysis: vecuronium 0. 1 mg/kg PRN • Thermistors: bladder, rectal, esophageal, or blood temperature, ? Brain temperature • Radial artery and internal jugular lines • Intraparenchymal ICP & temperature monitor • Insulin drip for BS >180 mg/dl • Hypokalemia <3. 4 m. Eq/l replaced
Monitoring: Mild/Moderate Hypothermia Protocol (33° C) • Endotracheal intubation • Sedation: fentanyl & midazolam • Paralysis: vecuronium 0. 1 mg/kg PRN • Thermistors: bladder, rectal, esophageal, or blood temperature, ? Brain temperature • Radial artery and internal jugular lines • Intraparenchymal ICP & temperature monitor • Insulin drip for BS >180 mg/dl • Hypokalemia <3. 4 m. Eq/l replaced
 Monitoring: Mild/Moderate Hypothermia Protocol • ABGs at room temp (alpha-stat) • Vasopressors to keep CPP >70 mm Hg • ICP >20 mm Hg treated per protocol • Feedings held x 48 hours • Cultures/antibiotics as indicated • Passive controlled rewarming (0. 5° / hr) • Active cooling is maintained at 36. 5°C • thereafter for 24 hrs to avoid “overshoot” Need to adjust medications during hypothermia?
Monitoring: Mild/Moderate Hypothermia Protocol • ABGs at room temp (alpha-stat) • Vasopressors to keep CPP >70 mm Hg • ICP >20 mm Hg treated per protocol • Feedings held x 48 hours • Cultures/antibiotics as indicated • Passive controlled rewarming (0. 5° / hr) • Active cooling is maintained at 36. 5°C • thereafter for 24 hrs to avoid “overshoot” Need to adjust medications during hypothermia?
 Example of Anti-Shivering Protocol • Focal Counterwarming – – – Feet and hands Face Body (Bear Hugger) • Buspirone 20 q 8 H • Meperidine 25 -100 mg q 4 H – Alt: dexmendetomidine, fentanyl, propofol • If use NMB, need to monitor EEG – Sub-clinical seizures may be more common than clinically recognized – should we load with anticonvulsants?
Example of Anti-Shivering Protocol • Focal Counterwarming – – – Feet and hands Face Body (Bear Hugger) • Buspirone 20 q 8 H • Meperidine 25 -100 mg q 4 H – Alt: dexmendetomidine, fentanyl, propofol • If use NMB, need to monitor EEG – Sub-clinical seizures may be more common than clinically recognized – should we load with anticonvulsants?
 Detrimental Effects of Hypothermia • Circulatory: afterload, 3 rd spacing, viscosity, • • • diuresis, hypovolemia, hypotension Cardiac: shivering, cardiac output, arrhythmias Pulmonary: pulm edema Neurologic: ICP w/ rewarming, affects neuromonitoring Coagulation: plt dysfxn, fibrinolysis, bleeding Metabolic: shifts O 2 dissociation curve left, metabolic acidosis, respiratory alkalosis, Hypokalemia, hyperglycemia, ileus, drug metab Immunologic: leuk mobility & phagocytosis
Detrimental Effects of Hypothermia • Circulatory: afterload, 3 rd spacing, viscosity, • • • diuresis, hypovolemia, hypotension Cardiac: shivering, cardiac output, arrhythmias Pulmonary: pulm edema Neurologic: ICP w/ rewarming, affects neuromonitoring Coagulation: plt dysfxn, fibrinolysis, bleeding Metabolic: shifts O 2 dissociation curve left, metabolic acidosis, respiratory alkalosis, Hypokalemia, hyperglycemia, ileus, drug metab Immunologic: leuk mobility & phagocytosis
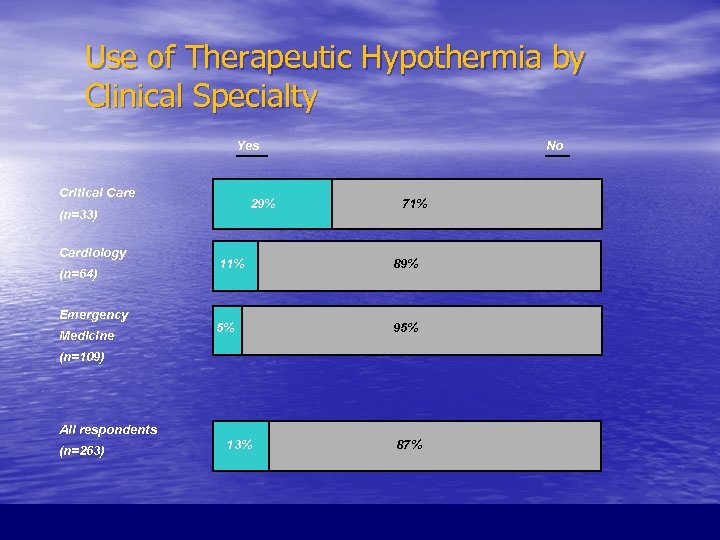 Use of Therapeutic Hypothermia by Clinical Specialty Yes Critical Care 29% (n=33) Cardiology (n=64) Emergency Medicine No 71% 11% 89% 5% 95% (n=109) All respondents (n=263) 13% 87%
Use of Therapeutic Hypothermia by Clinical Specialty Yes Critical Care 29% (n=33) Cardiology (n=64) Emergency Medicine No 71% 11% 89% 5% 95% (n=109) All respondents (n=263) 13% 87%
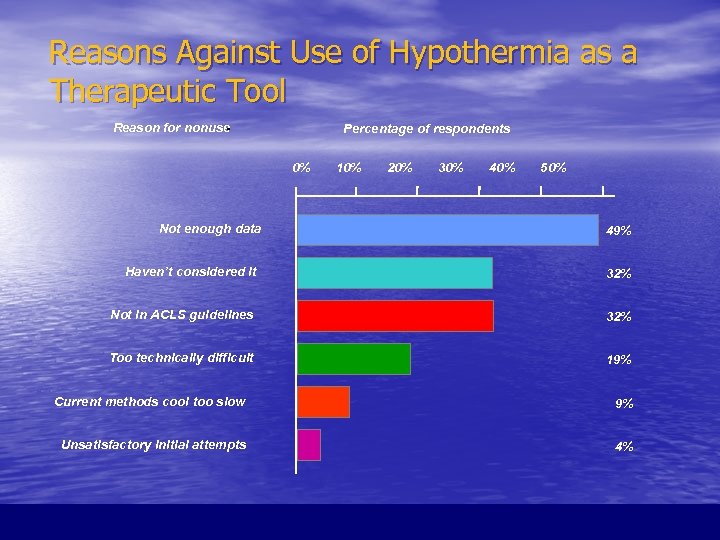 Reasons Against Use of Hypothermia as a Therapeutic Tool Reason for nonuse - Percentage of respondents 0% Not enough data 10% 20% 30% 40% 50% 49% Haven’t considered it 32% Not in ACLS guidelines 32% Too technically difficult 19% Current methods cool too slow 9% Unsatisfactory initial attempts 4%
Reasons Against Use of Hypothermia as a Therapeutic Tool Reason for nonuse - Percentage of respondents 0% Not enough data 10% 20% 30% 40% 50% 49% Haven’t considered it 32% Not in ACLS guidelines 32% Too technically difficult 19% Current methods cool too slow 9% Unsatisfactory initial attempts 4%
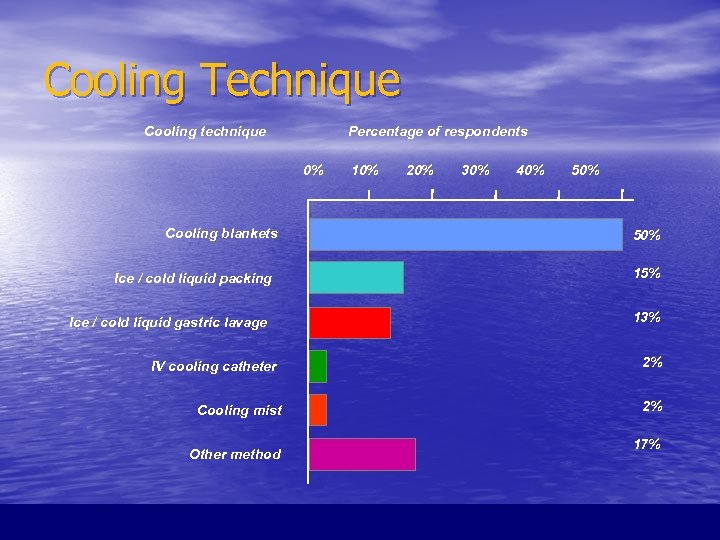 Cooling Technique Cooling technique Percentage of respondents 0% Cooling blankets Ice / cold liquid packing Ice / cold liquid gastric lavage IV cooling catheter Cooling mist Other method 10% 20% 30% 40% 50% 15% 13% 2% 2% 17%
Cooling Technique Cooling technique Percentage of respondents 0% Cooling blankets Ice / cold liquid packing Ice / cold liquid gastric lavage IV cooling catheter Cooling mist Other method 10% 20% 30% 40% 50% 15% 13% 2% 2% 17%
 Take home messages • Strong evidence that mild hypothermia is neuro-protective after return of spontaneous circulation. • Fever is detrimental post resuscitation (and for any neuro patient) • Hypothermia is underutilized so far but should be included in post resuscitaion care of cardiac arrest victims
Take home messages • Strong evidence that mild hypothermia is neuro-protective after return of spontaneous circulation. • Fever is detrimental post resuscitation (and for any neuro patient) • Hypothermia is underutilized so far but should be included in post resuscitaion care of cardiac arrest victims
 Critical Care is A Promise ﺍﻥ ﺍﻟﻠﻪ ﻳﺤﺐﺍﻟﻌﺒﺪ ﺍﺫﺍﻋﻤﻞ ﻋﻤﻼ ﺃﻦﻳﺘﻘﻨﻪ
Critical Care is A Promise ﺍﻥ ﺍﻟﻠﻪ ﻳﺤﺐﺍﻟﻌﺒﺪ ﺍﺫﺍﻋﻤﻞ ﻋﻤﻼ ﺃﻦﻳﺘﻘﻨﻪ
 If you are admitted to our ICU after cardiac arrest: • You will get cooled
If you are admitted to our ICU after cardiac arrest: • You will get cooled
 ﻛﻞ ﻧﻔﺲ ﺫﺍﺋﻘﺔ ﺍﻟﻤﻮﺕ ﺳﻮﺭﺓ آﻞ ﻋﻤﺮﺍﻥ - آﻴﺔ 581 ﻟﻜﻞ ﺃﺠﻞ ﻛﺘﺎﺏ Thank You ﺳﻮﺭﺓ ﺍﻟﺮﻋﺪ – آﻴﺔ 83
ﻛﻞ ﻧﻔﺲ ﺫﺍﺋﻘﺔ ﺍﻟﻤﻮﺕ ﺳﻮﺭﺓ آﻞ ﻋﻤﺮﺍﻥ - آﻴﺔ 581 ﻟﻜﻞ ﺃﺠﻞ ﻛﺘﺎﺏ Thank You ﺳﻮﺭﺓ ﺍﻟﺮﻋﺪ – آﻴﺔ 83


