934d7c6f0b4a0cf9402b40db3e48b9ea.ppt
- Количество слайдов: 46


HYPOTENSIVE ANESTHESIA By Khosrou Naghibi MD Isfahan University of Medical Sciences

Synonyms of DH • Controlled hypotension • Induced hypotension • Circulatory control • Hypotensive anesthesia

Purpose of DH: • This technique was deployed to: • Decrease Blood loss • Improve operative field • Decrease duration of Sx.

DELIBERATE HYPOTENSION To reduce bleeding • To reduce blood transfusions • Indicated: Oromaxillofacial surgery Endoscopic sinus microsurgery Middle ear microsurgery Spinal surgery Neuro surgery Major orthopaedic surgery Prostatectomy CV surgery Liver transplant surgery • • •

DH Cont. . Definition Ø Reduction in systolic blood pressure to 80 -90 mm. Hg Ø Decrease in MAP to 50 -65 mm. Hg in normotensive patients Ø Reduction in MAP by one-third of its baseline values

DELIBERATE HYPOTENSION DEFINITION: Reduction of the systolic blood pressure • to 80 -90 mm. Hg Reduction of mean arterial pressure • (MAP) to 50 -65 mm. Hg 30% reduction of baseline MAP • DRUG. 2007; 67 (7): 1053 -76

DH Cont. . Safe level of DH • Depends on the pt. • Healthy young pt. tolerate mean B. P. as low as 50 -60 mm. Hg. • Ch. hypertensive pts. tolerate a mean of B. P. no more than 25% lower than the base line. • Pts. with TIA may not tolerate any decrease in cerebral perfusion pressure.

• Extremes : • Hypotension always avoided • Hypotension produced for any desire of surgeon.
DH Cont. . Indication Ø Neurosurgery Ø Orthopedics: THR, spine fusion ØEar, Nose, Throat/Oral Surgery Ø Gynecologic/urologic: radical pelvic surgery, prostatectomy Ø Religious blood refusal, rare blood type, difficult cross matching

DH Cont. . Contraindications • Infants • Systemic disease compromising major organ function • Renal, cerebral, coronary artery diseases • Pt. with sickle cell anemia • Polycythemia (uncorrected)

DH Cont. . Significant reduction in O 2 delivery: • ANEMIA • SEVER LUNG DISEASE • LOW CARDIAC OUTPUT

DH Cont. . Absolute contraindications • Cerebrovascular disease • Inexperience of the anesthesiologist

DH Cont. . Complications • Underperfusion of major organ: • Cerebral thrombosis • Hemiplegia • ATN • Massive hepatic necrosis • Blindness • Retinal artery thrombosis • Ischemic optic neuropathy • Surgical complications • Reactionary hemorrhage • Hematoma formation

COMPLICATIONS OF DELIBERATE HYPOTENSION COMPLICATION INCIDENCE(%) Cerebral thrombosis 0, 1 – 0, 2 Coronary artery thrombosis COMMENT 0, 3 – 0, 7 Renal failure 0 – 0, 2 Hepatic failure Postop pulmonary dysfunction Rebound hypertension Increased bleeding at operative site Inadequate hemostasis (due to hypotension)

RELATIVE CONTRA INDICATIONS TO INDUCED HYPOTENSION Ischemic cerebrovascular desease • Coronary artery desease • Hypovolemia • Anemia • Severe hypertension • Extremes of age •

Hemodynamic effects of Hypotensive drugs: TACHYPHYLAXIS: • Response despite repeated administration of the drug • More frequently seen in young adults • Has been reported with most drugs. TACHYCARDIA.

Control of heart rate: The key to preventing tachyphylaxia is control of heart rate: • Inhalational anesthesia • Avoiding fluid overload • Pre-Op. sedation + IV opioid.
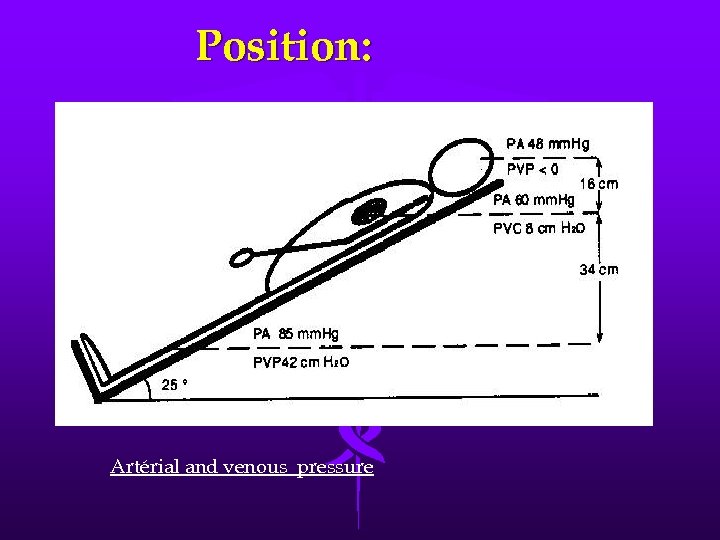
Position: Artérial and venous pressure
Reduction of bleeding : position 10 -15° head up tilt position Head position : head rest rotation - controlateral ear - jugular vein - bracchial plexus - carotid artery

DELIBERATE HYPOTENSION: NEW TECHNIQUES Use the natural hypotensive effects of • anaesthetic drugs with regard to the definition of the ideal hypotensive agent: Easy to administer Short onset time Disappears quickly when stopped Rapid elimination No toxic metabolites Negligible effect on vital organs Predictable effect Dose dependent effect • •

Remifentanil Key Concepts Remifentanil is an OPIOID l Pure m agonist l little binding at k, s, and d receptors¡ The effects of remifentanil are identical l with other commonly used opioids fentanyl¡ alfentanil¡ sufentanil¡

DELIBERATE HYPOTENSION: NEW TECHNIQUES Epidural anaesthesia • Remifentanil: - Propofol • Remifentanil: - Isoflurane • - Desflurane - Sevoflurane Epinephrine and inhalation anesthetics 5. 4 mcg/kg with isoflurane 10 mcg/kg with sevoflurane 10 mcg/kg with desflurane BJA 2008 Jan; 100(1): 50 -4 Rhinology 2007 mar; 45 (1): 72 -8 Eur J. Anaesthesiol 2007 may; 24 (5): 441 -6 AM J. Rhinol 2005 sept-oct; 19 (5): 514 -20 Laryngoscopie 2003 aug; 113 (8): 1369 -73

Monitoring during Controlled hypotension

DH Cont. . 1. Arterial blood pressure 2. ECG – myocardial perfusion Risk of: Tachycardia Bradycardia Arrhythmias St-sigment changes Ishcemia

3. Gas exchange: Capnography is essential: • • As a disconnection alarm Indicator of air embolism • ( Correlation between ETCO 2 & Pa. CO 2 is limited VD/VT) during DH • Helps avoid hyperventilation in DH Pulse oximetry 4. Temperature

Method • Physiologic technique • Pharmacologic technique

DELIBERATE HYPOTENSION AGENTS USED ALONE: • Inhalation anaesthetics Sodium nitroprusside Nitroglycerin Trimethaphan Prostaglandine E 1 Adenosine Remifentanil Agents for spinal anaesthesia • • ALONE OR COMBINED: • Calcium channel antagonists Beta-Blockers Fenoldopam • • • COMBINED: • ACE inhibitors • Clonidine •

Physiologic technique § Body positioning § Hemodynamic effects of mechanical ventilation § Changes in heart rate & circulatory volume

Pharmacologic technique • Ideal agent - Ease of administration - Predictable & dose-dependent effect - Rapid onset/offset - Quick elimination without the production of toxic metabolites - Minimal effects on blood flow to vital organs

1)Inhalational anesthetics – negative inotropic effect vasodilation • • Advantage Provides surgical anesthesia Rapid onset/offset Easy to titrate Cerebral protection Disadvantage • Decreases CO • Cerebral vasodilation
3)Sodium nitroprusside Direct vasodilator (nitric oxide release) • • Disadvantage Cyanide/thiocyanate toxicity Increased ICP Increased pulm. shunt Sympathetic stimulation Rebound hypertension Coronary steal Tachycardia Advantage • Rapid onset/offset • East to titrate • Increases CO

4)Nitroglycerin Direct vasodilator • • (nitric oxide release) Advantage Rapid onset/offset East to titrate Limited increase in heart rate No coronary steal • • • Disadvantage Lack of efficacydepending on anesthetic technique Increased ICP Increased pulm. shunt Methemoglobinemia Inhibition of plt. aggregation

5)Beta adrenergic antagonist Beta adrenergic blockade contractility) • • Advantage Rapid onset/offset Decreased myocardial O 2 consumption No increase in ICP No increase in pulm. shunt (decreased myocardial Disadvantage • • Decreased CO Heart block Bronchospasm Limited efficacy when used alone
6)Calcium channel blocker - vasodilation • • • Advantage Rapid onset Limited increase in HR Increase CO No effect on airway reactivity Increased GFR/urine output Disadvantage • Prolonged duration of action • Increased ICP • Increased pulm. shunt

Intravenous drugs

7)Remifentanil • Remifentanil is an OPIOID • Pure m agonist • little binding at k, s, and d receptors § § § Rapid onset/offset Decreases blood pressure & heart rate No need for additional use of a potent hypotensive or adjunct agents

Remifentanil Key Concepts • Remifentanil is an ESTER. Metabolized by nonspecific esterases in blood and tissue • Anesthesia maintained with high-dose remifentanil will be associated with rapid recovery. l Within 5 -10 minutes of turning off an infusion there is virtually no residual remifentanil drug effect

Remifentanil Potential Benefits • Changes in remifentanil drug effect rapidly follow changes in the remifentanil infusion rate. • The analgesic effects are evanescent. • Post-operative analgesic needs must be anticipated.

Remifentanil Metabolism • Extremely rapid • Not influenced by: • • • Hepatic disease Renal disease Pseudocholinesterase deficiency Administration of neostigmine Very young age • Modest decrease in elderly patients

Anesthesia Technique • Monitoring • Induction • Position head up 450 • BP drop range 20% - 40% of baseline • HR range 50 – 60 beat/min

Observation, cont’d • PONV: • Nausea & Vomiting. • prophylactic anti-emetics are given perioperatively.

DH… • Ear Sx. • Produce bloodless surgical field for microscopy • Stapedectomy : • <0. 75 ml of blood loss condition • >1. 5 ml of blood loss good op. bad op. condition • In middle ear Sx. Even slight hemorrhage fibrosis so B. P. Improves the results.

Deliberate Hypotension In FESS § Moderate DH (systolic pressure 80 80 mm. Hg) • Reduces the capillary bleeding § Bloodless operative field provides good sinuses surgical conditions

CONCLUSION • Proper initiation of DH depends on the anesthesiologist. • Desired level of blood pressure can be achieved by skillful use of gravity, ventilation & drugs helped by proper monitoring and adequate Post Op. care. • Teamwork with cooperation between anesthesiologist and surgeon is of great importance in the care of pts. who undergo deliberate hypotension.

THANK YOU
934d7c6f0b4a0cf9402b40db3e48b9ea.ppt