84d205cfebf55126feaaca4e64a66d81.ppt
- Количество слайдов: 71

Human Immunodeficiency Virus: An Overview Elizabeth W. Delamater, Ph. D. Manager, Microbiological Sciences Division Laboratory Services Section Texas Department of State Health Services
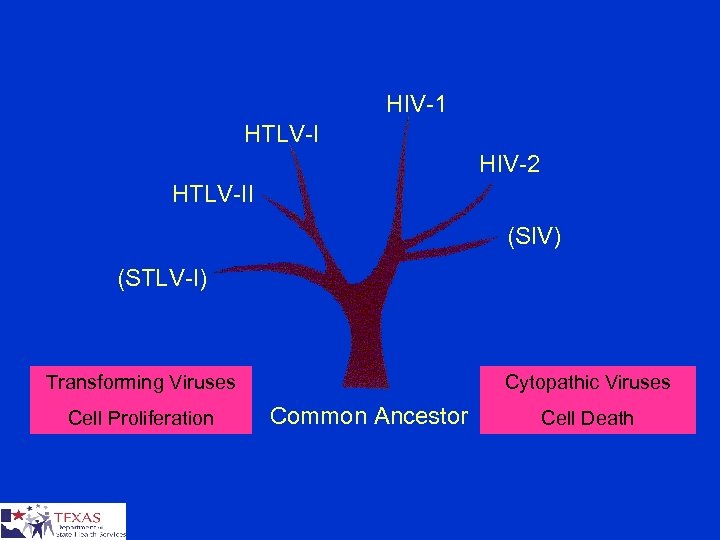
HIV-1 HTLV-I HIV-2 HTLV-II (SIV) (STLV-I) Transforming Viruses Cell Proliferation Cytopathic Viruses Common Ancestor Cell Death

Human Retroviruses - Nomenclature § Human Immunodeficiency Viruses ¤ HIV-1 (1983) • HIV, HTLV III, LAV, ARV – AIDS and related conditions ¤ HIV-2 (1986) • LAV-2, HTLV IV – AIDS (primarily in West Africa)

Human Retrovirus – Characteristics § RNA Tumor (transforming) and immunodeficiency (cytopathic) viruses § Reverse Transcriptase § Integration of the viral genome into the host DNA as a provirus § Primarily infect T-lymphocytes and some neural cells § Exogenous (transmisssible, infectious agents) § Latency (long incubation period)

Brief History of Retroviruses § Transmissible agents capable of causing leukemias and solid-tissue tumors were discovered ¤ ¤ ¤ 1970 – Reverse transcriptase was discovered 1980 – HTLV-I and HTLV-II were isolated 1981 – First AIDS case was discovered 1983 – HIV-1 was isolated 1985 – EIA test for anti-HIV-1 antibodies was licensed by the FDA

Where did HIV come from? • Estimated origin around 1930. • Estimated origin in Africa. • Thought to come from SIV in primates (blood exposure) • Change in travel and social norms caused the world wide epidemic.
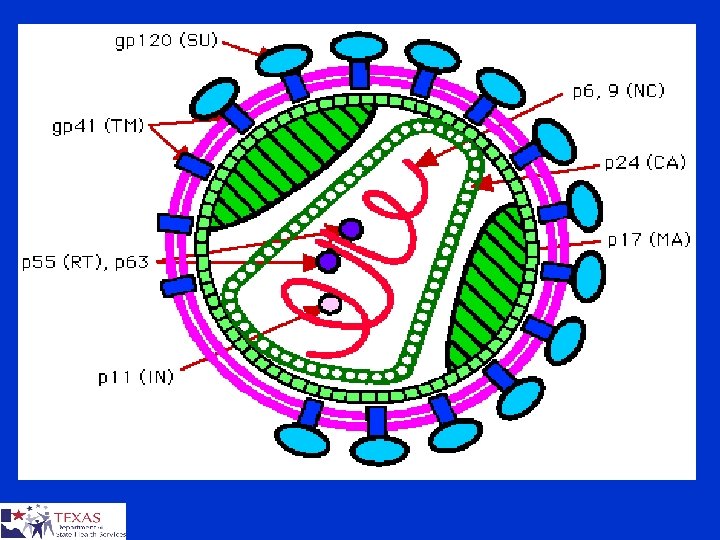
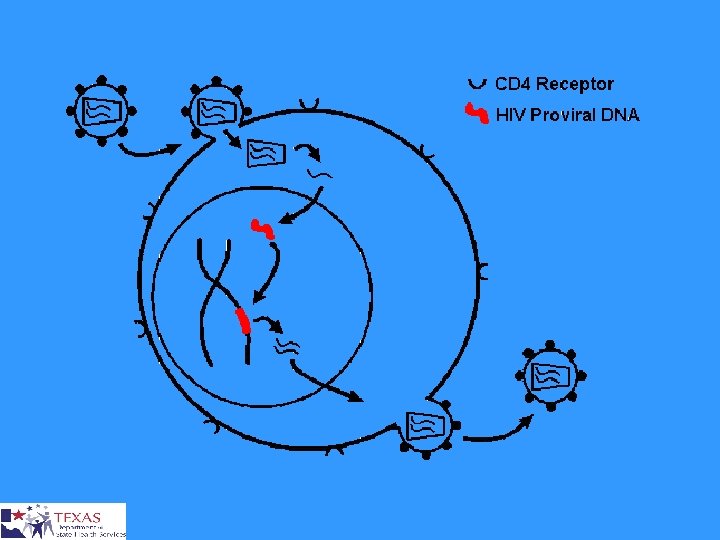

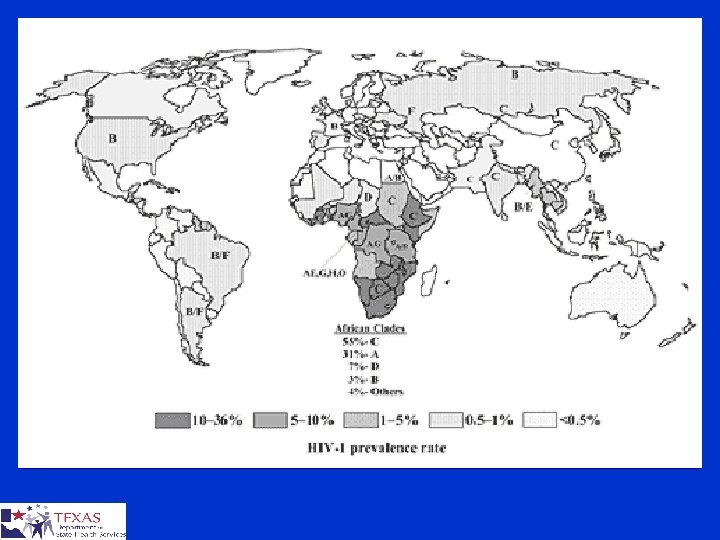
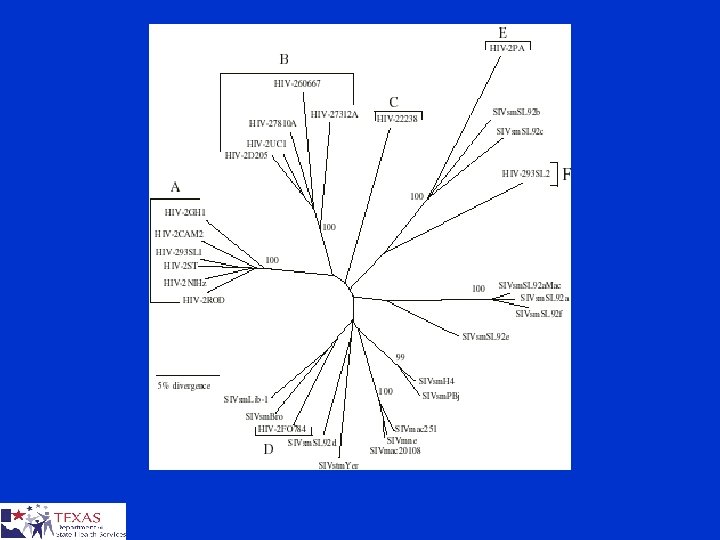
HIV Subtypes § HIV isolates are classified into three different groups ¤ Major group (M) ¤ Outlier group (O) ¤ Non-M / non-O (N) § Groups N and O restricted to West Africa § Based on the analysis of the envelope gene, there at least nine pure subtypes or clades A-D, F-H, J and K

HIV Transmission Requires: 1) Infected body fluid. Blood, Semen, Vaginal Secretions & Breast Milk 2) Entry into the body. Mucous Membrane--Anal, Oral or Vaginal Sex Blood to Blood--Needle or Broken Skin Perinatal- In utero, During birth, Breastfeeding

Routes of Transmission of HIV § Sexual § Homosexual between men § Heterosexual from men to women and women to men § Exposure to blood § Drug user needle sharing § Transfusion of blood, plasma § Occupational needlestick injury and other blood exposures § Perinatal § During pregnancy, intrapartum and postpartum (via breastfeeding)

Perinatal transmission § Greatly reduced due to use of antiretroviral therapy during pregnancy ¤ decrease from 24 to 8% vertical transmission with AZT § Trials using high doses of new antiretrovirals during labor and to newborn--success of Nevirapine § Women with higher viral loads more likely to transmit

Factors Affecting Transmission STD Co-infection More likely to become infected More likely to transmit infection Viral Load Stage of infection Treatment

Disease Progression § Infection § Primary Infection/Antibody Development § Asymptomatic Period (10 -12 yrs average) § AIDS (Opportunistic infections, CD 4 200 or below)
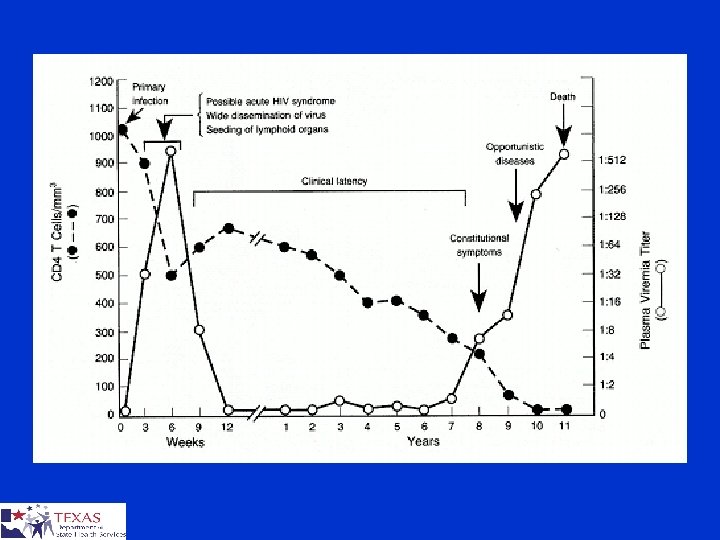

AIDS HIV infected + immune system breakdown (CD 4 count < 200 or AIDS Defining illness) AIDS Defining Illnesses Pnuemocystis pnuemonia Toxoplasmosis Kaposi’s sarcoma Mycobacterium avium complex Invasive cervical cancer etc. . .

Antiretroviral Treatment Triple Drug Cocktail--Attack the virus at different points in the replication process • Difficult Drug Regimens • Importance of Adherence • Side Effects • Expensive
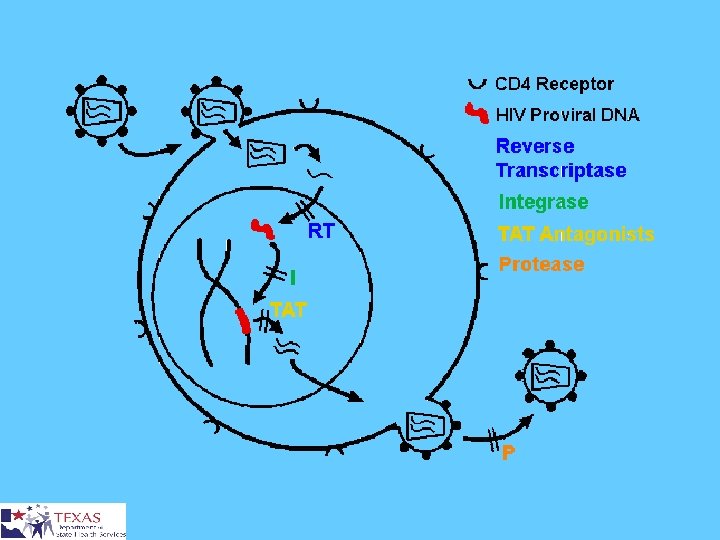

Other Treatment Prophylaxis for Opportunistic Infections Treatment of Opportunistic Infections Vaccines (future) Immune Therapy Alternative Treatment

Difficulties in Treatment § § § Access to Care Family Care Burdens Language Barriers Fragmentation of Care Fears / Myths About Medical Care

Post Exposure Prophylaxis § Treatment with antiretroviral drugs after an exposure to HIV. § Must be started within 72 hours (sooner the better) and continued for a month. § PEP showed a 80% reduction in HIV infections for occupational exposures. § Concerns for drug and sexual exposures
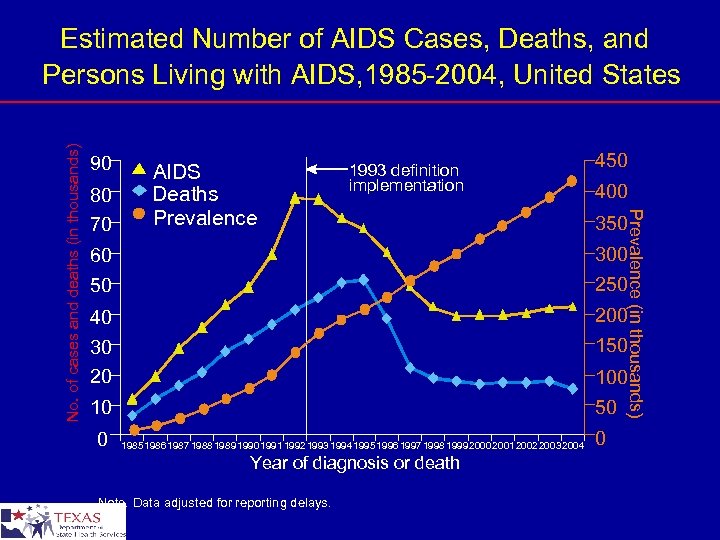
90 80 70 AIDS Deaths Prevalence 1993 definition implementation 450 400 Prevalence (in thousands) No. of cases and deaths (in thousands) Estimated Number of AIDS Cases, Deaths, and Persons Living with AIDS, 1985 -2004, United States 350 60 50 300 250 40 200 150 30 20 10 0 50 198519861987 19881989199019911992199319941995199619971998199920002001 200220032004 Year of diagnosis or death Note. Data adjusted for reporting delays. 0

Awareness of HIV Status among Persons with HIV, United States Number HIV infected Number unaware of their HIV infection Estimated new infections annually 1, 039, 000 – 1, 185, 000 252, 000 - 312, 000 (24%-27%) 40, 000 Glynn M, Rhodes P. 2005 HIV Prevention Conference
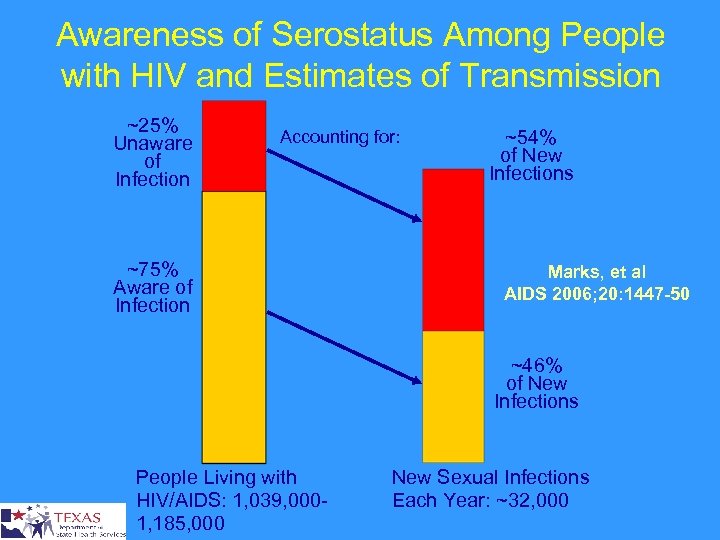
Awareness of Serostatus Among People with HIV and Estimates of Transmission ~25% Unaware of Infection Accounting for: ~75% Aware of Infection ~54% of New Infections Marks, et al AIDS 2006; 20: 1447 -50 ~46% of New Infections People Living with HIV/AIDS: 1, 039, 0001, 185, 000 New Sexual Infections Each Year: ~32, 000
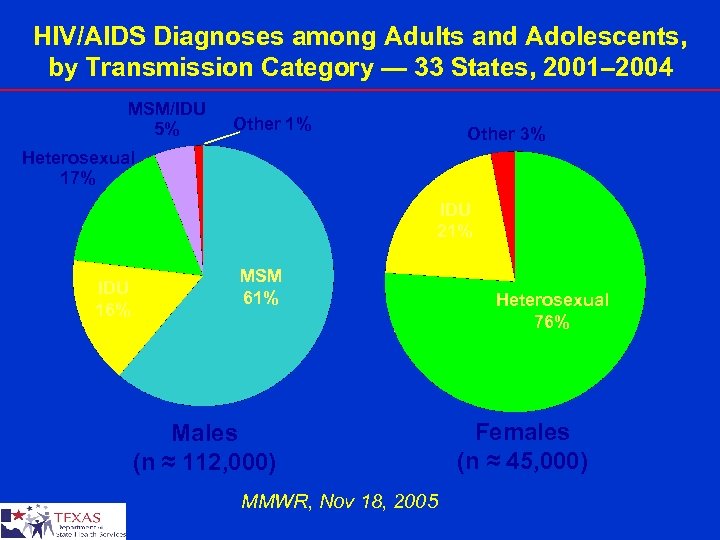
HIV/AIDS Diagnoses among Adults and Adolescents, by Transmission Category — 33 States, 2001– 2004 MSM/IDU 5% Other 1% Other 3% Heterosexual 17% IDU 21% IDU 16% MSM 61% Males (n ≈ 112, 000) MMWR, Nov 18, 2005 Heterosexual 76% Females (n ≈ 45, 000)
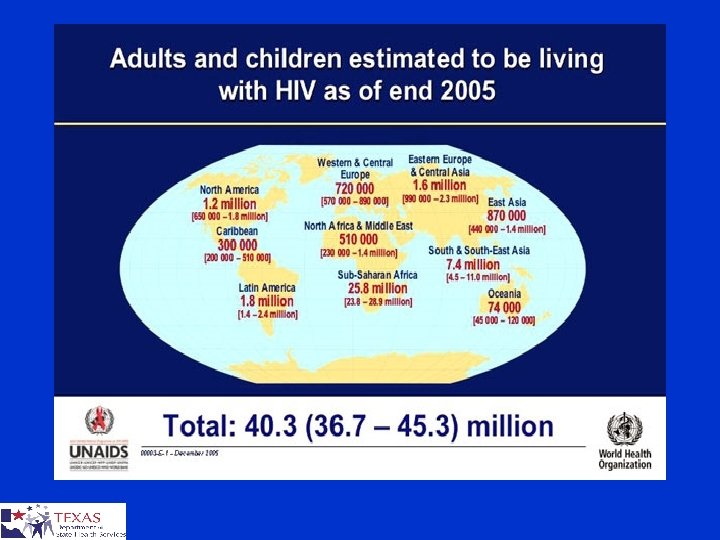
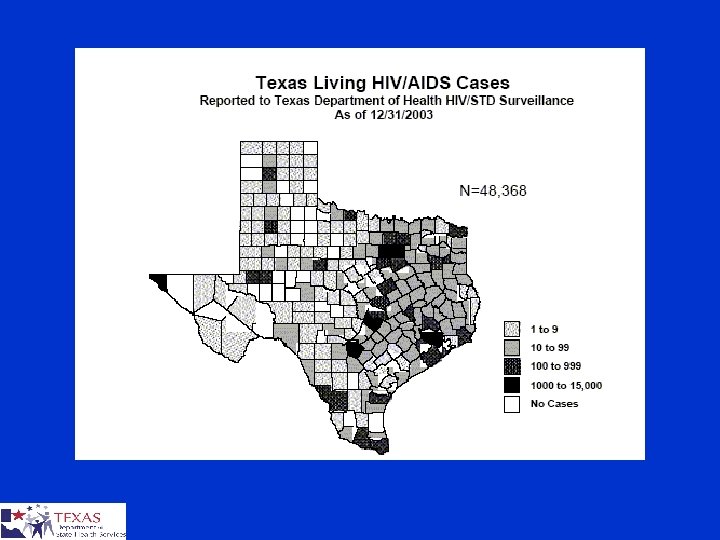

USA § § Numbers of AIDS deaths are falling Number of AIDS diagnosis are falling Rates of HIV infection have NOT changed Trends ¤ ¤ Younger People (25% under age 25) Low Socioeconomic Status IDU Disease of the Marginalized

Knowing You Are Infected: § Primary Infection • 2 -6 wks average • 75 -90% have symptoms § Only way to know for sure: HIV Antibody Test “Window Period”: time to develop antibodies • 3 -6 weeks 85% • 3 months >99%

Testing Technology Technologies § More accurate serum EIA § Oral fluids test § Home test system § Rapid test § Urine test Strategies § Phone results § Augmented counseling § Outreach ¤ Bars, coffee shops, bath houses ¤ Syringe exchanges ¤ Street (vans)
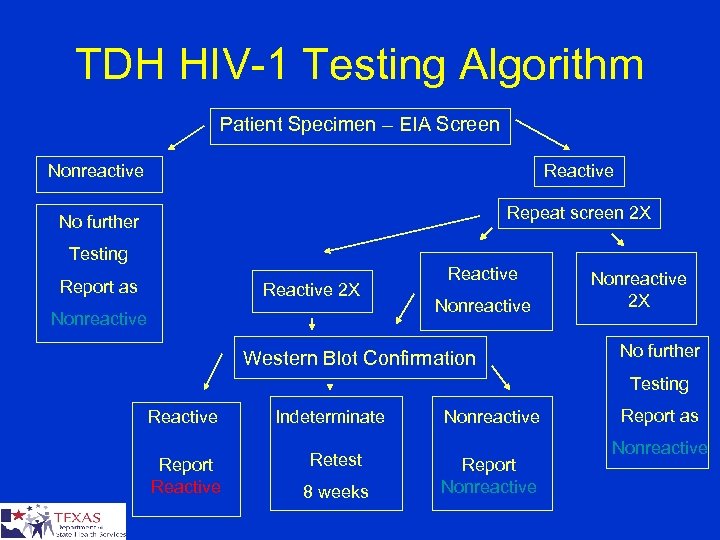
TDH HIV-1 Testing Algorithm Patient Specimen – EIA Screen Nonreactive Reactive No further Repeat screen 2 X Testing Report as Reactive 2 X Nonreactive Reactive Nonreactive Western Blot Confirmation Nonreactive 2 X No further Testing Reactive Report Reactive Indeterminate Retest 8 weeks Nonreactive Report as Nonreactive

HIV Screening Enzyme Immunoassay EIA or ELISA

EIA or ELISA Advantages § § § Simple Sensitive Rapid Can be Automated Suitable for High Volume Testing

EIA or ELISA Limitations § Potential for False Positives § Initial High Reactives must be Repeated

Types of Specimens for Testing Serum or Plasma
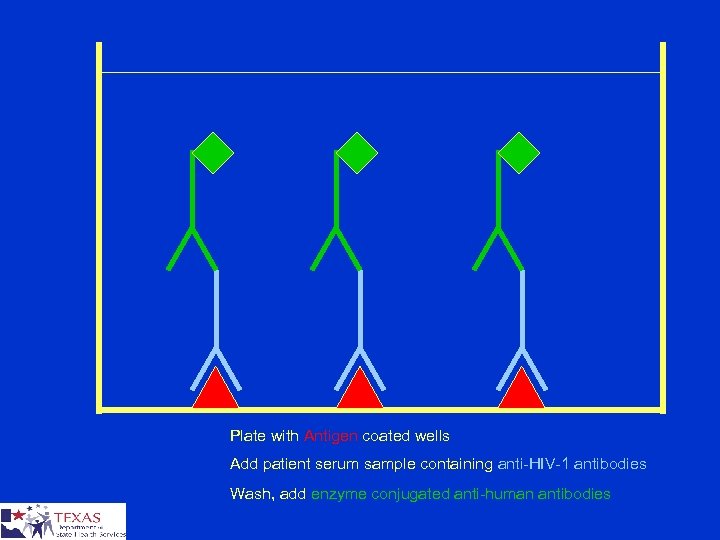
Plate with Antigen coated wells Add patient serum sample containing anti-HIV-1 antibodies Wash, add enzyme conjugated anti-human antibodies
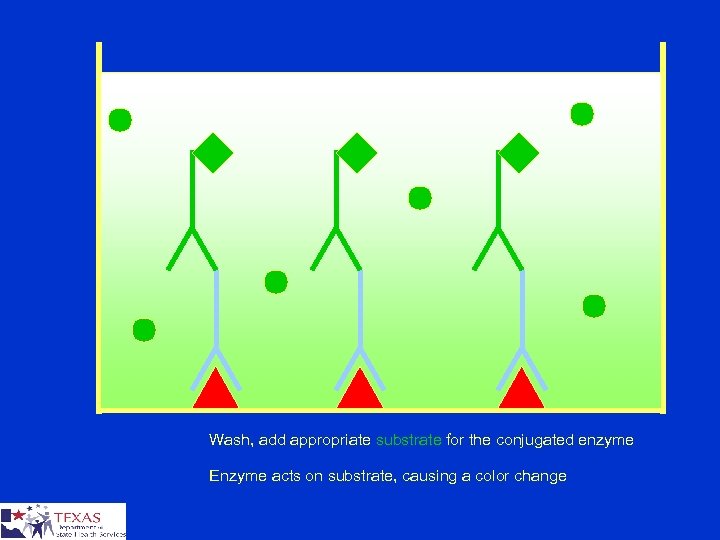
Wash, add appropriate substrate for the conjugated enzyme Enzyme acts on substrate, causing a color change








Types of Specimens for Testing Serum or Plasma Dried Blood Spots


Types of Specimens for Testing Serum or Plasma Dried Blood Spots Oral Fluid

Types of Specimens for Testing Serum or Plasma Dried Blood Spots Oral Fluid Urine

HIV Confirmation Western Blot Immunofluorescent Assay Laboratory Only
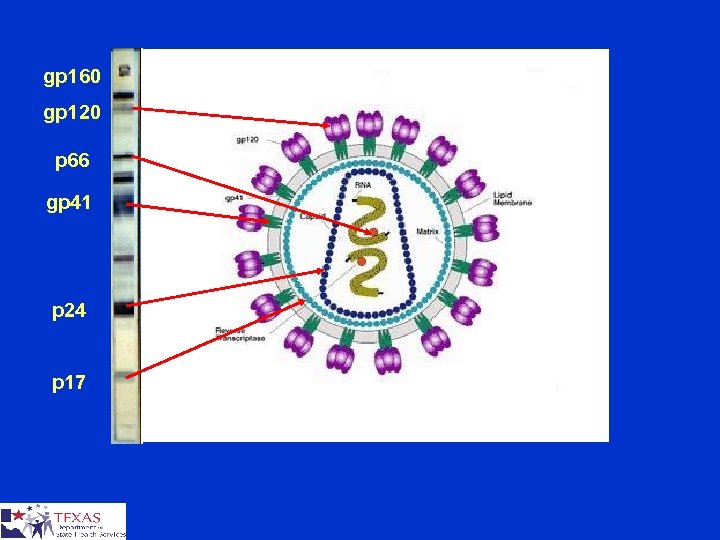
gp 160 gp 120 p 66 gp 41 p 24 p 17

What about HIV-2? Not common in the United States Only about 72 cases confirmed as of 2000
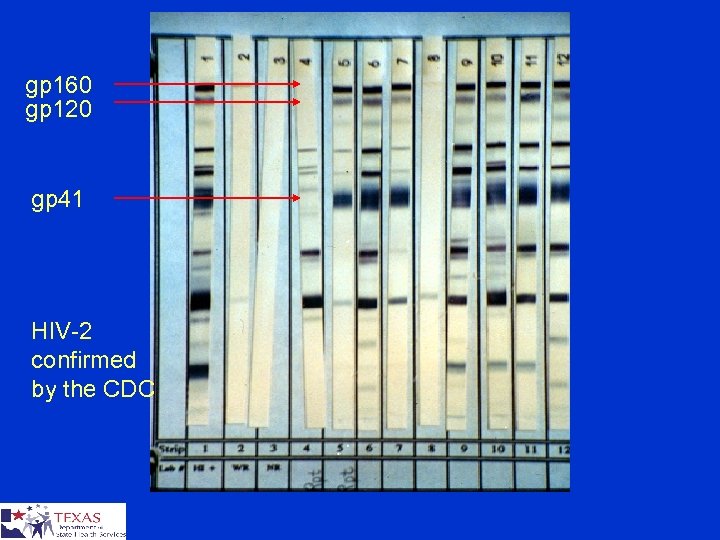
gp 160 gp 120 gp 41 HIV-2 confirmed by the CDC

HIV Rapid Tests

Public Health Need for Rapid HIV Tests § High rates of non-return for test results ¤ In 2000, 31% did not return for results of HIV-positive conventional tests at publicly funded sites § Need for immediate information or referral for treatment choices ¤ Perinatal settings ¤ Post-exposure treatment settings § Screening in high-volume, high-prevalence settings
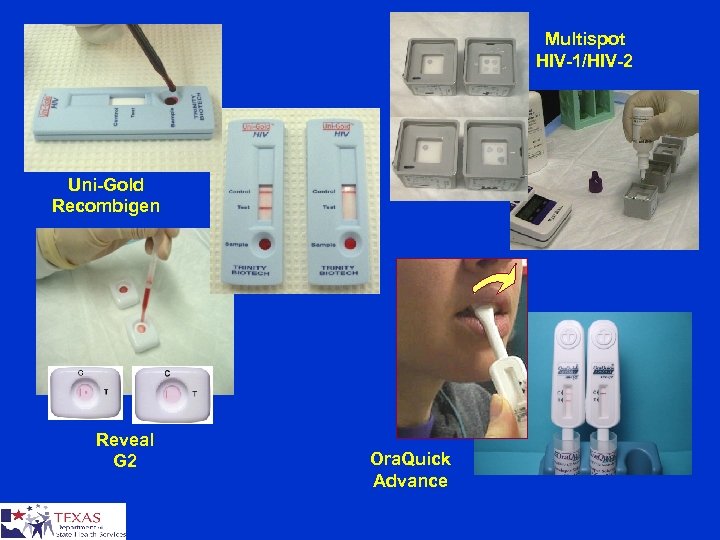
Multispot HIV-1/HIV-2 Uni-Gold Recombigen Reveal G 2 Ora. Quick Advance

Four FDA-approved Rapid HIV Tests Sensitivity (95% C. I. ) Specificity (95% C. I. ) Ora. Quick Advance - whole blood 99. 6 (98. 5 - 99. 9) - oral fluid 99. 3 (98. 4 - 99. 7) - plasma 99. 6 (98. 5 - 99. 9) 100 (99. 7 -100) 99. 8 (99. 6 – 99. 9) 99. 9 (99. 6 – 99. 9) Uni-Gold Recombigen - whole blood 100 (99. 5 – 100) - serum/plasma 100 (99. 5 – 100) 99. 7 (99. 0 – 100) 99. 8 (99. 3 – 100)

Four FDA-approved Rapid HIV Tests Sensitivity (95% C. I. ) Reveal G 2 serum plasma Specificity (95% C. I. ) 99. 8(99. 2 – 100) 99. 8(99. 0 – 100) 99. 1 (98. 8 – 99. 4) 98. 6 (98. 4 – 98. 8) Multispot serum/plasma 100 (99. 9 – 100) 100 (99. 7 – 100) HIV-2 99. 9 (99. 8 – 100)

Revised Recommendations Adults and Adolescents - I § Routine, voluntary HIV screening for all persons 13 -64 in health care settings, not based on risk § Repeat HIV screening of persons with known risk at least annually § Opt-out HIV screening with the opportunity to ask questions and the option to decline § Include HIV consent with general consent for care; separate signed informed consent not recommended § Prevention counseling in conjunctions with HIV screening in health care settings is not required

Opt-Out Screening Prenatal HIV testing for pregnant women: § RCT of 4 counseling models with opt-in consent: ¤ 35% accepted testing ¤ Some women felt accepting an HIV test indicated high risk behavior § Testing offered as routine, opportunity to decline ¤ 88% accepted testing ¤ Significantly less anxious about testing Simpson W, et al, BMJ June, 1999
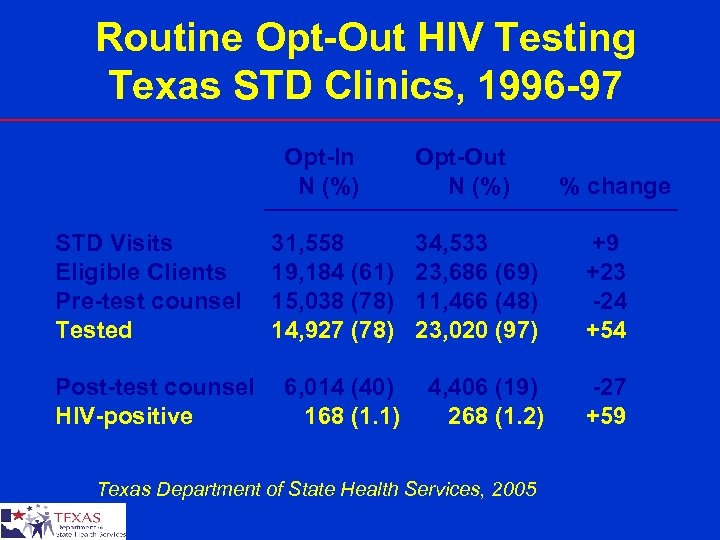
Routine Opt-Out HIV Testing Texas STD Clinics, 1996 -97 Opt-In N (%) STD Visits Eligible Clients Pre-test counsel Tested Post-test counsel HIV-positive Opt-Out N (%) % change 31, 558 19, 184 (61) 15, 038 (78) 14, 927 (78) 34, 533 23, 686 (69) 11, 466 (48) 23, 020 (97) +9 +23 -24 +54 6, 014 (40) 168 (1. 1) 4, 406 (19) 268 (1. 2) -27 +59 Texas Department of State Health Services, 2005

Revised Recommendations Adults and Adolescents - II § Intended for all health care settings, including inpatient services, EDs, urgent care clinics, STD clinics, TB clinics, public health clinics, community clinics, substance abuse treatment centers, correctional health facilities, primary care settings § Communicate test results in same manner as other diagnostic/screening tests § Provide clinical HIV care or establish reliable referral to qualified providers

Revised Recommendations Adults and Adolescents - III § Low prevalence settings: ¤ Initiate screening ¤ If yield from screening is less than 1 per 1000, continued screening is not warranted § Steps should be considered to resolve conflicts between the recommendations and state or local regulations

Revised Recommendations Pregnant Women - I § Universal opt-out HIV screening ¤ Include HIV in routine panel of prenatal screening tests ¤ Consent for prenatal care includes HIV testing ¤ Notification and option to decline § Second test in 3 rd trimester for pregnant women: ¤ Known to be at risk for HIV ¤ In jurisdictions with elevated HIV incidence ¤ In high HIV prevalence health care facilities

Revised Recommendations Pregnant Women - II § Opt-out rapid testing with option to decline for women with undocumented HIV status in L&D ¤ Initiate ARV prophylaxis on basis of rapid test result § Rapid testing of newborn recommended if mother’s status unknown at delivery ¤ Initiate ARV prophylaxis within 12 hours of birth on basis of rapid test result

Summary § There is an urgent need to increase the proportion of persons who are aware of their HIV-infection status § Expanded, routine, voluntary, opt-out screening in health care settings is needed § Such screening is cost-effective § Recommendations Revised: September 2006 § Several jurisdictions have already begun

Key Messages § The large majority of people with HIV continue to be men who have sex with men. People of color are disproportionately represented among new infections § The basic modes of transmission and prevention of HIV have not changed in 20 years § The AIDS epidemic is not over, but there is more hope than ever for those that are infected
84d205cfebf55126feaaca4e64a66d81.ppt