bf159ffe41c028836ecedf141963e75f.ppt
- Количество слайдов: 32

Human Capital: The Critical Role of Behavioral Services and How New Approaches Will Drive Dollar Savings and Improved Personal Outcomes Integrated Health Services Seminar David Whitehouse, M. D. Optum. Health Behavioral Solutions CMO Strategy and Innovation

The Importance of Health and Human Capital Just as a company focuses on its financial capital and economic assets, it needs to focus on its human capital and health assets. The health of a workforce is inextricably linked to the productivity of the workforce and therefore the health of the bottom line. Investing in health not only controls expenses, but also protects, supports, and enhances human capital – which will be one of the differentiators for companies in the global marketplace. It is an investment to be leveraged rather than a cost to be justified. Dr. Pamela Hymel ACOEM Board of Directors Consensus growing among employers that better employee health equals better business Mercer, United States New York, 24 October 2007 2
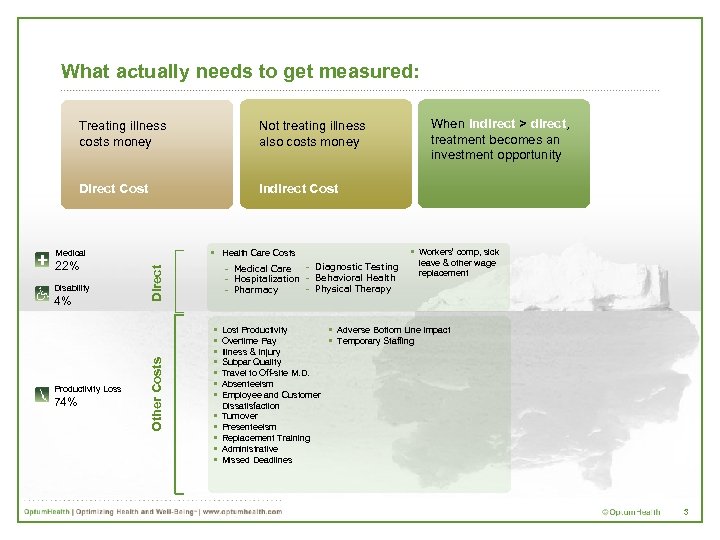
What actually needs to get measured: Treating illness costs money Not treating illness also costs money Direct Cost Indirect Cost § Health Care Costs Disability 4% Productivity Loss Other Costs 22% - Diagnostic Testing - Medical Care - Hospitalization - Behavioral Health - Physical Therapy - Pharmacy Direct Medical 74% When indirect > direct, treatment becomes an investment opportunity § § § § Workers’ comp, sick leave & other wage replacement Lost Productivity § Adverse Bottom Line Impact Overtime Pay § Temporary Staffing Illness & Injury Subpar Quality Travel to Off-site M. D. Absenteeism Employee and Customer Dissatisfaction Turnover Presenteeism Replacement Training Administrative Missed Deadlines 3
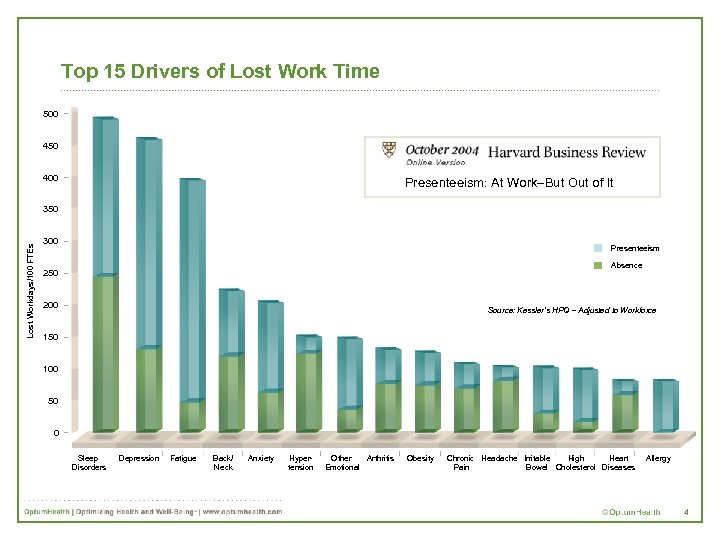
Top 15 Drivers of Lost Work Time 500 450 400 Presenteeism: At Work–But Out of It Lost Workdays/100 FTEs 350 300 Presenteeism Absence 250 200 Source: Kessler’s HPQ – Adjusted to Workforce 150 100 50 0 Sleep Disorders Depression Fatigue Back/ Neck Anxiety Hypertension Other Arthritis Emotional Obesity Chronic Headache Irritable High Heart Pain Bowel Cholesterol Diseases Allergy 4
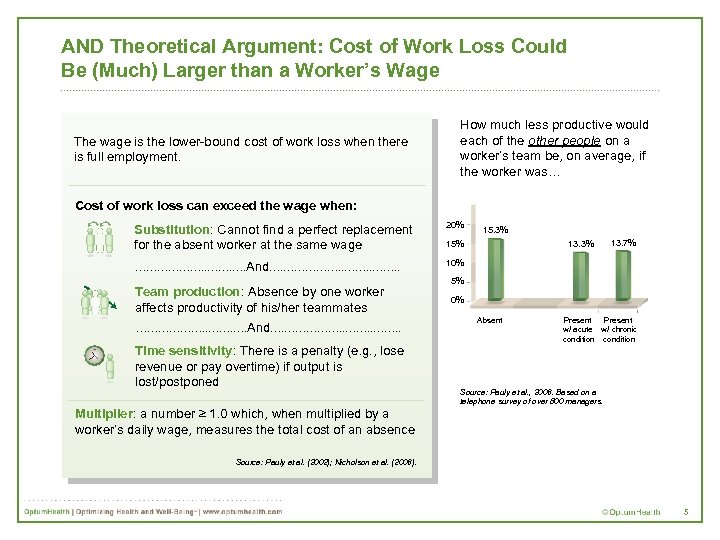
AND Theoretical Argument: Cost of Work Loss Could Be (Much) Larger than a Worker’s Wage The wage is the lower-bound cost of work loss when there is full employment. How much less productive would each of the other people on a worker’s team be, on average, if the worker was… Cost of work loss can exceed the wage when: Substitution: Cannot find a perfect replacement for the absent worker at the same wage 20% ………………. …. And…. ……………. . 10% Team production: Absence by one worker affects productivity of his/her teammates ………………. …. And…. ……………. . Time sensitivity: There is a penalty (e. g. , lose revenue or pay overtime) if output is lost/postponed 15. 3% 13. 3% 15% 13. 7% 5% 0% Absent Present w/ acute w/ chronic condition Source: Pauly et al. , 2006. Based on a telephone survey of over 800 managers. Multiplier: a number ≥ 1. 0 which, when multiplied by a worker’s daily wage, measures the total cost of an absence Source: Pauly et al. (2002); Nicholson et al. (2006). 5
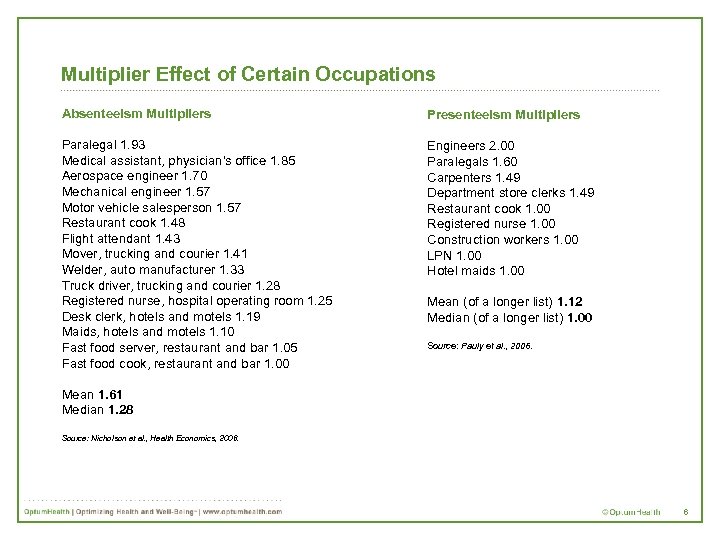
Multiplier Effect of Certain Occupations Absenteeism Multipliers Presenteeism Multipliers Paralegal 1. 93 Medical assistant, physician's office 1. 85 Aerospace engineer 1. 70 Mechanical engineer 1. 57 Motor vehicle salesperson 1. 57 Restaurant cook 1. 48 Flight attendant 1. 43 Mover, trucking and courier 1. 41 Welder, auto manufacturer 1. 33 Truck driver, trucking and courier 1. 28 Registered nurse, hospital operating room 1. 25 Desk clerk, hotels and motels 1. 19 Maids, hotels and motels 1. 10 Fast food server, restaurant and bar 1. 05 Fast food cook, restaurant and bar 1. 00 Engineers 2. 00 Paralegals 1. 60 Carpenters 1. 49 Department store clerks 1. 49 Restaurant cook 1. 00 Registered nurse 1. 00 Construction workers 1. 00 LPN 1. 00 Hotel maids 1. 00 Mean (of a longer list) 1. 12 Median (of a longer list) 1. 00 Source: Pauly et al. , 2006. Mean 1. 61 Median 1. 28 Source: Nicholson et al. , Health Economics, 2006. 6
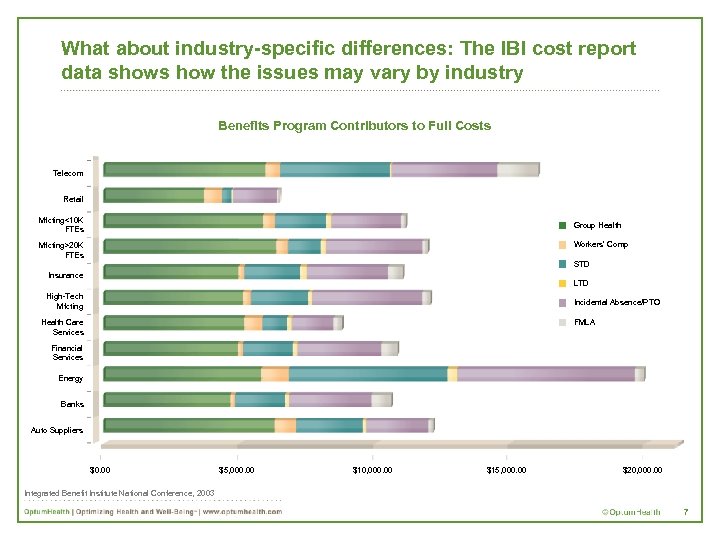
What about industry-specific differences: The IBI cost report data shows how the issues may vary by industry Benefits Program Contributors to Full Costs Telecom Retail Mfcting<10 K FTEs Group Health Workers’ Comp Mfcting>20 K FTEs STD Insurance LTD High-Tech Mfcting Incidental Absence/PTO FMLA Health Care Services Financial Services Energy Banks Auto Suppliers $0. 00 $5, 000. 00 $10, 000. 00 $15, 000. 00 $20, 000. 00 Integrated Benefit Institute National Conference, 2003 7

Other Drivers of Employer Decisions Awareness of: § Investment in Health § The Quality Problem: § The role of behavior in determining health status …and changing it Ø incentives, deterrents, responsibility, consumerism, motivation, health psychology § Ecological Medicine § Personalized Medicine We have the most expensive repair and recovery health system in the world… Bob Galvin, NBGH On average, patients receive 55% of recommended processes, including preventive care, acute care and care for chronic conditions. Source: Mc. Glynn, et al, 2003 Preventable adverse events are a leading cause of death in the United States. Source: IOM, 1999 8

Consumer-centric It is more important to know what sort of person has a disease than to know what sort of disease a person has. Hippocrates 470 -410 BCE You don’t know me. You don’t know my life. Why would I trust you? It is all about being personal; personal in interactions and personal in medical approach. 9
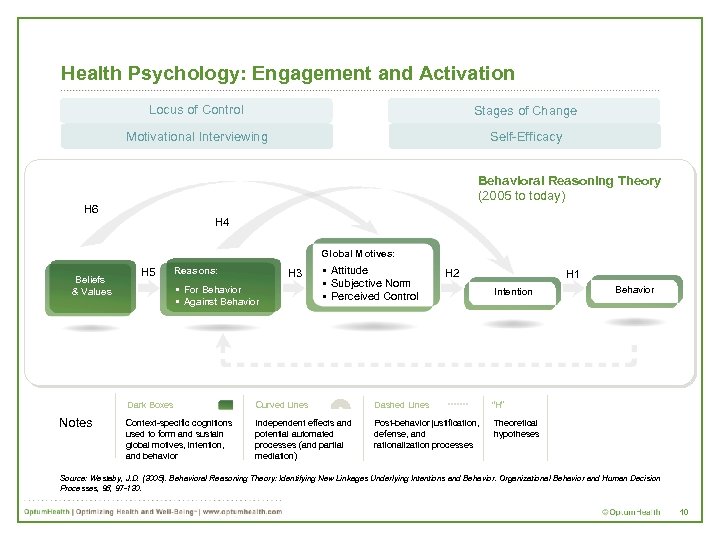
Health Psychology: Engagement and Activation Locus of Control Stages of Change Motivational Interviewing Self-Efficacy Behavioral Reasoning Theory (2005 to today) H 6 H 4 Global Motives: Beliefs & Values H 5 Reasons: H 3 § For Behavior § Against Behavior § Attitude § Subjective Norm § Perceived Control H 2 H 1 Intention Reasons: Dark Boxes Notes Curved Lines Dashed Lines “H” Context-specific cognitions used to form and sustain global motives, intention, and behavior Independent effects and potential automated processes (and partial mediation) Post-behavior justification, defense, and rationalization processes Behavior Theoretical hypotheses Source: Westaby, J. D. (2005). Behavioral Reasoning Theory: Identifying New Linkages Underlying Intentions and Behavior. Organizational Behavior and Human Decision Processes, 98, 97 -120. 10
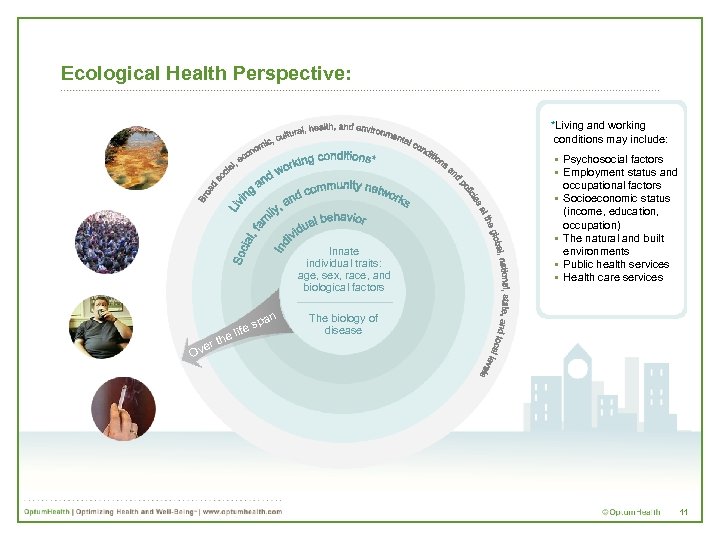
Ecological Health Perspective: *Living and working conditions may include: Innate individual traits: age, sex, race, and biological factors er Ov th spa ife e l n § Psychosocial factors § Employment status and occupational factors § Socioeconomic status (income, education, occupation) § The natural and built environments § Public health services § Health care services The biology of disease 11

Mental Health: The Critical Success Factor 12

Impact of Diseases of the Nervous System § Affect 1 in 3 Americans* § Exact an economic cost of over $500 billion per year** § Have a major impact on: - Academic performance - Workplace productivity - Social functioning - Quality of life Sources: * CDC; ** Sf. N Fact Page 13

Causes of Disability by Illness Category United States and Canada 15 -44 years old October 2, 2007 Mental Illness* 1. 3 billion mental health days Alcohol and Drug Use Injuries, including self-inflicted Disorders like anxiety and depression top the list of work absences, a study says, with back and neck pain close behind. Adult Americans with depression, anxiety or other Musculoskeletal Disease psychological disorders annually miss 1. 3 billion days Sense Organ Disease work, school or other daily activity, according to the of report today in the Archives of General Psychiatry. Back Cardiovascular Disease and neck pain cause sufferers to miss 1. 2 billion days, the report said. Migraine Among mental disorders, depression accounted for the Infectious Disease, most sick days, 387 million. Other reasons included social excluding HIV phobia, 214 million days; post-traumatic stress disorder, 113 million; generalized anxiety disorder, 110 million; 0 5 10 15 20 25 30 bipolar disorder, 103 million; panic disorders, 101 million; substance abuse, 93 million; agoraphobia, 37 million; and separation anxiety disorder, 20 million. WHO World Health Report 2002 Respiratory Disease 35 40 WHO World Health Report 2002 14
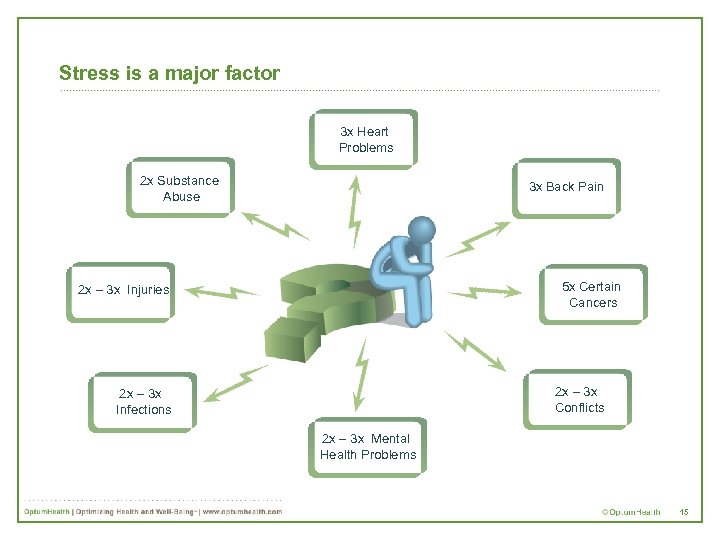
Stress is a major factor 3 x Heart Problems 2 x Substance Abuse 3 x Back Pain 5 x Certain Cancers 2 x – 3 x Injuries 2 x – 3 x Conflicts 2 x – 3 x Infections 2 x – 3 x Mental Health Problems 15
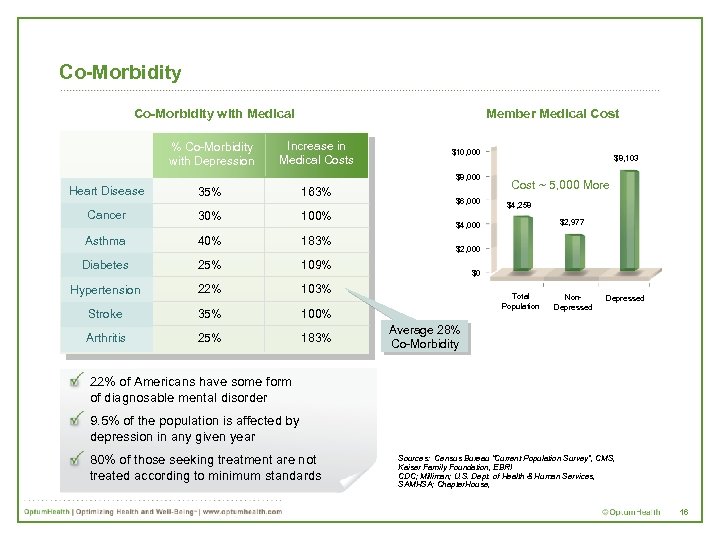
Co-Morbidity with Medical % Co-Morbidity with Depression Member Medical Cost Increase in Medical Costs $10, 000 $8, 000 Heart Disease 35% 163% Cancer 30% 100% Asthma 40% 183% Diabetes 25% 109% Hypertension 22% 103% Stroke 35% 100% Arthritis 25% 183% $6, 000 $8, 103 Cost ~ 5, 000 More $4, 258 $2, 977 $4, 000 $2, 000 $0 Total Population Non. Depressed Average 28% Co-Morbidity 22% of Americans have some form of diagnosable mental disorder 9. 5% of the population is affected by depression in any given year 80% of those seeking treatment are not treated according to minimum standards Sources: Census Bureau “Current Population Survey”, CMS, Kaiser Family Foundation, EBRI CDC; Milliman; U. S. Dept. of Health & Human Services, SAMHSA; Chapter. House, 16
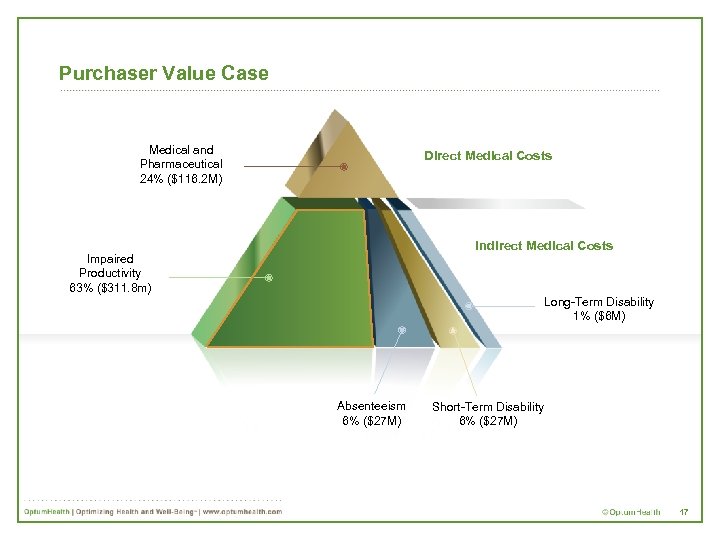
Purchaser Value Case Medical and Pharmaceutical 24% ($116. 2 M) Impaired Productivity 63% ($311. 8 m) Direct Medical Costs Copyri ght © 2004 Harvar d Busine ss School Publis hing Corpor ation. All rights reserv ed. Sourc e: Bank One. Figure s based on 2000 annual data. Worke rs’ compe nsatio n accou nted for < 1% of indirec t medic al costs. Indirect Medical Costs Long-Term Disability 1% ($6 M) Absenteeism 6% ($27 M) Short-Term Disability 6% ($27 M) 17
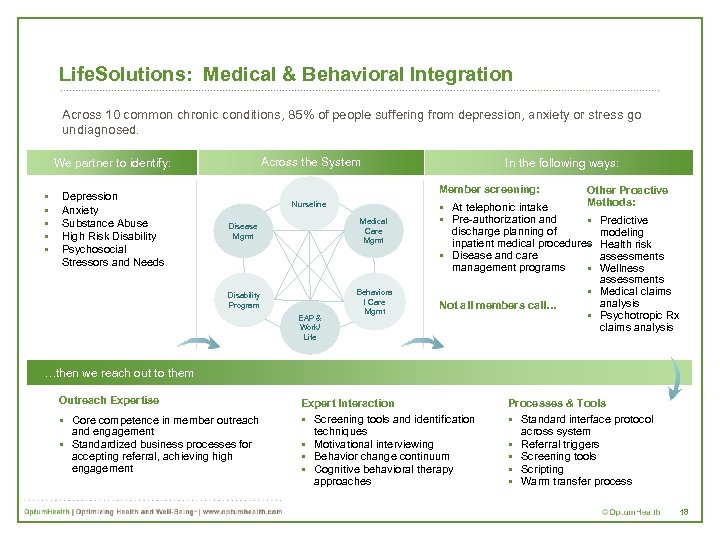
Life. Solutions: Medical & Behavioral Integration Across 10 common chronic conditions, 85% of people suffering from depression, anxiety or stress go undiagnosed. § § § Depression Anxiety Substance Abuse High Risk Disability Psychosocial Stressors and Needs In the following ways: Across the System We partner to identify: Member screening: Nurseline Disease Mgmt Medical Care Mgmt Disability Program Behaviora l Care Mgmt EAP & Work/ Life § At telephonic intake § Pre-authorization and Other Proactive Methods: § Predictive discharge planning of inpatient medical procedures § § Disease and care management programs § Not all members call… modeling Health risk assessments Wellness assessments § Medical claims analysis § Psychotropic Rx claims analysis …then we reach out to them Outreach Expertise § Core competence in member outreach and engagement § Standardized business processes for accepting referral, achieving high engagement Expert Interaction § Screening tools and identification techniques § Motivational interviewing § Behavior change continuum § Cognitive behavioral therapy approaches Processes & Tools § Standard interface protocol across system § Referral triggers § Screening tools § Scripting § Warm transfer process 18

Life. Solutions 2007 Results 1 Increase in Percent of Members Using Any BH Services § Participants were nearly three times more likely than non-participants to use services in the three months following their referral - statistically significant. § 14% increase in number of participants using any bh services vs. only a 4% increase in number of non-participants (below) - statistically significant. § Increase in percent of members using outpatient services alone was even greater (18% increase in participants vs. 7% in non-participants) - statistically significant. 40 Average percent of members using any bh services (3 mos. ) 35 35 30 % 25 21 20 15 22 18 10 5 0 3 mos. Before Participants 3 mos. After Non-Participants Program Membership 2007 Referral Activity: § 19, 744 members were referred to the program – 11, 308 members referred via a referral partner – 70% contacted, 87% of those contacted were engaged § 8, 436 members referred via data driven identification (claims, HRA, etc. ) – 22% who received a letter and phone outreach were contacted, 71% of those contacted were engaged 19
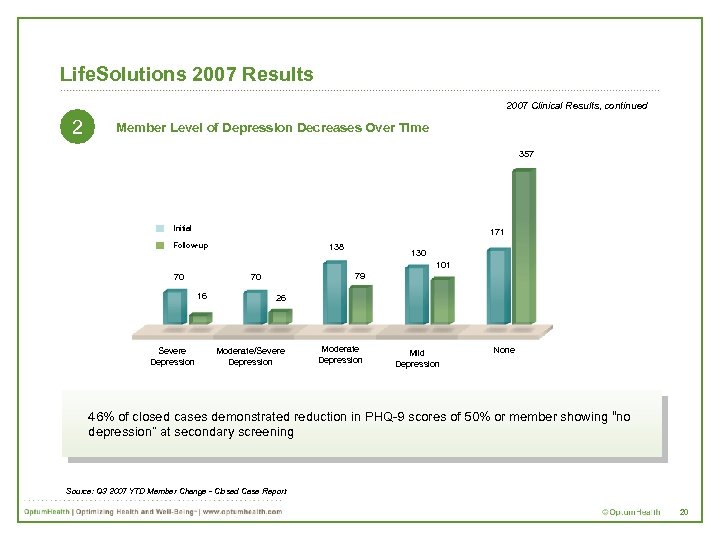
Life. Solutions 2007 Results 2007 Clinical Results, continued 2 Member Level of Depression Decreases Over Time 357 Initial 171 Follow-up 138 130 101 70 16 Severe Depression 79 70 26 Moderate/Severe Depression Moderate Depression Mild Depression None 46% of closed cases demonstrated reduction in PHQ-9 scores of 50% or member showing “no depression” at secondary screening Source: Q 3 2007 YTD Member Change - Closed Case Report 20
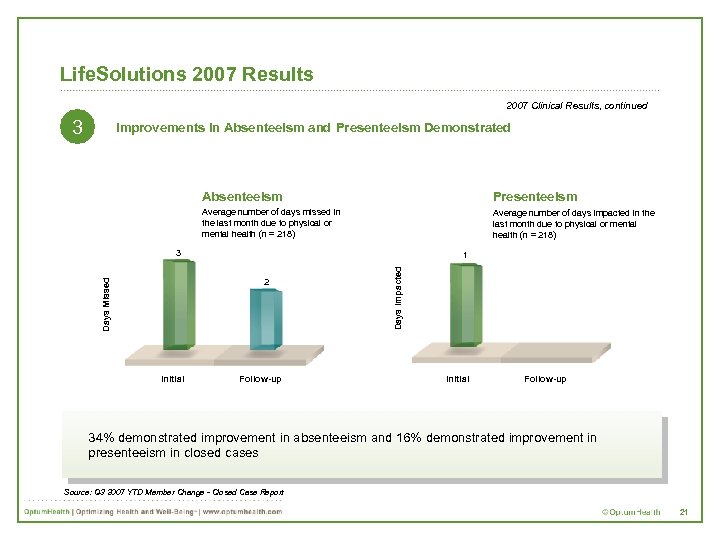
Life. Solutions 2007 Results 2007 Clinical Results, continued 3 Improvements in Absenteeism and Presenteeism Demonstrated Absenteeism Presenteeism Average number of days missed in the last month due to physical or mental health (n = 218) Average number of days impacted in the last month due to physical or mental health (n = 218) 3 Days Missed 2 Initial Follow-up Days Impacted 1 Initial Follow-up 34% demonstrated improvement in absenteeism and 16% demonstrated improvement in presenteeism in closed cases Source: Q 3 2007 YTD Member Change - Closed Case Report 21

Optum. Health Behavioral Solutions Intervention and Productivity Impact Telephone Screening, Outreach, and Care Management for Depressed Workers and Impact on Clinical and Work Productivity Outcomes – A Randomized Controlled Trial Philip S. Wang, M. D. , Dr. P. H. ; Gregory E. Simon, M. D. , MPH; Jerry Avorn, M. D. ; Francisca Azocar, Ph. D. ; Evette J. Ludman, Ph. D. ; Joyce Mc. Culloch, M. S. ; Maria Z. Petukhova, Ph. D. ; Ronald C. Kessler, Ph. D. JAMA. 2007; 298: 1401 -1411. § Landmark study conducted by Harvard Medical Group, Optum. Health Behavioral Solutions, and Group Health Cooperative’s Center for Health Studies § Demonstrated a 2. 6 hour improvement per week in overall work function for intervention group § Lower depression severity for the intervention group § Intervention group was more likely to seek specialist intervention for depression Study: Firms should help unhappy workers By Lindsey Tanner, AP Medical Writer | September 25, 2007 § Employees who received aggressive intervention worked on average about two weeks more during the year-long study than those who received usual care–advice to see their doctor or seek a mental health specialist. § More workers in the intervention group were still employed by year's end– 93 percent vs. 88 percent– savings that helped employers avoid hiring and training costs, the researchers said. § Intervention employees were almost 40 percent more likely to recover from depression during the yearlong study, which is reported in the JAMA article. § Researchers haven't finalized a formal cost-benefits analysis but early results suggest savings from more hours worked averaged to about $1, 800 per employee. This estimate far exceeds the program's initial $100 to $400 per worker cost. § Preliminary findings also show benefits likely exceed other costs, including drugs and therapy. 22
Global Service Centers § § § § § § U. S. U. K. Belgium Germany Spain Greece Italy South Africa Israel Mexico India China Hong Kong Japan Singapore Malaysia Indonesia Korea Australia New Zealand Brazil Argentina 23

Current Solutions: § Access to Treatment § Treatment Effectiveness § The Status Quo Is Unacceptable § Innovation Is Essential 24
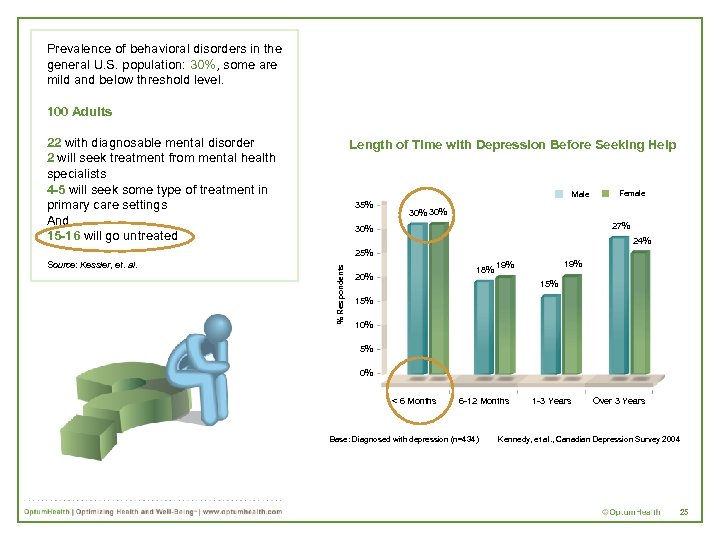
Prevalence of behavioral disorders in the general U. S. population: 30%, some are mild and below threshold level. 100 Adults 22 with diagnosable mental disorder 2 will seek treatment from mental health specialists 4 -5 will seek some type of treatment in primary care settings And 15 -16 will go untreated Length of Time with Depression Before Seeking Help Male 35% Female 30% 27% 30% 24% % Respondents 25% Source: Kessler, et. al. 19% 18% 19% 20% 15% 10% 5% 0% < 6 Months 6 -12 Months Base: Diagnosed with depression (n=434) 1 -3 Years Over 3 Years Kennedy, et al. , Canadian Depression Survey 2004 25
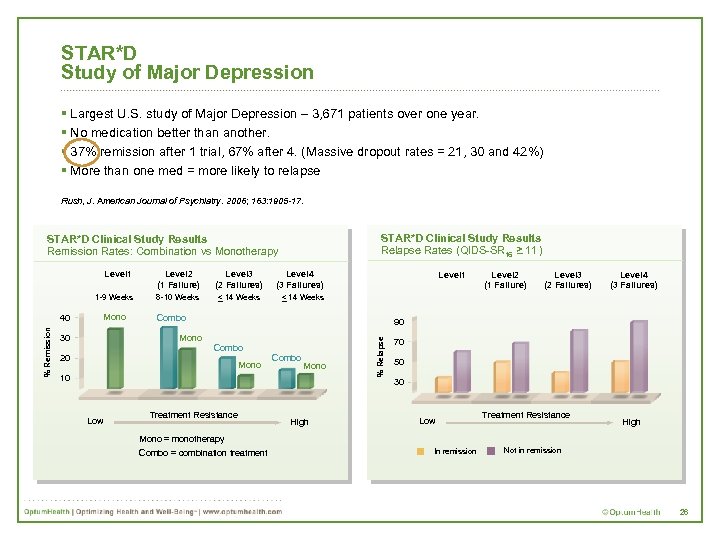
STAR*D Study of Major Depression § Largest U. S. study of Major Depression – 3, 671 patients over one year. § No medication better than another. § 37% remission after 1 trial, 67% after 4. (Massive dropout rates = 21, 30 and 42%) § More than one med = more likely to relapse Rush, J. American Journal of Psychiatry. 2006; 163: 1905 -17. STAR*D Clinical Study Results _ Relapse Rates (QIDS-SR ) 16 > 11 STAR*D Clinical Study Results Remission Rates: Combination vs Monotherapy Level 1 Level 4 (3 Failures) 8 -10 Weeks _ < 14 Weeks Mono 30 Combo Level 2 (1 Failure) Level 3 (2 Failures) Level 4 (3 Failures) 90 Mono Combo 20 Level 1 Mono Combo Mono 10 % Relapse % Remission Level 3 (2 Failures) 1 -9 Weeks 40 Level 2 (1 Failure) 70 50 30 Low Treatment Resistance High Mono = monotherapy Combo = combination treatment In remission Not in remission 26

Methods and Findings We obtained data on all clinical trials submitted to the U. S. Food and Drug Administration (FDA) for the licensing of the four new-generation antidepressants for which full datasets were available. We then used metaanalytic techniques to assess linear and quadratic effects of initial severity on improvement scores for drug and placebo groups and on drug–placebo difference scores. Drug–placebo differences increased as a function of initial severity, rising from virtually no difference at moderate levels of initial depression to a relatively small difference for patients with very severe depression, reaching conventional criteria for clinical significance only for patients at the upper end of the very severely depressed category. Metaregression analyses indicated that the relation of baseline severity and improvement was curvilinear in drug groups and showed a strong, negative linear component in placebo groups. Conclusions Drug–placebo differences in antidepressant efficacy increase as a function of baseline severity, but are relatively small even for severely depressed patients. The relationship between initial severity and antidepressant efficacy is attributable to decreased responsiveness to placebo among very severely depressed patients, rather than to increased responsiveness to medication. 27

Mental Health Care in the Pre-Genomic Era? ? ? § Depressive disorders are prevalent, disabling, often chronic/recurrent. § Long-term outcomes are poorly studied. § Acute response/remission rates decline with the need for more acute treatments. § Relapse rates rise with greater levels of resistance. § Biomarkers hold the promise of individualized clinical decision-making. 28

What if? § What if we could really identify the people at risk for depression? § What if we could tell whether stress and anxiety were impacting people’s ability to be effective at work (even the alexithymics)? § What if, when people became disabled, we could tell precisely and specifically how their illness was impacting them in terms of really being able to quantify and track decline or improvement in their specific emotional, cognitive, and executive functioning capacities? § What if we could use the above to also make better, more patient-specific treatment selections? § What if we could tell not only whether people’s symptoms were improving but whether they had regained full functionality? § What if we could do all this cost-effectively, easily, and readily? 29

Why Personalized Medicine? The right treatment for the right person at the right time § Current clinical practice: “one size fits all” population-based treatment model comparing member to signs and symptoms § The harsh reality is that many treatments do not work in a significant percentage of patients; with serious side effects, lack of compliance, and modest benefit beyond placebo effects § Trial-and-error solutions lead to over-servicing escalation of costs/inefficiencies, increased morbidity, failure to fill scripts § These limitations, negative impacts, patient morbidity, and economic imperatives are driving a new paradigm of “Personalized Medicine” (PM) 30

Elements of Personalized Medicine Establishing a baseline: better science means better health care at a lower cost Personalized Medicine proactively tailors treatment programs to each individual’s biological and psychological profile in an integrative approach. I am persuaded that personalized health care creates value; The goal is to have better health care at lower cost for every American. Honorable Mike Leavitt, Secretary of Health and Human Services as quoted by Cooney, Boston Globe, 11/29/07. Personalized medicine begins with a baseline screening: Individuals then serve as their own controls to objectively monitor response to solution options based on their unique identity. 31
Why Does Cardiology Have to Be So Different? 32
bf159ffe41c028836ecedf141963e75f.ppt