12a1f005b4f6d6f62bd48d63c0812061.ppt
- Количество слайдов: 37
 How to conduct an excellent sign-out Leora Horwitz, MD Medicine Boot Camp leora. horwitz@yale. edu
How to conduct an excellent sign-out Leora Horwitz, MD Medicine Boot Camp leora. horwitz@yale. edu
 Why is sign-out important? • Frequent • Skill set • Potentially dangerous
Why is sign-out important? • Frequent • Skill set • Potentially dangerous
 Safety attitude questionnaire • Shift changes are problematic for patients in this hospital • Important patient care information is often lost during shift changes • Problems often occur in the exchange of information across hospital units • Things “fall between the cracks” when transferring patients from one unit to another
Safety attitude questionnaire • Shift changes are problematic for patients in this hospital • Important patient care information is often lost during shift changes • Problems often occur in the exchange of information across hospital units • Things “fall between the cracks” when transferring patients from one unit to another
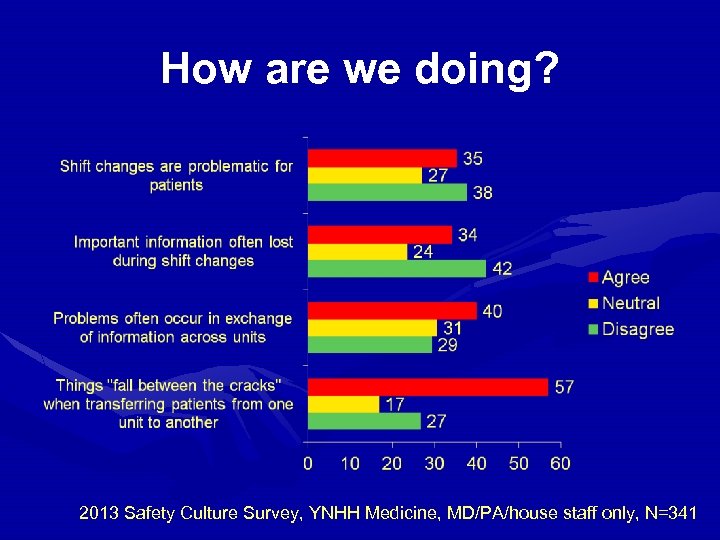 How are we doing? 2013 Safety Culture Survey, YNHH Medicine, MD/PA/house staff only, N=341
How are we doing? 2013 Safety Culture Survey, YNHH Medicine, MD/PA/house staff only, N=341
 What information is needed? • Name, age, gender, room, family contact info, language, attending, consultants • Code status • Past medical history, allergies, meds, labs • Admission diagnosis • Hospital course • Scheduled events • Clinical condition • To dos, anticipatory guidance
What information is needed? • Name, age, gender, room, family contact info, language, attending, consultants • Code status • Past medical history, allergies, meds, labs • Admission diagnosis • Hospital course • Scheduled events • Clinical condition • To dos, anticipatory guidance
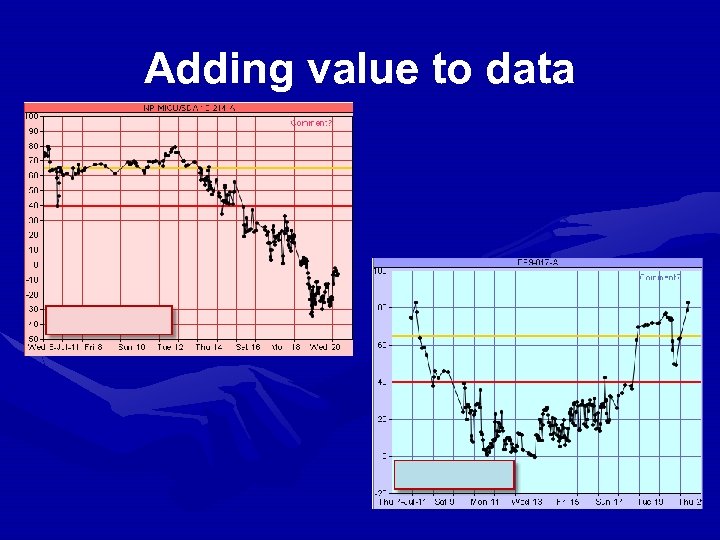 Adding value to data
Adding value to data
 Why written and oral sign-out?
Why written and oral sign-out?
 Why written and oral sign-out? Oral sign-out Written sign-out What’s new and old Most important info Highlights Complete info Details Interaction, read-back Critical thinking Memory aid Consistent info transfer
Why written and oral sign-out? Oral sign-out Written sign-out What’s new and old Most important info Highlights Complete info Details Interaction, read-back Critical thinking Memory aid Consistent info transfer
 How should we say it? • Consistently
How should we say it? • Consistently
 Standardization
Standardization
 Sign-out structure S ick? DNR? I D line (name, age, gender, dx) G eneral info re: hospital course N ew events of day, scheduled events O verall health status (clinical condition) U pcoming possibilities + plan & rationale T asks to complete + plan & rationale ? Any questions?
Sign-out structure S ick? DNR? I D line (name, age, gender, dx) G eneral info re: hospital course N ew events of day, scheduled events O verall health status (clinical condition) U pcoming possibilities + plan & rationale T asks to complete + plan & rationale ? Any questions?
 How should we say it? • Consistently • Concretely
How should we say it? • Consistently • Concretely
 Vague language • “If the nurse calls you with increased sugars, can you start insulin? ” • “Over the weekend he was unstable, but not any more. ” • “He’s DNR/DNI, but kind of do things if they’re reversible. ”
Vague language • “If the nurse calls you with increased sugars, can you start insulin? ” • “Over the weekend he was unstable, but not any more. ” • “He’s DNR/DNI, but kind of do things if they’re reversible. ”
 Concrete language “And then his blood pressure, if it’s greater than 165/105, you can push 40 of iv labetalol or 10 -20 of hydralazine iv. And then he has scheduled labetalol, and that should be given to him unless he’s really hypotensive, like less than 100/60 is what they’ve had. ”
Concrete language “And then his blood pressure, if it’s greater than 165/105, you can push 40 of iv labetalol or 10 -20 of hydralazine iv. And then he has scheduled labetalol, and that should be given to him unless he’s really hypotensive, like less than 100/60 is what they’ve had. ”
 How should we say it? • Consistently • Concretely • Closed loop
How should we say it? • Consistently • Concretely • Closed loop
 Open loop language - “If her Doppler’s positive maybe you could look at the cat scan. I mean it’s not going to be helpful because there’s no contrast. But, she’s going to get that done. Otherwise, it’s not something that you absolutely need to follow up with. ” - “OK. ”
Open loop language - “If her Doppler’s positive maybe you could look at the cat scan. I mean it’s not going to be helpful because there’s no contrast. But, she’s going to get that done. Otherwise, it’s not something that you absolutely need to follow up with. ” - “OK. ”
 Closing the loop Intern providing sign-out: “Neck CT is ordered, and I guess it got done today. I didn’t see anything in the computer, but the neck CT is to - in the setting of cervical lymphadenopathy and a breast mass, concern for malignancy…” Intern receiving sign-out: “OK. Is the neck CT something that needs follow-up? ” Intern providing sign-out: “No, I think it won’t change management tonight. ”
Closing the loop Intern providing sign-out: “Neck CT is ordered, and I guess it got done today. I didn’t see anything in the computer, but the neck CT is to - in the setting of cervical lymphadenopathy and a breast mass, concern for malignancy…” Intern receiving sign-out: “OK. Is the neck CT something that needs follow-up? ” Intern providing sign-out: “No, I think it won’t change management tonight. ”
 How should we say it? • • Consistently Concretely Closed loop Concisely
How should we say it? • • Consistently Concretely Closed loop Concisely
 Concise, but… • This is a 56 year old male who presents with chest pain. • What is this patient’s probability of cardiac disease?
Concise, but… • This is a 56 year old male who presents with chest pain. • What is this patient’s probability of cardiac disease?
 Just the facts, ma’am? • This is a 56 year old male smoker with diabetes, hypertension, hyperlipidemia, who presents with several days of chest pain/pressure after walking up 2 flights of stairs, relieved by rest.
Just the facts, ma’am? • This is a 56 year old male smoker with diabetes, hypertension, hyperlipidemia, who presents with several days of chest pain/pressure after walking up 2 flights of stairs, relieved by rest.
 Concise AND Clinical synthesis • This is a 56 year old male with multiple cardiac risk factors who presents with…
Concise AND Clinical synthesis • This is a 56 year old male with multiple cardiac risk factors who presents with…
 Concise AND Clinical synthesis • This is a 56 year old male with multiple cardiac risk factors who presents with several days of classic exertional angina.
Concise AND Clinical synthesis • This is a 56 year old male with multiple cardiac risk factors who presents with several days of classic exertional angina.
 How should we say it? • • • Consistently Concretely Closed loop Concisely, with clinical synthesis Question
How should we say it? • • • Consistently Concretely Closed loop Concisely, with clinical synthesis Question
 Is this a good handoff?
Is this a good handoff?
 Lack of interaction Intern providing sign-out: “This woman is a new person with COPD exacerbation. Severe COPD. Not really much going on. The resident ordered ambulatory O 2 sat, just to pass on to the tomorrow morning people, just so they know. ” Intern receiving sign-out: “OK. ”
Lack of interaction Intern providing sign-out: “This woman is a new person with COPD exacerbation. Severe COPD. Not really much going on. The resident ordered ambulatory O 2 sat, just to pass on to the tomorrow morning people, just so they know. ” Intern receiving sign-out: “OK. ”
 Practice time • Recall our patient: – 64 year old man – Admitted with new non-valvular atrial fibrillation – HTN, DM 2, GI bleed – EF 50%, mildly dilated left atrium – Unsuccessful cardioversion today • What will you say in oral sign-out? • What will you write?
Practice time • Recall our patient: – 64 year old man – Admitted with new non-valvular atrial fibrillation – HTN, DM 2, GI bleed – EF 50%, mildly dilated left atrium – Unsuccessful cardioversion today • What will you say in oral sign-out? • What will you write?

 Sign-out structure S ick? DNR? I D line (name, age, gender, dx) G eneral info re: hospital course N ew events of day, scheduled events O verall health status (clinical condition) U pcoming possibilities + plan & rationale T asks to complete + plan & rationale ? Any questions?
Sign-out structure S ick? DNR? I D line (name, age, gender, dx) G eneral info re: hospital course N ew events of day, scheduled events O verall health status (clinical condition) U pcoming possibilities + plan & rationale T asks to complete + plan & rationale ? Any questions?
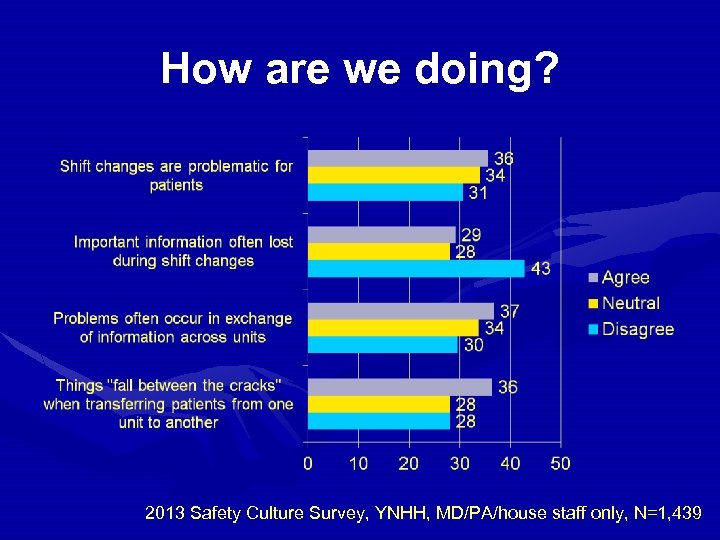 How are we doing? 2013 Safety Culture Survey, YNHH, MD/PA/house staff only, N=1, 439
How are we doing? 2013 Safety Culture Survey, YNHH, MD/PA/house staff only, N=1, 439
 Signs of a bad hand-off
Signs of a bad hand-off
 Uncertainty • “She’s being heparinized. I think she’s had a heart attack. ” • “And then the other thing is, what’s the other thing for him tonight? You know, he’s on antibiotics for a UTI. He’s on Zosyn. Or, zosyn or ceftaz? Or, one of those, for a UTI. ”
Uncertainty • “She’s being heparinized. I think she’s had a heart attack. ” • “And then the other thing is, what’s the other thing for him tonight? You know, he’s on antibiotics for a UTI. He’s on Zosyn. Or, zosyn or ceftaz? Or, one of those, for a UTI. ”
 Omissions First sign-out, 4 pm • Primary intern to on-call intern; 48 seconds • “[Ms. X]…went and had an EUS today and they found a pancreatic mass. And so they did brushings… They were not able to stent it with ERCP… Something happened during the procedure; they said submucosal contrast or something… They said if she has an increase in pain or spikes a fever, they said low threshold for CT of her belly and calling them. I started her on cipro iv. ”
Omissions First sign-out, 4 pm • Primary intern to on-call intern; 48 seconds • “[Ms. X]…went and had an EUS today and they found a pancreatic mass. And so they did brushings… They were not able to stent it with ERCP… Something happened during the procedure; they said submucosal contrast or something… They said if she has an increase in pain or spikes a fever, they said low threshold for CT of her belly and calling them. I started her on cipro iv. ”
 Second sign-out, 7 pm • On-call intern to night float intern • 12 seconds long – “Ms. X. She’s got obstructive jaundice. She was found to have a mass. They said it wasn’t able to be stented but I think they sent a biopsy. So there’s nothing to do tonight. ”
Second sign-out, 7 pm • On-call intern to night float intern • 12 seconds long – “Ms. X. She’s got obstructive jaundice. She was found to have a mass. They said it wasn’t able to be stented but I think they sent a biopsy. So there’s nothing to do tonight. ”
 Delay “It was a step-down patient. And there was a question about the patient’s low blood pressure, but the patient was not on the sign-out… So it took a phone call to figure out who the patient’s attending was, who the last note was from, and then figure out indeed it’s [my cross-cover] patient, and then go and see the patient. ” - Post-call interview
Delay “It was a step-down patient. And there was a question about the patient’s low blood pressure, but the patient was not on the sign-out… So it took a phone call to figure out who the patient’s attending was, who the last note was from, and then figure out indeed it’s [my cross-cover] patient, and then go and see the patient. ” - Post-call interview
 Adverse event “I had a patient who I had to send to the unit. She had some unanticipated bronchospasm, and apparently she had been a little bit bronchospastic during the day, and this wasn’t an issue that had really been discussed. ” - Post-call interview
Adverse event “I had a patient who I had to send to the unit. She had some unanticipated bronchospasm, and apparently she had been a little bit bronchospastic during the day, and this wasn’t an issue that had really been discussed. ” - Post-call interview
 What it takes for an error to reach a patient Reason, 1990
What it takes for an error to reach a patient Reason, 1990


