f88a2f296dab927b7729e729ae921d14.ppt
- Количество слайдов: 47

How to best minimize the effects of anesthesia in the elderly and very elderly patients Sheila Ryan Barnett, MD Associate Professor of Anesthesiology Harvard Medical School Beth Israel Deaconess Medical Center Boston, MA

> 65 y Population USA >85 y

35% of surgeries in USA on patients > 65 years 16, 000 year surgeries per 60% of patients of general surgeons > 65 y Growth in specialty surgery expected: 3547%

Annual anesthesia-related death rates per million population by sex US 1999 – 2005 Li et al Anesthesiology 2009; 110: 698 -9

To consider Aging & comorbidities Medications – modifications Medications – to avoid Risk reduction Inevitability

Aging and Risk Aging involves physiological changes AND The pathophysiology of superimposed disease
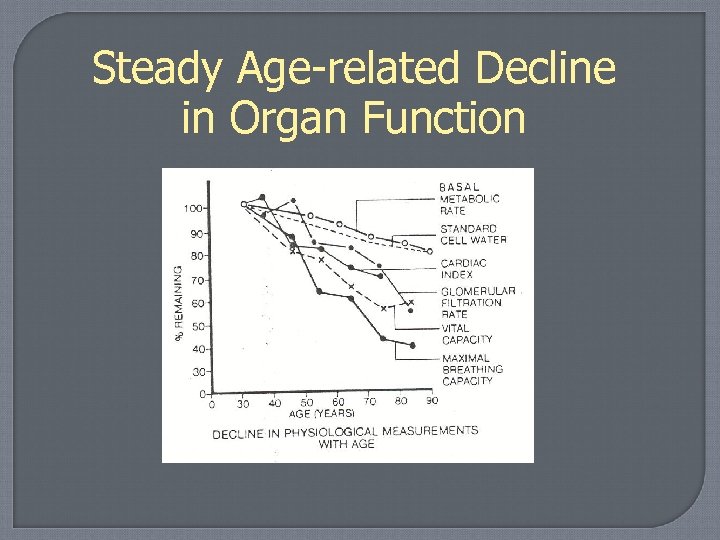
Steady Age-related Decline in Organ Function

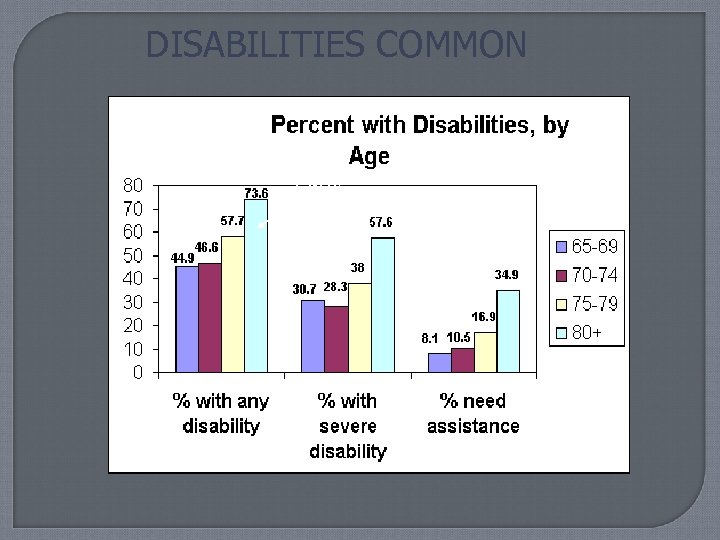
DISABILITIES COMMON > 80 y
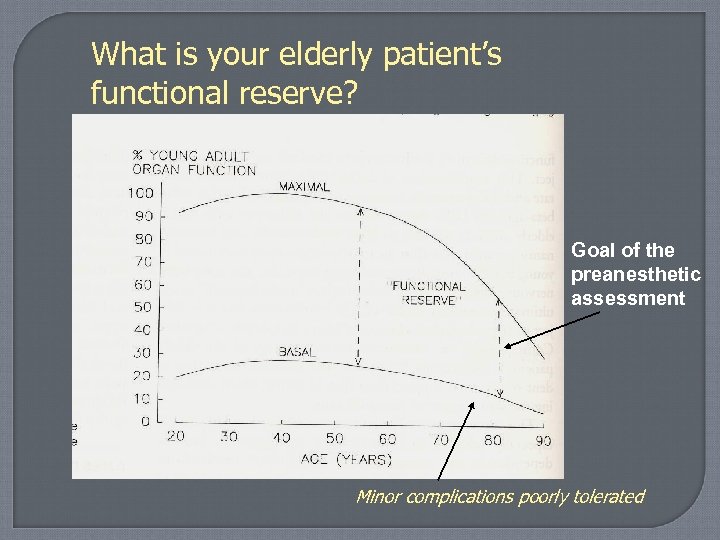
What is your elderly patient’s functional reserve? Goal of the preanesthetic assessment Minor complications poorly tolerated

Cardiovascular Vascular stiffening, HTN, loss elasticity Ventricular • Increased impedance - wall hypertrophy • decreased compliance, atrial dependence Conduction issues: • Decline in pacemaker cells, increase in atrial ectopy, & conduction defects Reduction in maximal HR – • reduced response to catecholamines Increased ischemic heart disease
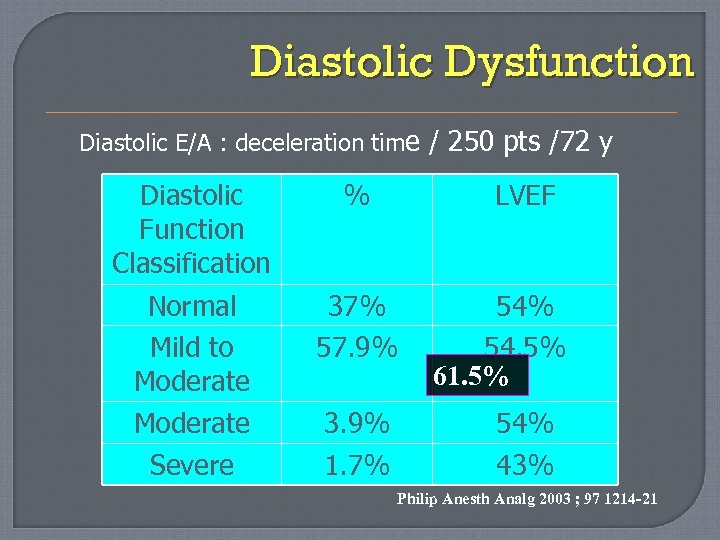
Diastolic Dysfunction Diastolic E/A : deceleration time / 250 pts /72 y Diastolic Function Classification % LVEF Normal Mild to Moderate 37% 57. 9% Moderate Severe 3. 9% 1. 7% 54. 5% 61. 5% 54% 43% Philip Anesth Analg 2003 ; 97 1214 -21

Pulmonary Function and Aging Thorax stiffens: • reduced chest wall compliance & decreased thoracic skeletal muscle mass = Increased work of maximal breathing Lung volumes change – reduced reserve volume Decrease in elastic lung recoil – closing volume increase More V/Q mismatch & greater P(A-a) O 2 gradient Reduction in hypoxic and hypercarbic drive Increased narcotic-induced apnea Decreased pharyngeal reflexes - ? More aspiration
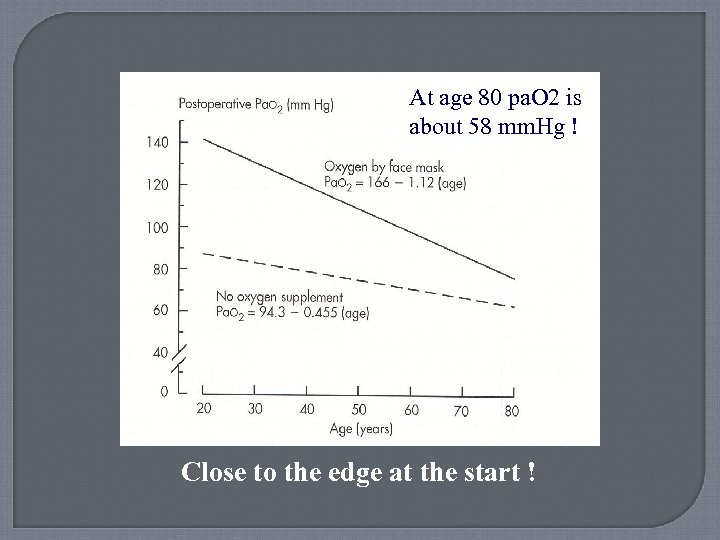
At age 80 pa. O 2 is about 58 mm. Hg ! Close to the edge at the start !

Intraoperative oxygen • • • Case controlled study of Spinal surgery patients Compared patients with & without Surgical Site Infection (SSI) Independent risk factors: – Long surgery OR 4. 7 p<0. 001 – ASA 3 + OR 9. 7 p< 0. 001 – Obesity 4. 0 p<0. 01 – Intraoperative oxygen <50% OR 12 p <0. 001 • Potential impact for elderly ? Maragakis Anesth 2009; 110: 556 -62

Central Nervous System Cortical grey matter attrition – • starts in middle age Cerebral atrophy – disease vs. aging Increased intracranial CSF CBF and auto regulation largely maintained Postoperative cognitive dysfunction

#1. Aging Recommendations 1. 2. 3. 4. Appreciate reduction in reserve function Understand age related organ changes and the impact of common disease Beware of ‘under-diagnosis’ e. g. DHF & fluids Provide supplemental extra oxygen, (increased risk hypoxemia)

Medications. . modification

Drugs – in general Dose reduction • Pharmacokinetic • Pharmacodynamic Interval extension

Specific Drug Considerations Anesthesiology 2009; 110: 1050 -1060
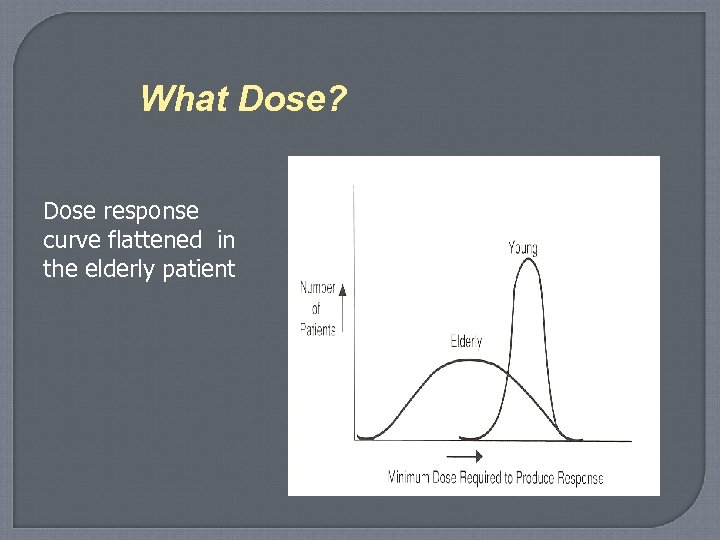
What Dose? Dose response curve flattened in the elderly patient
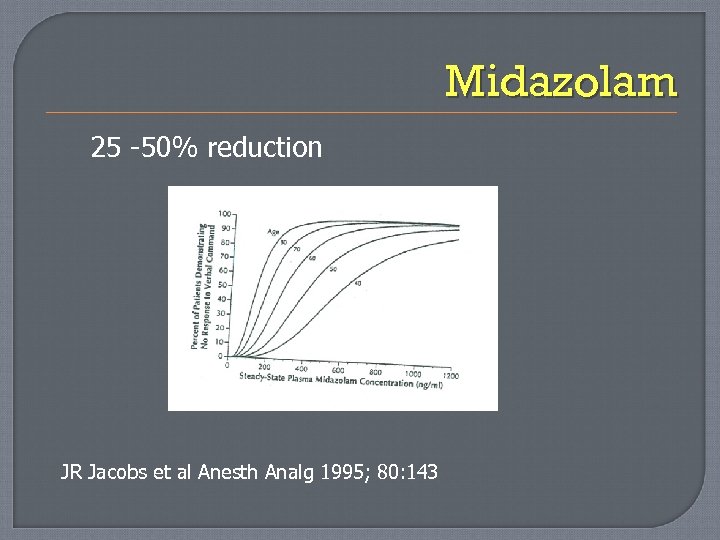
Midazolam 25 -50% reduction JR Jacobs et al Anesth Analg 1995; 80: 143
Opioids 50% reduction in initial doses for fentanyl Significant decrease in pharmacodynamic response All opioids increased risk apnea & hypercapnia

Propofol Increased & delayed hemodynamic impact leading to hypotension

Inhalational Agents Anesthesiology 2009; 110: 1050 -1060

# 2. Medication recommendations “Start low, go slow” Benzodiazepines • Low dosing with Midazolam to start Opioids • Beware respiratory depression • Titrate to effect Reduce inhalation agent Complete reversal of muscle relaxants

Drugs to avoid … & not always considered • Anticholinergic side effects – Central: Falls, delirium, cognitive dysfunction – Peripheral : Dry mouth, constipation, confusion • Anticholinergic Risk Scale – List of drugs with varying anticholinergic properties – Avoid or limit use if possible • Beers Criteria – Long acting Benzodiazepines – Multiple medications , many with anticholinergic properties

Anticholinergic Risk • High risk 3 points – Atropine products – Hydroxyzine (Atarax or Visteril) – Diphenyhydramine (Benadryl) – Promethazine (Phenergan) • Intermediate 2 points – Prochlorperazine (Compazine) • Low 1 point – Haloperidol – Metoclopramide ( Reglan) Rudolph Arch Int Med 2008; 168: 508 -13

Meperidine Active metabolites normeperidine • Renal excretion • T ½ 14 -21 hrs in elderly up to 30 hrs with CRI Causes myoclonus, twitching and seizures Associated with delirium in elderly Not recommended: use of meperidine in patients 75 yrs or older for analgesia is considered indicator of poor care by the Assessing Care of vulnerable elderly.

Polypharmacy • Survey of 3000 community dwelling 57 -85 y – 81% minimum of 1 prescription drug (PD) – 49% used dietary supplements – 29% used at least 5 PDs • • • Among PD users 46% also used over the counter drugs 4% at risk of major drug interaction, half with non prescription drugs Anti-coagulants most commonly involved Unknown true impact on the perianesthetic course Qato JAMA 2008; 300 (24) 2876

# 3. Avoidance Recommendations 1. Avoid meperidine, long acting muscle relaxants & benzo’s and anticholinergic 2. Look for Polypharmacy

Risk Reduction Timing of surgery Comprehensive preoperative assessments Beta Blockade … again

Can we go to the OR now? Meta-analysis of >250, 000 hip fx pts Mortality at 30 days and 1 year When delayed over 48 hours • 41% increase 30 d mortality • 32% all cause mortality How practical is this? Shiga et al Can J Anesth 2008; 55: 3; 146 -154

Comprehensive Geriatric Assessments (CGA) 120 patients CGA >60 y • ADLs, IADLs (Barhtel Index) , comorbidity, nutrition, MMSE All undergoing thoracic surgery 17% post op complications Predictors – • Low Barthel Index • Surgery >300 mins • Dementia – low MMSE Fukuse Chest 2005; 127: 886

Intervention Program to Reduce Delirium 400 patients > 70 y Admitted to Intervention Ward • Assessment, prevention treatment education Assessment day 1, 3, 7 Delirious patients in the Intervention ward • Shorter duration: by day 7 30% vs 60% (p 0. 001 ) • Shorter LOS: 9 vs 13 days (p 0. 001) • Reduced mortality: 2 vs. 9 patients died (p 0. 03) Lundstrom et al JAGS 2005: 53: 622

Beta Blockade & Risk Reduction Mangano NEJM 1996; 335: 1713 • • 100/200 patients received Atenolol preop and for 7 days Atenolol group improved survival 6 months & up to 2 y. Diabetes major risk But later data mixed results with increased stroke and mortality

What about orthopedic patients ? Beta blockade (BB) on low risk intermediate surgery • • Observational study 5158 THR/THR patients – 19% Beta blockers • BB for 7 days (740) • BB DOS & d/c’ed (252) 25% – No BB (4166) • Total 1. 5% (77) had POMI • BB continued -22 POMI; 7 deaths • BB discontinued -20 POMI; 19 deaths • No BB – 35 POMI; 28 deaths • • Event rate 3% BB vs. 7. 9% for d/c’ed BB In those discontinued beta blockers 2 fold increase in POMI and death ( OR 2. 0) Van Klei et al Anesthesiology 2009; 111: 117 -24
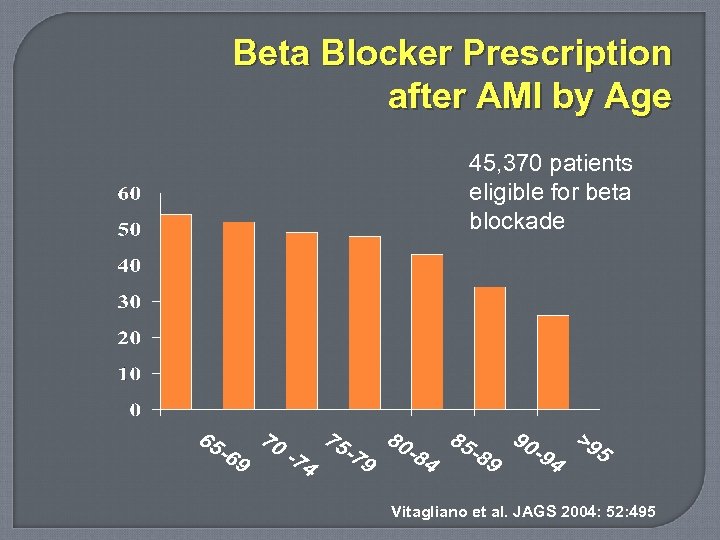
Beta Blocker Prescription after AMI by Age 45, 370 patients eligible for beta blockade Vitagliano et al. JAGS 2004: 52: 495

#4. Risk Reduction Recommendations 1. 2. 3. 4. Careful preoperative assessment is a priority Get to the OR in a timely manner Risk reduction medication – possible beta blockers Role of blood transfusions (not discussed)

Vulnerable times Unanticipated day of surgery deaths – > 800 000 patients NSQIP - Death rate 0. 08% – Older age 60 vs. 67 y and males P<0. 0001 • Complications increased death rate • PACU/ICU transfer most unstable • Opportunity to improve in 31% (chart review ) Improvement: hypovolemia, MI and transport period • Bishop Anesth Analg 2008 107: 1924 -35
80 years and up Veterans Hospital Data • 26 648 > 80 y • 568 263 < 80 y 30 day mortality 8% vs. 3%, p<0. 001 <2% if > 80 y undergoing simple procedures • TURP, IH, TKR, CEA 20% had complications in > 80 y Once a complication – 26% vs 4% mortality Hamel et al JAGS 2005; 53: 424

Intraoperative factors Cardiac events post non cardiac surgery 7700 patients, 83 (1%) Cardiac event 9 independent predictors In patients experiencing a cardiac event, intraoperative data more likely to show episode of hypotension +/- tachycardia Kheterpal et al Anesthesiology 2009; 110: 58 -66

# 5. Recommendation Avoid complications Hemodynamics

Geriatric M & M: Should we just accept this? Surgical mortality Surgical morbidity Turrentine et al J Am Coll Surg 2006; 203: 865

Is excess mortality truly preventable … 300 unselected hip fractures All received similar multimodal anesthesia & defined rehabilitation Outcomes: • 30 d mortality 13% • >30 d 7 more died Combined mortality 16% Foss & Kehlet Br J Anaesth 2005; 94: 24 -29

Analysis 47 deaths • 28% (13) unavoidable, terminal cancer or refused care • 15% (7) probably unavoidable • 34% (16) potentially avoidable ; active care curtailed • 23% (11) received maximal care ? Potentially avoidable

In summary … taking care of geriatric patients is inevitable Best outcomes if: Avoid complications Preoperative optimization OR without delay (when feasible) ? Beta blockers / transfusions Age appropriate drug dosing Postoperative: pain meds, oxygen
f88a2f296dab927b7729e729ae921d14.ppt