fe560ac27e319e14b5e0c88594c8b1f8.ppt
- Количество слайдов: 33
 Housing Authority Quality Improvement in the Non-Clinical Community Employment Medical Benefits October 15, 2015 Emergency Assistance Food Bank Case Managers Making A Difference 1
Housing Authority Quality Improvement in the Non-Clinical Community Employment Medical Benefits October 15, 2015 Emergency Assistance Food Bank Case Managers Making A Difference 1
 Webinar Participation • Actively participate and write your questions into the chat area during the presentation • Introduce yourself using the chat room function (name, role, location) • Please do not put us on hold • If instructed to do so, un-mute your line by pressing #6 2
Webinar Participation • Actively participate and write your questions into the chat area during the presentation • Introduce yourself using the chat room function (name, role, location) • Please do not put us on hold • If instructed to do so, un-mute your line by pressing #6 2
 AGENDA 1. Quality improvement is……. 2. Quality improvement is not…… 3. Why do Case Managers do quality improvement activities? 4. What roles do Case Managers play and how does quality improvement fit into our programs? 5. Deciding what to do! 6. Real World Experiences 7. Open discussion / questions 3
AGENDA 1. Quality improvement is……. 2. Quality improvement is not…… 3. Why do Case Managers do quality improvement activities? 4. What roles do Case Managers play and how does quality improvement fit into our programs? 5. Deciding what to do! 6. Real World Experiences 7. Open discussion / questions 3
 What is Quality Improvement? • More than simply comparing yourself against a national standard (Quality Assurance) • Process / systems oriented, not person oriented • Data driven, not measured by gut reactions! • Based on activities designed to make specific improvements • Involves recurring measuring and assessing and adjusting…. . in other words, it’s CONTINUOUS! 4
What is Quality Improvement? • More than simply comparing yourself against a national standard (Quality Assurance) • Process / systems oriented, not person oriented • Data driven, not measured by gut reactions! • Based on activities designed to make specific improvements • Involves recurring measuring and assessing and adjusting…. . in other words, it’s CONTINUOUS! 4
 Quality Improvement is NOT: • Judgmental – No program is perfect, no program performs at 100% for every activity • Critical – No one is belittled chastised because they perform poorly at any given activity • Punitive – Programs and staff are not punished if they make attempts to improve and fail! Note: The only time you would experience negative feedback or actions from federal authorities is if you do nothing!! We expect that there will be challenges, barriers and slip backs, but we MUST show that we are trying something! 5
Quality Improvement is NOT: • Judgmental – No program is perfect, no program performs at 100% for every activity • Critical – No one is belittled chastised because they perform poorly at any given activity • Punitive – Programs and staff are not punished if they make attempts to improve and fail! Note: The only time you would experience negative feedback or actions from federal authorities is if you do nothing!! We expect that there will be challenges, barriers and slip backs, but we MUST show that we are trying something! 5
 Why Do We Do It? 1. Federal legislative mandates • Ryan White Care Act • National HIV/AIDS Strategy • July 2013 White House Executive Care Continuum Order 2. Creating your RW grant application to HRSA 3. Every support service that is improved, just nudges that patient a few steps closer to medical engagement 4. It improves the lives of the people we serve. 5. It’s just the right thing to do! 6
Why Do We Do It? 1. Federal legislative mandates • Ryan White Care Act • National HIV/AIDS Strategy • July 2013 White House Executive Care Continuum Order 2. Creating your RW grant application to HRSA 3. Every support service that is improved, just nudges that patient a few steps closer to medical engagement 4. It improves the lives of the people we serve. 5. It’s just the right thing to do! 6
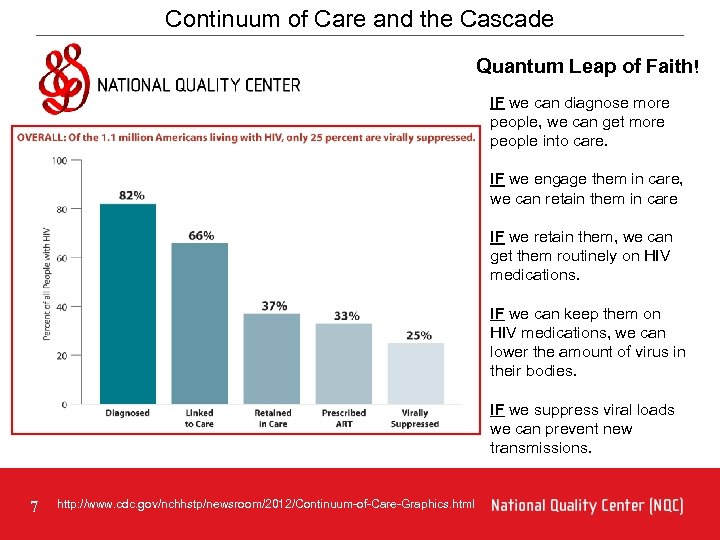 Continuum of Care and the Cascade Quantum Leap of Faith! IF we can diagnose more people, we can get more people into care. IF we engage them in care, we can retain them in care IF we retain them, we can get them routinely on HIV medications. IF we can keep them on HIV medications, we can lower the amount of virus in their bodies. IF we suppress viral loads we can prevent new transmissions. 7 http: //www. cdc. gov/nchhstp/newsroom/2012/Continuum-of-Care-Graphics. html
Continuum of Care and the Cascade Quantum Leap of Faith! IF we can diagnose more people, we can get more people into care. IF we engage them in care, we can retain them in care IF we retain them, we can get them routinely on HIV medications. IF we can keep them on HIV medications, we can lower the amount of virus in their bodies. IF we suppress viral loads we can prevent new transmissions. 7 http: //www. cdc. gov/nchhstp/newsroom/2012/Continuum-of-Care-Graphics. html
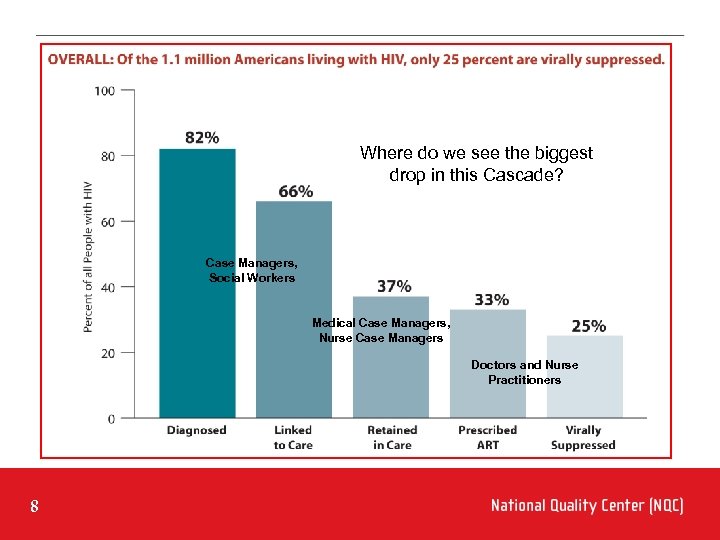 Where do we see the biggest drop in this Cascade? Case Managers, Social Workers Medical Case Managers, Nurse Case Managers Doctors and Nurse Practitioners 8
Where do we see the biggest drop in this Cascade? Case Managers, Social Workers Medical Case Managers, Nurse Case Managers Doctors and Nurse Practitioners 8
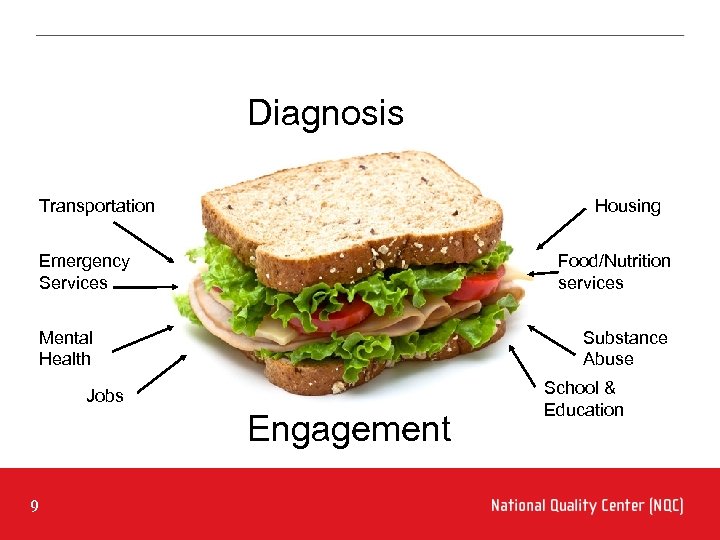 Diagnosis Transportation Housing Emergency Services Food/Nutrition services Mental Health Substance Abuse Jobs Engagement 9 School & Education
Diagnosis Transportation Housing Emergency Services Food/Nutrition services Mental Health Substance Abuse Jobs Engagement 9 School & Education
 How Does CQI Fit Into My Position? Empower Every improvement you make in your service, contributes to the patient’s ability to become actively engaged in their medical care. Support Prepare Enable Assess Readiness 10 Let’s think about how we can help move patients from the left side of the continuum to the right side!
How Does CQI Fit Into My Position? Empower Every improvement you make in your service, contributes to the patient’s ability to become actively engaged in their medical care. Support Prepare Enable Assess Readiness 10 Let’s think about how we can help move patients from the left side of the continuum to the right side!
 How Do I Know What To Work On? Listen to Patients and Staff Consumer Case Manager/Agency • I had to wait over an hour for my or ride home!! • I hate green beans and they keep or putting them in my meals! • They just don’t want to eat what’s good for them! • I can’t keep the MH appointments, I have no child care and no transportation. 11 • Patients call for a ride the day before their appointment! • I am constantly trying to get several of the patients in here…. . they just don’t come!. or
How Do I Know What To Work On? Listen to Patients and Staff Consumer Case Manager/Agency • I had to wait over an hour for my or ride home!! • I hate green beans and they keep or putting them in my meals! • They just don’t want to eat what’s good for them! • I can’t keep the MH appointments, I have no child care and no transportation. 11 • Patients call for a ride the day before their appointment! • I am constantly trying to get several of the patients in here…. . they just don’t come!. or
 How Do I Get That Information? Surveys: • Satisfaction or Needs Assessment • Electronic, Paper, Patient Completed, Peer or Staff Facilitated • Suggestion Boxes • Focus Groups Patient Satisfaction • With the services • • • With the facility With the staff With their outcomes Data: • Chart reviews • EMR/Database queries • Trend charts • Project-specific data collection Needs Assessment • • Ancillary services Access Health literacy / numeracy Other support services OR……Walk thru the service agency in your patient’s shoes. (Fake appointment/visit/phone call)…. How long did you wait, how were you treated, did you get what you came for? 12
How Do I Get That Information? Surveys: • Satisfaction or Needs Assessment • Electronic, Paper, Patient Completed, Peer or Staff Facilitated • Suggestion Boxes • Focus Groups Patient Satisfaction • With the services • • • With the facility With the staff With their outcomes Data: • Chart reviews • EMR/Database queries • Trend charts • Project-specific data collection Needs Assessment • • Ancillary services Access Health literacy / numeracy Other support services OR……Walk thru the service agency in your patient’s shoes. (Fake appointment/visit/phone call)…. How long did you wait, how were you treated, did you get what you came for? 12
 How Do I Decide Which Issue To Choose? • How many patients will be impacted? • What will the impact for the patient be? • Will it cost my agency any money? • How much staff and time will it take? • Will I get buy-in from other staff? • Is it something I am able to measure? • What are the chances of success? 13
How Do I Decide Which Issue To Choose? • How many patients will be impacted? • What will the impact for the patient be? • Will it cost my agency any money? • How much staff and time will it take? • Will I get buy-in from other staff? • Is it something I am able to measure? • What are the chances of success? 13
 ACT: Act on what you learned. Do you need to tweak your plan or test it in on a larger scale? STUDY: Document what happened and decide if your plan produced the results you hoped for. 14 PLAN: Brainstorm for a strategy and then make the plan. Decide who will do what, when, where, and how. DO: Carry out your plan in a sample population or in a specific designated time slot. Just test it on a small scale! What Does The Improvement Process Look Like? First ID a problem, then just PDSA it!
ACT: Act on what you learned. Do you need to tweak your plan or test it in on a larger scale? STUDY: Document what happened and decide if your plan produced the results you hoped for. 14 PLAN: Brainstorm for a strategy and then make the plan. Decide who will do what, when, where, and how. DO: Carry out your plan in a sample population or in a specific designated time slot. Just test it on a small scale! What Does The Improvement Process Look Like? First ID a problem, then just PDSA it!
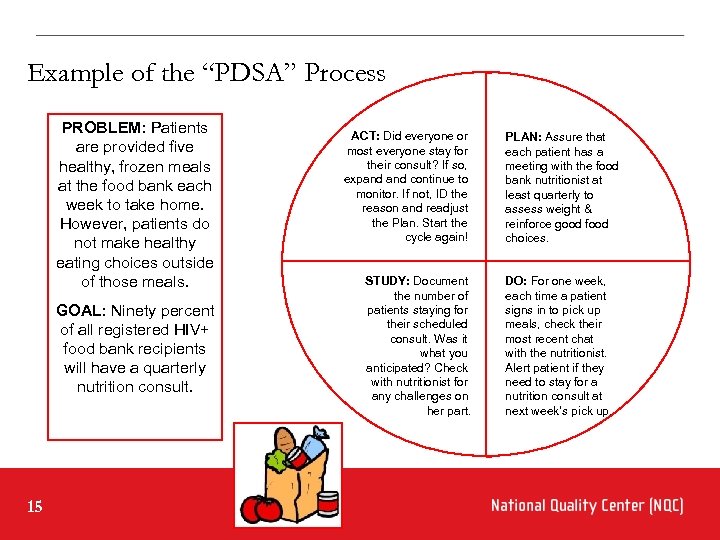 Example of the “PDSA” Process PROBLEM: Patients are provided five healthy, frozen meals at the food bank each week to take home. However, patients do not make healthy eating choices outside of those meals. GOAL: Ninety percent of all registered HIV+ food bank recipients will have a quarterly nutrition consult. 15 ACT: Did everyone or most everyone stay for their consult? If so, expand continue to monitor. If not, ID the reason and readjust the Plan. Start the cycle again! STUDY: Document the number of patients staying for their scheduled consult. Was it what you anticipated? Check with nutritionist for any challenges on her part. PLAN: Assure that each patient has a meeting with the food bank nutritionist at least quarterly to assess weight & reinforce good food choices. DO: For one week, each time a patient signs in to pick up meals, check their most recent chat with the nutritionist. Alert patient if they need to stay for a nutrition consult at next week’s pick up.
Example of the “PDSA” Process PROBLEM: Patients are provided five healthy, frozen meals at the food bank each week to take home. However, patients do not make healthy eating choices outside of those meals. GOAL: Ninety percent of all registered HIV+ food bank recipients will have a quarterly nutrition consult. 15 ACT: Did everyone or most everyone stay for their consult? If so, expand continue to monitor. If not, ID the reason and readjust the Plan. Start the cycle again! STUDY: Document the number of patients staying for their scheduled consult. Was it what you anticipated? Check with nutritionist for any challenges on her part. PLAN: Assure that each patient has a meeting with the food bank nutritionist at least quarterly to assess weight & reinforce good food choices. DO: For one week, each time a patient signs in to pick up meals, check their most recent chat with the nutritionist. Alert patient if they need to stay for a nutrition consult at next week’s pick up.
 Did I Make A Difference? • What was the OUTPUT? This measures what your activity produced: How many patients had a quarterly visit with the food bank nutritionist? • What was the OUTCOME? This is result of your outputs: What percentage of patients now enjoy an appropriate body weight? • What was the IMPACT? This is a long term change and will be harder to measure and assess: Are patients reporting that they feel better or healthier? Are they better prepared to maintain their HIV treatment protocols or participate in school or hold a job? Have better eating habits impacted other aspects of their lives? 16
Did I Make A Difference? • What was the OUTPUT? This measures what your activity produced: How many patients had a quarterly visit with the food bank nutritionist? • What was the OUTCOME? This is result of your outputs: What percentage of patients now enjoy an appropriate body weight? • What was the IMPACT? This is a long term change and will be harder to measure and assess: Are patients reporting that they feel better or healthier? Are they better prepared to maintain their HIV treatment protocols or participate in school or hold a job? Have better eating habits impacted other aspects of their lives? 16
 When Does It End? Hint: CQI is a “continuous” process and does not have an “end”! • I have reached my goal, what next? § Decide if there is still room for more improvement and goal should be reset higher. § Decide if another project might now have higher priority § Maintain measurements…. possibly less frequently, to make sure you don’t slide backwards and your gains are maintained! § Every attained goal deserves a celebration! 17
When Does It End? Hint: CQI is a “continuous” process and does not have an “end”! • I have reached my goal, what next? § Decide if there is still room for more improvement and goal should be reset higher. § Decide if another project might now have higher priority § Maintain measurements…. possibly less frequently, to make sure you don’t slide backwards and your gains are maintained! § Every attained goal deserves a celebration! 17
 Real World Experiences! Let’s listen to the experiences of our fellow grantees! 18
Real World Experiences! Let’s listen to the experiences of our fellow grantees! 18
 Vulnerability Index for Housing A QI collaborative among Ryan White and Supportive Housing Services 19
Vulnerability Index for Housing A QI collaborative among Ryan White and Supportive Housing Services 19
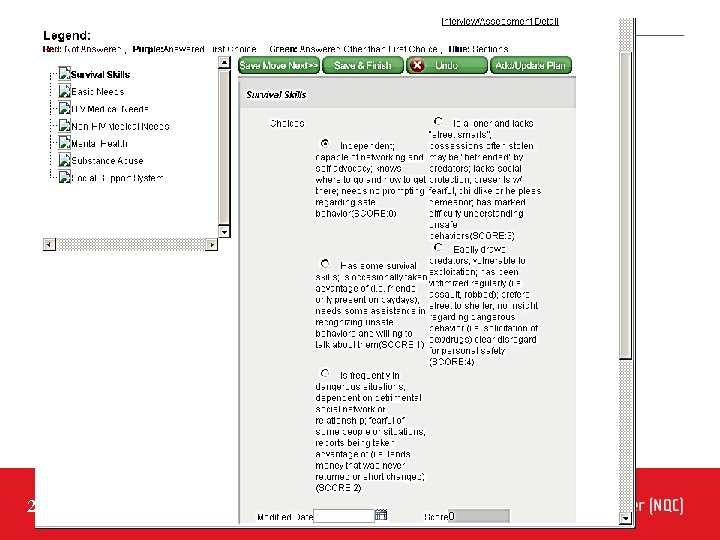
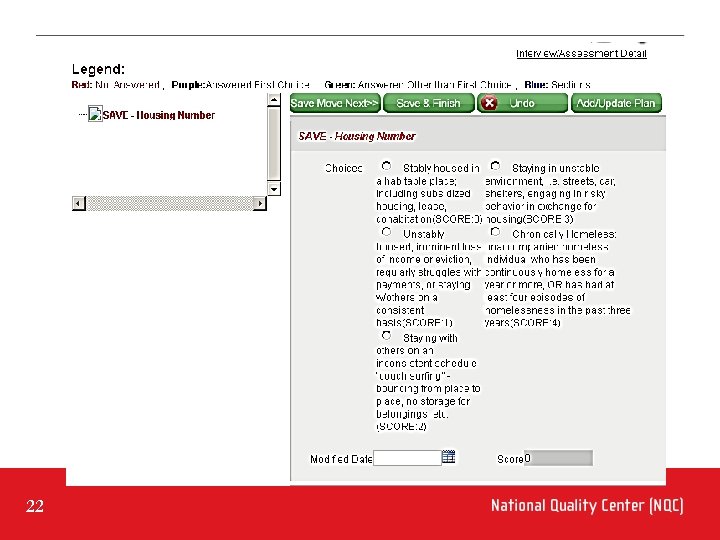
 How it all began… Problem: • Tension over how housing voucher openings were filled • Some clients had a higher need; waited longer • Sense of the current system being “not fair” Plan: • Devise a new selection process for voucher openings • Assemble a team (Housing agency representatives; Quality Manager; Medical Case Managers) • Examine current approach Our Plan Stage led to… • Examining a number of assessment tools • Using these resources as models • Developing our own assessment and naming it Vulnerability Index 20
How it all began… Problem: • Tension over how housing voucher openings were filled • Some clients had a higher need; waited longer • Sense of the current system being “not fair” Plan: • Devise a new selection process for voucher openings • Assemble a team (Housing agency representatives; Quality Manager; Medical Case Managers) • Examine current approach Our Plan Stage led to… • Examining a number of assessment tools • Using these resources as models • Developing our own assessment and naming it Vulnerability Index 20
 21
21
 22
22
 Testing the Theory The “Do” stage: • Develop the assessment electronically in the database • Provide introduction and training • Launch pilot program Checking the Results • Expanded use of index to a second agency • Extending the length of the pilot program due to a low number of housing openings 23
Testing the Theory The “Do” stage: • Develop the assessment electronically in the database • Provide introduction and training • Launch pilot program Checking the Results • Expanded use of index to a second agency • Extending the length of the pilot program due to a low number of housing openings 23
 Potential Future Uses Measuring Performance • Getting feedback from those who use the index • Analyzing the efficiency of the process 24
Potential Future Uses Measuring Performance • Getting feedback from those who use the index • Analyzing the efficiency of the process 24
 Multnomah County Health Department Portland OR TGA HIV Care Services Program Margy Robinson, HIV Care Services Manager Marisa Mc. Laughlin, Quality Improvement Specialist
Multnomah County Health Department Portland OR TGA HIV Care Services Program Margy Robinson, HIV Care Services Manager Marisa Mc. Laughlin, Quality Improvement Specialist
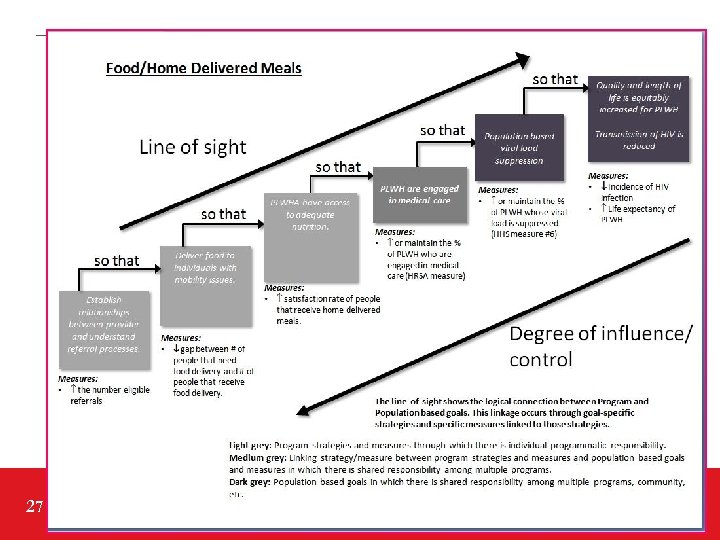
 Line of Sight • A QI Plan where providers use, “So that”…. to understand the continuum from social service support to medical care. Three providers/agencies focus on different social service/support needs: housing, food, community building. • Grantee provides the QI training, providers choose and implement two projects relevant to the population they serve. Grantee monitors progress and assists with challenges. 26
Line of Sight • A QI Plan where providers use, “So that”…. to understand the continuum from social service support to medical care. Three providers/agencies focus on different social service/support needs: housing, food, community building. • Grantee provides the QI training, providers choose and implement two projects relevant to the population they serve. Grantee monitors progress and assists with challenges. 26
 27
27
 Food • Goal – Home delivery of meals to patients unable to leave home. • Feed the people who are injured or too sick to otherwise secure food. • Use food delivery as a way to check on patients and report back any obvious issues. • Track the patients receiving food and see if they have had a recent medical visit. 28
Food • Goal – Home delivery of meals to patients unable to leave home. • Feed the people who are injured or too sick to otherwise secure food. • Use food delivery as a way to check on patients and report back any obvious issues. • Track the patients receiving food and see if they have had a recent medical visit. 28
 Housing • Goal – Move more people from transitional RW supported housing, to patient-supported stable housing. • Component 1 – Develop an “income sustainability plan” that evaluates patient income, employment potential. • Component 2 – Develop and Acuity Scale that would standard the priority process across all case managers. Who needs what the most? 29
Housing • Goal – Move more people from transitional RW supported housing, to patient-supported stable housing. • Component 1 – Develop an “income sustainability plan” that evaluates patient income, employment potential. • Component 2 – Develop and Acuity Scale that would standard the priority process across all case managers. Who needs what the most? 29
 Building Community • Goal – Engage more patients in group activities to promote peer support. • Bring patients into group activities by offering topics of interest (holistic health, Raki, crafting). • Build a safe place for patients to interact, and develop trust. • Hypothesis: Confident, empowered patients will engage more fully in medical care. 30
Building Community • Goal – Engage more patients in group activities to promote peer support. • Bring patients into group activities by offering topics of interest (holistic health, Raki, crafting). • Build a safe place for patients to interact, and develop trust. • Hypothesis: Confident, empowered patients will engage more fully in medical care. 30
 Lesson of the Day: The ultimate outcome, Viral Load Suppression, is a TEAM effort. Case Managers are the initial impetus and provide the potential for the healthiest of outcomes. Any improvement made by a Case Manager is an improvement in a patient’s life. 31
Lesson of the Day: The ultimate outcome, Viral Load Suppression, is a TEAM effort. Case Managers are the initial impetus and provide the potential for the healthiest of outcomes. Any improvement made by a Case Manager is an improvement in a patient’s life. 31
 Questions later? Jane Caruso, NQC Consultant janecaruso@comcast. net Kevin Garrett, NQC Senior Manager kevin. garrett@health. ny. gov 32
Questions later? Jane Caruso, NQC Consultant janecaruso@comcast. net Kevin Garrett, NQC Senior Manager kevin. garrett@health. ny. gov 32
 Recording Link To hear the recording of this webinar, please go to: https: //meetny. webex. com/meetny/lsr. php? RCID=7 0269 e 1 c 25 e 143 ae 903 f 969 bbcd 48 ba 2 33
Recording Link To hear the recording of this webinar, please go to: https: //meetny. webex. com/meetny/lsr. php? RCID=7 0269 e 1 c 25 e 143 ae 903 f 969 bbcd 48 ba 2 33


