224f8b85fcc736e680007676b2022773.ppt
- Количество слайдов: 95
 HIV / AIDS 2005 Mother To Child Transmission - Sky R. Blue, MD
HIV / AIDS 2005 Mother To Child Transmission - Sky R. Blue, MD
 -
-
 HIV - The Numbers u Number of people living with HIV/AIDS n Total 40 million (34 - 46 million) u u u People newly infected with HIV in 2003 n Total 5 million (4. 2 - 5. 8 million) u u u Adults 37 million (31 - 43 million) Children under 15 years 2. 5 million (2. 1 - 2. 9 million) Adults 4. 2 million (3. 6 - 4. 8 million) Children under 15 years 700 000 (590 000 - 810 000) AIDS deaths in 2003 n Total 3 million (2. 5 - 3. 5 million) u u Adults 2. 5 million (2. 1 - 2. 9 million) Children under 15 years 500 000 (420 000 - 580 000 -
HIV - The Numbers u Number of people living with HIV/AIDS n Total 40 million (34 - 46 million) u u u People newly infected with HIV in 2003 n Total 5 million (4. 2 - 5. 8 million) u u u Adults 37 million (31 - 43 million) Children under 15 years 2. 5 million (2. 1 - 2. 9 million) Adults 4. 2 million (3. 6 - 4. 8 million) Children under 15 years 700 000 (590 000 - 810 000) AIDS deaths in 2003 n Total 3 million (2. 5 - 3. 5 million) u u Adults 2. 5 million (2. 1 - 2. 9 million) Children under 15 years 500 000 (420 000 - 580 000 -
 Adults and Children Living with HIV/AIDS 2003 N. America 950, 000 44, 000 Caribbean 420, 000 53, 000 Latin America 1. 5 million 240, 000 Western Europe 550, 000 21, 000 - Eastern Europe 1 million 210, 000 North Africa 500, 000 Asia & Pacific 6. 6 million 92, 000 1, 800, 000 Sub-Saharan Africa 28. 5 million 3, 100, 000 Total: 40 million Data from UNAIDS New Cases Australia & New Zealand 15, 000
Adults and Children Living with HIV/AIDS 2003 N. America 950, 000 44, 000 Caribbean 420, 000 53, 000 Latin America 1. 5 million 240, 000 Western Europe 550, 000 21, 000 - Eastern Europe 1 million 210, 000 North Africa 500, 000 Asia & Pacific 6. 6 million 92, 000 1, 800, 000 Sub-Saharan Africa 28. 5 million 3, 100, 000 Total: 40 million Data from UNAIDS New Cases Australia & New Zealand 15, 000
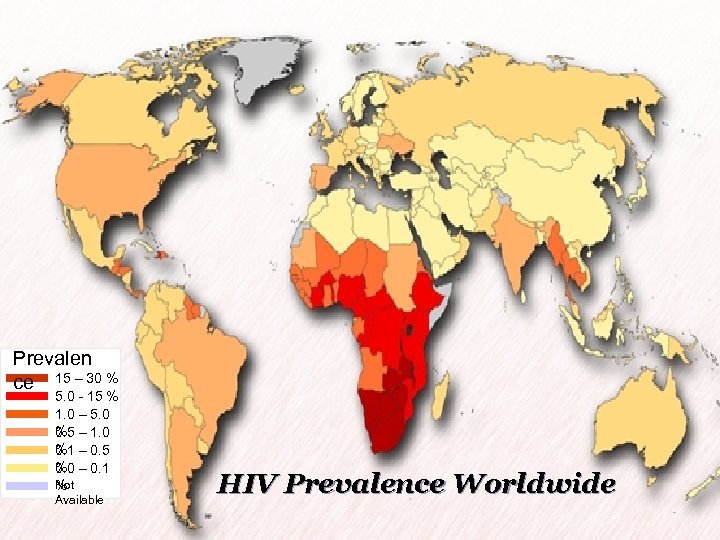 - Prevalen ce 15 – 30 % 5. 0 - 15 % 1. 0 – 5. 0 % 0. 5 – 1. 0 % 0. 1 – 0. 5 % 0. 0 – 0. 1 Not % Available HIV Prevalence Worldwide
- Prevalen ce 15 – 30 % 5. 0 - 15 % 1. 0 – 5. 0 % 0. 5 – 1. 0 % 0. 1 – 0. 5 % 0. 0 – 0. 1 Not % Available HIV Prevalence Worldwide
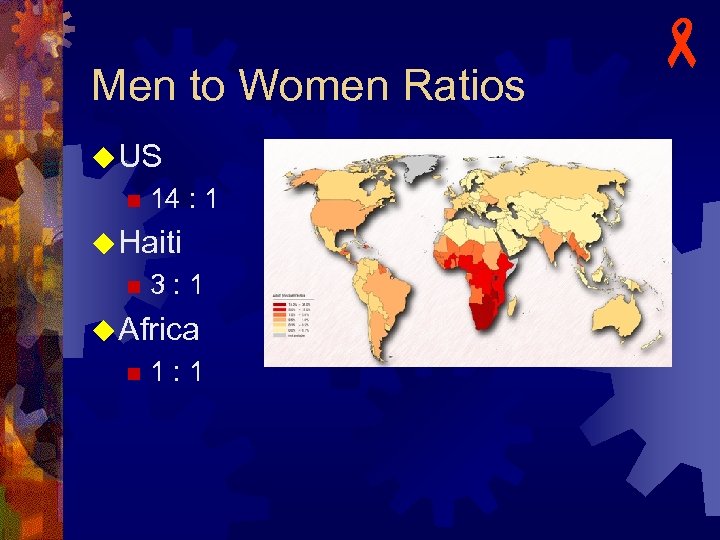 Men to Women Ratios u US n 14 : 1 u Haiti n 3 : 1 u Africa n 1 : 1 -
Men to Women Ratios u US n 14 : 1 u Haiti n 3 : 1 u Africa n 1 : 1 -
 -
-
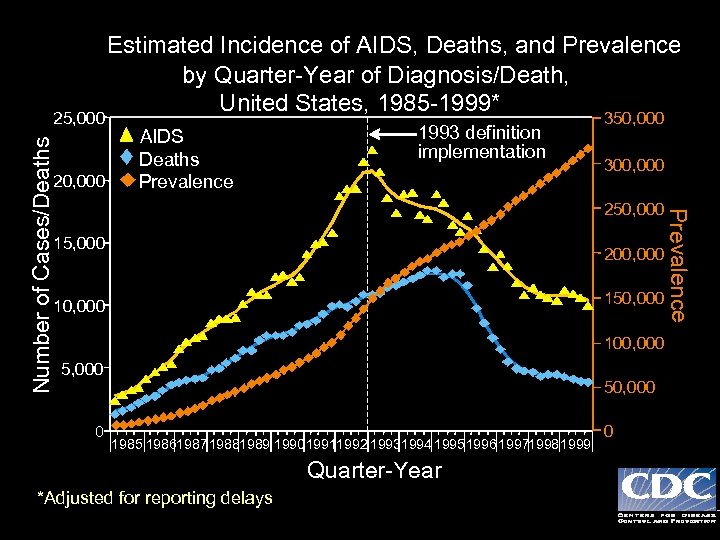 - Estimated Incidence of AIDS, Deaths, and Prevalence by Quarter-Year of Diagnosis/Death, United States, 1985 -1999* 20, 000 AIDS Deaths Prevalence 1993 definition implementation 350, 000 300, 000 250, 000 15, 000 200, 000 150, 000 100, 000 5, 000 0 50, 000 1985 1986198719881989 199019911992 19931994 19951996 199719981999 Quarter-Year *Adjusted for reporting delays 0 Prevalence Number of Cases/Deaths 25, 000
- Estimated Incidence of AIDS, Deaths, and Prevalence by Quarter-Year of Diagnosis/Death, United States, 1985 -1999* 20, 000 AIDS Deaths Prevalence 1993 definition implementation 350, 000 300, 000 250, 000 15, 000 200, 000 150, 000 100, 000 5, 000 0 50, 000 1985 1986198719881989 199019911992 19931994 19951996 199719981999 Quarter-Year *Adjusted for reporting delays 0 Prevalence Number of Cases/Deaths 25, 000
 -
-
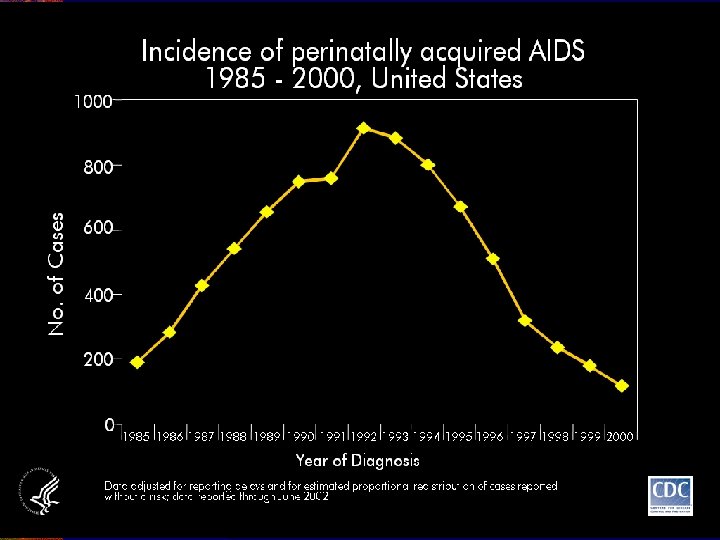 -
-
 - Epidemiology u Distribution of AIDS/HIV status 1 1000 K 950 K 800 K 280 K Undiagnosed 600 K 200 K HIV+ but not in care 400 K 130 K HIV+ 200 K 340 K AIDS
- Epidemiology u Distribution of AIDS/HIV status 1 1000 K 950 K 800 K 280 K Undiagnosed 600 K 200 K HIV+ but not in care 400 K 130 K HIV+ 200 K 340 K AIDS
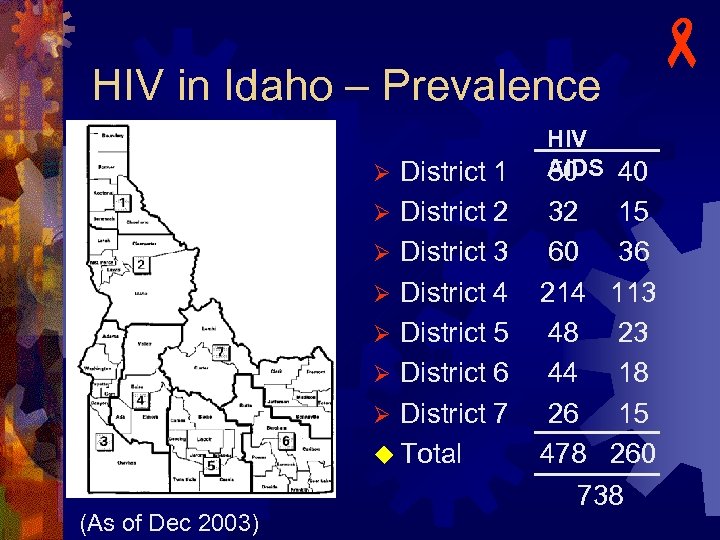 HIV in Idaho – Prevalence - HIV AIDS Ø District 1 50 40 District 2 32 15 Ø District 3 60 36 Ø District 4 214 113 Ø District 5 48 23 Ø District 6 44 18 Ø District 7 26 15 u Total 478 260 738 Ø (As of Dec 2003)
HIV in Idaho – Prevalence - HIV AIDS Ø District 1 50 40 District 2 32 15 Ø District 3 60 36 Ø District 4 214 113 Ø District 5 48 23 Ø District 6 44 18 Ø District 7 26 15 u Total 478 260 738 Ø (As of Dec 2003)
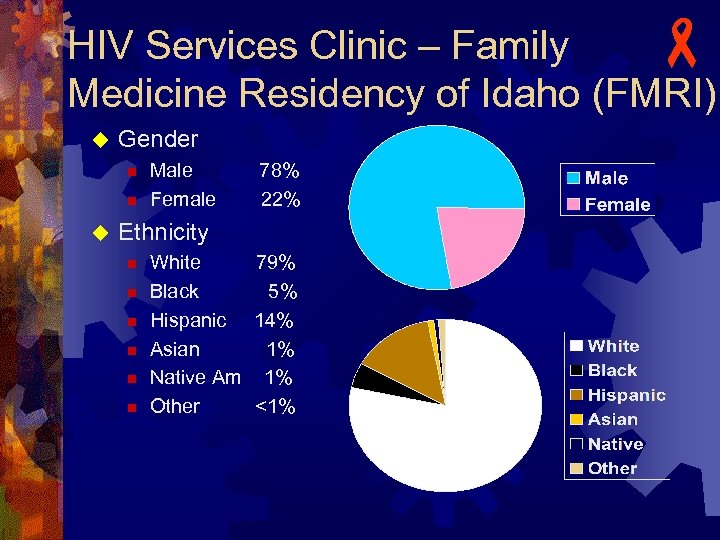 HIV Services Clinic – Family Medicine Residency of Idaho (FMRI) u Gender n n u Male 78% Female 22% Ethnicity n n n White 79% Black 5% Hispanic 14% Asian 1% Native Am 1% Other <1%
HIV Services Clinic – Family Medicine Residency of Idaho (FMRI) u Gender n n u Male 78% Female 22% Ethnicity n n n White 79% Black 5% Hispanic 14% Asian 1% Native Am 1% Other <1%
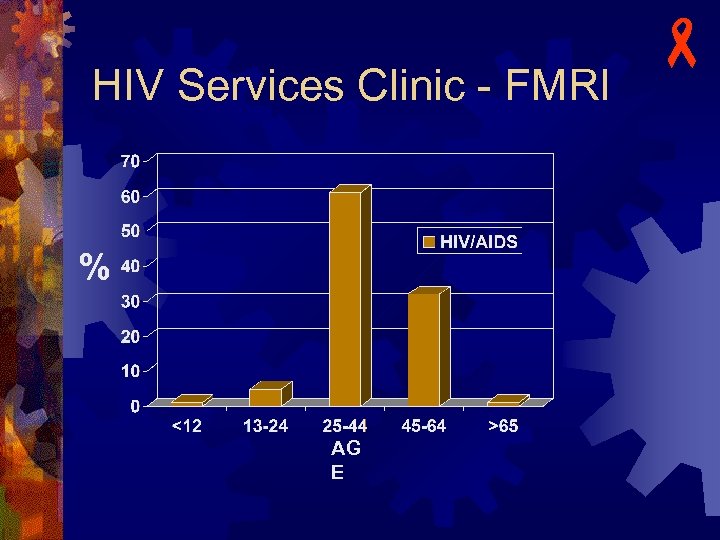 HIV Services Clinic - FMRI % AG E -
HIV Services Clinic - FMRI % AG E -
 HIV and Pregnancy - u AIDS in women has risen from 7% of adult cases early in the epidemic to 27% today u 7, 000 -10, 000 babies are born each year to HIV infected mothers u 2, 000 -3, 000 would be born with HIV u Universal screening and perinatal treatment could reduce this to <500
HIV and Pregnancy - u AIDS in women has risen from 7% of adult cases early in the epidemic to 27% today u 7, 000 -10, 000 babies are born each year to HIV infected mothers u 2, 000 -3, 000 would be born with HIV u Universal screening and perinatal treatment could reduce this to <500
 HIV Testing in Pregnancy - u National Recommendations u Universal voluntary testing with patient notification as a routine component of prenatal care n n American Academy of Pediatrics and American College of Obstetricians and Gynecologists. Human Immunodeficiency Virus screening: joint statement of the AAP and ACOG. Pediatrics 1999; 104: 128. Institute of Medicine. Reducing the odds: preventing perinatal transmission of HIV in the United States. Washington, DC: National Academy Press, 1999
HIV Testing in Pregnancy - u National Recommendations u Universal voluntary testing with patient notification as a routine component of prenatal care n n American Academy of Pediatrics and American College of Obstetricians and Gynecologists. Human Immunodeficiency Virus screening: joint statement of the AAP and ACOG. Pediatrics 1999; 104: 128. Institute of Medicine. Reducing the odds: preventing perinatal transmission of HIV in the United States. Washington, DC: National Academy Press, 1999
 HIV Testing in Pregnancy - u CDC (USPHS) recommendations for HIV screening of pregnant women n n Prenatal: routine HIV screening for all pregnant women using the “opt out” approach — women will be notified that they will be tested unless they decline Labor and delivery: routine rapid testing for women whose HIV status is unknown Postnatal: rapid testing for all infants whose mother’s status is unknown. MMWR November 15, 2002 u Regulations, laws, & policies about HIV screening of pregnant women vary state to state
HIV Testing in Pregnancy - u CDC (USPHS) recommendations for HIV screening of pregnant women n n Prenatal: routine HIV screening for all pregnant women using the “opt out” approach — women will be notified that they will be tested unless they decline Labor and delivery: routine rapid testing for women whose HIV status is unknown Postnatal: rapid testing for all infants whose mother’s status is unknown. MMWR November 15, 2002 u Regulations, laws, & policies about HIV screening of pregnant women vary state to state
 Untreated Populations - u 15% of women with HIV infection have no prenatal care compared to 2% of all pregnant women (MMWR, 1998) u Risk of HIV infection at least 2 - to 4 -fold higher among women presenting for delivery without prenatal care E Aaron, CRNP. Presented at Clinical Pathway, August 2002.
Untreated Populations - u 15% of women with HIV infection have no prenatal care compared to 2% of all pregnant women (MMWR, 1998) u Risk of HIV infection at least 2 - to 4 -fold higher among women presenting for delivery without prenatal care E Aaron, CRNP. Presented at Clinical Pathway, August 2002.
 Missed Opportunities - u Women who do not receive prenatal care u Pregnant women who seek prenatal care erratically u Non-legal residents u Injection drug users u Homeless u Women who receive prenatal care but are not offered testing E Aaron, CRNP. Presented at Clinical Pathway, August 2002.
Missed Opportunities - u Women who do not receive prenatal care u Pregnant women who seek prenatal care erratically u Non-legal residents u Injection drug users u Homeless u Women who receive prenatal care but are not offered testing E Aaron, CRNP. Presented at Clinical Pathway, August 2002.
 rd Trimester Testing 3 - u Retesting in the third trimester, preferably before 36 weeks of gestation, is recommended for women known to be at high risk for acquiring HIV: n n n who have a history of sexually transmitted diseases, who exchange sex for money or drugs, who have multiple sex partners during pregnancy, who use illicit drugs, who have sex partner(s) known to be HIV-positive or at high risk who have signs and symptoms of seroconversion. CDC. Revised US Public Health Service recommendations for human immunodeficiency virus screening of pregnant women. MMWR 2001; 50(No. RR-19): 59 --86.
rd Trimester Testing 3 - u Retesting in the third trimester, preferably before 36 weeks of gestation, is recommended for women known to be at high risk for acquiring HIV: n n n who have a history of sexually transmitted diseases, who exchange sex for money or drugs, who have multiple sex partners during pregnancy, who use illicit drugs, who have sex partner(s) known to be HIV-positive or at high risk who have signs and symptoms of seroconversion. CDC. Revised US Public Health Service recommendations for human immunodeficiency virus screening of pregnant women. MMWR 2001; 50(No. RR-19): 59 --86.
 Rapid Testing at Delivery - u High risk of perinatal transmission in women without antenatal care and without HIV counseling and testing u Rapid testing during labor can make it possible to initiate ART prophylaxis and to refer the woman for care u ART prophylaxis should be initiated as soon as possible after a positive rapid HIV test (before confirmatory test results are available)
Rapid Testing at Delivery - u High risk of perinatal transmission in women without antenatal care and without HIV counseling and testing u Rapid testing during labor can make it possible to initiate ART prophylaxis and to refer the woman for care u ART prophylaxis should be initiated as soon as possible after a positive rapid HIV test (before confirmatory test results are available)
 HIV Antibody Tests u Serum antibody (EIA) u Saliva and urine antibody tests (EIA) u Rapid tests n SUDS (Microfiltration EIA) u n Laboratory-based Ora. Quick u Point of care u Western blot assay n Confirmatory test -
HIV Antibody Tests u Serum antibody (EIA) u Saliva and urine antibody tests (EIA) u Rapid tests n SUDS (Microfiltration EIA) u n Laboratory-based Ora. Quick u Point of care u Western blot assay n Confirmatory test -
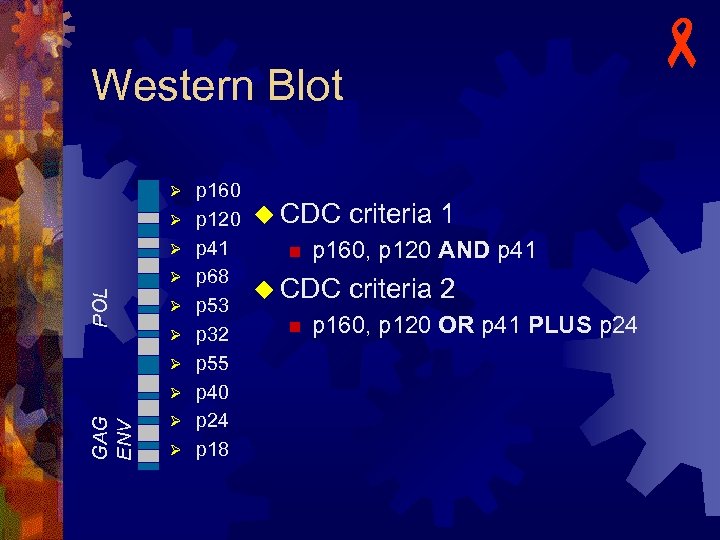 Western Blot Ø Ø Ø POL Ø Ø GAG ENV Ø Ø Ø p 160 p 120 u CDC criteria 1 p 41 n p 160, p 120 AND p 41 p 68 u CDC criteria 2 p 53 n p 160, p 120 OR p 41 PLUS p 24 p 32 p 55 p 40 p 24 p 18 -
Western Blot Ø Ø Ø POL Ø Ø GAG ENV Ø Ø Ø p 160 p 120 u CDC criteria 1 p 41 n p 160, p 120 AND p 41 p 68 u CDC criteria 2 p 53 n p 160, p 120 OR p 41 PLUS p 24 p 32 p 55 p 40 p 24 p 18 -
 HIV Direct Tests u Viral Load Qualitative / quantitative n RNA through b. DNA or PCR n u p 24 antigen tests -
HIV Direct Tests u Viral Load Qualitative / quantitative n RNA through b. DNA or PCR n u p 24 antigen tests -
 -
-
 HIV care During Pregnancy - u Use optimal ART for the woman’s health u Add ZDV to regimen to reduce perinatal HIV transmission u Discuss preventable risk factors u Counsel on cesarean delivery u Support decision-making by woman following discussion of known and unknown benefits and risks u Acceptance or refusal of ART or ZDV should not result in denial of care or punitive action
HIV care During Pregnancy - u Use optimal ART for the woman’s health u Add ZDV to regimen to reduce perinatal HIV transmission u Discuss preventable risk factors u Counsel on cesarean delivery u Support decision-making by woman following discussion of known and unknown benefits and risks u Acceptance or refusal of ART or ZDV should not result in denial of care or punitive action
 Pregnancy Effects on HIV - u In all women, the absolute CD 4 count decreases no matter whether HIVpositive or negative (pregnancy does not make HIV worse) u In HIV-positive women, percentage of CD 4 cells should not change and viral load should not change because of pregnancy
Pregnancy Effects on HIV - u In all women, the absolute CD 4 count decreases no matter whether HIVpositive or negative (pregnancy does not make HIV worse) u In HIV-positive women, percentage of CD 4 cells should not change and viral load should not change because of pregnancy
 Adult Treatment Guidelines Clinical Category CD 4+ count Any value Symptomatic HIV RNA Any value - Recommendations Treat Asymptomatic, AIDS CD 4+ T cells <200/mm 3 Any value Treat Asymptomatic CD 4+ T cells >200/mm 3 but <350 /mm 3 Any value Treatment should be offered Asymptomatic CD 4+ T cells >350/mm 3 >100, 000 Most recommend deferring treatment, but some would treat. Asymptomatic CD 4+ T cells >350/mm 3 <100, 000 Defer therapy
Adult Treatment Guidelines Clinical Category CD 4+ count Any value Symptomatic HIV RNA Any value - Recommendations Treat Asymptomatic, AIDS CD 4+ T cells <200/mm 3 Any value Treat Asymptomatic CD 4+ T cells >200/mm 3 but <350 /mm 3 Any value Treatment should be offered Asymptomatic CD 4+ T cells >350/mm 3 >100, 000 Most recommend deferring treatment, but some would treat. Asymptomatic CD 4+ T cells >350/mm 3 <100, 000 Defer therapy
 Antiretroviral Agents - 1 u - Nucleoside / nucleotide analogues (NRTIs) n ABC Ø C – No studies. Concern for hypersensitivity n dd. I Ø B – Concern for lactic acidosis (do not use w/ d 4 T) n FTC Ø B – No studies. n 3 TC Ø C – Well tolerated. Widely used. n d 4 T Ø C – Concern for lactic acidosis (do not use w/ dd. I) n TDF Ø B – No studies. Animal reports of bone abnls n dd. C Ø C – No studies. Teratogenic in animals. n ZDV/ Ø C – Well tolerated. The most experience. AZT
Antiretroviral Agents - 1 u - Nucleoside / nucleotide analogues (NRTIs) n ABC Ø C – No studies. Concern for hypersensitivity n dd. I Ø B – Concern for lactic acidosis (do not use w/ d 4 T) n FTC Ø B – No studies. n 3 TC Ø C – Well tolerated. Widely used. n d 4 T Ø C – Concern for lactic acidosis (do not use w/ dd. I) n TDF Ø B – No studies. Animal reports of bone abnls n dd. C Ø C – No studies. Teratogenic in animals. n ZDV/ Ø C – Well tolerated. The most experience. AZT
 Antiretroviral Agents - 2 - u Non-nucleoside RT inhibitors (NNRTIs) Ø n DLV EFV n NVP Ø n Ø Ø C – No studies. D – Teratogenic. 4/142 birth defects. Avoid in 1 st trimester C – Well tolerated. Avoid initiating if CD 4 >250 cells/mm 3. Used as single-dose Rx in labor to prevent perinatal transmission (consider adding ZDV/3 TC for 3 -7 days to reduce risk of NVP resistance).
Antiretroviral Agents - 2 - u Non-nucleoside RT inhibitors (NNRTIs) Ø n DLV EFV n NVP Ø n Ø Ø C – No studies. D – Teratogenic. 4/142 birth defects. Avoid in 1 st trimester C – Well tolerated. Avoid initiating if CD 4 >250 cells/mm 3. Used as single-dose Rx in labor to prevent perinatal transmission (consider adding ZDV/3 TC for 3 -7 days to reduce risk of NVP resistance).
 Antiretroviral Agents - 3 - u Protease inhibitors (PIs) n APV Ø C – No studies. Oral solution contraindicated. n ATV Ø B – No studies. Concern hyperbilirubinemia n FPV Ø C – No studies n IDV Ø C – Unboosted: poor blood levels in preg n LP/r Ø C – No studies n NFV Ø B – Registry data shows no incr in birth def n RTV Ø B –Not used alone due to GI side effects n SQV Ø B – Well tolerated, used boosted n TPV Ø C – No studies
Antiretroviral Agents - 3 - u Protease inhibitors (PIs) n APV Ø C – No studies. Oral solution contraindicated. n ATV Ø B – No studies. Concern hyperbilirubinemia n FPV Ø C – No studies n IDV Ø C – Unboosted: poor blood levels in preg n LP/r Ø C – No studies n NFV Ø B – Registry data shows no incr in birth def n RTV Ø B –Not used alone due to GI side effects n SQV Ø B – Well tolerated, used boosted n TPV Ø C – No studies
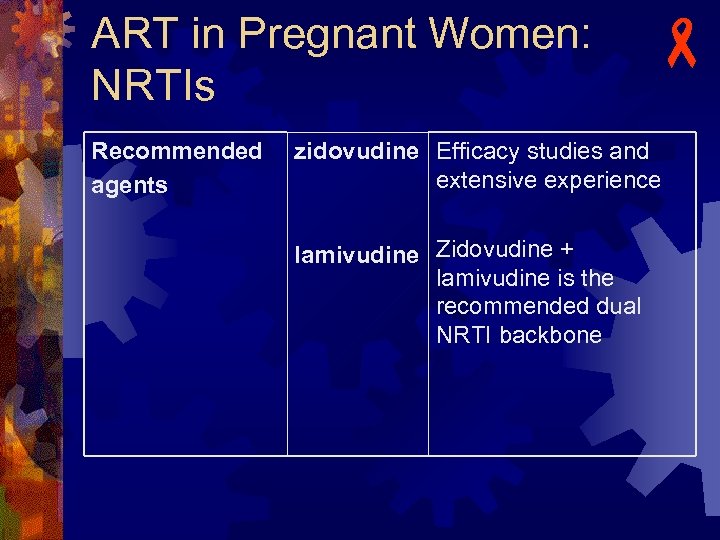 ART in Pregnant Women: NRTIs Recommended agents - zidovudine Efficacy studies and extensive experience lamivudine Zidovudine + lamivudine is the recommended dual NRTI backbone
ART in Pregnant Women: NRTIs Recommended agents - zidovudine Efficacy studies and extensive experience lamivudine Zidovudine + lamivudine is the recommended dual NRTI backbone
 ART in Pregnant Women: NRTIs - Alternate agents abacavir didanosine emtricitabine stavudine Cases of lactic acidosis with didanosine + stavudine; use only if no other alternatives Insufficient data to recommend tenofovir No studies in human pregnancy; bone toxicity in monkey studies Not zalcitabine recommended Teratogenic in animals
ART in Pregnant Women: NRTIs - Alternate agents abacavir didanosine emtricitabine stavudine Cases of lactic acidosis with didanosine + stavudine; use only if no other alternatives Insufficient data to recommend tenofovir No studies in human pregnancy; bone toxicity in monkey studies Not zalcitabine recommended Teratogenic in animals
 ART in Pregnant Women: NNRTIs - Recommended nevirapine No evidence of teratogenicity agent Increased risk of liver toxicity in women who start nevirapine with CD 4>250; monitor closely, especially for first 18 weeks of therapy Not recommended efavirenz Teratogenic in monkeys Avoid in first trimester; consider after second trimester only if no other alternatives delavirdine Teratogenic in rodent studies
ART in Pregnant Women: NNRTIs - Recommended nevirapine No evidence of teratogenicity agent Increased risk of liver toxicity in women who start nevirapine with CD 4>250; monitor closely, especially for first 18 weeks of therapy Not recommended efavirenz Teratogenic in monkeys Avoid in first trimester; consider after second trimester only if no other alternatives delavirdine Teratogenic in rodent studies
 - ART in Pregnant Women: PIs Recommended nelfinavir agents saquinavir (soft gel capsule)/ ritonavir PK studies and extensive experience Preferred PI for combination therapy PK studies and moderate experience Unboosted saquinavir: inadequate drug levels in pregnant women No PK data on saquinavir hard gel capsule
- ART in Pregnant Women: PIs Recommended nelfinavir agents saquinavir (soft gel capsule)/ ritonavir PK studies and extensive experience Preferred PI for combination therapy PK studies and moderate experience Unboosted saquinavir: inadequate drug levels in pregnant women No PK data on saquinavir hard gel capsule
 - ART in Pregnant Women: PIs Alternate indinavir agents Lower drug levels during pregnancy May require boosting with ritonavir; PK study underway Concern for possible hyperbilirubinemia in the neonate lopinavir/ ritonavir Limited experience; study underway Dosing recommendations not established; may require increased dose during pregnancy ritonavir Lower drug levels in pregnancy Minimal experience
- ART in Pregnant Women: PIs Alternate indinavir agents Lower drug levels during pregnancy May require boosting with ritonavir; PK study underway Concern for possible hyperbilirubinemia in the neonate lopinavir/ ritonavir Limited experience; study underway Dosing recommendations not established; may require increased dose during pregnancy ritonavir Lower drug levels in pregnancy Minimal experience
 - ART in Pregnant Women: PIs Insufficient data to recommend amprenavir No studies in human pregnancy Oral solution contraindicated (contains propylene glycol) atazanavir No studies in human pregnancy Concern for possible hyperbilirubinemia in neonate fosamprenavir No studies in human pregnancy
- ART in Pregnant Women: PIs Insufficient data to recommend amprenavir No studies in human pregnancy Oral solution contraindicated (contains propylene glycol) atazanavir No studies in human pregnancy Concern for possible hyperbilirubinemia in neonate fosamprenavir No studies in human pregnancy
 ART in Pregnant Women: Fusion Inhibitors Insufficient data to recommend enfuvirtide No studies in human pregnancy -
ART in Pregnant Women: Fusion Inhibitors Insufficient data to recommend enfuvirtide No studies in human pregnancy -
 NRTI Toxicity u Bone marrow suppression ZDV (AZT) n Anemia(1%- severe, 50%-mild) u Mitochondrial toxicity Related to inhibition of DNA polymerase u dd. C > dd. I > d 4 T > ZDV > 3 TC > ABC > TDF u n Peripheral neuropathy(15 -35%) u n dd. C > dd. I > d 4 T Pancreatitis (6 -10%) u dd. I > dd. C > 3 TC u Hypersensitivity rash (3 -5%) n Abacavir n Not related to mitochondria -
NRTI Toxicity u Bone marrow suppression ZDV (AZT) n Anemia(1%- severe, 50%-mild) u Mitochondrial toxicity Related to inhibition of DNA polymerase u dd. C > dd. I > d 4 T > ZDV > 3 TC > ABC > TDF u n Peripheral neuropathy(15 -35%) u n dd. C > dd. I > d 4 T Pancreatitis (6 -10%) u dd. I > dd. C > 3 TC u Hypersensitivity rash (3 -5%) n Abacavir n Not related to mitochondria -
 - NRTI Toxicity During Pregnancy u Symptoms may be subtle, insidious, and non- specific n Fatigue, nausea, anorexia, abdominal pain, weakness u May be synergistic with maternal changes seen during pregnancy u Overlaps with other complications of pregnancy n n Acute fatty liver of pregnancy HELLP syndrome
- NRTI Toxicity During Pregnancy u Symptoms may be subtle, insidious, and non- specific n Fatigue, nausea, anorexia, abdominal pain, weakness u May be synergistic with maternal changes seen during pregnancy u Overlaps with other complications of pregnancy n n Acute fatty liver of pregnancy HELLP syndrome
 Lactic Acidosis u u u - Lactic acidosis is a rare life-threatening complication of antiretroviral therapy Nucleoside analogue therapy-induced mitochondrial toxicity appears to be the cause of this syndrome Diagnosis is difficult because symptoms are vague and non-specific Routine monitoring of lactate levels is not recommended in asymptomatic patients; however, lactate should be measured in patients with unexplained weight loss, nausea, or abdominal pain Treatment includes discontinuing NRTIs, followed by supportive care measures
Lactic Acidosis u u u - Lactic acidosis is a rare life-threatening complication of antiretroviral therapy Nucleoside analogue therapy-induced mitochondrial toxicity appears to be the cause of this syndrome Diagnosis is difficult because symptoms are vague and non-specific Routine monitoring of lactate levels is not recommended in asymptomatic patients; however, lactate should be measured in patients with unexplained weight loss, nausea, or abdominal pain Treatment includes discontinuing NRTIs, followed by supportive care measures
 - Lactic Acidosis u Symptoms n n n u Laboratory Findings Nausea and vomiting Abdominal pain Weight loss Malaise Dyspnea/tachypnea n n n Increased anion gap Increased lactic acid levels Increased lactate/pyruvate Adapted from: Boxwell DE, Styrt BA. 39 th ICAAC, San Francisco, CA, 1999. Abstract 1284.
- Lactic Acidosis u Symptoms n n n u Laboratory Findings Nausea and vomiting Abdominal pain Weight loss Malaise Dyspnea/tachypnea n n n Increased anion gap Increased lactic acid levels Increased lactate/pyruvate Adapted from: Boxwell DE, Styrt BA. 39 th ICAAC, San Francisco, CA, 1999. Abstract 1284.
 NNRTI Toxicities - u Rash 5 -20% u Delavirdine > nevirapine > efavirenz u CNS 5% n Dizziness, vivid dreams, psychiatric u Efavirenz >> nevirapine u Nausea/diarrhea u Any u Liver toxicity 2 -5% u Nevirapine (400 mg QD > 200 mg BID; risk greater if CD 4 count before initiation of NVP in women is >250 cells/mm 3) u Fetal abnormalities u Efavirenz
NNRTI Toxicities - u Rash 5 -20% u Delavirdine > nevirapine > efavirenz u CNS 5% n Dizziness, vivid dreams, psychiatric u Efavirenz >> nevirapine u Nausea/diarrhea u Any u Liver toxicity 2 -5% u Nevirapine (400 mg QD > 200 mg BID; risk greater if CD 4 count before initiation of NVP in women is >250 cells/mm 3) u Fetal abnormalities u Efavirenz
 -
-
 PI Toxicities - u Lipodystrophy (up to 84%, severe in 12%) u Glucose intolerance (up to 23%) u Dyslipidemia (up to 90%) u Cutaneous changes, e. g. , dry skin
PI Toxicities - u Lipodystrophy (up to 84%, severe in 12%) u Glucose intolerance (up to 23%) u Dyslipidemia (up to 90%) u Cutaneous changes, e. g. , dry skin
 Glucose Metabolism - u Abnormalities of glucose homeostasis (primarily insulin resistance) are common in patients on ART u Higher incidence in patients receiving PIs u Mechanisms remain unclear at this time u Treatment with insulin-sensitizing agents may be beneficial
Glucose Metabolism - u Abnormalities of glucose homeostasis (primarily insulin resistance) are common in patients on ART u Higher incidence in patients receiving PIs u Mechanisms remain unclear at this time u Treatment with insulin-sensitizing agents may be beneficial
 Insulin Resistance u Increased insulin levels found Blood sugars normal n State of compensated insulin resistance n -
Insulin Resistance u Increased insulin levels found Blood sugars normal n State of compensated insulin resistance n -
 - Antiretroviral Pregnancy Registry u Collaborative project managed by Pharma. Research Corporation on behalf of an advisory committee (specialists in OB/GYN, ID, teratology, epidemiology, and CDC and NIH members) and sponsored by: n Abbott Laboratories, Agouron Pharmaceuticals, Inc. , Boehringer Ingelheim Company, Bristol-Myers Squibb, Co. , Gilead Sciences, Inc. , Glaxo. Smith. Kline, F. Hoffmann. La. Roche Ltd. , Merck & Co. , Inc. and Pharma. Research. Purpose: To assess safety of ARVs during pregnancy u Telephone: (800) 258 -4263 Fax: (800) 800 -1052 available at http: //www. apregistry. com u
- Antiretroviral Pregnancy Registry u Collaborative project managed by Pharma. Research Corporation on behalf of an advisory committee (specialists in OB/GYN, ID, teratology, epidemiology, and CDC and NIH members) and sponsored by: n Abbott Laboratories, Agouron Pharmaceuticals, Inc. , Boehringer Ingelheim Company, Bristol-Myers Squibb, Co. , Gilead Sciences, Inc. , Glaxo. Smith. Kline, F. Hoffmann. La. Roche Ltd. , Merck & Co. , Inc. and Pharma. Research. Purpose: To assess safety of ARVs during pregnancy u Telephone: (800) 258 -4263 Fax: (800) 800 -1052 available at http: //www. apregistry. com u
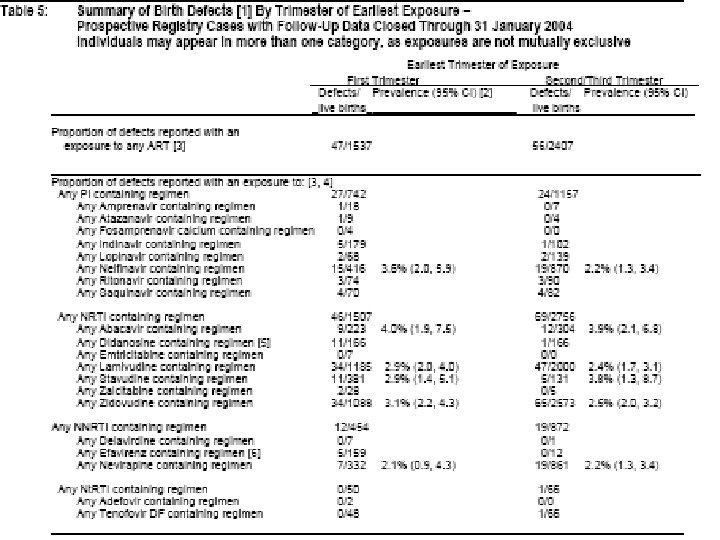
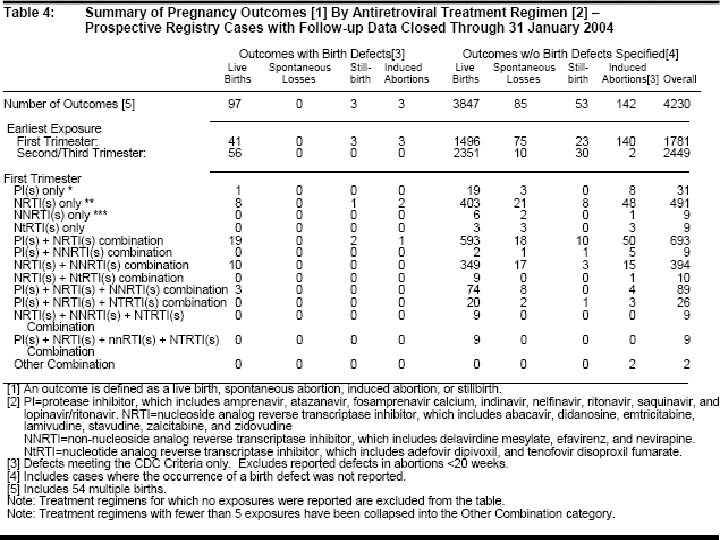
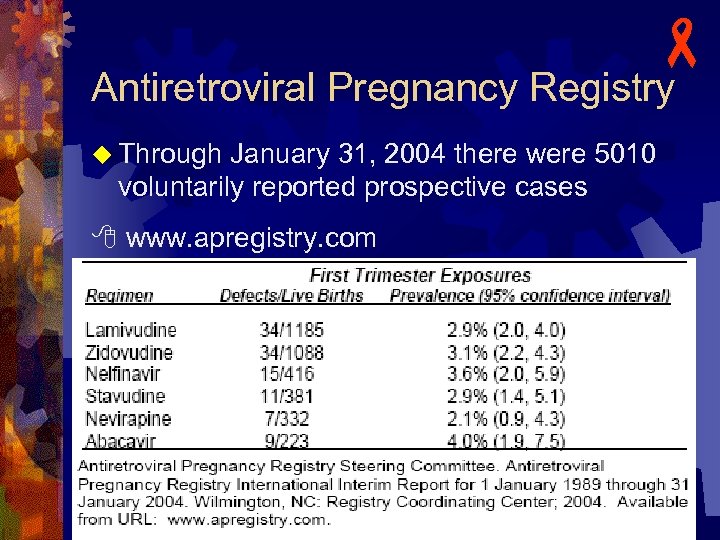 - Antiretroviral Pregnancy Registry u Through January 31, 2004 there were 5010 voluntarily reported prospective cases www. apregistry. com
- Antiretroviral Pregnancy Registry u Through January 31, 2004 there were 5010 voluntarily reported prospective cases www. apregistry. com
 -
-
 -
-
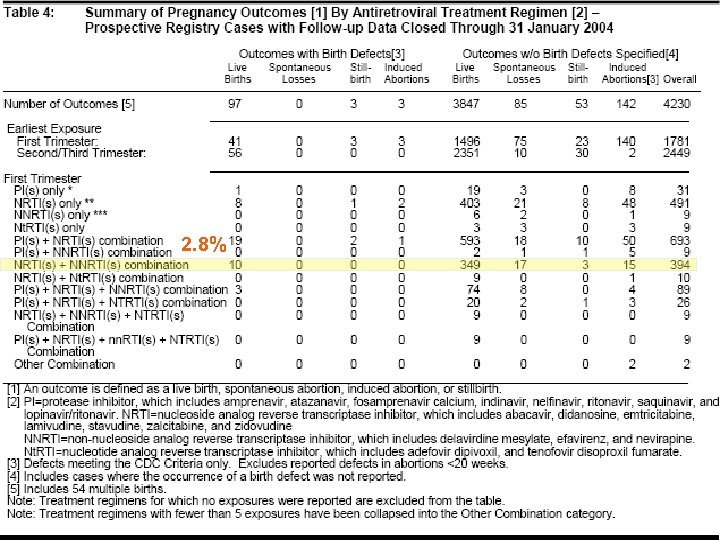 - 2. 8%
- 2. 8%
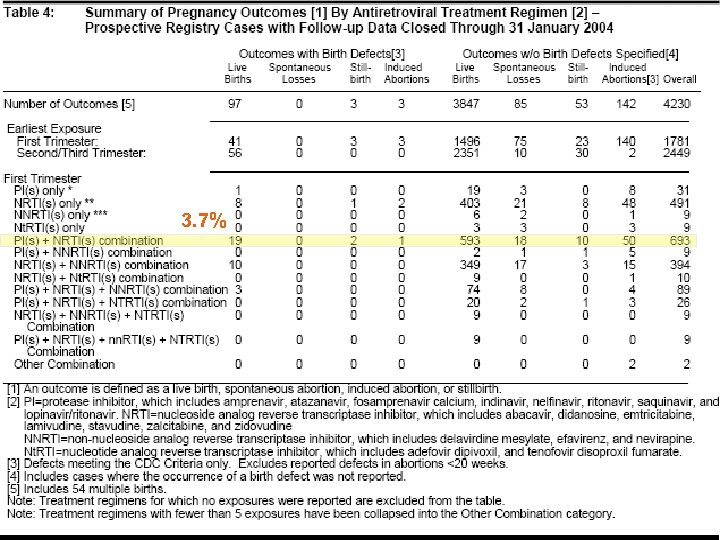 3. 7%
3. 7%
 HIV and Pregnancy - u Perinatal Transmission Historical risk: 28% n ACTG 076: 8% n Effective ART (VL<50 copies/mm 3) : <1% n C-section: 50% n
HIV and Pregnancy - u Perinatal Transmission Historical risk: 28% n ACTG 076: 8% n Effective ART (VL<50 copies/mm 3) : <1% n C-section: 50% n
 Perinatal HIV Transmission - u Documented transmission: intrauterine, intrapartum, and postpartum through breastfeeding In utero 25%– 40% of cases n Intrapartum 60%– 75% of cases n Postpartum additional risk with breastfeeding n 14% risk with established infection u 29% risk with primary infection u
Perinatal HIV Transmission - u Documented transmission: intrauterine, intrapartum, and postpartum through breastfeeding In utero 25%– 40% of cases n Intrapartum 60%– 75% of cases n Postpartum additional risk with breastfeeding n 14% risk with established infection u 29% risk with primary infection u
 Perinatal HIV Transmission Timing In utero At delivery - Intervention ç Effective ART ç Decrease fetal trauma ç Intrapartum ART ç C-section After delivery ç Alternatives to breast feeding ç Postpartum prophylaxis for baby
Perinatal HIV Transmission Timing In utero At delivery - Intervention ç Effective ART ç Decrease fetal trauma ç Intrapartum ART ç C-section After delivery ç Alternatives to breast feeding ç Postpartum prophylaxis for baby
 - Risk Factors for Transmission u u u u HIV viral load (HIVRNA level) Genital tract viral load CD 4 cell count Clinical stage of HIV Smoking cigarettes Substance abuse Vitamin A deficiency Unprotected sex with multiple partners u u u u STDs and other coinfections Antiretroviral agents Preterm delivery Placental disruption Invasive fetal monitoring Duration of membrane rupture (2% per hr) Breastfeeding Vaginal delivery vs. cesarean section 1 Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland.
- Risk Factors for Transmission u u u u HIV viral load (HIVRNA level) Genital tract viral load CD 4 cell count Clinical stage of HIV Smoking cigarettes Substance abuse Vitamin A deficiency Unprotected sex with multiple partners u u u u STDs and other coinfections Antiretroviral agents Preterm delivery Placental disruption Invasive fetal monitoring Duration of membrane rupture (2% per hr) Breastfeeding Vaginal delivery vs. cesarean section 1 Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland.
 ACTG 076 - A phase III randomized placebo-controlled trial of zidovudine (ZDV, AZT) for the prevention of maternalfetal HIV transmission u Treatment Regimen u n n n Antepartum 100 mg ZDV po 5 x day, started at 14 -34 weeks gestation Intrapartum During labor, 1 - hour initial dose 2 mg/kg IV followed by continuous infusion of 1 mg/kg until delivery Postpartum/Infant 2 mg/kg po q 6 hr for 6 weeks, started within 8 -12 hours after birth
ACTG 076 - A phase III randomized placebo-controlled trial of zidovudine (ZDV, AZT) for the prevention of maternalfetal HIV transmission u Treatment Regimen u n n n Antepartum 100 mg ZDV po 5 x day, started at 14 -34 weeks gestation Intrapartum During labor, 1 - hour initial dose 2 mg/kg IV followed by continuous infusion of 1 mg/kg until delivery Postpartum/Infant 2 mg/kg po q 6 hr for 6 weeks, started within 8 -12 hours after birth
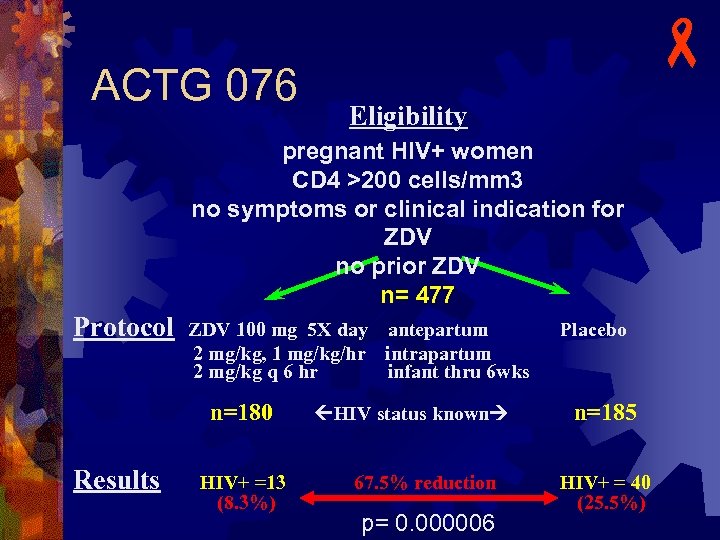 ACTG 076 Eligibility pregnant HIV+ women CD 4 >200 cells/mm 3 no symptoms or clinical indication for ZDV no prior ZDV n= 477 Protocol ZDV 100 mg 5 X day antepartum 2 mg/kg, 1 mg/kg/hr intrapartum 2 mg/kg q 6 hr infant thru 6 wks n=180 Results HIV+ =13 (8. 3%) HIV status known 67. 5% reduction p= 0. 000006 Placebo n=185 HIV+ = 40 (25. 5%)
ACTG 076 Eligibility pregnant HIV+ women CD 4 >200 cells/mm 3 no symptoms or clinical indication for ZDV no prior ZDV n= 477 Protocol ZDV 100 mg 5 X day antepartum 2 mg/kg, 1 mg/kg/hr intrapartum 2 mg/kg q 6 hr infant thru 6 wks n=180 Results HIV+ =13 (8. 3%) HIV status known 67. 5% reduction p= 0. 000006 Placebo n=185 HIV+ = 40 (25. 5%)
 ACTG 076 Follow-up - u Follow-up of uninfected infants PACTG 076 n No significant differences in infant growth, development, or immune function in placebo vs. ZDV n No differences in Bayley developmental scores in uninfected infants (ACTG 219) n No other safety abnormalities have been identified n Follow-up of infants with exposure to nucleoside analogues is ongoing due to the potential for mitochondrial toxicity n In the U. S. no cases of mitochondrial toxicity have been identified
ACTG 076 Follow-up - u Follow-up of uninfected infants PACTG 076 n No significant differences in infant growth, development, or immune function in placebo vs. ZDV n No differences in Bayley developmental scores in uninfected infants (ACTG 219) n No other safety abnormalities have been identified n Follow-up of infants with exposure to nucleoside analogues is ongoing due to the potential for mitochondrial toxicity n In the U. S. no cases of mitochondrial toxicity have been identified
 ACTG 076 Follow-up - u Follow-Up of Mothers (ACTG 288) Median follow-up 4. 2 years n No substantial differences in CD 4 count, time to progression to AIDS, or death in women who received ZDV vs. placebo n
ACTG 076 Follow-up - u Follow-Up of Mothers (ACTG 288) Median follow-up 4. 2 years n No substantial differences in CD 4 count, time to progression to AIDS, or death in women who received ZDV vs. placebo n
 ACTG 076 Protocol - u Should be used as part of ART regimen in all pregnant women, if possible Antepartum: AZT 300 bid or 200 tid po, from week 14 until delivery n Intrapartum: AZT 2 mg/kg IV over first hour, then 1 mg/kg/hr until delivery n Postpartum: (Infant): AZT syrup 2 mg/kg po q 6 h (or 1. 5 mg/kg q 6 h IV) x 6 wks n
ACTG 076 Protocol - u Should be used as part of ART regimen in all pregnant women, if possible Antepartum: AZT 300 bid or 200 tid po, from week 14 until delivery n Intrapartum: AZT 2 mg/kg IV over first hour, then 1 mg/kg/hr until delivery n Postpartum: (Infant): AZT syrup 2 mg/kg po q 6 h (or 1. 5 mg/kg q 6 h IV) x 6 wks n
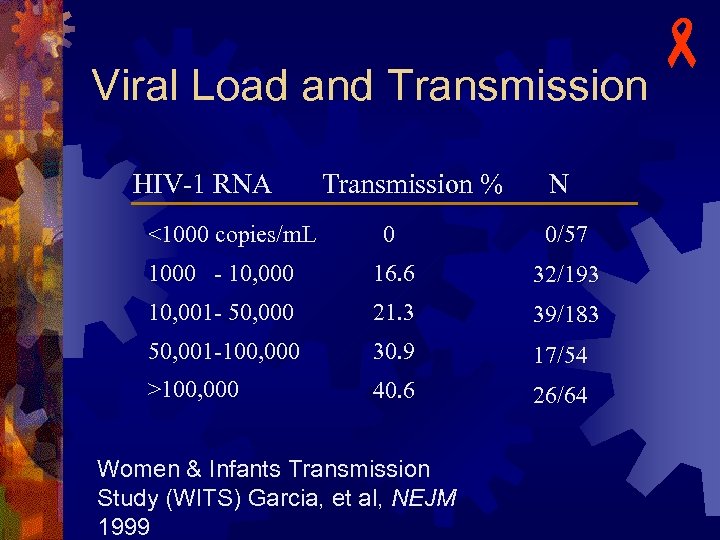 Viral Load and Transmission HIV-1 RNA Transmission % N 0 0/57 1000 - 10, 000 16. 6 32/193 10, 001 - 50, 000 21. 3 39/183 50, 001 -100, 000 30. 9 17/54 >100, 000 40. 6 26/64 <1000 copies/m. L Women & Infants Transmission Study (WITS) Garcia, et al, NEJM 1999 -
Viral Load and Transmission HIV-1 RNA Transmission % N 0 0/57 1000 - 10, 000 16. 6 32/193 10, 001 - 50, 000 21. 3 39/183 50, 001 -100, 000 30. 9 17/54 >100, 000 40. 6 26/64 <1000 copies/m. L Women & Infants Transmission Study (WITS) Garcia, et al, NEJM 1999 -
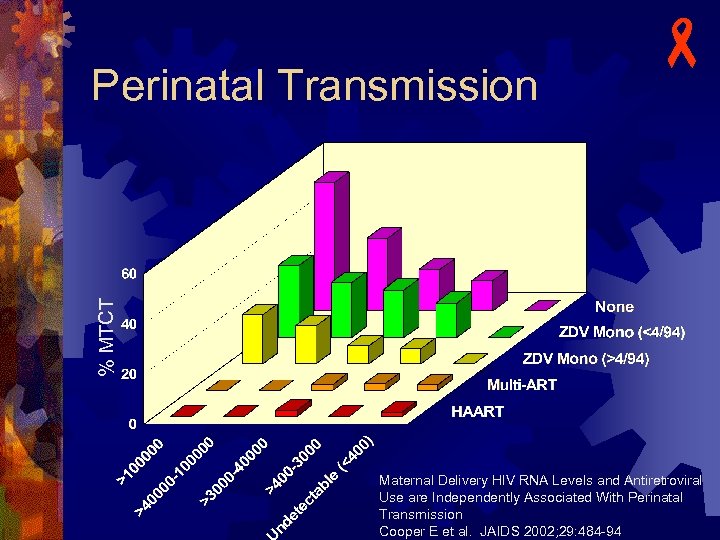 % MTCT Perinatal Transmission - Maternal Delivery HIV RNA Levels and Antiretroviral Use are Independently Associated With Perinatal Transmission Cooper E et al. JAIDS 2002; 29: 484 -94
% MTCT Perinatal Transmission - Maternal Delivery HIV RNA Levels and Antiretroviral Use are Independently Associated With Perinatal Transmission Cooper E et al. JAIDS 2002; 29: 484 -94
 - Studies of Short Course Therapy u Oral ZDV in a non-breastfeeding population (Thailand) from 36 weeks and during labor n n u Petra study – intrapartum/postpartum oral ZDV/3 TC in a breast-feeding population (Uganda, S. Africa, Tanzania) n n u Transmission rate: 9. 4 % ZDV vs 18. 9 % placebo Lancet. 1999 Mar 6; 353(9155): 773 -80 Transmission rate: 10% ZDV/3 TC vs 17% placebo Lancet. 2002 Apr 6; 359(9313): 1178 -86 HIVNet 012 – intrapartum/postpartum/neonatal nevirapine (NVP) vs short course/neonatal ZDV in a breast-feeding population (Uganda) n n Transmission rate: 12% NVP vs 21% ZDV Lancet. 1999 Sep 4; 354(9181): 795 -802
- Studies of Short Course Therapy u Oral ZDV in a non-breastfeeding population (Thailand) from 36 weeks and during labor n n u Petra study – intrapartum/postpartum oral ZDV/3 TC in a breast-feeding population (Uganda, S. Africa, Tanzania) n n u Transmission rate: 9. 4 % ZDV vs 18. 9 % placebo Lancet. 1999 Mar 6; 353(9155): 773 -80 Transmission rate: 10% ZDV/3 TC vs 17% placebo Lancet. 2002 Apr 6; 359(9313): 1178 -86 HIVNet 012 – intrapartum/postpartum/neonatal nevirapine (NVP) vs short course/neonatal ZDV in a breast-feeding population (Uganda) n n Transmission rate: 12% NVP vs 21% ZDV Lancet. 1999 Sep 4; 354(9181): 795 -802
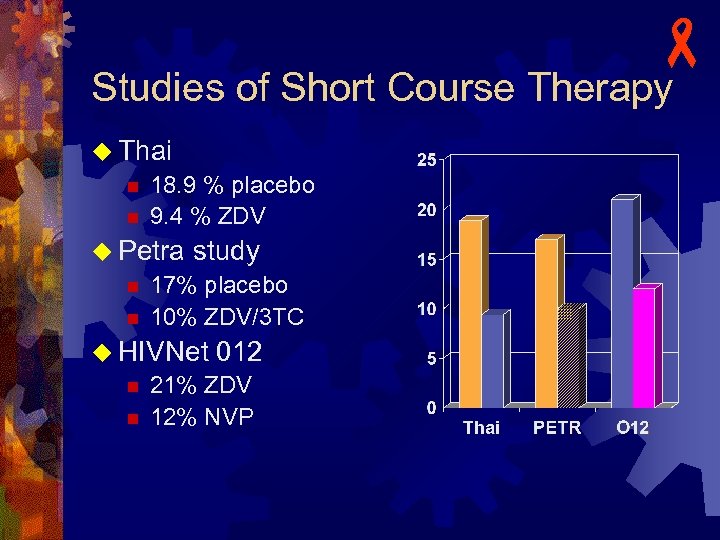 - Studies of Short Course Therapy u Thai n 18. 9 % placebo n 9. 4 % ZDV u Petra study n 17% placebo n 10% ZDV/3 TC u HIVNet 012 n 21% ZDV n 12% NVP
- Studies of Short Course Therapy u Thai n 18. 9 % placebo n 9. 4 % ZDV u Petra study n 17% placebo n 10% ZDV/3 TC u HIVNet 012 n 21% ZDV n 12% NVP
 Suboptimal Regimens - u HIV transmission rates with partial ZDV (AZT) regimens (New York cohort): u 6. 1% with prenatal, intrapartum, and infant ZDV 10% with only intrapartum ZDV n 9. 3% with only infant ZDV started within first 48 hours n 26. 6% with no ZDV n
Suboptimal Regimens - u HIV transmission rates with partial ZDV (AZT) regimens (New York cohort): u 6. 1% with prenatal, intrapartum, and infant ZDV 10% with only intrapartum ZDV n 9. 3% with only infant ZDV started within first 48 hours n 26. 6% with no ZDV n
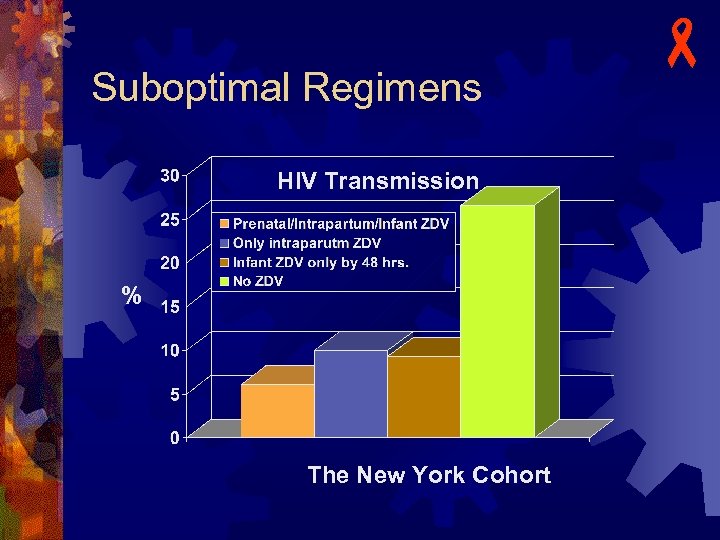 Suboptimal Regimens HIV Transmission % The New York Cohort -
Suboptimal Regimens HIV Transmission % The New York Cohort -
 Perinatal Guidelines - u USPHS Task Force n n Recommendations for the Use of Antiretroviral Drugs in Pregnant HIV-1 Infected Women for Maternal Health and to Reduce Perinatal HIV-1 Transmission in the United States Developed in 1994 in response to ACTG 076 Working Group reconvened in December 1999 and meets monthly Last Updated November 17, 2005
Perinatal Guidelines - u USPHS Task Force n n Recommendations for the Use of Antiretroviral Drugs in Pregnant HIV-1 Infected Women for Maternal Health and to Reduce Perinatal HIV-1 Transmission in the United States Developed in 1994 in response to ACTG 076 Working Group reconvened in December 1999 and meets monthly Last Updated November 17, 2005
 Clinical Scenario - 1 u - HIV-1 -infected pregnant women who have not received prior antiretroviral therapy. n n n Pregnant women with HIV-1 infection must receive standard clinical, immunologic, and virologic evaluation. Recommendations for initiation and choice of antiretroviral therapy should be based on the same parameters used for persons who are not pregnant, although the known and unknown risks and benefits of such therapy during pregnancy must be considered and discussed. The three-part ZDV chemoprophylaxis regimen, initiated after the first trimester, is recommended for all pregnant women with HIV-1 infection regardless of antenatal HIV RNA copy number to reduce the risk for perinatal transmission. The combination of ZDV chemoprophylaxis with additional antiretroviral drugs for treatment of HIV-1 infection is recommended for infected women whose clinical, immunologic or virologic status requires treatment or who have HIV-1 RNA over 1, 000 copies/m. L regardless of clinical or immunologic status, and can be considered for women with HIV-1 RNA < 1, 000 copies/m. L. Women who are in the first trimester of pregnancy may consider delaying initiation of therapy until after 10 -12 weeks’ gestation.
Clinical Scenario - 1 u - HIV-1 -infected pregnant women who have not received prior antiretroviral therapy. n n n Pregnant women with HIV-1 infection must receive standard clinical, immunologic, and virologic evaluation. Recommendations for initiation and choice of antiretroviral therapy should be based on the same parameters used for persons who are not pregnant, although the known and unknown risks and benefits of such therapy during pregnancy must be considered and discussed. The three-part ZDV chemoprophylaxis regimen, initiated after the first trimester, is recommended for all pregnant women with HIV-1 infection regardless of antenatal HIV RNA copy number to reduce the risk for perinatal transmission. The combination of ZDV chemoprophylaxis with additional antiretroviral drugs for treatment of HIV-1 infection is recommended for infected women whose clinical, immunologic or virologic status requires treatment or who have HIV-1 RNA over 1, 000 copies/m. L regardless of clinical or immunologic status, and can be considered for women with HIV-1 RNA < 1, 000 copies/m. L. Women who are in the first trimester of pregnancy may consider delaying initiation of therapy until after 10 -12 weeks’ gestation.
 Clinical Scenario - 2 u - HIV-1 -infected women receiving antiretroviral therapy during the current pregnancy. n HIV-1 infected women receiving antiretroviral therapy in whom pregnancy is identified after the first trimester should continue therapy. u n For women receiving antiretroviral therapy in whom pregnancy is recognized during the first trimester u u u n ZDV should be a component of the antenatal antiretroviral treatment regimen after the first trimester whenever possible, although this may not always be feasible. The woman should be counseled regarding the benefits and potential risks of antiretroviral administration during this period Continuation of therapy should be considered If therapy is discontinued during the first trimester, all drugs should be stopped and reintroduced simultaneously to avoid the development of drug resistance. Regardless of the antepartum antiretroviral regimen, ZDV administration is recommended during the intrapartum period and for the newborn.
Clinical Scenario - 2 u - HIV-1 -infected women receiving antiretroviral therapy during the current pregnancy. n HIV-1 infected women receiving antiretroviral therapy in whom pregnancy is identified after the first trimester should continue therapy. u n For women receiving antiretroviral therapy in whom pregnancy is recognized during the first trimester u u u n ZDV should be a component of the antenatal antiretroviral treatment regimen after the first trimester whenever possible, although this may not always be feasible. The woman should be counseled regarding the benefits and potential risks of antiretroviral administration during this period Continuation of therapy should be considered If therapy is discontinued during the first trimester, all drugs should be stopped and reintroduced simultaneously to avoid the development of drug resistance. Regardless of the antepartum antiretroviral regimen, ZDV administration is recommended during the intrapartum period and for the newborn.
 Clinical Scenario – 3 (1) u - HIV-1 -infected women in labor who have had no prior therapy. n Several effective regimens are available. These include: 1. intrapartum intravenous ZDV followed by six weeks of ZDV for the newborn; 2. oral ZDV and 3 TC during labor, followed by one week of oral ZDV-3 TC for the newborn; 3. a single dose nevirapine at the onset of labor followed by a single dose of nevirapine for the newborn at age 48 hours; and 4. the two-dose nevirapine regimen combined with intrapartum intravenous ZDV and six week ZDV for the newborn.
Clinical Scenario – 3 (1) u - HIV-1 -infected women in labor who have had no prior therapy. n Several effective regimens are available. These include: 1. intrapartum intravenous ZDV followed by six weeks of ZDV for the newborn; 2. oral ZDV and 3 TC during labor, followed by one week of oral ZDV-3 TC for the newborn; 3. a single dose nevirapine at the onset of labor followed by a single dose of nevirapine for the newborn at age 48 hours; and 4. the two-dose nevirapine regimen combined with intrapartum intravenous ZDV and six week ZDV for the newborn.
 Clinical Scenario – 3 (2) u - HIV-1 -infected women in labor who have had no prior therapy. § If single-dose NVP is given to the mother, alone or in combination with ZDV, consider adding maternal ZDV/3 TC starting as soon as possible (intrapartum or immediately postpartum) and continuing for 3 to 7 days. This may reduce development of NVP resistance. n In the immediate postpartum period, the woman should have appropriate assessments (e. g. , CD 4 count and HIV-1 RNA viral load) to determine whether antiretroviral therapy is recommended for her own health.
Clinical Scenario – 3 (2) u - HIV-1 -infected women in labor who have had no prior therapy. § If single-dose NVP is given to the mother, alone or in combination with ZDV, consider adding maternal ZDV/3 TC starting as soon as possible (intrapartum or immediately postpartum) and continuing for 3 to 7 days. This may reduce development of NVP resistance. n In the immediate postpartum period, the woman should have appropriate assessments (e. g. , CD 4 count and HIV-1 RNA viral load) to determine whether antiretroviral therapy is recommended for her own health.
 Clinical Scenario - 4 u - Infants born to mothers who have received no antiretroviral therapy during pregnancy or intrapartum. n n n The six-week neonatal ZDV component of the ZDV chemoprophylactic regimen should be discussed with the mother and offered for the newborn. ZDV should be initiated as soon as possible after delivery - preferably within 6 -12 hours of birth. Some clinicians may choose to use ZDV in combination with other antiretroviral drugs, particularly if the mother is known or suspected to have ZDV-resistant virus. u n However, the efficacy of this approach for prevention of transmission has not been proven in clinical trials, and appropriate dosing regimens for neonates are incompletely defined for many drugs. In the immediate postpartum period, the woman should undergo appropriate assessments (e. g. , CD 4 count and HIV-1 RNA viral load) to determine if antiretroviral therapy is required for her own health. The infant should undergo early diagnostic testing so that if HIV-infected, treatment can be initiated as soon as possible.
Clinical Scenario - 4 u - Infants born to mothers who have received no antiretroviral therapy during pregnancy or intrapartum. n n n The six-week neonatal ZDV component of the ZDV chemoprophylactic regimen should be discussed with the mother and offered for the newborn. ZDV should be initiated as soon as possible after delivery - preferably within 6 -12 hours of birth. Some clinicians may choose to use ZDV in combination with other antiretroviral drugs, particularly if the mother is known or suspected to have ZDV-resistant virus. u n However, the efficacy of this approach for prevention of transmission has not been proven in clinical trials, and appropriate dosing regimens for neonates are incompletely defined for many drugs. In the immediate postpartum period, the woman should undergo appropriate assessments (e. g. , CD 4 count and HIV-1 RNA viral load) to determine if antiretroviral therapy is required for her own health. The infant should undergo early diagnostic testing so that if HIV-infected, treatment can be initiated as soon as possible.
 Cesarean vs. Vaginal Birth u u u u - Risk of transmission increased 2% each hour after membranes have been ruptured Cesarean before labor and/or rupture of membranes reduces risk of transmission by 50– 80% compared with other modes of delivery in women on no antiretroviral therapy or on ZDV alone and VL >1000 No clear benefit with cesarean after onset of labor or membranes have been ruptured Cesarean increases morbidity and possible mortality to mother Give antibiotic prophylaxis for cesarean in HIVinfected women Complications of similar to HIV uninfected women Patient’s decision should be respected and honored
Cesarean vs. Vaginal Birth u u u u - Risk of transmission increased 2% each hour after membranes have been ruptured Cesarean before labor and/or rupture of membranes reduces risk of transmission by 50– 80% compared with other modes of delivery in women on no antiretroviral therapy or on ZDV alone and VL >1000 No clear benefit with cesarean after onset of labor or membranes have been ruptured Cesarean increases morbidity and possible mortality to mother Give antibiotic prophylaxis for cesarean in HIVinfected women Complications of similar to HIV uninfected women Patient’s decision should be respected and honored
 Delivery Clinical Situation A u - HIV+ woman presenting late in pregnancy (after 36 weeks), not receiving ART, VL and CD 4 count pending, unlikely to be available before delivery n n n Discuss options for therapy Start ART, including at least 076 ZDV regimen Counsel about scheduled cesarean delivery If cesarean chosen, schedule for 38 weeks; start IV ZDV 3 hours before surgery Infant should receive 6 weeks ZDV after birth Discuss options for continuing/starting combination therapy as soon as HIV viral load and CD 4 count available
Delivery Clinical Situation A u - HIV+ woman presenting late in pregnancy (after 36 weeks), not receiving ART, VL and CD 4 count pending, unlikely to be available before delivery n n n Discuss options for therapy Start ART, including at least 076 ZDV regimen Counsel about scheduled cesarean delivery If cesarean chosen, schedule for 38 weeks; start IV ZDV 3 hours before surgery Infant should receive 6 weeks ZDV after birth Discuss options for continuing/starting combination therapy as soon as HIV viral load and CD 4 count available
 Delivery Clinical Situation B u HIV+ women who began prenatal care early in 3 rd trimester, are receiving and responding to ART, but still have VL > 1000 at 36 weeks gestation n Continue ART because VL is decreasing n Inform woman u VL level falling but unlikely to be <1000 before delivery u Scheduled cesarean may reduce risk of intrapartum transmission u Increased risks of cesarean delivery n If chosen, schedule cesarean for 38 weeks; start IV ZDV 3 hours before surgery; continue other ART n Infant should receive 6 weeks ZDV after birth n Stress importance of adherence to therapy after delivery
Delivery Clinical Situation B u HIV+ women who began prenatal care early in 3 rd trimester, are receiving and responding to ART, but still have VL > 1000 at 36 weeks gestation n Continue ART because VL is decreasing n Inform woman u VL level falling but unlikely to be <1000 before delivery u Scheduled cesarean may reduce risk of intrapartum transmission u Increased risks of cesarean delivery n If chosen, schedule cesarean for 38 weeks; start IV ZDV 3 hours before surgery; continue other ART n Infant should receive 6 weeks ZDV after birth n Stress importance of adherence to therapy after delivery
 Delivery Clinical Situation C - u HIV+ women receiving ART with undetectable VL at 36 weeks gestation n n Inform woman that her risk of perinatal transmission is low (approximately 2% or less), even with vaginal delivery Current information suggests cesarean will not lower her risk further Cesarean delivery has increased risks of complication compared to vaginal delivery Risks should be balanced against uncertain benefit of cesarean in this case Infant should receive 6 weeks ZDV after birth
Delivery Clinical Situation C - u HIV+ women receiving ART with undetectable VL at 36 weeks gestation n n Inform woman that her risk of perinatal transmission is low (approximately 2% or less), even with vaginal delivery Current information suggests cesarean will not lower her risk further Cesarean delivery has increased risks of complication compared to vaginal delivery Risks should be balanced against uncertain benefit of cesarean in this case Infant should receive 6 weeks ZDV after birth
 Delivery Clinical Situation D u - HIV+ women who have elected scheduled cesarean delivery but present in early labor or shortly after rupture of membranes n n n n IV ZDV should be started immediately If cervical dilatation is minimal and a long period of labor is anticipated administer loading dose of ZDV and proceed expeditiously with cesarean Alternatively, consider oxytocin augmentation to expedite vaginal delivery If labor is progressing rapidly—allow for vaginal delivery If allowed to labor, avoid invasive monitoring, and operative delivery Continue oral ART during labor Infant should receive 6 weeks ZDV after birth
Delivery Clinical Situation D u - HIV+ women who have elected scheduled cesarean delivery but present in early labor or shortly after rupture of membranes n n n n IV ZDV should be started immediately If cervical dilatation is minimal and a long period of labor is anticipated administer loading dose of ZDV and proceed expeditiously with cesarean Alternatively, consider oxytocin augmentation to expedite vaginal delivery If labor is progressing rapidly—allow for vaginal delivery If allowed to labor, avoid invasive monitoring, and operative delivery Continue oral ART during labor Infant should receive 6 weeks ZDV after birth
 Obstetric Procedures - u Because of increased fetal exposure to infected maternal blood and secretions, increased risk of transmission may come from: Amniotomy n Fetal scalp electrode/sampling n Forceps/vacuum extractor n Episiotomy n Vaginal tears n
Obstetric Procedures - u Because of increased fetal exposure to infected maternal blood and secretions, increased risk of transmission may come from: Amniotomy n Fetal scalp electrode/sampling n Forceps/vacuum extractor n Episiotomy n Vaginal tears n
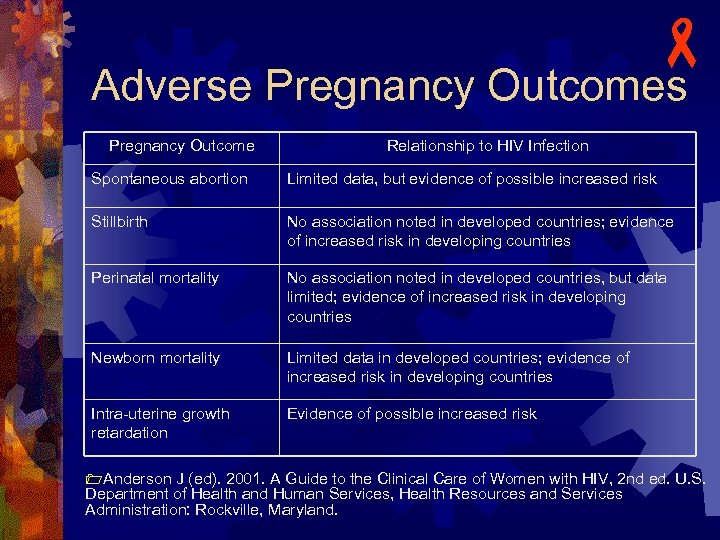 - Adverse Pregnancy Outcomes Pregnancy Outcome Relationship to HIV Infection Spontaneous abortion Limited data, but evidence of possible increased risk Stillbirth No association noted in developed countries; evidence of increased risk in developing countries Perinatal mortality No association noted in developed countries, but data limited; evidence of increased risk in developing countries Newborn mortality Limited data in developed countries; evidence of increased risk in developing countries Intra-uterine growth retardation Evidence of possible increased risk 1 Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland.
- Adverse Pregnancy Outcomes Pregnancy Outcome Relationship to HIV Infection Spontaneous abortion Limited data, but evidence of possible increased risk Stillbirth No association noted in developed countries; evidence of increased risk in developing countries Perinatal mortality No association noted in developed countries, but data limited; evidence of increased risk in developing countries Newborn mortality Limited data in developed countries; evidence of increased risk in developing countries Intra-uterine growth retardation Evidence of possible increased risk 1 Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland.
 - Adverse Pregnancy Outcomes Pregnancy Outcome Relationship to HIV Infection Low birth weight Evidence of possible increased risk Preterm delivery Evidence of possible increased risk, especially w/ more advanced disease Pre-eclampsia No data Gestational diabetes No data Amnionitis Limited data; more recent studies do not suggest an increased risk; some earlier studies found increased histologic placental inflammation, particularly in those with preterm deliveries Oligohydramnios Minimal data Fetal malformation No evidence of increased risk 1 Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland.
- Adverse Pregnancy Outcomes Pregnancy Outcome Relationship to HIV Infection Low birth weight Evidence of possible increased risk Preterm delivery Evidence of possible increased risk, especially w/ more advanced disease Pre-eclampsia No data Gestational diabetes No data Amnionitis Limited data; more recent studies do not suggest an increased risk; some earlier studies found increased histologic placental inflammation, particularly in those with preterm deliveries Oligohydramnios Minimal data Fetal malformation No evidence of increased risk 1 Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland.
 - Breastfeeding and HIV Infection u Women with HIV infection in the U. S. should not breastfeed u Women considering breastfeeding should know their HIV status
- Breastfeeding and HIV Infection u Women with HIV infection in the U. S. should not breastfeed u Women considering breastfeeding should know their HIV status
 Neonates u u u Wash newborn after birth, especially face Avoid hypothermia ZDV (AZT) prophylaxis for 6 weeks n n u u Hemoglobin at baseline and 6 wks Adherence Referral to an HIV specialist HIV diagnostic testing to establish or rule out HIV infection as early as possible n u u u - Negative virologic tests during first 6 wks should be repeated after completion of ZDV PCP prophylaxis initiated at 6 weeks of age Long-term follow-up of HIV- and ART-exposed infants Support services for the family
Neonates u u u Wash newborn after birth, especially face Avoid hypothermia ZDV (AZT) prophylaxis for 6 weeks n n u u Hemoglobin at baseline and 6 wks Adherence Referral to an HIV specialist HIV diagnostic testing to establish or rule out HIV infection as early as possible n u u u - Negative virologic tests during first 6 wks should be repeated after completion of ZDV PCP prophylaxis initiated at 6 weeks of age Long-term follow-up of HIV- and ART-exposed infants Support services for the family
 Summary - u HIV testing in pregnancy should be universal u Mother-to-child-transmission of HIV can be reduced to < 2% with appropriate care n n Antiretroviral therapy including zidovudine Obstetric interventions Avoid amniotomy u Avoid procedures: forceps/vacuum extractor, scalp electrode, scalp blood sampling u Restrict episiotomy u Elective cesarean section in certain cases u n n Neonate prophylaxis Avoid breastfeeding
Summary - u HIV testing in pregnancy should be universal u Mother-to-child-transmission of HIV can be reduced to < 2% with appropriate care n n Antiretroviral therapy including zidovudine Obstetric interventions Avoid amniotomy u Avoid procedures: forceps/vacuum extractor, scalp electrode, scalp blood sampling u Restrict episiotomy u Elective cesarean section in certain cases u n n Neonate prophylaxis Avoid breastfeeding
 HIV Services for Pregnant Women n n n Counseling and confidential testing Comprehensive medical care Case management Adherence counseling Mental health Support groups Clinical trials
HIV Services for Pregnant Women n n n Counseling and confidential testing Comprehensive medical care Case management Adherence counseling Mental health Support groups Clinical trials
 Resources - http: //www. aidsinfo. nih. gov/guidelines Guidelines for the Use of Antiretroviral Agents in HIV-Infected Adults and Adolescents Updated October 6, 2005 Public Health Service Task Force Recommendations for Use of Antiretroviral Drugs in Pregnant HIV-1 -Infected Women for Maternal Health and Interventions to Reduce Perinatal HIV 1 Transmission in the United States Updated November 17, 2005
Resources - http: //www. aidsinfo. nih. gov/guidelines Guidelines for the Use of Antiretroviral Agents in HIV-Infected Adults and Adolescents Updated October 6, 2005 Public Health Service Task Force Recommendations for Use of Antiretroviral Drugs in Pregnant HIV-1 -Infected Women for Maternal Health and Interventions to Reduce Perinatal HIV 1 Transmission in the United States Updated November 17, 2005
 -
-
![Resources - www. aidsetc. org Perinatal Antiretroviral Guidelines Slide Set [PPT] Date: 11/2005 Source: Resources - www. aidsetc. org Perinatal Antiretroviral Guidelines Slide Set [PPT] Date: 11/2005 Source:](https://present5.com/presentation/224f8b85fcc736e680007676b2022773/image-89.jpg) Resources - www. aidsetc. org Perinatal Antiretroviral Guidelines Slide Set [PPT] Date: 11/2005 Source: National Resource Center Note: 68 slides, includes 6 case studies and speaker notes
Resources - www. aidsetc. org Perinatal Antiretroviral Guidelines Slide Set [PPT] Date: 11/2005 Source: National Resource Center Note: 68 slides, includes 6 case studies and speaker notes
 -
-
 -
-
 References 1 1 1 - Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland. Coutsoudis A et al. 1999. Influence of infant-feeding patterns on early mother-to-child transmission of HIV-1 in Durban, South Africa: A prospective cohort study. Lancet 354: 471– 476. De. Cock K et al. 2000. Prevention of mother-to-child transmission in resource-poor countries: Translating research into policy and practice. J Am Med Assoc 283(9): 1175– 1182. Dunn D et al. 1992. Risk of HIV-1 transmission through breastfeeding. Lancet 340(8819): 585– 588. Gray G. 2000. The PETRA study: Early and late efficacy of three short ZDV/3 TC combinations regimens to prevent mother-to-child transmission of HIV-1. XIII International AIDS Conference, Durban, South Africa. Comparison of two strategies for administering nevirapine to prevent perinatal HIV transmission in high-prevalence, resource-poor settings Stringer JS, Sinkala M, Stout JP, Goldenberg RL, Acosta EP, Chapman V, Kumwenda-Phiri R, Vermund SH. J Acquir Immune Defic Syndr. 2003 Apr 15; 32(5): 506 -13.
References 1 1 1 - Anderson J (ed). 2001. A Guide to the Clinical Care of Women with HIV, 2 nd ed. U. S. Department of Health and Human Services, Health Resources and Services Administration: Rockville, Maryland. Coutsoudis A et al. 1999. Influence of infant-feeding patterns on early mother-to-child transmission of HIV-1 in Durban, South Africa: A prospective cohort study. Lancet 354: 471– 476. De. Cock K et al. 2000. Prevention of mother-to-child transmission in resource-poor countries: Translating research into policy and practice. J Am Med Assoc 283(9): 1175– 1182. Dunn D et al. 1992. Risk of HIV-1 transmission through breastfeeding. Lancet 340(8819): 585– 588. Gray G. 2000. The PETRA study: Early and late efficacy of three short ZDV/3 TC combinations regimens to prevent mother-to-child transmission of HIV-1. XIII International AIDS Conference, Durban, South Africa. Comparison of two strategies for administering nevirapine to prevent perinatal HIV transmission in high-prevalence, resource-poor settings Stringer JS, Sinkala M, Stout JP, Goldenberg RL, Acosta EP, Chapman V, Kumwenda-Phiri R, Vermund SH. J Acquir Immune Defic Syndr. 2003 Apr 15; 32(5): 506 -13.
 1 1 1 1 International Perinatal HIV Group. 1999. The mode of delivery and the risk of vertical transmission of human immunodeficiency virus type 1. N Engl J Med 340(14): 977– 987. Mandelbrot L et al. 1996. Obstetric factors and mother-to-child transmission of human immunodeficiency virus type 1: The French perinatal cohorts. Amer J Obstet Gynecol 175(3 pt 1): 661– 667. Semprini AE et al. 1995. The incidence of complications after cesarean section in 156 women. AIDS 9: 913– 917. Shaffer N et al. 1999. Short-course ZDV for perinatal HIV-1 transmission in Bangkok, Thailand: A randomized controlled trial. Lancet 353: 773– 780. Sperling RS et al. 1996. Maternal viral load, ZDV treatment, and the risk of transmission of HIV type 1 from mother to infant. N Engl J Med 335(22): 1621– 1629. UNICEF/UNAIDS/WHO Technical Consultation on HIV and Infant Feeding. 1998. HIV and Infant Feeding: Implementation of Guidelines. WHO: Geneva. World Health Organization (WHO)/Joint United Nations Programme on HIV/AIDS (UNAIDS). 1999. HIV In Pregnancy: A Review. WHO/UNAIDS: Geneva.
1 1 1 1 International Perinatal HIV Group. 1999. The mode of delivery and the risk of vertical transmission of human immunodeficiency virus type 1. N Engl J Med 340(14): 977– 987. Mandelbrot L et al. 1996. Obstetric factors and mother-to-child transmission of human immunodeficiency virus type 1: The French perinatal cohorts. Amer J Obstet Gynecol 175(3 pt 1): 661– 667. Semprini AE et al. 1995. The incidence of complications after cesarean section in 156 women. AIDS 9: 913– 917. Shaffer N et al. 1999. Short-course ZDV for perinatal HIV-1 transmission in Bangkok, Thailand: A randomized controlled trial. Lancet 353: 773– 780. Sperling RS et al. 1996. Maternal viral load, ZDV treatment, and the risk of transmission of HIV type 1 from mother to infant. N Engl J Med 335(22): 1621– 1629. UNICEF/UNAIDS/WHO Technical Consultation on HIV and Infant Feeding. 1998. HIV and Infant Feeding: Implementation of Guidelines. WHO: Geneva. World Health Organization (WHO)/Joint United Nations Programme on HIV/AIDS (UNAIDS). 1999. HIV In Pregnancy: A Review. WHO/UNAIDS: Geneva.
 1 1 1 HIV and infant feeding: issues in developed and developing countries Jackson DJ, Chopra M, Witten C, Sengwana MJ. J Obstet Gynecol Neonatal Nurs 2003 Jan-Feb; 32(1): 117 -27. Nevirapine resistance after single dose prophylaxis Eshleman SH, Jackson JB. AIDS Rev 2002 Apr-Jun; 4(2): 59 -63. HIV Infection in Women: Selected Issues in Pregnancy Currier JS. Topics in HIV Medicine, International AIDS Society-USA May 2002. [PDF, 45 K] Antiretrovirals for reducing the risk of mother-to-child transmission of HIV infection Brocklehurst P, Volmink J Cochrane Database Syst Rev 2002: CD 003510. Effect of breastfeeding on mortality among HIV-1 infected women: a randomised trial Nduati R, Richardson BA, John G, Mbori-Ngacha D, Mwatha A, Ndinya. Achola J, Bwayo J, Onyango FE, Kreiss J. Lancet 2001 May 26; 357(9269): 1651 -55. Free registration required.
1 1 1 HIV and infant feeding: issues in developed and developing countries Jackson DJ, Chopra M, Witten C, Sengwana MJ. J Obstet Gynecol Neonatal Nurs 2003 Jan-Feb; 32(1): 117 -27. Nevirapine resistance after single dose prophylaxis Eshleman SH, Jackson JB. AIDS Rev 2002 Apr-Jun; 4(2): 59 -63. HIV Infection in Women: Selected Issues in Pregnancy Currier JS. Topics in HIV Medicine, International AIDS Society-USA May 2002. [PDF, 45 K] Antiretrovirals for reducing the risk of mother-to-child transmission of HIV infection Brocklehurst P, Volmink J Cochrane Database Syst Rev 2002: CD 003510. Effect of breastfeeding on mortality among HIV-1 infected women: a randomised trial Nduati R, Richardson BA, John G, Mbori-Ngacha D, Mwatha A, Ndinya. Achola J, Bwayo J, Onyango FE, Kreiss J. Lancet 2001 May 26; 357(9269): 1651 -55. Free registration required.
 Breastmilk RNA viral load in HIV-infected South African women: effects of subclinical mastitis and infant feeding Willumsen JF, Filteau SM, Coutsoudis A, Newell ML, Rollins NC, Coovadia HM, Tomkins AM. AIDS 2003 Feb 14; 17(3): 407 -14. 1 Timing of breast milk HIV-1 transmission: a meta-analysis John GC, Richardson BA, Nduati RW, Mbori-Ngacha D, Kreiss JK. East Afr Med J 2001 Feb; 78(2): 75 -9. 1 Mastitis and transmission of human immunodeficiency virus through breast milk Semba RD. Ann N Y Acad Sci 2000 Nov; 918: 156 -62. Reproduced with permission. 1 Vaginal lavage with chlorhexidine during labour to reduce mother-to-child HIV transmission: clinical trial in Mombasa, Kenya Gaillard P, Mwanyumba F, Verhofstede C, Claeys P, Chohan V, Goetghebeur E, Mandaliya K, Ndinya-Achola J, Temmerman M. AIDS 2001 Feb 16; 15(3): 389 -96. 1
Breastmilk RNA viral load in HIV-infected South African women: effects of subclinical mastitis and infant feeding Willumsen JF, Filteau SM, Coutsoudis A, Newell ML, Rollins NC, Coovadia HM, Tomkins AM. AIDS 2003 Feb 14; 17(3): 407 -14. 1 Timing of breast milk HIV-1 transmission: a meta-analysis John GC, Richardson BA, Nduati RW, Mbori-Ngacha D, Kreiss JK. East Afr Med J 2001 Feb; 78(2): 75 -9. 1 Mastitis and transmission of human immunodeficiency virus through breast milk Semba RD. Ann N Y Acad Sci 2000 Nov; 918: 156 -62. Reproduced with permission. 1 Vaginal lavage with chlorhexidine during labour to reduce mother-to-child HIV transmission: clinical trial in Mombasa, Kenya Gaillard P, Mwanyumba F, Verhofstede C, Claeys P, Chohan V, Goetghebeur E, Mandaliya K, Ndinya-Achola J, Temmerman M. AIDS 2001 Feb 16; 15(3): 389 -96. 1


