3208655b24338ca52c823c061fd36e85.ppt
- Количество слайдов: 73
 Highest Quality Care for the Hospitalized Elderly Quality Improvement in the Hospital Jason Stein, MD Emory Reynolds Faculty Scholar Emory Hospital Medicine Service
Highest Quality Care for the Hospitalized Elderly Quality Improvement in the Hospital Jason Stein, MD Emory Reynolds Faculty Scholar Emory Hospital Medicine Service
 Quality Improvement in the Hospital: Goals for this Primer § Understand fundamental concepts in quality improvement § Identify the environment and key steps for a successful quality improvement project § Become familiar with several quality improvement tools and their use Emory Reynolds Program Emory Hospital Medicine Service
Quality Improvement in the Hospital: Goals for this Primer § Understand fundamental concepts in quality improvement § Identify the environment and key steps for a successful quality improvement project § Become familiar with several quality improvement tools and their use Emory Reynolds Program Emory Hospital Medicine Service
 Highest Quality Hospital Care § Processes § Outcomes What do you care more about?
Highest Quality Hospital Care § Processes § Outcomes What do you care more about?
 Highest Quality Hospital Care Optimal Process: identify correctable problem Optimal Outcome: correctable problem identify preventable problem
Highest Quality Hospital Care Optimal Process: identify correctable problem Optimal Outcome: correctable problem identify preventable problem
 Highest Quality Hospital Care Processes vs Physicians Is one more effective?
Highest Quality Hospital Care Processes vs Physicians Is one more effective?
 Highest Quality Hospital Care Processes vs Physicians Is one more reliable?
Highest Quality Hospital Care Processes vs Physicians Is one more reliable?
 Highest Quality Hospital Care Processes vs Physicians If your hospital lacks a specific process to drive a specific outcome, do individual physicians fill the gap?
Highest Quality Hospital Care Processes vs Physicians If your hospital lacks a specific process to drive a specific outcome, do individual physicians fill the gap?
 Progress Quality Improvement: Bridging the Implementation Gap How good is American healthcare? Patient care Time
Progress Quality Improvement: Bridging the Implementation Gap How good is American healthcare? Patient care Time
 Progress Quality Improvement: Bridging the Implementation Gap We get it right 54% of the time. -Brent James, MD, MStat Executive Director, Intermountain Health Care Patient care Time
Progress Quality Improvement: Bridging the Implementation Gap We get it right 54% of the time. -Brent James, MD, MStat Executive Director, Intermountain Health Care Patient care Time
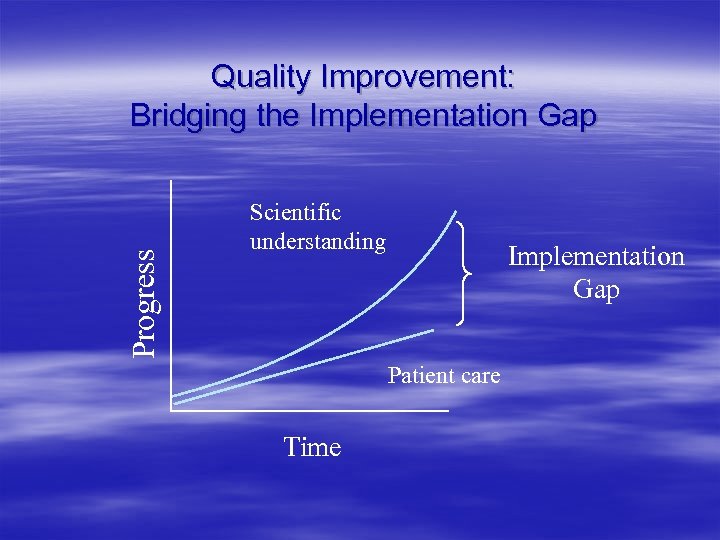 Progress Quality Improvement: Bridging the Implementation Gap Scientific understanding Implementation Gap Patient care Time
Progress Quality Improvement: Bridging the Implementation Gap Scientific understanding Implementation Gap Patient care Time
 Hospitalists and Quality Improvement § Complex process problems need multidisciplinary solutions § We are at the frontlines seeing system failures, process errors, and performance gaps with our own eyes -- which is our competitive advantage § Improved quality delivers: – – – better patient care… at lower costs… with potentially higher reimbursements (pay-forperformance)… And it can make our jobs more interesting, fun, and rewarding.
Hospitalists and Quality Improvement § Complex process problems need multidisciplinary solutions § We are at the frontlines seeing system failures, process errors, and performance gaps with our own eyes -- which is our competitive advantage § Improved quality delivers: – – – better patient care… at lower costs… with potentially higher reimbursements (pay-forperformance)… And it can make our jobs more interesting, fun, and rewarding.
 Section I: Quality Improvement and Change in the Hospital Atmosphere
Section I: Quality Improvement and Change in the Hospital Atmosphere
 Definition of Quality § Meeting the needs and exceeding the expectations of those we serve § Delivering all and only the care that the patient and family needs
Definition of Quality § Meeting the needs and exceeding the expectations of those we serve § Delivering all and only the care that the patient and family needs
 “Definition” of Improvement § § § It is NOT… yelling at people to work harder, faster, or safer creating order sets or protocols and then failing to monitor their use or effect § traditional Quality Assurance § research (but they can co-exist nicely)
“Definition” of Improvement § § § It is NOT… yelling at people to work harder, faster, or safer creating order sets or protocols and then failing to monitor their use or effect § traditional Quality Assurance § research (but they can co-exist nicely)
 Principle #1: Improvement Requires Change Every system is perfectly designed to achieve exactly the results it gets To improve the system, change the system…
Principle #1: Improvement Requires Change Every system is perfectly designed to achieve exactly the results it gets To improve the system, change the system…
 Principle #2: Less is More You cannot destroy productivity When changing the system, keep it simple
Principle #2: Less is More You cannot destroy productivity When changing the system, keep it simple
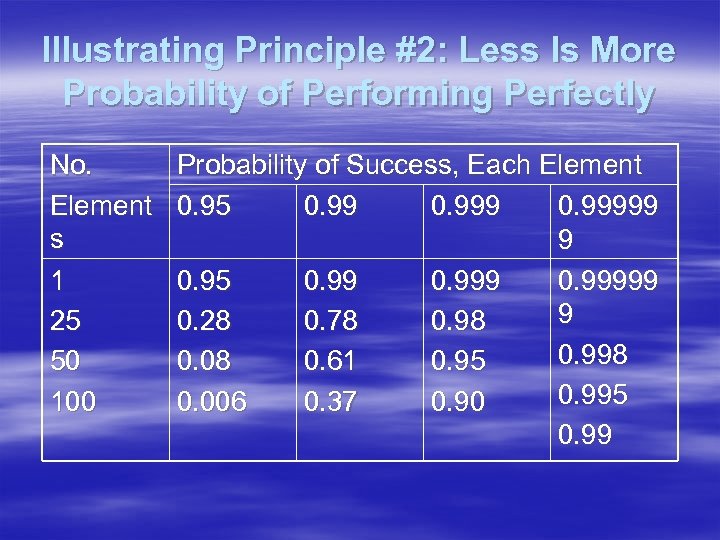 Illustrating Principle #2: Less Is More Probability of Performing Perfectly No. Element s 1 25 50 100 Probability of Success, Each Element 0. 95 0. 999 0. 99999 9 0. 28 0. 78 0. 998 0. 08 0. 61 0. 95 0. 995 0. 006 0. 37 0. 90 0. 99
Illustrating Principle #2: Less Is More Probability of Performing Perfectly No. Element s 1 25 50 100 Probability of Success, Each Element 0. 95 0. 999 0. 99999 9 0. 28 0. 78 0. 998 0. 08 0. 61 0. 95 0. 995 0. 006 0. 37 0. 90 0. 99
 Understanding Change in the Hospital Atmosphere § Change = not just doing something different, but engineering something different § at least one step in at least one process § Hospital Atmosphere = hospitals tend to be viscous, complex systems with default levels of performance § change engineered to improve performance can be a foreign concept or even overtly resisted
Understanding Change in the Hospital Atmosphere § Change = not just doing something different, but engineering something different § at least one step in at least one process § Hospital Atmosphere = hospitals tend to be viscous, complex systems with default levels of performance § change engineered to improve performance can be a foreign concept or even overtly resisted
 Understanding Change in the Hospital Atmosphere A Common Strategy Which Commonly Fails: § Experts design a comprehensive protocol using EBM over several months § Protocol is presented as a finished, stand alone product § Customization of protocol is discouraged § Compliance depends on vigilance and hard work § Monitoring for success or failure is the exception to the rule (with failures coming to light after patients are harmed) § Flawed implementation leads to repetitive efforts down the road
Understanding Change in the Hospital Atmosphere A Common Strategy Which Commonly Fails: § Experts design a comprehensive protocol using EBM over several months § Protocol is presented as a finished, stand alone product § Customization of protocol is discouraged § Compliance depends on vigilance and hard work § Monitoring for success or failure is the exception to the rule (with failures coming to light after patients are harmed) § Flawed implementation leads to repetitive efforts down the road
 Understanding Change in the Hospital Atmosphere High-Reliability Strategies Commonly Succeed: § Build a “decision aide” or reminder into the system § Make the desired action the default action (not doing the desired action requires opting out) § Build redundancy into responsibilities (e. g. if one person in the chain overlooks it, someone else will catch it) § Schedule steps to occur at known intervals or events § Standardize a process so that deviation feels weird § Take advantage of work habits or reliable patterns of behavior Build at least one - if not more - of these high-reliability strategies into any changed process.
Understanding Change in the Hospital Atmosphere High-Reliability Strategies Commonly Succeed: § Build a “decision aide” or reminder into the system § Make the desired action the default action (not doing the desired action requires opting out) § Build redundancy into responsibilities (e. g. if one person in the chain overlooks it, someone else will catch it) § Schedule steps to occur at known intervals or events § Standardize a process so that deviation feels weird § Take advantage of work habits or reliable patterns of behavior Build at least one - if not more - of these high-reliability strategies into any changed process.
 Understanding Change in the Hospital Atmosphere Change engineered to drive improvement depends on… § Workplace Culture: personnel must be receptive to change § Awareness: administrative and medical staffs must care about performance and support its improvement through change § Evidence: local experts must identify which research to translate into practice § Experience: a skilled team must choose, implement, and follow up changes to ensure: 1) improvement efforts are ongoing and yielding better performance 2) productivity is preserved
Understanding Change in the Hospital Atmosphere Change engineered to drive improvement depends on… § Workplace Culture: personnel must be receptive to change § Awareness: administrative and medical staffs must care about performance and support its improvement through change § Evidence: local experts must identify which research to translate into practice § Experience: a skilled team must choose, implement, and follow up changes to ensure: 1) improvement efforts are ongoing and yielding better performance 2) productivity is preserved
 An Atmosphere for Change AWARENESS EXPERIENCE OF THE LOCAL PERFORMANCE GAP WITH SIMILAR IMPROVEMENT EFFORTS Patient Medical Staff Administrative Support Hospitalist Quality Officer Multidisciplinary Team Members Success Stories From Other Institutions EVIDENCE WORKPLACE CULTURE TO TRANSLATE INTO PRACTICE READY TO ACCEPT CHANGE “Bedside” Teaching Didactic Teaching Sessions Local Expertise in Disease Literature Task Load Culture of Improvement Culture of Negative Expectations
An Atmosphere for Change AWARENESS EXPERIENCE OF THE LOCAL PERFORMANCE GAP WITH SIMILAR IMPROVEMENT EFFORTS Patient Medical Staff Administrative Support Hospitalist Quality Officer Multidisciplinary Team Members Success Stories From Other Institutions EVIDENCE WORKPLACE CULTURE TO TRANSLATE INTO PRACTICE READY TO ACCEPT CHANGE “Bedside” Teaching Didactic Teaching Sessions Local Expertise in Disease Literature Task Load Culture of Improvement Culture of Negative Expectations
 An Atmosphere for Change Patient AWARENESS OF THE LOCAL PERFORMANCE GAP Patient Medical Staff Hospital Administration At mercy and increasingly aware of underperforming status quo Now can access a new resource promoting transparency in hospital performance: www. hospitalcompare. hhs. gov Hospital Administration Medical Staff Understands status quo is unacceptable (IOM, Leapfrog, NQF, JCAHO) Sees fiscal health tied to performance against national benchmarks, ability to reduce costs & LOS, improve margins, and competitive reputation in the community Has professional responsibility to improve Knows all too well where system fails Recognizes that professional livelihood will depend on paying attention to outcomes: Pay-for-Performance
An Atmosphere for Change Patient AWARENESS OF THE LOCAL PERFORMANCE GAP Patient Medical Staff Hospital Administration At mercy and increasingly aware of underperforming status quo Now can access a new resource promoting transparency in hospital performance: www. hospitalcompare. hhs. gov Hospital Administration Medical Staff Understands status quo is unacceptable (IOM, Leapfrog, NQF, JCAHO) Sees fiscal health tied to performance against national benchmarks, ability to reduce costs & LOS, improve margins, and competitive reputation in the community Has professional responsibility to improve Knows all too well where system fails Recognizes that professional livelihood will depend on paying attention to outcomes: Pay-for-Performance
 An Atmosphere for Change Hospitalist Team Facilitator Technical expert on Quality Improvement theory and tools Owns the team process, enforces ground rules, helps judge feasibility Teaches the team while doing EXPERIENCE WITH SIMILAR IMPROVEMENT EFFORTS Hospitalist Team Facilitator Multidisciplinary Team Members Successful Strategies of Others Multidisciplinary Team Members Learn from mistakes of others Adapt successes of others (tools and methods): steal shamelessly Get specific advice in ’Ask the Expert’ forums or other consortiums that collect and share experience Chosen for hands-on, fundamental knowledge of key processes Inclusive, open, & consensus seeking Impact not only the change(s) but the implementation
An Atmosphere for Change Hospitalist Team Facilitator Technical expert on Quality Improvement theory and tools Owns the team process, enforces ground rules, helps judge feasibility Teaches the team while doing EXPERIENCE WITH SIMILAR IMPROVEMENT EFFORTS Hospitalist Team Facilitator Multidisciplinary Team Members Successful Strategies of Others Multidisciplinary Team Members Learn from mistakes of others Adapt successes of others (tools and methods): steal shamelessly Get specific advice in ’Ask the Expert’ forums or other consortiums that collect and share experience Chosen for hands-on, fundamental knowledge of key processes Inclusive, open, & consensus seeking Impact not only the change(s) but the implementation
 An residents or students Atmosphere for Change To an audience of “Bedside” Teaching To build cadre of “experts” (and to help meet ACGME requirements) Download teaching pearls from SHM resource rooms EVIDENCE TO TRANSLATE INTO PRACTICE “Bedside” Teaching Didactic Teaching Sessions Local Expertise in Disease Literature Didactic Teaching Sessions To an audience of peers, administrators, nurses, or support staff To boost awareness, knowledge, enthusiasm, and support Download slide sets from SHM resource rooms Local Expertise in Disease Literature Decide what changes to make based on the level of evidence Establishes team’s credibility Extends team’s authority when local sub-specialists or experts participate in selecting and implementing change
An residents or students Atmosphere for Change To an audience of “Bedside” Teaching To build cadre of “experts” (and to help meet ACGME requirements) Download teaching pearls from SHM resource rooms EVIDENCE TO TRANSLATE INTO PRACTICE “Bedside” Teaching Didactic Teaching Sessions Local Expertise in Disease Literature Didactic Teaching Sessions To an audience of peers, administrators, nurses, or support staff To boost awareness, knowledge, enthusiasm, and support Download slide sets from SHM resource rooms Local Expertise in Disease Literature Decide what changes to make based on the level of evidence Establishes team’s credibility Extends team’s authority when local sub-specialists or experts participate in selecting and implementing change
 An Atmosphere for Change Task Load Be sensitive about piling new tasks onto over-tasked personnel Use the input of personnel who will be responsibile for implementing Make it easy and desirable to do the right thing Culture of Improvement Extend it, one person and one project at a time Advertise successes Use or adapt this online ‘cultural survey: ’ http: //www. patientsafetygroup. org/program/step 1 c. cfm Culture of Negative Expectations Overcome it, one person and one project at a time Attach pride to balance between performance successes and failures Consider using a ‘cultural survey’ to identify problems and address them through proper channels WORKPLACE CULTURE READY TO ACCEPT CHANGE Task Load Culture of Improvement vs. Culture of Negative Expectations
An Atmosphere for Change Task Load Be sensitive about piling new tasks onto over-tasked personnel Use the input of personnel who will be responsibile for implementing Make it easy and desirable to do the right thing Culture of Improvement Extend it, one person and one project at a time Advertise successes Use or adapt this online ‘cultural survey: ’ http: //www. patientsafetygroup. org/program/step 1 c. cfm Culture of Negative Expectations Overcome it, one person and one project at a time Attach pride to balance between performance successes and failures Consider using a ‘cultural survey’ to identify problems and address them through proper channels WORKPLACE CULTURE READY TO ACCEPT CHANGE Task Load Culture of Improvement vs. Culture of Negative Expectations
 Section II: The Multidisciplinary Team Defining an Approach to Change
Section II: The Multidisciplinary Team Defining an Approach to Change
 The Driving Force for Change THE MULTIDISCIPLINARY TEAM Leverages frontline expertise and experience. Impacts not only the change/interventions, but also the implementation
The Driving Force for Change THE MULTIDISCIPLINARY TEAM Leverages frontline expertise and experience. Impacts not only the change/interventions, but also the implementation
 The Driving Force for Change: The Multidisciplinary Team A team is not the same as a committee… Committee § individuals bring representation § productive capacity = single most able member Team § individuals bring fundamental knowledge § productive capacity = synergistic (more than the sum of all individual team members together)
The Driving Force for Change: The Multidisciplinary Team A team is not the same as a committee… Committee § individuals bring representation § productive capacity = single most able member Team § individuals bring fundamental knowledge § productive capacity = synergistic (more than the sum of all individual team members together)
 The Driving Force for Change: The Multidisciplinary Team Features of a good team… § Safe (no ad hominem attacks) § Inclusive (values all potential contributors including diverse views; not a clique) § Open (considers all ideas fairly) § Consensus seeking
The Driving Force for Change: The Multidisciplinary Team Features of a good team… § Safe (no ad hominem attacks) § Inclusive (values all potential contributors including diverse views; not a clique) § Open (considers all ideas fairly) § Consensus seeking
 The Driving Force for Change: The Multidisciplinary Team Consensus… § definition: finding a solution acceptable enough that all members can support it; no member opposes it § It is not: – A unanimous vote (consensus may not represent everyone’s first priorities) – A majority vote (in a majority vote, only the majority gets something they are happy with; people in the minority may get something they don’t want at all, which is not what consensus is all about) – Everyone totally satisfied
The Driving Force for Change: The Multidisciplinary Team Consensus… § definition: finding a solution acceptable enough that all members can support it; no member opposes it § It is not: – A unanimous vote (consensus may not represent everyone’s first priorities) – A majority vote (in a majority vote, only the majority gets something they are happy with; people in the minority may get something they don’t want at all, which is not what consensus is all about) – Everyone totally satisfied
 The Driving Force for Change: The Multidisciplinary Team Three types of team members… 1) Team Leader 2) Team Facilitator 3) Process Owners (members with operational, hands-on fundamental knowledge of the process)
The Driving Force for Change: The Multidisciplinary Team Three types of team members… 1) Team Leader 2) Team Facilitator 3) Process Owners (members with operational, hands-on fundamental knowledge of the process)
 The Driving Force for Change: The Multidisciplinary Team Leader… § § § schedules and chairs team meetings sets the agenda (printed at each meeting) records team activities (working documents in binder) § reports to management (Steering Team) § often a member of Steering Team
The Driving Force for Change: The Multidisciplinary Team Leader… § § § schedules and chairs team meetings sets the agenda (printed at each meeting) records team activities (working documents in binder) § reports to management (Steering Team) § often a member of Steering Team
 The Driving Force for Change: The Multidisciplinary Team Facilitator… § § owns the team process (enforces ground rules) technical expert on QI theory and tools assists Team Leader teaches while doing, within team
The Driving Force for Change: The Multidisciplinary Team Facilitator… § § owns the team process (enforces ground rules) technical expert on QI theory and tools assists Team Leader teaches while doing, within team
 The Driving Force for Change: The Multidisciplinary Team Process Owners… § § § chosen for fundamental knowledge will help implement should become leaders (so choose wisely)
The Driving Force for Change: The Multidisciplinary Team Process Owners… § § § chosen for fundamental knowledge will help implement should become leaders (so choose wisely)
 The Driving Force for Change: The Multidisciplinary Team Ground Rules… § All team members and opinions are equal § Team members will speak freely and in turn – We will listen attentively to others – Each must be heard – No one may dominate § Problems will be discussed, analyzed, or attacked (not people) § All agreements are kept unless renegotiated § Once we agree, we will speak with "One Voice" (especially after leaving the meeting) § Honesty before cohesiveness § Consensus vs. democracy: each gets his say, not his way § Silence equals agreement § Members will attend regularly § Meetings will start and end on time
The Driving Force for Change: The Multidisciplinary Team Ground Rules… § All team members and opinions are equal § Team members will speak freely and in turn – We will listen attentively to others – Each must be heard – No one may dominate § Problems will be discussed, analyzed, or attacked (not people) § All agreements are kept unless renegotiated § Once we agree, we will speak with "One Voice" (especially after leaving the meeting) § Honesty before cohesiveness § Consensus vs. democracy: each gets his say, not his way § Silence equals agreement § Members will attend regularly § Meetings will start and end on time
 A Brief Digression into Quality Improvement Theory
A Brief Digression into Quality Improvement Theory
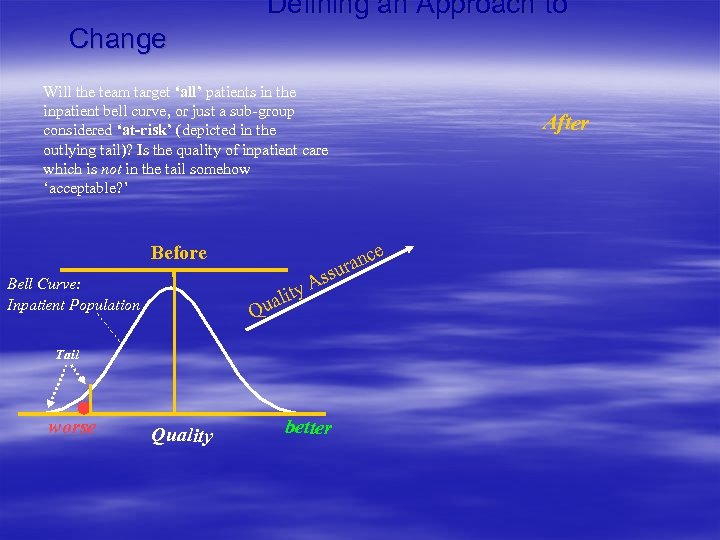 Defining an Approach to Change Will the team target ‘all’ patients in the inpatient bell curve, or just a sub-group considered ‘at-risk’ (depicted in the outlying tail)? Is the quality of inpatient care which is not in the tail somehow ‘acceptable? ’ e Before Bell Curve: Inpatient Population c ran u i al Qu Ass ty Tail worse Quality After better
Defining an Approach to Change Will the team target ‘all’ patients in the inpatient bell curve, or just a sub-group considered ‘at-risk’ (depicted in the outlying tail)? Is the quality of inpatient care which is not in the tail somehow ‘acceptable? ’ e Before Bell Curve: Inpatient Population c ran u i al Qu Ass ty Tail worse Quality After better
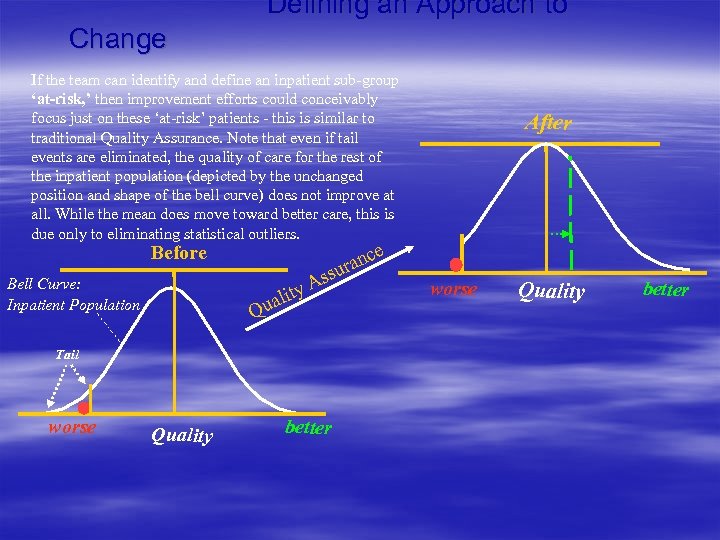 Defining an Approach to Change If the team can identify and define an inpatient sub-group ‘at-risk, ’ then improvement efforts could conceivably focus just on these ‘at-risk’ patients - this is similar to traditional Quality Assurance. Note that even if tail events are eliminated, the quality of care for the rest of the inpatient population (depicted by the unchanged position and shape of the bell curve) does not improve at all. While the mean does move toward better care, this is due only to eliminating statistical outliers. e Before Bell Curve: Inpatient Population c ran u i ual Q Ass ty Tail worse Quality After better worse Quality better
Defining an Approach to Change If the team can identify and define an inpatient sub-group ‘at-risk, ’ then improvement efforts could conceivably focus just on these ‘at-risk’ patients - this is similar to traditional Quality Assurance. Note that even if tail events are eliminated, the quality of care for the rest of the inpatient population (depicted by the unchanged position and shape of the bell curve) does not improve at all. While the mean does move toward better care, this is due only to eliminating statistical outliers. e Before Bell Curve: Inpatient Population c ran u i ual Q Ass ty Tail worse Quality After better worse Quality better
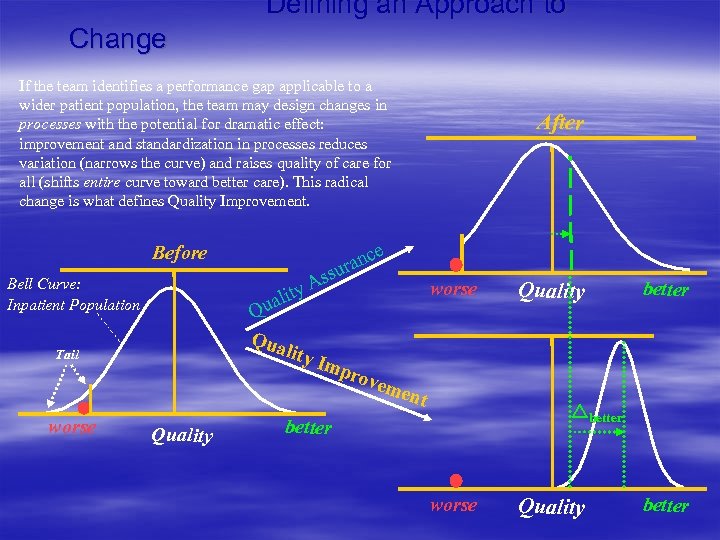 Defining an Approach to Change If the team identifies a performance gap applicable to a wider patient population, the team may design changes in processes with the potential for dramatic effect: improvement and standardization in processes reduces variation (narrows the curve) and raises quality of care for all (shifts entire curve toward better care). This radical change is what defines Quality Improvement. e Before Bell Curve: Inpatient Population worse c ran u i ual Q Qua Ass ty lity Tail Quality After Imp r worse Quality better ovem ent better worse Quality better
Defining an Approach to Change If the team identifies a performance gap applicable to a wider patient population, the team may design changes in processes with the potential for dramatic effect: improvement and standardization in processes reduces variation (narrows the curve) and raises quality of care for all (shifts entire curve toward better care). This radical change is what defines Quality Improvement. e Before Bell Curve: Inpatient Population worse c ran u i ual Q Qua Ass ty lity Tail Quality After Imp r worse Quality better ovem ent better worse Quality better
 Section III: Tools for Engineering Change
Section III: Tools for Engineering Change
 Engineering Change § Hospitals have two dynamic levels impacting performance: 1) Processes § tasks performed in series or in parallel, impacting patient care and potentially patient outcomes 2) Personnel § skilled people with hearts and minds, with variable levels of attention, time, and expertise
Engineering Change § Hospitals have two dynamic levels impacting performance: 1) Processes § tasks performed in series or in parallel, impacting patient care and potentially patient outcomes 2) Personnel § skilled people with hearts and minds, with variable levels of attention, time, and expertise
 Engineering Change: What Variables Impact Quality Outcomes of Care? Structure Processes Inputs Steps • Patients • Equipment • Supplies • Training • Environment • Inventory Methods • Coordination • Physician orders • Nursing Care • Ancillary staff • Housekeeping • Transport Outcomes of Care Outputs • Physiologic parameters • Functional status • Satisfaction • Cost
Engineering Change: What Variables Impact Quality Outcomes of Care? Structure Processes Inputs Steps • Patients • Equipment • Supplies • Training • Environment • Inventory Methods • Coordination • Physician orders • Nursing Care • Ancillary staff • Housekeeping • Transport Outcomes of Care Outputs • Physiologic parameters • Functional status • Satisfaction • Cost
 Engineering Change: What Variables Impact Quality Outcomes of Care? The two most dynamic levels impacting performance Processes Steps • Inventory Methods • Coordination • Physician orders • Nursing Care • Ancillary staff • Housekeeping Personnel • Transport
Engineering Change: What Variables Impact Quality Outcomes of Care? The two most dynamic levels impacting performance Processes Steps • Inventory Methods • Coordination • Physician orders • Nursing Care • Ancillary staff • Housekeeping Personnel • Transport
 Engineering Change § Processes – all those affecting relevant aspects of patient care § clinical decision making, order writing, admission intake, medication delivery, direct patient care, discharge planning, PCP communication, discharge follow-up, etc
Engineering Change § Processes – all those affecting relevant aspects of patient care § clinical decision making, order writing, admission intake, medication delivery, direct patient care, discharge planning, PCP communication, discharge follow-up, etc
 Engineering Change § Personnel – anybody who touches the patient or a relevant process in the system § departments, physicians, clerks, pharmacy, nursing, RT, PT/OT/ST, care technicians, phlebotomist, patient transport, administration
Engineering Change § Personnel – anybody who touches the patient or a relevant process in the system § departments, physicians, clerks, pharmacy, nursing, RT, PT/OT/ST, care technicians, phlebotomist, patient transport, administration
 Engineering Change: The Multidisicplinary Team Asks “What? ” § What? – is the right thing to do? – will make the system more effective?
Engineering Change: The Multidisicplinary Team Asks “What? ” § What? – is the right thing to do? – will make the system more effective?
 Engineering Change: The Multidisicplinary Team Asks “Where? ” § Where? – are the processes to improve? § § § Brainstorming Multivoting & nominal group technique Affinity grouping – do we start? (dissect and understand the processes) § § § § Cause and effect diagrams (Ishikawa or ‘fishbone’ diagrams) Tally sheets Pareto charts Flow (conceptual flow, decision flow) charts Run charts SPC charts Scatter charts
Engineering Change: The Multidisicplinary Team Asks “Where? ” § Where? – are the processes to improve? § § § Brainstorming Multivoting & nominal group technique Affinity grouping – do we start? (dissect and understand the processes) § § § § Cause and effect diagrams (Ishikawa or ‘fishbone’ diagrams) Tally sheets Pareto charts Flow (conceptual flow, decision flow) charts Run charts SPC charts Scatter charts
 Tools for Engineering Change: Cause-and-Effect Diagram § sometimes also called a ‘fishbone’ or Ishikawa diagram § graphically displays list of possible factors, focused on one topic or objective § used to quickly organize and categorize ideas during a brainstorming session, often as an interactive part of the session itself (the added organization can help produce balanced ideas during a brainstorming session)
Tools for Engineering Change: Cause-and-Effect Diagram § sometimes also called a ‘fishbone’ or Ishikawa diagram § graphically displays list of possible factors, focused on one topic or objective § used to quickly organize and categorize ideas during a brainstorming session, often as an interactive part of the session itself (the added organization can help produce balanced ideas during a brainstorming session)
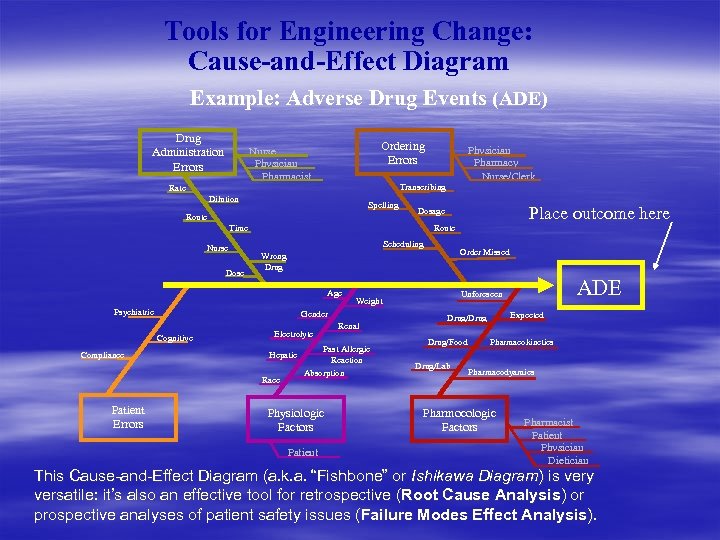 Tools for Engineering Change: Cause-and-Effect Diagram Example: Adverse Drug Events (ADE) Drug Administration Errors Ordering Errors Nurse Physician Pharmacist Transcribing Rate Dilution Spelling Route Dose Route Scheduling Psychiatric Compliance Electrolyte Hepatic Renal Past Allergic Reaction Absorption Physiologic Factors Patient ADE Unforeseen Weight Gender Race Patient Errors Order Missed Wrong Drug Age Cognitive Place outcome here Dosage Time Nurse Physician Pharmacy Nurse/Clerk Expected Drug/Drug/Food Drug/Lab Pharmacokinetics Pharmacodyamics Pharmocologic Factors Pharmacist Patient Physician Dietician This Cause-and-Effect Diagram (a. k. a. “Fishbone” or Ishikawa Diagram) is very versatile: it’s also an effective tool for retrospective (Root Cause Analysis) or prospective analyses of patient safety issues (Failure Modes Effect Analysis).
Tools for Engineering Change: Cause-and-Effect Diagram Example: Adverse Drug Events (ADE) Drug Administration Errors Ordering Errors Nurse Physician Pharmacist Transcribing Rate Dilution Spelling Route Dose Route Scheduling Psychiatric Compliance Electrolyte Hepatic Renal Past Allergic Reaction Absorption Physiologic Factors Patient ADE Unforeseen Weight Gender Race Patient Errors Order Missed Wrong Drug Age Cognitive Place outcome here Dosage Time Nurse Physician Pharmacy Nurse/Clerk Expected Drug/Drug/Food Drug/Lab Pharmacokinetics Pharmacodyamics Pharmocologic Factors Pharmacist Patient Physician Dietician This Cause-and-Effect Diagram (a. k. a. “Fishbone” or Ishikawa Diagram) is very versatile: it’s also an effective tool for retrospective (Root Cause Analysis) or prospective analyses of patient safety issues (Failure Modes Effect Analysis).
 Tools for Engineering Change: Pareto Chart • graphical display of the relative weights or frequencies of competing events, choices, or options • a bar chart, sorted from greatest to smallest, that summarizes the relative frequencies of events, choices, or options within a class • often includes a cumulative total line • used to focus within a broad category containing many choices, based on factual or opinion-based information • can combine factors that contribute to each item's practical significance
Tools for Engineering Change: Pareto Chart • graphical display of the relative weights or frequencies of competing events, choices, or options • a bar chart, sorted from greatest to smallest, that summarizes the relative frequencies of events, choices, or options within a class • often includes a cumulative total line • used to focus within a broad category containing many choices, based on factual or opinion-based information • can combine factors that contribute to each item's practical significance
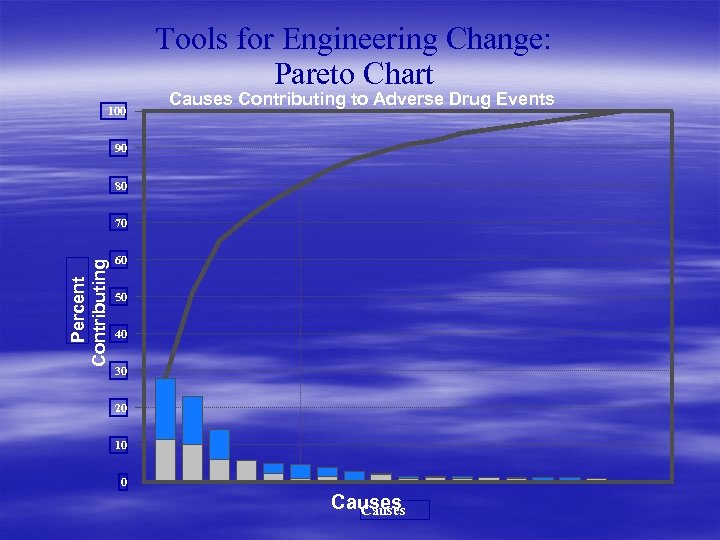 Tools for Engineering Change: Pareto Chart 100 Causes Contributing to Adverse Drug Events 90 80 Percent Contributing 70 60 50 40 30 20 10 0 Causes
Tools for Engineering Change: Pareto Chart 100 Causes Contributing to Adverse Drug Events 90 80 Percent Contributing 70 60 50 40 30 20 10 0 Causes
 Tools for Engineering Change: Sketching Processes or Flow § Macro Process Maps § Decision Flow Diagrams
Tools for Engineering Change: Sketching Processes or Flow § Macro Process Maps § Decision Flow Diagrams
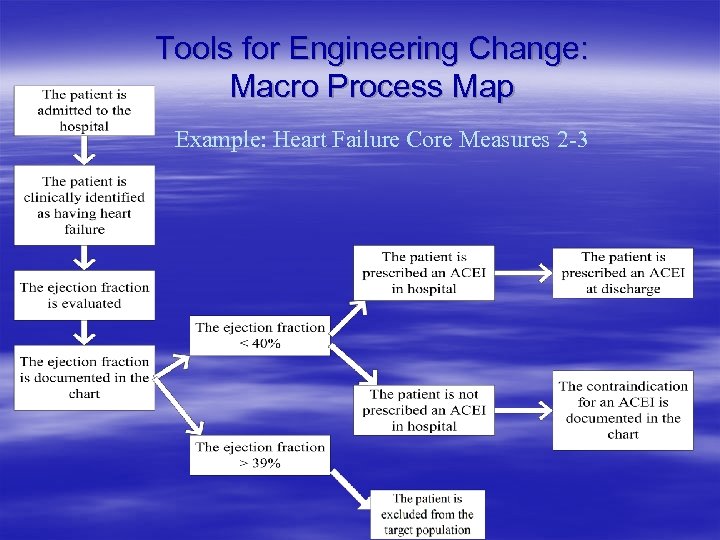 Tools for Engineering Change: Macro Process Map Example: Heart Failure Core Measures 2 -3
Tools for Engineering Change: Macro Process Map Example: Heart Failure Core Measures 2 -3
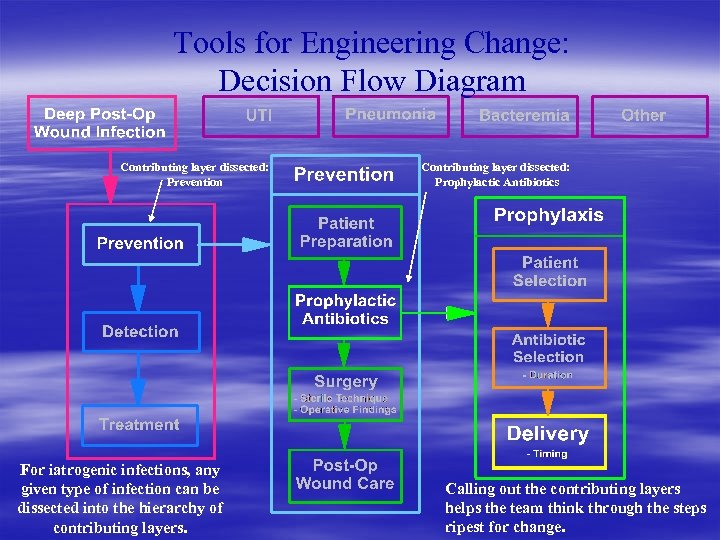 Tools for Engineering Change: Decision Flow Diagram Contributing layer dissected: Prevention For iatrogenic infections, any given type of infection can be dissected into the hierarchy of contributing layers. Contributing layer dissected: Prophylactic Antibiotics Calling out the contributing layers helps the team think through the steps ripest for change.
Tools for Engineering Change: Decision Flow Diagram Contributing layer dissected: Prevention For iatrogenic infections, any given type of infection can be dissected into the hierarchy of contributing layers. Contributing layer dissected: Prophylactic Antibiotics Calling out the contributing layers helps the team think through the steps ripest for change.
 Tools for Engineering Change: Run Charts § Our brains understand graphics better than tables § Tabular information doesn’t convey trends over time very well § Keep it simple § In center of horizontal axis place: baseline mean performance § In center of vertical axis place: implementation point § Can add upper and lower control limits, but usually not needed
Tools for Engineering Change: Run Charts § Our brains understand graphics better than tables § Tabular information doesn’t convey trends over time very well § Keep it simple § In center of horizontal axis place: baseline mean performance § In center of vertical axis place: implementation point § Can add upper and lower control limits, but usually not needed
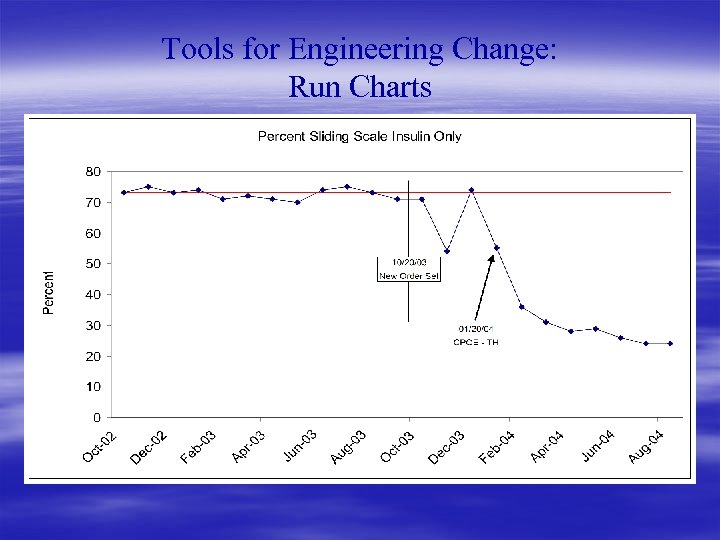 Tools for Engineering Change: Run Charts
Tools for Engineering Change: Run Charts
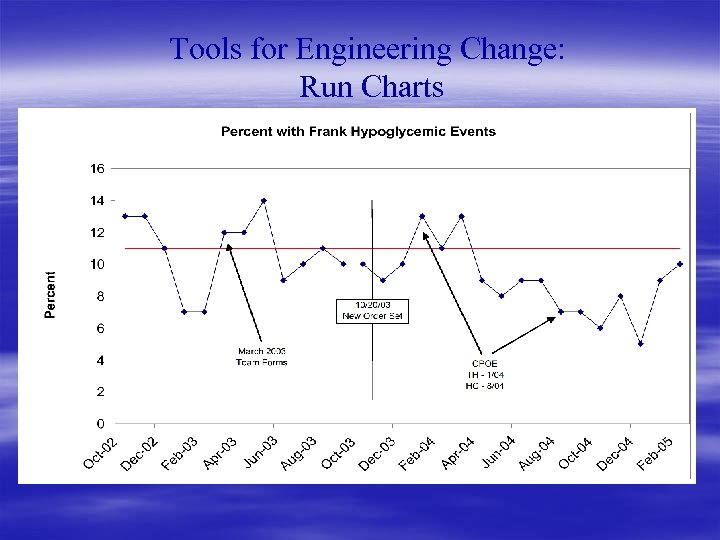 Tools for Engineering Change: Run Charts
Tools for Engineering Change: Run Charts
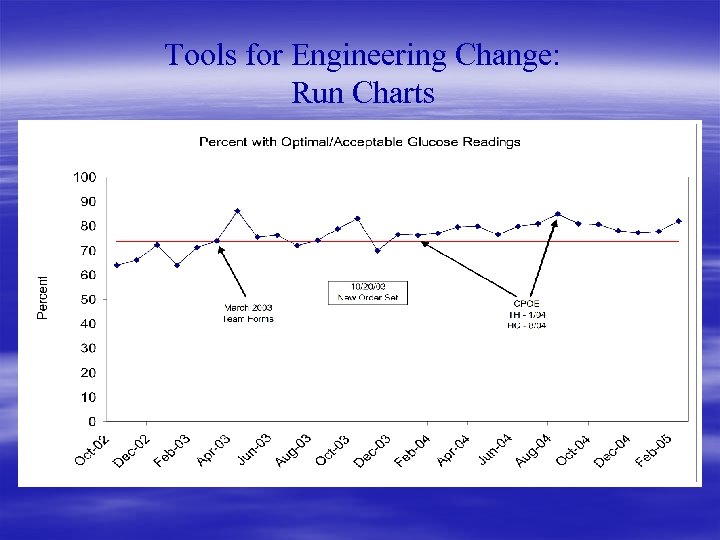 Tools for Engineering Change: Run Charts
Tools for Engineering Change: Run Charts
 Engineering Change: The Multidisicplinary Team Asks “How? ” § How? – can you make it easy to do the right thing? § You cannot destroy productivity – Changes must maintain, or enhance, workplace efficiency or balance § You must devote as much attention to fitting changes into clinical work flow as you do to the evidence-based guideline – Changes must be blended into the flow of clinical care – Important variables to consider: staffing, training, supplies, physical layout, information flow, and educational materials
Engineering Change: The Multidisicplinary Team Asks “How? ” § How? – can you make it easy to do the right thing? § You cannot destroy productivity – Changes must maintain, or enhance, workplace efficiency or balance § You must devote as much attention to fitting changes into clinical work flow as you do to the evidence-based guideline – Changes must be blended into the flow of clinical care – Important variables to consider: staffing, training, supplies, physical layout, information flow, and educational materials
 Engineering Change Improve incrementally. Learn through action. Plan Do Study Act PDSA PDSA Test your changes. Assess their effect. Then re-work the changes and do it again…and again…
Engineering Change Improve incrementally. Learn through action. Plan Do Study Act PDSA PDSA Test your changes. Assess their effect. Then re-work the changes and do it again…and again…
 Engineering Change: PDSA (the Benefits of Repeated Cycles) § Increases belief that change will result in improvement § Allows opportunities for “failures” without impacting performance § Provides documentation of improvement § Adapts to meet changing environment § Evaluates costs and side-effects of the change § Minimizes resistance upon implementation
Engineering Change: PDSA (the Benefits of Repeated Cycles) § Increases belief that change will result in improvement § Allows opportunities for “failures” without impacting performance § Provides documentation of improvement § Adapts to meet changing environment § Evaluates costs and side-effects of the change § Minimizes resistance upon implementation
 Engineering Change: PDSA § Overview: – scientific method for action-oriented learning: shorthand for testing a change in the real world setting – test a change by: planning it, trying it, measuring its results… and then trying to do it better the next time – multiple rounds of changes – some failures and some successes - should lead to improved aggregate outcome
Engineering Change: PDSA § Overview: – scientific method for action-oriented learning: shorthand for testing a change in the real world setting – test a change by: planning it, trying it, measuring its results… and then trying to do it better the next time – multiple rounds of changes – some failures and some successes - should lead to improved aggregate outcome
 Engineering Change: PDSA § Principles for Success: – start new changes on the smallest possible scale, e. g. one patient, one nurse, one doctor – run just as many PDSA cycles as necessary to gain confidence in your change – then expand – expand incrementally to more patients – expand to involve more nurses, more doctors, more departments – balance changes within system to ensure other processes not adversely stressed
Engineering Change: PDSA § Principles for Success: – start new changes on the smallest possible scale, e. g. one patient, one nurse, one doctor – run just as many PDSA cycles as necessary to gain confidence in your change – then expand – expand incrementally to more patients – expand to involve more nurses, more doctors, more departments – balance changes within system to ensure other processes not adversely stressed
 What do we want to achieve? What changes will drive our progress? How will we measure our progress? How should we modify our latest changes? modified from: The Foundation of Improvement by Thomas W. Nolan et. al
What do we want to achieve? What changes will drive our progress? How will we measure our progress? How should we modify our latest changes? modified from: The Foundation of Improvement by Thomas W. Nolan et. al
 Engineering Change What do we want to achieve? Set an outcome aim. (It should be ambitious, must be measurable and must specify a time-period and a definite population in your hospital. ) List the outcome aim again, then: – – ask “why” three times, ask “how” three times, look at the new aim statements, and pick the best one “Function Expansion” modified from: The Foundation of Improvement by Thomas W. Nolan et. al
Engineering Change What do we want to achieve? Set an outcome aim. (It should be ambitious, must be measurable and must specify a time-period and a definite population in your hospital. ) List the outcome aim again, then: – – ask “why” three times, ask “how” three times, look at the new aim statements, and pick the best one “Function Expansion” modified from: The Foundation of Improvement by Thomas W. Nolan et. al
 Engineering Change What changes will drive our progress ? Select change(s) to your system, the one(s) most likely to improve outcomes. (Recognize that not all changes improve outcomes or offer balance. ) modified from: The Foundation of Improvement by Thomas W. Nolan et. al
Engineering Change What changes will drive our progress ? Select change(s) to your system, the one(s) most likely to improve outcomes. (Recognize that not all changes improve outcomes or offer balance. ) modified from: The Foundation of Improvement by Thomas W. Nolan et. al
 Engineering Change Principles of Measurement: Seek usefulness, not perfection. Integrate measurement into the daily routine. Use qualitative and quantitative data. Use sampling. Plot data over time. How will we measure our progress? Define what you will measure quantitatively. (Collect data, chart measures regularly over specified time-period, and chart against benchmarks & goal lines. ) Three Types of Measures: 1) Outcomes 2) Process 3) Balancing measures (Use a balanced set of measures for all improvement efforts. ) modified from: The Foundation of Improvement by Thomas W. Nolan et. al
Engineering Change Principles of Measurement: Seek usefulness, not perfection. Integrate measurement into the daily routine. Use qualitative and quantitative data. Use sampling. Plot data over time. How will we measure our progress? Define what you will measure quantitatively. (Collect data, chart measures regularly over specified time-period, and chart against benchmarks & goal lines. ) Three Types of Measures: 1) Outcomes 2) Process 3) Balancing measures (Use a balanced set of measures for all improvement efforts. ) modified from: The Foundation of Improvement by Thomas W. Nolan et. al

 Engineering Change How should we modify our latest changes? Test your changes. (Run PDSA cycles to learn from the work setting. ) modified from: The Foundation of Improvement by Thomas W. Nolan et. al
Engineering Change How should we modify our latest changes? Test your changes. (Run PDSA cycles to learn from the work setting. ) modified from: The Foundation of Improvement by Thomas W. Nolan et. al
 Engineering Change: Hints for Success § § § Empower nursing Expedite order set and protocol passage through appropriate medical staff committees Better to implement an imperfect, compromise change than no change at all Pilot newest changes on smallest scale Provide hot line or support for difficult implementation situations Use your new system as a shared baseline, with clinicians free to vary based on individual patient needs Follow metrics continuously as you implement Feed metrics back into subsequent PDSA cycles Measure, learn, and over time eliminate variation arising from professionals; retain variation arising from patients Keep big picture in mind Negotiate ‘speed bumps’ – – – Time delays in getting data Incomplete buy-in Go around obstacles instead of through them (can always go back to them later) Some who disagree with you may be correct Make changes painless as possible: make it easy to do the right thing
Engineering Change: Hints for Success § § § Empower nursing Expedite order set and protocol passage through appropriate medical staff committees Better to implement an imperfect, compromise change than no change at all Pilot newest changes on smallest scale Provide hot line or support for difficult implementation situations Use your new system as a shared baseline, with clinicians free to vary based on individual patient needs Follow metrics continuously as you implement Feed metrics back into subsequent PDSA cycles Measure, learn, and over time eliminate variation arising from professionals; retain variation arising from patients Keep big picture in mind Negotiate ‘speed bumps’ – – – Time delays in getting data Incomplete buy-in Go around obstacles instead of through them (can always go back to them later) Some who disagree with you may be correct Make changes painless as possible: make it easy to do the right thing
 QI Theory: Quality Improvement in the Hospital § Suggested next steps: 1) Share this primer in QI Theory with other hospitalists in your group 2) Identify an important QI project at your hospital 3) Lead the QI project using all available resources 4) Learn from your experience and be among the first to mentor other hospitalists
QI Theory: Quality Improvement in the Hospital § Suggested next steps: 1) Share this primer in QI Theory with other hospitalists in your group 2) Identify an important QI project at your hospital 3) Lead the QI project using all available resources 4) Learn from your experience and be among the first to mentor other hospitalists
 Acknowledgments § Brent James, MD, MStat (Intermountain Health Care's Institute for Health Care Delivery Research): concepts, content, figures § Thomas Nolan, Ph. D (Institute for Healthcare Improvement): concepts, content, figures § Greg Maynard, MD, MSc (University of California, San Diego): editorial composition and review § Jason Stein, MD (Emory University School of Medicine): editorial composition
Acknowledgments § Brent James, MD, MStat (Intermountain Health Care's Institute for Health Care Delivery Research): concepts, content, figures § Thomas Nolan, Ph. D (Institute for Healthcare Improvement): concepts, content, figures § Greg Maynard, MD, MSc (University of California, San Diego): editorial composition and review § Jason Stein, MD (Emory University School of Medicine): editorial composition


