08499d8a9abe61cbf273168daf5bedb7.ppt
- Количество слайдов: 25
 Healthier Together Joint Committee Wednesday 15 th June 2016
Healthier Together Joint Committee Wednesday 15 th June 2016
 Primary Care Update Developing Integrated care in GM Building on our Healthier Together Commitments Rob Bellingham, Director of Commissioning
Primary Care Update Developing Integrated care in GM Building on our Healthier Together Commitments Rob Bellingham, Director of Commissioning
 Context o The Healthier Together made a series of commitments relating to the development of primary and joined up care, (integrated care) across GM. This has given us a platform upon which significant aspects of our GM Strategic Plan, “Taking Charge” has been built. This presentation describes these next steps in the context of the wider GM transformation programme. o Members will recall the “venn diagram” depicting Primary, Integrated and Acute Care and our ambition to achieve a so called “total eclipse” of the Primary and Integrated Care circles. We believe that the work described in this presentation achieves this objective via the development of our GM Locality Plans and their vision for integrated care serving neighbourhoods of circa 3050 k populations. o Scaled, population health and wellbeing management is core to our strategy to transform community based care and support. o This part of our new models of care and support are central to our ability to maximise the demand reducing potential of those new models. An understanding of those characteristics of the new models essential to managing population health improvement and reducing demand on acute services is key to ensuring all parts of GM are developing models which will contribute to clinical and financial sustainability
Context o The Healthier Together made a series of commitments relating to the development of primary and joined up care, (integrated care) across GM. This has given us a platform upon which significant aspects of our GM Strategic Plan, “Taking Charge” has been built. This presentation describes these next steps in the context of the wider GM transformation programme. o Members will recall the “venn diagram” depicting Primary, Integrated and Acute Care and our ambition to achieve a so called “total eclipse” of the Primary and Integrated Care circles. We believe that the work described in this presentation achieves this objective via the development of our GM Locality Plans and their vision for integrated care serving neighbourhoods of circa 3050 k populations. o Scaled, population health and wellbeing management is core to our strategy to transform community based care and support. o This part of our new models of care and support are central to our ability to maximise the demand reducing potential of those new models. An understanding of those characteristics of the new models essential to managing population health improvement and reducing demand on acute services is key to ensuring all parts of GM are developing models which will contribute to clinical and financial sustainability
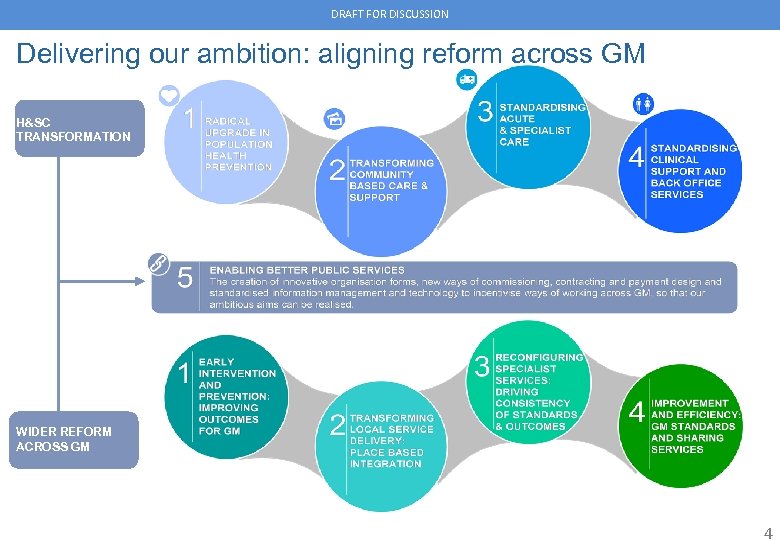 DRAFT FOR DISCUSSION Delivering our ambition: aligning reform across GM H&SC TRANSFORMATION WIDER REFORM ACROSS GM 4
DRAFT FOR DISCUSSION Delivering our ambition: aligning reform across GM H&SC TRANSFORMATION WIDER REFORM ACROSS GM 4
 DRAFT FOR DISCUSSION Proposed method for a consistent approach to developing an LCO 1. Identify target population 2. Assess potential impact by area of spend 3. Use ‘logic model’ to define reinvestment potential 4. Define core elements of delivery model 5. Translate the core elements to activity 6. Identify and model the workforce requirements 7. Model the financial requirement 8. Conduct segment level Cost Benefit Analysis comparing savings and investment 9. Translate into payment mechanisms 10. Identify performance “dashboard” and approach The 10 stage approach to the left starts to illustrate an overall development approach to fully establishing an LCO. GM colleagues consider the value of consistent approaches at key stages such as: • Risk stratification & population segmentation approaches • how we define an LCOs core characteristics at both a basic and advanced level to reach for the higher ambition on scope and development • A reliable costing methodology inform investment and implementation considerations and • a standard GM approach to Cost Benefit utilising the New Economy model, of interventions delivered by an LCO.
DRAFT FOR DISCUSSION Proposed method for a consistent approach to developing an LCO 1. Identify target population 2. Assess potential impact by area of spend 3. Use ‘logic model’ to define reinvestment potential 4. Define core elements of delivery model 5. Translate the core elements to activity 6. Identify and model the workforce requirements 7. Model the financial requirement 8. Conduct segment level Cost Benefit Analysis comparing savings and investment 9. Translate into payment mechanisms 10. Identify performance “dashboard” and approach The 10 stage approach to the left starts to illustrate an overall development approach to fully establishing an LCO. GM colleagues consider the value of consistent approaches at key stages such as: • Risk stratification & population segmentation approaches • how we define an LCOs core characteristics at both a basic and advanced level to reach for the higher ambition on scope and development • A reliable costing methodology inform investment and implementation considerations and • a standard GM approach to Cost Benefit utilising the New Economy model, of interventions delivered by an LCO.
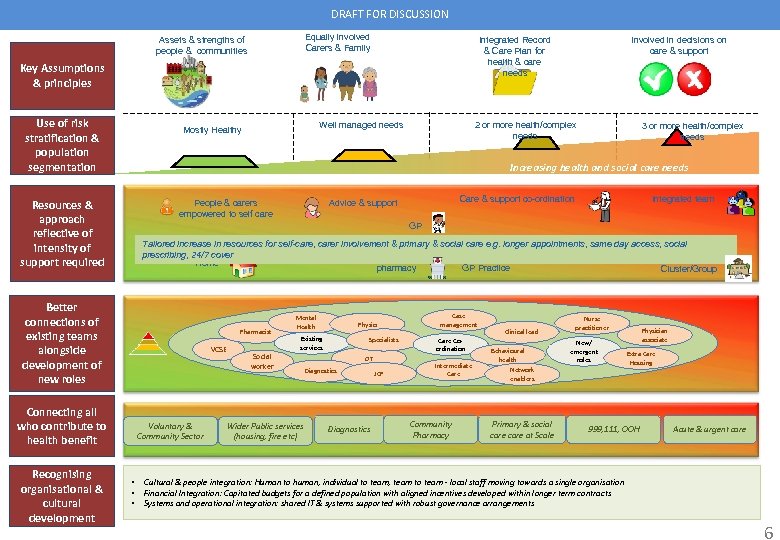 DRAFT FOR DISCUSSION Equally involved Carers & Family Assets & strengths of people & communities Integrated Record & Care Plan for health & care needs Key Assumptions & principles Use of risk stratification & population segmentation 2 or more health/complex needs 3 or more health/complex needs Increasing health and social care needs Resources & approach reflective of intensity of support required People & carers empowered to self care Care & support co-ordination Advice & support Integrated team GP Tailored increase in resources for self-care, carer involvement & primary & social care e. g. longer appointments, same day access, social prescribing, 24/7 cover Home GP Practice pharmacy Cluster/Group Better connections of existing teams alongside development of new roles Pharmacist VCSE Connecting all who contribute to health benefit Recognising organisational & cultural development Well managed needs Mostly Healthy Involved in decisions on care & support Voluntary & Community Sector • • • Mental Health Physio Existing services Social worker Wider Public services (housing, fire etc) Specialists OT Diagnostics JCP Case management Care Coordination Intermediate Care Community Pharmacy Clinical lead Behavioural health Nurse practitioner New/ emergent roles Network enablers Primary & social care at Scale Physician associate Extra Care Housing 999, 111, OOH Acute & urgent care Cultural & people integration: Human to human, individual to team, team to team - local staff moving towards a single organisation Financial Integration: Capitated budgets for a defined population with aligned incentives developed within longer term contracts Systems and operational integration: shared IT & systems supported with robust governance arrangements 6
DRAFT FOR DISCUSSION Equally involved Carers & Family Assets & strengths of people & communities Integrated Record & Care Plan for health & care needs Key Assumptions & principles Use of risk stratification & population segmentation 2 or more health/complex needs 3 or more health/complex needs Increasing health and social care needs Resources & approach reflective of intensity of support required People & carers empowered to self care Care & support co-ordination Advice & support Integrated team GP Tailored increase in resources for self-care, carer involvement & primary & social care e. g. longer appointments, same day access, social prescribing, 24/7 cover Home GP Practice pharmacy Cluster/Group Better connections of existing teams alongside development of new roles Pharmacist VCSE Connecting all who contribute to health benefit Recognising organisational & cultural development Well managed needs Mostly Healthy Involved in decisions on care & support Voluntary & Community Sector • • • Mental Health Physio Existing services Social worker Wider Public services (housing, fire etc) Specialists OT Diagnostics JCP Case management Care Coordination Intermediate Care Community Pharmacy Clinical lead Behavioural health Nurse practitioner New/ emergent roles Network enablers Primary & social care at Scale Physician associate Extra Care Housing 999, 111, OOH Acute & urgent care Cultural & people integration: Human to human, individual to team, team to team - local staff moving towards a single organisation Financial Integration: Capitated budgets for a defined population with aligned incentives developed within longer term contracts Systems and operational integration: shared IT & systems supported with robust governance arrangements 6
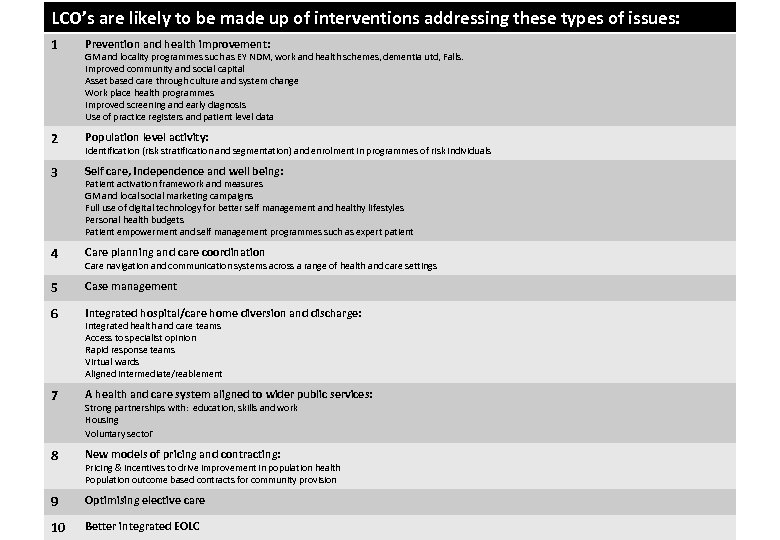 LCO’s are likely to be made up of interventions addressing these types of issues: 1 Prevention and health improvement: 2 Population level activity: 3 Self care, Independence and well being: 4 Care planning and care coordination 5 Case management 6 Integrated hospital/care home diversion and discharge: 7 A health and care system aligned to wider public services: 8 New models of pricing and contracting: 9 Optimising elective care 10 Better integrated EOLC GM and locality programmes such as EY NDM, work and health schemes, dementia utd, Falls. Improved community and social capital Asset based care through culture and system change Work place health programmes Improved screening and early diagnosis Use of practice registers and patient level data Identification (risk stratification and segmentation) and enrolment in programmes of risk individuals Patient activation framework and measures GM and local social marketing campaigns Full use of digital technology for better self management and healthy lifestyles Personal health budgets Patient empowerment and self management programmes such as expert patient Care navigation and communication systems across a range of health and care settings Integrated health and care teams Access to specialist opinion Rapid response teams Virtual wards Aligned intermediate/reablement Strong partnerships with: education, skills and work Housing Voluntary sector Pricing & incentives to drive improvement in population health Population outcome based contracts for community provision
LCO’s are likely to be made up of interventions addressing these types of issues: 1 Prevention and health improvement: 2 Population level activity: 3 Self care, Independence and well being: 4 Care planning and care coordination 5 Case management 6 Integrated hospital/care home diversion and discharge: 7 A health and care system aligned to wider public services: 8 New models of pricing and contracting: 9 Optimising elective care 10 Better integrated EOLC GM and locality programmes such as EY NDM, work and health schemes, dementia utd, Falls. Improved community and social capital Asset based care through culture and system change Work place health programmes Improved screening and early diagnosis Use of practice registers and patient level data Identification (risk stratification and segmentation) and enrolment in programmes of risk individuals Patient activation framework and measures GM and local social marketing campaigns Full use of digital technology for better self management and healthy lifestyles Personal health budgets Patient empowerment and self management programmes such as expert patient Care navigation and communication systems across a range of health and care settings Integrated health and care teams Access to specialist opinion Rapid response teams Virtual wards Aligned intermediate/reablement Strong partnerships with: education, skills and work Housing Voluntary sector Pricing & incentives to drive improvement in population health Population outcome based contracts for community provision
 Summary and recommendations • The Healthier Together Joint Committee is asked to: – Note that the work which initially took place in line with the initial Healthier Together commitments has developed as described in this presentation – Note that this new phase of work directly connects to the GM Strategic Plan, “Taking Charge” and the development of the 10 Locality Plans – Note that each area of GM is developing Locality Care Organisations, in line with the models and characteristics set out in this presentation – Consider, in the light of the above, how the Joint Committee wishes to be appraised of progress on this agenda.
Summary and recommendations • The Healthier Together Joint Committee is asked to: – Note that the work which initially took place in line with the initial Healthier Together commitments has developed as described in this presentation – Note that this new phase of work directly connects to the GM Strategic Plan, “Taking Charge” and the development of the 10 Locality Plans – Note that each area of GM is developing Locality Care Organisations, in line with the models and characteristics set out in this presentation – Consider, in the light of the above, how the Joint Committee wishes to be appraised of progress on this agenda.
 Programme Update Sophie Hargreaves, Programme Director
Programme Update Sophie Hargreaves, Programme Director
 Purpose of meeting • Joint Committee’s role is to assess whether adequate progress is being made towards implementation of Healthier Together • This meeting is structured to provide an update on the GM and sector progress as well as key risks and dependencies • The Committee will be asked to comment on this at the end of the agenda 10
Purpose of meeting • Joint Committee’s role is to assess whether adequate progress is being made towards implementation of Healthier Together • This meeting is structured to provide an update on the GM and sector progress as well as key risks and dependencies • The Committee will be asked to comment on this at the end of the agenda 10
 Highlights since March Joint Committee Assurance: • 3 of 4 sector stage 1 reviews completed HR and workforce: • Recruitment principles agreed • Baseline taken Finance: • Finance ongoing discussions regarding capital Equalities: • Standards baseline taken • Access appraisal underway Clinical: • Standards baseline taken Clarification of the general surgery model completed • Quick win recommendations identified (item 7) • NWAS audit underway Evaluation: • Manchester University partnership established 11
Highlights since March Joint Committee Assurance: • 3 of 4 sector stage 1 reviews completed HR and workforce: • Recruitment principles agreed • Baseline taken Finance: • Finance ongoing discussions regarding capital Equalities: • Standards baseline taken • Access appraisal underway Clinical: • Standards baseline taken Clarification of the general surgery model completed • Quick win recommendations identified (item 7) • NWAS audit underway Evaluation: • Manchester University partnership established 11
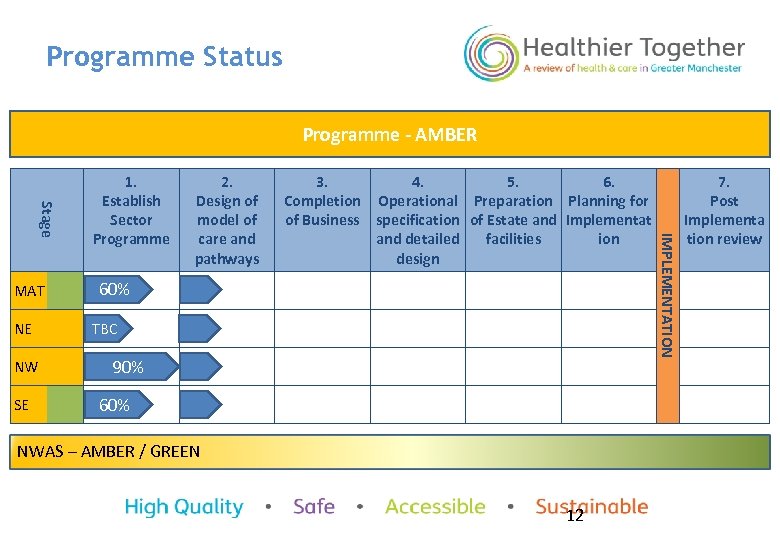 Programme Status Programme - AMBER NE NW SE 2. Design of model of care and pathways 3. 4. 5. 6. Completion Operational Preparation Planning for of Business specification of Estate and Implementat and detailed facilities ion design 60% TBC 90% 60% NWAS – AMBER / GREEN 12 IMPLEMENTATION Stage MAT 1. Establish Sector Programme 7. Post Implementa tion review
Programme Status Programme - AMBER NE NW SE 2. Design of model of care and pathways 3. 4. 5. 6. Completion Operational Preparation Planning for of Business specification of Estate and Implementat and detailed facilities ion design 60% TBC 90% 60% NWAS – AMBER / GREEN 12 IMPLEMENTATION Stage MAT 1. Establish Sector Programme 7. Post Implementa tion review
 Programme Plan - Approach • Complex made up of many moving parts! • Many dependencies and interconnected activities • Risks and dependencies to be identified through Programme Board and managed through Risk/Dependency register • Therefore reviewed on a rolling basis – and updated quarterly for Joint Committee 13
Programme Plan - Approach • Complex made up of many moving parts! • Many dependencies and interconnected activities • Risks and dependencies to be identified through Programme Board and managed through Risk/Dependency register • Therefore reviewed on a rolling basis – and updated quarterly for Joint Committee 13
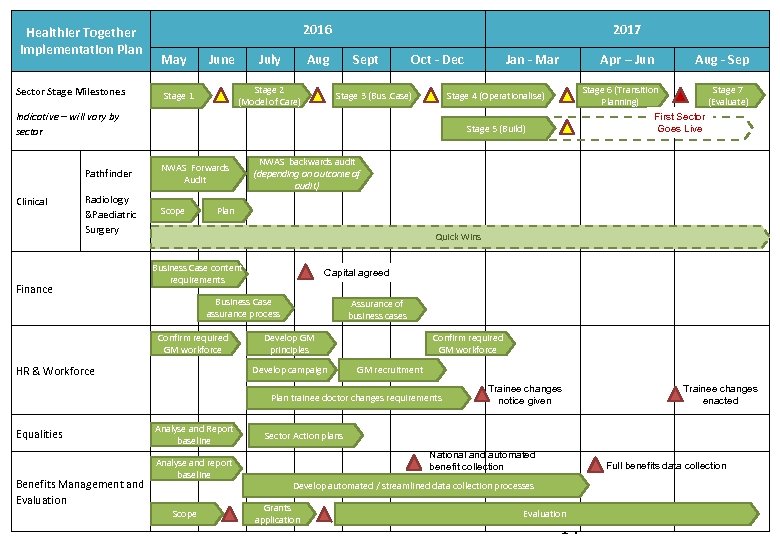 Healthier Together Implementation Plan Sector Stage Milestones 2016 May June July Aug Stage 2 (Model of Care) Stage 1 2017 Sept Oct - Dec Stage 3 (Bus. Case) NWAS Forwards Audit Radiology &Paediatric Surgery Scope First Sector Goes Live NWAS backwards audit (depending on outcome of audit) Quick Wins Business Case content requirements Capital agreed Business Case assurance process HR & Workforce Assurance of business cases Develop GM principles Develop campaign Confirm required GM workforce GM recruitment Plan trainee doctor changes requirements Benefits Management and Evaluation Stage 7 (Evaluate) Plan Confirm required GM workforce Equalities Aug - Sep Stage 6 (Transition Planning) Stage 5 (Build) Pathfinder Finance Apr – Jun Stage 4 (Operationalise) Indicative – will vary by sector Clinical Jan - Mar Analyse and Report baseline Analyse and report baseline Scope Trainee changes notice given Trainee changes enacted Sector Action plans National and automated benefit collection Full benefits data collection Develop automated / streamlined data collection processes Grants application Evaluation 14
Healthier Together Implementation Plan Sector Stage Milestones 2016 May June July Aug Stage 2 (Model of Care) Stage 1 2017 Sept Oct - Dec Stage 3 (Bus. Case) NWAS Forwards Audit Radiology &Paediatric Surgery Scope First Sector Goes Live NWAS backwards audit (depending on outcome of audit) Quick Wins Business Case content requirements Capital agreed Business Case assurance process HR & Workforce Assurance of business cases Develop GM principles Develop campaign Confirm required GM workforce GM recruitment Plan trainee doctor changes requirements Benefits Management and Evaluation Stage 7 (Evaluate) Plan Confirm required GM workforce Equalities Aug - Sep Stage 6 (Transition Planning) Stage 5 (Build) Pathfinder Finance Apr – Jun Stage 4 (Operationalise) Indicative – will vary by sector Clinical Jan - Mar Analyse and Report baseline Analyse and report baseline Scope Trainee changes notice given Trainee changes enacted Sector Action plans National and automated benefit collection Full benefits data collection Develop automated / streamlined data collection processes Grants application Evaluation 14
 Pan GM timeline (as of Wednesday 30 th March 2016) September 2016 to March 2017 Beyond March 2017 Baseline audit returned analysed Recruitment Framework complete Finance Framework complete Source of capital and transition funding agreed Paediatric surgery and radiology plans completed NWAS Pathfinder audit completed Doctors in Training - agreement of the impact 1 st wave of Recruitment to workforce Business cases completed and assured First clinical ‘quick wins’ delivered Agreement on requirements for NWAS Pathfinder tool Capital builds underway, where possible • • Radiology Hubs in place First high risk general surgery patient movements (Sectors to have been through stages 1 -6 of the Assurance Framework) • April to September 2016 • • • Implementation of outstanding sectors following required capital build and assurance
Pan GM timeline (as of Wednesday 30 th March 2016) September 2016 to March 2017 Beyond March 2017 Baseline audit returned analysed Recruitment Framework complete Finance Framework complete Source of capital and transition funding agreed Paediatric surgery and radiology plans completed NWAS Pathfinder audit completed Doctors in Training - agreement of the impact 1 st wave of Recruitment to workforce Business cases completed and assured First clinical ‘quick wins’ delivered Agreement on requirements for NWAS Pathfinder tool Capital builds underway, where possible • • Radiology Hubs in place First high risk general surgery patient movements (Sectors to have been through stages 1 -6 of the Assurance Framework) • April to September 2016 • • • Implementation of outstanding sectors following required capital build and assurance
 Progress to date - assessment • 3 / 4 Stage 1 reviews complete • Good progress in areas, common themes of areas to work on • Agreement of model of care key on critical path • Stage 1 themes paper sets out actions for sectors on these themes • GM levers can also be used to support implementation 16
Progress to date - assessment • 3 / 4 Stage 1 reviews complete • Good progress in areas, common themes of areas to work on • Agreement of model of care key on critical path • Stage 1 themes paper sets out actions for sectors on these themes • GM levers can also be used to support implementation 16
 Recommendations for sectors 1. Understand current performance issues relevant to HT and develop action plans to address identified risks 2. Develop plans to support relationship building across clinical teams and to address the cultural changes 3. Review and share outputs from the Clinical Alliance in sectors 4. Development of ‘quick win’ plans for each specialty, supported by HT Clinical Champions 5. Identification of resource to commence modelling work and standardisation of baseline data 6. Sectors to establish Patient Participation Groups and integrate patient participation into their plans Joint Committee asked to support this and ensure actions are completed in sectors 17
Recommendations for sectors 1. Understand current performance issues relevant to HT and develop action plans to address identified risks 2. Develop plans to support relationship building across clinical teams and to address the cultural changes 3. Review and share outputs from the Clinical Alliance in sectors 4. Development of ‘quick win’ plans for each specialty, supported by HT Clinical Champions 5. Identification of resource to commence modelling work and standardisation of baseline data 6. Sectors to establish Patient Participation Groups and integrate patient participation into their plans Joint Committee asked to support this and ensure actions are completed in sectors 17
 Commissioning Levers • Demonstrate commitment to change through commissioning intentions: – Specifying single teams for general surgery in commissioning intentions from a set date – for example January 2017 – Specifying movement of high risk elective patients (~100 per site per year) in commissioning intentions from a set date – the date will need exploration but could be for example April 2017 • Action: Joint Committee are asked to endorse this approach and reflect in local commissioning intentions. • Action: CCGs to report proposed commissioning intentions for Healthier Together to September Joint Committee. • Action: Sector to identify Head of Commissioning Lead to work with CFO lead on this 18
Commissioning Levers • Demonstrate commitment to change through commissioning intentions: – Specifying single teams for general surgery in commissioning intentions from a set date – for example January 2017 – Specifying movement of high risk elective patients (~100 per site per year) in commissioning intentions from a set date – the date will need exploration but could be for example April 2017 • Action: Joint Committee are asked to endorse this approach and reflect in local commissioning intentions. • Action: CCGs to report proposed commissioning intentions for Healthier Together to September Joint Committee. • Action: Sector to identify Head of Commissioning Lead to work with CFO lead on this 18
 Other GM Levers • Supporting model of care agreement: – Stage 2 review meeting dates set – GM event is planned for sectors to share this in August – Support in finalising data • Clinical Effectiveness: – Sharing of national data and the baseline – identifying leads for best practice from across GM – ‘Theme of the month’ • Cultural challenges: – Engagement with GM Organisational Development Group to discuss the implementation challenge Healthier Together poses and draw on existing experience in managing change in GM – Collation of key clinical concerns and mitigations across sectors 19
Other GM Levers • Supporting model of care agreement: – Stage 2 review meeting dates set – GM event is planned for sectors to share this in August – Support in finalising data • Clinical Effectiveness: – Sharing of national data and the baseline – identifying leads for best practice from across GM – ‘Theme of the month’ • Cultural challenges: – Engagement with GM Organisational Development Group to discuss the implementation challenge Healthier Together poses and draw on existing experience in managing change in GM – Collation of key clinical concerns and mitigations across sectors 19
 Healthier Together HR & Workforce Update – Katy Coope, Assistant Director HR & Workforce
Healthier Together HR & Workforce Update – Katy Coope, Assistant Director HR & Workforce
 Recruitment Framework Approach Key Principles: • Current Recruitment: What can and should be actioned immediately • Future Recruitment: The proposed way we will manage recruitment to ‘new’ vacancies as a direct result of the Healthier Together changes. 21
Recruitment Framework Approach Key Principles: • Current Recruitment: What can and should be actioned immediately • Future Recruitment: The proposed way we will manage recruitment to ‘new’ vacancies as a direct result of the Healthier Together changes. 21
 Recruitment Approach • Work as a sector • Inform Candidates Current • Job Role Information Recruitment: • Follow Recruitment Process 22
Recruitment Approach • Work as a sector • Inform Candidates Current • Job Role Information Recruitment: • Follow Recruitment Process 22
 Recruitment Approach • Develop an attractive offer Future Recruitment • Use new recruits flexibly (Recruitment • GM Recruitment Plan): Campaign for some roles • International Recruitment 23
Recruitment Approach • Develop an attractive offer Future Recruitment • Use new recruits flexibly (Recruitment • GM Recruitment Plan): Campaign for some roles • International Recruitment 23
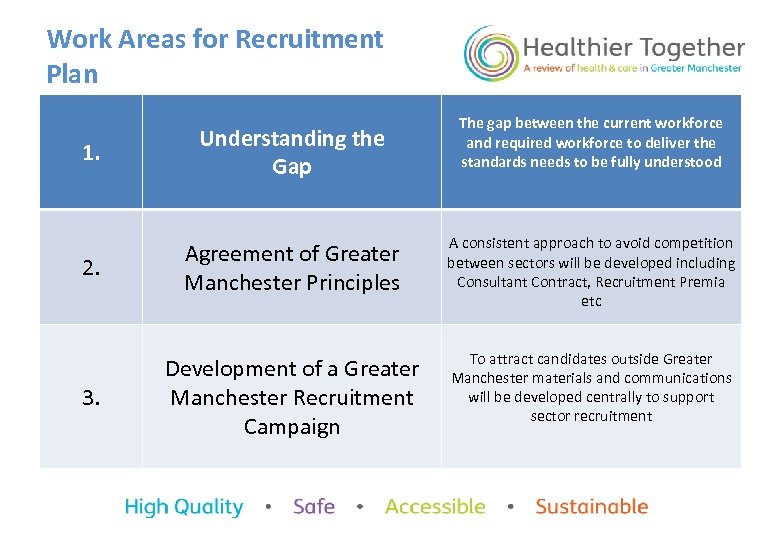 Work Areas for Recruitment Plan The gap between the current workforce and required workforce to deliver the standards needs to be fully understood 1. Understanding the Gap 2. Agreement of Greater Manchester Principles A consistent approach to avoid competition between sectors will be developed including Consultant Contract, Recruitment Premia etc Development of a Greater Manchester Recruitment Campaign To attract candidates outside Greater Manchester materials and communications will be developed centrally to support sector recruitment 3.
Work Areas for Recruitment Plan The gap between the current workforce and required workforce to deliver the standards needs to be fully understood 1. Understanding the Gap 2. Agreement of Greater Manchester Principles A consistent approach to avoid competition between sectors will be developed including Consultant Contract, Recruitment Premia etc Development of a Greater Manchester Recruitment Campaign To attract candidates outside Greater Manchester materials and communications will be developed centrally to support sector recruitment 3.
 Suggested Timeframe for Recruitment Plan Central Team Timeframe May - June -Analysis of the baseline -Clarification of the baseline -Comparison to April 15 and confirmation of -Provide details to central team around required consultant workforce for GM current Consultant Contract, Recruitment & Retention premia etc - July - August – November Provider - Development of Greater Manchester Principles Development of a Greater Manchester Recruitment campaign - Share materials and comms with sectors Commence GM Recruitment for specific roles Sector workforce modelling to deliver model of care and understand recruitment locally Share rota design Commence Recruitment
Suggested Timeframe for Recruitment Plan Central Team Timeframe May - June -Analysis of the baseline -Clarification of the baseline -Comparison to April 15 and confirmation of -Provide details to central team around required consultant workforce for GM current Consultant Contract, Recruitment & Retention premia etc - July - August – November Provider - Development of Greater Manchester Principles Development of a Greater Manchester Recruitment campaign - Share materials and comms with sectors Commence GM Recruitment for specific roles Sector workforce modelling to deliver model of care and understand recruitment locally Share rota design Commence Recruitment


