98911ae7828c32ccdd4c40a07ae0f545.ppt
- Количество слайдов: 108

Health Promotion Interventions for beginners… and for those who’ve been there and got the T-Shirt Kathy Cobain, Amanda Drakeley & Beck Taylor 4 th July 2012

Agenda for today: 0930 0950 1020 1030 1100 1245 1430 1500 Introduction & overview PART 1: What is health promotion? Break PART 2: The role of theory and evidence in health promotion PART 3: Approaches to health promotion Lunch PART 4: Implementing a health promotion intervention in the real world: a practical exercise and post-mortem (coffee to be taken during this time) PART 5: Reflective practice Close

Introduction and overview

Aim of today: To deliver a session on health promotion to allow novices to the areas to learn the fundamentals but for experienced practitioners in this area to be able to discuss, reflect and evaluate their current practice.

Learning outcomes: By the end of this masterclass the practitioner should be able to: 1. Understand key points in history 2. Understand key terms 3. Discuss of the role of, and how to find and use health promotion theories/models 4. Understand importance of evidence and policy 5. Describe the different approaches to health promotion 6. Consider design, planning, barriers, monitoring and evaluation 7. Understand realities of implementing health promotion

The pre-masterclass survey • We decided to send out the pre-masterclass survey to gain an understanding of who we would have in attendance, particularly: – – Knowledge about health promotion Qualifications in health promotion Experience in delivering health promotion Current job role in relation to health promotion • Sent to 39 proposed attendees. • Response of n = 22 (56% response rate) The results are as follows…
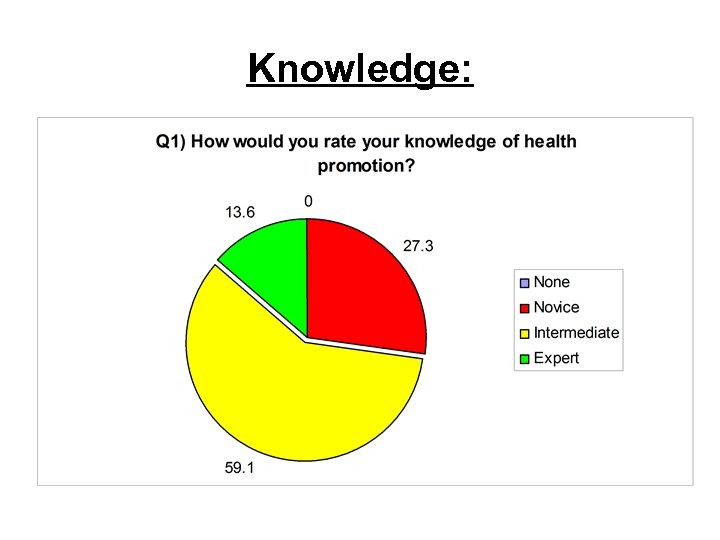
Knowledge:

Qualifications:

Experience:

Current job role:

A range of roles… • Tobacco Control Co-ordinator • Senior Health Improvement Specialist • Health Development Officer • Environmental Health Officer • Public Health Epidemiologist • Health Intelligence Analyst • Health Check Co-ordinator • Health Improvement Practitioner Specialist • Health Trainer • Health & Wellbeing Strategy Officer • Falls Management Lead • Health Information & Social Marketing Officer • Specialist Stop Smoking Advisor in Pregnancy • Breastfeeding Support Coordinator • Public Health Adviser • Health Improvement Worker – Smoking Cessation • Lifestyle risk implementation Manager

So that’s all of you…. But what about us?

Kathy • Specialty Registrar in Public Health, Year 2 based at Worcester PCT. • Previous experience: – Clinical Nurse Specialist Drug and Alcohol – Ph. D "Alcohol Treatment in the NHS: Challenging the Paradigm” – involved in a national alcohol needs assessment for the DH – Research Fellow Public Health and Primary Care (NHS and University) – BSc Psychology & MSc Health Psychology

Amanda • Specialty Registrar in Public Health, Year 4 based at Staffordshire Public Health. • Previous experience in planning, developing and implementing health promotion initiatives: – – – Walking for Health Scheme Exercise on referral programme “Sport Relief” events “Fruity Friday” campaigns No smoking day events Community health fairs, etc.

Beck • Clinical Research Fellow in Public Health, based at Birmingham University (having completed the public health training scheme). • Current experience: – Working on a Ph. D (lay health worker interventions). – Research interests include health inequalities, lay worker interventions, policy evaluation and the role of theory in public health. – The use of realistic evaluation and its application in complex interventions (Health Trainers).

So, in summary… This health promotion masterclass is about: • Understanding the fundamentals • Exploring further • Sharing, reflecting on and evaluating your own practice And why is this relevant to you? In public health roles, you may need to: • Develop your own idea • Project manage local implementation • Advise on how to develop/implement • Assess the evidence for an ‘evidence based’ intervention • Decide whether or not to fund an intervention

PART 1 - Agenda Learning Outcome 1: Understand the key points in the history and evolution of health promotion (including the relationship between health education and health improvement). Learning Outcome 2: Understand the key terms around health promotion What is health promotion? • • • A brief history & the Ottawa Charter Understanding health Factors that influence health Inequalities in health Group work task

The “old” public health • In the 19 th century: • Most histories of public health begin with this “sanitation phase” – a period characterised by environmental issues such as housing, working conditions, supply of clean water and safe disposal of waste. Reduction in infectious diseases

The rise of health education • In the early 20 th century: a second phase known as the “Personal hygiene era”. – Prevention is better than cure! – Local authorities extended services beyond preventing disease to improving health through health education. • Examples: – School children were taught hygiene principles (i. e. teeth brushing) – Parents (mothers) were taught hygiene, nutrition and childcare in the home (through home visiting). • Central Council for Health Education was first established in 1927 – financed by local authority public health departments. • Health Education Council created in England 1968 as an Non Government Organisation. – Create a climate of opinion generally favourable to health educ. – Develop blanket programmes of education and (target) selected priority subjects.

The health promotion movement By the mid-1980 s: it became wider acknowledged that effective health education involved making healthier choices easier: – Proposing a wider agenda which involved modifying circumstances, environment and policy to become more “health promoting”. – So people had opportunities to choose a healthier lifestyle. – Recognised that people’s capacity to take action was limited by environmental / social circumstances. The first International Conference on Health Promotion was held in Ottawa on November 21, 1986. It was at this conference that The Ottawa Charter for Health Promotion was adopted.

The Ottawa Charter (WHO 1986) The Ottawa Charter for Health Promotion provided a further impetus to an emerging modern health promotion movement. Definition: “Health promotion is the process of enabling people to increase control over, and to improve their health”. Ottawa Charter for Health Promotion. WHO, Geneva, 1986 Over the last 25 years, the Ottawa Charter has been highly influential, constant point of reference for those involved in promoting health: http: //www. who. int/healthpromotion/en/

Health Promotion Emblem It identified: 3 basic strategies: "enabling, mediating, and advocacy” 5 key themes: 1. 2. 3. 4. 5. Build healthy public policy Create supportive environments Strengthen community action Develop personal skills Reorientation of health services Logo visualises the idea that health promotion is a comprehensive multi-strategy approach

Understanding health? In order to fully understand health we should consider the following two questions: 1. How should health be defined? 2. Why is defining it so important when promoting public health?

Definitions of health • Health as “absence of disease” – Medical model of health – Can be traced back as far as the ancient Greeks • Health as “well being” Health is a state of complete physical, mental and social wellbeing and not merely the absence of disease or infirmity (WHO 1948) • Health as “a resource” Health is a resource for everyday life, not the object of living. It is a positive concept emphasizing social and personal resources as well as physical capabilities (Ottawa Charter for Health Promotion. WHO, Geneva, 1986)

A new definition? (June 2011) The WHO definition of health as “complete wellbeing” is no longer fit for purpose given the rise of chronic disease. Huber and colleagues propose changing the emphasis towards the ability to adapt and self manage in the face of social, physical, and emotional challenges… BMJ 2011; 343: d 4163 doi: 10. 1136/bmj. d 4163

Why is defining health so important? The answer? : The way in which people think about health and well being influences their health behaviours. Hughner & Kleine (2004). Thus in order to effectively promote health, we need to interrogate its meaning (UKPHR indicator 5 e) to: Individuals An individual’s perspective and expectation of health is highly fluid and interchangeable (depending on both their characteristics and experiences) – – Lay concepts of health Young Vs old Women Vs men Lower socioeconomic groups Societal / Cultural – Health & illness influenced by magic / witch craft, fatness seen as healthy, etc.

Factors that influence health The factors which influence health are: – multiple and interactive – both within and outside an individual’s control – modifiable or non-modifiable Health promotion is fundamentally concerned with action and advocacy to address the full range of potentially modifiable determinants of health: – not only those which are related to the actions of individuals (health behaviours and lifestyles) – but also factors such education, employment and working conditions and the physical environments. Non-modifiable determinants of health: – biology and genetics.
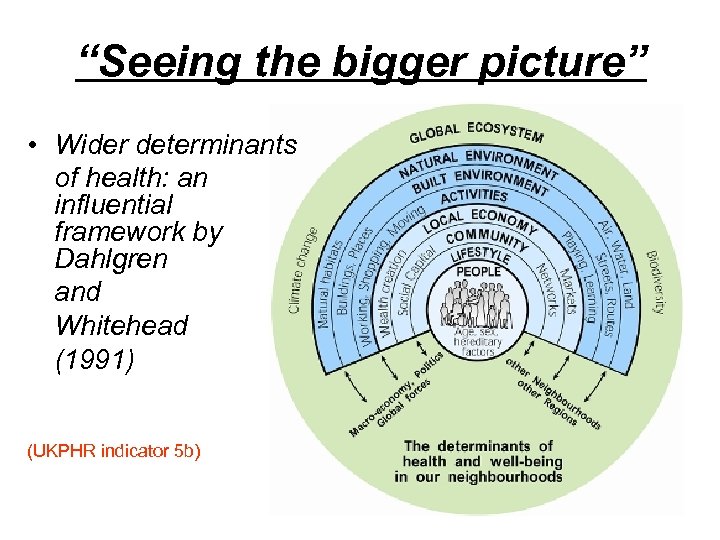
“Seeing the bigger picture” • Wider determinants of health: an influential framework by Dahlgren and Whitehead (1991) (UKPHR indicator 5 b)

Dahlgren and Whitehead (1991) Illustration of the wider determinants of health, identifying layers which influence health from individual to societal to global. Used to flag inequalities in health, identifying socio-economic, cultural and environmental factors which affect health. Identifies the need for structural interventions to impact on the causes.

Social Determinants of Health • The social determinants of health “are the conditions in which people are born, grow, live, work and age, including the health system”. – These circumstances are shaped by the distribution of money, power and resources at global, national and local levels, which are themselves influenced by policy choices. • Healthy public policy = “characterized by an explicit concern for health and equity in all areas of policy, and by an accountability for health impact. The main aim…to create a supportive environment to enable people to lead healthy lives…makes healthy choices possible or easier. It makes social and physical environments health enhancing”. (WHO Health Promotion Glossary) • The social determinants of health are mostly responsible for health inequities – the unfair and avoidable differences in health status seen within and between countries.

Inequalities in health • What are health inequalities? • Examples of ways of measuring inequalities: – Individual level – Area level • Explanations for inequalities? • UKPHR indicator 5 d

What are health inequalities? • Inequality: unequal “differences in health status, or in the distribution of health determinants, between different population groups”. • Deprivation: a relative and broad concept, referring to not having something that others have. “a state of …observable and demonstrable disadvantage relative to the local community or the wider society or nation to which an individual, family or group belong. ” (Townsend, 1987). • Inequality Vs Inequity

Measuring inequalities • Individual level: socio-economic position Education, occupation, social class, employment status, income, access to amenities, housing, etc. • Ecological/Area level: deprivation Townsend, Carstairs, Jarman, Indices of Deprivation 2010, etc.

If you’re really keen… • The Indices of Deprivation 2010 (ID 2010) is the 3 rd release in a series of statistics produced to measure multiple forms of deprivation at the small spatial scale. • Updates the Indices of Deprivation 2007 and 2004 – retaining broadly the same methodology, domains and indicators 145 pages later…. http: //www. communities. gov. uk/pu blications/corporate/statistics/indic es 2010 technicalreport

Explanations for inequalities? Artefact • Artefact, biases and changes in the way the statistics are produced. Social factors • Social selection • Stressors & coping capacity Behaviour • Lifestyle factors Material circumstances • Poverty • Poor environments

TASK 1: Understand the key terms around health promotion Mapping of the World Health Organisation (WHO) Health Promotion Glossary of key terms. This Health Promotion Glossary was prepared on behalf of WHO by Don Nutbeam. Includes both basic and an extended list of 54 terms which are commonly used in health promotion. (UKPHR indicator 5 c) FIND THIS GLOSSARY AT: http: //www. who. int/healthpromotion/about/HPG/en/

Time for a short break…

PART 2 - Agenda Learning Outcome 3: Discuss the role of theories and models of health and health promotion, and understand how to find and use them. Learning Outcome 4: Understand the importance of evidence and policy and its impact of health promotion. The role of theory and evidence in health promotion • • What is theory / different types Theoretical perspectives / using theories in context The role of evidence Group work task

What is theory? • The ‘journey’ from A to Z, or ‘present state to health improvement’ – Not just one step or academic theory, e. g. “We used the transtheoretical model”. • Purpose: so that everybody understands it – You and your team, commissioner, client, wider PH etc. – Success in implementation can be measured – It can be replicated and adapted by you and others • Ask yourself: – What are you trying to do? – How is it supposed to work? – What needs to be in place for it to work?

Types of theory • • • Management and business Psychology and behaviour Communications Community / social And many, many others… Several theories (or none? ) can be used to build your own intervention’s theoretical pathway.

A very useful introduction to health promotion theory Today isn’t about us teaching you all the different health promotion theories or models… For further reading: this book is recommended.

Theoretical perspectives? • Is it possible to promote public health successfully without an understanding of some of theoretical, conceptual or research issues than underpin public health practice? – The answer is probably yes. • However, to promote health effectively, practice should be underpinned by relevant knowledge (theoretical, conceptual, methodological) AND appropriate skills AND…

Depending on the context! • When promoting health, practitioners may draw from the many theories and models from different disciplines, depending on their focus. • Theories and models can be categorised in a variety of ways, but the key to ensure those chosen are appropriate to the task. • Therefore, match theory to the task and context.

Why re-invent the wheel? • Finding and using promising and evidence based practices, as well as models and tools developed by others, is an important way to learn from one another as we strive to deliver the most effective initiatives possible • Increasingly, we are able to base health promotion decisions and interventions on evidence. This involves using information derived from formal research, and program evaluation. • Thus our evidence base for health promotion could draw from theory / models, research and practice.

The role of evidence • We live in an ‘evidence-based’ world. • Several steps: – – Find it: know how to use resources (or who to ask) Appraise quality: is it any good? Appraise results: is it effective? Appraise relevance: is it important to me? Can it be applied locally? • Problems with HP evidence: – Often ‘grey’ – ask the experts – Often pragmatic / ‘low quality’ – Often complex and specific

Lessons learned from practice • It isn’t ‘evidence based’ if your evidence only explains some of it. • Understand context of intervention: will this work with my population/organisation? • Some things with no evidence may still be worth doing – this is hard to explain to commissioners!

TASK 2: Matching evidence to the task and context • Working with your table as a group. • You will be given a health promotion topic / setting: – – – Alcohol abuse Teenage Pregnancy Breast screening (increasing uptake) Workplace Breastfeeding peer support service Cardiac Rehabilitation

Task 2 (continued) In 15 minutes, discuss in your group how you would: 1. Define the intervention 2. Find evidence to design and implement it • Would you use research, best practice, real-world evaluations, theories/models, etc… 3. Use the evidence that you find • Identify any strengths and weaknesses. • Would the evidence actually be useful in practice? 4. Prepare 1 -2 minutes feedback for the whole group • Describe how you have gone about the task for your topic / setting.

PART 3 - Agenda Learning Outcome 5: Describe the different approaches to health promotion. Approaches to health promotion • Discussion: experiences in health promotion • National policy and its impact on heath promotion • Different health promotion approaches • Group work task

What kinds of experiences do you have of doing health promotion (or health education or health improvement) with citizens in local communities?

Healthy lives, Healthy people (DH, 2010. ) ² ² ² Radical localism: local authorities leading role. ‘Health and well-being boards’: strategic planning for public health. Emphasis on prevention and health improvement. Health improvement not defined clearly. Health promotion by ‘any willing provider’? Key messages: ² Help citizens make better choices. ² Power and responsibility in the hands of the people. ² Strengthen individual’s self esteem, confidence and sense of responsibility. ² Ladder of interventions. ² Least intrusive approach.

What are Health behaviours? ²Health behaviour refers to activity that a well person would engage in order to prevent illness. ²Illness behaviour concerns the behaviour someone would engage in order to find out what is wrong with him or her and to procure a remedy. ²Sick-role behaviour concerns the behaviour a patient engages in to overcome their illness.

The 'ideology of health promotion' Health promotion is concerned with strategies for promoting health. Assumptions (a) good health is a universally shared objective. (b) there is agreement on what being healthy means. (c) there is a scientific consensus about which behaviours facilitate good health.

Health Promotion Approaches Naidoo and Wills (2009) identified five different ‘approaches’. These approaches are not theories or models, but descriptions of the practice of health promotion: ² Medical ² Education ² Behaviour change ² Empowerment ² Social change

Medical Approach - What is it? Aim Reducing morbidity or mortality, by targeting risk groups or risk behaviours with medical interventions. Objectives Detection and prevention to avoid of mitigate disease Process Concepts of primary, secondary and tertiary prevention. Through immunisation, screening, surgery, medication Assumptions Application of Medical knowledge (evidenced based practice) Expertise: technical, professional authority of professionals important. Compliance/concordance by patients required

Medical Approach - An example

Criticisms - Medical Approach ² Conceptualized around absence of disease ² Does not seek to promote positive health ² Ignores the social and environmental dimensions of health ² Encourages dependence on medical knowledge ² Removes health decisions from lay people

Education Approach - What is it? Aim To provide knowledge and information and develop necessary skills so that people can make an informed choice about their health behaviour. Objectives To enable personal choice Process Giving knowledge, information and skills development to make an informed choice. It does not set out to persuade or motivate change in a particular direction. Psychological theories; Cognitive, Affective and Behavioural. Provision of leaflets, booklets Assumptions The relationship between knowledge and behaviour; that by increasing knowledge there will be a change in attitudes which may lead to changed behaviour.

Education Approach - An example

Social Marketing (NSMC, 2006) ² Argued to be different to commercial marketing: values of individual autonomy, equity and social justice integrated. ² Complements other public health and health promotion activities and measures. ² Theory: derived from advertising knowledge, psychology, sociology, social psychology, communication theory, ecological theory. ² Methods: market research, communication, media campaigns, advertising, promoting health literacy. ² Offers potential for assisting with learning and behaviour change.

Criticisms - Education Approach ² Approach used widely, informally and opportunistically, in many settings and sectors. ² Increasing knowledge and changing beliefs or attitudes does not necessarily lead to changes in behaviour.

Behaviour Change Approach. What is it? Aim To increase individuals' knowledge about the causes of health and illness. Objective To bring about changes in individual behaviour through changes in individuals' cognitions. Process Provision of information about health risks and hazards. Conceptually under-pinned by psychological theory. Most commonly top-down expert-led. (targeted/population) Assumption: Humans are rational decision-makers whose cognitions inform their actions. Health a property of individuals. People can make real changes by choosing to. Blameworthy.

Behaviour Change - An example Stages of Change Model (Transtheoretical model, Prochaska & Di. Clemente 1992) – – – Precontemplation Contemplation Planning Action Maintenance Termination

Criticisms - Behaviour Change Approach ² Is unable to target the major socio-economic causes of ill health. ² Operates top-down. ² Assumes that there is a direct link between knowledge, attitudes and behaviour. ² Assumes homogeneity among the receivers of health promotion messages. ² Blameworthy. ² Priority agenda of policy makers, commissioners, managers (but not necessarily clients or citizens)? ² Change may take place over months and years? ² Does not adequately address the problem of ‘endless’ stress in communities where material deprivation is a key social determinant of health?

Do multiple stresses and strains undermine the capacity of those, in poverty, to change?

Empowerment Approach – What is it? Aim To increase control over one's physical, social and internal environments. Objective To empower individuals to make healthy choices. “Health promotion is the process of enabling people to increase control over, and to improve their health” WHO (1984). Process Participatory learning techniques. Assumption Power is a universal resource which can be mobilised by every individual.

Empowerment Approach Techniques • • Participatory learning Group work Problem solving Client-centred counselling Assertiveness training Social skills training Educational drama
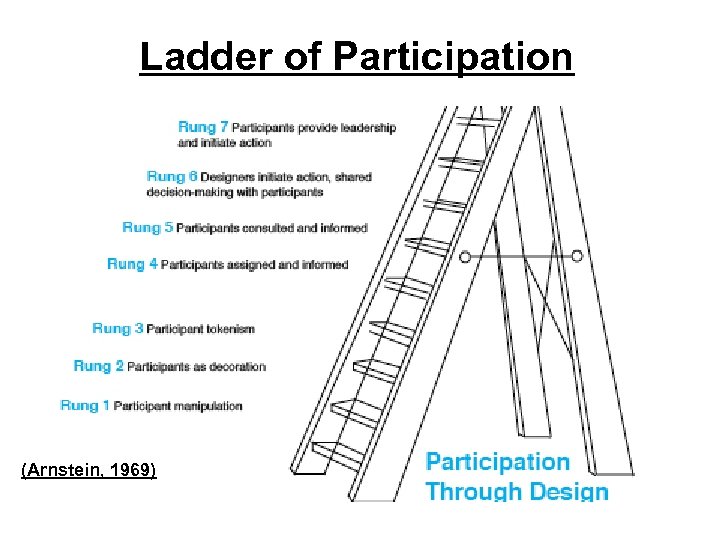
Ladder of Participation (Arnstein, 1969)
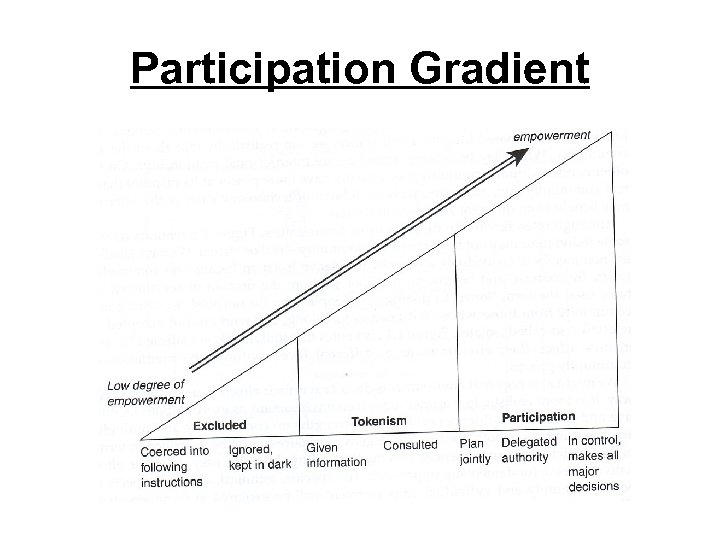
Participation Gradient

Criticisms - Empowerment Approach • It is assumed that rational choices are healthy choices; • Strong reliance upon simulation; • Inadequate concept of power. • What if citizens choose issues that are at odds with health policy priorities? • Long term, time consuming? Cost effective? • Outcomes difficult to measure (as aims may change)? • How serious are policy makers, commissioners and managers about participation? • An under resourced alternative to public investment?

Aim Social Change Approach - What is it? To modify social, economic and physical structures which generate ill health. Objective To improve health by addressing socio-economic and environmental causes of ill health. Process Individuals organize and act collectively in order to change their physical and social environments. Lobbying, change within organisations. Assumption Communities of individuals share interests which allows them to act collectively

Social Change Approach - Some examples ²Changing Organisations (HCAI; Nutritional standards for school meals) ²Changing Communities (Health Action Zones; Healthy Cities; Children’s Centres) ²Changing Policies and Legislation (Seatbelts, Cigarette Advertising, Smokefree legislation)

Criticisms - Social Change Approach ² Most health care professionals have a limited role in developing policy (may be policy literate or implement policy)? ² Wider political activity more likely to take place outside of professional and semi-professional roles (BMA, RCN, UKPHA, Politics of Health Group, trade unions, political parties, social movements)? ² Wider political structural change more possible in societies with strong egalitarian culture e. g. Sweden, Germany, New Zealand (Blank and Burau, 2010)? ² Vulnerable to lack of funding and to official oppositions ² Danger of creeping professionalisation ² Problematic concept of 'community’

Summary 5 approaches identified by Naidoo and Wills (2009): ² Medical ² Educational ² Behaviour change ² Empowerment ² Social change

TASK 3: Applying health promotion approaches In 15 minutes, read the case study and answer these questions in your groups: 1. Which health promotion approach(es) are appropriate for this case and why? 2. Which approach is the highest priority? And why?

Other Approaches ² Settings (hospital, school workplace) ² Lifespan ² Targeted ² Population

PART 4 - Agenda Learning Outcome 6: Give consideration to key areas of health promotion in practice, such as design, planning, barriers to implementation, monitoring and evaluation. Learning Outcome 7: Have an understanding of the realities of developing, implementing and evaluating a complex health promotion intervention (e. g. Health Trainers). Real world implementation: a practical exercise & post mortem • What is a complex intervention? • Designing and planning Health Trainers • Monitoring and evaluating Health Trainers • Barriers to implementing health promotion initiatives

Complex interventions? • Mark Petticrew. When are complex interventions ‘complex’? When are simple interventions ‘simple’? Eur J Public Health (2011) 21(4): 397 -398 The issue of complexity, and how one evaluates complex interventions, remains a key one for health service and public health researchers…. Have a quick read…

What we can take away from the article? • Complex interventions: – May consist of several components. – Some, or all, of the components may contribute to its effect (numerous outcomes) – The components may, or may not, interact. – The components may act at different levels (e. g. at the level of the participant and at the organisational level). – Flexibility in delivery (staff adapting to participants) – Could be “unpacked” and analysed as simple components – BUT… is the whole greater than the sum of the parts? A real life example now…

Real world implementation: a practical exercise & post mortem on NHS Health Trainers NOTE: Please take your coffee during this afternoon’s task

The idea: what is a Health Trainer? • A (relatively) new type of NHS worker • Drawn from, or knowledgeable about, local communities • Trained to provide practical support to improve health • Work 1: 1 with (usually) disadvantaged clients • Assess lifestyle, set goals and support behaviour change • Focus on diet, exercise, smoking and alcohol

TASK 4 a: Where to start? • In groups, imagine that you are a Public Health Practitioner and you have been tasked with implementing ‘Health Trainers’ in England based on the ‘idea’ outlined in the previous slide. • Spend 15 minutes sketching a strategy to develop the Health Trainers idea – don’t worry about lots of detail. Clue: remember this is just a ‘good idea’ at this stage - don’t roll it out across the whole PCT before some further exploration.

Feedback: strategy task

Strategy: key points • Define intervention (theory, evidence, expert opinion, etc. ) • Test on a small scale and evaluate • Roll out incrementally • Programme of evaluation, expansion and continuous improvement (basically the commissioning cycle) • Cost is increasingly important • Involve all stakeholders at each stage, particularly clients

TASK 4 b: Monitoring and Evaluation • It is essential to include evaluation in any implementation plan. • In your groups, spend 10 minutes coming up with some measures that could be used to evaluate Health Trainers.

Feedback: evaluation task

Evaluation: key points Aim for a balance of: • Structure – Service in place, staff in post, funding secured • Process – Number of clients recruited to service, whether clients were in target groups • Outcome – Short term – Clients achieving/maintaining goals, satisfaction – Long term – Reduction in risk factor prevalence/ mortality/morbidity, qualitative change in life

There is no right answer! The Department of Health used the ‘DCRS’ database for Health Trainers.

A common conflict…
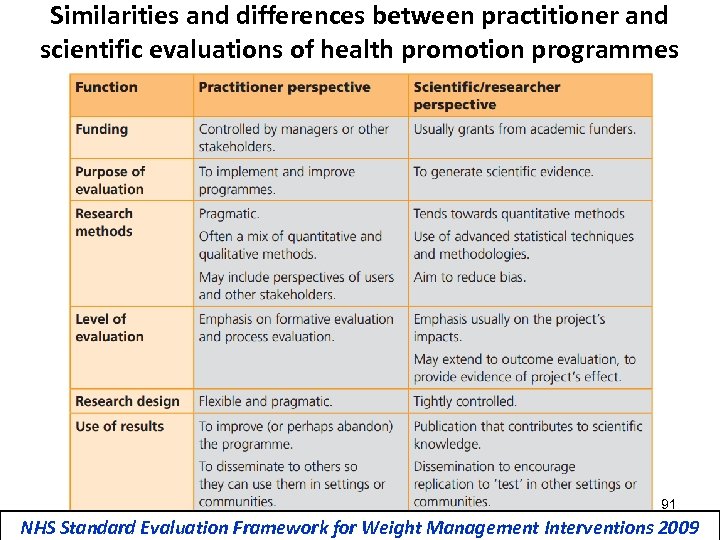

Similarities and differences between practitioner and scientific evaluations of health promotion programmes 91 NHS Standard Evaluation Framework for Weight Management Interventions 2009

A note on controlled trials… • The Medical Research Council advocates controlled trials as part of phased development • What are the advantages disadvantages of this approach? and • Has anybody here ever been involved in a trial?

Trial feasibility • Is it possible to standardise communities? • Is it possible to blind communities? • If an intervention fails to ‘work’, are we sure it’s because it is ineffective?

If in doubt, return to the question you want to answer (but remember that trials are not always the answer)

TASK 4 c: Barriers to implementation In your groups spend 15 minutes identifying the potential barriers to implementing Health Trainers.

Feedback: barriers task

Common barriers • • Resources Communication (in all directions) People (power, politics, negativity) Policy (and shifting goalposts) Ethics Ideology, e. g. libertarianism Demand (or lack of) Lack of clear strategy.

Comments on HT task?

PART 5 Time for some reflection and learning…

Reflection “Follow effective action with quiet reflection-from the quiet reflection will come even more effective action” Peter F Drucker (1909) Educator and Writer

What is it? Reflection provides a structured opportunity for individuals and groups to consider the ramifications of the service they provided. Why? • Better role understanding. • Makes a connection between the service you have provided and the broader social issues that are impacting that population or community. • A time for personal growth when individuals can look within, by processing the knowledge and skills one acquires through service. • Adds meaning and depth to any service project. • Enables better recognition of the positive personal and societal aspects of the activity. • Provides evidence of development for your portfolio.

Models of Reflection • Gibbs (1988) • Johns (1995) • Rolfe et al. (2001).
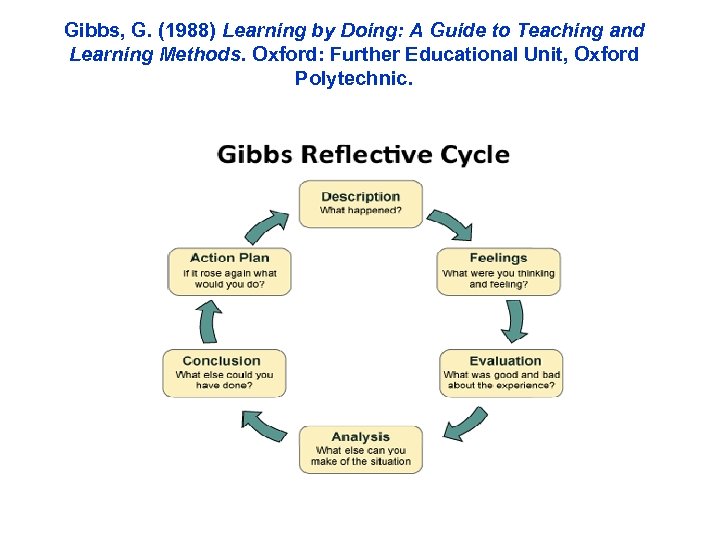
Gibbs, G. (1988) Learning by Doing: A Guide to Teaching and Learning Methods. Oxford: Further Educational Unit, Oxford Polytechnic.

Johns C (1995) Framing learning through reflection within Carper’s fundamental ways of knowing in nursing. Journal of Advanced Nursing. 22, 2, 226 -234 Description of the experience Describe the experience and what were the significant factors? Reflection What was I trying to achieve and what are the consequences? Influencing factors What things like internal/external/knowledge affected my decision making? Could I have dealt with it better? What other choices did I have and what were those consequences? Learning What will change because of this experience and how did I feel about the experience How has this experience changed my ways of knowing • Empirics – scientific • Ethics – moral knowledge • Personal – self-awareness • Aesthetics – the art of what we do, our own experiences

Rolfe, G. , Freshwater, D. , Jasper, M. (2001) Critical Reflection in Nursing and the Helping Professions: a Users Guide. Basingstoke: Palgrave Macmillan; 2001 What: – Describe the situation; achievements, consequences, responses, feelings, and problems. So what: – Discuss what has been learnt; learning about self, relationships, models, attitudes, cultures, actions, thoughts, understanding, and improvements. Now what: –

So…. over to you!

And finally… Please provide some feedback for us…

Thank you and safe journey home! Best wishes Kathy, Amanda & Beck
98911ae7828c32ccdd4c40a07ae0f545.ppt