563c4f884bf12d9eeca785ed6ddf4e44.ppt
- Количество слайдов: 28

Health Care Workers Screening: A Public Health Strategy Dr. Rasha Salama M. Sc. , Ph. D Public Health- Suez Canal University Dubai Health Authority

Burden of HCAI • Health care-associated infections occur worldwide and affect both developed and resource-limited countries. • About 5%– 10% of patients admitted to acute care hospitals in developed countries acquire health care-associated infections and the risk of acquiring infection is 5– 20 times higher in developing countries - a growing challenge to quality of health care in the region. • The economic cost of health care-associated infections as well as the opportunity cost to health services is enormous. preventing a case of health care associated infections saves on an average of US$ 10000 and reduces the patient’s risk of death from 7% to 1. 6%. .

Introduction • Health care-associated infections (HCAI) can be acquired anywhere along the continuum of health care settings. • • Affect a large number of patients and health care workers and frequently result in amplification of epidemics. • Impact of health care-associated infections includes ▫ ▫ ▫ ▫ Prolonged hospital stay, Long-term disability, Increased resistance of microorganisms to antimicrobials, Massive additional financial burden for health systems, High cost for patients and their family Unnecessary deaths Low quality of patient care
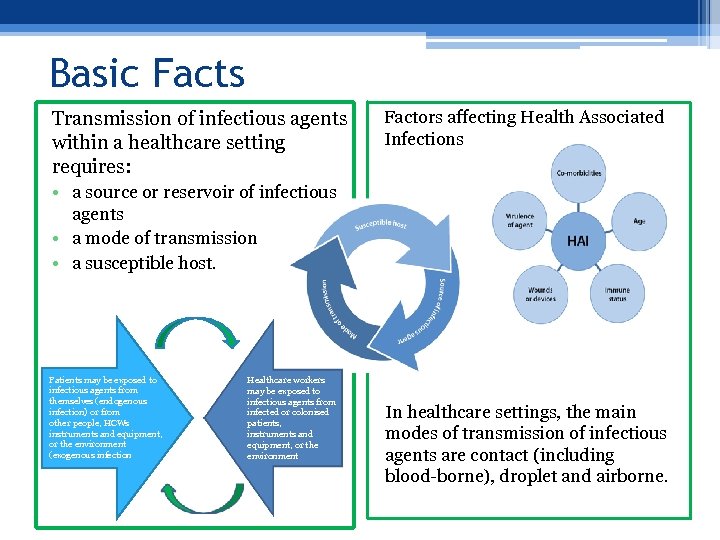
Basic Facts Transmission of infectious agents within a healthcare setting requires: Factors affecting Health Associated Infections • a source or reservoir of infectious agents • a mode of transmission • a susceptible host. Patients may be exposed to infectious agents from themselves (endogenous infection) or from other people, HCWs instruments and equipment, or the environment (exogenous infection Healthcare workers may be exposed to infectious agents from infected or colonised patients, instruments and equipment, or the environment In healthcare settings, the main modes of transmission of infectious agents are contact (including blood-borne), droplet and airborne.

Who are Health Care Workers? A healthcare worker (HCW) is an individual who may have the potential to acquire or transmit an infectious agent during the course of his or her work in the healthcare setting while providing direct care. It may include all persons working in the healthcare facility comprising nursing staff, physicians, lab technicians, home-care workers, students and others.

Screening of health care workers: is it worthwhile? The global burden of hepatitis B (HBV), hepatitis C (HCV), and human immunodeficiency virus (HIV) infection due to percutaneous injuries among health care workers (HCWs) is estimated: • Overall, 16, 000 HCV, 66, 000 HBV, and 1, 000 HIV infections may have occurred in the year 2005 worldwide among HCWs due to their occupational exposure to percutaneous injuries. The fraction of infections with HCV, HBV, and HIV in HCWs attributable to occupational exposure to percutaneous injuries fraction reaches 39%, 37%, and 4. 4% respectively. • These infections are highly preventable and should be eliminated • Estimation of the global burden of disease attributable to contaminated sharps injuries among health-care workers : Am J Ind Med. 2005 Dec; 48(6): 482 -90.
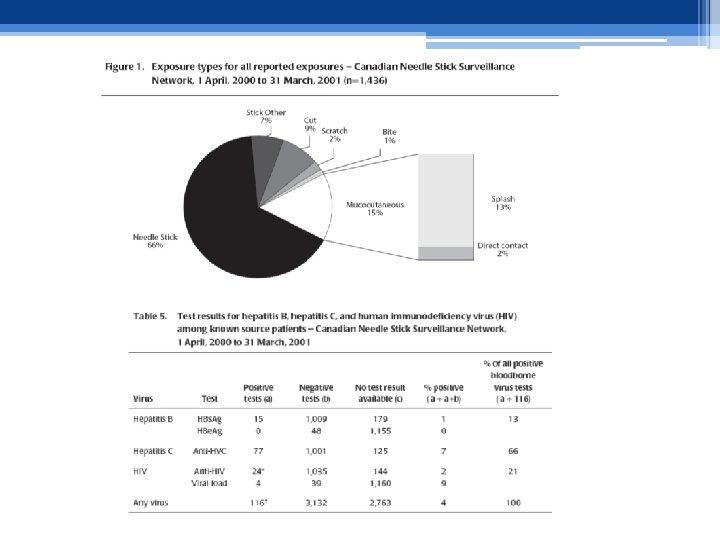
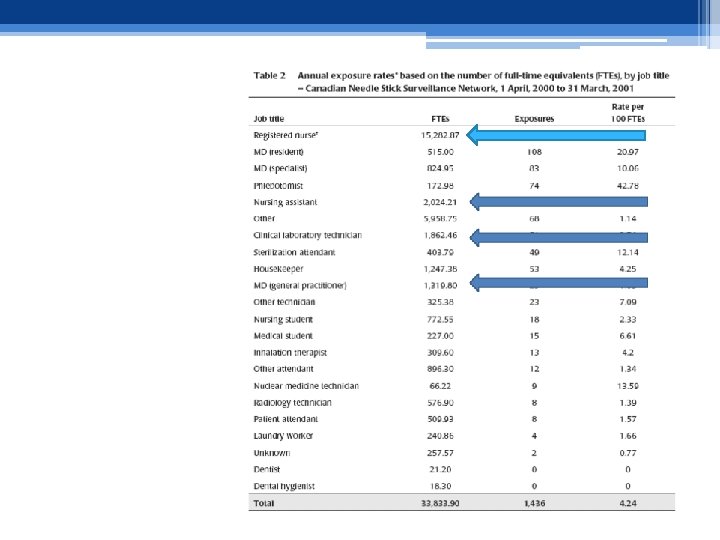

Transmission of blood-borne pathogens in health care settings • The 2009 global burden of disease study revealed that as many as 5%– 10% of new HIV infections, 30%– 32% of new HBV infections, and around 40% of new HCV infections in low and middle-income countries may be attributable to exposure in health care settings, including unsafe injections, unsafe blood and occupational exposures (25).

Infection prevention and control is everybody’s business! • The current global evidence clearly demonstrates that a considerable proportion of the burden of disease attributable to health care-associated infections can be prevented with low-cost interventions. • The implementation of evidence-based infection control measures needs more public health actions and organizational control for universal application of evidence-based prevention and control practices, compliance with those practices, behavioral change, risk management, standardized surveillance methods, and quality assurance

The Goal • Effective infection prevention and control is central to providing high quality health care for ▫ patients and ▫ a safe working environment for those that work in healthcare settings. • GOAL: The creation of safe healthcare environments through the implementation of practices that minimize the risk of transmission of infectious agents.

Policy for Infection Control in Health Care Facilities • Personal Hygiene • Employee Health ▫ Employee health: Initial and periodical physical examination, communicable diseases screening, vaccination (hepatitis B, influenza, other vaccinations) ▫ Prevention of occupational exposure to blood borne pathogens (e. g. HBV, HCV and HIV) and post-exposure prophylaxis • Prevention, surveillance, control and reporting of health-care acquired infections • Surveillance, management and reporting of multi-resistant pathogens or pathogens with relevant resistance; antimicrobials policy • Isolation precautions and management of specific infectious diseases • Cleaning and disinfection • Sterilization and storage of sterile supplies • Unit specific infection control • Infection control in supply and disposal • Environmental and Engineering Controls

Positive Aspects of Policy Application • Providing a healthy, safe environment free of risk of transmission of infection between patient and health care provider. • Ensuring means of prevention, such as providing immunization services and changing the workplace in some required cases. • Confirming the application of health care workers screening policy for all workers in the public and private health sectors.

Action plan ……………. . • Formation of a team of specialists from different parties • Current situation analysis • Review of legislation and laws • Provide scientific evidence and best practices • Initial development of the proposed policy • Discussion of the proposal with relevant authorities and stakeholders • Final Edition of the policy

Evidence base • The policy was based on the best available evidence and knowledge of the practicalities of clinical procedures. • They draw from other work in the area, including the national, international infection control guidelines and policies, systematic literature reviews conducted to inform the development of this policy, work on HAI prevention from CDC, WHO, SHEA guidelines, US preventive Task force, Canadian Task force on Preventive Healthcare, national discipline-based infection control guidelines, and National Standards laws and regulations relevant to infection prevention and control.

Objectives • Confirm that HCWs are free of infectious diseases • Assure safety of Patients/co-patients • Provision of preventive services • Provision of the appropriate early management

The Main Domains • Diseases that must be screened: - AIDS - Hepatitis B and C - Pulmonary tuberculosis - Chickenpox - Syphilis • Determination of the measures of prevention
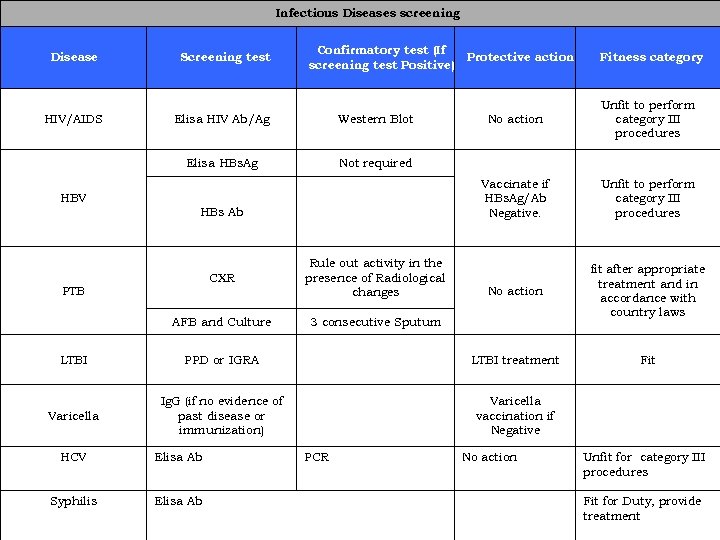
Infectious Diseases screening Disease HIV/AIDS Screening test Confirmatory test (If Protective action screening test Positive) Western Blot No action Unfit to perform category III procedures Vaccinate if HBs. Ag/Ab Negative. Elisa HIV Ab/Ag Elisa HBs. Ag HBV Fitness category Unfit to perform category III procedures No action fit after appropriate treatment and in accordance with country laws Fit Not required HBs Ab CXR Rule out activity in the presence of Radiological changes AFB and Culture 3 consecutive Sputum PTB LTBI PPD or IGRA LTBI treatment Varicella Ig. G (if no evidence of past disease or immunization) Varicella vaccination if Negative HCV Elisa Ab Syphilis Elisa Ab PCR No action Unfit for category III procedures Fit for Duty, provide treatment

Category I Procedures with the minimum risk of blood borne virus transmission q. Regular history-taking and/or physical or dental examinations, q. Routine dental preventive procedures q. Routine rectal or vaginal examination q. Minor surface suturing q. Elective peripheral phlebotomy

Category II Procedures for which blood borne virus transmission is theoretically possible but unlikely q. Locally anesthetized ophthalmologic surgery q. Locally anesthetized operative, prosthetic, and endodontic dental procedures q. Periodontal scaling and root planting q. Minor local procedures (e. g. , skin excision, abscess drainage, biopsy) q. Percutaneous and other minor orthopedic procedures q. Subcutaneous pacemaker implantation q. Bronchoscopy q. Upper gastrointestinal tract endoscopic procedures

Category III Procedures for which there is definite risk of blood borne virus transmission q. General surgery q. General oral surgery, including surgical extraction, tissue biopsy q. Cardiothoracic surgery q. Neurosurgery. q. Obstetrical/gynecological surgery, including cesarean delivery, hysterectomy, forceps delivery q. Orthopedic procedures q. Trauma surgery, including open head injuries, facial and jaw fracture

Interventions following Screening Support, awareness and direction Provide vaccinations Transfer to low risk area or job 1. Counseling for HCWs with positive results 2. Raising awareness: • Risk and mode of transmission. • Personal protective measures • Hepatitis B • Varicella • Others: Influenza, Tetanus, Pneumococcal • From area/job of high risk of transmission to a low risk one • Based on type of work and infection • Standard classification of 3 categories

Evidence for Action

Evidence for Action (cont. )

Hepatitis B, Varicella vaccination, and optional vaccines • Hepatitis B vaccination is recommended for all healthcare workers - 3 doses • Booster doses are not recommended for persons with normal immune status who were vaccinated. • All HCWs lacking immunity to varicella should receive two doses of varicella vaccine, 4 weeks apart, unless contraindicated. • Flu vaccine is recommend for all HCWs annually. Only the inactivated vaccine if any immuno-compromised state exists. • Tetanus and Diphtheria vaccinations are indicated if there is history of incomplete primary vaccination or if the last booster was more than 10 years ago. • Pneumococcal vaccine: Recommended for all HCWs above 65 years -single dose

HCWs with NCDs • • • Screening for NCDs is important. Confirm diagnosis Provision of counseling Direction for management and follow-up. Assure life style modification.

Desired Outcomes • Reducing transmission rates through health facilities. • Ensuring the quality of health services provided by the healthy care workers in the health sector • Reducing the cost of treatment for workers in case of exposure to infection - the indirect cost

Thank You
563c4f884bf12d9eeca785ed6ddf4e44.ppt