1a8bf4332e608ca9bb9ce30acc2362d5.ppt
- Количество слайдов: 22

Health. Bound Get in the Game to Re-direct the U. S. Health System Bobby Milstein Centers for Disease Control and Prevention BMilstein@cdc. gov Syndemics Prevention Network Jack Homer Gary Hirsch Homer Consulting JHomer@comcast. net Independent Consultant GBHirsch@comcast. net The name “Health. Bound” is used courtesy of Associates & Wilson, Inc. …In support of Healthiest Nation
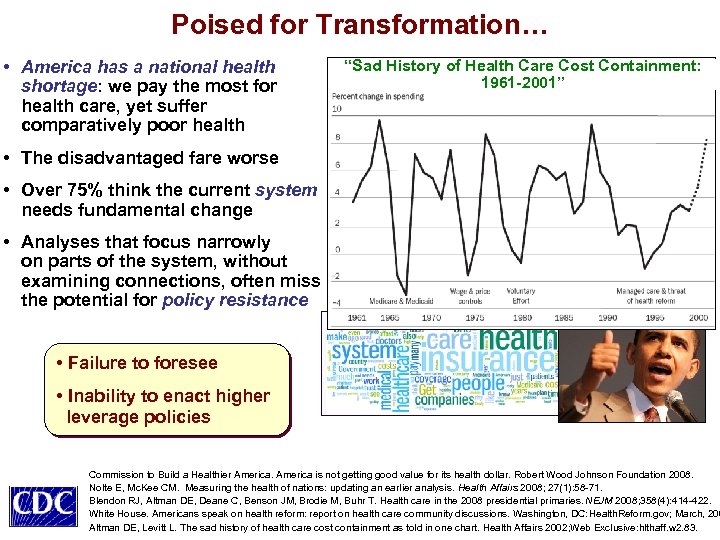
Poised for Transformation… • America has a national health shortage: we pay the most for health care, yet suffer comparatively poor health “Sad History of Health Care Cost Containment: Persistent Money for Shorter Income in Health by More Gaps 1961 -2001” Lives Percent of Adults with Activity Limitation • The disadvantaged fare worse • Over 75% think the current system needs fundamental change • Analyses that focus narrowly on parts of the system, without examining connections, often miss the potential for policy resistance • Failure to foresee • Inability to enact higher leverage policies Commission to Build a Healthier America is not getting good value for its health dollar. Robert Wood Johnson Foundation 2008. Nolte E, Mc. Kee CM. Measuring the health of nations: updating an earlier analysis. Health Affairs 2008; 27(1): 58 -71. Blendon RJ, Altman DE, Deane C, Benson JM, Brodie M, Buhr T. Health care in the 2008 presidential primaries. NEJM 2008; 358(4): 414 -422. White House. Americans speak on health reform: report on health care community discussions. Washington, DC: Health. Reform. gov; March, 200 Altman DE, Levitt L. The sad history of health care cost containment as told in one chart. Health Affairs 2002; Web Exclusive: hlthaff. w 2. 83.
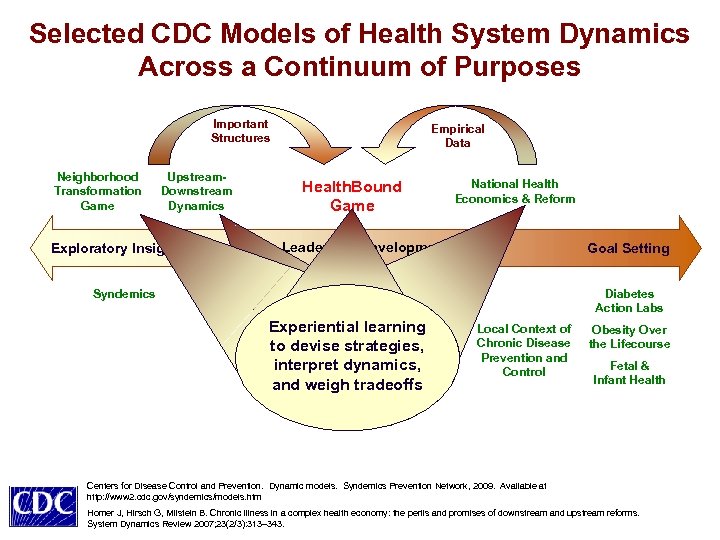
Selected CDC Models of Health System Dynamics Across a Continuum of Purposes Important Structures Neighborhood Transformation Game Upstream. Downstream Dynamics Exploratory Insight Empirical Data Health. Bound Game National Health Economics & Reform Leadership Development Goal Setting Syndemics Inflationary trends Causal diagrams with Experiential learning Creative and self-sustaining practical policies for to devise definitions strategies, moving out of an tendencies of the of states, dynamics, interpret rates, and entrenched and downstream andinterventions weigh tradeoffs unhealthy state healthcare industry Diabetes Action Labs Local Context of Chronic Disease Prevention and Control Obesity Over the Lifecourse Fetal & Infant Health Centers for Disease Control and Prevention. Dynamic models. Syndemics Prevention Network, 2009. Available at http: //www 2. cdc. gov/syndemics/models. htm Homer J, Hirsch G, Milstein B. Chronic illness in a complex health economy: the perils and promises of downstream and upstream reforms. System Dynamics Review 2007; 23(2/3): 313– 343.

Health. Bound is a Simplified Health System to be Explored Through Game-based Learning Health. Bound • • Cognitive and experiential learning for health leaders Four simultaneous goals: save lives, improve health, achieve health equity, and lower health care cost Intervene without expense, risk, or delay Not a prediction, but a way for diverse stakeholders to explore how the health system can change Milstein B, Homer J, Hirsch G. The "Health. Bound" policy simulation game: an adventure in US health reform. International System Dynamics Conference; Albuquerque, NM; July 26 -30, 2009.
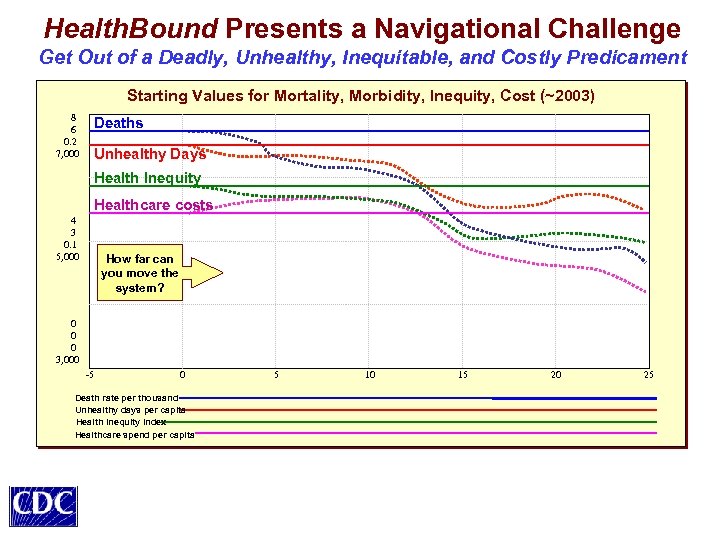
Health. Bound Presents a Navigational Challenge Get Out of a Deadly, Unhealthy, Inequitable, and Costly Predicament Starting Values for Mortality, Morbidity, Inequity, Cost (~2003) 8 6 0. 2 7, 000 Deaths Unhealthy Days Health Inequity Healthcare costs 4 3 0. 1 5, 000 How far can you move the system? 0 0 0 3, 000 -5 0 Death rate per thousand Unhealthy days per capita Health inequity index Healthcare spend per capita 5 10 15 20 25
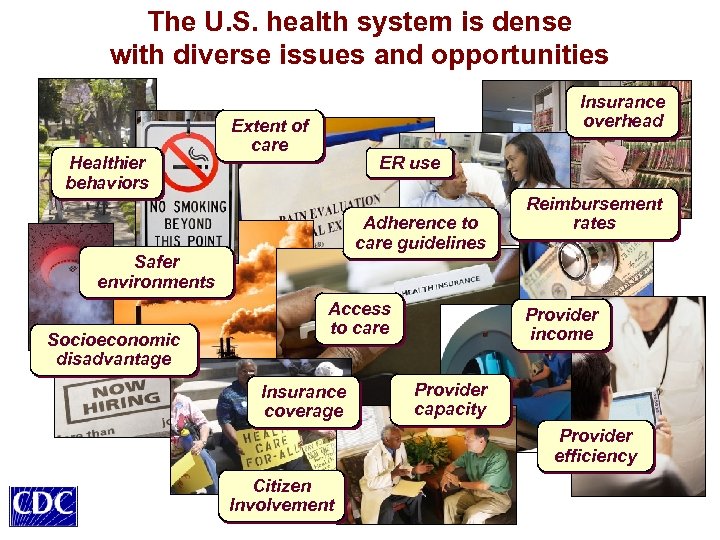
The U. S. health system is dense with diverse issues and opportunities Healthier behaviors Insurance overhead Extent of care ER use Adherence to care guidelines Safer environments Socioeconomic disadvantage Access to care Insurance coverage Reimbursement rates Provider income Provider capacity Provider efficiency Citizen Involvement
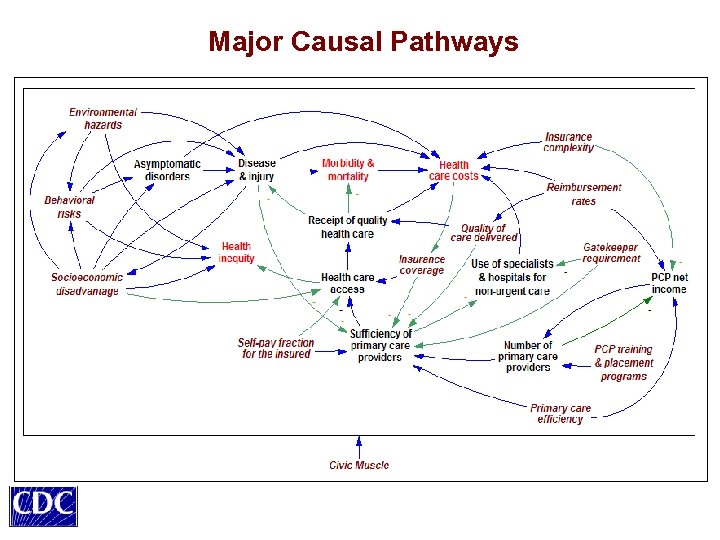
Major Causal Pathways

Science Behind the Game Integrating prior findings and estimates • On costs, prevalence, risk factors, inequity, utilization, insurance, quality of care, etc. (8 databases and large professional literatures) Using sound methodology • Reflecting real-world accumulations, resource constraints, delays, behavioral feedback Simplifying as appropriate • Three states of health: Healthy, Asymptomatic disorder, Disease/injury • Two SES categories: Advantaged, Disadvantaged (allowing study of disparities and equity) • Some complicating trends not included in simplified game (e. g. , aging, technology, economy); an extended model incorporates such factors

Combining Information into a Single Testable Framework
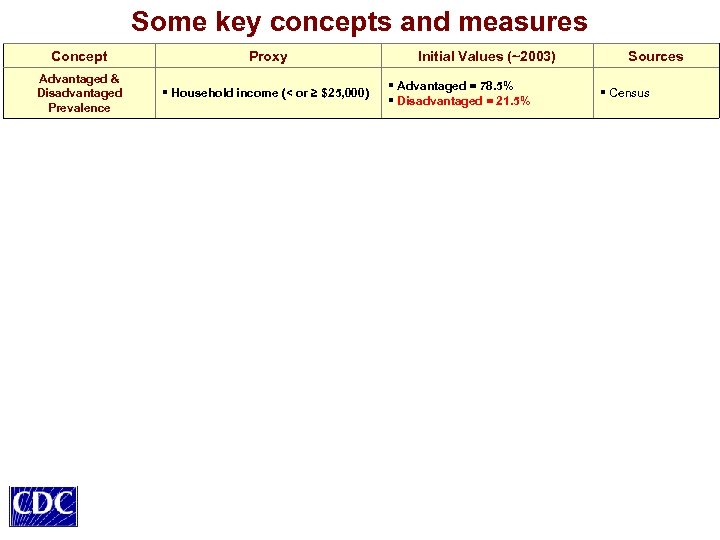

Some key concepts and measures Concept Proxy Advantaged & Disadvantaged Prevalence § Household income (< or ≥ $25, 000) Initial Values (~2003) § Advantaged = 78. 5% § Disadvantaged = 21. 5% Sources § Census
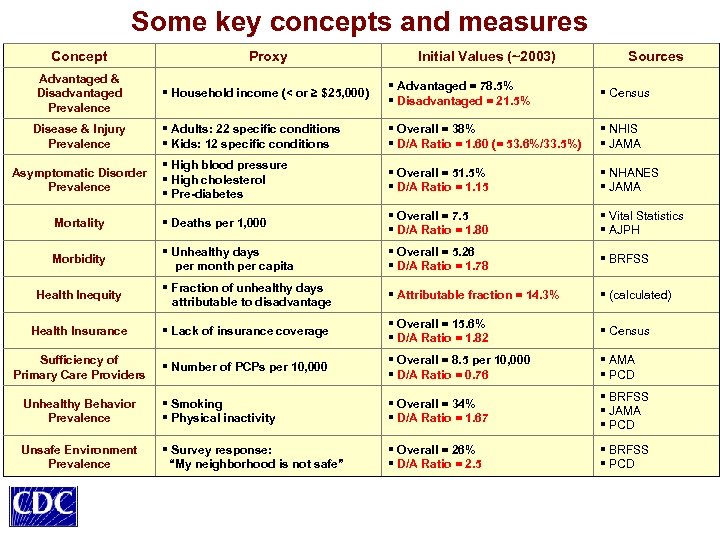
Some key concepts and measures Concept Proxy Advantaged & Disadvantaged Prevalence § Household income (< or ≥ $25, 000) § Advantaged = 78. 5% § Disadvantaged = 21. 5% § Census § Adults: 22 specific conditions § Kids: 12 specific conditions § Overall = 38% § D/A Ratio = 1. 60 (= 53. 6%/33. 5%) § NHIS § JAMA § High blood pressure § High cholesterol § Pre-diabetes § Overall = 51. 5% § D/A Ratio = 1. 15 § NHANES § JAMA Mortality § Deaths per 1, 000 § Overall = 7. 5 § D/A Ratio = 1. 80 § Vital Statistics § AJPH Morbidity § Unhealthy days per month per capita § Overall = 5. 26 § D/A Ratio = 1. 78 § BRFSS Health Inequity § Fraction of unhealthy days attributable to disadvantage § Attributable fraction = 14. 3% § (calculated) Health Insurance § Lack of insurance coverage § Overall = 15. 6% § D/A Ratio = 1. 82 § Census Sufficiency of Primary Care Providers § Number of PCPs per 10, 000 § Overall = 8. 5 per 10, 000 § D/A Ratio = 0. 76 § AMA § PCD Unhealthy Behavior Prevalence § Smoking § Physical inactivity § Overall = 34% § D/A Ratio = 1. 67 § BRFSS § JAMA § PCD Unsafe Environment Prevalence § Survey response: “My neighborhood is not safe” § Overall = 26% § D/A Ratio = 2. 5 § BRFSS § PCD Disease & Injury Prevalence Asymptomatic Disorder Prevalence Initial Values (~2003) Sources
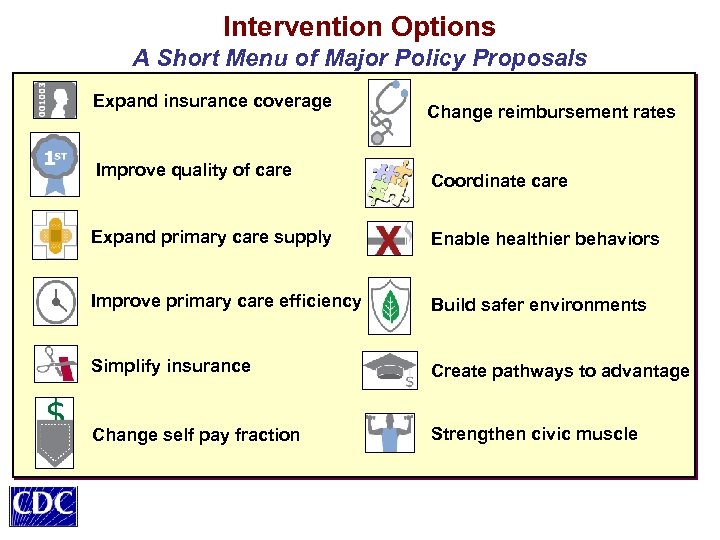
Intervention Options A Short Menu of Major Policy Proposals Expand insurance coverage Improve quality of care Change reimbursement rates Coordinate care Expand primary care supply Enable healthier behaviors Improve primary care efficiency Build safer environments Simplify insurance Create pathways to advantage Change self pay fraction Strengthen civic muscle
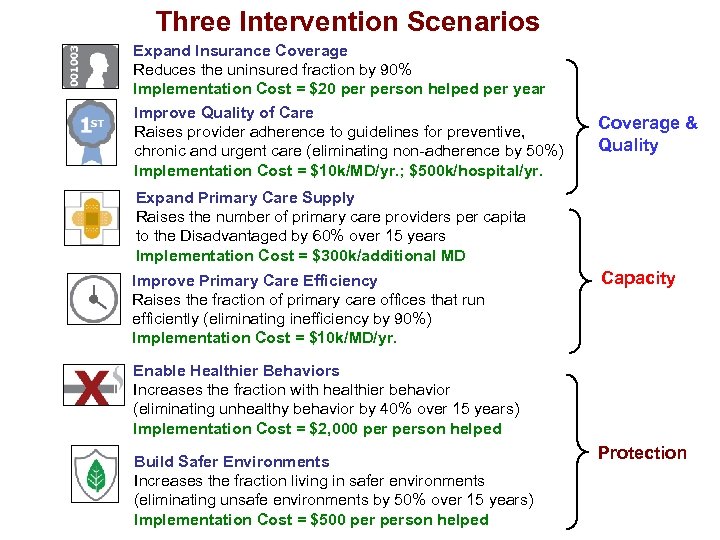
Three Intervention Scenarios Expand Insurance Coverage Reduces the uninsured fraction by 90% Implementation Cost = $20 person helped per year Improve Quality of Care Raises provider adherence to guidelines for preventive, chronic and urgent care (eliminating non-adherence by 50%) Implementation Cost = $10 k/MD/yr. ; $500 k/hospital/yr. Coverage & Quality Expand Primary Care Supply Raises the number of primary care providers per capita to the Disadvantaged by 60% over 15 years Implementation Cost = $300 k/additional MD Improve Primary Care Efficiency Raises the fraction of primary care offices that run efficiently (eliminating inefficiency by 90%) Implementation Cost = $10 k/MD/yr. Capacity Enable Healthier Behaviors Increases the fraction with healthier behavior (eliminating unhealthy behavior by 40% over 15 years) Implementation Cost = $2, 000 person helped Build Safer Environments Increases the fraction living in safer environments (eliminating unsafe environments by 50% over 15 years) Implementation Cost = $500 person helped Protection
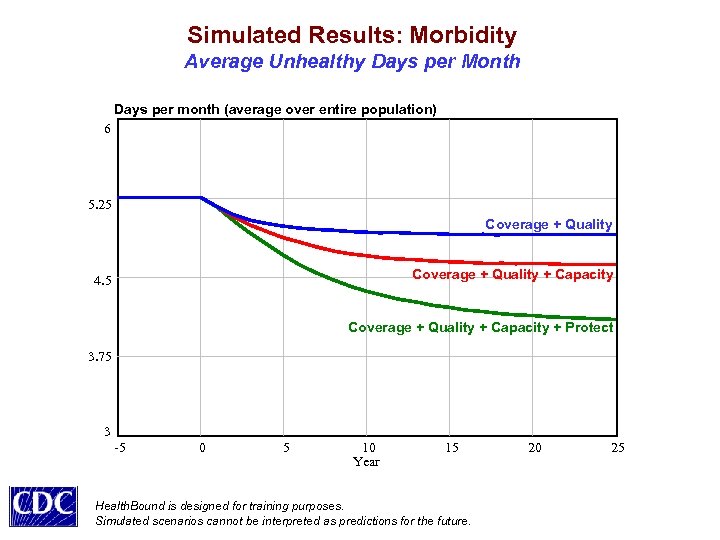
Simulated Results: Morbidity Average Unhealthy Days per Month Days per month (average over entire population) 6 5. 25 Coverage + Quality + Capacity 4. 5 Coverage + Quality + Capacity + Protect 3. 75 3 -5 0 5 10 Year 15 Health. Bound is designed for training purposes. Simulated scenarios cannot be interpreted as predictions for the future. 20 25
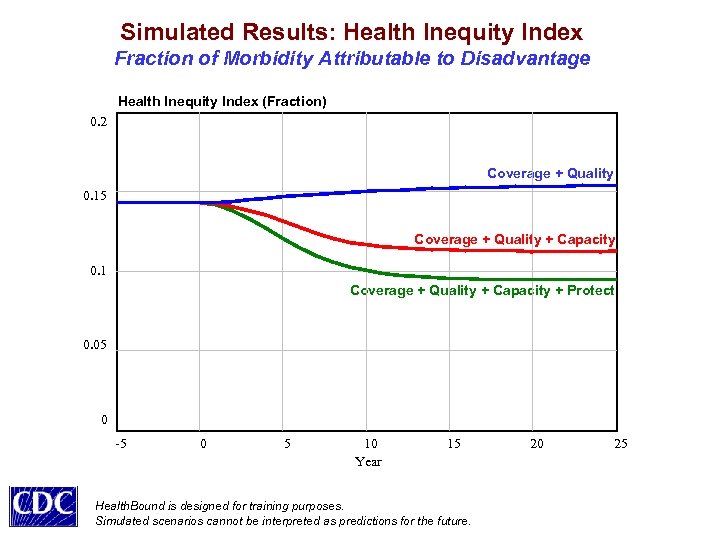
Simulated Results: Health Inequity Index Fraction of Morbidity Attributable to Disadvantage Health Inequity Index (Fraction) 0. 2 Coverage + Quality 0. 15 Coverage + Quality + Capacity 0. 1 Coverage + Quality + Capacity + Protect 0. 05 0 -5 0 5 10 Year 15 Health. Bound is designed for training purposes. Simulated scenarios cannot be interpreted as predictions for the future. 20 25
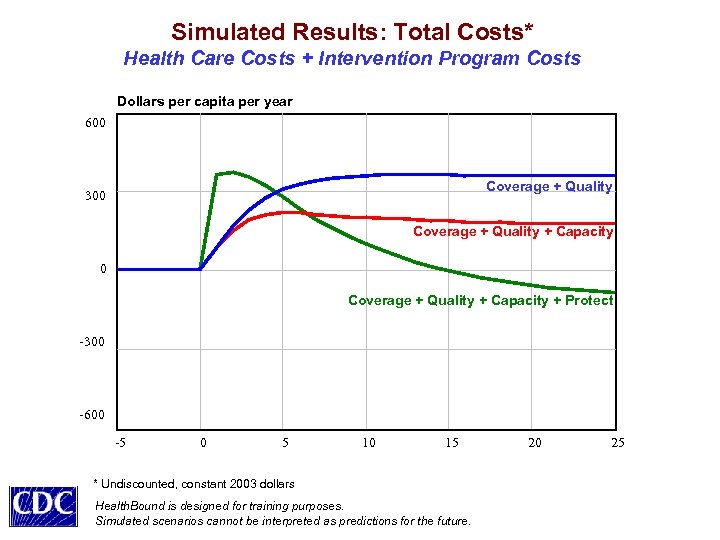
Simulated Results: Total Costs* Health Care Costs + Intervention Program Costs Dollars per capita per year 600 Coverage + Quality 300 Coverage + Quality + Capacity + Protect -300 -600 -5 0 5 10 15 * Undiscounted, constant 2003 dollars Health. Bound is designed for training purposes. Simulated scenarios cannot be interpreted as predictions for the future. 20 25
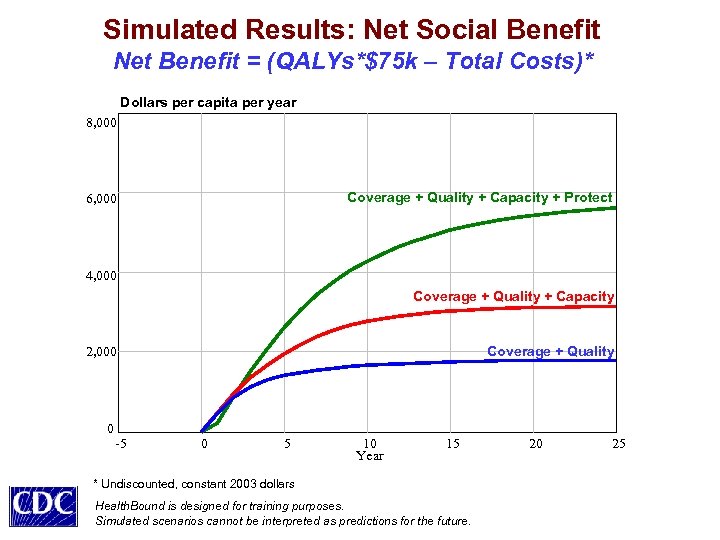
Simulated Results: Net Social Benefit Net Benefit = (QALYs*$75 k – Total Costs)* Dollars per capita per year 8, 000 Coverage + Quality + Capacity + Protect 6, 000 4, 000 Coverage + Quality + Capacity Coverage + Quality 2, 000 0 -5 0 5 10 Year 15 * Undiscounted, constant 2003 dollars Health. Bound is designed for training purposes. Simulated scenarios cannot be interpreted as predictions for the future. 20 25

Some Policy Insights Value Tradeoffs Come to the Foreground • Expanded coverage and higher quality of care may improve health but, if done alone, would likely raise costs and worsen equity • Additional primary care supply and greater efficiency could eliminate current shortages (esp. for the poor), reducing costs and improving equity • Upstream health protection (behavioral + environmental remedies) could reduce costs, elevate health, and improve equity, with an initial investment and a time delay, but the benefits would grow over time Milstein B, Homer J, Hirsch G. Are coverage and quality enough? A dynamic systems approach to health policy. AJPH (under review).
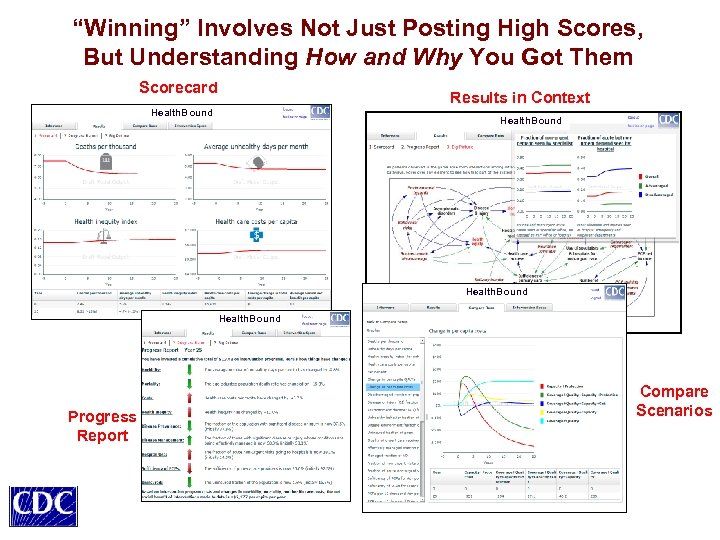
“Winning” Involves Not Just Posting High Scores, But Understanding How and Why You Got Them Scorecard Results in Context Health. Bound Progress Report Compare Scenarios

Why a Game? To Build Foresight, Experience, and Motivation to Act Expert Recommendations Experiential Learning “Wayfinding” Who Has Been Playing? (N~500) • • Citizen organizations • Labor unions • University faculty and students • Think tanks • Syndemics Public health leadership institutes • Prevention Network Federal, state, local health officials Philanthropists
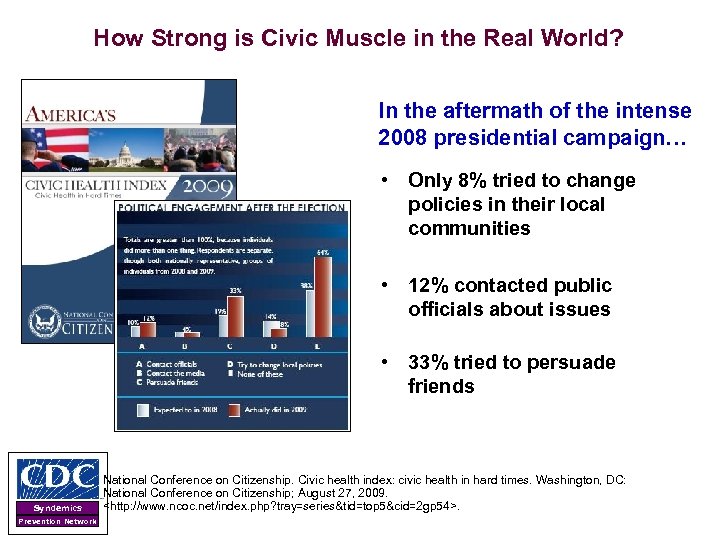
How Strong is Civic Muscle in the Real World? In the aftermath of the intense 2008 presidential campaign… • Only 8% tried to change policies in their local communities • 12% contacted public officials about issues • 33% tried to persuade friends Syndemics Prevention Network National Conference on Citizenship. Civic health index: civic health in hard times. Washington, DC: National Conference on Citizenship; August 27, 2009. <http: //www. ncoc. net/index. php? tray=series&tid=top 5&cid=2 gp 54>.
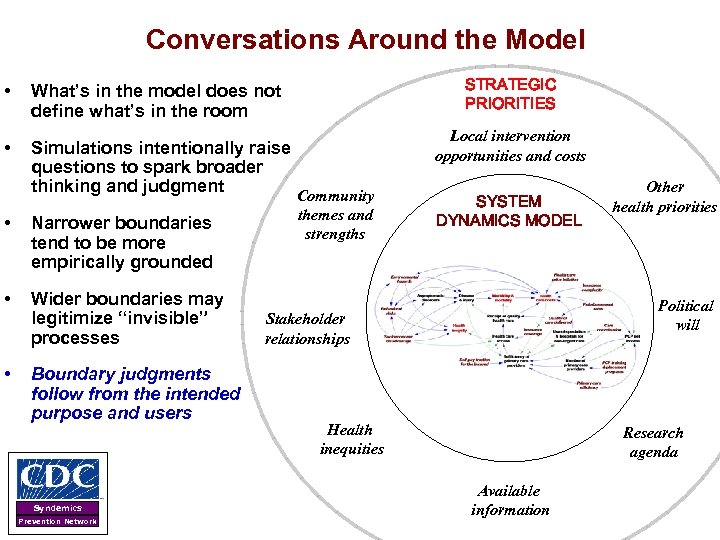
Conversations Around the Model STRATEGIC PRIORITIES • What’s in the model does not define what’s in the room • Simulations intentionally raise questions to spark broader thinking and judgment Community • Narrower boundaries tend to be more empirically grounded • Wider boundaries may legitimize “invisible” processes • Boundary judgments follow from the intended purpose and users Syndemics Prevention Network themes and strengths Local intervention opportunities and costs SYSTEM DYNAMICS MODEL Other health priorities Political will Stakeholder relationships Health inequities Research agenda Available information
1a8bf4332e608ca9bb9ce30acc2362d5.ppt