Headaches.pptx
- Количество слайдов: 48
 Headaches Gerald F. Smith, MPH, MS, PA-C Neurology and Neurophysiology Associates Philadelphia University Spring 2015
Headaches Gerald F. Smith, MPH, MS, PA-C Neurology and Neurophysiology Associates Philadelphia University Spring 2015
 Headache presentation Onset Location Precipitating events Progression Provocative
Headache presentation Onset Location Precipitating events Progression Provocative
 Headache presentation Quality Radiation Timing Severity Associated manifestations
Headache presentation Quality Radiation Timing Severity Associated manifestations
 Classification of headaches Primary Secondary
Classification of headaches Primary Secondary
 Headaches requiring immediate intervention Vascular Infectious Mass lesions Pre-eclampsia CO poisoning
Headaches requiring immediate intervention Vascular Infectious Mass lesions Pre-eclampsia CO poisoning
 CT imaging: “ to contrast or not to contrast” Non-contrast CT of the head is sufficient to exclude intracranial hypertension with impending herniation, hemorrhages, and most types of mass lesions
CT imaging: “ to contrast or not to contrast” Non-contrast CT of the head is sufficient to exclude intracranial hypertension with impending herniation, hemorrhages, and most types of mass lesions
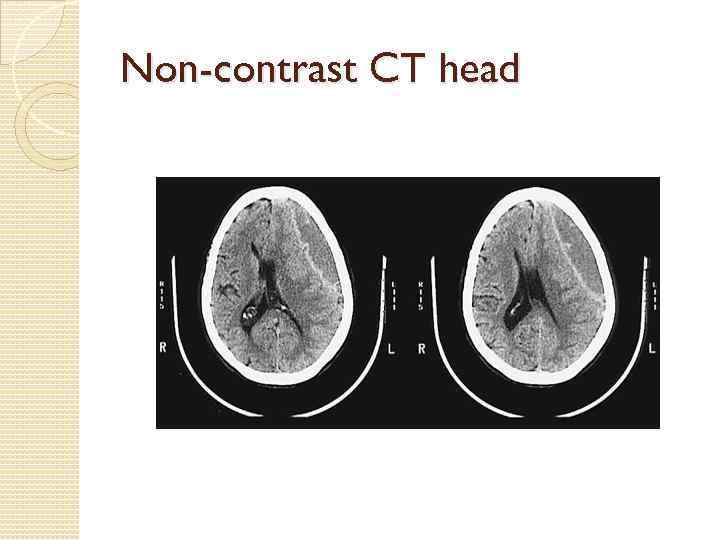 Non-contrast CT head
Non-contrast CT head
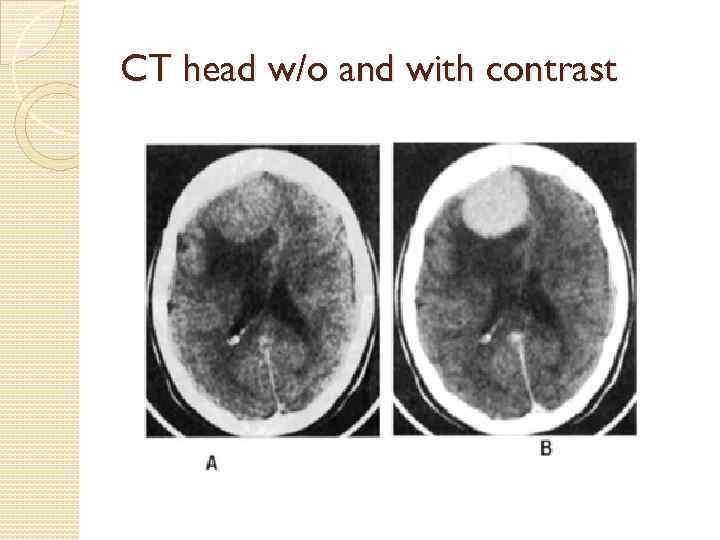 CT head w/o and with contrast
CT head w/o and with contrast
 CT imaging: non-contrast or contrast” However, noncontrast CT may not identify brain abscess, herpes simplex encephalitis, and lymphoma and toxoplasmosis in HIV+ patients Clinical presentation would guide ordering of contrast-enhanced CT
CT imaging: non-contrast or contrast” However, noncontrast CT may not identify brain abscess, herpes simplex encephalitis, and lymphoma and toxoplasmosis in HIV+ patients Clinical presentation would guide ordering of contrast-enhanced CT
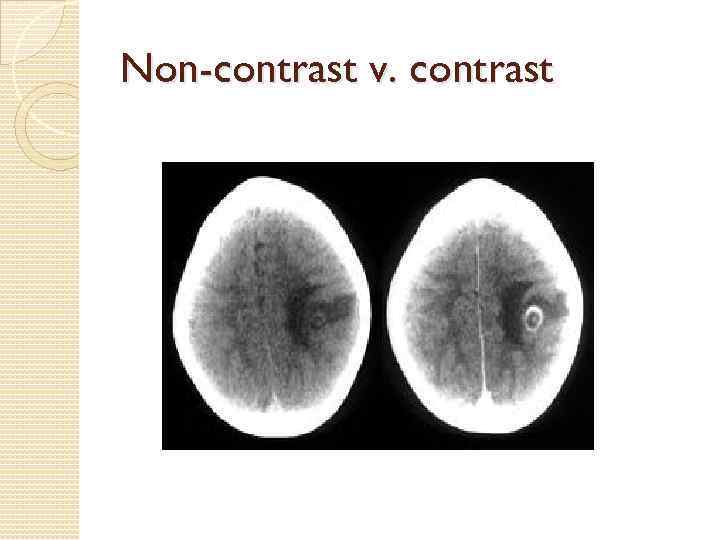 Non-contrast v. contrast
Non-contrast v. contrast
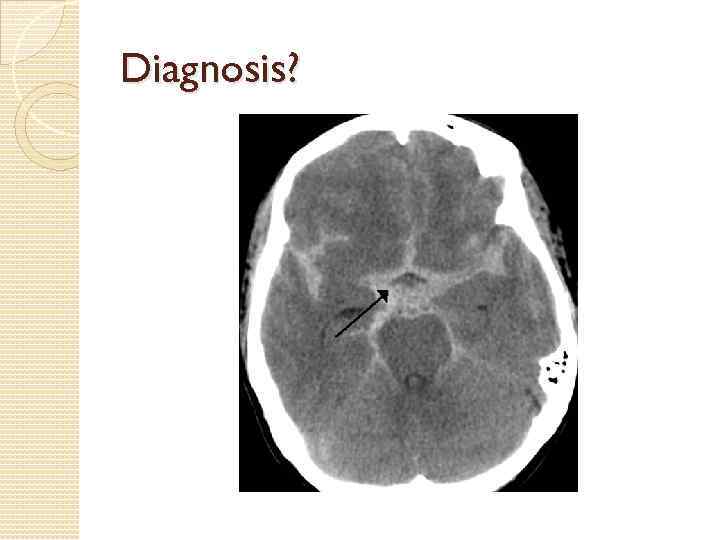 Diagnosis?
Diagnosis?
 Subarachnoid hemorrhage 5 -10% of CVA secondary to SAH Trauma most common cause Spontaneous SAH most often 2˚ to rupture of berry aneurysm Sentinel headache can occur
Subarachnoid hemorrhage 5 -10% of CVA secondary to SAH Trauma most common cause Spontaneous SAH most often 2˚ to rupture of berry aneurysm Sentinel headache can occur
 Subarachnoid hemorrhage “Worst headache of my life” Nausea/vomiting Meningismus Alteration of consciousness Focal deficits often absent
Subarachnoid hemorrhage “Worst headache of my life” Nausea/vomiting Meningismus Alteration of consciousness Focal deficits often absent
 Subarachnoid hemorrhage Risk factors for SAH Ø Older age Ø Female Ø Non-white Ø HTN Ø Tobacco/High ETOH use Ø Previous symptoms Ø Larger aneurysms (>10 mm)
Subarachnoid hemorrhage Risk factors for SAH Ø Older age Ø Female Ø Non-white Ø HTN Ø Tobacco/High ETOH use Ø Previous symptoms Ø Larger aneurysms (>10 mm)
 SAH workup CT (with CTA) STAT! LP Cerebral arteriography (diagnostic and therapeutic). If neg, f/u study p 2 wks
SAH workup CT (with CTA) STAT! LP Cerebral arteriography (diagnostic and therapeutic). If neg, f/u study p 2 wks
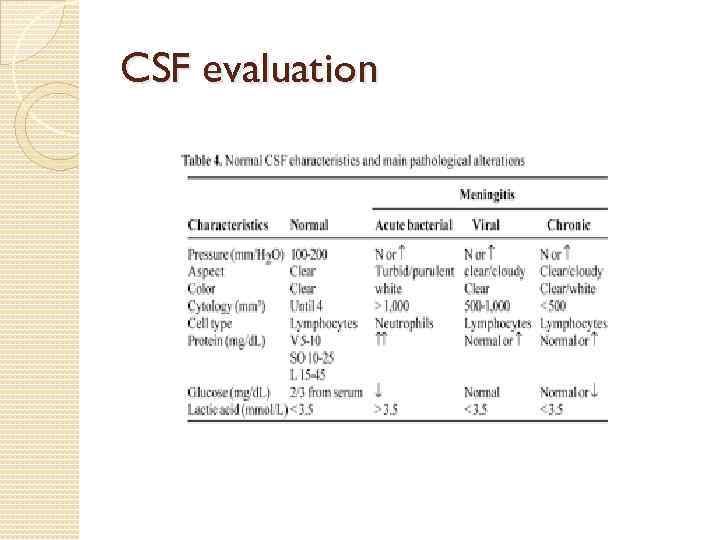 CSF evaluation
CSF evaluation
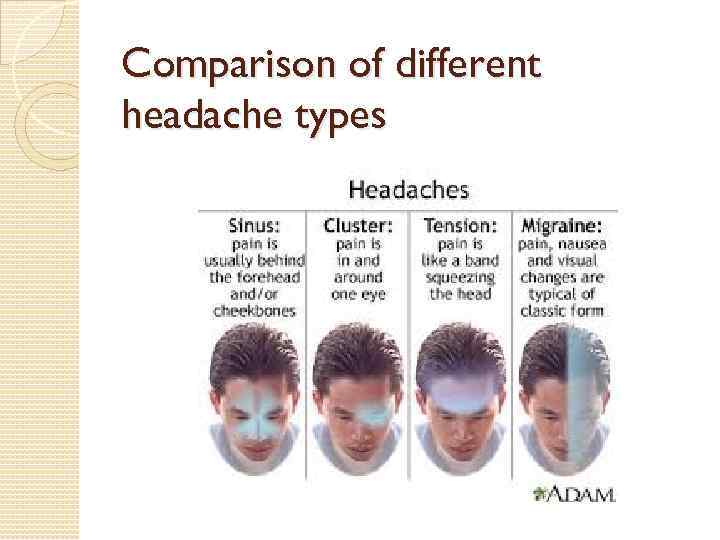 Comparison of different headache types
Comparison of different headache types
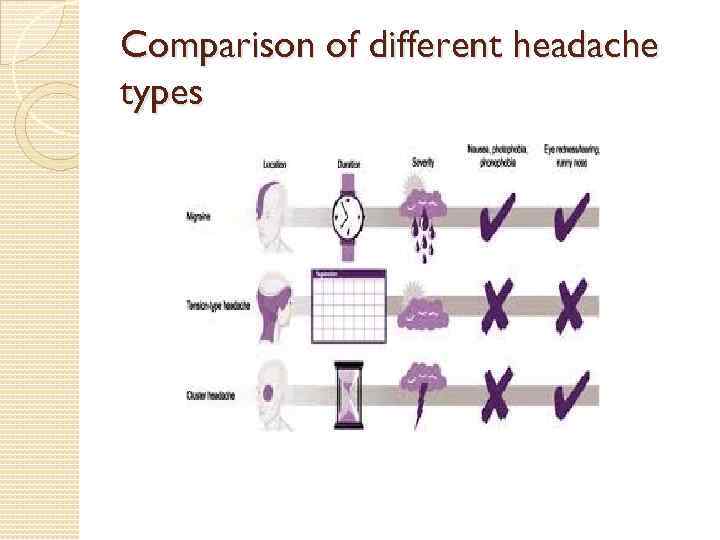 Comparison of different headache types
Comparison of different headache types
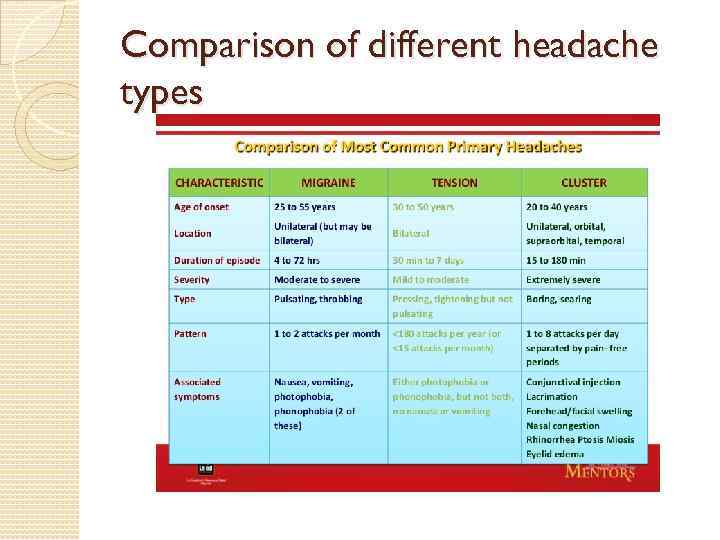 Comparison of different headache types
Comparison of different headache types
 Tension headache Most common type of primary headache Characterized by band-like localization, although they can be generalized Pathophysiology is not well-defined; myofascial component thought to be involved, with secondary activation through trigger points of trigeminal nucleus
Tension headache Most common type of primary headache Characterized by band-like localization, although they can be generalized Pathophysiology is not well-defined; myofascial component thought to be involved, with secondary activation through trigger points of trigeminal nucleus
 Tension headache
Tension headache
 Tension headache Management is multi-factorial Regulation of sleep and meals Exercise Stress management (significant comorbidities include MDD, GAD and panic d/o)
Tension headache Management is multi-factorial Regulation of sleep and meals Exercise Stress management (significant comorbidities include MDD, GAD and panic d/o)
 Tension headache Non-pharmacologic management includes: biofeedback and CBT approaches Pharmacologic: acetaminophen, ibuprofen, naproxen, asa, caffeine If chronic in nature, TCA or anticonvulsants
Tension headache Non-pharmacologic management includes: biofeedback and CBT approaches Pharmacologic: acetaminophen, ibuprofen, naproxen, asa, caffeine If chronic in nature, TCA or anticonvulsants
 Migraine headache
Migraine headache
 Migraine headache Typically begin in adolescence or early adulthood Classically, lateralized in location, throbbing in quality Accompanied by nausea +/- vomiting Photophobia and phonophobia Acute vision changes
Migraine headache Typically begin in adolescence or early adulthood Classically, lateralized in location, throbbing in quality Accompanied by nausea +/- vomiting Photophobia and phonophobia Acute vision changes
 Migraine headache Headaches typically evolve gradually Can last up to 72 hours (+++) Visual phenomena preceding headache (aura) Focal deficits may occur (dysequilibrium, parasthesias, aphasia)
Migraine headache Headaches typically evolve gradually Can last up to 72 hours (+++) Visual phenomena preceding headache (aura) Focal deficits may occur (dysequilibrium, parasthesias, aphasia)
 Migraine headache Basilar artery migraine variant occurs uncommonly Characterized by blindness or binocular visual disturbances Dysarthria, tinnitus, perioral and distal parasthesias precede headache Headache typically occipital
Migraine headache Basilar artery migraine variant occurs uncommonly Characterized by blindness or binocular visual disturbances Dysarthria, tinnitus, perioral and distal parasthesias precede headache Headache typically occipital
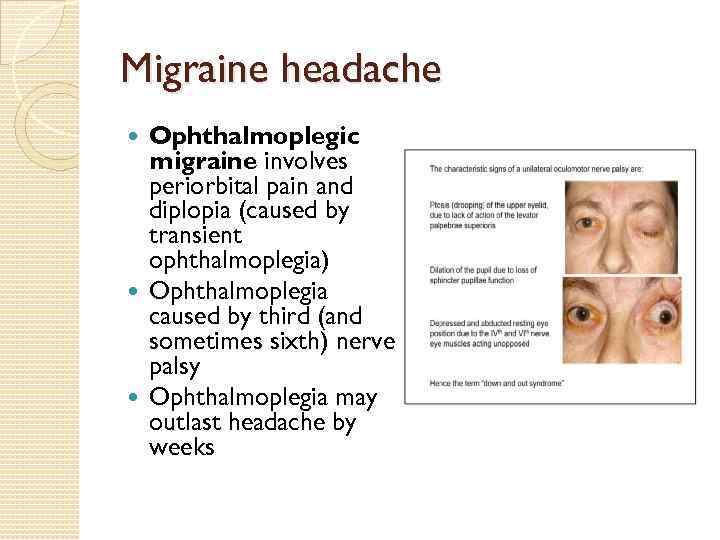 Migraine headache Ophthalmoplegic migraine involves periorbital pain and diplopia (caused by transient ophthalmoplegia) Ophthalmoplegia caused by third (and sometimes sixth) nerve palsy Ophthalmoplegia may outlast headache by weeks
Migraine headache Ophthalmoplegic migraine involves periorbital pain and diplopia (caused by transient ophthalmoplegia) Ophthalmoplegia caused by third (and sometimes sixth) nerve palsy Ophthalmoplegia may outlast headache by weeks
 Migraine headache Migraine equivalent refers to the neurologic or somatic complaint occurring in isolation “Migraine without headache” Patients will often develop headache later, or may have had a “milder” headache preceding this
Migraine headache Migraine equivalent refers to the neurologic or somatic complaint occurring in isolation “Migraine without headache” Patients will often develop headache later, or may have had a “milder” headache preceding this
 Migraine headache pathophysiology https: //youtu. be/y. Zr 9 Joe 85 wg
Migraine headache pathophysiology https: //youtu. be/y. Zr 9 Joe 85 wg
 Migraine treatment Three-pronged approach to treatment Avoidance of triggers and recognition of premonitory symptoms Abortive therapy Prophylactic therapy
Migraine treatment Three-pronged approach to treatment Avoidance of triggers and recognition of premonitory symptoms Abortive therapy Prophylactic therapy
 Migraine treatment Food triggers include those containing tyramine or phenylethylamine: chocolate, cheese, vinegar, soy, nuts, citrus, beer, red wine, nitrites, tannins, sulfites, MSG, yeast extract, aspartame, and caffeine (? ) Use of a headache diary can be useful in identifying food triggers
Migraine treatment Food triggers include those containing tyramine or phenylethylamine: chocolate, cheese, vinegar, soy, nuts, citrus, beer, red wine, nitrites, tannins, sulfites, MSG, yeast extract, aspartame, and caffeine (? ) Use of a headache diary can be useful in identifying food triggers
 Precipitating factors for migraine and cluster Migraine Ø Stress Ø Foods Ø Sleep (+/-) Ø Light Ø Noise Ø Menstrual cycle Ø OCP Cluster Ø Alcohol Ø Stress Ø Light Ø Foods
Precipitating factors for migraine and cluster Migraine Ø Stress Ø Foods Ø Sleep (+/-) Ø Light Ø Noise Ø Menstrual cycle Ø OCP Cluster Ø Alcohol Ø Stress Ø Light Ø Foods
 Migraine treatment Abortive therapy is designed to be used at the first sign of headache Can try OTC analgesics: ASA, acetaminophen, ibuprofen, naproxen Rx NSAIDS: dicolfenac, etodolac
Migraine treatment Abortive therapy is designed to be used at the first sign of headache Can try OTC analgesics: ASA, acetaminophen, ibuprofen, naproxen Rx NSAIDS: dicolfenac, etodolac
 Migraine treatment Ergotamines: original migraine treatment DHE is available as nasal spray or injection; Cafergot is po preparation with caffeine Good efficacy Side effects include vasoconstriction, n/v, diarrhea Contraindicated in HTN, vascular disease, pregnancy, complex migraine
Migraine treatment Ergotamines: original migraine treatment DHE is available as nasal spray or injection; Cafergot is po preparation with caffeine Good efficacy Side effects include vasoconstriction, n/v, diarrhea Contraindicated in HTN, vascular disease, pregnancy, complex migraine
 Migraine treatment Triptans are considered first-line therapy in moderate to severe migraines Selective serotonin 5 HT receptor agonists whose mechanisms include neuronal inhibition and vasoconstriction Available in multiple forms: injectable, oral, nasal spray, and soon to be patch
Migraine treatment Triptans are considered first-line therapy in moderate to severe migraines Selective serotonin 5 HT receptor agonists whose mechanisms include neuronal inhibition and vasoconstriction Available in multiple forms: injectable, oral, nasal spray, and soon to be patch
 Migraine treatment Efficacy highest in injectable sumatriptan Orals all have similar efficacy Choice determined by patient experience, tolerability and insurance coverage Contraindicated in vascular disease or complex migraine
Migraine treatment Efficacy highest in injectable sumatriptan Orals all have similar efficacy Choice determined by patient experience, tolerability and insurance coverage Contraindicated in vascular disease or complex migraine
 Migraine treatment Imitrex (PO, SC, intranasal) Maxalt (PO, MLT) Relpax (PO) Zomig (PO, intranasal) Amerge (PO) Axert (PO) Frova (PO)
Migraine treatment Imitrex (PO, SC, intranasal) Maxalt (PO, MLT) Relpax (PO) Zomig (PO, intranasal) Amerge (PO) Axert (PO) Frova (PO)
 Migraine treatment Most triptans pregnancy category C Variable lactation guidelines Side effects include vascular complications, chest and neck tightness Variability of response/tolerability in same patient
Migraine treatment Most triptans pregnancy category C Variable lactation guidelines Side effects include vascular complications, chest and neck tightness Variability of response/tolerability in same patient
 Migraine prophylaxis 3 or more episodes per month Significant impact on daily activity Abortive medications ineffective, contraindicated, or overused Adverse effect from abortive medications Patient preference
Migraine prophylaxis 3 or more episodes per month Significant impact on daily activity Abortive medications ineffective, contraindicated, or overused Adverse effect from abortive medications Patient preference
 Migraine prophylaxis § Beta Blockers (propranolol, timolol) § Calcium Channel Blockers § Anti-Depressants (SSRI’s/Tricyclics) § Seizure Medicines (Topamax, Depakote, Neurontin, Zonisamide) § Botox Injections – 1 st FDA approved (October 2010) prophylactic treatment for chronic migraine § Cefaly Headband – nerve stimulating headband, TENS technology
Migraine prophylaxis § Beta Blockers (propranolol, timolol) § Calcium Channel Blockers § Anti-Depressants (SSRI’s/Tricyclics) § Seizure Medicines (Topamax, Depakote, Neurontin, Zonisamide) § Botox Injections – 1 st FDA approved (October 2010) prophylactic treatment for chronic migraine § Cefaly Headband – nerve stimulating headband, TENS technology
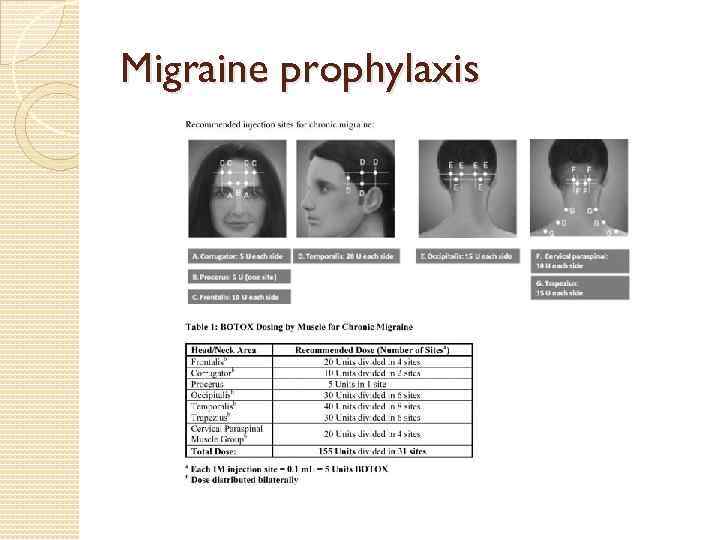 Migraine prophylaxis
Migraine prophylaxis
 Cluster headache Short, severe unilateral headaches that occur in clusters (once to many times a day from 2 weeks to months). Episodes last from 15 minutes to 3 hours May awaken patient at night Typically periorbital Mostly affects middle aged men
Cluster headache Short, severe unilateral headaches that occur in clusters (once to many times a day from 2 weeks to months). Episodes last from 15 minutes to 3 hours May awaken patient at night Typically periorbital Mostly affects middle aged men
 Cluster headache ◦ Lacrimation ◦ Rhinorrhea or nasal congestion ◦ Eyelid swelling ◦ Fatigue
Cluster headache ◦ Lacrimation ◦ Rhinorrhea or nasal congestion ◦ Eyelid swelling ◦ Fatigue
 Cluster headache Oxygen at 12 -15 L/min via nonrebreather for 15 -20 minutes Sumatriptan injection Zolmitriptan nasal spray Viscous lidocaine intranasally or D. H. E. IM Verapamil recommended as first-line preventive
Cluster headache Oxygen at 12 -15 L/min via nonrebreather for 15 -20 minutes Sumatriptan injection Zolmitriptan nasal spray Viscous lidocaine intranasally or D. H. E. IM Verapamil recommended as first-line preventive
 Cluster headache Significant majority of patients with cluster headache (80%) may have extended pain-free intervals (9 -11 months) Seasonal pattern Chronic cluster patients don’t experience this period of remission
Cluster headache Significant majority of patients with cluster headache (80%) may have extended pain-free intervals (9 -11 months) Seasonal pattern Chronic cluster patients don’t experience this period of remission
 Summary Differentiating between primary and secondary headaches Recognizing causes of headache requiring immediate attention Identifying characteristics of SAH Describing migraine, cluster and tension headache presentation and management strategies
Summary Differentiating between primary and secondary headaches Recognizing causes of headache requiring immediate attention Identifying characteristics of SAH Describing migraine, cluster and tension headache presentation and management strategies
 Let’s take 10
Let’s take 10


