2d5ca481db8d81d324abcc3a041018f6.ppt
- Количество слайдов: 30

Hb. F induction 3 rd Pan-European Conference on Haemoglobinopathies & Rare Anaemias Limassol, 24 – 26 October 2012 Mehran Karimi Shiraz University of Medical Sciences, Shiraz, Iran

Agenda ● Hb. F structure ● Regulation of Hb. F production ● Hb. F inducers ● Conclusions

Fetal Hb ● Hemoglobin F is the major Hb of the fetus and the newborn infant ● Hb. F levels reach the adult levels of <1% of the total Hb from about 18– 24 months of age and its replaced by adult Hb (Hb. A) ● Hb. F is able to bind oxygen with greater affinity than Hb. A
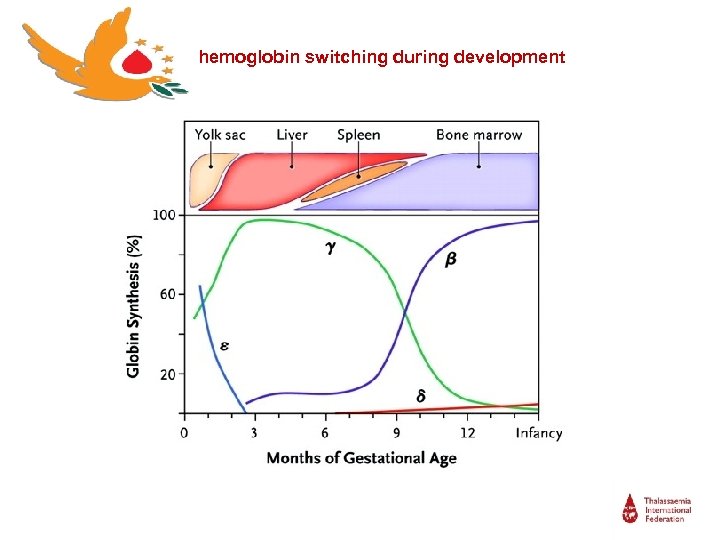
hemoglobin switching during development
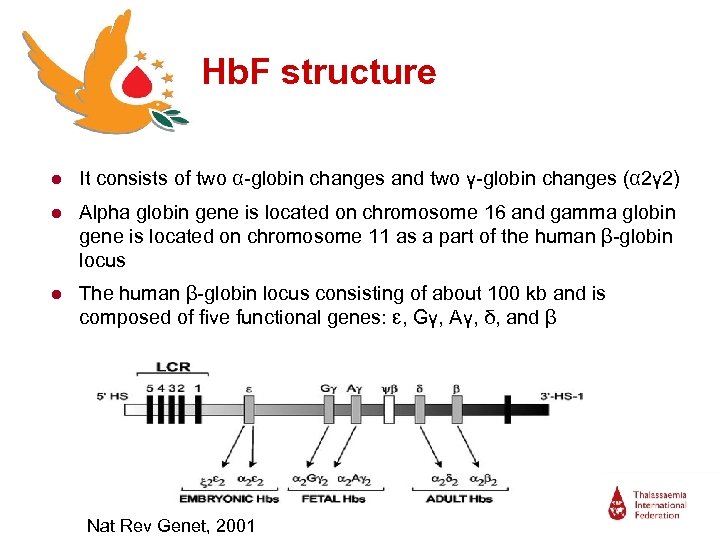
Hb. F structure ● It consists of two α-globin changes and two γ-globin changes (α 2γ 2) ● Alpha globin gene is located on chromosome 16 and gamma globin gene is located on chromosome 11 as a part of the human β-globin locus ● The human β-globin locus consisting of about 100 kb and is composed of five functional genes: ɛ, Gγ, Aγ, δ, and β Nat Rev Genet, 2001

Hb. F structure ● The two α-chains composed of 142 and two γ-chains, composed of 147 -amino-acid residues ● γ-chains are the results of two γ-globin genes which differ by one amino acid at position 136, having either alanine (Aγ) or glycine (Gγ) ● In adult erythrocytes, Hb. F is composed by about 40% Gγ and 60% Aγ, while in the newborn by about 70% Gγ and 30% Aγ ● There is no functional deference between two types of Hb. F Br J Haematol, 2008

Regulation of Hb. F production ● Adult production of Hb F is regulated by multiple genetic loci including (5 QTL): Ø The HMIP locus at chromosome 6 q 23 Ø The bcl 11 A locus on chromosome 2 Ø Xp 22. 2 region of the X chromosome Ø 8 q region on chromosome 8 Ø 11 p 15 region on chromosome 11 (including the Xmn 1 - HBG 1 site in the β-globin locus) Human Molecular Genetics, 2009
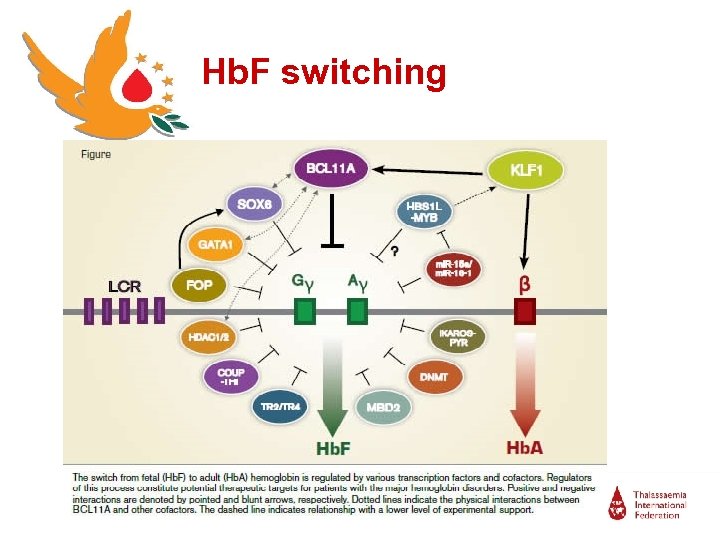
Hb. F switching
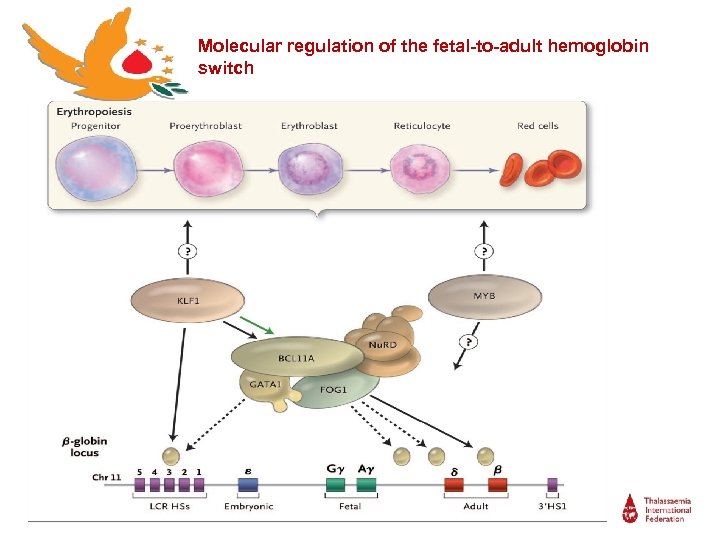
Molecular regulation of the fetal-to-adult hemoglobin switch

Hb. F induction ● Experimental and clinical data revealed that increased Hb. F levels can ameliorate the severity of sickle cell disease and β-thalassemia ● So there has been a longstanding interest in developing therapeutic approaches for inducing Hb. F ● The increase in Hb. F in response to Hb. F inducers varies among patients with β-thalassemia due to individual genetic determinants Ann Hematol, 2009
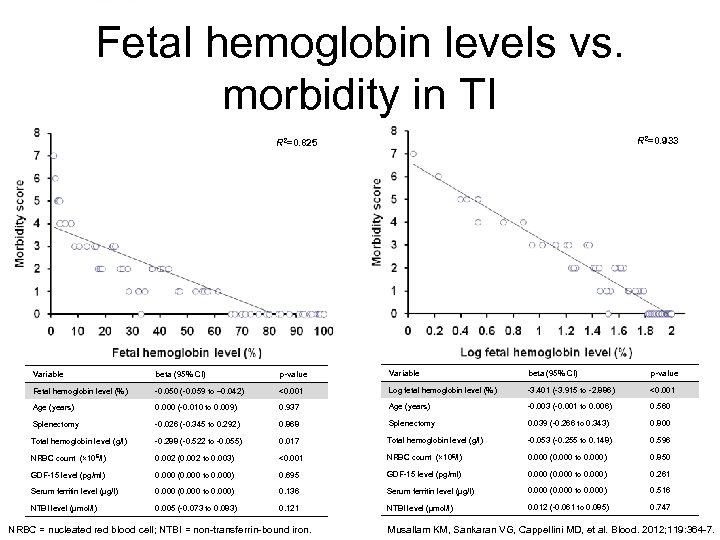
Fetal hemoglobin levels vs. morbidity in TI R 2=0. 933 R 2=0. 825 Variable beta (95% CI) p-value Fetal hemoglobin level (%) -0. 050 (-0. 059 to – 0. 042) <0. 001 Log fetal hemoglobin level (%) -3. 401 (-3. 915 to -2. 886) <0. 001 Age (years) 0. 000 (-0. 010 to 0. 009) 0. 937 Age (years) -0. 003 (-0. 001 to 0. 006) 0. 560 Splenectomy -0. 026 (-0. 345 to 0. 292) 0. 868 Splenectomy 0. 039 (-0. 266 to 0. 343) 0. 800 Total hemoglobin level (g/l) -0. 288 (-0. 522 to -0. 055) 0. 017 Total hemoglobin level (g/l) -0. 053 (-0. 255 to 0. 148) 0. 596 NRBC count (× 10 6/l) 0. 002 (0. 002 to 0. 003) <0. 001 NRBC count (× 10 6/l) 0. 000 (0. 000 to 0. 000) 0. 850 GDF-15 level (pg/ml) 0. 000 (0. 000 to 0. 000) 0. 695 GDF-15 level (pg/ml) 0. 000 (0. 000 to 0. 000) 0. 261 Serum ferritin level (µg/l) 0. 000 (0. 000 to 0. 000) 0. 136 Serum ferritin level (µg/l) 0. 000 (0. 000 to 0. 000) 0. 516 NTBI level (µmol/l) 0. 005 (-0. 073 to 0. 083) 0. 121 NTBI level (µmol/l) 0. 012 (-0. 061 to 0. 085) 0. 747 NRBC = nucleated red blood cell; NTBI = non-transferrin-bound iron. Musallam KM, Sankaran VG, Cappellini MD, et al. Blood. 2012; 119: 364 -7.

Hb. F inducers ● Hb. F inducers should have some effect on molecule targets to induce Hb. F including: Ø BCL 11 A (B-cell lymphoma/leukemia 11 A) Ø EKLF 1 (Erythroid Kruppel-like factor 1) Ø c. MYB (transcription factor) Ø SOX 6 (transcription factor) Ø mi. RNAs 15 a and 16 -1 Ø Histone deacetylase 1 and 2 (HDAC 1/2)
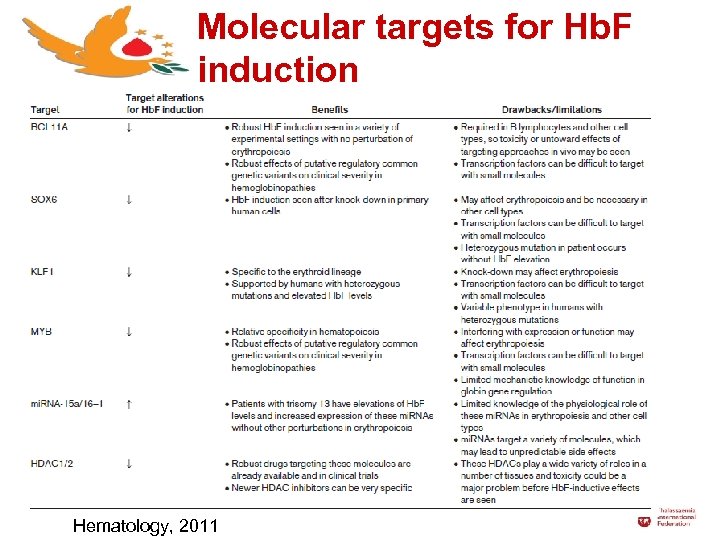

Molecular targets for Hb. F induction Hematology, 2011

Hb. F inducers ● The Hb. F inducers can be grouped in several classes based on their chemical structures and mechanisms of action including Ø Hypomethylating agents (eg; 5 -azacytidine and decitibine) Ø Short Chain Fatty acids: Histone deacetylase inhibitors (eg; sodium butyrate) Ø Chemotherapeutic agents (eg; hydroxyurea) Ø Stem cell factor and erythropoietin Ø Others

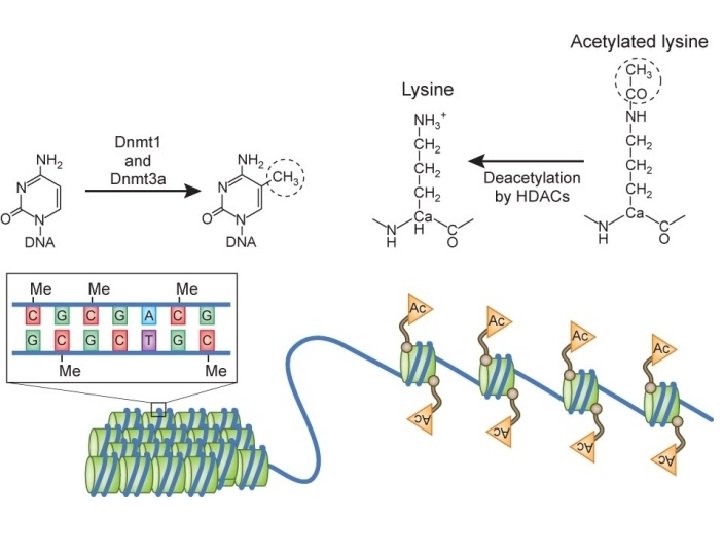
Hypomethylating agents ● DNA methylation is one of gene silencing mechanisms ● Genes with heavily methylated promoter regions cannot be transcribed and are effectively silenced ● Analysis of γ- and β-globin promoter methylation showed that, in general, promoter methylation and globin gene expression are inversely related ● In fetal erythroid progenitors, the γ-globin promoter is hypomethylated and becomes progressively more methylated as erythroid differentiation progresses and is hypermethylated in the mature erythroid progeny Exp Hematol, 2007

Hypomethylating agents ● 5 -Azacytidine (5 -Aza) was the first agent able to reactivate Hb. F synthesis in humans used for the treatment of β-thalassemia and sickle cell disease ● Although the mechanism through which 5 -Aza stimulates Hb. F synthesis is unclear but one hypothesis is based on the capacity of 5 -Aza to inhibit DNA methyltransferase enzymes, resulting in inhibition of DNA methylation ● Increased in Hb levels was seen 2. 5 gr/dl (1. 5 -4) Blood, 2008 Br J Haematol, 2004

Hypomethylating agents • Decitabine (5 -aza-2 -deoxycytidine): demethylate and reactivate expression of the gamma globin gene • Dosage: 0. 2 mg/kg /sc two times per week • It can increase hemoglobin levels about 1. 6 gr/dl Blood, 2008 Br J Haematol, 2004

Histone deacetylase inhibitors ● Gene expression is controlled by alterations in chromatin structure produced by acetylation and deacetylation of histone tails ● Histone deacetylase (HDAC) enzymes determine deacetylation of histone tails, causing chromatin condensation and repression of transcription ● Many experimental evidences have indicated that inhibition of the activity of HDAC causes an increased Hb. F synthesis Hematology, 2004

Histone deacetylase inhibitors ● Several HDAC inhibitors, such as sodium butyrate, adipicin, scriptaid and trichostatin A (TSA), have been shown to induce Hb. F synthesis in vitro ● Some studies have been carried out using valproic acid, a compound related to short fatty acid derivatives, reported increased Hb. F levels

Butyrate ● Butyrate was shown to promote cell differentiation and to enhance globin gene expression to cause higher Hb. F levels ● The mechanism through which butyrate stimulates Hb. F synthesis remains unclear but since butyrate is an inhibitor of histone deacetylase, it was proposed that butyrate increases Hb. F levels by enhancing the transcription rate of the γ-globin gene via changes in histone acetylation at the levels of critical promoter regions Blood, 1998

Butyrate ● Studies showed that not all sickle cell disease patients responded to butyrate treatment: Particularly, those exhibiting >2% Hb. F baseline levels responded to treatment, while those with lower Hb. F levels were resistant to this treatment ● Butyrate was also assayed in β-thalassemia patients ● Na phenyl butyrate: increase Hb levels 2 gr/dl(1 -2. 5) ● Arginine butyrate ± EPO: increase Hb levels 2. 7 gr/dl (1 -5). It is one of the most effective compound ● New generations of SCFADs: Na 2, 2 -dimethylbutyrate and α-methylhydrocinnamate. Blood, 1999 J Clin Invest, 2007

Hydroxyurea ● Hydroxyurea is a well-known drug used for treatment of myeloproliferative disorders ● Initial studies carried out in 1984 in sickle cell anemia patients showed that HU could stimulate Hb. F production ● As a consequence placebo-controlled study, HU was approved by the FDA for the treatment of sickle cell disease patients ● Hydroxyurea response in β-thalassemia has been extensively studied and, according to the majority of the reports, its administration was safe and able to significantly decrease transfusion requirements JAMA, 2003 Blood, 1997

Hydroxyurea ● More recent studies have confirmed in various types of β-thalassemia major and β-thalassemia intermedia patients a significant clinical benefit following hydroxyurea therapy, with elimination of transfusion requirements in a significant proportion of transfusiondependent β-thalassemic children ● Hydroxyurea seems to have a good role in the treatment of thalassemia especially TI, but resistance to this drug is observed in some cases ● It can increase Hb levels 0. 6 -2. 7 gr/dl Blood, 2003, Int. J. Hematology 2012

Stem cell factor (SCF) ● Because of pronounced effects of SCF on erythropoiesis, it seemed important to evaluate a possible effect of this cytokine on Hb. F synthesis ● The majority of these studies have been carried out by investigating in vitro the effect of SCF on Hb. F synthesis in cultures of adult erythroid cells ● The effect of SCF was also investigated in cultures of β-thalassemic erythroid cells ● It induces and expansion of erythropoiesis and the reactivation of Hb. F synthesis ● There is strong evidence of synergy effect of SCF with Epo Blood, 2008

Erythropoietin (EPO) • It promotes red blood cell survival and increased Hb levels. • It can use alone or combine by hydroxyurea • EPO, Darbopoietin: increase Hb levels 1. 6 -2 gr/dl • EPO is expensive Blood, 2008

Other compounds ● Thalidomide, Lenalidomide and pomalidomide are other components that induces increased expression of the γ-globin gene and Hb. F production ● when combined with hydroxyurea, pomalidomide and, to a lesser extent, lenalidomide were found to have synergistic effects on Hb. F up-regulation ● Rapamycin (immunosuppressant drug) and Resveratrol ( antioxidant) both can increase Hb F production, natural products, not associated with cytotoxicity or cell growth inhibition J Clin Invest, 2008 and blood review 2012

Conclusions (1) ● An ideal Hb F inducers should have three characteristics: 1. orally active and tolerable 2. not inhibit erythropoiesis 3. Not be mutagenic ● The experimental and clinical observations support the idea that agents enhancing Hb. F synthesis represent a rational approach for the treatment of β -thalassemia and it is expected to be critical for developing countries with low economic status

Conclusions (2) ● Multiple modalities approach to induce Hb F have relatively satisfactory with different variation response ● However it is important to note that therapy of hemoglobinopathies based on the administration of agents stimulating Hb. F synthesis cannot be curative and needs a chronic administration ● Therefore, better agents that more effective targeted therapies to induce higher levels of Hb. F are needed to develop in future

THANKS FOR YOUR ATTENTION karimim@sums. ac. ir
2d5ca481db8d81d324abcc3a041018f6.ppt