d39de91f9d4455fe60361df96f90d552.ppt
- Количество слайдов: 45
 Guidelines for the Diagnosis and Management of Asthma National Asthma Education and Prevention Program Expert Panel Report 3 Laura T. Mulreany, MD LTC, MC Pediatric Pulmonologist
Guidelines for the Diagnosis and Management of Asthma National Asthma Education and Prevention Program Expert Panel Report 3 Laura T. Mulreany, MD LTC, MC Pediatric Pulmonologist
 OVERVIEW v Not a comprehensive review of childhood asthma v What we have learned since 2002 v Major changes in new NHLBI guidelines Ø Assessment and monitoring Ø Patient education Ø Control of factors contributing to severity Ø Pharmacologic treatment
OVERVIEW v Not a comprehensive review of childhood asthma v What we have learned since 2002 v Major changes in new NHLBI guidelines Ø Assessment and monitoring Ø Patient education Ø Control of factors contributing to severity Ø Pharmacologic treatment
 ASTHMA KNOWLEDGE 2007
ASTHMA KNOWLEDGE 2007
 CHILDHOOD ASTHMA v Chronic inflammatory disorder v Recurrent episodes of potentially-reversible airflow obstruction v Key features: Ø Bronchoconstriction Ø Airway hyperresponsiveness Ø Airway edema
CHILDHOOD ASTHMA v Chronic inflammatory disorder v Recurrent episodes of potentially-reversible airflow obstruction v Key features: Ø Bronchoconstriction Ø Airway hyperresponsiveness Ø Airway edema
 CHILDHOOD ASTHMA v. Major advances in understanding ØRole of inflammation ØGene-by-environmental interactions ØEarly, recognizable risk factors ØTreatment and disease progression
CHILDHOOD ASTHMA v. Major advances in understanding ØRole of inflammation ØGene-by-environmental interactions ØEarly, recognizable risk factors ØTreatment and disease progression
 INFLAMMATION v Many cell types and mediators Ø Different phenotypes may have specific patterns and require different treatments v Causes airflow limitation and enhanced hyperresponsiveness v Response to treatment may be slow or incomplete v Airway remodeling may result from abnormallyregulated repair Ø Loss of lung function or reduced lung growth
INFLAMMATION v Many cell types and mediators Ø Different phenotypes may have specific patterns and require different treatments v Causes airflow limitation and enhanced hyperresponsiveness v Response to treatment may be slow or incomplete v Airway remodeling may result from abnormallyregulated repair Ø Loss of lung function or reduced lung growth
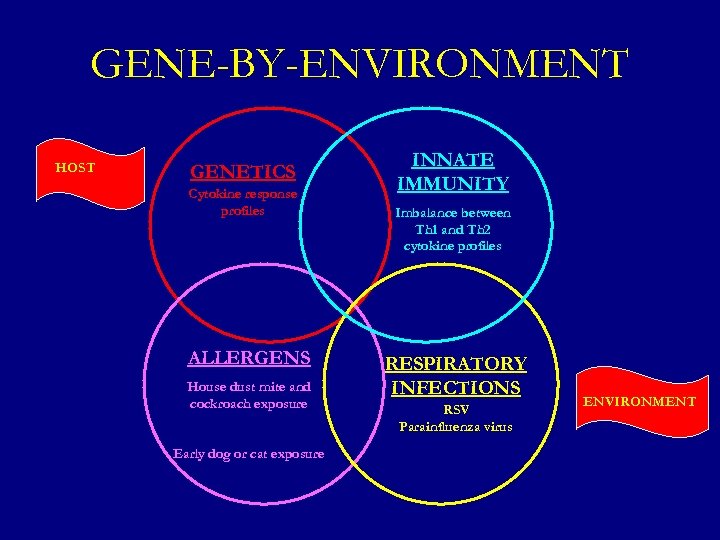 GENE-BY-ENVIRONMENT HOST GENETICS Cytokine response profiles ALLERGENS House dust mite and cockroach exposure Early dog or cat exposure INNATE IMMUNITY Imbalance between Th 1 and Th 2 cytokine profiles RESPIRATORY INFECTIONS RSV Parainfluenza virus ENVIRONMENT
GENE-BY-ENVIRONMENT HOST GENETICS Cytokine response profiles ALLERGENS House dust mite and cockroach exposure Early dog or cat exposure INNATE IMMUNITY Imbalance between Th 1 and Th 2 cytokine profiles RESPIRATORY INFECTIONS RSV Parainfluenza virus ENVIRONMENT
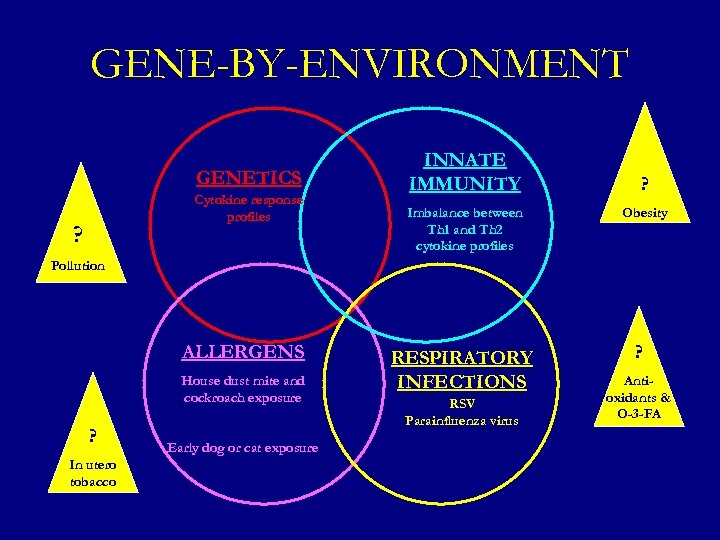 GENE-BY-ENVIRONMENT GENETICS Cytokine response profiles ? INNATE IMMUNITY Imbalance between Th 1 and Th 2 cytokine profiles ? Obesity Pollution ALLERGENS House dust mite and cockroach exposure ? In utero tobacco Early dog or cat exposure RESPIRATORY INFECTIONS RSV Parainfluenza virus ? Antioxidants & O-3 -FA
GENE-BY-ENVIRONMENT GENETICS Cytokine response profiles ? INNATE IMMUNITY Imbalance between Th 1 and Th 2 cytokine profiles ? Obesity Pollution ALLERGENS House dust mite and cockroach exposure ? In utero tobacco Early dog or cat exposure RESPIRATORY INFECTIONS RSV Parainfluenza virus ? Antioxidants & O-3 -FA
 EARLY RISK FACTORS v. Age at onset influences decrease in lung function growth ØEarly onset (before 3 y/o) associated with decreased lung function growth v. Target for intervention - children under 3 ØBut majority of toddlers who wheeze do not develop asthma
EARLY RISK FACTORS v. Age at onset influences decrease in lung function growth ØEarly onset (before 3 y/o) associated with decreased lung function growth v. Target for intervention - children under 3 ØBut majority of toddlers who wheeze do not develop asthma
 ASTHMA PREDICTIVE INDEX v. Children under 3 y/o with 4 or more wheezing episodes / year ØDevelopment of persistent asthma increased if: • One of following: – Parental asthma, atopic dermatitis, aeroallergen sensitization OR… • Two of following – Sensitization to foods, ≥ 4% eosinophilia, wheezing apart from colds
ASTHMA PREDICTIVE INDEX v. Children under 3 y/o with 4 or more wheezing episodes / year ØDevelopment of persistent asthma increased if: • One of following: – Parental asthma, atopic dermatitis, aeroallergen sensitization OR… • Two of following – Sensitization to foods, ≥ 4% eosinophilia, wheezing apart from colds
 TREATMENT & PROGRESSION v. Anti-inflammatory therapy does not prevent disease progression v. Inhaled corticosteroids provide ØBetter control ØPrevention of symptoms and exacerbations ØBut… • Symptoms and airway hyperresponsiveness worsen when treatment withdrawn
TREATMENT & PROGRESSION v. Anti-inflammatory therapy does not prevent disease progression v. Inhaled corticosteroids provide ØBetter control ØPrevention of symptoms and exacerbations ØBut… • Symptoms and airway hyperresponsiveness worsen when treatment withdrawn
 ASTHMA MANAGEMENT 2007
ASTHMA MANAGEMENT 2007
 AFTER DIAGNOSIS… v. Identify precipitating factors v. Identify co-morbid conditions v. Assess patient’s knowledge & skills for selfmanagement v. Classify asthma severity
AFTER DIAGNOSIS… v. Identify precipitating factors v. Identify co-morbid conditions v. Assess patient’s knowledge & skills for selfmanagement v. Classify asthma severity
 ASTHMA MANAGEMENT v. Four components ØAssessment and monitoring ØEducation ØControl of environmental factors & comorbidities ØPharmacologic therapy
ASTHMA MANAGEMENT v. Four components ØAssessment and monitoring ØEducation ØControl of environmental factors & comorbidities ØPharmacologic therapy
 MAJOR CHANGES IN EPR-3 v. Severity and control v. Impairment and risk v. Step-wise approach to diagnosis and treatment v. Education v. Environmental control v. Treatment of acute asthma
MAJOR CHANGES IN EPR-3 v. Severity and control v. Impairment and risk v. Step-wise approach to diagnosis and treatment v. Education v. Environmental control v. Treatment of acute asthma
 SEVERITY AND CONTROL v Severity Ø Intrinsic intensity of disease Ø Measured best before therapy Ø May be inferred from least amount of tx needed for control Ø Guides decisions about treatment v Control Ø Degree manifestations are minimized & goals met Ø Measured at follow-up Ø Guides adjustments in treatment Ø Responsiveness - ease of achieving control
SEVERITY AND CONTROL v Severity Ø Intrinsic intensity of disease Ø Measured best before therapy Ø May be inferred from least amount of tx needed for control Ø Guides decisions about treatment v Control Ø Degree manifestations are minimized & goals met Ø Measured at follow-up Ø Guides adjustments in treatment Ø Responsiveness - ease of achieving control
 RESPONSIVENESS v. Ease of achieving control v. Uncertainty in ØClinically-significant outcomes ØTime needed to assess response v. Resistance to therapy ØHigh prevalence of co-morbidities
RESPONSIVENESS v. Ease of achieving control v. Uncertainty in ØClinically-significant outcomes ØTime needed to assess response v. Resistance to therapy ØHigh prevalence of co-morbidities
 CLASSIFICATION OF ASTHMA SEVERITY CHILDREN 0 -4 YEARS OF AGE Components of severity Intermittent Mild persistent Moderate persistent Severe persistent Symptoms ≤ 2 days/wk > 2 days/wk but not daily Daily Throughout day Nighttime awakenings None 1 -2 x/month 3 -4 x/month > 1 x/week Short acting beta agonist ≤ 2 days/wk > 2 days/wk but not daily Daily Several times per day Interference with activity None Minor limitation Some limitation Extremely limited
CLASSIFICATION OF ASTHMA SEVERITY CHILDREN 0 -4 YEARS OF AGE Components of severity Intermittent Mild persistent Moderate persistent Severe persistent Symptoms ≤ 2 days/wk > 2 days/wk but not daily Daily Throughout day Nighttime awakenings None 1 -2 x/month 3 -4 x/month > 1 x/week Short acting beta agonist ≤ 2 days/wk > 2 days/wk but not daily Daily Several times per day Interference with activity None Minor limitation Some limitation Extremely limited
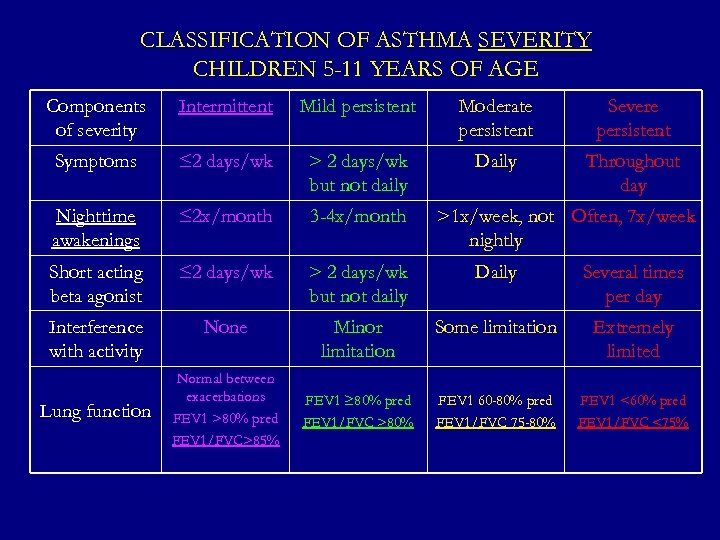 CLASSIFICATION OF ASTHMA SEVERITY CHILDREN 5 -11 YEARS OF AGE Components of severity Intermittent Mild persistent Moderate persistent Severe persistent Symptoms ≤ 2 days/wk > 2 days/wk but not daily Daily Throughout day Nighttime awakenings ≤ 2 x/month 3 -4 x/month Short acting beta agonist ≤ 2 days/wk > 2 days/wk but not daily Daily Several times per day Interference with activity None Minor limitation Some limitation Extremely limited FEV 1 ≥ 80% pred FEV 1/FVC >80% FEV 1 60 -80% pred FEV 1/FVC 75 -80% FEV 1 <60% pred FEV 1/FVC <75% Lung function Normal between exacerbations FEV 1 >80% pred FEV 1/FVC>85% >1 x/week, not Often, 7 x/week nightly
CLASSIFICATION OF ASTHMA SEVERITY CHILDREN 5 -11 YEARS OF AGE Components of severity Intermittent Mild persistent Moderate persistent Severe persistent Symptoms ≤ 2 days/wk > 2 days/wk but not daily Daily Throughout day Nighttime awakenings ≤ 2 x/month 3 -4 x/month Short acting beta agonist ≤ 2 days/wk > 2 days/wk but not daily Daily Several times per day Interference with activity None Minor limitation Some limitation Extremely limited FEV 1 ≥ 80% pred FEV 1/FVC >80% FEV 1 60 -80% pred FEV 1/FVC 75 -80% FEV 1 <60% pred FEV 1/FVC <75% Lung function Normal between exacerbations FEV 1 >80% pred FEV 1/FVC>85% >1 x/week, not Often, 7 x/week nightly
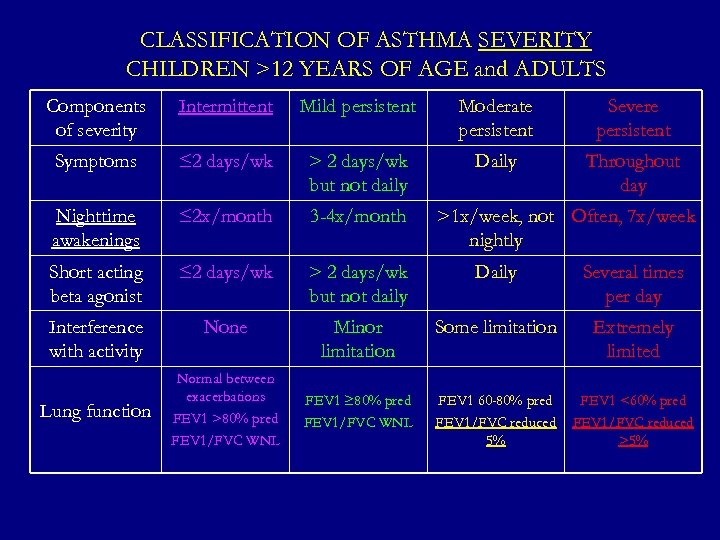 CLASSIFICATION OF ASTHMA SEVERITY CHILDREN >12 YEARS OF AGE and ADULTS Components of severity Intermittent Mild persistent Moderate persistent Severe persistent Symptoms ≤ 2 days/wk > 2 days/wk but not daily Daily Throughout day Nighttime awakenings ≤ 2 x/month 3 -4 x/month Short acting beta agonist ≤ 2 days/wk > 2 days/wk but not daily Daily Several times per day Interference with activity None Minor limitation Some limitation Extremely limited FEV 1 ≥ 80% pred FEV 1/FVC WNL FEV 1 60 -80% pred FEV 1/FVC reduced 5% FEV 1 <60% pred FEV 1/FVC reduced >5% Lung function Normal between exacerbations FEV 1 >80% pred FEV 1/FVC WNL >1 x/week, not Often, 7 x/week nightly
CLASSIFICATION OF ASTHMA SEVERITY CHILDREN >12 YEARS OF AGE and ADULTS Components of severity Intermittent Mild persistent Moderate persistent Severe persistent Symptoms ≤ 2 days/wk > 2 days/wk but not daily Daily Throughout day Nighttime awakenings ≤ 2 x/month 3 -4 x/month Short acting beta agonist ≤ 2 days/wk > 2 days/wk but not daily Daily Several times per day Interference with activity None Minor limitation Some limitation Extremely limited FEV 1 ≥ 80% pred FEV 1/FVC WNL FEV 1 60 -80% pred FEV 1/FVC reduced 5% FEV 1 <60% pred FEV 1/FVC reduced >5% Lung function Normal between exacerbations FEV 1 >80% pred FEV 1/FVC WNL >1 x/week, not Often, 7 x/week nightly
 SPIROMETRY v. Pre and post-bronchodilator testing v. Measures often do not correlate with sxs v. FEV 1/FVC more sensitive measure of severity in children v. FEV 1 useful measure of risk of exacerbations
SPIROMETRY v. Pre and post-bronchodilator testing v. Measures often do not correlate with sxs v. FEV 1/FVC more sensitive measure of severity in children v. FEV 1 useful measure of risk of exacerbations
 ASSIGNING SEVERITY – AFTER TX STARTED Intermittent Lowest level of treatment required to maintain control Mild persistent Moderate persistent Severe persistent Step 1 Step 2 Step 3 or 4 Step 5 or 6
ASSIGNING SEVERITY – AFTER TX STARTED Intermittent Lowest level of treatment required to maintain control Mild persistent Moderate persistent Severe persistent Step 1 Step 2 Step 3 or 4 Step 5 or 6
 IMPAIRMENT AND RISK v Impairment Ø Frequency and intensity of disease • Symptoms • Lung function Ø Functional limitations v Risk Ø Likelihood of exacerbations, decline in lung function or reduced lung growth Ø Risk of adverse effects from medications
IMPAIRMENT AND RISK v Impairment Ø Frequency and intensity of disease • Symptoms • Lung function Ø Functional limitations v Risk Ø Likelihood of exacerbations, decline in lung function or reduced lung growth Ø Risk of adverse effects from medications
 RISK v Severity of disease does not necessarily correlate with intensity of exacerbations v Predictors Ø More frequent or intense exacerbations Ø Severe airflow obstruction Ø Reporting feeling in danger or frightened Ø Female, non-white Ø Non-use of ICS Ø Smoking Ø Psychosocial factors Ø Attitudes and beliefs about medications
RISK v Severity of disease does not necessarily correlate with intensity of exacerbations v Predictors Ø More frequent or intense exacerbations Ø Severe airflow obstruction Ø Reporting feeling in danger or frightened Ø Female, non-white Ø Non-use of ICS Ø Smoking Ø Psychosocial factors Ø Attitudes and beliefs about medications
 RISK - CHILDREN 0 -4 y/o Intermittent 0 -1 / year RISK Exacerbations requiring oral systemic corticosteroids Mild persistent Moderate persistent Severe persistent ≥ 2 exacerbations in 6 months requiring oral steroids, or ≥ 4 wheezing episodes/1 year lasting >1 day AND risk factors for asthma Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time Exacerbations of any severity ay occur in patients in any severity category
RISK - CHILDREN 0 -4 y/o Intermittent 0 -1 / year RISK Exacerbations requiring oral systemic corticosteroids Mild persistent Moderate persistent Severe persistent ≥ 2 exacerbations in 6 months requiring oral steroids, or ≥ 4 wheezing episodes/1 year lasting >1 day AND risk factors for asthma Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time Exacerbations of any severity ay occur in patients in any severity category
 RISK - CHILDREN 5 -11 y/o Intermittent 0 -1 / year RISK Exacerbations requiring oral systemic corticosteroids Mild persistent Moderate persistent Severe persistent ≥ 2 exacerbations in 1 year Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time Relative annual risk of exacerbations may be related to FEV 1
RISK - CHILDREN 5 -11 y/o Intermittent 0 -1 / year RISK Exacerbations requiring oral systemic corticosteroids Mild persistent Moderate persistent Severe persistent ≥ 2 exacerbations in 1 year Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time Relative annual risk of exacerbations may be related to FEV 1
 RISK - YOUTHS ≥ 12 y/o and older Intermittent 0 -1 / year RISK Exacerbations requiring oral systemic corticosteroids Mild persistent Moderate persistent Severe persistent ≥ 2 exacerbations in 1 year Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time Relative annual risk of exacerbations may be related to FEV 1
RISK - YOUTHS ≥ 12 y/o and older Intermittent 0 -1 / year RISK Exacerbations requiring oral systemic corticosteroids Mild persistent Moderate persistent Severe persistent ≥ 2 exacerbations in 1 year Consider severity and interval since last exacerbation. Frequency and severity may fluctuate over time Relative annual risk of exacerbations may be related to FEV 1
 TREATMENT OF ASTHMA
TREATMENT OF ASTHMA
 GOALS OF THERAPY v Prevent chronic or troublesome sxs v Prevent / reduce severity of exacerbations v Require infrequent use of quick-relief meds v Maintain (near) “normal” lung function v Maintain normal activity levels v Optimal meds with minimal / no side effects v Meet pt expectations of & satisfaction with asthma care Identical for all levels of severity
GOALS OF THERAPY v Prevent chronic or troublesome sxs v Prevent / reduce severity of exacerbations v Require infrequent use of quick-relief meds v Maintain (near) “normal” lung function v Maintain normal activity levels v Optimal meds with minimal / no side effects v Meet pt expectations of & satisfaction with asthma care Identical for all levels of severity
 MEDICAL MANAGEMENT v. Most effective medications for long term control have anti-inflammatory effects v. Inhaled corticosteroids (ICS) are most potent and consistently effective ØSafe for use in children ØSensitivity and response to ICS may vary ØIn mild-moderate asthma, dose-response relationship flattens in low-medium dose range
MEDICAL MANAGEMENT v. Most effective medications for long term control have anti-inflammatory effects v. Inhaled corticosteroids (ICS) are most potent and consistently effective ØSafe for use in children ØSensitivity and response to ICS may vary ØIn mild-moderate asthma, dose-response relationship flattens in low-medium dose range
 MEDICAL MANAGEMENT v Long acting beta agonists (LABA) Ø Black box warning Ø Adjunct to ICS, not monotherapy Ø Consider if not controlled on low dose ICS (pts older than 4 y/o) v Leukotriene modifiers, methylxanthines Ø Alternatives, not preferred v Omalizumab Ø Consider in severe asthma
MEDICAL MANAGEMENT v Long acting beta agonists (LABA) Ø Black box warning Ø Adjunct to ICS, not monotherapy Ø Consider if not controlled on low dose ICS (pts older than 4 y/o) v Leukotriene modifiers, methylxanthines Ø Alternatives, not preferred v Omalizumab Ø Consider in severe asthma
 INITIATING THERAPY 0 -4 y/o v. Start long term controller for: Ø 4 or more wheezing episodes in past year (lasting > 1 day and affecting sleep) AND risk factors ØSymptomatic tx > 2 days/week for > 4 weeks ØSecond exacerbation req oral steroids in 6 mo Ø(may consider use only during periods of consistently documented risk)
INITIATING THERAPY 0 -4 y/o v. Start long term controller for: Ø 4 or more wheezing episodes in past year (lasting > 1 day and affecting sleep) AND risk factors ØSymptomatic tx > 2 days/week for > 4 weeks ØSecond exacerbation req oral steroids in 6 mo Ø(may consider use only during periods of consistently documented risk)
 STEP-WISE TREATMENT v Combine impairment and risk v Assign severity to most severe category Age Recommended step for initiating therapy Intermittent Mild persistent Moderate persistent Severe persistent 0 -4 Step 1 Step 2 Step 3 and consider short course of oral steroids 5 -11 Step 2 Step 3, med dose Step 3 med dose ICS option (consider option or step 4 short course oral (consider short steroids) course oral steroids) 12+ Step 1 Step 2 Step 3 (and consider short course oral steroids) Step 4 or 5 (and consider short course oral steroids)
STEP-WISE TREATMENT v Combine impairment and risk v Assign severity to most severe category Age Recommended step for initiating therapy Intermittent Mild persistent Moderate persistent Severe persistent 0 -4 Step 1 Step 2 Step 3 and consider short course of oral steroids 5 -11 Step 2 Step 3, med dose Step 3 med dose ICS option (consider option or step 4 short course oral (consider short steroids) course oral steroids) 12+ Step 1 Step 2 Step 3 (and consider short course oral steroids) Step 4 or 5 (and consider short course oral steroids)
 MANAGEMENT - 0 -4 y/o Step 6 Step 5 Step 4 Step 3 Step 2 Step 1 Preferred: Low dose ICS Preferred : SABA prn Alternative: Cromolyn or Montelukast Preferred: Medium dose ICS + either LABA or Montelukast Preferred: High dose ICS + Either LABA Or Montelukast Preferred: High dose ICS + either LABA or Montelukast Oral systemic corticosteroid
MANAGEMENT - 0 -4 y/o Step 6 Step 5 Step 4 Step 3 Step 2 Step 1 Preferred: Low dose ICS Preferred : SABA prn Alternative: Cromolyn or Montelukast Preferred: Medium dose ICS + either LABA or Montelukast Preferred: High dose ICS + Either LABA Or Montelukast Preferred: High dose ICS + either LABA or Montelukast Oral systemic corticosteroid
 MANAGEMENT - 5 -11 y/o Step 6 Step 5 Step 4 Step 2 Step 1 Preferred : SABA prn Preferred: Low dose ICS Alternative: Cromolyn or LTRA or Nedocromil or Therophylline Step 3 Preferred: EITHER Low dose ICS + Either LABA, LTRA, or Theophylline OR Medium dose ICS Preferred: Medium dose ICS + LABA Alternative: Medium dose ICS + either LTRA or theophylline Preferred: High dose ICS + LABA Alternative: High dose ICS + Either LTRA or Theophylline Preferred: High dose ICS+ LABA +Oral systemic steroids Alternative: High dose ICS + either LTRA Or theophylline + oral systemic corticosteroids
MANAGEMENT - 5 -11 y/o Step 6 Step 5 Step 4 Step 2 Step 1 Preferred : SABA prn Preferred: Low dose ICS Alternative: Cromolyn or LTRA or Nedocromil or Therophylline Step 3 Preferred: EITHER Low dose ICS + Either LABA, LTRA, or Theophylline OR Medium dose ICS Preferred: Medium dose ICS + LABA Alternative: Medium dose ICS + either LTRA or theophylline Preferred: High dose ICS + LABA Alternative: High dose ICS + Either LTRA or Theophylline Preferred: High dose ICS+ LABA +Oral systemic steroids Alternative: High dose ICS + either LTRA Or theophylline + oral systemic corticosteroids
 ASSESSMENT OF CONTROL v Clinician and patient assessments v Six components Ø Signs and symptoms Ø Pulmonary function Ø Quality of life Ø Exacerbations Ø Medications - adherence and side effects Ø Patient satisfaction, communication w/ provider (minimally invasive markers and pharmacogenetics under consideration)
ASSESSMENT OF CONTROL v Clinician and patient assessments v Six components Ø Signs and symptoms Ø Pulmonary function Ø Quality of life Ø Exacerbations Ø Medications - adherence and side effects Ø Patient satisfaction, communication w/ provider (minimally invasive markers and pharmacogenetics under consideration)
 CLASSIFICATION OF ASTHMA CONTROL CHILDREN 0 -4 YEARS OF AGE Components of control Well controlled Not well controlled Very poorly controlled Symptoms ≤ 2 days/wk > 2 days/wk Throughout day Nighttime awakenings 1 x/month > 1 x/week Short acting beta agonist ≤ 2 days/wk > 2 days/wk Several times per day Interference with activity None Some limitation Extremely limited
CLASSIFICATION OF ASTHMA CONTROL CHILDREN 0 -4 YEARS OF AGE Components of control Well controlled Not well controlled Very poorly controlled Symptoms ≤ 2 days/wk > 2 days/wk Throughout day Nighttime awakenings 1 x/month > 1 x/week Short acting beta agonist ≤ 2 days/wk > 2 days/wk Several times per day Interference with activity None Some limitation Extremely limited
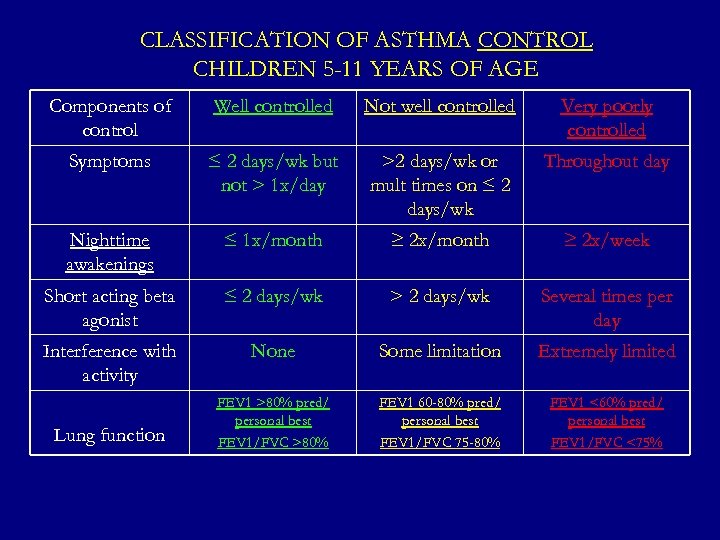 CLASSIFICATION OF ASTHMA CONTROL CHILDREN 5 -11 YEARS OF AGE Components of control Well controlled Not well controlled Very poorly controlled Symptoms ≤ 2 days/wk but not > 1 x/day >2 days/wk or mult times on ≤ 2 days/wk Throughout day Nighttime awakenings ≤ 1 x/month ≥ 2 x/week Short acting beta agonist ≤ 2 days/wk > 2 days/wk Several times per day Interference with activity None Some limitation Extremely limited FEV 1 >80% pred/ personal best FEV 1/FVC >80% FEV 1 60 -80% pred/ personal best FEV 1/FVC 75 -80% FEV 1 <60% pred/ personal best FEV 1/FVC <75% Lung function
CLASSIFICATION OF ASTHMA CONTROL CHILDREN 5 -11 YEARS OF AGE Components of control Well controlled Not well controlled Very poorly controlled Symptoms ≤ 2 days/wk but not > 1 x/day >2 days/wk or mult times on ≤ 2 days/wk Throughout day Nighttime awakenings ≤ 1 x/month ≥ 2 x/week Short acting beta agonist ≤ 2 days/wk > 2 days/wk Several times per day Interference with activity None Some limitation Extremely limited FEV 1 >80% pred/ personal best FEV 1/FVC >80% FEV 1 60 -80% pred/ personal best FEV 1/FVC 75 -80% FEV 1 <60% pred/ personal best FEV 1/FVC <75% Lung function
 CLASSIFICATION OF ASTHMA CONTROL CHILDREN >12 YEARS OF AGE and ADULTS Components of control Well controlled Not well controlled Very poorly controlled Symptoms ≤ 2 days/week > 2 days/week Throughout day Nighttime awakenings ≤ 2 x/month 1 -3 x/week ≥ 4 x/week Short acting beta agonist ≤ 2 days/week > 2 days/week Several times per day Interference with activity None Some limitation Extremely limited FEV 1 or peak flow >80% predicted/ personal best 60 -80% predicted/ personal best <60% predicted/ personal best Validated questionnaires also used in assessment of control
CLASSIFICATION OF ASTHMA CONTROL CHILDREN >12 YEARS OF AGE and ADULTS Components of control Well controlled Not well controlled Very poorly controlled Symptoms ≤ 2 days/week > 2 days/week Throughout day Nighttime awakenings ≤ 2 x/month 1 -3 x/week ≥ 4 x/week Short acting beta agonist ≤ 2 days/week > 2 days/week Several times per day Interference with activity None Some limitation Extremely limited FEV 1 or peak flow >80% predicted/ personal best 60 -80% predicted/ personal best <60% predicted/ personal best Validated questionnaires also used in assessment of control
 ASSESSING CONTROL & ADJUSTING THERAPY Well controlled Not well controlled Poorly controlled Maintain current treatment Step up 1 step Consider short course oral steroids Re-evaluate in 2 -6 weeks Recommended action for treatment Regular f/u every 1 -6 months Consider step down if well-controlled for at least 3 months For side effects, consider alternative tx options Step up 1 -2 steps Re-evaluate in 2 weeks For side effects, consider alternate tx options For 0 -4 y/o– if no clear benefit in 4 -6 weeks, consider alter diagnoses or adjusting therapy
ASSESSING CONTROL & ADJUSTING THERAPY Well controlled Not well controlled Poorly controlled Maintain current treatment Step up 1 step Consider short course oral steroids Re-evaluate in 2 -6 weeks Recommended action for treatment Regular f/u every 1 -6 months Consider step down if well-controlled for at least 3 months For side effects, consider alternative tx options Step up 1 -2 steps Re-evaluate in 2 weeks For side effects, consider alternate tx options For 0 -4 y/o– if no clear benefit in 4 -6 weeks, consider alter diagnoses or adjusting therapy
 SPECIALTY REFERRAL v Life-threatening exacerbation v Not meeting goals of therapy v Atypical signs/sxs v Complicating conditions v Additional testing v Additional education v Consideration for immunotherapy v Step 3 for child 0 -4, or step 4 for older pts v > 2 oral steroid bursts/year v Environmental or occupational exposure concern
SPECIALTY REFERRAL v Life-threatening exacerbation v Not meeting goals of therapy v Atypical signs/sxs v Complicating conditions v Additional testing v Additional education v Consideration for immunotherapy v Step 3 for child 0 -4, or step 4 for older pts v > 2 oral steroid bursts/year v Environmental or occupational exposure concern
 EDUCATION v Repetition and reinforcement v Self-management Ø Review of goals of tx Ø Written action plan Ø Environmental control Ø Management of co-morbidities v All points of care v Patient satisfaction, quality of life, cultural and ethnic considerations
EDUCATION v Repetition and reinforcement v Self-management Ø Review of goals of tx Ø Written action plan Ø Environmental control Ø Management of co-morbidities v All points of care v Patient satisfaction, quality of life, cultural and ethnic considerations
 TREATMENT OF ACUTE ASTHMA – new recommendations v HOME Ø Action plan Ø Monitor signs/sxs • (Consider peak flows) Ø Increase frequency of SABA • Albuterol HFA 4 -8 puffs q 20 min X 3, then every 1 -4 hours Ø Oral steroids • 1 -2 mg/kg for 3 to 10 days Ø Doubling ICS not sufficient v ED/HOSPITAL Ø Ø Ø Supplemental O 2 SABA for all Ipratropium in ED only Systemic steroids Consider adjuncts (magnesium, heliox) Ø Does not recommend: methylxanthines, antibiotics, excessive hydration, chest PT, mucolytics, sedation
TREATMENT OF ACUTE ASTHMA – new recommendations v HOME Ø Action plan Ø Monitor signs/sxs • (Consider peak flows) Ø Increase frequency of SABA • Albuterol HFA 4 -8 puffs q 20 min X 3, then every 1 -4 hours Ø Oral steroids • 1 -2 mg/kg for 3 to 10 days Ø Doubling ICS not sufficient v ED/HOSPITAL Ø Ø Ø Supplemental O 2 SABA for all Ipratropium in ED only Systemic steroids Consider adjuncts (magnesium, heliox) Ø Does not recommend: methylxanthines, antibiotics, excessive hydration, chest PT, mucolytics, sedation
 DISCHARGE TO HOME v. At ED or hospital D/C ØWritten discharge plan ØMedications • SABA, oral steroids to complete course • Consider ICS for 1 -2 months ØTechniques –devices, self-monitoring ØFollow-up ØReferral for education, specialty care (if indicated)
DISCHARGE TO HOME v. At ED or hospital D/C ØWritten discharge plan ØMedications • SABA, oral steroids to complete course • Consider ICS for 1 -2 months ØTechniques –devices, self-monitoring ØFollow-up ØReferral for education, specialty care (if indicated)
 QUESTIONS?
QUESTIONS?


