db369941f553849163117e1eef166a94.ppt
- Количество слайдов: 151
 Guidelines for Management of Ischaemic Stroke 2008 The European Stroke Organization - ESO - Executive Committee and Writing Committee
Guidelines for Management of Ischaemic Stroke 2008 The European Stroke Organization - ESO - Executive Committee and Writing Committee
 MISSION OF ESO To reduce the incidence and burden of stroke by changing the way stroke is viewed and treated in Europe Guidelines Ischaemic Stroke 2008
MISSION OF ESO To reduce the incidence and burden of stroke by changing the way stroke is viewed and treated in Europe Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 ESO Writing Committee • Chair: – Werner Hacke, Heidelberg, Germany • Co-Chairs: – Marie-Germaine Bousser, Paris, France – Gary Ford, Newcastle, UK Guidelines Ischaemic Stroke 2008
ESO Writing Committee • Chair: – Werner Hacke, Heidelberg, Germany • Co-Chairs: – Marie-Germaine Bousser, Paris, France – Gary Ford, Newcastle, UK Guidelines Ischaemic Stroke 2008
 ESO Writing Committee • Education, Referral and Emergency room – Co-Chairs: Michael Brainin, Krems, Austria; José Ferro, Lisbon, Portugal – Members: Charlotte Cordonnier, Lille, France; Heinrich P. Mattle, Bern, Switzerland; Keith Muir, Glasgow, UK; Peter D. Schellinger, Erlangen, Germany • Stroke Units – Co-Chairs: Hans-Christoph Diener, Essen, Germany; Peter Langhorne, Glasgow, UK – Members: Antony Davalos, Barcelona, Spain; Gary Ford, Newcastle, UK; Veronika Skvortsova, Moscow, Russia Guidelines Ischaemic Stroke 2008
ESO Writing Committee • Education, Referral and Emergency room – Co-Chairs: Michael Brainin, Krems, Austria; José Ferro, Lisbon, Portugal – Members: Charlotte Cordonnier, Lille, France; Heinrich P. Mattle, Bern, Switzerland; Keith Muir, Glasgow, UK; Peter D. Schellinger, Erlangen, Germany • Stroke Units – Co-Chairs: Hans-Christoph Diener, Essen, Germany; Peter Langhorne, Glasgow, UK – Members: Antony Davalos, Barcelona, Spain; Gary Ford, Newcastle, UK; Veronika Skvortsova, Moscow, Russia Guidelines Ischaemic Stroke 2008
 ESO Writing Committee • Imaging and Diagnostics – Co-Chairs: Michael Hennerici, Mannheim, Germany; Markku Kaste, Helsinki, Finland – Members: Hugh S. Markus, London, UK; E. Bernd Ringelstein, Münster, Germany; Rüdiger von Kummer, Dresden, Germany; Joanna Wardlaw, Edinburgh, UK • Prevention – Co-Chairs: Phil Bath, Nottingham, UK; Didier Leys, Lille, France – Members: Álvaro Cervera, Barcelona, Spain; László Csiba, Debrecen, Hungary; Jan Lodder, Maastricht, The Netherlands; Nils Gunnar Wahlgren, Stockholm Guidelines Ischaemic Stroke 2008
ESO Writing Committee • Imaging and Diagnostics – Co-Chairs: Michael Hennerici, Mannheim, Germany; Markku Kaste, Helsinki, Finland – Members: Hugh S. Markus, London, UK; E. Bernd Ringelstein, Münster, Germany; Rüdiger von Kummer, Dresden, Germany; Joanna Wardlaw, Edinburgh, UK • Prevention – Co-Chairs: Phil Bath, Nottingham, UK; Didier Leys, Lille, France – Members: Álvaro Cervera, Barcelona, Spain; László Csiba, Debrecen, Hungary; Jan Lodder, Maastricht, The Netherlands; Nils Gunnar Wahlgren, Stockholm Guidelines Ischaemic Stroke 2008
 ESO Writing Committee • General Treatment – Co-Chairs: Christoph Diener, Essen, Germany; Peter Langhorne, Glasgow, UK – Members: Antony Davalos, Barcelona, Spain; Gary Ford, Newcastle, UK; Veronika Skvortsova, Moscow, Russia • Acute Treatment and Treatment of Complications – Co-Chairs: Angel Chamorro, Barcelona, Spain; Bo Norrving, Lund, Sweden – Members: Valerica Caso, Perugia, Italy; Jean-Louis Mas, Paris, France; Victor Obach, Barcelona, Spain; Peter A. Ringleb, Heidelberg, Germany; Lars Thomassen, Bergen, Norway Guidelines Ischaemic Stroke 2008
ESO Writing Committee • General Treatment – Co-Chairs: Christoph Diener, Essen, Germany; Peter Langhorne, Glasgow, UK – Members: Antony Davalos, Barcelona, Spain; Gary Ford, Newcastle, UK; Veronika Skvortsova, Moscow, Russia • Acute Treatment and Treatment of Complications – Co-Chairs: Angel Chamorro, Barcelona, Spain; Bo Norrving, Lund, Sweden – Members: Valerica Caso, Perugia, Italy; Jean-Louis Mas, Paris, France; Victor Obach, Barcelona, Spain; Peter A. Ringleb, Heidelberg, Germany; Lars Thomassen, Bergen, Norway Guidelines Ischaemic Stroke 2008
 ESO Writing Committee • Rehabilitation – Co-Chairs: Kennedy Lees, Glasgow, UK; Danilo Toni, Rome, Italy – Members: Stefano Paolucci, Rome, Italy; Juhani Sivenius, Kuopio, Finland; Katharina Stibrant Sunnerhagen, Göteborg, Sweden; Marion F. Walker, Nottingham, UK; Substantial assistance: Yvonne Teuschl, Isabel Henriques, Terence Quinn Guidelines Ischaemic Stroke 2008
ESO Writing Committee • Rehabilitation – Co-Chairs: Kennedy Lees, Glasgow, UK; Danilo Toni, Rome, Italy – Members: Stefano Paolucci, Rome, Italy; Juhani Sivenius, Kuopio, Finland; Katharina Stibrant Sunnerhagen, Göteborg, Sweden; Marion F. Walker, Nottingham, UK; Substantial assistance: Yvonne Teuschl, Isabel Henriques, Terence Quinn Guidelines Ischaemic Stroke 2008
 Definitions of Levels of Evidence Level A Established as useful/predictive or not useful/predictive for a diagnostic measure or established as effective, ineffective or harmful for a therapeutic intervention; requires at least one convincing Class I study or at least two consistent, convincing Class II studies. Level B Established as useful/predictive or not useful/predictive for a diagnostic measure or established as effective, ineffective or harmful for a therapeutic intervention; requires at least one convincing Class II study or overwhelming Class III evidence. Level C Established as useful/predictive or not useful/predictive for a diagnostic measure or established as effective, ineffective or harmful for a therapeutic intervention; requires at least two Class III studies. Good Clinical Practice (GCP) Recommended best practice based on the experience of the guideline development group. Usually based on Class IV evidence indicating large clinical uncertainty, such GCP points can be useful for health workers. Guidelines Ischaemic Stroke 2008
Definitions of Levels of Evidence Level A Established as useful/predictive or not useful/predictive for a diagnostic measure or established as effective, ineffective or harmful for a therapeutic intervention; requires at least one convincing Class I study or at least two consistent, convincing Class II studies. Level B Established as useful/predictive or not useful/predictive for a diagnostic measure or established as effective, ineffective or harmful for a therapeutic intervention; requires at least one convincing Class II study or overwhelming Class III evidence. Level C Established as useful/predictive or not useful/predictive for a diagnostic measure or established as effective, ineffective or harmful for a therapeutic intervention; requires at least two Class III studies. Good Clinical Practice (GCP) Recommended best practice based on the experience of the guideline development group. Usually based on Class IV evidence indicating large clinical uncertainty, such GCP points can be useful for health workers. Guidelines Ischaemic Stroke 2008
 Classification of Evidence classification scheme for a therapeutic intervention Class I An adequately powered, prospective, randomized, controlled clinical trial with masked outcome assessment in a representative population or an adequately powered systematic review of prospective randomized controlled clinical trials with masked outcome assessment in representative populations. Class II Prospective matched-group cohort study in a representative population with masked outcome assessment or a randomized, controlled trial in a representative population that lacks one criterion for class I evidence. Class III All other controlled trials (including well-defined natural history controls or patients serving as own controls) in a representative population, where outcome assessment is independent of patient treatment. Class IV Evidence from uncontrolled studies, case series, case reports, or expert opinion. Guidelines Ischaemic Stroke 2008
Classification of Evidence classification scheme for a therapeutic intervention Class I An adequately powered, prospective, randomized, controlled clinical trial with masked outcome assessment in a representative population or an adequately powered systematic review of prospective randomized controlled clinical trials with masked outcome assessment in representative populations. Class II Prospective matched-group cohort study in a representative population with masked outcome assessment or a randomized, controlled trial in a representative population that lacks one criterion for class I evidence. Class III All other controlled trials (including well-defined natural history controls or patients serving as own controls) in a representative population, where outcome assessment is independent of patient treatment. Class IV Evidence from uncontrolled studies, case series, case reports, or expert opinion. Guidelines Ischaemic Stroke 2008
 Classification of Evidence classification scheme for a diagnostic measure Class I A prospective study in a broad spectrum of persons with the suspected condition, using a ‘gold standard’ for case definition, where the test is applied in a blinded evaluation, and enabling the assessment of appropriate tests of diagnostic accuracy. Class II A prospective study of a narrow spectrum of persons with the suspected condition, or a well-designed retrospective study of a broad spectrum of persons with an established condition (by ‘gold standard’) compared to a broad spectrum of controls, where test is applied in a blinded evaluation, and enabling the assessment of appropriate tests of diagnostic accuracy. Class III Evidence provided by a retrospective study where either persons with the established condition or controls are of a narrow spectrum, and where test is applied in a blinded evaluation. Class IV Evidence from uncontrolled studies, case series, case reports, or expert opinion. Guidelines Ischaemic Stroke 2008
Classification of Evidence classification scheme for a diagnostic measure Class I A prospective study in a broad spectrum of persons with the suspected condition, using a ‘gold standard’ for case definition, where the test is applied in a blinded evaluation, and enabling the assessment of appropriate tests of diagnostic accuracy. Class II A prospective study of a narrow spectrum of persons with the suspected condition, or a well-designed retrospective study of a broad spectrum of persons with an established condition (by ‘gold standard’) compared to a broad spectrum of controls, where test is applied in a blinded evaluation, and enabling the assessment of appropriate tests of diagnostic accuracy. Class III Evidence provided by a retrospective study where either persons with the established condition or controls are of a narrow spectrum, and where test is applied in a blinded evaluation. Class IV Evidence from uncontrolled studies, case series, case reports, or expert opinion. Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke as an Emergency • Background – Stroke is the most important cause of morbidity and long term disability in Europe 1 – Demographic changes are likely to result in an increase in both incidence and prevalence – Stroke is also the second most common cause of dementia, the most frequent cause of epilepsy in the elderly, and a frequent cause of depression 2, 3 1: Lopez AD et al. Lancet (2006) 367: 1747 -1757 2: Rothwell PM et al. Lancet (2005) 366: 1773 -1783 3: O'Brien JT et al. Lancet Neurol (2003) 2: 89 -98 Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke as an Emergency • Background – Stroke is the most important cause of morbidity and long term disability in Europe 1 – Demographic changes are likely to result in an increase in both incidence and prevalence – Stroke is also the second most common cause of dementia, the most frequent cause of epilepsy in the elderly, and a frequent cause of depression 2, 3 1: Lopez AD et al. Lancet (2006) 367: 1747 -1757 2: Rothwell PM et al. Lancet (2005) 366: 1773 -1783 3: O'Brien JT et al. Lancet Neurol (2003) 2: 89 -98 Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke as an Emergency • Background – Stroke is a medical and occasionally a surgical emergency – The majority of ischaemic stroke patients do not reach the hospital quickly enough – The delay between stroke onset and hospital admission is; • reduced if the Emergency Medical Systems (EMS) are used • increased if doctors outside the hospital are consulted first Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke as an Emergency • Background – Stroke is a medical and occasionally a surgical emergency – The majority of ischaemic stroke patients do not reach the hospital quickly enough – The delay between stroke onset and hospital admission is; • reduced if the Emergency Medical Systems (EMS) are used • increased if doctors outside the hospital are consulted first Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke as an Emergency • Emergency care in acute stroke depends on a four-step chain: – Rapid recognition of, and reaction to, stroke signs and symptoms – Immediate EMS contact and priority EMS dispatch – Priority transport with notification of the receiving hospital – Immediate emergency room triage, clinical, laboratory and imaging evaluation, accurate diagnosis, and administration of appropriate treatments at the receiving hospital. Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke as an Emergency • Emergency care in acute stroke depends on a four-step chain: – Rapid recognition of, and reaction to, stroke signs and symptoms – Immediate EMS contact and priority EMS dispatch – Priority transport with notification of the receiving hospital – Immediate emergency room triage, clinical, laboratory and imaging evaluation, accurate diagnosis, and administration of appropriate treatments at the receiving hospital. Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke as an Emergency • Delays during acute stroke management have been identified at three different levels 1 – at the population level, due to failure to recognize the symptoms of stroke and contact emergency services – at the level of the emergency services and emergency physicians, due to a failure to prioritize transport of stroke patients – at the hospital level, due to delays in neuroimaging and inefficient in-hospital care 1: Kwan J et al. Ageing (2004) 33: 116 -121 Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke as an Emergency • Delays during acute stroke management have been identified at three different levels 1 – at the population level, due to failure to recognize the symptoms of stroke and contact emergency services – at the level of the emergency services and emergency physicians, due to a failure to prioritize transport of stroke patients – at the hospital level, due to delays in neuroimaging and inefficient in-hospital care 1: Kwan J et al. Ageing (2004) 33: 116 -121 Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Education Recommendations § Educational programmes to increase awareness of stroke at the population level are recommended (Class II, Level B) § Educational programmes to increase stroke awareness among professionals (paramedics, emergency physicians) are recommended (Class II, Level B) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Education Recommendations § Educational programmes to increase awareness of stroke at the population level are recommended (Class II, Level B) § Educational programmes to increase stroke awareness among professionals (paramedics, emergency physicians) are recommended (Class II, Level B) Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Referral Recommendations (1/2) § Immediate EMS contact and priority EMS dispatch are recommended (Class II, Level B) § Priority transport with advance notification of the receiving hospital is recommended (Class III, Level B) § Suspected stroke victims should be transported without delay to the nearest medical centre with a stroke unit that can provide ultra-early treatment (Class III, Level B) § Patients with suspected TIA should be referred without delay to a TIA clinic or a stroke unit (Class III, Level B) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Referral Recommendations (1/2) § Immediate EMS contact and priority EMS dispatch are recommended (Class II, Level B) § Priority transport with advance notification of the receiving hospital is recommended (Class III, Level B) § Suspected stroke victims should be transported without delay to the nearest medical centre with a stroke unit that can provide ultra-early treatment (Class III, Level B) § Patients with suspected TIA should be referred without delay to a TIA clinic or a stroke unit (Class III, Level B) Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Referral Recommendations (2/2) § Dispatchers and ambulance personnel should be trained to recognise stroke using simple instruments such as the Face-Arm-Speech-Test (Class IV, GCP) § Immediate emergency room triage, clinical, laboratory and imaging evaluation, accurate diagnosis, therapeutic decision and administration of appropriate treatments are recommended (Class III, Level B) § In remote or rural areas helicopter transfer and telemedicine should be considered to improve access to treatment (Class III, Level C) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Referral Recommendations (2/2) § Dispatchers and ambulance personnel should be trained to recognise stroke using simple instruments such as the Face-Arm-Speech-Test (Class IV, GCP) § Immediate emergency room triage, clinical, laboratory and imaging evaluation, accurate diagnosis, therapeutic decision and administration of appropriate treatments are recommended (Class III, Level B) § In remote or rural areas helicopter transfer and telemedicine should be considered to improve access to treatment (Class III, Level C) Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Emergency Management • The time window for treatment of patients with acute stroke is narrow – Acute emergency management of stroke requires parallel processes operating at different levels of patient management – Acute assessment of neurological and vital functions parallels the treatment of acutely life-threatening conditions • Time is the most important factor Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Emergency Management • The time window for treatment of patients with acute stroke is narrow – Acute emergency management of stroke requires parallel processes operating at different levels of patient management – Acute assessment of neurological and vital functions parallels the treatment of acutely life-threatening conditions • Time is the most important factor Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Emergency Management • The initial examination should include – Observation of breathing and pulmonary function and concomitant heart disease – Assessment of blood pressure and heart rate – Determination of arterial oxygen saturation – Blood samples for clinical chemistry, coagulation and haematology studies – Observation of early signs of dysphagia – Targeted neurological examination – Careful medical history focussing on risk factors for arteriosclerosis and cardiac disease Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Emergency Management • The initial examination should include – Observation of breathing and pulmonary function and concomitant heart disease – Assessment of blood pressure and heart rate – Determination of arterial oxygen saturation – Blood samples for clinical chemistry, coagulation and haematology studies – Observation of early signs of dysphagia – Targeted neurological examination – Careful medical history focussing on risk factors for arteriosclerosis and cardiac disease Guidelines Ischaemic Stroke 2008
 Ancillary Diagnostic Tests • In all patients Diagnostics – Brain Imaging: CT or MRI – ECG – Laboratory Tests • Complete blood count and platelet count, prothrombin time or INR, PTT • Serum electrolytes, blood glucose • CRP or sedimentation rate • Hepatic and renal chemical analysis Guidelines Ischaemic Stroke 2008
Ancillary Diagnostic Tests • In all patients Diagnostics – Brain Imaging: CT or MRI – ECG – Laboratory Tests • Complete blood count and platelet count, prothrombin time or INR, PTT • Serum electrolytes, blood glucose • CRP or sedimentation rate • Hepatic and renal chemical analysis Guidelines Ischaemic Stroke 2008
 Ancillary Diagnostic Tests • In selected patients Diagnostics – Duplex / Doppler ultrasound – MRA or CTA – Diffusion and perfusion MR or perfusion CT – Echocardiography, Chest X-ray – Pulse oximetry and arterial blood gas analysis – Lumbar puncture – EEG – Toxicology screen Guidelines Ischaemic Stroke 2008
Ancillary Diagnostic Tests • In selected patients Diagnostics – Duplex / Doppler ultrasound – MRA or CTA – Diffusion and perfusion MR or perfusion CT – Echocardiography, Chest X-ray – Pulse oximetry and arterial blood gas analysis – Lumbar puncture – EEG – Toxicology screen Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Emergency Management Recommendations § Organization of pre-hospital and in-hospital pathways and systems for acute stroke patients is recommended (Class III, Level C) § All patients should receive brain imaging, ECG, and laboratory tests. Additional diagnostic examinations are necessary in selected patients (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Emergency Management Recommendations § Organization of pre-hospital and in-hospital pathways and systems for acute stroke patients is recommended (Class III, Level C) § All patients should receive brain imaging, ECG, and laboratory tests. Additional diagnostic examinations are necessary in selected patients (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke Unit • A stroke unit – Is a dedicated and geographically defined part of a hospital that takes care of stroke patients – Has specialised staff with coordinated multidisciplinary expert approach to treatment and care – Comprises core disciplines: medical, nursing, physiotherapy, occupational therapy, speech and language therapy, social work 1 1: Langhorne P et al. Ageing (2002) 31: 365 -371 Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke Unit • A stroke unit – Is a dedicated and geographically defined part of a hospital that takes care of stroke patients – Has specialised staff with coordinated multidisciplinary expert approach to treatment and care – Comprises core disciplines: medical, nursing, physiotherapy, occupational therapy, speech and language therapy, social work 1 1: Langhorne P et al. Ageing (2002) 31: 365 -371 Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke Unit • Typical components of stroke units include – Assessment • Medical assessment and diagnosis, early assessment of nursing and therapy needs – Early management policies • Early mobilisation, prevention of complications, treatment of hypoxia, hyperglycaemia, pyrexia and dehydration – Ongoing rehabilitation policies • Coordinated multidisciplinary team care • Early assessments of needs after discharge Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke Unit • Typical components of stroke units include – Assessment • Medical assessment and diagnosis, early assessment of nursing and therapy needs – Early management policies • Early mobilisation, prevention of complications, treatment of hypoxia, hyperglycaemia, pyrexia and dehydration – Ongoing rehabilitation policies • Coordinated multidisciplinary team care • Early assessments of needs after discharge Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke Unit • Treatment at a stroke unit compared to treatment in a general ward 1 – reduces mortality (absolute risk reduction of 3%) – reduces dependency (5%) – reduces need for institutional care (2%) • All types of patients, irrespective of gender, age, stroke subtype and stroke severity, appear to benefit from treatment in stroke units 1 1: Stroke Unit Trialists' Collaboration Cochrane Rev (2007) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke Unit • Treatment at a stroke unit compared to treatment in a general ward 1 – reduces mortality (absolute risk reduction of 3%) – reduces dependency (5%) – reduces need for institutional care (2%) • All types of patients, irrespective of gender, age, stroke subtype and stroke severity, appear to benefit from treatment in stroke units 1 1: Stroke Unit Trialists' Collaboration Cochrane Rev (2007) Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Stroke Services and Stroke Units Recommendations § All stroke patients should be treated in a stroke unit (Class I, Level A) § Healthcare systems must ensure that acute stroke patients can access high technology medical and surgical stroke care when required (Class III, Level B) § The development of clinical networks, including telemedicine, is recommended to expand the access to high technology specialist stroke care (Class II, Level B) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Stroke Services and Stroke Units Recommendations § All stroke patients should be treated in a stroke unit (Class I, Level A) § Healthcare systems must ensure that acute stroke patients can access high technology medical and surgical stroke care when required (Class III, Level B) § The development of clinical networks, including telemedicine, is recommended to expand the access to high technology specialist stroke care (Class II, Level B) Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests • Differentiate between different types of stroke Diagnostics – Assess the underlying cause of brain ischaemia – Assess prognosis • Provide a basis for physiological monitoring of the stroke patient • Identify concurrent diseases or complications associated with stroke • Rule out other brain diseases Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests • Differentiate between different types of stroke Diagnostics – Assess the underlying cause of brain ischaemia – Assess prognosis • Provide a basis for physiological monitoring of the stroke patient • Identify concurrent diseases or complications associated with stroke • Rule out other brain diseases Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests Diagnostics • Cranial Computed Tomography (CT) – Immediate plain CT scanning distinguishes reliably between haemorrhagic and ischaemic stroke – Detects signs of ischaemia as early as 2 h after stroke onset 1 – Helps to identify other neurological diseases (e. g. neoplasms) – Most cost-effective strategy for imaging acute stroke patients 2 1: von Kummer R et al. Radiology (2001) 219: 95 -100 2: Wardlaw J et al. Stroke (2004) 35: 2477 -2483 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests Diagnostics • Cranial Computed Tomography (CT) – Immediate plain CT scanning distinguishes reliably between haemorrhagic and ischaemic stroke – Detects signs of ischaemia as early as 2 h after stroke onset 1 – Helps to identify other neurological diseases (e. g. neoplasms) – Most cost-effective strategy for imaging acute stroke patients 2 1: von Kummer R et al. Radiology (2001) 219: 95 -100 2: Wardlaw J et al. Stroke (2004) 35: 2477 -2483 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests Diagnostics • Magnetic Resonance Imaging (MRI) – Diffusion-weighted MRI (DWI) is more sensitive for detection of early ischaemic changes than CT – DWI can be negative in patients with definite stroke 1 – Identifies ischaemic lesions in the posterior fossa reliably – Detects even small intracerebral haemorrhages reliably on T 2* sequences – MRI is particularly important in acute stroke patients with unusual presentations 1: Ay H et al. Cerebrovasc Dis (2002) 14: 177 -186 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests Diagnostics • Magnetic Resonance Imaging (MRI) – Diffusion-weighted MRI (DWI) is more sensitive for detection of early ischaemic changes than CT – DWI can be negative in patients with definite stroke 1 – Identifies ischaemic lesions in the posterior fossa reliably – Detects even small intracerebral haemorrhages reliably on T 2* sequences – MRI is particularly important in acute stroke patients with unusual presentations 1: Ay H et al. Cerebrovasc Dis (2002) 14: 177 -186 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests Diagnostics • Mismatch Concept – Mismatch between tissue abnormal on DWI and tissue with reduced perfusion may reflect tissue at risk of further ischaemic damage 1 – There is disagreement on how to best identify irreversible ischaemic brain injury and to define critically impaired blood flow 2 – There is no clear evidence that patients with particular perfusion patterns are more or less likely to benefit from thrombolysis 3 1: Jansen O et al. Lancet (1999) 353: 2036 -2037 2: Kane I et al. Stroke (2007) 38: 3158 -3164 3: Albers GW et al. Ann Neurol (2006) 60: 508 -517 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests Diagnostics • Mismatch Concept – Mismatch between tissue abnormal on DWI and tissue with reduced perfusion may reflect tissue at risk of further ischaemic damage 1 – There is disagreement on how to best identify irreversible ischaemic brain injury and to define critically impaired blood flow 2 – There is no clear evidence that patients with particular perfusion patterns are more or less likely to benefit from thrombolysis 3 1: Jansen O et al. Lancet (1999) 353: 2036 -2037 2: Kane I et al. Stroke (2007) 38: 3158 -3164 3: Albers GW et al. Ann Neurol (2006) 60: 508 -517 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests Diagnostics • Ultrasound studies – Cerebrovascular ultrasound is fast and non-invasive and can be administered using portable machines. – It is therefore applicable to patients unable to cooperate with MRA or CTA 1 – Combinations of ultrasound imaging techniques and MRA can produce excellent results that are equal to Digital subtraction angiography (DSA)2 1: Allendörfer J et al. Lancet Neurology (2005) 5: 835 -840 2: Nederkoorn P et al. Stroke (2003) 34: 1324 -1332 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests Diagnostics • Ultrasound studies – Cerebrovascular ultrasound is fast and non-invasive and can be administered using portable machines. – It is therefore applicable to patients unable to cooperate with MRA or CTA 1 – Combinations of ultrasound imaging techniques and MRA can produce excellent results that are equal to Digital subtraction angiography (DSA)2 1: Allendörfer J et al. Lancet Neurology (2005) 5: 835 -840 2: Nederkoorn P et al. Stroke (2003) 34: 1324 -1332 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests • Imaging in TIA-patients Diagnostics – Up to 10% recurrence risk in the first 48 hours 1 – Simple clinical scoring systems can be used to identify patients at particularly high risk 1 – Up to 50% of patients with TIAs have acute ischaemic lesions on DWI. These patients are at increased risk of early recurrent disabling stroke 2 – There is currently no evidence that DWI provides better stroke prediction than clinical risk scores 3 1: Rothwell P et al. Lancet Neurol (2005) 5: 323 -331 2: Coutts S et al. Ann Neurol (2005) 57: 848 -854 3: Redgrave J et al. Stroke (2007) 38: 1482 -1488 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests • Imaging in TIA-patients Diagnostics – Up to 10% recurrence risk in the first 48 hours 1 – Simple clinical scoring systems can be used to identify patients at particularly high risk 1 – Up to 50% of patients with TIAs have acute ischaemic lesions on DWI. These patients are at increased risk of early recurrent disabling stroke 2 – There is currently no evidence that DWI provides better stroke prediction than clinical risk scores 3 1: Rothwell P et al. Lancet Neurol (2005) 5: 323 -331 2: Coutts S et al. Ann Neurol (2005) 57: 848 -854 3: Redgrave J et al. Stroke (2007) 38: 1482 -1488 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests Diagnostics • Electrocardiogram (ECG) – Cardiac abnormalities are common in acute stroke patients 1 – Arrhythmias may induce stroke, stroke may cause arrhythmias – Holter monitoring is superior to routine ECG for the detection of atrial fibrillation (AF)2 – It is unclear whether continuous ECG recording at the bedside is equivalent to Holter monitoring for the detection of AF 1: Christensen H et al. Neurol Sci (2005) 234: 99 – 103 2: Gunalp M et al. Adv Ther (2006) 23: 854 -60 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests Diagnostics • Electrocardiogram (ECG) – Cardiac abnormalities are common in acute stroke patients 1 – Arrhythmias may induce stroke, stroke may cause arrhythmias – Holter monitoring is superior to routine ECG for the detection of atrial fibrillation (AF)2 – It is unclear whether continuous ECG recording at the bedside is equivalent to Holter monitoring for the detection of AF 1: Christensen H et al. Neurol Sci (2005) 234: 99 – 103 2: Gunalp M et al. Adv Ther (2006) 23: 854 -60 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests Diagnostics • Echocardiography (TTE / TOE) – Echocardiography can detect many potential causes of stroke 1 – It is particularly required in patients with history of cardiac disease, ECG pathologies, suspected source of embolism, suspected aortic disease, suspected paradoxical embolism – Transoesophageal echocardiography (TOE) might be superior to transthoracic echocardiography (TTE) for the detection of potential cardiac sources of embolism 2 1: Lerakis S et al. Am J Med Sci (2005) 329: 310 -6 2: de Bruijn SF et al. Stroke (2006) 37: 2531 -4 Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests Diagnostics • Echocardiography (TTE / TOE) – Echocardiography can detect many potential causes of stroke 1 – It is particularly required in patients with history of cardiac disease, ECG pathologies, suspected source of embolism, suspected aortic disease, suspected paradoxical embolism – Transoesophageal echocardiography (TOE) might be superior to transthoracic echocardiography (TTE) for the detection of potential cardiac sources of embolism 2 1: Lerakis S et al. Am J Med Sci (2005) 329: 310 -6 2: de Bruijn SF et al. Stroke (2006) 37: 2531 -4 Guidelines Ischaemic Stroke 2008
 Emergency Diagnostic Tests • Laboratory tests Diagnostics – Haematology (RBC, WBC, platelet count) – Basic clotting parameters – Electrolytes – Renal and hepatic chemistry – Blood Glucose – CRP, sedimentation rate Guidelines Ischaemic Stroke 2008
Emergency Diagnostic Tests • Laboratory tests Diagnostics – Haematology (RBC, WBC, platelet count) – Basic clotting parameters – Electrolytes – Renal and hepatic chemistry – Blood Glucose – CRP, sedimentation rate Guidelines Ischaemic Stroke 2008
 Education, Referral, Emergency management Diagnostic Imaging Recommendations § In patients with suspected TIA or stroke, urgent cranial CT (Class I), or alternatively MRI (Class II), is recommended (Level A) § If MRI is used, the inclusion of diffusion weighted imaging (DWI) and T 2*-weighted gradient echo sequences is recommended (Class II, Level A) § In patients with TIA, minor stroke, or early spontaneous recovery immediate diagnostic work-up, including urgent vascular imaging (ultrasound, CT-angiography, or MR angiography) is recommended (Class I, Level A) Guidelines Ischaemic Stroke 2008
Education, Referral, Emergency management Diagnostic Imaging Recommendations § In patients with suspected TIA or stroke, urgent cranial CT (Class I), or alternatively MRI (Class II), is recommended (Level A) § If MRI is used, the inclusion of diffusion weighted imaging (DWI) and T 2*-weighted gradient echo sequences is recommended (Class II, Level A) § In patients with TIA, minor stroke, or early spontaneous recovery immediate diagnostic work-up, including urgent vascular imaging (ultrasound, CT-angiography, or MR angiography) is recommended (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Other Diagnostics Recommendations (1/2) § In patients with acute stroke and TIA, early evaluation of physiological parameters, routine blood tests, and electrocardiography (ECG) is recommended (Class I, Level A) § All acute stroke and TIA patients should have a 12 channel ECG. Continuous ECG recording is recommended for ischaemic stroke and TIA patients (Class I, Level A) Guidelines Ischaemic Stroke 2008
Other Diagnostics Recommendations (1/2) § In patients with acute stroke and TIA, early evaluation of physiological parameters, routine blood tests, and electrocardiography (ECG) is recommended (Class I, Level A) § All acute stroke and TIA patients should have a 12 channel ECG. Continuous ECG recording is recommended for ischaemic stroke and TIA patients (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Other Diagnostics Recommendations (2/2) § For stroke and TIA patients seen after the acute phase, 24 -hour Holter ECG monitoring should be performed when arrhythmias are suspected and no other causes of stroke are found (Class I, Level A) § For all stroke and TIA patients, a sequence of blood tests is recommended § Echocardiography is recommended in selected patients (Class III, Level B) Guidelines Ischaemic Stroke 2008
Other Diagnostics Recommendations (2/2) § For stroke and TIA patients seen after the acute phase, 24 -hour Holter ECG monitoring should be performed when arrhythmias are suspected and no other causes of stroke are found (Class I, Level A) § For all stroke and TIA patients, a sequence of blood tests is recommended § Echocardiography is recommended in selected patients (Class III, Level B) Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Primary Prevention • Content – Management of vascular risk factors – Antithrombotic therapy – Carotid surgery and angioplasty Guidelines Ischaemic Stroke 2008
Primary Prevention • Content – Management of vascular risk factors – Antithrombotic therapy – Carotid surgery and angioplasty Guidelines Ischaemic Stroke 2008
 Vascular Risk Factors Primary Prevention • Conditions and lifestyle characteristics identified as a risk factors for stroke High blood pressure High Cholesterol Atrial fibrillation Hyper-homocysteinaemia Diabetes mellitus Smoking Carotid artery disease Heavy alcohol use Myocardial infarction Physical inactivity Obesity Guidelines Ischaemic Stroke 2008
Vascular Risk Factors Primary Prevention • Conditions and lifestyle characteristics identified as a risk factors for stroke High blood pressure High Cholesterol Atrial fibrillation Hyper-homocysteinaemia Diabetes mellitus Smoking Carotid artery disease Heavy alcohol use Myocardial infarction Physical inactivity Obesity Guidelines Ischaemic Stroke 2008
 High blood pressure (BP) Primary Prevention • Background – High blood pressure (>120/80 mm. Hg) is the most important and prevalent modifiable risk factor for stroke – Significant reduction of stroke incidence with a decrease in BP 1 – No class of antihypertensive is clearly superior • LIFE: lorsatan is superior to atenolol 2 • ALLHAT: chlorthalidone is more effective than amlodipine and lisinopril 3 1: Neal B et al. Lancet (2000) 356: 1955 -64 2: Dahlof B et al. Lancet (2002) 359: 995 -1003. 3: Mancia G et al. Eur Heart J (2007) 28: 1462 -536 Guidelines Ischaemic Stroke 2008
High blood pressure (BP) Primary Prevention • Background – High blood pressure (>120/80 mm. Hg) is the most important and prevalent modifiable risk factor for stroke – Significant reduction of stroke incidence with a decrease in BP 1 – No class of antihypertensive is clearly superior • LIFE: lorsatan is superior to atenolol 2 • ALLHAT: chlorthalidone is more effective than amlodipine and lisinopril 3 1: Neal B et al. Lancet (2000) 356: 1955 -64 2: Dahlof B et al. Lancet (2002) 359: 995 -1003. 3: Mancia G et al. Eur Heart J (2007) 28: 1462 -536 Guidelines Ischaemic Stroke 2008
 Diabetes mellitus Primary Prevention • Background – Independent risk factor for ischaemic stroke – Improving glucose control may not reduce stroke 1 – BP in patients with diabetes should be <130/80 mm. Hg 2 – Statin treatment reduces the risk of major vascular events, including stroke 3 – Elevated blood glucose in the early phase of stroke is associated with death and poor recovery 1: Turner RC et al. JAMA (1999) 281: 2005 -12 2: Mancia GJ: Hypertens Suppl (2007) 25: S 7 -12 3: Sever PS et al. Diabetes Care (2005) 28: 1151 -7 Guidelines Ischaemic Stroke 2008
Diabetes mellitus Primary Prevention • Background – Independent risk factor for ischaemic stroke – Improving glucose control may not reduce stroke 1 – BP in patients with diabetes should be <130/80 mm. Hg 2 – Statin treatment reduces the risk of major vascular events, including stroke 3 – Elevated blood glucose in the early phase of stroke is associated with death and poor recovery 1: Turner RC et al. JAMA (1999) 281: 2005 -12 2: Mancia GJ: Hypertens Suppl (2007) 25: S 7 -12 3: Sever PS et al. Diabetes Care (2005) 28: 1151 -7 Guidelines Ischaemic Stroke 2008
 High Cholesterol Primary Prevention • Background – Statin treatment reduces the incidence of stroke from 3. 4% to 2. 7%1 – No significant effect for prevention of fatal stroke 1 – Heart Protection Study found an excess of myopathy of one per 10, 000 patients per annum 2 – No data support statin treatment in patients with LDLcholesterol <150 mg/dl (3. 9 mmol/l) 1: Amarenco P et al. : Stroke (2004) 35: 2902 -2909 2: HPS Group: Lancet (2002) 360: 7 -22. Guidelines Ischaemic Stroke 2008
High Cholesterol Primary Prevention • Background – Statin treatment reduces the incidence of stroke from 3. 4% to 2. 7%1 – No significant effect for prevention of fatal stroke 1 – Heart Protection Study found an excess of myopathy of one per 10, 000 patients per annum 2 – No data support statin treatment in patients with LDLcholesterol <150 mg/dl (3. 9 mmol/l) 1: Amarenco P et al. : Stroke (2004) 35: 2902 -2909 2: HPS Group: Lancet (2002) 360: 7 -22. Guidelines Ischaemic Stroke 2008
 Cigarette Smoking Primary Prevention • Background – Independent risk factor for ischaemic stroke in men and women – 2 -3 fold increased risk compared to non-smokers 1 – Spousal cigarette smoking may be associated with an increased stroke risk 2 – 50% risk reduction by 2 years after stopping smoking 3 1: Shinton R et al. : BMJ (1989) 298: 789 -94. 2: Qureshi A et al. : Stroke (2005) 36: 74 -76 3: Colditz GA et al. : N Engl J Med (1988) 318: 937 -41. Guidelines Ischaemic Stroke 2008
Cigarette Smoking Primary Prevention • Background – Independent risk factor for ischaemic stroke in men and women – 2 -3 fold increased risk compared to non-smokers 1 – Spousal cigarette smoking may be associated with an increased stroke risk 2 – 50% risk reduction by 2 years after stopping smoking 3 1: Shinton R et al. : BMJ (1989) 298: 789 -94. 2: Qureshi A et al. : Stroke (2005) 36: 74 -76 3: Colditz GA et al. : N Engl J Med (1988) 318: 937 -41. Guidelines Ischaemic Stroke 2008
 Alcohol Consumption Primary Prevention • Background – Increased risk for both ischaemic (RR 1. 69) and haemorrhagic stroke (RR 2. 18) with heavy alcohol consumption (>60 g/day)1 – BP elevation might be a reasonable explanation 3 – Light alcohol consumption (<12 g/day) associated with reduced ischaemic (RR 0. 80) and haemorrhagic stroke 1 – Red wine consumption carries the lowest risk 2 1: Reynolds K et al. : JAMA (2003) 289: 579 -88 2: Mukamal K et al. : Ann Intern Med (2005) 142: 11 -19 3: Bazzano LA et al. : Ann Neurol (2007) Guidelines Ischaemic Stroke 2008
Alcohol Consumption Primary Prevention • Background – Increased risk for both ischaemic (RR 1. 69) and haemorrhagic stroke (RR 2. 18) with heavy alcohol consumption (>60 g/day)1 – BP elevation might be a reasonable explanation 3 – Light alcohol consumption (<12 g/day) associated with reduced ischaemic (RR 0. 80) and haemorrhagic stroke 1 – Red wine consumption carries the lowest risk 2 1: Reynolds K et al. : JAMA (2003) 289: 579 -88 2: Mukamal K et al. : Ann Intern Med (2005) 142: 11 -19 3: Bazzano LA et al. : Ann Neurol (2007) Guidelines Ischaemic Stroke 2008
 Physical Activity Primary Prevention • Background – Regular exercise (at least 3 x 30 min/week) is associated with a decreased risk of stroke – Physically active individuals have a lower risk of stroke or death than those with low activity (RR 0. 73)1 – This is mediated, in part, through beneficial effects on body weight, blood pressure, serum cholesterol, and glucose tolerance 2 1: Lee C et al. : Stroke (2003) 34: 2475 -2481 2: Deplanque D et al. : Neurology (2006) 67: 1403 -1410) Guidelines Ischaemic Stroke 2008
Physical Activity Primary Prevention • Background – Regular exercise (at least 3 x 30 min/week) is associated with a decreased risk of stroke – Physically active individuals have a lower risk of stroke or death than those with low activity (RR 0. 73)1 – This is mediated, in part, through beneficial effects on body weight, blood pressure, serum cholesterol, and glucose tolerance 2 1: Lee C et al. : Stroke (2003) 34: 2475 -2481 2: Deplanque D et al. : Neurology (2006) 67: 1403 -1410) Guidelines Ischaemic Stroke 2008
 Body Weight, Diet, Nutrition Primary Prevention • Background – High body mass index (BMI ≥ 25) increases risk of stroke in men and women 1 – Abdominal adiposity is a risk factor for stroke in men but not women 2 – A randomized trial in women found no effect of dietary interventions to reduce the incidence of stroke 3 – Tocopherol and beta carotene supplementation do not reduce the risk of stroke. Vitamin E might increase mortality when used at high-dose (≥ 400 IU/d) 1: Kurth T et al. : Circulation (2005) 111: 1992 -1998 2: Hu G et al. : Arch Intern Med (2007) 167: 1420 -1427 3: Howard B et al. : JAMA (2006) 295: 655 -666 Guidelines Ischaemic Stroke 2008
Body Weight, Diet, Nutrition Primary Prevention • Background – High body mass index (BMI ≥ 25) increases risk of stroke in men and women 1 – Abdominal adiposity is a risk factor for stroke in men but not women 2 – A randomized trial in women found no effect of dietary interventions to reduce the incidence of stroke 3 – Tocopherol and beta carotene supplementation do not reduce the risk of stroke. Vitamin E might increase mortality when used at high-dose (≥ 400 IU/d) 1: Kurth T et al. : Circulation (2005) 111: 1992 -1998 2: Hu G et al. : Arch Intern Med (2007) 167: 1420 -1427 3: Howard B et al. : JAMA (2006) 295: 655 -666 Guidelines Ischaemic Stroke 2008
 Hormone Replacement Therapy Primary Prevention • Background – Stroke rates rise rapidly in women after the menopause – Hormone replacement therapy in postmenopausal women is associated with an 44% increased risk of stroke 1 1: Gabriel S et al. : Cochrane Review (2005) CD 002229 Guidelines Ischaemic Stroke 2008
Hormone Replacement Therapy Primary Prevention • Background – Stroke rates rise rapidly in women after the menopause – Hormone replacement therapy in postmenopausal women is associated with an 44% increased risk of stroke 1 1: Gabriel S et al. : Cochrane Review (2005) CD 002229 Guidelines Ischaemic Stroke 2008
 Risk Factor Management Primary Prevention Recommendations (1/4) § Blood pressure should be checked regularly. High blood pressure should be managed with lifestyle modification and individualized pharmacological therapy (Class I, Level A) aiming at normal levels of 120/80 mm. Hg (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Risk Factor Management Primary Prevention Recommendations (1/4) § Blood pressure should be checked regularly. High blood pressure should be managed with lifestyle modification and individualized pharmacological therapy (Class I, Level A) aiming at normal levels of 120/80 mm. Hg (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Risk Factor Management Primary Prevention Recommendations (2/4) § Blood glucose should be checked regularly. Diabetes should be managed with lifestyle modification and individualized pharmacological therapy (Class IV, Level C). § In diabetic patients, high blood pressure should be managed intensively (Class I, Level A) aiming for levels below 130/80 mm. Hg (Class IV, Level C). Where possible, treatment should include an angiotensin converting enzyme inhibitor or angiotensin receptor antagonist (Class I, Level A) Guidelines Ischaemic Stroke 2008
Risk Factor Management Primary Prevention Recommendations (2/4) § Blood glucose should be checked regularly. Diabetes should be managed with lifestyle modification and individualized pharmacological therapy (Class IV, Level C). § In diabetic patients, high blood pressure should be managed intensively (Class I, Level A) aiming for levels below 130/80 mm. Hg (Class IV, Level C). Where possible, treatment should include an angiotensin converting enzyme inhibitor or angiotensin receptor antagonist (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Risk Factor Management Primary Prevention Recommendations (3/4) § Blood cholesterol should be checked regularly. High blood cholesterol (e. g. LDL>150 mg/dl [3, 9 m. Mol/l]) should be managed with lifestyle modification (Class IV, Level C) and a statin (Class I, Level A) § Cigarette smoking should be discouraged (Class III, Level B) § Heavy use of alcohol should be discouraged (Class III, Level B) § Regular physical activity is recommended (Class III, Level B) Guidelines Ischaemic Stroke 2008
Risk Factor Management Primary Prevention Recommendations (3/4) § Blood cholesterol should be checked regularly. High blood cholesterol (e. g. LDL>150 mg/dl [3, 9 m. Mol/l]) should be managed with lifestyle modification (Class IV, Level C) and a statin (Class I, Level A) § Cigarette smoking should be discouraged (Class III, Level B) § Heavy use of alcohol should be discouraged (Class III, Level B) § Regular physical activity is recommended (Class III, Level B) Guidelines Ischaemic Stroke 2008
 Risk Factor Management Primary Prevention Recommendations (4/4) § A diet low in salt and saturated fat, high in fruit and vegetables and rich in fibre is recommended (Class III, Level B) § Subjects with an elevated body mass index are recommended to take a weight-reducing diet (Class III, Level B) § Antioxidant vitamin supplements are not recommended (Class I, Level A) § Hormone replacement therapy is not recommended for the primary prevention of stroke (Class I, Level A) Guidelines Ischaemic Stroke 2008
Risk Factor Management Primary Prevention Recommendations (4/4) § A diet low in salt and saturated fat, high in fruit and vegetables and rich in fibre is recommended (Class III, Level B) § Subjects with an elevated body mass index are recommended to take a weight-reducing diet (Class III, Level B) § Antioxidant vitamin supplements are not recommended (Class I, Level A) § Hormone replacement therapy is not recommended for the primary prevention of stroke (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Primary Prevention • Background – In low risk persons low dose aspirin reduced coronary events, but not stroke 1 – In women over 45 years aspirin reduces the risk of ischaemic stroke (OR 0. 76; 95%CI 0. 63 -0. 93) 2 – Aspirin reduces MI in patients with asymptomatic carotid artery disease 3 1: Bartolucci A et al. : Am J Cardiol (2006) 98: 746 -750 2: Berger J et al. : JAMA (2006) 295: 306 -313 3: Hobson R, 2 nd et al. : J Vasc Surg (1993) 17: 257 -263 Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Primary Prevention • Background – In low risk persons low dose aspirin reduced coronary events, but not stroke 1 – In women over 45 years aspirin reduces the risk of ischaemic stroke (OR 0. 76; 95%CI 0. 63 -0. 93) 2 – Aspirin reduces MI in patients with asymptomatic carotid artery disease 3 1: Bartolucci A et al. : Am J Cardiol (2006) 98: 746 -750 2: Berger J et al. : JAMA (2006) 295: 306 -313 3: Hobson R, 2 nd et al. : J Vasc Surg (1993) 17: 257 -263 Guidelines Ischaemic Stroke 2008
 Atrial fibrillation (AF) Primary Prevention • Background – Average stroke rate of 5% per year – Aspirin reduces stroke (RR 0. 78) in patients with nonvalvular AF 1 – Warfarin (INR 2. 0 -3. 0) is more effective than aspirin at reducing stroke (RR 0. 36; 95%CI 0. 26 -0. 51)1 – Combination of aspirin and clopidogrel is less effective than warfarin and has a similar bleeding rate 2 1: Hart RG et al. : Ann Intern Med (2007) 146: 857 -867 2: Connolly S et al. : Lancet (2006) 367: 1903 -1912 Guidelines Ischaemic Stroke 2008
Atrial fibrillation (AF) Primary Prevention • Background – Average stroke rate of 5% per year – Aspirin reduces stroke (RR 0. 78) in patients with nonvalvular AF 1 – Warfarin (INR 2. 0 -3. 0) is more effective than aspirin at reducing stroke (RR 0. 36; 95%CI 0. 26 -0. 51)1 – Combination of aspirin and clopidogrel is less effective than warfarin and has a similar bleeding rate 2 1: Hart RG et al. : Ann Intern Med (2007) 146: 857 -867 2: Connolly S et al. : Lancet (2006) 367: 1903 -1912 Guidelines Ischaemic Stroke 2008
 Atrial fibrillation (AF) Primary Prevention • Background – Anticoagulation with an INR below 2. 0 is not effective – Increased risk for bleeding complications with an INR > 3. 5 – Patients <65 years of age with “lone AF” (without other risk factors) are at low risk, whereas patients older than 65 years are at a higher risk for embolic stroke – Anticoagulation can be safe and effective in older individuals 1, 2 1: Rash A et al. : Ageing (2007) 36: 151 -156 2: Mant J et al. : Lancet (2007) 370: 493 -503 Guidelines Ischaemic Stroke 2008
Atrial fibrillation (AF) Primary Prevention • Background – Anticoagulation with an INR below 2. 0 is not effective – Increased risk for bleeding complications with an INR > 3. 5 – Patients <65 years of age with “lone AF” (without other risk factors) are at low risk, whereas patients older than 65 years are at a higher risk for embolic stroke – Anticoagulation can be safe and effective in older individuals 1, 2 1: Rash A et al. : Ageing (2007) 36: 151 -156 2: Mant J et al. : Lancet (2007) 370: 493 -503 Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Primary Prevention Recommendations (1/4) § Low-dose aspirin is recommended in women aged 45 years or more who are not at increased risk for intracerebral haemorrhage and who have good gastrointestinal tolerance; however, its effect is very small (Class I, Level A) § Low-dose aspirin may be considered in men for the primary prevention of myocardial infarction; however, it does not reduce the risk of ischaemic stroke (Class I, Level A) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Primary Prevention Recommendations (1/4) § Low-dose aspirin is recommended in women aged 45 years or more who are not at increased risk for intracerebral haemorrhage and who have good gastrointestinal tolerance; however, its effect is very small (Class I, Level A) § Low-dose aspirin may be considered in men for the primary prevention of myocardial infarction; however, it does not reduce the risk of ischaemic stroke (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Primary Prevention Recommendations (2/4) § Antiplatelet agents other than aspirin are not recommended for primary stroke prevention (Class IV, GCP) § Aspirin may be recommended for patients with nonvalvular AF who are younger than 65 years and free of vascular risk factors (Class I, Level A) § Unless contraindicated, either aspirin or an oral anticoagulant (international normalized ratio [INR] 2. 0 -3. 0) is recommended for patients with non-valvular AF who are aged 65 -75 years and free of vascular risk factors (Class I, Level A) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Primary Prevention Recommendations (2/4) § Antiplatelet agents other than aspirin are not recommended for primary stroke prevention (Class IV, GCP) § Aspirin may be recommended for patients with nonvalvular AF who are younger than 65 years and free of vascular risk factors (Class I, Level A) § Unless contraindicated, either aspirin or an oral anticoagulant (international normalized ratio [INR] 2. 0 -3. 0) is recommended for patients with non-valvular AF who are aged 65 -75 years and free of vascular risk factors (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Primary Prevention Recommendations (3/4) § Unless contraindicated, an oral anticoagulant (INR 2. 0– 3. 0) is recommended for patients with non-valvular AF who are aged >75, or who are younger but have risk factors such as high blood pressure, left ventricular dysfunction, or diabetes mellitus (Class I, Level A) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Primary Prevention Recommendations (3/4) § Unless contraindicated, an oral anticoagulant (INR 2. 0– 3. 0) is recommended for patients with non-valvular AF who are aged >75, or who are younger but have risk factors such as high blood pressure, left ventricular dysfunction, or diabetes mellitus (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Primary Prevention Recommendations (4/4) § Patients with AF who are unable to receive oral anticoagulants should be offered aspirin (Class I, Level A) § Patients with AF who have mechanical prosthetic heart valves should receive long-term anticoagulation with a target INR based on the prosthesis type, but not less than INR 2– 3 (Class II, Level B) § Low dose aspirin is recommended for patients with asymptomatic internal carotid artery (ICA) stenosis >50% to reduce their risk of vascular events (Class II, Level B) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Primary Prevention Recommendations (4/4) § Patients with AF who are unable to receive oral anticoagulants should be offered aspirin (Class I, Level A) § Patients with AF who have mechanical prosthetic heart valves should receive long-term anticoagulation with a target INR based on the prosthesis type, but not less than INR 2– 3 (Class II, Level B) § Low dose aspirin is recommended for patients with asymptomatic internal carotid artery (ICA) stenosis >50% to reduce their risk of vascular events (Class II, Level B) Guidelines Ischaemic Stroke 2008
 Asymptomatic carotid artery (ICA) stenosis Primary Prevention • Background 1, 2 – Carotid endarterectomy (CEA) is still a matter of controversy in asymptomatic individuals • RRR for stenosis >60%NASCET is 38 -53% • ARR is 5. 9 -12. 6% • NNT to avoid one stroke/year is 63 -166 – The combined surgical risk must not exceed 3% 1: ACAS: JAMA (1995) 273: 1421 -8. 2: ACST: Lancet (2004) 363: 1491 -1502 Guidelines Ischaemic Stroke 2008
Asymptomatic carotid artery (ICA) stenosis Primary Prevention • Background 1, 2 – Carotid endarterectomy (CEA) is still a matter of controversy in asymptomatic individuals • RRR for stenosis >60%NASCET is 38 -53% • ARR is 5. 9 -12. 6% • NNT to avoid one stroke/year is 63 -166 – The combined surgical risk must not exceed 3% 1: ACAS: JAMA (1995) 273: 1421 -8. 2: ACST: Lancet (2004) 363: 1491 -1502 Guidelines Ischaemic Stroke 2008
 Asymptomatic carotid artery (ICA) stenosis Primary Prevention • Specific issues – No prospective trials tested the benefit of antiplatelet drugs in patients with asymptomatic carotid stenosis 1 – The ipsilateral stroke risk increases with the degree of the stenosis 2 – Patients with an occlusion of the contralateral ICA do not benefit from endarterectomy 3 – Women have lower benefit from CEA than men 3 – Aspirin reduces stroke risk during and after CEA 4 1: Chambers BR et al. : Cochrane Review (2005) 2: ECST Group: Lancet (1995) 345: 209 -12 3: Baker WH et al. : Stroke (2000) 31: 2330 -4 4: Engelter S et al. : Cochrane Reviews (2003) Guidelines Ischaemic Stroke 2008
Asymptomatic carotid artery (ICA) stenosis Primary Prevention • Specific issues – No prospective trials tested the benefit of antiplatelet drugs in patients with asymptomatic carotid stenosis 1 – The ipsilateral stroke risk increases with the degree of the stenosis 2 – Patients with an occlusion of the contralateral ICA do not benefit from endarterectomy 3 – Women have lower benefit from CEA than men 3 – Aspirin reduces stroke risk during and after CEA 4 1: Chambers BR et al. : Cochrane Review (2005) 2: ECST Group: Lancet (1995) 345: 209 -12 3: Baker WH et al. : Stroke (2000) 31: 2330 -4 4: Engelter S et al. : Cochrane Reviews (2003) Guidelines Ischaemic Stroke 2008
 Carotid Surgery and Angioplasty Primary Prevention Recommendations § Carotid surgery is not recommended for asymptomatic individuals with significant carotid stenosis (NASCET 6099%), except in those at high risk of stroke (Class I, Level C) § Carotid angioplasty, with or without stenting, is not recommended for patients with asymptomatic carotid stenosis (Class IV, GCP) § Patients should take aspirin before and after CEA (Class I, Level A) Guidelines Ischaemic Stroke 2008
Carotid Surgery and Angioplasty Primary Prevention Recommendations § Carotid surgery is not recommended for asymptomatic individuals with significant carotid stenosis (NASCET 6099%), except in those at high risk of stroke (Class I, Level C) § Carotid angioplasty, with or without stenting, is not recommended for patients with asymptomatic carotid stenosis (Class IV, GCP) § Patients should take aspirin before and after CEA (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Secondary Prevention • Content – Management of vascular risk factors – Antithrombotic therapy – Surgery and angioplasty Guidelines Ischaemic Stroke 2008
Secondary Prevention • Content – Management of vascular risk factors – Antithrombotic therapy – Surgery and angioplasty Guidelines Ischaemic Stroke 2008
 Blood pressure control Secondary Prevention • Background – Antihypertensive drugs reduce stroke recurrence risk after stroke or TIA (RR 0. 76; 95%CI 0. 63 -0. 92)1 – Target BP level and reduction should be individualized – The reduction in stroke occurs regardless of baseline BP and type of stroke 2 1: Rashid P et al. : Stroke (2003) 34: 2741 -8 2: PROGRESS group: Lancet (2001) 358: 1033 -41 Guidelines Ischaemic Stroke 2008
Blood pressure control Secondary Prevention • Background – Antihypertensive drugs reduce stroke recurrence risk after stroke or TIA (RR 0. 76; 95%CI 0. 63 -0. 92)1 – Target BP level and reduction should be individualized – The reduction in stroke occurs regardless of baseline BP and type of stroke 2 1: Rashid P et al. : Stroke (2003) 34: 2741 -8 2: PROGRESS group: Lancet (2001) 358: 1033 -41 Guidelines Ischaemic Stroke 2008
 Diabetes mellitus Secondary Prevention • Background – In people with type 2 diabetes with previous stroke pioglitazone reduces fatal or nonfatal stroke (HR 0. 53; 95%CI 0. 34 -0. 85; P=0. 0085)1 – In addition there is a trend to reduce the combined end point of death and major vascular events (HR 0. 78; 95%CI 0. 60 -1. 02; P=0. 067)1 1: Wilcox R et al. : Stroke (2007) 38: 865 -73 Guidelines Ischaemic Stroke 2008
Diabetes mellitus Secondary Prevention • Background – In people with type 2 diabetes with previous stroke pioglitazone reduces fatal or nonfatal stroke (HR 0. 53; 95%CI 0. 34 -0. 85; P=0. 0085)1 – In addition there is a trend to reduce the combined end point of death and major vascular events (HR 0. 78; 95%CI 0. 60 -1. 02; P=0. 067)1 1: Wilcox R et al. : Stroke (2007) 38: 865 -73 Guidelines Ischaemic Stroke 2008
 High Cholesterol Secondary Prevention • Background – Atorvastatin (80 mg) reduces stroke recurrence by 16%1 – Simvastatin (40 mg) reduces risk of vascular events in patients with prior stroke, and of stroke in patients with other vascular disease (RR 0. 76)2 – ARR for statin treatment is low (NNT 112 -143 for 1 year)1 – Statin withdrawal at the acute stage of stroke may be harmful 3 1: Amarenco P et al. : N Engl J Med (2006) 355: 549 -559 2: Heart Protection Study: Lancet (2002) 360: 7 -22 3: Blanco M et al. : Neurology (2007) 69: 904 -10 Guidelines Ischaemic Stroke 2008
High Cholesterol Secondary Prevention • Background – Atorvastatin (80 mg) reduces stroke recurrence by 16%1 – Simvastatin (40 mg) reduces risk of vascular events in patients with prior stroke, and of stroke in patients with other vascular disease (RR 0. 76)2 – ARR for statin treatment is low (NNT 112 -143 for 1 year)1 – Statin withdrawal at the acute stage of stroke may be harmful 3 1: Amarenco P et al. : N Engl J Med (2006) 355: 549 -559 2: Heart Protection Study: Lancet (2002) 360: 7 -22 3: Blanco M et al. : Neurology (2007) 69: 904 -10 Guidelines Ischaemic Stroke 2008
 Vitamins Secondary Prevention • Background – Beta carotene increased the risk (RR 1. 10) of cardiovascular death 1 – Antioxidant supplements may increase mortality 2 – Folate, B 12, B 6 vitamins given to lower homocysteine levels may not reduce stroke recurrence and may increase vascular events 3 1: Vivekananthan D et al. : Lancet (2003) 361: 2017 -2023 2: Bjelakovic G et al. : JAMA (2007) 297: 842 -857 3: Bonaa K et al. : N Engl J Med (2006) 354: 1578 -1588 Guidelines Ischaemic Stroke 2008
Vitamins Secondary Prevention • Background – Beta carotene increased the risk (RR 1. 10) of cardiovascular death 1 – Antioxidant supplements may increase mortality 2 – Folate, B 12, B 6 vitamins given to lower homocysteine levels may not reduce stroke recurrence and may increase vascular events 3 1: Vivekananthan D et al. : Lancet (2003) 361: 2017 -2023 2: Bjelakovic G et al. : JAMA (2007) 297: 842 -857 3: Bonaa K et al. : N Engl J Med (2006) 354: 1578 -1588 Guidelines Ischaemic Stroke 2008
 Hormone Replacement Therapy Secondary Prevention • Background – Oestrogen therapy is not effective in secondary prevention after TIA or stroke and may increase stroke severity 1 1: Viscoli CM et al. : N Engl J Med (2001) 345: 1243 -9. Guidelines Ischaemic Stroke 2008
Hormone Replacement Therapy Secondary Prevention • Background – Oestrogen therapy is not effective in secondary prevention after TIA or stroke and may increase stroke severity 1 1: Viscoli CM et al. : N Engl J Med (2001) 345: 1243 -9. Guidelines Ischaemic Stroke 2008
 Sleep-disordered Breathing Secondary Prevention • Background – Sleep-disordered breathing (SDB) is both a risk factor and a consequence of stroke – More than 50% of stroke patients have SDB, mostly in the form of obstructive sleep apnoea (OSA). – SDB is linked with poorer long-term outcome and increased long-term stroke mortality 1 – Continuous positive airway pressure is the treatment of choice for OSA. 1: Bassetti CL: Semin Neurol (2005) 25: 19 -32 Guidelines Ischaemic Stroke 2008
Sleep-disordered Breathing Secondary Prevention • Background – Sleep-disordered breathing (SDB) is both a risk factor and a consequence of stroke – More than 50% of stroke patients have SDB, mostly in the form of obstructive sleep apnoea (OSA). – SDB is linked with poorer long-term outcome and increased long-term stroke mortality 1 – Continuous positive airway pressure is the treatment of choice for OSA. 1: Bassetti CL: Semin Neurol (2005) 25: 19 -32 Guidelines Ischaemic Stroke 2008
 Risk Factor Management Secondary Prevention Recommendations (1/3) § Blood pressure should be checked regularly. Blood pressure lowering is recommended after the acute phase, including in patients with normal blood pressure (Class I, Level A) § Blood glucose should be checked regularly. Diabetes should be managed with lifestyle modification and individualized pharmacological therapy (Class IV, GCP) § In patients with type 2 diabetes who do not need insulin, treatment with pioglitazone is recommended after stroke (Class III, Level B) Guidelines Ischaemic Stroke 2008
Risk Factor Management Secondary Prevention Recommendations (1/3) § Blood pressure should be checked regularly. Blood pressure lowering is recommended after the acute phase, including in patients with normal blood pressure (Class I, Level A) § Blood glucose should be checked regularly. Diabetes should be managed with lifestyle modification and individualized pharmacological therapy (Class IV, GCP) § In patients with type 2 diabetes who do not need insulin, treatment with pioglitazone is recommended after stroke (Class III, Level B) Guidelines Ischaemic Stroke 2008
 Risk Factor Management Secondary Prevention Recommendations (2/3) § Statin therapy is recommended (Class I, Level A) § Cigarette smoking should be stopped (Class III, Level C) § Heavy use of alcohol should be discouraged (Class IV, GCP) § Regular physical activity is recommended (Class IV, GCP) § A diet low in salt and saturated fat, high in fruit and vegetables, and rich in fibre is recommended (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Risk Factor Management Secondary Prevention Recommendations (2/3) § Statin therapy is recommended (Class I, Level A) § Cigarette smoking should be stopped (Class III, Level C) § Heavy use of alcohol should be discouraged (Class IV, GCP) § Regular physical activity is recommended (Class IV, GCP) § A diet low in salt and saturated fat, high in fruit and vegetables, and rich in fibre is recommended (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Risk Factor Management Secondary Prevention Recommendations (3/3) § Subjects with an elevated body mass index are recommended to take a weight-reducing diet (Class IV, Level C) § Antioxidant vitamins supplements are not recommended (Class I, Level A) § Hormone replacement therapy is not recommended for the secondary prevention of stroke (Class I, Level A) § Sleep-disordered breathing such as obstructive sleep apnoea is recommended to be treated with continuous positive airway pressure breathing (Class III, Level GCP) Guidelines Ischaemic Stroke 2008
Risk Factor Management Secondary Prevention Recommendations (3/3) § Subjects with an elevated body mass index are recommended to take a weight-reducing diet (Class IV, Level C) § Antioxidant vitamins supplements are not recommended (Class I, Level A) § Hormone replacement therapy is not recommended for the secondary prevention of stroke (Class I, Level A) § Sleep-disordered breathing such as obstructive sleep apnoea is recommended to be treated with continuous positive airway pressure breathing (Class III, Level GCP) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention • Background: Aspirin – 13% relative risk reduction for stroke after TIA or stroke 1 – Most widely studied dosages of aspirin are 50 -150 mg – The incidence of GI-disturbances with aspirin is dose dependent – No difference in effectiveness amongst low (< 160 mg), medium (160 – 325 mg) or high (500 - 1500 mg) dose aspirin 1: Antithrombotic Trialists' Collaboration: BMJ (2002) 324: 71 -86 Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention • Background: Aspirin – 13% relative risk reduction for stroke after TIA or stroke 1 – Most widely studied dosages of aspirin are 50 -150 mg – The incidence of GI-disturbances with aspirin is dose dependent – No difference in effectiveness amongst low (< 160 mg), medium (160 – 325 mg) or high (500 - 1500 mg) dose aspirin 1: Antithrombotic Trialists' Collaboration: BMJ (2002) 324: 71 -86 Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention • Background: Dipyridamole plus aspirin – Relative risk reduction of vascular death, stroke or myocardial infarction with the combination is significantly greater (RR 0. 82; 95%CI 0. 71 -0. 91) than with aspirin alone 1, 2 – ARR 1. 0% per year (NNT 100)2 – Incidence of dipyridamole induced headache may be reduced by increasing the dose gradually 3 1: Diener HC et al. : J Neurol Sci (1996) 143: 1 -13 2: Halkes P et al. : Lancet (2006) 367: 1665 -1673 3: Chang YJ et al. : Cerebrovasc Dis (2006) 22: 258 -62 Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention • Background: Dipyridamole plus aspirin – Relative risk reduction of vascular death, stroke or myocardial infarction with the combination is significantly greater (RR 0. 82; 95%CI 0. 71 -0. 91) than with aspirin alone 1, 2 – ARR 1. 0% per year (NNT 100)2 – Incidence of dipyridamole induced headache may be reduced by increasing the dose gradually 3 1: Diener HC et al. : J Neurol Sci (1996) 143: 1 -13 2: Halkes P et al. : Lancet (2006) 367: 1665 -1673 3: Chang YJ et al. : Cerebrovasc Dis (2006) 22: 258 -62 Guidelines Ischaemic Stroke 2008
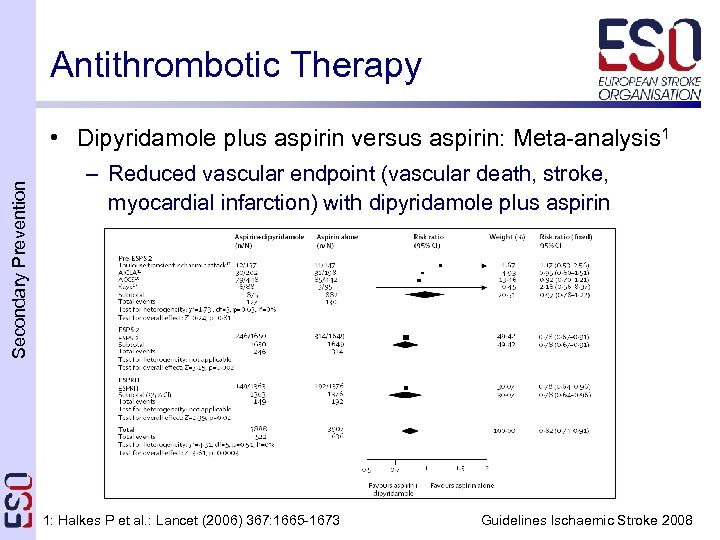 Antithrombotic Therapy Secondary Prevention • Dipyridamole plus aspirin versus aspirin: Meta-analysis 1 – Reduced vascular endpoint (vascular death, stroke, myocardial infarction) with dipyridamole plus aspirin 1: Halkes P et al. : Lancet (2006) 367: 1665 -1673 Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention • Dipyridamole plus aspirin versus aspirin: Meta-analysis 1 – Reduced vascular endpoint (vascular death, stroke, myocardial infarction) with dipyridamole plus aspirin 1: Halkes P et al. : Lancet (2006) 367: 1665 -1673 Guidelines Ischaemic Stroke 2008
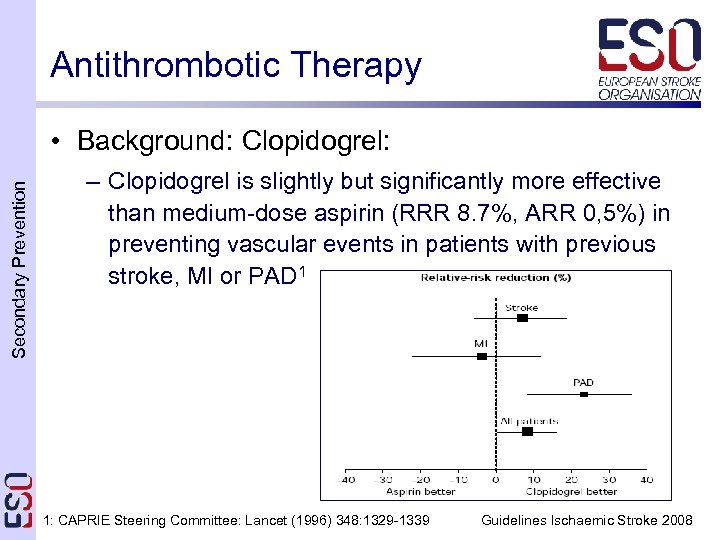 Antithrombotic Therapy Secondary Prevention • Background: Clopidogrel: – Clopidogrel is slightly but significantly more effective than medium-dose aspirin (RRR 8. 7%, ARR 0, 5%) in preventing vascular events in patients with previous stroke, MI or PAD 1 1: CAPRIE Steering Committee: Lancet (1996) 348: 1329 -1339 Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention • Background: Clopidogrel: – Clopidogrel is slightly but significantly more effective than medium-dose aspirin (RRR 8. 7%, ARR 0, 5%) in preventing vascular events in patients with previous stroke, MI or PAD 1 1: CAPRIE Steering Committee: Lancet (1996) 348: 1329 -1339 Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention • Background: Clopidogrel plus aspirin – Compared with clopidogrel the combination of aspirin and clopidogrel does not reduce the risk of ischaemic stroke, myocardial infarction, vascular death, or rehospitalisation 1 – Compared with aspirin alone the combination does not reduce the risk of myocardial infarction, stroke, or cardiovascular death 2 – Risk of life-threatening or major bleeding is increased 1, 2 1: Diener H et al. : Lancet (2004) 364: 331 -337 2: Bhatt D et al. : N Engl J Med (2006) 354: 1706 -1717 Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention • Background: Clopidogrel plus aspirin – Compared with clopidogrel the combination of aspirin and clopidogrel does not reduce the risk of ischaemic stroke, myocardial infarction, vascular death, or rehospitalisation 1 – Compared with aspirin alone the combination does not reduce the risk of myocardial infarction, stroke, or cardiovascular death 2 – Risk of life-threatening or major bleeding is increased 1, 2 1: Diener H et al. : Lancet (2004) 364: 331 -337 2: Bhatt D et al. : N Engl J Med (2006) 354: 1706 -1717 Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention Recommendations (1/4) § Patients should receive antithrombotic therapy (Class I, Level A) § Patients not requiring anticoagulation should receive antiplatelet therapy (Class I, Level A). Where possible, combined aspirin and dipyridamole, or clopidogrel alone, should be given. Alternatively, aspirin alone, or triflusal alone, may be used (Class I, Level A) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention Recommendations (1/4) § Patients should receive antithrombotic therapy (Class I, Level A) § Patients not requiring anticoagulation should receive antiplatelet therapy (Class I, Level A). Where possible, combined aspirin and dipyridamole, or clopidogrel alone, should be given. Alternatively, aspirin alone, or triflusal alone, may be used (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention Recommendations (2/4) § The combination of aspirin and clopidogrel is not recommended in patients with recent ischaemic stroke, except in patients with specific indications (e. g. unstable angina or non-Q-wave MI during the last 12 months, or recent stenting); treatment should be given for up to 9 months after the event (Class I, Level A) § Patients who have a stroke on antiplatelet therapy should be re-evaluated for pathophysiology and risk factors (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention Recommendations (2/4) § The combination of aspirin and clopidogrel is not recommended in patients with recent ischaemic stroke, except in patients with specific indications (e. g. unstable angina or non-Q-wave MI during the last 12 months, or recent stenting); treatment should be given for up to 9 months after the event (Class I, Level A) § Patients who have a stroke on antiplatelet therapy should be re-evaluated for pathophysiology and risk factors (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Anticoagulation Secondary Prevention • Background – Oral antiocoagulation (target INR 2. 0 – 3. 0) reduces the risk of recurrent stroke in patients with AF 1 – Oral anticoagulation is well established for other causes of embolism such as mechanical prosthetic valve replacement, rheumatic valvular heart disease, ventricular aneurysm and cardiomyopathy – There is no indication for oral anticoagulation in patients with non-cardiac cause of ischaemic stroke 2 1: EAFT Study Group: Lancet (1993) 342: 1255 -1262 2: Mohr JP et al. : N Engl J Med (2001) 345: 1444 -1451 Guidelines Ischaemic Stroke 2008
Anticoagulation Secondary Prevention • Background – Oral antiocoagulation (target INR 2. 0 – 3. 0) reduces the risk of recurrent stroke in patients with AF 1 – Oral anticoagulation is well established for other causes of embolism such as mechanical prosthetic valve replacement, rheumatic valvular heart disease, ventricular aneurysm and cardiomyopathy – There is no indication for oral anticoagulation in patients with non-cardiac cause of ischaemic stroke 2 1: EAFT Study Group: Lancet (1993) 342: 1255 -1262 2: Mohr JP et al. : N Engl J Med (2001) 345: 1444 -1451 Guidelines Ischaemic Stroke 2008
 Anticoagulation Secondary Prevention • Specific issues – In patients with AF and stable coronary disease, aspirin should not be added to oral anticoagulation 1 – Some retrospective studies suggest that anticoagulation may be beneficial in aortic atheroma 2, fusiform basilar artery aneurysms 3, or arterial dissection 4 – It is unclear if patients with patent foramen ovale (PFO) benefit from oral anticoagulation 5 1: Flaker GC et al. : Am Heart J (2006) 152: 967 -73 2: Dressler FA et al. : J Am Coll Cardiol (1998) 31: 134 -8 3: Echiverri HC et al. : Stroke (1989) 20: 1741 -7 4: Engelter ST et al. : Stroke (2007) 38: 2605 -11 5: Mas JL et al. : N Engl J Med (2001) 345: 1740 -6 Guidelines Ischaemic Stroke 2008
Anticoagulation Secondary Prevention • Specific issues – In patients with AF and stable coronary disease, aspirin should not be added to oral anticoagulation 1 – Some retrospective studies suggest that anticoagulation may be beneficial in aortic atheroma 2, fusiform basilar artery aneurysms 3, or arterial dissection 4 – It is unclear if patients with patent foramen ovale (PFO) benefit from oral anticoagulation 5 1: Flaker GC et al. : Am Heart J (2006) 152: 967 -73 2: Dressler FA et al. : J Am Coll Cardiol (1998) 31: 134 -8 3: Echiverri HC et al. : Stroke (1989) 20: 1741 -7 4: Engelter ST et al. : Stroke (2007) 38: 2605 -11 5: Mas JL et al. : N Engl J Med (2001) 345: 1740 -6 Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention Recommendations (3/4) § Anticoagulation should not be used after non-cardioembolic ischaemic stroke, except in some specific situations, such as aortic atheromas, fusiform aneurysms of the basilar artery, cervical artery dissection, or patent foramen ovale in the presence of proven deep vein thrombosis (DVT) or atrial septal aneurysm (Class IV, GCP) § If oral anticoagulation is contraindicated, combined low dose aspirin and dipyridamole should be given (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention Recommendations (3/4) § Anticoagulation should not be used after non-cardioembolic ischaemic stroke, except in some specific situations, such as aortic atheromas, fusiform aneurysms of the basilar artery, cervical artery dissection, or patent foramen ovale in the presence of proven deep vein thrombosis (DVT) or atrial septal aneurysm (Class IV, GCP) § If oral anticoagulation is contraindicated, combined low dose aspirin and dipyridamole should be given (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Antithrombotic Therapy Secondary Prevention Recommendations (4/4) § Oral anticoagulation (INR 2. 0– 3. 0) is recommended after ischaemic stroke associated with AF (Class I, Level A). Oral anticoagulation is not recommended in patients with co-morbid conditions such as falls, poor compliance, uncontrolled epilepsy, or gastrointestinal bleeding (Class III, Level C). Increasing age alone is not a contraindication to oral anticoagulation (Class I, Level A) § Patients with cardioembolic stroke unrelated to AF should receive anticoagulants (INR 2. 0 -3. 0) if the risk of recurrence is high (Class III, Level C) Guidelines Ischaemic Stroke 2008
Antithrombotic Therapy Secondary Prevention Recommendations (4/4) § Oral anticoagulation (INR 2. 0– 3. 0) is recommended after ischaemic stroke associated with AF (Class I, Level A). Oral anticoagulation is not recommended in patients with co-morbid conditions such as falls, poor compliance, uncontrolled epilepsy, or gastrointestinal bleeding (Class III, Level C). Increasing age alone is not a contraindication to oral anticoagulation (Class I, Level A) § Patients with cardioembolic stroke unrelated to AF should receive anticoagulants (INR 2. 0 -3. 0) if the risk of recurrence is high (Class III, Level C) Guidelines Ischaemic Stroke 2008
 Carotid Endarterectomy (CEA) Secondary Prevention • Background 1, 2 – CEA reduces the risk by 48% of recurrent disabling stroke or death in patients with 70 -99%NASCET ipsilateral carotid artery stenosis – If perioperative complications exceed 6%, the benefit of CEA will diminish; if it approaches 10%, the benefit will vanish entirely – There is also some risk reduction in male patients with 50 - 69% stenosis of the ipsilateral carotid artery, provided that the complication rate is below 3% 1: NASCET Collaborators: NEJM (1991) 325: 445 -453 2: Warlow C: Lancet (1991) 337: 1235 -1243 Guidelines Ischaemic Stroke 2008
Carotid Endarterectomy (CEA) Secondary Prevention • Background 1, 2 – CEA reduces the risk by 48% of recurrent disabling stroke or death in patients with 70 -99%NASCET ipsilateral carotid artery stenosis – If perioperative complications exceed 6%, the benefit of CEA will diminish; if it approaches 10%, the benefit will vanish entirely – There is also some risk reduction in male patients with 50 - 69% stenosis of the ipsilateral carotid artery, provided that the complication rate is below 3% 1: NASCET Collaborators: NEJM (1991) 325: 445 -453 2: Warlow C: Lancet (1991) 337: 1235 -1243 Guidelines Ischaemic Stroke 2008
 Carotid Endarterectomy Secondary Prevention • Specific issues – CEA should be performed as soon as possible (ideally within 2 weeks) after the last cerebrovascular event 1, 2 – Elderly patients (>75 years) without organ failure or serious cardiac dysfunction benefit from CEA 1 – Women with symptomatic stenosis >70% should undergo CEA. Women with moderate stenosis should be treated medically 2 1: Rothwell PM et al. : Lancet (2004) 363: 915 -924 2: Rothwell PM et al. : Stroke (2004) 35: 2855 -61 Guidelines Ischaemic Stroke 2008
Carotid Endarterectomy Secondary Prevention • Specific issues – CEA should be performed as soon as possible (ideally within 2 weeks) after the last cerebrovascular event 1, 2 – Elderly patients (>75 years) without organ failure or serious cardiac dysfunction benefit from CEA 1 – Women with symptomatic stenosis >70% should undergo CEA. Women with moderate stenosis should be treated medically 2 1: Rothwell PM et al. : Lancet (2004) 363: 915 -924 2: Rothwell PM et al. : Stroke (2004) 35: 2855 -61 Guidelines Ischaemic Stroke 2008
 Carotid Endarterectomy Secondary Prevention Effect of time from last symptomatic event to randomisation on the 5 year relative risk (RR) of ipsilateral ischaemic stroke and any operative stroke or death with CEA (pooled data from ECST and NASCET 1) 1: Rothwell PM et al. : Stroke (2004) 35: 2855 -61 Guidelines Ischaemic Stroke 2008
Carotid Endarterectomy Secondary Prevention Effect of time from last symptomatic event to randomisation on the 5 year relative risk (RR) of ipsilateral ischaemic stroke and any operative stroke or death with CEA (pooled data from ECST and NASCET 1) 1: Rothwell PM et al. : Stroke (2004) 35: 2855 -61 Guidelines Ischaemic Stroke 2008
 Carotid Endarterectomy Secondary Prevention • Specific issues – The benefit from CEA is lower with lacunar stroke – Patients with leuko-araiosis should be made aware of the increased operative risk – Occlusion of the contralateral ICA carries a higher perioperative risk – Continuation of aspirin is required until surgery, but heparin may be used in very severe stenosis – All grading of stenoses should be according to NASCET-criteria Guidelines Ischaemic Stroke 2008
Carotid Endarterectomy Secondary Prevention • Specific issues – The benefit from CEA is lower with lacunar stroke – Patients with leuko-araiosis should be made aware of the increased operative risk – Occlusion of the contralateral ICA carries a higher perioperative risk – Continuation of aspirin is required until surgery, but heparin may be used in very severe stenosis – All grading of stenoses should be according to NASCET-criteria Guidelines Ischaemic Stroke 2008
 Carotid Artery Stenting (CAS) Secondary Prevention • Background – No randomized trial has demonstrated equivalent periprocedural risk for CAS compared to CEA in treatment of symptomatic carotid artery stenosis – A European study only marginally failed to prove the non-inferiority of CAS compared to CEA – A French study was stopped prematurely because of a 2. 5 fold higher risk of any stroke or death after CAS 2 1: Ringleb PA et al. : Lancet (2006) 368: 1239 -1247 2: Mas JL et al. : NEJM (2006) 355: 1660 -1671 Guidelines Ischaemic Stroke 2008
Carotid Artery Stenting (CAS) Secondary Prevention • Background – No randomized trial has demonstrated equivalent periprocedural risk for CAS compared to CEA in treatment of symptomatic carotid artery stenosis – A European study only marginally failed to prove the non-inferiority of CAS compared to CEA – A French study was stopped prematurely because of a 2. 5 fold higher risk of any stroke or death after CAS 2 1: Ringleb PA et al. : Lancet (2006) 368: 1239 -1247 2: Mas JL et al. : NEJM (2006) 355: 1660 -1671 Guidelines Ischaemic Stroke 2008
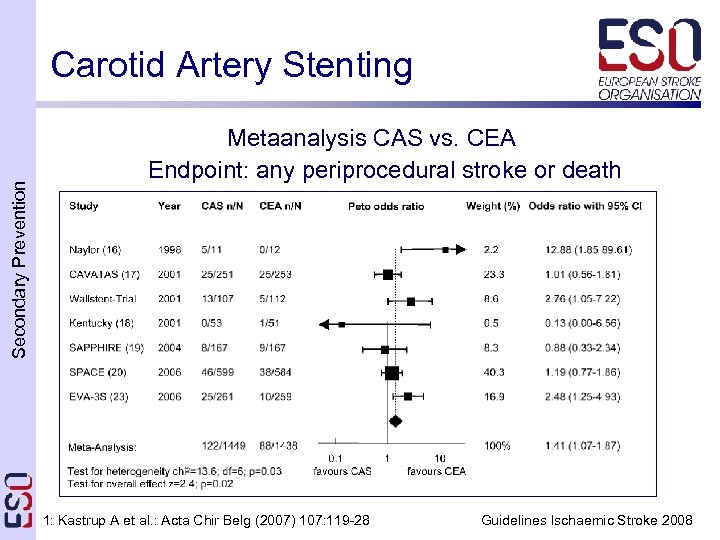 Secondary Prevention Carotid Artery Stenting Metaanalysis CAS vs. CEA Endpoint: any periprocedural stroke or death 1: Kastrup A et al. : Acta Chir Belg (2007) 107: 119 -28 Guidelines Ischaemic Stroke 2008
Secondary Prevention Carotid Artery Stenting Metaanalysis CAS vs. CEA Endpoint: any periprocedural stroke or death 1: Kastrup A et al. : Acta Chir Belg (2007) 107: 119 -28 Guidelines Ischaemic Stroke 2008
 Intracranial Occlusive Disease Secondary Prevention • Background – Extracranial-Intracranial bypass is not beneficial in preventing stroke in patients with MCA or ICA stenosis or occlusion 1 – No randomized controlled trials have evaluated angioplasty, stenting, or both for intracranial stenosis – Several non-randomized trials have shown feasibility and acceptable safety of intracranial stenting, but the risk of re-stenosis remains high 2, 3 1: The EC/IC Bypass Grp: N Engl J Med (1985) 313: 1191 -200 2: Bose A et al. : Stroke (2007) 38: 1531 -7 3: SSYLVIA Study investigators: Stroke (2004) 35: 1388 -92 Guidelines Ischaemic Stroke 2008
Intracranial Occlusive Disease Secondary Prevention • Background – Extracranial-Intracranial bypass is not beneficial in preventing stroke in patients with MCA or ICA stenosis or occlusion 1 – No randomized controlled trials have evaluated angioplasty, stenting, or both for intracranial stenosis – Several non-randomized trials have shown feasibility and acceptable safety of intracranial stenting, but the risk of re-stenosis remains high 2, 3 1: The EC/IC Bypass Grp: N Engl J Med (1985) 313: 1191 -200 2: Bose A et al. : Stroke (2007) 38: 1531 -7 3: SSYLVIA Study investigators: Stroke (2004) 35: 1388 -92 Guidelines Ischaemic Stroke 2008
 Surgery and Angioplasty Secondary Prevention Recommendations (1/4) § CEA is recommended for patients with 70– 99% stenosis (NASCET criteria) (Class I, Level A). CEA should only be performed in centres with a perioperative complication rate (all strokes and death) of less than 6% (Class I, Level A) § CEA should be performed as soon as possible after the last ischaemic event, ideally within 2 weeks (Class II, Level B) Guidelines Ischaemic Stroke 2008
Surgery and Angioplasty Secondary Prevention Recommendations (1/4) § CEA is recommended for patients with 70– 99% stenosis (NASCET criteria) (Class I, Level A). CEA should only be performed in centres with a perioperative complication rate (all strokes and death) of less than 6% (Class I, Level A) § CEA should be performed as soon as possible after the last ischaemic event, ideally within 2 weeks (Class II, Level B) Guidelines Ischaemic Stroke 2008
 Surgery and Angioplasty Secondary Prevention Recommendations (2/4) § CEA may be indicated for certain patients with stenosis of 50– 69% (NASCET criteria); males with very recent hemispheric symptoms are most likely to benefit (Class III, Level C). CEA for stenosis of 50– 69% (NASCET criteria) should only be performed in centres with a perioperative complication rate (all stroke and death) of less than 3% (Class I, Level A) § CEA is not recommended for patients with stenosis of less than 50% (NASCET criteria) (Class I, Level A) Guidelines Ischaemic Stroke 2008
Surgery and Angioplasty Secondary Prevention Recommendations (2/4) § CEA may be indicated for certain patients with stenosis of 50– 69% (NASCET criteria); males with very recent hemispheric symptoms are most likely to benefit (Class III, Level C). CEA for stenosis of 50– 69% (NASCET criteria) should only be performed in centres with a perioperative complication rate (all stroke and death) of less than 3% (Class I, Level A) § CEA is not recommended for patients with stenosis of less than 50% (NASCET criteria) (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Surgery and Angioplasty Secondary Prevention Recommendations (3/4) § Patients should remain on antiplatelet therapy both before and after surgery (Class I, Level A) § Carotid percutaneous transluminal angioplasty and/or stenting (CAS) is only recommended in selected patients (Class I, Level A). It should be restricted to the following subgroups of patients with severe symptomatic carotid artery stenosis: those with contra-indications to CEA, stenosis at a surgically inaccessible site, re-stenosis after earlier CEA, and post-radiation stenosis (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Surgery and Angioplasty Secondary Prevention Recommendations (3/4) § Patients should remain on antiplatelet therapy both before and after surgery (Class I, Level A) § Carotid percutaneous transluminal angioplasty and/or stenting (CAS) is only recommended in selected patients (Class I, Level A). It should be restricted to the following subgroups of patients with severe symptomatic carotid artery stenosis: those with contra-indications to CEA, stenosis at a surgically inaccessible site, re-stenosis after earlier CEA, and post-radiation stenosis (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Surgery and Angioplasty Secondary Prevention Recommendations (4/4) § Patients should receive a combination of clopidogrel and aspirin immediately before and for at least 1 months after stenting (Class IV, GCP) § Endovascular treatment may be considered in patients with symptomatic intracranial stenosis (Class IV, GPC) Guidelines Ischaemic Stroke 2008
Surgery and Angioplasty Secondary Prevention Recommendations (4/4) § Patients should receive a combination of clopidogrel and aspirin immediately before and for at least 1 months after stenting (Class IV, GCP) § Endovascular treatment may be considered in patients with symptomatic intracranial stenosis (Class IV, GPC) Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 General Stroke Treatment • Content General Treatment – Monitoring – Pulmonary and airway care – Fluid balance – Blood pressure – Glucose metabolism – Body temperature Guidelines Ischaemic Stroke 2008
General Stroke Treatment • Content General Treatment – Monitoring – Pulmonary and airway care – Fluid balance – Blood pressure – Glucose metabolism – Body temperature Guidelines Ischaemic Stroke 2008
 Monitoring • Continuous monitoring General Treatment – Heart rate – Breathing rate – O 2 saturation • Discontinuous monitoring – Blood pressure – Blood glucose – Vigilance (GCS), pupils – Neurological status (e. g. NIH stroke scale or Scandinavian stroke scale) Guidelines Ischaemic Stroke 2008
Monitoring • Continuous monitoring General Treatment – Heart rate – Breathing rate – O 2 saturation • Discontinuous monitoring – Blood pressure – Blood glucose – Vigilance (GCS), pupils – Neurological status (e. g. NIH stroke scale or Scandinavian stroke scale) Guidelines Ischaemic Stroke 2008
 Pulmonary function • Background General Treatment – Adequate oxygenation is important – Improve blood oxygenation by administration of > 2 l O 2 – Risk for aspiration in patients with side positioning – Hypoventilation may be caused by pathological respiration pattern – Risk of airway obstruction (vomiting, oropharyngeal muscular hypotonia): mechanical airway protection Guidelines Ischaemic Stroke 2008
Pulmonary function • Background General Treatment – Adequate oxygenation is important – Improve blood oxygenation by administration of > 2 l O 2 – Risk for aspiration in patients with side positioning – Hypoventilation may be caused by pathological respiration pattern – Risk of airway obstruction (vomiting, oropharyngeal muscular hypotonia): mechanical airway protection Guidelines Ischaemic Stroke 2008
 Blood pressure • Background General Treatment – Elevated in most patients with acute stroke – BP drops spontaneously during the first days after stroke – Blood flow in the critical penumbra passively dependent on the mean arterial pressure – There are no adequately sized randomised, controlled studies guiding BP management Guidelines Ischaemic Stroke 2008
Blood pressure • Background General Treatment – Elevated in most patients with acute stroke – BP drops spontaneously during the first days after stroke – Blood flow in the critical penumbra passively dependent on the mean arterial pressure – There are no adequately sized randomised, controlled studies guiding BP management Guidelines Ischaemic Stroke 2008
 Blood pressure General Treatment • Specific issues – Elevated BP (e. g. up to 200 mm. Hg systolic or 110 mm. Hg diastolic) may be tolerated in the acute phase of ischaemic stroke without intervention – BP may be lowered if this is required by cardiac conditions – Upper level of systolic BP in patients undergoing thrombolytic therapy is 180 mm. Hg – Avoid and treat hypotension – Avoid drastic reduction in BP Guidelines Ischaemic Stroke 2008
Blood pressure General Treatment • Specific issues – Elevated BP (e. g. up to 200 mm. Hg systolic or 110 mm. Hg diastolic) may be tolerated in the acute phase of ischaemic stroke without intervention – BP may be lowered if this is required by cardiac conditions – Upper level of systolic BP in patients undergoing thrombolytic therapy is 180 mm. Hg – Avoid and treat hypotension – Avoid drastic reduction in BP Guidelines Ischaemic Stroke 2008
 Glucose metabolism General Treatment • Background – High glucose levels in acute stroke may increase the size of the infarction and reduce functional outcome – Hypoglycemia can mimic acute ischaemic infarction – Routine use of glucose potassium insulin (GKI) infusion regimes in patients with mild to moderate hyperglycaemia did not improve outcome 1 • It is common practise to treat hyperglycemia with insulin when blood glucose exceeds 180 mg/dl 2 (10 mmol/l) 1: Gray CS et al. : Lancet Neurol (2007) 6: 397 -406 2: Langhorne P et al. : Ageing (2002) 31: 365 -71. Guidelines Ischaemic Stroke 2008
Glucose metabolism General Treatment • Background – High glucose levels in acute stroke may increase the size of the infarction and reduce functional outcome – Hypoglycemia can mimic acute ischaemic infarction – Routine use of glucose potassium insulin (GKI) infusion regimes in patients with mild to moderate hyperglycaemia did not improve outcome 1 • It is common practise to treat hyperglycemia with insulin when blood glucose exceeds 180 mg/dl 2 (10 mmol/l) 1: Gray CS et al. : Lancet Neurol (2007) 6: 397 -406 2: Langhorne P et al. : Ageing (2002) 31: 365 -71. Guidelines Ischaemic Stroke 2008
 Body temperature General Treatment • Background – Fever is associated with poorer neurological outcome after stroke – Fever increases infarct size in experimental stroke – Many patients with acute stroke develop a febrile infection • There are no adequately sized trials guiding temperature management after stroke • It is common practice treat fever (and its cause) when the temperature reaches 37. 5°C Guidelines Ischaemic Stroke 2008
Body temperature General Treatment • Background – Fever is associated with poorer neurological outcome after stroke – Fever increases infarct size in experimental stroke – Many patients with acute stroke develop a febrile infection • There are no adequately sized trials guiding temperature management after stroke • It is common practice treat fever (and its cause) when the temperature reaches 37. 5°C Guidelines Ischaemic Stroke 2008
 General Stroke Treatment General Treatment Recommendations (1/4) § Intermittent monitoring of neurological status, pulse, blood pressure, temperature and oxygen saturation is recommended for 72 hours in patients with significant persisting neurological deficits (Class IV, GCP) § Oxygen should be administered if s. PO 2 falls below 95% (Class IV, GCP) § Regular monitoring of fluid balance and electrolytes is recommended in patients with severe stroke or swallowing problems (Class IV, GCP) Guidelines Ischaemic Stroke 2008
General Stroke Treatment General Treatment Recommendations (1/4) § Intermittent monitoring of neurological status, pulse, blood pressure, temperature and oxygen saturation is recommended for 72 hours in patients with significant persisting neurological deficits (Class IV, GCP) § Oxygen should be administered if s. PO 2 falls below 95% (Class IV, GCP) § Regular monitoring of fluid balance and electrolytes is recommended in patients with severe stroke or swallowing problems (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 General Stroke Treatment General Treatment Recommendations (2/4) § Normal saline (0. 9%) is recommended for fluid replacement during the first 24 hours after stroke (Class IV, GCP) § Routine blood pressure lowering is not recommended following acute stroke (Class IV, GCP) § Cautious blood pressure lowering is recommended in patients with any of the following; extremely high blood pressures (>220/120 mm. Hg) on repeated measurements, or severe cardiac failure, aortic dissection, or hypertensive encephalopathy (Class IV, GCP) Guidelines Ischaemic Stroke 2008
General Stroke Treatment General Treatment Recommendations (2/4) § Normal saline (0. 9%) is recommended for fluid replacement during the first 24 hours after stroke (Class IV, GCP) § Routine blood pressure lowering is not recommended following acute stroke (Class IV, GCP) § Cautious blood pressure lowering is recommended in patients with any of the following; extremely high blood pressures (>220/120 mm. Hg) on repeated measurements, or severe cardiac failure, aortic dissection, or hypertensive encephalopathy (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 General Stroke Treatment General Treatment Recommendations (3/4) § Abrupt blood pressure lowering should be avoided (Class II, Level C) § Low blood pressure secondary to hypovolaemia or associated with neurological deterioration in acute stroke should be treated with volume expanders (Class IV GCP) § Monitoring serum glucose levels is recommended (Class IV, GCP) § Treatment of serum glucose levels >180 mg/dl (>10 mmol/l) with insulin titration is recommended (Class IV, GCP) Guidelines Ischaemic Stroke 2008
General Stroke Treatment General Treatment Recommendations (3/4) § Abrupt blood pressure lowering should be avoided (Class II, Level C) § Low blood pressure secondary to hypovolaemia or associated with neurological deterioration in acute stroke should be treated with volume expanders (Class IV GCP) § Monitoring serum glucose levels is recommended (Class IV, GCP) § Treatment of serum glucose levels >180 mg/dl (>10 mmol/l) with insulin titration is recommended (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 General Stroke Treatment General Treatment Recommendations (4/4) § Severe hypoglycaemia (<50 mg/dl [<2. 8 mmol/l]) should be treated with intravenous dextrose or infusion of 10– 20% glucose (Class IV, GCP points) § The presence of pyrexia (temperature >37. 5°C) should prompt a search for concurrent infection (Class IV, GCP) § Treatment of pyrexia (>37. 5°C) with paracetamol and fanning is recommended (Class III, Level C) § Antibiotic prophylaxis is not recommended immunocompetent patients (Class II, Level B) in Guidelines Ischaemic Stroke 2008
General Stroke Treatment General Treatment Recommendations (4/4) § Severe hypoglycaemia (<50 mg/dl [<2. 8 mmol/l]) should be treated with intravenous dextrose or infusion of 10– 20% glucose (Class IV, GCP points) § The presence of pyrexia (temperature >37. 5°C) should prompt a search for concurrent infection (Class IV, GCP) § Treatment of pyrexia (>37. 5°C) with paracetamol and fanning is recommended (Class III, Level C) § Antibiotic prophylaxis is not recommended immunocompetent patients (Class II, Level B) in Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Specific Stroke Treatment • Content Specific Treatment – Thrombolytic therapy – Early antithrombotic treatment – Treatment of elevated intracranial pressure – Prevention and management of complications Guidelines Ischaemic Stroke 2008
Specific Stroke Treatment • Content Specific Treatment – Thrombolytic therapy – Early antithrombotic treatment – Treatment of elevated intracranial pressure – Prevention and management of complications Guidelines Ischaemic Stroke 2008
 Thrombolytic Therapy (i. v. rt. PA) Specific Treatment • Background (NINDS 1, ECASS I 2 + II 3, ATLANTIS 4) – Intravenous rt. PA (0. 9 mg/kg, max 90 mg) given within 3 hours of stroke onset, significantly improves outcome in patients with acute ischaemic stroke – Benefit from the use of i. v. rt. PA beyond 3 hours is smaller, but may be present up to at least 4. 5 hours – Several contraindications 1: NINDS rt-PA Grp: New Engl J Med (1995) 333: 1581 -1587 2: Hacke W et al. : JAMA (1995) 274: 1017 -1025 3: Hacke W et al. : Lancet (1998) 352: 1245 -1251 4: Clark WM et al. : Jama (1999) 282: 2019 -26. Guidelines Ischaemic Stroke 2008
Thrombolytic Therapy (i. v. rt. PA) Specific Treatment • Background (NINDS 1, ECASS I 2 + II 3, ATLANTIS 4) – Intravenous rt. PA (0. 9 mg/kg, max 90 mg) given within 3 hours of stroke onset, significantly improves outcome in patients with acute ischaemic stroke – Benefit from the use of i. v. rt. PA beyond 3 hours is smaller, but may be present up to at least 4. 5 hours – Several contraindications 1: NINDS rt-PA Grp: New Engl J Med (1995) 333: 1581 -1587 2: Hacke W et al. : JAMA (1995) 274: 1017 -1025 3: Hacke W et al. : Lancet (1998) 352: 1245 -1251 4: Clark WM et al. : Jama (1999) 282: 2019 -26. Guidelines Ischaemic Stroke 2008
 Thrombolytic Therapy (i. v. rt. PA) Specific Treatment • Specific issues – A pooled analysis of the 6 i. v. rt. PA trials confirms that i. v. thrombolysis may work up to 4. 5 hours 1 – Caution is advised when considering i. v. rt. PA in persons with severe stroke (NIHSSS>25), or if the CT demonstrates extended early infarcts signs – Thrombolytic therapy must be given by an experienced stroke physician after the imaging of the brain is assessed by physicians experienced in reading this imaging study 2 1: Hacke W et al. : Lancet (2004) 363: 768 -74 2: Wahlgren N et al. : Lancet (2007) 369: 275 -82 Guidelines Ischaemic Stroke 2008
Thrombolytic Therapy (i. v. rt. PA) Specific Treatment • Specific issues – A pooled analysis of the 6 i. v. rt. PA trials confirms that i. v. thrombolysis may work up to 4. 5 hours 1 – Caution is advised when considering i. v. rt. PA in persons with severe stroke (NIHSSS>25), or if the CT demonstrates extended early infarcts signs – Thrombolytic therapy must be given by an experienced stroke physician after the imaging of the brain is assessed by physicians experienced in reading this imaging study 2 1: Hacke W et al. : Lancet (2004) 363: 768 -74 2: Wahlgren N et al. : Lancet (2007) 369: 275 -82 Guidelines Ischaemic Stroke 2008
 Thrombolytic Therapy (i. v. rt. PA) • Specific issues Specific Treatment – Factors associated with increased bleeding risk 1 • elevated serum glucose • history of diabetes • baseline symptom severity • advanced age • increased time to treatment • previous aspirin use • history of congestive heart failure • NINDS protocol violations – None of these reversed the overall benefit of rt. PA 1: Lansberg MG et al. : Stroke (2007) 38: 2275 -8 Guidelines Ischaemic Stroke 2008
Thrombolytic Therapy (i. v. rt. PA) • Specific issues Specific Treatment – Factors associated with increased bleeding risk 1 • elevated serum glucose • history of diabetes • baseline symptom severity • advanced age • increased time to treatment • previous aspirin use • history of congestive heart failure • NINDS protocol violations – None of these reversed the overall benefit of rt. PA 1: Lansberg MG et al. : Stroke (2007) 38: 2275 -8 Guidelines Ischaemic Stroke 2008
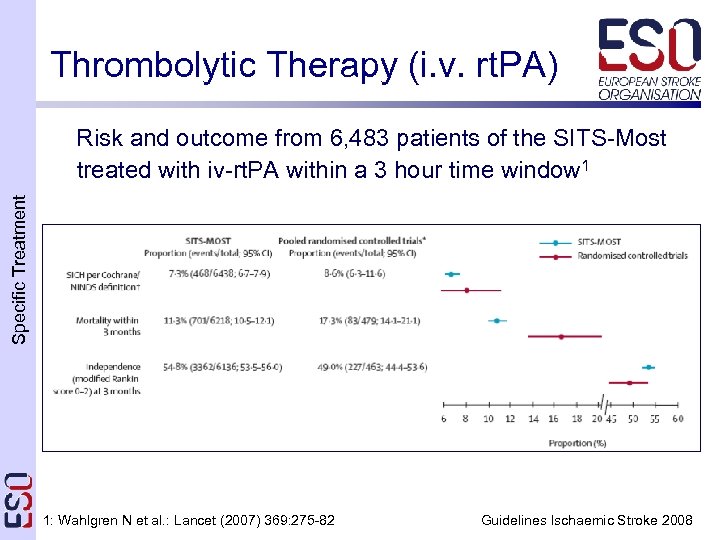 Thrombolytic Therapy (i. v. rt. PA) Specific Treatment Risk and outcome from 6, 483 patients of the SITS-Most treated with iv-rt. PA within a 3 hour time window 1 1: Wahlgren N et al. : Lancet (2007) 369: 275 -82 Guidelines Ischaemic Stroke 2008
Thrombolytic Therapy (i. v. rt. PA) Specific Treatment Risk and outcome from 6, 483 patients of the SITS-Most treated with iv-rt. PA within a 3 hour time window 1 1: Wahlgren N et al. : Lancet (2007) 369: 275 -82 Guidelines Ischaemic Stroke 2008
 Thrombolytic Therapy (i. v. rt. PA) Specific Treatment • Mismatch based therapy – The use of multimodal imaging criteria may be useful for patient selection 1, 2 – Available data on mismatch, as defined by multimodal MRI or CT, are too limited to guide thrombolysis in routine practice 3 – Data regarding the use of intravenous desmoteplase administered 3 to 9 hours after acute ischaemic stroke in patients selected on the basis of perfusion/diffusion mismatch are conflicting 1: Köhrmann M et al. : Lancet Neurol (2006) 5: 661 -7 2: Chalela J et al. : Lancet (2007) 369: 293 -298 3: Kane I et al. : JNNP (2007) 78: 485 -490 Guidelines Ischaemic Stroke 2008
Thrombolytic Therapy (i. v. rt. PA) Specific Treatment • Mismatch based therapy – The use of multimodal imaging criteria may be useful for patient selection 1, 2 – Available data on mismatch, as defined by multimodal MRI or CT, are too limited to guide thrombolysis in routine practice 3 – Data regarding the use of intravenous desmoteplase administered 3 to 9 hours after acute ischaemic stroke in patients selected on the basis of perfusion/diffusion mismatch are conflicting 1: Köhrmann M et al. : Lancet Neurol (2006) 5: 661 -7 2: Chalela J et al. : Lancet (2007) 369: 293 -298 3: Kane I et al. : JNNP (2007) 78: 485 -490 Guidelines Ischaemic Stroke 2008
 Thrombolytic Therapy (i. a. ) Specific Treatment • Background: the use of i. a. rt. PA, i. a. urokinase – Only cases and some prospective uncontrolled case series • Facts: about use of i. a. pro-urokinase – Efficacy demonstrated in small RCT, 6 h window 1 – Not approved and substance not available 1: Furlan A et al. : JAMA (1999) 282: 2003 -11 Guidelines Ischaemic Stroke 2008
Thrombolytic Therapy (i. a. ) Specific Treatment • Background: the use of i. a. rt. PA, i. a. urokinase – Only cases and some prospective uncontrolled case series • Facts: about use of i. a. pro-urokinase – Efficacy demonstrated in small RCT, 6 h window 1 – Not approved and substance not available 1: Furlan A et al. : JAMA (1999) 282: 2003 -11 Guidelines Ischaemic Stroke 2008
 Specific Treatment Recommendations (1/5) § Intravenous rt. PA (0. 9 mg/kg BW, maximum 90 mg), with 10% of the dose given as a bolus followed by a 60 -minute infusion, is recommended within 3 hours of onset of ischaemic stroke (Class I, Level A) § Intravenous rt. PA may be of benefit also for acute ischaemic stroke beyond 3 hours after onset (Class I, Level B) but is not recommended for routine clinical practice. The use of multimodal imaging criteria may be useful for patient selection (Class III, Level C) Guidelines Ischaemic Stroke 2008
Specific Treatment Recommendations (1/5) § Intravenous rt. PA (0. 9 mg/kg BW, maximum 90 mg), with 10% of the dose given as a bolus followed by a 60 -minute infusion, is recommended within 3 hours of onset of ischaemic stroke (Class I, Level A) § Intravenous rt. PA may be of benefit also for acute ischaemic stroke beyond 3 hours after onset (Class I, Level B) but is not recommended for routine clinical practice. The use of multimodal imaging criteria may be useful for patient selection (Class III, Level C) Guidelines Ischaemic Stroke 2008
 Specific Treatment Recommendations (2/5) § Blood pressures of 185/110 mm. Hg or higher must be lowered before thrombolysis (Class IV, GCP) § Intravenous rt. PA may be used in patients with seizures at stroke onset, if the neurological deficit is related to acute cerebral ischaemia (Class IV, GCP) § Intravenous rt. PA may also be administered in selected patients over 80 years of age, although this is outside the current European labelling (Class III, Level C) Guidelines Ischaemic Stroke 2008
Specific Treatment Recommendations (2/5) § Blood pressures of 185/110 mm. Hg or higher must be lowered before thrombolysis (Class IV, GCP) § Intravenous rt. PA may be used in patients with seizures at stroke onset, if the neurological deficit is related to acute cerebral ischaemia (Class IV, GCP) § Intravenous rt. PA may also be administered in selected patients over 80 years of age, although this is outside the current European labelling (Class III, Level C) Guidelines Ischaemic Stroke 2008
 Specific Treatment Recommendations (3/5) § Intra-arterial treatment of acute MCA occlusion within a 6 hour time window is recommended as an option (Class II, Level B) § Intra-arterial thrombolysis is recommended for acute basilar occlusion in selected patients (Class III, Level B) Intravenous thrombolysis for basilar occlusion is an acceptable alternative even after 3 hours (Class III, Level B) Guidelines Ischaemic Stroke 2008
Specific Treatment Recommendations (3/5) § Intra-arterial treatment of acute MCA occlusion within a 6 hour time window is recommended as an option (Class II, Level B) § Intra-arterial thrombolysis is recommended for acute basilar occlusion in selected patients (Class III, Level B) Intravenous thrombolysis for basilar occlusion is an acceptable alternative even after 3 hours (Class III, Level B) Guidelines Ischaemic Stroke 2008
 Antiplatelet therapy Specific Treatment • Background – Aspirin was tested in large RCTs in acute (<48 h) stroke 1, 2 – Significant reduction was seen in death and dependency (NNT 70) and recurrence of stroke (NNT 140) – A phase 3 trial for the glycoprotein-IIb-IIIa antagonist abciximab was stopped prematurely because of an increased rate of bleeding 3 1: International-Stroke-Trial: Lancet (1997) 349: 1569 -1581 2: CAST-Collaborative-Group: Lancet (1997) 349: 1641 -1649 3: Adams HP, Jr. et al. : Stroke (2007) Guidelines Ischaemic Stroke 2008
Antiplatelet therapy Specific Treatment • Background – Aspirin was tested in large RCTs in acute (<48 h) stroke 1, 2 – Significant reduction was seen in death and dependency (NNT 70) and recurrence of stroke (NNT 140) – A phase 3 trial for the glycoprotein-IIb-IIIa antagonist abciximab was stopped prematurely because of an increased rate of bleeding 3 1: International-Stroke-Trial: Lancet (1997) 349: 1569 -1581 2: CAST-Collaborative-Group: Lancet (1997) 349: 1641 -1649 3: Adams HP, Jr. et al. : Stroke (2007) Guidelines Ischaemic Stroke 2008
 Anticoagulation • Unfractionated heparin Specific Treatment – No formal trial available testing standard i. v. heparin – IST showed no net benefit for s. c. heparin treated patients because of increased risk of ICH 1 • Low molecular weight heparin – No benefit on stroke outcome for low molecular heparin (nadroparin, certoparin, tinzaparin, dalteparin) • Heparinoid (orgaran) – TOAST trial neutral 2 1: International-Stroke-Trial: Lancet (1997) 349: 1569 -1581 2: TOAST Investigators: JAMA (1998) 279: 1265 -72. Guidelines Ischaemic Stroke 2008
Anticoagulation • Unfractionated heparin Specific Treatment – No formal trial available testing standard i. v. heparin – IST showed no net benefit for s. c. heparin treated patients because of increased risk of ICH 1 • Low molecular weight heparin – No benefit on stroke outcome for low molecular heparin (nadroparin, certoparin, tinzaparin, dalteparin) • Heparinoid (orgaran) – TOAST trial neutral 2 1: International-Stroke-Trial: Lancet (1997) 349: 1569 -1581 2: TOAST Investigators: JAMA (1998) 279: 1265 -72. Guidelines Ischaemic Stroke 2008
 Specific Treatment Neuroprotection • No adequately sized trial has yet shown significant effect in predefined endpoints for any neuroprotective substance • A meta-analysis has suggested a mild benefit for citocoline 1 1: Davalos A et al. : Stroke (2002) 33: 2850 -7 Guidelines Ischaemic Stroke 2008
Specific Treatment Neuroprotection • No adequately sized trial has yet shown significant effect in predefined endpoints for any neuroprotective substance • A meta-analysis has suggested a mild benefit for citocoline 1 1: Davalos A et al. : Stroke (2002) 33: 2850 -7 Guidelines Ischaemic Stroke 2008
 Specific Treatment Recommendations (4/5) § Aspirin (160– 325 mg loading dose) should be given within 48 hours after ischaemic stroke (Class I, Level A) § If thrombolytic therapy is planned or given, aspirin or other antithrombotic therapy should not be initiated within 24 hours (Class IV, GCP) § The use of other antiplatelet agents (single or combined) is not recommended in the setting of acute ischaemic stroke (Class III, Level C) § The administration of glycoprotein-IIb-IIIa inhibitors is not recommended (Class I, Level A) Guidelines Ischaemic Stroke 2008
Specific Treatment Recommendations (4/5) § Aspirin (160– 325 mg loading dose) should be given within 48 hours after ischaemic stroke (Class I, Level A) § If thrombolytic therapy is planned or given, aspirin or other antithrombotic therapy should not be initiated within 24 hours (Class IV, GCP) § The use of other antiplatelet agents (single or combined) is not recommended in the setting of acute ischaemic stroke (Class III, Level C) § The administration of glycoprotein-IIb-IIIa inhibitors is not recommended (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Specific Treatment Recommendations (5/5) § Early administration of unfractionated heparin, low molecular weight heparin or heparinoids is not recommended for the treatment of patients with ischaemic stroke (Class I, Level A) § Currently, there is no recommendation to treat ischaemic stroke patients with neuroprotective substances (Class I, Level A) Guidelines Ischaemic Stroke 2008
Specific Treatment Recommendations (5/5) § Early administration of unfractionated heparin, low molecular weight heparin or heparinoids is not recommended for the treatment of patients with ischaemic stroke (Class I, Level A) § Currently, there is no recommendation to treat ischaemic stroke patients with neuroprotective substances (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Elevated Intracranial Pressure • Basic management Specific Treatment – Head elevation up to 30° – Pain relief and sedation – Osmotic agents (glycerol, mannitol, hypertonic saline) – Ventilatory support – Barbiturates, hyperventilation, or THAM-buffer – Achieve normothermia • Hypothermia may reduce mortality 1 1: Steiner T et al. : Neurology (2001) 57(Suppl 2): S 61 -8. Guidelines Ischaemic Stroke 2008
Elevated Intracranial Pressure • Basic management Specific Treatment – Head elevation up to 30° – Pain relief and sedation – Osmotic agents (glycerol, mannitol, hypertonic saline) – Ventilatory support – Barbiturates, hyperventilation, or THAM-buffer – Achieve normothermia • Hypothermia may reduce mortality 1 1: Steiner T et al. : Neurology (2001) 57(Suppl 2): S 61 -8. Guidelines Ischaemic Stroke 2008
 Elevated Intracranial Pressure • Malignant MCA/hemispheric infarction Specific Treatment – Pooled analysis of three European RCTs (N=93)1, 2: • Significantly decreases mortality after 30 days • Significantly more patients with m. RS <4 or m. RS <3 in the decompressive surgery group after one year • No increase of patients surviving with m. RS=5 – Surgery should be done within 48 hours 1, 2 – Side of infarction did affect outcome 1, 2 – Age >50 years is a predictor for poor outcome 3 1: Vahedi K et al. : Lancet Neurol (2007) 6: 215 -22 2: Jüttler E et al. : Stroke (2007) 38: 2518 -25 3: Gupta R et al. : Stroke (2004) 35: 539 -43 Guidelines Ischaemic Stroke 2008
Elevated Intracranial Pressure • Malignant MCA/hemispheric infarction Specific Treatment – Pooled analysis of three European RCTs (N=93)1, 2: • Significantly decreases mortality after 30 days • Significantly more patients with m. RS <4 or m. RS <3 in the decompressive surgery group after one year • No increase of patients surviving with m. RS=5 – Surgery should be done within 48 hours 1, 2 – Side of infarction did affect outcome 1, 2 – Age >50 years is a predictor for poor outcome 3 1: Vahedi K et al. : Lancet Neurol (2007) 6: 215 -22 2: Jüttler E et al. : Stroke (2007) 38: 2518 -25 3: Gupta R et al. : Stroke (2004) 35: 539 -43 Guidelines Ischaemic Stroke 2008
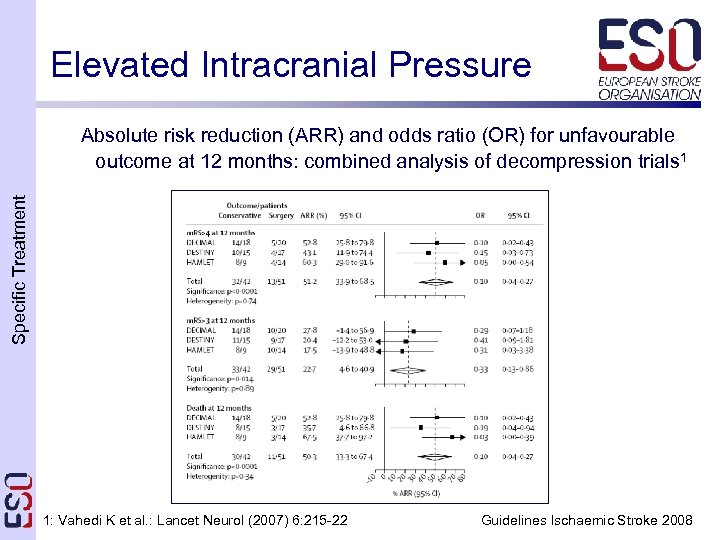 Elevated Intracranial Pressure Specific Treatment Absolute risk reduction (ARR) and odds ratio (OR) for unfavourable outcome at 12 months: combined analysis of decompression trials 1 1: Vahedi K et al. : Lancet Neurol (2007) 6: 215 -22 Guidelines Ischaemic Stroke 2008
Elevated Intracranial Pressure Specific Treatment Absolute risk reduction (ARR) and odds ratio (OR) for unfavourable outcome at 12 months: combined analysis of decompression trials 1 1: Vahedi K et al. : Lancet Neurol (2007) 6: 215 -22 Guidelines Ischaemic Stroke 2008
 Elevated Intracranial Pressure Specific Treatment Recommendations (1/2) § Surgical decompressive therapy within 48 hours after symptom onset is recommended in patients up to 60 years of age with evolving malignant MCA infarcts (Class I, Level A) § Osmotherapy can be used to treat elevated intracranial pressure prior to surgery if this is considered (Class III, Level C) Guidelines Ischaemic Stroke 2008
Elevated Intracranial Pressure Specific Treatment Recommendations (1/2) § Surgical decompressive therapy within 48 hours after symptom onset is recommended in patients up to 60 years of age with evolving malignant MCA infarcts (Class I, Level A) § Osmotherapy can be used to treat elevated intracranial pressure prior to surgery if this is considered (Class III, Level C) Guidelines Ischaemic Stroke 2008
 Elevated Intracranial Pressure Specific Treatment Recommendations (2/2) § No recommendation can be given regarding hypothermic therapy in patients with space-occupying infarctions (Class IV, GCP) § Ventriculostomy or surgical decompression can be considered for treatment of large cerebellar infarctions that compress the brainstem (Class III, Level C) Guidelines Ischaemic Stroke 2008
Elevated Intracranial Pressure Specific Treatment Recommendations (2/2) § No recommendation can be given regarding hypothermic therapy in patients with space-occupying infarctions (Class IV, GCP) § Ventriculostomy or surgical decompression can be considered for treatment of large cerebellar infarctions that compress the brainstem (Class III, Level C) Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment • Aspiration and pneumonia – Bacterial pneumonia is one of the most important complications in stroke patients 1 – Preventive strategies • Withhold oral feeding until demonstration of intact swallowing, preferable using a standardized test • Nasogastric (NG) or percutaneous enteral gastrostomy (PEG) • Frequent changes of the patient’s position in bed and pulmonary physical therapy – Prophylactic administration of levofloxacin is not superior to optimal care 2 1: Weimar C et al. : Eur Neurol (2002) 48: 133 -40 2: Chamorro A et al. : Stroke (2005) 36: 1495 -500 Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment • Aspiration and pneumonia – Bacterial pneumonia is one of the most important complications in stroke patients 1 – Preventive strategies • Withhold oral feeding until demonstration of intact swallowing, preferable using a standardized test • Nasogastric (NG) or percutaneous enteral gastrostomy (PEG) • Frequent changes of the patient’s position in bed and pulmonary physical therapy – Prophylactic administration of levofloxacin is not superior to optimal care 2 1: Weimar C et al. : Eur Neurol (2002) 48: 133 -40 2: Chamorro A et al. : Stroke (2005) 36: 1495 -500 Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment • Urinary tract infections – Most hospital-acquired urinary tract infections are associated with the use of indwelling catheters 1 – Intermittent catheterization does not reduce the risk of infection – If urinary infection is diagnosed, appropriate antibiotics should be chosen following basic medical principles 1: Gerberding JL: Ann Intern Med (2002) 137: 665 -70 c Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment • Urinary tract infections – Most hospital-acquired urinary tract infections are associated with the use of indwelling catheters 1 – Intermittent catheterization does not reduce the risk of infection – If urinary infection is diagnosed, appropriate antibiotics should be chosen following basic medical principles 1: Gerberding JL: Ann Intern Med (2002) 137: 665 -70 c Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment • Deep vein thrombosis and pulmonary embolism – Risk might be reduced by good hydration and early mobilization – Low-dose LMWH reduces the incidence of both DVT (OR 0. 34) and pulmonary embolism (OR 0. 36), without a significantly increased risk of intracerebral (OR 1. 39) or extracerebral haemorrhage (OR 1. 44)1, 2 1: Diener HC et al. : Stroke (2006) 37: 139 -44 2: Sherman DG et al. : Lancet (2007) 369: 1347 -55 Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment • Deep vein thrombosis and pulmonary embolism – Risk might be reduced by good hydration and early mobilization – Low-dose LMWH reduces the incidence of both DVT (OR 0. 34) and pulmonary embolism (OR 0. 36), without a significantly increased risk of intracerebral (OR 1. 39) or extracerebral haemorrhage (OR 1. 44)1, 2 1: Diener HC et al. : Stroke (2006) 37: 139 -44 2: Sherman DG et al. : Lancet (2007) 369: 1347 -55 Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment • Pressure ulcer – Use of support surfaces, frequent repositioning, optimizing nutritional status, and moisturizing sacral skin are appropriate preventive strategies 1 • Seizures – Prophylactic anticonvulsive treatment is not beneficial • Agitation – Causal treatment must precede any type of sedation or antipsychotic treatment 1: Reddy M et al. : JAMA (2006) 296: 974 -84 Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment • Pressure ulcer – Use of support surfaces, frequent repositioning, optimizing nutritional status, and moisturizing sacral skin are appropriate preventive strategies 1 • Seizures – Prophylactic anticonvulsive treatment is not beneficial • Agitation – Causal treatment must precede any type of sedation or antipsychotic treatment 1: Reddy M et al. : JAMA (2006) 296: 974 -84 Guidelines Ischaemic Stroke 2008
 Management of Complications • Falls Specific Treatment – Are common in every stage of stroke treatment – Risk factors include cognitive impairment, depression, polypharmacy and sensory impairment 1 – A multidisciplinary package focusing on personal and environmental factors might be preventive 2 – Exercise, calcium supplements and bisphonates improve bone strength and decrease fracture rates in stroke patients 3, 4 1: Aizen E et al. : Arch Gerontol Geriatr (2007) 44: 1 -12 2: Oliver D et al. : BMJ (2007) 334: 82 3: Pang MY et al. : Clin Rehabil (2006) 20: 97 -111 4: Sato Y et al. : Cerebrovasc Dis (2005) 20: 187 -92 Guidelines Ischaemic Stroke 2008
Management of Complications • Falls Specific Treatment – Are common in every stage of stroke treatment – Risk factors include cognitive impairment, depression, polypharmacy and sensory impairment 1 – A multidisciplinary package focusing on personal and environmental factors might be preventive 2 – Exercise, calcium supplements and bisphonates improve bone strength and decrease fracture rates in stroke patients 3, 4 1: Aizen E et al. : Arch Gerontol Geriatr (2007) 44: 1 -12 2: Oliver D et al. : BMJ (2007) 334: 82 3: Pang MY et al. : Clin Rehabil (2006) 20: 97 -111 4: Sato Y et al. : Cerebrovasc Dis (2005) 20: 187 -92 Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment • Dysphagia and feeding – Dysphagia occurs in up to 50% of patients with unilateral hemiplegic stroke and is an independent riskfactor for poor outcome 1 – For patients with continuing dysphagia, options for enteral nutrition include NG or PEG feeding – PEG does not provide better nutritional status or improved clinical outcome, compared to NG 2, 3 1: Martino R et al. : Stroke (2005) 36: 2756 -63 2: Dennis MS et al. : Lancet (2005) 365: 764 -72 3: Callahan CM et al. : J Am Geriatr Soc (2000) 48: 1048 -54 Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment • Dysphagia and feeding – Dysphagia occurs in up to 50% of patients with unilateral hemiplegic stroke and is an independent riskfactor for poor outcome 1 – For patients with continuing dysphagia, options for enteral nutrition include NG or PEG feeding – PEG does not provide better nutritional status or improved clinical outcome, compared to NG 2, 3 1: Martino R et al. : Stroke (2005) 36: 2756 -63 2: Dennis MS et al. : Lancet (2005) 365: 764 -72 3: Callahan CM et al. : J Am Geriatr Soc (2000) 48: 1048 -54 Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment Recommendations (1/4) § Infections after stroke should be treated with appropriate antibiotics (Class IV, GCP) § Prophylactic administration of antibiotics is not recommended, and levofloxacin can be detrimental in acute stroke patients (Class II, Level B) § Early rehydration and graded compression stockings are recommended to reduce the incidence of venous thromboembolism (Class IV, GCP) § Early mobilization is recommended to prevent complications such as aspiration pneumonia, DVT and pressure ulcers (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment Recommendations (1/4) § Infections after stroke should be treated with appropriate antibiotics (Class IV, GCP) § Prophylactic administration of antibiotics is not recommended, and levofloxacin can be detrimental in acute stroke patients (Class II, Level B) § Early rehydration and graded compression stockings are recommended to reduce the incidence of venous thromboembolism (Class IV, GCP) § Early mobilization is recommended to prevent complications such as aspiration pneumonia, DVT and pressure ulcers (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment Recommendations (2/4) § Low-dose s. c. heparin or low molecular weight heparins should be considered for patients at high risk of DVT or pulmonary embolism (Class I, Level A) § Administration of anticonvulsants is recommended to prevent recurrent seizures (Class I, Level A) § Prophylactic administration of anticonvulsants to patients with recent stroke who have not had seizures is not recommended (Class IV, GCP) § An assessment of falls risk is recommended for every stroke patient (Class IV, GCP) Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment Recommendations (2/4) § Low-dose s. c. heparin or low molecular weight heparins should be considered for patients at high risk of DVT or pulmonary embolism (Class I, Level A) § Administration of anticonvulsants is recommended to prevent recurrent seizures (Class I, Level A) § Prophylactic administration of anticonvulsants to patients with recent stroke who have not had seizures is not recommended (Class IV, GCP) § An assessment of falls risk is recommended for every stroke patient (Class IV, GCP) Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment Recommendations (3/4) § Calcium/vitamin-D supplements are recommended in stroke patients at risk of falls (Class II, Level B) § Bisphonates (alendronate, etidronate and risedronate) are recommended in women with previous fractures (Class II, Level B) § In stroke patients with urinary incontinence, specialist assessment and management is recommended (Class III, Level C) § Swallowing assessment is recommended but there are insufficient data to recommend a specific approach for treatment (Class III, GCP) Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment Recommendations (3/4) § Calcium/vitamin-D supplements are recommended in stroke patients at risk of falls (Class II, Level B) § Bisphonates (alendronate, etidronate and risedronate) are recommended in women with previous fractures (Class II, Level B) § In stroke patients with urinary incontinence, specialist assessment and management is recommended (Class III, Level C) § Swallowing assessment is recommended but there are insufficient data to recommend a specific approach for treatment (Class III, GCP) Guidelines Ischaemic Stroke 2008
 Management of Complications Specific Treatment Recommendations (4/4) § Oral dietary supplements are only recommended for nondysphagic stroke patients who are malnourished (Class II, Level B) § Early commencement of nasogastric (NG) feeding (within 48 hours) is recommended in stroke patients with impaired swallowing (Class II, Level B) § Percutaneous enteral gastrostomy (PEG) feeding should not be considered in stroke patients in the first 2 weeks (Class II, Level B) Guidelines Ischaemic Stroke 2008
Management of Complications Specific Treatment Recommendations (4/4) § Oral dietary supplements are only recommended for nondysphagic stroke patients who are malnourished (Class II, Level B) § Early commencement of nasogastric (NG) feeding (within 48 hours) is recommended in stroke patients with impaired swallowing (Class II, Level B) § Percutaneous enteral gastrostomy (PEG) feeding should not be considered in stroke patients in the first 2 weeks (Class II, Level B) Guidelines Ischaemic Stroke 2008
 ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
ESO Guidelines 2008 • Content: – Education, Referral and Emergency room – Stroke Unit – Imaging and Diagnostics – Prevention – General Treatment – Acute Treatment – Management of Complications – Rehabilitation Guidelines Ischaemic Stroke 2008
 Rehabilitation • Early rehabilitation – More than 40 % of stroke patients need active rehabilitation – Active rehabilitation should start early, providing the patient is clinically stable – Passive rehabilitation should be given if the patient is unconscious or paralysed – Rehabilitation should be continued as long as perceptable recovery is taking place Guidelines Ischaemic Stroke 2008
Rehabilitation • Early rehabilitation – More than 40 % of stroke patients need active rehabilitation – Active rehabilitation should start early, providing the patient is clinically stable – Passive rehabilitation should be given if the patient is unconscious or paralysed – Rehabilitation should be continued as long as perceptable recovery is taking place Guidelines Ischaemic Stroke 2008
 Rehabilitation • Multidisciplinary stroke team for rehabilitation Rehabilitation – Stroke physician – Nurses experienced in stroke management – Physiotherapist trained in stroke rehabilitation – Occupational therapist skilled in stroke – Speech therapist familiar with speech problems in stroke patients – Neuropsychologist accustomed to stroke rehabilitation – Social worker familiar with the problems of stroke patients Guidelines Ischaemic Stroke 2008
Rehabilitation • Multidisciplinary stroke team for rehabilitation Rehabilitation – Stroke physician – Nurses experienced in stroke management – Physiotherapist trained in stroke rehabilitation – Occupational therapist skilled in stroke – Speech therapist familiar with speech problems in stroke patients – Neuropsychologist accustomed to stroke rehabilitation – Social worker familiar with the problems of stroke patients Guidelines Ischaemic Stroke 2008
 Setting of Rehabilitation Recommendations (1/2) § Admission to a stroke unit is recommended for acute stroke patients to receive coordinated multidisciplinary rehabilitation (Class I, Level A) § Early discharge from stroke unit care is possible in medically stable patients with mild or moderate impairment providing that rehabilitation is delivered in the community by a multidisciplinary team with stroke expertise (Class I, Level A) Guidelines Ischaemic Stroke 2008
Setting of Rehabilitation Recommendations (1/2) § Admission to a stroke unit is recommended for acute stroke patients to receive coordinated multidisciplinary rehabilitation (Class I, Level A) § Early discharge from stroke unit care is possible in medically stable patients with mild or moderate impairment providing that rehabilitation is delivered in the community by a multidisciplinary team with stroke expertise (Class I, Level A) Guidelines Ischaemic Stroke 2008
 Setting of Rehabilitation Recommendations (2/2) § Rehabilitation should be continued after discharge during the first year after stroke (Class II, Level A) § Early initiation of rehabilitation is recommended (Class III, Level C) § It is recommended that the duration and intensity of rehabilitation is increased (Class II, Level B) Guidelines Ischaemic Stroke 2008
Setting of Rehabilitation Recommendations (2/2) § Rehabilitation should be continued after discharge during the first year after stroke (Class II, Level A) § Early initiation of rehabilitation is recommended (Class III, Level C) § It is recommended that the duration and intensity of rehabilitation is increased (Class II, Level B) Guidelines Ischaemic Stroke 2008
 Elements of Rehabilitation Recommendations (1/3) § Physiotherapy is recommended, but the optimal mode of delivery is unclear (Class I, Level A) § Occupational therapy is recommended, but the optimal mode of delivery is unclear (Class I, Level A) § While assessment for communication deficits is recommended, there are insufficient data to recommend specific treatments (Class III, GCP) § Information should be provided to patient and carers but evidence does not support use of a dedicated stroke liaison service for all patients (Class II, Level B) Guidelines Ischaemic Stroke 2008
Elements of Rehabilitation Recommendations (1/3) § Physiotherapy is recommended, but the optimal mode of delivery is unclear (Class I, Level A) § Occupational therapy is recommended, but the optimal mode of delivery is unclear (Class I, Level A) § While assessment for communication deficits is recommended, there are insufficient data to recommend specific treatments (Class III, GCP) § Information should be provided to patient and carers but evidence does not support use of a dedicated stroke liaison service for all patients (Class II, Level B) Guidelines Ischaemic Stroke 2008
 Elements of Rehabilitation Recommendations (2/3) § Rehabilitation must be considered for all stroke patients, but there is limited evidence to guide appropriate treatment for the most severely disabled (Class II, Level B) § While assessment for cognitive deficits appears desirable, there are insufficient data to recommend specific treatments (Class I, Level A) § Patients should be monitored for depression during hospital stay and throughout follow up (Class IV, Level B) Guidelines Ischaemic Stroke 2008
Elements of Rehabilitation Recommendations (2/3) § Rehabilitation must be considered for all stroke patients, but there is limited evidence to guide appropriate treatment for the most severely disabled (Class II, Level B) § While assessment for cognitive deficits appears desirable, there are insufficient data to recommend specific treatments (Class I, Level A) § Patients should be monitored for depression during hospital stay and throughout follow up (Class IV, Level B) Guidelines Ischaemic Stroke 2008
 Elements of Rehabilitation Recommendations (3/3) § Drug therapy and non-drug interventions recommended to improve mood (Class I, Level A) are § Drug therapy should be considered to treat post stroke emotionalism (Class II, Level B) § Tricyclic or anticonvulsant therapy are recommended to treat post-stroke neuropathic pain in selected patients (Class III, Level B) § Botulinum toxin should be considered to treat post-stroke spasticity, but functional benefits are uncertain (Class III, Level B) Guidelines Ischaemic Stroke 2008
Elements of Rehabilitation Recommendations (3/3) § Drug therapy and non-drug interventions recommended to improve mood (Class I, Level A) are § Drug therapy should be considered to treat post stroke emotionalism (Class II, Level B) § Tricyclic or anticonvulsant therapy are recommended to treat post-stroke neuropathic pain in selected patients (Class III, Level B) § Botulinum toxin should be considered to treat post-stroke spasticity, but functional benefits are uncertain (Class III, Level B) Guidelines Ischaemic Stroke 2008


