b2d1d68551ee0a9e1b3e24ff9c1c8d06.ppt
- Количество слайдов: 107

Group B – AHD Dr. Gary Greenberg SPINAL NERVE ROOT COMPRESSION AND PERIPHERAL NERVE DISORDERS

Objectives Review Assessment and Management of Important Spinal Nerve Disorders Involving the Cervical, Thoracic and Lumbar Spine. Review Assessment and Management of Common Peripheral Nerve Disorders. Review Assessment of Important Mono/Polyneuropathies.

Case 1 70 year old male, history of mild neck pain for 2 yrs. Gradual worsening mid cervical pain for 1 month. Radiating down right arm to hand. Numbness, tingling and weakness. Now pain severe, unremitting. Unable to sleep in spite of taking Tylenol #3. What historical factors would help you assess this patient?

Historical Factors? 1) Trauma – recent falls. 2) Cancer- remote/recent history. 3) Cervical spondylosis. 4) Fever, weight loss. 5) Immunosuppression. 6) Bone thinning disease ( Rheumatoid arthritis, Multiple Myeloma ).

RED FLAGS What are some of the RED FLAGS that come up in taking a history that make you think there might be a more serious condition present?

RED FLAGS Significant trauma pt. < 50 yrs. Mild trauma pt. > 50 yrs. Unexplained weight loss. Unexplained fever. Immunosupression. Cancer Hx. Night pain. IV drug use.

Red Flags Osteoporosis. Prolonged Steroid use. Age >70. Focal Neuro Deficits. Disabling symptoms. Duration > 6 weeks. Pain not relieved by laying supine.

What physical examination findings would you look for?

Physical Examination TENDERNESS CERVICAL SPINE. MOTION IN THE NECK FOCAL WEAKNESS SENSORY LOSS REFLEX LOSS

Case 1 What are some of the causes of Neck Pain + Radicular Pain + Weakness ?
Causes: Neck pain + Radicular pain + Weakness Idiopathic- congenital spinal stenosis. Traumatic- fracture. Degenerative- Disc herniation, foraminal stenosis, cervical spondylosis. Neoplasm. Infection.

Neck Pain Can Cervical Disc Disease cause gait disturbance?

Important notes Central Disc Disease – can cause gait disturbance, neurogenic bladder, loss of anal tone.

Neck Pain Are Neoplastic mets to C-spine common?

Important notes Neoplasm- mets to C-spine 8 -20% of all spinal mets.

Neck Pain What is the classic presentation of Neoplastic mets to the C-spine?

Important notes Neoplasm- neuro symptoms + severe pain.

Neck Pain Is fever a common finding in infection of the C- spine?

Important notes Infection- C-spine least common site, only 50 % have fever.

Neck Pain Name important risk factors for infection in the C- spine.

Important notes Infection risk factors- IV drug use, diabetes, alcoholism, malignancy, corticosteroids.
Cervical Radiculopathy Describe the incidence , Reflex, Sensory and motor loss for the following levels involved: C 5 radiculopathy. C 6 radiculopathy C 7 radiculopathy. C 8 radiculopathy.
What level of Cervical radiculopathy is involved ? C 5 – 2% incidence. Reflex loss- Biceps. C 6 - 22% incidence. Reflex loss- None. C 7 - 70% incidence. Reflex loss- Triceps. C 8 - 6% incidence. Reflex loss- None.
Cervical Radiculopathy Sensory loss C 5 - proximal lat. arm C 6 - lat. Forearm/thumb. C 7 -2 -4 th fingers. C 8 - 5 th finger.
Cervical Radiculopathy Motor loss C 5 - Deltoid, infra/supraspinatus, biceps. C 6 - Biceps, deltoid, brachioradialis, pronator teres. C 7 – Triceps , wrist flexors and extensors. C 8 - Thumb abduction, finger flexion and extension.
Cervical Imaging What is the value of a C-spine x-ray?

IMAGING X-rays- fractures, confirms degenerative changes.
Cervical Imaging When should an MRI be ordered?

IMAGING MRI- shows foramina and discs best.
Cervical Imaging When should a CT scan be ordered?

IMAGING CT- Only good for occult fractures.

Neck Pain How long does it take for most neck pain from non pathological causes to resolve?
Neck pain Most neck pain resolves in 3 -6 weeks.

Neck Pain What factors may extend that time frame?

Neck pain Automobile related neck injuries- 20 -70% have pain after 6 months. Work related neck injuries- may last years if not resolved in 8 weeks.

Thoracic Pain Name some common causes of persistent thoracic back pain.

Thoracic Spinal Nerves Causes: Diskitis Thoracic disc bulge. Compression fractures- trauma, osteoporosis. Tumour- most common site in spine.

Thoracic Pain What is the most common tumor to cause mets to the thoracic spine?
Thoracic Spinal Nerves Tumour: Lung, Breast, Prostate, Kidney, Thyroid.

Thoracic Pain If a Thoracic Spinal nerve is compressed, is there motor weakness?

Thoracic Spinal Nerves Most usually have pain without motor weakness.

Thoracic Pain If the spinal cord is compressed, what are the clinical findings ?

Thoracic Spinal Nerves If motor Involvement- often complete weakness of both legs with areflexia due to spinal cord compression.

Case 2 45 year old male. Acute onset low back pain radiating down left leg to toes. Initial Rx Tylenol & Advil. After 1 week, severe constant unremitting pain in left leg. Unable to sit, bend forward , sleep. What historical features should be asked?

Historical Factors? 1) Trauma – recent falls. 2) Cancer- remote/recent history. 3) Lumbar spondylosis. 4) Fever, weight loss. 5) Immunosuppression. 6) Bone thinning disease ( Rheumatoid arthritis, Multiple Myeloma ).

RED FLAGS What are some of the RED FLAGS that might come up in a history of low back pain that make you think there might be a more serious condition present?

RED FLAGS Significant trauma pt. < 50 yrs. Mild trauma pt. > 50 yrs. Unexplained weight loss. Unexplained fever. Immunosupression. Cancer Hx. Night pain. IV drug use.

Red Flags Osteoporosis. Prolonged Steroid use. Age >70. Focal Neuro Deficits. Disabling symptoms. Duration > 6 weeks. Pain not relieved by laying supine.

Historical features RED Flags + Saddle anaesthesia Bowel symptoms Bladder symptoms

Questions What levels are the most common sites for fractures of the lumbar spine? What levels are the most common sites for disc herniations? What cancers metastasize to the lumbar spine?

Answers Most common site for fractures are L 1, L 2. Most common site for Disc herniations are L 4 -5, L 5 - S 1. Cancers that metastasize to lumbar spine are: Colorectal, Breast, Cervical, Lymphoma, Sarcoma.

Sciatica How often does sciatica due to disc herniation occur in low back pain patients? How often does sciatica due to disc herniation go on to develop quada equinae? Generally what nerve root does the L 4 -5 disk herniation affect?
Notes Sciatic pain secondary to disk herniation occurs in only 2% of patients with low back pain. < 1% of sciatica goes on to develop cauda equinae. Nerve roots exit below vertebra body, above the disk. Eg. L 4 -5 disk affects the L 5 nerve root. 95 % lumbar disk herniations occur from L 4 -S 1 levels.

Sciatica Why do most sciatica patients get better over time and do not require surgery?

Notes Many patients have degenerative changes in the vertebrae, especially the facet joints. With age- disk dehydration, loss of disk height, disk herniation can result in nerve root compression. As the disk desicates over time, it shrinks, pulling away from the nerve root.

Sciatica What is the value of SLR, reflexes in the examination of sciatica?

Sciatica + SLR only if lifting leg causes increased LEG pain. Radicular sciatica goes beyond the knee. Check sensation with sharp objects, not light touch. Reflexes not useful especially in the elderly.
Assessment Describe the motor , sensory, reflex findings for the following nerve root compressions: L 1 L 2 L 3 L 4 L 5 S 1 S 2 -4
Assessment- Sensory findings for the following nerve root compressions: reduced pin prick L 1 - inguinal area L 2 -middle inner thigh L 3 - distal medial thigh. L 4 - inner aspect calf, medial aspect big toe. L 5 - 1 st web space between 1 st & 2 nd toes S 1 - lateral aspect of foot, 5 th toe. S 2 -4 – perianal area.

Assessment- Reflex findings for the following nerve root compressions: L 1 -loss of superficial anal reflex, cremasteric reflex. L 2 -loss of superficial anal reflex, cremasteric reflex. L 3 - no reflex loss. L 4 - loss of patellar tendon reflex. L 5 - no reflex loss. S 1 - loss of achilles tendon reflex. S 2 -4 – no reflex loss
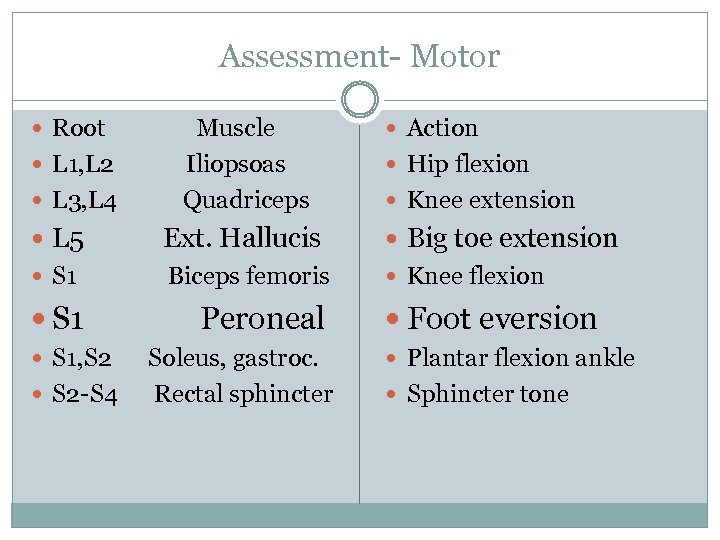
Assessment- Motor Root L 1, L 2 L 3, L 4 Muscle Iliopsoas Quadriceps Action Hip flexion Knee extension L 5 Ext. Hallucis Big toe extension S 1 Biceps femoris Knee flexion S 1, S 2 -S 4 Peroneal Soleus, gastroc. Rectal sphincter Foot eversion Plantar flexion ankle Sphincter tone
Assessment Root L 1 L 2, L 3 L 4 L 5 S 1 S 2 -S 4 Sensory Area Inguinal crease Medial thigh Medial calf 1 st web space ( 1 st – 2 nd toes ) Lateral aspect of foot Perianal sensation

Imaging What is the value of plain x-rays of the lumbar spine?
Imaging X-rays if: <18 , > 50 yrs. old. Hx Cancer- won’t show change till 30% bone destruction. Hx fever, IV drug use, immunocompromise. Major trauma. Osteoporosis. Symptoms > 6 weeks.

Imaging What is the value of a CT scan of the lumbar spine?

Imaging Can be used for known fractures.

Imaging What is the value of MRI of the lumbar spine?

Imaging MRI better than CT ( no radiation exposure ) Better resolution of soft tissue, spinal cord, epidural space.
Treatment of Back pain Most patients have non specific low back pain. Most have pain resolution in 4 weeks. Subacute LBP last 4 -2 weeks. Chronic LBP lasts > 12 weeks. WHAT WOULD BE POSSIBLE TREATMENT OPTIONS FOR LOW BACK PAIN ?

Literature Review- NO BENEFIT Firmer mattress TENS Lumbar support Ultrasound Muscle relaxants Traction Benzodiazepines Short wave diathermy Gabapentin Low level laser Bed rest Interferential Epidural corticosteroids

Recommend NSAIDS + Acetominophen for acute exacerbations of subacute and chronic LBP. Opoids only for short duration in pts. with low vulnerability for drug abuse. Trycyclics are good for chronic LBP. Home & supervised exercise program ( stretching and strengthening ). Some people may benefit from Cognitive behavioural therapy, Yoga, massage, spinal manipulation ( all moderately more effective than sham/placebo Rx ).

Surgery for Sciatica What are the indications for surgery for sciatica?

Surgery for Sciatica 50 % of sciatica pts. get better in 6 weeks on their own. Surgery is good for : Intractable pain. Worsening neuro deficits. No improvement in 6 weeks with conservative treatment.

Spinal Stenosis Describe the features of a patient with Spinal Stenosis?
Spinal Stenosis Local segmental or generalized narrowing of the central spinal canal by bone or soft tissue elements ( Hypertrophic facets, thick ligamentum flavum ). Features: Diffuse back pain in older patient. Transient tingling in legs ( both ). Ambulation induced pain in calf/lower leg. Resolves with sitting, forward flexion, rest. Worse with back extension. SLR + ve in 50%. Treatment conservative unless failed Rx > 3 months.

Cauda Equinae Describe the clinical features of Cauda Equina. What are some of the causes?

Cauda Equinae Loss of Bowel / Bladder control ( 90 % have retention ) Saddle anaesthesia. Reduced rectal tone. Weakness in lower extremities. Related to compression of spinal nerve roots due to: Tumour, bony stenosis or disc herniation ( central ). Tumours- Prostate, colorectal, non Hodgkins lymphoma, sarcoma, GYN tumours, Renal Cell Ca, multiple myeloma.

Cauda Equinae How do you check for anal tone? What amount of residual post void urine would qualify as urinary retention? What is the imaging of choice?
Cauda Equinae Check anal tone – resistance to finger entering. - buttock squeeze test. Post void test – if > 200 cc ( urinary retention ). MRI imaging of choice Refer to Neurosurgeon if confirmed.
Other Peripheral Nerve Compression Syndromes Median Nerve Entrapment- Carpal Tunnel, Pronator Teres Syndromes. Ulnar Nerve Compression- at elbow, at wrist. Radial Nerve Compression- Spiral groove, posterior interosseus.

Median Nerve Compression Describe the causes, symptoms and clinical findings of carpal tunnel syndrome?
Median Nerve- Carpal Tunnel Syndrome Compression of median nerve thru carpal tunnel ( axonal dysfunction ). Causes: Pain, Paraethesias in hands and later weakness of median nerve. Assoc. Conditions- pregnancy, diabetes, hypothyroid, renal failure. Usually caused by overuse- swelling of flexor tendons. Findings: Sensory loss volar 1 st 3 fingers + lat. 4 th finger, normal thenar Motor loss: weak thumb abduction, flexion MCP jts. Examination: Tinel sign ( taping tunnel ) 50 -60%sens. 67 -77% specific. Phalens sign ( palmar flexion > 30 sec. ) 70 % sens. , 47 -73 % specific.

Median Nerve- Carpal Tunnel Syndrome Describe the initial treatment for Carpal Tunnel. Are NSAIDS useful? Predictive factors for failure of conservative measures? Place for surgery?

Median Nerve – Carpal Tunnel Treatment Conservative: Nocturnal splinting, oral corticosteroids ( 2 weeks ), corticosteroid injections, Yoga. NSAIDS no help compared to placebo. Prediction of failure Conservative RX: Age > 50, Duration > 10 months, constant paraethesias, impaired 2 point discrimination, +ve Phalens sign < 30 seconds, Prolonged motor and sensory latency on NCS& EMG. Surgery- Best long term relief of symptoms.

Median Nerve – Pronator Teres Syndrome What are the different features compared to Carpal Tunnel Syndrome?

Median Nerve- Pronator Teres Syndrome Median nerve entrapment in proximal forearm. Forearm flexor pain. Same findings as carpal tunnel EXCEPT: Numbness thenar eminence and weak thenar muscles. Treatment: rest, corticosteroid inj. , surgery if persistent symptoms.

Ulnar Nerve Compression Describe the findings of ulnar nerve compression at the elbow. Describe ulnar nerve compression at the wrist.
Ulnar Nerve Compression At the Elbow: at the epicondylar groove. Leaning on the elbow. Numbness 4 th-5 th fingers. Weak finger and wrist FLEXION, Ulnar deviation wrist. , weak abduction of the index finger. At the wrist: in Guyon’s canal. Numbness 4 th-5 th fingers. Weak interossei, Finger FLEXION Spared.

Radial Nerve Compression Describe the findings of Radial nerve compression at the spiral groove. Describe the findings of Posterior interosseus Neuropathy.

Radial Nerve Compression At Spiral Groove: Saturday night palsy- shoulder vs arm of sofa. Numbness 1 st web space dorsally Weak wrist ( drop ) and finger extension, brachioradialis. Triceps spared. Recovery with wrist splint in 6 -8 weeks. Posterior Interosseus Neuropathy- a branch of radial nerve proximal to elbow, innervates forearm extensorsweak 3 rd finger extension and forearm supination.

Nerve Conduction studies Good for delineation of severity of Median, Ulnar or Radial nerve dysfunction.

Mono and Polyneuropathies Important to know if sensorimotor findings are: Symmetric or Asymmetric. Distal or distal and proximal. Sensory only, Motor only or mixed.

Guillain-Barre Syndrome Acute Inflammatory Polyradiculoneuropathy. Immune mediated inflammation of peripheral nerves disrupting myelin and causing axonal loss. Most common acute motor neuropathy. Usually has a preceding history of a URI or GI illness preceeding the onset. Describe the symptoms and findings.

Guillain Barre Syndrome Progressive Symmetric WEAKNESS of proximal + distal muscles. May involve cranial nerves in up to 50 % cases. Loss of DTR. Variable sensory findings ( can occur in 33%) Sparing of anal tone. May have urinary retention ( autonomic dysfunction). Patients with primarily sensory signs are unlikely to have respiratory distress.

Guillain Barre Syndrome 50% have autonomic dysfunction- fluctuating BP, pulse. Peaks at 1 week. Some cranial nerve dysfunction ( 7 th nerve ). 33 % require respiratory support. 3% mortaility / recurrence rate. Describe the lab and imaging abnormalities:

Guillain Barre Syndrome CSF analysis: Elevated protein, no increased WBC. EMG/NCS- show demyelination disorder, loss of 80 % of normal muscle action potential suggests poor prognosis. MRI shows enhancement of anterior spinal nerve roots. FEV 1. 0, ABG, to check for CO 2 retention. May need prophylactic intubation. Check for extensor neck strength.

Guillain Barre Syndrome What is the treatment for GBS?

Treatment Plasmapheresis. Pooled IV gammaglobulin. Supportive care. Ventilatory help if needed. Corticosteroids not helpful.

Distal Symmetric Polyneuropathy Stocking glove sensory distribution. Motor findings lag behind sensory. Progress distal to proximal. Causes: Diabetes, Alcoholism, Neoplasm, HIV, Toxins, drugs. Describe the findings in Diabetic neuropathy:

Diabetic Neuropathy Dysaesthesias ( tingling, burning ) plantar aspect feet. Weakness big toe extension 1 st motor sign. Followed by weak dorsiflexion ankle, foot drop, loss of ankle jerks. Sensory loss moves to knees and fingers. DTR eventually lost. Proprioception loss and may develop sensory ataxia.

Diabetic Neuropathy Treatment: Tricyclics ( Elavil 25 mg qhs ). Tegretol 200 mg Q 8 h. SSRI ( Paroxetine ). No help from Trazadone, Dilantin, topical capsaicin.

Mononeuropathy Multiplex Asymmetric Sensorimotor peripheral neuroathy. Sensory findings match the motor findings. May have reflex loss depending on the nerve involved. Causes: Diabetes most common, vasculitis second. Others Neoplasm, Lyme disease, HIV, Sarcoid

Anterior horn cell Neuronopathy- ALS Amyotrophic Lateral Sclerosis. Asymmetrical distal motor weakness with no sensory loss. Subclinical Autonomic dysfunction. Has both Upper and Lower motor neuron signs. What are they?

ALS Upper Motor Neuron findings: Hyperreflexia – sustained ankle clonus Spasticity. Positive Babinski. Lower motor Neuron findings: Fasiculations. Cramps. Asymmetrical distal weakness with atrophy.

ALS EMG confirms the diagnosis. Treatment supportive only.
Sensory Neuronopathies Affects dorsal root ganglions. Pure sensory syndrome. No motor weakness. Loss of DTR. Loss of proprioception. Sensory ataxia.
Sensory Neuronopathy Causes: Herpes Simplex, Paraneoplastic syndromes, Sjogrens, Vitamin deficiencies. Diagnoses via MRI of the spinal cord.
b2d1d68551ee0a9e1b3e24ff9c1c8d06.ppt