d9d35e406165cd902cb6de62c1aed471.ppt
- Количество слайдов: 85
 Glycemic Control In The Hospital Setting
Glycemic Control In The Hospital Setting
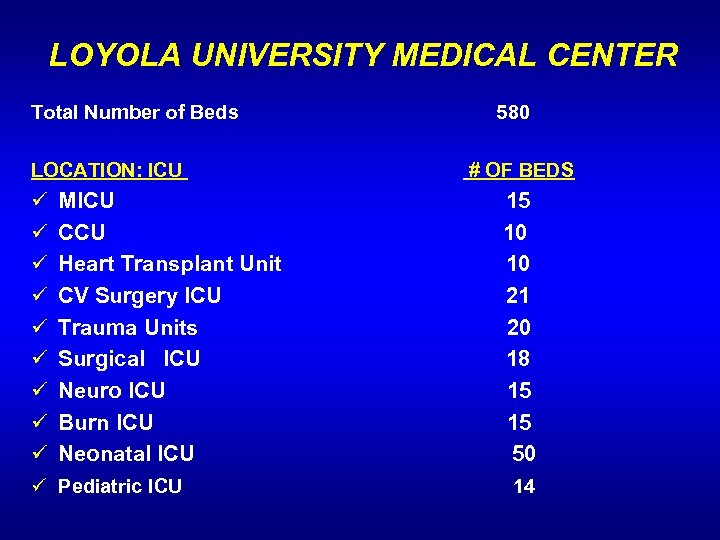 LOYOLA UNIVERSITY MEDICAL CENTER Total Number of Beds LOCATION: ICU 580 # OF BEDS MICU 15 CCU 10 Heart Transplant Unit 10 CV Surgery ICU 21 Trauma Units 20 Surgical ICU 18 Neuro ICU 15 Burn ICU 15 Neonatal ICU 50 ü Pediatric ICU 14 ü ü ü ü ü
LOYOLA UNIVERSITY MEDICAL CENTER Total Number of Beds LOCATION: ICU 580 # OF BEDS MICU 15 CCU 10 Heart Transplant Unit 10 CV Surgery ICU 21 Trauma Units 20 Surgical ICU 18 Neuro ICU 15 Burn ICU 15 Neonatal ICU 50 ü Pediatric ICU 14 ü ü ü ü ü
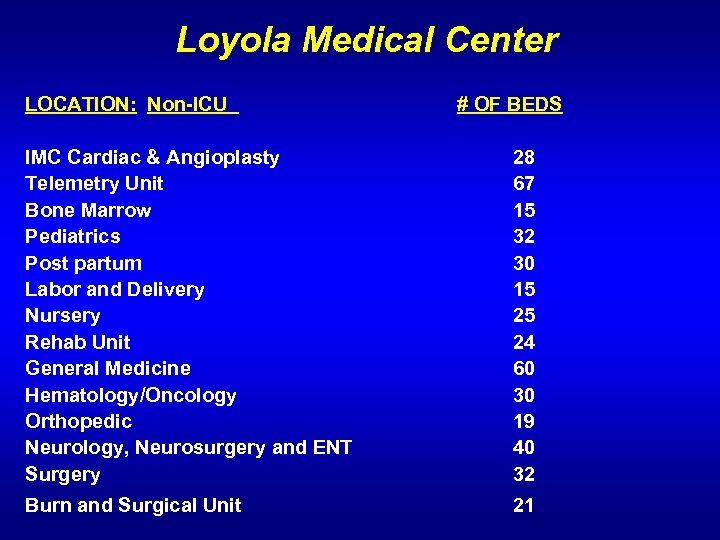 Loyola Medical Center LOCATION: Non-ICU # OF BEDS IMC Cardiac & Angioplasty 28 Telemetry Unit 67 Bone Marrow 15 Pediatrics 32 Post partum 30 Labor and Delivery 15 Nursery 25 Rehab Unit 24 General Medicine 60 Hematology/Oncology 30 Orthopedic 19 Neurology, Neurosurgery and ENT 40 Surgery 32 Burn and Surgical Unit 21
Loyola Medical Center LOCATION: Non-ICU # OF BEDS IMC Cardiac & Angioplasty 28 Telemetry Unit 67 Bone Marrow 15 Pediatrics 32 Post partum 30 Labor and Delivery 15 Nursery 25 Rehab Unit 24 General Medicine 60 Hematology/Oncology 30 Orthopedic 19 Neurology, Neurosurgery and ENT 40 Surgery 32 Burn and Surgical Unit 21
 Glycemic Control In The Hospital Setting ÊThe Evidence For Tight Glycemic Control ÊThe Achievement of Better Control: Strategies and Protocols
Glycemic Control In The Hospital Setting ÊThe Evidence For Tight Glycemic Control ÊThe Achievement of Better Control: Strategies and Protocols
 Insulin In The Hospital Setting Retrospective Studies
Insulin In The Hospital Setting Retrospective Studies
 Hyperglycemia in the Hospital CABG Ê Tight Control Hospital Mortality 50% Kalin. Diabetes. 1998; 47: a 87 Ê Tight Control Postop Infections 75% Golden SH, Et Al. Diabetes Care. 1999; 22: 1408 -1414 Ê Tight Control Sternal Wounds 60% Furnary AP, Et Al. Ann Thorac Surg. 1999; 67: 352 -362 Ê Tight Control Sternal Wounds 60% Zerr KJ, Et Al. Ann Thorac Surg. 1997; 63: 356 -361 General Surgery Ê Hyperglycemia Serious Infections X 6 Pomposelli JJ, Et Al. J Parenter Enteral Nutr. 1998; 12: 628 -652
Hyperglycemia in the Hospital CABG Ê Tight Control Hospital Mortality 50% Kalin. Diabetes. 1998; 47: a 87 Ê Tight Control Postop Infections 75% Golden SH, Et Al. Diabetes Care. 1999; 22: 1408 -1414 Ê Tight Control Sternal Wounds 60% Furnary AP, Et Al. Ann Thorac Surg. 1999; 67: 352 -362 Ê Tight Control Sternal Wounds 60% Zerr KJ, Et Al. Ann Thorac Surg. 1997; 63: 356 -361 General Surgery Ê Hyperglycemia Serious Infections X 6 Pomposelli JJ, Et Al. J Parenter Enteral Nutr. 1998; 12: 628 -652
 Hyperglycemia in the Hospital Stroke Ê Hyperglycemia Independent Determinent of Infarct Expansion Baird TA, et al. Stroke. 2003; 34: 2208 -14 Ê Hyperglycemia Hospital Mortality X 2 Weir CJ, et al. BMJ. 1997; 314: 1303 -1306 Ê Hyperglycemia Hospital Mortality X 2 Jorgensen H, et al. Stroke. 1994; 25: 1977 -1984
Hyperglycemia in the Hospital Stroke Ê Hyperglycemia Independent Determinent of Infarct Expansion Baird TA, et al. Stroke. 2003; 34: 2208 -14 Ê Hyperglycemia Hospital Mortality X 2 Weir CJ, et al. BMJ. 1997; 314: 1303 -1306 Ê Hyperglycemia Hospital Mortality X 2 Jorgensen H, et al. Stroke. 1994; 25: 1977 -1984
 Hyperglycemia In Critical Illness Targeting Risk? From The VA Inpatient Evaluation Center ÊFrom 177 ICUs In 73 VA Hospitals Ê216, 000 Patients Ê Glycemia Independent Predictor Of Mortality Starting At 1 mg% Above Normal (Normal = 70 -110 mg%) Ê True In Medical, Surgical & Cardiac ICUs Falciglia, M. et al Annual Meeting of the American Diabetes Association, 2006
Hyperglycemia In Critical Illness Targeting Risk? From The VA Inpatient Evaluation Center ÊFrom 177 ICUs In 73 VA Hospitals Ê216, 000 Patients Ê Glycemia Independent Predictor Of Mortality Starting At 1 mg% Above Normal (Normal = 70 -110 mg%) Ê True In Medical, Surgical & Cardiac ICUs Falciglia, M. et al Annual Meeting of the American Diabetes Association, 2006
 Hyperglycemia In Critical Illness Targeting Risk? From The VA Inpatient Evaluation Center Different Disease States Variably Affected Condition Risk Of Death* Acute MI 1. 6 -5 Unstable Angina 1. 7 -6. 2 Stroke 3. 4 -15. 1 Outcomes Worse In “Non-Diabetics” * Fold Increase Falciglia, M. et al Annual Meeting of the American Diabetes Association, 2006
Hyperglycemia In Critical Illness Targeting Risk? From The VA Inpatient Evaluation Center Different Disease States Variably Affected Condition Risk Of Death* Acute MI 1. 6 -5 Unstable Angina 1. 7 -6. 2 Stroke 3. 4 -15. 1 Outcomes Worse In “Non-Diabetics” * Fold Increase Falciglia, M. et al Annual Meeting of the American Diabetes Association, 2006
 Insulin In The Hospital Setting Prospective Studies
Insulin In The Hospital Setting Prospective Studies
 DIGAMI Study 620 Randomized to 2 Groups At 19 Swedish Hospitals Control: Standard Coronary Care for Their Center ü Intensive: Insulin-Glucose Infusion for >24 Hrs ü n n Target Serum Glucose 126 – 180 mg/dl Multidose (4/day) Insulin for Minimum of 3 Months Following Discharge BMJ 314: 1512 -1515, 1997
DIGAMI Study 620 Randomized to 2 Groups At 19 Swedish Hospitals Control: Standard Coronary Care for Their Center ü Intensive: Insulin-Glucose Infusion for >24 Hrs ü n n Target Serum Glucose 126 – 180 mg/dl Multidose (4/day) Insulin for Minimum of 3 Months Following Discharge BMJ 314: 1512 -1515, 1997
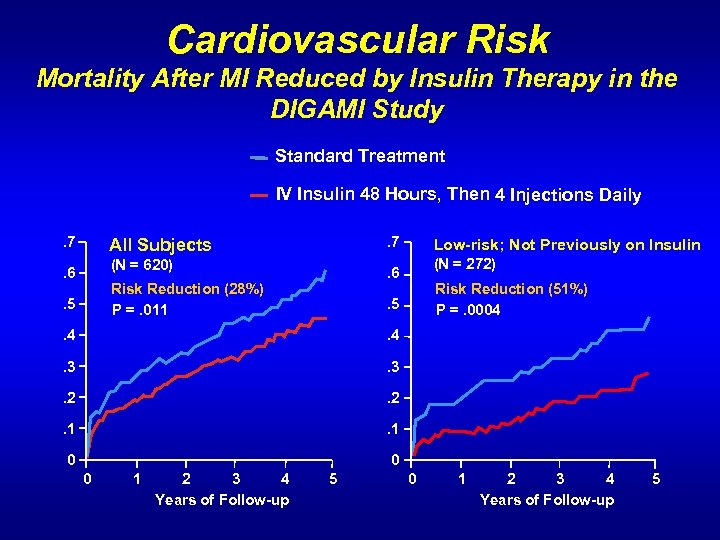 Cardiovascular Risk Mortality After MI Reduced by Insulin Therapy in the DIGAMI Study Standard Treatment IV Insulin 48 Hours, Then 4 Injections Daily. 7 All Subjects (N = 620) . 6 (N = 272) . 6 Risk Reduction (28%) P =. 011 . 5 Low-risk; Not Previously on Insulin Risk Reduction (51%) P =. 0004 . 5 . 4 . 3 . 2 . 1 0 0 0 1 2 3 4 Years of Follow-up 5
Cardiovascular Risk Mortality After MI Reduced by Insulin Therapy in the DIGAMI Study Standard Treatment IV Insulin 48 Hours, Then 4 Injections Daily. 7 All Subjects (N = 620) . 6 (N = 272) . 6 Risk Reduction (28%) P =. 011 . 5 Low-risk; Not Previously on Insulin Risk Reduction (51%) P =. 0004 . 5 . 4 . 3 . 2 . 1 0 0 0 1 2 3 4 Years of Follow-up 5
 Intensive Insulin Therapy in Critically Ill Patients Van Den Berghe, G et al. NEJM 345: 1359 -1367. 2001
Intensive Insulin Therapy in Critically Ill Patients Van Den Berghe, G et al. NEJM 345: 1359 -1367. 2001
 Intensive Insulin Therapy in Critically Ill Patients 1548 Mechanically Ventilated Patients in SICU Glucose Achieved: 2 Glycemic Treatment Groups: n n Control 153 mg/dl Insulin Infusion to Keep Blood Glucose 80 -110 mg/dl Intensive 103 mg/dl Insulin Treatment Only If Blood Glucose >215 mg/dl to Maintain Glucose 180 - 210 mg/dl van den Berghe G. N Engl J Med 2001; 345: 1359
Intensive Insulin Therapy in Critically Ill Patients 1548 Mechanically Ventilated Patients in SICU Glucose Achieved: 2 Glycemic Treatment Groups: n n Control 153 mg/dl Insulin Infusion to Keep Blood Glucose 80 -110 mg/dl Intensive 103 mg/dl Insulin Treatment Only If Blood Glucose >215 mg/dl to Maintain Glucose 180 - 210 mg/dl van den Berghe G. N Engl J Med 2001; 345: 1359
 Intensive Insulin Therapy in Critically Ill Patients n 87% Diagnosed With DM in the ICU n 13% Had Previous Dx of Diabetes Mellitus n 5% Had Previous Insulin Treatment van den Berghe G. N Engl J Med 2001; 345: 1359
Intensive Insulin Therapy in Critically Ill Patients n 87% Diagnosed With DM in the ICU n 13% Had Previous Dx of Diabetes Mellitus n 5% Had Previous Insulin Treatment van den Berghe G. N Engl J Med 2001; 345: 1359
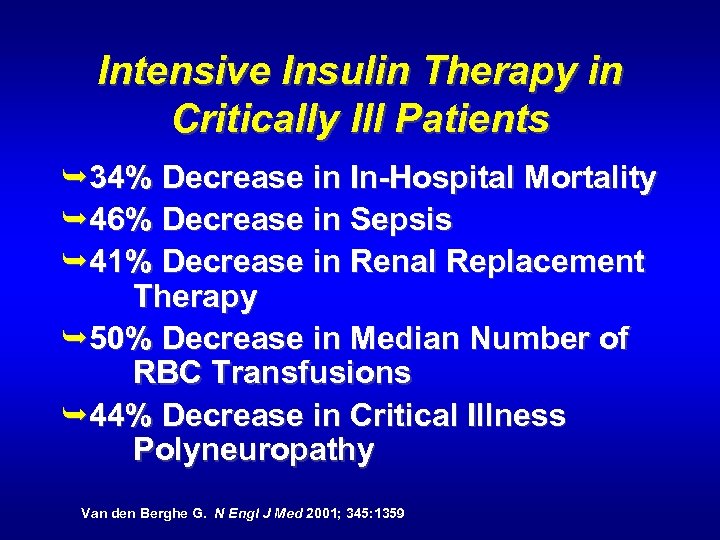 Intensive Insulin Therapy in Critically Ill Patients Ê34% Decrease in In-Hospital Mortality Ê46% Decrease in Sepsis Ê41% Decrease in Renal Replacement Therapy Ê50% Decrease in Median Number of RBC Transfusions Ê44% Decrease in Critical Illness Polyneuropathy Van den Berghe G. N Engl J Med 2001; 345: 1359
Intensive Insulin Therapy in Critically Ill Patients Ê34% Decrease in In-Hospital Mortality Ê46% Decrease in Sepsis Ê41% Decrease in Renal Replacement Therapy Ê50% Decrease in Median Number of RBC Transfusions Ê44% Decrease in Critical Illness Polyneuropathy Van den Berghe G. N Engl J Med 2001; 345: 1359
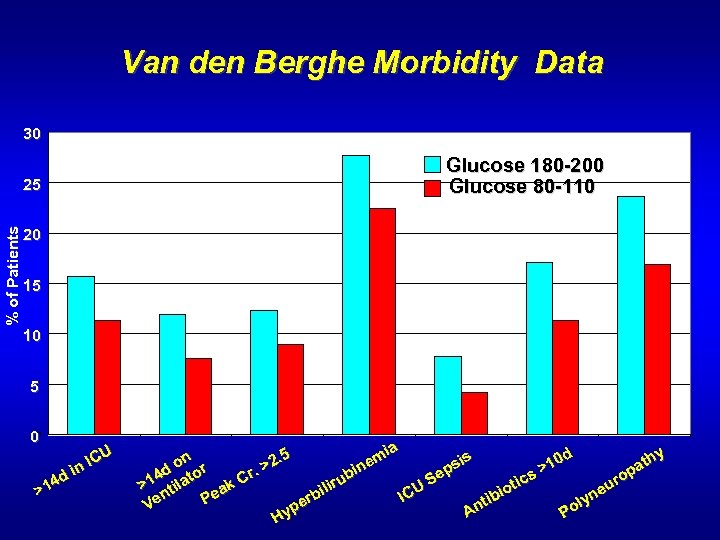 Van den Berghe Morbidity Data 30 % of Patients 25 Glucose 180 -200 Glucose 80 -110 20 15 10 5 0 U IC in 4 d >1 a y d mi n 2. 5 e 10 sis o r > ath p in. > d op ub Se 14 ilato Cr ics t ur ir k > t U a e il io IC rb Pe en tib lyn V pe An Po Hy
Van den Berghe Morbidity Data 30 % of Patients 25 Glucose 180 -200 Glucose 80 -110 20 15 10 5 0 U IC in 4 d >1 a y d mi n 2. 5 e 10 sis o r > ath p in. > d op ub Se 14 ilato Cr ics t ur ir k > t U a e il io IC rb Pe en tib lyn V pe An Po Hy
 Lazar, H. et al Circulation 109: 1997 -1502, 2004
Lazar, H. et al Circulation 109: 1997 -1502, 2004
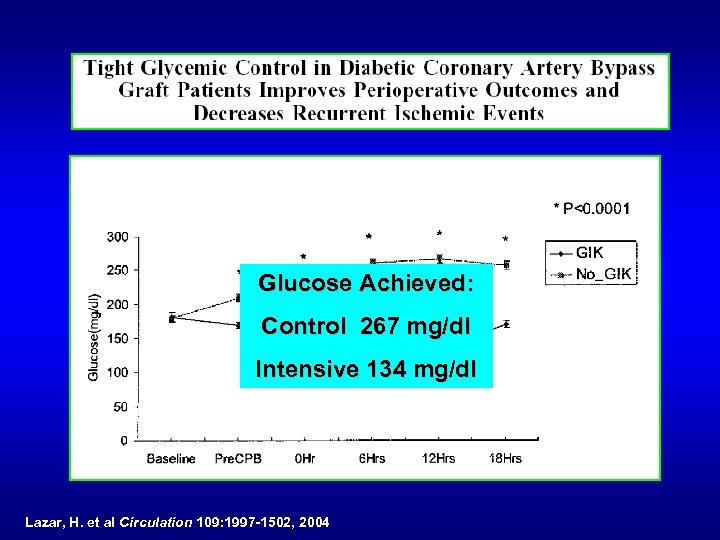 Glucose Achieved: Control 267 mg/dl Intensive 134 mg/dl Lazar, H. et al Circulation 109: 1997 -1502, 2004
Glucose Achieved: Control 267 mg/dl Intensive 134 mg/dl Lazar, H. et al Circulation 109: 1997 -1502, 2004
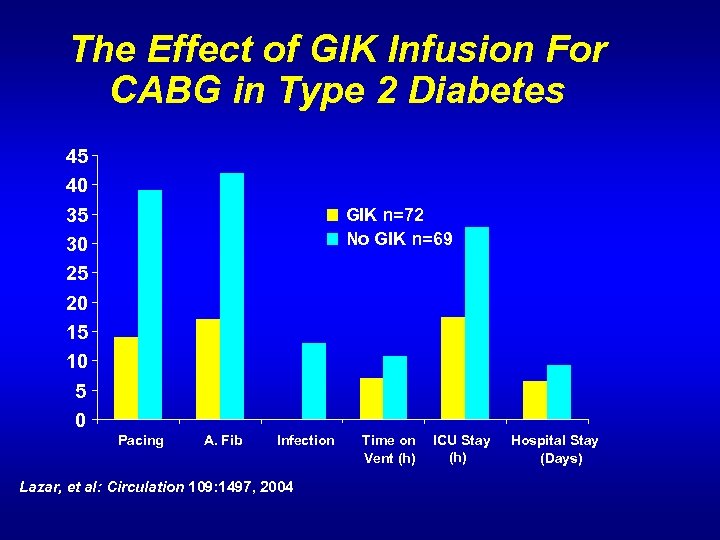 The Effect of GIK Infusion For CABG in Type 2 Diabetes 45 40 35 30 25 20 15 10 5 0 GIK n=72 No GIK n=69 Pacing A. Fib Infection Lazar, et al: Circulation 109: 1497, 2004 Time on Vent (h) ICU Stay (h) Hospital Stay (Days)
The Effect of GIK Infusion For CABG in Type 2 Diabetes 45 40 35 30 25 20 15 10 5 0 GIK n=72 No GIK n=69 Pacing A. Fib Infection Lazar, et al: Circulation 109: 1497, 2004 Time on Vent (h) ICU Stay (h) Hospital Stay (Days)
 And Now Van den Berghe -2 Van den Berghe, G. et al NEJM 354: 449 -61, 2006
And Now Van den Berghe -2 Van den Berghe, G. et al NEJM 354: 449 -61, 2006
 Intensive Insulin Therapy in the Medical ICU Greet Van den Berghe, M. D. , Ph. D. , Alexander Wilmer, M. D. , Ph. D. , Greet Hermans, M. D. , Wouter Meersseman, M. D. , Pieter J. Wouters, M. Sc. , Ilse Milants, R. N. , Eric Van Wijngaerden, M. D. , Ph. D. , Herman Bobbaers, M. D. , Ph. D. , and Roger Bouillon, M. D. , Ph. D.
Intensive Insulin Therapy in the Medical ICU Greet Van den Berghe, M. D. , Ph. D. , Alexander Wilmer, M. D. , Ph. D. , Greet Hermans, M. D. , Wouter Meersseman, M. D. , Pieter J. Wouters, M. Sc. , Ilse Milants, R. N. , Eric Van Wijngaerden, M. D. , Ph. D. , Herman Bobbaers, M. D. , Ph. D. , and Roger Bouillon, M. D. , Ph. D.
 Intensive Insulin Therapy in Critically Ill Patients: Van den Berghe 2 1200 Patients in MICU 2 Glycemic Treatment Groups: n n Glucose Achieved: Insulin Infusion to Keep Blood Glucose Control 153 mg/dl 80 -110 mg/dl Intensive 111 mg/dl Insulin Treatment Only If Blood Glucose >215 mg/dl to Maintain Glucose 180 - 200 mg/dl van den Berghe G. N Engl J Med 2006; 354: 449
Intensive Insulin Therapy in Critically Ill Patients: Van den Berghe 2 1200 Patients in MICU 2 Glycemic Treatment Groups: n n Glucose Achieved: Insulin Infusion to Keep Blood Glucose Control 153 mg/dl 80 -110 mg/dl Intensive 111 mg/dl Insulin Treatment Only If Blood Glucose >215 mg/dl to Maintain Glucose 180 - 200 mg/dl van den Berghe G. N Engl J Med 2006; 354: 449
 With Intensive Insulin Therapy ÊReduced Newly Acquired Kidney Disease ÊEarlier Weaning From Ventilator ÊFaster Discharge from ICU ÊShorter Hospital Length of Stay Van den Berghe, G. et al NEJM 354: 449 -61, 2006
With Intensive Insulin Therapy ÊReduced Newly Acquired Kidney Disease ÊEarlier Weaning From Ventilator ÊFaster Discharge from ICU ÊShorter Hospital Length of Stay Van den Berghe, G. et al NEJM 354: 449 -61, 2006
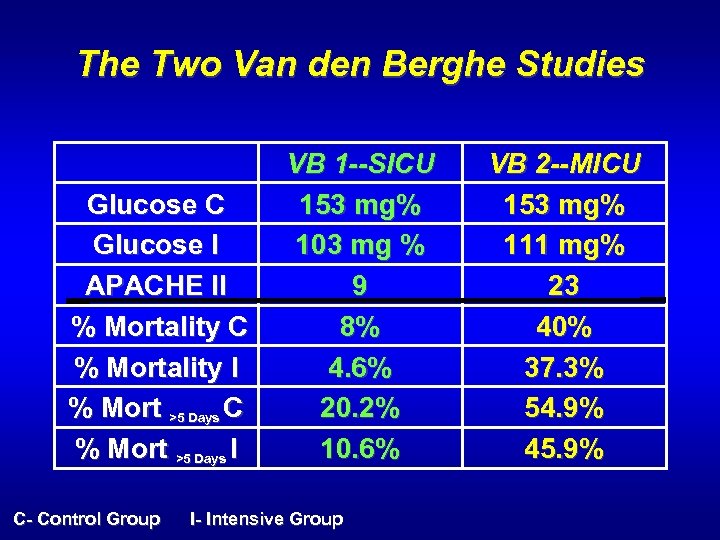 The Two Van den Berghe Studies Glucose C Glucose I APACHE II % Mortality C % Mortality I % Mort >5 Days C % Mort >5 Days I VB 1 --SICU 153 mg% 103 mg % 9 8% 4. 6% 20. 2% 10. 6% C- Control Group I- Intensive Group VB 2 --MICU 153 mg% 111 mg% 23 40% 37. 3% 54. 9% 45. 9%
The Two Van den Berghe Studies Glucose C Glucose I APACHE II % Mortality C % Mortality I % Mort >5 Days C % Mort >5 Days I VB 1 --SICU 153 mg% 103 mg % 9 8% 4. 6% 20. 2% 10. 6% C- Control Group I- Intensive Group VB 2 --MICU 153 mg% 111 mg% 23 40% 37. 3% 54. 9% 45. 9%

 New Trials On The Horizon… Ê NICE (Normo. Glycemia In Intensive Care Evaluation: 4, 000 Patients in 20 ICU’s In NICE + SUGAR = Australia & New Zealand NICE-SUGAR Ê SUGAR (Survival Using Glucose Algorithm Regulation): Another 1, 000 ICU Patients In Canada
New Trials On The Horizon… Ê NICE (Normo. Glycemia In Intensive Care Evaluation: 4, 000 Patients in 20 ICU’s In NICE + SUGAR = Australia & New Zealand NICE-SUGAR Ê SUGAR (Survival Using Glucose Algorithm Regulation): Another 1, 000 ICU Patients In Canada
 Is It Less Serious If a Patient Has Not Had a Previous Diagnosis of Diabetes?
Is It Less Serious If a Patient Has Not Had a Previous Diagnosis of Diabetes?
 Hyperglycemia: An Independent Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes n n Question: Does Hyperglycemia, New or Established, Predict Mortality? 2030 Consecutive Records of Adults Admitted to Georgia Baptist Hospital Hyperglycemia: FBG ≥ 126 mg/dl or Random Glucose ≥ 200 mg/dl New Hyperglycemia 223 Pts. (12%) Umpierrez GR et al. J Clin Endocrinol Metab 2002; 87: 978
Hyperglycemia: An Independent Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes n n Question: Does Hyperglycemia, New or Established, Predict Mortality? 2030 Consecutive Records of Adults Admitted to Georgia Baptist Hospital Hyperglycemia: FBG ≥ 126 mg/dl or Random Glucose ≥ 200 mg/dl New Hyperglycemia 223 Pts. (12%) Umpierrez GR et al. J Clin Endocrinol Metab 2002; 87: 978
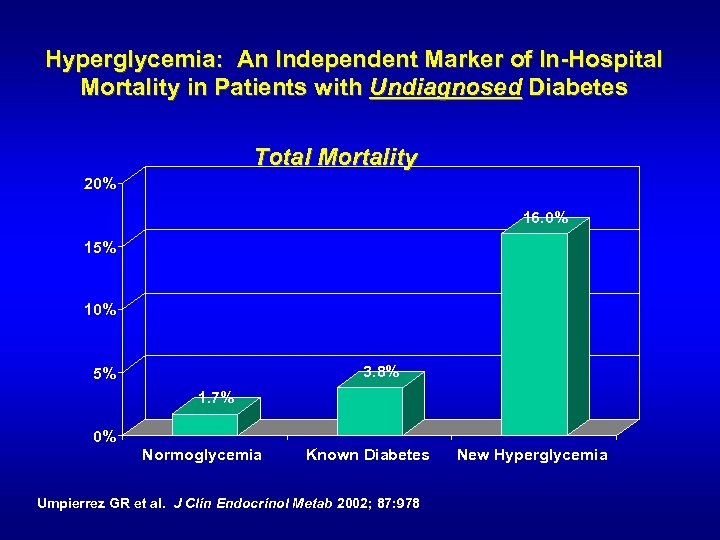 Hyperglycemia: An Independent Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes Total Mortality 20% 16. 0% 15% 10% 3. 8% 5% 1. 7% 0% Normoglycemia Known Diabetes Umpierrez GR et al. J Clin Endocrinol Metab 2002; 87: 978 New Hyperglycemia
Hyperglycemia: An Independent Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes Total Mortality 20% 16. 0% 15% 10% 3. 8% 5% 1. 7% 0% Normoglycemia Known Diabetes Umpierrez GR et al. J Clin Endocrinol Metab 2002; 87: 978 New Hyperglycemia
 A Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes n n New Hyperglycemia Patients ~3 x’s As Likely to Be Admitted to ICU New Hyperglycemia Patients Had Twice the Length of Stay Umpierrez GR et al. J Clin Endocrinol Metab 2002; 87: 978
A Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes n n New Hyperglycemia Patients ~3 x’s As Likely to Be Admitted to ICU New Hyperglycemia Patients Had Twice the Length of Stay Umpierrez GR et al. J Clin Endocrinol Metab 2002; 87: 978
 There are other benefits…
There are other benefits…
 Glycemic Management In The Hospital Financial Aspects Van den Berghe, G. et al Crit Care Med 34: 612 -616, 2006
Glycemic Management In The Hospital Financial Aspects Van den Berghe, G. et al Crit Care Med 34: 612 -616, 2006
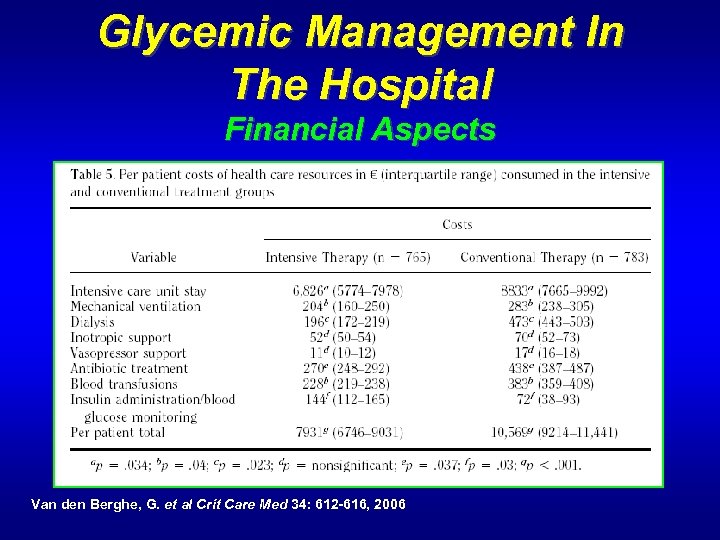 Glycemic Management In The Hospital Financial Aspects Van den Berghe, G. et al Crit Care Med 34: 612 -616, 2006
Glycemic Management In The Hospital Financial Aspects Van den Berghe, G. et al Crit Care Med 34: 612 -616, 2006
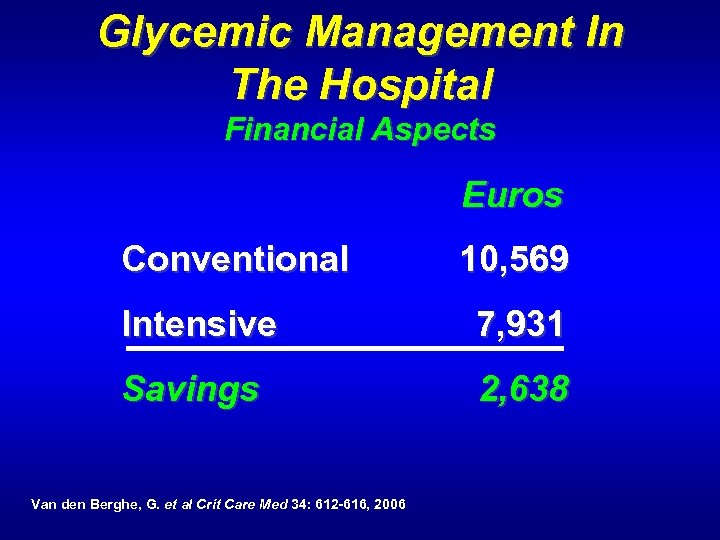 Glycemic Management In The Hospital Financial Aspects Euros Conventional 10, 569 Intensive 7, 931 Savings Van den Berghe, G. et al Crit Care Med 34: 612 -616, 2006 2, 638
Glycemic Management In The Hospital Financial Aspects Euros Conventional 10, 569 Intensive 7, 931 Savings Van den Berghe, G. et al Crit Care Med 34: 612 -616, 2006 2, 638
 Glycemic Control In The Hospital Setting The days of casual glycemic control for critically ill patients should be over!
Glycemic Control In The Hospital Setting The days of casual glycemic control for critically ill patients should be over!
 Glycemic Control In The Hospital Setting ÊThe Evidence For Tight Glycemic Control ÊThe Achievement of Better Control: Strategies and Protocols
Glycemic Control In The Hospital Setting ÊThe Evidence For Tight Glycemic Control ÊThe Achievement of Better Control: Strategies and Protocols
 What Are The Treatment Goals?
What Are The Treatment Goals?
 Hospital Glycemic Goals Intensive Care Units: Non-Critical Care Units: Pre-Prandial Max. Glucose Endocrine Practice 10: 77 -82, 2004 Diabetes Care 27: 553 -591, 2004 AACE Consensus Conference - 2003 110 mg/d. L 180 mg/d. L
Hospital Glycemic Goals Intensive Care Units: Non-Critical Care Units: Pre-Prandial Max. Glucose Endocrine Practice 10: 77 -82, 2004 Diabetes Care 27: 553 -591, 2004 AACE Consensus Conference - 2003 110 mg/d. L 180 mg/d. L
 Strategies and Protocols for Achieving Inpatient Glycemic Control
Strategies and Protocols for Achieving Inpatient Glycemic Control
 IV Insulin Infusion Protocols
IV Insulin Infusion Protocols
 The Ideal IV Insulin Protocol ü Easily Ordered (Signature Only) ü Effective (Reach Goal Quickly) ü Safe (Minimal Risk Of Hypoglycemia) ü Easily Implemented
The Ideal IV Insulin Protocol ü Easily Ordered (Signature Only) ü Effective (Reach Goal Quickly) ü Safe (Minimal Risk Of Hypoglycemia) ü Easily Implemented
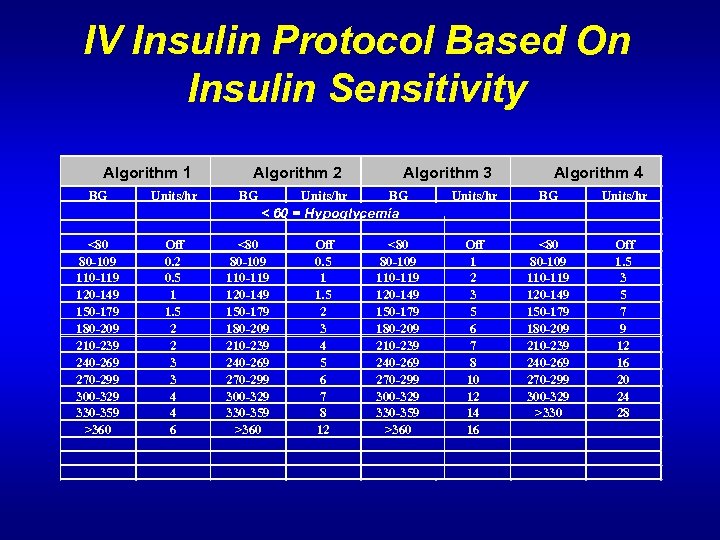 IV Insulin Protocol Based On Insulin Sensitivity Algorithm 1 BG Units/hr Algorithm 2 BG Units/hr Algorithm 3 BG Algorithm 4 Units/hr BG Units/hr Off 1 2 3 5 6 7 8 10 12 14 16 <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 >330 Off 1. 5 3 5 7 9 12 16 20 24 28 < 60 = Hypoglycemia <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 330 -359 >360 Off 0. 2 0. 5 1 1. 5 2 2 3 3 4 4 6 <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 330 -359 >360 Off 0. 5 1 1. 5 2 3 4 5 6 7 8 12 <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 330 -359 >360
IV Insulin Protocol Based On Insulin Sensitivity Algorithm 1 BG Units/hr Algorithm 2 BG Units/hr Algorithm 3 BG Algorithm 4 Units/hr BG Units/hr Off 1 2 3 5 6 7 8 10 12 14 16 <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 >330 Off 1. 5 3 5 7 9 12 16 20 24 28 < 60 = Hypoglycemia <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 330 -359 >360 Off 0. 2 0. 5 1 1. 5 2 2 3 3 4 4 6 <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 330 -359 >360 Off 0. 5 1 1. 5 2 3 4 5 6 7 8 12 <80 80 -109 110 -119 120 -149 150 -179 180 -209 210 -239 240 -269 270 -299 300 -329 330 -359 >360
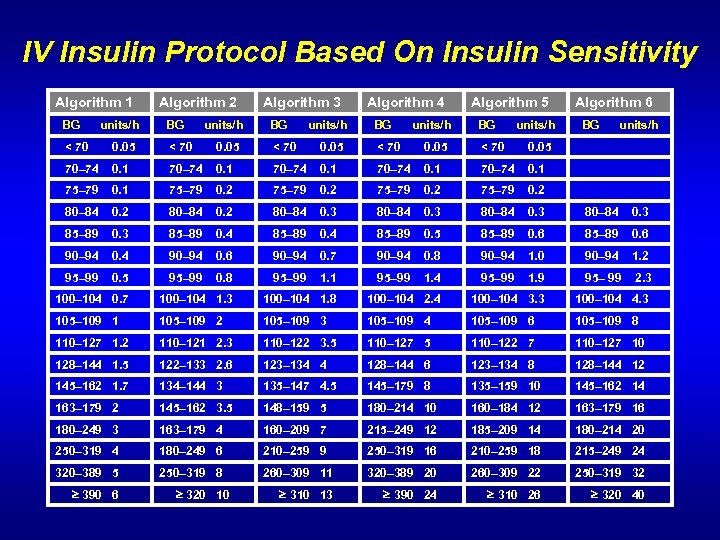 IV Insulin Protocol Based On Insulin Sensitivity Algorithm 1 Algorithm 2 Algorithm 3 Algorithm 4 Algorithm 5 Algorithm 6 BG units/h BG units/h < 70 0. 05 70– 74 0. 1 75– 79 0. 2 80– 84 0. 3 85– 89 0. 4 85– 89 0. 5 85– 89 0. 6 90– 94 0. 4 90– 94 0. 6 90– 94 0. 7 90– 94 0. 8 90– 94 1. 0 90– 94 1. 2 95– 99 0. 5 95– 99 0. 8 95– 99 1. 1 95– 99 1. 4 95– 99 1. 9 95– 99 2. 3 100– 104 0. 7 100– 104 1. 3 100– 104 1. 8 100– 104 2. 4 100– 104 3. 3 100– 104 4. 3 105– 109 1 105– 109 2 105– 109 3 105– 109 4 105– 109 6 105– 109 8 110– 127 1. 2 110– 121 2. 3 110– 122 3. 5 110– 127 5 110– 122 7 110– 127 10 128– 144 1. 5 122– 133 2. 6 123– 134 4 128– 144 6 123– 134 8 128– 144 12 145– 162 1. 7 134– 144 3 135– 147 4. 5 145– 179 8 135– 159 10 145– 162 14 163– 179 2 145– 162 3. 5 148– 159 5 180– 214 10 160– 184 12 163– 179 16 180– 249 3 163– 179 4 160– 209 7 215– 249 12 185– 209 14 180– 214 20 250– 319 4 180– 249 6 210– 259 9 250– 319 16 210– 259 18 215– 249 24 320– 389 5 250– 319 8 260– 309 11 320– 389 20 260– 309 22 250– 319 32 390 6 320 10 310 13 390 24 310 26 320 40
IV Insulin Protocol Based On Insulin Sensitivity Algorithm 1 Algorithm 2 Algorithm 3 Algorithm 4 Algorithm 5 Algorithm 6 BG units/h BG units/h < 70 0. 05 70– 74 0. 1 75– 79 0. 2 80– 84 0. 3 85– 89 0. 4 85– 89 0. 5 85– 89 0. 6 90– 94 0. 4 90– 94 0. 6 90– 94 0. 7 90– 94 0. 8 90– 94 1. 0 90– 94 1. 2 95– 99 0. 5 95– 99 0. 8 95– 99 1. 1 95– 99 1. 4 95– 99 1. 9 95– 99 2. 3 100– 104 0. 7 100– 104 1. 3 100– 104 1. 8 100– 104 2. 4 100– 104 3. 3 100– 104 4. 3 105– 109 1 105– 109 2 105– 109 3 105– 109 4 105– 109 6 105– 109 8 110– 127 1. 2 110– 121 2. 3 110– 122 3. 5 110– 127 5 110– 122 7 110– 127 10 128– 144 1. 5 122– 133 2. 6 123– 134 4 128– 144 6 123– 134 8 128– 144 12 145– 162 1. 7 134– 144 3 135– 147 4. 5 145– 179 8 135– 159 10 145– 162 14 163– 179 2 145– 162 3. 5 148– 159 5 180– 214 10 160– 184 12 163– 179 16 180– 249 3 163– 179 4 160– 209 7 215– 249 12 185– 209 14 180– 214 20 250– 319 4 180– 249 6 210– 259 9 250– 319 16 210– 259 18 215– 249 24 320– 389 5 250– 319 8 260– 309 11 320– 389 20 260– 309 22 250– 319 32 390 6 320 10 310 13 390 24 310 26 320 40
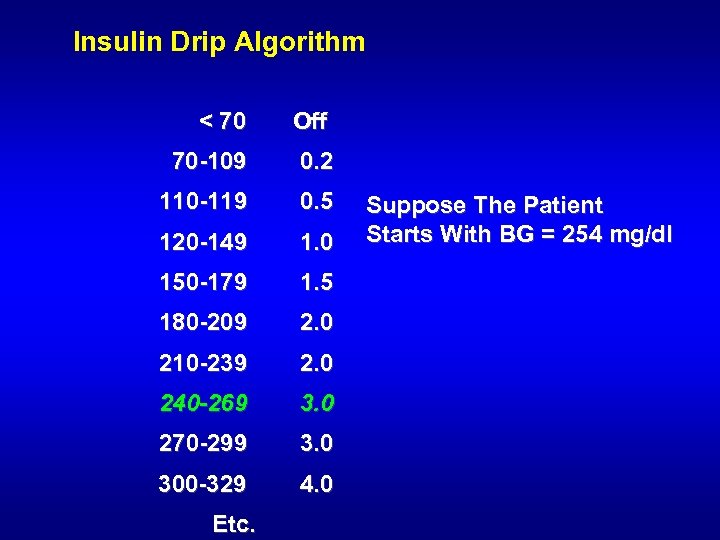 Insulin Drip Algorithm < 70 Off 70 -109 0. 2 110 -119 0. 5 120 -149 1. 0 150 -179 1. 5 180 -209 2. 0 210 -239 2. 0 240 -269 3. 0 270 -299 3. 0 300 -329 4. 0 Etc. Suppose The Patient Starts With BG = 254 mg/dl
Insulin Drip Algorithm < 70 Off 70 -109 0. 2 110 -119 0. 5 120 -149 1. 0 150 -179 1. 5 180 -209 2. 0 210 -239 2. 0 240 -269 3. 0 270 -299 3. 0 300 -329 4. 0 Etc. Suppose The Patient Starts With BG = 254 mg/dl
 Shifting Between Several Algorithms Makes It Possible To Discover The Insulin Requirement That Maintains Normoglycemia
Shifting Between Several Algorithms Makes It Possible To Discover The Insulin Requirement That Maintains Normoglycemia
 Recommended IV Fluids To Prevent Hypoglycemia, Hypokalemia & Ketosis: ü Glucose: 5 -10 gms/hour ü Potassium: 20 meq/L ü The Primary Service Should Choose the Type and the Rate of the Fluid Depending on the Underlying Disease
Recommended IV Fluids To Prevent Hypoglycemia, Hypokalemia & Ketosis: ü Glucose: 5 -10 gms/hour ü Potassium: 20 meq/L ü The Primary Service Should Choose the Type and the Rate of the Fluid Depending on the Underlying Disease
 Other Protocols Exist Ê DIGAMI (Studied In Acute MI Setting) Ê Van den Berghe (Critical Care Setting) Ê Portland Protocol (Surgical Setting) Ê Markovitz (Postoperative Heart Surgery) Ê Yale Protocol (Medical Intensive Care Setting) Ê Glucommander. com; Endotool. com; Medicaldecisions. com (Critical Care & Non. Critical Care)
Other Protocols Exist Ê DIGAMI (Studied In Acute MI Setting) Ê Van den Berghe (Critical Care Setting) Ê Portland Protocol (Surgical Setting) Ê Markovitz (Postoperative Heart Surgery) Ê Yale Protocol (Medical Intensive Care Setting) Ê Glucommander. com; Endotool. com; Medicaldecisions. com (Critical Care & Non. Critical Care)
 Life After The Drip…. Transition From IV to SQ Insulin In The Adult Patient
Life After The Drip…. Transition From IV to SQ Insulin In The Adult Patient
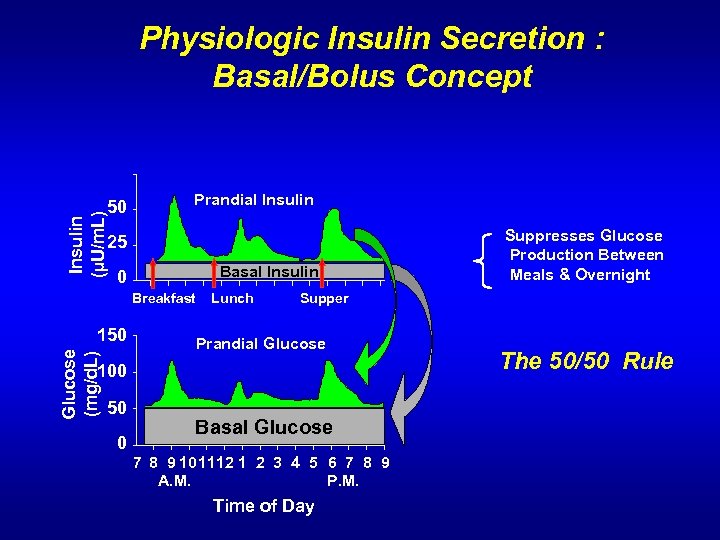 Physiologic Insulin Secretion : Basal/Bolus Concept Insulin (µU/m. L) 50 Prandial Insulin 25 0 Glucose (mg/d. L) 150 Basal Insulin Breakfast Lunch Supper Prandial Glucose 100 50 0 Suppresses Glucose Production Between Meals & Overnight Basal Glucose 7 8 9 101112 1 2 3 4 5 6 7 8 9 A. M. P. M. Time of Day The 50/50 Rule
Physiologic Insulin Secretion : Basal/Bolus Concept Insulin (µU/m. L) 50 Prandial Insulin 25 0 Glucose (mg/d. L) 150 Basal Insulin Breakfast Lunch Supper Prandial Glucose 100 50 0 Suppresses Glucose Production Between Meals & Overnight Basal Glucose 7 8 9 101112 1 2 3 4 5 6 7 8 9 A. M. P. M. Time of Day The 50/50 Rule
 Transition From IV to SQ Insulin In The Adult Patient ÊBasal Insulin ÊBolus Insulin üPrandial Insulin üCorrection Factor Insulin
Transition From IV to SQ Insulin In The Adult Patient ÊBasal Insulin ÊBolus Insulin üPrandial Insulin üCorrection Factor Insulin
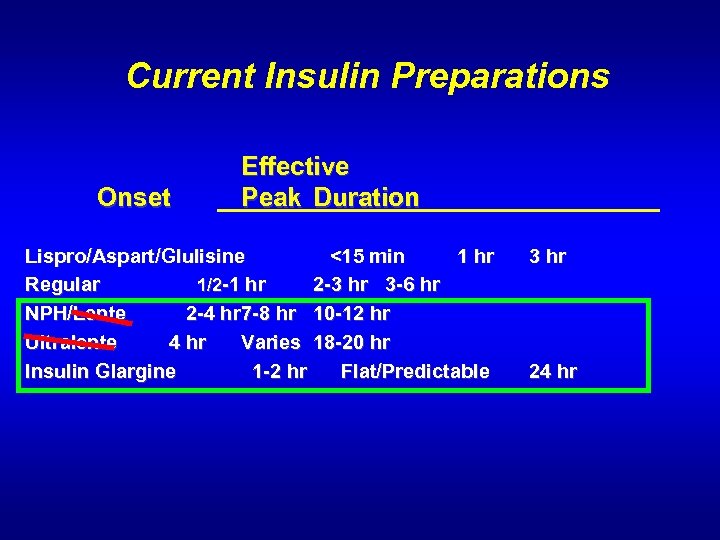 Current Insulin Preparations Onset Effective Peak Duration Lispro/Aspart/Glulisine <15 min 1 hr Regular 1/2 -1 hr 2 -3 hr 3 -6 hr NPH/Lente 2 -4 hr 7 -8 hr 10 -12 hr Ultralente 4 hr Varies 18 -20 hr Insulin Glargine 1 -2 hr Flat/Predictable 3 hr 24 hr
Current Insulin Preparations Onset Effective Peak Duration Lispro/Aspart/Glulisine <15 min 1 hr Regular 1/2 -1 hr 2 -3 hr 3 -6 hr NPH/Lente 2 -4 hr 7 -8 hr 10 -12 hr Ultralente 4 hr Varies 18 -20 hr Insulin Glargine 1 -2 hr Flat/Predictable 3 hr 24 hr
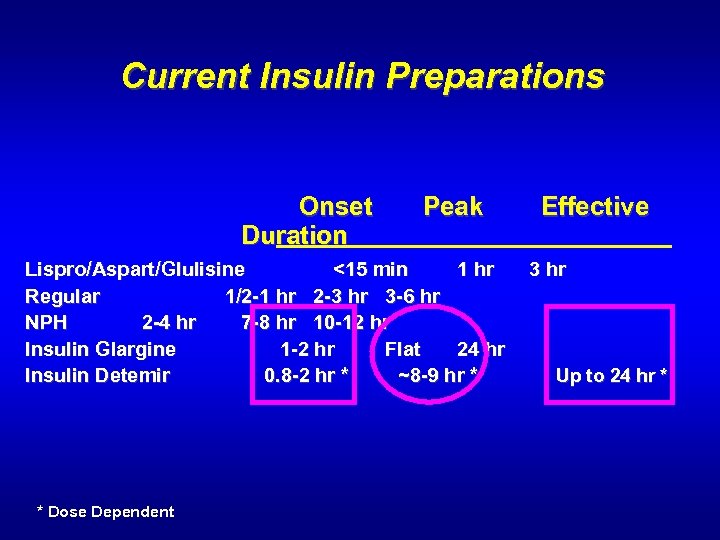 Current Insulin Preparations Onset Peak Effective Duration Lispro/Aspart/Glulisine <15 min 1 hr 3 hr Regular 1/2 -1 hr 2 -3 hr 3 -6 hr NPH 2 -4 hr 7 -8 hr 10 -12 hr Insulin Glargine 1 -2 hr Flat 24 hr Insulin Detemir 0. 8 -2 hr * ~8 -9 hr * Up to 24 hr * * Dose Dependent
Current Insulin Preparations Onset Peak Effective Duration Lispro/Aspart/Glulisine <15 min 1 hr 3 hr Regular 1/2 -1 hr 2 -3 hr 3 -6 hr NPH 2 -4 hr 7 -8 hr 10 -12 hr Insulin Glargine 1 -2 hr Flat 24 hr Insulin Detemir 0. 8 -2 hr * ~8 -9 hr * Up to 24 hr * * Dose Dependent
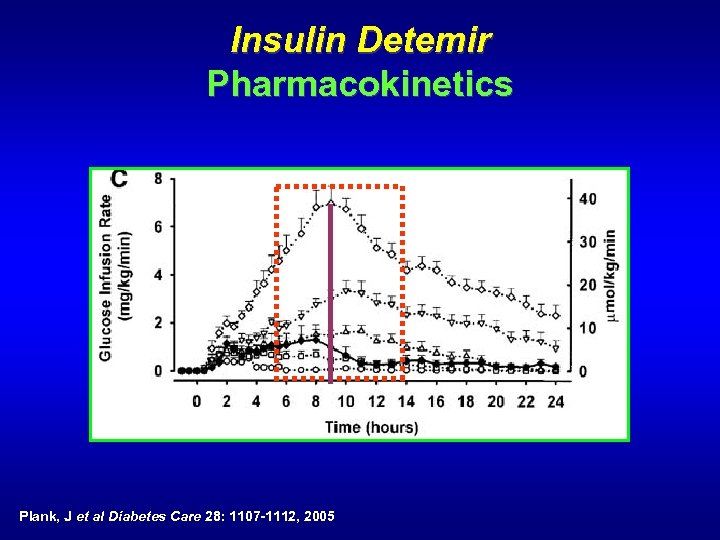 Insulin Detemir Pharmacokinetics Plank, J et al Diabetes Care 28: 1107 -1112, 2005
Insulin Detemir Pharmacokinetics Plank, J et al Diabetes Care 28: 1107 -1112, 2005
 Transition to SQ: An Approach To Transition A Patient From An IV Insulin Infusion To SQ Insulin: Multiply Last Drip Dose By 20, And Give This Amount As Glargine Turn The IV Drip Off 2 Hours Later
Transition to SQ: An Approach To Transition A Patient From An IV Insulin Infusion To SQ Insulin: Multiply Last Drip Dose By 20, And Give This Amount As Glargine Turn The IV Drip Off 2 Hours Later
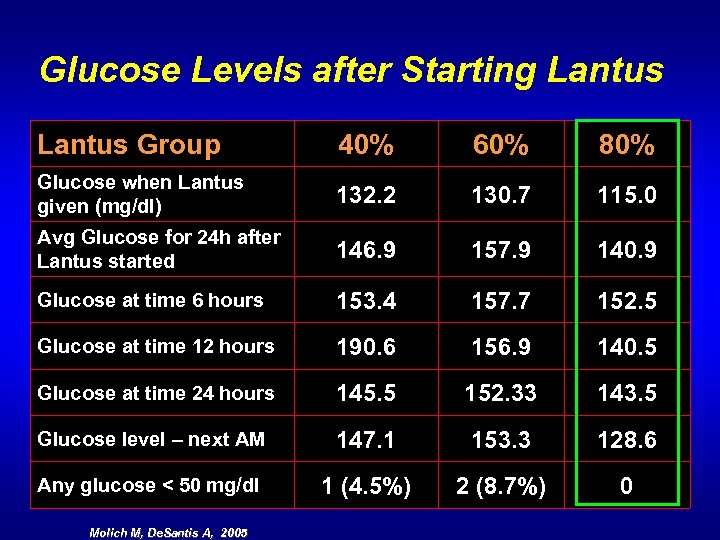 Glucose Levels after Starting Lantus Group 40% 60% 80% Glucose when Lantus given (mg/dl) 132. 2 130. 7 115. 0 Avg Glucose for 24 h after Lantus started 146. 9 157. 9 140. 9 Glucose at time 6 hours 153. 4 157. 7 152. 5 Glucose at time 12 hours 190. 6 156. 9 140. 5 Glucose at time 24 hours 145. 5 152. 33 143. 5 Glucose level – next AM 147. 1 153. 3 128. 6 Any glucose < 50 mg/dl 1 (4. 5%) 2 (8. 7%) 0 Molich M, De. Santis A, 2005
Glucose Levels after Starting Lantus Group 40% 60% 80% Glucose when Lantus given (mg/dl) 132. 2 130. 7 115. 0 Avg Glucose for 24 h after Lantus started 146. 9 157. 9 140. 9 Glucose at time 6 hours 153. 4 157. 7 152. 5 Glucose at time 12 hours 190. 6 156. 9 140. 5 Glucose at time 24 hours 145. 5 152. 33 143. 5 Glucose level – next AM 147. 1 153. 3 128. 6 Any glucose < 50 mg/dl 1 (4. 5%) 2 (8. 7%) 0 Molich M, De. Santis A, 2005
 Transition to SQ: An Approach To Transition A Patient From An IV Insulin Infusion To SQ Insulin: Multiply Last Drip Dose By 20, And Give This Amount As Glargine Turn The IV Drip Off 2 Hours Later
Transition to SQ: An Approach To Transition A Patient From An IV Insulin Infusion To SQ Insulin: Multiply Last Drip Dose By 20, And Give This Amount As Glargine Turn The IV Drip Off 2 Hours Later
 Transition to SQ: An Approach To Transition A Patient From An IV Insulin Infusion To SQ Insulin: Multiply Last Drip Dose By 20, And Give This Amount As Glargine Turn The IV Drip Off 2 Hours Later
Transition to SQ: An Approach To Transition A Patient From An IV Insulin Infusion To SQ Insulin: Multiply Last Drip Dose By 20, And Give This Amount As Glargine Turn The IV Drip Off 2 Hours Later
 g Example: Last Drip Dose Is 1. 5 Unit/Hour; Give 1. 5 X 20 = 30 units Of Glargine SQ; Discontinue Drip Two Hours Later This Is Basal Insulin
g Example: Last Drip Dose Is 1. 5 Unit/Hour; Give 1. 5 X 20 = 30 units Of Glargine SQ; Discontinue Drip Two Hours Later This Is Basal Insulin
 Adjust Basal Insulin By FBS: n Decrease 4 U if FBS are below 60 mg/d. L Decrease 2 U if FBS Is 60 -80 mg/d. L n If FBS Is 80 -100 mg/d. L, At Goal-No Change is Needed n n n Increase 2 U If FBS Is 100 to 120 mg/d. L Increase 4 U If FBS Is 121 to 140 mg/d. L Increase 6 U If FBS Is 141 to 160 mg/d. L Increase 8 U If FBS Is 161 to 180 mg/d. L Increase 10 U If FBS Is > 180 mg/d. L Or Adjust Based On Previous Days Correction Factor Doses
Adjust Basal Insulin By FBS: n Decrease 4 U if FBS are below 60 mg/d. L Decrease 2 U if FBS Is 60 -80 mg/d. L n If FBS Is 80 -100 mg/d. L, At Goal-No Change is Needed n n n Increase 2 U If FBS Is 100 to 120 mg/d. L Increase 4 U If FBS Is 121 to 140 mg/d. L Increase 6 U If FBS Is 141 to 160 mg/d. L Increase 8 U If FBS Is 161 to 180 mg/d. L Increase 10 U If FBS Is > 180 mg/d. L Or Adjust Based On Previous Days Correction Factor Doses
 Transition From IV to SQ Insulin In The Adult Patient ÊBasal Insulin ÊBolus Insulin üPrandial Insulin üCorrection Factor Insulin
Transition From IV to SQ Insulin In The Adult Patient ÊBasal Insulin ÊBolus Insulin üPrandial Insulin üCorrection Factor Insulin
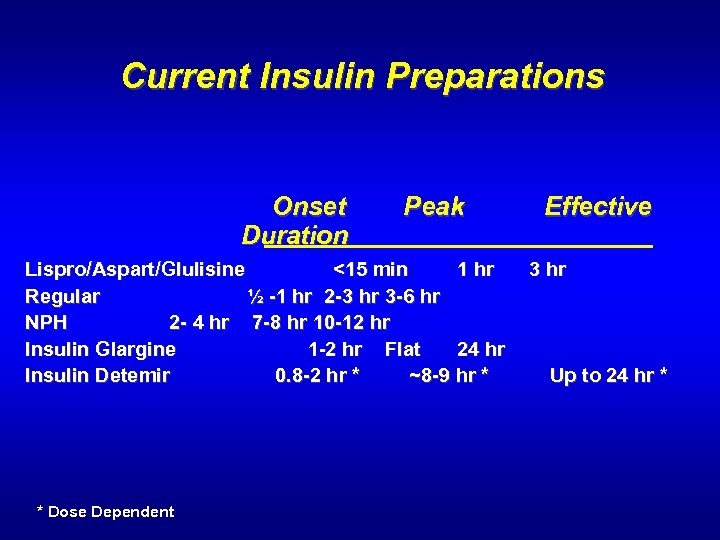 Current Insulin Preparations Onset Peak Effective Duration Lispro/Aspart/Glulisine <15 min 1 hr 3 hr Regular ½ -1 hr 2 -3 hr 3 -6 hr NPH 2 - 4 hr 7 -8 hr 10 -12 hr Insulin Glargine 1 -2 hr Flat 24 hr Insulin Detemir 0. 8 -2 hr * ~8 -9 hr * Up to 24 hr * * Dose Dependent
Current Insulin Preparations Onset Peak Effective Duration Lispro/Aspart/Glulisine <15 min 1 hr 3 hr Regular ½ -1 hr 2 -3 hr 3 -6 hr NPH 2 - 4 hr 7 -8 hr 10 -12 hr Insulin Glargine 1 -2 hr Flat 24 hr Insulin Detemir 0. 8 -2 hr * ~8 -9 hr * Up to 24 hr * * Dose Dependent
 When Patient Is Able To Eat, ü Add Rapid Acting Insulin For Mealtime Coverage ü Rule Of Thumb: 50% Basal 50% Prandial, Divided Over 3 Meals
When Patient Is Able To Eat, ü Add Rapid Acting Insulin For Mealtime Coverage ü Rule Of Thumb: 50% Basal 50% Prandial, Divided Over 3 Meals
 Example: Patient Is On 30 units Glargine Daily; Give 10 units With Each Meal Of Lispro (Humalog), Aspart (Novolog), Or Glulisine (Apidra) This Is Prandial Insulin
Example: Patient Is On 30 units Glargine Daily; Give 10 units With Each Meal Of Lispro (Humalog), Aspart (Novolog), Or Glulisine (Apidra) This Is Prandial Insulin
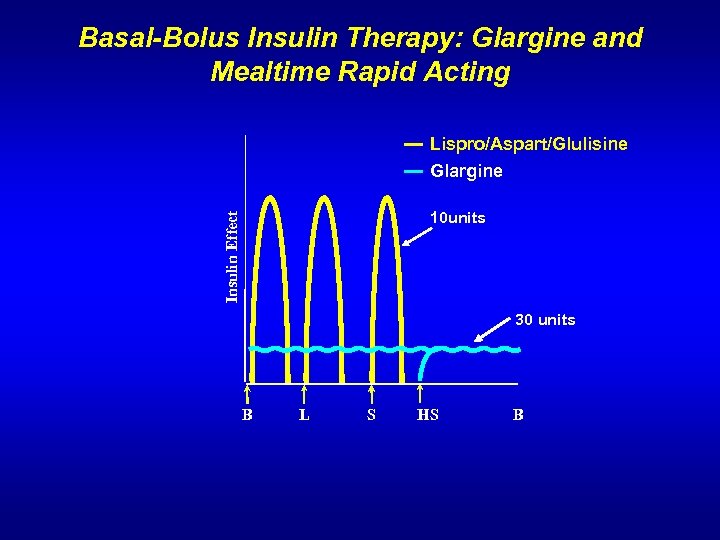 Basal-Bolus Insulin Therapy: Glargine and Mealtime Rapid Acting Lispro/Aspart/Glulisine Glargine Insulin Effect 10 units 30 units B L S HS B
Basal-Bolus Insulin Therapy: Glargine and Mealtime Rapid Acting Lispro/Aspart/Glulisine Glargine Insulin Effect 10 units 30 units B L S HS B
 Transition From IV to SQ Insulin In The Adult Patient ÊBasal Insulin ÊBolus Insulin üPrandial Insulin üCorrection Factor Insulin
Transition From IV to SQ Insulin In The Adult Patient ÊBasal Insulin ÊBolus Insulin üPrandial Insulin üCorrection Factor Insulin
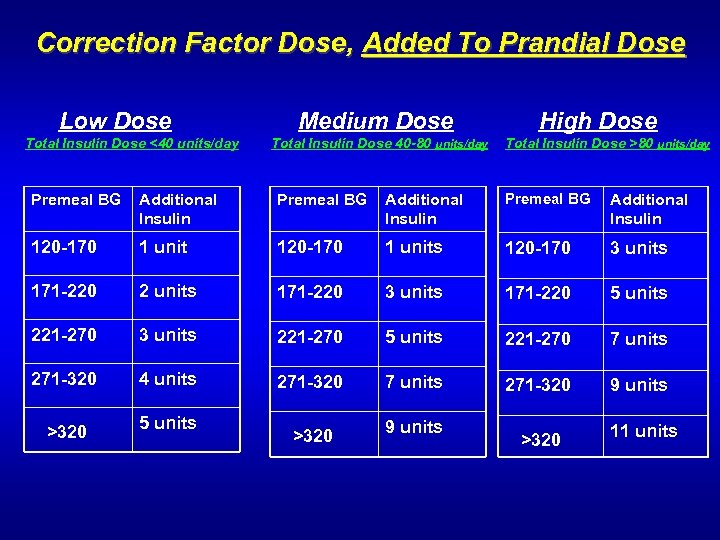 Correction Factor Dose, Added To Prandial Dose Low Dose Total Insulin Dose <40 units/day Medium Dose Total Insulin Dose 40 -80 units/day High Dose Total Insulin Dose >80 units/day Premeal BG Additional Premeal BG Insulin Premeal BG Additional Insulin Additional Insulin 120 -170 1 units 120 -170 3 units 171 -220 2 units 171 -220 3 units 171 -220 5 units 221 -270 3 units 221 -270 5 units 221 -270 7 units 271 -320 4 units 271 -320 7 units 271 -320 9 units >320 5 units >320 9 units >320 11 units
Correction Factor Dose, Added To Prandial Dose Low Dose Total Insulin Dose <40 units/day Medium Dose Total Insulin Dose 40 -80 units/day High Dose Total Insulin Dose >80 units/day Premeal BG Additional Premeal BG Insulin Premeal BG Additional Insulin Additional Insulin 120 -170 1 units 120 -170 3 units 171 -220 2 units 171 -220 3 units 171 -220 5 units 221 -270 3 units 221 -270 5 units 221 -270 7 units 271 -320 4 units 271 -320 7 units 271 -320 9 units >320 5 units >320 9 units >320 11 units
 What About Patients Admitted With Hyperglycemia On The Floor?
What About Patients Admitted With Hyperglycemia On The Floor?
 Sliding Scale Episodic Bolus Insulin WITHOUT Basal Insulin
Sliding Scale Episodic Bolus Insulin WITHOUT Basal Insulin
 Pitfalls of Sliding Scale Common Problems With SS Only Ê Ê Is Reactive Rather Than Proactive Often Mismatched With Changes In Patient’s Insulin Sensitivity It Does Not Meet The Physiologic Needs Of The Patient Leads To Insulin Stacking
Pitfalls of Sliding Scale Common Problems With SS Only Ê Ê Is Reactive Rather Than Proactive Often Mismatched With Changes In Patient’s Insulin Sensitivity It Does Not Meet The Physiologic Needs Of The Patient Leads To Insulin Stacking
 Starting Basal-Bolus From Scratch Calculate Starting Total Daily Dose (TDD) ü Previous Total Daily Insulin Units Used or ü 0. 4 units/kg (Type 1 DM) ü 0. 6 units/kg (New Onset Or Lean Type 2) ü 0. 8 units/kg (Type 2 DM) This Is Very Conservative and Actual Needs May Turn Out to Be Substantially More
Starting Basal-Bolus From Scratch Calculate Starting Total Daily Dose (TDD) ü Previous Total Daily Insulin Units Used or ü 0. 4 units/kg (Type 1 DM) ü 0. 6 units/kg (New Onset Or Lean Type 2) ü 0. 8 units/kg (Type 2 DM) This Is Very Conservative and Actual Needs May Turn Out to Be Substantially More
 NPH or Combination Insulin n n Discontinue this while an inpatient Disadvantages ü Insulin peaks ü Less reliable timing ü Variation in food intake ü Often poorer control n Conversion ü Add all doses of insulin total daily dose
NPH or Combination Insulin n n Discontinue this while an inpatient Disadvantages ü Insulin peaks ü Less reliable timing ü Variation in food intake ü Often poorer control n Conversion ü Add all doses of insulin total daily dose
 Starting Basal-Bolus From Scratch Basal Insulin = ½ TDD Give All of Calculated Glargine Dose Q 24 h Goal: FBS And Pre-Meal Glucose = 80 -110 mg/dl Bolus Doses = ½ TDD Prandial Dose + Correction Factor AFTER THE MEAL Goal: 2 h Post-Prandial <180 mg/dl
Starting Basal-Bolus From Scratch Basal Insulin = ½ TDD Give All of Calculated Glargine Dose Q 24 h Goal: FBS And Pre-Meal Glucose = 80 -110 mg/dl Bolus Doses = ½ TDD Prandial Dose + Correction Factor AFTER THE MEAL Goal: 2 h Post-Prandial <180 mg/dl
 Hypoglycemia: Most Frequent Causes ÊNot Lowering Insulin Dose For Decreased Caloric Intake ÊInterrupted Tube Feeding ÊUnrecognized Renal Insufficiency ÊSulfonylurea’s In Addition To Insulin Very Rare: Ê Adrenal Insufficiency & Drugs
Hypoglycemia: Most Frequent Causes ÊNot Lowering Insulin Dose For Decreased Caloric Intake ÊInterrupted Tube Feeding ÊUnrecognized Renal Insufficiency ÊSulfonylurea’s In Addition To Insulin Very Rare: Ê Adrenal Insufficiency & Drugs
 A Word About Oral Agents….
A Word About Oral Agents….
 Therapy of Type 2 Diabetes Mellitus: Hospital Use of Oral Agents Secretagogues Not for Acute Illness With Variable Intake Glucosidase Inhibitors Not for Acute Illness With Variable Intake Metformin Glitazones Hold for Acute Illness If Renal, Cardiac, or Liver Function Unstable, or Surgery, or Radiocontrast Can Give or Not
Therapy of Type 2 Diabetes Mellitus: Hospital Use of Oral Agents Secretagogues Not for Acute Illness With Variable Intake Glucosidase Inhibitors Not for Acute Illness With Variable Intake Metformin Glitazones Hold for Acute Illness If Renal, Cardiac, or Liver Function Unstable, or Surgery, or Radiocontrast Can Give or Not
 Common Errors in Glucose Management in Hospital Patients ü Discontinuing All Diabetes Medicines On Admission (Some Pills Must Be Stopped) ü Setting High Glycemic Targets (>200 mg/d. L) ü Not Changing Therapy With The Situation Or The Glucose Profile ü Overutilization Of Sliding Scale Insulin ü Underutilization Of Insulin Infusions and Basal Insulin Metchick LN. Am J Med 2002; 113: 317
Common Errors in Glucose Management in Hospital Patients ü Discontinuing All Diabetes Medicines On Admission (Some Pills Must Be Stopped) ü Setting High Glycemic Targets (>200 mg/d. L) ü Not Changing Therapy With The Situation Or The Glucose Profile ü Overutilization Of Sliding Scale Insulin ü Underutilization Of Insulin Infusions and Basal Insulin Metchick LN. Am J Med 2002; 113: 317
 Have A Discharge Plan
Have A Discharge Plan
 Can A Patient Go Back To Oral Agents At Discharge? n Admission Hb. A 1 C Very Helpful
Can A Patient Go Back To Oral Agents At Discharge? n Admission Hb. A 1 C Very Helpful
 Can A Patient Go Back To Oral Agents At Discharge? n n n Admission Hb. A 1 C Very Helpful If Known Diabetic and Pre-Admission Control Acceptable YES!!! If > 7. 5% on Maximum Oral Agents, Needs Basal Insulin
Can A Patient Go Back To Oral Agents At Discharge? n n n Admission Hb. A 1 C Very Helpful If Known Diabetic and Pre-Admission Control Acceptable YES!!! If > 7. 5% on Maximum Oral Agents, Needs Basal Insulin
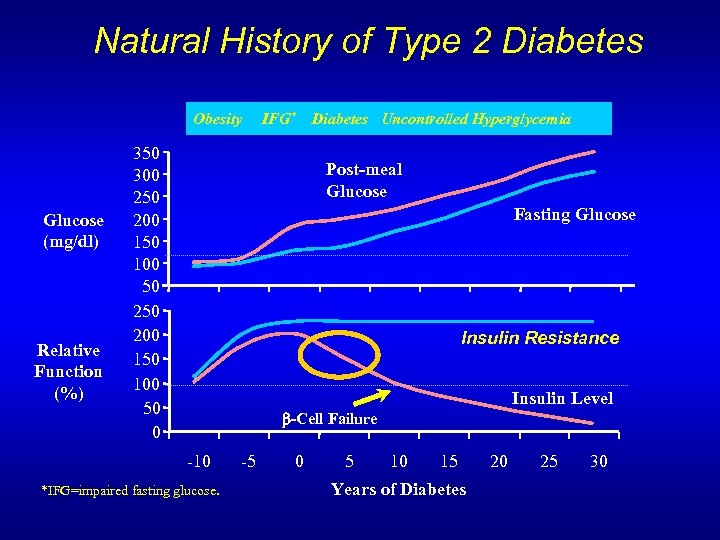 Natural History of Type 2 Diabetes Obesity Glucose (mg/dl) Relative Function (%) 350 300 250 200 150 100 50 0 IFG* Diabetes Uncontrolled Hyperglycemia Post-meal Glucose Fasting Glucose Insulin Resistance Insulin Level -Cell Failure -10 *IFG=impaired fasting glucose. -5 0 5 10 15 Years of Diabetes 20 25 30
Natural History of Type 2 Diabetes Obesity Glucose (mg/dl) Relative Function (%) 350 300 250 200 150 100 50 0 IFG* Diabetes Uncontrolled Hyperglycemia Post-meal Glucose Fasting Glucose Insulin Resistance Insulin Level -Cell Failure -10 *IFG=impaired fasting glucose. -5 0 5 10 15 Years of Diabetes 20 25 30
 Glycemic Management Teams: ü Review Scheduled Insulin Orders ü Examine Bedside Glucose Levels To Assess Recent Responses To Treatment ü Use These Responses To Revise Insulin Orders
Glycemic Management Teams: ü Review Scheduled Insulin Orders ü Examine Bedside Glucose Levels To Assess Recent Responses To Treatment ü Use These Responses To Revise Insulin Orders
 Glycemic Management Teams: ü Mild Hypoglycemia Adjust Downward, Especially Rapid-Acting Analogue ü Review Notes For Unusual Occurrences, i. e. , Late Insulin, Decreased Caloric Intake, Physical Activity, Hypoglycemia Treatment ü Provide Education/Inservice For Nurses, Provide Pharmacists, Physicians & Physician Assistants ü Code and Bill Appropriately
Glycemic Management Teams: ü Mild Hypoglycemia Adjust Downward, Especially Rapid-Acting Analogue ü Review Notes For Unusual Occurrences, i. e. , Late Insulin, Decreased Caloric Intake, Physical Activity, Hypoglycemia Treatment ü Provide Education/Inservice For Nurses, Provide Pharmacists, Physicians & Physician Assistants ü Code and Bill Appropriately
 Inpatient Diabetes Management: Is Cost a Barrier? Use of a Diabetes Management Team: Ê Reduction in LOS Ê Cost Reduction of $2353/ Patient Ê MICU: Annual Savings $40, 000/ ICU Bed Ê SICU: Savings $3, 000/Patient Inpatient Diabetes and Glycemic Control: A Call To Action Feb 7, 2006
Inpatient Diabetes Management: Is Cost a Barrier? Use of a Diabetes Management Team: Ê Reduction in LOS Ê Cost Reduction of $2353/ Patient Ê MICU: Annual Savings $40, 000/ ICU Bed Ê SICU: Savings $3, 000/Patient Inpatient Diabetes and Glycemic Control: A Call To Action Feb 7, 2006
 Hospital Diabetic Management: ü Medical Benefits Unequivocal ü Few Studies Address Optimal Method ü Principles Borrowed From Outpatient Management ü Insulin Strategy Should Be Physiologic Ê All Regimens Must Include Adequate Basal Insulin Ê Prandial and Correction Factor ü Team Approach Essential ü Financial Incentives
Hospital Diabetic Management: ü Medical Benefits Unequivocal ü Few Studies Address Optimal Method ü Principles Borrowed From Outpatient Management ü Insulin Strategy Should Be Physiologic Ê All Regimens Must Include Adequate Basal Insulin Ê Prandial and Correction Factor ü Team Approach Essential ü Financial Incentives


