270df75b88f2221de518b40ba737318e.ppt
- Количество слайдов: 78


Gestational Trophoblastic Neoplasia (GTN) Zohreh Yousefi Professor of Obstetrics and Gynecology, Fellowship of Gynecology Oncology , Ghaem Hospital, website: www. zohrehyousefi. com

Danforth's Williams Obstetrics, 23 e B erek and Hacker's Gynecologic Oncology Up To Dat GESTATIONAL TROPHOBLASTIC DISEASE PATHOGENESIS DIAGNOSIS MANAGEMENT GESTATIONAL TROPHOBLASTIC NEOPLASIA TREATMENT SUBSEQUENT PREGNANCY

Gestational trophoblastic disease (GTD) is term group of tumors with abnormal trophoblast proliferation produce human chorionic gonadotropin (h. CG)

GTD histologically is divided into benign hydatidiform moles ( complete and partial) Malignant Invasive mole
Non -molar trophoblastic neoplasms • Choriocarcinoma • Placental site trophoblastic tumor • Epithelioid trophoblastic tumor

Gestational trophoblastic neoplasia (GTN ) Malignant forms of gestational trophoblastic disease GT N is all GTD except hydatidiform mole Weeks or years following any type of pregnancy But frequently occur after a hydatidiform mole

Hydatidiform mole Microscopic (classic findings) Absence embryonic elements Trophoblastic proliferation (cytotrophoblast and syncytiotrophoblast) Stromal edema and hydropic degeneration Absence of blood vessels

Macroscopic of Hydatidiform mole Hydropic villi Grapelike vesicles filled clear material usually 1 to 3 cm diameter proliferation of the trophoblast

Hydatidiform mole Complete mole Partial mole Partial mol ( fetal tissue) Grossly placenta a mixture of normal and hydropic villi Fetus Severe growth restriction Multiple congenital anomalies

Risk Factors hydatidiform mole Strongest risk factors are Age and a history of prior hydatidiform mole Both extremes of reproductive age adolescents twofold risk Older than 40 tenfold risk

• • history of Prior mole the risk of another mole Complete mole is 1. 5 percent Partial mole is 2. 7 percent • Two prior molar pregnancies • the risk is 23 percent

• • • An ethnic predisposition Diet (Deficiencies of protein or) (Vitamin A deficiency) animal fat Smoking Increased paternal age
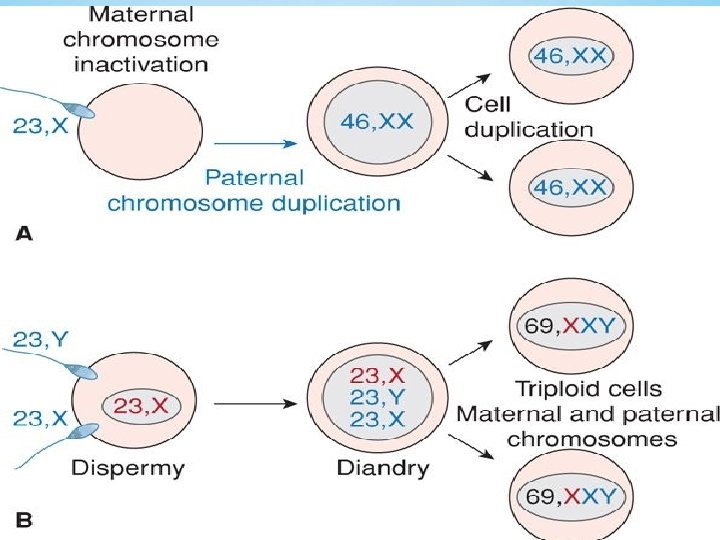
Pathogenesis Abnormal fertilization process Normal ovum with a duplicated haploid sperm Inactive ovum chromosomes Karyotype 46, XX diploid and result from androgenesis Partial moles triploid karyotype 69, XXX, 69, XXY

Clinical Findings Because universal sonography in prenatal care Typically diagnosed at a mean of 10 weeks • Vaginal bleeding • spotting to profuse hemorrhage • Moderate iron-deficiency anemia

• Exaggerated early pregnancy symptoms • Nausea and vomiting ( hyperemesis) • Abdominal cramp

Abnormally enlarged and soft uterus uterine growth Theca-lutein cysts (h. CG) 25 to 60% (Torsion, infarction, rupture and hemorrhage) Releases antiangiogenic factors that activate endothelial damage Severe preeclampsia hypoxic trophoblastic mass

All hydatidiform moles secrete h. CG Thyrotrophic -like effects of h. CG acts a thyrotrophic substance Elevated serum free thyroxine (T 4) (TSH) levels to be decreased thyroid hyper –function “thyroid storm”
Diagnosis Amenorrhea followed by irregular bleeding Spontaneous passage of molar tissue High values Serum β-HCG measurement confirming the diagnosis IHC stain positively for p 57

Sonography Echogenic uterine mass with anechoic cystic spaces without a fetus or amnionic sac The appearance as “snowstorm
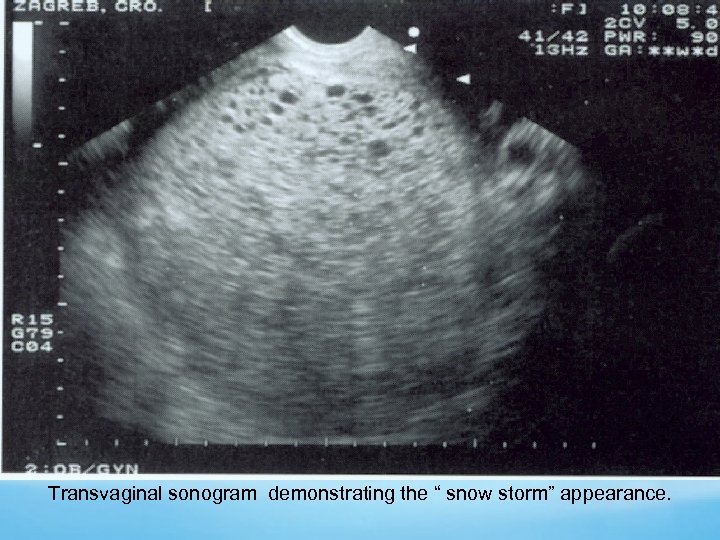
Transvaginal sonogram demonstrating the “ snow storm” appearance.

Mis-diagnosis • • Incomplete abortion missed abortion Cystic degeneration uterine leiomyoma

• which of the following symptoms will a highly intelligent physician assistant immediately consider hydatidiform mole? – pelvic pain at night during the first trimester – significantly elevated BP in the first trimester – significant bloody vaginal discharge in the first trimester – nausea and vomiting in the first trimester

• Answer is B

Management Termination of Molar Pregnancy • Evacuation and Curettage • Hysterectomy (rarely and select cases • no desired future pregnancy ) • Chest radiograph • Initiate effective contraception • OCP or MPA } poor compliance}

Serum h. CG levels: 48 hours of evacuation (baseline) Weekly until undetectable Weekly until normal for 3 consecutive weeks monthly until normal for at least 6 consecutive months Median time for resolution is 9 weeks for complete 7 weeks for partial Hysterectomy reduces the incidence of malignant sequelae does not eliminate follow-up

h. CG change HM: 84 -100 days Spontaneous abortion: 19 days Normal delivery: 12 days Ectopic pregnancy 8 -9 days

After molar evacuation risk factors for malignant squeal 15 - 20 % complete moles 1 - 5 % partial moles 1 5% of HM become invasion moles 2. 5% progress into choriocarcinoma

Twin Pregnancy (Normal Fetus and Coexistent Complete Mole) Diagnosis is difficult (early pregnancy ultrasound) A single partial molar pregnancy with abnormal fetus Distinguished

A few cases the diagnosis is not suspected until examination of the placenta following delivery

Amniocentesis ( fetal karyotype ) diploid or triploid If fetal karyotype is normal Major fetal malformations are excluded by ultrasound Chest X-ray performed Serum h. CG values If there is no evidence of metastatic disease to allow the pregnancy

Possible risk for developing • • Subsequent GTN Preterm delivery Preeclampsia Sever hemorrhage

Persistent GTD : Persistently elevated serum h. CG level Irregular vaginal bleeding Persistent theca lute in cysts (2 to 4 months regress spontaneously) Uterine sub involution Risk factors for GTN

Risk factors of GTN Older age β-h. CG levels > 100, 000 m. IU/m. L Large uterine size for-gestational age Theca-lutein cysts > 6 cm Earlier recognition and evacuation of molar pregnancies not lower risk neoplasia

Criteria for Diagnosis of Gestational Trophoblastic Neoplasia Criteria for the diagnosis of postmolar GTN 1. Plateau or rise of serum β-h. CG level 2. Detectable serum β-h. CG level for 6 months or more 3. Histological criteria for choriocarcinoma 4 -Irregular bleeding , uterine sub involution

Plateau of serum β-h. CG level (± 10 percent) for four easurements during a period of 3 weeks or longer days 1, 7, 14, 21 Rise of serum β-h. CG level > 10 percent during three weekly consecutive , during a period of 2 weeks or more—days 1, 7, 14 •

Diagnosis Sonography Abdomino pelvic or trans vaginal sonography Radiograph of chest CT scan Brain CT scan or MRI

SPESIAL 1 -Selective angiography of abdominal and pelvic or hepatic (if indicated ) 2 -Whole body PET Less commonly (occult disease ) 3 -Stool guaiac tests If positive test is or if gastrointestinal symptoms be routinely performed in persistent GTN 4 - complete radiographic evaluation of the gastrointestinal tract

GTN CLASSIFICATION Invasive Mole Almost all invasive moles arise from partial or complete moles Deep penetration into the myometrium or peritoneum Involvement of vaginal vault
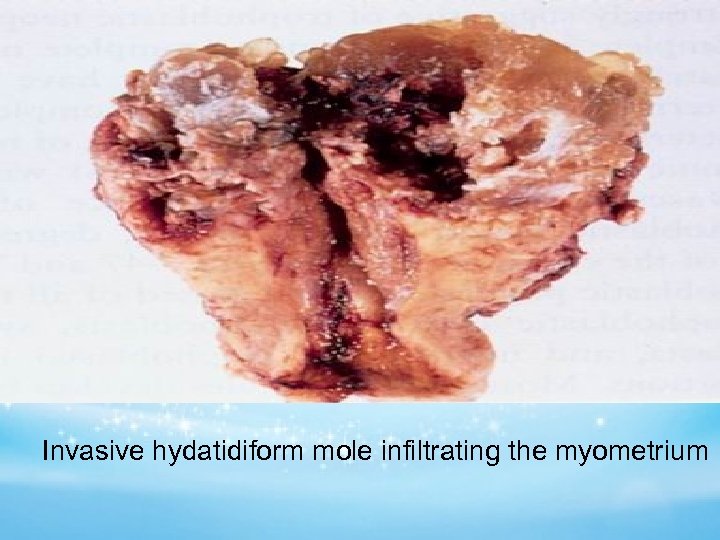
Invasive hydatidiform mole infiltrating the myometrium

Choriocarcinoma Most common follow a term pregnancy or miscarriage Rapidly growing both myometrium and blood vessels Blood-borne metastases

differentiation between invasive mole and choriocarcinoma if we see villi, it must be invasion mole if we can’t see villi, it is choriocarcinoma

Common Sites for Metastatic Gestational Trophoblastic Tumors Site Lung Vagina Vulva/cervix Brain Liver Kidney Spleen Gastrointestinal Per cent 60 -95 40 -50 10 -15 5 -15 0 -5 0 -5

Symptoms • Metastatic symptoms • Profuse vaginal bleeding • Vaginal or cervical metastasis • (bluish nodule in vaginal) • Abdominal pain (intra-abdominal hemorrhage) • Cough, hemoptysis • Headache, nausea, vomit, paralysis or coma • Urologic hemorrhage

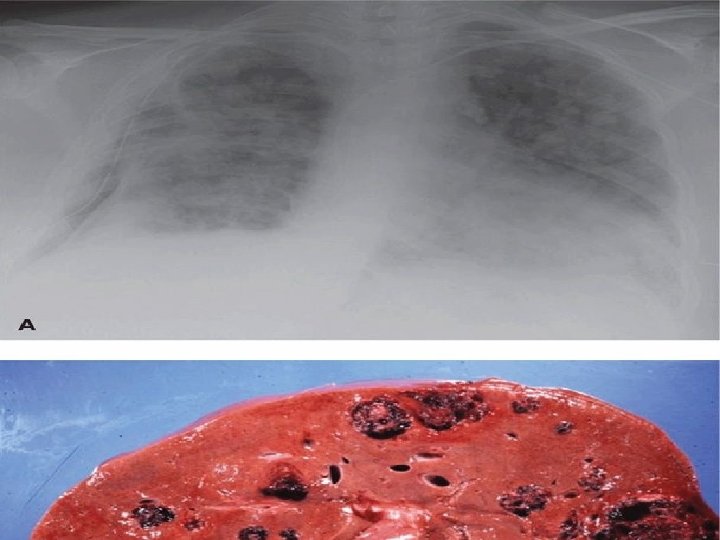
Lung metastasis Four principal pulmunary radiologic patterns: • Snowstorm pattern (Alveolar pattern ) • Discrete rounded densities • Plural effusion • Embolic pattern

Brain metastasis • • • Plasma CSF /h. CG level ratio is normally >60: 1 In patients with CNS metastases <60: 1 Falsely lowered plasma CSF /h. CG level First -trimester abortions In the absence of lung or vaginal metastasis Risk of cerebral and hepatic spread is exceedingly low

Generally in GTN Serum h. CG levels combined Clinical findings Rather than a histological specimen Diagnose and treat this malignancy

Follow-up of GTN patients β-subunit until h. CG Weekly until normal for 3 consecutive weeks monthly until normal for at least 3 consecutive months at 1 -month interval for 1 year: at 1 - month interval for 2 years in high stage at yearly interval for many years (increased risk of late recurrence)

• Be careful : • h. CG • Pelvic examination • Chest X-ray unusual rise of serum h. CG • Rule out Normal pregnancy • Ectopic pregnancy • False-Positive h. CG

• False-Positive h. CG: • Quiescent GTN • Phantom h. CG • Pituitary h. CG • Non-gynecologic tumors secreted -h. CG

Quiescent GTN Constant, low level of h. CG <100 IU/L Without evidence of a primary or metastatic malignancy Persisting for periods 3 months to 16 years Slow-growing Oral contraceptive pills and avoid pregnancy until h. CG has been undetectable for six months 20 percent will eventually have recurrent active

H CG variants Hyperglycosylated h. CG (H -h. CG) h. CG produced by syncytiotrophoblasts (H -h. CG) synthesized by cytotrophoblast (H -h. CG) absolute marker of ongoing invasion h. CG-H is detectable >1 ng/ml: active GTN To discriminate quiescent disease

Phantom h. CG False positive serum h. CG Send the serum to two laboratories Using different commercial assays If negative in one or both false positive h. CG Presence of h. CG in serum but not urine

Heterothallic antibodies may results false-positive False positive are at risk for recurrent Risk for other false positives, such as CA-125 and thyroid antibodies

Pituitary h. CG Secreted LH and h. CG pulsatile and paralleled Higher levels of h CG in postmenopausal than premenopausal Cross-reactivity with LH Pituitary production h. CG ranges from 1 to 32 m. IU/m. L HRT or BSO or OCP after 2– 3 weeks Suppress h. CG Pituitary production

Staging of GTN WHO Scoring System

Staging International staging of WHO may be summarized as follows: Ⅰ: lesion localized in uterus, no metastasis; Ⅱ: lesion extends beyond uterus, but still confined to internal genitalias; Ⅲ: pulmonary lesion Ⅳ: metastasis to other distant sites.
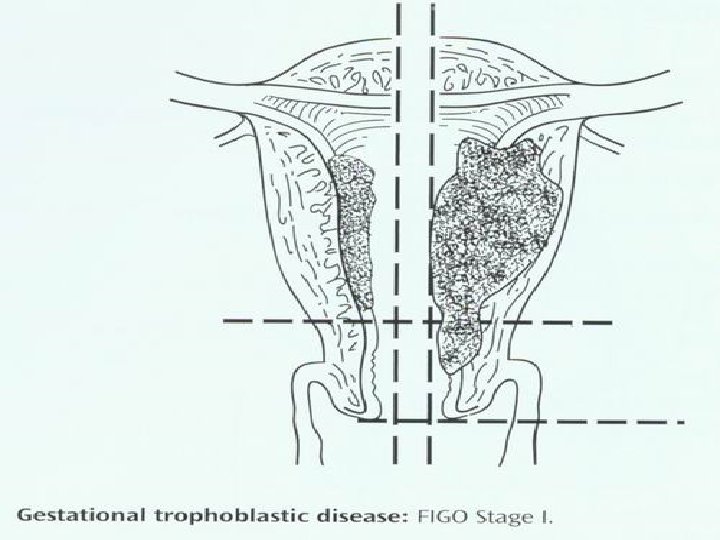
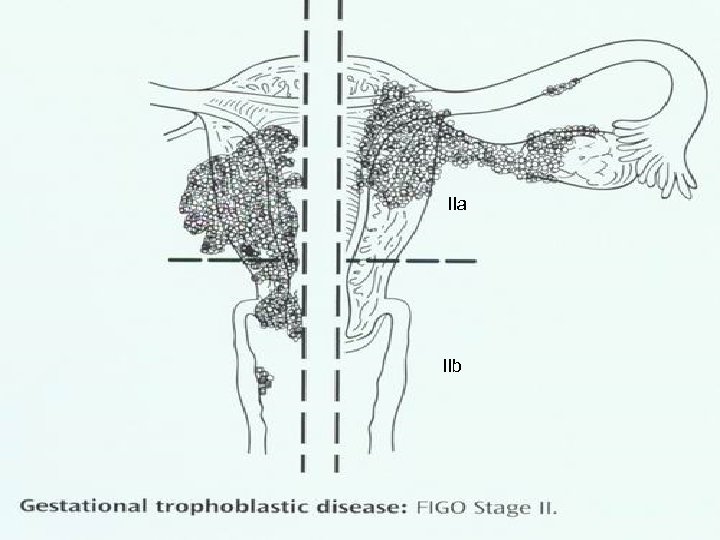
IIa IIb
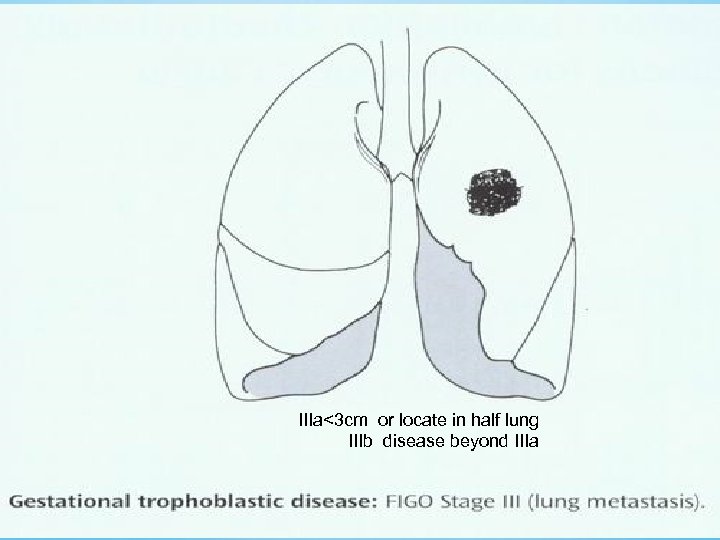
IIIa<3 cm or locate in half lung IIIb disease beyond IIIa
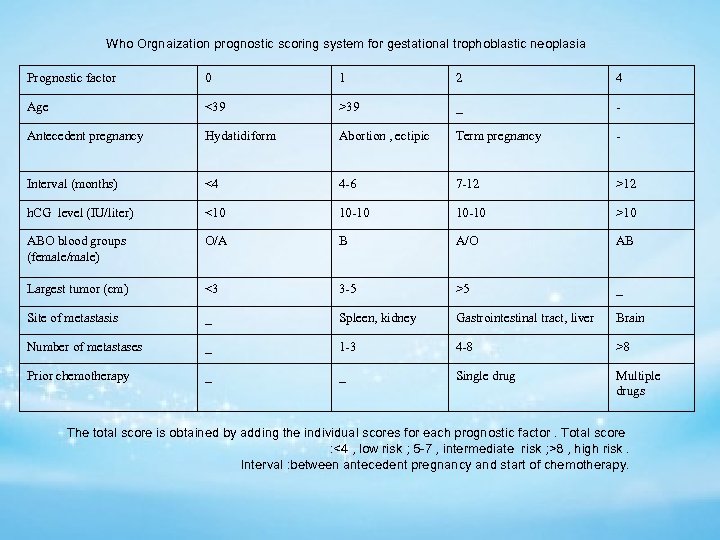
Who Orgnaization prognostic scoring system for gestational trophoblastic neoplasia Prognostic factor 0 1 2 4 Age <39 >39 _ - Antecedent pregnancy Hydatidiform Abortion , ectipic Term pregnancy - Interval (months) <4 4 -6 7 -12 >12 h. CG level (IU/liter) <10 10 -10 >10 ABO blood groups (female/male) O/A B A/O AB Largest tumor (cm) <3 3 -5 >5 _ Site of metastasis _ Spleen, kidney Gastrointestinal tract, liver Brain Number of metastases _ 1 -3 4 -8 >8 Prior chemotherapy _ _ Single drug Multiple drugs The total score is obtained by adding the individual scores for each prognostic factor. Total score : <4 , low risk ; 5 -7 , intermediate risk ; >8 , high risk. Interval : between antecedent pregnancy and start of chemotherapy.

• According to the FIGO staging of gestational trophoblastic tumors • a lady with choriocarcinoma having • lung metastasis will belong to which stage

protocol for treatment of GTD Clinically staging( FIGO) WHO scoring Again, it is stressed that the diagnosis of GTN made by persistently elevated serum β-h. CG without confirmation by pathological tissue study
Choice of treatment • Chemotherapy ( highly sensitive ) • Surgery ( unresponsive or drug fails ) • Irradiation (brain and liver )

Chemotherapy are best management Protocols: Single-agent for low-risk Methotrexate Combination for high-risk disease EMA -CO Early-stage GTN is typically cured Later -stage disease usually responds to chemotherapy

Surgery in malignant GTN • • • Hysterectomy Laparoscopy Craniotomy (brain hemorrhage) Thoracotomy (solitary nodules in drug-resistant disease ) selective resection of lesion in uterus or liver

Main causes of death: • Hemorrhage • Infection • Metastasis

Placental Site Trophoblastic Tumor (PSST) PSTT or non-trophoblastic malignancy Uncommon tumor arises from implantation siteintermediate trophoblast Secrete (h. PL) from intermediate cells Relatively small amounts of h. CG free β-subunit is more than one third of h. CG (30%)

Typically local myometrial invasion Rare systemic metastases Treatment of ( PSST) is preferred hysterectomy Because resistant to chemotherapy For higher-risk than stage I combination chemotherapy given

Epithelioid Trophoblastic Tumor This rare tumor Intermediate trophoblast -type Grossly a nodular fashion Primary treatment is hysterectomy Relatively resistant to chemotherapy Approximately a fourth this neoplasm will have metastatic disease, combination chemotherapy

SUBSEQUENT PREGNANCY Pregnancy outcomes are usually normal May develop: 1 -Repeat molar gestation 2 -percent 2 -Spontaneous abortions 3 -Congenital anomalies 4 -Ovarian failure (chemotherapy) 5 -Secondary tumors including leukemia colon cancer, melanoma and breast cancer


After Termination of Subsequent Pregnancy Sonographic evaluation in early pregnancy pathological evaluation placenta after delivery serum β-h. CG level is measured 6 weeks postpartum

Conclusion The possibility of metastatic GTN should be considered In any woman of the reproductive age Presenting with metastatic disease Or an unknown primary site of malignancy

www. zohrehyousefi. com
270df75b88f2221de518b40ba737318e.ppt