3a1cb558ada7e0e2513611129b497a84.ppt
- Количество слайдов: 43
 Gene-Environment Interactions International Society for Nurses in Genetics May 2007 Jan Dorman, Ph. D University of Pittsburgh, PA, USA
Gene-Environment Interactions International Society for Nurses in Genetics May 2007 Jan Dorman, Ph. D University of Pittsburgh, PA, USA
 Objectives n Identify gene-environment interactions n Determine if the interaction follows an additive or multiplicative model n Assess the importance of the interaction for clinical practice n Apply ACMG guidelines for genetic testing for Factor V Leiden mutations and followup
Objectives n Identify gene-environment interactions n Determine if the interaction follows an additive or multiplicative model n Assess the importance of the interaction for clinical practice n Apply ACMG guidelines for genetic testing for Factor V Leiden mutations and followup
 Evidence of Gene-Environment Interactions n Familial aggregation of disease – Greater prevalence of disease in 1 st degree relatives vs. spouses – Higher disease concordance among MZ vs. DZ twins – Earlier age at onset among familial vs. non-familial cases – Stronger phenotypic correlations between parents and biologic vs. adopted children
Evidence of Gene-Environment Interactions n Familial aggregation of disease – Greater prevalence of disease in 1 st degree relatives vs. spouses – Higher disease concordance among MZ vs. DZ twins – Earlier age at onset among familial vs. non-familial cases – Stronger phenotypic correlations between parents and biologic vs. adopted children
 Evidence of Gene-Environment Interactions n International studies – Geographic variation in rates of disease – Temporal trends worldwide – Higher disease incidence among immigrants vs. source population • Age differences in risk depending on age at migration
Evidence of Gene-Environment Interactions n International studies – Geographic variation in rates of disease – Temporal trends worldwide – Higher disease incidence among immigrants vs. source population • Age differences in risk depending on age at migration
 Example: Multiple Sclerosis n Incidence is higher in countries far from the equator – High risk countries • US, Canada, Northern Europe – Low risk countries • Southern Europe, SE Asia, Africa
Example: Multiple Sclerosis n Incidence is higher in countries far from the equator – High risk countries • US, Canada, Northern Europe – Low risk countries • Southern Europe, SE Asia, Africa
 Incidence of MS per 100, 000 / yr Among Immigrants to Israel Age at Migration Source Population European Asian/African < 15 yrs 0. 76 0. 65 15 -29 yrs 3. 54 0. 40 30 -34 yrs 1. 35 0. 26 Gordis, 1996
Incidence of MS per 100, 000 / yr Among Immigrants to Israel Age at Migration Source Population European Asian/African < 15 yrs 0. 76 0. 65 15 -29 yrs 3. 54 0. 40 30 -34 yrs 1. 35 0. 26 Gordis, 1996
 Gene-Environment Interactions n Often tested in case control studies n Require careful definitions of n Stratify cases and controls – Disorder (phenotype) – Environmental risk factors – High-risk genotypes (genetic susceptibility) – Susceptible • With / without exposure – Not susceptible • With / without exposure
Gene-Environment Interactions n Often tested in case control studies n Require careful definitions of n Stratify cases and controls – Disorder (phenotype) – Environmental risk factors – High-risk genotypes (genetic susceptibility) – Susceptible • With / without exposure – Not susceptible • With / without exposure
 Gene-Environment Interactions n Occur when the risk of disease in exposed and susceptible individuals differs from that expected based on their individual effects – Expected effects can be additive or multiplicative n Positive interaction n Negative interaction – Synergistic – Antagonistic
Gene-Environment Interactions n Occur when the risk of disease in exposed and susceptible individuals differs from that expected based on their individual effects – Expected effects can be additive or multiplicative n Positive interaction n Negative interaction – Synergistic – Antagonistic
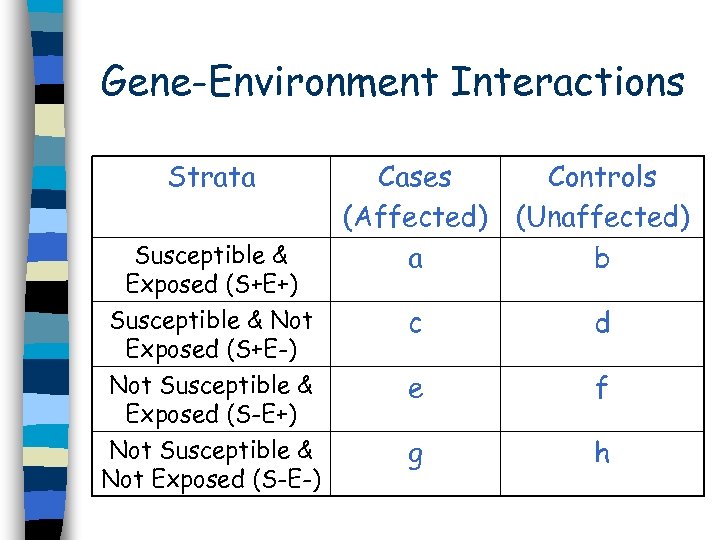 Gene-Environment Interactions Strata Susceptible & Exposed (S+E+) Susceptible & Not Exposed (S+E-) Not Susceptible & Exposed (S-E+) Not Susceptible & Not Exposed (S-E-) Cases (Affected) a Controls (Unaffected) b c d e f g h
Gene-Environment Interactions Strata Susceptible & Exposed (S+E+) Susceptible & Not Exposed (S+E-) Not Susceptible & Exposed (S-E+) Not Susceptible & Not Exposed (S-E-) Cases (Affected) a Controls (Unaffected) b c d e f g h
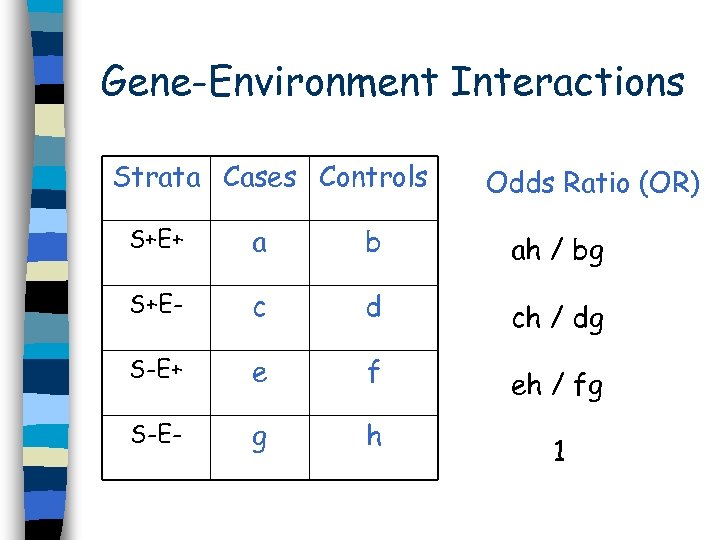 Gene-Environment Interactions Strata Cases Controls Odds Ratio (OR) S+E+ a b ah / bg S+E- c d ch / dg S-E+ e f eh / fg S-E- g h 1
Gene-Environment Interactions Strata Cases Controls Odds Ratio (OR) S+E+ a b ah / bg S+E- c d ch / dg S-E+ e f eh / fg S-E- g h 1
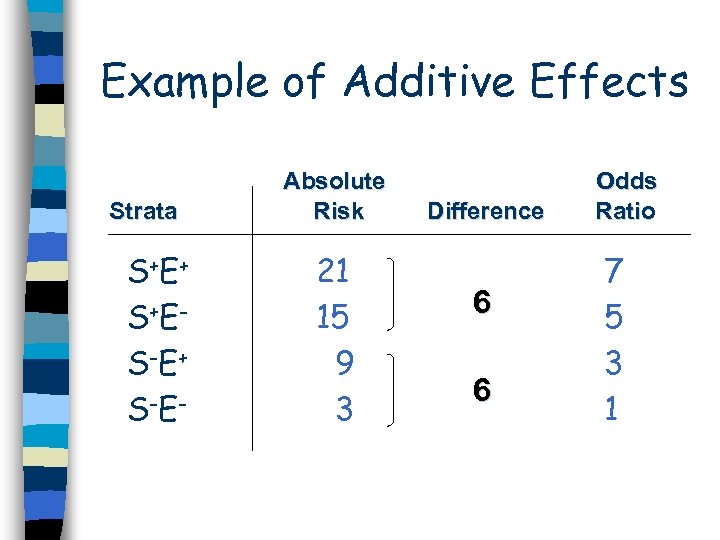 Example of Additive Effects Strata S+E + S+E S-E + S-E - Absolute Risk 21 15 9 3 Difference 6 6 Odds Ratio 7 5 3 1
Example of Additive Effects Strata S+E + S+E S-E + S-E - Absolute Risk 21 15 9 3 Difference 6 6 Odds Ratio 7 5 3 1
 Example of Additive Effects OR Interaction = ORS+E+ - (ORS+E- + ORS-E+ - 1) If OR Interaction Example: = 0, additive effects OR Interaction =7 – (5 + 3 – 1) OR Interaction = 0 Effects are additive, which is expected
Example of Additive Effects OR Interaction = ORS+E+ - (ORS+E- + ORS-E+ - 1) If OR Interaction Example: = 0, additive effects OR Interaction =7 – (5 + 3 – 1) OR Interaction = 0 Effects are additive, which is expected
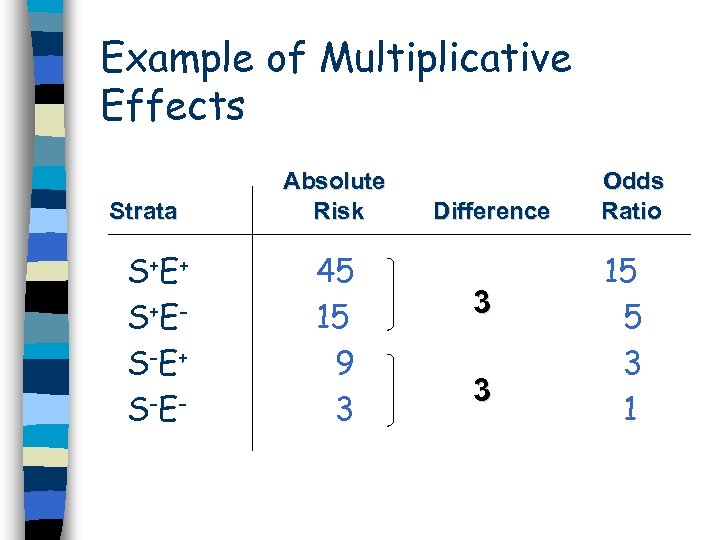 Example of Multiplicative Effects Strata S+E + S+E S-E + S-E - Absolute Risk 45 15 9 3 Difference 3 3 Odds Ratio 15 5 3 1
Example of Multiplicative Effects Strata S+E + S+E S-E + S-E - Absolute Risk 45 15 9 3 Difference 3 3 Odds Ratio 15 5 3 1
 Example of Multiplicative Effects OR Interaction = ORS+E+ / ORS+E- X ORS-E+ If OR Interaction Example: = 1, multiplicative effects OR Interaction = 15 / 5 x 3 OR Interaction = 1 Effects are multiplicative, which is expected
Example of Multiplicative Effects OR Interaction = ORS+E+ / ORS+E- X ORS-E+ If OR Interaction Example: = 1, multiplicative effects OR Interaction = 15 / 5 x 3 OR Interaction = 1 Effects are multiplicative, which is expected
 Advantages of 2 x 4 Table n Data displayed clearly and completely n OR for joint effects are readily generated and directly comparable – Based on same reference group n Can easily evaluate additive or multiplicative effects and identify interactions n Highlights sample size issues
Advantages of 2 x 4 Table n Data displayed clearly and completely n OR for joint effects are readily generated and directly comparable – Based on same reference group n Can easily evaluate additive or multiplicative effects and identify interactions n Highlights sample size issues
 Limitations of 2 x 4 Table n Only 2 risk factors are considered n Are not evaluating dose-response effects in exposure or susceptibility n Can only examine additive or multiplicative effects – Most gene-environment interactions are more complicated
Limitations of 2 x 4 Table n Only 2 risk factors are considered n Are not evaluating dose-response effects in exposure or susceptibility n Can only examine additive or multiplicative effects – Most gene-environment interactions are more complicated
 Evaluating Gene-Environment Interactions – Clinical Example n Vandenbroucke JP, Koster T, Briet E, et al. Increased risk of venous thrombosis in oral contraceptive users who are carriers of factor V Leiden mutation. Lancet 1994; 344: 1453 -1547
Evaluating Gene-Environment Interactions – Clinical Example n Vandenbroucke JP, Koster T, Briet E, et al. Increased risk of venous thrombosis in oral contraceptive users who are carriers of factor V Leiden mutation. Lancet 1994; 344: 1453 -1547
 Venous Thrombosis n Most frequent cardiovascular event in young women n Generally manifests as thrombosis of deep leg veins or pulmonary embolism n Incidence in women age 20 -49 yrs is ~ 2 /10, 000 persons/yr n Case fatality rate is ~ 1% to 2%
Venous Thrombosis n Most frequent cardiovascular event in young women n Generally manifests as thrombosis of deep leg veins or pulmonary embolism n Incidence in women age 20 -49 yrs is ~ 2 /10, 000 persons/yr n Case fatality rate is ~ 1% to 2%
 Oral Contraceptive Pills (OCP) and Venous Thrombosis (VT) n Association between OCP and VT has been known since early 1960 s n Led to development of OCP with lower estrogen content – Incidence of VT is ~12 to 34 / 10, 000 in OCP users n Risk of VTis highest during the 1 st year of exposure
Oral Contraceptive Pills (OCP) and Venous Thrombosis (VT) n Association between OCP and VT has been known since early 1960 s n Led to development of OCP with lower estrogen content – Incidence of VT is ~12 to 34 / 10, 000 in OCP users n Risk of VTis highest during the 1 st year of exposure
 Factor V Leiden Mutations n R 506 Q mutation – amino acid substitution n Geographic variation in mutation prevalence n Prevalence among individuals with VT n Relative risk of VT among carriers – Frequency of the mutation in Caucasians is~2% to 10% – Rare in African and Asians – 14% to 21% have the mutation – 3 - to 7 -fold higher than non-carriers
Factor V Leiden Mutations n R 506 Q mutation – amino acid substitution n Geographic variation in mutation prevalence n Prevalence among individuals with VT n Relative risk of VT among carriers – Frequency of the mutation in Caucasians is~2% to 10% – Rare in African and Asians – 14% to 21% have the mutation – 3 - to 7 -fold higher than non-carriers
 OCP, Factor V Leiden Mutations and Venous Thrombosis n What is risk of venous thrombosis among women who use OCP and carry the mutation? n Is there a gene-environment interaction? n If so, what are the clinical implications?
OCP, Factor V Leiden Mutations and Venous Thrombosis n What is risk of venous thrombosis among women who use OCP and carry the mutation? n Is there a gene-environment interaction? n If so, what are the clinical implications?
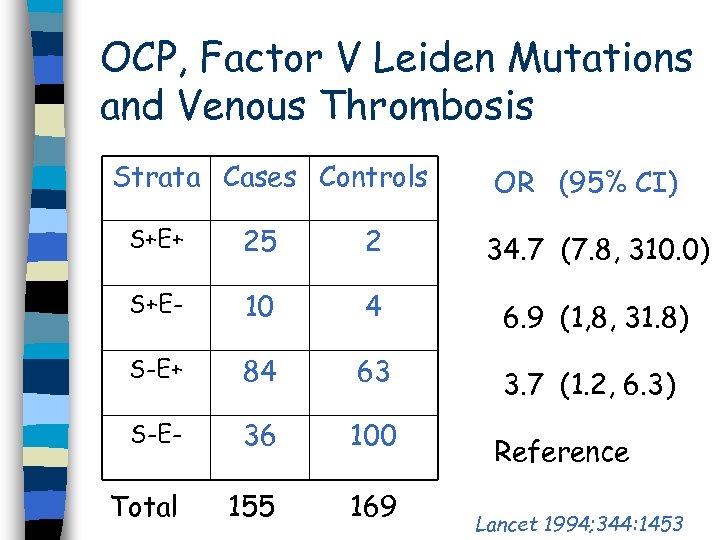 OCP, Factor V Leiden Mutations and Venous Thrombosis Strata Cases Controls OR (95% CI) S+E+ 25 2 34. 7 (7. 8, 310. 0) S+E- 10 4 6. 9 (1, 8, 31. 8) S-E+ 84 63 3. 7 (1. 2, 6. 3) S-E- 36 100 Total 155 169 Reference Lancet 1994; 344: 1453
OCP, Factor V Leiden Mutations and Venous Thrombosis Strata Cases Controls OR (95% CI) S+E+ 25 2 34. 7 (7. 8, 310. 0) S+E- 10 4 6. 9 (1, 8, 31. 8) S-E+ 84 63 3. 7 (1. 2, 6. 3) S-E- 36 100 Total 155 169 Reference Lancet 1994; 344: 1453
 Additive Effect? Strata OR S+E+ 34. 7 S+E- 6. 9 S-E+ 3. 7 S-E- Ref OR Interaction = 34. 7 – (6. 9 + 3. 7 - 1) = 25. 1
Additive Effect? Strata OR S+E+ 34. 7 S+E- 6. 9 S-E+ 3. 7 S-E- Ref OR Interaction = 34. 7 – (6. 9 + 3. 7 - 1) = 25. 1
 Multiplicative Effect? Strata OR S+E+ 34. 7 S+E- 6. 9 S-E+ 3. 7 S-E- Ref OR Interaction = 34. 7 / 6. 9 x 3. 7 = 1. 4
Multiplicative Effect? Strata OR S+E+ 34. 7 S+E- 6. 9 S-E+ 3. 7 S-E- Ref OR Interaction = 34. 7 / 6. 9 x 3. 7 = 1. 4
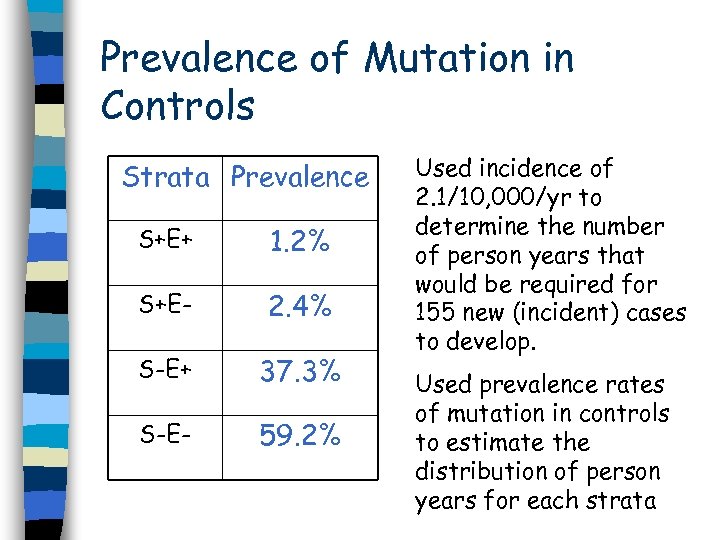 Prevalence of Mutation in Controls Strata Prevalence S+E+ 1. 2% S+E- 2. 4% S-E+ 37. 3% S-E- 59. 2% Used incidence of 2. 1/10, 000/yr to determine the number of person years that would be required for 155 new (incident) cases to develop. Used prevalence rates of mutation in controls to estimate the distribution of person years for each strata
Prevalence of Mutation in Controls Strata Prevalence S+E+ 1. 2% S+E- 2. 4% S-E+ 37. 3% S-E- 59. 2% Used incidence of 2. 1/10, 000/yr to determine the number of person years that would be required for 155 new (incident) cases to develop. Used prevalence rates of mutation in controls to estimate the distribution of person years for each strata
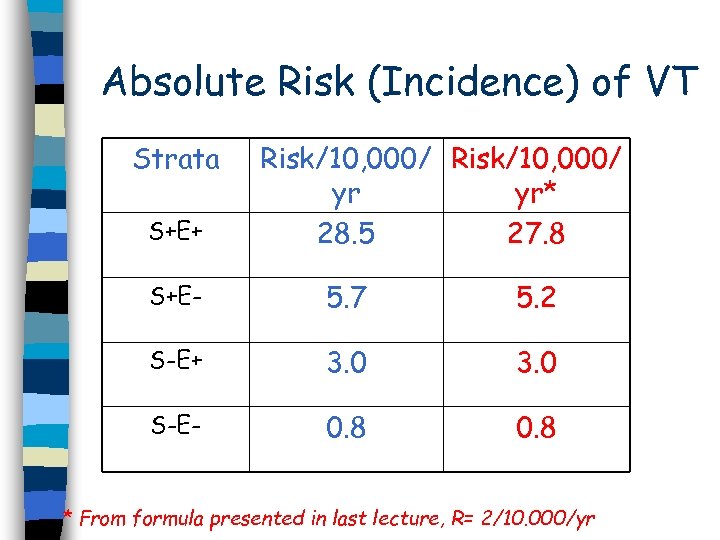 Absolute Risk (Incidence) of VT Strata S+E+ Risk/10, 000/ yr yr* 28. 5 27. 8 S+E- 5. 7 5. 2 S-E+ 3. 0 S-E- 0. 8 * From formula presented in last lecture, R= 2/10. 000/yr
Absolute Risk (Incidence) of VT Strata S+E+ Risk/10, 000/ yr yr* 28. 5 27. 8 S+E- 5. 7 5. 2 S-E+ 3. 0 S-E- 0. 8 * From formula presented in last lecture, R= 2/10. 000/yr
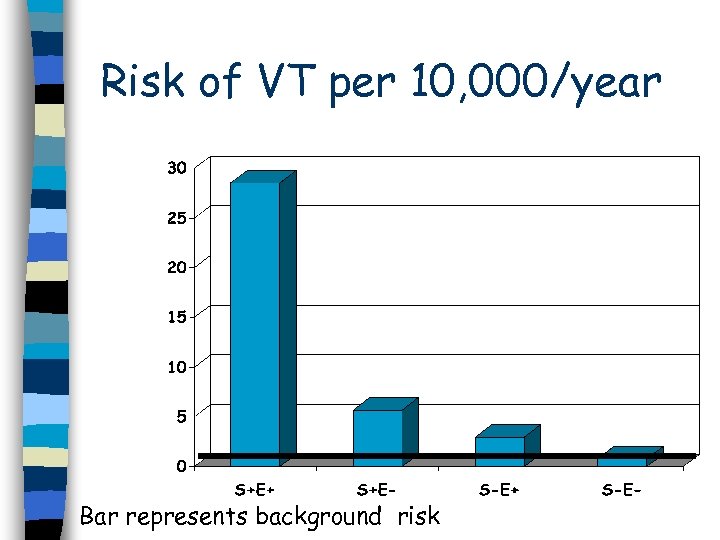 Risk of VT per 10, 000/year Bar represents background risk
Risk of VT per 10, 000/year Bar represents background risk
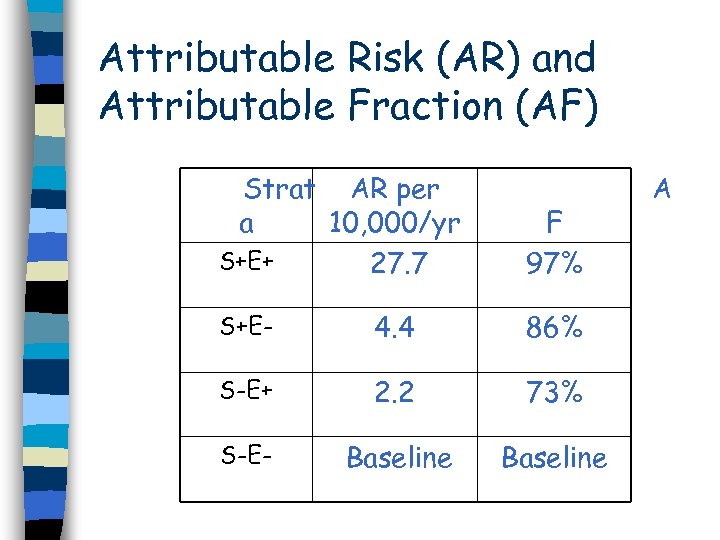 Attributable Risk (AR) and Attributable Fraction (AF) Strat AR per a 10, 000/yr S+E+ 27. 7 F 97% S+E- 4. 4 86% S-E+ 2. 2 73% S-E- Baseline A
Attributable Risk (AR) and Attributable Fraction (AF) Strat AR per a 10, 000/yr S+E+ 27. 7 F 97% S+E- 4. 4 86% S-E+ 2. 2 73% S-E- Baseline A
 Genetic Testing for Factor V Leiden n Debate about the need to test for Factor V Leiden mutations before prescribing OCP – Mutation is prevalent (~2% to 10%) – May prevent death in carriers – Testing is readily available n May be appropriate for women with a positive family history – Offer genetic testing prior to prescribing OCP
Genetic Testing for Factor V Leiden n Debate about the need to test for Factor V Leiden mutations before prescribing OCP – Mutation is prevalent (~2% to 10%) – May prevent death in carriers – Testing is readily available n May be appropriate for women with a positive family history – Offer genetic testing prior to prescribing OCP
 Genetic Testing for Factor V Leiden n Arguments – – – – against genetic testing Carriers will not receive OCP Small number of deaths prevented Results have implications for relatives Possible insurance discrimination Psychological distress/anxiety False positive/negative results Requires genetic counseling
Genetic Testing for Factor V Leiden n Arguments – – – – against genetic testing Carriers will not receive OCP Small number of deaths prevented Results have implications for relatives Possible insurance discrimination Psychological distress/anxiety False positive/negative results Requires genetic counseling
 Genetic Testing for Factor V Leiden n ACMG – – – – Recommendations Age <50, any VT VT in unusual sites Recurrent VT VT with positive family history VT in a pregnant woman VT in a women on OP Relatives of individuals with VT <50 yrs MI in women who smoke <50 yrs
Genetic Testing for Factor V Leiden n ACMG – – – – Recommendations Age <50, any VT VT in unusual sites Recurrent VT VT with positive family history VT in a pregnant woman VT in a women on OP Relatives of individuals with VT <50 yrs MI in women who smoke <50 yrs
 Screening Questions Developed by Nurse Practitioners Why do you want to be on HRT? 2. Have you had a blood clot? 3. Any family history of blood clots? 4. Any family history of stroke? 5. Lifestyle with prolonged immobility? 6. Breast, ovarian or cervical cancer? 7. Cancers in sister, mother, grandmother? 8. Any family history of CHD? If yes to #2 -5, may be candidate for testing 1. Park et al, 2003
Screening Questions Developed by Nurse Practitioners Why do you want to be on HRT? 2. Have you had a blood clot? 3. Any family history of blood clots? 4. Any family history of stroke? 5. Lifestyle with prolonged immobility? 6. Breast, ovarian or cervical cancer? 7. Cancers in sister, mother, grandmother? 8. Any family history of CHD? If yes to #2 -5, may be candidate for testing 1. Park et al, 2003
 Individuals with Factor V Leiden Mutation n Study of 110 mutation positive individuals identified in a North Carolina, US lab between 9/95 and 10/01 n Assessed knowledge; information needs, resources, satisfaction; health perception and anxiety; genetic testing issues – Quantitative and qualitative methods J Thromb Haemost 2003; 1: 2335
Individuals with Factor V Leiden Mutation n Study of 110 mutation positive individuals identified in a North Carolina, US lab between 9/95 and 10/01 n Assessed knowledge; information needs, resources, satisfaction; health perception and anxiety; genetic testing issues – Quantitative and qualitative methods J Thromb Haemost 2003; 1: 2335
 Individuals with Factor V Leiden Mutation n Knowledge – 39% did not recall giving consent – 13% did not know that they carried the mutation (excluded) – 94% knew mutation increased risk for clots – 30% did not know to exercise/not smoke – 79% overestimated their risk of VT – 50% did not understand its inheritance
Individuals with Factor V Leiden Mutation n Knowledge – 39% did not recall giving consent – 13% did not know that they carried the mutation (excluded) – 94% knew mutation increased risk for clots – 30% did not know to exercise/not smoke – 79% overestimated their risk of VT – 50% did not understand its inheritance
 Individuals with Factor V Leiden Mutations n Satisfaction – 64% said they received little information – Varied according to seeing a hematologist • 40% satisfied if with hematologist • 19% satisfied if not with hematologist – 68% had many more questions – Confidence in providers knowledge • 65% for males • 33% for females
Individuals with Factor V Leiden Mutations n Satisfaction – 64% said they received little information – Varied according to seeing a hematologist • 40% satisfied if with hematologist • 19% satisfied if not with hematologist – 68% had many more questions – Confidence in providers knowledge • 65% for males • 33% for females
 Individuals with Factor V Leiden Mutations n Information Needs – Most needed more information – 50% used internet as primary source n Health Perception – 28% spent much time trying to understand health implications – 51% made positive lifestyle changes – 43% reported increased worry – 85% were glad to know carrier status
Individuals with Factor V Leiden Mutations n Information Needs – Most needed more information – 50% used internet as primary source n Health Perception – 28% spent much time trying to understand health implications – 51% made positive lifestyle changes – 43% reported increased worry – 85% were glad to know carrier status
 Implications for Future n Patients interested in genetic testing for any condition need: – More information about genetic and environmental risk factors – Genetic counseling • • • Disclosure Testing in children Insurance discrimination Other risks/benefits Meaning of test results Follow-up
Implications for Future n Patients interested in genetic testing for any condition need: – More information about genetic and environmental risk factors – Genetic counseling • • • Disclosure Testing in children Insurance discrimination Other risks/benefits Meaning of test results Follow-up
 Implications for Future n Nurses are key – Genetic epidemiology literature (estimates of OR and incidence rates) are useful resources for estimating risk associated with genetic and environmental risk factors
Implications for Future n Nurses are key – Genetic epidemiology literature (estimates of OR and incidence rates) are useful resources for estimating risk associated with genetic and environmental risk factors
 References n American College of Medical Genetics Consensus Statement on Factor V Leiden Mutation Testing. Genet Med 2001; 3: 139148. n Bank I, Scavenius MPRB, Buller H, et al. Social aspects of genetic testing for factor V leiden mutation in healthy individuals and their importance for daily practice. Thrombosis Research 2004; 113: 7 -12.
References n American College of Medical Genetics Consensus Statement on Factor V Leiden Mutation Testing. Genet Med 2001; 3: 139148. n Bank I, Scavenius MPRB, Buller H, et al. Social aspects of genetic testing for factor V leiden mutation in healthy individuals and their importance for daily practice. Thrombosis Research 2004; 113: 7 -12.
 References n Botto LD, Khoury MJ. Commentary: facing the challenge of gene-environment interaction: the 2 x 4 table. Am J Epidemiol 2001; 153: 1016 -1020 n Burton PR, Tobin MD, Hopper JL. Key concepts in genetic epidemiology. Lancet 2005; 366: 941 -951.
References n Botto LD, Khoury MJ. Commentary: facing the challenge of gene-environment interaction: the 2 x 4 table. Am J Epidemiol 2001; 153: 1016 -1020 n Burton PR, Tobin MD, Hopper JL. Key concepts in genetic epidemiology. Lancet 2005; 366: 941 -951.
 References n Clayton D, Mc. Keigue PM. Epidemiological methods for studying genes and environmental factors in complex diseases. Lancet 2001; 358: 1356 -1360. n Gordis L. Epidemiology. WB Saunders Co. , Phildelphia, 1996. n Hellmann EA, Leslie ND, Moll S. Knowledge and educational needs of individuals with the factor V Leiden mutation. J Thromb Haemost 2003; 1: 2335 -2339.
References n Clayton D, Mc. Keigue PM. Epidemiological methods for studying genes and environmental factors in complex diseases. Lancet 2001; 358: 1356 -1360. n Gordis L. Epidemiology. WB Saunders Co. , Phildelphia, 1996. n Hellmann EA, Leslie ND, Moll S. Knowledge and educational needs of individuals with the factor V Leiden mutation. J Thromb Haemost 2003; 1: 2335 -2339.
 References n Horne MK and Mc. Closkey DJ. Factor V Leiden as a common genetic risk factor for venous thromboembolism. J Nursing Scholarsh 2006; 38: 19 -25. n Park BD, Lookinland S, Beckstrand RL, et al. Factor V Leiden and Venous Thromboembolism: risk Associated with Hormone Replacement Therapy. J Am Acad Nurse Pract 2004; 15: 458 -466.
References n Horne MK and Mc. Closkey DJ. Factor V Leiden as a common genetic risk factor for venous thromboembolism. J Nursing Scholarsh 2006; 38: 19 -25. n Park BD, Lookinland S, Beckstrand RL, et al. Factor V Leiden and Venous Thromboembolism: risk Associated with Hormone Replacement Therapy. J Am Acad Nurse Pract 2004; 15: 458 -466.
 References n Vandenbroucke JP, Koster T, Briet E, et al. Increased risk of venous thrombosis in oral contraceptive users who are carriers of factor V Leiden mutation. Lancet 1994; 344: 1453 -1547. n Vandenbroucke JP, van der Meer FJM, Helmerhorst FM, et al. Factor V Leiden: should we screen oral contraceptive users and pregnant women? BMJ 1996; 313: 11271130.
References n Vandenbroucke JP, Koster T, Briet E, et al. Increased risk of venous thrombosis in oral contraceptive users who are carriers of factor V Leiden mutation. Lancet 1994; 344: 1453 -1547. n Vandenbroucke JP, van der Meer FJM, Helmerhorst FM, et al. Factor V Leiden: should we screen oral contraceptive users and pregnant women? BMJ 1996; 313: 11271130.


