Gastric and duodenal ulcers Checked by:Sainova M.B Prepared


Gastric and duodenal ulcers Checked by:Sainova M.B Prepared by:Beken O.SH Faculty:GM Course:2 Group:027-2 Almaty,2017

Plan: I.Introduction What is an ulcer? II.Main section Diagnosis Causes & Risk Factors Why are they important? Consequences III.Conclusion IV.Used books

What is an ulcer? Acid breaks through protective substances on gut wall Duodenum (1st part small intestine) – most common site “Gastric” ulcers – in stomach Pain, bloating, nausea, “fullness”, weight loss, tiredness Complications: bleeding, perforation, obstruction

Diagnosis Endoscopy (>55yrs, first time). Capture all cases? Faecal / breath tests for H. pylori GI series (rare) False positive tests Missed cases? – risk of transmission / disease progression

Why are they important? HPA – “infectious disease” but main effects are from chronic burden Potential “medical emergency” Chronic symptoms – health and economic costs H. pylori also linked to: Functional dypepsia Cancer (2-6x more likely, though still rare) Differential clinical outcome - interaction between bacterial properties (phenotypic variation), genetics and environmental / behavioural factors
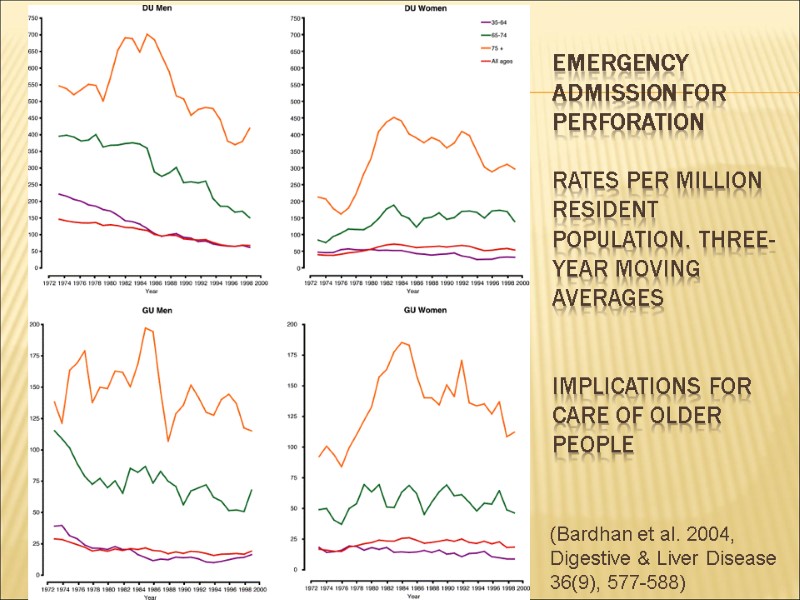
Emergency admission for perforation Rates per million resident population. Three-year moving averages Implications for care of older people (Bardhan et al. 2004, Digestive & Liver Disease 36(9), 577-588)

Causes? Ulcers are only found in white people, usually in long thin types given to worry and irritability (Robinson & Bruce 1940)

Causes & Risk Factors Helicobacter pylori 90% duodenal ulcers 70-75% gastric ulcers NSAIDs Lifestyle factors increase risk – smoking, physical stress, salt (GU) Genetic susceptibility / protection against H. pylori infection (twin studies, mouse models) Rarely…Zollinger-Ellison syndrome & others

Treatment & Outcome (NICE) 10% cases fail treatment (HPA) 1 course of combination therapy clears most cases (74% duodenal ulcers) Relapse greater for gastric ulcers (affected by lifestyle factors). At 3-12 months: Duodenal ulcers: 39% clear (acid suppression only); 91% (combination therapy) Gastric ulcers: 45% clear (acid suppression only); 77% (combination therapy)

Consequences Primary care – GP consultations, drug costs (increasing resistance) Secondary care – complications, surgery Tertiary care – rarely needed Socio-economic cost: Standardised average annual years of life lost (up to age 75) = 2.6 (per 10,000) (Females=1.8; Males=3.5) (1999 & 2001 pooled data, ONS)

Consequences… “Mass eradication of H pylori is impractical because of…generating antibiotic resistance, so we need to know how to target prophylaxis.” (Calam & Baron 2001) Ulcers occurring in absence of H. pylori or NSAIDs / aspirin. Combination therapies less effective in absence of H. pylori – data needed Screening? Cost-effective cost/LYS < £10,000 over 80yrs. But effects of eradication on morbidity / mortality?
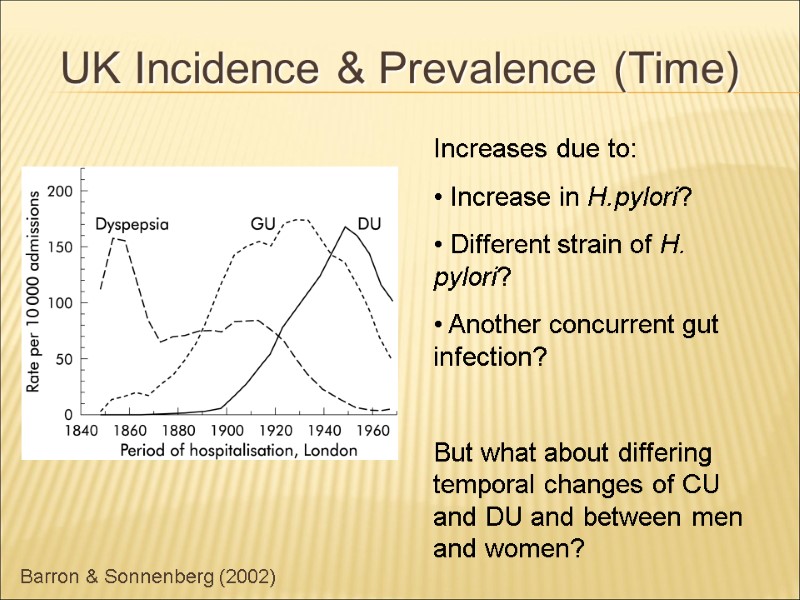
Barron & Sonnenberg (2002) UK Incidence & Prevalence (Time) Increases due to: Increase in H.pylori? Different strain of H. pylori? Another concurrent gut infection? But what about differing temporal changes of CU and DU and between men and women?

UK Incidence & Prevalence (Time) Evidence of cohort effect 1970-1986: (Primatesta et al. 1994) Decreased hospitalized morbidity and mortality Related more to changes in risk factors (e.g. smoking) in different cohorts than new pharmacological treatments? - implications for public health! OR: Genetic factors may be more important (Malaty et al. 1994)

UK Incidence & Prevalence (Person) H. pylori infection Incidence: 1-3% of adults p.a. (HPA) Prevalence infection: 40% population (HPA: >50% of 50+yr olds) Ulceration Incidence: DU in 30-50yrs old; higher incidence in men GU in >60yr olds; higher incidence in women Low prevalence in younger age groups Duodenal ulcer: up to 10% of population

UK Incidence & Prevalence (Person) Current trends: Annual age-standardized period prevalence decreased 1994-1998, particularly deprived areas (men 3.3/1000 - 1.5/1000; women 1.8/1000 - 0.9/1000) Sex incidence evening out – decreasing incidence in young men; increasing in older women But emergency admission rates for complications unchanged in last 30yrs Kang et al. (2006) – increase in case fatality for DU. Due to concomitant comorbidity / increasing ulceration (NSAIDs) / H.pylori (i.e. changing natural history)? Future decrease in prevalence?
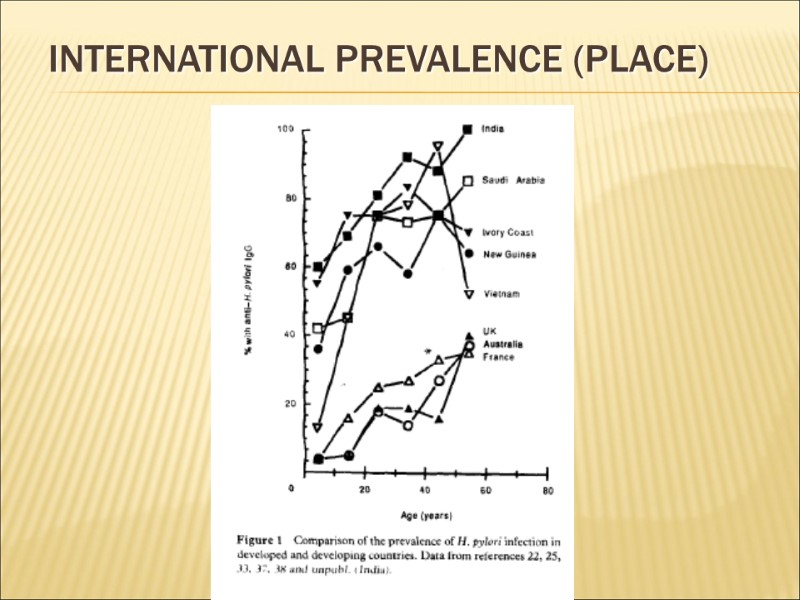
International prevalence (Place)

Place Worldwide. Prevalence 100% in developing countries Potential for “re-spread” in UK through travel? H. pylori - oral / faeco-oral transmission associated with poverty / overcrowding in childhood Increased prevalence in children with history of ulcer in the mothers – due to common environmental factors? Variation between ethnic groups even within countries
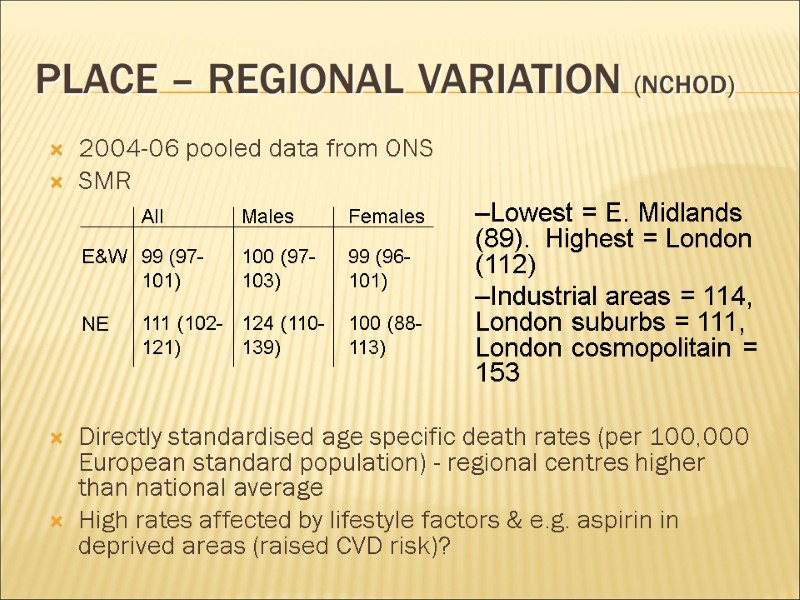
Place – Regional variation (NCHOD) 2004-06 pooled data from ONS SMR Directly standardised age specific death rates (per 100,000 European standard population) - regional centres higher than national average High rates affected by lifestyle factors & e.g. aspirin in deprived areas (raised CVD risk)? Lowest = E. Midlands (89). Highest = London (112) Industrial areas = 114, London suburbs = 111, London cosmopolitain = 153

NCHOD data - critique Based on original underlying cause of death (death certification) Numerator - mortality data 1993-2006 (ONS) with codes assigned using postcode of usual residence Changes to coding causes of death in England & Wales. Data based on new coding Denominator data - latest revisions of ONS mid-year population estimates, current at Oct 2007 - quite accurate NCHOD regularly updated
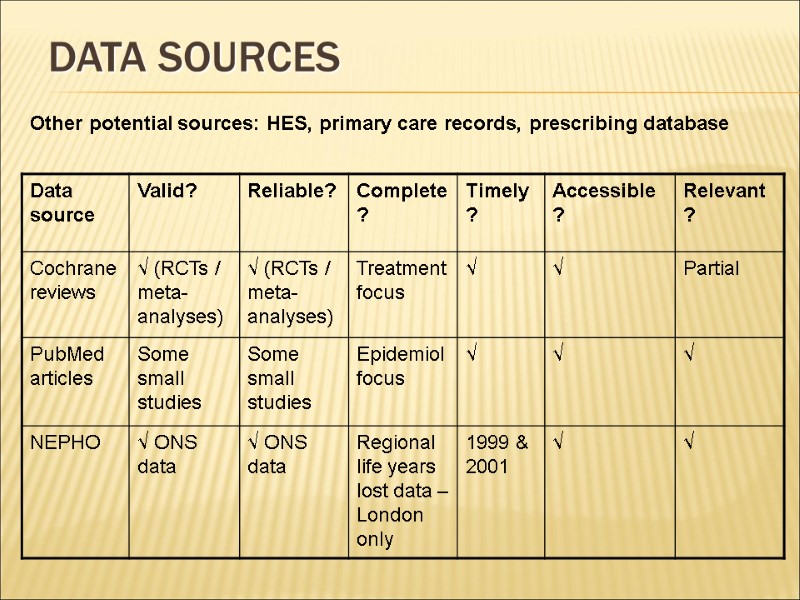
Data sources Other potential sources: HES, primary care records, prescribing database
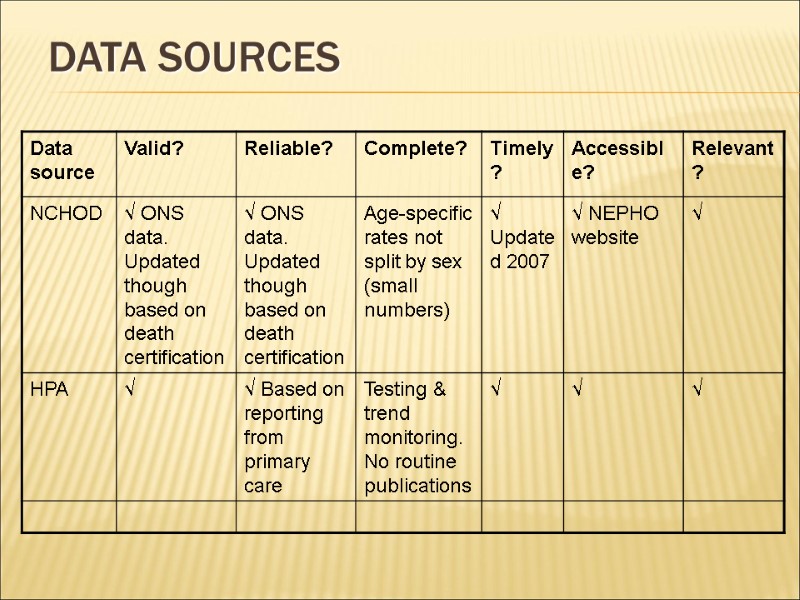
Data sources
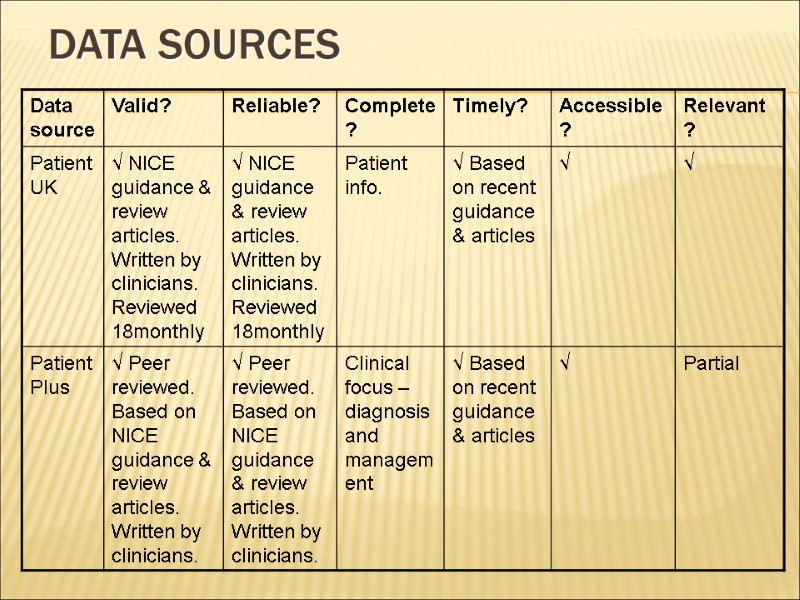
Data sources

Conclusion Disease mechanism / transmission poorly understood Risk factors multiple & interacting H. pylori is main cause but has changing natural history “Each generation has carried its own particular risk of bearing ulcers throughout adult life” (Susser & Stein 1962) Current pattern = exposure to H. pylori + genetics + exposure to drugs + environmental / behavioural factors DU / GU likely to continue causing significant chronic disease burden and personal / societal cost. Predicting future pattern difficult

Used books Tuberculosis Fact sheet N°104". WHO. October 2015. Retrieved 11 February 2016. "Basic TB Facts". CDC. March 13, 2012. Retrieved 11 February 2016 Medical Laboratory Science: Theory and Practice. New Delhi: Tata McGraw-Hill. 2000. p. 473 "Acid-Fast Stain Protocols". 21 August 2013. Retrieved 26 March 2016. Wkipedia.org
16060-gastric_and_duodenal_ulcers_srs.ppt
- Количество слайдов: 24

