cfbc08d17c053e139ddd8a8684ae1175.ppt
- Количество слайдов: 79
 Future of Infection Control in the 21 st Century: Predictions, Warnings and Challenges William A. Rutala, Ph. D, MPH Director, Hospital Epidemiology, Occupational Health and Safety; Research Professor of Medicine and Director, Statewide Program for Infection Control and Epidemiology University of North Carolina at Chapel Hill and UNC Health Care, Chapel Hill, NC
Future of Infection Control in the 21 st Century: Predictions, Warnings and Challenges William A. Rutala, Ph. D, MPH Director, Hospital Epidemiology, Occupational Health and Safety; Research Professor of Medicine and Director, Statewide Program for Infection Control and Epidemiology University of North Carolina at Chapel Hill and UNC Health Care, Chapel Hill, NC
 DISCUSSION TOPICS Impact of healthcare-associated infections Challenges in infection prevention
DISCUSSION TOPICS Impact of healthcare-associated infections Challenges in infection prevention
 HEALTHCARE-ASSOCIATED INFECTIONS: IMPACT IN UNITED STATES • • 1. 7 million infections per year 98, 987 deaths due to HAI n n • n Pneumonia 35, 967 Bloodstream 30, 665 Urinary tract 13, 088 SSI 8, 205 Other 11, 062 6 th leading cause of death (after heart disease, cancer, stroke, chronic lower respiratory diseases, and accidents)1 1 National Center for Health Statistics, 2004
HEALTHCARE-ASSOCIATED INFECTIONS: IMPACT IN UNITED STATES • • 1. 7 million infections per year 98, 987 deaths due to HAI n n • n Pneumonia 35, 967 Bloodstream 30, 665 Urinary tract 13, 088 SSI 8, 205 Other 11, 062 6 th leading cause of death (after heart disease, cancer, stroke, chronic lower respiratory diseases, and accidents)1 1 National Center for Health Statistics, 2004
 INCREMENTAL HOSPITAL DAYS DUE TO COMMON HAIs
INCREMENTAL HOSPITAL DAYS DUE TO COMMON HAIs
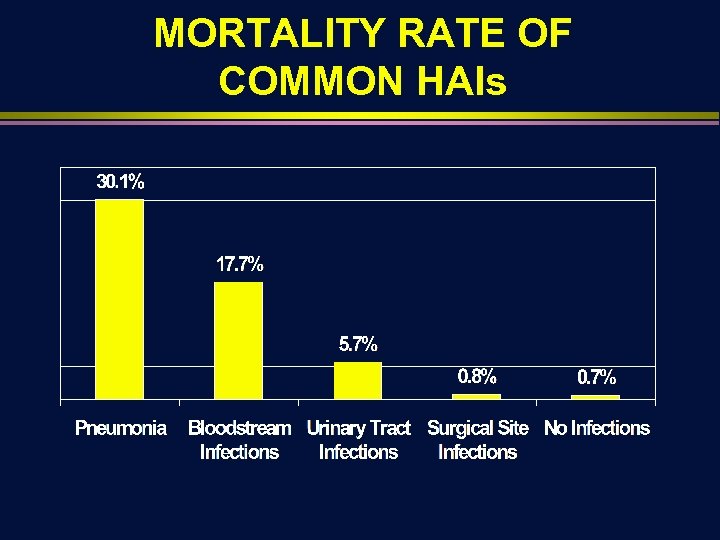 MORTALITY RATE OF COMMON HAIs
MORTALITY RATE OF COMMON HAIs
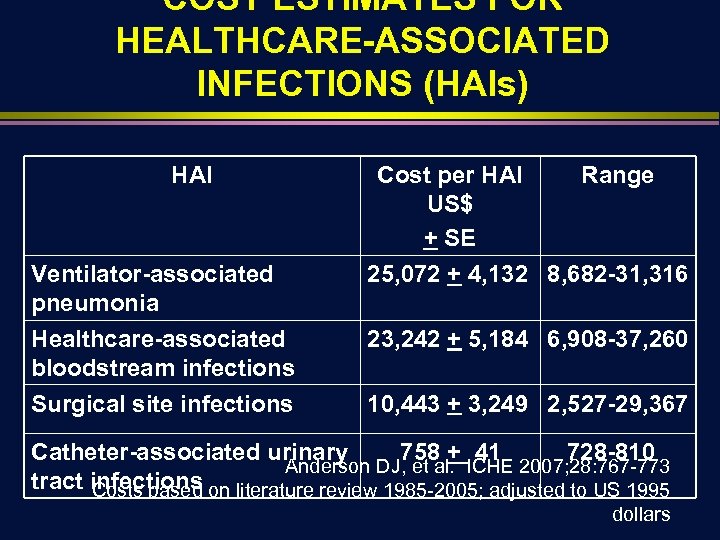 COST ESTIMATES FOR HEALTHCARE-ASSOCIATED INFECTIONS (HAIs) HAI Ventilator-associated pneumonia Healthcare-associated bloodstream infections Surgical site infections Cost per HAI Range US$ + SE 25, 072 + 4, 132 8, 682 -31, 316 23, 242 + 5, 184 6, 908 -37, 260 10, 443 + 3, 249 2, 527 -29, 367 Catheter-associated urinary 758 + 41 728 -810 Anderson DJ, et al. ICHE 2007; 28: 767 -773 tract infections on literature review 1985 -2005; adjusted to US 1995 Costs based dollars
COST ESTIMATES FOR HEALTHCARE-ASSOCIATED INFECTIONS (HAIs) HAI Ventilator-associated pneumonia Healthcare-associated bloodstream infections Surgical site infections Cost per HAI Range US$ + SE 25, 072 + 4, 132 8, 682 -31, 316 23, 242 + 5, 184 6, 908 -37, 260 10, 443 + 3, 249 2, 527 -29, 367 Catheter-associated urinary 758 + 41 728 -810 Anderson DJ, et al. ICHE 2007; 28: 767 -773 tract infections on literature review 1985 -2005; adjusted to US 1995 Costs based dollars
 PATHOGENS ASSOCIATED WITH HAIs*: NHSN, 2006 -2007 HAI: CLA-BSI, CA-UTI, VAP, SSI Hidron AI, et al. ICHE 2008; 29: 996 -1011
PATHOGENS ASSOCIATED WITH HAIs*: NHSN, 2006 -2007 HAI: CLA-BSI, CA-UTI, VAP, SSI Hidron AI, et al. ICHE 2008; 29: 996 -1011
 FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised/older patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant and emerging pathogens Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,
FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised/older patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant and emerging pathogens Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,
 FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by TJC Reduced funds for new infection prevention technologies
FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by TJC Reduced funds for new infection prevention technologies
 FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised/older patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant and emerging pathogens Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,
FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised/older patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant and emerging pathogens Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,
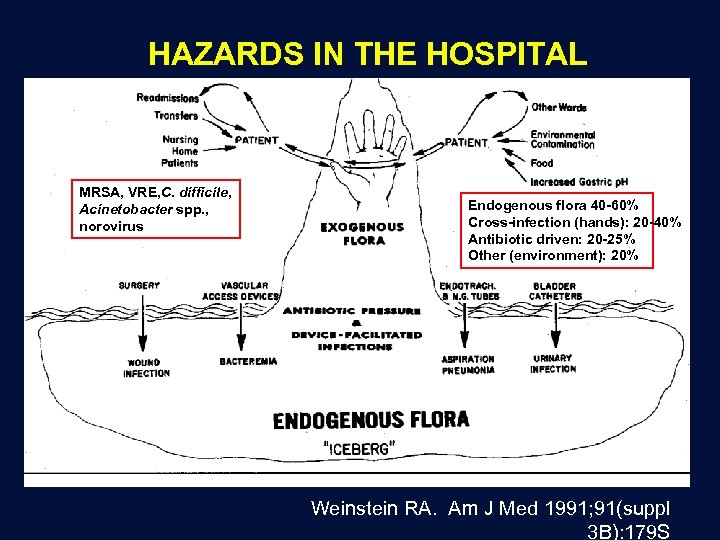 HAZARDS IN THE HOSPITAL MRSA, VRE, C. difficile, Acinetobacter spp. , norovirus Endogenous flora 40 -60% Cross-infection (hands): 20 -40% Antibiotic driven: 20 -25% Other (environment): 20% Weinstein RA. Am J Med 1991; 91(suppl 3 B): 179 S
HAZARDS IN THE HOSPITAL MRSA, VRE, C. difficile, Acinetobacter spp. , norovirus Endogenous flora 40 -60% Cross-infection (hands): 20 -40% Antibiotic driven: 20 -25% Other (environment): 20% Weinstein RA. Am J Med 1991; 91(suppl 3 B): 179 S
 RISK FACTORS FOR HEALTHCARE-ASSOCIATED INFECTIONS
RISK FACTORS FOR HEALTHCARE-ASSOCIATED INFECTIONS
 More HCPs and more invasive devices = higher HAI rates
More HCPs and more invasive devices = higher HAI rates
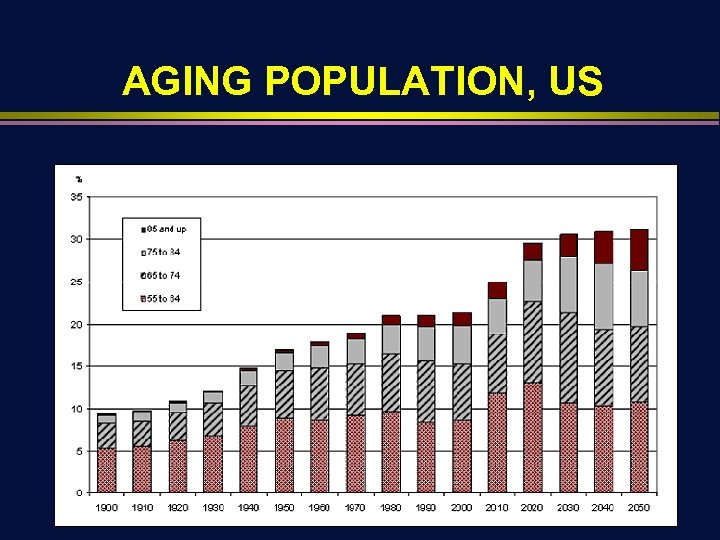 AGING POPULATION, US
AGING POPULATION, US
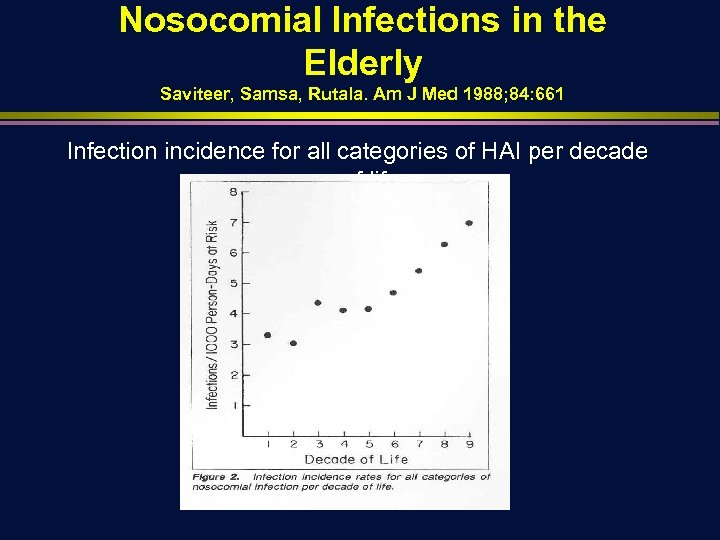 Nosocomial Infections in the Elderly Saviteer, Samsa, Rutala. Am J Med 1988; 84: 661 Infection incidence for all categories of HAI per decade of life
Nosocomial Infections in the Elderly Saviteer, Samsa, Rutala. Am J Med 1988; 84: 661 Infection incidence for all categories of HAI per decade of life
 FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised/older patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant pathogens and emerging pathogens Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,
FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised/older patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant pathogens and emerging pathogens Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,

 EMERGING RESISTANT PATHOGENS: HEALTH CARE FACILITIES l l l Staphylococcus aureus: Oxacillin (occ. vancomycin, linezolid) Enterococcus: Penicillin, aminoglycosides, vancomycin, linezolid, dalfopristin-quinupristin Enterobacteriaceae: ESBL producers, carbapenems CRE Pseudomonas aeruginosa, Acinetobacter sp: Multidrug resistant Mycobacterium tuberculosis: MDR (INH, rifampin), XDR (multiple)
EMERGING RESISTANT PATHOGENS: HEALTH CARE FACILITIES l l l Staphylococcus aureus: Oxacillin (occ. vancomycin, linezolid) Enterococcus: Penicillin, aminoglycosides, vancomycin, linezolid, dalfopristin-quinupristin Enterobacteriaceae: ESBL producers, carbapenems CRE Pseudomonas aeruginosa, Acinetobacter sp: Multidrug resistant Mycobacterium tuberculosis: MDR (INH, rifampin), XDR (multiple)
 EMERGING INFECTIOUS DISEASES RELEVANT TO THE HOSPITAL • • 1977 (US) – Legionnaire’s disease 1978 (US) – Staphylococcal toxic shock syndrome 1996 (England US) – Variant Creutzfeld-Jakob disease (v. CJD) 2001 (US) - Anthrax (attack via letters)* 2002 (US) – Vancomycin-resistant S. aureus* 2002 (Canada US) – Hypervirulent C. difficile* 2003 (China worldwide) - SARS* * HCWs at risk for infection
EMERGING INFECTIOUS DISEASES RELEVANT TO THE HOSPITAL • • 1977 (US) – Legionnaire’s disease 1978 (US) – Staphylococcal toxic shock syndrome 1996 (England US) – Variant Creutzfeld-Jakob disease (v. CJD) 2001 (US) - Anthrax (attack via letters)* 2002 (US) – Vancomycin-resistant S. aureus* 2002 (Canada US) – Hypervirulent C. difficile* 2003 (China worldwide) - SARS* * HCWs at risk for infection
 EMERGING INFECTIOUS DISEASES RELEVANT TO THE HOSPITAL • • 2003 (US) – Monkeypox* 2004 (Asia) – Avian influenza (H 5 N 1)* 2006 (Worldwide) – XDR-TB* 2009 -Novel H 1 N 1 influenza 2010 -2013 KPC-Klebsiella pneumoniae carbapenemase (KPC) , New Delhi metallo-betalactamase (NDM) Enterobacteriaceae, Carbapenenresistant Enterobacteriaceae (CRE) 2012 -13 (Worldwide) – Middle East Respiratory Symptoms-Coronavirus * HCP at risk for 2014 -Ebola, Enterovirus D 68 infection
EMERGING INFECTIOUS DISEASES RELEVANT TO THE HOSPITAL • • 2003 (US) – Monkeypox* 2004 (Asia) – Avian influenza (H 5 N 1)* 2006 (Worldwide) – XDR-TB* 2009 -Novel H 1 N 1 influenza 2010 -2013 KPC-Klebsiella pneumoniae carbapenemase (KPC) , New Delhi metallo-betalactamase (NDM) Enterobacteriaceae, Carbapenenresistant Enterobacteriaceae (CRE) 2012 -13 (Worldwide) – Middle East Respiratory Symptoms-Coronavirus * HCP at risk for 2014 -Ebola, Enterovirus D 68 infection
 FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant pathogens and emerging pathogen Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,
FUTURE OF INFECTION CONTROL • Changing population of hospital patients n n n • • Increased severity of illness Increased numbers of immunocompromised patients Shorter duration of hospitalization More and larger intensive care units Larger step-down units Growing frequency of antimicrobial-resistant pathogens and emerging pathogen Lack of compliance with hand hygiene and other infection preventive measures (e. g. ,

 RATIONALE FOR HAND HYGIENE • Many infectious agents are acquired via hand contact with contaminated surfaces Contact transmission: healthcare (MRSA, VRE), day care (MRSA), home (MRSA, “cold viruses”, herpes simplex) n Fecal-oral transmission: day care (Shigella, E. coli O 157: H 7), home (Salmonella, E. coli O 157: H 7, Cryptosporidium) n • • • Hand hygiene effective in reducing or eliminating transient flora Hand hygiene demonstrated to be effective in preventing illness (especially fecal-oral diarrheal illnesses) in healthcare facilities, child care centers/homes, and households ~40% of healthcare-associated infections due to cross-transmission
RATIONALE FOR HAND HYGIENE • Many infectious agents are acquired via hand contact with contaminated surfaces Contact transmission: healthcare (MRSA, VRE), day care (MRSA), home (MRSA, “cold viruses”, herpes simplex) n Fecal-oral transmission: day care (Shigella, E. coli O 157: H 7), home (Salmonella, E. coli O 157: H 7, Cryptosporidium) n • • • Hand hygiene effective in reducing or eliminating transient flora Hand hygiene demonstrated to be effective in preventing illness (especially fecal-oral diarrheal illnesses) in healthcare facilities, child care centers/homes, and households ~40% of healthcare-associated infections due to cross-transmission
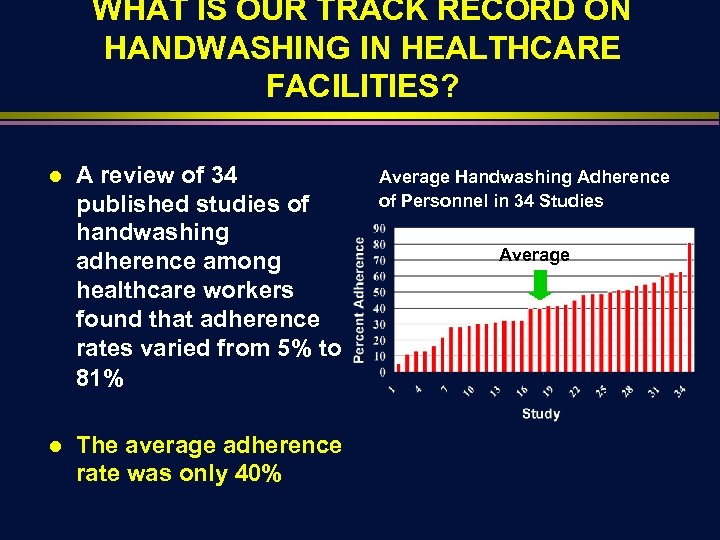 WHAT IS OUR TRACK RECORD ON HANDWASHING IN HEALTHCARE FACILITIES? l l A review of 34 published studies of handwashing adherence among healthcare workers found that adherence rates varied from 5% to 81% The average adherence rate was only 40% Average Handwashing Adherence of Personnel in 34 Studies Average
WHAT IS OUR TRACK RECORD ON HANDWASHING IN HEALTHCARE FACILITIES? l l A review of 34 published studies of handwashing adherence among healthcare workers found that adherence rates varied from 5% to 81% The average adherence rate was only 40% Average Handwashing Adherence of Personnel in 34 Studies Average
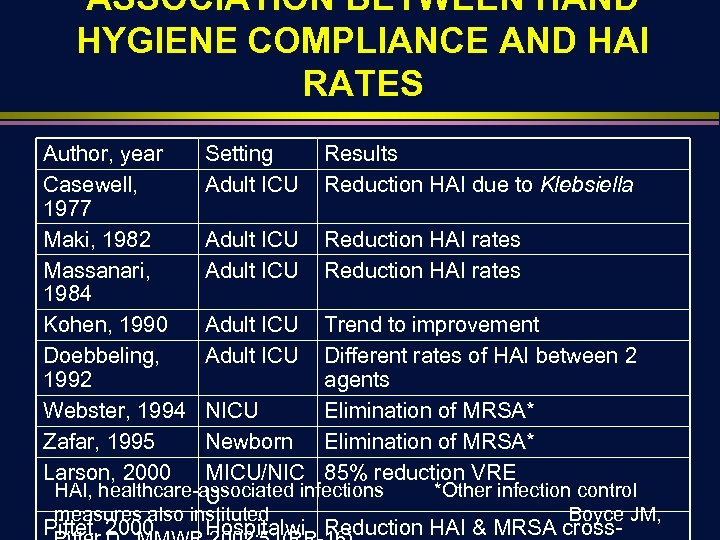 ASSOCIATION BETWEEN HAND HYGIENE COMPLIANCE AND HAI RATES Author, year Casewell, 1977 Maki, 1982 Massanari, 1984 Kohen, 1990 Doebbeling, 1992 Webster, 1994 Zafar, 1995 Larson, 2000 Setting Adult ICU Results Reduction HAI due to Klebsiella Adult ICU Reduction HAI rates Adult ICU Trend to improvement Different rates of HAI between 2 agents NICU Elimination of MRSA* Newborn Elimination of MRSA* MICU/NIC 85% reduction VRE HAI, healthcare-associated infections *Other infection control U measures also instituted Boyce JM, Pittet, 2000 Hospitalwi Reduction HAI & MRSA cross-
ASSOCIATION BETWEEN HAND HYGIENE COMPLIANCE AND HAI RATES Author, year Casewell, 1977 Maki, 1982 Massanari, 1984 Kohen, 1990 Doebbeling, 1992 Webster, 1994 Zafar, 1995 Larson, 2000 Setting Adult ICU Results Reduction HAI due to Klebsiella Adult ICU Reduction HAI rates Adult ICU Trend to improvement Different rates of HAI between 2 agents NICU Elimination of MRSA* Newborn Elimination of MRSA* MICU/NIC 85% reduction VRE HAI, healthcare-associated infections *Other infection control U measures also instituted Boyce JM, Pittet, 2000 Hospitalwi Reduction HAI & MRSA cross-
 HAND HYGIENE ADHERENCE AN INSTITUTIONAL PRIORITY • Multidisciplinary Program n n n Administrative support (IOC, Executive Staff, Dept Heads) Monitor HCWs adherence to policy and provide staff with information about performance Provide HCWs with accessible hand hygiene (HH) products to include alcohol based hand rubs Education regarding types of activities that result in hand contamination and indications for hand hygiene Reminders in the workplace (e. g. , posters) Considering ways to include HH in management standards (loss of hospital privileges, tickets for noncompliance, coffee coupons)
HAND HYGIENE ADHERENCE AN INSTITUTIONAL PRIORITY • Multidisciplinary Program n n n Administrative support (IOC, Executive Staff, Dept Heads) Monitor HCWs adherence to policy and provide staff with information about performance Provide HCWs with accessible hand hygiene (HH) products to include alcohol based hand rubs Education regarding types of activities that result in hand contamination and indications for hand hygiene Reminders in the workplace (e. g. , posters) Considering ways to include HH in management standards (loss of hospital privileges, tickets for noncompliance, coffee coupons)
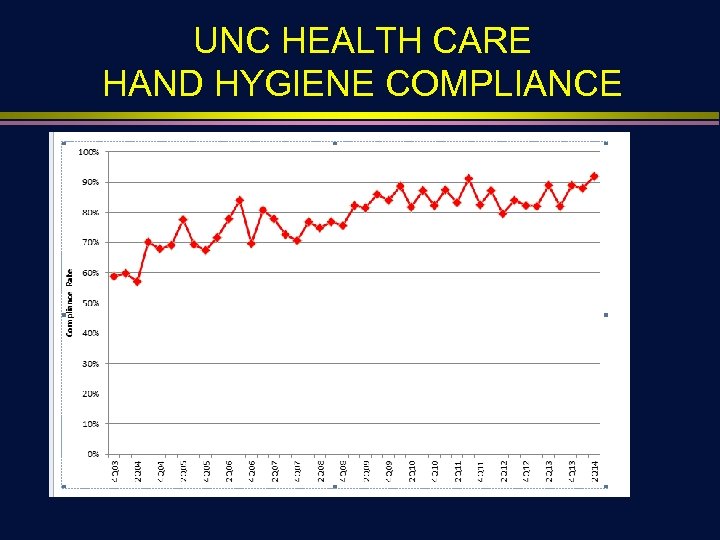 UNC HEALTH CARE HAND HYGIENE COMPLIANCE
UNC HEALTH CARE HAND HYGIENE COMPLIANCE
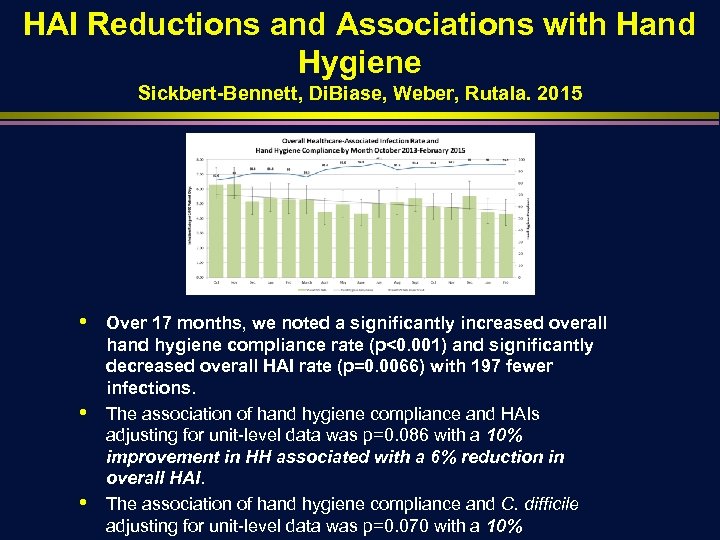 HAI Reductions and Associations with Hand Hygiene Sickbert-Bennett, Di. Biase, Weber, Rutala. 2015 • • • Over 17 months, we noted a significantly increased overall hand hygiene compliance rate (p<0. 001) and significantly decreased overall HAI rate (p=0. 0066) with 197 fewer infections. The association of hand hygiene compliance and HAIs adjusting for unit-level data was p=0. 086 with a 10% improvement in HH associated with a 6% reduction in overall HAI. The association of hand hygiene compliance and C. difficile adjusting for unit-level data was p=0. 070 with a 10%
HAI Reductions and Associations with Hand Hygiene Sickbert-Bennett, Di. Biase, Weber, Rutala. 2015 • • • Over 17 months, we noted a significantly increased overall hand hygiene compliance rate (p<0. 001) and significantly decreased overall HAI rate (p=0. 0066) with 197 fewer infections. The association of hand hygiene compliance and HAIs adjusting for unit-level data was p=0. 086 with a 10% improvement in HH associated with a 6% reduction in overall HAI. The association of hand hygiene compliance and C. difficile adjusting for unit-level data was p=0. 070 with a 10%
 Endoscope Reprocessing: Current Status of Cleaning and Disinfection • Guidelines n Multi-Society Guideline, 12 professional organizations, 2011 n Centers for Disease Control and Prevention, 2008 n Society of Gastroenterology Nurses and Associates, 2010 n AAMI Technical Information Report, Endoscope Reprocessing, In preparation n Food and Drug Administration, 2009 n Endoscope Reprocessing, Health Canada, 2010 n Association for Professional in Infection Control and Epidemiology, 2000
Endoscope Reprocessing: Current Status of Cleaning and Disinfection • Guidelines n Multi-Society Guideline, 12 professional organizations, 2011 n Centers for Disease Control and Prevention, 2008 n Society of Gastroenterology Nurses and Associates, 2010 n AAMI Technical Information Report, Endoscope Reprocessing, In preparation n Food and Drug Administration, 2009 n Endoscope Reprocessing, Health Canada, 2010 n Association for Professional in Infection Control and Epidemiology, 2000
 ENDOSCOPE INFECTIONS • Infections traced to deficient practices n Inadequate cleaning (clean all channels) n Inappropriate/ineffective disinfection (time exposure, perfuse channels, test concentration) n Failure to follow recommended disinfection practices (drying, contaminated water bottles, irrigating solutions) n Flaws in design/manufacture of endoscopes or AERs
ENDOSCOPE INFECTIONS • Infections traced to deficient practices n Inadequate cleaning (clean all channels) n Inappropriate/ineffective disinfection (time exposure, perfuse channels, test concentration) n Failure to follow recommended disinfection practices (drying, contaminated water bottles, irrigating solutions) n Flaws in design/manufacture of endoscopes or AERs
 Endoscope Reprocessing Methods Ofstead , Wetzler, Snyder, Horton, Gastro Nursing 2010; 33: 204
Endoscope Reprocessing Methods Ofstead , Wetzler, Snyder, Horton, Gastro Nursing 2010; 33: 204
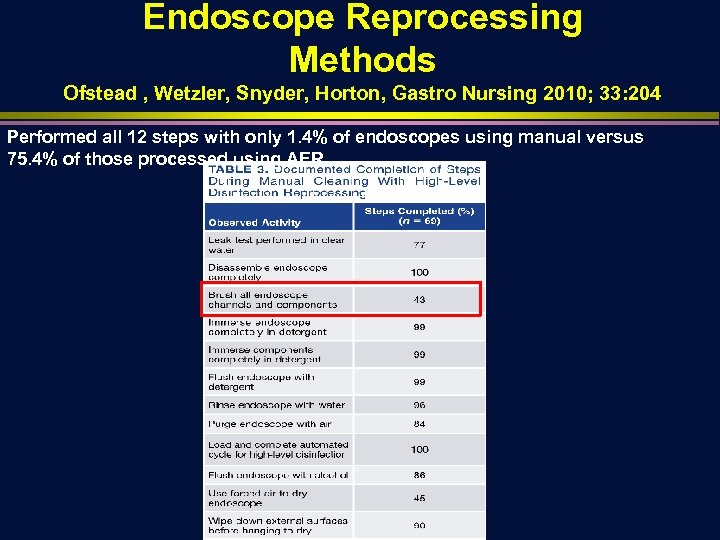 Endoscope Reprocessing Methods Ofstead , Wetzler, Snyder, Horton, Gastro Nursing 2010; 33: 204 Performed all 12 steps with only 1. 4% of endoscopes using manual versus 75. 4% of those processed using AER
Endoscope Reprocessing Methods Ofstead , Wetzler, Snyder, Horton, Gastro Nursing 2010; 33: 204 Performed all 12 steps with only 1. 4% of endoscopes using manual versus 75. 4% of those processed using AER
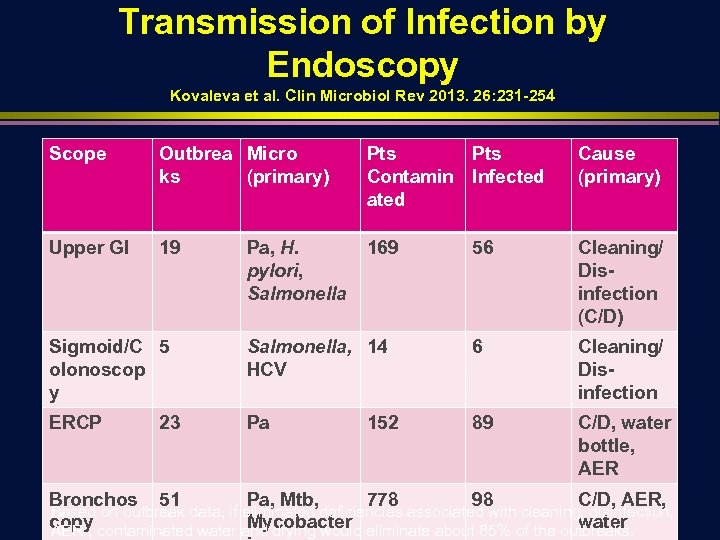 Transmission of Infection by Endoscopy Kovaleva et al. Clin Microbiol Rev 2013. 26: 231 -254 Scope Outbrea Micro ks (primary) Pts Contamin Infected ated Cause (primary) Upper GI 19 169 56 Cleaning/ Disinfection (C/D) Pa, H. pylori, Salmonella Sigmoid/C 5 olonoscop y Salmonella, 14 HCV 6 Cleaning/ Disinfection ERCP Pa 89 C/D, water bottle, AER 23 152 Bronchos 51 Pa, Mtb, 778 98 C/D, AER, Based on outbreak data, if eliminated deficiencies associated with cleaning, disinfection, copy contaminated water and drying would eliminate about 85% of the outbreaks. Mycobacter water AER ,
Transmission of Infection by Endoscopy Kovaleva et al. Clin Microbiol Rev 2013. 26: 231 -254 Scope Outbrea Micro ks (primary) Pts Contamin Infected ated Cause (primary) Upper GI 19 169 56 Cleaning/ Disinfection (C/D) Pa, H. pylori, Salmonella Sigmoid/C 5 olonoscop y Salmonella, 14 HCV 6 Cleaning/ Disinfection ERCP Pa 89 C/D, water bottle, AER 23 152 Bronchos 51 Pa, Mtb, 778 98 C/D, AER, Based on outbreak data, if eliminated deficiencies associated with cleaning, disinfection, copy contaminated water and drying would eliminate about 85% of the outbreaks. Mycobacter water AER ,
 TRANSMISSION OF INFECTION • Gastrointestinal endoscopy >150 infections transmitted n Salmonella sp. and P. aeruginosa n Clinical spectrum ranged from colonization to death n • Bronchoscopy ~100 infections transmitted n M. tuberculosis, atypical Mycobacteria, P. aeruginosa n • Endemic transmission may go unrecognized (e. g. , inadequate surveillance, low frequency, asymptomatic infections) Kovaleva et al. Clin Microbiol Rev 2013. 26: 231 -254
TRANSMISSION OF INFECTION • Gastrointestinal endoscopy >150 infections transmitted n Salmonella sp. and P. aeruginosa n Clinical spectrum ranged from colonization to death n • Bronchoscopy ~100 infections transmitted n M. tuberculosis, atypical Mycobacteria, P. aeruginosa n • Endemic transmission may go unrecognized (e. g. , inadequate surveillance, low frequency, asymptomatic infections) Kovaleva et al. Clin Microbiol Rev 2013. 26: 231 -254
 FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
 INCREASING DEMANDS ON IPs WITH ACCOUNTABILITY Public expectation of 0 rate of healthcareassociated infections? Buy in by legislatures and CMS IC accountability and attention rich but resource poor
INCREASING DEMANDS ON IPs WITH ACCOUNTABILITY Public expectation of 0 rate of healthcareassociated infections? Buy in by legislatures and CMS IC accountability and attention rich but resource poor
 IP ACTIVITIES l 1975 to 1990 n n n n Surveillance Outbreak investigations Exposure evaluations Education JCAHO Policy development and review Sterilizer monitoring Dialysis water l 1991 to 2003 (new) n n n n Targeted surveillance OSHA TB OSHA Bloodborne Molecular epidemiology MRSA, VRE BT preparedness Construction rounds
IP ACTIVITIES l 1975 to 1990 n n n n Surveillance Outbreak investigations Exposure evaluations Education JCAHO Policy development and review Sterilizer monitoring Dialysis water l 1991 to 2003 (new) n n n n Targeted surveillance OSHA TB OSHA Bloodborne Molecular epidemiology MRSA, VRE BT preparedness Construction rounds
 IP ACTIVITIES l 2004 to 2012 n n n n n IHI bundles CMS core measures NSQUIP (VAs, others) NDNQI (ANA) Other CQI initiatives MRSA active surveillance Unannounced TJC visits Avian influenza preparedness Endoscope sampling l Future n n n n Public health reporting Mandated influenza vaccine Mandated MRSA surveillance Cost analyses Comprehensive surveillance Transparency Electronic medical records
IP ACTIVITIES l 2004 to 2012 n n n n n IHI bundles CMS core measures NSQUIP (VAs, others) NDNQI (ANA) Other CQI initiatives MRSA active surveillance Unannounced TJC visits Avian influenza preparedness Endoscope sampling l Future n n n n Public health reporting Mandated influenza vaccine Mandated MRSA surveillance Cost analyses Comprehensive surveillance Transparency Electronic medical records
 FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
 SOURCE OF INFECTION PREVENTION STRATEGIES • • • Centers for Disease Control and Prevention The Joint Commission Centers for Medicare and Medicaid Services Institute for Healthcare Improvement (IHI) Professional Organizations: APIC, SHEA, AAMI, AORN, SGNA, AIA,
SOURCE OF INFECTION PREVENTION STRATEGIES • • • Centers for Disease Control and Prevention The Joint Commission Centers for Medicare and Medicaid Services Institute for Healthcare Improvement (IHI) Professional Organizations: APIC, SHEA, AAMI, AORN, SGNA, AIA,
 INFECTION PREVENTION STRATEGIES • Centers for Disease Control and Prevention n n Prevention of Catheter-Associated UTI, 2009 Guideline for D/S in Healthcare Facilities, 2008 Guideline for Isolation Precautions, 2007 Management of MDR Organisms, 2006 Preventing HA Pneumonia, 2003 Environmental Infection Control in HCF, 2003 Hand Hygiene in Healthcare Settings, 2002 Prevention of Intravascular Device-Related Infections, 2002 Prevention of Surgical Site Infections, 1999 Management of Occupational Exposure to HBV, HCV, HIV, 2002 Infection Control in Healthcare Personnel, 1998
INFECTION PREVENTION STRATEGIES • Centers for Disease Control and Prevention n n Prevention of Catheter-Associated UTI, 2009 Guideline for D/S in Healthcare Facilities, 2008 Guideline for Isolation Precautions, 2007 Management of MDR Organisms, 2006 Preventing HA Pneumonia, 2003 Environmental Infection Control in HCF, 2003 Hand Hygiene in Healthcare Settings, 2002 Prevention of Intravascular Device-Related Infections, 2002 Prevention of Surgical Site Infections, 1999 Management of Occupational Exposure to HBV, HCV, HIV, 2002 Infection Control in Healthcare Personnel, 1998
 INFECTION PREVENTION STRATEGIES • SHEA Management of HCWs Infected with HBV, HCV, HIV, March 2010 n Disinfection and Sterilization of Prion. Contaminated Medical Instruments, February 2010 n Compendium of Strategies to Prevent HAIs, September 2014 n u Surgical Site Infection u CLA-Bloodstream Infection u Catheter-Associated UTI u Ventilator-Associated Pneumonia u Clostridium difficile u Methicillin-resistant S. aureus u Hand Hygiene
INFECTION PREVENTION STRATEGIES • SHEA Management of HCWs Infected with HBV, HCV, HIV, March 2010 n Disinfection and Sterilization of Prion. Contaminated Medical Instruments, February 2010 n Compendium of Strategies to Prevent HAIs, September 2014 n u Surgical Site Infection u CLA-Bloodstream Infection u Catheter-Associated UTI u Ventilator-Associated Pneumonia u Clostridium difficile u Methicillin-resistant S. aureus u Hand Hygiene
 INSTITUTE FOR HEALTHCARE IMPROVEMENT VAP AND CA-BSI BUNDLES VAP Bundle l l Elevation of the head of the bed to between 30 and 45 degrees Daily “sedation vacation” and daily assessment of readiness to extubate Peptic ulcer disease (PUD) prophylaxis Deep venous thrombosis (DVT) prophylaxis (unless contraindicated) CA-BSI l l l Hand hygiene Maximal barrier precautions Chlorhexidine skin antisepsis Optimal catheter site selection, with subclavian vein as the preferred site for nontunneled catheters Daily review of line necessity, with prompt removal of unnecessary lines
INSTITUTE FOR HEALTHCARE IMPROVEMENT VAP AND CA-BSI BUNDLES VAP Bundle l l Elevation of the head of the bed to between 30 and 45 degrees Daily “sedation vacation” and daily assessment of readiness to extubate Peptic ulcer disease (PUD) prophylaxis Deep venous thrombosis (DVT) prophylaxis (unless contraindicated) CA-BSI l l l Hand hygiene Maximal barrier precautions Chlorhexidine skin antisepsis Optimal catheter site selection, with subclavian vein as the preferred site for nontunneled catheters Daily review of line necessity, with prompt removal of unnecessary lines
 INFECTION CONTROL INTERVENTIONS • • 2000: Addition of 2% chlorhexadine/70% isopropyl alcohol (Chora. Prep®) to the central line dressing kit. 2001: Mandatory training for nurses on IV line site care and maintenance. 2003: Full body drape added to central line kit. MD could choose kit containing a catheter impregnated with antiseptic or antibiotic. 2005: 2 nd generation impregnated catheter included in all central line kits (except for Neonatal ICU). 2006: Pilot in MICU of IHI bundle to prevent CLA-BSI. 2007: Implementation of the IHI bundle in all ICUs. 2008: Implementation of Infection Control Liaison Program 2009: Implementation of CHG patch.
INFECTION CONTROL INTERVENTIONS • • 2000: Addition of 2% chlorhexadine/70% isopropyl alcohol (Chora. Prep®) to the central line dressing kit. 2001: Mandatory training for nurses on IV line site care and maintenance. 2003: Full body drape added to central line kit. MD could choose kit containing a catheter impregnated with antiseptic or antibiotic. 2005: 2 nd generation impregnated catheter included in all central line kits (except for Neonatal ICU). 2006: Pilot in MICU of IHI bundle to prevent CLA-BSI. 2007: Implementation of the IHI bundle in all ICUs. 2008: Implementation of Infection Control Liaison Program 2009: Implementation of CHG patch.
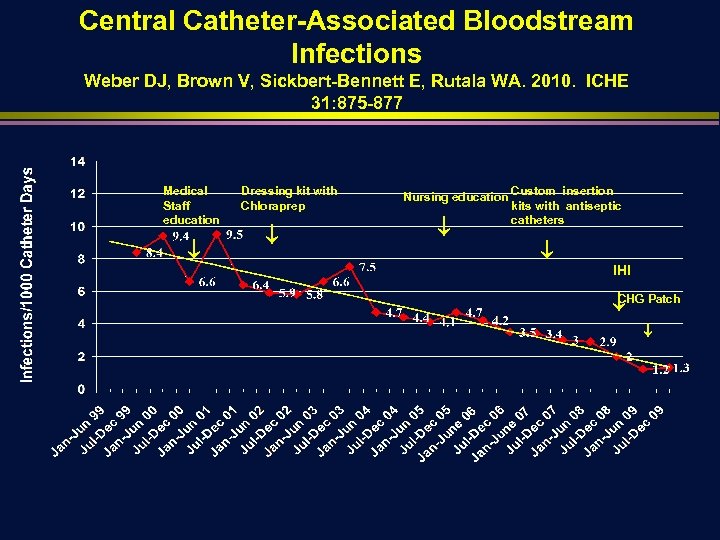 Central Catheter-Associated Bloodstream Infections Weber DJ, Brown V, Sickbert-Bennett E, Rutala WA. 2010. ICHE 31: 875 -877 Medical Staff education Dressing kit with Chloraprep Nursing education Custom insertion kits with antiseptic catheters IHI CHG Patch
Central Catheter-Associated Bloodstream Infections Weber DJ, Brown V, Sickbert-Bennett E, Rutala WA. 2010. ICHE 31: 875 -877 Medical Staff education Dressing kit with Chloraprep Nursing education Custom insertion kits with antiseptic catheters IHI CHG Patch
 IMPACT OF UNC REDUCTION IN CLA-BSI, 19992008 Weber DJ, Brown V, Sickbert-Bennett E, Rutala WA. 2010. ICHE 31: 875877 • Infections prevented n • Deaths prevented (based on attributable mortality) n • 887 222 to 266 death preventing (attributable mortality 25% to 30%) Savings (2005 dollars) n $20, 615, 654
IMPACT OF UNC REDUCTION IN CLA-BSI, 19992008 Weber DJ, Brown V, Sickbert-Bennett E, Rutala WA. 2010. ICHE 31: 875877 • Infections prevented n • Deaths prevented (based on attributable mortality) n • 887 222 to 266 death preventing (attributable mortality 25% to 30%) Savings (2005 dollars) n $20, 615, 654
 Given the choice of changing human behavior (e. g. , improving aseptic technique) or designing a better device, the device will always be more successful… Robert A. Weinstein
Given the choice of changing human behavior (e. g. , improving aseptic technique) or designing a better device, the device will always be more successful… Robert A. Weinstein
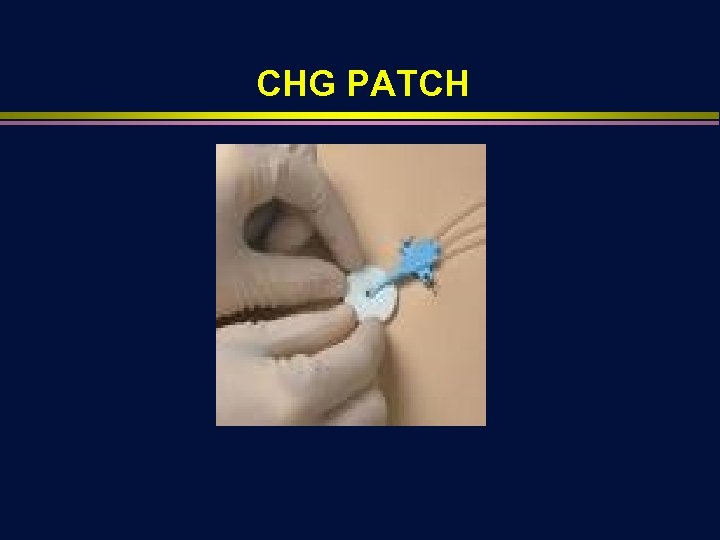 CHG PATCH
CHG PATCH
 PROTECTIVE DISK WITH CHG • • • Bacteria can recolonize the skin and CHG suppresses regrowth CHG patch provides contact around the insertion site and 7 day continuous release of CHG provides ongoing antimicrobial protection Randomized, controlled trials show CHG patch reduces risk of infection (JAMA 2009; 301: 1231 and Ann Hematol 2009; 88: 267)
PROTECTIVE DISK WITH CHG • • • Bacteria can recolonize the skin and CHG suppresses regrowth CHG patch provides contact around the insertion site and 7 day continuous release of CHG provides ongoing antimicrobial protection Randomized, controlled trials show CHG patch reduces risk of infection (JAMA 2009; 301: 1231 and Ann Hematol 2009; 88: 267)
 CHG SPONGE EFFICACY: RCT IN ADULT ICU PATIENTS • • • Study design: Accessor-blind, 3 x 3 factorial, randomized clinical trial Setting: 7 ICUs in 5 French hospitals (age >18 years) Interventions: Use of CHG sponge vs standard dressing; CHG sponge changed every 7 days, standard dressing changed every 3 days Study size: 2, 095 patients, 3, 778 catheters, 28, 931 catheter days Results CHG sponge reduce catheter-related infection (0. 6/1000 Pt-d vs 1. 1/1000 Pt-d, p=0. 03) n CHG sponge reduced CLA-BSIs (0. 4/1000 Pt-d vs 1. 3/1000 Pt-d, HR=0. 24) Timsit J-F, et al. JAMA 2009; 301: 1231 -1241 n CHG dressings not associated with increased resistance in skin bacteria n
CHG SPONGE EFFICACY: RCT IN ADULT ICU PATIENTS • • • Study design: Accessor-blind, 3 x 3 factorial, randomized clinical trial Setting: 7 ICUs in 5 French hospitals (age >18 years) Interventions: Use of CHG sponge vs standard dressing; CHG sponge changed every 7 days, standard dressing changed every 3 days Study size: 2, 095 patients, 3, 778 catheters, 28, 931 catheter days Results CHG sponge reduce catheter-related infection (0. 6/1000 Pt-d vs 1. 1/1000 Pt-d, p=0. 03) n CHG sponge reduced CLA-BSIs (0. 4/1000 Pt-d vs 1. 3/1000 Pt-d, HR=0. 24) Timsit J-F, et al. JAMA 2009; 301: 1231 -1241 n CHG dressings not associated with increased resistance in skin bacteria n
 ENVIRONMENTAL CONTAMINATION LEADS TO HAIs Suboptimal Cleaning • • There is increasing evidence to support the contribution of the environment to disease transmission This supports comprehensive disinfecting regimens (goal is not sterilization) to reduce the risk of acquiring a pathogen from the healthcare environment
ENVIRONMENTAL CONTAMINATION LEADS TO HAIs Suboptimal Cleaning • • There is increasing evidence to support the contribution of the environment to disease transmission This supports comprehensive disinfecting regimens (goal is not sterilization) to reduce the risk of acquiring a pathogen from the healthcare environment
 Risk of Acquiring MRSA and VRE from Prior Room Occupants • • • Admission to a room previously occupied by an MRSA-positive patient or VRE-positive patient significantly increased the odds of acquisition for MRSA and VRE (although this route is a minor contributor to overall transmission). Arch Intern Med 2006; 166: 1945. Prior environmental contamination, whether measured via environmental cultures or prior room occupancy by VRE-colonized patients, increases the risk of acquisition of VRE. Clin Infect Dis 2008; 46: 678. Prior room occupant with CDAD is a significant risk for CDAD acquisition. Shaughnessy et al. ICHE 2011; 32: 201
Risk of Acquiring MRSA and VRE from Prior Room Occupants • • • Admission to a room previously occupied by an MRSA-positive patient or VRE-positive patient significantly increased the odds of acquisition for MRSA and VRE (although this route is a minor contributor to overall transmission). Arch Intern Med 2006; 166: 1945. Prior environmental contamination, whether measured via environmental cultures or prior room occupancy by VRE-colonized patients, increases the risk of acquisition of VRE. Clin Infect Dis 2008; 46: 678. Prior room occupant with CDAD is a significant risk for CDAD acquisition. Shaughnessy et al. ICHE 2011; 32: 201
 RELATIVE RISK OF PATHOGEN ACQUISITION IF PRIOR ROOM OCCUPANT INFECTED * Prior room occupant infected; ^Any room occupant in prior 2 weeks infected
RELATIVE RISK OF PATHOGEN ACQUISITION IF PRIOR ROOM OCCUPANT INFECTED * Prior room occupant infected; ^Any room occupant in prior 2 weeks infected
 NEW APPROACHES TO ROOM DECONTAMINATION
NEW APPROACHES TO ROOM DECONTAMINATION
 USE OF HPV TO REDUCE RISK OF ACQUISITION OF MDROs • • Design: 30 mo prospective cohort study with hydrogen peroxide vapor (HPV) intervention to assess risks of colonization or infection with MDROs Methods n • 12 mo pre-intervention phase followed by HPV use on 3 units for terminal disinfection Results Prior room occupant colonized or infected with MDRO in 22% of cases n Patients admitted to HPV decontaminated rooms 64% less likely to acquire any MDRO (95% CI, 0. 19 -0. 70) and 80% less likely to acquire VRE (95% CI, 0. 08 -0. 52) n Risk of C. difficile, MRSA and MDR-GNRs individually reduced but Passaretti CL, et al. Clin Infect Dis not significantly 2013; 56: 27 -35 n Proportion of rooms environmentally contaminated with MDROs n
USE OF HPV TO REDUCE RISK OF ACQUISITION OF MDROs • • Design: 30 mo prospective cohort study with hydrogen peroxide vapor (HPV) intervention to assess risks of colonization or infection with MDROs Methods n • 12 mo pre-intervention phase followed by HPV use on 3 units for terminal disinfection Results Prior room occupant colonized or infected with MDRO in 22% of cases n Patients admitted to HPV decontaminated rooms 64% less likely to acquire any MDRO (95% CI, 0. 19 -0. 70) and 80% less likely to acquire VRE (95% CI, 0. 08 -0. 52) n Risk of C. difficile, MRSA and MDR-GNRs individually reduced but Passaretti CL, et al. Clin Infect Dis not significantly 2013; 56: 27 -35 n Proportion of rooms environmentally contaminated with MDROs n
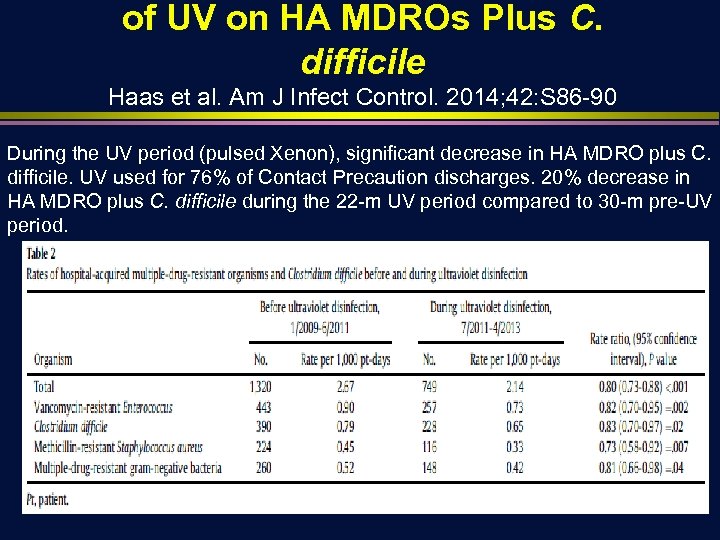 of UV on HA MDROs Plus C. difficile Haas et al. Am J Infect Control. 2014; 42: S 86 -90 During the UV period (pulsed Xenon), significant decrease in HA MDRO plus C. difficile. UV used for 76% of Contact Precaution discharges. 20% decrease in HA MDRO plus C. difficile during the 22 -m UV period compared to 30 -m pre-UV period.
of UV on HA MDROs Plus C. difficile Haas et al. Am J Infect Control. 2014; 42: S 86 -90 During the UV period (pulsed Xenon), significant decrease in HA MDRO plus C. difficile. UV used for 76% of Contact Precaution discharges. 20% decrease in HA MDRO plus C. difficile during the 22 -m UV period compared to 30 -m pre-UV period.
 FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentives goals tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by TJC Reduced funds for new infection prevention technologies
FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentives goals tied to quality goals State and federal laws legislating care issues Greater emphasis on infection prevention by TJC Reduced funds for new infection prevention technologies
 FUTURE OF INFECTION CONTROL • • Health insurance reimbursement (e. g. , BCBS) tied to meeting quality goals Employee incentive package involves metrics that are clinically meaningful and measurable. n n n Patient and employee satisfaction goals Fiscal goals, 4% operating margin Quality goals u Ventilator-associated pneumonia, 5 -10% below past FY u Central-line associated bacteremia, 5 -10% below past FY u Prophylactic antibiotics within one hour of surgical incision u Catheter-associated urinary tract infections, 5% below past FY
FUTURE OF INFECTION CONTROL • • Health insurance reimbursement (e. g. , BCBS) tied to meeting quality goals Employee incentive package involves metrics that are clinically meaningful and measurable. n n n Patient and employee satisfaction goals Fiscal goals, 4% operating margin Quality goals u Ventilator-associated pneumonia, 5 -10% below past FY u Central-line associated bacteremia, 5 -10% below past FY u Prophylactic antibiotics within one hour of surgical incision u Catheter-associated urinary tract infections, 5% below past FY
 Infection Prevention Goals (FY 2015) • • • Clean In, Clean Out-Increase hand hygiene among staff to 90% from October 1, 2014 -May 31, 2015 n FY 15 Performance-maintained compliance >90% in inpatient areas Clean In, Clean Out-Increase hand hygiene among staff to 90% from October 1, 2014 -May 31, 2015 n FY 15 Performance-maintained compliance >90% in outpatient areas Reduce SSI infections for colon surgeries and abdominal hysterectmoies by 5% below CY 2013 rate n CY 2013: 5. 17 SSIs/100 surgeries; 51 SSIs n Target rate: 4. 91 SSIs/100 surgeries; 48 SSIs
Infection Prevention Goals (FY 2015) • • • Clean In, Clean Out-Increase hand hygiene among staff to 90% from October 1, 2014 -May 31, 2015 n FY 15 Performance-maintained compliance >90% in inpatient areas Clean In, Clean Out-Increase hand hygiene among staff to 90% from October 1, 2014 -May 31, 2015 n FY 15 Performance-maintained compliance >90% in outpatient areas Reduce SSI infections for colon surgeries and abdominal hysterectmoies by 5% below CY 2013 rate n CY 2013: 5. 17 SSIs/100 surgeries; 51 SSIs n Target rate: 4. 91 SSIs/100 surgeries; 48 SSIs
 ‘Clean in, Clean Out’ • • At UNC Hospitals we "Clean in, Clean Out" : each employee is responsible for cleaning in and cleaning out any time s/he enters and exits a patient’s room. Each employee is asked to observe other employees and report on proper (or improper) hand hygiene and provide immediate feedback. Organizational hospital-wide quality goal tied to financial incentive. http: //www. youtube. com/watch? v=n. Sek 2 n. VUUx. M
‘Clean in, Clean Out’ • • At UNC Hospitals we "Clean in, Clean Out" : each employee is responsible for cleaning in and cleaning out any time s/he enters and exits a patient’s room. Each employee is asked to observe other employees and report on proper (or improper) hand hygiene and provide immediate feedback. Organizational hospital-wide quality goal tied to financial incentive. http: //www. youtube. com/watch? v=n. Sek 2 n. VUUx. M
 CMS’s Final Rule for FY 14 Inpatient Payments Penalize Hospitals 1% • • Penalize hospitals with the highest Healthcare Associated Condition rates a full 1% of their inpatient Medicare revenue, starting in FY 15 Use historical data from Hospital Compare First domain-Patient Safety; considers AHRQ patient safety indicator score (35%) Second domain-Infection rates for CLABSI and CAUTI (65%) in FY 2015; colon and abdominal hysterectomy in FY 2016 and C. difficile rates in FY 2017.
CMS’s Final Rule for FY 14 Inpatient Payments Penalize Hospitals 1% • • Penalize hospitals with the highest Healthcare Associated Condition rates a full 1% of their inpatient Medicare revenue, starting in FY 15 Use historical data from Hospital Compare First domain-Patient Safety; considers AHRQ patient safety indicator score (35%) Second domain-Infection rates for CLABSI and CAUTI (65%) in FY 2015; colon and abdominal hysterectomy in FY 2016 and C. difficile rates in FY 2017.
 CMS Penalty Potential Problems • No risk-adjustment for patient populations (i. e. , immunocompromised, AIDS, burn) known to be at higher risk for HAIs Large academic medical centers are more likely to fall into the penalty range due to high-risk patients • Chances that a large, urban, major teaching hospital that has large numbers of poor patients will get the HAC penalty is 62% • • • No clinical significance of HAI data cut-points (relies on arbitrary statistical cut-points-i. e. , lowest quartile) No validation of surveillance
CMS Penalty Potential Problems • No risk-adjustment for patient populations (i. e. , immunocompromised, AIDS, burn) known to be at higher risk for HAIs Large academic medical centers are more likely to fall into the penalty range due to high-risk patients • Chances that a large, urban, major teaching hospital that has large numbers of poor patients will get the HAC penalty is 62% • • • No clinical significance of HAI data cut-points (relies on arbitrary statistical cut-points-i. e. , lowest quartile) No validation of surveillance
 FUTURE OF INFECTION CONTROL • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals Public reporting of HAIs State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention
FUTURE OF INFECTION CONTROL • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals Public reporting of HAIs State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention
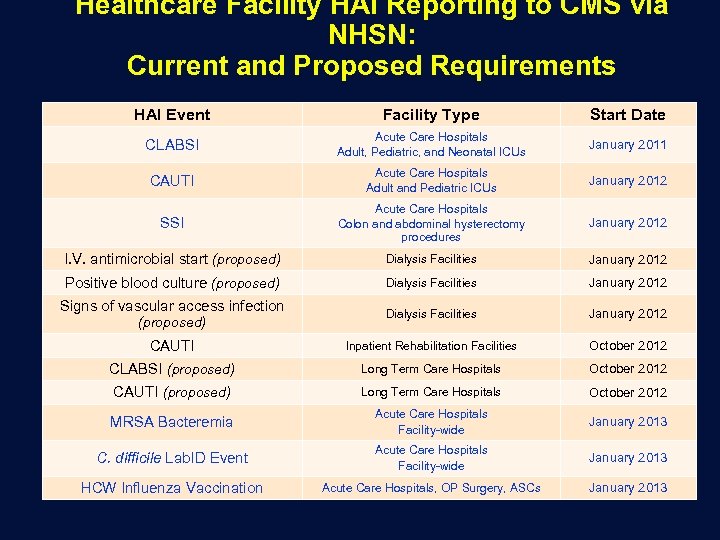 Healthcare Facility HAI Reporting to CMS via NHSN: Current and Proposed Requirements HAI Event Facility Type Start Date CLABSI Acute Care Hospitals Adult, Pediatric, and Neonatal ICUs January 2011 CAUTI Acute Care Hospitals Adult and Pediatric ICUs January 2012 SSI Acute Care Hospitals Colon and abdominal hysterectomy procedures January 2012 I. V. antimicrobial start (proposed) Dialysis Facilities January 2012 Positive blood culture (proposed) Dialysis Facilities January 2012 Signs of vascular access infection (proposed) Dialysis Facilities January 2012 CAUTI Inpatient Rehabilitation Facilities October 2012 CLABSI (proposed) Long Term Care Hospitals October 2012 CAUTI (proposed) Long Term Care Hospitals October 2012 MRSA Bacteremia Acute Care Hospitals Facility-wide January 2013 C. difficile Lab. ID Event Acute Care Hospitals Facility-wide January 2013 HCW Influenza Vaccination Acute Care Hospitals, OP Surgery, ASCs January 2013
Healthcare Facility HAI Reporting to CMS via NHSN: Current and Proposed Requirements HAI Event Facility Type Start Date CLABSI Acute Care Hospitals Adult, Pediatric, and Neonatal ICUs January 2011 CAUTI Acute Care Hospitals Adult and Pediatric ICUs January 2012 SSI Acute Care Hospitals Colon and abdominal hysterectomy procedures January 2012 I. V. antimicrobial start (proposed) Dialysis Facilities January 2012 Positive blood culture (proposed) Dialysis Facilities January 2012 Signs of vascular access infection (proposed) Dialysis Facilities January 2012 CAUTI Inpatient Rehabilitation Facilities October 2012 CLABSI (proposed) Long Term Care Hospitals October 2012 CAUTI (proposed) Long Term Care Hospitals October 2012 MRSA Bacteremia Acute Care Hospitals Facility-wide January 2013 C. difficile Lab. ID Event Acute Care Hospitals Facility-wide January 2013 HCW Influenza Vaccination Acute Care Hospitals, OP Surgery, ASCs January 2013
 CMS – HAI DIAGNOSES FOR WHICH REIMBURSEMENT NOT ALLOWED, FY 2013 • Inpatient Prospective Payment System (IPPS)- hospitals do not receive the higher payment for cases when one of the selected conditions is acquired during hospitalization n CAUTI n Vascular catheter-associated infection n SSI-mediastinitis, certain orthopedic procedures (spine, neck, shoulder, elbow), bariatric surgery for obesity, cardiac
CMS – HAI DIAGNOSES FOR WHICH REIMBURSEMENT NOT ALLOWED, FY 2013 • Inpatient Prospective Payment System (IPPS)- hospitals do not receive the higher payment for cases when one of the selected conditions is acquired during hospitalization n CAUTI n Vascular catheter-associated infection n SSI-mediastinitis, certain orthopedic procedures (spine, neck, shoulder, elbow), bariatric surgery for obesity, cardiac
 CHANGING REGULATORY ENVIRONMENT • New paradigm = All HAIs are preventable Public reporting of HAIs n Lack of reimbursement for HAIs n Public awareness of the issue n • Problems with paradigm shift Publically reported rates are NOT risk adjusted for patient risk factors n Unfunded mandate n May impact on accuracy of surveillance n No reimbursement for HAIs even if hospital followed all recommended practices n
CHANGING REGULATORY ENVIRONMENT • New paradigm = All HAIs are preventable Public reporting of HAIs n Lack of reimbursement for HAIs n Public awareness of the issue n • Problems with paradigm shift Publically reported rates are NOT risk adjusted for patient risk factors n Unfunded mandate n May impact on accuracy of surveillance n No reimbursement for HAIs even if hospital followed all recommended practices n
 FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals Public reporting of HAIs State and federal laws legislating care issues MRSA active surveillance n Influenza vaccination n • • Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals Public reporting of HAIs State and federal laws legislating care issues MRSA active surveillance n Influenza vaccination n • • Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
 FUTURE OF INFECTION CONTROL • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals Public reporting of HAIs State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission (sometimes do not use evidence-based guidelines for citations, e. g. , 7 -day endoscope reprocessing; risk assessments-1 m LLD, 20 m Glut) Reduced funds for new infection prevention
FUTURE OF INFECTION CONTROL • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Health insurance reimbursement and employee incentive payments tied to quality goals Public reporting of HAIs State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission (sometimes do not use evidence-based guidelines for citations, e. g. , 7 -day endoscope reprocessing; risk assessments-1 m LLD, 20 m Glut) Reduced funds for new infection prevention
 JOINT COMMISSION: NATIONAL PATIENT SAFETY GOALS • Old Comply with CDC hand hygiene guidelines n Manage as sentinel events all HAI-related deaths n • New (2009 -2015) Implement evidence-based practices to prevent HAIs due to MDROs (MRSA, VRE, MDR-GNR, C. difficile) n Implement evidence-based practices to prevent CLA-BSIs n Implement best practices to prevent SSIs n
JOINT COMMISSION: NATIONAL PATIENT SAFETY GOALS • Old Comply with CDC hand hygiene guidelines n Manage as sentinel events all HAI-related deaths n • New (2009 -2015) Implement evidence-based practices to prevent HAIs due to MDROs (MRSA, VRE, MDR-GNR, C. difficile) n Implement evidence-based practices to prevent CLA-BSIs n Implement best practices to prevent SSIs n
 FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Public reporting of HAIs State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
FUTURE OF INFECTION CONTROL • • • Limited infection prevention resources Implementation of guidelines/standards, bundles and new technology demonstrated to reduce HAIs Public reporting of HAIs State and federal laws legislating care issues Greater emphasis on infection prevention by The Joint Commission Reduced funds for new infection prevention technologies
 FUTURE OF INFECTION CONTROL Hospitals-budget cuts, job loses • • Hospitals reduce spending (job losses, service reductions) due to reduced revenues (reimbursement for service [2% reduction Medicare], no new volumes) Utilizing new technology to improve outcomes is superior to changing behavior New technology have played a critical role in reducing HAIs (CHG-Alc for SSI, CHG sponge, antiseptic/antibiotic impregnated central lines) Reduced hospital margins will force hospitals to limit investments in new technology
FUTURE OF INFECTION CONTROL Hospitals-budget cuts, job loses • • Hospitals reduce spending (job losses, service reductions) due to reduced revenues (reimbursement for service [2% reduction Medicare], no new volumes) Utilizing new technology to improve outcomes is superior to changing behavior New technology have played a critical role in reducing HAIs (CHG-Alc for SSI, CHG sponge, antiseptic/antibiotic impregnated central lines) Reduced hospital margins will force hospitals to limit investments in new technology
 CONCLUSIONS • • • Healthcare-associated infections are associated with significant patient morbidity and mortality Implementation of bundles (IHI) and products demonstrated to reduce HAIs (e. g. , CLA-BSI) Compliance with infection prevention recommendations needed to prevent HAIs
CONCLUSIONS • • • Healthcare-associated infections are associated with significant patient morbidity and mortality Implementation of bundles (IHI) and products demonstrated to reduce HAIs (e. g. , CLA-BSI) Compliance with infection prevention recommendations needed to prevent HAIs
 DISCUSSION TOPICS Impact of healthcare-associated infections Challenges in infection prevention
DISCUSSION TOPICS Impact of healthcare-associated infections Challenges in infection prevention
 CONCLUSIONS • Current challenges n n n Increased emphasis on preventing HAIs Increased demands on IP time Lack of compliance with hand hygiene and guidelines/policies Institution of IHI bundles and other CQI activities Public reporting, mandated vaccines, mandated practices Multidrug pathogens: VRSA, MDR-GNRs, XDR-TB Emerging pathogens: C. difficile, norovirus, MERS-Co. V, D 68, Ebola Public desire for 0 rate of healthcare-associated infections Older and sicker patient population Insurance reimbursement tied to quality goals (eg, HAI reductions) Reduced hospital margins, reduced investments in new technology
CONCLUSIONS • Current challenges n n n Increased emphasis on preventing HAIs Increased demands on IP time Lack of compliance with hand hygiene and guidelines/policies Institution of IHI bundles and other CQI activities Public reporting, mandated vaccines, mandated practices Multidrug pathogens: VRSA, MDR-GNRs, XDR-TB Emerging pathogens: C. difficile, norovirus, MERS-Co. V, D 68, Ebola Public desire for 0 rate of healthcare-associated infections Older and sicker patient population Insurance reimbursement tied to quality goals (eg, HAI reductions) Reduced hospital margins, reduced investments in new technology
 THANK YOU! www. disinfectionandsterilization. o rg
THANK YOU! www. disinfectionandsterilization. o rg


