be31e0046c5396d379d0902127dc931c.ppt
- Количество слайдов: 19

Further Tales from the British National Health Service. By Julian Le Grand Health Affairs, May/June 2002 Presented by Robin Mc. Cutcheon 1

Overview of article Ø Le Grand zeros in on the Labor Party’s attempts to reform the British National Health Service (NHS). Ø He argues that the reforms do not deliver on the Party’s promises of improved services, lesser wait times for medical services, and improved reallocation of resources. Ø Possible explanations are capacity constraints, and conflicting incentive structures for key players. 2

British National Health System ~ A Bit of History (1) NHS Inception Date: July 5, 1948. Core principle: healthcare is a basic human right. v. Mission: to provide fair & equal access to medical care. v. All under one roof: Hospitals, Family Practitioner services (Doctors, Pharmacists, opticians, dentists) Community-based services v. Originally Funded by: taxes & small fees 3

British National Health System ~ A Bit of History (2) Original structure of the NHS v. Family doctor (GP)—Gatekeeper to NHS services v. Community Health Centers (publicly used and funded) offered range of medical services v. Health Authorities (NHS Trusts)—hospitals/clinics, that serve a particular geographic region and employ doctors, nurses, pharmacists, therapists, etc. 4

British National Health System ~ A Bit of History (3) §In the 1980 s, NHS finally recognizes financial insolubility, cannot provide every medical treatment to everyone §Attempts made to reallocate resources equitability within the country §Performance indicators introduced §Concern about rising costs §Waiting for medical care & treatment common 5

British National Health System ~ A Bit of History (4) In 1991: NHS introduces new structure to system: v. Internal Market—doctors (now called GP fundholders) & health authorities (now called Trusts) given budgets to buy health care from providers (hospitals & other health organizations) v. Stipulation: any leftover “profit” was to be used for the benefit of patients, improving care v. Non-Fundholders were still controlled by Health Authorities (Has bought health care in bulk from NHS Trusts) v. Patients of GP Fundholders often able to get treatment faster than patients of nonfundholders…leads to accusations that NHS is 2 tiered system and contradicts founding principles (fair & equal access) 6
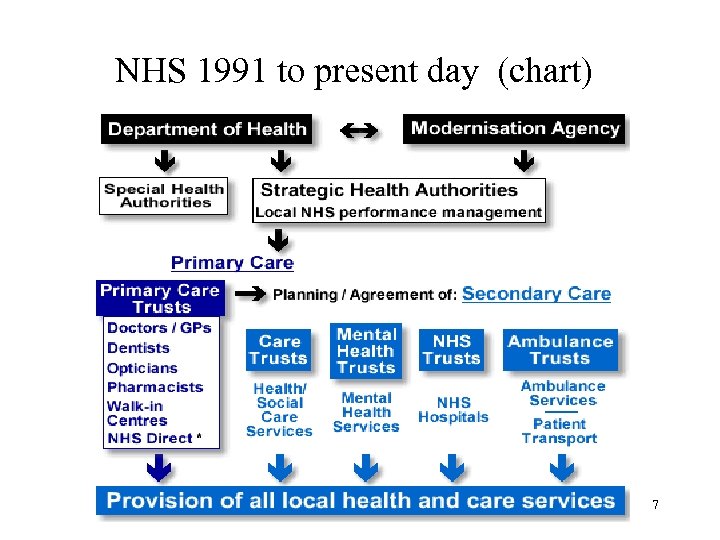
NHS 1991 to present day (chart) 7

Margaret Thatcher’s Internal Quasi-Market ~1991 v The government provides the money, yet “competition” exists between doctors (purchasers) and clinics/hospitals (providers) v Any surplus of funds was discouraged by insisting that surplus monies were to be spent to benefit patients & facilities v Considered to be “American-style” competition, to replace the Soviet-style command & control system. 8

Quasi-Market outcomes-efficiency? (1) Little improvement in overall efficiency, what little there is attributed to fundholder thrift relative to non-fundholders Ø Thatcher Gov’t didn’t sponsor its own evaluative studies Ø Few independent research firms that could undertake a large scale study Ø Plethora of confounding factors, time lags, measurement problems 9

Quasi-Market outcomes-efficiency? (2) § outreach services were provided more by fundholders than nonfundholders, § obtained faster admission & got better response from providers (hospitals) § kept Rx cost down § able to generate more surplus ($) than health authorities § also, fundholders given more money to play with than non-fundholders ü Hardly any “cream-skimming”—because fundholders were not liable for extra costs associated with very expensive patients, so health care was not withheld from these patients. ü Patient & purchasers choices continue to be limited 10

Le Grand Reviews Blair’s Reform of NHS ~ 1998 (1) v 1997 New Labour Party elected to power (Tony Blair), promises to rearrange and revise NHS, abolish the Internal Market, move away from competition and toward collaboration Ø Quasi-markets abolished, but purchasers (doctors) and providers (hospitals/clinics) still separate Ø Cooperative relationships encouraged, competition discouraged, accountability & harsher penalties instituted Ø At least 6 new Oversight agencies established, the top 2 are: § National Institute for Clinical Effectiveness (NICE)-assesses clinical & cost effectiveness of drugs/medical procedures and whether or not it should be available for NHS patients § Commission for Health Improvement (CHIMP)- an investigative agency that reports on performance of NHS institutions 11

Review of NHS Reform ~ 1998 (2) Two innovations v NHS Direct~ a national telephone service to obtain advice, manned by nurses v Walk-In Centers~ a walk-in clinic where medical advice can be obtained without appointment, also manned by nurses 12

Review of NHS Reform ~ 1998 (3) Wider levels of health control by government: Ø Community Health Improvement Programs~ in which health authorities, local trusts (hospitals/clinics) local gov’t agencies agree on a program that establishes public health & health service goals to be achieved in the community, thus earmarking funds for improvement. Ø Performance Assessment Framework~ central gov’t monitoring of all NHS organizations…includes • Health outcome indicators, fair access, effective delivery of appropriate health care, patient’s experience. 13

Review of NHS Reform ~ 1998 (4) Payment systems altered and rewarded based on: v Doctors now paid by block-contract instead of by capitation v Team bonuses—extra pay for teams of frontline hospital staff if ambitious target levels met v STAR Ratings—performance ratings based on how a Trust has performed against a set of Performance Indicators (PI) and a Clinical Governance Review (CGR) by CHIMP. ü ü ü 1. Patient’s opinion of a job well done 2. Standard of treatment & recovery of patient 3. Management of Trust 4. Patient’s access to quality 5. Improvement of overall health of population 14

Review of NHS Reform ~ 1998 (5) Overall pattern: ü Quasi-market abolished, market based competitive pressures eliminated ü Proliferation of central agencies & control instruments increased ü Successful reorganization and improved allocation of resources? Difficult to determine due to definition of what constitutes success. 15

Le Grand says the numbers speak for themselves v Finished Consultant Episode (FCE), a standard measure of hospital activity rose (1996 -97 to 1999 -00) by 2. 7%, which is a slower rate than the 4. 4% from Thatcher’s period of rule (1991 -97) v Total number of GP consultations fell from 270 Million (Thatcher years) to 251 Million (Blair years) v Wait times (for medical care) fell by 8. 5% (for people waiting 12 months or more for treatment) and 13. 3% (for people waiting 15 months or more) v Le Grand doesn’t give specific numbers for the above percentages, so we don’t know the magnitude of change 16

Do Expenditures change the story? Le Grand allows that changes in expenditures do not reflect changes in resources due to changes in input prices of the activities within the health care services offered. § § (1) Cost-Weighted Activity Index (CWAI) = different activities weighted by their unit costs (2) Volume of Resources Used dispensed by Hospital & Community Health Services (HCHS) = expenditures adjusted for changes in prices ü Divide (1) by (2) = Index of the units of resource used per unit of activity (crude indicator of the efficiency of resource use) § 1991 -95 upswing in efficiency (Thatcher years) § 1996 -99 downswing of efficiency (Blair years) • Health expenditures as a %GDP increasing, compare 5. 3% (1999 -00) to 7. 4% (2003 -04) —why so little increase in H/C activity? ? ? 17

Le Grand Surmises Why Ø Capacity—Shortage of Medical Staff, hospital acute care & Nursing home beds Ø Incentives—currently threaten job security & job loss if managers, regional director, chief exec’s of Trusts/Health Authorities & Primary Care Trusts don’t deliver on set goals (which have them competing against each other) AND at the same time they must collaborate with each other, i. e. , share good practices, and operate in the wider NHS interest—obviously the incentives breed mistrust and confusion Ø NHS Consultants (doctors) are paid for eleven sessions per week & are free to work additional hours in the private sector, where they can keep all their profits. Le Grand sees this as detrimental to NHS objectives Ø No Incentives for improvement from internal market 18

Works cited Le Grand, Julian. , “Further Tales from the British National Health Service, ” Health Affairs, May/June 2002, Vol. 21, Issue 3, p 116 -128. Le Grand, Julian. , “Competition, Cooperation, or Control? Tales from the British National Health Service, ” Health Affairs, May/June 1999: p 27 -39. The National Health Service—The NHS Explained http: //www. nhs. uk/ 19
be31e0046c5396d379d0902127dc931c.ppt