395932ff13b42f5bb4dcc83469e5f430.ppt
- Количество слайдов: 80

Fluids, Electrolytes and Shock Tom Archer, MD, MBA UCSD Anesthesia

Outline • • • Three fluid compartments (ICF, ISF, IVF) Three membranes Osmosis– theory and clinical Shock-- tissue needs and cardiac output Water and electrolytes in general (3 overlapping systems) • Hyponatremia– appropriate and inappropriate secretion of ADH • Hypernatremia and K+ disorders

Three fluid compartments Intracellular fluid (ICF) Interstitial fluid (ISF) Intravascular fluid (IVF)

Fractions to remember: 2/3, 3/4 • TBW (42 L) = 2/3 of body weight (70 kg). • ICF (28 L) = 2/3 of TBW. • ECF (14 L) = 1/3 of TBW. • Interstitial fluid (ISF, 10. 5 L) = ¾ of ECF • Intravascular fluid (IVF, 3. 5 L) = ¼ of ECF.
Three membranes Cell membrane Non- brain capillary endothelium Brain capillary endothelium (“bloodbrain barrier– BBB”)

Solutes Ions: Na+ , Cl-, K+, PO 4 --Sugars: glucose, mannitol Large molecules (colloids): albumin, hetastarch

Two types of membranes • Non-brain capillary endothelium is permeable to everything but colloid, therefore, only colloid is osmotically active at non-brain capillary membrane.

Two types of membranes • Cell membrane and healthy BBB are only permeable to water, therefore, all ions, sugars and large molecules are osmotically active at cell membrane and BBB.

Blood-brain barrier • Behaves just like the cell membrane– a tight, lipid rich membrane which is impermeable to everything but water (and lipophilic drugs).

Osmosis • What is osmosis? • Answer: diffusion of water down its concentration gradient.

For all osmosis questions: • What is the solute? • What is the membrane? • Is the membrane permeable to the solute? • If not, solute will "pull" water across the membrane.

Clinical examples of osmotic effects • Brain trauma: mannitol to shrink normal brain to make room for mass lesion. • Brain trauma or blood loss: Hypertonic saline to shrink normal brain or expand ISF and IVF. • Hyperglycemia causes osmotic diuresis and hypovolemia. • Hyperglycemia causes brain dehydration (with potential for cerebral edema with rapid correction of hyperglycemia).
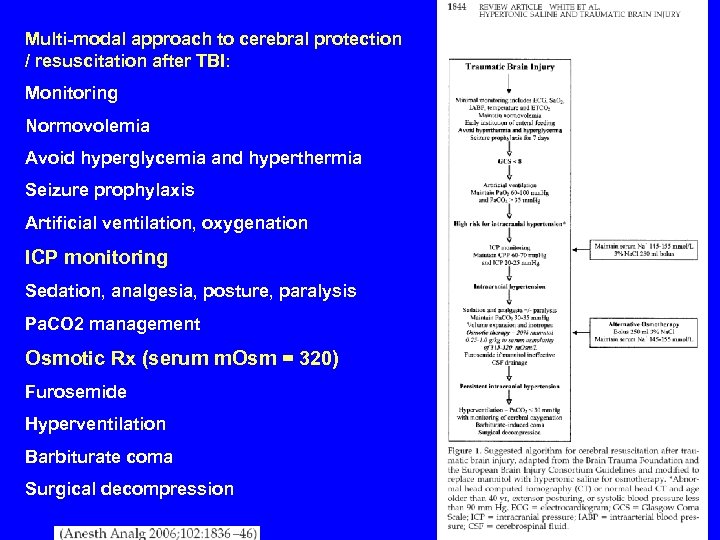
Multi-modal approach to cerebral protection / resuscitation after TBI: Monitoring Normovolemia Avoid hyperglycemia and hyperthermia Seizure prophylaxis Artificial ventilation, oxygenation ICP monitoring Sedation, analgesia, posture, paralysis Pa. CO 2 management Osmotic Rx (serum m. Osm = 320) Furosemide Hyperventilation Barbiturate coma Surgical decompression

Edema vs. Osmotic effects • Edema can be purely hydrostatic (6 hours head down during surgery) • Edema can be d/t low oncotic pressure (hypoalbuminemia in cirrhosis) • Can be due to both factors.

Intravenous fluids • “Crystalloids” – Normal saline (just Na. Cl). – Lactated ringers – Plasmalyte – Normosol – Last 3 have K+ and other stuff (acetate, Mg++, etc. )

Practical aspects • Crystalloids enter entire ECF: ISF (3/4 of ECF) and IVF (1/4 of ECF). • 3 or 4: 1 for replacement of blood loss with crystalloid • Colloids only enter IVF (in short term– 16 hour half-time for entrance into ISF) • 1: 1 replacement of blood loss with colloid

Homeostatic systems for water, electrolytes and circulation • Renin-angiotensin-aldosterone system (RAAS) • Osmoreceptors, thirst, ADH (V 1 vasocon and V 2 tubular) • Sympathetic nervous system • Aortic, carotid, atrial and ventricular stretch receptors-Atrial Natriuretic Peptide (ANP), Brain Natriuretic Peptide (BNP), vasogenic intestinal peptide… and others. • Kidney (glomerulus, tubules, collecting duct, glomerulotubular balance, macula densa).
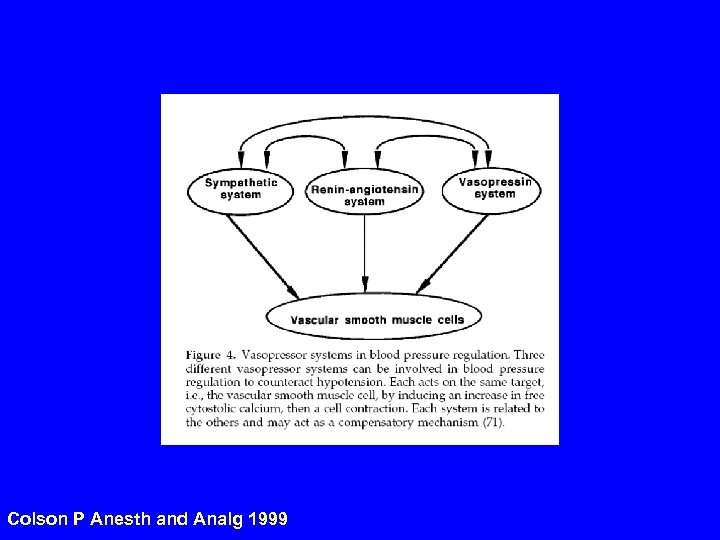
Colson P Anesth and Analg 1999

Fast and slow components of fluid volume homeostasis. • RAAS: angiotensin II is fast / aldosterone is slow. • ADH (“arginine vasopressin”): ADH in high concentration is immediate vasopressor on V 1 receptor. • ADH in low concentration retains free water (slowly) in collecting duct via V 2 stimulation.
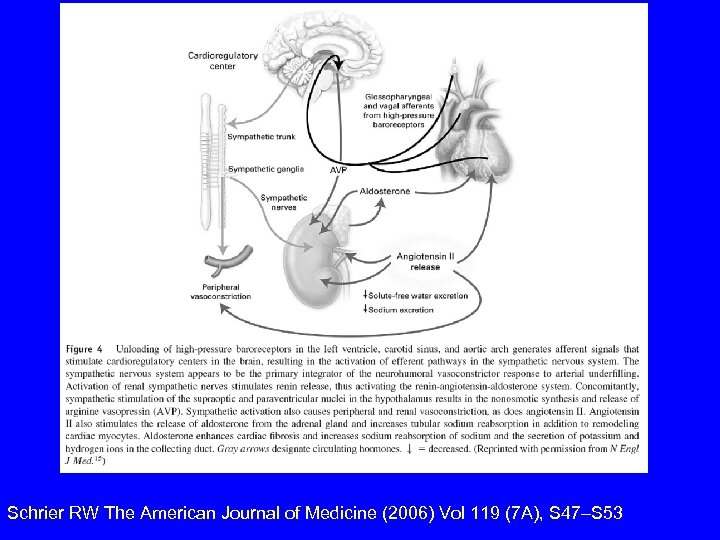
Schrier RW The American Journal of Medicine (2006) Vol 119 (7 A), S 47–S 53
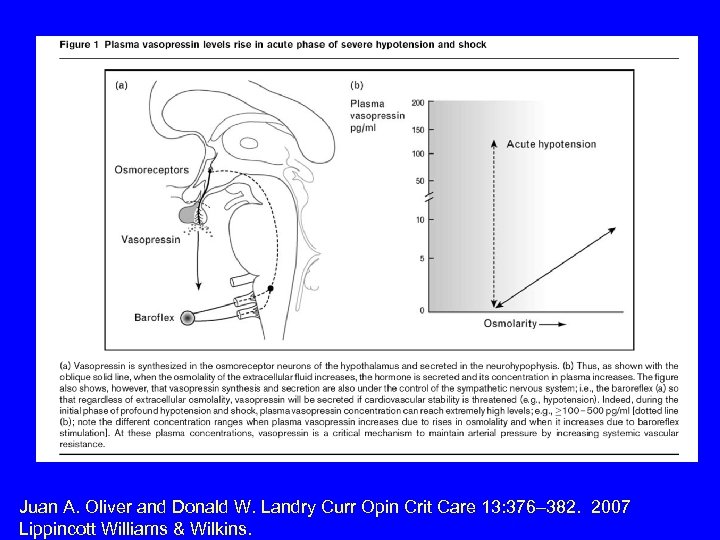
Juan A. Oliver and Donald W. Landry Curr Opin Crit Care 13: 376– 382. 2007 Lippincott Williams & Wilkins.

“Syndrome of Inappropriate ADH” A Garbage Term? • Seen in neurological disease or injury. • Seen in pulmonary disease (tumors, TB, etc. ) • ADH release by pain, stress, opioids and nausea is also “inappropriate. ” • Excessive and counter-productive ADH release in CHF and cirrhosis is also “inappropriate. ”

Big picture– Shock (1) • Inadequate circulation and supply of nutrients to tissues– either at the macro or micro level. • Intravascular volume loss (hemorrhage, burns, GI losses). Preload problem. • Cardiogenic (pump failure). • Spinal cord transection / anaphylaxis. Preload and afterload problems. • Microcirculatory failure by RBC sludging, stasis or microcirculatory coagulation (sepsis, DIC).

Causes of shock • Preload (How do we judge preload? CVP? , PAOP? , LVEDV? , SPV? , PPV? , SVV? ) • Pump (contractility, d. P/d. T) • Afterload (SVR) • Microcirculatory (endothelial) failure (sepsis, preeclampsia, DIC, ARDS, hyperglycemia, etc. )
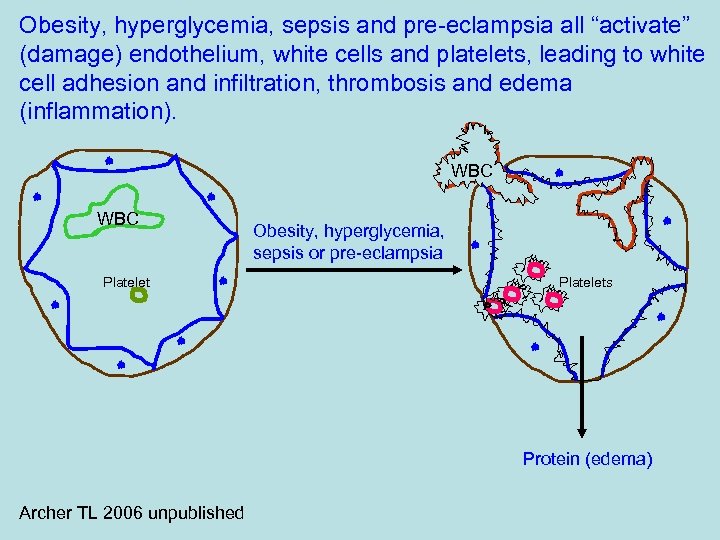
Obesity, hyperglycemia, sepsis and pre-eclampsia all “activate” (damage) endothelium, white cells and platelets, leading to white cell adhesion and infiltration, thrombosis and edema (inflammation). WBC Platelet Obesity, hyperglycemia, sepsis or pre-eclampsia Platelets Protein (edema) Archer TL 2006 unpublished

Big picture– Shock (2) • Hemodynamic manipulations of HR, SVR, preload, afterload, contractility, etc. may provide limited help to microcirculation deranged by sepsis (for example). • Hemodynamic manipulations may simply “buy us time” and support patient while we treat the underlying cause of the shock. • Endothelium must heal!
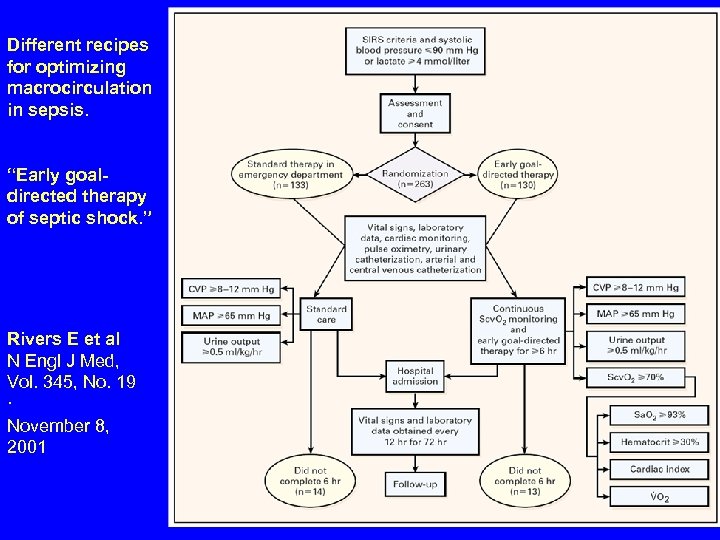
Different recipes for optimizing macrocirculation in sepsis. “Early goaldirected therapy of septic shock. ” Rivers E et al N Engl J Med, Vol. 345, No. 19 · November 8, 2001

Like the giant plant in “Little Shop of Horrors”, body tissues say, “Feed me!”
“Feed me!” Arteriole Capillary Hungry tissue says, “Feed me!” to pre-capillary sphincter.

Case #1 “The patient is overloaded…” “The patient is dry…” • 24 yo male, previously healthy, 4 days s/p GSW abdomen with shock, peritonitis, sepsis, hypotension. Controlled ventilation. BP = 90/60, HR = 130. • Weight gain 4 kg since admission. • Albumin = 1. 9. BUN / creat = 48 / 1. 9. • PAOP = 5 mm Hg. • Systolic pressure variation: 18%
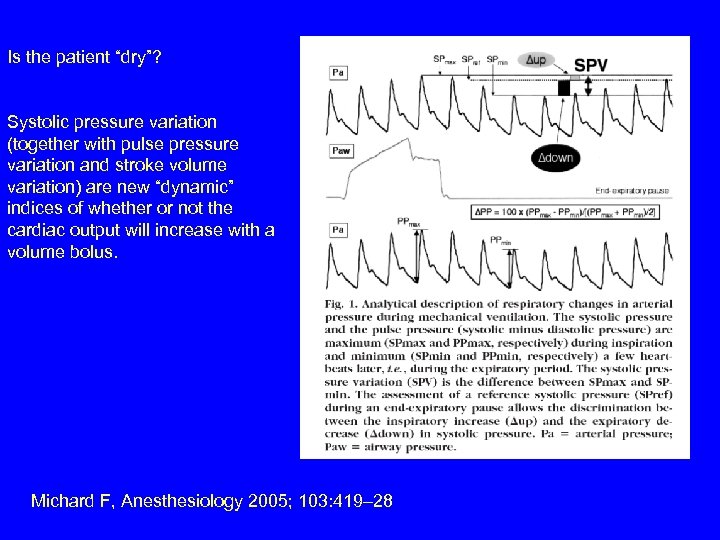
Is the patient “dry”? Systolic pressure variation (together with pulse pressure variation and stroke volume variation) are new “dynamic” indices of whether or not the cardiac output will increase with a volume bolus. Michard F, Anesthesiology 2005; 103: 419– 28
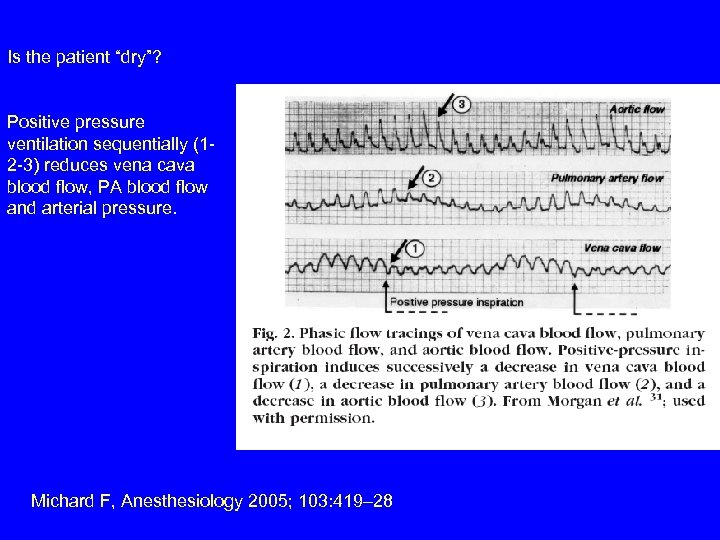
Is the patient “dry”? Positive pressure ventilation sequentially (12 -3) reduces vena cava blood flow, PA blood flow and arterial pressure. Michard F, Anesthesiology 2005; 103: 419– 28

Case #1 “The patient is overloaded…” “The patient is dry…” • Patient has low INTRAVASCULAR volume, but also has excessive INTERSTITIAL fluid (edema). • This is totally consistent with the “leaky capillary” picture of sepsis. • Systolic pressure variation >13% suggests fluid bolus will increase CO. CO is “fluid responsive”.

The Three Hyponatremias • Isotonic (proteins or lipids dilute Na+ on bulk basis). Often called “artifactual. ” “Watery” portion of serum has normal tonicity. • Hypertonic (osmotic agent “sucks” water out of ICF, diluting Na+, but tonicity stays high). • Hypotonic. By far the most common (and hardest to understand).
![Isotonic hyponatremia • Hyperproteinemia or hyperlipidemia dilutes out the Na+. [Na+] in the water Isotonic hyponatremia • Hyperproteinemia or hyperlipidemia dilutes out the Na+. [Na+] in the water](https://present5.com/presentation/395932ff13b42f5bb4dcc83469e5f430/image-35.jpg)
Isotonic hyponatremia • Hyperproteinemia or hyperlipidemia dilutes out the Na+. [Na+] in the water portion of the blood is normal. • Glycine solution with TURP. • Treatment is to work up and treat underlying cause
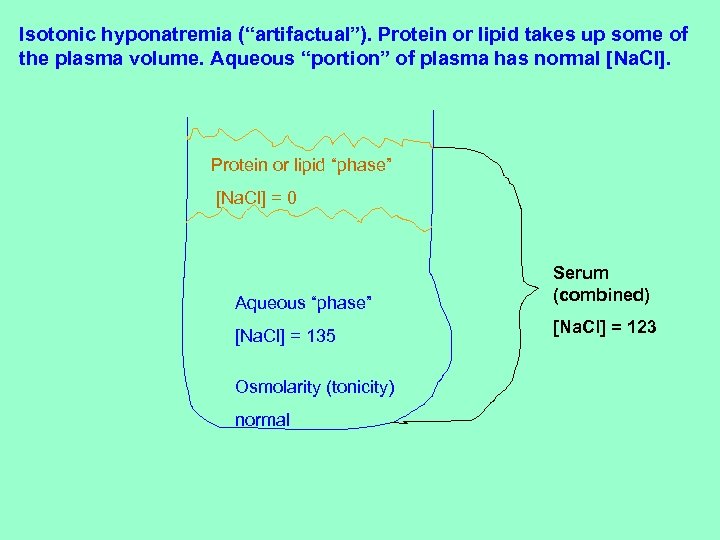
Isotonic hyponatremia (“artifactual”). Protein or lipid takes up some of the plasma volume. Aqueous “portion” of plasma has normal [Na. Cl]. Protein or lipid “phase” [Na. Cl] = 0 Aqueous “phase” Serum (combined) [Na. Cl] = 135 [Na. Cl] = 123 Osmolarity (tonicity) normal
![Hypertonic Hyponatremia-- causes • Due to hyperglycemia, mannitol or glycerol. • Decreased [Na+] in Hypertonic Hyponatremia-- causes • Due to hyperglycemia, mannitol or glycerol. • Decreased [Na+] in](https://present5.com/presentation/395932ff13b42f5bb4dcc83469e5f430/image-37.jpg)
Hypertonic Hyponatremia-- causes • Due to hyperglycemia, mannitol or glycerol. • Decreased [Na+] in serum, but osmolality is high (>290), due to sugar in the blood. • Sugar has “sucked” water out of cells, into the ECF. Water dilutes Na+.
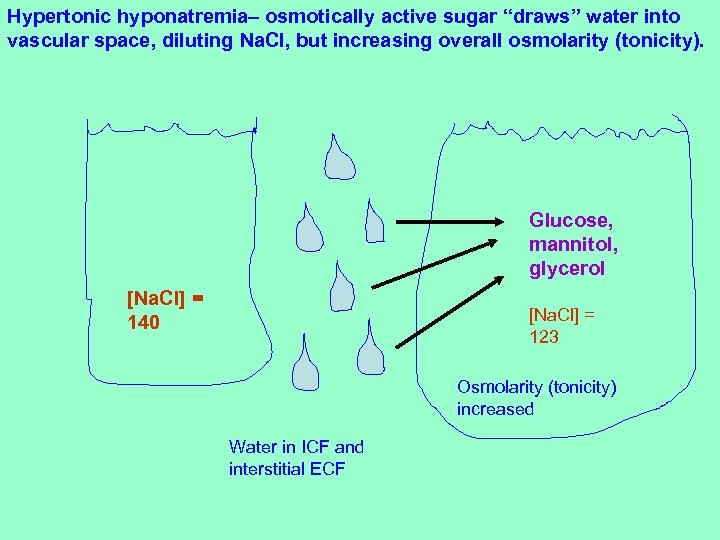
Hypertonic hyponatremia– osmotically active sugar “draws” water into vascular space, diluting Na. Cl, but increasing overall osmolarity (tonicity). Glucose, mannitol, glycerol [Na. Cl] = 140 [Na. Cl] = 123 Osmolarity (tonicity) increased Water in ICF and interstitial ECF

Hypertonic Hyponatremia-- Rx • Insulin to slowly reduce blood glucose. • NS volume replacement. • Complications of rapid reduction of serum glucose and tonicity: hypoglycemia, cerebral edema

Four causes of increased ADH • Normal osmotic ADH release: osmoreceptors in hypothalamus release ADH via posterior pituitary in response to serum m. Osm > 290. Makes physiological sense. Stress-related ADH release (pain, nausea, opioids, running a marathon). • Non-osmotic increased ADH (in hypovolemia): – “Defense of intravascular volume”-- severe volume contraction. Makes physiological sense. – Diuretics, GI losses, burns, hemorrhage, sweating, adrenal insufficiency. • Non-osmotic increased ADH (causing hypervolemia): – Pathological states (CHF, cirrhosis, pulmonary, CNS). These are classically called “SIADH”.

All these conditions are associated with increased ADH secretion. Achinger, Moritz, and Ayus • Dysnatremias: Why Are Patients Still Dying? Southern Medical Journal • Volume 99, Number 4, April 2006
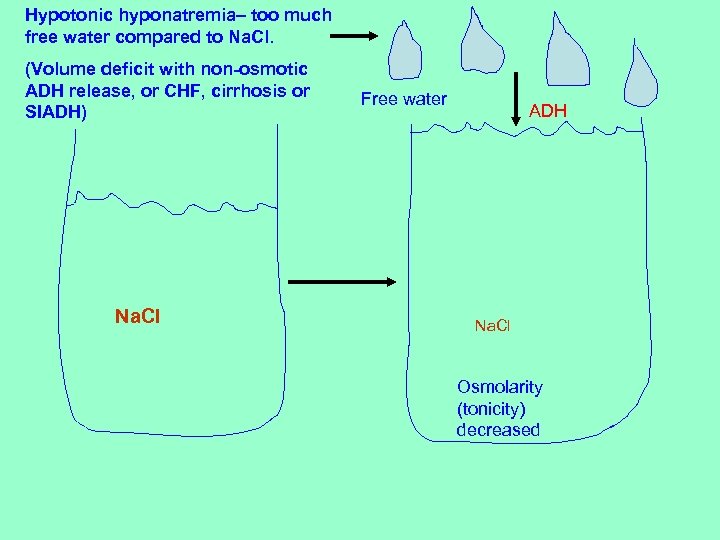
Hypotonic hyponatremia– too much free water compared to Na. Cl. (Volume deficit with non-osmotic ADH release, or CHF, cirrhosis or SIADH) Na. Cl Free water ADH Na. Cl Osmolarity (tonicity) decreased

Stress- induced, non-osmotic ADH release: • This is why we DON’T give D 51/4 NS in surgery. • This is why we DO give NS, Normosol or LR. • We don’t give free water because of kidney’s reduced ability to excrete it (due to non-osmotic ADH release).

Hypotonic, Hypovolemic Hyponatremia-- Rx • Volume restoration with NS if hypovolemic (GI losses, diuretics). • Explanation: Severe hypovolemia causes nonosmotic ADH release. Body tries to “defend intravascular volume” by secreting ADH. • Volume restoration suppresses non-osmotic ADH release and cures hyponatremia by allowing free water excretion.

Hypotonic, Hypervolemic Hyponatremia-- Rx • Fluid restriction if hypervolemic (CHF, liver failure). • Diuretics (causing Na+ and water loss) are currently used for ECF overload. We want to get rid of water, but we get rid of Na+ as well. • Emerging Rx: “Aquaretics” are ADH V 2 receptor antagonists which prevent inappropriate free water retention in CHF or cirrhosis. Courtesy Dr. Jaydeep Shah

Case #2: Perioperative hyponatremia • 34 yo female, no significant past medical history. • Elective L/S BTL 0900. During the surgery, D 5 ¼ NS at 125 cc/ hr. • Pt in PACU until afternoon. “Too sedated to go home. ” Got IV meperidine. No PO intake, IV D 5 1/4 NS continued. • 2: 45 AM next day, pt. C/O headache, verbal order for Tylenol #3. • At 9: 00 AM, nurse tells surgeon of a sodium of 127 m. Eq/L. No • new orders, IV fluids were continued. • At 1: 30 pm, pt. lethargic and pain medications, pain meds held. • At 3: 30 pm, she had sz and respiratory failure. The patient intubated and ventilated. Serum sodium 122 m. Eq/L. Achinger, Moritz, and Ayus • Dysnatremias: Why Are Patients Still Dying? Southern Medical Journal • Volume 99, Number 4, April 2006

Case #2: Perioperative hyponatremia Stress, pain, nausea all cause increased ADH secretion from posterior pituitary. Free water administration with D 5 1/4 NS allows free water retention. Biggest danger in children, menstruating females and patients having suffered hypoxic episodes. Achinger, Moritz, and Ayus • Dysnatremias: Why Are Patients Still Dying? Southern Medical Journal • Volume 99, Number 4, April 2006
![How aggressively do we Rx hyponatremic encephalopathy? • Depends on symptoms, not the [Na++]. How aggressively do we Rx hyponatremic encephalopathy? • Depends on symptoms, not the [Na++].](https://present5.com/presentation/395932ff13b42f5bb4dcc83469e5f430/image-49.jpg)
How aggressively do we Rx hyponatremic encephalopathy? • Depends on symptoms, not the [Na++]. • In symptomatic hyponatremic encephalopathy, use 3% saline until sx improve.

Case #3 Hyponatremic encephalopathy • 31 yo female collapses 30 min after running marathon. Disoriented and SOB. • Crackles in all lung fields. CXR pulmonary edema. [Na+] = 126 m. Eq / L. • What is going on?

Case #3 Hyponatremic encephalopathy • Patient had been told to “drink as much water as possible to prevent dehydration. ” • Increased ADH with stress + free water leads to hyponatremia. • Pulmonary edema d/t cerebral edema. • Rx is 3% saline both encephalopahy and pulmonary edema resolved. • Sports drinks are hypotonic. Athletes need to drink only when thirsty.

Case #4 Hyponatremic encephalopathy • 72 yo male in nursing home. S/P neurogenic bladder followed by TURP. • On nasal DDAVP HS to avoid incontinence at night. [Na+] = 139 m. Eq / L. • Staff requests increased DDAVP to BID, to prevent incontinence during PT.

Case #4 Hyponatremic encephalopathy • Two days later patient becomes incoherent and lethargic. • [Na+] = 108 m. Eq / L. • What is going on? • What should we do?
![Case #4 Hyponatremic encephalopathy • 3% saline given until sx improved at [Na+] = Case #4 Hyponatremic encephalopathy • 3% saline given until sx improved at [Na+] =](https://present5.com/presentation/395932ff13b42f5bb4dcc83469e5f430/image-54.jpg)
Case #4 Hyponatremic encephalopathy • 3% saline given until sx improved at [Na+] = 122 m. Eq / L, then stopped. DDAVP was stopped. • Patient diuresed promptly with a rapid rise in serum [Na+]. • “Best management would have been to continue DDAVP and restrict fluid to prevent excessively rapid correction. ” • Get a consult!

Case #5 Hyponatremic encephalopathy • 69 yo female for screening colonoscopy. • Oral polyethylene glycol bowel prep the day before (Go-lytely) • Pt. gets nauseated and vomits repeatedly along with having diarrhea. Gets HA. • Husband finds her unresponsive next AM. Pt. has tonic-clonic sz. Serum [Na+] = 114. • What is going on?

Case #5 Hyponatremic encephalopathy • Dehydration with bowel prep and vomiting thirst + increased ADH. • Free water retention hyponatremia. • Rx: 3% saline until sz stop and mental status better. Restore volume also with NS. • Was patient also taking a thiazide diuretic?

Rx of hyponatremia Based on symptoms– not numbers.

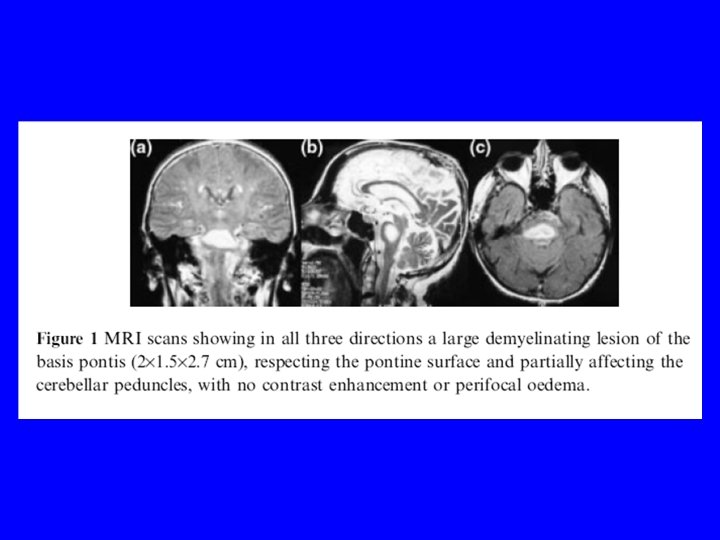
Case #6 Central Pontine Myelinolysis • 79 yo female with Hx of HBP Rx’d with thiazides. Had elective colonoscopy after bowel prep. • Six hours after the examination of confusion followed by sz. The patient stayed comatose. Serum [Na+] = 108. • Brain-CT was normal. No signs of cerebral edema, but Rx with IV dexamethasone was begun. (3% NS used to correct)… hyponatraemia (>2 m. Eq/L/hr) up to 132. • Pt. regained consciousness but was unable to speak and swallow. This condition remained stable for 3 days, when … neurological evaluation was… (requested). Spengos K. Vassilopoulou S. Tsivgoulis G. Dimitrakopoulos A. Toulas P. Vassilapoulos D. Hyponatraemia and central pontine myelinolysis after elective colonoscopy. [Letter] European Journal of Neurology. 12(4): 322 -3, 2005 Apr.

Hyponatremia– clinical manifestations • Asymptomatic > 125 m. Eq / L • 110 – 125 m. Eq / L: MS changes (confusion, seizures, coma). • < 110 m. Eq / L: Medical emergency

Hypotonic Hyponatremia-- Rx • Slow correction (0. 5 m. Eq / L / hr) to avoid central pontine myelinolysis. • Get consultation and go very slow!

Case #7 Dialysis patient • 57 yo obese male, DM, HBP, CRF on dialysis. Needs AV shunt revision. • How do we evaluate this patient? • Be highly specific.

Case #7 Dialysis patient • Airway, IV access. Don’t use IV dialysis catheter. • Exercise tolerance, chronic and recent. • Has patient been getting dialyzed with a venous catheter? If so, when was the last time? Needs to be dialyzed day before surgery. • BP, lungs (rales? ), can he lie flat? • Do we need to recheck lytes AM of surgery if patient was dialyzed day before?

Case #8 Do we discontinue ACEI and ARBs before surgery? • 48 yo male with DM and HBP, on insulin and enalapril, for Whipple procedure, (resection head of pancreas for CA). • What are the advantages or disadvantages of D/Cing the enalapril prior to surgery?

Case #8 Do we discontinue ACEI and ARBs before surgery? • Worry is “refractory hypotension” due to vasodilatory effect of anesthetics plus loss of angiotensin II vasoconstriction. • Controversial area. • If we do not D/C ACEI and ARBs, we “go easy” with the vasodilating anesthetics and have the vasopressors ready. • Big volume loss procedure would predispose us to D/C enalapril.

Case #9: Hyponatremic encephalopathy • 78 yo female, incoherent, limping, bruise on face. Bruise over L hip L femur fx. • Totally OK until recently. Started on new BP (thiazide diuretic) med 2 weeks ago • Serum Na+ = 104 m. Eq / L. • What is going on ?

Case #9 Hyponatremic encephalopathy • Thiazide diuretic blocks Na+ reabsorption in distal tubule and cortical collecting duct. Causes volume loss and trouble diluting urine. • Free water retention (+ weight gain) from increased ADH. • Patients should be weighed 48 hrs. after starting thiazide. • Check lytes in patients on diuretics (we are checking K+ AND Na+).

Hypernatremia– causes (1) • Free water loss: – Evaporative loss of water (sweat, burns). – Lungs (insensible loss) – Renal (nephrogenic diabetes insipidus) – CNS (lack of ADH secretion).

Hypernatremia– causes (2) • Limited water intake – Comatose or disoriented patients – Hypothalamic tumor / disordered thirst mechanism

Hypernatremia– causes (3) • Increased body sodium content – Excessive salt intake – Decreased sodium excretion

Hypernatremia– clinical manifestations • Intracellular dehydration • CNS tissue volume loss (across BBB). Possible tearing of cerebral vessels. Mannitol sometimes used to increase [Na+] to decrease ICP. • Restlessness, tremor, ataxia, seizures, death.

Hypernatremia– Rx • Replace free water, orally or IV • For every liter of free water deficit, [Na+] will increase 3 m. Eq / L. • As with hyponatremia, correct slowly. Brain cells accommodate by increasing osmolarity. Too rapid decrease in extracellular [Na+] can cause brain cell swelling.

Potassium and Phosphate • K+ and PO 4 --- are the most abundant intracellular ions. MOST K+ AND PO 4 --ARE INSIDE CELLS! • K+ gradient across cell membrane sets the resting transmembrane potential. • PO 4 --- essential for DNA, ATP, etc.

Hypokalemia • Inside of nerve / muscle cells are increasingly negative due to hyperpolarized cell membrane. • EKG changes, decreased contractility • Neuromuscular changes– cramps, weakness, paresthesias

Hypokalemia-- causes • GI losses (NG suction, diarrhea, vomiting, bowel obstruction, fistulas, bowel prep) • Renal losses (diuretics, mineralocorticoid excess, nephropathy) • Intracellular shifts (alkalosis, insulin, TPN, catecholamine effect) • Inadequate intake (diet, IV fluids).

Hypokalemia-- Rx • Most of deficit is intracellular. • Hyperkalemia is always a danger. • Replace SLOWLY. Oral is best. 40 m. Eq q 6 h. IV can replace up to 25 m. Eq / hr.

Hyperkalemia • Transmembrane potential becomes less negative- goes toward easy depolarization. • EKG is most sensitive indicator: peaked T waves- prolonged P-R interval- absent P waves- widened QRS- sine wave- Vtach- V-fib- asystole

Hyperkalemia--- causes • Renal failure (can’t excrete) • Drugs (succinylcholine, K+ sparing diuretics, ACE inhibitors. • Hemolysis. • Tissue breakdown (burns, crush injury) • Acidosis • Exogenous K+ (old blood). • Factitious– hemolyzed blood sample, contamination from K+ infusion.

Hyperkalemia--- Rx Short term-- minutes (temporizing): 1) Ca. Cl 2 5 -10 mg/kg. Stabilizes cardiac cell membrane. 2) Push K+ into cells: – – Produce alkalosis (hyperventilation, Na. HCO 3) Insulin and glucose administration 3) Beta agonist (albuterol, epi) Longer term-- hours: 4) Increase K+ excretion (loop diuretics, dialysis, lactulose to produce diarrhea-- Kayexelate enemas no longer used)

The End
395932ff13b42f5bb4dcc83469e5f430.ppt