100336e209bcb97805593c3537492de5.ppt
- Количество слайдов: 65
 Fertility Sparing in Gynecological Cancers Fırat Ortaç, MD Güven Hospital Department of Obstetrics and Gynecology
Fertility Sparing in Gynecological Cancers Fırat Ortaç, MD Güven Hospital Department of Obstetrics and Gynecology
 Cancer Treatment Objective Cure Adverse Effects l l Psychological effects Cosmetic problems Loss of organ function Sexual and reproductive dysfunction Fertility sparing surgery
Cancer Treatment Objective Cure Adverse Effects l l Psychological effects Cosmetic problems Loss of organ function Sexual and reproductive dysfunction Fertility sparing surgery
 Goals of Fertility-Sparing Surgery(FSS) l. Preservation of reproductive potential l. Preservation of hormonal function l. Preservation of healthy body image l. No compromise in curability
Goals of Fertility-Sparing Surgery(FSS) l. Preservation of reproductive potential l. Preservation of hormonal function l. Preservation of healthy body image l. No compromise in curability
 FSS Objectives l. Similiar oncologic outcomes to standard therapy l. Favorable obstetric outcome l. Benefits > risks l. Low morbidity
FSS Objectives l. Similiar oncologic outcomes to standard therapy l. Favorable obstetric outcome l. Benefits > risks l. Low morbidity
 Defining prognostic factors Evidence-based Data Physician Fertility Sparing Surgery
Defining prognostic factors Evidence-based Data Physician Fertility Sparing Surgery
 Fertility-Sparing in Gynecologic Oncology l The patient and family must be: «aware of the problem «involved in the final decision l Once the fertility has been completed, demolitive procedure should be considered
Fertility-Sparing in Gynecologic Oncology l The patient and family must be: «aware of the problem «involved in the final decision l Once the fertility has been completed, demolitive procedure should be considered
 Fertility-Sparing in Gynecologic Oncology l. Age l. Desire to preserve fertility l. Tumor factors Histologic type, grade, others l. Stage of disease
Fertility-Sparing in Gynecologic Oncology l. Age l. Desire to preserve fertility l. Tumor factors Histologic type, grade, others l. Stage of disease
 Principles in Treatment of Early. Stage Cervical Cancer Patient’s general status Desire of fertility Tumor factors « Depth and width of invasion « Size of cervical lesion « LVSI
Principles in Treatment of Early. Stage Cervical Cancer Patient’s general status Desire of fertility Tumor factors « Depth and width of invasion « Size of cervical lesion « LVSI
 Traditional treatment of early stage cervical cancer beyond micro-invasion Radical hysterectomy + PPLND Loss of fertility
Traditional treatment of early stage cervical cancer beyond micro-invasion Radical hysterectomy + PPLND Loss of fertility
 LVSI Pelvik lenf nodu metastazı Pelvik rekürens Lenfadenektomi – Radikal cerrahi
LVSI Pelvik lenf nodu metastazı Pelvik rekürens Lenfadenektomi – Radikal cerrahi
 Spread of Cervical Cancer Laterally (Dominant) Parametrium Vertically (rare) Stage Ib and IIa 0% Stage IIb 20%
Spread of Cervical Cancer Laterally (Dominant) Parametrium Vertically (rare) Stage Ib and IIa 0% Stage IIb 20%
 Fertility Sparing Surgery in Early-Stage Cervical Cancer ID<3 mm LVSI(-) CONIZATION MARGIN (-) FOLLOW-UP
Fertility Sparing Surgery in Early-Stage Cervical Cancer ID<3 mm LVSI(-) CONIZATION MARGIN (-) FOLLOW-UP
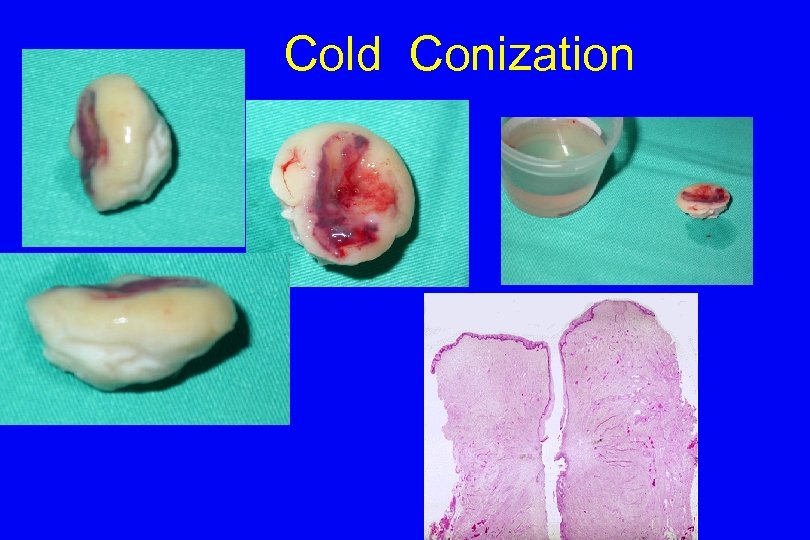 Cold Conization
Cold Conization
 CONIZATION < 10 mm Does not affect fertility potential Clin. Exp. Obstet. Gynecol, 1992: 19(1): 40 -2
CONIZATION < 10 mm Does not affect fertility potential Clin. Exp. Obstet. Gynecol, 1992: 19(1): 40 -2
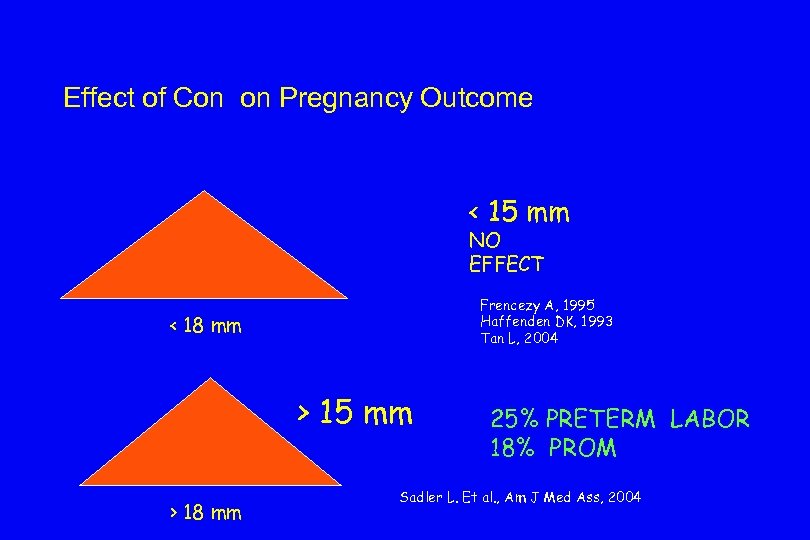 Effect of Con on Pregnancy Outcome < 15 mm NO EFFECT Frencezy A, 1995 Haffenden DK, 1993 Tan L, 2004 < 18 mm > 15 mm > 18 mm 25% PRETERM LABOR 18% PROM Sadler L. Et al. , Am J Med Ass, 2004
Effect of Con on Pregnancy Outcome < 15 mm NO EFFECT Frencezy A, 1995 Haffenden DK, 1993 Tan L, 2004 < 18 mm > 15 mm > 18 mm 25% PRETERM LABOR 18% PROM Sadler L. Et al. , Am J Med Ass, 2004
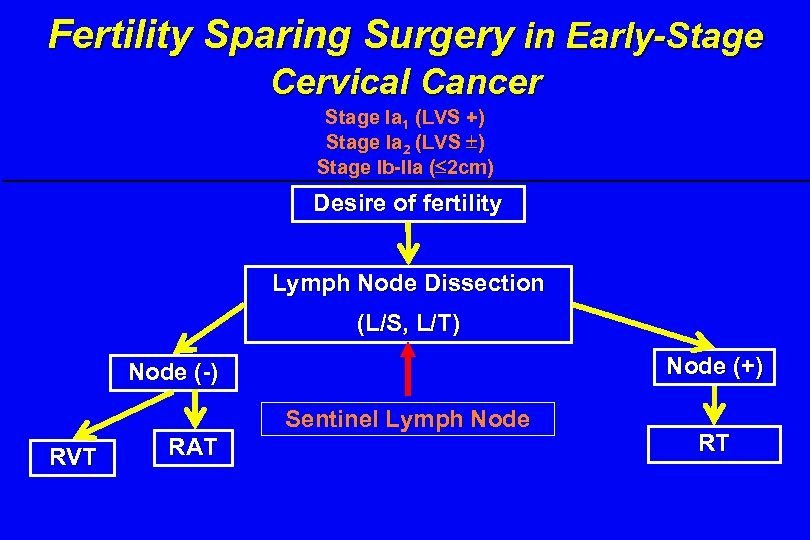 Fertility Sparing Surgery in Early-Stage Cervical Cancer Stage Ia 1 (LVS +) Stage Ia 2 (LVS ) Stage Ib-IIa ( 2 cm) Desire of fertility Lymph Node Dissection (L/S, L/T) Node (+) Node (-) Sentinel Lymph Node RVT RAT RT
Fertility Sparing Surgery in Early-Stage Cervical Cancer Stage Ia 1 (LVS +) Stage Ia 2 (LVS ) Stage Ib-IIa ( 2 cm) Desire of fertility Lymph Node Dissection (L/S, L/T) Node (+) Node (-) Sentinel Lymph Node RVT RAT RT
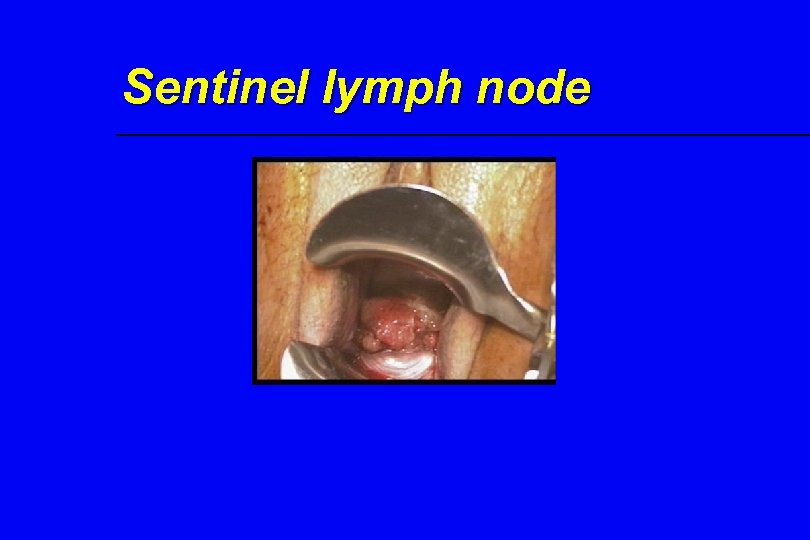 Sentinel lymph node
Sentinel lymph node
 Radical Trachelectomy 1994 Dargent
Radical Trachelectomy 1994 Dargent
 Vaginal Radical Trachelectomy (VRT) in Early-Stage Cervical Cancar by Dargent in Lyon, France Modification of the Schauta-Stoeckel technique of vaginal radical hysterectomy L/S Pelvic lymphadenectomy Preservation of the upper endocervix and uterine corpus
Vaginal Radical Trachelectomy (VRT) in Early-Stage Cervical Cancar by Dargent in Lyon, France Modification of the Schauta-Stoeckel technique of vaginal radical hysterectomy L/S Pelvic lymphadenectomy Preservation of the upper endocervix and uterine corpus
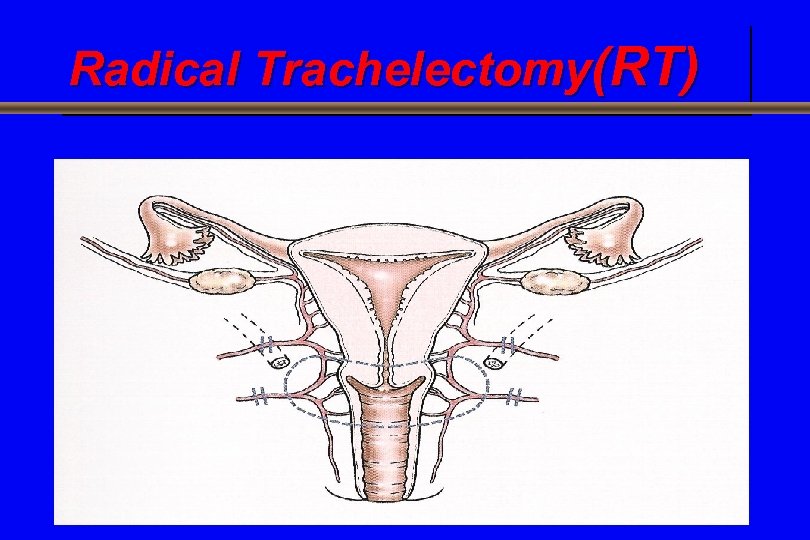 Radical Trachelectomy(RT)
Radical Trachelectomy(RT)
 VRT-Ab. RT Indications l Patient who desires preservation of fertility l FIGO Stage Ia 1 (+LVSI), Ia 2, Ib 1 l Lesions 2 cm in diameter l Limited endocervical involvement - MRI and colposcopy
VRT-Ab. RT Indications l Patient who desires preservation of fertility l FIGO Stage Ia 1 (+LVSI), Ia 2, Ib 1 l Lesions 2 cm in diameter l Limited endocervical involvement - MRI and colposcopy
 Surgıcal procedure § Lymph node dissection(Sentinel lymph node) § Parametrectomy § Trachelectomy (FS analyse- free margin 5 -8 mm) § Cervical circlage
Surgıcal procedure § Lymph node dissection(Sentinel lymph node) § Parametrectomy § Trachelectomy (FS analyse- free margin 5 -8 mm) § Cervical circlage
 RT Feasibility « No evidence of lymph node metastasis (Frozen section at L/S)(ultrastaging) « Upper endocervical margins free of tumor (Frozen section)
RT Feasibility « No evidence of lymph node metastasis (Frozen section at L/S)(ultrastaging) « Upper endocervical margins free of tumor (Frozen section)
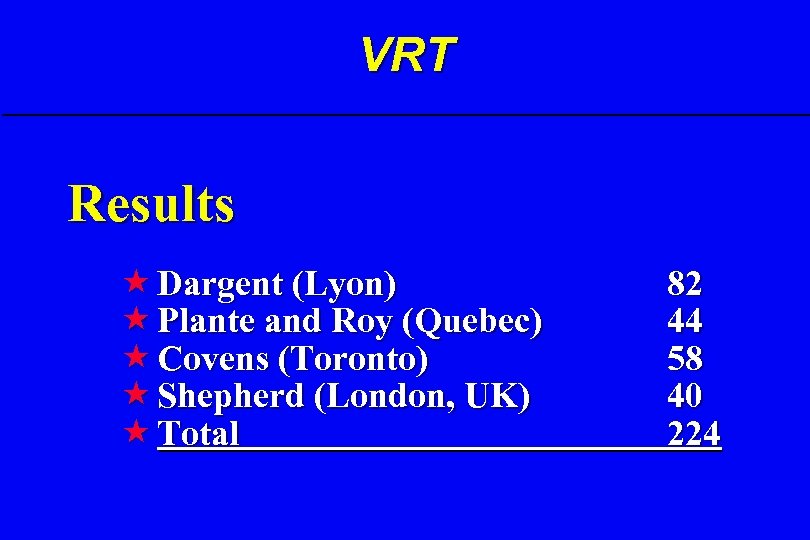 VRT Results « Dargent (Lyon) « Plante and Roy (Quebec) « Covens (Toronto) « Shepherd (London, UK) « Total 82 44 58 40 224
VRT Results « Dargent (Lyon) « Plante and Roy (Quebec) « Covens (Toronto) « Shepherd (London, UK) « Total 82 44 58 40 224
 VRT Oncologic Outcome (N: 24) Follow-up (months) Recurrences « Parametrium « Pelvic side wall « Distant 30 7(3. 1%) 3 1 3 No cervico-uterine recurrence
VRT Oncologic Outcome (N: 24) Follow-up (months) Recurrences « Parametrium « Pelvic side wall « Distant 30 7(3. 1%) 3 1 3 No cervico-uterine recurrence
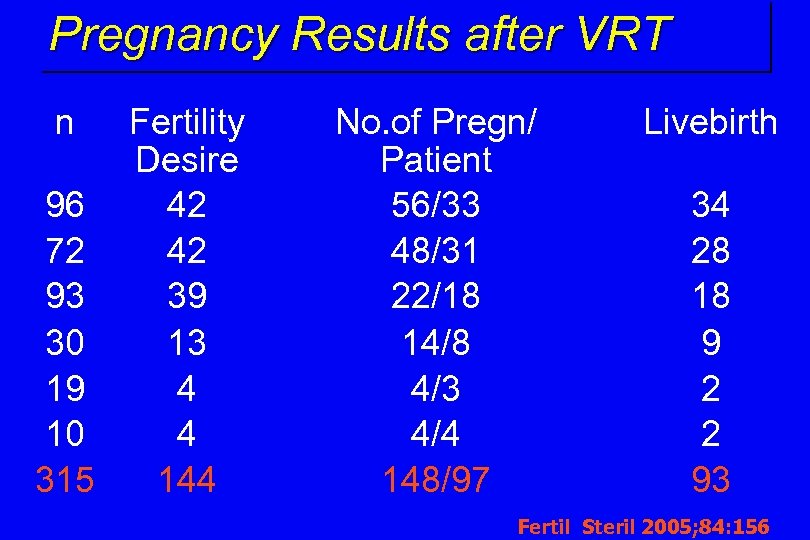 Pregnancy Results after VRT n Fertility Desire 96 42 72 42 93 39 30 13 19 4 10 4 315 144 No. of Pregn/ Patient 56/33 48/31 22/18 14/8 4/3 4/4 148/97 Livebirth 34 28 18 9 2 2 93 Fertil Steril 2005; 84: 156
Pregnancy Results after VRT n Fertility Desire 96 42 72 42 93 39 30 13 19 4 10 4 315 144 No. of Pregn/ Patient 56/33 48/31 22/18 14/8 4/3 4/4 148/97 Livebirth 34 28 18 9 2 2 93 Fertil Steril 2005; 84: 156
 VRT Conclusions l Abdominal way is possible l The risk of recurrence is unchanged l Fertility is preserved l But pregnancies are at high risk l An international study is required to confirm indications and limits of this conservative technique
VRT Conclusions l Abdominal way is possible l The risk of recurrence is unchanged l Fertility is preserved l But pregnancies are at high risk l An international study is required to confirm indications and limits of this conservative technique
 Preserving Fertility in Endometrial Cancer 2% -14 % of endometrial cancer 40 years Up to 25% PCOS G 1 Early stage Respond to progestin treatment
Preserving Fertility in Endometrial Cancer 2% -14 % of endometrial cancer 40 years Up to 25% PCOS G 1 Early stage Respond to progestin treatment
 Preserving Fertility in Endometrial Cancer Stage Ia, G 1 Standart treatment TAH + BSO
Preserving Fertility in Endometrial Cancer Stage Ia, G 1 Standart treatment TAH + BSO
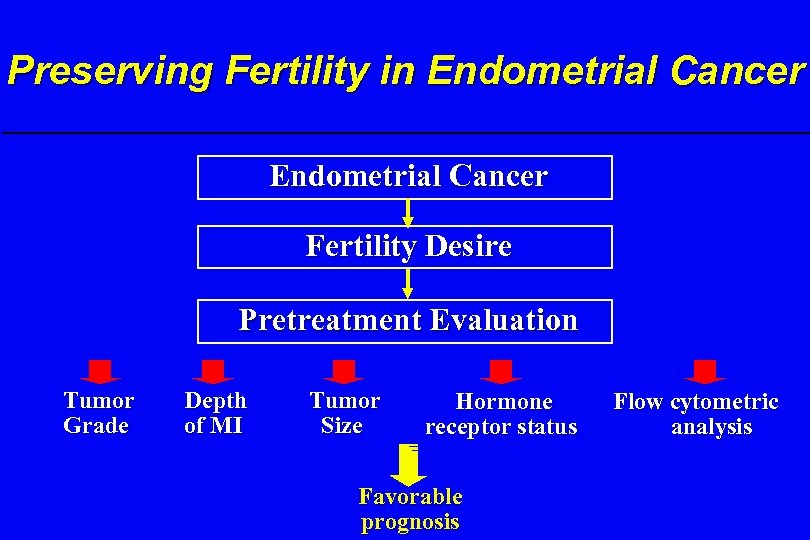 Preserving Fertility in Endometrial Cancer Fertility Desire Pretreatment Evaluation Tumor Grade Depth of MI Tumor Size Hormone receptor status Favorable prognosis Flow cytometric analysis
Preserving Fertility in Endometrial Cancer Fertility Desire Pretreatment Evaluation Tumor Grade Depth of MI Tumor Size Hormone receptor status Favorable prognosis Flow cytometric analysis
 Preserving Fertility in Endometrial Cancer Inclusion Criteria Ø Ø Ø Age < 40 years Nulliparous status Endometrioid Carcinoma G 1 Presence of Pg. R Normal serum levels of CA 125 (<35 u/m. L) and CEA (< 5 ng/m. L) Ø Tumor DNA index < 1. 3 Ø Absence of MI or extrauterine spread (by vaginal USG and MRI) , surgıcal staging
Preserving Fertility in Endometrial Cancer Inclusion Criteria Ø Ø Ø Age < 40 years Nulliparous status Endometrioid Carcinoma G 1 Presence of Pg. R Normal serum levels of CA 125 (<35 u/m. L) and CEA (< 5 ng/m. L) Ø Tumor DNA index < 1. 3 Ø Absence of MI or extrauterine spread (by vaginal USG and MRI) , surgıcal staging
 Pretreatment Evaluation l. History (infertility. . . ) l. Physicial Examination l. TVUSG l. D&C l. Abdominopelvic/ endovajinal coil MRI l. Ca-125 Laparoscopic evaluation or Staging Laparotomy Response to Progesterone
Pretreatment Evaluation l. History (infertility. . . ) l. Physicial Examination l. TVUSG l. D&C l. Abdominopelvic/ endovajinal coil MRI l. Ca-125 Laparoscopic evaluation or Staging Laparotomy Response to Progesterone
 Preserving Fertility in Endometrial Cancer Ø Explain the patient the risk of conservative treatment Ø Evaluate the patient for prognosis Ø Medical treatment (Megestrol acetate 40 -160 mg/d , MPA 30 mg/d Tamoxifen 30 mg/d or Gn. RHa) Ø Ø Repeated D&C; hysteroscopy (+tubal blockage) No residual disease Ø Assisted reproduction Ø Elective hysterectomy when the patient no longer desires to maintain fertility
Preserving Fertility in Endometrial Cancer Ø Explain the patient the risk of conservative treatment Ø Evaluate the patient for prognosis Ø Medical treatment (Megestrol acetate 40 -160 mg/d , MPA 30 mg/d Tamoxifen 30 mg/d or Gn. RHa) Ø Ø Repeated D&C; hysteroscopy (+tubal blockage) No residual disease Ø Assisted reproduction Ø Elective hysterectomy when the patient no longer desires to maintain fertility
 Progestogenic Agents MPA Megace IUD / Prog Response Rate Hyperplasia with Atypia End. Ca l Duration of Treatment Range Median l Recurrens Hyperplasia with Atypia End. Ca l l 30/mg/ day 40 -160 /mg/day %83 -94 %57 -75. 6 3 -6 months 9 months % 13 % 11 -50
Progestogenic Agents MPA Megace IUD / Prog Response Rate Hyperplasia with Atypia End. Ca l Duration of Treatment Range Median l Recurrens Hyperplasia with Atypia End. Ca l l 30/mg/ day 40 -160 /mg/day %83 -94 %57 -75. 6 3 -6 months 9 months % 13 % 11 -50
 There is no consensus Which progesterone formulation to use What schedule to use What dose to use How long to treat How often to resample
There is no consensus Which progesterone formulation to use What schedule to use What dose to use How long to treat How often to resample
 Preserving Fertility in Endometrial Cancer 72 cases in literature Positive response histologically documented 55 cases (76%)
Preserving Fertility in Endometrial Cancer 72 cases in literature Positive response histologically documented 55 cases (76%)
 Endometrial Cancer Literature Overview (1966 -2006) l No pts. = 53 l 80% were nulliparous l In 96% of them the tumor was well differentiated l At least 36 pregn. were obtained by ART l 70% of pts. Underwent a hysterectomy after completing gestation
Endometrial Cancer Literature Overview (1966 -2006) l No pts. = 53 l 80% were nulliparous l In 96% of them the tumor was well differentiated l At least 36 pregn. were obtained by ART l 70% of pts. Underwent a hysterectomy after completing gestation
 Uterine Leiomyosarcoma (LMS) l Diagnosis «Pre-operative? «Intra-operative frozen section? «Histopathological evaluation of hysterectomy or myomectomy specimen.
Uterine Leiomyosarcoma (LMS) l Diagnosis «Pre-operative? «Intra-operative frozen section? «Histopathological evaluation of hysterectomy or myomectomy specimen.
 Uterine LMS Incidence patients operated for presumed leiomyoma 0. 1 -0. 3%
Uterine LMS Incidence patients operated for presumed leiomyoma 0. 1 -0. 3%
 Fertility Sparing Surgery in LMS l Safe margin: 3 -5 mm. ? l <10 mitoses/per 10 HPF l Solitary pedinculated mass
Fertility Sparing Surgery in LMS l Safe margin: 3 -5 mm. ? l <10 mitoses/per 10 HPF l Solitary pedinculated mass
 Fertility Sparing Surgery in LMS Accurately restage the patients «Color doppler USG «Hysteroscopy «Chest X-ray «MRI or CT scan
Fertility Sparing Surgery in LMS Accurately restage the patients «Color doppler USG «Hysteroscopy «Chest X-ray «MRI or CT scan
 Fertility Sparing Surgery in LMS • Delivery Cesarean section Multiple uterine biopsies should be taken.
Fertility Sparing Surgery in LMS • Delivery Cesarean section Multiple uterine biopsies should be taken.
 Fertility Sparing Surgery in LMS Lissoni A (Gynecol Oncol 70(3): 348 -50 (1998) l l l l l Between 1982 -1996 (8 patients) Median age: 29 All nulliparous Tumor was confined to myoma Mean mitotic count 6 per 10 HPF 3 pregnancies Median follow-up 42 months 7 patients alive One patient died (26 months after diagnosis).
Fertility Sparing Surgery in LMS Lissoni A (Gynecol Oncol 70(3): 348 -50 (1998) l l l l l Between 1982 -1996 (8 patients) Median age: 29 All nulliparous Tumor was confined to myoma Mean mitotic count 6 per 10 HPF 3 pregnancies Median follow-up 42 months 7 patients alive One patient died (26 months after diagnosis).
 Fertility Sparing in Epithelial Ovarian Cancer and Borderline Tumors
Fertility Sparing in Epithelial Ovarian Cancer and Borderline Tumors
 Fertility Sparing Surgery in Epithelial Ovarian Cancer and Borderline Tumors Optimal Staging: l USO or cystectomy (in BOT) l Peritoneal washing and cytology l Inspection of the contralateral ovarian surface, biopsies of any suspicious lesions Wedge resection of the opposite ovary? l Staging biopsies of the peritoneal cavity l Sampling of retroperitoneal lymph nodes or radical lymphadenectomy since 1990 l Omentectomy, appendectomy.
Fertility Sparing Surgery in Epithelial Ovarian Cancer and Borderline Tumors Optimal Staging: l USO or cystectomy (in BOT) l Peritoneal washing and cytology l Inspection of the contralateral ovarian surface, biopsies of any suspicious lesions Wedge resection of the opposite ovary? l Staging biopsies of the peritoneal cavity l Sampling of retroperitoneal lymph nodes or radical lymphadenectomy since 1990 l Omentectomy, appendectomy.
 Fertility Sparing Surgery in Borderline Tumors l Recurrence rate in the patients underwent conservative surgery for border-line tumors is %7 Gynecol Oncol 55; 552 -6, 1994.
Fertility Sparing Surgery in Borderline Tumors l Recurrence rate in the patients underwent conservative surgery for border-line tumors is %7 Gynecol Oncol 55; 552 -6, 1994.
 Border-line Tumors of the Ovary Conservative Management and Pregnancy Outcome Cancer 1998 Jan, 1; 82(1): 141 -6 l Retrospective review l 82 patients l 39 patients underwent conservative management l Three patients had a contralateral recurrence (7%) l 22 pregnancies were achieved.
Border-line Tumors of the Ovary Conservative Management and Pregnancy Outcome Cancer 1998 Jan, 1; 82(1): 141 -6 l Retrospective review l 82 patients l 39 patients underwent conservative management l Three patients had a contralateral recurrence (7%) l 22 pregnancies were achieved.
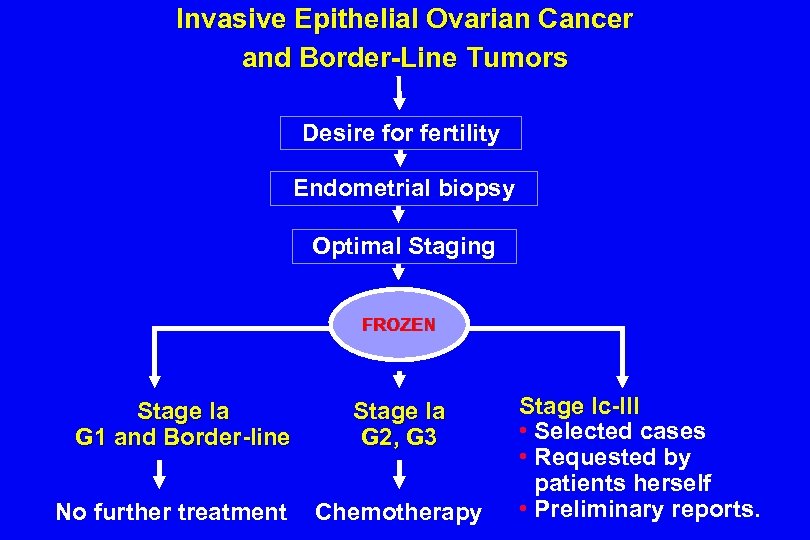 Invasive Epithelial Ovarian Cancer and Border-Line Tumors Desire for fertility Endometrial biopsy Optimal Staging FROZEN Stage Ia G 1 and Border-line No further treatment Stage Ia G 2, G 3 Chemotherapy Stage Ic-III • Selected cases • Requested by patients herself • Preliminary reports.
Invasive Epithelial Ovarian Cancer and Border-Line Tumors Desire for fertility Endometrial biopsy Optimal Staging FROZEN Stage Ia G 1 and Border-line No further treatment Stage Ia G 2, G 3 Chemotherapy Stage Ic-III • Selected cases • Requested by patients herself • Preliminary reports.
 Can conservative surgical approach be used in selected young patients with ovarian cancer who would usually undergo radical operations. Cancer 1998 Jan, 1; 82(1): 141 -6 l Retrospective study between 1980 -1994 l 10 patients with high grade or limited extraovarian disease • Stage Ia G 3 2 • Stage Ic 2 • Stage IIIa 2 • Stage IIIc 4 l All patients were given adjuvant CT l All patients were alive median follow-up 70 months l 9 patients were menstruating regularly l Three had became pregnant.
Can conservative surgical approach be used in selected young patients with ovarian cancer who would usually undergo radical operations. Cancer 1998 Jan, 1; 82(1): 141 -6 l Retrospective study between 1980 -1994 l 10 patients with high grade or limited extraovarian disease • Stage Ia G 3 2 • Stage Ic 2 • Stage IIIa 2 • Stage IIIc 4 l All patients were given adjuvant CT l All patients were alive median follow-up 70 months l 9 patients were menstruating regularly l Three had became pregnant.
 Ovarian Cancer Treatment with Fertility-Sparing Therapy l l l Stage IA and IC epithelial ovarian cancer 1965 to 2000, n=52 20 (%38) received chemotherapy 9 (17%) eventual TAH 5(10%) recurred, 2 died 24 (46%) attempted, 17 (33%) conceived « 26 term, 5 SAb l 33% take home baby Schilder et al. , Gynecol Oncol, 2002
Ovarian Cancer Treatment with Fertility-Sparing Therapy l l l Stage IA and IC epithelial ovarian cancer 1965 to 2000, n=52 20 (%38) received chemotherapy 9 (17%) eventual TAH 5(10%) recurred, 2 died 24 (46%) attempted, 17 (33%) conceived « 26 term, 5 SAb l 33% take home baby Schilder et al. , Gynecol Oncol, 2002
 Fertility Sparing Surgery in Epithelial Ovarian Cancer and Borderline Tumors CONCLUSIONS l For more advanced stages, additional investigation is needed. l After completion of fertility, residual ovary should be taken out. « Incidence of ovarian cancer gets higher with age. « Screening method are unreliable.
Fertility Sparing Surgery in Epithelial Ovarian Cancer and Borderline Tumors CONCLUSIONS l For more advanced stages, additional investigation is needed. l After completion of fertility, residual ovary should be taken out. « Incidence of ovarian cancer gets higher with age. « Screening method are unreliable.
 Germ Cell Tumors of the Ovary l Incidence: less than %5 of all ovarian neoplasm. l Age: the first and second decade l Usually unilateral
Germ Cell Tumors of the Ovary l Incidence: less than %5 of all ovarian neoplasm. l Age: the first and second decade l Usually unilateral
 FSS in Germ Cell Tumors of the Ovary l 1978 Forney first reported a case of successful pregnancy in a 18 year-old with EST of ovary. Obstet Gynecol 52, 360 -62 (1978) l 1985 Gershenson at the MD Anderson Hospital. 48 patients with malignant germ cell tumors Full-term pregnancies in 6 cases Cancer 56, 2756 -2761 (1985)
FSS in Germ Cell Tumors of the Ovary l 1978 Forney first reported a case of successful pregnancy in a 18 year-old with EST of ovary. Obstet Gynecol 52, 360 -62 (1978) l 1985 Gershenson at the MD Anderson Hospital. 48 patients with malignant germ cell tumors Full-term pregnancies in 6 cases Cancer 56, 2756 -2761 (1985)
 FSS in Germ Cell Tumors of the Ovary Rationales l Unilaterality of tumor l Improvement of prognosis by modern combination chemotherapy 1970 s the VAC regimen 1980 s the PVB regimen POMP/ACE.
FSS in Germ Cell Tumors of the Ovary Rationales l Unilaterality of tumor l Improvement of prognosis by modern combination chemotherapy 1970 s the VAC regimen 1980 s the PVB regimen POMP/ACE.
 Treatment of Malignant Ovarian Germ Cell Tumors With Preservation of Fertility A Report of 28 Cases / Cancer 42, 1152 -1160 (1978) l Tumor was confined to one ovary in all cases. l All patients were taken chemotherapy except two with stage I immature teratoma. l More than 5 years survival in 13 cases (59. 1%) l 7 of 12 married patients, became pregnant, all had term delivery.
Treatment of Malignant Ovarian Germ Cell Tumors With Preservation of Fertility A Report of 28 Cases / Cancer 42, 1152 -1160 (1978) l Tumor was confined to one ovary in all cases. l All patients were taken chemotherapy except two with stage I immature teratoma. l More than 5 years survival in 13 cases (59. 1%) l 7 of 12 married patients, became pregnant, all had term delivery.
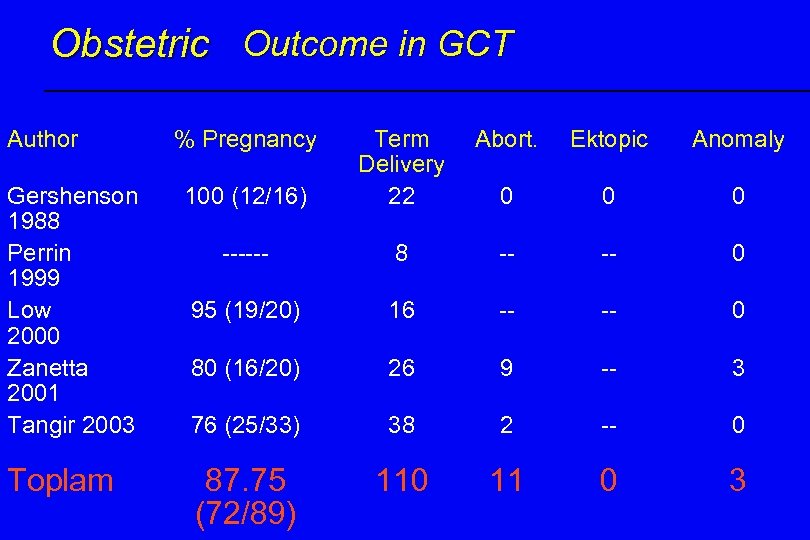 Obstetric Outcome in GCT Author Gershenson 1988 Perrin 1999 Low 2000 Zanetta 2001 Tangir 2003 Toplam % Pregnancy Abort. Ektopic Anomaly 100 (12/16) Term Delivery 22 0 0 0 ------ 8 -- -- 0 95 (19/20) 16 -- -- 0 80 (16/20) 26 9 -- 3 76 (25/33) 38 2 -- 0 87. 75 (72/89) 110 11 0 3
Obstetric Outcome in GCT Author Gershenson 1988 Perrin 1999 Low 2000 Zanetta 2001 Tangir 2003 Toplam % Pregnancy Abort. Ektopic Anomaly 100 (12/16) Term Delivery 22 0 0 0 ------ 8 -- -- 0 95 (19/20) 16 -- -- 0 80 (16/20) 26 9 -- 3 76 (25/33) 38 2 -- 0 87. 75 (72/89) 110 11 0 3
 Fertility Sparing Surgery in Germ Cell Tumors of the Ovary Conclusion Regardless of the stage is a safe and practicable procedure in the absence of involvement of CONTRALATERAL OVARY AND UTERUS
Fertility Sparing Surgery in Germ Cell Tumors of the Ovary Conclusion Regardless of the stage is a safe and practicable procedure in the absence of involvement of CONTRALATERAL OVARY AND UTERUS

 History of ART l The new millenium: « 2001 Clinic Specific Success about 28% per cycle overall «Oocyte and ovarian slice cryopreservation with function (Oktay) «İnvitro maturation matures
History of ART l The new millenium: « 2001 Clinic Specific Success about 28% per cycle overall «Oocyte and ovarian slice cryopreservation with function (Oktay) «İnvitro maturation matures
 Lancet, March 13, 2004
Lancet, March 13, 2004
 Fertility Preservation Strategies Treatment can be delayed IVF – embryo freezing Oocyte freezing Add tamoxifen or aromatase inhibitors for estrogen-sensitive Treatment cannot be delayed Ovarian tissue freezing In vitro maturation in high risk for ovarian involvement
Fertility Preservation Strategies Treatment can be delayed IVF – embryo freezing Oocyte freezing Add tamoxifen or aromatase inhibitors for estrogen-sensitive Treatment cannot be delayed Ovarian tissue freezing In vitro maturation in high risk for ovarian involvement
 As we discover what can be done, we need to learn what should done
As we discover what can be done, we need to learn what should done
 Thank you…
Thank you…
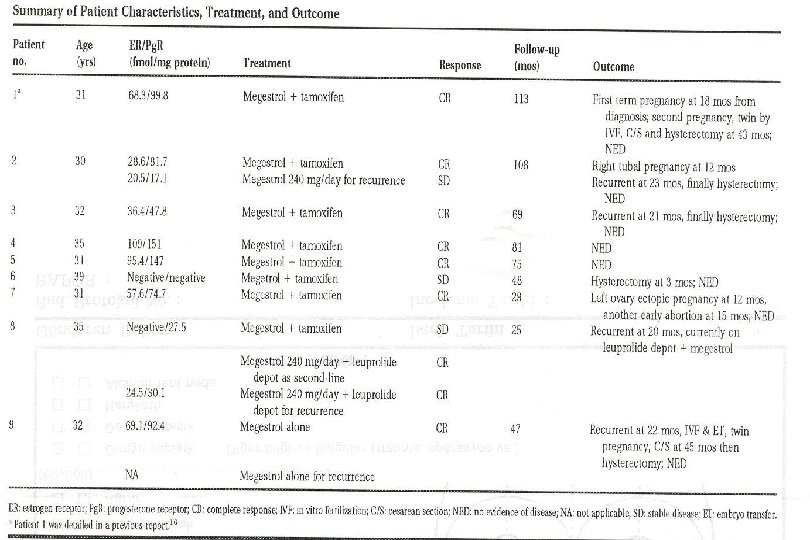
 Fertility-Preserving Treatment in Endometrial Adenocarcinoma l l l Stage IA, grade 1, 1991 -9 N=9, average 32 years Megace, tamoxifen, +Gn. RHa 8 CR, 1 TAH 4 pregnant « 2 term after ART, 2 ectopic l %22 take home baby Wang et al. , Cancer, 2002
Fertility-Preserving Treatment in Endometrial Adenocarcinoma l l l Stage IA, grade 1, 1991 -9 N=9, average 32 years Megace, tamoxifen, +Gn. RHa 8 CR, 1 TAH 4 pregnant « 2 term after ART, 2 ectopic l %22 take home baby Wang et al. , Cancer, 2002


