dc8ead43c0a937e6e10314783307d3cc.ppt
- Количество слайдов: 29

Feasibility study Monitoring childhood heights and weights in Wales Dr C Humphreys Specialist Registrar in Public Health

Overview • • • Childhood obesity Why measure it What is currently available The experiences of England NCMP European developments Our task

Obesity • 60% popn. could be obese by 2050 • ‘Obesogenic environment’ • Life course component – Early growth patterns (weeks/months) may affect later risk of obesity & disease • Generational component – Parents weight are greatest predictor of obesity Foresight Tackling Obesities: Future Choices – Project report UK Government Foresight programme. Image reproduced with permission.
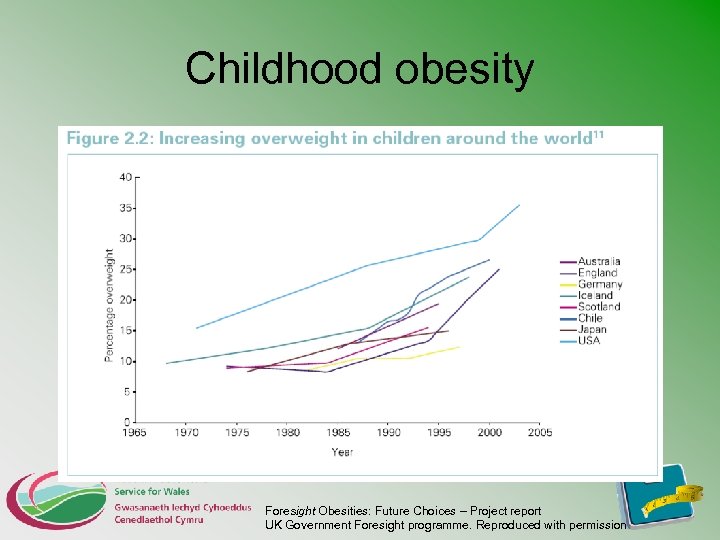
Childhood obesity Foresight Obesities: Future Choices – Project report UK Government Foresight programme. Reproduced with permission

Childhood obesity • “Global public health crisis” 1 • Consequences include 2 – Social and psychological, low self esteem • affecting future physical and mental health – risk factors for heart disease: • blood pressure, cholesterol, blood sugar – Persistence into adulthood • rates of ill-health / death than those obese as adults only – Type 2 diabetes in children & adolescents 1 Knai C, Lobstein T, Mckee M (2005) “Childhood obesity: the case for binding international legislation”, European Journal of Public Health, 15(6): 559 -563. 2 Storing up the problems, RCPCH, FPH 2002, Royal College of Physicians: London.

Policy context in Wales • Food & Fitness Plan (2006) – 1. 2. 3. 4. 5. 6. 7. Integrating nutrition & physical activity Extend Network of Healthy School Improve food & drink consumed High quality PE & practical cookery Opportunities for exercise/healthy foods Develop skills: physical activity/food preparation Training for those working with young people Ensure evidence based or innovative with evaluation

Possible reasons for monitoring • To monitor trends in order to: – Inform strategies and service development (prevention and management) • National / local level – Assess the effectiveness of interventions • Monitor change in trends • More robust methods such as cluster randomization for interventions – National level / local level • To provide a basis for epidemiological research • To feedback results to individuals – to support weight reduction for those individuals

Possible reasons for monitoring • Surveillance - to monitor trends in order to: – Inform strategies and service development (prevention and management) • National / local level (LHB; unfeasible at school level) – Assess the effectiveness of interventions/policy • Monitor change in trends • More robust methods such as cluster randomization for interventions – National level (unfeasible at local level) Perhaps – e. g. deprivation • To provide a basis for epidemiological research • To feedback results to individuals – to support weight reduction for those individuals Not for now

Surveillance vs Screening • Public health surveillance – ongoing, systematic – collection, analysis, interpretation, and dissemination of data – regarding a health-related event – for use in public health action – to reduce morbidity and mortality and to improve health CDC • Population screening – members of a defined population – who do not necessarily perceive they are at risk of or affected by disease – are offered a test – to identify individuals who are more likely to be helped than harmed by – further tests or treatment to reduce the risk of a disease or its complications NSC

Should we apply population screening to Obesity? • Should not screen: – NSC: Screening not recommended (2007) – Hall 4: ‘BMI at school entry (age 5) as a public health indictor, not for use with individual children’ (2006) – HTA: “Value questionable …in absence of evidence of effective interventions” (2007) • Conflicting messages: – House of Commons Select Committee on Health (2004) • “Throughout time at school children should have BMI measured annually…results should be sent home in confidence to parents…with advice…” – House of Commons Committee of Public Accounts (2006) • Recommended NCMP results disclosed to parents Hall DMB (200) ‘Growth monitoring and nutrition’ Health for all Children, 4 th Edition updated. p 187 Fayter D, Nixon J, Hartley S, Rithalia A, Butelr G, Rudolf M, et al. (2007) “A systematic review of the routine monitoring of growth in children of primary school age to identify growth-related conditions” Health Technology Assessment, 11(22): xii.
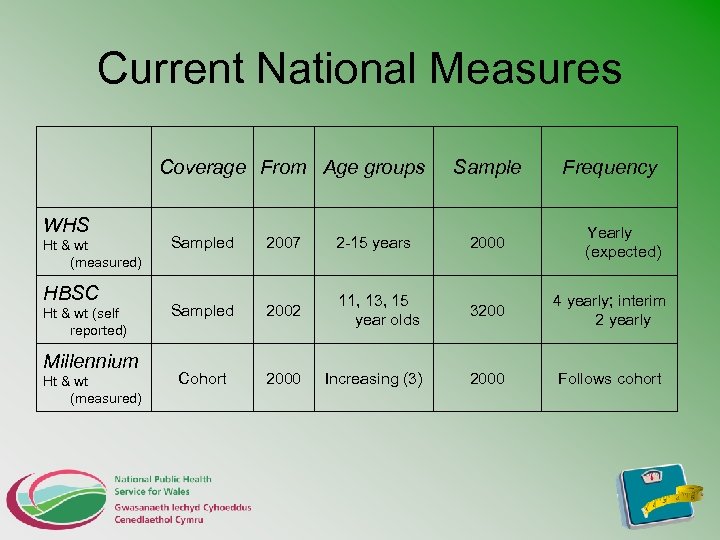
Current National Measures Coverage From Age groups WHS Ht & wt (measured) HBSC Ht & wt (self reported) Millennium Ht & wt (measured) Sample Frequency Yearly (expected) Sampled 2007 2 -15 years 2000 Sampled 2002 11, 13, 15 year olds 3200 4 yearly; interim 2 yearly Cohort 2000 Increasing (3) 2000 Follows cohort
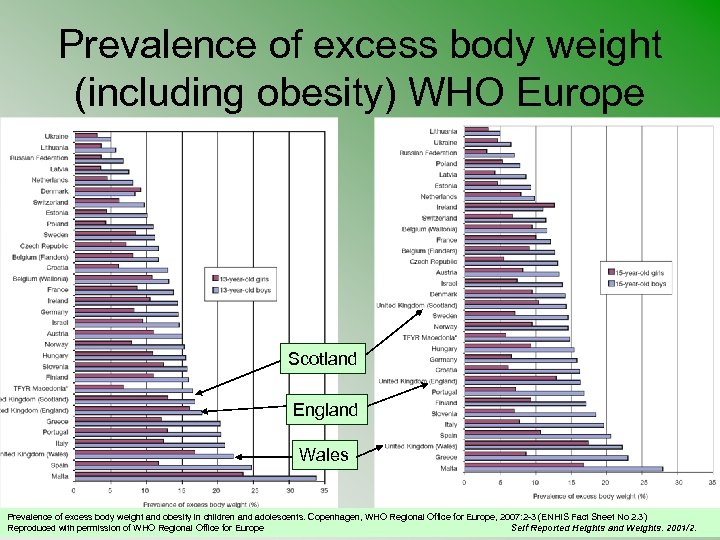
Prevalence of excess body weight (including obesity) WHO Europe Scotland England Wales Prevalence of excess body weight and obesity in children and adolescents. Copenhagen, WHO Regional Office for Europe, 2007: 2 -3 (ENHIS Fact Sheet No 2. 3) Reproduced with permission of WHO Regional Office for Europe Self Reported Heights and Weights. 2001/2.

Trust child health records • All 13 measure during early school – Reception year: – Year one: – School entry: 5 3 5 • Two Trusts measure later – 1 during year six; 1 during year seven. • Seven Trusts report routinely measuring pre-school As reported by Professional Leads for Health Visiting and Schools (Apr 06) Source: Roberts L, Fox R (2006) Monitoring Childhood Obesity in Wales

National coverage • A review to estimate childhood obesity – Pre-school focus - due to higher coverage – Only 7 of 13 Trusts (/LHB) supplied data • 53% had pre-school assessment • 66% of these had a BMI • 5% of these were invalid Gully K, Williams R, Lester N, Aitken S (2007) “Measuring children and monitoring childhood obesity” Journal of Public Health, 29(2): 210 -212

Local studies from Child Health System Year Age Coverage Swansea 1 1986/7 - 2001/2 5 87 -99% Pembrokeshire 2 1987 -2002 3, 6, 14 74% Rhondda Ely 3 1998/9 6 65% 1 Jones SE, James-Ellison M, Young S, Gravenor MB, Williams R (2004) “Monitoring trends in obesity in South Wales using routine data” Archives of Disease in Childhood , 90: 464 -467. 2 Averill J (2004) An Examination of the Pattern and Trends in Underweight, Overweight and Obesity among Pembrokeshire Children. Dissertation, University of Birmingham. 3 Baneerjee S, Morgan RJH, Rees SA, Latif AHA (2003) “Height screening at school: ineffective without high standards and adequate resources” Archives of Disease in Childhood, 88: 477 -481

Most recent school based measure published • Swansea NHS Trust (1986/7 -2001/2) – 5 year old children – IOTF cut-offs used: • Obese: – 1986/7: 2. 5% – 2001/2: 6. 9% • Overweight (exclusive) – 1986/7: 11. 3% – 2001/2: 19. 5% *Excluding year when system was in transition • Statistically significant increase Jones SE, James-Ellison M, Young S, Gravenor MB, Williams R (2004) “Monitoring trends in obesity in South Wales using routine data” Archieves of Disease in Childhood , 90: 464 -467.

What has been happening in England? • Public Service Agreement: Childhood Obesity – Originally: to halt year-on-year increase in obesity < 11 years by 2010 • Measure: Health Survey for England • Local progress: National Childhood Measurement Programme established 2005/6 – Responsibility of PCTs – Height & weight collected: • Reception year (age 4/5) • Year 6 (age 10/11)

How did process work? • Opt-out consent based on public health surveillance (current guidance): – Privacy and dignity of child safeguarded • Sensitive measuring – Measures gathered with minimal physical contact – Process overseen by health professional – Letter giving option to withdraw – Only children who can stand on scales/height measures unaided

How do children feel? • Children’s Commissioner, England report • Primary school children will react positively providing concerns & wishes are addressed: – Children know & understand why – Children can choose someone to go with them if they wish – Private space – Whole school approach to health & wellbeing – Address anxieties sensitively/appropriately National Children’s Bureau (2005) A Report for the Children’s Commissioners Office on NCB’s consultations with primary school children on measuring children’s height and weight in school. https: //www. childrenscommissioner. org/

How did it go? - Database • Review of first year of data * • Poor response rate: 48% – 57% reception year (4/5 yr) – 42% year 6 (11/12 yr) • PCTs that provided no data: – 24% reception year – 39% year 6 • Heavy children more likely to opt out by: – Anecdotal evidence – Higher response rates assoc with higher obesity rates *Crowther R, Dinsdale H, Rutter H, Kyffin R (2007) Analysis of the National Childhood Obesity Database 2005 -06, South East Public Health Observatory.

How did it go? - Families • In-depth interviews: parent & child • Limited awareness • Important – Advance information – opt-out – feedback • Prevent body image anxiety/bullying Unpublished feedback from PCTs was also discussed in the original presentation BMBR Social Research (2007) Research into parental attitudes towards the routine measurement of children’s height and weight, DH.

How did it go? - Families • Feedback – not just ht/wt, but whether ht/wt is healthy • Information on BMI supplied was confusing – A coloured-in graph showing ranges felt to be more useful • They suggested information would be helpful & could be put it into practice

2006/7 Changes • • • 4 regional workshops (DH) “Improved guidance” Legal basis needed more clarity Stressed importance of more resources Need more emphasis on school engagement

Plans for the future • New legislation enables: – Using childhood obesity for performance monitoring • Initially coverage • Later performance of PCT/LA – Routine feedback to families • Exact mechanism unclear • BMI calculator is an option

What happens elsewhere • Scotland: – Clear direction at ages to take measures to enable national monitoring: • School entry; Primary 7 – every 3 years – Many other countries rely on sampled approaches for population monitoring, • e. g. National Health and Nutrition Examination Survey, USA Scottish Executive (2005) Health for all Children 4, guidance on Implementation in Scotland. Scottish Executive: Edinburgh.

European developments – childhood obesity • WHO European Ministerial Council – Need to standardise surveillance systems • Starts Spring 2008 – – – Protocol near finalisation Children age 6 -9 Nationally representative sample of primary schools 2, 800 children per age group (6. 0 -6. 9 etc) BMI; +/- anthropomorphic measures Feedback to individuals on request only

Our task (objectives of study) • What – Pilot a population monitoring system for childhood obesity – Routine feedback is not being considered now • Who – Population based not sampled – School setting • For what – Process effectiveness – Costs – Problems

Our task contd. • Where – Four pilot Trusts • • Pembrokeshire & Derwen Powys LHB North East Wales North Glamorgan – Outstanding aspects to be agreed (see objectives)

Particular thanks to: Prof R Williams, Swansea University Cath Roberts, Welsh Assembly Government Chris Roberts, Welsh Assembly Government Rosie Taylor, Department of Health London Bronwyn Petrie, Department of Health London Trudy Wijnhoven, Obesity Surveillance, WHO Europe
dc8ead43c0a937e6e10314783307d3cc.ppt