24dfdb764aaa701451bbf7a4c9e737c1.ppt
- Количество слайдов: 9
 Expanding Health Insurance Coverage James R. Tallon, Jr. President, United Hospital Fund Bipartisan Congressional Health Policy Conference January 13, 2007
Expanding Health Insurance Coverage James R. Tallon, Jr. President, United Hospital Fund Bipartisan Congressional Health Policy Conference January 13, 2007
 Three questions in expanding health insurance coverage: 1. Who pays? 2. Is it voluntary or mandatory? 3. How is the program designed? • Public vs. private • Federal vs. state roles • Pooling risk • Benefit package • Cost control features
Three questions in expanding health insurance coverage: 1. Who pays? 2. Is it voluntary or mandatory? 3. How is the program designed? • Public vs. private • Federal vs. state roles • Pooling risk • Benefit package • Cost control features
 UHF-Commonwealth Fund Blueprint for Universal Coverage Principles for Reform: • Access and affordability for all • Administrative simplicity • Stability of coverage • Shared responsibility • Continuity with existing programs • Choice • Pooled risk • Efficiency and quality
UHF-Commonwealth Fund Blueprint for Universal Coverage Principles for Reform: • Access and affordability for all • Administrative simplicity • Stability of coverage • Shared responsibility • Continuity with existing programs • Choice • Pooled risk • Efficiency and quality
 Blueprint Building Blocks • Public Programs – Simplification – Eligibility Expansion – Family Health Plus “Buy-In” • Purchasing Entity – Administer the Family Health Plus “buy-in” – Make coverage available to individuals at group rates • Mandates – Two versions of employer assessment for those not providing coverage – Individual mandate, with income protection
Blueprint Building Blocks • Public Programs – Simplification – Eligibility Expansion – Family Health Plus “Buy-In” • Purchasing Entity – Administer the Family Health Plus “buy-in” – Make coverage available to individuals at group rates • Mandates – Two versions of employer assessment for those not providing coverage – Individual mandate, with income protection
 Comparing Massachusetts and New York Prior to Reform • New York has a larger share of low-income people and a larger share of uninsured low-income people • New York has a lower rate of employer-sponsored insurance • New York has a larger eligible but uninsured population (41% vs. 23%)
Comparing Massachusetts and New York Prior to Reform • New York has a larger share of low-income people and a larger share of uninsured low-income people • New York has a lower rate of employer-sponsored insurance • New York has a larger eligible but uninsured population (41% vs. 23%)
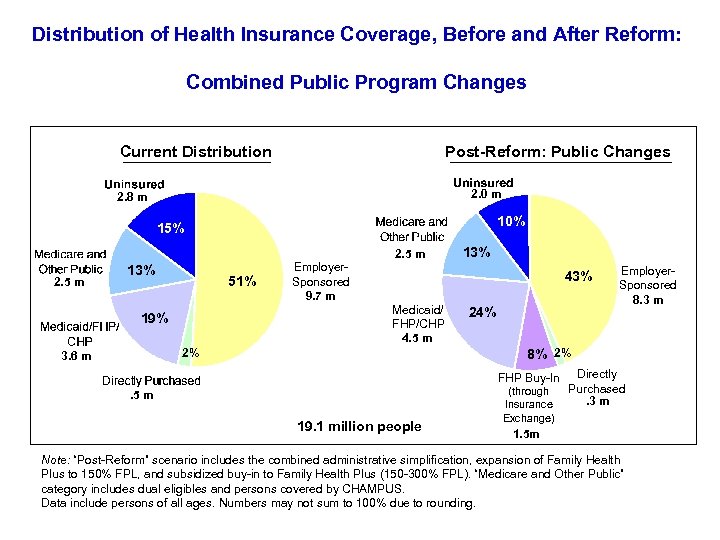 Distribution of Health Insurance Coverage, Before and After Reform: Combined Public Program Changes Current Distribution Post-Reform: Public Changes 2. 0 m 2. 8 m 10% 15% 2. 5 m 13% 51% 43% Medicaid/ FHP/CHP 4. 5 m 19% 2% 3. 6 m 13% Employer. Sponsored 9. 7 m 24% Employer. Sponsored 8. 3 m 8% 2% FHP Buy-In . 5 m 19. 1 million people (through Insurance Exchange) Directly Purchased. 3 m 1. 5 m Note: “Post-Reform” scenario includes the combined administrative simplification, expansion of Family Health Plus to 150% FPL, and subsidized buy-in to Family Health Plus (150 -300% FPL). “Medicare and Other Public” category includes dual eligibles and persons covered by CHAMPUS. Data include persons of all ages. Numbers may not sum to 100% due to rounding.
Distribution of Health Insurance Coverage, Before and After Reform: Combined Public Program Changes Current Distribution Post-Reform: Public Changes 2. 0 m 2. 8 m 10% 15% 2. 5 m 13% 51% 43% Medicaid/ FHP/CHP 4. 5 m 19% 2% 3. 6 m 13% Employer. Sponsored 9. 7 m 24% Employer. Sponsored 8. 3 m 8% 2% FHP Buy-In . 5 m 19. 1 million people (through Insurance Exchange) Directly Purchased. 3 m 1. 5 m Note: “Post-Reform” scenario includes the combined administrative simplification, expansion of Family Health Plus to 150% FPL, and subsidized buy-in to Family Health Plus (150 -300% FPL). “Medicare and Other Public” category includes dual eligibles and persons covered by CHAMPUS. Data include persons of all ages. Numbers may not sum to 100% due to rounding.
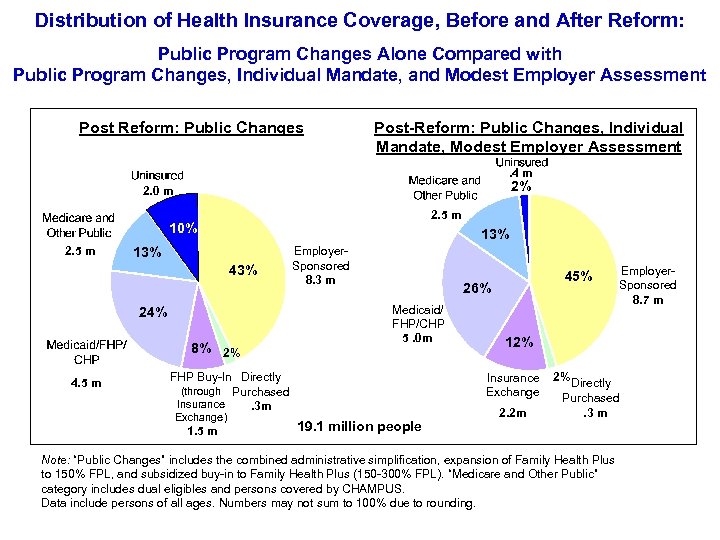 Distribution of Health Insurance Coverage, Before and After Reform: Public Program Changes Alone Compared with Public Program Changes, Individual Mandate, and Modest Employer Assessment Post Reform: Public Changes Post-Reform: Public Changes, Individual Mandate, Modest Employer Assessment. 4 m 2% 2. 0 m 2. 5 m 10% 2. 5 m 13% 43% 24% 8% 2% 4. 5 m Employer. Sponsored 8. 3 m 26% Medicaid/ FHP/CHP 5. 0 m FHP Buy-In Directly (through Purchased Insurance. 3 m Exchange) 1. 5 m 45% 12% Insurance Exchange 19. 1 million people Employer. Sponsored 8. 7 m 2. 2 m 2% Directly Purchased. 3 m Note: “Public Changes” includes the combined administrative simplification, expansion of Family Health Plus to 150% FPL, and subsidized buy-in to Family Health Plus (150 -300% FPL). “Medicare and Other Public” category includes dual eligibles and persons covered by CHAMPUS. Data include persons of all ages. Numbers may not sum to 100% due to rounding.
Distribution of Health Insurance Coverage, Before and After Reform: Public Program Changes Alone Compared with Public Program Changes, Individual Mandate, and Modest Employer Assessment Post Reform: Public Changes Post-Reform: Public Changes, Individual Mandate, Modest Employer Assessment. 4 m 2% 2. 0 m 2. 5 m 10% 2. 5 m 13% 43% 24% 8% 2% 4. 5 m Employer. Sponsored 8. 3 m 26% Medicaid/ FHP/CHP 5. 0 m FHP Buy-In Directly (through Purchased Insurance. 3 m Exchange) 1. 5 m 45% 12% Insurance Exchange 19. 1 million people Employer. Sponsored 8. 7 m 2. 2 m 2% Directly Purchased. 3 m Note: “Public Changes” includes the combined administrative simplification, expansion of Family Health Plus to 150% FPL, and subsidized buy-in to Family Health Plus (150 -300% FPL). “Medicare and Other Public” category includes dual eligibles and persons covered by CHAMPUS. Data include persons of all ages. Numbers may not sum to 100% due to rounding.
 Overview of Results • Public program changes achieve a one-third reduction in the uninsured • Significant subsidies are needed to gain participation and protection of low-income persons • Universal coverage requires mandatory features – Employer mandates alone are not enough – Individual mandates are necessary for universal coverage
Overview of Results • Public program changes achieve a one-third reduction in the uninsured • Significant subsidies are needed to gain participation and protection of low-income persons • Universal coverage requires mandatory features – Employer mandates alone are not enough – Individual mandates are necessary for universal coverage
 Spitzer Agenda Restructure: • Close and consolidate certain hospitals • Shift spending from institutional nursing homes to community and home-based care • Negotiate lower prices for prescription drugs • Aggressively fight Medicaid fraud Reinvest: • Universal coverage for children (year one) • Streamline enrollment in order to enroll eligible but uninsured adults (over 4 years) • Better management of high-cost cases
Spitzer Agenda Restructure: • Close and consolidate certain hospitals • Shift spending from institutional nursing homes to community and home-based care • Negotiate lower prices for prescription drugs • Aggressively fight Medicaid fraud Reinvest: • Universal coverage for children (year one) • Streamline enrollment in order to enroll eligible but uninsured adults (over 4 years) • Better management of high-cost cases


