bactsyndromes_BMedSc_new.ppt
- Количество слайдов: 43

Examples of bacterial infections and their interaction with the host We ask the lab for a diagnosis, expecting a yes or no, but often end up with just a maybe… Professor Mark Pallen
Microbes and humans Very few microbes are always pathogenic Many microbes are potentially pathogenic Most microbes are never pathogenic

Definitions • Pathogen – an organism that can cause infection in individuals with normal host defences, e. g. , Salmonella enteritidis, Vibrio cholerae • Commensal – an organism that is found normally on those parts of the body that are exposed to, or communicate with, the external environment, eg. Bacteroides fragilis, Staphylococcus epidermidis; the 'normal flora' • Opportunistic pathogen ('opportunist') – an organism that can cause infection in individuals with abnormal host defences. Commensals may be opportunistic pathogens.

Microbes and humans Disease can come about in several overlapping ways 1. Some bacteria are entirely adapted to the pathogenic way of life in humans. They are never part of the normal flora but may cause subclinical infection, e. g. M. tuberculosis 2. Some bacteria which are part of the normal flora acquire extra virulence factors making them pathogenic, e. g. E. coli 3. Some bacteria which are part of the normal flora can cause disease if they gain access to deep tissues by trauma, surgery, lines, e. g. S. epidermidis 4. In immunocompromised patients many free-living bacteria and components of the normal flora can cause disease, especially if introduced into deep tissues, e. g. Acinetobacter

How do we know that a given pathogen causes a specific disease? • Koch's postulates – the pathogen must be present in every case of the disease – the pathogen must be isolated from the diseased host & grown in pure culture – the specific disease must be reproduced when a pure culture of the pathogen is inoculated into a healthy susceptible host – the pathogen must be recoverable from the experimentally infected host
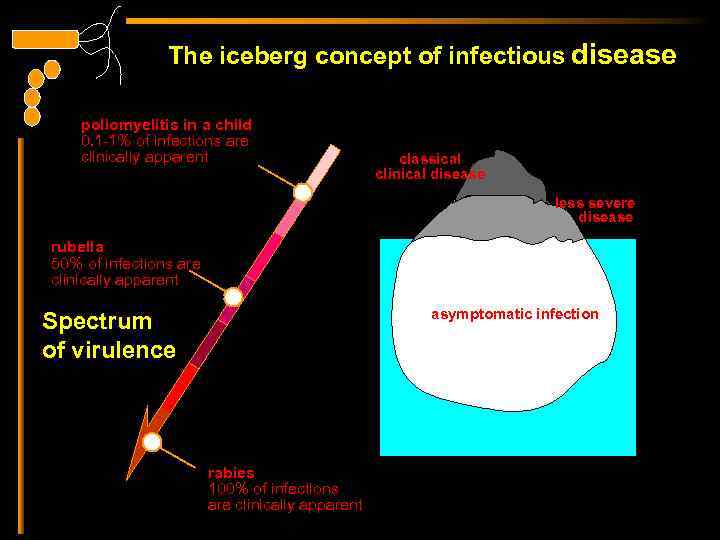
The iceberg concept of infectious disease poliomyelitis in a child 0. 1 -1% of infections are clinically apparent classical clinical disease less severe disease rubella 50% of infections are clinically apparent asymptomatic infection Spectrum of virulence rabies 100% of infections are clinically apparent
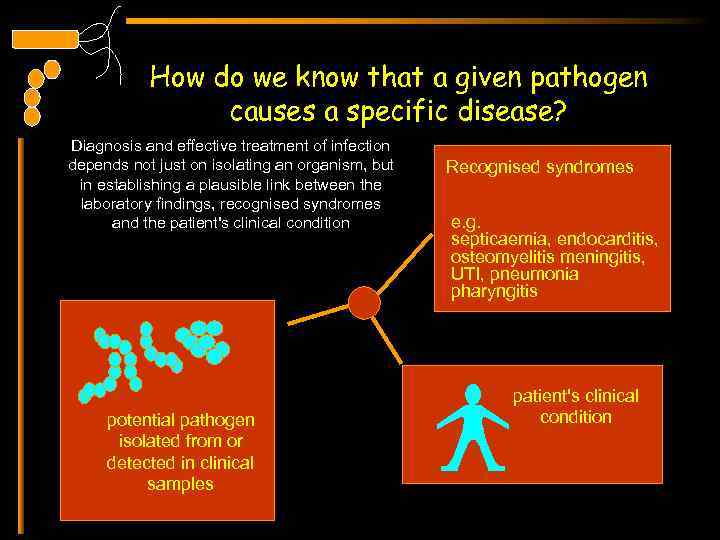
How do we know that a given pathogen causes a specific disease? Diagnosis and effective treatment of infection depends not just on isolating an organism, but in establishing a plausible link between the laboratory findings, recognised syndromes and the patient's clinical condition potential pathogen isolated from or detected in clinical samples Recognised syndromes e. g. septicaemia, endocarditis, osteomyelitis meningitis, UTI, pneumonia pharyngitis patient's clinical condition

Microbes and humans • Evidence for a potential pathogen being clinical significant (particularly for bacteria) – – – – Isolated in abundance Isolated in pure culture Isolated on more than one occasion Isolated from deep tissues Evidence of local inflammation Evidence of immune response to pathogen Fits with clinical picture

The Normal Flora “A New Year Greeting After an article by Mary J. Marples in Scientific American, January, 1969 On this day tradition allots to taking stock of our lives, my greetings to all of you, Yeasts, Bacteria, Viruses, Aerobics and Anaerobics: A Very Happy New Year to all for whom my ectoderm is as Middle-Earth to me. For creatures your size I offer a free choice of habitat, so settle yourselves in the zone that suits you best, in the pools of my pores or the tropical forests of arm-pit and crotch, in the deserts of my fore-arms, or the cool woods of my scalp. Build colonies: I will supply adequate warmth and moisture, the sebum and lipids you need, on condition you never do me annoy with your presence, but behave as good guests should, not rioting into acne or athlete's-foot or a boil. . ” W. H. Auden

The Normal Flora • Our bodies are like mobile warm-blooded coral reefs, rich in microbial biodiversity and home to vast numbers of bacterial cells – • • • more bacterial cells (1014) associated with the human body than there are human ones (only 1013)! What are they? – – Bacteria, Protozoa, Fungi, Archaea Metazoa? Viruses? Where are they? – External surfaces (not internal!) composition of normal flora varies from individual to individual – – – some bacterial species carried only transiently most fairly permanent difficult to alter composition of the normal flora of gut in a healthy individual

Relevance of normal flora • (1) Diagnostic microbiology – Which microorganism is a pathogen? • (2) Opportunistic Infections – Normal flora can cause disease – Even organisms not normally considered invasive or pathogenic occur in compromised hosts – E. g. , immunocompromised, skin breaches, other infections – Can be medically induced (iatrogenic), e. g. , urinary catheters, venous catheters

Microbial Loads on “External” Surfaces • • • Large intestine Skin Vagina Mouth Nose Throat 1014 1012 1010

Anaerobic Normal Flora Site Ratio of Anaerobes: Aerobes skin ~ 1: 1 large intestine 1000: 1 vagina 10: 1

Changes in normal flora • with changes in hormal physiology and development – female genital tract and lactobacilli • when antibiotics select for a 'resistant flora’ – Candida overgrowth in mouth, vagina – Clostridium difficile (antibiotic-associated colitis) • new organisms may be acquired – neonate from maternal genital tract during birth – Gram-negative colonisation of gut and URT in hospitalised patients – Cross-infection with C. difficile, MRSA, VRE etc
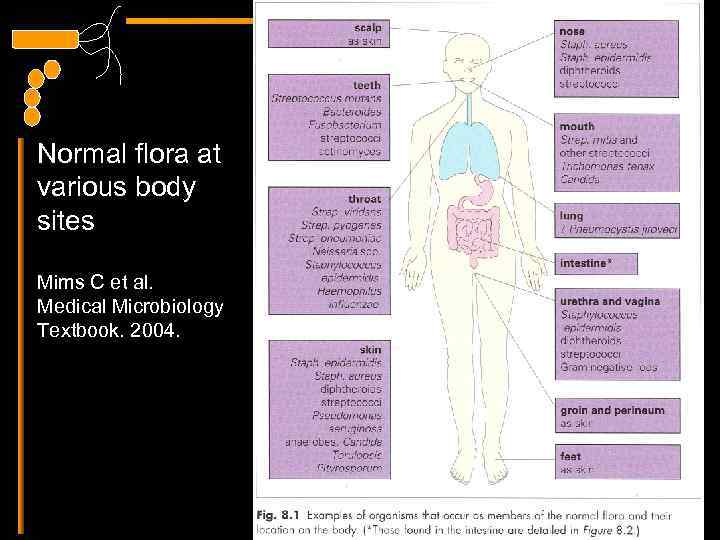
Normal flora at various body sites Mims C et al. Medical Microbiology Textbook. 2004.

Why care about the normal flora? it may be good for you! • colonization resistance: – competition for space and nutrients with pathogens • release of bacteriocins and colicins (antibacterial substances) to prevent pathogen growth • vitamin K production in gut • continued antigenic stimulation from commensals – cross-reacting protective immunity against pathogens – commensal neisseriaceae and Neisseria meningitidis

Why care about the normal flora? • commensal bacteria may cause disease at their site of carriage or nearby, e. g. – Streptococcus mutans (mouth) • causes dental caries – Streptococcus pneumoniae (upper airways) • causes otitis media, sinusitis • Some members of the normal flora can become pathogenic if they acquire additional virulence factors (e. g. E. coli) or are introduced into normally sterile sites (e. g. Staphylococcus aureus)

Why care about the normal flora? Normal flora as contaminants • To allow interpretation of • Skin flora in blood cultures • Perineal flora in urine • Throat flora in sputum – Gram stains on clinical samples – Culture results – BUT coagulase-negative staphylococci can be pathogens in deviceassociated sepsis, so can be hard to interpret – Take an MSU! – Mixed culture=contamination – Need to assess whether • Heavy pure growth • Obtained repeatedly • Fits clinical picture
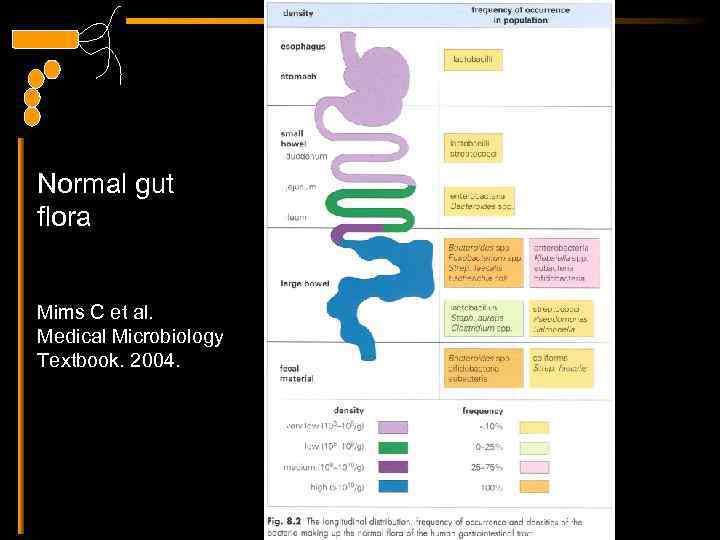
Normal gut flora Mims C et al. Medical Microbiology Textbook. 2004.

Harmful effects of gut bacteria • escape of normal flora to abnormal sites – perforated appendix leads to peritonitis with – Bacteroides spp. and facultative aerobes inc. E. coli • cholecystitis and cholangitis – often mixed infection, E. coli predominant, also including enterococci • urinary tract infection – most frequent organism in normal urinary tract is E. coli • vaginal candiosis

Harmful effects of alterations in normal gut flora • antibiotic use • sensitive gut flora killed • overgrowth with resistant flora inc. Clostridium difficile – leads to • C. difficile toxin production • Diarrhoea, pseudomembraneous colitis – leads to • Treatment – stop precipitating antibiotic – give oral metronidazole or vancomycin – recovery requires reestablishment of normal flora • ? probiotics

Bacterial infections & clinical syndromes • Syndromes caused by bacterial infection can be classified into two basic types: – those defined on basis of pathogen, where a given species of bacterium causes a clearly defined syndrome – those defined on the basis of anatomical site of infection • caused by many different sorts of bacteria, individually or even in combination. • There is overlap between these types of syndrome because some bacteria cause characteristic infections at several sites (e. g. Haemophilus influenzae meningitis and epiglotitis).
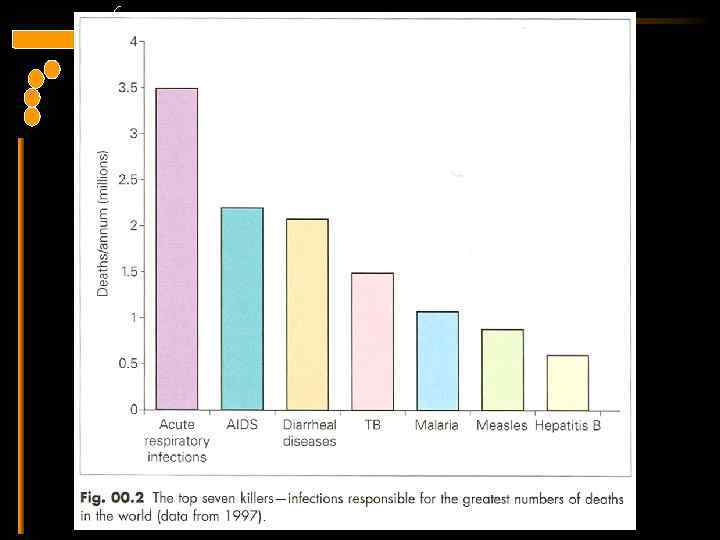
The top 7 killers Mims C et al. Medical Microbiology. 2004.

Some syndromes defined by pathogen • • typhoid fever legionnaires disease tuberculosis diphtheria

Some syndromes defined by site • • urinary tract infection pharyngitis pneumonia septicaemia endocarditis meningitis osteomyelitis
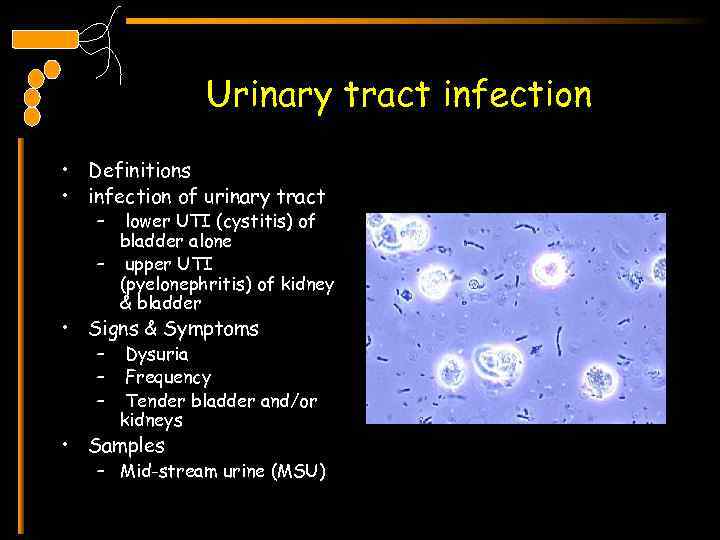
Urinary tract infection • Definitions • infection of urinary tract – lower UTI (cystitis) of bladder alone – upper UTI (pyelonephritis) of kidney & bladder • Signs & Symptoms – – – Dysuria Frequency Tender bladder and/or kidneys • Samples – Mid-stream urine (MSU)
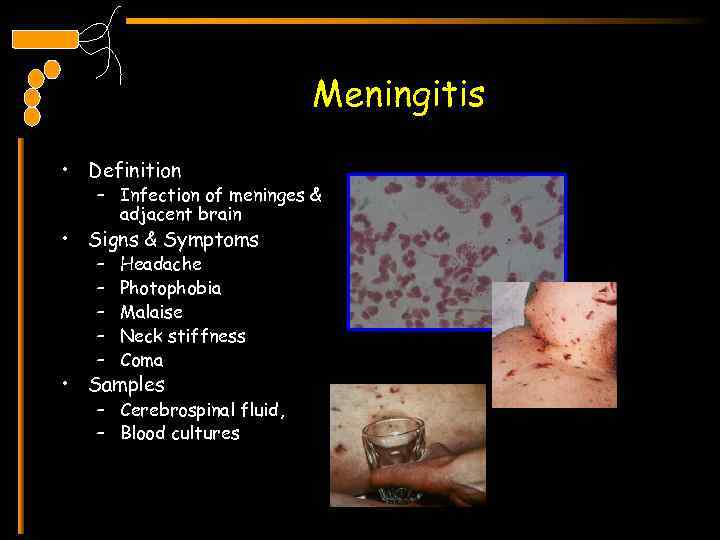
Meningitis • Definition – Infection of meninges & adjacent brain • Signs & Symptoms – – – Headache Photophobia Malaise Neck stiffness Coma • Samples – Cerebrospinal fluid, – Blood cultures

Septicaemia • Definition – Infection of the blood ("blood poisoning") – Bacteria multiply in the blood • Signs & Symptoms – Fever – Malaise – Hypotension ( "septic shock") – Tachycardia • Samples – Blood cultures
Endocarditis • Definition – Infection of the heart valves • Signs & Symptoms – – Fever Malaise Weight loss Heart failure • Samples – Blood cultures

Osteomyelitis • Definition – Infection of bone • Signs & Symptoms – Fever – Malaise – Local pain & tenderness • Samples – Blood culture – Bone chippings

Gastroenteritis • Definition – Infection of gut • Signs & Symptoms – Nausea – Vomiting – Diarrhoea • Samples – faeces
Pneumonia • Definition – Infection of lungs • Signs & Symptoms – Dyspnoea – Cough – Chest pain • Samples – sputum • Various clinical syndromes –Bronchopneumonia • Diffuse patchy consolidation • S. pneumoniae, H. influenzae –Lobar pneumonia • Typically S. pneumoniae –Interstitial pneumonia • Characteristically viral –Lung abscess –Atypical pneumonia

Pharyngitis • Definition – throat infection • Signs & Symptoms – sore throat – malaise • Samples – throat swab

Pyrexia of unknown origin • Definition – varies - a common definition is that of a fever of more than 2 -3 weeks duration, with no cause that be ascertained from initial tests. • Signs & Symptoms – various • Samples – many & varied
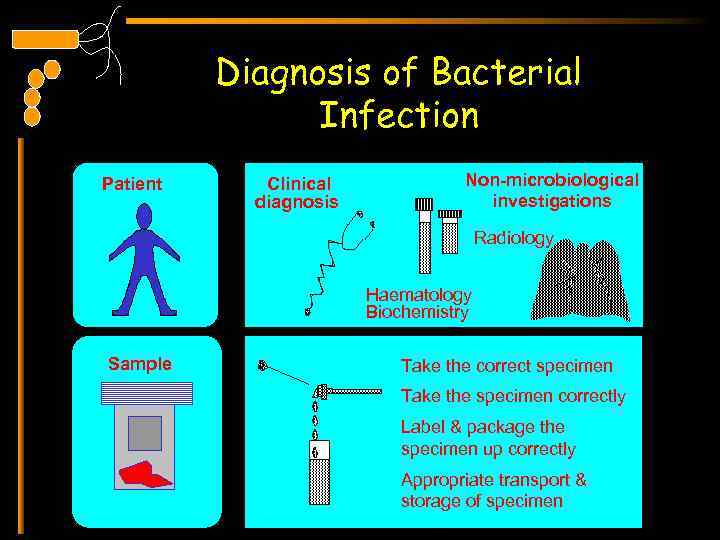
Diagnosis of Bacterial Infection Patient Clinical diagnosis Non-microbiological investigations Radiology Haematology Biochemistry Sample Take the correct specimen Take the specimen correctly Label & package the specimen up correctly Appropriate transport & storage of specimen
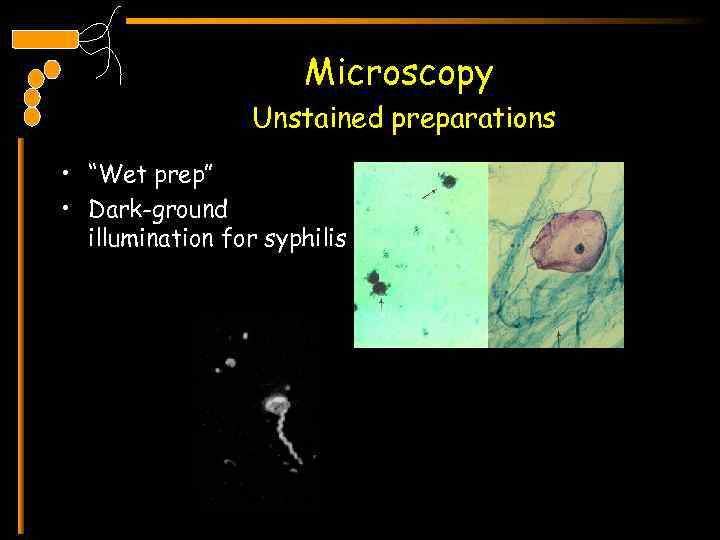
Microscopy Unstained preparations • “Wet prep” • Dark-ground illumination for syphilis
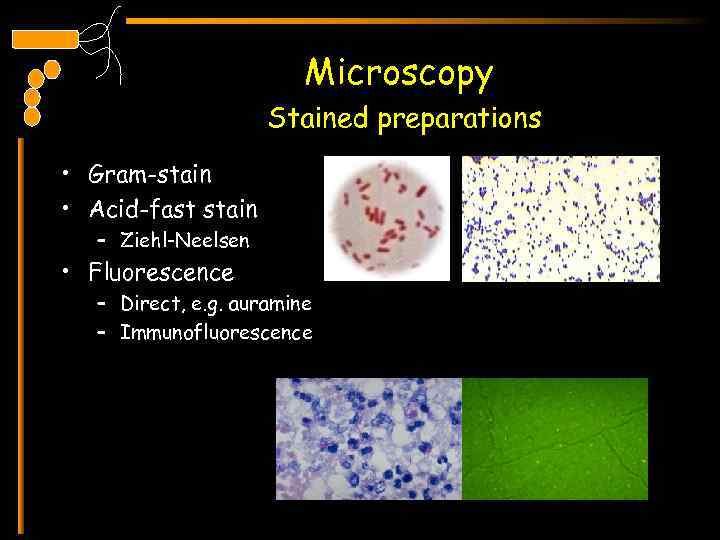
Microscopy Stained preparations • Gram-stain • Acid-fast stain – Ziehl-Neelsen • Fluorescence – Direct, e. g. auramine – Immunofluorescence
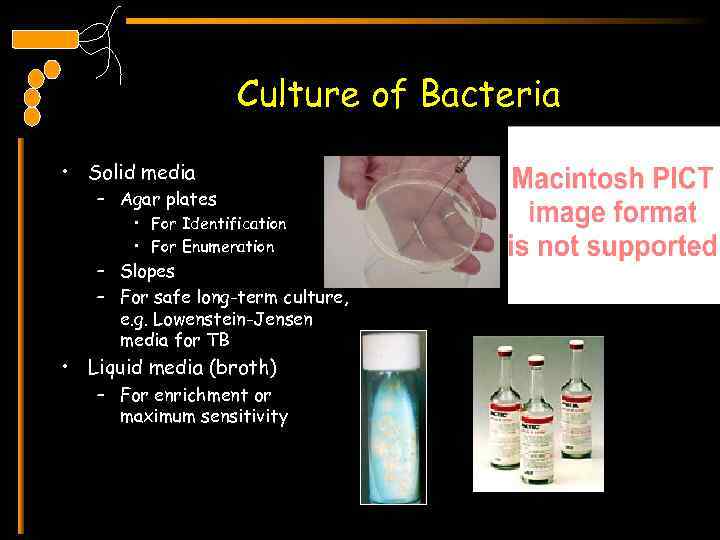
Culture of Bacteria • Solid media – Agar plates • For Identification • For Enumeration – Slopes – For safe long-term culture, e. g. Lowenstein-Jensen media for TB • Liquid media (broth) – For enrichment or maximum sensitivity

Advantages of Solid Media • isolation of single clonal colonies – get bacterium in pure culture • identify by colonial morphology • quantification by colony-forming units
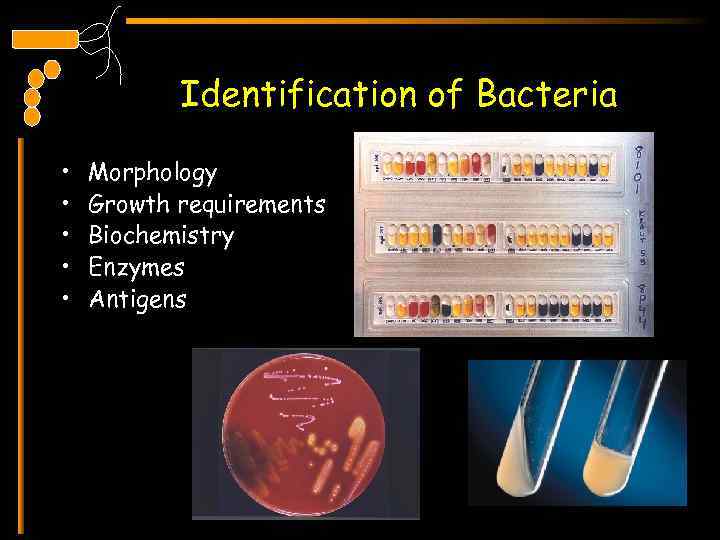
Identification of Bacteria • • • Morphology Growth requirements Biochemistry Enzymes Antigens

Non-cultural diagnostic methods • Antigen detection – e. g. latex agglutination • Antibody detection – e. g. agglutination tests, complement fixation tests, indirect immunofluorescence • Molecular methods – Polymerase Chain Reaction

Sensitivity tests • on solid media – disc diffusion technique • in liquid media – minimum inhibitory concentration (MIC) test • Breakpoint methods • E-test

Summary • • Bacteria and humans Normal Flora Bacterial infection syndromes Diagnosis of bacterial infection
bactsyndromes_BMedSc_new.ppt