860bcee85bf56f292e35e320f06c51c2.ppt
- Количество слайдов: 40

Evidence Based Medicine ﺍﻟﻄﺐ ﺍﻟﻤﺴﻨﺪ )ﺍﻟﻤﺒﻨﻲ( ﻋﻠﻰ ﺍﻟﺪﻟﻴﻞ ﻃﺐ ﺍﻟﺒﻧﺔ
EBM ?

ﺑﺴﻢ ﺍﻟﻠﻪ ﺍﻟﺮﺣﻤﻦ ﺍﻟﺮﺣﻴﻢ )ﺍﻗﺮﺍ ﺑﺎﺳﻢ ﺭﺑﻚ ﺍﻟﺬﻱ ﺧﻠﻖ * ﺧﻠﻖ ﺍﻻﻧﺴﺎﻥ ﻣﻦ ﻋﻠﻖ * ﺍﻗﺮﺍ ﻭﺭﺑﻚ ﺍﻻﻛﺮﻡ ﺍﻟﺬﻱ ﻋﻠﻢ ﺑﺎﻟﻘﻠﻢ * ﻋﻠﻢ ﺍﻻﻧﺴﺎﻥ ﻣﺎ ﻟﻢ ﻳﻌﻠﻢ( ﺟﺎﺀ ﻓﻲ ﺍﻟﺤﺪﻳﺚ ﺍﻟﺸﺮﻳﻒ ﻻ ﻳﺆﻤﻦ ﺍﺣﺪﻛﻢ ﺣﺘﻰ ﻳﺤﺐ ﻷﺨﻴﻪ ﻣﺎ ﻳﺤﺐ ﻟﻨﻔﺴﻪ

Evidence-Based Medicine (EBM) Evidence-based medicine is the process of lifelong, 1. self-directed learning, 2. caring for patients by search for the most valid and clinical important information about diagnosis, prognosis, therapy, and other clinical and health-care issues.

Evidence-based medicine (EBM) Is the process of systematically reviewing, appraising and using clinical research findings to aid the delivery of optimum clinical care to patients.

“Evidence-based medicine is the integration of: (1)best research evidence with (2)clinical expertise and (3)patient values” - Sackett, et al 2001
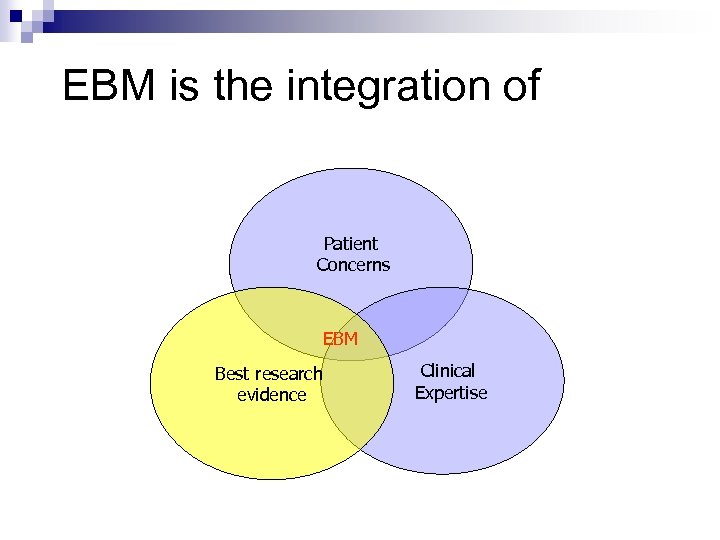
EBM is the integration of Patient Concerns EBM Best research evidence Clinical Expertise

Evidence is said to be the new bright star of health care. Any term with the word “evidence” automatically confers a sense of scientific authority. Some say EBM is “the development of best health-care practices based on most valid & reliable data. Best evidence should be derived from the findings of randomized controlled trials (RCTs)—the so-called “gold standard” in research— and meta-analysis, which is the “mean” or “conclusion” of a systematic review of research studies.

The recommendations that physicians make to patients without EBM depend on: - His current state of knowledge. - Colleagues suggestions and advices. - His experience with patients and diseases. Textbooks.

? Which doctor do you want William Osler, 1900 Smart young doctor

? Which doctor do you want Wise & experienced smart young doctor

Life long learning The hardest conviction to get into the mind of a beginner doctor is that the education upon which he is engaged is not … a medical course, but a life course, for which the work of a few years under teachers is, not more than a preparation. Sir William Osler (1849 -1919), from: ¨ The Student of Medicine ¨

But, Experience “alone” can be a poor (and even dangerous) teacher !!!! Why our professors are not professing now? ? ? ?

The Slippery Slope 100% r = -0. 54 p<0. 001. . . Choudhry, Fletcher and Soumerai, knowledge Ann Intern Med 2005; 142: 260 -73. . . 50% of current studies found decreasing -94% of 62. . . best care. . . . competence for at least some tasks, with. . increasing physician age. . . 0% years since graduation
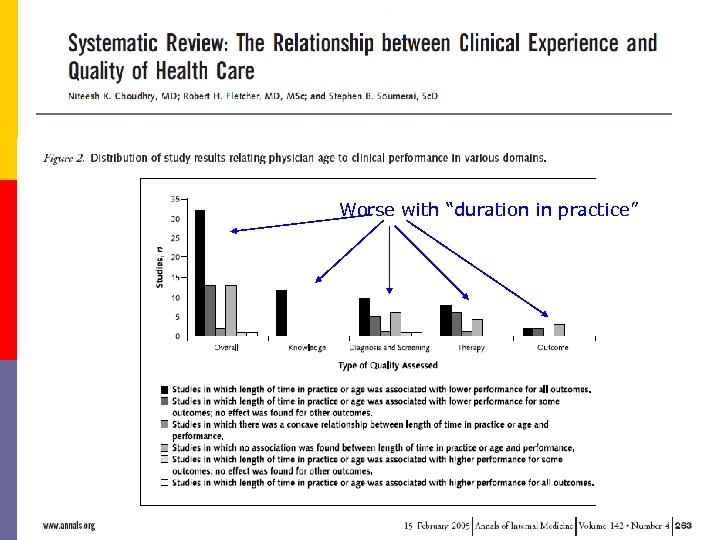
The Prognosis of Ignorance is Poor Worse with “duration in practice”

Important facts -The knowledge base of clinical medicine is continuously expanded. - The history of medicine include countless examples of therapies that were once widely accepted but later were shown to be ineffective or even harmful for patients. -The physicians, ethically should search the latest available knowledge. -It is very difficult job when we faced with conflicting or inconclusive results. -Even in most respected journals, it is not guarantee that the research results are valid, or even if valid, are relevant and applicable for daily practice.

Systematic review of bed rest after medical procedures * 10 trials of bed rest after spinal puncture ► no change in headache with bed rest ► Increase in back pain * Protocols in UK neurology units - 80% still recommend bed rest after LP …evidence of harm available for 17 years preceding. . . Serpell M, BMJ 1998; 316: 1709– 10
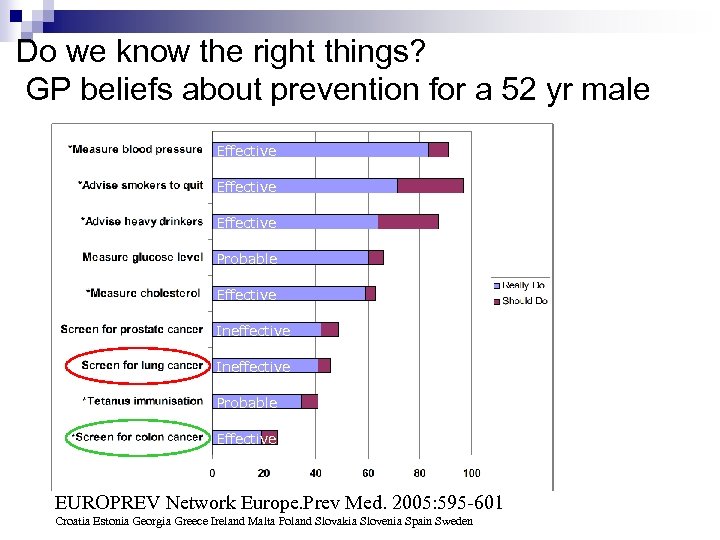
Do we know the right things? GP beliefs about prevention for a 52 yr male Effective Probable Effective Ineffective Probable Effective EUROPREV Network Europe. Prev Med. 2005: 595 -601 Croatia Estonia Georgia Greece Ireland Malta Poland Slovakia Slovenia Spain Sweden

Only about 15% of medical interventions (treatments) are supported by solid scientific evidence” (BMJ Editorial). This would put 80 to 90 per cent of accepted medical procedures all over the world under the heading of controversy.

Problems of Modern Medicine 1. The success paradox (↑ life expectancy of patient with CNCDs). 2. The tax of advance (economical issues). 3. The side effects of modern medicine (perforated PU). 4. The weakness of the modern medicine (AIDS & malaria). 5. The modern doctors (beurocratic authority over patients). 6. The information overload (oceans of scientific articles).

As Haines, stated, there are currently over 20 000 medical journals world-wide, and they publish a total of two million articles each year (if stacked on top of another, the pile would be 500 meter high). He estimated that any physician would have to digest 19 original articles "every day" in order to keep up to date in his subject. Is it possible? ? ?

WHAT ARE YOU DOING ? YOUR PATIENT DIED !!!!
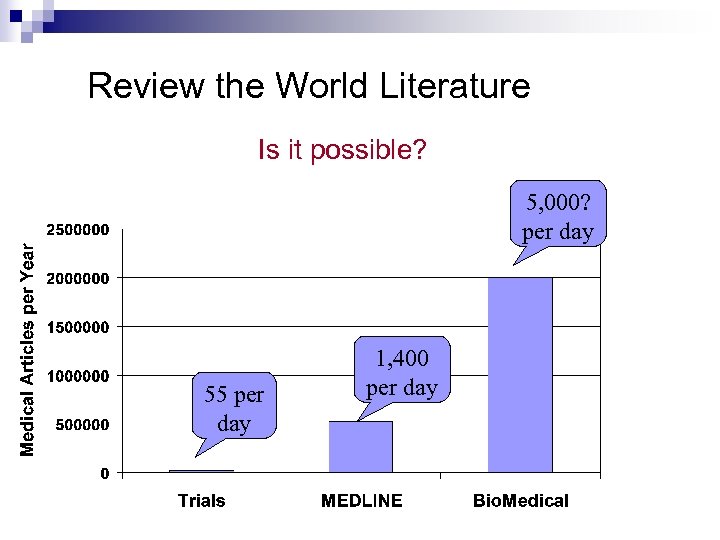
Review the World Literature Is it possible? 5, 000? per day 55 per day 1, 400 per day

These oceans of articles, carry the following features: Most of all research is not valid and not reliable (armchaired research) only a tiny proportion of all research is “ready for application” only a tiny fraction of the “ready” research is “relevant” to the practice of a given clinician only a tiny proportion of the “relevant” research for a given practitioner is “interesting” in the sense of being something new, important, actionable, and applicable to that specific patient.

Did you end or what? ? ?

Important facts - It is not possible for any physicians to read, as it is published, everything relevant to his or to her practice. - By the advent of computers, now it is possible to search in automated manner, but we still with problems of choosing and to reach among oceans of articles. - One of the apparently promising solution for this problem is the introduction of "Evidence-Based Medicine" and "Metanalysis", which both can actually filter all valid and reliable information and medical news into those more accurate, more relevant, and more specific to the subject of concern.

Evidence-Based Journals Critical Appraisal Filters 60, 000 articles/yr from 120 journals ~3, 500 articles/yr meet critical appraisal and content criteria (95% noise reduction)
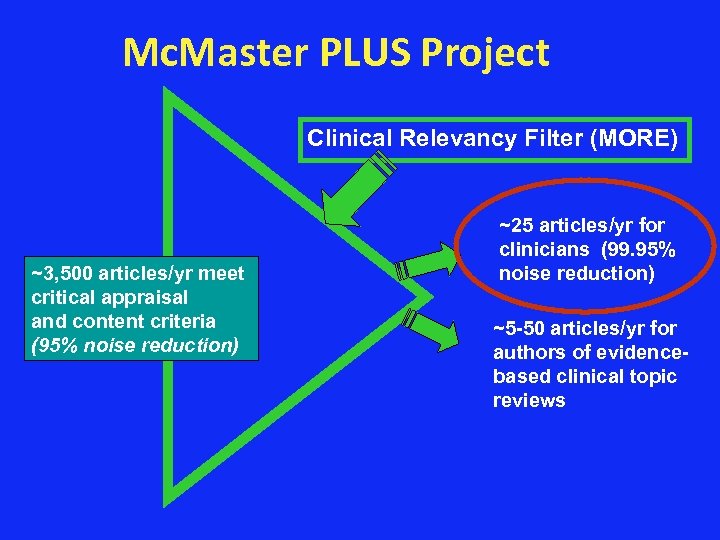
Mc. Master PLUS Project Clinical Relevancy Filter (MORE) ~3, 500 articles/yr meet critical appraisal and content criteria (95% noise reduction) ~25 articles/yr for clinicians (99. 95% noise reduction) ~5 -50 articles/yr for authors of evidencebased clinical topic reviews

Evidence-Based Journals: Choose only 120 trusted journals from 20 000 to apply 60 000 articles / year to critically appraisal filter to yield only 3 500 articles / year This lead to 95% noise reduction. Mc. Master Plus Project: Apply these 3 500 articles / year to clinical relevancy filter to yield only 25 -50 article / year with 99. 95% noise reduction.
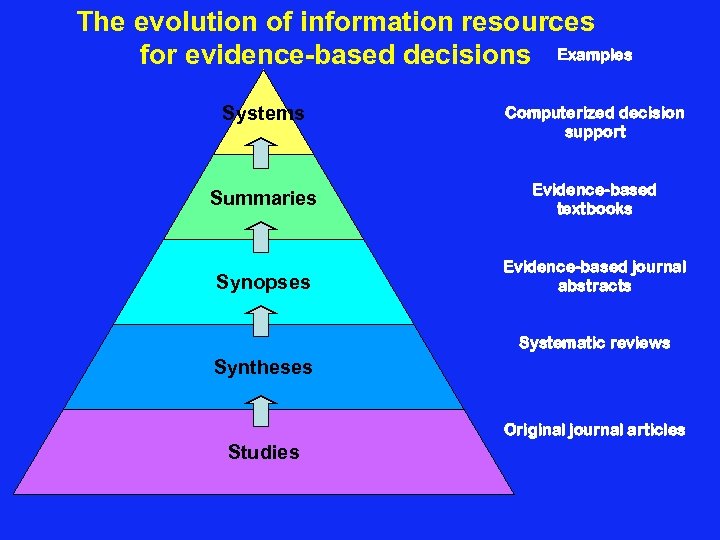
The evolution of information resources for evidence-based decisions Examples Systems Computerized decision support Summaries Evidence-based textbooks Synopses Evidence-based journal abstracts Systematic reviews Syntheses Original journal articles Studies

Evidence-Based Medicine is published in: English French German Italian Portuguese Spanish

Why we should use EBM? 1. Any wise physician wants to provide the best available health services to his patients. 2. We need evidence (about the accuracy of diagnostic tests, the power of prognostic markers, the comparative efficacy and safety of interventions. 3. Replaces currently accepted diagnostic tests and treatments with new ones that are more powerful, more accurate, more efficacious, and safer. 4. To prevent or at least decrease medical malpractice claims. 5. To keep ourselves really up-to date in our practice. 6. Suppose you are the patient (what you urgently need from medicine? ). 7. To keep our medical colleges in the international accreditation system.

If you are not willing in EBM, now, you will rely on what? Experience !! Textbooks !! Colleagues advice !! Search the net haphazardly !!

Problems of continuous Medical Education (CME): 1. No wonder, then, that CME is growing. 2. Big, and getting huge. 3. Usually instructionally (fact) oriented. 4. But, several randomized trials have shown that it does not improve clinical performance. 5. The solution, is to make CME an EBM oriented, otherwise there is no need for it.

The problems of guidelines ? ? 1. In one study of 279 guidelines, only 7. 5 % of the guidelines described how the developers combined evidence and expert opinion, and only 6. 1 % described the values that were used to make recommendations. 2. Conflicting guidelines, Individual vs. population, Narrow focus, Specialty bias, Poor research, Comorbidities, Not reality-based, Reduction in care, Patients are not involved in development, Impact not studied and finally Hinder medical advances. 3. The solution, is to make guidelines, an EBM oriented and continuously updated, otherwise, there is no need for them.

Three solutions: Clinical performance can keep valid & up to date: 1. by learning how to practice evidence-based medicine ourselves. 2. by seeking and applying evidence-based medical summaries generated by others. 3. by applying evidence-based strategies for changing our clinical behavior.

The history of EBM: Although the formal assessment of medical interventions using controlled trials was already becoming established in the 1940 s, it was not until 1972 that Archie Cochrane, Professor of Epidemiology & director of the Medical Research Council Epidemiology Research Unit in Cardiff, expressed what later came to be known as evidence-based medicine (EBM) in his book Effectiveness and Efficiency: Random Reflections on Health Services.

Sir Archie Cochrane, The founder of EBM 1972

The history of EBM: These concepts were developed into a practical methodology by groups working at Duke University in North Carolina and Mc. Master University in Toronto in the late 1980 s and early 1990 s. In 1992, the UK government funded the establishment of the Cochrane Centre in Oxford, with the objective to facilitate the preparation of systematic reviews of randomized controlled trials of healthcare. Then it expanded into an international collaboration of centers, of which there are now thirteen, whose role is to co-ordinate the activities of 11, 500 researchers.

Steps in EBM process 1. Formulate an answerable question. 2. Find the best evidence. 3. Critically appraise the evidence. 4. Integrate with clinical expertise and patient values.
860bcee85bf56f292e35e320f06c51c2.ppt