6e3185bf4a6a6bd61c4842a0a5ffa8ad.ppt
- Количество слайдов: 20
 Evaluating Factors that Affect Nurses’ comfort Level with Emergency Interventions in the Rural Hospital Setting By: Erin Ross RN. BSN.
Evaluating Factors that Affect Nurses’ comfort Level with Emergency Interventions in the Rural Hospital Setting By: Erin Ross RN. BSN.
 Introduction The purpose of this study was to look at the educational training, certifications, technical training, and experience level of rural nurses and compare these to the nurses’ expressed level of comfort in emergency situations. The goal was to determine of each of these factors individually or in combination increased the comfort level and overall performance of rural nurses in emergency and stressful situations
Introduction The purpose of this study was to look at the educational training, certifications, technical training, and experience level of rural nurses and compare these to the nurses’ expressed level of comfort in emergency situations. The goal was to determine of each of these factors individually or in combination increased the comfort level and overall performance of rural nurses in emergency and stressful situations
 Background Nurses working in rural hospitals have several challenges when it comes to emergency situations. They have very minimal staff to assist, they have little experience with many situations, they have no specialty fields, often not physician in house, lack of adequate transport, and often minimal equipment. They must be able to perform under pressure and often alone. The situations they encounter may be ones they have rarely or never performed. These factors often lead to increased stress for these nurses.
Background Nurses working in rural hospitals have several challenges when it comes to emergency situations. They have very minimal staff to assist, they have little experience with many situations, they have no specialty fields, often not physician in house, lack of adequate transport, and often minimal equipment. They must be able to perform under pressure and often alone. The situations they encounter may be ones they have rarely or never performed. These factors often lead to increased stress for these nurses.
 Research Hypotheses 1) A greater number of years of experience will lead to a higher comfort level in the implementation of nursing interventions for nurses practicing in rural areas. 2) The greater number of current technical training and certifications held will lead to a higher comfort level in the implementation of nursing interventions for nurses practicing in rural areas 3) Experience will be a bigger factor than education or certification training in expressed comfort level for nurses practicing in rural areas.
Research Hypotheses 1) A greater number of years of experience will lead to a higher comfort level in the implementation of nursing interventions for nurses practicing in rural areas. 2) The greater number of current technical training and certifications held will lead to a higher comfort level in the implementation of nursing interventions for nurses practicing in rural areas 3) Experience will be a bigger factor than education or certification training in expressed comfort level for nurses practicing in rural areas.
 Theoretical Framework This study was based on the Middle Range Theory of Reasoned Action and Planned Behavior. It is felt that attitudes either positive or negative will affect the nurses’ perceived control, motivation, intention, the actual behavior, and the overall action and performance.
Theoretical Framework This study was based on the Middle Range Theory of Reasoned Action and Planned Behavior. It is felt that attitudes either positive or negative will affect the nurses’ perceived control, motivation, intention, the actual behavior, and the overall action and performance.
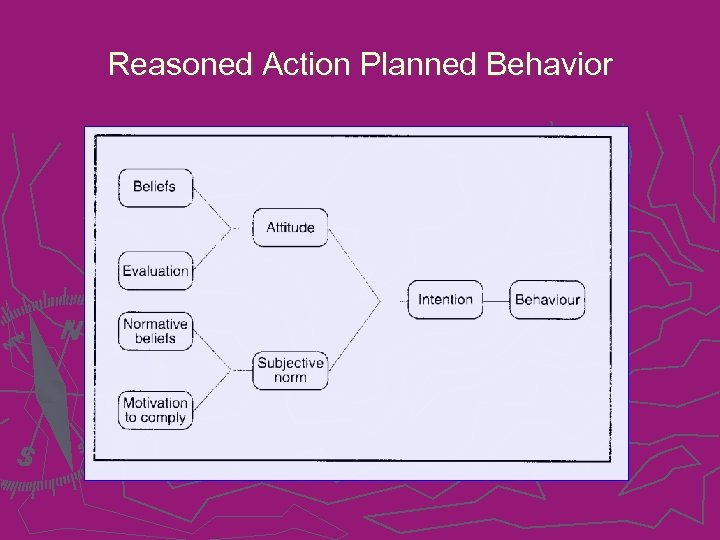 Reasoned Action Planned Behavior
Reasoned Action Planned Behavior
 Variables Dependent Variables: - Expressed comfort level -Rural hospitals Independent Variables: -Years of experience in the nursing field, as an RN, and in a rural health care setting. -Level of education -Technical training or current certifications -CPR -ACLS -CALS -PALS -Neonatal resuscitation -TNCC
Variables Dependent Variables: - Expressed comfort level -Rural hospitals Independent Variables: -Years of experience in the nursing field, as an RN, and in a rural health care setting. -Level of education -Technical training or current certifications -CPR -ACLS -CALS -PALS -Neonatal resuscitation -TNCC
 Methodology The study was conducted by a non-experimental self-reported survey. Questionnaires consisting of 17 questions were sent to 10 Critical access hospitals throughout Minnesota. The questionnaires were dispersed to the nurses by attaching them to their paycheck or in their mailbox. The nurses were asked to complete the questionnaire and return them to the researcher in a self addressed and stamped envelope provided.
Methodology The study was conducted by a non-experimental self-reported survey. Questionnaires consisting of 17 questions were sent to 10 Critical access hospitals throughout Minnesota. The questionnaires were dispersed to the nurses by attaching them to their paycheck or in their mailbox. The nurses were asked to complete the questionnaire and return them to the researcher in a self addressed and stamped envelope provided.
 Population and Sample The targeted population for this study was Registered Nurses working in rural hospitals designated as critical access hospitals in an upper midwestern state (Minnesota). The sample was Registered Nurses working in hospitals licensed for 25 beds or less in communities of less than 4, 500 people in the upper midwest (Minnesota)
Population and Sample The targeted population for this study was Registered Nurses working in rural hospitals designated as critical access hospitals in an upper midwestern state (Minnesota). The sample was Registered Nurses working in hospitals licensed for 25 beds or less in communities of less than 4, 500 people in the upper midwest (Minnesota)
 Description of Sample -Age of the respondents range from 24 -65 years old with an average of 44. 81 years old. -47 of the respondents held an Associates Degree, 15 held a Diploma in nursing, 24 held a Bachelor of Science degree, and none of the respondents held a Masters degree. -85 of the respondents were female and 1 was male -Years of experience in nursing ranged from 5. 5 months to 43 years and 5. 1 months with an average of 21 years and 5 months. -Years as an RN ranged from 5. 5 months to 43 years 2 months for an average of 14. 9 years and 5. 4 months -Years of experience in rural healthcare ranged from 5. 5 months to 38 years 3 months for an average of 14. 9 years and 4. 9 months. -All 86 respondents currently had CPR, 83 were certified in ACLS, 62 were certified in CALS, 48 were certified in neonatal resuscitation, 29 were certified in PALS, and 52 were certified in TNCC
Description of Sample -Age of the respondents range from 24 -65 years old with an average of 44. 81 years old. -47 of the respondents held an Associates Degree, 15 held a Diploma in nursing, 24 held a Bachelor of Science degree, and none of the respondents held a Masters degree. -85 of the respondents were female and 1 was male -Years of experience in nursing ranged from 5. 5 months to 43 years and 5. 1 months with an average of 21 years and 5 months. -Years as an RN ranged from 5. 5 months to 43 years 2 months for an average of 14. 9 years and 5. 4 months -Years of experience in rural healthcare ranged from 5. 5 months to 38 years 3 months for an average of 14. 9 years and 4. 9 months. -All 86 respondents currently had CPR, 83 were certified in ACLS, 62 were certified in CALS, 48 were certified in neonatal resuscitation, 29 were certified in PALS, and 52 were certified in TNCC
 Data Collection A total of 147 questionnaires were sent to 10 Critical Access Hospitals in Minnesota. 86 completed questionnaires were returned for a return rate of 59%.
Data Collection A total of 147 questionnaires were sent to 10 Critical Access Hospitals in Minnesota. 86 completed questionnaires were returned for a return rate of 59%.
 -The questionnaire asked several demographic data. -The questionnaire asked the nurses if they felt comfortable performing emergency nursing interventions. -The quustionnaire asked the nurses to rank their comfort of each of the seven interventions on a scale of 1 -5 (1 being very comfortable and 5 being very uncomfortable). If they had no experience with the intervention they were to indicate it by circling 6. -The questionnaire also asked two open ended questions. The first asked the respondents to explain strategies used to increase comfort. The second asked for any additional comments about working in a rural hospital setting.
-The questionnaire asked several demographic data. -The questionnaire asked the nurses if they felt comfortable performing emergency nursing interventions. -The quustionnaire asked the nurses to rank their comfort of each of the seven interventions on a scale of 1 -5 (1 being very comfortable and 5 being very uncomfortable). If they had no experience with the intervention they were to indicate it by circling 6. -The questionnaire also asked two open ended questions. The first asked the respondents to explain strategies used to increase comfort. The second asked for any additional comments about working in a rural hospital setting.
 Findings -The overall comfort level expressed was 70% -Full code/cardiac arrest was 2. 4 with no experience -Chest tube insertion was 2. 7 with 13 with no experience -Thoracedntesis was 2. 3 with 5 nurses reporting no experience -Traumatic head injuries was 2. 8 with seven with no experience -Precip delivery was 3. 6 with 20 with no experience -RSI was 3. 0 with 11 with no experience -Managing drug overdose was 2. 9 with 5 with no experience.
Findings -The overall comfort level expressed was 70% -Full code/cardiac arrest was 2. 4 with no experience -Chest tube insertion was 2. 7 with 13 with no experience -Thoracedntesis was 2. 3 with 5 nurses reporting no experience -Traumatic head injuries was 2. 8 with seven with no experience -Precip delivery was 3. 6 with 20 with no experience -RSI was 3. 0 with 11 with no experience -Managing drug overdose was 2. 9 with 5 with no experience.
 Findings (continued) Age. Years of nursing experience. Years as an RNYears of experience in a rural health care setting. Degree held. Certifications curently held-
Findings (continued) Age. Years of nursing experience. Years as an RNYears of experience in a rural health care setting. Degree held. Certifications curently held-
 Common Themes Strategies Used to Increase Comfort Level -Continuing education, training, and certifications -Self review and Study -Personal experience -Observing others with more experience -Reviewing policies, procedures, and equipment periodically -Working as a team -Be aggressive to get as much experience as possible -Being overall organized and prepared -Utilizing additional staff when needed -Know you are doing the best you can with what you have -Stay calm, don’t panic -Evaluate after the situation and make necessary changes to policies and procedures
Common Themes Strategies Used to Increase Comfort Level -Continuing education, training, and certifications -Self review and Study -Personal experience -Observing others with more experience -Reviewing policies, procedures, and equipment periodically -Working as a team -Be aggressive to get as much experience as possible -Being overall organized and prepared -Utilizing additional staff when needed -Know you are doing the best you can with what you have -Stay calm, don’t panic -Evaluate after the situation and make necessary changes to policies and procedures
 Common Themes Additional Comments about Working in a Rural Hospital -37 Positive comments (including diversity, great experience, knowing you patients, knowing your team members, using all of your skills, and caring for people you know) -26 Negative comments (including poor staffing, unpredictable census, no physician in house, difficulty retaining skills not used frequently, overwhelming responsibility, and limited resources) -24 Neutral comments (including being prepared for anything, caring for people you know, and relying on your team members)
Common Themes Additional Comments about Working in a Rural Hospital -37 Positive comments (including diversity, great experience, knowing you patients, knowing your team members, using all of your skills, and caring for people you know) -26 Negative comments (including poor staffing, unpredictable census, no physician in house, difficulty retaining skills not used frequently, overwhelming responsibility, and limited resources) -24 Neutral comments (including being prepared for anything, caring for people you know, and relying on your team members)
 “We’re a Jack/Jane of all Trades Yet Master at None!!”
“We’re a Jack/Jane of all Trades Yet Master at None!!”
 Conclusions -Age of the nurse is a significant factor. -Years of experience in nursing was significant for greater than 5 years of experience -Years of experience as an RN was a significant factor, peaking at 21 -30 years of experience as an RN having the highest overall comfort level of any factors. -Years of experience in rural nursing was significant for nurses with more than 5 years of experience. -Nurses with a Diploma in nursing were more comfortable - Certifications increase comfort level. Nurses with CALS and TNCC were significantly more comfortable than nurses with CPR only or ACLS. -Nurses with neonatal resuscitation were most comfortable in delivering a precipitous delivery. -Nurses with PALS were most comfortable in managing drug overdoses
Conclusions -Age of the nurse is a significant factor. -Years of experience in nursing was significant for greater than 5 years of experience -Years of experience as an RN was a significant factor, peaking at 21 -30 years of experience as an RN having the highest overall comfort level of any factors. -Years of experience in rural nursing was significant for nurses with more than 5 years of experience. -Nurses with a Diploma in nursing were more comfortable - Certifications increase comfort level. Nurses with CALS and TNCC were significantly more comfortable than nurses with CPR only or ACLS. -Nurses with neonatal resuscitation were most comfortable in delivering a precipitous delivery. -Nurses with PALS were most comfortable in managing drug overdoses
 Recommendations -Develop a mentoring program where a nurse in a larger urban hospital would pair with nurses in the rural setting. -Shadow in a larger emergency room setting to visually experience emergency situations. -Have organized policies and procedures with all equipment needed together in a box/cart -Practicing mock codes and case scenarios - Monthly scavenger hunts - Consistent and properly functioning equipment - Proper training and certification in all areas in which the nurse if expected to function. - Pair newer nurses with more experienced nurses
Recommendations -Develop a mentoring program where a nurse in a larger urban hospital would pair with nurses in the rural setting. -Shadow in a larger emergency room setting to visually experience emergency situations. -Have organized policies and procedures with all equipment needed together in a box/cart -Practicing mock codes and case scenarios - Monthly scavenger hunts - Consistent and properly functioning equipment - Proper training and certification in all areas in which the nurse if expected to function. - Pair newer nurses with more experienced nurses
 Recommendations for Further Research -Study be conducted with a larger sample size -Study be conducted throughout several states -Perform a study comparing comfort level of nurses working in larger urban emergency room settings compared to nurses working in rural hospital settings -Evaluate the helplessness experienced by nurses working in rural hospitals where they don’t have the manpower, resources, or equipment to adequately care for someone in an emergency, leading to a poor outcome for the patient.
Recommendations for Further Research -Study be conducted with a larger sample size -Study be conducted throughout several states -Perform a study comparing comfort level of nurses working in larger urban emergency room settings compared to nurses working in rural hospital settings -Evaluate the helplessness experienced by nurses working in rural hospitals where they don’t have the manpower, resources, or equipment to adequately care for someone in an emergency, leading to a poor outcome for the patient.


