d2b2b82bc28691d16ff1c95429a8a62a.ppt
- Количество слайдов: 45
 Epidemiology of Maternal and Neonatal Mortality in Malawi Dr. Chisale Mhango FRCOG NPC Training in MNH 1
Epidemiology of Maternal and Neonatal Mortality in Malawi Dr. Chisale Mhango FRCOG NPC Training in MNH 1
 MATERNAL MORTALITY IN LOW RESOURCE COUNTRIES: How to accelerated reduction Objectives: • Understand the issues relating to MMR • Review Global and Local Progress on Reduction of MMR – Key article from The Lancet • Discuss effective strategies
MATERNAL MORTALITY IN LOW RESOURCE COUNTRIES: How to accelerated reduction Objectives: • Understand the issues relating to MMR • Review Global and Local Progress on Reduction of MMR – Key article from The Lancet • Discuss effective strategies
 Outline of presentation 1. 2. 3. 4. 5. Definitions of terms Global and Local Trends in MMR and NNM Causes of maternal and neonatal mortality Current data on place of delivery in Malawi Coverage for Skilled Birth Attendants in Malawi 6. Rationale for new roles for TBAs NPC Training in MNH 3
Outline of presentation 1. 2. 3. 4. 5. Definitions of terms Global and Local Trends in MMR and NNM Causes of maternal and neonatal mortality Current data on place of delivery in Malawi Coverage for Skilled Birth Attendants in Malawi 6. Rationale for new roles for TBAs NPC Training in MNH 3
 Statistical measurements. . Definitions Maternal Mortality Number of Ratio maternal deaths during a given period per 100, 000 live births during the same timeperiod Maternal Mortality Rate Adult life time risk of maternal death Number of maternal deaths in a given period per 100, 000 women of reproductive age during the same time-period The probability of dying from a maternal cause during a woman’s reproductive lifespan. Alternative definition of MD in ICD 10 (1992) Pregnancy-related death The death of a woman while pregnant or within 42 days of termination of pregnancy, irrespective of the duration or the site of the pregnancy, from any cause related to or aggravated by the pregnancy or its management but not from accidental or incidental causes. Late maternal death The death of a woman from direct or indirect obstetric causes, more than 42 days but less than one year after termination of pregnancy. 4
Statistical measurements. . Definitions Maternal Mortality Number of Ratio maternal deaths during a given period per 100, 000 live births during the same timeperiod Maternal Mortality Rate Adult life time risk of maternal death Number of maternal deaths in a given period per 100, 000 women of reproductive age during the same time-period The probability of dying from a maternal cause during a woman’s reproductive lifespan. Alternative definition of MD in ICD 10 (1992) Pregnancy-related death The death of a woman while pregnant or within 42 days of termination of pregnancy, irrespective of the duration or the site of the pregnancy, from any cause related to or aggravated by the pregnancy or its management but not from accidental or incidental causes. Late maternal death The death of a woman from direct or indirect obstetric causes, more than 42 days but less than one year after termination of pregnancy. 4
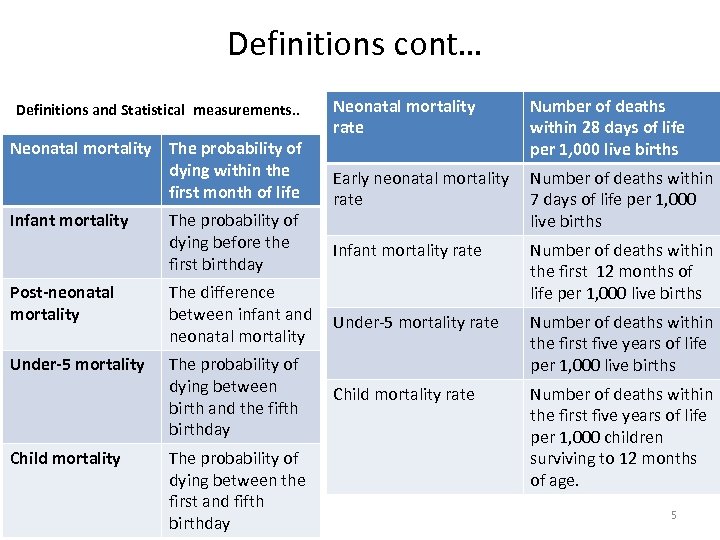 Definitions cont… Definitions and Statistical measurements. . Neonatal mortality The probability of dying within the first month of life Infant mortality The probability of dying before the first birthday Neonatal mortality rate Number of deaths within 28 days of life per 1, 000 live births Early neonatal mortality rate Number of deaths within 7 days of life per 1, 000 live births Infant mortality rate Number of deaths within the first 12 months of life per 1, 000 live births Post-neonatal mortality The difference between infant and neonatal mortality Under-5 mortality rate Under-5 mortality The probability of dying between birth and the fifth birthday Number of deaths within the first five years of life per 1, 000 live births Child mortality rate Number of deaths within the first five years of life per 1, 000 children surviving to 12 months of age. Child mortality The probability of dying between the first and fifth birthday 5
Definitions cont… Definitions and Statistical measurements. . Neonatal mortality The probability of dying within the first month of life Infant mortality The probability of dying before the first birthday Neonatal mortality rate Number of deaths within 28 days of life per 1, 000 live births Early neonatal mortality rate Number of deaths within 7 days of life per 1, 000 live births Infant mortality rate Number of deaths within the first 12 months of life per 1, 000 live births Post-neonatal mortality The difference between infant and neonatal mortality Under-5 mortality rate Under-5 mortality The probability of dying between birth and the fifth birthday Number of deaths within the first five years of life per 1, 000 live births Child mortality rate Number of deaths within the first five years of life per 1, 000 children surviving to 12 months of age. Child mortality The probability of dying between the first and fifth birthday 5
 Methods of defining Maternal Mortality
Methods of defining Maternal Mortality
 Millennium Development Goal 5: Improve Maternal Health Target 5. A: Reduce by 3/4, between 1990 and 2015, the maternal mortality ratio Indicators: Maternal mortality ratio Proportion of births attended by skilled health personnel Target 5. B: Achieve, by 2015, universal access to reproductive health Indicators: Contraceptive prevalence rate Adolescent birth rate Antenatal care coverage Unmet need for family planning
Millennium Development Goal 5: Improve Maternal Health Target 5. A: Reduce by 3/4, between 1990 and 2015, the maternal mortality ratio Indicators: Maternal mortality ratio Proportion of births attended by skilled health personnel Target 5. B: Achieve, by 2015, universal access to reproductive health Indicators: Contraceptive prevalence rate Adolescent birth rate Antenatal care coverage Unmet need for family planning
 Millennium Development Goal 4: Reduce Child Mortality Target 4: Reduce by 2/3, between 1990 and 2015, the child mortality rate Indicators: Under-five mortality rate Infant mortality rate Proportion of 1 year-old children immunized against measles 8
Millennium Development Goal 4: Reduce Child Mortality Target 4: Reduce by 2/3, between 1990 and 2015, the child mortality rate Indicators: Under-five mortality rate Infant mortality rate Proportion of 1 year-old children immunized against measles 8
 The Lancet Article Maternal mortality for 181 countries, 1980– 2008: a systematic analysis of progress towards Millennium Development Goal 5 Margaret C Hogan, Kyle J Foreman, Mohsen Naghavi, Stephanie Y Ahn, Mengru Wang, Susanna M Makela, Alan D Lopez, Rafael Lozano, Christopher J L Murray Volume 375 May 8, 2010, pp. 1609 -1623.
The Lancet Article Maternal mortality for 181 countries, 1980– 2008: a systematic analysis of progress towards Millennium Development Goal 5 Margaret C Hogan, Kyle J Foreman, Mohsen Naghavi, Stephanie Y Ahn, Mengru Wang, Susanna M Makela, Alan D Lopez, Rafael Lozano, Christopher J L Murray Volume 375 May 8, 2010, pp. 1609 -1623.

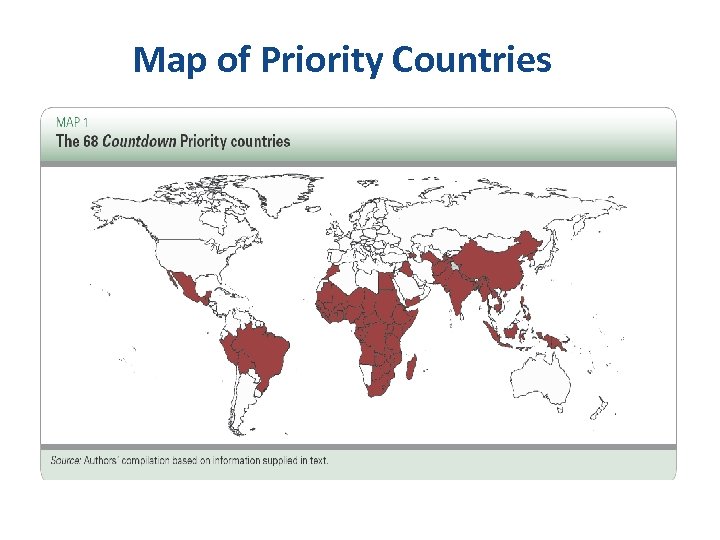 Map of Priority Countries
Map of Priority Countries
 Global Situation • 180 -210 million pregnancies annually • 80 million unwanted pregnancies • 50 million induced abortions • 20 million unsafe abortions • 68, 000 deaths from unsafe abortion • 20 million women suffer from maternal morbidity • Estimated 350, 000 to 450, 000 maternal deaths • 3 million babies are born dead • Almost 10 million children under age of 5 die • Of which 3 million newborns die within the first week • 500, 000 infants are infected with HIV
Global Situation • 180 -210 million pregnancies annually • 80 million unwanted pregnancies • 50 million induced abortions • 20 million unsafe abortions • 68, 000 deaths from unsafe abortion • 20 million women suffer from maternal morbidity • Estimated 350, 000 to 450, 000 maternal deaths • 3 million babies are born dead • Almost 10 million children under age of 5 die • Of which 3 million newborns die within the first week • 500, 000 infants are infected with HIV
 Every Single minute… … 380 women become pregnant … 190 women face an unplanned or unwanted pregnancy … 110 women experience pregnancy-related complications … 40 women have an unsafe abortion … 1 woman dies
Every Single minute… … 380 women become pregnant … 190 women face an unplanned or unwanted pregnancy … 110 women experience pregnancy-related complications … 40 women have an unsafe abortion … 1 woman dies
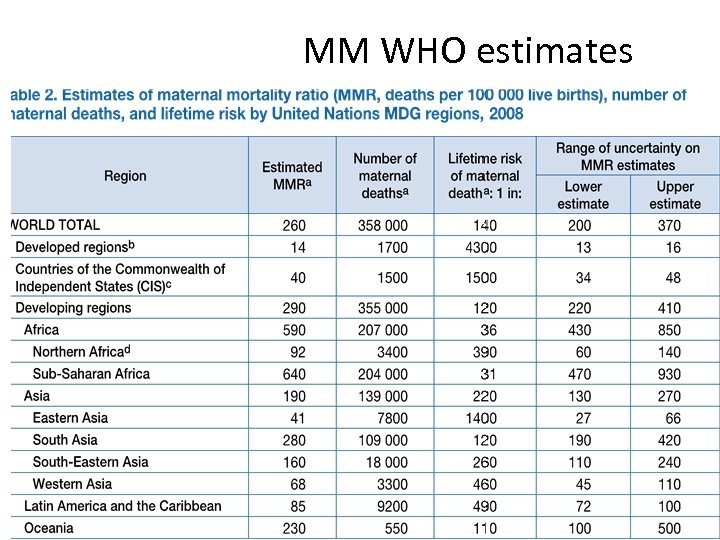 MM WHO estimates
MM WHO estimates
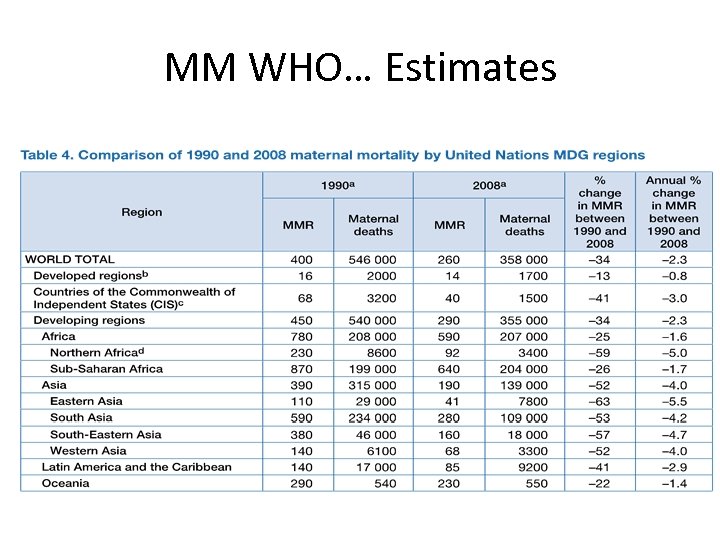 MM WHO… Estimates
MM WHO… Estimates
 Maternal Mortality: The latest data • For the first time, new data indicate that we are seeing real progress in reducing maternal mortality worldwide. • A new study published in The Lancet in May 2010 revealed that the number of women dying from pregnancy-related causes has declined from 526, 300 in 1980 to 342, 900 in 2008. • The finding contradict previous research which showed very little change in reducing maternal mortality, and represent a powerful opportunity to show that investments to reduce maternal mortality actually work. “These numbers should now act as a catalyst, not a brake, for accelerated action on MDG-5, including scaled-up resource commitments. Investment incontrovertibly saves the lives of women during pregnancy. ” Richard Horton Source: Hogan MC et al. Maternal mortality for 181 countries, 1980 -2008: a systematic analysis of progress towards Millennium Development Goal 5. The Lancet 2010: published online April 12. doi: 10. 1016/S 0140 -6736(10)60518 -1.
Maternal Mortality: The latest data • For the first time, new data indicate that we are seeing real progress in reducing maternal mortality worldwide. • A new study published in The Lancet in May 2010 revealed that the number of women dying from pregnancy-related causes has declined from 526, 300 in 1980 to 342, 900 in 2008. • The finding contradict previous research which showed very little change in reducing maternal mortality, and represent a powerful opportunity to show that investments to reduce maternal mortality actually work. “These numbers should now act as a catalyst, not a brake, for accelerated action on MDG-5, including scaled-up resource commitments. Investment incontrovertibly saves the lives of women during pregnancy. ” Richard Horton Source: Hogan MC et al. Maternal mortality for 181 countries, 1980 -2008: a systematic analysis of progress towards Millennium Development Goal 5. The Lancet 2010: published online April 12. doi: 10. 1016/S 0140 -6736(10)60518 -1.
 Current Situation 6 Countries Account for 50% of Maternal Mortality - India - Afghanistan - Nigeria - Ethiopia - Pakistan - Democratic Republic of the Congo
Current Situation 6 Countries Account for 50% of Maternal Mortality - India - Afghanistan - Nigeria - Ethiopia - Pakistan - Democratic Republic of the Congo
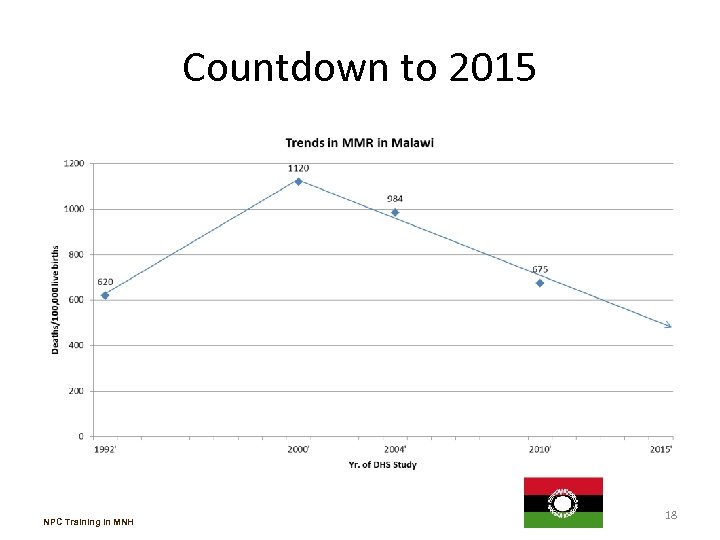 Countdown to 2015 NPC Training in MNH 18
Countdown to 2015 NPC Training in MNH 18
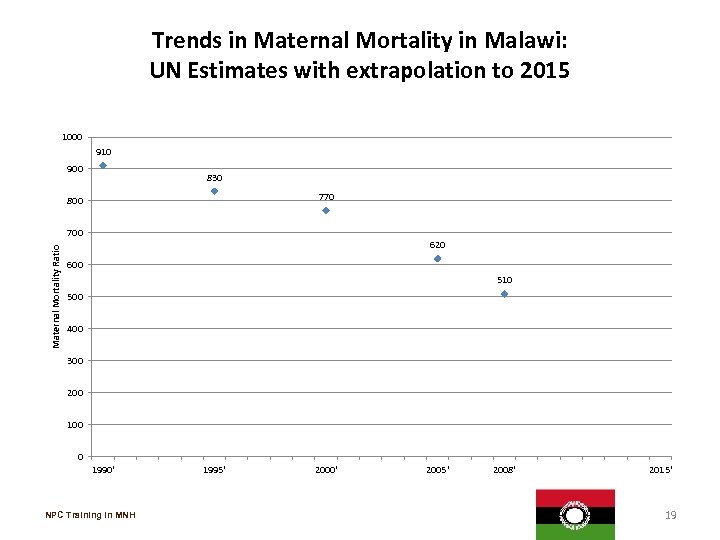 Trends in Maternal Mortality in Malawi: UN Estimates with extrapolation to 2015 1000 910 900 830 770 800 Maternal Mortality Ratio 700 620 600 510 500 400 300 200 100 0 1990' NPC Training in MNH 1995' 2000' 2005' 2008' 2015' 19
Trends in Maternal Mortality in Malawi: UN Estimates with extrapolation to 2015 1000 910 900 830 770 800 Maternal Mortality Ratio 700 620 600 510 500 400 300 200 100 0 1990' NPC Training in MNH 1995' 2000' 2005' 2008' 2015' 19
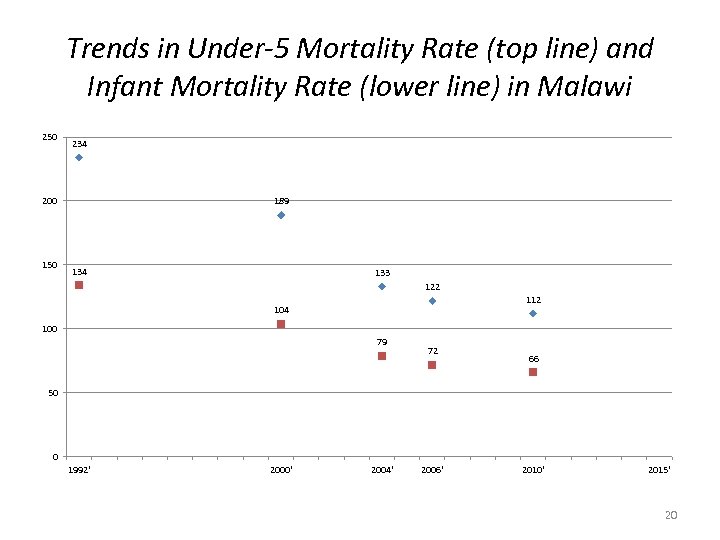 Trends in Under-5 Mortality Rate (top line) and Infant Mortality Rate (lower line) in Malawi 250 234 200 150 189 134 133 122 112 104 100 79 72 66 50 0 1992' 2000' 2004' 2006' 2010' 2015' 20
Trends in Under-5 Mortality Rate (top line) and Infant Mortality Rate (lower line) in Malawi 250 234 200 150 189 134 133 122 112 104 100 79 72 66 50 0 1992' 2000' 2004' 2006' 2010' 2015' 20
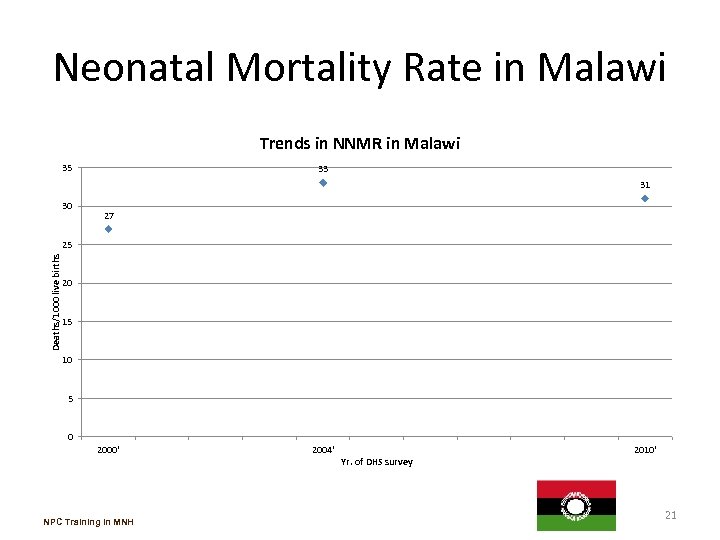 Neonatal Mortality Rate in Malawi Trends in NNMR in Malawi 35 33 31 30 27 Deaths/1000 live births 25 20 15 10 5 0 2000' NPC Training in MNH 2004' Yr. of DHS survey 2010' 21
Neonatal Mortality Rate in Malawi Trends in NNMR in Malawi 35 33 31 30 27 Deaths/1000 live births 25 20 15 10 5 0 2000' NPC Training in MNH 2004' Yr. of DHS survey 2010' 21
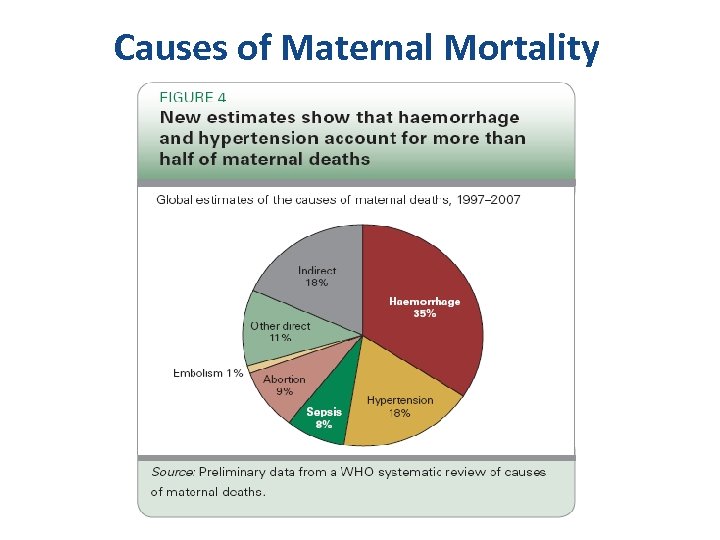 Causes of Maternal Mortality
Causes of Maternal Mortality
 Main direct causes of maternal deaths in Malawi 1. 2. 3. 4. Haemorrhage after childbirth (27%) Sepsis after childbirth (23%) Hypertension of Pregnancy (17%) Complications of unsafe abortion (16%) ALL THESE CONDITIONS ARE COMMONEST WITH CHILDBIRTH OR ABORTION OUTSIDE HEALTH FACILITIES NPC Training in MNH Source: MDHS 2010 23
Main direct causes of maternal deaths in Malawi 1. 2. 3. 4. Haemorrhage after childbirth (27%) Sepsis after childbirth (23%) Hypertension of Pregnancy (17%) Complications of unsafe abortion (16%) ALL THESE CONDITIONS ARE COMMONEST WITH CHILDBIRTH OR ABORTION OUTSIDE HEALTH FACILITIES NPC Training in MNH Source: MDHS 2010 23
 Main causes of neonatal deaths 1. Birth asphyxia – lack of resuscitation skills at birth 2. Low birth weight – Prematurity leading to • Cold injury • RDS – HIV 3. Severe infections – Home births NPC Training in MNH 24
Main causes of neonatal deaths 1. Birth asphyxia – lack of resuscitation skills at birth 2. Low birth weight – Prematurity leading to • Cold injury • RDS – HIV 3. Severe infections – Home births NPC Training in MNH 24
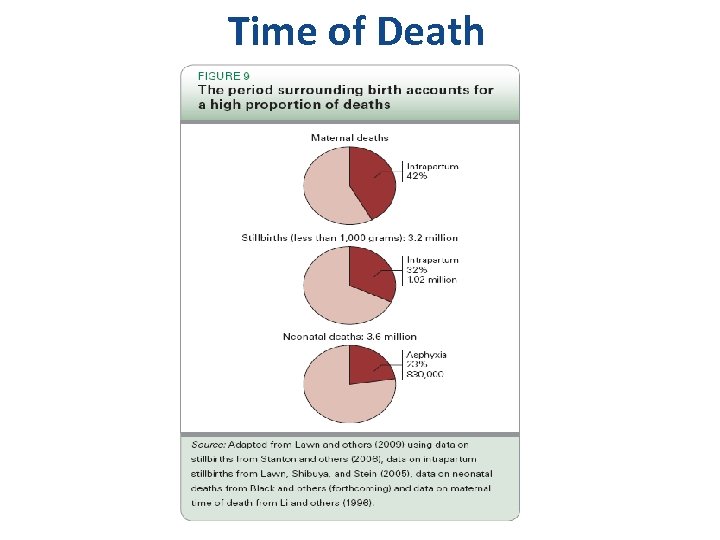 Time of Death
Time of Death
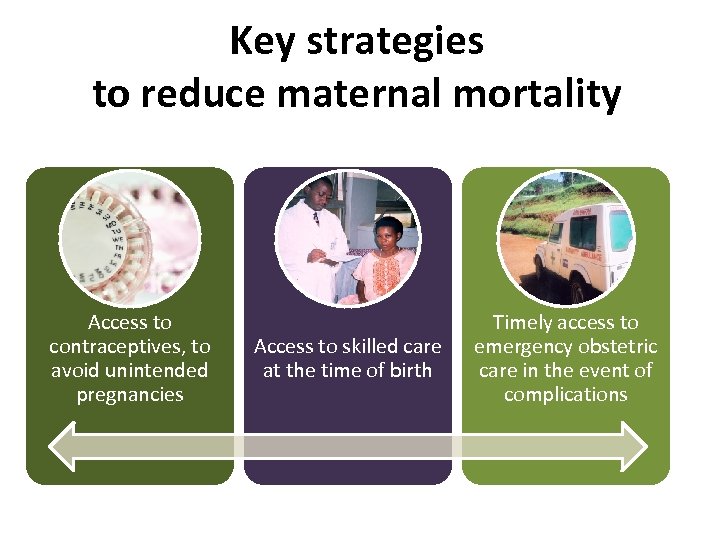 Key strategies to reduce maternal mortality Access to contraceptives, to avoid unintended pregnancies Access to skilled care at the time of birth Timely access to emergency obstetric care in the event of complications
Key strategies to reduce maternal mortality Access to contraceptives, to avoid unintended pregnancies Access to skilled care at the time of birth Timely access to emergency obstetric care in the event of complications
 What factors are driving maternal mortality in Malawi? Not only medical issues, but also a social, economic, political and human rights issues • Poverty – No food security • Low female literacy rates – Cultural factors • High fertility rate • Poor functioning health infrastructure – Contraceptive services – – • Insufficient focus on quality of care Inadequate number of skilled health workers. Physical infrastructure Basic tools of the trade Slow adoption of evidence based policy “I am going to fetch a baby. The journey is dangerous and I may not return …”
What factors are driving maternal mortality in Malawi? Not only medical issues, but also a social, economic, political and human rights issues • Poverty – No food security • Low female literacy rates – Cultural factors • High fertility rate • Poor functioning health infrastructure – Contraceptive services – – • Insufficient focus on quality of care Inadequate number of skilled health workers. Physical infrastructure Basic tools of the trade Slow adoption of evidence based policy “I am going to fetch a baby. The journey is dangerous and I may not return …”
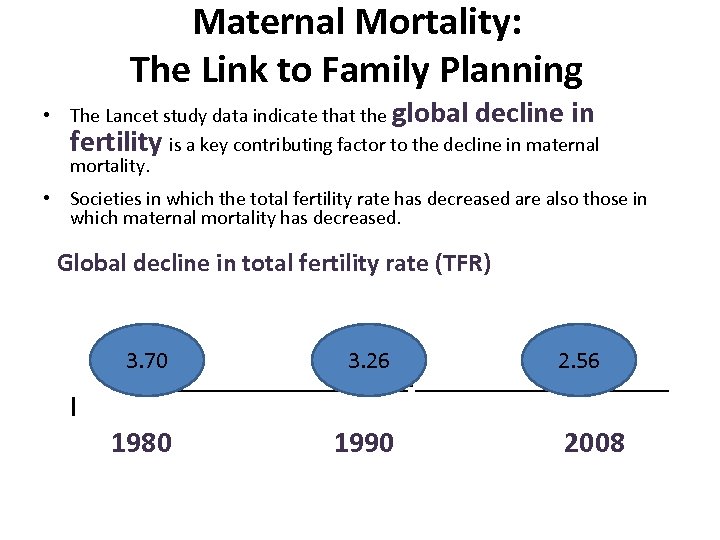 Maternal Mortality: The Link to Family Planning • The Lancet study data indicate that the global decline in fertility is a key contributing factor to the decline in maternal mortality. • Societies in which the total fertility rate has decreased are also those in which maternal mortality has decreased. Global decline in total fertility rate (TFR) 3. 70 I 3. 26 1980 1990 2. 56 I_________I_________ 2008
Maternal Mortality: The Link to Family Planning • The Lancet study data indicate that the global decline in fertility is a key contributing factor to the decline in maternal mortality. • Societies in which the total fertility rate has decreased are also those in which maternal mortality has decreased. Global decline in total fertility rate (TFR) 3. 70 I 3. 26 1980 1990 2. 56 I_________I_________ 2008
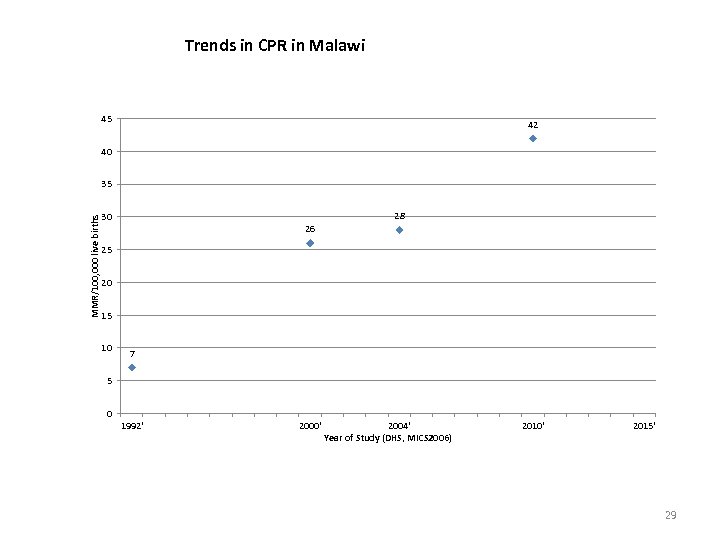 Trends in CPR in Malawi 45 42 40 MMR/100, 000 live births 35 28 30 26 25 20 15 10 7 5 0 1992' 2000' 2004' Year of Study (DHS, MICS 2006) 2010' 2015' 29
Trends in CPR in Malawi 45 42 40 MMR/100, 000 live births 35 28 30 26 25 20 15 10 7 5 0 1992' 2000' 2004' Year of Study (DHS, MICS 2006) 2010' 2015' 29
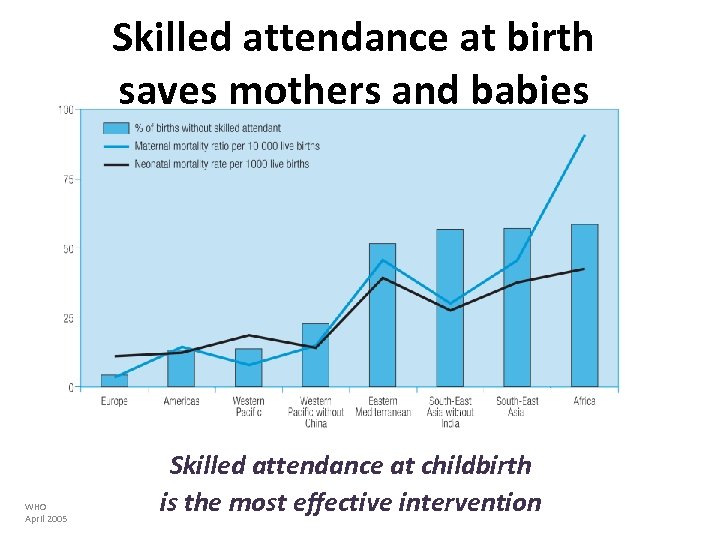 Skilled attendance at birth saves mothers and babies WHO April 2005 Skilled attendance at childbirth is the most effective intervention
Skilled attendance at birth saves mothers and babies WHO April 2005 Skilled attendance at childbirth is the most effective intervention
 Access to skilled birth attendants About 35 % of pregnant women in developing countries have no access to, or contact with, health personnel before delivery, and only 57 % give birth with a skilled attendant present.
Access to skilled birth attendants About 35 % of pregnant women in developing countries have no access to, or contact with, health personnel before delivery, and only 57 % give birth with a skilled attendant present.
 Access to emergency obstetric care Em. OC 42 % of all pregnancies everywhere experience a complication. In 15 % of all pregnancies, the complications are life- threatening. 61 % of maternal deaths occur just before, during, or just after delivery, often from complications that cannot be predicted and are difficult to prevent Therefore… it is critical that every woman have access to emergency obstetric care
Access to emergency obstetric care Em. OC 42 % of all pregnancies everywhere experience a complication. In 15 % of all pregnancies, the complications are life- threatening. 61 % of maternal deaths occur just before, during, or just after delivery, often from complications that cannot be predicted and are difficult to prevent Therefore… it is critical that every woman have access to emergency obstetric care
 Why Women Do Not Access Health Services? Distance from health services Lack of transportation Cost Multiple demands on women’s time Lack of decision-making power within the family Attitude of health care providers Limited access to education Inadequate health care services Discriminatory or inadequate laws or health care policies Culture Community
Why Women Do Not Access Health Services? Distance from health services Lack of transportation Cost Multiple demands on women’s time Lack of decision-making power within the family Attitude of health care providers Limited access to education Inadequate health care services Discriminatory or inadequate laws or health care policies Culture Community
 Reasons for decrease of maternal mortality • • Global decrease in Total Fertility Rate (TFR) Increase of income in low-income countries Increase in maternal education Increase in skilled birth attendants from approximately 25% to 45– 55%
Reasons for decrease of maternal mortality • • Global decrease in Total Fertility Rate (TFR) Increase of income in low-income countries Increase in maternal education Increase in skilled birth attendants from approximately 25% to 45– 55%
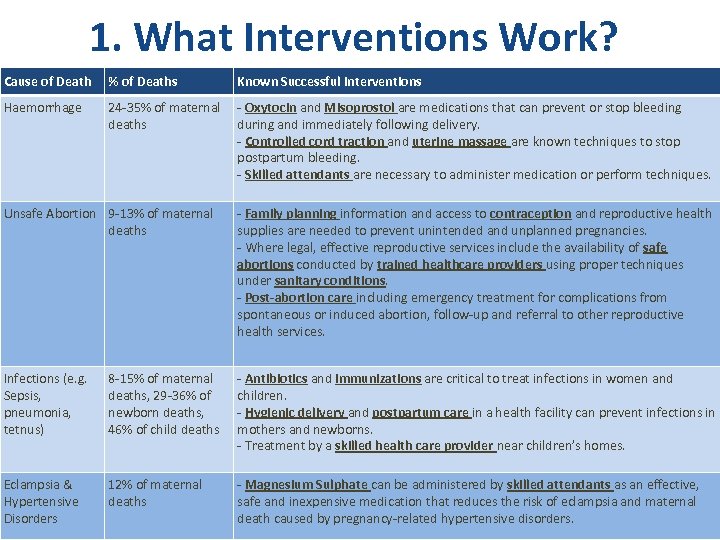 1. What Interventions Work? Cause of Death % of Deaths Known Successful Interventions Haemorrhage 24 -35% of maternal deaths - Oxytocin and Misoprostol are medications that can prevent or stop bleeding during and immediately following delivery. - Controlled cord traction and uterine massage are known techniques to stop postpartum bleeding. - Skilled attendants are necessary to administer medication or perform techniques. Unsafe Abortion 9 -13% of maternal deaths - Family planning information and access to contraception and reproductive health supplies are needed to prevent unintended and unplanned pregnancies. - Where legal, effective reproductive services include the availability of safe abortions conducted by trained healthcare providers using proper techniques under sanitary conditions. - Post-abortion care including emergency treatment for complications from spontaneous or induced abortion, follow-up and referral to other reproductive health services. Infections (e. g. Sepsis, pneumonia, tetnus) 8 -15% of maternal deaths, 29 -36% of newborn deaths, 46% of child deaths - Antibiotics and immunizations are critical to treat infections in women and children. - Hygienic delivery and postpartum care in a health facility can prevent infections in mothers and newborns. - Treatment by a skilled health care provider near children’s homes. Eclampsia & Hypertensive Disorders 12% of maternal deaths - Magnesium Sulphate can be administered by skilled attendants as an effective, safe and inexpensive medication that reduces the risk of eclampsia and maternal death caused by pregnancy-related hypertensive disorders.
1. What Interventions Work? Cause of Death % of Deaths Known Successful Interventions Haemorrhage 24 -35% of maternal deaths - Oxytocin and Misoprostol are medications that can prevent or stop bleeding during and immediately following delivery. - Controlled cord traction and uterine massage are known techniques to stop postpartum bleeding. - Skilled attendants are necessary to administer medication or perform techniques. Unsafe Abortion 9 -13% of maternal deaths - Family planning information and access to contraception and reproductive health supplies are needed to prevent unintended and unplanned pregnancies. - Where legal, effective reproductive services include the availability of safe abortions conducted by trained healthcare providers using proper techniques under sanitary conditions. - Post-abortion care including emergency treatment for complications from spontaneous or induced abortion, follow-up and referral to other reproductive health services. Infections (e. g. Sepsis, pneumonia, tetnus) 8 -15% of maternal deaths, 29 -36% of newborn deaths, 46% of child deaths - Antibiotics and immunizations are critical to treat infections in women and children. - Hygienic delivery and postpartum care in a health facility can prevent infections in mothers and newborns. - Treatment by a skilled health care provider near children’s homes. Eclampsia & Hypertensive Disorders 12% of maternal deaths - Magnesium Sulphate can be administered by skilled attendants as an effective, safe and inexpensive medication that reduces the risk of eclampsia and maternal death caused by pregnancy-related hypertensive disorders.
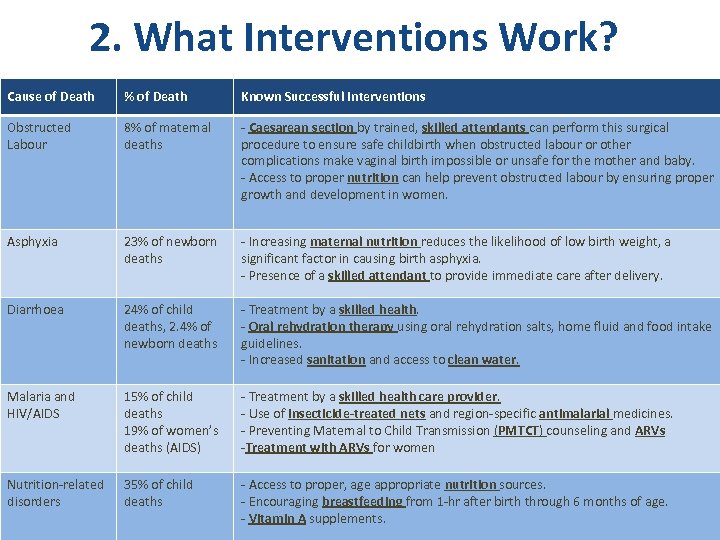 2. What Interventions Work? Cause of Death % of Death Known Successful Interventions Obstructed Labour 8% of maternal deaths - Caesarean section by trained, skilled attendants can perform this surgical procedure to ensure safe childbirth when obstructed labour or other complications make vaginal birth impossible or unsafe for the mother and baby. - Access to proper nutrition can help prevent obstructed labour by ensuring proper growth and development in women. Asphyxia 23% of newborn deaths - Increasing maternal nutrition reduces the likelihood of low birth weight, a significant factor in causing birth asphyxia. - Presence of a skilled attendant to provide immediate care after delivery. Diarrhoea 24% of child deaths, 2. 4% of newborn deaths - Treatment by a skilled health. - Oral rehydration therapy using oral rehydration salts, home fluid and food intake guidelines. - Increased sanitation and access to clean water. Malaria and HIV/AIDS 15% of child deaths 19% of women’s deaths (AIDS) - Treatment by a skilled health care provider. - Use of insecticide-treated nets and region-specific antimalarial medicines. - Preventing Maternal to Child Transmission (PMTCT) counseling and ARVs -Treatment with ARVs for women Nutrition-related disorders 35% of child deaths - Access to proper, age appropriate nutrition sources. - Encouraging breastfeeding from 1 -hr after birth through 6 months of age. - Vitamin A supplements.
2. What Interventions Work? Cause of Death % of Death Known Successful Interventions Obstructed Labour 8% of maternal deaths - Caesarean section by trained, skilled attendants can perform this surgical procedure to ensure safe childbirth when obstructed labour or other complications make vaginal birth impossible or unsafe for the mother and baby. - Access to proper nutrition can help prevent obstructed labour by ensuring proper growth and development in women. Asphyxia 23% of newborn deaths - Increasing maternal nutrition reduces the likelihood of low birth weight, a significant factor in causing birth asphyxia. - Presence of a skilled attendant to provide immediate care after delivery. Diarrhoea 24% of child deaths, 2. 4% of newborn deaths - Treatment by a skilled health. - Oral rehydration therapy using oral rehydration salts, home fluid and food intake guidelines. - Increased sanitation and access to clean water. Malaria and HIV/AIDS 15% of child deaths 19% of women’s deaths (AIDS) - Treatment by a skilled health care provider. - Use of insecticide-treated nets and region-specific antimalarial medicines. - Preventing Maternal to Child Transmission (PMTCT) counseling and ARVs -Treatment with ARVs for women Nutrition-related disorders 35% of child deaths - Access to proper, age appropriate nutrition sources. - Encouraging breastfeeding from 1 -hr after birth through 6 months of age. - Vitamin A supplements.
 3. What Interventions Work? childbirth Ø Access to quality care – Antenatal care for --pregnancy and childbirth – Skilled attendance at birth, including Ø - Antenatal care and neonatal care emergency obstetric – Skilled attendance for mothers - - Immediate postnatal care at birth, and newborns including emergency obstetric and neonatal care Access to family planning - Immediate postnatal care for – - Counseling – - Services and newborns mothers – - Modern contraception Ø Access to family planning Ø Access to safe abortion (when legal) - Counseling - Services - Modern contraception Ø Access to safe abortion (when legal) Ø Strong health systems – - Scaling-up critical health interventions – - Training health care professionals – - Training of mid-wives Ø Accelerated access to life-saving, interventions, medicines and vaccines – - Vaccines to target pneumonia, tetanus, and diarrhea – - Prevention, screening and treatment of HIV and STIs – - Treatment and prevention of 37 malaria, pneumonia and diarrhea
3. What Interventions Work? childbirth Ø Access to quality care – Antenatal care for --pregnancy and childbirth – Skilled attendance at birth, including Ø - Antenatal care and neonatal care emergency obstetric – Skilled attendance for mothers - - Immediate postnatal care at birth, and newborns including emergency obstetric and neonatal care Access to family planning - Immediate postnatal care for – - Counseling – - Services and newborns mothers – - Modern contraception Ø Access to family planning Ø Access to safe abortion (when legal) - Counseling - Services - Modern contraception Ø Access to safe abortion (when legal) Ø Strong health systems – - Scaling-up critical health interventions – - Training health care professionals – - Training of mid-wives Ø Accelerated access to life-saving, interventions, medicines and vaccines – - Vaccines to target pneumonia, tetanus, and diarrhea – - Prevention, screening and treatment of HIV and STIs – - Treatment and prevention of 37 malaria, pneumonia and diarrhea
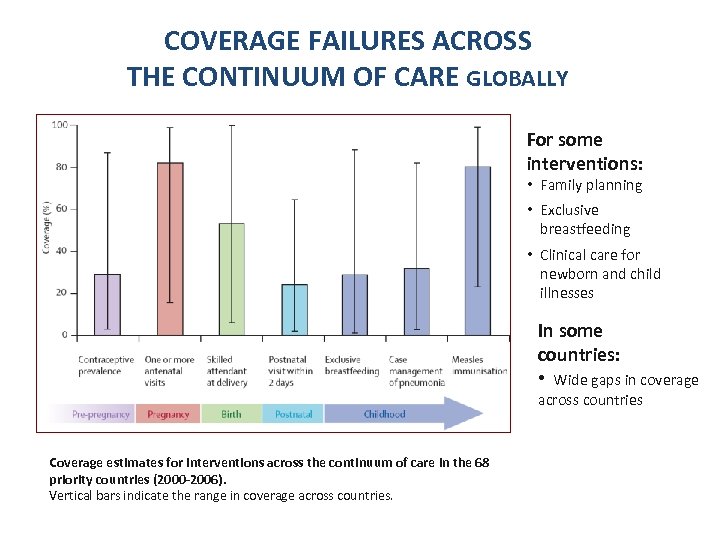 COVERAGE FAILURES ACROSS THE CONTINUUM OF CARE GLOBALLY For some interventions: • Family planning • Exclusive breastfeeding • Clinical care for newborn and child illnesses In some countries: • Wide gaps in coverage across countries Coverage estimates for interventions across the continuum of care in the 68 priority countries (2000 -2006). Vertical bars indicate the range in coverage across countries.
COVERAGE FAILURES ACROSS THE CONTINUUM OF CARE GLOBALLY For some interventions: • Family planning • Exclusive breastfeeding • Clinical care for newborn and child illnesses In some countries: • Wide gaps in coverage across countries Coverage estimates for interventions across the continuum of care in the 68 priority countries (2000 -2006). Vertical bars indicate the range in coverage across countries.
 Place of Delivery in Malawi URBAN 1. RURAL 84% in health facilities a. 85% had skilled attendance at birth 2. For all Malawi 72% delivered in health facilities 3. 98% women with tertiary education had skilled attendance at childbirth compared to 63% women without education. NPC Training in MNH 1. 71% in health facilities a. 70% had skilled attendance at birth 2. For all Malawi, 73% women had skilled attendance at childbirth Source: MDHS 2010 39
Place of Delivery in Malawi URBAN 1. RURAL 84% in health facilities a. 85% had skilled attendance at birth 2. For all Malawi 72% delivered in health facilities 3. 98% women with tertiary education had skilled attendance at childbirth compared to 63% women without education. NPC Training in MNH 1. 71% in health facilities a. 70% had skilled attendance at birth 2. For all Malawi, 73% women had skilled attendance at childbirth Source: MDHS 2010 39
 Which women and newborns were dying the most in Malawi? Mothers Neonates • Women who delivered or procured abortion outside the health facilities, especially when they developed, PPH, PIH and sepsis • Babies born without skilled attendant present at birth. – Women who developed these complications while in health facility, had treatment initiated earlier and were less likely to die. NPC Training in MNH – Suffered the most from birth asphyxia, cold injury and infection, especially if they were under weight or premature 40
Which women and newborns were dying the most in Malawi? Mothers Neonates • Women who delivered or procured abortion outside the health facilities, especially when they developed, PPH, PIH and sepsis • Babies born without skilled attendant present at birth. – Women who developed these complications while in health facility, had treatment initiated earlier and were less likely to die. NPC Training in MNH – Suffered the most from birth asphyxia, cold injury and infection, especially if they were under weight or premature 40
 Rationale for Change of TBA roles 1. International WHO and local studies revealed that investment in TBAs did not contribute significantly to reduction of maternal and neonatal deaths 2. The option of TBA births prevented the scale up of skilled attendance at child births – As soon as the TBA option was removed in Malawi, health facility births soared, distance of health facility had been overestimated NPC Training in MNH 41
Rationale for Change of TBA roles 1. International WHO and local studies revealed that investment in TBAs did not contribute significantly to reduction of maternal and neonatal deaths 2. The option of TBA births prevented the scale up of skilled attendance at child births – As soon as the TBA option was removed in Malawi, health facility births soared, distance of health facility had been overestimated NPC Training in MNH 41
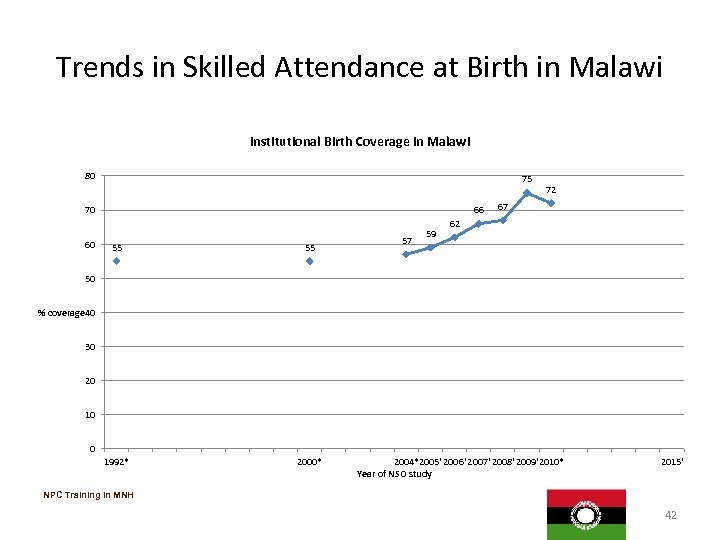 Trends in Skilled Attendance at Birth in Malawi Institutional Birth Coverage in Malawi 80 75 66 70 60 55 55 1992* 2000* 57 59 72 67 62 50 % coverage 40 30 20 10 0 2004*2005' 2006' 2007' 2008' 2009'2010* Year of NSO study 2015' NPC Training in MNH 42
Trends in Skilled Attendance at Birth in Malawi Institutional Birth Coverage in Malawi 80 75 66 70 60 55 55 1992* 2000* 57 59 72 67 62 50 % coverage 40 30 20 10 0 2004*2005' 2006' 2007' 2008' 2009'2010* Year of NSO study 2015' NPC Training in MNH 42
 There is no better time to reduce maternal and child death in Malawi - Commited leadership critical
There is no better time to reduce maternal and child death in Malawi - Commited leadership critical
 References/reading • • • • B-Lynch C, Keith LG, Lalonde AB, Karoshi M. A Textbook of Post Partum Hemorrhage: A comprehensive guide to evaluation, management and surgical intervention. Sapiens Publishing, 2006. Chowdhury ME, Botlero R, Koblinsky M, Saha SK, Dieltiens G, Ronsmans C. Determinants of reduction in maternal mortality in Matlab, Bangladesh: a 30 -year cohort study. Lancet 2007; 370: 1320– 28. Countdown Coverage Writing Group, on behalf of the Countdown to 2015 Core Group. Countdown to 2015 for maternal, newborn, and child survival: the 2008 report on tracking coverage of interventions. Lancet 2008; 371: 1247– 58 Deneux-Tharaux C, Berg C, Bouvier-Colle MH, et al. Underreporting of pregnancy-related mortality in the United States and Europe. Obstet Gynecol 2005; 106: 684– 92. Fortney JA, Leong M. Saving Mother’s Lives: Programs that work. Clin Obstet Gynecol 2009; 52: 224. Graham WJ, Ahmed S, Stanton C, Abou-Zahr CL, Campbell OM. Measuring maternal mortality: an overview of opportunities and options for developing countries. BMC Med 2008; 6: 12. Hogan MC, Foreman KJ, Naghavi M, Ahn SY, Wang M, Makela SM, Lopez AD, Lozano R, Landagan OZ, Barrios EB. An estimation procedure for a spatial-temporal model. Stat Probab Lett 2007; 77: 401– 06. The Millennium Development Goals Report 2008. New York: United Nations, 2008. Murray CJL, et al. Maternal mortality for 181 countries, 1980– 2008: a systematic analysis of progress towards Millennium Development Goal 5. Lancet 2010, 375: 1609 -1623 Ronsmans C, Graham WJ, on behalf of The Lancet Maternal Survival Series steering group. Maternal mortality: who, when, where, and why. Lancet 2006; 368: 1189– 200. WHO. International statistical classification of diseases and related health problems, tenth revision instruction manual (2 edn). Geneva: World Health Organization, 2004. WHO, PMNCH. Joint Action Plan for Women’s and Children’s health. Geneva: World Health Organization, Partnership for Maternal, Newborn and Child Health, 2010 Draft. WHO, UNICEF. Countdown to 2015 Decade Report (2000 -2010): Taking stock of maternal, newborn and child survival. Geneva: World Health Organization and UNICEF, 2010. WHO, UNICEF, UNFPA, World Bank. Maternal mortality in 2005: estimates developed by WHO, UNICEF, UNFPA and the World Bank. Geneva: World Health Organization. 2007. WHO Mortality Database. Geneva: World Health Organization, 2010. http: //www. who. int/whosis/mort/download/en/index. html (accessed March 23, 2010).
References/reading • • • • B-Lynch C, Keith LG, Lalonde AB, Karoshi M. A Textbook of Post Partum Hemorrhage: A comprehensive guide to evaluation, management and surgical intervention. Sapiens Publishing, 2006. Chowdhury ME, Botlero R, Koblinsky M, Saha SK, Dieltiens G, Ronsmans C. Determinants of reduction in maternal mortality in Matlab, Bangladesh: a 30 -year cohort study. Lancet 2007; 370: 1320– 28. Countdown Coverage Writing Group, on behalf of the Countdown to 2015 Core Group. Countdown to 2015 for maternal, newborn, and child survival: the 2008 report on tracking coverage of interventions. Lancet 2008; 371: 1247– 58 Deneux-Tharaux C, Berg C, Bouvier-Colle MH, et al. Underreporting of pregnancy-related mortality in the United States and Europe. Obstet Gynecol 2005; 106: 684– 92. Fortney JA, Leong M. Saving Mother’s Lives: Programs that work. Clin Obstet Gynecol 2009; 52: 224. Graham WJ, Ahmed S, Stanton C, Abou-Zahr CL, Campbell OM. Measuring maternal mortality: an overview of opportunities and options for developing countries. BMC Med 2008; 6: 12. Hogan MC, Foreman KJ, Naghavi M, Ahn SY, Wang M, Makela SM, Lopez AD, Lozano R, Landagan OZ, Barrios EB. An estimation procedure for a spatial-temporal model. Stat Probab Lett 2007; 77: 401– 06. The Millennium Development Goals Report 2008. New York: United Nations, 2008. Murray CJL, et al. Maternal mortality for 181 countries, 1980– 2008: a systematic analysis of progress towards Millennium Development Goal 5. Lancet 2010, 375: 1609 -1623 Ronsmans C, Graham WJ, on behalf of The Lancet Maternal Survival Series steering group. Maternal mortality: who, when, where, and why. Lancet 2006; 368: 1189– 200. WHO. International statistical classification of diseases and related health problems, tenth revision instruction manual (2 edn). Geneva: World Health Organization, 2004. WHO, PMNCH. Joint Action Plan for Women’s and Children’s health. Geneva: World Health Organization, Partnership for Maternal, Newborn and Child Health, 2010 Draft. WHO, UNICEF. Countdown to 2015 Decade Report (2000 -2010): Taking stock of maternal, newborn and child survival. Geneva: World Health Organization and UNICEF, 2010. WHO, UNICEF, UNFPA, World Bank. Maternal mortality in 2005: estimates developed by WHO, UNICEF, UNFPA and the World Bank. Geneva: World Health Organization. 2007. WHO Mortality Database. Geneva: World Health Organization, 2010. http: //www. who. int/whosis/mort/download/en/index. html (accessed March 23, 2010).
 45
45


