6f9bbbb2cb2b8659a9a8d71d31a9e59e.ppt
- Количество слайдов: 24

EMERGENCY CARE FOR THE ELDER WITH ABDOMINAL PAIN Module # 1 Ed Vandenberg MD CMD Geriatric section OVAMC & Section of Geriatrics 981320 UNMC Omaha NE 68198 -1320 evandenb@unmc. edu Web: geriatrics. unmc. edu 402 -559 -7512 Adapted from Bill Lyons, M. D. & (from R. M. Mc. Namara, M. D. for SAEM) Updated 11 -20 -06

PROCESS Series of modules and questions Step #1: Power point module with voice overlay Step #2: Case-based question and answer Step # 3: Proceed to additional modules or take a break

Overview of All Three Modules objectives Module 1 & 2 Ø List the unique features and (atypical) presentations of abdominal pain in elders Ø Identify priorities for initial triage Ø List initial management to stabilize Ø List appropriate historical information to elicit Ø Describe appropriate physical exam Ø List appropriate and timely lab and diagnostic evaluation Module 3 Ø Describe the presentations and diagnostic approach to: l Other diagnostic possibilities of acute abdominal pain in this population

CASE HISTORY Ø 70 year old male Ø “Passed out in bathroom” Ø Wife drove him to hospital, as he refused ambulance transport ( transfer via Coupe de Ville) Ø Questions you want the triage nurse to ask his wife? ( besides where did you park your “aircraft carrier”?

PATIENT’S TRIAGE REPORT Ø Straining on the toilet Ø Felt lightheaded Ø “Woke up” on floor Ø Bloating, abdominal discomfort Ø What additional information do you want?

ESSENTIAL TRIAGE HISTORY Injury from fall (especially neck pain)? Ø Exact location of abdominal pain? Ø Ø Ø Patients History Ø No reported injury Ø Pain in mid to low abdomen Chest pain? Dyspnea? Any major medical problems? No chest pain, No dyspnea Ø History of CHF Ø

PATIENT STATUS IN TRIAGE Ø Appearance: pale, diaphoretic Ø BP 96/70 HR 110 RR 22 T 37. 6 What’s wrong with these vital signs? QUESTIONS TO ANSWER IMMEDIATELY Ø What should this patient’s priority status be? Ø What measures should be instituted now?

Decisions on Status TRIAGE CONSIDERATIONS Ø Ø Ø Serious illness (syncope) Ill appearance is red flag Abnormal V. S. worrisome Abdominal pain is red flag Prior heart disease is red flag Upper abdominal pain ( must also include possibility of Acute MI) Ø Classify patient as Ø High priority or urgent ( unstable)

What measures would you want immediately instituted by triage staff? Immediate Ø Venous access Ø Cardiac monitoring Ø Physician notification Ø 12 -lead ECG Ø CBC and BMP Ø Cardiac enzymes Delayed; Ø Review of Advance directives ( but in this patient this shouldn’t’ be delayed too long)

ABDOMINAL PAIN IN ELDERLY PATIENTS (2) Issues to keep in mind about Elders Ø Abdominal pain is presenting complaint in 3 -6% of elders presenting to ED. Ø 50 -60% require admission Ø About a third require surgery Issues to “tighten your sphincter” about Elders Ø Mortality 9 X that of younger patients Ø Overall mortality 10 -14%
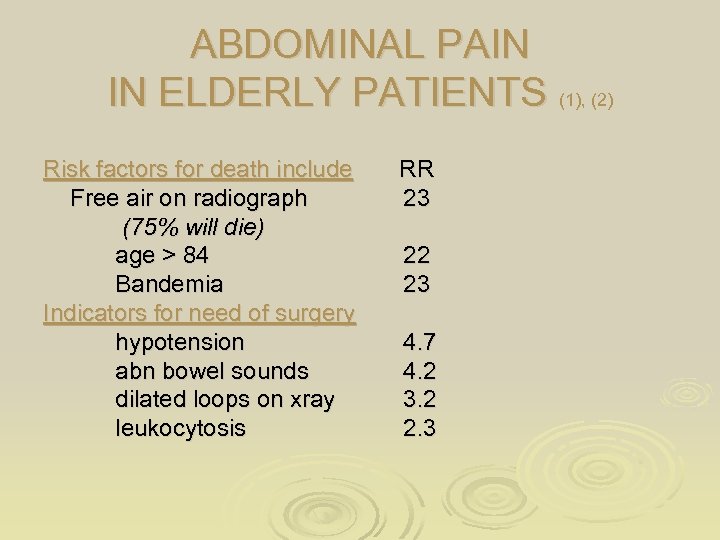
ABDOMINAL PAIN IN ELDERLY PATIENTS (1), (2) Risk factors for death include Free air on radiograph (75% will die) age > 84 Bandemia Indicators for need of surgery hypotension abn bowel sounds dilated loops on xray leukocytosis RR 23 22 23 4. 7 4. 2 3. 2 2. 3

ABDOMINAL PAIN IN ELDERLY PATIENTS (1) Diagnoses Infection Mechanical problems Ulcers Genitourinary dz Malignancy Billiary dz Cardiac dz Pulmonary dz Other % 19% 16% 8% 8% 7% 6% 4% 2% 29%

ABDOMINAL PAIN IN ELDERLY PATIENTS (3) Ø The “Bad news” ED Physicians diagnoses correctly < 65 y. o. 67% of the time > 65 y. o. 44% of the time

CASE UPDATE Transferred to monitored bed Ø Rhythm: sinus tachycardia Ø Near syncope therefore checking orthostatic BP Ø IV fluids Ø IV Fluid type and Rate? How to decide? -First best choice ( NS or LR) -Know Maintenance : 30 cc/kg/hr -Then estimate based on fluid deficits and stability of patient -Most common bolus in elderly: 250 – 500 cc and reevaluate

FOREMOST CONSIDERATION What’s the most life threatening diagnosis? Ø Ruptured AAA (Elderly man with hypotension and abdominal pain) Ø Health care provider should quickly assess: appearance, airway, breathing, circulation, Trauma? Ø Time, nature of pain onset Ø Back pain? Ø Size, tenderness of abdominal aorta? Ø Our patient Ø Appearance: pale, diaphoretic, Ø BP 96/70 HR 110 RR 22 T 37. 6, Sa. O 2 95% RA Ø No evidence of trauma Ø Diffuse Abdominal pain X 4 d. Ø No back pain Ø Aorta not enlarged or tender

“Book larning” ABDOMINAL AORTIC ANEURYSM (1), (2), (5) Ø Common in elders (6% of 80 yo males) Ø #1 cause of fatalities per case in elders with abdominal pain Ø Rupture can be lethal (70% mortality) Ø Consider admission if abdominal aorta diameter > 5 cm
RUPTURED AAA: PRESENTATION Ø Abdominal pain in 70 -80% Ø Pain often sudden, severe Ø Back pain in >50% Ø Syncope Ø Hypotension in 70 -96% Ø Key: tender, enlarged aorta

RUPTURED AAA: MISDIAGNOSIS Ø Up to 30% initially missed Ø Atypical pain locations (back, flank) Ø Leading wrong diagnosis: renal colic Ø Hypotension incorrectly called “vagal”

The AAA scenario can be prevented (3), (4) SCREEN for ABDOMINAL AORTIC ANEURYSM (AAA) “new in 2005” Recomendations: one-time screening for abdominal aortic aneurysm (AAA) by ultrasonography in men aged 65 to 75 who have ever smoked. [i] USPSTF ( B ) Ø ( not beneficial to screen: women, never-smoker men, all men > 75 yo) Data: Ø Ø -screening for AAA and surgical repair of large AAAs (5. 5 cm or more) in men aged 65 to 75 who have ever smoked (current and former smokers) leads to decreased AAA-specific mortality. -good evidence that abdominal ultrasonography is an accurate screening test for AAA -still beneficial despite; Major treatment harms: operative mortality rate of 2% to 6%

The End of Module One on the EMERGENCY CARE FOR THE ELDER WITH ADOMINAL PAIN

Post-test Asymptomatic aneurysms in the elderly should be 1. Considered to be a normal variant for the aged 2. Followed only if increasing in size 3. Ignored in patients under age 75 y. o. 4. Considered for surgical repair if > 5 cm

Answer: 4. Considered for surgical repair if > 5 cm Aneurysms and Dissections Ø Aneurysms and dissections are primarily diseases of older persons. Aneurysms most commonly occur in the abdominal aorta, thoracic aorta, popliteal arteries, and iliac arteries, and they are usually atherosclerotic. Symptomatic aneurysms are medical emergencies that require immediate surgery. Asymptomatic aneurysms should be followed for rate of growth. Older persons with an abdominal aortic aneurysm > 5 cm should be considered for surgical repair. Elective surgical repair of a descending thoracic aortic aneurysm or a thoracoabdominal aortic aneurysm in older persons should be considered if the aneurysm is ≥ 5 cm in maximal diameter. All older persons considered for elective surgical repair should be evaluated for coexistent CAD.

The pain associated with thoracic aortic dissection is severe and often tearing. Stroke, paraplegia, syncope, pulse loss with or without ischemic pain, and CHF resulting from severe AR secondary to the dissection may occur. Diagnosis is best made by transesophageal echocardiography, magnetic resonance imaging, or computed tomography. Surgical intervention is the treatment of choice for acute proximal dissection and for complicated acute distal dissection (ie, complicated by rupture, expansion, saccular aneurysm formation, vital organ or limb ischemia, or continued pain). Endostenting, a new procedure for treating aneurysm, is under investigation. Medical treatment with afterload reduction and βblockers is the treatment of choice for uncomplicated distal dissection, for stable, isolated arch dissection, and for uncomplicated dissection presenting 2 weeks or later after onset. Ø End Ø

Readings and References Recommended Readings and references Society of Academic Emergency Medicine (SAEM) References: (1)Solomon DH, Lo. Cicero J, Rosenthal RA. New Frontiers in Geriatrics Research: An Agenda for Surgical and Related Medical Specialties. 2004 (1)Marco CA, Schoenfeld CN, Keyl PM, et. al. Abdominal pain in geriatric emergency patients: variables associated with adverse outcomes. Acad Emerg Med 1998; Dec; 5(12): 1163 -1168. (2)Kizer KW, Vassar MJ. Emergency department diagnosis of abdomina disorders in the elderly. Am J Emerg Med 1998; Jul 16(4): 357 -362. (3) Craig Fleming, M. D. , Screening for Abdominal Aortic Aneurysm: A Best-Evidence Systematic Review. Ann Intern Med 2005; 142: 203 -11 (4) Wilmink AB, Forshaw M, Quick CR, et. al. Accuracy of serial screening for abdominal aortic aneurysms by ultrasound. J Med Screen 2002; 9(3): 125 -127. (5) Johansen K, Kohler TR, Nicholls SC, et. al. Ruputured abdominal aortic aneurysm: the Harborview experience. J Vasc Surg. 1991 Feb; 13(2): 240 -245; discussion 245 -247.
6f9bbbb2cb2b8659a9a8d71d31a9e59e.ppt