8abc83b2039cd68869c9e6c3c822b3c7.ppt
- Количество слайдов: 39

Electronic Medical Record Benefits to Clinicians March 27, 2009 Curtis L. Whitehair, MD, FAAPMR

Curtis L. Whitehair, MD, FAAPMR v. Board Certified Physiatrist Physical Medicine & Rehabilitation v. Fellow American Academy of Physical Medicine & Rehabilitation • President – Maryland Society of PM&R v. National Rehabilitation Hospital, Washington, DC Medical Director – Outpatient Center for Orthopedic Rehabilitation Medical Director – Oncology Rehabilitation Program, NRH/NRH Regional Rehab

Shepherd University, Shepherdstown WV ◦ Major Business Administration Information Systems & Computer Programming ◦ Minor Communications CASE Consultant – Datatel, Inc. ◦ 3 Books ETK: Introduction to Screen Processing ETK: Introduction to Batch and Report Writing Managing Custom Source

Ross University School of Medicine, NY/Dominica Internship – Family Medicine at Medical College of Virginia (VCU), Richmond VA Residency – Physical Medicine & Rehabilitation at NRH/GTUH, Washington, DC

What are Electronic Medical Records? According to the IOM, an EHR system has several key capabilities: ◦ It’s a longitudinal collection of electronic health information for and about persons. ◦ It provides immediate electronic access to person- and population-level information by authorized users. ◦ It provides knowledge and decision-support systems that enhance the quality, safety, and efficiency of patient care. ◦ It supports efficient processes for health care delivery.

What are we trying to solve? Where’s the problem? When are we going to do it?

Physicians spend 38% of their time writing chart notes. 35 -39% of total hospital operating cost are spent on patient and provider communication activates. Medical records could not be located 30% of the time when needed. Once found the volume of information in them was often so large that it became unmanageable. It was shown that simply organizing information flow sheets accelerated retrieval of needed data at least 4 fold.
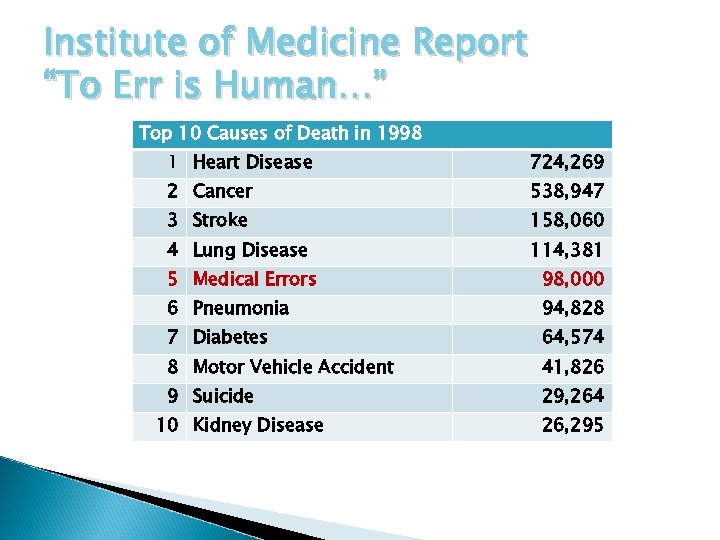
Institute of Medicine Report “To Err is Human…” Top 10 Causes of Death in 1998 1 Heart Disease 724, 269 2 Cancer 538, 947 3 Stroke 158, 060 4 Lung Disease 114, 381 5 Medical Errors 98, 000 6 Pneumonia 94, 828 7 Diabetes 64, 574 8 Motor Vehicle Accident 41, 826 9 Suicide 29, 264 10 Kidney Disease 26, 295

Medicare No-pay List – Oct. 1, 2008 Stage III, IV pressure ulcers Fall or trauma resulting in serious injury Vascular catheter-associated infection Catheter-associated urinary tract infection Foreign object retained after surgery Certain surgical site infections Air embolism Blood incompatibility Certain manifestations of poor blood sugar control Certain deep vein thromboses or pulmonary embolisms
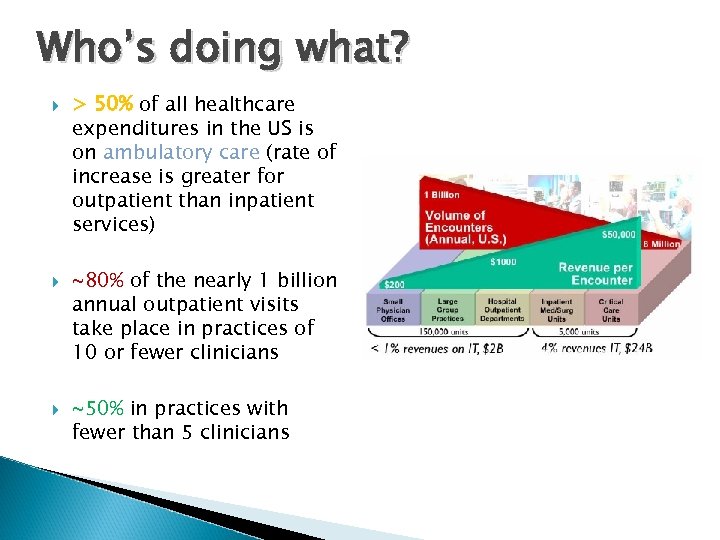
Who’s doing what? > 50% of all healthcare expenditures in the US is on ambulatory care (rate of increase is greater for outpatient than inpatient services) ~80% of the nearly 1 billion annual outpatient visits take place in practices of 10 or fewer clinicians ~50% in practices with fewer than 5 clinicians
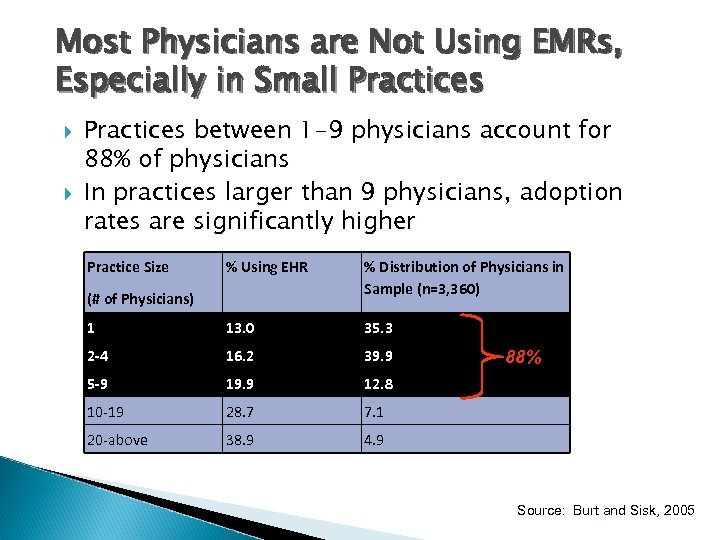
Most Physicians are Not Using EMRs, Especially in Small Practices between 1 -9 physicians account for 88% of physicians In practices larger than 9 physicians, adoption rates are significantly higher Practice Size % Using EHR % Distribution of Physicians in Sample (n=3, 360) 1 13. 0 35. 3 2 -4 16. 2 39. 9 5 -9 19. 9 12. 8 10 -19 28. 7 7. 1 20 -above 38. 9 4. 9 (# of Physicians) 88% Source: Burt and Sisk, 2005

And what was once considered good care… Reactive episodic visits “Top-of-mind” decisions Paper-based ad hoc prescribing Non-interactive documentation No news = good news

…is no longer Reactive episodic visits Reactive and proactive care “Top-of-mind” decisions Embedded CDSS/guidelines Paper-based ad hoc prescribing Non-interactive documentation No news = good news Knowledge based Medication Management (e. Rx) Interactive documentation Orders loop management

A Moment in the Physician Office While promoting medical quality and E/M compliance, in 15 minutes a provider must be able to: ◦ Perform and complete documentation of a medically indicated, audit-proof, level 4 or level 5 patient visit with individualized narrative information in all appropriate areas of the medical record including completion of counseling the patient ordering test ordering treatment charge entry

Value Configuration of the Organization A value configuration describes how value is created in a company for its customers. It shows how the most important primary and secondary activates function to create value for customers. It represents the way a particular organization conducts business.
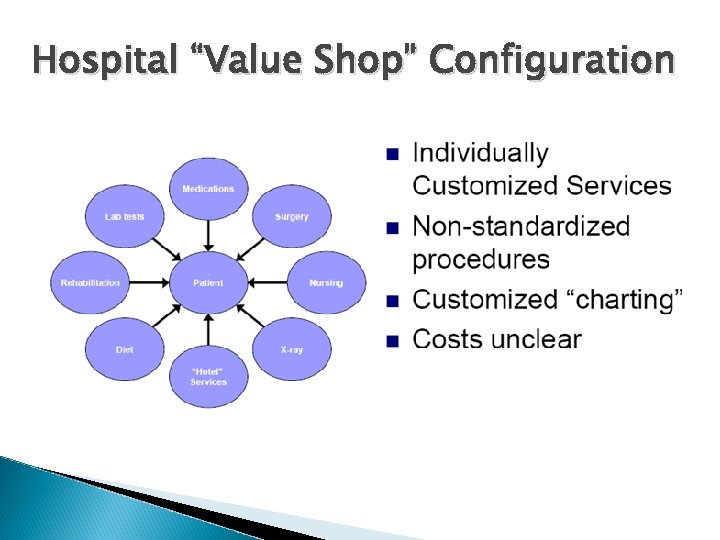
Hospital “Value Shop” Configuration
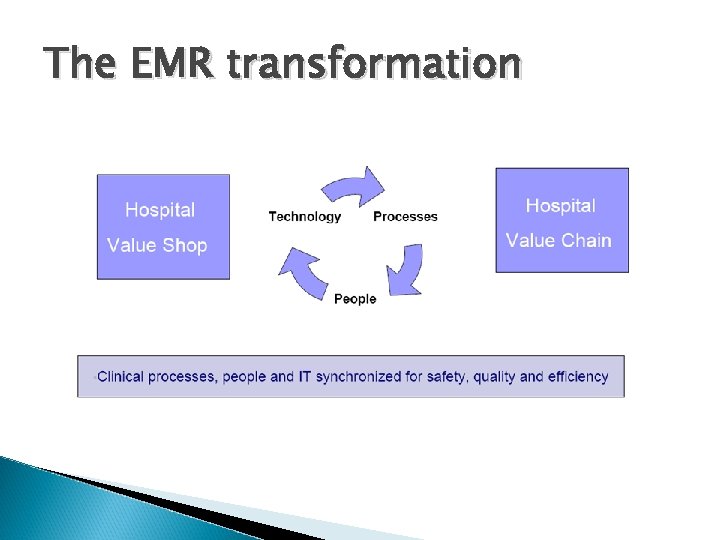
The EMR transformation
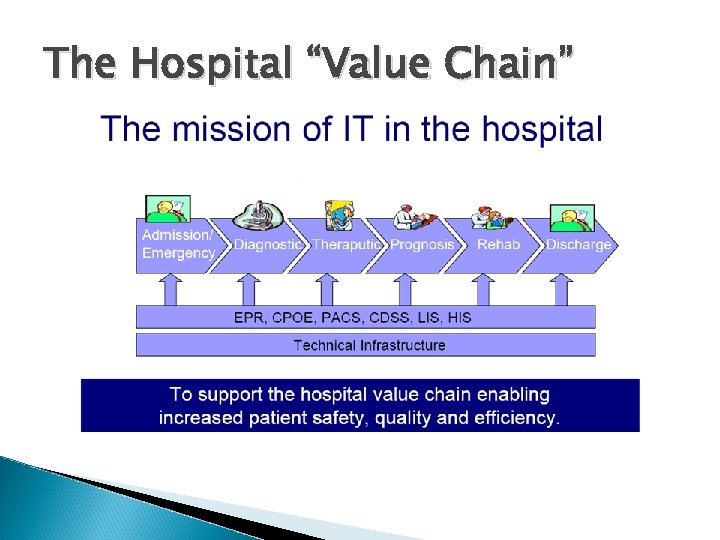
The Hospital “Value Chain”

Remember The development of an Electronic Medical Record is not merely the construction of an IT system but a continual organizational improvement process aimed at bringing the healthcare organization to a higher achievement level through people, processes and technology. The process changes with the users needs and requirements as they learn as well as technology and knowledge evolves.
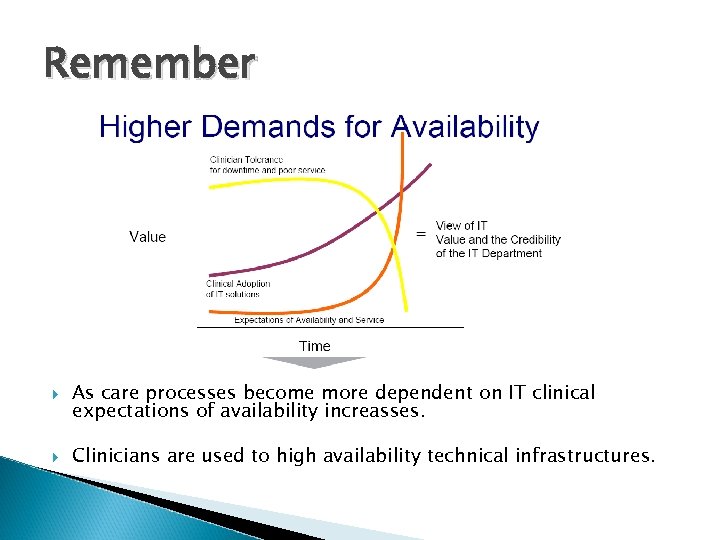
Remember As care processes become more dependent on IT clinical expectations of availability increasses. Clinicians are used to high availability technical infrastructures.

Benefits of Implementing EMRs Improve Quality Care Avoid Adverse Drug Events Improve Quality Measures Enhance Patient Safety Improve Operational Efficiencies and Reallocate Staff Increase Reimbursements Decreased cost
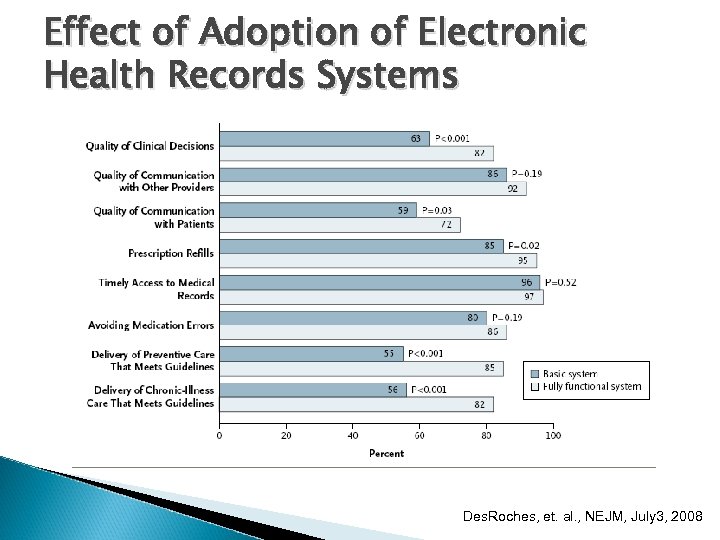
Effect of Adoption of Electronic Health Records Systems Des. Roches, et. al. , NEJM, July 3, 2008

Improve Quality of Care Simultaneous 24/7 health record availability ◦ Emergency/On Call physician Improved chronic disease management ◦ Prompts doctors and nurses whenever health maintenance services are past due. ◦ Prompts doctors and nurses to perform chronic disease management services and identifies when parameters are not met. Improved continuity of care and preventative care among different providers Record is legible and timely Record is more consistent across different providers

Avoid Adverse Drug Events

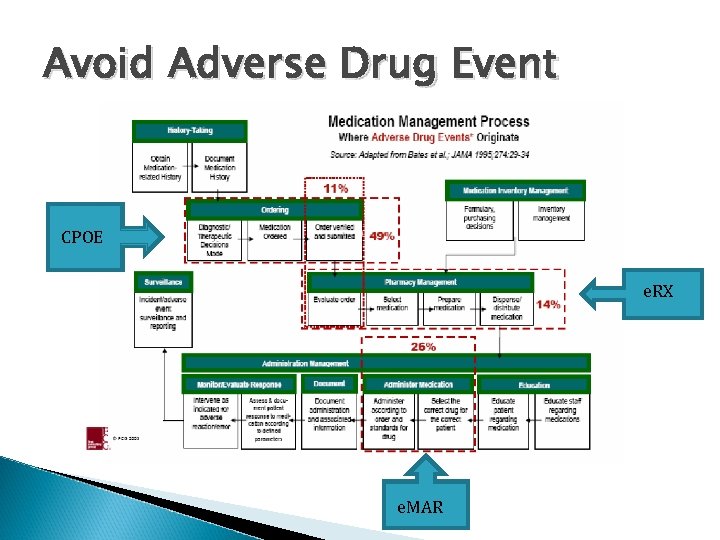
Avoid Adverse Drug Event CPOE e. RX e. MAR
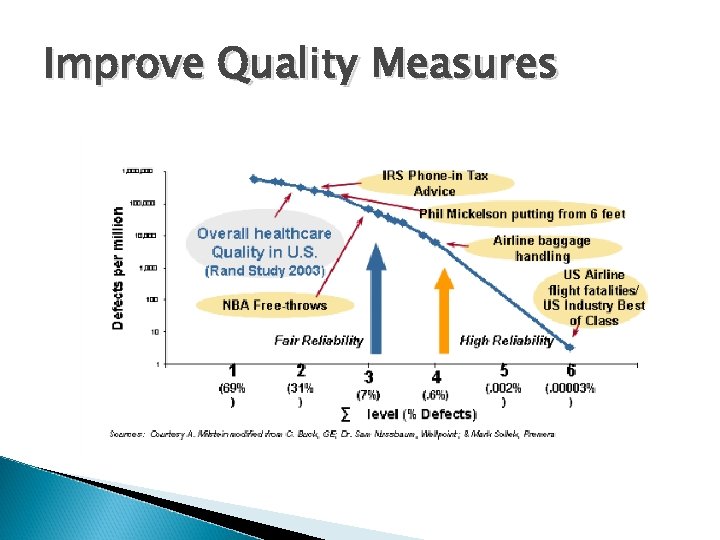
Improve Quality Measures

Improve Quality Measures Standardize and integrate data capture for quality measurement into the normal documentation of care within the ambulatory EMR. Reporting abilities of flow and process allow better understanding of process and procedures. ◦ Data can flow into PI modules/software with import and export Implementation of an automated system for data extraction including valid, reliable reports that provide actionable insight for the measurement, analysis and improvement of care.

Enhance Patient Safety Increased safety in prescribing due to drug interactions and allergy alerts. Ease of accessing patient prescription information in case of drug recall. More efficient phone triage due to immediate access to patient records. Consultant Reports and legible and timely.

Improve Operational Efficiencies and Reallocate Staff Increased staff job satisfaction ◦ Reduced staff stress related to failed searches for paper records ◦ Improved communication among staff Staff to physician ratio decreased below national ratio average ◦ FTE decrease 1 – 2. 5 per physician. Physical Plan reduction ◦ Convert filing area to 3 exam rooms.
Increase Reimbursements Decreased cost Better E/M documentation enhances provider confidence to code and bill appropriately for services rendered ◦ It is common to down-code for fear of the audit or denials. ◦ Service Notes are more defensible from a billing perspective Transcription cost saved Discounts from malpractice insurer ◦ The malpractice insurer believes EMR greatly reduces potential of drug errors / misunderstood notes Improve charge capture ◦ Reduction in delays in billing activities ◦ Reduction in payer denials

Wang et al. (2003) Showed the More Advanced the EMR the Greater the Net Benefits (per provider) Basic EHR On line chart with: - Clinical note documentation - Results viewing ($18, 200) Net Cost Intermediate EHR Advanced EHR Basic plus: - Electronic prescribing with: - Adverse drug prevention capability - Alternative drug suggestion Intermediate plus: - Lab order entry with testing guidance - Radiology order entry with test guidance - Electronic Charge Capture $44, 600 Net Benefit $86, 400 Net Benefit
A EMR/EHR system can take you from this

to this…

Valley View Case Study Goshen, NY 520 Beds 4 Buildings 15 Units – Sub-Acute Rehabilitation – Long Term – Dementia/Alzheimer's – Palliative Care Over 600 Employees

Valley View’s Business Issues Lost Revenue Medicare billing inefficiencies Inaccurate data capture Increasing Costs Formulary non-compliance was resulting in escalating drug costs Inefficient Work Flow Renewal process lengthy and error prone Difficult to manage off-hour admissions Cumbersome communication within facility Nursing staff mired in paperwork Resident Safety Concerns Difficult to manage quality with paper and retrospective MDS data Incomplete or ambiguous orders DUR alerts missed or late Less time on resident care due to inefficiencies Clinician and staff frustration high In danger of losing reference lab Inefficiencies resulted in an underlying concern for resident safety

Valley View’s Return on Investment Business Process Automated Medication order renewal process Formulary updates, communication and control Facility communication and order data entry (telephone, ADT, etc. ) Pharmacy communication and order data entry Residentification, alert and room/bed assignment * Through attrition Direct Financial Benefit 5 FTE Staff Reduction* Medication savings Renewal efficiencies Efficiencies in formulary training Consultation forms Medicare billing improvement Lab billing improvement Additional Efficiencies 92% reduction in adverse drug events (from avg. of $ 250, 000 2. 81 per month to. 23 per $ 262, 000 month) $ 120, 000 $ 8, 000 9% additional time for over 200 employees (700 hours per week) to focus on $ 20, 000 direct resident care $ 15, 000 $ 10, 000 Reporting (resident safety, quality indicators, DUR, shift productivity, census) Compliance with State, Federal and accreditation audits, surveys and ad hoc requests

Thank You! Questions ?
8abc83b2039cd68869c9e6c3c822b3c7.ppt