31594817e09d6dbf32eaa58295c56acd.ppt
- Количество слайдов: 26
 Economics of Scaling up New HIV Prevention Interventions: Male Circumcision Example Nalinee Sangrujee and Albena Godlove Constella Futures, Gayle Martin, World Bank International AIDS Economics Network 22 February 2008
Economics of Scaling up New HIV Prevention Interventions: Male Circumcision Example Nalinee Sangrujee and Albena Godlove Constella Futures, Gayle Martin, World Bank International AIDS Economics Network 22 February 2008
 Outline • • Background Estimating resource needs Resource allocation Implementation challenges – Supply side – Demand side • Monitoring and evaluation • Areas for further economics research
Outline • • Background Estimating resource needs Resource allocation Implementation challenges – Supply side – Demand side • Monitoring and evaluation • Areas for further economics research
 Epidemiology behind the intervention • Weiss et al. (2000): Meta-analysis – 48% (95% CI: 32%-60%) • Auvert et al. (2005): Randomized clinical trial – 60% (95% CI: 32%– 76%) • Siegfried et al. (2006): Cochrane Review/Meta-analysis – “We found insufficient evidence to support an interventional effect of male circumcision on HIV acquisition in heterosexual men. ” – Pointed to protective effect among high risk males – Pointed to limitations of observational studies and the need for RCT evidence • NIH funded trials (2006): Randomized clinical trials – 51% (Uganda) – 60% (Kenya)
Epidemiology behind the intervention • Weiss et al. (2000): Meta-analysis – 48% (95% CI: 32%-60%) • Auvert et al. (2005): Randomized clinical trial – 60% (95% CI: 32%– 76%) • Siegfried et al. (2006): Cochrane Review/Meta-analysis – “We found insufficient evidence to support an interventional effect of male circumcision on HIV acquisition in heterosexual men. ” – Pointed to protective effect among high risk males – Pointed to limitations of observational studies and the need for RCT evidence • NIH funded trials (2006): Randomized clinical trials – 51% (Uganda) – 60% (Kenya)
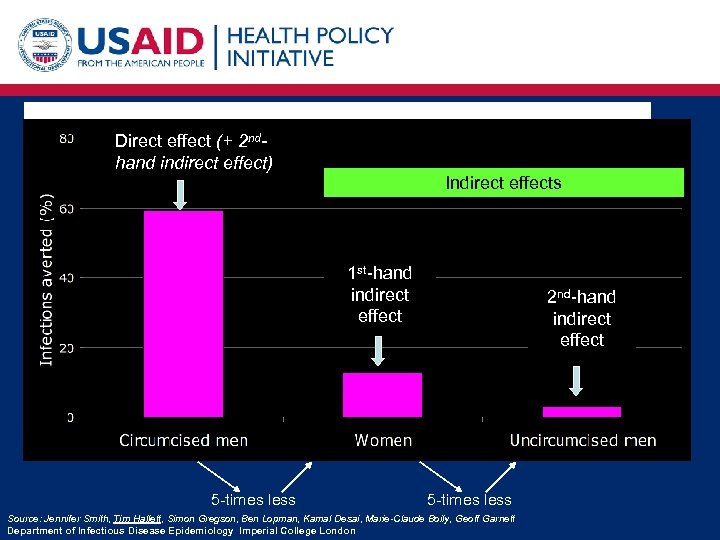 Male circumcision intervention could have two benefits: Direct effect (+ 2 nd. DIRECT - accrues to men that receive circumcision hand indirect effect) INDIRECT – accrues to everyone in the population (to different degrees) Indirect effects HIV infections averted over the first 20 years of the intervention 1 st-hand indirect effect 5 -times less 2 nd-hand indirect effect 5 -times less Source: Jennifer Smith, Tim Hallett, Simon Gregson, Ben Lopman, Kamal Desai, Marie-Claude Boily, Geoff Garnett Department of Infectious Disease Epidemiology Imperial College London
Male circumcision intervention could have two benefits: Direct effect (+ 2 nd. DIRECT - accrues to men that receive circumcision hand indirect effect) INDIRECT – accrues to everyone in the population (to different degrees) Indirect effects HIV infections averted over the first 20 years of the intervention 1 st-hand indirect effect 5 -times less 2 nd-hand indirect effect 5 -times less Source: Jennifer Smith, Tim Hallett, Simon Gregson, Ben Lopman, Kamal Desai, Marie-Claude Boily, Geoff Garnett Department of Infectious Disease Epidemiology Imperial College London
 Estimating Resource Needs Cost Analysis Resource Needs
Estimating Resource Needs Cost Analysis Resource Needs
 Cost of Male Circumcision and Implications for Cost. Effectiveness of Circumcision as an HIV Intervention* • 3 countries: Lesotho, Swaziland, Zambia • Cost data collected on how circumcision currently implemented – Adult circumcision – Public provider perspective • Considered also services not currently part of circumcision (counseling with or without testing, training, communications) * In alphabetical order: Lori Bollinger, Steven Forsythe, Bafana Khumalo, Gayle Martin; Rejoice Nkambule, Tanvi Pandit-Rajani, Dean Peacock, Tshehlo Relebohile, John Stover conducted in 2007
Cost of Male Circumcision and Implications for Cost. Effectiveness of Circumcision as an HIV Intervention* • 3 countries: Lesotho, Swaziland, Zambia • Cost data collected on how circumcision currently implemented – Adult circumcision – Public provider perspective • Considered also services not currently part of circumcision (counseling with or without testing, training, communications) * In alphabetical order: Lori Bollinger, Steven Forsythe, Bafana Khumalo, Gayle Martin; Rejoice Nkambule, Tanvi Pandit-Rajani, Dean Peacock, Tshehlo Relebohile, John Stover conducted in 2007
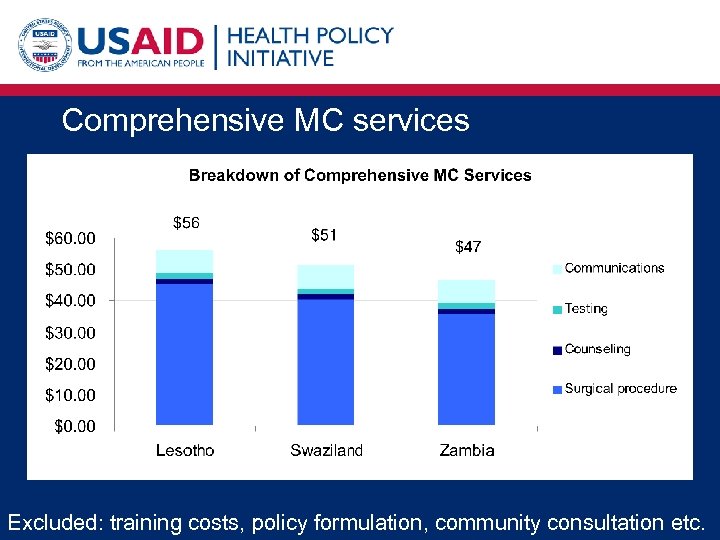 Comprehensive MC services Excluded: training costs, policy formulation, community consultation etc.
Comprehensive MC services Excluded: training costs, policy formulation, community consultation etc.
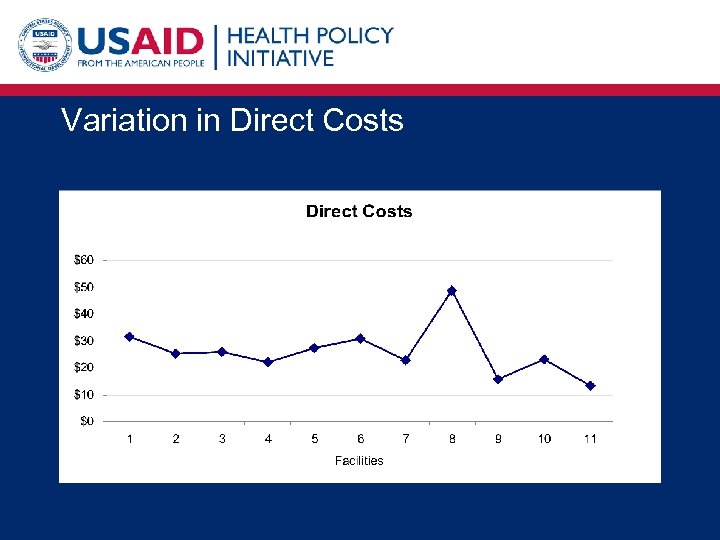 Variation in Direct Costs
Variation in Direct Costs
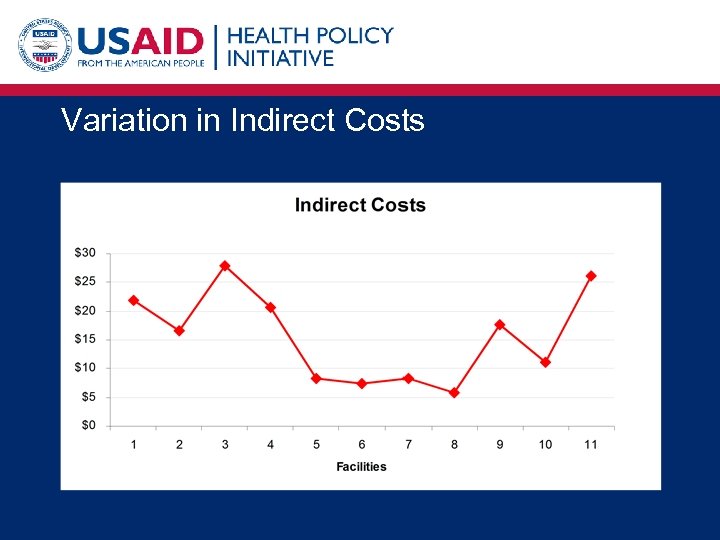 Variation in Indirect Costs
Variation in Indirect Costs
 How do the costs compare to existing cost estimates? • Other cost studies: – – – Orange Farm (South Africa) Rakai (Uganda) Kisumu (Kenya) Mankayane (Swaziland) Mozambique (Fieno) $55 $69 $25 $82 $45 • Problems: – These costs are not directly comparable because it is unclear what is included in the studies
How do the costs compare to existing cost estimates? • Other cost studies: – – – Orange Farm (South Africa) Rakai (Uganda) Kisumu (Kenya) Mankayane (Swaziland) Mozambique (Fieno) $55 $69 $25 $82 $45 • Problems: – These costs are not directly comparable because it is unclear what is included in the studies
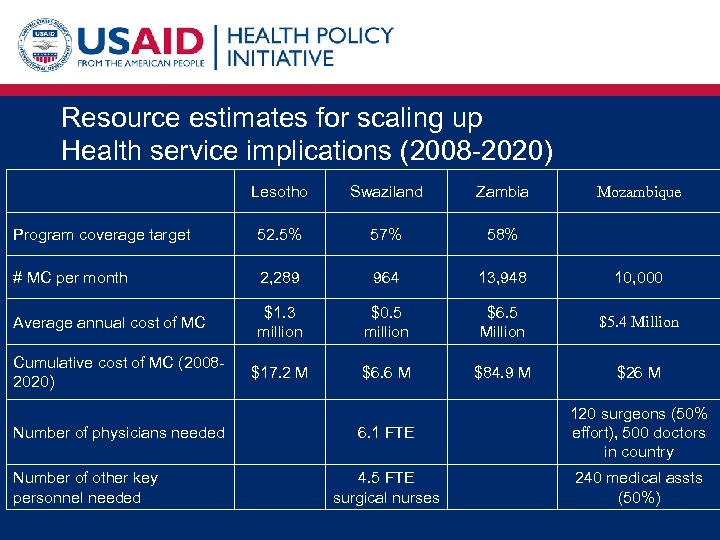 Resource estimates for scaling up Health service implications (2008 -2020) Lesotho Swaziland Zambia Program coverage target 52. 5% 57% 58% # MC per month 2, 289 964 13, 948 10, 000 Average annual cost of MC $1. 3 million $0. 5 million $6. 5 Million $5. 4 Million $17. 2 M $6. 6 M $84. 9 M $26 M Cumulative cost of MC (20082020) Number of physicians needed Number of other key personnel needed Mozambique 6. 1 FTE 120 surgeons (50% effort), 500 doctors in country 4. 5 FTE surgical nurses 240 medical assts (50%)
Resource estimates for scaling up Health service implications (2008 -2020) Lesotho Swaziland Zambia Program coverage target 52. 5% 57% 58% # MC per month 2, 289 964 13, 948 10, 000 Average annual cost of MC $1. 3 million $0. 5 million $6. 5 Million $5. 4 Million $17. 2 M $6. 6 M $84. 9 M $26 M Cumulative cost of MC (20082020) Number of physicians needed Number of other key personnel needed Mozambique 6. 1 FTE 120 surgeons (50% effort), 500 doctors in country 4. 5 FTE surgical nurses 240 medical assts (50%)
 Resource needs estimates: current approach for male circumcision Catherine Hankins, Chief Scientific Adviser to UNAIDS and Associate Director, Department of Evidence, Monitoring and Policy • • Only for sub-Saharan African countries Overall target is 80% of 15 -24 year old males circumcised • Three scenarios being considered: 1. Historical growth in coverage of VCT and PMTCT applied to prevention and care & treatment 2. Universal access by 2015 3. Universal access to prevention by 2010 and to care and treatment by 2015. • Target for each country: reduce the gap between current male circumcision prevalence and the 80% target by half by 2015 (scenario 2) or by half by 2010 (scenario 3) With these assumptions, resources needed for male circumcision: – $60 -160 million in 2010 (implying about 950, 000 - 2. 5 million circumcisions in the year 2010) – $50 -60 million in 2015 •
Resource needs estimates: current approach for male circumcision Catherine Hankins, Chief Scientific Adviser to UNAIDS and Associate Director, Department of Evidence, Monitoring and Policy • • Only for sub-Saharan African countries Overall target is 80% of 15 -24 year old males circumcised • Three scenarios being considered: 1. Historical growth in coverage of VCT and PMTCT applied to prevention and care & treatment 2. Universal access by 2015 3. Universal access to prevention by 2010 and to care and treatment by 2015. • Target for each country: reduce the gap between current male circumcision prevalence and the 80% target by half by 2015 (scenario 2) or by half by 2010 (scenario 3) With these assumptions, resources needed for male circumcision: – $60 -160 million in 2010 (implying about 950, 000 - 2. 5 million circumcisions in the year 2010) – $50 -60 million in 2015 •
 Key Methodological Assumptions for Cost Analysis • Differences defining the “MC service package” • Establishment of targets – Age groups – By HIV status • Number of trained providers needed to reach targets • Estimation of complication rates and their cost in a non clinical setting • Non-service delivery costs: – Provider training, policy formulation, operationalization and enforcement; quality control; advocacy, community outreach
Key Methodological Assumptions for Cost Analysis • Differences defining the “MC service package” • Establishment of targets – Age groups – By HIV status • Number of trained providers needed to reach targets • Estimation of complication rates and their cost in a non clinical setting • Non-service delivery costs: – Provider training, policy formulation, operationalization and enforcement; quality control; advocacy, community outreach
 Resource Allocation Global perspective National perspective
Resource Allocation Global perspective National perspective
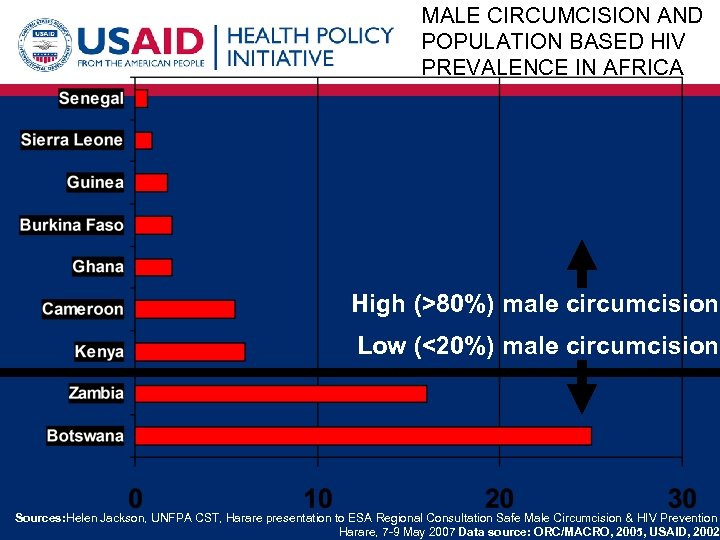 MALE CIRCUMCISION AND POPULATION BASED HIV PREVALENCE IN AFRICA High (>80%) male circumcision Low (<20%) male circumcision Sources: Helen Jackson, UNFPA CST, Harare presentation to ESA Regional Consultation Safe Male Circumcision & HIV Prevention Harare, 7 -9 May 2007 Data source: ORC/MACRO, 2005, USAID, 2002
MALE CIRCUMCISION AND POPULATION BASED HIV PREVALENCE IN AFRICA High (>80%) male circumcision Low (<20%) male circumcision Sources: Helen Jackson, UNFPA CST, Harare presentation to ESA Regional Consultation Safe Male Circumcision & HIV Prevention Harare, 7 -9 May 2007 Data source: ORC/MACRO, 2005, USAID, 2002
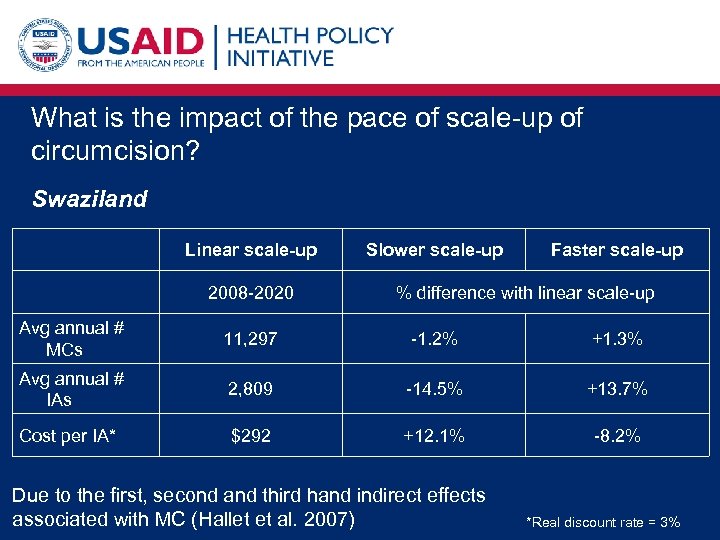 What is the impact of the pace of scale-up of circumcision? Swaziland Linear scale-up 2008 -2020 Slower scale-up Faster scale-up % difference with linear scale-up Avg annual # MCs 11, 297 -1. 2% +1. 3% Avg annual # IAs 2, 809 -14. 5% +13. 7% Cost per IA* $292 +12. 1% -8. 2% Due to the first, second and third hand indirect effects associated with MC (Hallet et al. 2007) *Real discount rate = 3%
What is the impact of the pace of scale-up of circumcision? Swaziland Linear scale-up 2008 -2020 Slower scale-up Faster scale-up % difference with linear scale-up Avg annual # MCs 11, 297 -1. 2% +1. 3% Avg annual # IAs 2, 809 -14. 5% +13. 7% Cost per IA* $292 +12. 1% -8. 2% Due to the first, second and third hand indirect effects associated with MC (Hallet et al. 2007) *Real discount rate = 3%
 How cost-effective is MC relative to other prevention interventions? • Cost per infection averted: – Lesotho: – Swaziland: – Zambia: $292 $180 $315 • Cost per HIV infection averted for selected HIV interventions (from cost-effectiveness literature)*: – – – condom distribution: VCT: PMTCT: STI treatment: school-based education: Alban, Kahn et al, 2006 $10–$2, 188 $393–$482 $20–$2, 198 $271–$514 $7, 288–$13, 326
How cost-effective is MC relative to other prevention interventions? • Cost per infection averted: – Lesotho: – Swaziland: – Zambia: $292 $180 $315 • Cost per HIV infection averted for selected HIV interventions (from cost-effectiveness literature)*: – – – condom distribution: VCT: PMTCT: STI treatment: school-based education: Alban, Kahn et al, 2006 $10–$2, 188 $393–$482 $20–$2, 198 $271–$514 $7, 288–$13, 326
 Financing
Financing
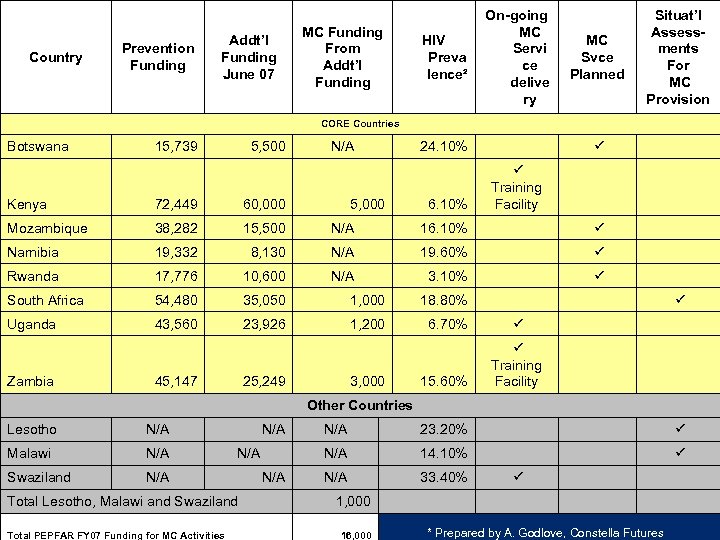 Country Prevention Funding Addt’l Funding June 07 MC Funding From Addt’l Funding HIV Preva lence² On-going MC Servi ce delive ry 24. 10% MC Svce Planned Situat’l Assessments For MC Provision ü CORE Countries Botswana 15, 739 5, 500 N/A Kenya 72, 449 60, 000 Mozambique 38, 282 15, 500 N/A 16. 10% ü Namibia 19, 332 8, 130 N/A 19. 60% ü Rwanda 17, 776 10, 600 N/A 3. 10% ü South Africa 54, 480 35, 050 1, 000 18. 80% Uganda 43, 560 23, 926 1, 200 6. 70% 15. 60% Zambia 45, 147 5, 000 ü Training Facility 25, 249 3, 000 6. 10% ü ü ü Training Facility Other Countries Lesotho N/A Malawi N/A Swaziland N/A Total Lesotho, Malawi and Swaziland Total PEPFAR FY 07 Funding for MC Activities N/A 23. 20% ü N/A N/A 14. 10% ü N/A 33. 40% 1, 000 16, 000 ü * Prepared by A. Godlove, Constella Futures
Country Prevention Funding Addt’l Funding June 07 MC Funding From Addt’l Funding HIV Preva lence² On-going MC Servi ce delive ry 24. 10% MC Svce Planned Situat’l Assessments For MC Provision ü CORE Countries Botswana 15, 739 5, 500 N/A Kenya 72, 449 60, 000 Mozambique 38, 282 15, 500 N/A 16. 10% ü Namibia 19, 332 8, 130 N/A 19. 60% ü Rwanda 17, 776 10, 600 N/A 3. 10% ü South Africa 54, 480 35, 050 1, 000 18. 80% Uganda 43, 560 23, 926 1, 200 6. 70% 15. 60% Zambia 45, 147 5, 000 ü Training Facility 25, 249 3, 000 6. 10% ü ü ü Training Facility Other Countries Lesotho N/A Malawi N/A Swaziland N/A Total Lesotho, Malawi and Swaziland Total PEPFAR FY 07 Funding for MC Activities N/A 23. 20% ü N/A N/A 14. 10% ü N/A 33. 40% 1, 000 16, 000 ü * Prepared by A. Godlove, Constella Futures
 Implementation Challenges Supply side Demand side
Implementation Challenges Supply side Demand side
 Supply side: • Who will carry out safe MC? – Traditional practitioners of ritual circumcision – Private sector • HR shortages in Government facilities already significantly affects service delivery before MC demands came into effect. • How does this procedure become part of the overall package of HIV Interventions – – • MC is an elective surgery Circumcision Sundays Coordinated with other health services What screening procedures are needed if only circumcise HIV+ men What Quality Assurance measures – Rapid scale up without proper training could increase complication rates – What services need to be scaled up to address complications?
Supply side: • Who will carry out safe MC? – Traditional practitioners of ritual circumcision – Private sector • HR shortages in Government facilities already significantly affects service delivery before MC demands came into effect. • How does this procedure become part of the overall package of HIV Interventions – – • MC is an elective surgery Circumcision Sundays Coordinated with other health services What screening procedures are needed if only circumcise HIV+ men What Quality Assurance measures – Rapid scale up without proper training could increase complication rates – What services need to be scaled up to address complications?
 Demand side • Biggest barriers to MC are cost, and concerns about safety (risk of infection or mutilation), and pain • What are the out-of-pocket costs to the individual? Subsidies? • What additional barriers (cultural, economic) to demand access? • Shifting demand from ritual circumcision.
Demand side • Biggest barriers to MC are cost, and concerns about safety (risk of infection or mutilation), and pain • What are the out-of-pocket costs to the individual? Subsidies? • What additional barriers (cultural, economic) to demand access? • Shifting demand from ritual circumcision.
 Monitoring and Evaluation • Financial – Funding flows – Provider payments • Programmatic – Exposure to other programs – Number of HIV+ and non HIV+ men circumcised • Behavioral – Risk compensation – Attribution of program effect • Epidemiological – new infections – STIs – complication rates
Monitoring and Evaluation • Financial – Funding flows – Provider payments • Programmatic – Exposure to other programs – Number of HIV+ and non HIV+ men circumcised • Behavioral – Risk compensation – Attribution of program effect • Epidemiological – new infections – STIs – complication rates
 Conclusion • Cost analysis suggests that: – Level in the health service where MC is provided matters – Pace of scaling up matters • Cost effectiveness analysis suggests: – MC can be a cost effective intervention – Benefits accrue over time • Scaling up MC is not without challenges … – Carefully crafted communication messages needed – Indirect costs should not be underestimated – Health service, financial and human resource implications are significant but not insurmountable – Innovative ways have to be found to involve all providers (including the private sector and NGOs)
Conclusion • Cost analysis suggests that: – Level in the health service where MC is provided matters – Pace of scaling up matters • Cost effectiveness analysis suggests: – MC can be a cost effective intervention – Benefits accrue over time • Scaling up MC is not without challenges … – Carefully crafted communication messages needed – Indirect costs should not be underestimated – Health service, financial and human resource implications are significant but not insurmountable – Innovative ways have to be found to involve all providers (including the private sector and NGOs)
 Areas for further research • Neonatal MC (more complicated and the trainings costs higher) • Age differential in risk of infection and circumcision (young men compared to older men given their wealth and sexual behavior) • Rate of complications outside of a trial setting • Estimating additional benefits and costs (complications) • Examining other implementation strategies – combined with other (male) RH services, PMTCT, safe delivery – Analysis of synergies with other HIV prevention interventions • Is there a impact on gender imbalance? Effect of male circumcision on women’s services and delivery. Task shifting – this further complicates the problem. • Legal obstacles: the context in which non physicians (nurses) cannot conduct procedures • Protective effect for other groups: women, MSM, uncircumcised men
Areas for further research • Neonatal MC (more complicated and the trainings costs higher) • Age differential in risk of infection and circumcision (young men compared to older men given their wealth and sexual behavior) • Rate of complications outside of a trial setting • Estimating additional benefits and costs (complications) • Examining other implementation strategies – combined with other (male) RH services, PMTCT, safe delivery – Analysis of synergies with other HIV prevention interventions • Is there a impact on gender imbalance? Effect of male circumcision on women’s services and delivery. Task shifting – this further complicates the problem. • Legal obstacles: the context in which non physicians (nurses) cannot conduct procedures • Protective effect for other groups: women, MSM, uncircumcised men
 Thank You!
Thank You!


