58e9c305253bb6e3b78f2c60bbeccb24.ppt
- Количество слайдов: 66
 e. Health Technologies for Lithuanian Health Care Prof. Arūnas Lukoševičius Biomedical Engineering Institute Kaunas University of Technology, , e. Baltic Forum Riga 2006 04 06
e. Health Technologies for Lithuanian Health Care Prof. Arūnas Lukoševičius Biomedical Engineering Institute Kaunas University of Technology, , e. Baltic Forum Riga 2006 04 06
 Biomedical Engineering Institute Kaunas University of Technology Activities: • Telemedicine support centre • e. Health architecture and implementation • Clinical decision support systems • Signal and processing methods and software • Ultrasonic medical diagnostics • Prototyping of hardware, sensors and transducers • Wireless technologies Studentų street. 50, Kaunas, LT-51368, tel. 407118, ISDN: 407114 -407119 http: //www. bmii. ktu. lt
Biomedical Engineering Institute Kaunas University of Technology Activities: • Telemedicine support centre • e. Health architecture and implementation • Clinical decision support systems • Signal and processing methods and software • Ultrasonic medical diagnostics • Prototyping of hardware, sensors and transducers • Wireless technologies Studentų street. 50, Kaunas, LT-51368, tel. 407118, ISDN: 407114 -407119 http: //www. bmii. ktu. lt
 Topics • Why e. Health? Lithuanian statistics and arguments • Principles of proposed architecture: patient centered • Principles of implementation: standard based • Electronic Health Record • Data mining and clinical decision support • Building bricks: international projects • Efficiency of e. Health: user benefits and functionalities • Cross - boarder cooperation and networking
Topics • Why e. Health? Lithuanian statistics and arguments • Principles of proposed architecture: patient centered • Principles of implementation: standard based • Electronic Health Record • Data mining and clinical decision support • Building bricks: international projects • Efficiency of e. Health: user benefits and functionalities • Cross - boarder cooperation and networking
 Why e. Health? Lithuanian statistics and arguments
Why e. Health? Lithuanian statistics and arguments
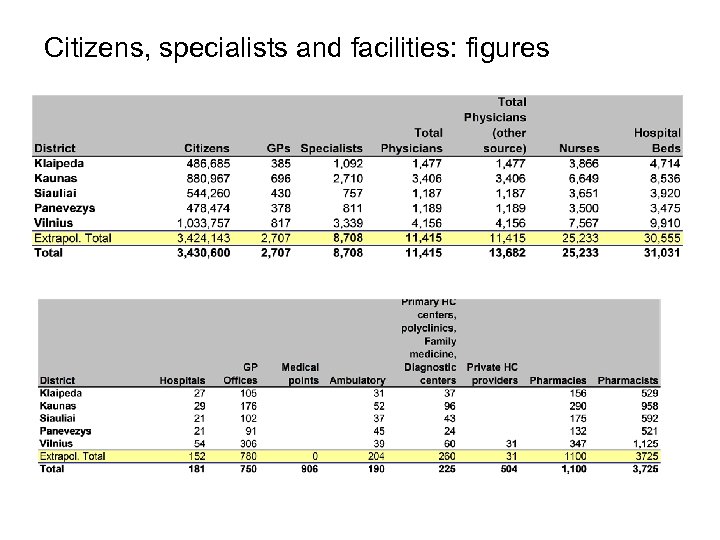 Citizens, specialists and facilities: figures
Citizens, specialists and facilities: figures
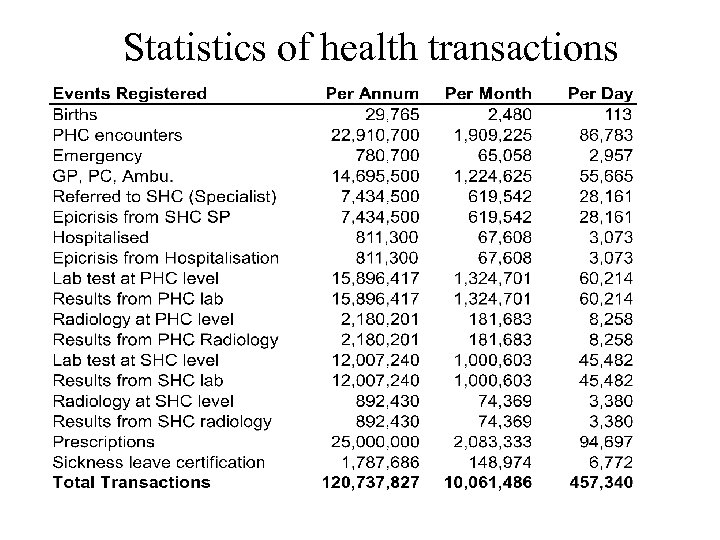 Statistics of health transactions
Statistics of health transactions
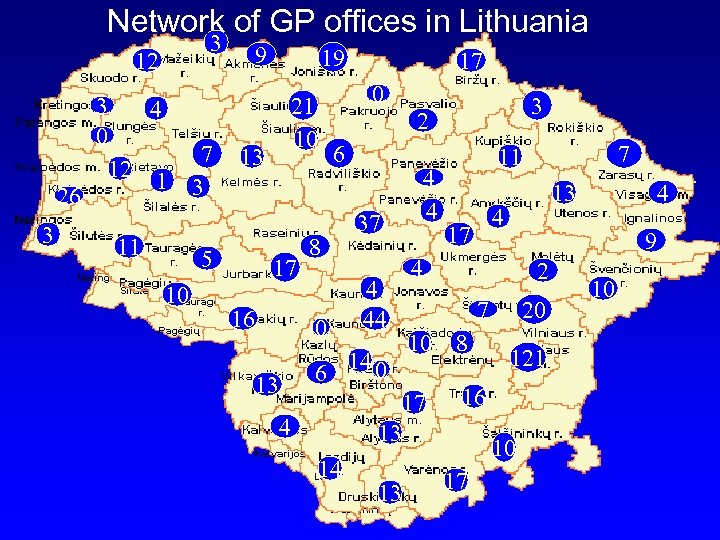 Network of GP offices in Lithuania 3 12 26 3 3 4 0 12 1 11 7 3 9 17 16 3 2 6 8 0 13 17 0 21 10 13 5 10 19 4 4 37 17 13 20 121 16 13 10 17 4 9 2 10 8 17 14 4 7 6 14 0 4 13 4 4 44 7 11 10
Network of GP offices in Lithuania 3 12 26 3 3 4 0 12 1 11 7 3 9 17 16 3 2 6 8 0 13 17 0 21 10 13 5 10 19 4 4 37 17 13 20 121 16 13 10 17 4 9 2 10 8 17 14 4 7 6 14 0 4 13 4 4 44 7 11 10
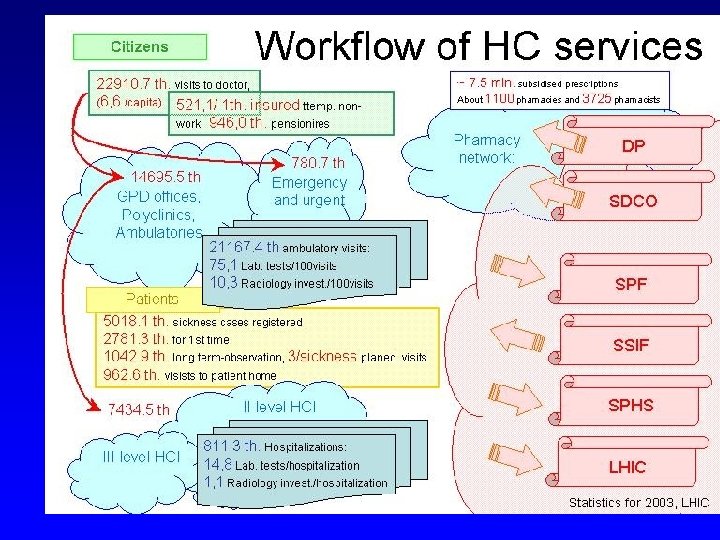
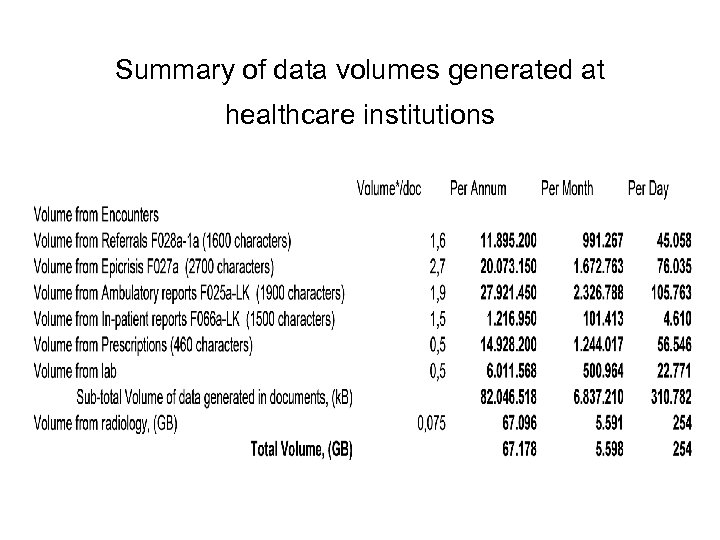 Summary of data volumes generated at healthcare institutions
Summary of data volumes generated at healthcare institutions
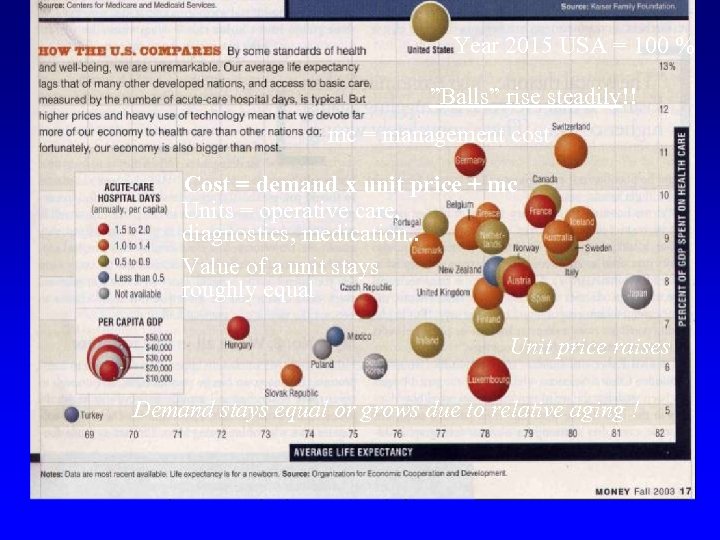 Year 2015 USA = 100 % ”Balls” rise steadily!! mc = management cost Cost = demand x unit price + mc Units = operative care, diagnostics, medication. . Value of a unit stays roughly equal Unit price raises Demand stays equal or grows due to relative aging !
Year 2015 USA = 100 % ”Balls” rise steadily!! mc = management cost Cost = demand x unit price + mc Units = operative care, diagnostics, medication. . Value of a unit stays roughly equal Unit price raises Demand stays equal or grows due to relative aging !
 ICT assistance is necessary Proposed e. Health system
ICT assistance is necessary Proposed e. Health system
 • The project submitted in 2004 by Mo. H of Lithuania • Development of the Lithuanian Electronic Health Services Infostructure (EHSI): Implementation of an official health and healthcare information sharing and exchange system, to support lifelong continuity-of-care for healthcare professionals and citizens. (expert team lead by Dr. Dimitris Kalogeropoulos) First part - WB financed pilot national e. Health project 2005 -6
• The project submitted in 2004 by Mo. H of Lithuania • Development of the Lithuanian Electronic Health Services Infostructure (EHSI): Implementation of an official health and healthcare information sharing and exchange system, to support lifelong continuity-of-care for healthcare professionals and citizens. (expert team lead by Dr. Dimitris Kalogeropoulos) First part - WB financed pilot national e. Health project 2005 -6
 Principles of proposed architecture: patient centered
Principles of proposed architecture: patient centered
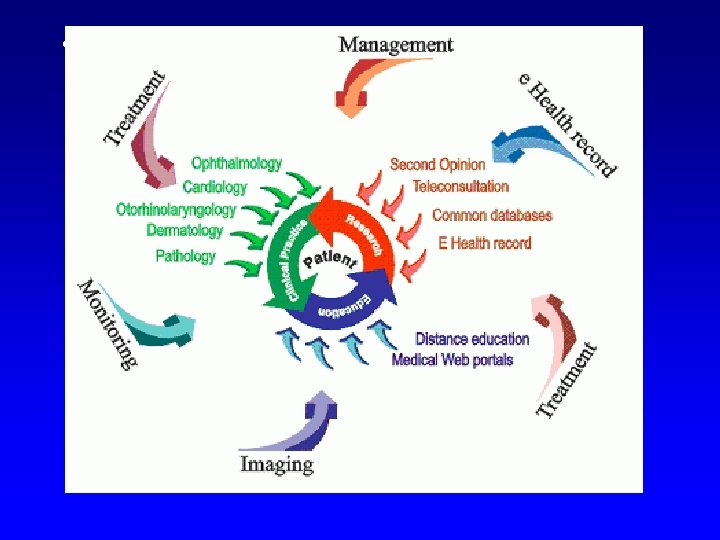
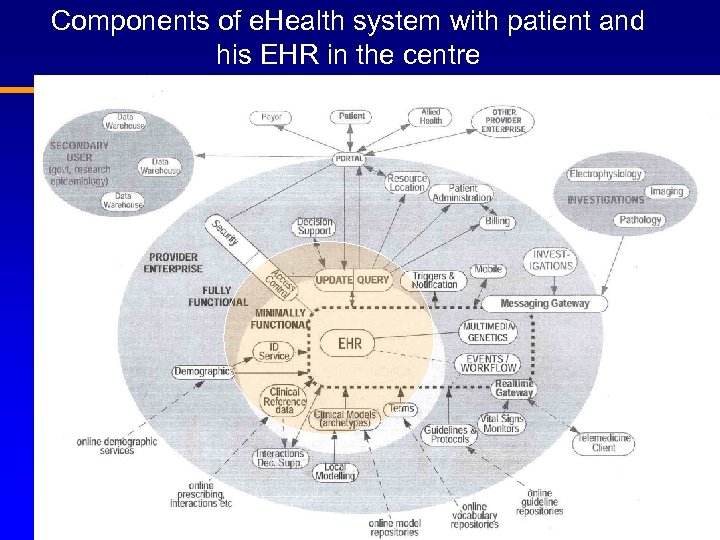 Components of e. Health system with patient and his EHR in the centre
Components of e. Health system with patient and his EHR in the centre
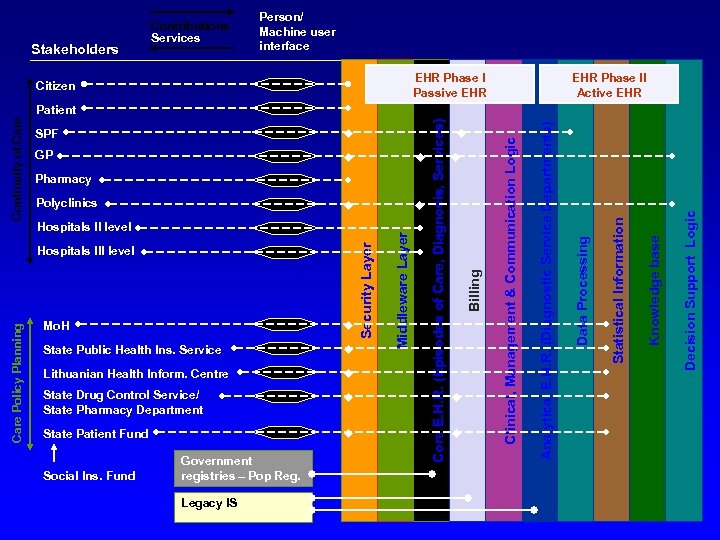 Stakeholders Contributions Services Person/ Machine user interface EHR Phase I Passive EHR Citizen EHR Phase II Active EHR State Public Health Ins. Service Lithuanian Health Inform. Centre State Drug Control Service/ State Pharmacy Department State Patient Fund Social Ins. Fund Government registries – Pop Reg. Legacy IS Decision Support Logic Mo. H Knowledge base Care Policy Planning Hospitals III level Middleware Layer Hospitals II level Statistical Information Polyclinics Data Processing Pharmacy Analytical E. H. R. (Diagnostic Service Departments) Clinical, Management & Communication Logic Billing GP E H R based billing Core E. H. R. (Episodes of Care, Diagnosis, Services) SPF Security Layer Continuity of Care Patient
Stakeholders Contributions Services Person/ Machine user interface EHR Phase I Passive EHR Citizen EHR Phase II Active EHR State Public Health Ins. Service Lithuanian Health Inform. Centre State Drug Control Service/ State Pharmacy Department State Patient Fund Social Ins. Fund Government registries – Pop Reg. Legacy IS Decision Support Logic Mo. H Knowledge base Care Policy Planning Hospitals III level Middleware Layer Hospitals II level Statistical Information Polyclinics Data Processing Pharmacy Analytical E. H. R. (Diagnostic Service Departments) Clinical, Management & Communication Logic Billing GP E H R based billing Core E. H. R. (Episodes of Care, Diagnosis, Services) SPF Security Layer Continuity of Care Patient
 Electronic Health Record
Electronic Health Record
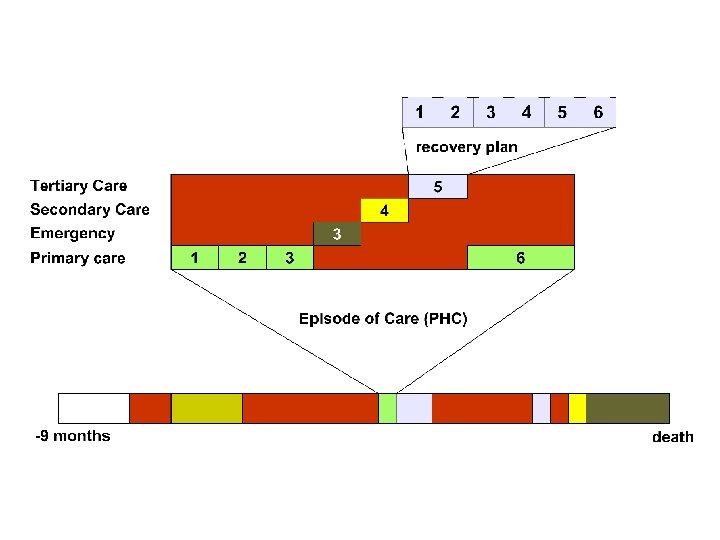 Continuous episode oriented health record
Continuous episode oriented health record
 Principles of implementation: standard based
Principles of implementation: standard based
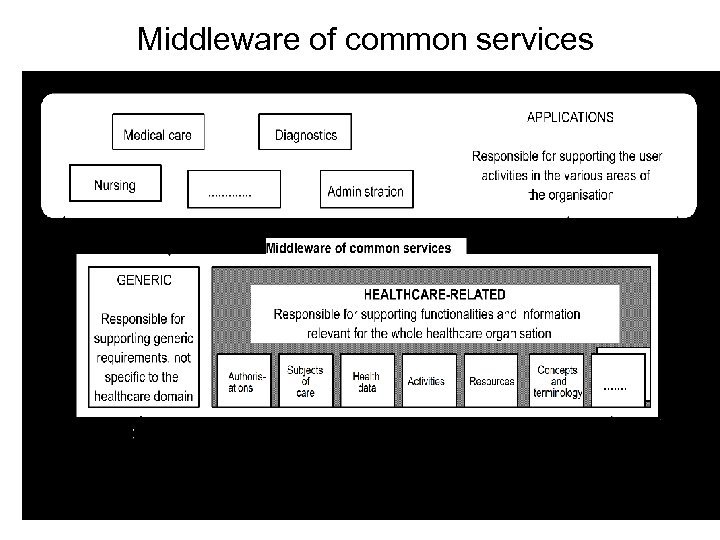 Middleware of common services
Middleware of common services
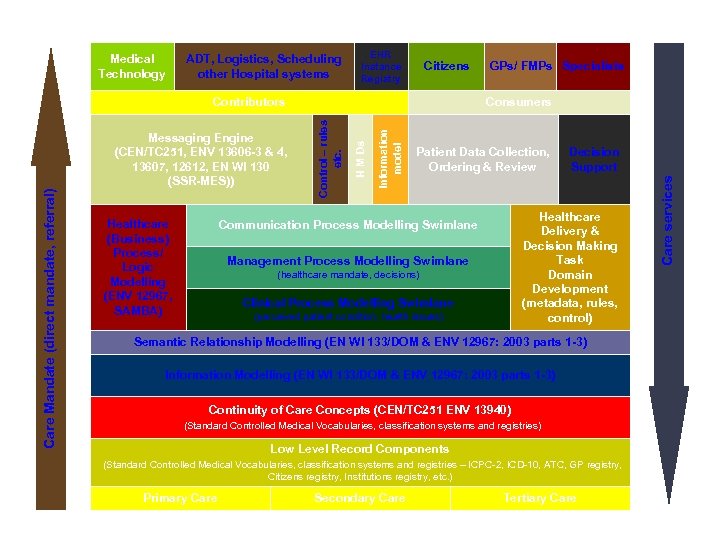 ADT, Logistics, Scheduling other Hospital systems EHR Instance Registry Citizens Healthcare (Business) Process/ Logic Modelling (ENV 12967, SAMBA) H M Ds Information model Care Mandate (direct mandate, referral) Messaging Engine (CEN/TC 251, ENV 13606 -3 & 4, 13607, 12612, EN WI 130 (SSR-MES)) Consumers Control – rules etc. Contributors GPs/ FMPs Specialists Patient Data Collection, Ordering & Review Decision Support Healthcare Delivery & Decision Making Task Domain Development (metadata, rules, control) Communication Process Modelling Swimlane Management Process Modelling Swimlane (healthcare mandate, decisions) Clinical Process Modelling Swimlane (perceived patient condition, health issues) Semantic Relationship Modelling (EN WI 133/DOM & ENV 12967: 2003 parts 1 -3) Information Modelling (EN WI 133/DOM & ENV 12967: 2003 parts 1 -3) Continuity of Care Concepts (CEN/TC 251 ENV 13940) (Standard Controlled Medical Vocabularies, classification systems and registries) Low Level Record Components (Standard Controlled Medical Vocabularies, classification systems and registries – ICPC-2, ICD-10, ATC, GP registry, Citizens registry, Institutions registry, etc. ) Primary Care Secondary Care Tertiary Care services Medical Technology
ADT, Logistics, Scheduling other Hospital systems EHR Instance Registry Citizens Healthcare (Business) Process/ Logic Modelling (ENV 12967, SAMBA) H M Ds Information model Care Mandate (direct mandate, referral) Messaging Engine (CEN/TC 251, ENV 13606 -3 & 4, 13607, 12612, EN WI 130 (SSR-MES)) Consumers Control – rules etc. Contributors GPs/ FMPs Specialists Patient Data Collection, Ordering & Review Decision Support Healthcare Delivery & Decision Making Task Domain Development (metadata, rules, control) Communication Process Modelling Swimlane Management Process Modelling Swimlane (healthcare mandate, decisions) Clinical Process Modelling Swimlane (perceived patient condition, health issues) Semantic Relationship Modelling (EN WI 133/DOM & ENV 12967: 2003 parts 1 -3) Information Modelling (EN WI 133/DOM & ENV 12967: 2003 parts 1 -3) Continuity of Care Concepts (CEN/TC 251 ENV 13940) (Standard Controlled Medical Vocabularies, classification systems and registries) Low Level Record Components (Standard Controlled Medical Vocabularies, classification systems and registries – ICPC-2, ICD-10, ATC, GP registry, Citizens registry, Institutions registry, etc. ) Primary Care Secondary Care Tertiary Care services Medical Technology
 Data mining and clinical decision support • Rationale • Technologies
Data mining and clinical decision support • Rationale • Technologies
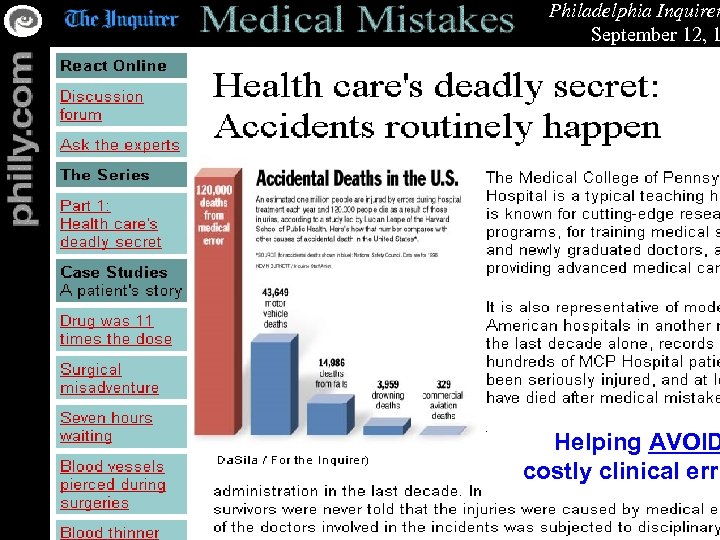 Philadelphia Inquirer September 12, 1 Helping AVOID costly clinical erro
Philadelphia Inquirer September 12, 1 Helping AVOID costly clinical erro
 World population
World population
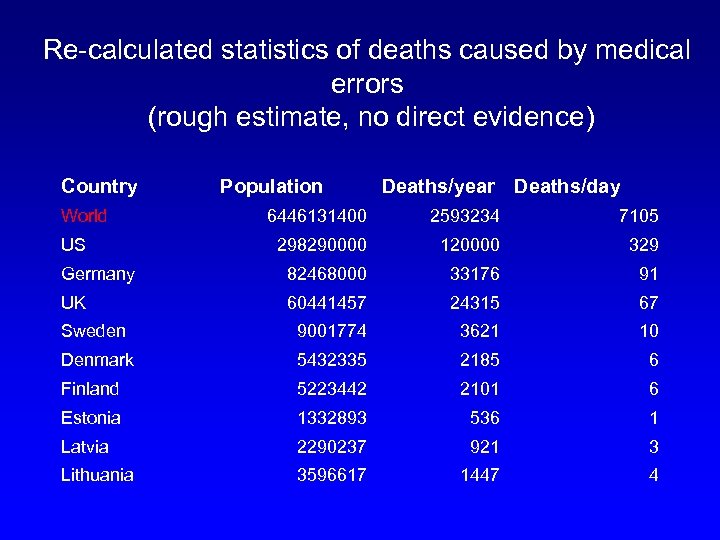 Re-calculated statistics of deaths caused by medical errors (rough estimate, no direct evidence) Country World Population Deaths/year Deaths/day 6446131400 2593234 7105 298290000 120000 329 Germany 82468000 33176 91 UK 60441457 24315 67 Sweden 9001774 3621 10 Denmark 5432335 2185 6 Finland 5223442 2101 6 Estonia 1332893 536 1 Latvia 2290237 921 3 Lithuania 3596617 1447 4 US
Re-calculated statistics of deaths caused by medical errors (rough estimate, no direct evidence) Country World Population Deaths/year Deaths/day 6446131400 2593234 7105 298290000 120000 329 Germany 82468000 33176 91 UK 60441457 24315 67 Sweden 9001774 3621 10 Denmark 5432335 2185 6 Finland 5223442 2101 6 Estonia 1332893 536 1 Latvia 2290237 921 3 Lithuania 3596617 1447 4 US
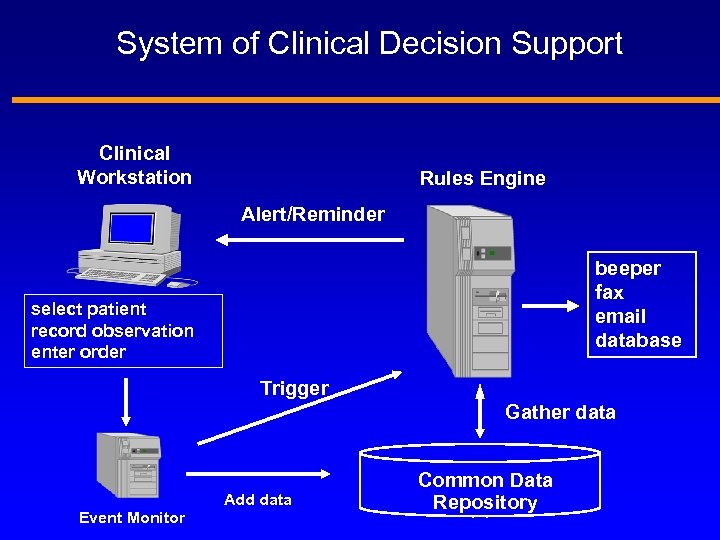 System of Clinical Decision Support Clinical Workstation Rules Engine Alert/Reminder beeper fax email database select patient record observation enter order Trigger Gather data Add data Event Monitor Common Data Repository
System of Clinical Decision Support Clinical Workstation Rules Engine Alert/Reminder beeper fax email database select patient record observation enter order Trigger Gather data Add data Event Monitor Common Data Repository
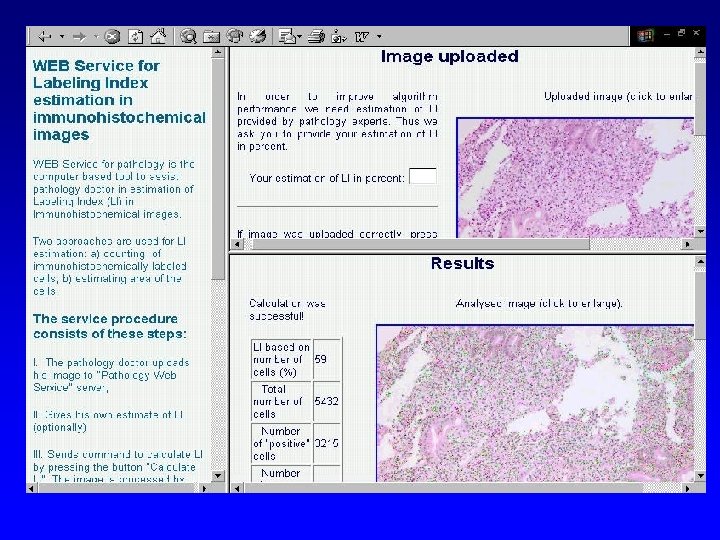
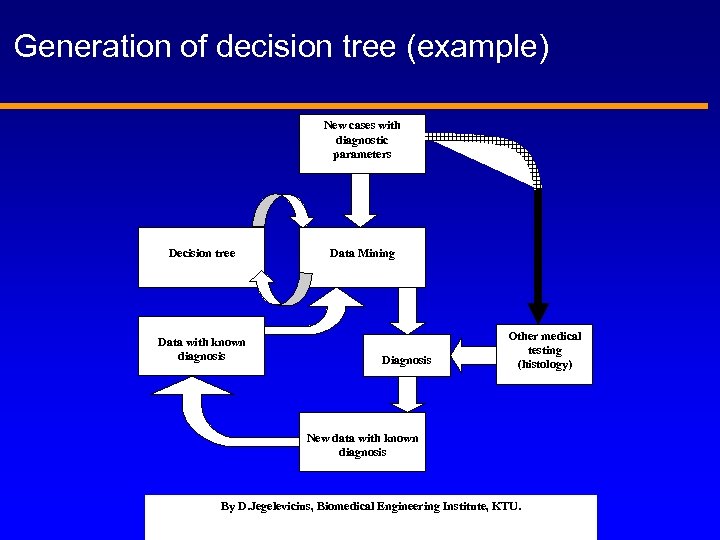 Generation of decision tree (example) New cases with diagnostic parameters Decision tree Data with known diagnosis Data Mining Diagnosis Other medical testing (histology) New data with known diagnosis By D. Jegelevicius, Biomedical Engineering Institute, KTU.
Generation of decision tree (example) New cases with diagnostic parameters Decision tree Data with known diagnosis Data Mining Diagnosis Other medical testing (histology) New data with known diagnosis By D. Jegelevicius, Biomedical Engineering Institute, KTU.
 Example of decision tree automatically generated to support decision about differential diagnostics of intraocular tumours
Example of decision tree automatically generated to support decision about differential diagnostics of intraocular tumours
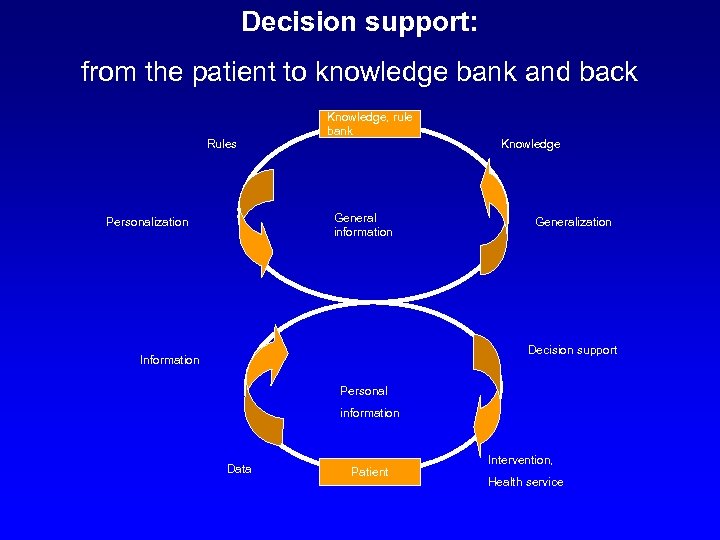 Decision support: from the patient to knowledge bank and back Rules Knowledge, rule bank General information Personalization Knowledge Generalization Decision support Information Personal information Data Patient Intervention, Health service
Decision support: from the patient to knowledge bank and back Rules Knowledge, rule bank General information Personalization Knowledge Generalization Decision support Information Personal information Data Patient Intervention, Health service
 Expert foresights Gartner Group: Predicts through 2002, >75% of healthcare organizations will implement rule-based technologies Beginning in 2000, computer-based patient record systems and data repositories that do not support an Arden Syntax-based, user-definable rulesprocessing system will lose market share. Vendors using Arden: Siemens Mc. Kesson. HBOC Eclipsys IBM
Expert foresights Gartner Group: Predicts through 2002, >75% of healthcare organizations will implement rule-based technologies Beginning in 2000, computer-based patient record systems and data repositories that do not support an Arden Syntax-based, user-definable rulesprocessing system will lose market share. Vendors using Arden: Siemens Mc. Kesson. HBOC Eclipsys IBM
 Building bricks: international projects
Building bricks: international projects
 Kaunas e. Health cluster • Medical Component - Kaunas Medical University, Biomedical Research Institute, University hospital (largest in Lithuania, 2000 beds) other Kaunas hospitals and polyclinics, Society of GP of Lithuania • Technological Component – Kaunas University of Technology, (KTU), ( the greatest technical university in Baltic countries, with 11 faculties, it’s Biomedical Engineering Institute having Telemedicine Support Center, (TSC), Biomedical Engineering Master Program, other Kaunas universities (5 in total); • Industry component – SMS companies Kardiosignalas[7], Elinta[8], Elintos prietaisai[9], Elsis[10] and other.
Kaunas e. Health cluster • Medical Component - Kaunas Medical University, Biomedical Research Institute, University hospital (largest in Lithuania, 2000 beds) other Kaunas hospitals and polyclinics, Society of GP of Lithuania • Technological Component – Kaunas University of Technology, (KTU), ( the greatest technical university in Baltic countries, with 11 faculties, it’s Biomedical Engineering Institute having Telemedicine Support Center, (TSC), Biomedical Engineering Master Program, other Kaunas universities (5 in total); • Industry component – SMS companies Kardiosignalas[7], Elinta[8], Elintos prietaisai[9], Elsis[10] and other.
 EU FP 5 PROJECT TELEMEDICARE • • "The Telemedi. Care system permits advanced home care with maintained medical safety. The result is increased quality of life without increased costs. " - Bo Lundell, Acting Division Manager, Astrid Lindgren Children's Hospital. New Market Possibilities Advances on modern information and communication technology have together with miniaturization of health diagnostic equipment given birth to a new revolution within health care. Body sensor technology facilitating mobile, multi-modal and wireless functionality will be key components to future intelligent and user friendly medical monitors. The integration of such sensors with new wireless network technology has given life to new possibilities for cost-efficient patient treatment.
EU FP 5 PROJECT TELEMEDICARE • • "The Telemedi. Care system permits advanced home care with maintained medical safety. The result is increased quality of life without increased costs. " - Bo Lundell, Acting Division Manager, Astrid Lindgren Children's Hospital. New Market Possibilities Advances on modern information and communication technology have together with miniaturization of health diagnostic equipment given birth to a new revolution within health care. Body sensor technology facilitating mobile, multi-modal and wireless functionality will be key components to future intelligent and user friendly medical monitors. The integration of such sensors with new wireless network technology has given life to new possibilities for cost-efficient patient treatment.
 •
•

 Efficiency of e. Health: user benefits and functionalities
Efficiency of e. Health: user benefits and functionalities
 Users (beneficiaries) of e. Health srevices • • Patients Citizens General Practitioners (GP) Primary Care Centers Specialists Polyclinics Hospitals Health Information Centre (HIS) under the State Public Health Service (SPHS) • State Patient Fund (SPF) • Dept. of Pharmacy, State Drug Control Office (SDCO) • Software industry
Users (beneficiaries) of e. Health srevices • • Patients Citizens General Practitioners (GP) Primary Care Centers Specialists Polyclinics Hospitals Health Information Centre (HIS) under the State Public Health Service (SPHS) • State Patient Fund (SPF) • Dept. of Pharmacy, State Drug Control Office (SDCO) • Software industry
 Benefits and rationale categories • Benefits and rationale are already discussed evident enough to be structurised and even numbered !!! • HL 7 EHR System functional Model and Standard Release 1. 0. , August, 2003, Why rationale categories, v. 1. 2
Benefits and rationale categories • Benefits and rationale are already discussed evident enough to be structurised and even numbered !!! • HL 7 EHR System functional Model and Standard Release 1. 0. , August, 2003, Why rationale categories, v. 1. 2
 1 To serve: ( HL 7 EHR System functional Model and Standard Release 1. 0. , August, 2003, Why rationale categories, v. 1. 2) 1. 1 Patient-centered/oriented care 1. 2 Longitudinal, interdisciplinary healthcare delivery (per episode, disease, problem) 1. 3 Point of service, point of care: immediate, real-time 1. 4 Multiple care settings: acute inpatient, emergent (including trauma and mobile care, ambulance), ambulatory, long term, home, school, occupational, military 1. 5 Personal health record: per patient 1. 6 Provider business record: per organization, per business unit 1. 7 Practitioner service record: per caregiver 1. 8 Primary and secondary record uses
1 To serve: ( HL 7 EHR System functional Model and Standard Release 1. 0. , August, 2003, Why rationale categories, v. 1. 2) 1. 1 Patient-centered/oriented care 1. 2 Longitudinal, interdisciplinary healthcare delivery (per episode, disease, problem) 1. 3 Point of service, point of care: immediate, real-time 1. 4 Multiple care settings: acute inpatient, emergent (including trauma and mobile care, ambulance), ambulatory, long term, home, school, occupational, military 1. 5 Personal health record: per patient 1. 6 Provider business record: per organization, per business unit 1. 7 Practitioner service record: per caregiver 1. 8 Primary and secondary record uses
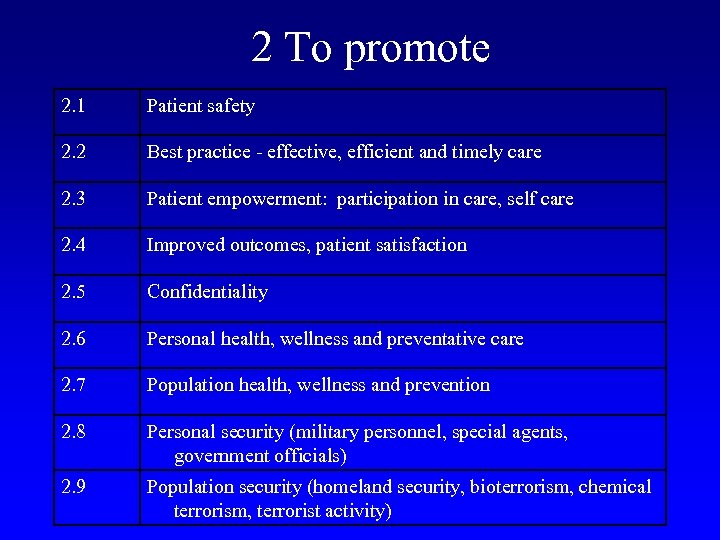 2 To promote 2. 1 Patient safety 2. 2 Best practice - effective, efficient and timely care 2. 3 Patient empowerment: participation in care, self care 2. 4 Improved outcomes, patient satisfaction 2. 5 Confidentiality 2. 6 Personal health, wellness and preventative care 2. 7 Population health, wellness and prevention 2. 8 Personal security (military personnel, special agents, government officials) 2. 9 Population security (homeland security, bioterrorism, chemical terrorism, terrorist activity)
2 To promote 2. 1 Patient safety 2. 2 Best practice - effective, efficient and timely care 2. 3 Patient empowerment: participation in care, self care 2. 4 Improved outcomes, patient satisfaction 2. 5 Confidentiality 2. 6 Personal health, wellness and preventative care 2. 7 Population health, wellness and prevention 2. 8 Personal security (military personnel, special agents, government officials) 2. 9 Population security (homeland security, bioterrorism, chemical terrorism, terrorist activity)
 3 To ensure and ascribe 3. 1 Accountability: of organizations, of business units, of persons 3. 2 Continuous record availability and access 3. 3 Integrity of clinical decision making/Effectiveness of clinical decisions 3. 4 Integrity of the health record 3. 5 Integrity of the health(care) delivery process 3. 6 Health record privacy, PHI protection
3 To ensure and ascribe 3. 1 Accountability: of organizations, of business units, of persons 3. 2 Continuous record availability and access 3. 3 Integrity of clinical decision making/Effectiveness of clinical decisions 3. 4 Integrity of the health record 3. 5 Integrity of the health(care) delivery process 3. 6 Health record privacy, PHI protection
 4 To facilitate and enable 4. 1 Health(care) delivery: immediate, real-time point of service, point of care 4. 2 Efficient work flow and operations performance - streamline the way people work 4. 3 Communication: inter-practitioner 4. 4 Clinical decision making 4. 5 Trusted record management 4. 6 Trusted record/information flow 4. 7 Correlated business, clinical and caregiver record 4. 8/. Continuous quality improvement and monitoring, measures of quality, 9 performance and outcomes 4. 10 Payment and eligibility determination 4. 11 Effective communication between patient, family, caregiver and care team
4 To facilitate and enable 4. 1 Health(care) delivery: immediate, real-time point of service, point of care 4. 2 Efficient work flow and operations performance - streamline the way people work 4. 3 Communication: inter-practitioner 4. 4 Clinical decision making 4. 5 Trusted record management 4. 6 Trusted record/information flow 4. 7 Correlated business, clinical and caregiver record 4. 8/. Continuous quality improvement and monitoring, measures of quality, 9 performance and outcomes 4. 10 Payment and eligibility determination 4. 11 Effective communication between patient, family, caregiver and care team
 5 Based on 5. Patient safety and best practice guidance 1 5. Legal and regulatory requirements - national 2 and regional mandates 5. Accreditation and professional practice 3 standards
5 Based on 5. Patient safety and best practice guidance 1 5. Legal and regulatory requirements - national 2 and regional mandates 5. Accreditation and professional practice 3 standards
![Functionalities for nurses ( an example of function – benefit relation) ID Function E/D[1] Functionalities for nurses ( an example of function – benefit relation) ID Function E/D[1]](https://present5.com/presentation/58e9c305253bb6e3b78f2c60bbeccb24/image-51.jpg) Functionalities for nurses ( an example of function – benefit relation) ID Function E/D[1] Benefits CC 1. Clinical communication E 1. 1; 1. 2; 1. 3; 1. 8; 2. 2; 2. 6; 2. 7; 3. 2; 3. 3; 3. 4; 3. 5; 4. 1; 4. 3; 4. 4; 4. 6; 4. 7; 4. 8; 4. 11; 5. 2; 5. 3. CC 6. Support for clinical guidance E 1. 1; 1. 3; 2. 2; 2. 4; 2. 7; 3. 3; 5. 1. CC 10. Sharing of laboratory test results E 1. 1; 1. 2; 1. 3; 1. 8; 2. 2; 3. 4; 3. 5; 4. 2; 4. 3; CC 14. Support for chronic disease protocols D 1. 2; 2. 6; 2. 3; 3. 3; 4. 2. AM 3. Clinical workflow tasking, scheduling D 1. 2; 2. 2; 3. 3; 4. 2; 4. 3. AM 4. Referrals and registration for care E 1. 2; 1. 3; 2. 2; 2. 3; 2. 4; 4. 1; 4. 2; 4. 3. AM 8. Claims and encounter reports for reimbursement E 1. 6; 1. 7; 3. 1; 4. 7; 4. 10. AM 11. Report generation (EHR data extraction in accordance with analysis and reporting requirements) E 1. 6; 3. 1; 4. 2; 4. 8; 5. 2; 5. 3. CS 7. Controlled vocabulary [2] E 1. 2; 3. 4; 3. 5; 4. 3; 4. 4; 4. 6; 5. 1; 5. 2; 4. 11; CS 12. Axessibility from point of care E 1. 1; 1. 3; 2. 4; 3. 3; 3. 5; 4. 4; 5. 1. E - Essential function, to be implemented within present stage of project; D - Desirable function, to be implemented if possible or in the next stage of the project. Codification and terminology vocabularies(e. g. SNOMED), Classification of diseases ICD -10, International Classification of Primary Care (ICPC – 2 ) should be app
Functionalities for nurses ( an example of function – benefit relation) ID Function E/D[1] Benefits CC 1. Clinical communication E 1. 1; 1. 2; 1. 3; 1. 8; 2. 2; 2. 6; 2. 7; 3. 2; 3. 3; 3. 4; 3. 5; 4. 1; 4. 3; 4. 4; 4. 6; 4. 7; 4. 8; 4. 11; 5. 2; 5. 3. CC 6. Support for clinical guidance E 1. 1; 1. 3; 2. 2; 2. 4; 2. 7; 3. 3; 5. 1. CC 10. Sharing of laboratory test results E 1. 1; 1. 2; 1. 3; 1. 8; 2. 2; 3. 4; 3. 5; 4. 2; 4. 3; CC 14. Support for chronic disease protocols D 1. 2; 2. 6; 2. 3; 3. 3; 4. 2. AM 3. Clinical workflow tasking, scheduling D 1. 2; 2. 2; 3. 3; 4. 2; 4. 3. AM 4. Referrals and registration for care E 1. 2; 1. 3; 2. 2; 2. 3; 2. 4; 4. 1; 4. 2; 4. 3. AM 8. Claims and encounter reports for reimbursement E 1. 6; 1. 7; 3. 1; 4. 7; 4. 10. AM 11. Report generation (EHR data extraction in accordance with analysis and reporting requirements) E 1. 6; 3. 1; 4. 2; 4. 8; 5. 2; 5. 3. CS 7. Controlled vocabulary [2] E 1. 2; 3. 4; 3. 5; 4. 3; 4. 4; 4. 6; 5. 1; 5. 2; 4. 11; CS 12. Axessibility from point of care E 1. 1; 1. 3; 2. 4; 3. 3; 3. 5; 4. 4; 5. 1. E - Essential function, to be implemented within present stage of project; D - Desirable function, to be implemented if possible or in the next stage of the project. Codification and terminology vocabularies(e. g. SNOMED), Classification of diseases ICD -10, International Classification of Primary Care (ICPC – 2 ) should be app
 Levels of services • Basic services • Integrated common services • High level professional medical services
Levels of services • Basic services • Integrated common services • High level professional medical services
 Registries Integration • Population Registry (Mo. I) • State Registry of Managers of Personal Data • Drug Registry: State Drug Control Office (+ve lists), State Pharmacy Department (prices) • Doctor & Nurse License Identification Codes (Mo. H) • Services Codes (SPF) in ICD-10 context? • Classification systems (SCMV) – ICPC-2 ?
Registries Integration • Population Registry (Mo. I) • State Registry of Managers of Personal Data • Drug Registry: State Drug Control Office (+ve lists), State Pharmacy Department (prices) • Doctor & Nurse License Identification Codes (Mo. H) • Services Codes (SPF) in ICD-10 context? • Classification systems (SCMV) – ICPC-2 ?
 Functions ensured for patient 1 • Information support of Continuity of Health Care in time and across institutions • Clinical communication • Practitioner – patient relationship • Support for preventive care and wellness • Capture and manage patient – reported or externally available patient clinical history • Create and maintain patient-specific problem, procedure and medication list • Medication and medication management
Functions ensured for patient 1 • Information support of Continuity of Health Care in time and across institutions • Clinical communication • Practitioner – patient relationship • Support for preventive care and wellness • Capture and manage patient – reported or externally available patient clinical history • Create and maintain patient-specific problem, procedure and medication list • Medication and medication management
 Functions ensured for patient 2 • • • Pharmacy communication Sharing of laboratory test results Support for chronic disease protocols Identification of citizen/patient and his status Provider/practitioner registry Report generation (EHR data extraction in accordance with analysis and reporting requirements) • Secure access to the system, secure data routing, privacy[1], authentication, role-based authorisation • Axessibility from point of care • Capture of insurance information from state register reportable and traceable over time
Functions ensured for patient 2 • • • Pharmacy communication Sharing of laboratory test results Support for chronic disease protocols Identification of citizen/patient and his status Provider/practitioner registry Report generation (EHR data extraction in accordance with analysis and reporting requirements) • Secure access to the system, secure data routing, privacy[1], authentication, role-based authorisation • Axessibility from point of care • Capture of insurance information from state register reportable and traceable over time
 Functions ensured for GP 1 • • • • • Clinical communication Practitioner – patient relationship Support for preventive care and wellness Capture and manage patient – reported or externally available patient clinical history Create and maintain patient-specific problem, procedure and medication list Support for clinical guidance Medication and medication management Support medication prescriptions Pharmacy communication Sharing of laboratory test results ECG cardiology Imaging Support for chronic disease protocols Integrate device monitoring and remote health services such as telehealth data Present clinical guidelines Identification of citizen/patient and his status Provider/practitioner registry
Functions ensured for GP 1 • • • • • Clinical communication Practitioner – patient relationship Support for preventive care and wellness Capture and manage patient – reported or externally available patient clinical history Create and maintain patient-specific problem, procedure and medication list Support for clinical guidance Medication and medication management Support medication prescriptions Pharmacy communication Sharing of laboratory test results ECG cardiology Imaging Support for chronic disease protocols Integrate device monitoring and remote health services such as telehealth data Present clinical guidelines Identification of citizen/patient and his status Provider/practitioner registry
 Functions ensured for GP 2 • • • Clinical workflow tasking, scheduling Referrals and registration for care Registration of care encounters Health service reports at the end of episode of care Integration of clinical data with administrative and financial data Claims and encounter reports for reimbursement Integrate cost management information Data availability Report generation (EHR data extraction in accordance with analysis and reporting requirements) Disease registries Data analysis and research
Functions ensured for GP 2 • • • Clinical workflow tasking, scheduling Referrals and registration for care Registration of care encounters Health service reports at the end of episode of care Integration of clinical data with administrative and financial data Claims and encounter reports for reimbursement Integrate cost management information Data availability Report generation (EHR data extraction in accordance with analysis and reporting requirements) Disease registries Data analysis and research
 Functions ensured for GP 3 • • • • Audit trial Standard based interoperablity, messaging and integration[1] Maintain and identify a single patient record for each patient. Secure access to the system, secure data routing, privacy[2], authentication, role-based authorisation Authorisation of the access to the EHR Authentication of record authorship EHR data extraction in accordance with analysis and reporting requirements Controlled vocabulary [3] Capture and creation of clinical documents and notes Responsiveness, user response time Axessibility from point of care Capture demographical information from state register, reportable and traceable over time Capture of insurance information from state register reportable and traceable over time
Functions ensured for GP 3 • • • • Audit trial Standard based interoperablity, messaging and integration[1] Maintain and identify a single patient record for each patient. Secure access to the system, secure data routing, privacy[2], authentication, role-based authorisation Authorisation of the access to the EHR Authentication of record authorship EHR data extraction in accordance with analysis and reporting requirements Controlled vocabulary [3] Capture and creation of clinical documents and notes Responsiveness, user response time Axessibility from point of care Capture demographical information from state register, reportable and traceable over time Capture of insurance information from state register reportable and traceable over time
 Cross - boarder cooperation and networking
Cross - boarder cooperation and networking
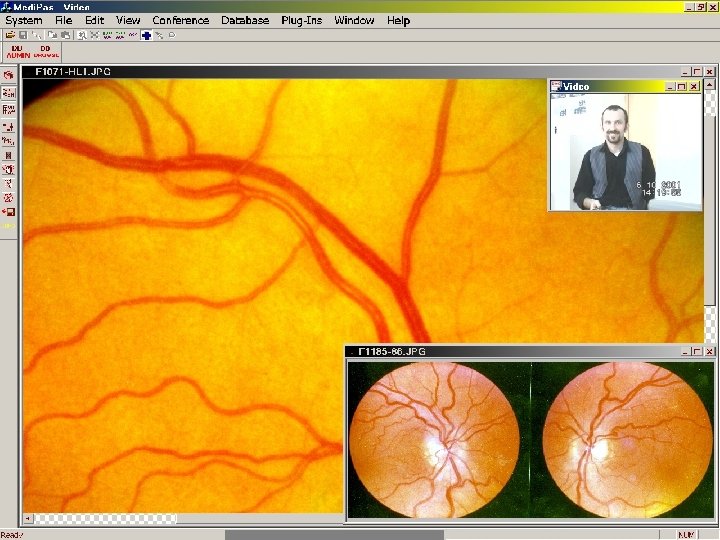
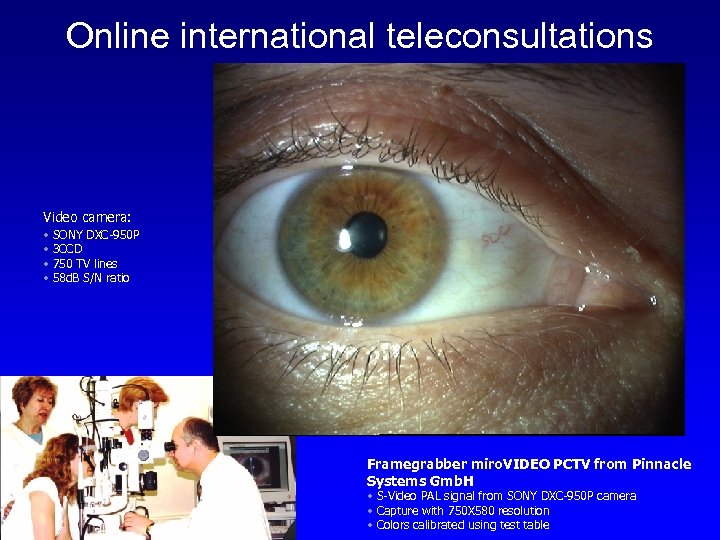 Online international teleconsultations Video camera: • SONY DXC-950 P • 3 CCD • 750 TV lines • 58 d. B S/N ratio Framegrabber miro. VIDEO PCTV from Pinnacle Systems Gmb. H • S-Video PAL signal from SONY DXC-950 P camera • Capture with 750 X 580 resolution • Colors calibrated using test table
Online international teleconsultations Video camera: • SONY DXC-950 P • 3 CCD • 750 TV lines • 58 d. B S/N ratio Framegrabber miro. VIDEO PCTV from Pinnacle Systems Gmb. H • S-Video PAL signal from SONY DXC-950 P camera • Capture with 750 X 580 resolution • Colors calibrated using test table
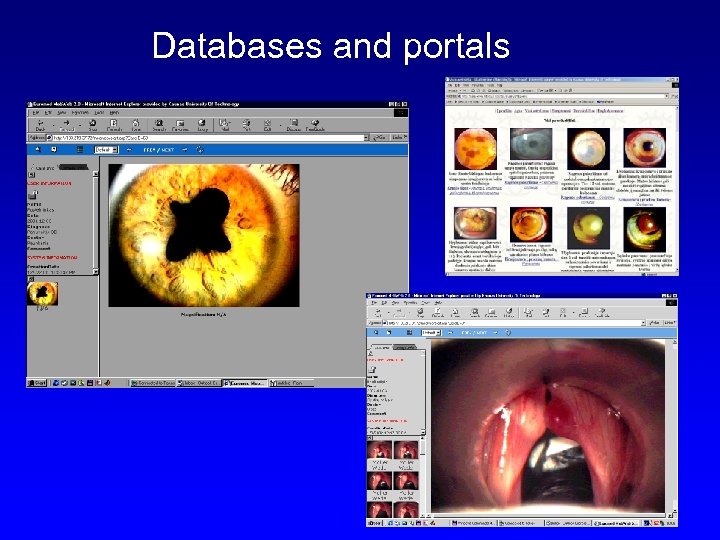 Databases and portals
Databases and portals
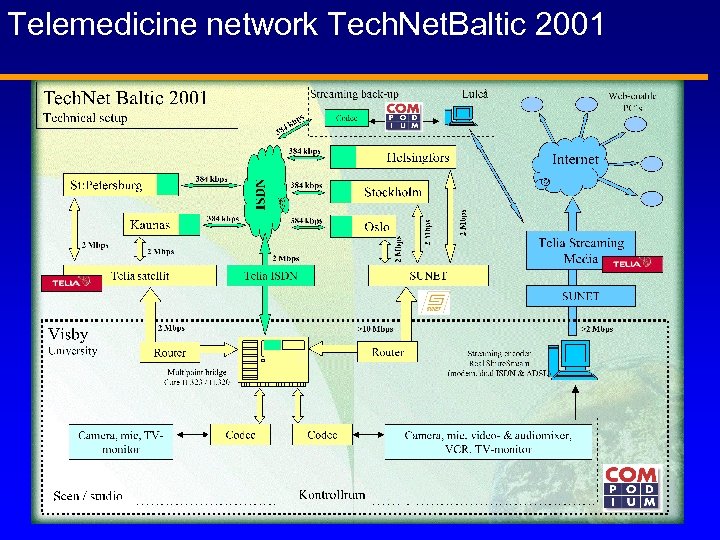 Telemedicine network Tech. Net. Baltic 2001
Telemedicine network Tech. Net. Baltic 2001
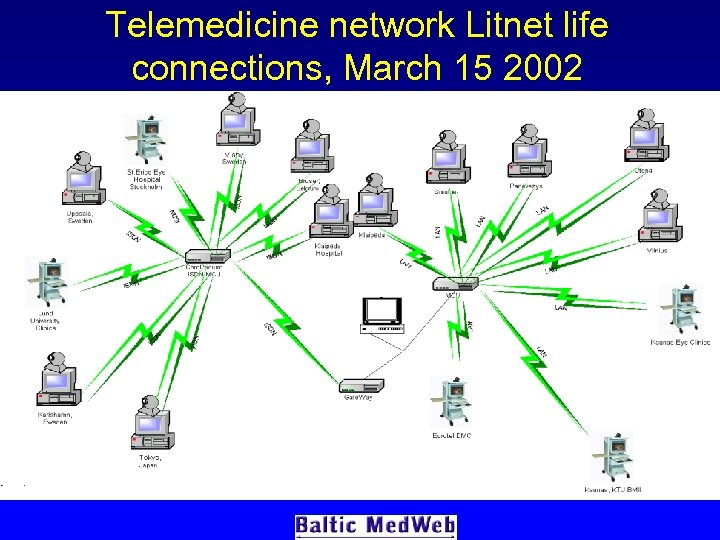 Telemedicine network Litnet life connections, March 15 2002
Telemedicine network Litnet life connections, March 15 2002
 Conclusions • • e. Health comes inevitably It’s important to start from right architecture Lithuania is taking pilot steps Data mining and clinical decision support are important goals • User benefits and funcionalities are highly evident • R&D projects and collaboration are vital
Conclusions • • e. Health comes inevitably It’s important to start from right architecture Lithuania is taking pilot steps Data mining and clinical decision support are important goals • User benefits and funcionalities are highly evident • R&D projects and collaboration are vital
 Thanks for kind attention arunas. lukosevicius@ktu. lt
Thanks for kind attention arunas. lukosevicius@ktu. lt


