ca5d6275773c324181a3cbe02db7dc00.ppt
- Количество слайдов: 43

Door-to-Balloon Time: Are there still challenges to success? Perspectives from the Front Line Regina Deible, RN

MY DRIVEWAY FEB 2010

Door to Balloon Time takes on a whole new meaning in the winter!

WHOSE DOOR IS IT ANYWAY? ? ?

Does a delay impact mortality contingent on who’s door it is? • Our door to Our balloon? • Their door (at home) to our balloon? • The referring hospital door to our balloon?

Forge ahead … the patient always comes first

Perspective…circa 1999 • Assigned topic for presentation @ TCT XI: • “The Impact of Primary Angioplasty, Stenting and Pharmacologic Agents in Acute Myocardial Infarction”. • Session concluded with timely debates about the value of “time is muscle” and the need for an efficient process to open the occluded vessel. – (This isn’t a new obsession)

No easy solution • There isn’t a single formula that will work for all cath labs…as not all cath labs are created equal; nor are all EMS systems. • Practices, referral patterns and patient population all need to be factored in for a reasonable plan. • However, there are many guidelines to build upon….

The D 2 B Alliance. TM • Guidelines launched by ACC and partnered with AHA and NHLBI to save time and save lives by reducing the door-to-balloon times in U. S. hospitals performing primary PCI. • “Sustain the Gain”

Goal: D 2 B time ≤ 90 minutes >75% of patients in participating hospitals Evidenced-based strategies: 1. ED physician activates the catheterization lab 2. One call activates the catheterization lab 3. Catheterization team ready in 20 – 30 minutes 4. Prompt data feedback 5. Senior hospital management commitment 6. Team-based approach • Optional: Activate based on pre-hospital ECG Source- ACC : D 2 B Alliance http: //www. d 2 balliance. org

RACE Primary PCI Center* 1. 24/7 PCI capability within 30 minutes 2. Single number activation (immediate) 3. Accept patients regardless of bed availability 4. Ongoing data monitoring and feedback 5. STEMI Team with strong administrative support and dedicated STEMI coordinator 6. Improve STEMI care for all hospitals in region regardlessof affiliation www. race-er. org Duke University

Successful Themes of Top Performing Hospitals for PPCI D 2 B < 90 minutes) Commitment to an explicit goal to improve D-B time Senior management support Innovative protocols Flexibility in refining standardized protocols Collaborative teams Uncompromising individual clinical leaders Data feedback to monitor progress, identify problems and successes Organization structure resilient to challenges or setbacks

Recommendation for reperfusion strategies in STEMI Source: JOINT 2010 EACTS GUIDELINES

THOUGHTS ON GUIDELINES…. . Ø are not a text book. Ø . . . are the result of the scientific analysis of the available data. Ø . . . refer only to a part of the patients - due to the usually strict inclusion / exclusion criteria of the randomized trials. Ø . . . therefore do not replace medical experience. Ø . . . are recommendations what you should do or could do - but not what you must do. Ø . . . are not legally binding. Ø but they are more and more read and applied by health care providers and patients / relatives. Ø and - if you do not follow the guidelines and complications occur, you may need to justify, why you did not follow the guidelines ! Source: Dr. Sigmund Silber TCT 10

Textbook of STEMI Interventions by Sameer Mehta, MD, FACC • Dedicated career to conquering obstacles to STEMI interventions and states there is one simple goal: “Master the Process and Procedure” • With skilled hands and a dedicated process you can relieve CP, observe ST resolution, obtain TIMI grade III flow and have brisk myocardial perfusion.
Keys to success • Focus on the culprit lesion in the infarctrelated vessel; • Achieve all 4 parameters of a successful preprofusion: – relief of chest pain; – ST-segment resolution; – Restoration of TIMI grade 3 flow; – Myocardial perfusion grade 3 Sameer Mehta, M. D.

Back to the question: Are there still challenges to success? Perspectives from the Front Line

A Bit of Perspective…circa 1970 • Dr. Kelly Brackett M. D. : [into transmitter link] 51, go. Paramedic Roy De. Soto: [over biophone] We have a male, tunnel worker, approximate age 60, was trapped under a digging machine. Patient had a cardiac history. He is now diaphoretic. Vital signs: 80 over 50; rate: 100 and irregular; respirations: 12 and shallow. Dr. Kelly Brackett M. D. : Do you have your EKG hooked up? Paramedic Roy De. Soto: Affirmitive, doctor. Dr. Kelly Brackett M. D. : Send me something so I can get a reading. [turns on EKG printer] Paramedic Roy De. Soto: This will be Lead 2. [turns on ELG transmitter] Dr. Kelly Brackett M. D. : [reads EKG strip] Multiple PVC's. [sees reading change] V-Tac. [reading changes again] He's starting to fibrillate. [to De. Soto] Defibrillate! 400 watt/seconds! Nurse Dixie Mc. Call: Kell! They're not authorized to. . . Dr. Kelly Brackett M. D. : [into link] Are you receiving? Come on, 51! You've got a dying man on your hands

So, how can we save some time?

Tracking Form makes a difference!

Top Myths about Pre-hospital 12 lead EKG’s • If you’re close to the hospital, performing a PH 12 ECG is a waste of precious time. • PH 12 ECG monitors are incapable of capturing diagnostic quality 12 leads. • It’s important for the ED staff to perform another 12 lead ECG to confirm that it’s really a STEMI. • If ST segment elevation resolves by the patient’s arrival at the hospital, then it’s not a STEMI, and the patient doesn’t need an emergent cath.

• If the hospital ignores the PH 12 ECG, then there’s no point in performing one • It’s easy to identify STEMI on the PH 12 ECG. • It’s impossible to identify STEMI in the presence of LBBB Source: http: //ems 12 lead. com/2009/04/21/top-10 -mythsabout-prehospital-12 -lead-ecgs
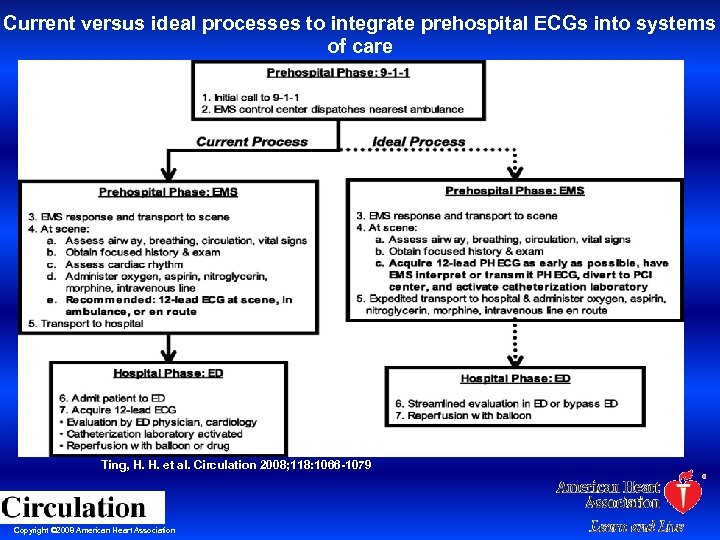
Current versus ideal processes to integrate prehospital ECGs into systems of care Ting, H. H. et al. Circulation 2008; 118: 1066 -1079 Copyright © 2008 American Heart Association

American Heart: Mission Lifeline • Prehospital electrocardiograms (ECGs) in patients with ST-elevation myocardial infarction (STEMI) are associated with a reduction in door-to-needle time of 10 minutes, and a reduction of 10 -20 minutes in door-toballoon time. • Emergency medical service (EMS) systems serving over 90% of the 200 largest cities in the United States have 12 -lead ECG equipment available in their ambulance systems. • Trained paramedics can identify STEMI with high sensitivity (71 -97%), specificity (91 -100%), and with good agreement between paramedics and emergency department physicians.

• Studies using wireless transmission of ECG have demonstrated a reduction in time to reperfusion. Systems for prehospital wireless transmission are commercially available from Medtronic , Welch Allyn , Zoll Medical and Phillips Healthcare • Appropriate training and ongoing quality assurance for EMS providers and medical control physicians is a key requirement for an effective prehospital ECGbased STEMI care system

• EMS providers or the emergency physician should activate the catheterization laboratory while the patient is en route to the hospital. • Hospitals providing percutaneous coronary intervention (PCI) need to organize reliable wireless networks and technologies, have protocols in place for advanced preparation to receive and evaluate the patient with STEMI, and streamline emergency department evaluation or bypass emergency department evaluation altogether. • Communities need to develop prehospital triage so that the EMS can bypass non-PCI hospitals when a patient is diagnosed with STEMI

http: //www. montgomerycountymd. gov/firtmpl. asp? url=/content/Fire. Rescue/ems/ 12 lead/index. asp
Technological help. . Web based integration Web based email / phone
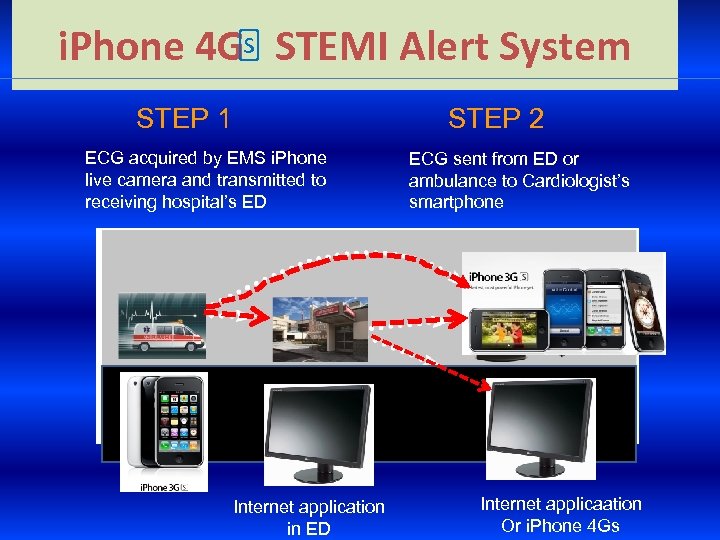
i. Phone 4 Gs STEMI Alert System STEP 1 STEP 2 ECG acquired by EMS i. Phone live camera and transmitted to receiving hospital’s ED Internet application in ED ECG sent from ED or ambulance to Cardiologist’s smartphone Internet applicaation Or i. Phone 4 Gs

All Phone Carriers are jumping on apps

LIFENET • The LIFENET® STEMI Management Solution from Physio. Control. Using the latest broadband technology, this all-digital system enables paramedics to transmit 12 -lead. ECGs from the LIFEPAK® 12 defibrillator/monitor in the field to a secure web -based system. The system then relays the information securely via the Internet to hospital care teams and cath labs, or directly to a cardiologist’s handheld device. The LIFENET STEMI • Management Solution bridges the gap between prehospital assessment and in-hospital care, ensuring critical patients receive the right treatment at the right place and at the right time.

EMS Training and ongoing quality assurance for EMS providers and medical control physicians Acquiring prehospital ECG as early as possible during initial scene evaluation Minimize scene time when STEMI is diagnosed Advanced notification of destination hospital Activation of catheterization laboratory by EMS providers or emergency physician while patient is en route to hospital PCI Hospital Organize reliable wireless networks and technologies Advanced preparation to receive and evaluate patient Activation of catheterization laboratory by emergency physician while patient is en route to hospital Streamline emergency department evaluation or bypass emergency department Prehospital triage for regional hospital networks to bypass non-PCI hospitals Research and Quality Assurance Monitor quality measures, including first medical contact to drug/balloon Monitor false-positive and false-negative rates Evaluate whether EMT-basic and EMT-intermediate can acquire prehospital ECG reliably and efficiently Promote systematic and routine feedback of performance to all stakeholders, including EMS, emergency department, and cardiology http: //circ. ahajournals. org/cgi/content/full/118/10/1066/TBL 3190402
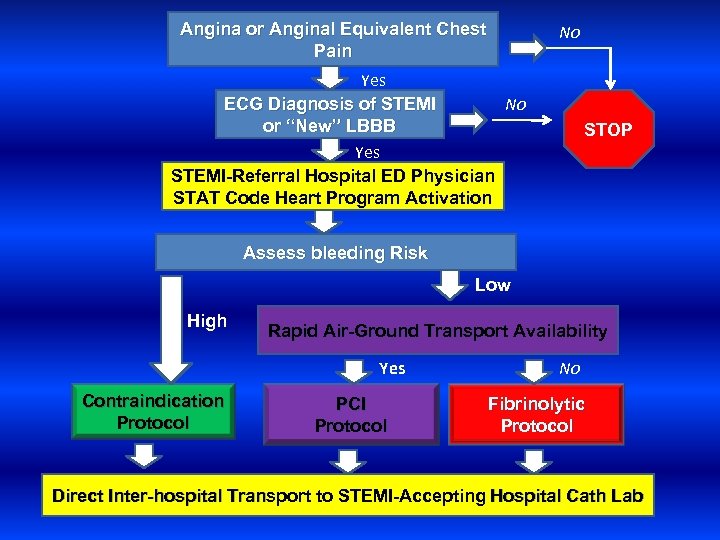
Angina or Anginal Equivalent Chest Pain No Yes ECG Diagnosis of STEMI No or “New” LBBB Yes STEMI-Referral Hospital ED Physician STAT Code Heart Program Activation STOP Assess bleeding Risk Low High Rapid Air-Ground Transport Availability Yes Contraindication Protocol PCI Protocol No Fibrinolytic Protocol Direct Inter-hospital Transport to STEMI-Accepting Hospital Cath Lab

Barriers • Only 50% of STEMI in US use EMS • Lack of integrated healthcare system • Lack of well organized inter-hospital transfer systems • Hospital bed capacity issue Source: Tim Henry, MD

Institutional help: Establishing Core Measures • Door – EKG time : < 10 minutes (direct admits) • EKG – Activation Time: < 10 minutes • Activation Time – Cath lab: < 45 minutes • Door to Cath lab: < 60 minutes • Cath lab to Perfusion: < 30 minutes • Door to Perfusion: < 90 minutes

Ways to streamline process v. Empower EMT’s for pre-hospital activation. v“One call does all” team activation v. Bypass ER…go directly to cath lab v. Program Pyxis for STEMI patient v. Have call teams either on site or ready within 30 minutes v. Maximize your resources (Use in-house resource team for after hours)

Emergency Department (Not part of medical record ) S. T. E. M. I. Treatment Worksheet – Handover Report Criteria: Patient presenting with symptoms consistent with and confirmed on EKG for ST elevation M. I. A. Initial Nursing Intervention EKG Done ≤ 10 min Shown to ED Attending ______(name) Patient placed on monitor/alarms on Pulse Oximetry and Vitals q 15 min Oxygen 2 -4 L NC or alternative O 2 source STAT portable CXR (diagnosis CP) 2 Large Bore IV’s (at least 1 AC line) STEMI Labs drawn Labs sent (cbc, compmet, cardiac enzymes, PT/INR PTT, magnesium, lipids, Type and Screen, dig level when applicable) B. Initial Medication ASA 81 mg x 4 (chew and swallow) (HOLD if allergic and or has taken with in 1 hour PTA) Plavix 300 mg PO x 1 NTG 0. 4 SL x 1 now (hold for SBP<100) Nitro drip titrate to CP free and or SBP>120 Lopressor 5 mg IV x 1 if vitals are: Pulse >100 and SBP>130 on NTG drip C. Secondary Medication Normal Saline Bolus 250 cc 500 cc 1000 cc x _____ Morphine Sulfate IVP _______ mg x 1 Morphine Sulfate IVP _______ mg may repeat x _____ Lopressor 5 mg IV q _____min x _____ Time _____/Initials _____ Heparin 3000 unit bolus Time _____/Initials _____ Heparin 4000 unit bolus Time _____/Initials _____ Heparin 5000 unit bolus Time _____/Initials _____ GIIb/IIIa Inhibitor _______ per protocol Time _____/Initials _____ D. Additional Orders Repeat EKG Right Sided EKG I-Stat Consent for “Cardiac catheterization with possible percutaneous coronary intervention” to be done by DR. ___________(Cardiologist Name). Other _________________ Emergency Physician ________________ (Signature) revised 1 -2 -08

Questions • • Does your site have 24/7 ON SITE coverage? Site meeting D 2 B goals? Mandate for time for on-call team? Who activates the team? Does EMS always give Aspirin? Does EMS fax EKG for activation of team? Is there a resource RN to help call team? Heparin w/ IIb/IIIa or Angiomax for STEMI?

Take home message: • Create a “Code Heart” STEMI Team • Educate the team & streamline your process: Every minute counts. • Involve EMS, ED, Cath lab Staff and resource staff to perfect the process. Feedback is key! • Communication and Teamwork are critical components of any successful program • Who knows where the clock will be geared soon….

No Better reason to smile than after a record breaking D 2 B during a bliizzard in D. C. ! Suburban Hosp January ‘ 11


• • References Dr. Sigmund Silber , Munich Germany www. race-er. org / Duke University WWW. ESCARDIO. ORG/GUIDELINES ACC : D 2 B Alliance http: //www. d 2 balliance. org Dr. Lowell Satler, Washington Hospital Center Dr. Tim Henry, Minneapolis Heart Brodie, B, Gersh, B et al: Analysis from the Horizons-AMI and Cadillac Trials. http: //www. emsworld. com/print/EMSWorld/Out-of-Hospital-STEMI-Alert/1$5009

Thanks for your attention
ca5d6275773c324181a3cbe02db7dc00.ppt